Long-term urinary catheter-associated urinary tract infection (UTI)
|
|
|
- Rudolf Allison
- 8 years ago
- Views:
Transcription
1 Peer reviewed article Long-term urinary catheter-associated urinary tract infection (UTI) Abstract This paper reviews the literature on the current management of symptomatic urinary tract infections (UTIs) in those with long-term urinary catheters. Long-term is defined as being in situ for more than 1 month. The discussion refers to published guidelines and relevant clinical trials. As bacteriuria is universal in people with long-term urinary catheters, diagnosis of symptomatic UTIs is made chiefly by the presence of clinical symptoms, which usually include fever. Urine culture is then performed in order to direct an appropriate antibiotic choice. Urinary catheter change at the time of initiating treatment is likely to lead to earlier clinical improvement, and a more accurate assessment of infecting organisms when a culture is taken via the new catheter. Antibiotic treatment should be for as short a time as possible, 5-7 days, to reduce the selection of resistant microorganisms. Regular catheter change and newer catheter materials have not been proven to reduce the incidence of symptomatic UTIs in those with a long-term urinary catheter in situ. Key words: urinary tract infection, urinary catheter, antibiotics, urinalysis. Introduction Urinary tract infections (UTIs) were studied extensively in the 1980s; this led to the development of evidence-based guidelines for treatment in those with normal urinary tracts 1, 2. Since that time, further areas have been elucidated by excellent trials, such as the treatment of UTIs in pregnancy and in those in long-term care facilities 2, 3, and also whether treatment of asymptomatic bacteriuria is appropriate 4, 5. Studies on the prevention of UTIs in patients with a urinary catheter have mainly addressed those with short-term urinary catheterisation (usually less than 14 days) in recent years 6. In respect to long-term urinary catheterisation, various clinical issues have been investigated such as presentation, diagnosis and treatment of symptomatic UTIs focussing on particular groups, including the institutionalised elderly and those with spinal cord lesions 7, 8. This has resulted in a number of recommendations regarding long-term urinary catheter-related UTIs, but many areas remain to be clarified by further studies 3. Dr Miriam Paul Microbiologist and Infectious Diseases Physician Douglass Hanly Moir Pathology MacQuarie Park, NSW Tel: (02) mpaul@dhm.com.au This paper was developed from the author s presentation at the Continence Foundation of Australia 12th National Conference, Manly, The author is employed part-time as a pathologist by a laboratory that performs urine cultures The purpose of this article is to present what is a current evidence-based management strategy for those with long-term catheter-associated UTIs. Literature review methodology Material for this article was identified by searches of Medline, Cochrane Reviews and references from relevant original articles published in English between 1994 and Search terms included catheter, urinary catheter, urinary tract infection, and were combined with the terms review and guidelines. Bacterial urinary tract colonisation and persistence Following insertion of a urinary catheter, bacteria spread to the bladder and establish persistence there, with subsequent intermittent invasion leading to symptomatic UTIs. A long-term urinary catheter is defined as: one that is required for more than a month; is most commonly used either to manage incontinence, particularly in women; or as an intervention for bladder outlet obstruction with retention, more commonly in men 7, 9. A normal bladder has very effective defences against transient bacteriuria, with most organisms being removed by the next urination. Unfortunately, inserting an indwelling urinary catheter bypasses many of these host defences, allowing access of organisms to the bladder. Initially, the urethra will become colonised, then organisms ascend to cause bladder colonisation 9. These colonising perineal organisms usually consist of normal bowel flora such as Enterococcus, Escherichia coli and other Gram-negative bacilli, skin flora such as coagulase-negative 4 Vol. 11, No. 1 Autumn 2005
2 Staphylococci and Candida 9. In women, colonising organisms can include normal vaginal flora such as Group B Streptococcus 9. Colonising organisms may also include hospitalassociated organisms with which the person has come in contact such as methicillin resistant Staphylococcus aureus (MRSA). Closed urinary catheter drainage systems have been successful in greatly reducing access of organisms to the bladder via the lumen of the catheter, with the result that most ascending colonisation now occurs via the external surface of the catheter 6. However, with closed drainage systems, detaching the collection tube from the catheter can allow organisms entry into the system, as can contamination of the emptying tube of the bag with a dirty container 6. In all urinary catheterisation, the catheter balloon prevents complete emptying of the bladder, causing a small volume of residual urine to accumulate, thus providing a suitable medium for persistence and multiplication of organisms once they have entered the urinary bladder. The development of persistent bacteriuria occurs at a rate of 3-10% per day following urinary catheterisation, with all urinary catheters becoming colonised after 1 month in situ 7. This persistence of bacteria in the urine of catheterised patients is termed asymptomatic bacteriuria or more correctly asymptomatic UTIs, as there is evidence of a host response involved implying a degree of tissue invasion rather than mere surface colonisation 3. Organism factors also facilitate bacterial persistence in the bladder, most notably those properties that promote their adherence to the bladder uroepithelial lining and catheter surface. A biofilm forms on the surface of the catheter, consisting of glycocalyx slime and minerals 10. This biofilm facilitates bacterial attachment and provides protection from normal host defences. In particular, there is a blunting of the host antibody and neutrophil response which might normally eradicate bacteria. Bacterial persistence occurs initially in the bladder but may extend to the kidneys, with biofilm being formed in the renal pelvis or tubules 7. Chronic renal inflammation has commonly been found at autopsy of those with long-term urinary catheters, but actual chronic pyelonephritis with scarring is much less frequent, occurring mainly in people with renal stones 7, 9. Long-term catheters are usually colonised by two to five different organisms 7. These organisms are replaced by other organisms regularly, and can change as frequently as every 2 weeks 7. Some organisms are more persistent as they adhere better to the uroepithelium, particularly E. coli and Providencia stuartii 7. Over time, more antibiotic-resistant organisms may be selected, particularly by the use of multiple antibiotic treatment courses. Prevention of symptomatic UTIs in catheterised persons Various measures have been suggested to prevent the development of urinary catheter-associated bacteriuria but, apart from the closed drainage system, to date, none have been proven to be effective. Periurethral topical antibiotics have not been shown to prevent the development of urinary catheter bacteriuria 11. Prophylactic antibiotics have been found to delay the development of bacteriuria in short-term catheterised patients, but eventually resistant organisms colonise the urinary catheter 9. In the long-term catheterised patient, urine sterility cannot be maintained with antibiotics 9. Routine urinary catheter change has not yet been proven, in any study, to reduce the incidence of UTIs in people with long-term urinary catheters 7. While published recommendations for the timing of urinary catheter change are few, it is reasonable that catheters not associated with complications be left in place for 12 weeks 8. Antibiotic prophylaxis at the time of urinary catheter change is not recommended as, despite a 4-10% incidence of transient bacteraemia associated with the procedure, symptomatic infection is uncommon 12. Routine catheter irrigation with antimicrobial agents has been shown to be ineffective in preventing UTIs 8. Suprapubic catheterisation, compared to urethral catheterisation, has been suggested as an alternative, as the abdominal skin carries less of a bacterial load than the periurethral area. However, this option has not been well studied in terms of UTI incidence in a long-term catheterised group and no conclusions can be drawn 13, 14. In an attempt to reduce bacterial adhesion, materials such as Teflon and silicon have been used in catheter construction, but no reduction in UTI incidence has been shown 9. In individual patients, however, more frequent routine catheter change and a silicon catheter may reduce urinary catheter blockage if this is the cause of their recurrent UTIs. Antimicrobial impregnated or silver-coated urinary catheters have had variable success in preventing UTIs in those catheterised for less than 14 days, with silver alloy coated catheters particularly showing some promise 15. There is insufficient evidence to comment on the use of these urinary catheters in long-term catheterised patients, but there is some concern regarding silver toxicity from prolonged use 6, 8. Future options for reducing symptomatic UTIs lie particularly in the development of alternatives to permanent indwelling catheters, such as urethral stents and condom drainage for males. Intermittent catheterisation is thought to be associated with a lower rate of symptomatic UTIs, although no definitive study has been performed 8. Vaccines against the common UTI Vol. 11, No. 1 Autumn
3 pathogens such as E. coli are being developed but, while these are very promising in people with normal urinary tracts, it remains to be seen whether they will be effective when there is a urinary catheter in situ 11. Symptomatic UTIs in the long-term catheterised Progression from an asymptomatic infection to symptomatic UTIs can be related to a number of factors. Catheter obstruction is the most common cause of symptomatic UTIs, with fever eight times more common in those with obstruction than with a patent urinary catheter 7. Obstruction leads to increased residual urine in the bladder in which colonising organisms multiply. Obstruction is often caused by a combination of precipitated crystals, biofilm, Tamm-Horsfall protein (antibacterial mucus normally made in the kidneys) and bacteria 9. Of particular note, urinary colonisation with Proteus species may lead to obstructive problems as the organism produces the enzyme urease 9. This catalysis of the breakdown of urea into ammonia and the subsequent alkaline urine allows the development of a precipitate of struvite and apatite crystals. A similar process may cause kidney and bladder stones. Obstruction does not necessarily lead to UTIs if the catheter is changed as soon as obstruction occurs 3. Catheter trauma also contributes to the development of symptomatic UTIs by causing mechanical uro-epithelial damage, facilitating invasion of organisms into deeper tissue 14. Clinical presentation Symptomatic UTIs in catheterised patients may be overdiagnosed, with non-specific signs such as delirium in an elderly mistakenly attributed to infection from a urinary source 16, 17. Purely lower UTI symptoms such as dysuria are uncommon and periurethral infection as a cause of these symptoms, particularly in men, should be excluded by examining the urethral meatus for discharge and checking for epididymitis or prostatitis 7. Bladder spasms may cause symptoms if the catheter is blocked but this cause should be obvious on examination. Symptoms of UTIs such as gross haematuria or loin pain consistent with pyelonephritis, or persistent fever with no other obvious source, correlate with acute symptomatic urinary infection 7, 9. In patients with a long-term urinary catheter, fever occurs at a rate of fevers per 100 days of catheterisation 7. However, the majority of these fevers only last 1 day and settle without treatment, leaving approximately 30% of fevers with no obvious source that are actually due to symptomatic UTIs 7. Elevated peripheral blood white cell count and, in some patients, positive blood cultures, also support the diagnosis of symptomatic UTIs compared to asymptomatic bacteriuria 16. Of note, the risk of death is 60 times higher in febrile catheterised patients with UTIs than in those who are afebrile 9. Laboratory findings When a clinical diagnosis of symptomatic UTIs has been made, urine microscopy and culture provides useful information to direct appropriate antibiotic therapy. Examination of urine in patients with a urinary catheter frequently shows pyuria due to mechanical irritation so the presence of white cells is unhelpful in diagnosing symptomatic UTIs 18. However, conversely the absence of white cells on urinalysis or microscopy has excellent negative predictive value and is useful as evidence against UTIs, suggesting than an alternative source of the patient s current symptoms should be sought 3. Diagnosis of UTIs cannot be based purely upon culture as almost all catheter urine specimens will grow organisms. When obtaining a specimen of urine for diagnostic purposes, it is important to realise that a urine sample taken from a urinary catheter reflects organisms present in the biofilm on the catheter, and not solely the organisms that are actually present in the bladder. A greater variety of organisms plus higher numbers of these organisms will be isolated from the colonised catheter compared to a sample taken from the bladder when a new catheter is inserted 7. Thus catheter culture samples are not necessarily representative of the actual organism causing an episode of symptomatic UTIs. Preferably a urine sample should be taken from a newly inserted urinary catheter at the time of symptomatic UTI diagnosis to determine what organisms are present in the bladder. Treatment Ideally the urinary catheter should be changed every time a symptomatic UTI is diagnosed and treated. The disadvantages of changing the urinary catheter are a 4-10% rate of transient, usually asymptomatic bacteraemia associated with the procedure, plus potential mechanical trauma involved and financial costs 9. A study of aged nursing home patients looking at catheter replacement prior to starting treatment of symptomatic UTIs found that inserting a new urinary catheter in addition to treating with antibiotics led to clinical improvement after 3 days in 93% versus 41% of patients without catheter change, although all had a similar clinical outcome eventually 19. There was also a lower rate of symptomatic relapse 4 weeks after treatment cessation in those who had urinary catheter replacement 20. This has led to a recommendation for replacement when the catheter has been in situ for more than 7 days 7. If the catheter is not being replaced, a sample of urine should be aspirated from the catheter port. 6 Vol. 11, No. 1 Autumn 2005
4 Antibiotic treatment of UTIs in people who have a urinary catheter in situ in the long-term is aimed at symptom relief rather than eradication of bacteriuria and thus should be for as short a time as possible, usually 5-7 days 3. This is because a longer antibiotic course will still not sterilise the urine for any prolonged time and may lead to bacteriuria with more resistant microorganisms. In mildly symptomatic patients with only a low-grade fever, it is appropriate to wait for urine culture results to enable an appropriate antibiotic to be chosen. Once susceptibilities are available, a suitable oral antibiotic can be prescribed from trimethoprim 300mg daily, cephalexin 500mg twice daily, amoxicillin plus clavulanate 500/125mg twice daily or nitrofurantoin 50mg four times a day 2. Empiric antibiotics should be started immediately in those with severe symptoms such as rigors or hypotension; for these people, a broadspectrum antibiotic should be chosen to cover a wide range of potential infecting organisms such as ciprofloxacin (not recommended for children) or intravenous gentamicin 5mg/kg/day as a single daily dose plus ampicillin 1g 6-hourly 2. For severely unwell patients in whom gentamicin is contraindicated, ceftriaxone 1g daily intravenously or intramuscularly may be used, but this has no activity against Pseudomonas 2. On occasion when the patient is known from past urine cultures to be persistently colonised with a microorganism that is resistant to the latter antibiotics, the empiric initial antibiotic used should be one that the organism is known to be susceptible to. There is no evidence that increased hydration improves further on the clinical response to antibiotic treatment for uncomplicated UTIs and it is not recommended 20. Forcing fluids has the theoretical disadvantage of causing increased vesico-ureteric reflux, and dilution of antibiotic and natural antibacterial substances in the urinary tract. It also leads to decreased acidification of the urine, which lessens the activity of some antibiotics 20. Urinary acidification with oral agents is rarely necessary in the treatment of UTI and is difficult to achieve as it requires dietary modification as well as the administration of agents such as ascorbic acid or methionine. These compounds may precipitate in the urine and cause urate or oxalate stones to form, or cause acidosis in patients with renal impairment 20. Urine ph alters the activity of some antibiotics, with nitrofurantoin more active in acid urine and aminoglycosides more active in alkaline urine; the effectiveness of these agents is adequate with normal urine ph 20. If infection symptoms fail to settle and the urinary catheter is not blocked, then investigation for stones in the kidneys or bladder should be performed. For men with relapsing infection with the same organism, a 4 week antibiotic course of treatment should be considered for possible occult prostatitis. Options include ciprofloxacin and trimethoprim as few antibiotics penetrate the prostate well 2. Urine culture following resolution of UTI symptoms and cessation of antibiotic is not recommended in patients with a long-term urinary catheter as it is likely to still show bacteriuria and does not influence further management 3. Conclusion UTIs are a common cause of morbidity in people with a longterm urinary catheter in situ. No measures, apart from the closed drainage system, have yet been proven to be effective in preventing UTIs in this group of patients. Diagnosis of UTIs should be based on symptoms, particularly fever. Urinary catheter change is recommended prior to starting treatment of symptomatic UTIs as symptoms resolve more rapidly and there is a lower rate of symptom recurrence in the following 4 weeks. A urine sample should be taken from the new catheter for culture and subsequent antibiotic treatment directed by the result. Antibiotic treatment should be given for 5-7 days to reduce the risk of acquisition of resistant microorganisms colonising the urinary tract. Further clinical trials of preventive measures regarding UTI in long-term catheterised persons are required to assist in formulating management strategies. References 1. Warren JW, Abrutyn E, Hebel JR et al. Guidelines for antimicrobial treatment of uncomplicated acute bacterial cystitis and acute pyelonephritis in women. Clin Infect Dis 1999; 29: Therapeutic Guidelines: Antibiotic. Version 12. Therapeutic Guidelines Ltd, Victoria, Australia, Nicolle LE. SHEA Long-Term Care Committee. Urinary tract infections in long-term care facilities. Infect Control Hosp Epidemiol 2001; 22(3): Harding GK, Zhanel GG, Nicolle LE & Cheang M Manitoba Diabetes Urinary Tract Infection Study Group. Antimicrobial treatment in diabetic women with asymptomatic bacteriuria. N Engl J Med 2002; 347(20): Nicolle LE. Asymptomatic bacteriuria: when to screen and when to treat. Infect Dis Clin North Am 2003; 17(2): Tambyah PA. Catheter-associated urinary tract infections: diagnosis and prophylaxis. Int J Antimicrob Agents 2004; 24 Suppl 1:S Nicolle LE. The chronic indwelling catheter and urinary infection in long-term-care facility residents. Infect Control Hosp Epidemiol 2001; 22(5): Biering-Sorensen F. Urinary tract infection in individuals with spinal cord lesion. Curr Opin Urol 2002; 12(1): Warren JW. Catheter-associated urinary tract infections. Infect Dis Clin North Am 1997; 11(3): Elves AW & Feneley RC. Long-term urethral catheterization and the urine-biomaterial interface. Br J Urol 1997; 80(1): Maki DG & Tambyah PA. Engineering out the risk for infection 8 Vol. 11, No. 1 Autumn 2005
5 with urinary catheters. Emerg Infect Dis 2001; 7(2): Bregenzer T, Frei R, Widmer AF et al. Low risk of bacteremia during catheter replacement in patients with long-term urinary catheters. Arch Intern Med 1997; 157(5): Jamison J, Maguire S & McCann J. Catheter policies for management of long term voiding problems in adults with neurogenic bladder disorders. The Cochrane Database of Systematic Reviews 2004, Issue 2, Art. No: CD DOI: / CD pub2. wiley.com/cochrane/clsysrev/articles/cd004375/toc.html Accessed 10 November Warren JW. Nosocomial urinary tract infections. In: Mandell, Douglas & Bennnett. Principles and Practice of Infectious Diseases (6th ed). Philadelphia, PA: Elsevier Churchill Livingstone, 2005, p Brosnahan J, Jull A & Tracy C. Types of urethral catheters for management of short-term voiding problems in hospitalised adults. The Cochrane Database of Systematic Reviews 2004, Issue 1, Art. No.: CD DOI: / CD pub2. CD004997/toc.html Accessed 10 November Bentley DW, Bradley S, High K et al. Practice guideline for evaluation of fever and infection in long-term care facilities. Clin Infect Dis 2000; 31(3): Orr PH, Nicolle LE, Duckworth H et al. Febrile urinary infection in the institutionalized elderly. Am J Med 1996; 100(1): Tambyah PA & Maki DG. The relationship between pyuria and infection in patients with indwelling urinary catheters: a prospective study of 761 patients. Arch Intern Med 2000; 160(5): Raz R, Schiller D & Nicolle LE. Chronic indwelling catheter replacement before antimicrobial therapy for symptomatic urinary tract infection. J Urol 2000; 164(4): Sobel JD & Kaye D. Urinary tract infection. In Mandell, Douglas & Bennnett. Principles and Practice of Infectious Diseases (6th ed). Philadelphia, PA: Elsevier Churchill Livingstone, 2005, p Peer review panel Experts from the various disciplines involved in continence treatment, management and promotion and also persons who are expert in research methods and statistical analysis are invited to nominate to join the Journal s Peer Review Panel. The introduction of the Peer Review Process during 2004 augers an exciting new era for the Journal and is aimed to increase the calibre of academic and research papers published and to raise the standing of the Journal. The Journal is proud to promote Australian and New Zealand scholarship. For details regarding the Peer Review Panel please contact: Jacinta Miller jacmil@bigpond.com THE NATIONAL CONTINENCE HELPLINE A team of continence consultants providing free and confidential advice about bladder and bowel control problems, plus local referrals, free brochures and product information. A free service for everyone, including all clinicians interested in continence > Supplementary information about incontinence for GPs, physiotherapists, pharmacists and allied health professionals > Free brochures and posters available in quantity as client resources ask for a sample range with the Helpline Order Form National Continence Helpline FREECALL Monday to Friday The Helpline is funded under the Australian Government s National Continence Management Strategy and managed by the Continence Foundation of Australia utility 1115 Vol. 11, No. 1 Autumn
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
PATIENT CARE MANUAL PROCEDURE
 PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
Catheter-Associated Urinary Tract Infections Lauren Tew, Bard Ltd, UK A Webber Training Teleclass Catheter-Associated Urinary Tract Infection
 Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
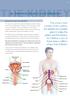 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
UTI in children. Quick reference guide. Issue date: August 2007. Urinary tract infection in children: diagnosis, treatment and long-term management
 Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Appropriate Urinary Catheter Use and Management
 Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Nosocomial Bloodstream infection. Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
 Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Preventing Catheter Blockages: A Guide for Health Professionals
 Introduction Preventing Catheter Blockages: A Guide for Health Professionals and Long term catheterisation is common for someone with a spinal cord injury (SCI). However, it poses a concern as this method
Introduction Preventing Catheter Blockages: A Guide for Health Professionals and Long term catheterisation is common for someone with a spinal cord injury (SCI). However, it poses a concern as this method
A Summary of the Guideline for the Diagnosis and Management of. Urinary Tract Infections in Long Term Care
 A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
Catheter Associated Urinary Tract Infection (CAUTI) Prevention. System CAUTI Prevention Team
 Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Understanding and Preventing Bladder Infections in Women
 Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Catheter Care. What you need to know. Jacinta Stewart Continence Nurse
 Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
Guideline for Preventing Catheter- Associated Urinary Tract Infections
 Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Catheter-associated Urinary Tract Infection (CAUTI) Toolkit
 Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
SECTION 12.1 URINARY CATHETERS
 SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters
 Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
Nosocomial Urinary Tract Infection
 Nosocomial Urinary Tract Infection Michael F. Ksycki, DO, Nicholas Namias, MD, MBA* KEYWORDS Nosocomial infection Urinary tract infection Urinary catheter Nosocomial urinary tract infection is a major
Nosocomial Urinary Tract Infection Michael F. Ksycki, DO, Nicholas Namias, MD, MBA* KEYWORDS Nosocomial infection Urinary tract infection Urinary catheter Nosocomial urinary tract infection is a major
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
Management of Urinary Tract Infections in Patients with Urinary Catheters
 Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
URINARY TRACT INFECTIONS IN YOUNG WOMEN
 URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: julkaisutilaukset@yths.fi Author:
URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: julkaisutilaukset@yths.fi Author:
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
Kaiser Oakland Urology
 Kaiser Oakland Urology The Main Purpose of Bladder Catheterization Complete Bladder Emptying! Help maintain a healthy bladder Help maintain healthy kidneys Reduce the chances of significant urinary tract
Kaiser Oakland Urology The Main Purpose of Bladder Catheterization Complete Bladder Emptying! Help maintain a healthy bladder Help maintain healthy kidneys Reduce the chances of significant urinary tract
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care
 Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization
 Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization H.J. Mulder MANP 1-11-2011 Henk-Jan Mulder MANP Department of Urology Martini General Hospital Van Swietenplein 1 9700
Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization H.J. Mulder MANP 1-11-2011 Henk-Jan Mulder MANP Department of Urology Martini General Hospital Van Swietenplein 1 9700
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Urinary Tract Infections
 Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
How To Find Out If A Diabetic Woman Has A Urinary Tract Infection
 Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS
 Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
Pyelonephritis: Kidney Infection
 Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Patient with: 3 or more UTI in 6 months 4 or more UTI in 12 months
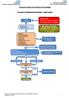 Recurrent UTI Management Pathway adult females Initial assessment Assessment questionnaire questionnaire bladder scan dipstick dipstick of of urine urine pregnancy neurological disease long - term catheters
Recurrent UTI Management Pathway adult females Initial assessment Assessment questionnaire questionnaire bladder scan dipstick dipstick of of urine urine pregnancy neurological disease long - term catheters
Don t Go With The Flow! Control and Management of UTIs in the Elderly
 Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
Beryl Navti SEPT Pharmacy Department. 24/06/2013 Beryl Navti, Clinical Pharmacist, SEPT
 URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study. Medical Student Research Project.
 Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study Medical Student Research Project Jordan Knepper Faculty advisor: Mark Langsfeld, MD Introduction Background
Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study Medical Student Research Project Jordan Knepper Faculty advisor: Mark Langsfeld, MD Introduction Background
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Catheter-Associated Urinary Tract Infection (CAUTI) Definitions and Reporting
 AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
Urinary Tract Infections. Clinical Scenario #1. Urinary Tract Infections. Clinical Scenario #1 : Labs
 Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Catheter Management. Justine Andrew Urology Nurse Specialist
 Catheter Management Justine Andrew Urology Nurse Specialist catheterisation to let or send down History of the catheter belongs to urology At the end of the 19 th C, patients carried catheters in the shafts
Catheter Management Justine Andrew Urology Nurse Specialist catheterisation to let or send down History of the catheter belongs to urology At the end of the 19 th C, patients carried catheters in the shafts
Managing the E coli UTI
 C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Welcome and Instructions
 Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
What s new? INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS. The Revised Guidance Includes: Interpretive Guidelines
 INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS The Revised Guidance Includes: Interpretive Guidelines Investigative Protocols Compliance & Severity Guidance What s new? The new guidance for
INVESTIGATIVE PROTOCOL FOR URINARY INCONTINENCE & CATHETERS The Revised Guidance Includes: Interpretive Guidelines Investigative Protocols Compliance & Severity Guidance What s new? The new guidance for
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Feline Lower Urinary Tract Disease (FLUTD)
 Feline Lower Urinary Tract Disease (FLUTD) VETERINARY GUIDE 2 What is FLUTD? FLUTD describes a collection of common conditions that affect the bladder and/or urethra the narrow tube that carries urine
Feline Lower Urinary Tract Disease (FLUTD) VETERINARY GUIDE 2 What is FLUTD? FLUTD describes a collection of common conditions that affect the bladder and/or urethra the narrow tube that carries urine
Urinary Tract Infections
 Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Age in years Females (% prevalence) Males (% prevalence) 6-15 Vesicoureteral reflux (4.4%) Vesicoureteral reflux (0.5%)
 Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Childhood Urinary Tract Infections
 Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER PROBLEMS
 PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One Outlines the process for staff
PROCEDURE FOR ADMINISTERING CATHETER MAINTENANCE SOLUTION AND RESOLVING CATHETER First Issued Issue Version Purpose of Issue/Description of Change Planned Review Date One Outlines the process for staff
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
URINARY TRACT INFECTION IN CHILDREN. Yap Hui Kim, Belinda Murugasu
 URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
Self Catheterization Guide
 Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
PATIENT URINARY CATHETER PASSPORT
 n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
Bard: Intermittent Catheters. A guide to. Bard: Pelvic Organ Prolapse. An REIMBURSEMENT. overview of OF INTERMITTENT. Prolapse CATHETERS
 Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
URINARY TRACT INFECTIONS
 URINARY TRACT INFECTIONS INTRODUCTION Urinary tract infections are a very common medical problem. The term urinary tract infection is frequently used to refer to an infection of the bladder. However, although
URINARY TRACT INFECTIONS INTRODUCTION Urinary tract infections are a very common medical problem. The term urinary tract infection is frequently used to refer to an infection of the bladder. However, although
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Male Urinary Catheterisation & Catheter Care
 Male Urinary Catheterisation & Catheter Care Mark Jones, Martin Steggall & Marsh Gelbart City University, London. Good practice Consent gain informed consent. Who can catheterise any Registered Nurse who
Male Urinary Catheterisation & Catheter Care Mark Jones, Martin Steggall & Marsh Gelbart City University, London. Good practice Consent gain informed consent. Who can catheterise any Registered Nurse who
Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections
 Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections Reprinted 2004 Scope The purpose of this protocol is to avoid unnecessary testing in routine cases while
Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections Reprinted 2004 Scope The purpose of this protocol is to avoid unnecessary testing in routine cases while
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
Feline Cystitis (Feline Lower Urinary Tract Disease)
 Feline Cystitis (Feline Lower Urinary Tract Disease) The term "cystitis" literally means inflammation of the urinary bladder. Although this term is rather general, there is a common form of cystitis that
Feline Cystitis (Feline Lower Urinary Tract Disease) The term "cystitis" literally means inflammation of the urinary bladder. Although this term is rather general, there is a common form of cystitis that
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES
 & CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES Amela Dedeić-Ljubović*, Mirsada Hukić Institute of Clinical Microbiology, Clinical Centre of the University of
& CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES Amela Dedeić-Ljubović*, Mirsada Hukić Institute of Clinical Microbiology, Clinical Centre of the University of
Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance
 Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance Antibiotic resistance is an increasing concern for everyone. This module: Defines antibiotic
Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance Antibiotic resistance is an increasing concern for everyone. This module: Defines antibiotic
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
associated Urinary Tract Infection Case Definitions
 CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D.
 ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
Location: Clinical Practice Manual
 Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Are venous catheters safe in terms of blood tream infection? What should I know?
 Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
SARI. Guidelines for the Prevention of Catheterassociated Urinary Tract Infection
 Guidelines for the Prevention of Catheterassociated Urinary Tract Infection Published on behalf of SARI by HSE Health Protection Surveillance Centre 2011 SARI A Strategy for the Control of Antimicrobial
Guidelines for the Prevention of Catheterassociated Urinary Tract Infection Published on behalf of SARI by HSE Health Protection Surveillance Centre 2011 SARI A Strategy for the Control of Antimicrobial
190.12 - Urine Culture, Bacterial Summary Information Highlighted items indicate most frequently used codes.
 Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW
 PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
PROCEDURE FOR CATHETER AFTERCARE
 PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
PROCEDURE FOR CATHETER AFTERCARE First Issued May 2010 Issue Version Two Purpose of Issue/Description of Change To promote safe and effective emptying of urinary drainage bags, closed drainage systems
Indwelling urinary catheter. Information for patients and carers. RDaSH. Doncaster Community Integrated Services
 Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
Indwelling urinary catheter Information for patients and carers RDaSH Doncaster Community Integrated Services What is a catheter? A catheter is a hollow flexible tube designed to drain urine from the bladder.
2015 RN.ORG, S.A., RN.ORG, LLC
 Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed
 Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Patient Information:
 Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
Patient Information: Care of an indwelling Urinary Catheter What is a Urinary Catheter? A catheter is a hollow, flexible tube designed to drain urine from the bladder. Following insertion into the bladder,
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care
 COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
Bowel and Bladder Dysfunction in MS. Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center. Bladder Dysfunction
 Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth
 CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline RECOMMENDATIONS 1 Conditional: Clinicians who are making
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
Long-term result of Memokath urethral sphincter stent in. spinal cord injury patients
 1 Long-term result of Memokath urethral sphincter stent in spinal cord injury patients Subramanian Vaidyanathan 1 E-mail: vaidyanathansiu@hotmail.com Bakul M Soni 1 E-mail: Bakul.Soni@mail.soh-tr.nwest.nhs.uk
1 Long-term result of Memokath urethral sphincter stent in spinal cord injury patients Subramanian Vaidyanathan 1 E-mail: vaidyanathansiu@hotmail.com Bakul M Soni 1 E-mail: Bakul.Soni@mail.soh-tr.nwest.nhs.uk
Managing your bladder with a suprapubic catheter at home
 Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
Managing your bladder with a suprapubic catheter at home Gateshead Primary Care Trust South Tyneside Primary Care Trust Sunderland Teaching Primary Care Trust What is a suprapubic catheter? A suprapubic
Care of the Catheterised Patient and Urinalysis
 Care of the Catheterised Patient and Urinalysis Male Pelvic Anatomy Female Pelvic Anatomy What does a urinary catheter do? Urinary Catheters Urinary Catheters Urinary Catheters Why do patients have catheters?
Care of the Catheterised Patient and Urinalysis Male Pelvic Anatomy Female Pelvic Anatomy What does a urinary catheter do? Urinary Catheters Urinary Catheters Urinary Catheters Why do patients have catheters?
Infection Prevention & Control Team. Your urinary catheter & how to care for it 0151 430 2452 / 0151 430 1384. Patient Information Leaflet
 Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
Contact details Infection prevention team - 0151 430 2452 This leaflet can be made available in alternative languages/formats on request. Infection Prevention & Control Team 0151 430 2452 / 0151 430 1384
