Catheter-Associated Urinary Tract Infection (CAUTI) Event
|
|
|
- Shannon Riley
- 8 years ago
- Views:
Transcription
1 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only to SSIs. UTIs account for more than 15% of infections reported by acute care hospitals 1. Virtually all healthcare-associated UTIs are caused by instrumentation of the urinary tract. can lead to such complications as cystitis, pyelonephritis, gram-negative bacteremia, prostatitis, epididymitis, orchitis in males, less commonly, endocarditis, vertebral osteomyelitis, septic arthritis, endophthalmitis, meningitis in all patients. Complications associated with cause discomfort to the patient, prolonged hospital stay, increased cost mortality 2. Each year, more than 13,000 deaths are associated with UTIs. 3 Prevention of s is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4. Settings: Surveillance will occur in any inpatient locations where denominator data can be collected, which may include critical intensive care units (ICU), specialty care areas (SCA), step down units, long term care wards. Neonatal ICUs may participate, but only off plan (not as a part of their monthly reporting plan). A complete listing of inpatient locations instructions for mapping can be found in CDC Locations Descriptions chapter. NOTE: It is not required to monitor for s after the patient is discharged from the facility. However, if discovered, any occurring on the day of discharge or the next day should be reported to NHSN; day of discharge is considered Day 1. No additional indwelling catheter days are reported. Requirements: Surveillance for HAI is performed in at least one inpatient location in the healthcare institution for at least one calendar month as indicated in the Patient Safety Monthly Reporting Plan (CDC ). Definitions: Healthcare-associated infections (HAI): An infection is considered an HAI if all elements of a CDC/NHSN site-specific infection criterion were first present together on or after the 3 rd hospital day (day of hospital admission is day 1). For an HAI, an element of the infection criterion may be present during the first 2 hospital days as long as it is also present on or after day 3. All elements used to meet the infection criterion must occur within a timeframe that does not exceed a gap of 1 calendar day between elements. January
2 Urinary tract infections (UTI) are defined using symptomatic urinary tract infection (SUTI) criteria or Asymptomatic Bacteremic UTI (ABUTI) criteria (Table 1 Figures 1-5). Date of event: For a UTI the date of event is the date when the last element used to meet the UTI infection criterion occurred. Synonyms: infection date, date of infection. Indwelling catheter: A drainage tube that is inserted into the urinary bladder through the urethra is left in place, is connected to a drainage bag (including leg bags), also called a Foley catheter. This does not include suprapubic, condom, or straight in--out catheters. This definition includes indwelling urethral catheters that are used for intermittent or continuous irrigation. Catheter-associated UTI (): A UTI where an indwelling urinary catheter was in place for >2 calendar days when all elements of the UTI infection criterion were first present together, with day of device placement being Day 1, an indwelling urinary catheter was in place on the date of event or the day before. EXAMPLE: A patient has a Foley catheter inserted on an inpatient unit the following morning the patient meets criteria for a UTI. Because the catheter has not been in place >2 calendar days when all elements of the infection criterion were first present together, this is not a. NOTE: 1. SUTI 1b 2b other UTI (OUTI), as defined in the HAI Definitions chapter cannot be catheter-associated. Location of attribution: The inpatient location where the patient was assigned on the date of the UTI event, which is further defined as the date when the last element used to meet the UTI criterion occurred (see exception below). EXCEPTION TO LOCATION OF ATTRIBUTION: Transfer Rule: If all elements of a are present within 2 calendar days of transfer from one inpatient location to another in the same facility or a new facility (i.e., on the day of transfer or the next day), the infection is attributed to the transferring location or facility. Receiving facilities should share information about such HAIs with the transferring facility to enable reporting. This is called the Transfer Rule examples are shown below: Patient with a Foley catheter in place in the SICU is transferred to the surgical ward. On the next day, all elements for UTI are first present together. This is reported to NHSN as a for the SICU. Patient is transferred in the morning to the medical ward from the MSICU after having the Foley catheter removed. Later that night, all elements for a UTI are first present together. This is reported to NHSN as a for the MSICU. January
3 On Monday, patient with a Foley catheter in place is transferred from the medical ward to the coronary care ICU (CCU). Wednesday in the CCU, all elements for UTI are first present together. This is reported to NHSN as a for the CCU, as the UTI event date is on the 3 rd calendar day after transfer. Patient on the urology ward of Hospital A had the Foley catheter removed after it had been in place for 5 days is discharged home a few hours later. The IP from Hospital B calls the next day to report that this patient has been admitted to Hospital B with a UTI. This should be reported to NHSN for Hospital A attributed to the urology ward. EXCEPTION TO TRANSFER RULE: Locations which do not house patients overnight (e.g., Emergency Department or Operating Room) will have no denominator data, i.e., patient days or catheter days. Therefore, s cannot be attributed to these locations. Instead, the must be attributed to the next inpatient location in which the patient stays. January
4 Table 1. Urinary Tract Infection Criteria Criterion 1a 1b Urinary Tract Infection (UTI) Symptomatic UTI (SUTI) Must meet at least 1 of the following criteria: Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. at least 1 of the following signs or symptoms: fever (>38 C); suprapubic tenderness*; costovertebral angle pain or tenderness* a positive urine culture of 10 5 colony-forming units (CFU)/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below) OR Patient had an indwelling urinary catheter in place for >2 calendar days had it removed the day of or the day before all elements of this criterion were first present together at least 1 of the following signs or symptoms: fever (>38 C); urgency*; frequency*; dysuria*; suprapubic tenderness*; costovertebral angle pain or tenderness* a positive urine culture of 10 5 colony-forming units (CFU)/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). Patient did not have an indwelling urinary catheter in place at the time of or the day before all elements of this criterion were first present together has at least 1 of the following signs or symptoms: fever (>38 C) in a patient that is 65 years of age; urgency*; frequency*; dysuria*; suprapubic tenderness*; costovertebral angle pain or tenderness* a positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). January
5 Criterion 2a Urinary Tract Infection (UTI) Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together at least 1 of the following signs or symptoms: fever (>38 C); suprapubic tenderness*; costovertebral angle pain or tenderness* at least 1 of the following findings: a. positive dipstick for leukocyte esterase /or nitrite b. pyuria (urine specimen with 10 white blood cells [WBC]/mm 3 of unspun urine or >5 WBC/high power field of spun urine) c. microorganisms seen on Gram s stain of unspun urine a positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below) OR Patient with an indwelling urinary catheter in place for > 2 calendar days had it removed the day of or the day before all elements of this criterion were first present together at least 1 of the following signs or symptoms: fever (>38 C); urgency*; frequency*; dysuria*; suprapubic tenderness*; costovertebral angle pain or tenderness* at least 1 of the following findings: a. positive dipstick for leukocyte esterase /or nitrite b. pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine c. microorganisms seen on Gram s stain of unspun urine a positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). January
6 Criterion 2b Urinary Tract Infection (UTI) Patient did not have an indwelling urinary catheter in place at the time of, or the day before all elements of this criterion were first present together has at least 1 of the following signs or symptoms: fever (>38 C) in a patient that is 65 years of age; urgency*; frequency*; dysuria*; suprapubic tenderness*; costovertebral angle pain or tenderness* at least 1 of the following findings: a. positive dipstick for leukocyte esterase /or nitrite b. pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine c. microorganisms seen on Gram s stain of unspun urine a positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). 3 Patient 1 year of age with** or without an indwelling urinary catheter has at least 1 of the following signs or symptoms: fever (>38 C core); hypothermia (<36 C core); apnea*; bradycardia*; dysuria*; lethargy*; vomiting* a positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). ** Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. 4 Patient 1 year of age with** or without an indwelling urinary catheter has at least 1 of the following signs or symptoms: fever (>38 C core); hypothermia (<36 C core); apnea*; bradycardia*; dysuria*; lethargy*; vomiting* at least 1 of the following findings: a. positive dipstick for leukocyte esterase /or nitrite b. pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine c. microorganisms seen on Gram s stain of unspun urine a positive urine culture of between 10 3 <10 5 CFU/ml with no more than two species of microorganisms. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section January
7 Criterion Urinary Tract Infection (UTI) below). ** Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. January
8 Criterion Asymptomatic Bacteremic Urinary Tract Infection (ABUTI) Patient with* or without an indwelling urinary catheter has no signs or symptoms (i.e., for any age patient, no fever (>38 C); urgency; frequency; dysuria; suprapubic tenderness; costovertebral angle pain or tenderness OR for a patient 1 year of age; no fever (>38 C core); hypothermia (<36 C core); apnea; bradycardia; dysuria; lethargy; or vomiting) a positive urine culture of 10 5 CFU/ml with no more than 2 species of uropathogen microorganisms** (see Comments section below) a positive blood culture with at least 1 matching uropathogen microorganism to the urine culture, or at least 2 matching blood cultures drawn on separate occasions if the matching pathogen is a common skin commensal. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day (see Comments section below). *Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. **Uropathogen microorganisms are: Gram-negative bacilli, Staphylococcus spp., yeasts, beta-hemolytic Streptococcus spp., Enterococcus spp., G. vaginalis, Aerococcus urinae, Corynebacterium (urease positive) +. + Report Corynebacterium (urease positive) as either Corynebacterium species unspecified (COS) or as C. urealyticum (CORUR) if so speciated. (See complete list of uropathogen microorganisms at Comments Laboratory cultures reported as mixed flora represent at least 2 species of organisms. Therefore an additional organism recovered from the same culture, would represent >2 species of microorganisms. Such a specimen cannot be used to meet the UTI criteria. Urinary catheter tips should not be cultured are not acceptable for the diagnosis of a urinary tract infection. Urine cultures must be obtained using appropriate technique, such as clean catch collection or catheterization. Specimens from indwelling catheters should be aspirated through the disinfected sampling ports. In infants, urine cultures should be obtained by bladder catheterization or suprapubic aspiration; positive urine cultures from bag specimens are unreliable should be confirmed by specimens aseptically obtained by catheterization or suprapubic aspiration. Urine specimens for culture should be processed as soon as possible, preferably within 1 to 2 hours. If urine specimens cannot be processed within 30 minutes of collection, they should be refrigerated, or inoculated into primary isolation medium before transport, or transported in an appropriate January
9 urine preservative. Refrigerated specimens should be cultured within 24 hours. Urine specimen labels should indicate whether or not the patient is symptomatic. Report secondary bloodstream infection = Yes for all cases of Asymptomatic Bacteremic Urinary Tract Infection (ABUTI). Report only pathogens in both blood urine specimens for ABUTI. Report Corynebacterium (urease positive) as either Corynebacterium species unspecified (COS) or as C. urealyticum (CORUR) if speciated. January
10 Laboratory Evidence Signs Symptoms Device-associated Module Figure 1: Identification Categorization of SUTI with Indwelling Catheter (see comments section page 7-7 thru 7-8 for important details) Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day. At least 1 of the following: fever (>38 C) suprapubic tenderness* costovertebral angle pain or tenderness* At least 1 of the following findings: positive dipstick for leukocyte esterase /or nitrite pyuria (urine specimen with 10 WBC/mm³ of unspun urine or >5 WBC/high power field of spun urine) microorganisms seen on Gram s stain of unspun urine A positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms A positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms SUTI-Criterion 1a SUTI-Criterion 2a January
11 Laboratory Evidence Signs Symptoms Device-associated Module Figure 2: Identification Categorization of SUTI When Indwelling Catheter has been removed (see comments section page 7-7 thru 7-8 for important details) Patient had an indwelling urinary catheter removed the day or the day before all elements of the infection criterion were first present together. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day. At least 1 of the following: fever (>38 C) dysuria* urgency* suprapubic tenderness* frequency* costovertebral angle pain or tenderness* At least 1 of the following findings: positive dipstick for leukocyte esterase /or nitrite pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine microorganisms seen on Gram s stain of unspun urine A positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms A positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms SUTI-Criterion 1a SUTI-Criterion 2a Was an indwelling urinary catheter in place on the date of or the day before all elements of the infection criterion were first present together? Yes No SUTI SUTI (not catheter-associated) January
12 Laboratory Evidence Signs Symptoms Device-associated Module Figure 3: Identification Categorization of SUTI without Indwelling Catheter (see comments section page 7-7 thru 7-8 for important details) Patient did not have an indwelling urinary catheter in place at the time of, or the day before all elements of this criterion were first present together. Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day. At least 1 of the following: fever (>38 C) in a patient that is 65 years of age urgency* suprapubic tenderness* frequency* costovertebral angle pain or tenderness* dysuria* At least 1 of the following findings: positive dipstick for leukocyte esterase /or nitrite pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine) microorganisms seen on Gram s stain of unspun urine A positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms A positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms SUTI- Criterion 1b SUTI- Criterion 2b January
13 Laboratory Evidence Signs Symptoms Device-associated Module Figure 4: Identification Categorization of SUTI in Patient 1 Year of Age (see comments section page 7-7 thru 7-8 for important details) Patient 1 year of age (with** or without an indwelling urinary catheter) Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day. At least 1 of the following: fever (>38 C core) hypothermia (<36 o C core) apnea* bradycardia* dysuria* lethargy* vomiting* At least 1 of the following findings: positive dipstick for leukocyte esterase /or nitrite pyuria (urine specimen with 10 WBC/mm 3 of unspun urine or >5 WBC/high power field of spun urine) microorganisms seen on Gram s stain of unspun urine A positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms A positive urine culture of 10 3 <10 5 CFU/ml with no more than 2 species of microorganisms SUTI- Criterion 3 SUTI- Criterion 4 Was an indwelling urinary catheter in place on the date of or the day before all elements of the infection criterion were first present together? Yes No SUTI ** Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. January
14 Culture Evidence Signs Symptoms Device-associated Module Figure 5: Identification of Asymptomatic Bacteremic Urinary Tract Infection (ABUTI) (see comments section page 7-7 thru 7-8 for important details) Patient with* or without an indwelling urinary catheter Elements of the criterion must occur within a timeframe that does not exceed a gap of 1 calendar day Patient of any age NONE of the following: fever (>38 o C) urgency frequency dysuria suprapubic pain costovertebral angle pain or tenderness Patient 1 year of age NONE of the following: fever >38 o C core) hypothermia (<36 o C core) apnea bradycardia lethargy vomiting dysuria A positive urine culture of 10 5 CFU/ml with no more than 2 species of microorganisms** A positive blood culture with at least 1 matching uropathogen microorganism** to the urine culture or at least 2 matching blood cultures*** drawn on separate occasions if the matching pathogen is a common skin commensal. Asymptomatic Bacteremic Urinary Tract Infection (ABUTI) Was an indwelling urinary catheter in place on the date of or the day before all elements of the infection criterion were first present together? Yes No ABUTI (catheter-associated) ABUTI (not catheter-associated) * Patient had an indwelling urinary catheter in place for >2 calendar days, with day of device placement being Day 1, catheter was in place when all elements of this criterion were first present together. **Uropathogen microorganisms are: Gram-negative bacilli, Staphylococcus spp., yeasts, beta-hemolytic Streptococcus spp., Enterococcus spp., G. vaginalis, Aerococcus urinae, Corynebacterium (urease positive). Only genus species identification should be utilized to determine the sameness of organisms (i.e. matching organisms). No additional comparative methods should be used (e.g., morphology or antibiograms) because laboratory testing capabilities protocols may vary between facilities. January Report Corynebacterium (urease positive) as either Corynebacterium species unspecified (COS) or as C. urealyticum (CORUR) if so speciated.
15 Numerator Data: The Urinary Tract Infection (UTI) form is used to collect report each that is identified during the month selected for surveillance. The Instructions for Completion of Urinary Tract Infection form include brief instructions for collection entry of each data element on the form. The UTI form includes patient demographic information information on whether or not an indwelling urinary catheter was present. Additional data include the specific criteria met for identifying the UTI, whether the patient developed a secondary bloodstream infection, whether the patient died, the organisms isolated from cultures their antimicrobial susceptibilities. REPORTING INSTRUCTIONS: If no s are identified during the month of surveillance, the Report No Events box must be checked on the appropriate denominator summary screen, e.g., Denominators for Intensive Care Unit (ICU)/Other Locations (Not NICU or SCA/ONC). Denominator Data: Device days patient days are used for denominators (See Key Terms chapter). Indwelling urinary catheter days, which are the number of patients with an indwelling urinary catheter device, are collected daily, at the same time each day, according to the chosen location using the appropriate form (CDC ). These daily counts are summed only the total for the month is entered into NHSN. Indwelling urinary catheter days patient days are collected separately for each of the locations monitored. When denominator data are available from electronic databases, these sources may be used as long as the counts are not substantially different (+/- 5%) from manually collected counts, validated for a minimum of 3 months. Data Analyses: The Stardized Infection Ratio (SIR) is calculated by dividing the number of observed infections by the number of expected infections. The number of expected infections, in the context of statistical prediction, is calculated using rates from a stard population during a baseline time period, which represents a stard population s experience. 5 NOTE: The SIR will be calculated only if the number of expected HAIs (numexp) is 1. SIR = Observed (O) HAIs Expected (E) HAIs While the SIR can be calculated for single locations, the measure also allows you to summarize your data by multiple locations, adjusting for differences in the incidence of infection among the location types. For example, you will be able to obtain one SIR adjusting for all locations reported. Similarly, you can obtain one SIR for all specialty care areas in your facility. January
16 The rate per 1000 urinary catheter days is calculated by dividing the number of s by the number of catheter days multiplying the result by The Urinary Catheter Utilization Ratio is calculated by dividing the number of urinary catheter days by the number of patient days. These calculations will be performed separately for the different types of ICUs, specialty care areas, other locations in the institution, except for neonatal locations. 1 Magill SS, Hellinger W, et al. Prevalence of healthcare-associated infections in acute care facilities. Infect Control Hosp Epidemiol. 2012;33: Scott Rd. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals the Benefits of Prevention, Division of Healthcare Quality Promotion, National Center for Preparedness, Detection, Control of Infectious Diseases, Coordinating Center for Infectious Diseases, Centers for Disease Control Prevention, February Klevens RM, Edward JR, et al. Estimating health care-associated infections deaths in U.S. hospitals, Public Health Reports 2007;122: Gould CV, Umscheid CA, Agarwal RK, Kuntz G, Pegues DA. Guideline for prevention of catheter-associated urinary tract infections Infect Control Hosp Epidemiol. 2010;31: Dudeck MA, Horan TC, Peterson KD, et al. National Healthcare Safety Network (NHSN) report, data summary for 2009, device-associated module, issued January Am J Infect Control 2011;39: January
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Welcome and Instructions
 Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 CAUTI Catheter-Associated Urinary Tract Infection (CAUTI) Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection,
CAUTI Catheter-Associated Urinary Tract Infection (CAUTI) Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection,
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
associated Urinary Tract Infection Case Definitions
 CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
Case Studies. Case Studies
 Case Studies Case Studies Purpose Training on use of definitions based on the January 2013 NHSN Patient Safety Manual Learn to accurately apply definitions Surveillance Clinical Optimize consistency in
Case Studies Case Studies Purpose Training on use of definitions based on the January 2013 NHSN Patient Safety Manual Learn to accurately apply definitions Surveillance Clinical Optimize consistency in
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth
 CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Catheter-Associated Urinary Tract Infection (CAUTI) Definitions and Reporting
 AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
Guideline for Preventing Catheter- Associated Urinary Tract Infections
 Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs)
 An APIC Guide 2008 Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs) Developing and Applying Facility-Based Prevention Interventions in Acute and Long-Term Care Settings
An APIC Guide 2008 Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs) Developing and Applying Facility-Based Prevention Interventions in Acute and Long-Term Care Settings
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS
 Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL
 A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
Using NHSN Data Validation for Improved CLABSI Surveillance and Prevention
 1 Using NHSN Data Validation for Improved CLABSI Surveillance and Prevention Distance-learning Course Part 1 of 3 Lynn Janssen, MS, CIC, CPHQ Coordinator, HAI Liaison Program Healthcare-Associated Infections
1 Using NHSN Data Validation for Improved CLABSI Surveillance and Prevention Distance-learning Course Part 1 of 3 Lynn Janssen, MS, CIC, CPHQ Coordinator, HAI Liaison Program Healthcare-Associated Infections
NURSE DRIVEN FOLEY CATHETER PROTOCOL
 NURSE DRIVEN FOLEY CATHETER PROTOCOL BACKGROUND There are over 1.7 million hospital-acquired infections in US hospitals annually, 40% of which are urinary tract infections. 80% of hospital-acquired UTIs
NURSE DRIVEN FOLEY CATHETER PROTOCOL BACKGROUND There are over 1.7 million hospital-acquired infections in US hospitals annually, 40% of which are urinary tract infections. 80% of hospital-acquired UTIs
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Catheter Associated Urinary Tract Infection (CAUTI) Prevention. System CAUTI Prevention Team
 Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
Instructions for Completion of Primary Bloodstream Infection (BSI) Form (CDC 57.108)
 Instructions for Completion of Primary Bloodstream Infection (BSI) Form (CDC 57.108) Facility ID Event # Patient ID Social Security # Secondary ID Medicare # Patient name Gender Date of Birth Ethnicity
Instructions for Completion of Primary Bloodstream Infection (BSI) Form (CDC 57.108) Facility ID Event # Patient ID Social Security # Secondary ID Medicare # Patient name Gender Date of Birth Ethnicity
Catheter-associated Urinary Tract Infection (CAUTI) Toolkit
 Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
Don t Go With The Flow! Control and Management of UTIs in the Elderly
 Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014
 PICU Urinary Catheter & Care Guideline September 2014 Introduction PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014 Background: Urinary catheterisation
PICU Urinary Catheter & Care Guideline September 2014 Introduction PICU Urinary Catheter Insertion & Care Guideline & Bundles Dr Vinayak Rai & Dr Simon Robinson March 2014 Background: Urinary catheterisation
Answers to Frequently Asked Questions on Reporting in NHSN
 Answers to Frequently Asked Questions on Reporting in NHSN 1. With multiple infection sites, if you are unsure of the primary site of the infection, what should you do? If more than one NHSN operative
Answers to Frequently Asked Questions on Reporting in NHSN 1. With multiple infection sites, if you are unsure of the primary site of the infection, what should you do? If more than one NHSN operative
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Appropriate Urinary Catheter Use and Management
 Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
A Summary of the Guideline for the Diagnosis and Management of. Urinary Tract Infections in Long Term Care
 A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
SECTION 12.1 URINARY CATHETERS
 SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
Criteria to Define CLABSI and SSI
 Criteria to Define CLABSI and SSI Teresa C. Horan, MPH Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic Infectious Diseases Objectives Review BSI and SSI criteria Review
Criteria to Define CLABSI and SSI Teresa C. Horan, MPH Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic Infectious Diseases Objectives Review BSI and SSI criteria Review
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Lab ID Events MRSA Bloodstream Infection and C. difficile
 Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Nosocomial Bloodstream infection. Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
 Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
MN HAI Prevention Plan 1
 Healthcare Associated Infections Plan Minnesota Department of Health Healthcare Associated Infections Program Introduction In response to the increasing concerns about the public health impact of healthcare-associated
Healthcare Associated Infections Plan Minnesota Department of Health Healthcare Associated Infections Program Introduction In response to the increasing concerns about the public health impact of healthcare-associated
Draft GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009. Draft Guideline for Prevention of CAUTI 2009
 Guideline for Prevention of CAUTI 2009 GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009 Carolyn V. Gould, MD, MSCR 1 ; Craig A. Umscheid, MD, MSCE 2 ; Rajender K. Agarwal,
Guideline for Prevention of CAUTI 2009 GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009 Carolyn V. Gould, MD, MSCR 1 ; Craig A. Umscheid, MD, MSCE 2 ; Rajender K. Agarwal,
UTI in children. Quick reference guide. Issue date: August 2007. Urinary tract infection in children: diagnosis, treatment and long-term management
 Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009
 GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009 Carolyn V. Gould, MD, MSCR 1 ; Craig A. Umscheid, MD, MSCE 2 ; Rajender K. Agarwal, MD, MPH 2 ; Gretchen Kuntz, MSW, MSLIS
GUIDELINE FOR PREVENTION OF CATHETER- ASSOCIATED URINARY TRACT INFECTIONS 2009 Carolyn V. Gould, MD, MSCR 1 ; Craig A. Umscheid, MD, MSCE 2 ; Rajender K. Agarwal, MD, MPH 2 ; Gretchen Kuntz, MSW, MSLIS
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Urinary Tract Infections. Clinical Scenario #1. Urinary Tract Infections. Clinical Scenario #1 : Labs
 Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
190.12 - Urine Culture, Bacterial Summary Information Highlighted items indicate most frequently used codes.
 Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
URINE CULTURES GENERAL PROCEDURE
 University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
Urinary Tract Infections
 Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Catheter-Associated Urinary Tract Infections Lauren Tew, Bard Ltd, UK A Webber Training Teleclass Catheter-Associated Urinary Tract Infection
 Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
Spotlight on Success: Implementing Nurse-Driven Protocols to Reduce CAUTIs
 Spotlight on Success: Implementing Nurse-Driven Protocols to Reduce CAUTIs Many hospitals today are increasingly allowing nurses to make decisions regarding patients care, treatment, and services without
Spotlight on Success: Implementing Nurse-Driven Protocols to Reduce CAUTIs Many hospitals today are increasingly allowing nurses to make decisions regarding patients care, treatment, and services without
National Healthcare Safety Network (NHSN) Introduction & Enrollment
 National Healthcare Safety Network (NHSN) Introduction & Enrollment Surveillance for Healthcare-Associated & Resistant Pathogens (SHARP) Unit 1 Introduction to NHSN Secure, internet-based surveillance
National Healthcare Safety Network (NHSN) Introduction & Enrollment Surveillance for Healthcare-Associated & Resistant Pathogens (SHARP) Unit 1 Introduction to NHSN Secure, internet-based surveillance
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
REPORT TO THE 26TH LEGISLATURE STATE OF HAWAII 2012
 REPORT TO THE 26TH LEGISLATURE STATE OF HAWAII 2012 PURSUANT TO ACT 177(11), SESSION LAWS OF HAWAII, 2011, RELATING TO HEALTHCARE ASSOCIATED INFECTIONS REPORTING Prepared by: State of Hawaii Department
REPORT TO THE 26TH LEGISLATURE STATE OF HAWAII 2012 PURSUANT TO ACT 177(11), SESSION LAWS OF HAWAII, 2011, RELATING TO HEALTHCARE ASSOCIATED INFECTIONS REPORTING Prepared by: State of Hawaii Department
Speaking the same language: Uniformly defining critically ill patients for Foley use to. decrease catheter utilizations in an Intermediate Care Unit.
 1 Speaking the same language: Uniformly defining critically ill patients for Foley use to decrease catheter utilizations in an Intermediate Care Unit. Abigail O. Imarhiagbe, RN, BSN-Student University
1 Speaking the same language: Uniformly defining critically ill patients for Foley use to decrease catheter utilizations in an Intermediate Care Unit. Abigail O. Imarhiagbe, RN, BSN-Student University
Implementing the Long-Term Care UTI Toolkit Wisconsin Coalition on HealthCare Association Infection in Long Term Care
 Implementing the Long-Term Care UTI Toolkit Wisconsin Coalition on HealthCare Association Infection in Long Term Care MetaStar Health Care Quality Symposium: The Value of Better Health Paula Kock RN paulak@parkmanorwi.com
Implementing the Long-Term Care UTI Toolkit Wisconsin Coalition on HealthCare Association Infection in Long Term Care MetaStar Health Care Quality Symposium: The Value of Better Health Paula Kock RN paulak@parkmanorwi.com
Analyzing Data in NHSN
 Analyzing Data in NHSN Lindsey Weiner, MPH Epidemiologist Alabama Hospital Quality Initiative Webinar September 16, 2015 National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare
Analyzing Data in NHSN Lindsey Weiner, MPH Epidemiologist Alabama Hospital Quality Initiative Webinar September 16, 2015 National Center for Emerging and Zoonotic Infectious Diseases Division of Healthcare
Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization
 Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization H.J. Mulder MANP 1-11-2011 Henk-Jan Mulder MANP Department of Urology Martini General Hospital Van Swietenplein 1 9700
Avoiding Urinary Tract Infections in Patients practising Intermittent Catheterization H.J. Mulder MANP 1-11-2011 Henk-Jan Mulder MANP Department of Urology Martini General Hospital Van Swietenplein 1 9700
Prevention of Catheter-Associated Urinary Tract Infections
 Prevention of Catheter-Associated Urinary Tract Infections Self-Study Module Created March 2012 2012 BJC HealthCare. All rights reserved. Reproduction is strictly prohibited without written consent. Overview
Prevention of Catheter-Associated Urinary Tract Infections Self-Study Module Created March 2012 2012 BJC HealthCare. All rights reserved. Reproduction is strictly prohibited without written consent. Overview
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
TECHNICAL REPORT FOR HEALTHCARE-ASSOCIATED INFECTIONS. New Jersey Department of Health Health Care Quality Assessment
 TECHNICAL REPORT FOR HEALTHCARE-ASSOCIATED INFECTIONS A SUPPLEMENT TO THE NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT New Jersey Department of Health Health Care Quality Assessment June 2013 Tables of
TECHNICAL REPORT FOR HEALTHCARE-ASSOCIATED INFECTIONS A SUPPLEMENT TO THE NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT New Jersey Department of Health Health Care Quality Assessment June 2013 Tables of
Bloodstream Infection Event (Central Line-Associated Bloodstream Infection and Non-central line-associated Bloodstream Infection)
 Bloodstream Infection Event (Central Line-Associated Bloodstream Infection and Non-central line-associated Bloodstream Infection) Introduction: Although a 46% decrease in CLAs has occurred in hospitals
Bloodstream Infection Event (Central Line-Associated Bloodstream Infection and Non-central line-associated Bloodstream Infection) Introduction: Although a 46% decrease in CLAs has occurred in hospitals
PATIENT CARE MANUAL PROCEDURE
 PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
Essential steps to safe, clean care
 Essential steps to safe, clean care Reducing healthcare-associated infections in Primary care trusts; Mental health trusts; Learning disability organisations; Independent healthcare; Care homes; Hospices;
Essential steps to safe, clean care Reducing healthcare-associated infections in Primary care trusts; Mental health trusts; Learning disability organisations; Independent healthcare; Care homes; Hospices;
1 Dawa K.K. Rn, Rm, Bnsc., 2 Kever R.T. Rn, Msc (Nursing), 3 Dathini H. Rn, Rm, Bnsc, Pgde., 4 Babaji M. Rn, Rm, Msc (Nursing), 5 Garba N.
 IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 3, Issue 4 Ver. I (Jul-Aug. 2014), PP 64-71 Assessment Of Risk Factors Influencing The Development Of
IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 3, Issue 4 Ver. I (Jul-Aug. 2014), PP 64-71 Assessment Of Risk Factors Influencing The Development Of
Age in years Females (% prevalence) Males (% prevalence) 6-15 Vesicoureteral reflux (4.4%) Vesicoureteral reflux (0.5%)
 Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
How To Find Out If A Diabetic Woman Has A Urinary Tract Infection
 Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Changing Clinical Behaviors to Lower Costs and Reduce Catheter-Associated Urinary Tract Infections (CAUTI)
 Changing Clinical Behaviors to Lower Costs and Reduce Catheter-Associated Urinary Tract Infections (CAUTI) ARKANSAS METHODIST MEDICAL CENTER: How a foley catheter management system combined with education
Changing Clinical Behaviors to Lower Costs and Reduce Catheter-Associated Urinary Tract Infections (CAUTI) ARKANSAS METHODIST MEDICAL CENTER: How a foley catheter management system combined with education
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
REDUCING USE OF INDWELLING URINARY CATHETERS AND ASSOCIATED URINARY TRACT INFECTIONS. C E 1.0 Hour. Patient Safety Issues
 Patient Safety Issues REDUCING USE OF INDWELLING URINARY CATHETERS AND ASSOCIATED URINARY TRACT INFECTIONS By Ellen H. Elpern, MSN, APN, CCNS, Kathryn Killeen, MSN, APN, CCNS, Alice Ketchem, RN, MSN, Amanda
Patient Safety Issues REDUCING USE OF INDWELLING URINARY CATHETERS AND ASSOCIATED URINARY TRACT INFECTIONS By Ellen H. Elpern, MSN, APN, CCNS, Kathryn Killeen, MSN, APN, CCNS, Alice Ketchem, RN, MSN, Amanda
Nosocomial Urinary Tract Infections
 15 Nosocomial Urinary Tract Infections Sonia Isabel Cuervo Maldonado and Jorge Alberto Cortés Luna Universidad Nacional de Colombia, Bogotá Colombia 1. Introduction Healthcare-associated urinary infection
15 Nosocomial Urinary Tract Infections Sonia Isabel Cuervo Maldonado and Jorge Alberto Cortés Luna Universidad Nacional de Colombia, Bogotá Colombia 1. Introduction Healthcare-associated urinary infection
Catheter Care. What you need to know. Jacinta Stewart Continence Nurse
 Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Healthcare-associated Infections in Utah
 2013 Healthcare-associated Infections in Utah Utah Department of Health Division of Disease Control and Prevention Published October 2014 2013 Annual Report Prepared by Rebecca L. Ward Division of Disease
2013 Healthcare-associated Infections in Utah Utah Department of Health Division of Disease Control and Prevention Published October 2014 2013 Annual Report Prepared by Rebecca L. Ward Division of Disease
Central Line-Associated Bloodstream Infection (CLABSI) Prevention. Basics of Infection Prevention 2-Day Mini-Course 2013
 Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
Central Line-Associated Bloodstream Infection (CLABSI) Prevention Basics of Infection Prevention 2-Day Mini-Course 2013 2 Objectives Describe the etiology and epidemiology of central line associated bloodstream
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care
 Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
After care following insertion of a suprapubic catheter
 Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
Nosocomial Urinary Tract Infection
 Nosocomial Urinary Tract Infection Michael F. Ksycki, DO, Nicholas Namias, MD, MBA* KEYWORDS Nosocomial infection Urinary tract infection Urinary catheter Nosocomial urinary tract infection is a major
Nosocomial Urinary Tract Infection Michael F. Ksycki, DO, Nicholas Namias, MD, MBA* KEYWORDS Nosocomial infection Urinary tract infection Urinary catheter Nosocomial urinary tract infection is a major
4/5/2013. Dee Webber RN BSN Staff Nurse EMMC CCU. Health care-associated infections are one of the most common complications of hospital care.
 Dee Webber RN BSN Staff Nurse EMMC CCU Critical Care Staff Nurse Leaders Sara Sabal ADN, RN Dee Webber BSN, RN Critical Care Leadership Joyce Hill BSN, RN Tina Closson BSN,RN, CCRN, CSC Cynthia Downs MSN,
Dee Webber RN BSN Staff Nurse EMMC CCU Critical Care Staff Nurse Leaders Sara Sabal ADN, RN Dee Webber BSN, RN Critical Care Leadership Joyce Hill BSN, RN Tina Closson BSN,RN, CCRN, CSC Cynthia Downs MSN,
T h e C e n t e r s f o r D i s e a s e C o n t r o l a n d P r e v e n t i o n ( C D C ) NHSN e-news
 T h e C e n t e r s f o r D i s e a s e C o n t r o l a n d P r e v e n t i o n ( C D C ) NHSN e-news Volume 9, Issue 3 September 2014 New NHSN Newsletter Format! Based on user feedback, NHSN has modified
T h e C e n t e r s f o r D i s e a s e C o n t r o l a n d P r e v e n t i o n ( C D C ) NHSN e-news Volume 9, Issue 3 September 2014 New NHSN Newsletter Format! Based on user feedback, NHSN has modified
HAI LEADERSHIP PARTNERING FOR ACCOUNTABLE CARE
 HAI LEADERSHIP PARTNERING FOR ACCOUNTABLE CARE Cepheid s Government Affairs Department Advocating for Patient Access to Molecular Diagnostics in the Era of Healthcare Reform A TEAM APPROACH Legislative
HAI LEADERSHIP PARTNERING FOR ACCOUNTABLE CARE Cepheid s Government Affairs Department Advocating for Patient Access to Molecular Diagnostics in the Era of Healthcare Reform A TEAM APPROACH Legislative
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
Complication Prevention
 Nursing Best Practice for the Stroke Patient Complication Prevention Tara Panazzolo, MSN, RN-BC Nursing Performance Improvement Advisor Hackensack University Medical Center New Jersey State Stroke Conference
Nursing Best Practice for the Stroke Patient Complication Prevention Tara Panazzolo, MSN, RN-BC Nursing Performance Improvement Advisor Hackensack University Medical Center New Jersey State Stroke Conference
Long-term urinary catheter-associated urinary tract infection (UTI)
 Peer reviewed article Long-term urinary catheter-associated urinary tract infection (UTI) Abstract This paper reviews the literature on the current management of symptomatic urinary tract infections (UTIs)
Peer reviewed article Long-term urinary catheter-associated urinary tract infection (UTI) Abstract This paper reviews the literature on the current management of symptomatic urinary tract infections (UTIs)
Case Studies in Urinary Tract Infections
 Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
Childhood Urinary Tract Infections
 Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
PATIENT URINARY CATHETER PASSPORT
 n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
Preventing CAUTI: A patient-centered approach
 Preventing CAUTI: A patient-centered approach The infection prevention community must assure that ongoing CAUTI prevention programs are inclusive and effective. By MaRiLyn HanCHett, Rn, Ma, CPHQ, CiC Photo
Preventing CAUTI: A patient-centered approach The infection prevention community must assure that ongoing CAUTI prevention programs are inclusive and effective. By MaRiLyn HanCHett, Rn, Ma, CPHQ, CiC Photo
Bard: Intermittent Catheters. A guide to. Bard: Pelvic Organ Prolapse. An REIMBURSEMENT. overview of OF INTERMITTENT. Prolapse CATHETERS
 Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
Business Case for National Healthcare Safety Network (NHSN) Infection Surveillance Database
 Business Case for National Healthcare Safety Network (NHSN) Infection Surveillance Database Executive Summary All hospitals understand the value of preventing healthcare-associated infections (HAIs) and
Business Case for National Healthcare Safety Network (NHSN) Infection Surveillance Database Executive Summary All hospitals understand the value of preventing healthcare-associated infections (HAIs) and
Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection
 Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection Monika Dutta, Prem Verma, A.K. Mandal Abstract : Indwelling urinary catheterization
Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection Monika Dutta, Prem Verma, A.K. Mandal Abstract : Indwelling urinary catheterization
2015 RN.ORG, S.A., RN.ORG, LLC
 Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Having a urinary catheter information for men
 Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
Having a urinary catheter information for men This leaflet explains what a catheter is, why you need it and how you should look after it. If you have any further questions, please contact your district
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
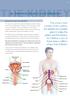 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
CAUTI TAP: Another Way to Hit the Bullseye. Peg Gilbert, RN, MS, CIC Nancy McDonald, RN, BSN, CPHQ
 CAUTI TAP: Another Way to Hit the Bullseye Peg Gilbert, RN, MS, CIC Nancy McDonald, RN, BSN, CPHQ What is the TAP Strategy? The Targeted Assessment for Prevention (TAP) strategy is a method developed by
CAUTI TAP: Another Way to Hit the Bullseye Peg Gilbert, RN, MS, CIC Nancy McDonald, RN, BSN, CPHQ What is the TAP Strategy? The Targeted Assessment for Prevention (TAP) strategy is a method developed by
NHSN e-news: SIRs Special Edition Updated December 10, 2010. Your Guide to the Standardized Infection Ratio (SIR)
 NHSN e-news: SIRs Special Edition 1 Special Edition! Your Guide to the Standardized Infection Ratio (SIR) October 2010, Updated December 2010 The Centers for Disease Control and Prevention (CDC) NHSN e-news
NHSN e-news: SIRs Special Edition 1 Special Edition! Your Guide to the Standardized Infection Ratio (SIR) October 2010, Updated December 2010 The Centers for Disease Control and Prevention (CDC) NHSN e-news
150640_Brochure_B 4/12/07 2:58 PM Page 2. Patient Information. Freedom From an Enlarged Prostate
 150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
