for hip fracture in fee-for-service and group/staff HMO delivery systems.
|
|
|
- Francine Webb
- 8 years ago
- Views:
Transcription
1 A Comparison of Functional Outcomes after Hip Fracture in Group/Staff HMOs and Fee-for-Service Systems CONTEXT. Previous studies examining differences in the quality of care between capitated and fee-for-service payment systems have focused on the care delivered in a single setting. No study to date has compared outcomes over an entire episode of care delivered across multiple settings. OBJECTIVE. To compare outcomes of care for patients receiving institutional rehabilitation for hip fracture in fee-for-service and group/staff HMO delivery systems. DESIGN. One-year prospective inception cohort. SETTING. Six hospital-based, integrated care systems paid on a traditional fee-forservice model and five group/staff HMOs (paid fixed capitation rate by Medicare). The 11 delivery systems were selected because of their commitment to geriatric rehabilitation. PATIENTS. 196 fee-for-service and 140 group/staff HMO patients with acute hip fracture were identified on admission to inpatient rehabilitation. MEASURES. Four primary outcomes recovery of activities of daily living, improvement in ambulation, return to community living, and mortality were measured at 3, 6, 9, and 12 months. Service utilization was assessed in the acute-care hospital setting, rehabilitation setting, and at each 3-month follow-up interval. Risk adjustment was performed by using multiple and logistic regression. RESULTS. Overall, no differences were found between patients in group/staff HMOs and fee-for-service patients. Group/staff HMO patients experienced improved functional recovery at 6 months (P ) and improved ambulation at 12 months (P =0.05) compared with fee-for-service patients, although these were isolated findings. With regard to utilization, group/staff HMO delivery systems used physician services less intensively and substituted less-skilled allied health personnel. CONCLUSION. Compared with fee-for-service delivery systems, with a similar commitment to excellence in geriatric rehabilitation, group/staff HMOs can achieve equivalent outcomes in older patients recovering from hip fracture with less-intense service utilization. ORIGINAL ARTICLE ERIC A. COLEMAN, MD, MPH ANDREW M. KRAMER, MD JACQUELINE C. KOWALSKY, MA DONALD ECKHOFF, MD MICHAEL LIN, MSPH ERIC J. HESTER, BA NORA MORGENSTERN, MD JOHN F. STEINER, MD, MPH University of Colorado Health Sciences Center Denver, Colo Eff Clin Pract. 2000;4: With the growing number of older adults in Medicare managed care, 1 much debate has centered on whether the quality of care under this capitated payment structure differs from care delivered under fee-for-service. Comparative studies conducted over the past decade suggest that the quality of care in HMOs is at least as good as that in fee-for-service care These previous studies, however, have primarily focused on care delivered in a single setting (i.e., acute-care in the hospital, Edited by John D. Birkmeyer, MD This paper is available at ecp.acponline.org American College of Physicians American Society of Internal Medicine 229
2 ambulatory care, or home care) or on a specific aspect of care (i.e., preventive services or a particular chronic disease). Yet older patients, particularly those with complex care needs, frequently require medical care delivered from multiple sites. Care fragmentation remains a serious threat to the quality of care that these patients receive. The ability of a delivery system to improve the health care outcomes of their older members across the continuum of care may be an even more sensitive measure of quality for comparison. The care of older patients with hip fracture is ideal for comparing quality of care across multiple settings with different payment structures. With over 250,000 cases of hip fracture occurring per year, 12,13 this condition is highly prevalent and has wide variations in outcomes of care. Following hip fracture, 50% to 70% of older patients do not regain their prefracture level of function, 14,15 46% to 79% do not regain their prefracture ability to ambulate, % to 50% do not return to community living, 17,18 and 17% to 32% die within the year Previous studies have demonstrated that the hospital care of patients with hip fracture is sensitive to the type of reimbursement structure under the implementation of diagnosis-related groups Patients with hip fracture have a discrete beginning to their episode of care (the fracture) and require treatment from different disciplines 27 in multiple sites of care. Institutional rehabilitation for hip fracture is typically provided in Medicare-certified skilled nursing facilities (SNFs), although a few patients are admitted to inpatient rehabilitation facilities (RFs). Approximately 47% to 67% of all patients with hip fracture receive rehabilitation in one of these institutional settings a subgroup comprising predominantly older, frailer patients with associated 28, 29 cognitive impairment and inadequate social support. In this study, we compare quality of care for patients receiving institutional rehabilitation for hip fracture in group/staff HMO and fee-for-service delivery systems for the primary outcomes of recovery of function, improvement in ambulation, return to community living, and mortality. We hypothesized that although group/staff HMO and fee-for-service systems might differ in the type and intensity of service delivered, primary outcomes of care would be the same. Settings Methods The six participating group/staff HMOs were selected on the basis of longstanding Medicare-risk contracts (greater than 10 years), the size of their Medicare-risk population, and an established commitment to geriatric rehabilitation. In the regions studied, three group/staff HMOs had 15,000 to 20,000 Medicare beneficiaries and three had 45,000 or more Medicare beneficiaries. Medicare enrollment in these group/staff HMOs represented between 8% and 32% of total enrollment in each region. These systems were selected because they had reputable Medicare-risk programs for geriatric rehabilitation in RFs or SNFs that offered physician-directed interdisciplinary teams and/or nurse practitioner rounding. 30 For each group/staff HMO, we included the institutions to which they admitted most (greater than 90% overall) of their patients with hip fracture for rehabilitation under their Medicare-risk contract. Two group/staff HMOs used subacute-care SNFs that they owned and operated and that were located close to their other services (representing three facilities). Two group/staff HMOs contracted with community-based, proprietary SNFs. They established payment contracts for hip fracture rehabilitation that were not subject to the fee-for-service limits and had a close working relationship with group/staff HMO rehabilitation staff (five facilities total). One group/staff HMO contracted with a hospital-based SNF in which the rehabilitation staff were employed by the HMO. The final system was part owner/operator of both a freestanding RF and an SNF that was connected to their major acute-care hospital. We also selected five vertically integrated fee-forservice delivery systems on the basis of size of the Medicare patient population, availability of both SNFs and RFs in their system, and similar geographic representation as the group/staff HMOs (West, Mountain, Midwest, and Northeast). These fee-for-service delivery systems also had a reputation for excellent geriatric care; were paid on a traditional fee-for-service model and through prearranged selective contracting; were organized to provide all of the essential components of care delivery, including the acute-care hospital, outpatient clinics, and/or attached physicians offices; and had an available RF and SNF and access to home-based care. In each system, we selected the institutions to which they discharged most (greater than 90% overall) of their Medicare patients with hip fracture. In four of the five systems, this included a hospital-based RF and a hospital-based SNF unit (eight facilities). In the other system, this included a freestanding RF and an SNF attached to the RF (two sites). All 11 delivery systems agreed to participate. The study was approved by the Human Subjects Review Committees at the University of Colorado as well as local review boards. Patients Potential participants undergoing rehabilitation for acute hip fracture were identified on admission to an RF 230 Effective Clinical Practice September/October 2000 Volume 3 Number 5
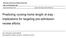
3 or SNF. Study inclusion criteria included age older than 64 years, English-speaking, Medicare or Medicare-risk coverage, acute-care hospital stay for hip fracture within the past 30 days, and no previous admission to a rehabilitation setting for this episode. Potential participants with hip fracture (e.g., femoral neck, intertrochanteric, subtrochanteric fractures) were identified on the basis of admission codes from The International Classification of Diseases, Ninth Revision, Clinical Modification (i.e., codes 820.0, , , , , , , , and 820.8) and confirmed by chart and radiograph review. Patients with cognitive impairment or aphasia to a degree that limited their ability to provide informed consent remained eligible provided that an appropriate proxy could be located. Patients who were receiving hospice care or who were comatose were excluded. The recruitment experience is summarized in Figure 1. An estimated 1197 patients receiving institutional rehabilitation for hip fracture were screened, and Hip fracture patients admitted for institutional rehabilitation (estimated n = 1197) Ineligible patients (n = 595) Not in study delivery system <65 years of age Non-English speaking Not hospitalized within the past 30 days Eligible patients (n = 602) Excluded patients (n = 266) Not interested (n = 148) Too sick or overwhelmed (n = 70) Dementia with no proxy (n = 46) No reason given (n = 2) Consented to participate (n = 336) Fee-for-service patients (n = 196) Group/staff HMO patients (n = 140) Died (n = 24) Lost to follow-up (n = 13) Missing values (n = 13) Died (n = 24) Lost to follow-up (n = 4) Missing values (n = 4) Patients with complete 12-month data (n = 146) Patients with complete 12-month data (n = 108) FIGURE 1. Study recruitment. Effective Clinical Practice September/October 2000 Volume 3 Number 5 231
4 a total of 602 patients were eligible to participate. We did not have consent to obtain demographic or health status information on ineligible persons and thus were not able to characterize these patients. Two hundred sixty-six (44%) persons did not participate for the following reasons: not interested (25%); too sick or overwhelmed by their condition (12%); and confusion or advanced dementia with no proxy (8%). No reason was given in 1%. The remaining 336 (56%) patients participated in the study and were included in this analysis. There were 196 patients in the fee-for-service group, and 140 patients in the group/staff HMO group. Study participants and nonparticipants were similar with respect to age, gender, and premorbid living arrangements. Participants had attained higher levels of education and were more likely to be of non-hispanic white ethnicity than nonparticipants. Fee-for-service nonparticipants were older and more likely to be of non-hispanic white ethnicity than were group/staff HMO nonparticipants. Because we did not have follow-up data on nonparticipants, we were not able to comment on whether their nonparticipation biased our findings. Six fee-for-service participants (3.1%) received assistance from a proxy, compared with 13 (9.3%) group/staff HMO participants. Study participants were enrolled between June 1993 and June 1995, with follow-up continuing until June Recruitment ranged from 5 to 84 patients per plan, with an overall average of 30 patients per plan. Data Collection Participant demographic and health status information was obtained through an in-person interview conducted on admission to the rehabilitation setting and by telephone at 3, 6, 9, and 12-month intervals. A proxy was deemed necessary for participants when their Mini- Mental Status Examination score was less than Additional information about participants health status (general health, function, type of fracture) was obtained from the medical records of the acute-care hospital and the rehabilitation setting, nursing staff interviews, and pre- and postoperative radiographs. Facility staff provided data on admission status, physician visits, number and duration of therapy sessions, and discharge status. Nursing effort was measured by using 24-hour time studies conducted weekly for all study participants during which nurses reported time devoted directly to patient care by type of staff for each encounter. Comorbid conditions were identified from the acutecare hospital record by using the Charlson Index. 32 Utilization data were obtained directly from the participating health plans and from Medicare claims files for the fee-for-service participants. Utilization data for fee-for-service patients were obtained from Medicare National Claims History Files Parts A and B and for group/staff HMO patients directly from participating health plans. Encounter data from the health plans were re-coded to coincide with uniform service definitions from claims data. Overall, plans provided 88% of the utilization requested. One of the group/staff HMO plans changed ownership over the course of the study and subsequently did not have the ability to provide complete utilization data on their 25 patients. Additional missing utilization data were attributed to nonmatching Medicare identification numbers (n=8) and no subsequent utilization because of death in the rehabilitation setting (n=4). Measures Primary outcomes, measured at 3, 6, 9, and 12 months, included recovery of function, improvement in ambulation, return to community living, and mortality. The measure of functional recovery was adapted from questions used in the Longitudinal Study on Aging. 33,34 Patients or proxies were asked to report degree of difficulty in basic activities of daily living (ADLs) (bathing, dressing, toileting, eating, transferring, and walking) using a 4-point scale (no difficulty, some difficulty, a lot of difficulty, and unable). Patients were categorized as having recovered if they attained their prefracture functional score or better. A composite score of the six individual measures of function was computed for each patient. 35 Ambulation was assessed by using a validated instrument that evaluates maximum walking capacity. 36 Patients were asked to report their level of difficulty (0 = not able; 1 = much difficulty; 2 = some difficulty; 3 = no difficulty) in walking 20, 50, 300, 600, and 900 feet. Level of difficulty was then multiplied by distance, divided by the maximum total possible score, and multiplied by 100 to provide a 0 to 100 scale. Community living was defined as living in a home, apartment, assisted-living facility, or board-and-care home. Mortality was assessed at each 3-month follow-up interval from either proxy report or health plan records. Design and Analysis The study design was a prospective 1-year inception cohort. The unit of analysis was the patient, and the primary comparison was between insurance types (group/staff HMO or fee-for-service). Demographic, health status, and utilization variables were compared by using the t-test for continuous variables and the chisquare test for categorical variables. Nonparametric comparisons were made by using the Wilcoxon rank sum test and the Fisher exact test. Multiple regression was used to analyze the primary outcomes of functional recovery and improved ambulation, and logistic regression was used to evaluate return 232 Effective Clinical Practice September/October 2000 Volume 3 Number 5
5 to community living. To ensure that the findings were not significantly affected by values from outlier individual delivery systems (rather than payment structure), we examined the contribution of each individual plan (i.e., dummy variables) to the overall regression models for the primary outcomes. To address potential concern for differential outcomes attributed to the use of proxy responses, the major outcome analyses were repeated comparing participants who did and did not rely on proxy report. These analyses did not differ from the main analyses and are not presented. Multiple regression (ProcReg) and logistic regression (ProcLogistic) analyses were performed by using SAS version 6.12 (SAS Institute Inc., Cary, NC). Previous studies of older patients with hip fractures have shown high rates of death over the course of 1 year. 15, 21, 22 In this study, the primary outcomes were analyzed with and without deaths. 37 Because the primary outcomes did not differ regardless of whether deaths were included in the analyses, only the former results are presented. Results Fee-for-service patients were older, better educated, and less likely to have an informal caregiver available (Table 1). Prefracture physical function and walking ability did not differ between the two groups. The type of hip fracture and the type of surgical repair did not differ. Hospital Stay On average, group/staff HMO patients underwent surgery sooner (1.1 vs. 1.4 days, P =0.04), received physical therapy sooner (1.5 vs. 1.8 days, P =0.05), and were discharged sooner to a rehabilitation setting than did fee-forservice patients (5.5 vs. 9.7 days, P ). Examination of surgical or nonsurgical adverse events during acute-care hospitalization revealed no significant differences. By virtue of a longer stay in the hospital after surgical repair, fee-for-service patients had received an average of 4 more days of rehabilitation on admission to the rehabilitation setting than did group/staff HMO patients. Rehabilitation Stay Comparisons of the care provided in the rehabilitation setting are reported in Table 2. Significantly more feefor-service patients were admitted to an RF than an SNF. On average, fee-for-service patients remained in the rehabilitation setting 2 days longer than did group/staff HMO patients. During their longer stays, fee-for-service patients received more care from physical and occupational therapists. Group/staff HMO patients, however, were more likely to receive care from physical therapy technicians, such that total physical therapy department time was not significantly different. Although the number of hours of licensed nursing care did not differ, group/staff HMO patients received more care from nursing staff with less formal training. No differences were detected in the total number of attending physician visits. Fee-for-service patients were more likely to be seen by an orthopedic surgeon, physiatrist, or consulting specialist physician, whereas group/staff HMO patients were more likely to be seen by a boardcertified geriatrician, nurse practitioner, and/or physician assistant. Group/staff HMO plans seem to have substituted care providers at all levels but provided similar service intensity overall. Post Rehabilitation Patients utilization patterns in the year after discharge from the index rehabilitation stay are provided in Table 3. There were no differences in rehospitalization rates or emergency department use. Fee-for-service patients received more outpatient physician visits (all-inclusive) and more primary care, orthopedist, and consulting specialist physician visits. Group/staff HMO patients had significantly more visits from home health nurses. Mortality rates between the two groups did not differ. Mortality rates for fee-for-service and group/staff HMO patients at 3, 6, 9, and 12 months were 4.7% versus 4.9% (P =0.99); 8.3% versus 11.4% (P =0.44); 10.3% versus 14.9% (P =0.23), and 12.0% versus 16.9% (P =0.26), respectively. After adjustment for age, comorbid conditions, and cognitive function, no differences in mortality were noted between the two groups. Functional Outcomes The other primary outcomes are compared in Figures 2 through 4. Overall, no differences were found between group/staff HMO and fee-for-service patients. Group/staff HMO patients had better functional recovery at 6 months (P ) and ambulation at 12 months (P =0.05) than did fee-for-service patients, although these were isolated findings. These regression analyses were adjusted as follows: Functional recovery was adjusted for prefracture function, type of fracture repair, age, marital status, cognitive function, and communicative ability; ambulation was adjusted for prefracture ambulation score, type of fracture, age, previous stroke, cognitive function, communicative ability, and depression; and return to community living was adjusted for prefracture functional status, type of fracture repair, marital status, cognitive function, and communicative ability. There was no evidence that outlying values for individual delivery systems influenced any of the primary outcomes. For example, in the 6-month comparison Effective Clinical Practice September/October 2000 Volume 3 Number 5 233
6 TABLE 1 Baseline Demographic and Functional Characteristics of Older Patients with Hip Fracture in Fee-for-Service and Group/Staff HMO Systems CHARACTERISTIC FEE-FOR-SERVICE (n=196) HMO (n=140) P VALUE Demographic characteristics Mean age ± SD, yr Female White Not a high school graduate Income <$10, ± % 96.9% 17.9% 35.7% 79.8 ± % 99.3% 27.3% 27.0% 0.04 Type of Social Support Married Living with others Able and willing caregiver Preadmission residence in institution 29.1% 45.0% 44.8% 1.0% 38.6% 49.6% 72.6% 0.7% 0.08 Comorbid conditions Charlson Index ± SD Diabetes Angina Previous myocardial infarction Congestive heart failure Peripheral vascular disease Cerebrovascular disease Moderate/severe renal disease Chronic pulmonary disease Any psychiatric diagnosis Mean number of medications ± SD 1.4 ± % 6.2% 9.2% 17.4% 9.2% 12.3% 1.5% 16.9% 10.3% 5.5 ± ± % 4.4% 10.3% 12.5% 8.8% 11.0% 0.0% 15.4% 4.4% 5.3 ± Conditions at admission to the rehabilitation facility Visual impairment Hearing impairment Pressure sore (any) Difficulty with communication 9.7% 15.9% 24.1% 14.8% 5.1% 3.7% 12.6% 16.3% Functional status before fracture Mean number of ADLs* performed with difficulty ± SD Mean maximum walking score (0 100) 0.56 ± ± ± ± Functional status on admission to rehabilitation Barthel Index (0 20) ± SD Mean number of ADLs* (0 6) Bladder incontinence Bowel incontinence 12.2 ± ± % 11.2% 11.9 ± ± % 23.1% Cognitive/psychological status Mean Mini-Mental Status Examination (0 30) Depression diagnosis 26.2 ± % 25.0 ± % Type of hip fracture and repair Femoral neck fracture Prosthesis Pins Nails Intertrochanteric fracture Subtrochanteric fracture 48.5% 69% 14% 12% 50.5% 1.0% 50.0% 74% 7% 11% 47.8% 2.2% *ADLs = activities of daily living, including bathing, dressing, eating, toileting, transferring, and walking. All intertrochanteric and subtrochanteric fractures were surgically managed with nails. of ADL recovery, all of the regression model parameter estimates for the group/staff HMO systems were positive, whereas all but one of the parameter estimates from the fee-for-service system were negative. This difference 234 Effective Clinical Practice September/October 2000 Volume 3 Number 5
7 TABLE 2 Services Provided to Hip Fracture Patients during the Index Rehabilitation Stay SERVICE FEE-FOR-SERVICE (n=196) HMO (n=140) P VALUE Initial rehabilitation admission to a skilled nursing facility 71.4% 93.6% Initial length of stay ± SD, d 22.5 ± ± Mean nursing time ± SD, hr Registered nurse, licensed practical nurse Aide/orderly/technician 19.8 ± ± ± ± Mean time in therapy ± SD, hr Physical therapist time Physical therapy department time* Occupational therapy department time 7.5 ± ± ± ± ± ± Provider visits Attending physician Consulting physician Physician s assistant/nurse practitioner Orthopedist Percentage with orthopedist visits Total physiatrist visits Percentage with physiatrist visits Total geriatrician visits Percentage with geriatrician visits % % % % % % 0.98 Hospitalization Rehospitalized during rehabilitation 1.5% 1.5% 0.99 *Includes time with the therapist as well as technicians. is not only consistent with the main result but also suggests that each health system made a similar contribution to the overall findings. Discussion Overall, we found little evidence to suggest that the outcomes of care for older adults with hip fracture receiving institutional rehabilitation differed between group/staff HMO and fee-for-service delivery systems. Our results add to the growing number of studies in the literature showing that the quality of care for patients within capitated payment systems is at least as good as that for patients in fee-for-service systems. What distinguishes our findings, however, is that we have shown that this relationship extends longitudinally across sites of geriatric care, to encompass an entire episode of care. When compared with previous studies that have examined the influence of reimbursement on the care delivered to persons with hip fracture, our study revealed a similar finding for the effect of bundled payment on the type of services provided. The intensity of physician services in particular was lower under the capitated payment of group/staff HMOs. Further, group/staff HMO plans seemed to have substituted personnel with less formal training for example, nurse practitioners and physician assistants for physicians, technicians for physical therapists, and aides and medical assistants for licensed nurses. Group/staff HMO patients had less intense involvement of orthopedic surgeons and physiatrists and more contact with geriatricians in the postacute care period. The association between greater geriatrician involvement with improved rehabilitative outcomes for hip fracture has been reported previously However, overall our findings are similar to these earlier studies, as differences in service intensity and care providers did not translate into meaningful differences in outcomes. Because of a potential for bias attributable to the disproportionately greater use of rehabilitation facilities by fee-for-service plans (29% vs. 6%), we conducted additional analyses of primary outcomes restricted to fee-for-service and group/staff HMO patients who were treated in SNFs. These results did not differ Effective Clinical Practice September/October 2000 Volume 3 Number 5 235
8 TABLE 3 Utilization in the Year after the Index Rehabilitation Stay* UTILIZATION VARIABLE FEE-FOR-SERVICE (n=187) GROUP/STAFF HMO (n=112) P VALUE Percentage rehospitalized by 12 months 39.0% 33.0% Number of emergency department visits Percentage of patients returning to rehabilitation after initial stay 15.0% 16.1% Average length of stay among those returning to rehabilitation after initial stay, d Total number of days in rehabilitation setting (initial + subsequent days) less ± SD 25.3 ± ± 27.6 Total physician visits outpatient Primary care visits outpatient Percentage receiving a primary care visit % % 0.04 Orthopedic surgeon visits outpatient Percentage receiving orthopedic surgeon visit % % Specialist physician (nonorthopedist) visits outpatient Percentage receiving a specialist visit % % Physician s assistant/nurse practitioner visits outpatient Home health visits ± SD Percentage receiving home health visit 2.8 ± % 8.8 ± % Physical therapy visits Percentage receiving physical therapy visit % % 0.10 Occupational therapy visits Percentage receiving occupational therapy visits % % 0.05 *Sample sizes reported in this table reflect absence of data due to a change in ownership in one managed care plan (n=25), nonmatching Medicare identification numbers among fee-for-service plans (n=8), and deaths that occurred during the index rehabilitation stay in fee-for-service (n=1) and group/staff HMO (n=3) facilities. from the main outcomes analyses and are not presented. These additional analyses support earlier published literature that outcomes among patients with hip fracture treated in SNFs differ little from those of patients 41, 42 treated in rehabilitation facilities and calls into question the value of the more resource-intensive rehabilitation facilities. However, these relationships between payment system, treatment setting, service intensity, and outcomes cannot be generalized beyond hip fracture. A similar study comparing patients with stroke in group/staff HMO and fee-for-service settings has found better functional and community discharge outcomes for persons with stroke treated in fee-forservice settings. 43 The patients in our study had better outcomes than those reported in previous studies. These improved outcomes may be partially explained by patient selection. Patients in this trial were more likely to recover by virtue of the fact that they were admitted for institutional rehabilitation (i.e., had a greater potential for recovery). Because of this sampling strategy, study participants were more similar and theoretically, more comparable. However, our results can only be generalized to those older patients with hip fracture receiving institutional rehabilitation. Our primary reason for targeting this particular population was that they have the greatest burden of disability, require the most services, and are the most costly to treat. Logically, a capitated 236 Effective Clinical Practice September/October 2000 Volume 3 Number 5
9 Number of Basic ADLs Recovered mo P < 0.05 FFS HMO 6 mo 9 mo 12 mo Time Participants Residing in Community 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% FFS HMO FIGURE 2. Recovery of basic activities of daily living (ADLs): fee-for-service (FFS) versus group/staff HMO systems. 0 3 mo 6 mo Time 9 mo 12 mo Ambulation Score mo mo Time FFS HMO P < mo 12 mo FIGURE 3. Ambulation score: fee-for-service (FFS) vs. group/staff HMOs. FIGURE 4. Community residence: fee-for-service (FFS) versus group/staff HMO systems. delivery system would focus cost-containment strategies on these patients and thus important differences may be revealed in studying this population. The results of our study need to be interpreted in light of several limitations. First, the facilities studied were not selected at random they were selected because of an established reputation for providing excellent geriatric rehabilitative services. Although studying these facilities is important for understanding the potential for improved outcomes for patients with hip fracture, this approach limits the generalizability of the findings. The delivery systems studied may not have been representative of capitated or fee-for-service delivery systems with a different organizational structure, longevity, or geographic location. Further, our focus was on a select population of older patients receiving institutional rehabilitation for hip fracture. We did not include patients who were able to return home immediately after their index hospitalization or those believed not to benefit from institutional rehabilitation. In addition, although we attempted to control for baseline differences between the two payment structure groups, we cannot exclude the possibility that our results were influenced by some degree of uncontrolled confounding. Study power may potentially have precluded detecting significant differences in the primary outcomes; however, our results revealed little suggestion of positive trends despite assessment of multiple outcome measures over four time points. Finally, although it would have strengthened these findings, a formal cost analysis was beyond the scope of this study s focus on clinical outcomes. In conclusion, we found no evidence that group/staff HMO systems delivered substandard care with respect to important clinical outcomes for older adults with hip fracture receiving institutional rehabilitation. Despite differences in service intensity, treatment location (i.e., subacute SNFs) and care providers, these well-integrated group/staff HMO plans were able to care for persons with hip fracture over the entire episode of care as effectively as select fee-for-service delivery systems. Although these results cannot be generalized to capitated or fee-for-service comparisons in other parts of the country, they do provide supportive evidence that the quality of acute hip fracture care in group/staff HMO delivery systems is at least as good as in fee-forservice delivery systems. Effective Clinical Practice September/October 2000 Volume 3 Number 5 237
10 Take-Home Points Although many studies have compared quality of care between capitated and fee-for-service payment systems in specific settings, none has compared outcomes for clinical conditions in which care is delivered longitudinally across multiple settings. We compared outcomes for patients receiving institutional rehabilitation after hip fracture in five group/staff HMO and six fee-for-service delivery systems with reputations for commitment to geriatric rehabilitation. Overall, there were no differences in functional recovery, ambulation scores, return to community living, or mortality between group/staff HMO and fee-for-service systems. Group/staff HMOs provided a lower intensity of physician services and substituted personnel with less formal training for physicians, physical therapists, and licensed nurses. Because the group/staff HMO and fee-for-service systems in our study were selected for their commitment to geriatric rehabilitation, caution is advised in generalizing our findings to other settings. References 1. Group Health Association of America. Patterns in HMO Enrollment. Washington, DC: Group Health Association of America; Miller RH, Luft HS. Does managed care lead to better or worse quality of care? Health Aff (Millwood). 1997;16: Retchin SM, Brown B. Management of colorectal cancer in Medicare health maintenance organizations. J Gen Intern Med. 1990;5: Retchin SM, Brown B. The quality of ambulatory care in Medicare health maintenance organizations. Am J Public Health. 1990;80: Carlisle DM, Siu AL, Keeler EB, et al. HMO vs fee-for-service care of older persons with acute myocardial infarction. Am J Public Health. 1992;82: Lurie N, Christianson J, Finch M, Moscovice I. The effects of capitation on health and functional status of the Medicaid elderly: a randomized trial. Ann Intern Med. 1994;120: Preston JA, Retchin SM. The management of geriatric hypertension in health maintenance organizations. J Am Geriatr Soc. 1991;39: Miller RH, Luft HS. Managed care plan performance since JAMA. 1994;271: Riley GF, Potosky AL, Klabunde CN, Warren JL, Ballard- Barbash R. Stage at diagnosis and treatment patterns among older women with breast cancer: an HMO and fee-for-service comparison. JAMA. 1999;281: Shaughnessy PW, Schlenker RE, Hittle DF. Home health care outcomes under capitated and fee-for-service payment. Health Care Financ Rev. 1994;16: Ware JE, Bayliss MS, Rogers WH, Kosinsiki M, Tarlov AR. Differences in 4-year health outcomes for elderly and poor chronically ill patients treated in HMO and fee-for-service systems. Results from the Medical Outcomes Study. JAMA. 1996; 276: Marottoli RA, Berkman LF, Leo-Summers L, Cooney LM. Predictors of mortality and institutionalization after hip fracture: The New Haven EPESE cohort. Am J Public Health. 1994;84: Cummings SR, Rubin SM, Black D. The future of hip fractures in the United States: numbers, costs, and potential effects of postmenopausal estrogen. Clin Orthop. 1990;252: Mossey JM, Mutran E, Knott K, Craik R. Determinants of recovery 12 months after hip fracture: the importance of psychosocial factors. Am J Public Health. 1989;79: Jette AM, Harris BA, Cleary PD, Campion EW. Functional recovery after hip fracture. Arch Phys Med Rehabil. 1987;68: Magaziner J, Simonsick E, Kashner M, Hebel JR, Kenzora JE. Predictors of functional recovery one year following hospital discharge for hip fracture: a prospective study. J Gerontol. 1990;45:M Lyons AR. Clinical outcomes and treatment of hip fractures. Am J Public Health. 1997;103:51S-63S. 18. Parker MJ, Palmer CR. Prediction of rehabilitation after hip fracture. Age Ageing. 1995;24: Lu-Yao GL, Baron JA, Barrett JA, Fisher ES. Treatment and survival among elderly Americans with hip fractures: a population-based study. Am J Public Health. 1994;84: Ray WA, Griffin MR, Baugh DK. Mortality following hip fracture before and after implementation of the prospective payment system. Arch Intern Med. 1990;150: Magaziner J, Simonsick EM, Kashner TM, Hebel JR, Kenzora JE. Survival experience of aged hip fracture patients. Am J Public Health. 1989;79: Ray WA, Griffin MR, Baugh DK. Mortality following hip fracture before and after implementation of the prospective payment system. Arch Intern Med. 1990;150: Gerety MB, Soderholm-Difatte V, Winograd CH. Impact of prospective payment and discharge location on the outcome of hip fracture. J Gen Intern Med. 1989;4: Fitzgerald JF, Fagan LF, Tierney WM, Dittus RS. Changing patterns of hip fracture care before and after the prospective payment system. JAMA. 1987;258: Fitzgerald JF, Moore DR. The care of elderly patients with hip fracture. Changes since implementation of the prospective payment system. N Engl J Med. 1989;320: Palmer RM, Saywell RM, Zollinger T, et al. The impact of the prospective payment system on the treatment of hip fractures in the elderly. Arch Intern Med. 1989;149: Morrison RS, Chassin MR, Siu AL. The medical consultant s role in caring for patients with hip fracture. Ann Intern Med. 1998;128: Kane RL, Finch M, Blewett L, Chen Q, Burns R, Moskowitz M. Use of post-hospital care by medicare patients. J Am Geriatr Soc. 1996;44: Prospective Payment Assessment Commission. The Changing Health Care Delivery Environment. In Medicare and the American Health Care System. Report to Congress. 1994;805: Kramer A, Steiner J, Kowalsky J. Rehab for the elderly. HMO Magazine. 1994;35: Effective Clinical Practice September/October 2000 Volume 3 Number 5
11 31. Folstein MF, Folstein SE, McHugh PR. Mini-Mental State : A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12: Charlson ME, Pompei P, Alex KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40: Wolinsky FD, Johnson RJ. The use of health services by older adults. J Gerontol. 1991;46:S Wolinsky FD, Callahan CM, Fitzgerald JF, Johnson RJ. The risk of nursing home placement and subsequent death among older adults. J Gerontol. 1992;47:S Fitzgerald JF, Smith DM, Martin DK, Freedman JA, Wolinsky FD. Replication of the multidimensionality of activities of daily living. J Gerontol. 1993;48:S Regensteinter JG, Steiner JF, Panzer RJ, Hiatt WR. Evaluation of walking impairment by questionnaire in patients with peripheral arterial disease. Journal of Vascular Medicine and Biology. 1990;2: Diehr P, Patrick DL, Hedrick S, et al. Including deaths when measuring health status over time. Med Care. 1995;33:AS Gustafson Y, Brännström B, Berggren D, et al. A geriatricanesthesiologic program to reduce acute confusional states in elderly patients treated for femoral neck fractures. J Am Geriatr Soc. 1991;39: Hempsall VJ, Robertson DRC, Campbell MJ, Briggs RS. Orthopedic geriatric care is it effective? J R Coll Physicians Lond. 1990;24: Zuckerman JD, Sakales SR, Fabian DR, Frankel VH. Hip fractures in geriatric patients: results of an interdisciplinary hospital care program. Clin Orthop. 1992;274: Kramer AM, Steiner JF, Schlenker RE, et al. Outcomes and costs after hip fracture and stroke. JAMA. 1997;277: Levi SJ. Posthospital setting, resource utilization, and self-care outcome in older women with hip fracture. Arch Phys Med Rehabil. 1997;78: Kramer AM, Kowalsky JC, Lin M, Grigsby J, Hughes R, Steiner J. Outcomes and utilization for acute stroke in HMO and fee-for-service delivery systems. J Am Geriatr Soc 2000; 48: Grant Support Supported by grant number from the Robert Wood Johnson Foundation. Dr. Coleman was a Hartford/Jahnigen Center of Excellence Faculty Recipient and Pfizer/American Geriatrics Society Fellow during preparation of this manuscript. Correspondence Eric A. Coleman, MD, MPH, Center on Aging Research, 3570 East 12th Avenue, Suite 300, Denver, CO 80206; telephone: ; fax: ; Eric.Coleman@uchsc.edu. Effective Clinical Practice September/October 2000 Volume 3 Number 5 239
AGS REHABILITATION/ POST-HOSPITAL CARE OF THE GERIATRIC FRACTURE PATIENT. Egan Allen, MD University of Rochester
 AGS REHABILITATION/ POST-HOSPITAL CARE OF THE GERIATRIC FRACTURE PATIENT Egan Allen, MD University of Rochester THE AMERICAN GERIATRICS SOCIETY Geriatrics Health Professionals. Leading change. Improving
AGS REHABILITATION/ POST-HOSPITAL CARE OF THE GERIATRIC FRACTURE PATIENT Egan Allen, MD University of Rochester THE AMERICAN GERIATRICS SOCIETY Geriatrics Health Professionals. Leading change. Improving
Where Should Rehabilitation Take Place?!
 Where Should Rehabilitation Take Place?! Three Basic Questions! 1. Is rehabilitation effective in improving a patient s functional abilities?!yes" yes" 2. Is rehabilitation cost effective?!yes" where"
Where Should Rehabilitation Take Place?! Three Basic Questions! 1. Is rehabilitation effective in improving a patient s functional abilities?!yes" yes" 2. Is rehabilitation cost effective?!yes" where"
Massachusetts PACE Evaluation Nursing Home Residency Summary Report. July 24, 2014
 Massachusetts PACE Evaluation Nursing Home Residency Summary Report July 24, 2014 JEN Associates, Inc. 5 Bigelow Street Cambridge, MA 02139 Phone: (617) 868-5578 Fax: (617) 868-7963 Contents Executive
Massachusetts PACE Evaluation Nursing Home Residency Summary Report July 24, 2014 JEN Associates, Inc. 5 Bigelow Street Cambridge, MA 02139 Phone: (617) 868-5578 Fax: (617) 868-7963 Contents Executive
Site-neutral payments for select conditions treated in inpatient rehabilitation facilities and skilled nursing facilities
 C h a p t e r6 Site-neutral payments for select conditions treated in inpatient rehabilitation facilities and skilled nursing facilities C H A P T E R 6 Site-neutral payments for select conditions treated
C h a p t e r6 Site-neutral payments for select conditions treated in inpatient rehabilitation facilities and skilled nursing facilities C H A P T E R 6 Site-neutral payments for select conditions treated
APROXIMAL FEMUR FRACTURE (hip fracture) is a
 ARTICLES Effect of Rehabilitation Site on Functional Recovery After Hip Fracture Michael C. Munin, MD, Karen Seligman, MS, Mary Amanda Dew, PhD, Tanya Quear, BS, Elizabeth R. Skidmore, PhD, OTR/L, Gary
ARTICLES Effect of Rehabilitation Site on Functional Recovery After Hip Fracture Michael C. Munin, MD, Karen Seligman, MS, Mary Amanda Dew, PhD, Tanya Quear, BS, Elizabeth R. Skidmore, PhD, OTR/L, Gary
How To Reduce Hospital Readmission
 Reducing Hospital Readmissions & The Affordable Care Act The Game Has Changed Drastically Reducing MSPB Measures Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE
Reducing Hospital Readmissions & The Affordable Care Act The Game Has Changed Drastically Reducing MSPB Measures Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE
There may be up to 5 to 6 million cases of. Treatment Costs of Community- Acquired Pneumonia in an Employed Population*
 Treatment Costs of Community- Acquired Pneumonia in an Employed Population* Gene L. Colice, MD, FCCP; Melissa A. Morley, MA; Carl Asche, PhD; and Howard G. Birnbaum, PhD Background: Community-acquired
Treatment Costs of Community- Acquired Pneumonia in an Employed Population* Gene L. Colice, MD, FCCP; Melissa A. Morley, MA; Carl Asche, PhD; and Howard G. Birnbaum, PhD Background: Community-acquired
Assisted living and nursing homes: Apples and oranges?
 Assisted living and nursing homes: Apples and oranges? Based upon the work of: Sheryl Zimmerman, MSW, PhD, Professor at the University of North Carolina, Chapel Hill School of Social Work Developed by
Assisted living and nursing homes: Apples and oranges? Based upon the work of: Sheryl Zimmerman, MSW, PhD, Professor at the University of North Carolina, Chapel Hill School of Social Work Developed by
Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge
 Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge PREPARED FOR: ARA Research Institute PRESENTED BY: Al Dobson, Ph.D. PREPARED
Assessment of Patient Outcomes of Rehabilitative Care Provided in Inpatient Rehabilitation Facilities (IRFs) and After Discharge PREPARED FOR: ARA Research Institute PRESENTED BY: Al Dobson, Ph.D. PREPARED
Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013
 Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013 GEORGIA HEALTH CARE ASSOCIATION Represents 336 skilled nursing facilities 13 SOURCE agencies 15 assisted living communities
Jon S. Howell, LNHA President & CEO Georgia Health Care Association November 18, 2013 GEORGIA HEALTH CARE ASSOCIATION Represents 336 skilled nursing facilities 13 SOURCE agencies 15 assisted living communities
Medicare- Medicaid Enrollee State Profile
 Medicare- Medicaid Enrollee State Profile Montana Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6
Medicare- Medicaid Enrollee State Profile Montana Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6
Measurements: Predisposing, enabling, and need measures were used to predict successful discharge to the community within 90 days.
 Conversion Diversion: Participation in a Social HMO Reduces the Likelihood of Converting From Short-Stay to Long-Stay Nursing Facility Placement Kathryn E. Thomas, PhD, Zachary D. Gassoumis, and Kathleen
Conversion Diversion: Participation in a Social HMO Reduces the Likelihood of Converting From Short-Stay to Long-Stay Nursing Facility Placement Kathryn E. Thomas, PhD, Zachary D. Gassoumis, and Kathleen
May 7, 2012. Submitted Electronically
 May 7, 2012 Submitted Electronically Secretary Kathleen Sebelius Department of Health and Human Services Office of the National Coordinator for Health Information Technology Attention: 2014 edition EHR
May 7, 2012 Submitted Electronically Secretary Kathleen Sebelius Department of Health and Human Services Office of the National Coordinator for Health Information Technology Attention: 2014 edition EHR
Abstract. Introduction. Number 84 n September 28, 2015
 Number 84 n September 28, 2015 Hospitalization, Readmission, and Death Experience of Noninstitutionalized Medicare Fee-for-service Beneficiaries Aged 65 and Over by Yelena Gorina M.S., M.P.H.; Laura A.
Number 84 n September 28, 2015 Hospitalization, Readmission, and Death Experience of Noninstitutionalized Medicare Fee-for-service Beneficiaries Aged 65 and Over by Yelena Gorina M.S., M.P.H.; Laura A.
Medicare- Medicaid Enrollee State Profile
 Medicare- Medicaid Enrollee State Profile North Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6 Spending...
Medicare- Medicaid Enrollee State Profile North Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6 Spending...
Background. Does the Organization of Post- Acute Stroke Care Really Matter? Changes in Provider Supply. Sites for Post-Acute Care.
 Does the Organization of Post- Acute Stroke Care Really Matter? Pamela W. Duncan, PhD, FAPTA University of Florida Brooks Center for Rehabilitation Studies Department of Veteran Affairs Rehabilitation
Does the Organization of Post- Acute Stroke Care Really Matter? Pamela W. Duncan, PhD, FAPTA University of Florida Brooks Center for Rehabilitation Studies Department of Veteran Affairs Rehabilitation
Attachment A Minnesota DHS Community Service/Community Services Development
 Attachment A Minnesota DHS Community Service/Community Services Development Applicant Organization: First Plan of Minnesota Project Title: Implementing a Functional Daily Living Skills Assessment to Predict
Attachment A Minnesota DHS Community Service/Community Services Development Applicant Organization: First Plan of Minnesota Project Title: Implementing a Functional Daily Living Skills Assessment to Predict
Comparison of Discharge Functional Status Rehabilitation: Hip Fracture Repair. Trudy Mallinson, PhD, OTR/L
 Comparison of Discharge Functional Status Rehabilitation: Hip Fracture Repair Trudy Mallinson, PhD, OTR/L Acknowledgements Co-authors Anne Deutsch, PhD, CRRN Jillian Bateman, OTD, OTR/L Hsiang-Yi Tseng,
Comparison of Discharge Functional Status Rehabilitation: Hip Fracture Repair Trudy Mallinson, PhD, OTR/L Acknowledgements Co-authors Anne Deutsch, PhD, CRRN Jillian Bateman, OTD, OTR/L Hsiang-Yi Tseng,
The Cost-Effectiveness of Homecare
 The Cost-Effectiveness of Homecare Homecare Reduces Costs by 37 Percent for Heart Failure Patients The May 2004 Journal of the American Geriatrics Society reports a study conducted at six Philadelphia
The Cost-Effectiveness of Homecare Homecare Reduces Costs by 37 Percent for Heart Failure Patients The May 2004 Journal of the American Geriatrics Society reports a study conducted at six Philadelphia
Care Transitions Model
 Supported by the john Care A. Hartford transitions foundation model 19 Care Transitions Model Starting when a patient is scheduled to be discharged from the hospital, the Care Transitions Model helps older
Supported by the john Care A. Hartford transitions foundation model 19 Care Transitions Model Starting when a patient is scheduled to be discharged from the hospital, the Care Transitions Model helps older
Health care accounts for a large and increasing share of the. Administrative and Claims Records as Sources of Health Care Cost Data
 CONDUCTING THE COST ANALYSIS Administrative and Claims Records as Sources of Health Care Cost Data Gerald F. Riley, MSPH Background: Many economic studies of disease require cost data at the person level
CONDUCTING THE COST ANALYSIS Administrative and Claims Records as Sources of Health Care Cost Data Gerald F. Riley, MSPH Background: Many economic studies of disease require cost data at the person level
October 2013 Family Choice: Best Practices in Care for Nursing Home Residents
 SNP Alliance Best Practices October 2013 Family Choice: Best Practices in Care for Nursing Home Residents Overview of Family Choice of New York I-SNP Independent Health s Medicare Advantage Family Choice
SNP Alliance Best Practices October 2013 Family Choice: Best Practices in Care for Nursing Home Residents Overview of Family Choice of New York I-SNP Independent Health s Medicare Advantage Family Choice
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION
 Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Performance Measurement for the Medicare and Medicaid Eligible (MME) Population in Connecticut Survey Analysis
 Performance Measurement for the Medicare and Medicaid Eligible (MME) Population in Connecticut Survey Analysis Methodology: 8 respondents The measures are incorporated into one of four sections: Highly
Performance Measurement for the Medicare and Medicaid Eligible (MME) Population in Connecticut Survey Analysis Methodology: 8 respondents The measures are incorporated into one of four sections: Highly
Patient and Hospital Characteristics Associated with Assessment For Rehabilitation During Hospitalization for Acute Stroke
 Patient and Hospital Characteristics Associated with Assessment For Rehabilitation During Hospitalization for Acute Stroke Lead Author: Janet Prvu Bettger, ScD, FAHA Duke University ; janet.bettger@duke.edu
Patient and Hospital Characteristics Associated with Assessment For Rehabilitation During Hospitalization for Acute Stroke Lead Author: Janet Prvu Bettger, ScD, FAHA Duke University ; janet.bettger@duke.edu
Discharge Planning. Home Care 1. Objectives. Where are they Going?
 Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Determinants of Nonrecovery following Hip Fracture in Older Adults: A Chronic Disease Trajectory Analysis Chapter I Introduction According to the
 Determinants of Nonrecovery following Hip Fracture in Older Adults: A Chronic Disease Trajectory Analysis Chapter I Introduction According to the American Academy of Orthopedic Surgeons (AAOS), the incidence
Determinants of Nonrecovery following Hip Fracture in Older Adults: A Chronic Disease Trajectory Analysis Chapter I Introduction According to the American Academy of Orthopedic Surgeons (AAOS), the incidence
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services. Discharge Planning
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services ICN 908184 October 2014 This booklet was current at the time it was published or uploaded onto the web. Medicare policy
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services ICN 908184 October 2014 This booklet was current at the time it was published or uploaded onto the web. Medicare policy
GENERAL ADMISSION CRITERIA INPATIENT REHABILITATION PROGRAMS
 Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
Admission to Inpatient Rehabilitation (Rehab) Services
 Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Nebraska Health Data Reporter
 Nebraska Health Data Reporter Volume 3, Number 1 May 2000 Demographic, health, and functional status characteristics of new residents to Nebraska nursing homes: A summary Joan Penrod, Ph.D. Jami Fletcher,
Nebraska Health Data Reporter Volume 3, Number 1 May 2000 Demographic, health, and functional status characteristics of new residents to Nebraska nursing homes: A summary Joan Penrod, Ph.D. Jami Fletcher,
OBJECTIVES FACTS AND FIGURES CMS CHRONIC CARE MANAGEMENT 10/20/2015. Another Step Towards Care Coordination
 CMS CHRONIC CARE MANAGEMENT Another Step Towards Care Coordination Care Coordination Patient/ Family Community Resources APARNA GUPTA, CRNP, MSN, PGDBA Transitions of Care Chronic Diseases OBJECTIVES AT
CMS CHRONIC CARE MANAGEMENT Another Step Towards Care Coordination Care Coordination Patient/ Family Community Resources APARNA GUPTA, CRNP, MSN, PGDBA Transitions of Care Chronic Diseases OBJECTIVES AT
Organization of Rehabilitation and Post-Acute Care
 Organization of Rehabilitation and Post-Acute Care Inaugural Meeting of NECC Boston, MA - September 13, 2006 Janet Prvu Bettger, ScD University of Pennsylvania Department of Physical Medicine and Rehabilitation
Organization of Rehabilitation and Post-Acute Care Inaugural Meeting of NECC Boston, MA - September 13, 2006 Janet Prvu Bettger, ScD University of Pennsylvania Department of Physical Medicine and Rehabilitation
Predicting nursing home length of stay : implications for targeting pre-admission review efforts
 Scholarly Commons at Miami University http://sc.lib.miamioh.edu Scripps Gerontology Center Scripps Gerontology Center Publications Predicting nursing home length of stay : implications for targeting pre-admission
Scholarly Commons at Miami University http://sc.lib.miamioh.edu Scripps Gerontology Center Scripps Gerontology Center Publications Predicting nursing home length of stay : implications for targeting pre-admission
Nurse Care Coordination of Older Patients in an Academic Family Medicine Clinic: 5-Year Outcomes
 Nurse Care Coordination of Older Patients in an Academic Family Medicine Clinic: 5-Year Outcomes Robin L. Kruse, PhD, Steven C. Zweig, MD, MSPH, Betty Nikodim, Joseph W. LeMaster, MD, MPH, Jared S. Coberly,
Nurse Care Coordination of Older Patients in an Academic Family Medicine Clinic: 5-Year Outcomes Robin L. Kruse, PhD, Steven C. Zweig, MD, MSPH, Betty Nikodim, Joseph W. LeMaster, MD, MPH, Jared S. Coberly,
Chapter 7: Inpatient & Outpatient Hospital Care
 7 Inpatient & Outpatient Hospital Care ACUTE INPATIENT ADMISSIONS All elective and emergent admissions require prior authorization and/or notification for all Health Choice Generations Members admissions.
7 Inpatient & Outpatient Hospital Care ACUTE INPATIENT ADMISSIONS All elective and emergent admissions require prior authorization and/or notification for all Health Choice Generations Members admissions.
Service delivery interventions
 Service delivery interventions S A S H A S H E P P E R D D E P A R T M E N T O F P U B L I C H E A L T H, U N I V E R S I T Y O F O X F O R D CO- C O O R D I N A T I N G E D I T O R C O C H R A N E E P
Service delivery interventions S A S H A S H E P P E R D D E P A R T M E N T O F P U B L I C H E A L T H, U N I V E R S I T Y O F O X F O R D CO- C O O R D I N A T I N G E D I T O R C O C H R A N E E P
Medicare- Medicaid Enrollee State Profile
 Medicare- Medicaid Enrollee State Profile Kentucky Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization...
Medicare- Medicaid Enrollee State Profile Kentucky Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization...
The Minnesota Senior Health Options Program: An Early Effort at Integrating Care for the Dually Eligible
 Journal of Gerontology: MEDICAL SCIENCES 2001, Vol. 56A, No. 9, M559 M566 Copyright 2001 by The Gerontological Society of America The Minnesota Senior Health Options Program: An Early Effort at Integrating
Journal of Gerontology: MEDICAL SCIENCES 2001, Vol. 56A, No. 9, M559 M566 Copyright 2001 by The Gerontological Society of America The Minnesota Senior Health Options Program: An Early Effort at Integrating
Functional recovery of hip fracture patients
 Functional recovery of hip fracture patients Lauren Beaupre July 7, 2011 ABSTRACT Hip fractures are common in the older population and are associated with loss of independence as well as high morbidity
Functional recovery of hip fracture patients Lauren Beaupre July 7, 2011 ABSTRACT Hip fractures are common in the older population and are associated with loss of independence as well as high morbidity
Medicare- Medicaid Enrollee State Profile
 Medicare- Medicaid Enrollee State Profile Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6 Spending...
Medicare- Medicaid Enrollee State Profile Centers for Medicare & Medicaid Services Introduction... 1 At a Glance... 1 Eligibility... 2 Demographics... 3 Chronic Conditions... 4 Utilization... 6 Spending...
HOSPITAL USE AND MORTALITY AMONG MEDICARE BENEFICIARIES IN BOSTON AND NEW HAVEN
 SPECIAL ARTICLE HOSPITAL USE AND MORTALITY AMONG MEDICARE BENEFICIARIES IN BOSTON AND NEW HAVEN JOHN E. WENNBERG, M.D., JEAN L. FREEMAN, PH.D., ROXANNE M. SHELTON, M.A., AND THOMAS A. BUBOLZ, PH.D. From
SPECIAL ARTICLE HOSPITAL USE AND MORTALITY AMONG MEDICARE BENEFICIARIES IN BOSTON AND NEW HAVEN JOHN E. WENNBERG, M.D., JEAN L. FREEMAN, PH.D., ROXANNE M. SHELTON, M.A., AND THOMAS A. BUBOLZ, PH.D. From
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY / PROCEDURE:
 PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
Inpatient rehabilitation facility services
 C h a p t e r10 Inpatient rehabilitation facility services R E C O M M E N D A T I O N 10 The Congress should eliminate the update to the Medicare payment rates for inpatient rehabilitation facilities
C h a p t e r10 Inpatient rehabilitation facility services R E C O M M E N D A T I O N 10 The Congress should eliminate the update to the Medicare payment rates for inpatient rehabilitation facilities
PREPARING THE PATIENT FOR TRANSFER TO AN INPATIENT REHABILITATON FACILITY (IRF) University Hospitals 8th Annual Neuroscience Nursing Symposium
 PREPARING THE PATIENT FOR TRANSFER TO AN INPATIENT REHABILITATON FACILITY (IRF) University Hospitals 8th Annual Neuroscience Nursing Symposium May 31, 2013 2 DEFINITION: INPATIENT REHABILITATION FACILITY
PREPARING THE PATIENT FOR TRANSFER TO AN INPATIENT REHABILITATON FACILITY (IRF) University Hospitals 8th Annual Neuroscience Nursing Symposium May 31, 2013 2 DEFINITION: INPATIENT REHABILITATION FACILITY
Using Objective Measures to Facilitate Rehabilitation Referral
 Using Objective Measures to Facilitate Rehabilitation Referral Mark Bayley MD, FRCPC Medical Director, Neuro Rehabilitation Program, Toronto Rehabilitation Institute Associate Professor, Division of Physiatry,
Using Objective Measures to Facilitate Rehabilitation Referral Mark Bayley MD, FRCPC Medical Director, Neuro Rehabilitation Program, Toronto Rehabilitation Institute Associate Professor, Division of Physiatry,
Hospitalization for acute medical illness frequently precipitates
 CLINICAL INVESTIGATION Recovery of Activities of Daily Living in Older Adults After Hospitalization for Acute Medical Illness Cynthia M. Boyd, MD, MPH, w C. Seth Landefeld, MD, z Steven R. Counsell, MD,
CLINICAL INVESTIGATION Recovery of Activities of Daily Living in Older Adults After Hospitalization for Acute Medical Illness Cynthia M. Boyd, MD, MPH, w C. Seth Landefeld, MD, z Steven R. Counsell, MD,
Nursing Homes, 1977 99:
 Nursing Homes, 1977 99: What Has Changed, What Has Not? Facts from the National Nursing Home Surveys by Frederic H. Decker, Ph.D., National Center for Health Statistics It has long been recognized that
Nursing Homes, 1977 99: What Has Changed, What Has Not? Facts from the National Nursing Home Surveys by Frederic H. Decker, Ph.D., National Center for Health Statistics It has long been recognized that
Home Health Care Today: Higher Acuity Level of Patients Highly skilled Professionals Costeffective Uses of Technology Innovative Care Techniques
 Comprehensive EHR Infrastructure Across the Health Care System The goal of the Administration and the Department of Health and Human Services to achieve an infrastructure for interoperable electronic health
Comprehensive EHR Infrastructure Across the Health Care System The goal of the Administration and the Department of Health and Human Services to achieve an infrastructure for interoperable electronic health
Risk Adjustment: Implications for Community Health Centers
 Risk Adjustment: Implications for Community Health Centers Todd Gilmer, PhD Division of Health Policy Department of Family and Preventive Medicine University of California, San Diego Overview Program and
Risk Adjustment: Implications for Community Health Centers Todd Gilmer, PhD Division of Health Policy Department of Family and Preventive Medicine University of California, San Diego Overview Program and
KEY POINTS TOWARDS QUALITY GERIATRIC CARE
 KEY POINTS TOWARDS QUALITY GERIATRIC CARE Carmel Bitondo Dyer, MD Professor and Director, Geriatric and Palliative Medicine Division Interim Chief of Staff, LBJ Hospital and Associate Dean of Harris County
KEY POINTS TOWARDS QUALITY GERIATRIC CARE Carmel Bitondo Dyer, MD Professor and Director, Geriatric and Palliative Medicine Division Interim Chief of Staff, LBJ Hospital and Associate Dean of Harris County
How Target: Heart Failure sm Can Help Facilitate Your Hospital s Efforts To Improve Quality and Reduce Heart Failure Readmissions
 How Target: Heart Failure sm Can Help Facilitate Your Hospital s Efforts To Improve Quality and Reduce Heart Failure Readmissions FACT SHEET THE PROBLEM It is estimated that one million heart failure patients
How Target: Heart Failure sm Can Help Facilitate Your Hospital s Efforts To Improve Quality and Reduce Heart Failure Readmissions FACT SHEET THE PROBLEM It is estimated that one million heart failure patients
Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required]
![Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required]](/thumbs/25/4903617.jpg) Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Medical Policy: MP-ME-05-09 Original Effective Date: February 18, 2009 Reviewed: April 22, 2011 Revised: This policy applies to products
Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Medical Policy: MP-ME-05-09 Original Effective Date: February 18, 2009 Reviewed: April 22, 2011 Revised: This policy applies to products
A Comprehensive Case Management Program to Improve Access to Palliative Care. Aetna s Compassionate Care SM
 A Comprehensive Case Management Program to Improve Access to Palliative Care Aetna s Compassionate Care SM Our chief want in life is somebody who shall make us do what we can. Ralph Waldo Emerson Marcia
A Comprehensive Case Management Program to Improve Access to Palliative Care Aetna s Compassionate Care SM Our chief want in life is somebody who shall make us do what we can. Ralph Waldo Emerson Marcia
The Home Health Pay-for-Performance Demonstration
 The Home Health Pay-for-Performance Demonstration Demonstration Overview and Terms & Conditions of Participation Centers for Medicare & Medicaid Services Office of Research, Development, and Information
The Home Health Pay-for-Performance Demonstration Demonstration Overview and Terms & Conditions of Participation Centers for Medicare & Medicaid Services Office of Research, Development, and Information
Summary Evaluation of the Medicare Lifestyle Modification Program Demonstration and the Medicare Cardiac Rehabilitation Benefit
 The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
The Centers for Medicare & Medicaid Services' Office of Research, Development, and Information (ORDI) strives to make information available to all. Nevertheless, portions of our files including charts,
The Panel Study of Income Dynamics Linked Medicare Claims Data
 Technical Series Paper #14-01 The Panel Study of Income Dynamics Linked Medicare Claims Data Vicki A. Freedman, Katherine McGonagle, Patricia Andreski Survey Research Center, Institute for Social Research
Technical Series Paper #14-01 The Panel Study of Income Dynamics Linked Medicare Claims Data Vicki A. Freedman, Katherine McGonagle, Patricia Andreski Survey Research Center, Institute for Social Research
Profile: Kessler Patients
 Profile: Kessler Patients 65 Breakthrough Years Kessler Institute has pioneered the course of medical rehabilitation since 1948. Today, as the nation s largest single rehabilitation hospital, we continue
Profile: Kessler Patients 65 Breakthrough Years Kessler Institute has pioneered the course of medical rehabilitation since 1948. Today, as the nation s largest single rehabilitation hospital, we continue
Care needs for dual-eligible beneficiaries
 C h a p t e r6 Care needs for dual-eligible beneficiaries C H A P T E R 6 Care needs for dual-eligible beneficiaries Chapter summary In this chapter Dual-eligible beneficiaries are eligible for both Medicare
C h a p t e r6 Care needs for dual-eligible beneficiaries C H A P T E R 6 Care needs for dual-eligible beneficiaries Chapter summary In this chapter Dual-eligible beneficiaries are eligible for both Medicare
ISSUED BY: TITLE: ISSUED BY: TITLE: President
 CLINICAL PRACTICE GUIDELINE PROFESSIONAL PRACTICE TITLE: Stroke Care Rehabilitation Unit DATE OF ISSUE: 2005, 05 PAGE 1 OF 7 NUMBER: CPG 20-3 SUPERCEDES: New ISSUED BY: TITLE: Chief of Medical Staff ISSUED
CLINICAL PRACTICE GUIDELINE PROFESSIONAL PRACTICE TITLE: Stroke Care Rehabilitation Unit DATE OF ISSUE: 2005, 05 PAGE 1 OF 7 NUMBER: CPG 20-3 SUPERCEDES: New ISSUED BY: TITLE: Chief of Medical Staff ISSUED
The Independent In-Person Assessment Process
 The Independent In-Person Assessment Process Jocelyn Gordon, Marc A. Cohen, and Jessica Miller Spring 2011 No. 4 The Community Living Assistance Services and Supports (CLASS) Plan a groundbreaking component
The Independent In-Person Assessment Process Jocelyn Gordon, Marc A. Cohen, and Jessica Miller Spring 2011 No. 4 The Community Living Assistance Services and Supports (CLASS) Plan a groundbreaking component
Predictors of Physical Therapy Use in Patients with Rheumatoid Arthritis
 Predictors of Physical Therapy Use in Patients with Rheumatoid Arthritis Maura Iversen,, PT, DPT, SD, MPH 1,2,3 Ritu Chhabriya,, MSPT 4 Nancy Shadick, MD 2,3 1 Department of Physical Therapy, Northeastern
Predictors of Physical Therapy Use in Patients with Rheumatoid Arthritis Maura Iversen,, PT, DPT, SD, MPH 1,2,3 Ritu Chhabriya,, MSPT 4 Nancy Shadick, MD 2,3 1 Department of Physical Therapy, Northeastern
GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services
 GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services Aged, Blind and Disabled Stakeholder Presentation Indiana Family and Social Services Administration August
GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services Aged, Blind and Disabled Stakeholder Presentation Indiana Family and Social Services Administration August
The role of t he Depart ment of Veterans Affairs (VA) as
 The VA Health Care System: An Unrecognized National Safety Net Veterans who use the VA health care system have a higher level of illness than the general population, and 60 percent have no private or Medigap
The VA Health Care System: An Unrecognized National Safety Net Veterans who use the VA health care system have a higher level of illness than the general population, and 60 percent have no private or Medigap
Stroke Rehabilitation Triage Severe Strokes
 The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
The London Stroke Rehab Data Base Project Robert Teasell MD FRCPC Professor and Chair-Chief Department of Phys Med Rehab London Ontario Retrospective Data Bases In stroke rehab limited funding for clinical
Impact of VA Home Based Primary Care: Access, Quality and Cost National Health Policy Forum
 Impact of VA Home Based Primary Care: Access, Quality and Cost National Health Policy Forum Thomas Edes, MD, MS Director, Geriatrics and Extended Care Office of Clinical Operations U.S. Department of Veterans
Impact of VA Home Based Primary Care: Access, Quality and Cost National Health Policy Forum Thomas Edes, MD, MS Director, Geriatrics and Extended Care Office of Clinical Operations U.S. Department of Veterans
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
Frequently Asked Questions about Fee-for-Service Medicare For People with Alzheimer s Disease
 Frequently Asked Questions about Fee-for-Service Medicare For People with Alzheimer s Disease This brochure answers questions Medicare beneficiaries with Alzheimer s disease, and their families, may have
Frequently Asked Questions about Fee-for-Service Medicare For People with Alzheimer s Disease This brochure answers questions Medicare beneficiaries with Alzheimer s disease, and their families, may have
Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education
 1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
Blueprint for Post-Acute
 Blueprint for Post-Acute Care Reform Post-acute care is a critical component within our nation s healthcare system and an essential aspect of care for many patients making a full recovery possible after
Blueprint for Post-Acute Care Reform Post-acute care is a critical component within our nation s healthcare system and an essential aspect of care for many patients making a full recovery possible after
PATTERNS OF POST-ACUTE UTILIZATION IN RURAL AND URBAN COMMUNITIES: HOME HEALTH, SKILLED NURSING, AND INPATIENT MEDICAL REHABILITATION.
 PATTERNS OF POST-ACUTE UTILIZATION IN RURAL AND URBAN COMMUNITIES: HOME HEALTH, SKILLED NURSING, AND INPATIENT MEDICAL REHABILITATION Final Report March 2005 Janet P. Sutton, Ph.D. NORC Walsh Center for
PATTERNS OF POST-ACUTE UTILIZATION IN RURAL AND URBAN COMMUNITIES: HOME HEALTH, SKILLED NURSING, AND INPATIENT MEDICAL REHABILITATION Final Report March 2005 Janet P. Sutton, Ph.D. NORC Walsh Center for
Utilization Review Cardiac Rehabilitation Services: Underutilized
 Utilization Review Cardiac Rehabilitation Services: Underutilized William J. Gill, MD Krannert Institute of Cardiology Indiana University School of Medicine Indianapolis, Indiana What is Cardiac Rehab?
Utilization Review Cardiac Rehabilitation Services: Underutilized William J. Gill, MD Krannert Institute of Cardiology Indiana University School of Medicine Indianapolis, Indiana What is Cardiac Rehab?
Providing and Billing Medicare for Transitional Care Management
 PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
Physician House Calls. vanishing practice, have experience a remarkable resurgence in interest in the last decade. 1
 Wayne Liang MPHP 439 Online Chapter Physician House Calls Outline: I. Introduction II. Why House Calls? Why Now? III. Comparing Physician House Calls & Home-Health Agencies IV. Modern House Call Programs
Wayne Liang MPHP 439 Online Chapter Physician House Calls Outline: I. Introduction II. Why House Calls? Why Now? III. Comparing Physician House Calls & Home-Health Agencies IV. Modern House Call Programs
Efficiency, Effectiveness, and Duration of Stroke Rehabilitation
 241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
Follow-up information from the November 12 provider training call
 Follow-up information from the November 12 provider training call Criteria I. Multiple Therapy Disciplines 1. Clarification regarding the use of group therapies in IRFs. Answer: CMS has not yet established
Follow-up information from the November 12 provider training call Criteria I. Multiple Therapy Disciplines 1. Clarification regarding the use of group therapies in IRFs. Answer: CMS has not yet established
Post Acute and Long Term Care: instrument for evaluating outcomes
 Post Acute and Long Term Care: instrument for evaluating outcomes National Network for Integrated Continuous Care Portugal RNCCI National Coordination Mission Unit for Integrated Continuous Care J.M. de
Post Acute and Long Term Care: instrument for evaluating outcomes National Network for Integrated Continuous Care Portugal RNCCI National Coordination Mission Unit for Integrated Continuous Care J.M. de
Stakeholder s Report. 2525 SW 75 th Ave Miami, Florida 33155 305.262.6800 www.westgablesrehabhospital.com
 212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
Measure Information Form (MIF) #275, adapted for quality measurement in Medicare Accountable Care Organizations
 ACO #9 Prevention Quality Indicator (PQI): Ambulatory Sensitive Conditions Admissions for Chronic Obstructive Pulmonary Disease (COPD) or Asthma in Older Adults Data Source Measure Information Form (MIF)
ACO #9 Prevention Quality Indicator (PQI): Ambulatory Sensitive Conditions Admissions for Chronic Obstructive Pulmonary Disease (COPD) or Asthma in Older Adults Data Source Measure Information Form (MIF)
Laura K Chiodo Meghan B Gerety Cynthia D Mulrow Mary C Rhodes Michael R Tuley. Key Words: Geriatncs, Long-term care, Nursing homes, Physical therapy.
 Research Report The Impact of Physical Therapy on Nursing Home Patient Outcomes The objective of this retrospective study was to assess the intensity and outcome of individual components of interdisciplinaly
Research Report The Impact of Physical Therapy on Nursing Home Patient Outcomes The objective of this retrospective study was to assess the intensity and outcome of individual components of interdisciplinaly
Fall 2013. A progress report on improving rehabilitative care in Waterloo Wellington
 Fall 2013 A progress report on improving rehabilitative care in Waterloo Wellington The Waterloo Wellington Rehabilitative Care Council Improving rehabilitative care in Waterloo Wellington, fall 2013,
Fall 2013 A progress report on improving rehabilitative care in Waterloo Wellington The Waterloo Wellington Rehabilitative Care Council Improving rehabilitative care in Waterloo Wellington, fall 2013,
FACTORS ASSOCIATED WITH HEALTHCARE COSTS AMONG ELDERLY PATIENTS WITH DIABETIC NEUROPATHY
 FACTORS ASSOCIATED WITH HEALTHCARE COSTS AMONG ELDERLY PATIENTS WITH DIABETIC NEUROPATHY Luke Boulanger, MA, MBA 1, Yang Zhao, PhD 2, Yanjun Bao, PhD 1, Cassie Cai, MS, MSPH 1, Wenyu Ye, PhD 2, Mason W
FACTORS ASSOCIATED WITH HEALTHCARE COSTS AMONG ELDERLY PATIENTS WITH DIABETIC NEUROPATHY Luke Boulanger, MA, MBA 1, Yang Zhao, PhD 2, Yanjun Bao, PhD 1, Cassie Cai, MS, MSPH 1, Wenyu Ye, PhD 2, Mason W
What Providers Need To Know Before Adopting Bundling Payments
 What Providers Need To Know Before Adopting Bundling Payments Dan Mirakhor Master of Health Administration University of Southern California Dan Mirakhor is a Master of Health Administration student at
What Providers Need To Know Before Adopting Bundling Payments Dan Mirakhor Master of Health Administration University of Southern California Dan Mirakhor is a Master of Health Administration student at
TORONTO STROKE FLOW INITIATIVE - Outpatient Rehabilitation Best Practice Recommendations Guide (updated July 26, 2013)
 Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
SMD# 13-001 ACA #23. Re: Health Home Core Quality Measures. January 15, 2013. Dear State Medicaid Director:
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-26-12 Baltimore, Maryland 21244-1850 SMD# 13-001 ACA #23 Re: Health Home Core Quality
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-26-12 Baltimore, Maryland 21244-1850 SMD# 13-001 ACA #23 Re: Health Home Core Quality
How To Cover Occupational Therapy
 Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
CMS Innovation Center Improving Care for Complex Patients
 CMS Innovation Center Improving Care for Complex Patients ECRI Institute Dr. Patrick Conway, M.D., MSc CMS Chief Medical Officer and Deputy Administrator for Innovation and Quality Director, Center for
CMS Innovation Center Improving Care for Complex Patients ECRI Institute Dr. Patrick Conway, M.D., MSc CMS Chief Medical Officer and Deputy Administrator for Innovation and Quality Director, Center for
Using Medicare Hospitalization Information and the MedPAR. Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota
 Using Medicare Hospitalization Information and the MedPAR Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota MedPAR Medicare Provider Analysis and Review Includes information
Using Medicare Hospitalization Information and the MedPAR Beth Virnig, Ph.D. Associate Dean for Research and Professor University of Minnesota MedPAR Medicare Provider Analysis and Review Includes information
Reducing Readmissions with Predictive Analytics
 Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
2014: Volume 4, Number 1. A publication of the Centers for Medicare & Medicaid Services, Office of Information Products & Data Analytics
 2014: Volume 4, Number 1 A publication of the Centers for Medicare & Medicaid Services, Office of Information Products & Data Analytics Medicare Post-Acute Care Episodes and Payment Bundling Melissa Morley,¹
2014: Volume 4, Number 1 A publication of the Centers for Medicare & Medicaid Services, Office of Information Products & Data Analytics Medicare Post-Acute Care Episodes and Payment Bundling Melissa Morley,¹
PL 111-148 and Amendments: Impact on Post-Acute Care for Health Care Systems
 PL 111-148 and Amendments: Impact on Post-Acute Care for Health Care Systems By Kathleen M. Griffin, PhD. There are three key provisions of the law that will have direct impact on post-acute care needs
PL 111-148 and Amendments: Impact on Post-Acute Care for Health Care Systems By Kathleen M. Griffin, PhD. There are three key provisions of the law that will have direct impact on post-acute care needs
North Carolina Online Stroke Rehabilitation Inventory
 North Carolina Online Stroke Rehabilitation Inventory Sarah Myer, MPH, CHES Community and Clinical Connections For Prevention and Health Branch Justus-Warren Heart Disease and Stroke Prevention Task Force
North Carolina Online Stroke Rehabilitation Inventory Sarah Myer, MPH, CHES Community and Clinical Connections For Prevention and Health Branch Justus-Warren Heart Disease and Stroke Prevention Task Force
MONTANA. Downloaded January 2011
 MONTANA Downloaded January 2011 37.40.202 PREADMISSION SCREENING, GENERAL REQUIREMENTS (1) This rule provides the preadmission screening requirements of the Montana Medicaid program for applicants to nursing
MONTANA Downloaded January 2011 37.40.202 PREADMISSION SCREENING, GENERAL REQUIREMENTS (1) This rule provides the preadmission screening requirements of the Montana Medicaid program for applicants to nursing
Continuity of Care for Elderly Patients with Diabetes Mellitus, Hypertension, Asthma, and Chronic Obstructive Pulmonary Disease in Korea
 ORIGINAL ARTICLE Medicine General & Social Medicine DOI: 10.3346/jkms.2010.25.9.1259 J Korean Med Sci 2010; 25: 1259-1271 Continuity of Care for Elderly Patients with Diabetes Mellitus, Hypertension, Asthma,
ORIGINAL ARTICLE Medicine General & Social Medicine DOI: 10.3346/jkms.2010.25.9.1259 J Korean Med Sci 2010; 25: 1259-1271 Continuity of Care for Elderly Patients with Diabetes Mellitus, Hypertension, Asthma,
Preventing Readmissions
 Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
PART I : NAVIGATING HEALTH CARE
 PART I : NAVIGATING HEALTH CARE SECTION ONE Hospitals, Clinical Trials & Ambulance Service 1. Should my dad just sign all those hospital consent forms or actually question them? 2. What is a hospital Patient
PART I : NAVIGATING HEALTH CARE SECTION ONE Hospitals, Clinical Trials & Ambulance Service 1. Should my dad just sign all those hospital consent forms or actually question them? 2. What is a hospital Patient
Inpatient rehabilitation facility services
 Inpatient rehabilitation facility services C H A P T E R9 R E C O M M E N D A T I O N 9 The Congress should eliminate the update to the Medicare payment rates for inpatient rehabilitation facilities in
Inpatient rehabilitation facility services C H A P T E R9 R E C O M M E N D A T I O N 9 The Congress should eliminate the update to the Medicare payment rates for inpatient rehabilitation facilities in
Transforming Care for Medicare Beneficiaries with Chronic Conditions and Long-Term Care Needs: Coordinating Care Across All Services
 Transforming Care for Medicare Beneficiaries with Chronic Conditions and Long-Term Care Needs: Coordinating Care Across All Services Harriet L. Komisar and Judy Feder Georgetown University October 2011
Transforming Care for Medicare Beneficiaries with Chronic Conditions and Long-Term Care Needs: Coordinating Care Across All Services Harriet L. Komisar and Judy Feder Georgetown University October 2011
Spinal cord injury hospitalisation in a rehabilitation hospital in Japan
 1994 International Medical Society of Paraplegia Spinal cord injury hospitalisation in a rehabilitation hospital in Japan Y Hasegawa MSW, l M Ohashi MD, l * N Ando MD, l T. Hayashi MD, l T Ishidoh MD,
1994 International Medical Society of Paraplegia Spinal cord injury hospitalisation in a rehabilitation hospital in Japan Y Hasegawa MSW, l M Ohashi MD, l * N Ando MD, l T. Hayashi MD, l T Ishidoh MD,
Dana L. Judd, PT, DPT
 CURRICULUM VITAE Dana L. Judd, PT, DPT University of Colorado Physical Therapy Program Muscle Performance Laboratory 13121 E 17 th Ave, Mail Stop C244 80045 303-724-9590 (w) 303-724-2444 (f) Dana.Judd@ucdenver.edu
CURRICULUM VITAE Dana L. Judd, PT, DPT University of Colorado Physical Therapy Program Muscle Performance Laboratory 13121 E 17 th Ave, Mail Stop C244 80045 303-724-9590 (w) 303-724-2444 (f) Dana.Judd@ucdenver.edu
