Care Transitions Model
|
|
|
- Easter Cameron
- 8 years ago
- Views:
Transcription
1 Supported by the john Care A. Hartford transitions foundation model 19 Care Transitions Model Starting when a patient is scheduled to be discharged from the hospital, the Care Transitions Model helps older patients at high risk for complications or rehospitalization. The Transition Coach, a specially trained nurse, visits with the patient and their caregivers over four weeks both in the hospital and at home and helps patients learn to manage multiple prescriptions, follow post-hospital recommendations, and present their other health care providers with the information they need to be effective. Over 100 hospitals and health care systems had adopted the model by Geriatric Interdisciplinary Teams in Practice Care Transitions Model Eric Coleman, MD, MPH, Principal Investigator, University of Colorado Supported by the John A. Hartford Foundation
2 2 HARTFORD Geriatric Interdisciplinary Teams in Practice Improving Transitions Across Sites of Geriatric Care To address the problems of uncoordinated and fragmented care around the period of hospitalization, the Foundation awarded the University of Colorado Health Sciences Center, Denver, Colorado, a five-year grant of $1,207,404 in 2000 to develop the Care Transitions Intervention. Dr. Eric Coleman served as principal investigator of this project. Dr. Coleman is a Robert Wood Johnson Clinical Scholar and a Beeson Scholar. He has served on the American Geriatrics Society health care systems committee and has worked with federal policy makers through convenings such as those of the National Health Policy Forum. Older patients with serious or multiple chronic illnesses are at risk for suffering new health problems or worsening of their existing conditions following a hospital stay. For example, a patient with diabetes who has received confusing or possibly conflicting information about a change in his medication regimen while in the hospital may wind up with uncontrolled blood sugar levels. Older patients with complicated health problems often see numerous health care providers, a number that increases if treatment in a hospital becomes necessary. The patient may be treated by a primary care physician and various specialists in their medical offices, a hospitalist physician and nursing team in the hospital, a different physician and nursing team during a stay in a skilled nursing facility, and a visiting nurse in the home. Care can become fragmented when these providers work independently of one another or, worse, at cross purposes. Even when each health care provider delivers high quality care, the result can be substandard care if their efforts are not coordinated. Eric Coleman, MD, MPH Principal Investigator, Care Transitions University of Colorado 12- Coleman EA, Min S, Chomiak A, Kramer AM. Post-hospital care transitions: patterns, complications, and risk identification. Health Serv Res. 2004;39: Centers for Medicare and Medicaid Services. Medicare Quality Monitoring System GenInfo/15_MQMS.asp. Shorter hospital stays and inefficient systems for transferring medical information from one health care site to another often place a burden on patients and their families to navigate the complex health care system. Yet patients and their families rarely receive adequate information and preparation to manage and coordinate care after a hospital stay. Lack of coordination on the part of health care providers and inadequate preparation of patients increases the risk for medication errors and health complications. This leads to avoidable readmissions to the hospital, leading to greater health care costs. National 30-day readmission rates among older Medicare beneficiaries range from 15 to 25 percent. 12,13
3 Care transitions model 3 Medication errors are of particular concern. A study by Dr. Eric Coleman and colleagues found that 14 percent of elderly patients admitted to the hospital experienced one or more discrepancies between their prehospital medication regimen, posthospital medication regimen, and what the patient reported actually taking. 14 Factors involving patients, such as misunderstandings and other reasons for not complying with the regimen, contributed to about half of the medication errors. The other half of the errors were attributable to prescribers or the broader health care system. Medication discrepancies led to a greater number of hospital readmissions within 30 days. Dr. Eric Coleman and his colleagues at the University of Colorado Health Sciences Center developed the Care Transitions Intervention team care model ( to address these problems. The Care Transitions Intervention focuses on providing support and education for the patient and family caregiver. Interdisciplinary team care generally does not extend beyond the walls of a given institution. The only common thread moving across all sites of care is the patient and the caregiver, who become de facto care coordinators. If you re selling umbrellas, you have to figure out how to make it rain. We make it rain by reshaping the health care environment to embrace these team care models. Eric Coleman, MD, MPH Principal Investigator, Care Transitions We need to fix the broken health care system where providers don t talk to each other, says Dr. Coleman. But in the meantime, we need to support patients and families in their self-management role. Placing the older adult patient (and caregiver) at the center of the interdisciplinary team in no way abdicates the responsibilities of the health care professionals. This arrangement encourages greater accountability for ensuring that the essential steps that need to take place before and after transfer are executed. The Four Pillars of Care Transitions During the four-week Care Transitions program, patients with complex care needs and family caregivers work with a Transition Coach and learn self-management skills that will ease their transition from hospital to home. The coach is an advanced practice nurse or a registered nurse who has received training in the Care Transitions Intervention program. This intervention is centered on four pillars: 1. Medication self-management 2. The Personal Health Record 3. Timely primary care/specialty care follow up 4. Knowledge of red flags that indicate a worsening in their condition and how to respond 14- Coleman EA, Smith JD, Raha D, Min S. Posthospital medication discrepancies. Arch Intern Med. 2005;165:
4 4 HARTFORD Geriatric Interdisciplinary Teams in Practice A low-tech but highly effective tool developed by the Care Transitions team the Personal Health Record helps patients track prescriptions and instructions from their different doctors and other health care providers. By bringing the record to each visit, patients can keep their different doctors informed and reduce the risk of rehospitalization or medication errors. The transition coach visits the patient for the first time just prior to discharge from the hospital and then makes a home visit a few days later. During this home visit, the coach reviews all of the medications the patient is taking. If errors are detected or if the regimen is confusing or impractical, the coach helps the patient and family caregiver to communicate their questions and concerns to the relevant health care provider. The coach also educates the patient about warning signs (red flags) that the patient s condition may be worsening and helps him or her to understand when to call the physician or other health care provider. If patients have particular questions or concerns about their care, if they ve received conflicting instructions from different care providers, or if they simply need clarification about something, the coach supports them in communicating with their care providers. The coach also instructs the patient in the use of the Personal Health Record, in which the patient records medicines and administration schedules, allergies, instructions from health care providers, red flags for his or her disease, and questions and concerns to discuss at future health care visits.
5 Care transitions model 5 The Care Transitions Model focuses on patients at high risk for complications or rehospitalization. Prior to discharge from the hospital, a specially trained nurse (the coach) visits the patient to begin the process of a successful transition to self management at home. The Transition Coach For patients released to a skilled nursing facility, the coach makes a second visit prior to discharge home. At the home visit, the coach: n Reviews medication orders n Educates about warning signs ( red flags ) of a worsening condition n Reviews the Personal Health Record n Provides support in communicating with care providers Three follow-up phone calls are made by the coach: two days later, a week after that, and then two weeks later. Geriatric Interdisciplinary Teams in Practice Care Transitions Model Eric Coleman, MD, MPH, Principal Investigator, University of Colorado Supported by the John A. Hartford Foundation
6 6 HARTFORD Geriatric Interdisciplinary Teams in Practice We recognized that even smart, innovative models can wind up with no takers if they turn out to be impractical from the standpoint of the delivery system. Eric Coleman, MD, MPH Principal Investigator, Care Transitions Structured visits and phone calls by the coach promote safe transitions during the critical first month at home following a hospitalization. The patient is encouraged to call the coach at any time with questions. For patients discharged from the hospital to a skilled nursing facility, once weekly the coach visits the skilled nursing facility until the patient returns home. Patients really have a chance to regain their independence through this program, says Kathryn Botinelli, Transitions Coach, Centura Home Health, Denver, Colorado. She has witnessed the change in patients from being confused and overwhelmed to feeling confident and being active participants in their own healing. The program, and particularly the Personal Health Record, helps them to feel that they can talk to the doctor instead of just being talked at by the doctor, she says. While the Care Transitions program lasts for just one month, the impact has been shown to be more long-lasting. The patients who participate in the program have complex chronic illnesses and therefore are at high risk for repeat hospitalizations. They use the self-management skills learned during the program in subsequent episodes of care transitions. Measuring the Success of Care Transitions With the Care Transitions Intervention model patient health and well-being are improved and the health care system derives cost savings from reduced readmission to the hospital. Both patients and health care providers report satisfaction with the program. 15- Coleman EA, Smith JD, Frank JC, Min SJ, Parry C, Kramer A. Preparing patients and caregivers to participate in care delivered across settings: the care transitions intervention. J Am Geriatr Soc. 2004;52: Coleman EA, Parry C, Chalmers S, Min SJ. The care transitions intervention: results of a randomized controlled trial. Arch Intern Med. 2006;166: These results were demonstrated in studies conducted by Dr. Coleman and his colleagues. In one study, performed in 2004, hospitalized patients who received the Care Transitions Intervention were approximately half as likely to return to the hospital as those who did not receive the intervention. 15 In a study from 2006, which was funded by the Hartford Foundation, patients receiving the Care Transitions Intervention also had lower rehospitalization rates. 16 This study also found that hospital costs were lower for patients with care transition coaches. The investigators estimated that the hospital, health plan, or clinic which employs the coach can realize annual net cost savings of $295,594 across 350 patients. Dr. Coleman s team has also shown that patients who were assisted by care transitions coaches had greater knowledge and skills regarding
7 Care transitions model 7 their illness. 17 They understood how to manage their medications and they confidently knew what was required of them during the transition period. The continuity of the coaching relationship fostered a sense of caring, safety, and predictability about the transition, which contributed to greater patient investment in the program. Moving the Model from Two Sites to 100 The Care Transitions model was initially tested in two health systems: Kaiser Permanente of Denver and Centura Health. Even after the demonstration project was completed, these institutions continue to utilize the Care Transitions Intervention. Efforts to disseminate the model to other institutions have resulted in 100 organizations adopting the model by the end of Of the four team care models in the dissemination of GIT-P grant, the Care Transitions model is the most widely disseminated. One surprise for Dr. Coleman and his team has been the diversity of health care delivery systems that have adopted the model. In developing the model, the team felt that it was a natural fit for Medicare Advantage (Medicare Managed Care Plans). They have also partnered with hospitals and home care agencies. One key to the Colorado team s success in disseminating their model lies in the groundwork laid from the beginning. Early on we were encouraged to think about what the end adopters would need, says Dr. Coleman. As part of the initial grant, the Hartford Foundation had asked them to write a business plan, which proved to be pivotal to the success of the program. He and his team put together a panel of experts (the key decision makers from health plans, hospitals, nursing homes, and home care agencies), presented the model, and sought input from the outset. They received concrete suggestions, which were used to alter the model. These recommendations, combined with input from patients and families, allowed Dr. Coleman and his colleagues to create a model that was likely to be implemented. Dr. Coleman also emphasizes that widespread dissemination depends on influencing the health care environment to build demand for this and other models of team care. Traditionally, a new model of care is developed and tested and then marketed to the end user or adopter. Dr. Coleman advocates a different approach. He works to influence the delivery system to make effective team care, including improved transitions across sites of care, a requirement. For example, Dr. Coleman and his colleagues partnered with the consumer The Care Transitions program is attractive because it is a relatively low cost and relatively simple intervention that has the potential to produce a very good return on the investment, both in terms of clinical outcomes and financially. Alan Lazaroff, MD Director of Geriatric Medicine, Centura Senior Life Center Denver, Colorado Adopter of Care Transitions Intervention In Denver, CO, Frank Yanni meets with his primary care physician, Alan Lazaroff, MD, at Centura Senior Life Center several weeks after being discharged from the hospital. 17- Parry C, Kramer H, Coleman EA. A qualitative exploration of a patient-centered coaching intervention to improve care transitions in chronically ill older adults. Home Health Serv Q. 2006;25(3-4):39-53.
8 8 HARTFORD Geriatric Interdisciplinary Teams in Practice A Transition Coach Makes Recovery from Surgery Faster, Easier When Frank Yanni, 69, a participant in the Care Transitions Intervention program, noticed that the pain he was experiencing weeks after surgery for a staph infection of the spinal cord was not only not getting better but was getting worse, he knew to insist that it be looked into. A magnetic resonance imaging test revealed a postoperative infection that required a second surgery. Had he let that go for even another week, he could have ended up in the ICU, septic and horribly sick, says Kathryn Botinelli, Frank s transition coach. As a former ICU nurse, Kathryn Bottinelli, RN, Transitions Coach, Centura Home Health, Denver, (Above) After coming home from spinal cord surgery, Frank Yanni and Transition Coach Kathryn Bottinelli, RN, review Mr. Yanni's upcoming appointments. (Right) The Personal Health Record provides Mr. Yanni and his wife Beatrice with an easy reference for medications information, post-hospital care needs, and space to log questions for the next time they visit the doctor. Colorado, has witnessed the devastating consequences when older adult patients fail to recognize early warning signs of an exacerbation of their illness and wind up critically ill. Now working as a Transitions Coach, Ms. Bottinelli is particularly interested in educating patients just discharged from the hospital about warning signs of complications that require early attention before a crisis occurs. Ms. Botinelli began working with Frank and his wife Beatrice in August She first met the Yannis in the hospital when Frank was preparing to go home. The first surgery for the infection had left Frank in pain, for which he needed potent medications. Ms. Botinelli focused much of her work with the Yannis on pain control issues. Frank relied heavily on his wife to keep track of his medication schedule. Our little purple book [the Personal Health Record] has been a great help to us, says Beatrice. I can keep track of all his medications. Because Frank s medications were changed frequently, Ms. Botinelli worked closely with the couple on medication reconciliation. Ms. Botinelli also helped Frank with goal setting. He set as his goals being free from pain and being able to walk unaided. After the second surgery, Frank began to feel markedly better. The pain was diminishing and he was able to start physical therapy, including water aerobics, to regain mobility. He is steadily getting better and is optimistic that he will achieve his goals. Having the opportunity to work with a Transitions Coach meant a lot to the Yannis. Kathryn has been a great help to us, says Beatrice. Working with her was very rewarding for me, adds Frank. Ms. Botinelli also derives great satisfaction from working with the Yannis and other patients and family caregivers as their coach. She sees patients who are able to maintain their independence largely because they have access to the tools provided by the program, such as the Personal Health Record where they can read about red flags for their condition, write down the content of conversations with their coach and health care providers, and keep track of medications. This can be especially helpful for patients experiencing memory difficulties. With the Personal Health Record, patients feel more intelligent talking to the doctor, says Ms. Botinelli. And it helps the physician, especially for patients seeing multiple health care providers at different sites. The patient feels more like a member of the team and the doctor talks to the patient with more respect, which motivates the patient to be more active in his or her own heath care, she adds, and the patients heal quicker.
9 Care transitions model 9 representatives to the Joint Commission, a national accrediting body for hospitals and other health settings. This ultimately led to changes in the requirements of the Joint Commission regarding how patients are moved across the health care system. A Joint Commission Resources publication, titled Improving Hand-Off Communication, features the Care Transitions Intervention model. This is how we create an environment that identifies a need for innovation and then we present our model as the logical solution, says Dr. Coleman. Other changes in health care policy also work to the advantage of dissemination of the Care Transitions Intervention model. For example, hospitals are now required to publicly report 30- day readmission rates. A program such as the Care Transitions Intervention, which has proven to reduce readmission rates, becomes even more desirable. Creating the Care Transitions Intervention model required creativity and innovation; developing the avenues for dissemination and widespread adoption necessitates a different skill set, but just as much innovation. Eric Coleman, MD, MPH Principal Investigator, Care Transitions Dr. Coleman continues to foster awareness of the poor quality of many care transitions, their adverse consequences for elderly patients and the need for reform. He does this through specially convened meetings of national and regional health care leaders, briefings with federal officials and other regulatory bodies, publications, speeches, and the Care Transitions Program Web site ( His efforts have paid off as there is now much more system-wide recognition of the importance of this problem and a willingness to address it. The long-standing commitment of the Hartford Foundation to the creation and dissemination of the Care Transitions Intervention model has allowed the University of Colorado Health Sciences Center to raise over $2.5 million in support of the model from additional funders. Sources of funding have come from the following: CMS (in partnership with the Colorado QIO) Community Health Foundation of Western and Central NY California Health Care Foundation Robert Wood Johnson Foundation Christus Health Care National Institutes of Health Aetna Foundation
THE CARE INTERVENTION: IMPROVING TRANSITIONS ACROSS SITES OF CARE
 THE CARE TRANSITIONS INTERVENTION: IMPROVING TRANSITIONS ACROSS SITES OF CARE FUNDING PROVIDED BY THE JOHN A. HARTFORD FOUNDATION AND THE ROBERT WOOD JOHNSON FOUNDATION RECOMMENDED CITATION: USERS MANUAL:
THE CARE TRANSITIONS INTERVENTION: IMPROVING TRANSITIONS ACROSS SITES OF CARE FUNDING PROVIDED BY THE JOHN A. HARTFORD FOUNDATION AND THE ROBERT WOOD JOHNSON FOUNDATION RECOMMENDED CITATION: USERS MANUAL:
What Do We Know? Does the Current Evidence Support Business as Usual? Eric A. Coleman, MD, MPH
 Listen to Your Patients They Are Telling You How to Improve the Quality of their Transitional Care Eric A. Coleman, MD, MPH, AGSF, FACP Professor of Medicine Director, Care Transitions Program University
Listen to Your Patients They Are Telling You How to Improve the Quality of their Transitional Care Eric A. Coleman, MD, MPH, AGSF, FACP Professor of Medicine Director, Care Transitions Program University
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION
 Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education
 1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
AVOID READMISSIONS through COLLABORATION March 23, 2011 ARC Webinar
 Mary D. Naylor, PhD, RN, FAAN Marian S. Ware Professor in Gerontology Director, NewCourtland Center for Transitions and Health University of Pennsylvania School of Nursing AVOID READMISSIONS through COLLABORATION
Mary D. Naylor, PhD, RN, FAAN Marian S. Ware Professor in Gerontology Director, NewCourtland Center for Transitions and Health University of Pennsylvania School of Nursing AVOID READMISSIONS through COLLABORATION
hospital readmission rate reduction: building better interfaces within the community.
 hospital readmission rate reduction: building better interfaces within the community. Whitepaper By Ken Taverner, M.Sc. the issue of hospital readmission rates Leaving the hospital after being admitted
hospital readmission rate reduction: building better interfaces within the community. Whitepaper By Ken Taverner, M.Sc. the issue of hospital readmission rates Leaving the hospital after being admitted
1900 K St. NW Washington, DC 20006 c/o McKenna Long
 1900 K St. NW Washington, DC 20006 c/o McKenna Long Centers for Medicare & Medicaid Services U. S. Department of Health and Human Services Attention CMS 1345 P P.O. Box 8013, Baltimore, MD 21244 8013 Re:
1900 K St. NW Washington, DC 20006 c/o McKenna Long Centers for Medicare & Medicaid Services U. S. Department of Health and Human Services Attention CMS 1345 P P.O. Box 8013, Baltimore, MD 21244 8013 Re:
Transitions of Care: The need for a more effective approach to continuing patient care
 H O T T O P I C S I N H E A L T H C A R E Transitions of Care: The need for a more effective approach to continuing patient care The need for a more effective approach to continuing patient care This paper
H O T T O P I C S I N H E A L T H C A R E Transitions of Care: The need for a more effective approach to continuing patient care The need for a more effective approach to continuing patient care This paper
Care Transitions. Provide Your Patients with Effective Transitional Care Without Changing Your Operating Model. Share This
 Care Transitions Provide Your Patients with Effective Transitional Care Without Changing Your Operating Model Brought to you by Amedisys: Architects of a leading patient-centered Care Transitions network.
Care Transitions Provide Your Patients with Effective Transitional Care Without Changing Your Operating Model Brought to you by Amedisys: Architects of a leading patient-centered Care Transitions network.
The CHCF Care Transition Projects Interim Progress Report and Meeting Summary
 C A LIFORNIA HEALTHCARE FOUNDATION The CHCF Care Transition Projects Interim Progress Report and Meeting Summary Prepared for California HealthCare Foundation by Susan Baird Kanaan, M.S.W. April 2008 About
C A LIFORNIA HEALTHCARE FOUNDATION The CHCF Care Transition Projects Interim Progress Report and Meeting Summary Prepared for California HealthCare Foundation by Susan Baird Kanaan, M.S.W. April 2008 About
MANITOWOC COUNTY CARE TRANSITION PROGRAM
 MANITOWOC COUNTY CARE TRANSITION PROGRAM A U G U S T 1 5, 2 0 1 3 Judy Rank Director Cathy Ley Supervisor Care Transitions Coach MANITOWOC COUNTY CARE TRANSITION PROGRAM Julie Place, Director of Nursing
MANITOWOC COUNTY CARE TRANSITION PROGRAM A U G U S T 1 5, 2 0 1 3 Judy Rank Director Cathy Ley Supervisor Care Transitions Coach MANITOWOC COUNTY CARE TRANSITION PROGRAM Julie Place, Director of Nursing
From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions
 From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions Cristiane L. Fukuda RN, MSN, ANP-BC Email: cristiane.fukuda@northside.com Office: 404-851-6914
From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions Cristiane L. Fukuda RN, MSN, ANP-BC Email: cristiane.fukuda@northside.com Office: 404-851-6914
Contact: Jessica Lorenzo, M.P.H., Senior Project Manager. E-mail: Jessica.Lorenzo@mountsinai.org
 Mount Sinai School of Medicine: Improving Access to High Quality Asthma Care in East Harlem Grant Results Report October 2008 BACKGROUND INFORMATION Mount Sinai School of Medicine Division of General Internal
Mount Sinai School of Medicine: Improving Access to High Quality Asthma Care in East Harlem Grant Results Report October 2008 BACKGROUND INFORMATION Mount Sinai School of Medicine Division of General Internal
Implementing an Evidence Based Hospital Discharge Process
 Implementing an Evidence Based Hospital Discharge Process Learning from the experience of Project Re-Engineered Discharge (RED) Webinar January 14, 2013 Chris Manasseh, MD Director, Boston HealthNet Inpatient
Implementing an Evidence Based Hospital Discharge Process Learning from the experience of Project Re-Engineered Discharge (RED) Webinar January 14, 2013 Chris Manasseh, MD Director, Boston HealthNet Inpatient
Care Transition Bundle Seven Essential Intervention Categories
 Seven 1. Medications Management Ensuring the safe use of medications by patients and their families and based on patients plans of care a. Assessment of patient s medications intake b. Patient and family
Seven 1. Medications Management Ensuring the safe use of medications by patients and their families and based on patients plans of care a. Assessment of patient s medications intake b. Patient and family
Preventing Avoidable Re-Hospitalizations: Where Do You Fit in the Quality Care Puzzle?
 Speaker Disclosures Care Transitions Interventions: The Sussex County Transitional Care Program Dr. Wang has disclosed that he has no relevant financial relationship(s). George C. Wang, MD, PhD Medical
Speaker Disclosures Care Transitions Interventions: The Sussex County Transitional Care Program Dr. Wang has disclosed that he has no relevant financial relationship(s). George C. Wang, MD, PhD Medical
Visiting Nurse Service of New York. New York State Department of Health Medicaid Incentive Payment System (MIPS) External Stakeholder Feedback
 New York State Department of Health Medicaid Incentive Payment System (MIPS) External Stakeholder Feedback Visiting Nurse Service of New York February 19, 2010 11:30 a.m. 12:30 p.m. New York State Department
New York State Department of Health Medicaid Incentive Payment System (MIPS) External Stakeholder Feedback Visiting Nurse Service of New York February 19, 2010 11:30 a.m. 12:30 p.m. New York State Department
Z Take this folder with you to your
 my health care notebook Why? Being an active part of your health care team helps you feel better and helps you get even better care. Starting on Day 1, you can keep track of important information and questions.
my health care notebook Why? Being an active part of your health care team helps you feel better and helps you get even better care. Starting on Day 1, you can keep track of important information and questions.
Care Transition Bundle Seven Essential Intervention Categories. Examples of Transition of Care Interventions
 1. Medications Management Ensuring the safe use of medications by patients and their families and based on patients plans of care a. Assessment of patient s medications intake b. Patient and family education
1. Medications Management Ensuring the safe use of medications by patients and their families and based on patients plans of care a. Assessment of patient s medications intake b. Patient and family education
Care Coordination and Transitions in Behavioral Health
 Care Coordination and Transitions in Behavioral Health Pam Pietruszewski Integrated Health Consultant The National Council for Behavioral Health This product is supported by the Florida Department of Children
Care Coordination and Transitions in Behavioral Health Pam Pietruszewski Integrated Health Consultant The National Council for Behavioral Health This product is supported by the Florida Department of Children
Discharge Planning. Home Care 1. Objectives. Where are they Going?
 Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Understanding Care Transitions as a Patient Safety Issue
 Article reprinted from Patient Safety & Quality Healthcare, May/June 2011 Understanding Care Transitions as a Patient Safety Issue By Sara Butterfield RN, BSN, CPHQ, CCM; Christine Stegel, RN, MS, CPHQ;
Article reprinted from Patient Safety & Quality Healthcare, May/June 2011 Understanding Care Transitions as a Patient Safety Issue By Sara Butterfield RN, BSN, CPHQ, CCM; Christine Stegel, RN, MS, CPHQ;
of the Nurse Practitioner
 The Emerging Role of the Nurse Practitioner Rhonda Hettinger DNP, NP C, CLS Introduction The American health care system is in need of a fundamental change (Institute t of Medicine, 2001). Nurse practitioner
The Emerging Role of the Nurse Practitioner Rhonda Hettinger DNP, NP C, CLS Introduction The American health care system is in need of a fundamental change (Institute t of Medicine, 2001). Nurse practitioner
Care Transitions: Evidence-based best practices for Case Managers
 Care Transitions: Evidence-based best practices for Case Managers Mary D. Naylor, PhD, FAAN, RN Marian S. Ware Professor in Gerontology Director, NewCourtlandCenter for Transitions & Health University
Care Transitions: Evidence-based best practices for Case Managers Mary D. Naylor, PhD, FAAN, RN Marian S. Ware Professor in Gerontology Director, NewCourtlandCenter for Transitions & Health University
Coaching Patients to Improve Care Transitions in Pennsylvania. May 26, 2010
 Coaching Patients to Improve Care Transitions in Pennsylvania Naomi Hauser, RN, MPA, CLNC Director Care Transitions Quality Insights of Pennsylvania Dr. Eric Coleman, MPH Professor of Medicine University
Coaching Patients to Improve Care Transitions in Pennsylvania Naomi Hauser, RN, MPA, CLNC Director Care Transitions Quality Insights of Pennsylvania Dr. Eric Coleman, MPH Professor of Medicine University
Health Care Leader Action Guide to Reduce Avoidable Readmissions
 Health Care Leader Action Guide to Reduce Avoidable Readmissions January 2010 TRANSFORMING HEALTH CARE THROUGH RESEARCH AND EDUCATION Osei-Anto A, Joshi M, Audet AM, Berman A, Jencks S. Health Care Leader
Health Care Leader Action Guide to Reduce Avoidable Readmissions January 2010 TRANSFORMING HEALTH CARE THROUGH RESEARCH AND EDUCATION Osei-Anto A, Joshi M, Audet AM, Berman A, Jencks S. Health Care Leader
A I S. San Diego s ADRC CARE TRANSITIONS INTERVENTION (CTI) 9/19/2011
 CARE TRANSITIONS INTERVENTION (CTI) Brenda Schmitthenner, MPA Aging Program Administrator (858) 495 5853 brenda.schmitthenner@sdcounty.ca.gov A I S RSVP Veterans Health Promotion Info & Assistance Outreach
CARE TRANSITIONS INTERVENTION (CTI) Brenda Schmitthenner, MPA Aging Program Administrator (858) 495 5853 brenda.schmitthenner@sdcounty.ca.gov A I S RSVP Veterans Health Promotion Info & Assistance Outreach
How Health Reform Will Affect Health Care Quality and the Delivery of Services
 Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
The Care Transitions Intervention: Geriatric Care. During an episode of illness, older patients may receive care in multiple settings; often resulting
 The Care Transitions Intervention: A Patient-Centered Approach to Ensuring Effective Transfers Between Sites of Geriatric Care Abstract During an episode of illness, older patients may receive care in
The Care Transitions Intervention: A Patient-Centered Approach to Ensuring Effective Transfers Between Sites of Geriatric Care Abstract During an episode of illness, older patients may receive care in
How To Help A Nursing Home And Hospital Collaborate
 Continuum of Care Bridging the Gap between the Hospital and Nursing Home Scott Wells, RN MSN Tiffany Noller, RN MSN Objectives Name key members involved in hospital/nursing home collaborative Identify
Continuum of Care Bridging the Gap between the Hospital and Nursing Home Scott Wells, RN MSN Tiffany Noller, RN MSN Objectives Name key members involved in hospital/nursing home collaborative Identify
Sutter Health, based in Sacramento, California and
 FACES of HOME HEALTH Caring for Frail Elderly Patients in the Home Sutter Health, based in Sacramento, California and serving Northern California, partners with its home care affiliate Sutter Care at Home,
FACES of HOME HEALTH Caring for Frail Elderly Patients in the Home Sutter Health, based in Sacramento, California and serving Northern California, partners with its home care affiliate Sutter Care at Home,
October 15, 2010. Re: National Health Care Quality Strategy and Plan. Dear Dr. Wilson,
 October 15, 2010 Dr. Nancy Wilson, R.N., M.D., M.P.H. Senior Advisor to the Director Agency for Healthcare Research and Quality (AHRQ) 540 Gaither Road Room 3216 Rockville, MD 20850 Re: National Health
October 15, 2010 Dr. Nancy Wilson, R.N., M.D., M.P.H. Senior Advisor to the Director Agency for Healthcare Research and Quality (AHRQ) 540 Gaither Road Room 3216 Rockville, MD 20850 Re: National Health
FROM DATA TO KNOWLEDGE: INTEGRATING ELECTRONIC HEALTH RECORDS MEANINGFULLY INTO OUR NURSING PRACTICE
 FROM DATA TO KNOWLEDGE: INTEGRATING ELECTRONIC HEALTH RECORDS MEANINGFULLY INTO OUR NURSING PRACTICE Rayne Soriano MS, RN Manager of Nursing Informatics and Clinical Transformation Program Kaiser Permanente
FROM DATA TO KNOWLEDGE: INTEGRATING ELECTRONIC HEALTH RECORDS MEANINGFULLY INTO OUR NURSING PRACTICE Rayne Soriano MS, RN Manager of Nursing Informatics and Clinical Transformation Program Kaiser Permanente
Eddy VNA Care Transitions Program
 Eddy VNA Care Transitions Program Patrick Archambeault RN, MS, CRNI Director of Clinical Specialties About Eddy VNA Large not for profit home care agency based in upstate New York CHHA, LTHHCP, Licensed
Eddy VNA Care Transitions Program Patrick Archambeault RN, MS, CRNI Director of Clinical Specialties About Eddy VNA Large not for profit home care agency based in upstate New York CHHA, LTHHCP, Licensed
Understanding and Improving Medication Reconciliation Between Hospitals and Nursing Homes
 Understanding and Improving Medication Reconciliation Between Hospitals and Nursing Homes Patient Safety Risk and Cost in Care Transitions White Paper November 2014 Stratis Health, based in Bloomington,
Understanding and Improving Medication Reconciliation Between Hospitals and Nursing Homes Patient Safety Risk and Cost in Care Transitions White Paper November 2014 Stratis Health, based in Bloomington,
DRIVING VALUE IN HEALTHCARE: PERSPECTIVES FROM TWO ACO EXECUTIVES, PART I
 DRIVING VALUE IN HEALTHCARE: PERSPECTIVES FROM TWO ACO EXECUTIVES, PART I A firm understanding of the key components and drivers of healthcare reform is increasingly important within the pharmaceutical,
DRIVING VALUE IN HEALTHCARE: PERSPECTIVES FROM TWO ACO EXECUTIVES, PART I A firm understanding of the key components and drivers of healthcare reform is increasingly important within the pharmaceutical,
ENHANCED TRANSITIONAL CARE MODEL:
 ENHANCED TRANSITIONAL CARE MODEL: A HOSPITAL TO HOME 30 DAY PILOT PROGRAM BROUGHT TO YOU BY INTRODUCTION One in five Medicare recipients discharged from the hospital today is reportedly readmitted within
ENHANCED TRANSITIONAL CARE MODEL: A HOSPITAL TO HOME 30 DAY PILOT PROGRAM BROUGHT TO YOU BY INTRODUCTION One in five Medicare recipients discharged from the hospital today is reportedly readmitted within
Six Communication Best Practices for Transitional Care Management
 WHITE PAPER Six Communication Best Practices for Transitional Care Management In the era of chronic illness and historically long lifespans, patient care transitions to home or another facility have become
WHITE PAPER Six Communication Best Practices for Transitional Care Management In the era of chronic illness and historically long lifespans, patient care transitions to home or another facility have become
Transitions of Care: The need for collaboration across entire care continuum
 H O T T O P I C S I N H E A L T H C A R E, I S S U E # 2 Transitions of Care: The need for collaboration across entire care continuum Safe, quality Transitions Effective C o l l a b o r a t i v e S u c
H O T T O P I C S I N H E A L T H C A R E, I S S U E # 2 Transitions of Care: The need for collaboration across entire care continuum Safe, quality Transitions Effective C o l l a b o r a t i v e S u c
Rehabilitation Where You Recover. Inpatient Rehabilitation Services at Albany Medical Center
 Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
RED, BOOST, and You: Improving the Discharge Transition of Care
 RED, BOOST, and You: Improving the Discharge Transition of Care Jeffrey L. Greenwald, MD, SFHM Massachusetts General Hospital - Clinician Educator Service Co-Investigator Project RED & Project BOOST The
RED, BOOST, and You: Improving the Discharge Transition of Care Jeffrey L. Greenwald, MD, SFHM Massachusetts General Hospital - Clinician Educator Service Co-Investigator Project RED & Project BOOST The
Transitional Care: Bridging the Gaps of a Fragmented Health System
 Transitional Care: Bridging the Gaps of a Fragmented Health System Amy J H Kind, MD, PhD Assistant Professor, Division of Geriatrics University of Wisconsin School of Medicine and Public Health Madison
Transitional Care: Bridging the Gaps of a Fragmented Health System Amy J H Kind, MD, PhD Assistant Professor, Division of Geriatrics University of Wisconsin School of Medicine and Public Health Madison
GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services
 GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services Aged, Blind and Disabled Stakeholder Presentation Indiana Family and Social Services Administration August
GRACE Team Care Integration of Primary Care with Geriatrics and Community-Based Social Services Aged, Blind and Disabled Stakeholder Presentation Indiana Family and Social Services Administration August
Ann Hablitzel, RN, BSN, MBA Hospice Care of California
 Ann Hablitzel, RN, BSN, MBA Hospice Care of California Objectives Describe the creations of new community based palliative care programs Identify criteria for admission Discuss philosophy and goals Analyze
Ann Hablitzel, RN, BSN, MBA Hospice Care of California Objectives Describe the creations of new community based palliative care programs Identify criteria for admission Discuss philosophy and goals Analyze
5/10/13 HEALTH CARE REFORM LONGITUDINAL CARE COORDINATION HEALTH CARE REFORM WHY = VALUE WHY WHAT HOW WHEN WHO WHY WHAT HOW WHEN WHO
 TRANSITION CARE TRANSITION CARE WHY WHAT HOW WHEN WHO HEALTH CARE REFORM HEALTH CARE REFORM WHY = VALUE WHY WHAT HOW WHEN WHO Cost/Quality equation Higher cost care has not/does not equate with higher
TRANSITION CARE TRANSITION CARE WHY WHAT HOW WHEN WHO HEALTH CARE REFORM HEALTH CARE REFORM WHY = VALUE WHY WHAT HOW WHEN WHO Cost/Quality equation Higher cost care has not/does not equate with higher
Care Management of Patients with Complex Health Care Needs
 Care Management of Patients with Complex Health Care Needs Thomas Bodenheimer, MD Rachel Berry-Millett, BA Center for Excellence in Primary Care Department of Family and Community Medicine University of
Care Management of Patients with Complex Health Care Needs Thomas Bodenheimer, MD Rachel Berry-Millett, BA Center for Excellence in Primary Care Department of Family and Community Medicine University of
Engaging Effective Post Acute Partners in New Models of Care. A Transitional Care Model
 Engaging Effective Post Acute Partners in New Models of Care A Transitional Care Model Please note that the views expressed by the conference speakers do not necessarily reflect the views of the American
Engaging Effective Post Acute Partners in New Models of Care A Transitional Care Model Please note that the views expressed by the conference speakers do not necessarily reflect the views of the American
Colorado Small Business Enrollment Guide A BETTER WAY to take care of business
 2015 SMALL BUSINESS HEALTH Colorado Small Business Enrollment Guide A BETTER WAY to take care of business Choose BETTER. 31 Important deadline Open enrollment begins on November 15, 2014 for coverage beginning
2015 SMALL BUSINESS HEALTH Colorado Small Business Enrollment Guide A BETTER WAY to take care of business Choose BETTER. 31 Important deadline Open enrollment begins on November 15, 2014 for coverage beginning
IDENTIFYING INFORMATION MANAGEMENT CHALLENGES FACED BY HOME HEALTHCARE PROFESSIONALS MANAGING OLDER ADULTS TRANSITIONS FROM HOSPITAL TO HOME CARE
 IDENTIFYING INFORMATION MANAGEMENT CHALLENGES FACED BY HOME HEALTHCARE PROFESSIONALS MANAGING OLDER ADULTS TRANSITIONS FROM HOSPITAL TO HOME CARE Alicia Arbaje, M.D., M.P.H. Assistant Professor of Medicine,
IDENTIFYING INFORMATION MANAGEMENT CHALLENGES FACED BY HOME HEALTHCARE PROFESSIONALS MANAGING OLDER ADULTS TRANSITIONS FROM HOSPITAL TO HOME CARE Alicia Arbaje, M.D., M.P.H. Assistant Professor of Medicine,
EMR: Putting Flexibility Up Front
 EMR: Putting Flexibility Up Front By Jeanne-Marie Phillips Orthopedists implement innovative electronic medical records system that adapts to their business needs. I wanted an EMR program that would reflect
EMR: Putting Flexibility Up Front By Jeanne-Marie Phillips Orthopedists implement innovative electronic medical records system that adapts to their business needs. I wanted an EMR program that would reflect
Managing Care Transitions in Medicaid: Spotlight on Community Care of North Carolina
 Managing Care Transitions in Medicaid: Spotlight on Community Care of North Carolina EXECUTIVE SUMMARY This second of three case studies examining key operational aspects of coordinated care initiatives
Managing Care Transitions in Medicaid: Spotlight on Community Care of North Carolina EXECUTIVE SUMMARY This second of three case studies examining key operational aspects of coordinated care initiatives
Following Up with Patients Discharged from the Emergency Department: A Look at Voice and UCSF
 Following Up with Patients Discharged from the Emergency Department: A Look at Voice and UCSF page 1 Introduction The transition from hospital to home is a sensitive time period for patients and care providers.
Following Up with Patients Discharged from the Emergency Department: A Look at Voice and UCSF page 1 Introduction The transition from hospital to home is a sensitive time period for patients and care providers.
As the prevalence of serious illness among the. Innovative models of home-based palliative care TECHNOLOGY INNOVATIONS AND PALLIATIVE CARE
 TECHNOLOGY INNOVATIONS AND PALLIATIVE CARE MARGHERITA C. LABSON, RN, MSHSA, CPHQ, CCM Executive Director, Home Care Program, The Joint Commission, Oak Brook Terrace, IL BETSY GORNET, FACHE Chief AIM and
TECHNOLOGY INNOVATIONS AND PALLIATIVE CARE MARGHERITA C. LABSON, RN, MSHSA, CPHQ, CCM Executive Director, Home Care Program, The Joint Commission, Oak Brook Terrace, IL BETSY GORNET, FACHE Chief AIM and
Care Management: Reducing Risks. Project ECHO Consultation. Amy J. Khan, MD, MPH. Mia McCallum-Crawford, RN
 Care Management: Improving Health & Reducing Risks Project ECHO Consultation February 19, 2015 Amy J. Khan, MD, MPH Lisa Moreno, RN Mia McCallum-Crawford, RN Objectives 1. Consider patient factors and
Care Management: Improving Health & Reducing Risks Project ECHO Consultation February 19, 2015 Amy J. Khan, MD, MPH Lisa Moreno, RN Mia McCallum-Crawford, RN Objectives 1. Consider patient factors and
Kaiser Permanente Southern California Depression Care Program
 Kaiser Permanente Southern California Depression Care Program Abstract In 2001, Kaiser Permanente of Southern California (KPSC) adopted the IMPACT model of collaborative care for depression, developed
Kaiser Permanente Southern California Depression Care Program Abstract In 2001, Kaiser Permanente of Southern California (KPSC) adopted the IMPACT model of collaborative care for depression, developed
Unforeseen Benefits: Addiction Treatment Reduces Health Care Costs CLOSING THE ADDICTION TREATMENT GAP
 Unforeseen Benefits: Addiction Treatment Reduces Health Care Costs CLOSING THE ADDICTION TREATMENT GAP Executive Summary Improving America s health care system, creating a healthier country, and containing
Unforeseen Benefits: Addiction Treatment Reduces Health Care Costs CLOSING THE ADDICTION TREATMENT GAP Executive Summary Improving America s health care system, creating a healthier country, and containing
Irene Fleshner, RN, MHSA, FACHE SVP, Strategic Nursing Initiatives Genesis HealthCare Principal, Reno, Davis and Associates, Inc.
 Irene Fleshner, RN, MHSA, FACHE SVP, Strategic Nursing Initiatives Genesis HealthCare Principal, Reno, Davis and Associates, Inc. Independent Living Continuing Care Retirement Community Home Care Assisted
Irene Fleshner, RN, MHSA, FACHE SVP, Strategic Nursing Initiatives Genesis HealthCare Principal, Reno, Davis and Associates, Inc. Independent Living Continuing Care Retirement Community Home Care Assisted
Accountable Care Organizations and Patient-Centered Medical Homes
 Emerging Topics in Healthcare Reform Accountable Care Organizations and Patient-Centered Medical Homes Janssen Pharmaceuticals, Inc. Accountable Care Organizations and Patient-Centered Medical Homes The
Emerging Topics in Healthcare Reform Accountable Care Organizations and Patient-Centered Medical Homes Janssen Pharmaceuticals, Inc. Accountable Care Organizations and Patient-Centered Medical Homes The
7/25/2015. Disclosure(s) Prescription for the Future: Pharmacists Influencing Positive Health Outcomes. Clinical Practice.
 49th Annual Meeting Prescription for the Future: Pharmacists Influencing Positive Health Outcomes Daniel E. Buffington, PharmD, MBA, FAPhA Clinical Pharmacology Services, Inc Tampa, FL Disclosure(s) Daniel
49th Annual Meeting Prescription for the Future: Pharmacists Influencing Positive Health Outcomes Daniel E. Buffington, PharmD, MBA, FAPhA Clinical Pharmacology Services, Inc Tampa, FL Disclosure(s) Daniel
PIPC: Hepatitis Roundtable Summary and Recommendations on Dissemination and Implementation of Clinical Evidence
 PIPC: Hepatitis Roundtable Summary and Recommendations on Dissemination and Implementation of Clinical Evidence On May 8, 2014, the Partnership to Improve Patient Care (PIPC) convened a Roundtable of experts
PIPC: Hepatitis Roundtable Summary and Recommendations on Dissemination and Implementation of Clinical Evidence On May 8, 2014, the Partnership to Improve Patient Care (PIPC) convened a Roundtable of experts
Community Health Needs Assessment Implementation Plan FY 14-16
 Community Health Needs Assessment Implementation Plan FY 14-16 South Miami Hospital conducted a community health needs assessment in 2013 to better understand the healthcare needs of the community it serves
Community Health Needs Assessment Implementation Plan FY 14-16 South Miami Hospital conducted a community health needs assessment in 2013 to better understand the healthcare needs of the community it serves
Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010
 Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010 As the Illinois Legislature prepares to act on the future of Medicaid, it is important
Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010 As the Illinois Legislature prepares to act on the future of Medicaid, it is important
RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home
 RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home Sergio Petrillo, PharmD Clinical Pharmacist Specialist, Rhode Island Hospital
RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home Sergio Petrillo, PharmD Clinical Pharmacist Specialist, Rhode Island Hospital
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment
 Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Transitions of Care Management Coding (TCM Code) Tutorial. 1. Introduction Meaning of moderately and high complexity 2
 Transitions of Care Management Coding (TCM Code) Tutorial Index 1. Introduction Meaning of moderately and high complexity 2 2. SETMA s Tools for using TCM Code 3 Alert that patient is eligible for TCM
Transitions of Care Management Coding (TCM Code) Tutorial Index 1. Introduction Meaning of moderately and high complexity 2 2. SETMA s Tools for using TCM Code 3 Alert that patient is eligible for TCM
Providing and Billing Medicare for Transitional Care Management
 PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
HealthPartners: Triple Aim Approach to ACO Development
 HealthPartners: Triple Aim Approach to ACO Development Brian Rank, MD Medical Director, HealthPartners Medical Group October 27, 2010 HealthPartners Integrated Care and Financing System 10,300 employees
HealthPartners: Triple Aim Approach to ACO Development Brian Rank, MD Medical Director, HealthPartners Medical Group October 27, 2010 HealthPartners Integrated Care and Financing System 10,300 employees
Johns Hopkins HealthCare LLC: Care Management and Care Coordination for Chronic Diseases
 Johns Hopkins HealthCare LLC: Care Management and Care Coordination for Chronic Diseases Epidemiology Over 145 million people ( nearly half the population) - suffer from asthma, depression and other chronic
Johns Hopkins HealthCare LLC: Care Management and Care Coordination for Chronic Diseases Epidemiology Over 145 million people ( nearly half the population) - suffer from asthma, depression and other chronic
AMERICAN MEDICAL DIRECTORS ASSOCIATION WHITE PAPER RESOLUTION C09
 AMERICAN MEDICAL DIRECTORS ASSOCIATION WHITE PAPER RESOLUTION C09 SUBJECT: IMPROVING CARE TRANSITIONS FROM THE NURSING FACILITY TO A COMMUNITY-BASED SETTING INTRODUCED BY: AMDA PUBLIC POLICY COMMITTEE
AMERICAN MEDICAL DIRECTORS ASSOCIATION WHITE PAPER RESOLUTION C09 SUBJECT: IMPROVING CARE TRANSITIONS FROM THE NURSING FACILITY TO A COMMUNITY-BASED SETTING INTRODUCED BY: AMDA PUBLIC POLICY COMMITTEE
Transitional Care Codes New Codes, New Requirements
 Transitional Care Codes New Codes, New Requirements Karen W. Foster, MSA, RN Project Facilitator New Jersey Academy of Family Physicians 2014. NJAFP This presentation and content shared during this session
Transitional Care Codes New Codes, New Requirements Karen W. Foster, MSA, RN Project Facilitator New Jersey Academy of Family Physicians 2014. NJAFP This presentation and content shared during this session
Hitting a Home Run: The Patient Centered Medical Home and Home Care
 Hitting a Home Run: The Patient Centered Medical Home and Home Care This paper has been prepared by the Home Care Alliance of Massachusetts to support home health agencies seeking to align with community
Hitting a Home Run: The Patient Centered Medical Home and Home Care This paper has been prepared by the Home Care Alliance of Massachusetts to support home health agencies seeking to align with community
Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions
 Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions Leslie Becker RN, BS Jennifer Smith RN, MSN, MBA Leslie Frain MSN, RN Jan Machanis
Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions Leslie Becker RN, BS Jennifer Smith RN, MSN, MBA Leslie Frain MSN, RN Jan Machanis
Value-Based Purchasing
 Emerging Topics in Healthcare Reform Value-Based Purchasing Janssen Pharmaceuticals, Inc. Value-Based Purchasing The Patient Protection and Affordable Care Act (ACA) established the Hospital Value-Based
Emerging Topics in Healthcare Reform Value-Based Purchasing Janssen Pharmaceuticals, Inc. Value-Based Purchasing The Patient Protection and Affordable Care Act (ACA) established the Hospital Value-Based
Care Coordination: Case managers connect the dots in new delivery models
 The Pathway to Certfication is CCMC IssueBrief VOLUME 1, ISSUE 2 Care Coordination: Case managers connect the dots in new delivery models Well before health reform was signed into law, new models for health
The Pathway to Certfication is CCMC IssueBrief VOLUME 1, ISSUE 2 Care Coordination: Case managers connect the dots in new delivery models Well before health reform was signed into law, new models for health
The Real Skinny on Medicare Billing Through an Accredited Diabetes Self- Management Program
 The Real Skinny on Medicare Billing Through an Accredited Diabetes Self- Management Program 1 Dallas Area Agency on Aging The Dallas Area Agency on Aging (DAAA) is the department under the umbrella of
The Real Skinny on Medicare Billing Through an Accredited Diabetes Self- Management Program 1 Dallas Area Agency on Aging The Dallas Area Agency on Aging (DAAA) is the department under the umbrella of
Community Care of North Carolina
 Community Care of North Carolina CCNC Transitional Care Management Jennifer Cockerham, RN, BSN, CDE Director, Chronic Care Programs & Quality Management 1 Chronic Care Population Within the NC Medicaid
Community Care of North Carolina CCNC Transitional Care Management Jennifer Cockerham, RN, BSN, CDE Director, Chronic Care Programs & Quality Management 1 Chronic Care Population Within the NC Medicaid
Care Management Plus Model
 Supported by the john A. Hartford foundation Care Management Plus Model In primary care clinics, Care Management Plus provides information technology systems to facilitate the work of a care manager and
Supported by the john A. Hartford foundation Care Management Plus Model In primary care clinics, Care Management Plus provides information technology systems to facilitate the work of a care manager and
From Hospital to Home:
 From Hospital to Home: For patients and providers, recovery at home means improved outcomes and reduced costs HOSPITAL TO HOME BY THE NUMBERS From July to December 2014, VNA Healthtrends enrolled 51 patients
From Hospital to Home: For patients and providers, recovery at home means improved outcomes and reduced costs HOSPITAL TO HOME BY THE NUMBERS From July to December 2014, VNA Healthtrends enrolled 51 patients
Post-Acute Care Transitions: An Essential Component of Accountable Care
 : An Essential Component of Accountable Care Bruce C. Smith, MD, FACP Associate Medical Director, Strategy Deployment Group Health Physicians, Seattle, WA Smith.bc@ghc.org AMGA 2012 Institute for Quality
: An Essential Component of Accountable Care Bruce C. Smith, MD, FACP Associate Medical Director, Strategy Deployment Group Health Physicians, Seattle, WA Smith.bc@ghc.org AMGA 2012 Institute for Quality
Virtual Integrated Practice Model
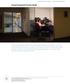 Supported by the john A. Hartford foundation Virtual Integrated Practice Model Virtual Integrated Practice (VIP) team care meeting at Rush Medical Center, Chicago, IL. In an early morning meeting via teleconference,
Supported by the john A. Hartford foundation Virtual Integrated Practice Model Virtual Integrated Practice (VIP) team care meeting at Rush Medical Center, Chicago, IL. In an early morning meeting via teleconference,
Clinical Nurse Specialists Practitioners Contributing to Primary Care: A Briefing Paper
 Clinical Nurse Specialists Practitioners Contributing to Primary Care: A Briefing Paper As the need grows for more practitioners of primary care, it is important to recognize the Clinical Nurse Specialist
Clinical Nurse Specialists Practitioners Contributing to Primary Care: A Briefing Paper As the need grows for more practitioners of primary care, it is important to recognize the Clinical Nurse Specialist
Admission to Inpatient Rehabilitation (Rehab) Services
 Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
EMR: Putting Flexibility Up Front
 EMR: Putting Flexibility Up Front By Jeanne-Marie Phillips Orthopedists implement innovative electronic medical records system that adapts to their business needs. I wanted an EMR program that would reflect
EMR: Putting Flexibility Up Front By Jeanne-Marie Phillips Orthopedists implement innovative electronic medical records system that adapts to their business needs. I wanted an EMR program that would reflect
PART I : NAVIGATING HEALTH CARE
 PART I : NAVIGATING HEALTH CARE SECTION ONE Hospitals, Clinical Trials & Ambulance Service 1. Should my dad just sign all those hospital consent forms or actually question them? 2. What is a hospital Patient
PART I : NAVIGATING HEALTH CARE SECTION ONE Hospitals, Clinical Trials & Ambulance Service 1. Should my dad just sign all those hospital consent forms or actually question them? 2. What is a hospital Patient
What is Geriatric Care Management?
 What is Geriatric Care Management? Printed in USA Arcadia Home Care & Staffing www.arcadiahomecare.com What is Geriatric Care Management and Why is it Important? As a health care service, geriatric care
What is Geriatric Care Management? Printed in USA Arcadia Home Care & Staffing www.arcadiahomecare.com What is Geriatric Care Management and Why is it Important? As a health care service, geriatric care
The London Primary Care Diabetes Support Program:
 The London Primary Care Diabetes Support Program: Diabetes Care with a Difference SUCC ESS STO R Y 1 A patient s first appointment here includes an intake assessment of the broader determinants of health
The London Primary Care Diabetes Support Program: Diabetes Care with a Difference SUCC ESS STO R Y 1 A patient s first appointment here includes an intake assessment of the broader determinants of health
Challenging Chronic Disease Through Telehealth
 CMMI Innovation Advisor Erin Denholm, Centura Health at Home: Challenging Chronic Disease Through Telehealth Erin Denholm, of Centura Health at Home, joins the Alliance for a discussion of her work with
CMMI Innovation Advisor Erin Denholm, Centura Health at Home: Challenging Chronic Disease Through Telehealth Erin Denholm, of Centura Health at Home, joins the Alliance for a discussion of her work with
2007 James A Vohs Award for Quality First-Place Selection A Multidisciplinary Approach to Transition Care: A Patient Safety Innovation Study
 available online: www.kp.org/permanentejournal Original article 2007 James A Vohs Award for Quality First-Place Selection A Multidisciplinary Approach to Transition Care: A Patient Safety Innovation Study
available online: www.kp.org/permanentejournal Original article 2007 James A Vohs Award for Quality First-Place Selection A Multidisciplinary Approach to Transition Care: A Patient Safety Innovation Study
Depression Support Resources: Telephonic/Care Management Follow-up
 Depression Support Resources: Telephonic/Care Management Follow-up Depression Support Resources: Telephonic/Care Management Follow-up Primary Care Toolkit September 2015 Page 29 Role of the Phone Clinician
Depression Support Resources: Telephonic/Care Management Follow-up Depression Support Resources: Telephonic/Care Management Follow-up Primary Care Toolkit September 2015 Page 29 Role of the Phone Clinician
Northern Colorado Companies. The Power of Innovative Integration
 Northern Colorado Companies The Power of Innovative Integration July 22, 2014 Agenda Introductions and Expectations Overview of Kaiser Permanente Northern Colorado Network Overview Integrated Medical Delivery
Northern Colorado Companies The Power of Innovative Integration July 22, 2014 Agenda Introductions and Expectations Overview of Kaiser Permanente Northern Colorado Network Overview Integrated Medical Delivery
Having Surgery? What you need to know. Questions to ask your doctor and your surgeon
 Having Surgery? What you need to know Questions to ask your doctor and your surgeon Agency for Healthcare Research and Quality Advancing Excellence in Health Care www.ahrq.gov This booklet was developed
Having Surgery? What you need to know Questions to ask your doctor and your surgeon Agency for Healthcare Research and Quality Advancing Excellence in Health Care www.ahrq.gov This booklet was developed
Congestive Heart Failure Management Program
 Congestive Heart Failure Management Program The Congestive Heart Failure Program is the third statewide disease management program developed by CCNC. The clinical directors reviewed prevalence and outcome
Congestive Heart Failure Management Program The Congestive Heart Failure Program is the third statewide disease management program developed by CCNC. The clinical directors reviewed prevalence and outcome
Designing the Role of the Embedded Care Manager
 Designing the Role of the Embedded By Patricia Hines, Ph.D., RN and Marge Mercury, RN, MS, CMCE The Embedded The use of an Embedded ( ECM ) to coordinate within the complex delivery system is sharply increasing.
Designing the Role of the Embedded By Patricia Hines, Ph.D., RN and Marge Mercury, RN, MS, CMCE The Embedded The use of an Embedded ( ECM ) to coordinate within the complex delivery system is sharply increasing.
WHAT IS MEDICAL MANAGEMENT? WHAT IS THE PURPOSE OF MEDICAL MANAGEMENT?
 WHAT IS MEDICAL MANAGEMENT? How health plans make decisions to approve payment for medical treatment is a poorly understood part of the healthcare system. One part of the process, known as medical management,
WHAT IS MEDICAL MANAGEMENT? How health plans make decisions to approve payment for medical treatment is a poorly understood part of the healthcare system. One part of the process, known as medical management,
DECISION QUALITY WORKSHEET TREATMENTS FOR SPINAL STENOSIS
 DECISION QUALITY WORKSHEET TREATMENTS FOR SPINAL STENOSIS Instructions This survey has questions about what it is like for you to make decisions about treating your spinal stenosis. Please check the box
DECISION QUALITY WORKSHEET TREATMENTS FOR SPINAL STENOSIS Instructions This survey has questions about what it is like for you to make decisions about treating your spinal stenosis. Please check the box
Regulatory and Legislative Action Since the September 2010 Membership Meeting:
 MEMBERSHIP MEETING January 19, 2011 Delivery System Reform: Healthcare Workforce Issue: The passage of health reform will bring millions of newly insured individuals into the system and drive patients
MEMBERSHIP MEETING January 19, 2011 Delivery System Reform: Healthcare Workforce Issue: The passage of health reform will bring millions of newly insured individuals into the system and drive patients
Understanding Prescription Assistance Programs (PAPs)
 Understanding Prescription Assistance Programs (PAPs) The use of prescription medicines has become an increasingly important part of quality medical care. Two out of every three visits to the doctor end
Understanding Prescription Assistance Programs (PAPs) The use of prescription medicines has become an increasingly important part of quality medical care. Two out of every three visits to the doctor end
Breathe Easier: Using Clinical Education and Redesign Techniques to Improve Pediatric Asthma Care
 Breathe Easier: Using Clinical Education and Redesign Techniques to Improve Pediatric Asthma Care Lalit Bajaj,, MD, MPH The Children s s Hospital, Denver Hoke Stapp,, MD, FAAP Colorado Pediatric Partners,
Breathe Easier: Using Clinical Education and Redesign Techniques to Improve Pediatric Asthma Care Lalit Bajaj,, MD, MPH The Children s s Hospital, Denver Hoke Stapp,, MD, FAAP Colorado Pediatric Partners,
An Integrated, Holistic Approach to Care Management Blue Care Connection
 An Integrated, Holistic Approach to Care Management Blue Care Connection With health care costs continuing to rise, both employers and health plans need innovative solutions to help employees manage their
An Integrated, Holistic Approach to Care Management Blue Care Connection With health care costs continuing to rise, both employers and health plans need innovative solutions to help employees manage their
At the Intersection of Care Transitions, Care Plan Goal Development, and Consistency of Outcomes Documentation
 At the Intersection of Care Transitions, Care Plan Goal Development, and Consistency of Outcomes Documentation Lorraine Cummings, quality improvement specialist, UCare Kathleen Albrecht, manager of regulatory
At the Intersection of Care Transitions, Care Plan Goal Development, and Consistency of Outcomes Documentation Lorraine Cummings, quality improvement specialist, UCare Kathleen Albrecht, manager of regulatory
