Nosocomial Urinary Tract Infection
|
|
|
- Alexis Stafford
- 8 years ago
- Views:
Transcription
1 Nosocomial Urinary Tract Infection Michael F. Ksycki, DO, Nicholas Namias, MD, MBA* KEYWORDS Nosocomial infection Urinary tract infection Urinary catheter Nosocomial urinary tract infection is a major cause of morbidity in hospitalized patients in general, and in postoperative surgical patients in particular. The major predisposing factor to the development of a urinary tract infection is the presence of a urinary catheter. The risk of infection increases with the duration of catheterization. It has been estimated that the risk of urinary tract infection increases by 5% to 10% per catheter day after the second day of catheterization. 1,2 RISK FACTORS A recent analysis of data from the National Surgical Infection Prevention Project revealed that 86% of patients undergoing major operations had indwelling urinary catheters in the perioperative period, with half of the patients remaining catheterized for more than 2 days. As expected, catheterization for more than 2 days was a significant risk factor for urinary tract infection (9.4% versus 4.5%; P 5.004). Prolonged catheterization was also associated with a decreased likelihood for discharge to home, and with increased 30-day mortality. 3 Previously, duration of catheterization had not been linked to mortality. 4 The National Health Safety Network, a project of the Centers for Disease Control and Prevention, also investigated catheter use and catheter-related urinary tract infection as part of its surveillance activities. In 2006, it reported a catheter use index in surgically oriented intensive care units (ICUs). This index, a ratio of urinary catheter days to patient days, ranged from 0.69 to In these same ICUs, there were 4.0 to 7.5 catheter-associated urinary tract infections per 1000 urinary catheter days. 5 Thus, perioperative catheterization is near ubiquitous, is a major risk factor for nosocomial urinary tract infection, and is linked to, if not directly causative of, a decreased likelihood of discharge to home and an increased 30-day mortality. MICROBIOLOGYAND DIAGNOSIS The most common causative agents of catheter-related urinary tract infection are the patients own colonic flora. Additional organisms are usually not found until duration of Miller School of Medicine, University of Miami, PO Box (D-40), Miami, FL 33101, USA * Corresponding author. address: nnamias@miami.edu (N. Namias). Surg Clin N Am 89 (2009) doi: /j.suc surgical.theclinics.com /08/$ see front matter ª 2009 Elsevier Inc. All rights reserved.
2 476 Ksycki & Namias catheterization exceeds 30 days. 6 The most common organisms causing these infections with short-term catheterizations are Escherichia coli, enterococci, Pseudomonas, Klebsiella, Enterobacter, Staphylococcus epidermidis, Staphylococcus aureus, and Serratia. Exogenous sources can also lead to catheter-related urinary tract infection, commonly with staphylococci, Serratia marcescens, Burkholderia cepacia, and Stenotrophomonas maltophilia. 7 Wagenlehner and colleagues 8 recently analyzed their 12-year experience with urinary tract infections in hospitalized urology patients in one German hospital. E coli initially accounted for approximately one third of the urinary tract infections. This increased over the 12 years to approximately 40%, primarily displacing infections due to Pseudomonas aeruginosa. Other gram negatives accounted for another one third of the infections, and gram positives caused the remaining one third. Increasing resistance of E coli to the commonly used trimethoprim/sulfamethoxazole was noted, highlighting the importance of culture and sensitivity data not only in treating the individual patient, but also for planning effective empiric treatment strategies. The investigators did not include fungal urinary tract infections as part of their study. Urinary cultures have been the standard means for diagnosing urinary tract infections. The standard cutoff has been the growth of 10 5 or more organisms per milliliter of urine. This number was originally based on studies of symptomatic patients with cystitis, and not hospitalized patients with infections related to indwelling urinary catheter. Nonetheless, this remains the number used to diagnose the presence of urinary tract infection in surgical patients, and in reporting the incidence of such infections to regulatory agencies. In more critically ill surgical patients, candiduria remains a vexing clinical problem. It typically occurs in patients who have a multitude of reasons to manifest sepsis. Sobel and Lundstrom 9 reviewed the development of candiduria in 2001 and pointed out that 10% to 15% of nosocomial urinary tract infections are now caused by Candida sp, with the highest prevalence being in patients housed in ICUs, and those with leukemia or who had undergone bone marrow transplant. Diabetes predisposes to the development of candiduria in multiple ways. In women, diabetes promotes colonization of the vulvovestibular area with Candida. Glycosuria, if present, enhances urinary fungal growth. Diabetes also impairs host defenses, particularly phagocytosis. Finally, the development of a neurogenic bladder allows for urinary stasis and increases the likelihood that the urinary tract will be instrumented. Fungal urinary tract infections are also promoted in diabetics and nondiabetics alike by antibiotic therapy, which leads to fungal overgrowth in the colon and perineal area due to suppression of normal bacterial flora; the fungal organisms can then ascend the Foley catheter into the urinary system. Bukhary 10 in 2008 also identified similar risk factors in a review of 37 years of English-language literature on the topic of candiduria. This review indicated that the risk factors for candiduria were indwelling urinary catheters, use of antibiotics, advanced age, underlying anatomic urologic abnormality, previous surgery, and the presence of diabetes. Sobel and Lundstrom 9 indicated that Candida albicans is the most common fungal species causing urinary fungal infections, with Candida glabrata being the second most common fungal pathogen. More than one candidal species are found simultaneously in 10% of cases. Bukhary 10 cited multiple reviews of the epidemiology of candiduria, and confirmed that with only one exception the overwhelming majority of candiduria is due to C albicans. C glabrata accounts for 12% to 18% of cases, Candida tropicalis for 8% to 22%, and all remaining species for less than 5% in almost all studies. Urinary tract infections due to noncandidal fungal organisms are very uncommon in surgical patients, and are usually encountered as part of a disseminated mycotic disease in highly immunosuppressed patients. 9
3 Urinary Tract Infection 477 The diagnosis of a urinary tract infection due to Candida is difficult because Candida in the urine can represent contamination, colonization of the drainage device, or a true infection. Small numbers of yeast from a colonized catheter, collection device, or the vulva may multiply rapidly in the collected urine, producing high colony counts that do not necessarily indicate infection. Further, although the presence of pyuria usually supports the diagnosis of infection, the mere presence of an indwelling catheter can lead to pyuria, as can a coexisting bacterial urinary tract infection. Thus, clinical judgment must be used in making the diagnosis, particularly in asymptomatic patients. Notably, asymptomatic candiduria rarely, if ever, leads to candidemia. 9 PREVENTION European and Asian guidelines have been developed based on a comprehensive review and meta-analysis of data on prevention and treatment of urinary catheter associated infections. Not surprisingly, the principal findings are that minimization of duration of catheterization and maintenance of a closed system are the best means of avoiding infection. 6 These 2008 European and Asian guidelines for the prevention of catheter-associated urinary tract infections are listed below. The letters in parentheses indicate the grade of the guideline recommendation. An A recommendation is based on clinical studies of good quality and consistency, including at least one randomized trial; a B recommendation is based on well-conducted clinical studies, but without randomized clinical trials; and a C recommendation is one developed by the expert panel in the absence of directly applicable clinical studies of good quality. The catheter system should remain closed (A). The duration of catheterization should be minimal (A). Topical antiseptics or antibiotics applied to the catheter, urethra, or meatus are not recommended (A). Benefits from prophylactic antibiotics and antiseptic substances have never been established; therefore, they are not recommended (A). Removal of the indwelling catheter after a nonurological operation before midnight may be beneficial (B). Long-term indwelling catheters should be changed in intervals adapted to the individual patient, but must be changed before blockage is likely to occur (B); however, there is no evidence for the exact intervals of changing catheters. Chronic antibiotic suppressive therapy is generally not recommended (A). Adherence to these basic recommendations could significantly decrease the risk of catheter-associated urinary tract infections. In a 10-year study of infection control and surveillance practices emphasizing some of these principles, there was a decrease of 70% over time in the risk of urinary tract infections in an ICU population. 11 Nonetheless, prolonged use of urinary catheters is necessary in certain surgical patients. In such cases, clinicians cannot use the best tool for preventing catheter-associated infections early removal of the devices. Therefore, there has been interest in the use of catheters that might be less prone to allowing an infection. One key way in which catheters predispose to urinary tract infection is by serving as a site for bacterial pathogens to create a biofilm. The organisms associated with catheter-associated urinary tract infection grow in a glycocalyx, protected from the antibiotics concentrated in the urine. This biofilm gradually thickens and can encapsulate all surfaces of the catheter. Within this dense biofilm, the bacteria create their own microenvironment,
4 478 Ksycki & Namias become metabolically inactive as compared with planktonic bacteria, and thereby become resistant to antibiotics because of the lack of metabolic activity. 12 Attempts have been made to reduce catheter-associated urinary tract infection through use of advanced catheters designed to inhibit biofilm formation. The primary technology for this is the use of antibiotic- or antiseptic-coated catheters. There have been two systematic reviews of silver alloy and nitrofurazone-impregnated urinary catheters in recent years. 13,14 The difficulty in evaluating the utility of these products is stressed in one of these reviews, 14 which included trials that were deemed to be of variable levels of quality. The combined data available on all 13,319 participants suggested that antimicrobial urinary catheters prevented or delayed the onset of catheter-associated bacteriuria compared with control catheters. However, the magnitude of this effect varied, and was systematically overestimated in many studies because of dropouts and exclusions. The effects of these catheters on morbidity, including bloodstream infection, remained unknown. 15 Thus, although these devises seem promising, the analysis of the literature by Tenke and colleagues 6 described in the European and Asian guidelines suggests that the role of these devices is limited at the present time, with the indications for their use remaining to be established. Recommendations and their level of evidence included: Antibiotic-impregnated catheters may decrease the frequency of asymptomatic bacteriuria within 1 week. There is, however, no evidence they decrease symptomatic infection. Therefore, they cannot be recommended routinely (B). Silver alloy catheters significantly reduce the incidence of asymptomatic bacteriuria, but only for less than 1 week. There was some evidence of reduced risk for symptomatic urinary tract infection. Therefore, such catheters may be useful in some settings (B). Research into urinary catheter design continues because of the clear need to reduce the incidence of catheter-associated urinary tract infections. The newest technology involves use of protamine sulfate and chlorhexidine to prevent or delay biofilm formation. These catheters proved less likely to become colonized in vivo than silvercoated or uncoated catheters, but their clinical efficacy, as with the older types of impregnated catheters, has yet to be proven. 15 TREATMENT Treatment of nosocomial urinary tract infections needs to be considered separately for patients with asymptomatic bacteriuria and for those with symptomatic urinary tract infection. In general, asymptomatic bacteriuria in catheterized patients should not be treated. Removal of the catheter allows resolution of bacteriuria in one third to one half of cases. 6 The European and Asian guidelines 1 recommend treatment of asymptomatic bacteriuria in the following circumstances: For patients undergoing urological surgery or implantation of prostheses (A) When treatment may be part of a plan to control nosocomial infection due to a particularly virulent organism prevailing in a treatment unit (B) For patients who have a high risk of serious infectious complications (eg, patients who are immunosuppressed) (C) For infections caused by strains causing a high incidence of bacteremia (eg, S marcescens) (B)
5 Urinary Tract Infection 479 Treatment of symptomatic urinary tract infection is usually more straightforward. Clinical symptoms and signs, such as frequency, dysuria, or suprapubic pain directly attributable to an infection, are an indication for treatment. The most common symptom attributed to a urinary tract infection in hospitalized patients is usually fever. Bacteriuria may or may not be the source of a fever or another nonspecific indicator of infection, such as leukocytosis. It has been suggested that if the patient has a low-grade fever, is clinically stable, and has no other indication for antibiotics, observation, rather than immediate antimicrobial therapy, can be entertained. In these patients, it may also be useful to replace the catheter with a new one to eliminate the burden of the existing biofilm. 7 If the patient is systemically ill, empiric antibiotics should be started, based on knowledge of the local bacterial ecology, and then tailored based on definitive culture and susceptibility results. There are no adequate clinical studies to guide the duration of therapy; clinical judgment and patient response should be used to determine the duration of the antibiotic course. 7 The choice of antibiotic may be complicated by the development of resistant bacteria. In particular, there is greater resistance of E coli, other Enterobacteriaceae, and P aeruginosa in catheterized patients compared with noncatheterized patients. 16 In the absence of an indwelling catheter, as with community-acquired urinary tract infections, resistance has not generally been an important issue because antibiotics typically used for community-acquired infections, such as amoxicillin, cephalexin, trimethoprim/sulfamethoxazole, ciprofloxacin, and levofloxacin, are highly concentrated in the urine, from nearly 100 up to several hundred times. 17 However, in patients with nosocomial urinary tract infections, who may have indwelling urinary catheters and highly resistant pathogens, the perception that bacterial susceptibilities are unimportant may not necessarily be accurate. Thus, clinical judgment and the patient s response to therapy dictate the degree to which susceptibility data are used to direct treatment of symptomatic urinary tract infections in hospitalized patients. Some of these same considerations apply to the dilemma as to whether or not to treat the patient with candiduria. In the past, when the only option for treatment was amphotericin B, patients were rarely treated. The development of fluconazole and other less toxic antifungal agents has greatly increased the likelihood that clinicians will treat patients with candiduria. As with other asymptomatic urinary tract infections, however, asymptomatic candiduria needs no pharmacologic therapy, and can usually be treated by removal of Foley catheters or replacement of the catheter to reduce the biofilm burden. Pharmacologic therapy with an antifungal agent should generally be limited to patients with symptomatic candiduria after confirmation of the infection from a second urine sample. 18 Unfortunately, the critically ill patient is the one most likely to have candiduria, and the one least likely to be able to complain of symptoms. Furthermore, this is the patient most likely to suffer a poor outcome if a necessary treatment is withheld. Thus, it is somewhat difficult to define which of these patients should be treated. Suggested indications for the treatment of candiduria include low birth weight infants and patients who have undergone renal transplantation, have neutropenia, or who have a planned invasive urologic procedure. If asymptomatic candiduria progresses to symptomatic cystitis, it ought to be treated as well. 9 Fluconazole is the antifungal agent most commonly given to eradicate candiduria. Oral fluconazole is both convenient and effective, and should be used if it is feasible to give the patient an oral or enteral agent. Because fluconazole concentrates in the urine to more than 100 mg/ml after a 400-mg dose, even C glabrata, which is relatively resistant to fluconazole with a minimal inhibitory concentration of 8 to 16 mg/ml, can
6 480 Ksycki & Namias be successfully treated with fluconazole. Candiduria frequently recurs 2 weeks after successful treatment with fluconazole if the underlying patient conditions conducive to the development of candiduria have not been eliminated. In the presence of renal failure, when a drug cannot be effectively delivered into the urinary tract, amphotericin B bladder irrigations can be used to treat a lower urinary tract infection due to Candida. 9 SUMMARY Nosocomial urinary tract infections are a common complication in surgical patients. The use of urinary catheters is the major risk factor for the development of these infections. Discontinuation of catheterization within 2 days is key to avoiding nosocomial urinary tract infections. Patients with asymptomatic bacteriuria can generally be treated initially with catheter removal or catheter exchange, and do not necessarily need antimicrobial therapy. Symptomatic patients should receive antibiotic therapy. Resistance of urinary pathogens to common antibiotics is not usually an issue because of the concentration of most antibiotics in the urine. However, it is uncertain if different empiric antimicrobial regimens are needed when highly resistant bacteria are involved in nosocomial urinary tract infections. The treatment of patients with candiduria generally follows the same principles. Patients with asymptomatic candiduria usually can be treated with catheter removal or exchange, and do not need specific antifungal therapy. However, selected high-risk patients as well as those with symptomatic fungal urinary tract infections should receive antifungal therapy, generally using fluconazole. REFERENCES 1. Schaeffer AJ. Catheter-associated bacteriuria. Urol Clin North Am 1986;13(4): Stamm WE. Guidelines for prevention of catheter-associated urinary tract infections. Ann Intern Med 1975;82(3): Wald HL, Ma A, Bratzler DW, et al. Indwelling urinary catheter use in the postoperative period: analysis of the national surgical infection prevention project data. Arch Surg 2008;143(6): Clec h C, Schwebel C, Francais A, et al. Does catheter-associated urinary tract infection increase mortality in critically ill patients? Infect Control Hosp Epidemiol 2007;28(12): Edwards JR, Peterson KD, Andrus ML, et al. National Healthcare Safety Network (NHSN) Report, data summary for 2006, issued June Am J Infect Control 2007;35(5): Tenke P, Kovacs B, Bjerklund Johansen TE, et al. European and Asian guidelines on management and prevention of catheter-associated urinary tract infections. Int J Antimicrob Agents 2008;31(Suppl 1):S Sedor J, Mulholland SG. Hospital-acquired urinary tract infections associated with the indwelling catheter. Urol Clin North Am 1999;26(4): Wagenlehner FM, Niemetz AH, Weidner W, et al. Spectrum and antibiotic resistance of uropathogens from hospitalised patients with urinary tract infections: Int J Antimicrob Agents 2008;31(Suppl 1):S Sobel JD, Lundstrom T. Management of candiduria. Curr Urol Rep 2001;2(4): Bukhary ZA. Candiduria: a review of clinical significance and management. Saudi J Kidney Dis Transpl 2008;19(3):
7 Urinary Tract Infection Vanhems P, Baratin D, Voirin N, et al. Reduction of urinary tract infections acquired in an intensive care unit during a 10-year surveillance program. Eur J Epidemiol 2008;23: Ha US, Cho YH. Catheter-associated urinary tract infections: new aspects of novel urinary catheters. Int J Antimicrob Agents 2006;28(6): Drekonja DM, Kuskowski MA, Wilt TJ, et al. Antimicrobial urinary catheters: a systematic review. Expert Rev Med Devices 2008;5(4): Johnson JR, Kuskowski MA, Wilt TJ, et al. Systematic review: antimicrobial urinary catheters to prevent catheter-associated urinary tract infection in hospitalized patients. Ann Intern Med 2006;144(2): Darouiche RO, Mansouri MD, Gawande PV, et al. Efficacy of combination of chlorhexidine and protamine sulphate against device-associated pathogens. J Antimicrob Chemother 2008;61(3): Ko MC, Liu CK, Woung LC, et al. Species and antimicrobial resistance of uropathogens isolated from patients with urinary catheter. Tohoku J Exp Med 2008; 214(4): Gupta K, Hooton TM, Stamm WE, et al. Increasing antimicrobial resistance and the management of uncomplicated community-acquired urinary tract infections. Ann Intern Med 2001;135(1): Sobel JD, Kauffman CA, McKinsey D, et al. Candiduria: a randomized, doubleblind study of treatment with fluconazole and placebo. The National Institute of Allergy and Infectious Diseases (NIAID) mycoses study group. Clin Infect Dis 2000;30(1):19 24.
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Surveillance cultures PRO. Kurt Espersen ICU 4131 Rigshospitalet Copenhagen
 Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
How To Find Out If A Diabetic Woman Has A Urinary Tract Infection
 Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Nosocomial Bloodstream infection. Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
 Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Welcome and Instructions
 Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Long-term urinary catheter-associated urinary tract infection (UTI)
 Peer reviewed article Long-term urinary catheter-associated urinary tract infection (UTI) Abstract This paper reviews the literature on the current management of symptomatic urinary tract infections (UTIs)
Peer reviewed article Long-term urinary catheter-associated urinary tract infection (UTI) Abstract This paper reviews the literature on the current management of symptomatic urinary tract infections (UTIs)
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Catheter-Associated Urinary Tract Infections Lauren Tew, Bard Ltd, UK A Webber Training Teleclass Catheter-Associated Urinary Tract Infection
 Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King debbie@webbertraining.com www.webbertraining.com Tew L, Pomfret I & King D (2005)
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
associated Urinary Tract Infection Case Definitions
 CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
CDC/NHSN Cather-associated associated Urinary Tract Infection Case Definitions Chaz M. Rhone, MPH Regional HAI Epidemiologist Florida Department of Health *all information is directly from the NHSN site
Catheter-associated Urinary Tract Infection (CAUTI) Toolkit
 Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
Activity C: ELC Prevention Collaboratives Catheter-associated Urinary Tract Infection (CAUTI) Toolkit Carolyn Gould, MD MSCR Division of Healthcare Quality Promotion Centers for Disease Control and Prevention
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Appropriate Urinary Catheter Use and Management
 Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Age in years Females (% prevalence) Males (% prevalence) 6-15 Vesicoureteral reflux (4.4%) Vesicoureteral reflux (0.5%)
 Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
Magdalena E. Sobieszczyk Urinary Tract Infections AIMS: 1. Understand epidemiology and microbiology of urinary tract infections 2. Understand pathogenesis of lower and upper urinary tract infections 3.
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Management of Urinary Tract Infections in Patients with Urinary Catheters
 Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Guideline for Preventing Catheter- Associated Urinary Tract Infections
 Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection
 Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection Monika Dutta, Prem Verma, A.K. Mandal Abstract : Indwelling urinary catheterization
Comparison of effectiveness of sterile vs. clean technique for indwelling catheter care in preventing urinary tract infection Monika Dutta, Prem Verma, A.K. Mandal Abstract : Indwelling urinary catheterization
A Summary of the Guideline for the Diagnosis and Management of. Urinary Tract Infections in Long Term Care
 A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
Engineering Out the Risk for Infection with Urinary Catheters
 Engineering Out the Risk for Infection with Urinary Catheters Dennis G. Maki* and Paul A. Tambyah *University of Wisconsin Medical School, Madison, Wisconsin, USA, and National University of Singapore
Engineering Out the Risk for Infection with Urinary Catheters Dennis G. Maki* and Paul A. Tambyah *University of Wisconsin Medical School, Madison, Wisconsin, USA, and National University of Singapore
healthcare associated infection 1.2
 healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
Don t Go With The Flow! Control and Management of UTIs in the Elderly
 Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth
 CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
CAUTI-The Challenge Continues IHA-Coalition for Care April 23, 2014 Presented by Linda Doerflein, BS, RN, CPHRM Director of Quality/Risk HealthSouth Deaconess Rehabilitation Hospital Did You Know?? The
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters
 Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW
 PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
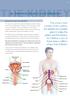 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
Rafael Carrion, MD Associate Professor of Urology University of South Florida School of Medicine
 Rafael Carrion, MD Associate Professor of Urology University of South Florida School of Medicine Prosthetics Most catastrophic complication is infection Original estimates were calculated: Virgin 3-5%
Rafael Carrion, MD Associate Professor of Urology University of South Florida School of Medicine Prosthetics Most catastrophic complication is infection Original estimates were calculated: Virgin 3-5%
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL
 A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
Controversies in Hospital Medicine: Antifungal Therapy. Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters
 Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
Catheter-associated urinary tract infections: diagnosis and prophylaxis
 International Journal of Antimicrobial Agents 24S (2004) S44 S48 Catheter-associated urinary tract infections: diagnosis and prophylaxis Paul A. Tambyah Division of Infectious Diseases, Department of Medicine,
International Journal of Antimicrobial Agents 24S (2004) S44 S48 Catheter-associated urinary tract infections: diagnosis and prophylaxis Paul A. Tambyah Division of Infectious Diseases, Department of Medicine,
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings
 Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
NURSE DRIVEN FOLEY CATHETER PROTOCOL
 NURSE DRIVEN FOLEY CATHETER PROTOCOL BACKGROUND There are over 1.7 million hospital-acquired infections in US hospitals annually, 40% of which are urinary tract infections. 80% of hospital-acquired UTIs
NURSE DRIVEN FOLEY CATHETER PROTOCOL BACKGROUND There are over 1.7 million hospital-acquired infections in US hospitals annually, 40% of which are urinary tract infections. 80% of hospital-acquired UTIs
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
Urinary Tract Infections
 Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
URINARY TRACT INFECTIONS IN YOUNG WOMEN
 URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: julkaisutilaukset@yths.fi Author:
URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: julkaisutilaukset@yths.fi Author:
Urinary Tract Infections. Clinical Scenario #1. Urinary Tract Infections. Clinical Scenario #1 : Labs
 Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Catheter-Associated Urinary Tract Infection (CAUTI) Definitions and Reporting
 AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
IDSA GUIDELINES Diagnosis, Prevention, and Treatment of Catheter- Associated Urinary Tract Infection in Adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America
UTI in children. Quick reference guide. Issue date: August 2007. Urinary tract infection in children: diagnosis, treatment and long-term management
 Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
Drug Sensitivity Pattern ofe. coli Causing Urinary Tract Infection in Diabetic and Non-diabetic Patients
 The Journal of International Medical Research 1996; 24: 296-301 in Diabetic and Non-diabetic Patients F JINNAH\ M S ISLAM\ M A K RUMI\ M G MORSHED 2 AND F H UQ3 'Department of Microbiology and Immunology,
The Journal of International Medical Research 1996; 24: 296-301 in Diabetic and Non-diabetic Patients F JINNAH\ M S ISLAM\ M A K RUMI\ M G MORSHED 2 AND F H UQ3 'Department of Microbiology and Immunology,
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS
 Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
Catheter Associated Urinary Tract Infections (CAUTI) TAKING PRECAU-TIONS Evidence-Based Practice in Prevention of Catheter Associated Urinary Tract Infections (CA-UTI) Catheter Associated Urinary Tract
Staphyloccus aureus sepsis: follow- up practice guidelines
 Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
Catheter Associated Urinary Tract Infection (CAUTI) Prevention. System CAUTI Prevention Team
 Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Catheter Associated Urinary Tract Infection (CAUTI) Prevention System CAUTI Prevention Team 1 Objectives At the end of this module, the participant will be able to: Identify risk factors for CAUTI Explain
Managing the E coli UTI
 C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
Nosocomial Urinary Tract Infections
 15 Nosocomial Urinary Tract Infections Sonia Isabel Cuervo Maldonado and Jorge Alberto Cortés Luna Universidad Nacional de Colombia, Bogotá Colombia 1. Introduction Healthcare-associated urinary infection
15 Nosocomial Urinary Tract Infections Sonia Isabel Cuervo Maldonado and Jorge Alberto Cortés Luna Universidad Nacional de Colombia, Bogotá Colombia 1. Introduction Healthcare-associated urinary infection
Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study. Medical Student Research Project.
 Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study Medical Student Research Project Jordan Knepper Faculty advisor: Mark Langsfeld, MD Introduction Background
Are Urinary Catheters necessary during Endovascular Procedures? A prospective randomized pilot study Medical Student Research Project Jordan Knepper Faculty advisor: Mark Langsfeld, MD Introduction Background
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
Usefulness of Urinary Catheterization in Patients Admitted to Infectious Ward of Sina Hospital, Tabriz, Iran
 http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 2, No. 4, October 2015, 106 110 eissn 2148-9696 Usefulness of Urinary Catheterization in Patients
http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 2, No. 4, October 2015, 106 110 eissn 2148-9696 Usefulness of Urinary Catheterization in Patients
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Pyelonephritis: Kidney Infection
 Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
State of Kuwait Ministry of Health Infection Control Directorate. Guidelines for Prevention of Surgical Site Infection (SSI)
 State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
MANAGEMENT OF CANDIDA INFECTIONS IN SURGICAL PATIENTS
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs)
 An APIC Guide 2008 Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs) Developing and Applying Facility-Based Prevention Interventions in Acute and Long-Term Care Settings
An APIC Guide 2008 Guide to the Elimination of Catheter-Associated Urinary Tract Infections (CAUTIs) Developing and Applying Facility-Based Prevention Interventions in Acute and Long-Term Care Settings
Principles of Disease and Epidemiology. Copyright 2010 Pearson Education, Inc.
 Principles of Disease and Epidemiology Pathology, Infection, and Disease Disease: An abnormal state in which the body is not functioning normally Pathology: The study of disease Etiology: The study of
Principles of Disease and Epidemiology Pathology, Infection, and Disease Disease: An abnormal state in which the body is not functioning normally Pathology: The study of disease Etiology: The study of
Understanding and Preventing Bladder Infections in Women
 Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM
 ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
2015 RN.ORG, S.A., RN.ORG, LLC
 Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Lower Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES
 APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
Probiotics for the Treatment of Adult Gastrointestinal Disorders
 Probiotics for the Treatment of Adult Gastrointestinal Disorders Darren M. Brenner, M.D. Division of Gastroenterology Northwestern University, Feinberg School of Medicine Chicago, Illinois What are Probiotics?
Probiotics for the Treatment of Adult Gastrointestinal Disorders Darren M. Brenner, M.D. Division of Gastroenterology Northwestern University, Feinberg School of Medicine Chicago, Illinois What are Probiotics?
Guideline for Prevention of Catheter-associated Urinary Tract Infections
 Guideline for Prevention of Catheter-associated Urinary Tract Infections Written by Edward S. Wong, M.D. In consultation with Thomas M. Hooton, M.D. WORKING GROUP Herbert W. Clegg II, M.D. Children's Hospital
Guideline for Prevention of Catheter-associated Urinary Tract Infections Written by Edward S. Wong, M.D. In consultation with Thomas M. Hooton, M.D. WORKING GROUP Herbert W. Clegg II, M.D. Children's Hospital
Sepsis Awareness Month
 Aon Kenya Insurance Brokers Ltd Aon Hewitt Healthcare Division Sepsis Awareness Month Issue 11 September 2015 In this Issue 2 Getting to understand Sepsis 3 Stages in Sepsis Advancement 4 Diagnosis & Treatment
Aon Kenya Insurance Brokers Ltd Aon Hewitt Healthcare Division Sepsis Awareness Month Issue 11 September 2015 In this Issue 2 Getting to understand Sepsis 3 Stages in Sepsis Advancement 4 Diagnosis & Treatment
PATIENT CARE MANUAL PROCEDURE
 PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PRIORITY RESEARCH TOPICS
 PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN NOSOCOMIAL INFECTIONS. SUMMARY.
 BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN NOSOCOMIAL INFECTIONS. SUMMARY. Bibliographical review on cost of Patient Safety Failings in nosocomial s. Summary This study has been conducted
BIBLIOGRAPHICAL REVIEW ON COST OF PATIENT SAFETY FAILINGS IN NOSOCOMIAL INFECTIONS. SUMMARY. Bibliographical review on cost of Patient Safety Failings in nosocomial s. Summary This study has been conducted
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
Health-Care Associated Infection Rates among Adult Patients in Bahrain Military Hospital: A Cross Sectional Survey
 Bahrain Medical Bulletin, Vol. 32, No. 1, March 2010 Health-Care Associated Infection Rates among Adult Patients in Bahrain Military Hospital: A Cross Sectional Survey Kelechi Austin Ofurum, M.Sc, B.Sc*,
Bahrain Medical Bulletin, Vol. 32, No. 1, March 2010 Health-Care Associated Infection Rates among Adult Patients in Bahrain Military Hospital: A Cross Sectional Survey Kelechi Austin Ofurum, M.Sc, B.Sc*,
URINE CULTURES GENERAL PROCEDURE
 University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
SURGICAL ANTIBIOTIC PROPHYLAXIS. Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc
 SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
The urinary tract is the most common
 PRINTER-FRIENDLY VERSION AT IDSE.NET Prevention and Management of Catheter- Associated UTIs DIANE K. NEWMAN, RNC, MSN, CRNP, FAAN Co-Director Penn Center for Continence and Pelvic Health University of
PRINTER-FRIENDLY VERSION AT IDSE.NET Prevention and Management of Catheter- Associated UTIs DIANE K. NEWMAN, RNC, MSN, CRNP, FAAN Co-Director Penn Center for Continence and Pelvic Health University of
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT
 Page 1 of 6 TITLE: PATIENTS CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT GUIDELINES: These are the 2011 Guidelines for the Treatment of Candida species infections in adult patients. These recommendations
Page 1 of 6 TITLE: PATIENTS CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT GUIDELINES: These are the 2011 Guidelines for the Treatment of Candida species infections in adult patients. These recommendations
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Develop an understanding of the differential diagnosis of pseudomembranous colitis
 Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey
 2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
Feline Lower Urinary Tract Disease (FLUTD)
 Feline Lower Urinary Tract Disease (FLUTD) VETERINARY GUIDE 2 What is FLUTD? FLUTD describes a collection of common conditions that affect the bladder and/or urethra the narrow tube that carries urine
Feline Lower Urinary Tract Disease (FLUTD) VETERINARY GUIDE 2 What is FLUTD? FLUTD describes a collection of common conditions that affect the bladder and/or urethra the narrow tube that carries urine
Antibiotic Prophylaxis for the Prevention of Infective Endocarditis and Prosthetic Joint Infections for Dentists
 PRACTICE ADVISORY SERVICE FAQ 6 Crescent Road, Toronto, ON Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Antibiotic Prophylaxis for the Prevention of Infective
PRACTICE ADVISORY SERVICE FAQ 6 Crescent Road, Toronto, ON Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Antibiotic Prophylaxis for the Prevention of Infective
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008
 Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D.
 ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
Urinary Tract Infection
 Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
Are venous catheters safe in terms of blood tream infection? What should I know?
 Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES
 & CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES Amela Dedeić-Ljubović*, Mirsada Hukić Institute of Clinical Microbiology, Clinical Centre of the University of
& CATHETER-RELATED URINARY TRACT INFECTION IN PATIENTS SUFFERING FROM SPINAL CORD INJURIES Amela Dedeić-Ljubović*, Mirsada Hukić Institute of Clinical Microbiology, Clinical Centre of the University of
