Immune checkpoint inhibitors in clinical trials
|
|
|
- Clara Fields
- 8 years ago
- Views:
Transcription
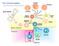
1 Chinese Journal of Cancer Review Immune checkpoint inhibitors in clinical trials Elad Sharon 1, Howard Streicher 1, Priscila Goncalves 2 and Helen X. Chen 1 Abstract Immunology-based therapy is rapidly developing into an effective treatment option for a surprising range of cancers. We have learned over the last decade that powerful immunologic effector cells may be blocked by inhibitory regulatory pathways controlled by specific molecules often called immune checkpoints. These checkpoints serve to control or turn off the immune response when it is no longer needed to prevent tissue injury and autoimmunity. Cancer cells have learned or evolved to use these mechanisms to evade immune control and elimination. The development of a new therapeutic class of drugs that inhibit these inhibitory pathways has recently emerged as a potent strategy in oncology. Three sets of agents have emerged in clinical trials exploiting this strategy. These agents are antibodybased therapies targeting cytotoxic T-lymphocyte antigen 4 (CTLA4), programmed cell death 1 (PD-1), and programmed cell death ligand 1 (PD-L1). These inhibitors of immune inhibition have demonstrated extensive activity as single agents and in combinations. Clinical responses have been seen in melanoma, renal cell carcinoma, non-small cell lung cancer, and several other tumor types. Despite the autoimmune or inflammatory immune-mediated adverse effects which have been seen, the responses and overall survival benefits exhibited thus far warrant further clinical development. Key words Immune checkpoints, PD-1, PD-L1, CTLA4, immunotherapy, immune modulators Immune checkpoints refer to regulatory pathways in the immunome that inhibit a portion of an active immune response against a specific target or set of targets [1]. Immune checkpoints are therefore seen as a normal part of the immune system s regulatory cascade and necessary to modulate and maintain immune homeostasis. These regulatory pathways are redundant, multifaceted, and complex (Figure 1). Their presence and evolutionary development are thought to reflect the fact that a normal immune response can also be potentially deadly to a host if not properly regulated, as evidenced by autoimmune disease. As immunotherapy has gained a foothold in the anticancer armamentarium, there is a commonly held belief among oncologists that cancers thwart these regulatory mechanisms to evade immune detection and continue their growth and spread. However, the whole picture is more complex. In many chronic infections, immune checkpoints are exploited by parasitic and viral Authors Affiliations: 1 Cancer Therapy Evaluation Program, Division of Cancer Treatment and Diagnosis, National Cancer Institute, Bethesda, MD 20892, USA; 2 Medical Oncology Service, Center for Cancer Research, National Cancer Institute, Bethesda, MD 20892, USA. Corresponding Author: Elad Sharon, 9609 Medical Center Drive, 5W502, Bethesda, MD 20892, USA. Tel: ; Fax: ; sharone@mail.nih.gov. doi: /cjc pathogens as evidenced by T-cell exhaustion in these conditions [2]. Cancer, however, arises from within the host. While some immune checkpoints are engaged to avoid immune-mediated eradication, others are merely a part of the normal immune response to stimuli. We are only beginning to understand these pathways. As a therapeutic class, drugs that inhibit these co-inhibitory signaling pathways, also known as immune checkpoint inhibitors, have emerged as a mainstay in melanoma therapy, with potential roles in the treatment of renal cell carcinoma (RCC), non small cell lung cancer (NSCLC), urothelial cancer, head and neck cancer, ovarian cancer, and various lymphomas [3-11]. In fact, ClinicalTrials. gov now lists dozens of trials with immune checkpoint inhibitors in a broad range of indications. As the targets of therapy are components of the immune system, there is currently no theoretical reason to exclude any potential histologies or tumor types from clinical evaluation. However, from a drug development perspective, this can be a challenge, as the resources are constantly constrained. It will be important to optimize the development of strategies to efficiently explore the therapeutic potentials. While a variety of agents could be deemed to interact with immune checkpoint inhibitors, the focus of this review are limited to the most advanced agents in clinical trials, those targeting the cytotoxic T-lymphocyte antigen 4 (CTLA4), programmed cell death CACA Chinese Anti-Cancer Association
2 (PD-1), and programmed cell death ligand 1 (PD-L1) pathway. The early trials involving CTLA4- and PD-1/PD-L1-targeting agents have shown how the addition of just one blocking antibody can reveal a hidden immune response, with potentially massive therapeutic benefit for patients. Immune modulators targeting other mechanisms (Table 1), such as indoleamine 2,3-dioxigenase (IDO) [12,13], lymphocyte-activation gene 3 (LAG3) [14], T-cell membrane protein 3 (TIM3) [15], signal transducer and activator of transcription 3 (STAT3) [16], glucocorticoid-induced tumor necrosis factor receptor (TNFR) familyrelated protein (GITR) [17], and agents against the human inhibitory killer IgG-like receptor (anti-kir) targeting natural killer (NK) cells have also entered the clinical trials arena [18-20]. Figure 1. Regulatory pathways in immuno-oncology. The immune system has multiple levels of co-stimulatory (shown in green) and co-inhibitory (shown in red) pathways, helping to maintain immune homeostasis in the midst of responding to antigenic stimulation. Antibodies blocking cytotoxic T-lymphocyte antigen 4 (CTLA4), programmed cell death 1 (PD-1), and programmed cell death ligand 1 (PD-L1) have shown remarkable clinical activity and further development is underway. Agonist antibodies, which directly interact with co-stimulatory pathways such as 41BB and CD40, are also in clinical development. Other means of affecting the immune responses are being explored, including direct actionon regulatory T (Treg) cells and natural killer (NK) cells. MHC, major histocompatibility complex; TCR, T-cell receptor. Table 1. Other immunotherapeutic agents in development Target Name Indication(s) Company Phase Clinical Trials.gov identifier (selected trials) B7.1 Galiximab Lymphoma Biogen Idec Phase II NCT B7H3 MGA271 Solid tumors Macrogenics Phase I NCT LAG3 IMP321 Solid tumors Immuntep Phase I/II NCT BMS Solid tumors Bristol-Myers Squibb Phase I NCT CD137 BMS Solid tumors Bristol-Myers Squibb Phase I/II NCT PF Lymphoma Pfizer Phase I NCT KIR IPH2101 Myeloma, AML Innate Pharma (BMS) Phase II NCT NCT CCR4 KW-0761 ATL, CTCL Kyowa Kirin Phase I/II NCT CD27 CDX-1127 Solid tumors & Heme CellDex Therapeutics Phase I NCT Ox40 MEDI-6469 Solid tumors MedImmune/AZ Phase I NCT CD40 CP-870,893 Pancreatic Genentech Phase I NCT Heme, hematologic tumors; ATL, acute T-cell leukemia; CTCL, cutaneous T-cell lymphoma; AML, acute myeloid leukemia. Chin J Cancer; 2014; Vol. 33 Issue 9 435
3 CTLA4 Inhibition and Human Cancers CTLA4 background CTLA4 is one of several co-inhibitory molecules that aid in modifying the T-cell response to antigen activation. The primary role of CTLA4 is to modify T-lymphocyte response to stimuli. CTLA4 regulates the clonal burst size during priming and secondary expansion, which is thought to be proportional to the activation strength of the complex formed by the T-cell receptor-major histocompatibility complex (TCR-MHC complex), both in terms of binding affinity and co-stimulation by accessory signals. CTLA4, also known as cluster of differentiation (CD) 152, is an inhibitory molecule found on T cells, and its counterpart is CD28. CD28 is a costimulatory signal, but it is important to note that CTLA4 has higher avidity for its ligands than CD28, which suggests a dominance of inhibitory signals in immune activation. The ligands for both CD28 and CTLA4 are known as B7 proteins, which are found on antigenpresenting cells (APCs). There are two types of B7 proteins: B7-1 (also known as CD80) and B7-2 (also known as CD86) [21,22]. In normal circumstances, T lymphocytes are thought to express CTLA4 on their surface immediately upon response to antigenic stimulation of TCR. Because a blocking antibody would attenuate the inhibitory signal, an anti-ctla4 antibody would appear to have a clear role in enhancing antitumor immunity, as the interaction of B7 with CD28 would thereby be enhanced. Indeed, in preclinical models, this is exactly what was seen [23]. However, B7 is rarely present in the tumor microenvironment, leading to a second hypothesis for how anti- CTLA4 antibodies may enhance immune-mediated tumor rejection [22]. CTLA4 is differentially expressed among separate T-lymphocyte subsets. Indeed, higher levels of surface expression of CTLA4 are seen in regulatory T cells (Treg cells) as compared with effector T cells (Teff cells). Researchers have established that higher Teff/ Treg ratios in both CD4-positive and CD8-positive tumor-infiltrating lymphocytes are associated with enhanced tumor eradication when CTLA4 blockade is employed in tumor models [24,25]. Other mechanisms of action involving Treg cells have been hypothesized. For example, Treg cells are known to reduce B7 expression on both human and animal APCs [26]. While B7 is thought to directly signal CTLA4, leading to its co-inhibitory effect, the reverse, or CTLA4 signaling to APCs via B7, also occurs. CTLA4 reverse signaling via B7 can lead to increased expression of IDO. IDO leads to a reduced level of local tryptophan stores in the microenvironment, which inhibits T-lymphocyte activation and proliferation [27]. Lastly, recently discovered alternatively spliced mrna molecules encode soluble CTLA4 molecules lacking transmembrane domains. These soluble inhibitors could also mediate immune suppression, either by down-regulating B7 expression as noted above or by blocking the potential interaction of B7 and the co-stimulatory molecule CD28 [28]. Ipilimumab The first anti-ctla4 agent in clinical development, ipilimumab, was approved by the United States Food and Drug Administration (FDA) and the European Medicines Agency for the treatment of metastatic melanoma following research showing improved survival [29]. Ipilimumab is a fully humanized immunoglobulin (Ig) G1 kappa monoclonal antibody that antagonizes CTLA4 and prevents ligand binding [30]. A phase III combination study of ipilimumab at 3 mg/kg with a glycoprotein 100 (gp100) peptide vaccine was conducted with 676 patients with stage III or IV unresectable melanoma, randomized in a 3:1:1 ratio. The results showed the median overall survival (OS) in the ipilimumab plus gp100 group was 10.0 months [95% confidence interval (CI), 8.5 to 11.5 months], as compared with 6.4 months (95% CI, 5.5 to 8.7 months) in the gp100 alone group [hazard ratio (HR) for death, 0.68; P < 0.001]. The median OS in the ipilimumab alone group was 10.1 months (95% CI, 8.0 to 13.8 months; HR for death with ipilimumab alone as compared with gp100 alone, 0.66; P = 0.003). Grade 3 or 4 immune-related adverse events occurred in 10% to 15% of patients treated with ipilimumab and in 3% of patients treated with gp100 alone. The investigators concluded that ipilimumab, with or without a gp100 peptide vaccine, as compared with gp100 alone, improved OS in patients with previously treated metastatic melanoma. Adverse events can be severe, long-lasting, or both, but most are reversible with appropriate treatment, particularly corticosteroids [29]. Another supportive study in metastatic melanoma involved 502 patients in a 1:1 randomized trial of ipilimumab at a dose of 10 mg/kg plus dacarbazine at a dose of 850 mg/m 2 of body surface area versus dacarbazine and placebo. The OS was longer in the group receiving ipilimumab-dacarbazine therapy than in the dacarbazine-placebo arm (11.2 months vs. 9.1 months). Survival rates were also higher for the ipilimumab-dacarbazine arm at 1 year (47.3% vs. 36.3%), 2 years (28.5% vs. 17.9%), and 3 years (20.8% vs. 12.2%), with an HR for death at 0.72 (P < 0.001). Grade 3 or 4 adverse events were recorded in 56.3% of patients in the experimental arm and only 27.5% in the control arm [31]. These findings further support the use of ipilimumab in metastatic melanoma. The preliminary results of the first adjuvant trial were reported at the 2014 Annual Meeting of the American Society of Clinical Oncology (ASCO). The European Organization for Research and Treatment of Cancer (EORTC) conducted a trial with 951 patients with stage III melanoma following complete resection (EORTC 18071, NCT ). Patients were randomized to receive ipilimumab at a dose of 10 mg/kg versus placebo every 3 weeks for 4 doses. The median relapse-free survival was 26.1 months for the ipilimumab arm and 17.1 months for the placebo arm, with an HR of 0.75 (95% CI, 0.64 to 0.90; P = 0.001). The adverse event profile was thought to be generally consistent with that seen in advanced melanoma, but a higher incidence of endocrinopathies were reported [32]. While the results were largely seen as positive, there are still unresolved issues that may limit the ability of regulatory agencies to approve ipilimumab in the adjuvant setting. In particular, patients with stage III melanoma have the option of high-dose interferon, which is the standard of care in the United States [33]. In addition, as noted above, the dose chosen in EORTC trial was 10 mg/kg of ipilimumab, higher than the dose used in the metastatic setting. 436 Chin J Cancer; 2014; Vol. 33 Issue 9 Chinese Journal of Cancer
4 Another large adjuvant trial, E1609 (NCT ), addresses the questions of the optimal dose of ipilumumab and its comparative effectiveness to high-dose interferon. In this trial, conducted by the Eastern Cooperative Oncology Group (ECOG) under the sponsorship of the United States National Cancer Institute (NCI), 1,500 patients with stage III or IV melanoma that has been fully resected are randomized to three arms: high-dose interferon, ipilimumab at 3 mg/ kg, and ipilimumab at 10 mg/kg [30]. The trial is close to completing accrual and the outcome data are eagerly awaited. Other indications with ipilimumab are still under clinical development. On ClinicalTrials.Gov, a search with the term ipilimumab returns 191 trials, over 100 of which remain open. Much of the attention in ipilimumab clinical development has moved to combination therapy, particularly with the anti-pd-1 agent nivolumab. The development of ipilumumab brought up interesting questions about the best endpoints of efficacy assessment for this class of agents. In the phase III melanoma trials with ipilimumab described above, improvements in OS seen in the metastatic setting were not accompanied by significant radiographic responses to therapy. This has complicated efficient drug development, as response rate is less likely to serve as a readout of efficacy, at least when ipilimumab is used as a monotherapy. Monotherapy is still being explored in various settings, however. In one example, in a single institution case series, 5 patients with recurrent glioblastoma multiforme (GBM) who were treated with ipilimumab were followed. Patients had time to progression ranging from 1 to 6 months, and 1 patient remains recurrence-free 19 months after therapy, suggesting penetration of this drug across the blood-brain barrier [34]. Currently, there are no biomarkers to predict which patients or tumor types are more likely to respond to anti-ctla4 therapies. Some analysis suggested that a high mutational load may be associated with a clinical benefit from ipilimumab. In particular, one group of researchers has focused on identifying a neoantigen signature that correlates with benefit. Findings are preliminary, but this suggests that tumor genetics might explain the divergent outcomes among patients treated with ipilimumab [35]. Tremelimumab Tremelimumab (formerly CP-675,206) is a human IgG2 monoclonal antibody specific for CTLA4. In a large, single-arm phase II trial, 241 response-evaluable patients with advanced refractory or relapsed melanoma were treated at a dose of 15 mg/kg intravenously every 3 months. Objective responses were observed in 6.6% of those patients, which led to a phase III trial in a similar patient population [36]. In the phase III trial in advanced melanoma, 655 patients were enrolled and randomly assigned to treatment with tremelimumab or chemotherapy. Median OS by intent to treat was 12.6 months (95% CI, 10.8 to 14.3 months) for tremelimumab and 10.7 months (95% CI, 9.36 to months) for chemotherapy (HR, 0.88; P = 0.127). Of note, while objective response rates were similar in the two arms (10.7% in the tremelimumab arm and 9.8% in the chemotherapy arm), duration of response was significantly longer among patients treated with tremelimumab (35.8 months vs months, P = ) [37]. Regardless, the study failed to demonstrate a statistically significant survival advantage of treatment with the investigational drug over standard-of-care chemotherapy. While the results were disappointing, there was a possibility that the dosing schedule of tremelimumab (once every 3 months) was insufficient to achieve results similar to that of ipilimumab. As a result, ongoing efforts with tremelimumab as a monotherapy have used more frequent dosing. The preferred dose and schedule for tremelimumab for ongoing trials has generally been 10 mg/kg intravenously, every 4 weeks for 6 months. A phase II, single-arm study of tremelimumab as a second-line treatment was conducted with 29 patients with malignant mesothelioma. Results showed a partial response in 4 patients (13.8%) and stable disease in 11 patients (37.9%), with OS of 11.5 months [38]. As a result, a phase III, double-blinded, randomized trial is currently underway using tremelimumab in mesothelioma [39]. Tremelimumab is also being tested in various combinations in a variety of other tumor types. PD-1/PD-L1 Inhibition and Human Cancers PD-1/PD-L1 background Compared to the limited development with CTLA4, there is an immense level of interest and investment by pharmaceutical companies in the PD-1/PD-L1 pathway (Table 2). Seven major companies have entered the fray, with multiple phase III registration trials already underway in a variety of malignancies, most notably melanoma, RCC, and NSCLC (Table 3). This enthusiasm is justified, as clinical trial results thus far confirm that targeting the PD-1/PD- L1 pathway represents the most exciting opportunity for advancing cancer immunotherapy to date. Whereas CTLA4 is involved in central tolerance and control, the PD-1 receptor is critical in peripheral tolerance. PD-1 is expressed on T lymphocytes during thymic development. Similar to CTLA4, PD-1 becomes expressed on CD4- and CD8-positive T lymphocytes during antigenic stimulation, serving as a co-inhibitory signal. In addition, PD-1 is expressed on numerous other immune cells, including natural killer T cells, B cells, monocytes, and certain dendritic cell subsets [40,41]. PD-1 has two main ligands, namely PD-L1 (also known as B7-H1) and PD-L2 (also known as B7-DC). While PD-L2 has a much higher affinity for PD-1, it is expressed chiefly on activated dendritic cells, macrophages, certain B-cell subsets, and other immune cells. PD-L1 is more widely expressed on hematologic and non-hematologic tissues [1]. As a co-inhibitory signal, PD-1 engagement results in reduced cytokine production, cytolytic activity, and lymphocyte proliferation [41]. PD-1 is up-regulated in T lymphocytes following viral infections and down-regulated following viral clearance. In chronic viral infections, however, CD8-positive T lymphocytes express PD-1 constitutively, likely through gene demethylation, contributing to what has been termed a T-cell exhaustion phenotype. In human immunodeficiency virus (HIV) infection, for example, high levels of PD-1 expression allow for persistent interaction between PD-L1 expressed by APCs Chin J Cancer; 2014; Vol. 33 Issue 9 437
5 Table 2. Agents targeting PD-1/PD-L1 in clinical development Company Agent targeting PD-1 Agent targeting PD-L1 Bristol-Myers Squibb BMS /MDX-1106 BMS /MDX-1105 (fully human IgG4 mab) Nivolumab (fully human IgG4 mab) CureTech CT-011 N/A Pidilizumab (humanized IgG1 mab) Genentech N/A MPDL3280A (IgG1 mab, Fc modified) MedImmune/AZ AMP-514 MEDI4736 (fully human mab) Merck MK-3475 N/A Pembrolizumab (humanized IgG4 mab) EMD Serono N/A MSB C Aurigene and Pierre Fabre AUNP 12 (peptide) N/A PD-1, programmed death 1 receptor; PD-L1, programmed cell death ligand 1; IgG4, immunoglobulin G4; mab, monoclonal antibody; N/A, not available. Table 3. Selected ongoing PD-1/PD-L1 trials in melanoma, renal cell cancer (RCC), and non small cell lung cancer (NSCLC) Sponsor Tumor Setting Phase Comparison Primary endpoint Sample size ORR, overall response rate; OS, overall survival; PFS, progression-free survival; ipi, ipilumumab. Other footnotes as in Table 2. Primary Clinical trials. completion date gov identifier Bristol-Myers Squibb Melanoma 1st-line II Ipilimumab +/ nivolumab ORR 150 Jul 2014 NCT Bristol-Myers Squibb NSCLC 3rd-line squamous cell II Nivolumab vs. docetaxel OS 264 Jan 2016 NCT Bristol-Myers Squibb NSCLC 2nd-/3rd-line nonsquamous III Nivolumab vs. docetaxel OS 582 May 2015 NCT cell Merck Melanoma 1st-/2nd-line (ipi-naïve) III Pembrolizumab vs. OS & PFS 645 Feb 2015 NCT ipilimumab Merck Melanoma 2nd-line II Pembrolizumab vs. OS & PFS 510 Mar 2015 NCT chemotherapy Bristol-Myers Squibb Melanoma 2nd-line post-ipi III Nivolumab vs. OS 405 May 2015 NCT chemotherapy Merck NSCLC 2nd-line II/III Pembrolizumab vs. OS & PFS 920 Sep 2015 NCT docetaxel Bristol-Myers Squibb Melanoma 1st-/2nd-line III Nivolumab vs. OS 410 Sept 2015 NCT chemotherapy Bristol-Myers Squibb RCC 2nd- to 4th-line III Nivolumab vs. everolimus OS 822 Feb 2016 NCT Genentech NSCLC 2nd-line II MPDL3280A vs. docetaxel OS 287 Mar 2016 NCT Bristol-Myers Squibb Melanoma 1st-line III Ipilimumab +/ nivolumab OS 915 Oct 2016 NCT Genentech NSCLC 2nd-line III MPDL3280A vs. docetaxel OS 850 Jun 2017 NCT AstraZeneca NSCLC 1st-line after concurrent III MEDI4736 vs. placebo OS & PFS 702 May 2017 NCT (stage III) chemoradiation and subsequent T-cell dysfunction. T-lymphocyte activation is essentially blocked in this setting. In an experiment using B cells from HIV-infected individuals, researchers were able to show increased responses to HIV antigens in the presence of PD-1 blocking antibodies in vitro [42]. This suggests that an active immune response can be induced if effective blockade of the PD-1/PD-L1 pathway can be implemented. A clinical trial sponsored by the US National Institutes of Health is currently planned to investigate that possibility using the anti-pd-l1 antibody, BMS (NCT ). Similarly, tumors use the same pathway, meant to induce peripheral immune tolerance, to evade T-lymphocyte-mediated immune eradication. Tumors evading an active immune response are thought to express PD-L1 following T lymphocyte infiltration and expression of interferon-gamma. Expression of PD-L1 has been associated with a poor prognosis in a wide variety of human tumors [11,43-51]. Interestingly, in one analysis of glioma cases, a better 438 Chin J Cancer; 2014; Vol. 33 Issue 9 Chinese Journal of Cancer
6 prognosis was seen in patients whose tumor-adjacent brain tissue expressed PD-L1 and whose tumors did not express PD-L1. This suggests a general role for PD-L1 in protecting normal tissue from immune attack, though it would be important to see these findings replicated elsewhere and in other tumor types [52]. In general, the results of PD-1/PD-L1 blockade have been encouraging. Higher response rates and durable responses were seen with PD-1/PD-L1 blocking antibodies than with CTLA4 blockade in melanoma, RCC, and unexpectedly, NSCLC. In addition, although similar immune-mediated adverse events were seen with both CTLA4 and PD-1/PD-L1 agents, the severity of adverse events has generally been lower, with the caveat that fatal pneumonitis was seen in 1% of the patients on the nivolumab phase I trial described below [53]. PD-1-targeting agents Nivolumab Nivolumab (BMS ) is a fully human IgG4 monoclonal antibody targeting PD-1. A phase I/II study was reported in 2012 in the New England Journal of Medicine in parallel with a plenary session at the 2012 ASCO Annual Meeting [53]. Patients on the trial had advanced melanoma, NSCLC, castration-resistant prostate cancer, RCC, or colorectal cancer (CRC). Patients received nivolumab at doses of 0.1 to 10.0 mg/kg of body weight every 2 weeks for up to 12 cycles until disease progression or a complete response occurred. Of the 296 patients enrolled, only 14% experienced grade 3 or 4 drug-related adverse events, but there were 3 deaths from pulmonary toxicity. No maximum tolerated dose (MTD) was defined. Cumulative response rates (all doses) were 18.4% (14/76) among patients with NSCLC, 27.6% (26/94) among patients with melanoma, and 27.3% (9/33) among patients with RCC [53]. A subsequent analysis of the 104 patients in that trial with metastatic melanoma was performed. The investigators reported that the median OS in nivolumab-treated metastatic melanoma patients was 16.8 months, and 1- and 2-year survival rates were 62% and 43%, respectively. Among the 33 patients (30.8%) with objective tumor regressions, the Kaplan-Meier estimated median response duration was 2 years. Of note, responses were not observed in prostate cancer and colon cancer patients on the trial [54]. While preliminary results from the phase I/II trial suggested that PD-L1 could be an appropriate biomarker for patient selection, subsequent analyses have shown numerous PD-L1-negative patients had responded to treatment with nivolumab, although lower rates are seen. Given the variability and limitation of the available PD-L1 assays, a true absence of PD-L1 expression in those patients cannot be confirmed. At this time it remains to be determined whether PD-L1 is a predictive marker of response for PD-1 pathway inhibitors. At the 2014 ASCO Annual Meeting, preliminary results of other nivolumab clinical trials were reported. In a small dose-escalation trial in Japan, 3 of 13 patients with platinum-resistant ovarian cancer had objective responses to nivolumab. The initial 10 patients were treated at a dose of 1 mg/kg, and 2 responders were from that cohort. The subsequent cohort that received 3 mg/kg had only 3 patients, but 1 was a responder. These results, though preliminary, were promising [3]. In addition, investigators reported early results using nivolumab at a dose of 3 mg/kg every 2 weeks in patients with treatment-naïve advanced NSCLC. The initial results on 20 patients revealed an objective response rate of 30%. Two patients had a greater than 80% target lesion reduction at 18 weeks. Of the 15 evaluable tumor samples, 9 were PD-L1-positive (defined as greater than 5% PD- L1 expression using a Dako kit), and the response rate was 67% in PD-L1-positive patients; whereas no responses were observed in the 6 PD-L1-negative patients [55]. Combinations of nivolumab with conventional chemotherapy or epidermal growth factor receptor (EGFR) inhibitors were also reported, but results are difficult to interpret in the absence of randomized comparisons [56,57]. Pembrolizumab Pembrolizumab (MK-3475, formerly lembrolizumab) is a humanized IgG4 monoclonal antibody targeting PD-1. Pembrolizumab has been very successful in treating melanoma and NSCLC, similar to nivolumab. Significant differences cannot be assessed in the absence of a randomized trial comparing the two agents. However, binding affinities of the agents are different. Nivolumab is a fully human IgG4, and pembrolizumab is humanized. In phase I trials, neither agent has been found to have a maximally tolerated dose. That said, more time and energy has been spent on searching for an appropriate dose for pembrolizumab. In the first major publication involving pembrolizumab, Hamid et al. [58] reported that patients with advanced melanoma were analyzed after being treated with three separate dosing strategies: 10 mg/ kg of body weight every 2 or 3 weeks or 2 mg/kg every 3 weeks. Ultimately, 135 patients with advanced melanoma were treated. Adverse events were similar to those found in patients treated with nivolumab, including fatigue, rash, pruritus, and diarrhea. Response rates across all dose levels were 38% (95% CI, 25% to 44%). Investigators found no difference among those with and without prior ipilimumab therapy. Responses were durable, and the median progression-free survival (PFS) among the 135 patients was longer than 7 months [58]. A subsequent prospective, randomized analysis was performed using both the 2 mg/kg and the 10 mg/kg doses, given every 3 weeks to patients with ipilimumab-refractory advanced melanoma. There were 89 patients in the 2 mg/kg cohort and 84 patients in the 10 mg/kg cohort. The response rate was 26% at both doses. Safety profiles were similar and there were no deaths reported [59]. Other attempts to analyze patients with melanoma have been reported, including an analysis of 411 melanoma patients treated across multiple dose levels and multiple trials, which was reported at the 2014 ASCO Annual Meeting. Median OS data was not available, but 1-year OS rate over all dose cohorts was 71%. Response rates were encouraging as well, ranging from 26% to 57%, varying based on ipilimumab prior treatment, dose, and schedule [60]. Investigators also reported preliminary results of a phase I trial of previously treated patients with locally advanced or metastatic NSCLC. Enrolled patients with PD-L1 detected in their tumors by a preliminary immunohistochemical assay were randomized to pembrolizumab at a dose of 10 mg/kg every 2 weeks or every Chin J Cancer; 2014; Vol. 33 Issue 9 439
7 3 weeks. In addition, some patients with tumors without PD-L1 expression who had received at least two prior lines of therapy were treated at a dose of 10 mg/kg every 2 weeks. Ultimately, 102 patients comprised the every-2-week cohort (including 43 whose tumors did not express PD-L1), and 119 patients comprised the every-3-week cohort. Investigators reported that 48% of patients experienced drugrelated adverse events, with 6% experiencing grade 3/4 adverse events. As in the nivolumab trial reported above, pneumonitis was a concern, with 3 cases of drug-related grade 3/4 pneumonitis. The Response Evaluation Criteria in Solid Tumors (RECIST) response rate in all patients was 21%. The response rate was slightly higher (24%) for patients with PD-L1-positive tumors (more specifically, 31% on the every-2-week cohort and 22% on the every-3-week cohort). RECIST response rates were 8% for patients without PD-L1 expression [61]. Pidilizumab Pidilizumab is a humanized IgG1 antibody targeting PD-1. The agent was initially evaluated in a phase I trial targeting hematologic malignancies. Presently, there are a number of clinical trials underway in both hematologic and solid tumors [62]. The results of two pidilizumab clinical trials were recently published in peer-reviewed journals. In a single-center, single-arm, phase II trial, 32 patients with relapsed follicular lymphoma received pidilizumab at a dose of 3 mg/kg every 4 weeks for 4 infusions with up to 8 additional infusions administered. In addition, rituximab was given at a dose of 375 mg/m 2 of body surface area every week for 4 weeks. Investigators reported that 19 of 29 evaluable patients achieved an objective response, with complete responses in 15 patients (51.7%) [63]. An additional phase II trial involved patients with diffuse large B-cell lymphoma (DLBCL) following autologous hematologic stem cell transplantation (AHSCT). Sixty-six patients were treated with 3 doses of pidilizumab in the first 1 to 3 months after AHSCT. The PFS rate was 72% at 6 months after AHSCT (90% CI, 60% to 82%), meeting the primary endpoint. Thirty-five patients had measurable disease following AHSCT, and the response rate in those patients was 51% [7]. Investigators also presented results on the use of pidilizumab in metastatic melanoma at the 2014 ASCO Annual Meeting. In this trial, 103 patients were randomized in a 1:1 ratio to receive either 1.5 mg/kg or 6 mg/kg every 2 weeks for 27 doses. Response rates were lower than those observed in patients treated with other PD- 1-targeting agents, but the OS rate at 12 months was 64.5% (90% CI, 55.6% to 72.0%). No significant differences were seen between different strata or dose groups [64]. PD-L1-targeting agents MPDL3280A MPDL3280A is an engineered human IgG1 monoclonal antibody that targets PD-L1. Of note, MPDL3280A was engineered to eliminate antibody-dependent cell-mediated cytotoxicity (ADCC) effector function. As a result, MPDL3280A, unlike some other anti-pd-l1 antibodies, does not deplete cells expressing PD-L1. Phase I results and data from multiple expansion cohorts in a variety of histologies were presented at the 2013 ASCO Annual Meeting. Pharmacokinetic data supported dosing at 15 mg/kg every 3 weeks or a fixed dose equivalent, as no maximally tolerated dose was defined. Patients were treated for up to 1 year [65]. In an expansion cohort for previously treated patients with metastatic NSCLC, 52 subjects were enrolled and treated at a dose of 15 mg/ kg. Of note, 62% of those patients had heavily pretreated NSCLC with more than 3 prior treatments. The response rate was 22% [66]. Similar results were seen in a RCC cohort, in which the response rate was 13% (6/47) [67]. In patients with metastatic melanoma treated in the phase I portion of the trial, the response rate was 26% (9 of 35 patients) [68]. In all of the above cohorts, patients were analyzed for PD-L1 status, and a correlation between PD-L1 status and efficacy was observed. Early results from patients with other tumor histologies were also considered promising [69]. At the 2014 ASCO Annual Meeting, investigators presented preliminary data from a clinical trial involving patients with metastatic bladder cancer. Patients were divided into PD-L1-positive and PD- L1-negative cohorts, based on an analysis of the PD-L1 expression of immune-infiltrating cells within tumor specimens. In the PD- L1-positive cohort, 20 patients were enrolled, and of those, 10 responded to therapy (9 partial responses and 1 complete response). Response rates for patients with PD-L1-negative tumors have yet to be published [5]. MEDI4736 MEDI4736 is a human IgG1 monoclonal antibody recognizing human PD-L1. It is similar to MPDL3280A, as the molecule also has mutations in the Fc receptor, which therefore eliminates complementmediated cytotoxicity and ADCC [70]. Results from early clinical trials are still pending. A phase I dose of 10 mg/kg every 2 weeks is currently being evaluated in several histologies in an expansion phase [71]. Of note, at the 2014 ASCO Annual Meeting, investigators reported the preliminary results of 13 NSCLC patients treated with MEDI4736, with 3 partial responses already observed [72]. Several large combination trials in lung cancers are ongoing. MSB C MSB C is a fully human IgG1 monoclonal antibody targeting PD-L1. As opposed to the PD-L1-targcting agents from Genentech and MedImmune/AstraZeneca, MSB C has a native Fc receptor, allowing for ADCC. Results from a phase I trial with the agent were reported at the 2014 ASCO Annual Meeting [66]. Twenty-seven patients with relapsed cancers were treated. No maximally tolerated dose was determined, and the investigators demonstrated that MSB C could be safely administered in doses up to 20 mg/kg every 2 weeks. Further clinical trials are planned in a variety of tumors. Combinations of Immunotherapeutic Agents In spite of the promising single agent indications mentioned 440 Chin J Cancer; 2014; Vol. 33 Issue 9 Chinese Journal of Cancer
8 above, a majority of patients will not respond to immune checkpoint inhibition in the histologies tested thus far. The need for newer combination strategies has become obvious. Early in the development of anti-ctla4 antibodies, there was an effort to combine these therapies with high-dose interferon in order to take advantage of the immunomodulatory effects already noted in advanced melanoma. In one such trial, tremelimumab was administered at a dose of 15 mg/kg every 12 weeks while high-dose interferon was administered concurrently in standard doses, involving U/m 2 of body surface area for 5 days a week, followed by maintenance interferon at a dose of U/m 2 of body surface area subcutaneously 3 times a week for 8 weeks. Thirty-six patients were ultimately enrolled. Of the 33 evaluable patients, there were 3 complete responses and 7 partial responses. The median OS was 15.9 months [36]. A similar trial with ipilimumab and high-dose interferon is currently enrolling patients (NCT ). A randomized phase II trial of ipilumumab investigated the potential synergy of adding granulocyte macrophage colonystimulating factor (GM-CSF, or sargramostim) with ipilumumab [73]. In this trial, patients with metastatic melanoma were randomized to either ipilumumab alone at a dose of 10 mg/kg every 3 weeks for 4 cycles followed by maintenance of ipilimumab every 12 weeks or to the same dose and schedule of ipilumumab in addition to GM-CSF at 250 μg subcutaneously on days 1-14 of 21-day cycles for 4 cycles. Toxicity and response rates did not differ significantly between the two arms. However, the median OS in the combination arm was 17.5 months versus 12.7 months in the ipilimumab alone arm, which was shown to translate to a 36% reduction in mortality risk (P = 0.014). Of note, there were 2 grade 5 adverse events in the combination arm and 7 grade 5 events in the ipilumumab alone arm, suggesting the possibility that GM-CSF improved the tolerability of ipilimumab therapy. One area of remarkable success involved the use of nivolumab and ipilimumab in patients with metastatic melanoma. In the first trial combining these two immune checkpoint inhibitors, 53 patients received concurrent therapy with nivolumab and ipilimumab, and 33 received sequenced treatment. Among all patients enrolled who received concurrent treatment, the response rate was 40%. In the concurrent arm using 3 mg of ipilimumab and 1 mg of nivolumab every 3 weeks, 53% of patients had an objective response, and all of those responding in that arm showed a tumor reduction of 80% References [[1] Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer, 2012,12: [2] Hotchkiss RS, Moldawer LL. Parallels between cancer and infectious disease. N Engl J Med, 2014,371: [3] Hamanishi J, Mandai M, Ikeda T, et al. Efficacy and safety of anti- PD-1 antibody (Nivolumab: BMS , ONO-4538) in patients with platinum-resistant ovarian cancer. J Clin Oncol, 2014,32 suppl: abstr [4] Seiwert TY, Burtness B, Weiss J, et al. A phase Ib study of MK in patients with human papillomavirus (HPV)-associated and non-hpv-associated head and neck (H/N) cancer. J Clin Oncol, or more. Grade 3 or 4 adverse events related to therapy occurred in 53% of patients in the concurrent treatment cohort. In the sequenced cohort, 18% of patients had grade 3 or 4 adverse events and a response rate of 20% was reported [74]. The combination of ipilimumab and nivolumab has subsequently been evaluated in a variety of malignancies. In RCC, two variations of the combination were tested. In the arm with nivolumab at a dose of 3 mg/kg and ipilimumab at a dose of 1 mg/kg, 21 patients were treated, and there were 6 objective responses and 7 patients with stable disease. In the arm with nivolumab at a dose of 1 mg/kg and ipilimumab at a dose of 3 mg/kg, 23 patients were treated, and there were 9 objective responses and 9 patients with stable disease [75]. The same regimen was evaluated in NSCLC, with disappointing results. Fewer responses were reported, in part due to early treatment discontinuation caused by adverse events. Further safety evaluations are now underway at lower doses (1 mg/kg of ipilimumab and 1 mg/kg of nivolumab) [76]. This stresses the need for investigators to carefully tailor regimens to specific patient populations. It is clear that the number and severity of co-morbidities, average age of patients, and number and intensity of prior treatments may alter the suitability of a given immunotherapy. A number of other combinations among immunotherapeutic agents are currently underway or planned. Time will tell if the remarkable successes of the combinations noted above will be replicated when other immunotherapeutic agents are used in combination. Conclusions Immunotherapy for cancer was declared to be the breakthrough of the year in 2013 as a result of the significant advances seen and described above [77]. While much has been accomplished, more still needs to be done. A wide variety of important clinical and scientific questions must be addressed efficiently to significantly benefit patients and to improve understanding of the interactions of tumor biology and human immunology. If translational scientists and clinical investigators work together to solve these problems, what is now thought to be the breakthrough of the year can soon be thought of as the medical breakthrough of the century. Received: ; accepted: ,32 suppl:abstr [5] Powles T, Vogelzang NJ, Fine GD, et al. Inhibition of PD-L1 by MPDL3280A and clinical activity in pts with metastatic urothelial bladder cancer (UBC). J Clin Oncol, 2014,32 suppl:abstr [6] Bachy E, Coiffier B. Anti-PD1 antibody: a new approach to treatment of lymphomas. Lancet Oncol, 2014,15:7-8. [7] Armand P, Nagler A, Weller EA, et al. Disabling immune tolerance by programmed death-1 blockade with pidilizumab after autologous hematopoietic stem-cell transplantation for diffuse large B-cell lymphoma: results of an international phase II trial. J Clin Oncol, 2013,31: Chin J Cancer; 2014; Vol. 33 Issue 9 441
9 [8] Malas S, Harrasser M, Lacy KE, et al. Antibody therapies for melanoma: new and emerging opportunities to activate immunity. Oncol Rep, [Epub ahead of print] [9] Srivastava N, McDermott D. Update on benefit of immunotherapy and targeted therapy in melanoma: the changing landscape. Cancer Manage Res, 2014,6: [10] Sundar R, Soong R, Cho BC, et al. Immunotherapy in the treatment of non-small cell lung cancer. Lung Cancer, 2014,85: [11] Gunturi A, McDermott DF. Potential of new therapies like anti-pd1 in kidney cancer. Curr Treat Options Oncol, 2014,15: [12] Kennedy E, Rossi GR, Vahanian NN, et al. Phase 1/2 trial of the indoleamine 2,3-dioxygenase pathway (IDO) inhibitor indoximod plus ipilimumab for the treatment of unresectable stage 3 or 4 melanoma. J Clin Oncol, 2014,32 suppl:abstr TPS9117. [13] Khleif S, Munn D, Nyak-Kapoor A, et al. First-in-human phase 1 study of the novel indoleamine-2,3-dioxygenase (IDO) inhibitor NLG-919. J Clin Oncol, 2014,32 suppl:abstr TPS3121. [14] Wang-Gillam A, Plambeck-Suess S, Goedegebuure P, et al. A phase I study of IMP321 and gemcitabine as the front-line therapy in patients with advanced pancreatic adenocarcinoma. Invest New Drugs, 2013,31: [15] Ferris RL, Lu B, Kane LP. Too much of a good thing? Tim-3 and TCR signaling in T cell exhaustion. J Immunol, 2014,193: [16] Ok CY, Chen J, Xu-Monette Z, et al. Clinical implications of phosphorylated STAT3 expression in de novo diffuse large B-cell lymphoma. Clin Cancer Res, [Epub ahead of print] [17] Lu L, Xu X, Zhang B, et al. Combined PD-1 blockade and GITR triggering induce a potent antitumor immunity in murine cancer models and synergizes with chemotherapeutic drugs. J Transl Med, 2014,12:36. [18] Benson DM Jr, Hofmeister CC, Padmanabhan S, et al. A phase 1 trial of the anti-kir antibody IPH2101 in patients with relapsed/ refractory multiple myeloma. Blood, 2012,120: [19] Vey N, Bourhis JH, Boissel N, et al. A phase 1 trial of the antiinhibitory KIR mab IPH2101 for AML in complete remission. Blood, 2012,120: [20] Kohrt HE, Thielens A, Marabelle A, et al. Anti-KIR antibody enhancement of anti-lymphoma activity of natural killer cells as monotherapy and in combination with anti-cd20 antibodies. Blood, 2014,123: [21] Linsley PS, Brady W, Grosmaire L, et al. Binding of the B cell activation antigen B7 to CD28 costimulates T cell proliferation and interleukin 2 mrna accumulation. J Exp Med, 1991,173: [22] Blank CU, Enk A. Therapeutic use of anti-ctla-4 antibodies. Int Immunol, [Epub ahead of print] [23] Leach DR, Krummel MF, Allison JP. Enhancement of antitumor immunity by CTLA-4 blockade. Science, 1996,271: [24] Quezada SA, Peggs KS, Curran MA, et al. CTLA4 blockade and GM-CSF combination immunotherapy alters the intratumor balance of effector and regulatory T cells. J Clin Invest, 2006,116: [25] Curran MA, Montalvo W, Yagita H, et al. PD-1 and CTLA-4 combination blockade expands infiltrating T cells and reduces regulatory T and myeloid cells within B16 melanoma tumors. Proc Natl Acad Sci U S A, 2010,107: [26] Qureshi OS, Zheng Y, Nakamura K, et al. Trans-endocytosis of CD80 and CD86: a molecular basis for the cell-extrinsic function of CTLA-4. Science, 2011,332: [27] Grohmann U, Orabona C, Fallarino F, et al. CTLA-4-Ig regulates tryptophan catabolism in vivo. Nat Immunol, 2002,3: [28] Magistrelli G, Jeannin P, Herbault N, et al. A soluble form of CTLA- 4 generated by alternative splicing is expressed by nonstimulated human T cells. Eur J Immunol, 1999,29: [29] Hodi FS, O Day SJ, McDermott DF, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med, 2010,363: [30] Tarhini AA, Thalanayar PM. Melanoma adjuvant therapy. Hematol Oncol Clin North Am, 2014,28: [31] Robert C, Thomas L, Bondarenko I, et al. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med, 2011,364: [32] Eggermont AM, Chiarion-Sileni V, Grob JJ, et al. Ipilimumab versus placebo after complete resection of stage III melanoma: initial efficacy and safety results from the EORTC phase III trial. J Clin Oncol, 2014,32 suppl:abstr LBA9008. [33] Kirkwood JM, Strawderman MH, Ernstoff MS, et al. Interferon alfa- 2b adjuvant therapy of high-risk resected cutaneous melanoma: the Eastern Cooperative Oncology Group Trial EST J Clin Oncol, 1996,14:7-17. [34] Hu JL, Sharma P, Yu J, et al. Ipilimumab for recurrent glioblastoma: a single-institution case series. J Clin Oncol, 2014,32 suppl:abstr e [35] Snyder Charen A, Makarov V, Merghoub T, et al. The neoantigen landscape underlying clinical response to ipilimumab. J Clin Oncol, 2014,32 suppl:abstr [36] Kirkwood JM, Lorigan P, Hersey P, et al. Phase II trial of tremelimumab (CP-675,206) in patients with advanced refractory or relapsed melanoma. Clin Cancer Res, 2010,16: [37] Ribas A, Kefford R, Marshall MA, et al. Phase III randomized clinical trial comparing tremelimumab with standard-of-care chemotherapy in patients with advanced melanoma. J Clin Oncol, 2013,31: [38] Calabro L, Morra A, Fonsatti E, et al. A phase 2 single-arm study with tremelimumab at an optimized dosing schedule in second-line mesothelioma patients. J Clin Oncol, 2014,32 suppl:abstr [39] Maio M, Scherpereel A, Di Pietro A, et al. Randomized, doubleblind, placebo-controlled study of tremelimumab for secondand third-line treatment of unresectable pleural or peritoneal mesothelioma. J Clin Oncol, 2014,32 suppl:abstr TPS7609. [40] Francisco LM, Sage PT, Sharpe AH. The PD-1 pathway in tolerance and autoimmunity. Immunol Rev, 2010,236: [41] Pedoeem A, Azoulay-Alfaguter I, Strazza M, et al. Programmed death-1 pathway in cancer and autoimmunity. Clin Immunol, 2014,153: [42] Nicholas KJ, Zern EK, Barnett L, et al. B cell responses to HIV antigen are a potent correlate of viremia in HIV-1 infection and improve with PD-1 blockade. PloS One, 2013,8:e Chin J Cancer; 2014; Vol. 33 Issue 9 Chinese Journal of Cancer
10 [43] Kim JR, Moon YJ, Kwon KS, et al. Tumor infiltrating PD1-positive lymphocytes and the expression of PD-L1 predict poor prognosis of soft tissue sarcomas. PloS One, 2013,8:e [44] Maine CJ, Aziz NH, Chatterjee J, et al. Programmed death ligand-1 over-expression correlates with malignancy and contributes to immune regulation in ovarian cancer. Cancer Immunol Immunother, 2014,63: [45] Muenst S, Schaerli AR, Gao F, et al. Expression of programmed death ligand 1 (PD-L1) is associated with poor prognosis in human breast cancer. Breast Cancer Res Treat, 2014,146: [46] Oba J, Nakahara T, Abe T, et al. Expression of programmed death receptor ligand 1 in melanoma may indicate tumor progression and poor patient survival. J Am Acad Dermatol, 2014,70: [47] Shi SJ, Wang LJ, Wang GD, et al. B7-H1 expression is associated with poor prognosis in colorectal carcinoma and regulates the proliferation and invasion of HCT116 colorectal cancer cells. PloS One, 2013,8:e [48] Tamai K, Nakamura M, Mizuma M, et al. Suppressive expression of CD274 increases tumorigenesis and cancer stem cell phenotypes in cholangiocarcinoma. Cancer Sci, 2014,105: [49] Xylinas E, Robinson BD, Kluth LA, et al. Association of T-cell coregulatory protein expression with clinical outcomes following radical cystectomy for urothelial carcinoma of the bladder. Eur J Surg Oncol, 2014,40: [50] Zhang Y, Wang L, Li Y, et al. Protein expression of programmed death 1 ligand 1 and ligand 2 independently predict poor prognosis in surgically resected lung adenocarcinoma. Onco Targets Ther, 2014,7: [51] Zheng Z, Bu Z, Liu X, et al. Level of circulating PD-L1 expression in patients with advanced gastric cancer and its clinical implications. Chin J Cancer Res, 2014,26: [52] Liu Y, Carlsson R, Ambjorn M, et al. PD-L1 expression by neurons nearby tumors indicates better prognosis in glioblastoma patients. J Neurosci, 2013,33: [53] Topalian SL, Hodi FS, Brahmer JR, et al. Safety, activity, and immune correlates of anti-pd-1 antibody in cancer. N Engl J Med, 2012,366: [54] Topalian SL, Sznol M, McDermott DF, et al. Survival, durable tumor remission, and long-term safety in patients with advanced melanoma receiving nivolumab. J Clin Oncol, 2014,32: [55] Gettinger SN, Shepherd FA, Antonia SJ, et al. First-line nivolumab (anti-pd-1; BMS , ONO-4538) monotherapy in advanced NSCLC: safety, efficacy, and correlation of outcomes with PD-L1 status. J Clin Oncol, 2014,32 suppl:abstr [56] Antonia SJ, Brahmer JR, Gettinger SN, et al. Nivolumab (anti-pd-1; BMS , ONO-4538) in combination with platinum-based doublet chemotherapy (PT-DC) in advanced non-small cell lung cancer (NSCLC). J Clin Oncol, 2014,32 suppl:abstr [57] Rizvi NA, Chow LQM, Borghaei H, et al. Safety and response with nivolumab (anti-pd-1; BMS , ONO-4538) plus erlotinib in patients (pts) with epidermal growth factor receptor mutant (EGFR MT) advanced NSCLC. J Clin Oncol, 2014,32 suppl:abstr [58] Hamid O, Robert C, Daud A, et al. Safety and tumor responses with lambrolizumab (anti-pd-1) in melanoma. N Engl J Med, 2013,369: [59] Robert C, Ribas A, Wolchok JD, et al. Anti-programmed-deathreceptor-1 treatment with pembrolizumab in ipilimumab-refractory advanced melanoma: a randomised dose-comparison cohort of a phase 1 trial. Lancet, [Epub ahead of print] [60] Ribas A, Hodi FS, Kefford R, et al. Efficacy and safety of the anti- PD-1 monoclonal antibody MK-3475 in 411 patients (pts) with melanoma (MEL). J Clin Oncol, 2014,32 suppl:abstr LBA9000. [61] Garon EB, Leighl NB, Rizvi NA, et al. Safety and clinical activity of MK-3475 in previously treated patients (pts) with non-small cell lung cancer (NSCLC). J Clin Oncol, 2014,32 suppl:abstr [62] Kyi C, Postow MA. Checkpoint blocking antibodies in cancer immunotherapy. FEBS Lett, 2014,588: [63] Westin JR, Chu F, Zhang M, et al. Safety and activity of PD1 blockade by pidilizumab in combination with rituximab in patients with relapsed follicular lymphoma: a single group, open-label, phase 2 trial. Lancet Oncol, 2014,15: [64] Atkins MB, Kudchadkar RR, Sznol M, et al. Phase 2, multicenter, safety and efficacy study of pidilizumab in patients with metastatic melanoma. J Clin Oncol, 2014,32 suppl:abstr [65] Herbst RS, Gordon MS, Fine GD, et al. A study of MPDL3280A, an engineered PD-L1 antibody in patients with locally advanced or metastatic tumors. J Clin Oncol, 2013,31 suppl:abstr [66] Spigel DR, Gettinger SN, Horn L, et al. Clinical activity, safety, and biomarkers of MPDL3280A, an engineered PD-L1 antibody in patients with locally advanced or metastatic non-small cell lung cancer (NSCLC). J Clin Oncol, 2013,31 suppl:abstr [67] Cho DC, Sosman JA, Sznol M, et al. Clinical activity, safety, and biomarkers of MPDL3280A, an engineered PD-L1 antibody in patients with metastatic renal cell carcinoma (mrcc). J Clin Oncol, 2013,31 suppl:abstr [68] Hamid O, Sosman JA, Lawrence DP, et al. Clinical activity, safety, and biomarkers of MPDL3280A, an engineered PD-L1 antibody in patients with locally advanced or metastatic melanoma (mm). J Clin Oncol, 2013,31 suppl:abstr [69] Tabernero J, Powderly JD, Hamid O, et al. Clinical activity, safety, and biomarkers of MPDL3280A, an engineered PD-L1 antibody in patients with locally advanced or metastatic CRC, gastric cancer (GC), SCCHN, or other tumors. J Clin Oncol, 2013,31 suppl:abstr [70] Khleif S, Lutzky J, Segal N, et al. MEDI4736, an anti-pd-l1 antibody with modified Fc domain: preclinical evaluation and early clinical results from a phase 1 study in patients with advanced solid tumors. Eur J Cancer, 2013:S161-S161. [71] Fairman D, Narwal R, Liang M, et al. Pharmacokinetics of MEDI4736, a fully human anti-pdl1 monoclonal antibody, in patients with advanced solid tumors. J Clin Oncol, 2014,32 suppl:abstr [72] Brahmer JR, Rizvi NA, Lutzky J, et al. Clinical activity and biomarkers of MEDI4736, an anti-pd-l1 antibody, in patients with NSCLC. J Clin Oncol, 2014,32 suppl:abstr [73] Hodi FS, Lee SJ, McDermott DF, et al. Multicenter, randomized phase II trial of GM-CSF (GM) plus ipilimumab (IPI) versus IPI alone in metastatic melanoma: E1608. J Clin Oncol, 2013,31 suppl:abstr Chin J Cancer; 2014; Vol. 33 Issue 9 443
ASCO 12. PD-1 Immunotherapy Makes a Splash at ASCO
 PD-1 Immunotherapy Makes a Splash at ASCO By Gregory R. Wolfe, PhD Epigenetic variation and genetic instability in tumor cells yield a variety of tumor antigens that the immune system can recognize to
PD-1 Immunotherapy Makes a Splash at ASCO By Gregory R. Wolfe, PhD Epigenetic variation and genetic instability in tumor cells yield a variety of tumor antigens that the immune system can recognize to
Anti-PD1 Agents: Immunotherapy agents in the treatment of metastatic melanoma. Claire Vines, 2016 Pharm.D. Candidate
 + Anti-PD1 Agents: Immunotherapy agents in the treatment of metastatic melanoma Claire Vines, 2016 Pharm.D. Candidate + Disclosure I have no conflicts of interest to disclose. + Objectives Summarize NCCN
+ Anti-PD1 Agents: Immunotherapy agents in the treatment of metastatic melanoma Claire Vines, 2016 Pharm.D. Candidate + Disclosure I have no conflicts of interest to disclose. + Objectives Summarize NCCN
Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development
 Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development Sanjeeve Bala, MD, MPH Ovarian Cancer Endpoints Workshop FDA White Oak September 3, 2015 Overview Immune agents from
Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development Sanjeeve Bala, MD, MPH Ovarian Cancer Endpoints Workshop FDA White Oak September 3, 2015 Overview Immune agents from
Immunotherapy Concept Turned Reality
 Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY. Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds
 NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
NEW CLINICAL RESEARCH OPTIONS IN PANCREATIC CANCER IMMUNOTHERAPY Alan Melcher Professor of Clinical Oncology and Biotherapy Leeds CANCER IMMUNOTHERAPY - Breakthrough of the Year in Science magazine 2013.
Oncologist-to-Oncologist: How to Treat Your Patients with Immunotherapy
 Oncologist-to-Oncologist: How to Treat Your Patients with Immunotherapy Michael A. Postow, M.D. Memorial Sloan Kettering Cancer Center Wednesday, June 10, 2015 11:00 a.m. EDT Brought to you by the Cancer
Oncologist-to-Oncologist: How to Treat Your Patients with Immunotherapy Michael A. Postow, M.D. Memorial Sloan Kettering Cancer Center Wednesday, June 10, 2015 11:00 a.m. EDT Brought to you by the Cancer
Cancer Treatments Subcommittee of PTAC Meeting held 18 September 2015. (minutes for web publishing)
 Cancer Treatments Subcommittee of PTAC Meeting held 18 September 2015 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the
Cancer Treatments Subcommittee of PTAC Meeting held 18 September 2015 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the
Anticancer Immunotherapy A New Weapon Against Cancer JON STEPHENS, MPHIL SENIOR ANALYST, ONCOLOGY
 Anticancer Immunotherapy A New Weapon Against Cancer JON STEPHENS, MPHIL SENIOR ANALYST, ONCOLOGY A robust new approach Since its inception in the mid-0th century, chemotherapy has been the mainstay of
Anticancer Immunotherapy A New Weapon Against Cancer JON STEPHENS, MPHIL SENIOR ANALYST, ONCOLOGY A robust new approach Since its inception in the mid-0th century, chemotherapy has been the mainstay of
Trials in Elderly Melanoma Patients (with a focus on immunotherapy)
 Trials in Elderly Melanoma Patients (with a focus on immunotherapy) Where we were Immunotherapy Trials: past and present Relevance for real world practice Where we are SIOG October 2012 James Larkin FRCP
Trials in Elderly Melanoma Patients (with a focus on immunotherapy) Where we were Immunotherapy Trials: past and present Relevance for real world practice Where we are SIOG October 2012 James Larkin FRCP
Immunotherapy for High-Risk and Metastatic Melanoma
 Immunotherapy for High-Risk and Metastatic Melanoma Timothy M. Kuzel, MD Professor of Medicine and Dermatology Feinberg School of Medicine Northwestern University Chicago ICLIO 1 st Annual National Conference
Immunotherapy for High-Risk and Metastatic Melanoma Timothy M. Kuzel, MD Professor of Medicine and Dermatology Feinberg School of Medicine Northwestern University Chicago ICLIO 1 st Annual National Conference
Foundational Issues Related to Immunotherapy and Melanoma
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Immuno-Oncology, The New Era of Cancer Treatment. Ted Lee, MD, MPH Disease Area Head, IO, Pac Rim, Bristol Myers Squibb
 Immuno-Oncology, The New Era of Cancer Treatment Ted Lee, MD, MPH Disease Area Head, IO, Pac Rim, Bristol Myers Squibb 1 Disclosures Dr. Ted Lee is an employee of Bristol-Myers Squibb Co. New Therapies
Immuno-Oncology, The New Era of Cancer Treatment Ted Lee, MD, MPH Disease Area Head, IO, Pac Rim, Bristol Myers Squibb 1 Disclosures Dr. Ted Lee is an employee of Bristol-Myers Squibb Co. New Therapies
Predictive Biomarkers for PD1 Pathway Inhibitor Immunotherapy
 Predictive Biomarkers for PD1 Pathway Inhibitor Immunotherapy Michael B. Atkins, M.D. Deputy Director Georgetown-Lombardi Comprehensive Cancer Center Michael Atkins, MD Consulting Fees (e.g., advisory
Predictive Biomarkers for PD1 Pathway Inhibitor Immunotherapy Michael B. Atkins, M.D. Deputy Director Georgetown-Lombardi Comprehensive Cancer Center Michael Atkins, MD Consulting Fees (e.g., advisory
What is the Optimal Front-Line Treatment for mrcc? Michael B. Atkins, MD Deputy Director, Georgetown-Lombardi Comprehensive Cancer Center
 What is the Optimal Front-Line Treatment for mrcc? Michael B. Atkins, MD Deputy Director, Georgetown-Lombardi Comprehensive Cancer Center The Case for Immunotherapy in mrcc 1. Achieves patient s goal 2.
What is the Optimal Front-Line Treatment for mrcc? Michael B. Atkins, MD Deputy Director, Georgetown-Lombardi Comprehensive Cancer Center The Case for Immunotherapy in mrcc 1. Achieves patient s goal 2.
Immuno-Oncology 2015: A New Landscape in Lung Cancer
 Immuno-Oncology 2015: A New Landscape in Lung Cancer David R. Spigel, M.D. Lung Cancer Program Director Sarah Cannon Research Institute/Tennessee Oncology, PLLC Nashville, TN Off-Label Use Disclosure(s)
Immuno-Oncology 2015: A New Landscape in Lung Cancer David R. Spigel, M.D. Lung Cancer Program Director Sarah Cannon Research Institute/Tennessee Oncology, PLLC Nashville, TN Off-Label Use Disclosure(s)
Oncos Therapeutics: ONCOS THERAPEUTICS Personalized Cancer Immunotherapy. March 2015. Antti Vuolanto, COO and co-founder
 Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
Oncos Therapeutics: Personalized Cancer Immunotherapy ONCOS THERAPEUTICS Personalized Cancer Immunotherapy March 2015 Antti Vuolanto, COO and co-founder 1 History of Oncos Therapeutics 2002 2007 2009 Research
BOLT Hem/Onc Thought Leader Panel #38 Cancer Immunotherapy 2014-05
 Syndicated Thought Leader Insight Healthcare & Pharmaceutical Research Cancer Immunotherapy Melanoma, Non- Small Cell Lung Cancer, Renal Cell Carcinoma Thought Leader Panel #38 2014-05 Therapeutic Area:
Syndicated Thought Leader Insight Healthcare & Pharmaceutical Research Cancer Immunotherapy Melanoma, Non- Small Cell Lung Cancer, Renal Cell Carcinoma Thought Leader Panel #38 2014-05 Therapeutic Area:
Melanoma and Immunotherapy
 Melanoma and Immunotherapy Sanjiv S. Agarwala, MD Professor of Medicine Temple University School of Medicine Chief, Oncology & Hematology St. Luke s Cancer Center, Bethlehem, PA The Transformed Landscape
Melanoma and Immunotherapy Sanjiv S. Agarwala, MD Professor of Medicine Temple University School of Medicine Chief, Oncology & Hematology St. Luke s Cancer Center, Bethlehem, PA The Transformed Landscape
10 th EADO Congress Vilnius, 7-10 May 2014. Ipilimumab update. Michele Maio
 10 th EADO Congress Vilnius, 7-10 May 2014 Ipilimumab update Michele Maio Medical Oncology and Immunotherapy, Department of Oncology University Hospital of Siena, Istituto Toscano Tumori SIENA, ITALY Evolving
10 th EADO Congress Vilnius, 7-10 May 2014 Ipilimumab update Michele Maio Medical Oncology and Immunotherapy, Department of Oncology University Hospital of Siena, Istituto Toscano Tumori SIENA, ITALY Evolving
Current Status of Immunotherapy For the Treatment of Metastatic Melanoma
 Current Status of Immunotherapy For the Treatment of Metastatic Melanoma The 2016 Arizona Clinical Oncology Society Meeting Richard W. Joseph, MD Assistant Professor Mayo Clinic Florida joseph.richard@mayo.edu
Current Status of Immunotherapy For the Treatment of Metastatic Melanoma The 2016 Arizona Clinical Oncology Society Meeting Richard W. Joseph, MD Assistant Professor Mayo Clinic Florida joseph.richard@mayo.edu
CheckMate -057, a Pivotal III Opdivo (nivolumab) Lung Cancer Trial, Stopped Early
 April 21, 2015 CheckMate -057, a Pivotal III Opdivo (nivolumab) Lung Cancer Trial, Stopped Early Opdivo Demonstrates Superior Overall Survival Compared to Docetaxel in Patients with Previously-Treated
April 21, 2015 CheckMate -057, a Pivotal III Opdivo (nivolumab) Lung Cancer Trial, Stopped Early Opdivo Demonstrates Superior Overall Survival Compared to Docetaxel in Patients with Previously-Treated
Latest advances in the treatment of mesothelioma
 Latest advances in the treatment of mesothelioma Assoc Prof Thomas John Medical Oncologist, NHMRC Fellow Olivia Newton-John Cancer Research Institute 28 th March 2015 Disclosures Nil relevant Honoraria:
Latest advances in the treatment of mesothelioma Assoc Prof Thomas John Medical Oncologist, NHMRC Fellow Olivia Newton-John Cancer Research Institute 28 th March 2015 Disclosures Nil relevant Honoraria:
Cancer Immunotherapy: immune checkpoint inhibitors, cancer vaccines, and adoptive T-cell therapies - Overview
 Brochure More information from http://www.researchandmarkets.com/reports/3066973/ Cancer Immunotherapy: immune checkpoint inhibitors, cancer vaccines, and adoptive T-cell therapies - Overview Description:
Brochure More information from http://www.researchandmarkets.com/reports/3066973/ Cancer Immunotherapy: immune checkpoint inhibitors, cancer vaccines, and adoptive T-cell therapies - Overview Description:
Enhancing Anti-Tumor Activity of Checkpoint Inhibition
 Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
Enhancing Anti-Tumor Activity of Checkpoint Inhibition Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Laboratory of Tumor
Immune Checkpoint Blockade in Acute Myeloid Leukemia. Kinsey McCormick Hematology Fellow s Conference January 10, 2014
 Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
Immune Checkpoint Blockade in Acute Myeloid Leukemia Kinsey McCormick Hematology Fellow s Conference January 10, 2014 Overview Overview of immune checkpoints Immune checkpoints as mechanism of immune evasion
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center
 Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Coordinating Immune Checkpoint Blockade For Cancer Immunotherapy In Combination
 Coordinating Immune Checkpoint Blockade For Cancer Immunotherapy In Combination Jennifer Mataraza, Ph.D. Senior Investigator Immune Oncology, NIBR March 25, 2015 (Image: Steve Gshmeisserner/Science Photo
Coordinating Immune Checkpoint Blockade For Cancer Immunotherapy In Combination Jennifer Mataraza, Ph.D. Senior Investigator Immune Oncology, NIBR March 25, 2015 (Image: Steve Gshmeisserner/Science Photo
PROSPETTIVE FUTURE NEL TRATTAMENTO. Cinzia Ortega Dipartimento di Oncologia Medica Fondazione del Piemonte per l Oncologia I.R.C.C.S.
 PROSPETTIVE FUTURE NEL TRATTAMENTO MEDICO DEL mrcc Cinzia Ortega Dipartimento di Oncologia Medica Fondazione del Piemonte per l Oncologia I.R.C.C.S. Candiolo Future strategies in mrcc Improve therapeutic
PROSPETTIVE FUTURE NEL TRATTAMENTO MEDICO DEL mrcc Cinzia Ortega Dipartimento di Oncologia Medica Fondazione del Piemonte per l Oncologia I.R.C.C.S. Candiolo Future strategies in mrcc Improve therapeutic
Maintenance therapy in in Metastatic NSCLC. Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai
 Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
CLINICAL POLICY Department: Medical Management Document Name: Opdivo Reference Number: CP.PHAR.121 Effective Date: 07/15
 Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
News Release. Merck KGaA, Darmstadt, Germany, and Pfizer Receive FDA Breakthrough Therapy Designation for Avelumab in Metastatic Merkel Cell Carcinoma
 Your Contacts News Release Merck KGaA, Darmstadt, Germany Media: Markus Talanow +49 6151 72 7144 Investor Relations +49 6151 72 3321 Pfizer Inc., New York, USA Media: Sally Beatty +1 212 733 6566 Investor
Your Contacts News Release Merck KGaA, Darmstadt, Germany Media: Markus Talanow +49 6151 72 7144 Investor Relations +49 6151 72 3321 Pfizer Inc., New York, USA Media: Sally Beatty +1 212 733 6566 Investor
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
18.5 Percent Overall Response Rate Observed in Pembrolizumab-Treated Patients with this Aggressive Form of Breast Cancer
 News Release Media Contacts: Annick Robinson Investor Contacts: Joseph Romanelli (514) 837-2550 (908) 740-1986 Stephanie Lyttle NATIONAL Public Relations (514) 843-2365 Justin Holko (908) 740-1879 Merck
News Release Media Contacts: Annick Robinson Investor Contacts: Joseph Romanelli (514) 837-2550 (908) 740-1986 Stephanie Lyttle NATIONAL Public Relations (514) 843-2365 Justin Holko (908) 740-1879 Merck
Attached from the following page is the press release made by BMS for your information.
 July 22, 2015 CheckMate -025 (global clinical trial), a Pivotal Phase III Opdivo (nivolumab) Renal Cancer Trial Stopped Early (PRINCETON, NJ, July 20, 2015) Bristol-Myers Squibb Company (NYSE:BMY) announced
July 22, 2015 CheckMate -025 (global clinical trial), a Pivotal Phase III Opdivo (nivolumab) Renal Cancer Trial Stopped Early (PRINCETON, NJ, July 20, 2015) Bristol-Myers Squibb Company (NYSE:BMY) announced
Immune Therapy for Pancreatic Cancer
 Immune Therapy for Pancreatic Cancer December 16, 2014 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only:
Immune Therapy for Pancreatic Cancer December 16, 2014 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only:
The Past, Present & Future of Cancer Immunotherapy:
 Article The Past, Present & Future of Cancer Immunotherapy: An Overview Recently BioWorld called cancer immunotherapy white hot based on unprecedented investments in private companies, partnerships between
Article The Past, Present & Future of Cancer Immunotherapy: An Overview Recently BioWorld called cancer immunotherapy white hot based on unprecedented investments in private companies, partnerships between
Breakthrough Cancer Therapies: Directing the Immune System to Eliminate Tumor Cells. Corporate Presentation May 2015
 Breakthrough Cancer Therapies: Directing the Immune System to Eliminate Tumor Cells Corporate Presentation May 2015 Forward-looking statements / safe harbor This presentation and the accompanying oral
Breakthrough Cancer Therapies: Directing the Immune System to Eliminate Tumor Cells Corporate Presentation May 2015 Forward-looking statements / safe harbor This presentation and the accompanying oral
Combination Immunotherapies: Melanoma
 Combination Immunotherapies: Melanoma Igor Puzanov, MD, MSCI, FACP Associate Professor of Medicine, Associate Director of Phase I Drug Development, Director, Melanoma Research, Clinical Director, Renal
Combination Immunotherapies: Melanoma Igor Puzanov, MD, MSCI, FACP Associate Professor of Medicine, Associate Director of Phase I Drug Development, Director, Melanoma Research, Clinical Director, Renal
This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking
 Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
Q1/2016 This presentation may contain forward-looking statements, which reflect Trillium's current expectation regarding future events. These forward-looking statements involve risks and uncertainties
Targeted immunotherapy: unleashing the immune system against cancer
 Targeted immunotherapy: unleashing the immune system against cancer Suzanne L. Topalian, MD Johns Hopkins University School of Medicine Sidney Kimmel Comprehensive Cancer Center 2013 MMS Annual Education
Targeted immunotherapy: unleashing the immune system against cancer Suzanne L. Topalian, MD Johns Hopkins University School of Medicine Sidney Kimmel Comprehensive Cancer Center 2013 MMS Annual Education
Comparing Immunotherapy with High Dose IL-2 and Ipilimumab
 Comparing Immunotherapy with High Dose IL-2 and Ipilimumab Michael K Wong MD PhD FRCPC mike.wong@med.usc.edu Disclosures Speaker s Bureau, Advisory Boards, Consultant: Prometheus Bristol Myers Squibb Novartis
Comparing Immunotherapy with High Dose IL-2 and Ipilimumab Michael K Wong MD PhD FRCPC mike.wong@med.usc.edu Disclosures Speaker s Bureau, Advisory Boards, Consultant: Prometheus Bristol Myers Squibb Novartis
Advances in immunotherapy for melanoma
 Redman et al. BMC Medicine (2016) 14:20 DOI 10.1186/s12916-016-0571-0 MINIREVIEW Open Access Advances in immunotherapy for melanoma Jason M. Redman 1,2, Geoffrey T. Gibney 1,2 and Michael B. Atkins 1,2*
Redman et al. BMC Medicine (2016) 14:20 DOI 10.1186/s12916-016-0571-0 MINIREVIEW Open Access Advances in immunotherapy for melanoma Jason M. Redman 1,2, Geoffrey T. Gibney 1,2 and Michael B. Atkins 1,2*
Immuno-Oncology Therapies to Treat Lung Cancer
 Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Decision to Continue the Development of Tecemotide (L-BLP25) in Non-Small Cell Lung Cancer to be Announced
 September 27, 2013 ONO PHARMACEUTICAL CO., LTD. Corporate Communications Phone: +81-6-6263-5670 Decision to Continue the Development of Tecemotide (L-BLP25) in Non-Small Cell Lung Cancer to be Announced
September 27, 2013 ONO PHARMACEUTICAL CO., LTD. Corporate Communications Phone: +81-6-6263-5670 Decision to Continue the Development of Tecemotide (L-BLP25) in Non-Small Cell Lung Cancer to be Announced
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
Additional 50 patients enrolled in KEYNOTE-001 with analyses planned using Merck s proprietary PD-L1 assay at one percent and 50 percent cut points
 News Release Media Contacts: Annick Robinson Dominique Quirion Merck NATIONAL Annick.robinson@merck.com dquirion@national.ca 514 428-2890 514 843-2302 Investor Contacts: Justin Holko: (+1 908-423-5088
News Release Media Contacts: Annick Robinson Dominique Quirion Merck NATIONAL Annick.robinson@merck.com dquirion@national.ca 514 428-2890 514 843-2302 Investor Contacts: Justin Holko: (+1 908-423-5088
Immunotherapy for Metastatic Renal Cell Carcinoma
 Immunotherapy for Metastatic Renal Cell Carcinoma Timothy M. Kuzel, MD Professor of Medicine and Dermatology Feinberg School of Medicine Northwestern University Chicago, Ilinois ICLIO 1 st Annual National
Immunotherapy for Metastatic Renal Cell Carcinoma Timothy M. Kuzel, MD Professor of Medicine and Dermatology Feinberg School of Medicine Northwestern University Chicago, Ilinois ICLIO 1 st Annual National
Endpoint Selection in Phase II Oncology trials
 Endpoint Selection in Phase II Oncology trials Anastasia Ivanova Department of Biostatistics UNC at Chapel Hill aivanova@bios.unc.edu Primary endpoints in Phase II trials Recently looked at journal articles
Endpoint Selection in Phase II Oncology trials Anastasia Ivanova Department of Biostatistics UNC at Chapel Hill aivanova@bios.unc.edu Primary endpoints in Phase II trials Recently looked at journal articles
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS
 MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
MOH Policy for dispensing NEOPLASTIC DISEASES DRUGS All prescriptions for antineoplastic drugs must be accompanied by the MOH special form. All the attachments mentioned on this form shall be submitted
The renaissance of immunotherapy is a revolution for cancer patients. Ira Mellman, Ph.D. Vice President, Cancer Immunology, Genentech
 The renaissance of immunotherapy is a revolution for cancer patients Ira Mellman, Ph.D. Vice President, Cancer Immunology, Genentech 1 This presentation contains certain forward-looking statements. These
The renaissance of immunotherapy is a revolution for cancer patients Ira Mellman, Ph.D. Vice President, Cancer Immunology, Genentech 1 This presentation contains certain forward-looking statements. These
Corporate Presentation June 2, 2015
 Corporate Presentation June 2, 2015 SAFE HARBOR STATEMENT This presentation contains forward-looking statements. Although the Company believes its expectations are based on reasonable assumptions, these
Corporate Presentation June 2, 2015 SAFE HARBOR STATEMENT This presentation contains forward-looking statements. Although the Company believes its expectations are based on reasonable assumptions, these
Your Immune System & Lung Cancer Treatment
 Your Immune System & Lung Cancer Treatment Immunotherapy and Lung Cancer Immunotherapy is quickly developing as an important approach to treating many forms of cancer, including lung cancer. Immunotherapy
Your Immune System & Lung Cancer Treatment Immunotherapy and Lung Cancer Immunotherapy is quickly developing as an important approach to treating many forms of cancer, including lung cancer. Immunotherapy
Transgene Presents Additional Positive Clinical Data from Phase 2b Part of TIME Trial with TG4010 at ESMO
 Transgene Presents Additional Positive Clinical Data from Phase 2b Part of TIME Trial with TG4010 at ESMO Statistically significant difference in progression-free survival continues to be seen in non-squamous
Transgene Presents Additional Positive Clinical Data from Phase 2b Part of TIME Trial with TG4010 at ESMO Statistically significant difference in progression-free survival continues to be seen in non-squamous
National Horizon Scanning Centre. Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer. December 2007
 Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Pfizer Forms Global Alliance with Merck KGaA, Darmstadt, Germany to Accelerate Presence in Immuno-Oncology. November 17, 2014
 Pfizer Forms Global Alliance with Merck KGaA, Darmstadt, Germany to Accelerate Presence in Immuno-Oncology November 17, 2014 Forward-looking statements Our discussions during this conference call will
Pfizer Forms Global Alliance with Merck KGaA, Darmstadt, Germany to Accelerate Presence in Immuno-Oncology November 17, 2014 Forward-looking statements Our discussions during this conference call will
CONTINUING EDUCATION FACULTY. Kathy Boltz, PhD. Phoenix, Arizona
 CONTINUING EDUCATION EDUCATIONAL OBJECTIVES After participating in this activity, clinicians should be better able to Identify the components of the immune system Describe the mechanism of action of various
CONTINUING EDUCATION EDUCATIONAL OBJECTIVES After participating in this activity, clinicians should be better able to Identify the components of the immune system Describe the mechanism of action of various
Understanding series. new. directions. 1-800-298-2436 LungCancerAlliance.org. A guide for the patient
 Understanding series LUNG CANCER: new treatment directions 1-800-298-2436 LungCancerAlliance.org A guide for the patient TABLE OF CONTENTS What s New in lung cancer? Advancements...4 Changes in genes that
Understanding series LUNG CANCER: new treatment directions 1-800-298-2436 LungCancerAlliance.org A guide for the patient TABLE OF CONTENTS What s New in lung cancer? Advancements...4 Changes in genes that
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
MOLOGEN AG. Q1 Results 2015 Conference Call Dr. Matthias Schroff Chief Executive Officer. Berlin, 12 May 2015
 Q1 Results 2015 Conference Call Dr. Matthias Schroff Chief Executive Officer Berlin, 12 May 2015 V1-6 Disclaimer Certain statements in this presentation contain formulations or terms referring to the future
Q1 Results 2015 Conference Call Dr. Matthias Schroff Chief Executive Officer Berlin, 12 May 2015 V1-6 Disclaimer Certain statements in this presentation contain formulations or terms referring to the future
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials)
 ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
Treating Patients with Hormone Receptor Positive, HER2 Positive Operable or Locally Advanced Breast Cancer
 Breast Studies Adjuvant therapy after surgery Her 2 positive Breast Cancer B 52 Docetaxel, Carboplatin, Trastuzumab, and Pertuzumab With or Without Estrogen Deprivation in Treating Patients with Hormone
Breast Studies Adjuvant therapy after surgery Her 2 positive Breast Cancer B 52 Docetaxel, Carboplatin, Trastuzumab, and Pertuzumab With or Without Estrogen Deprivation in Treating Patients with Hormone
Clinical Trials for Patients with
 Clinical Trials for Patients with Malignant Pleural Mesothelioma Lee M. Krug, M.D. Memorial Sloan-Kettering Cancer Center New York, New York Challenges in MPM Clinical Trials Mesothelioma is a rare disease,
Clinical Trials for Patients with Malignant Pleural Mesothelioma Lee M. Krug, M.D. Memorial Sloan-Kettering Cancer Center New York, New York Challenges in MPM Clinical Trials Mesothelioma is a rare disease,
Chimeric Antigen Receptor T Cell Therapy
 Chimeric Antigen Receptor T Cell Therapy Yi Lin, MD, PhD Mayo Clinic, Rochester, MN Alliance Spring Group Meeting - May 13, 2016 Presentation Objectives l Scientific overview of chimeric antigen receptor
Chimeric Antigen Receptor T Cell Therapy Yi Lin, MD, PhD Mayo Clinic, Rochester, MN Alliance Spring Group Meeting - May 13, 2016 Presentation Objectives l Scientific overview of chimeric antigen receptor
Activity of pemetrexed in thoracic malignancies
 Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
IMMUNOMEDICS, INC. February 2016. Advanced Antibody-Based Therapeutics. Oncology Autoimmune Diseases
 IMMUNOMEDICS, INC. Advanced Antibody-Based Therapeutics Oncology Autoimmune Diseases February 2016 Forward-Looking Statements This presentation, in addition to historical information, contains certain
IMMUNOMEDICS, INC. Advanced Antibody-Based Therapeutics Oncology Autoimmune Diseases February 2016 Forward-Looking Statements This presentation, in addition to historical information, contains certain
Emerging Drug List GEFITINIB
 Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study
 Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics
 Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics Disclosure(s) I do not intend to discuss an off-label use
Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics Disclosure(s) I do not intend to discuss an off-label use
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY
 CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
Future Oncology: Technology, Products, Market and Service Opportunities
 Brochure More information from http://www.researchandmarkets.com/reports/296370/ Future Oncology: Technology, Products, Market and Service Opportunities Description: Future Oncology is an analytical newsletter
Brochure More information from http://www.researchandmarkets.com/reports/296370/ Future Oncology: Technology, Products, Market and Service Opportunities Description: Future Oncology is an analytical newsletter
Advances in Treatment of Malignant Pleural Mesothelioma: A Reason for Hope
 Advances in Treatment of Malignant Pleural Mesothelioma: A Reason for Hope Daniel H. Sterman, M.D. Associate Professor of Medicine and Surgery Co-Director, PENN Mesothelioma and Pleural Program University
Advances in Treatment of Malignant Pleural Mesothelioma: A Reason for Hope Daniel H. Sterman, M.D. Associate Professor of Medicine and Surgery Co-Director, PENN Mesothelioma and Pleural Program University
Bioinformatics for cancer immunology and immunotherapy
 Bioinformatics for cancer immunology and immunotherapy Zlatko Trajanoski Biocenter, Division for Bioinformatics Innsbruck Medical University Innrain 80, 6020 Innsbruck, Austria Email: zlatko.trajanoski@i-med.ac.at
Bioinformatics for cancer immunology and immunotherapy Zlatko Trajanoski Biocenter, Division for Bioinformatics Innsbruck Medical University Innrain 80, 6020 Innsbruck, Austria Email: zlatko.trajanoski@i-med.ac.at
Update in Hematology Oncology Targeted Therapies. Mark Holguin
 Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
BADO meeting. Immunotherapy. in Metastatic Melanoma
 BADO meeting Immunotherapy in Metastatic Melanoma UCL Université catholique de Louvain Prof J-Fr. BAURAIN Medical Oncology Department BADO Meeting Inaugural Lecture 07 december 2013 Melanoma Treatment
BADO meeting Immunotherapy in Metastatic Melanoma UCL Université catholique de Louvain Prof J-Fr. BAURAIN Medical Oncology Department BADO Meeting Inaugural Lecture 07 december 2013 Melanoma Treatment
Immunotherapy or Molecularly Targeted Therapy: What Is the Best Initial Treatment for Stage IV BRAF-Mutant Melanoma?
 Immunotherapy or Molecularly Targeted Therapy: What Is the Best Initial Treatment for Stage IV BRAF-Mutant Melanoma? Geoffrey T. Gibney, MD, and Michael B. Atkins, MD Geoffrey T. Gibney, MD, is an attending
Immunotherapy or Molecularly Targeted Therapy: What Is the Best Initial Treatment for Stage IV BRAF-Mutant Melanoma? Geoffrey T. Gibney, MD, and Michael B. Atkins, MD Geoffrey T. Gibney, MD, is an attending
TKCC/Garvan Cancer Biology Seminars Melanoma & Cancer Immunotherapy
 TKCC/Garvan Cancer Biology Seminars Melanoma & Cancer Immunotherapy 19/02/2016 A/Prof Anthony Joshua Head, Dept of Medical Oncology St Vincent s Hospital, Sydney Immunotherapy Progress: A Long Time Coming
TKCC/Garvan Cancer Biology Seminars Melanoma & Cancer Immunotherapy 19/02/2016 A/Prof Anthony Joshua Head, Dept of Medical Oncology St Vincent s Hospital, Sydney Immunotherapy Progress: A Long Time Coming
Moving forward, where are we with Clinical Trials?
 Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Pharmacogenomic markers in EGFR-targeted therapy of lung cancer
 Pharmacogenomic markers in EGFR-targeted therapy of lung cancer Rafal Dziadziuszko, MD, PhD University of Colorado Cancer Center, Aurora, CO, USA Medical University of Gdansk, Poland EMEA Workshop on Biomarkers,
Pharmacogenomic markers in EGFR-targeted therapy of lung cancer Rafal Dziadziuszko, MD, PhD University of Colorado Cancer Center, Aurora, CO, USA Medical University of Gdansk, Poland EMEA Workshop on Biomarkers,
Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress
 Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress Lung Cancer Accounts for 14% of All New Cancer Diagnoses in the United States 1 Lung cancer is the second most common malignancy
Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress Lung Cancer Accounts for 14% of All New Cancer Diagnoses in the United States 1 Lung cancer is the second most common malignancy
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
A disease and antibody biology approach to antibody drug discovery
 A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Corporate Medical Policy
 Corporate Medical Policy Ado-Trastuzumab Emtansine (Trastuzumab-DM1) for Treatment of File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ado_trastuzumab_emtansine_(trastuzumab-dm1)_for_treatment_of_her-2_positivemalignancies
Corporate Medical Policy Ado-Trastuzumab Emtansine (Trastuzumab-DM1) for Treatment of File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ado_trastuzumab_emtansine_(trastuzumab-dm1)_for_treatment_of_her-2_positivemalignancies
ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER
 AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer
 LONDON CANCER NEWS DRUGS GROUP RAPID REVIEW Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer Everolimus plus exemestane for second-line
LONDON CANCER NEWS DRUGS GROUP RAPID REVIEW Everolimus plus exemestane for second-line endocrine treatment of oestrogen receptor positive metastatic breast cancer Everolimus plus exemestane for second-line
Background. t 1/2 of 3.7 4.7 days allows once-daily dosing (1.5 mg) with consistent serum concentration 2,3 No interaction with CYP3A4 inhibitors 4
 Abstract No. 4501 Tivozanib versus sorafenib as initial targeted therapy for patients with advanced renal cell carcinoma: Results from a Phase III randomized, open-label, multicenter trial R. Motzer, D.
Abstract No. 4501 Tivozanib versus sorafenib as initial targeted therapy for patients with advanced renal cell carcinoma: Results from a Phase III randomized, open-label, multicenter trial R. Motzer, D.
An Introduction To Immunotherapy And The Promise Of Tissue Phenomics
 An Introduction To Immunotherapy And The Promise Of Tissue Phenomics INSIDE: n The Potential of Immunotherapy n Towards an Understanding of Immunotherapy n Current Approaches to Immunotherapy n The Immunotherapy
An Introduction To Immunotherapy And The Promise Of Tissue Phenomics INSIDE: n The Potential of Immunotherapy n Towards an Understanding of Immunotherapy n Current Approaches to Immunotherapy n The Immunotherapy
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
Prior Authorization Guideline Guideline: PS Inj - Alimta Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antifolates Client: PS Inj Approval Date: 8/2/2004 Revision Date: 12/5/2006 I. BENEFIT
National Pharmaceutical Pricing Authority 3 rd Floor, YMCA Cultural Centre 1 Jai Singh Road New Delhi 110001 File No. 23(01)2014/Div.
 Dated 21 st November 2014 NPPA Invites Comments of Pharmaceutical Industry & Trade, Consumer Organisations, Public Health Experts and other Stakeholders on the Recommendations of Tata Memorial Centre under
Dated 21 st November 2014 NPPA Invites Comments of Pharmaceutical Industry & Trade, Consumer Organisations, Public Health Experts and other Stakeholders on the Recommendations of Tata Memorial Centre under
Sommaire projets sélectionnés mesure 29: Soutien à la recherche translationnelle
 Sommaire projets sélectionnés mesure 29: Soutien à la recherche translationnelle TITLE PROJET NOM HOPITAL Assessment of tumor angiogenesis using PET/CT with 18 F-Galacto- RGD. (PNC_29_001) Division of
Sommaire projets sélectionnés mesure 29: Soutien à la recherche translationnelle TITLE PROJET NOM HOPITAL Assessment of tumor angiogenesis using PET/CT with 18 F-Galacto- RGD. (PNC_29_001) Division of
This report focuses on the rising potential for the newest and most promising of cancer treatments:
 1 Cancer Immunotherapy: Immune Checkpoint Inhibitors, Cancer Vaccines, and Adoptive T-cell Therapies Allan B. Haberman. Ph.D. This report focuses on the rising potential for the newest and most promising
1 Cancer Immunotherapy: Immune Checkpoint Inhibitors, Cancer Vaccines, and Adoptive T-cell Therapies Allan B. Haberman. Ph.D. This report focuses on the rising potential for the newest and most promising
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
PARP Inhibitors in Lung Cancer. Primo N. Lara, Jr., MD Professor of Medicine UC Davis Comprehensive Cancer Center
 PARP Inhibitors in Lung Cancer Primo N. Lara, Jr., MD Professor of Medicine UC Davis Comprehensive Cancer Center Poly (ADP-ribose) Polymerase (PARP): Mechanism of Action PARPs: family of enzymes that repair
PARP Inhibitors in Lung Cancer Primo N. Lara, Jr., MD Professor of Medicine UC Davis Comprehensive Cancer Center Poly (ADP-ribose) Polymerase (PARP): Mechanism of Action PARPs: family of enzymes that repair
Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer
 Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer Review Article [1] December 01, 2003 By George W. Sledge, Jr, MD [2] Gemcitabine (Gemzar) and paclitaxel show good activity as single
Gemcitabine, Paclitaxel, and Trastuzumab in Metastatic Breast Cancer Review Article [1] December 01, 2003 By George W. Sledge, Jr, MD [2] Gemcitabine (Gemzar) and paclitaxel show good activity as single
Lung Cancer: More than meets the eye
 Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Molecular markers and clinical trial design parallels between oncology and rare diseases?
 Molecular markers and clinical trial design parallels between oncology and rare diseases?, Harriet Sommer Institute for Medical Biometry and Statistics, University of Freiburg Medical Center 6. Forum Patientennahe
Molecular markers and clinical trial design parallels between oncology and rare diseases?, Harriet Sommer Institute for Medical Biometry and Statistics, University of Freiburg Medical Center 6. Forum Patientennahe
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
 Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
DCVax Novel Personalized Immune Therapies For Solid Tumor Cancers. SMi 4 th Annual Cancer Vaccines Conference September 16, 2015
 DCVax Novel Personalized Immune Therapies For Solid Tumor Cancers SMi 4 th Annual Cancer Vaccines Conference September 16, 2015 Disclaimer Certain statements made in this presentation are forward-looking
DCVax Novel Personalized Immune Therapies For Solid Tumor Cancers SMi 4 th Annual Cancer Vaccines Conference September 16, 2015 Disclaimer Certain statements made in this presentation are forward-looking
