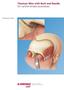
Zimmer M/L Taper Hip Prosthesis with Modular Neck Kinectiv Technology March 12, :00 PM EDT
|
|
|
- Osborne Powell
- 10 years ago
- Views:
Transcription
1 Zimmer M/L Taper Hip Prosthesis with Modular Neck Kinectiv Technology March 12, :00 PM EDT Welcome to this "OR Live" Webcast presentation brought to you by Zimmer. During the program, it s easy for you to learn more about the procedure. Just click on the Request Information button on your Webcast screen and open the door to informed medical care. "OR Live", the vision of improving health. Good morning. Welcome to Northwest Medical Center here in Tucson, Arizona. My name is Dr. Audrey Tsao from Sun Valley Orthopaedics in Phoenix, Arizona. We're here with Dr. John Maltry in his operating room doing an "OR Live" Webcast on the Kinectiv Total Hip System. At this time, let s join Dr. Maltry in the operating room. Hello, everybody. My name is Dr. John Maltry with the Tucson Orthopaedic Institute. Today we have Dr. Brian Lenius doing anesthesia for us. Here s Kim McNurlin will be our PA assisting, Mr. Denton McGeshey as a second assist, Christina Marble handling instruments, Dave Elling on bass fiddle, I guess. And we'll get started here. The procedure today is going to be the minimally invasive anterial lateral approach to the right hip in this gentleman. We're going to be installing the Zimmer Kinectiv Hip System today and we'll walk you through that. If we have questions throughout the procedure, please feel free to send those to Dr. Tao and we'll get those answered or you as we proceed. Patient s in the lateral position. We've already marked out the boundary of the greater choke header and the anterior superior at the spine of the right hip. And at this point we'll begin. All right, the incision starts from the superior anterior portion of the greater trochanter and carried to a point approximately one or two centimeters behind the ASIS, for a distance of about 8 to 10 centimeters. There you go, spongee. We'll simply carry that down through the skin and subcutaneous here. We're going to go down to the level of the tensor. We've already made a little perforation in the tensor but it s clearly visible. We'll incise in line with the wound and in line with the fibers of the tensor, being careful just to go through the fascia and not injuring the gluteus medius beneath it. We'll simply undermine underneath the anterior flap, reach around the anterior board of the medius and underneath it, put a retractor over the femoral neck at this level. See if I can -- this a little better. Now John, you're doing this all bluntly with basically digital palpation? Exactly true and I simply have got my thumb on the femoral neck here. Going to put one retractor just posterior to the neck. But we'll put another anteriorly. And here with a few interposed fibers of the minimus here, we're up on the capsule of the femoral neck here. In the inferior posterior aspect of the wound I can palpate though the capsule, the greater trochanter. And I'll begin my incision though the capsule at the tip of the trochanter and I'm going to ultimately make an H shaped incision in the capsule. I can be pretty aggressive with this because immediately underneath me is simply the femoral neck. And I'll carry that superiorly here until I am physically stopped by the mouth of the acetabulum. Is there any we could get a little bit of more in shot right directly above the capsular incision? I'll make this and then I'll stop and let you all have a look. 1
2 Okay. And if -- So John, this is a intermuscular plane but not an internervous plane, is that correct? That's correct. We he the plane between the gluteus medius posteriorly and the tensor anterioraly. And often when we develop this interval -- not today, we're not seeing -- there are fine connecting fibers of the superior luteal nerve here. And you just saw the light twitch as we stimulated one of those fibers. What I'm going to do now is -- Deb you can lift a little -- we'll take a little pressure off of the abductors. And I'm just going to take my same retractors and slide those interarticularly. So now you're inserting this interarticularly on the bone, itself, inside the capsular incision? Indeed, and I'll release this capsule here a little more. Do you ever have any problems with any type of weakness, post-operatively, with those little nervous fibers that you might be getting at the superior portion of your incision? We don't seem to. I suspect there s multiple fibers. And as long as we don't carry the incision too far superiorly up on to the lateral wall of the ileum, we don't seem to get into those fibers really much at all. We'll reposition you a little, Kim. That's better, all right. Here we can actually see the femoral head, its cartilaginous articulating surface. And in the superior aspect of the wound, this is the rim of the acetabulum. What we're going to do now is attempt to transect the femoral head directly in line with the acetabulum. And I try not to make that cut completely through because we certainly don't want to injure the acetabulum underneath. And your retractors are protecting your acetabulum? Right. They're around, both posteriorly and anteriorly around the acetabulum, but inferiorly either articularly in theory I could plunge that saw through and do some damage to my acetabulum. So be gentle. So we try just to get that about, oh, perhaps 2/3 to a little more of the way through and then I'll insert a -- this is cob elevator -- into that wound and complete this so we can get that neck to start elevating to indicate that we have indeed completed our osteotomy and can begin to displace that osteotomy. I see. Let s remove these retractors. What we're going to do now is externally rotate the leg and see if we can adduct it a bit and displace this osteotomy. It didn t move. Sometimes that osteotomy remains in place and the hip doesn't dislocate. As is the case here, we can simply with gentle external rotation pressure, we can identify our osteotomy once again. We'll just have the cob. Jeron, can you show us that osteotomy? We're getting an overhead view now. Okay. Varying now, okay. Here's the cob in the osteotomy. Okay, and then we'll simply attempt to elevate that femoral neck up into the wound and completely and further displace that osteotomy into this position. That allows our leg holder now to get this leg into this position of essential 90 degrees of external rotation. And we'll try to 2
3 keep the femur now parallel with the floor so that I have good reference points as I begin to examine the femoral neck. Jeron, can you show us that leg position one more time? Can we show his front view of how they're holding the leg? Okay, once again the patient s up in the lateral decubitus position. This leg is now extended posterior to the other leg and externally rotated at 90 degrees. So you're going posterior to the down leg? Yes, I am. Okay. All right, we'll place one retractor now just inferior to the femoral neck. A little lift then. And I'll place the posterior retractor over the greater trochanter, over the posterior aspect of the greater trochanter. Let me reposition you a little more inferiorly on this neck. Good. What I'll do now is simply get rid of the last bit of capsule that I didn't -- wasn t able to get on my initial approach to begin to orient -- this is the dorsal aspect of the femoral neck in the area that we'll call the saddle which is the junction between the greater trochanter and the superior femoral neck. I'll simply remote a little more capsule from this. Need a little more light on the subject here. There we go. I'm going to try to not to cut these fibers or muscle but simply work underneath them and get the capsule taken out the inferior neck here. Now you actually haven't done a capsular incision here. You ve left the wings of the capsule in the wound. The -- we have not done a capsulectomy, we've done a capsulotomy at this point. Okay. Give me a little lift, Denton, see if I can show you that greater trochanter a little better. All right, cleared a little more capsule here. Once again, working in that saddle region. Now as you do this release, what tells you how much and when to stop? Actually at this point it s really not a release. What I want to do is get a clear visualization of this saddle region and of the anterior portion of the femoral neck. My preoperative templating -- see a broach -- tells me that from this saddle I need to measure down, interiorly down the femur, approximately one centimeter to the shoulder of my prosthesis. And then I will simply use the prosthesis to guide me to make a cut along the face of the -- which will mimic the face of this -- the broach. Anybody have a saw? So using the broach as a guide to give me my angle -- there you go, Christian. And once again -- I don't know if we can see this -- but beginning the apex of my cut one centimeter down from the saddle, we'll begin our cut. And if we're careful with our saw, we can easily feel when we've completed these cuts. Got an osteotome? Our neck fragment should now be free and we simply displace it utilizing an osteotome. And have we got a Lane? And now we'll try to get it out of here. This is our neck fragment that we've just taken out, put it back in its anatomic position. This is the cut that we've made which comes down from the saddle. This is our osteotomy of the femoral neck. This is our osteotomy that we made originally through the femoral head. We've simply removed that piece at this point. Now we'll reposition our leg again, which is basically into an anatomic position with simple slight external rotation. And now I can feel the acetabulum with my thumb and that small retained piece of femoral head. Take a single retractor and place it just over posterior rim of the acetabulum. Another retractor, which I'm going to punch through the capsule and place now just on the anterior rim of the acetabulum. And we can see this retained fragment of head, which moves pretty freely within the acetabulum. Let s have a pony Hohman. I noticed you're not using the lighted retractors, so you're basically doing this with MIS retractors and not using the additional lighted components. You think that you're comfortable with that exposure and 3
4 lighting? Yeah, that s correct. This -- certainly with just reasonable overhead surgical lights, we seem to see just fine. What I'm doing here is simply levering the femoral head now out of the acetabulum. Let s have a Lane once again. And just utilizing a Lane bone-holding forceps here, see if I can capture that head. Now one thing I notice, as you ve made your osteotomy, do you do any free determination of anteversion of the femoral head and neck on the femur at the -- prior to doing any of the osteotomy work or removal of the femoral head or by looking at the leg position? Generally not. We try to make the determination of whether anteversion and angle of the femoral neck is relatively within normal boundaries with our preoperative templating. Okay. People that have -- such as CDH ers for instance -- that have excessive anteversion, I would not recommend this procedure for, owing to the fact that the stems that we're using can allow for addition of some additional anteversion but certainly not the degree that we sometimes see in those conditions. Now, with the head up. Can we have a 15? Yeah. We'll see if we can use a large curved retractor just posterior to the acetabulum. I like this because it presents a nice, flat, broad base to retract the gluteus medius. Nice rounded edges so that we minimize our trauma to our muscle? Exactly true. And without removing any labrum yet, we can see that we get very nice exposure of our acetabular fossa. Let s go deep, deep. Now in terms of patient positioning for acetabular orientation, anything special you do in that arena? Yeah, as we -- I think it s critical that we put the patient on the table in a very predictable fashion. In this case, we've used a device, called the Montreal Positioner, which anteriorly allows us to have a very rigid post that s fixed to the table. And I can roll the patient up on their side, placing both anterior superior iliac spines against that post, which then assures me that I'm directly lateral, also assures me that my pelvis isn't tipped one way or the other. That will become critical ultimately as we then try to ream and try to position our acetabular component. While we've been simply cleaning away inter-acetabular labrum remnants, at this point we're going to look and see if we think we have any severe osteophytes. We've identified on preoperative films that in this case we don't, but this is a very nice time that we can access those osteophytes that we tend to get about the acetabulum. While we've been preparing here, Christina I back has been measuring that femoral head, all right, and beginning to assist us with thought on where we're going to start our reaming. We're going to use these cutaway reamers with square teeth that Zimmer provides for these minimally invasive procedures. And indeed they are very sharp. One of our minimally invasive principles that we like to obey is to try to have as few passes of these sharp reamers through this tender muscle bed as we can. So generally, we'll start with about 3 millimeters below our anticipated size, which today on templating and here with measurement is going to be hopefully a final size of about 58 millimeters. So you're starting with a what size reamer? 55. A 55? And what size did you measure your femoral head? 58, right. Simply introduce this into the acetabulum, all right. Now positioning, do you medialize at all if you feel there is a medial osteophyte or do you go directly to the position you want your acetabulum component to ultimately be? 4
5 All right, I tend to medialize but only to the point where I can get a good leading hemisphere. I am not fanatic about medializing all the way down to the inner table. And do you like to release the inferior labral ligament or do any foveal debridement? I'll only debride the fovea if, during my reaming, the obdurator branch starts to bleed that tends to come up through there. But today we can see that we still have down in our obtuator, this soft tissue. I'll simply tend to ignore that if it s not in the way. I don't know if we can show in the posterior inferior aspect of the incision it s a heavy band of tissue coming across which certainly can be commonly mistaken for the transverse acetabular ligament. Indeed, that s not in this case. This is simply a fold of capsule. We shouldn t take that capsule out. It will help -- see we want to keep it and help with stability. Now at this point in time, do you ever do a capsular release if you have a very stiff hip and you're having problems mobilizing the femoral portion of the patient out of the way of your acetabulum? Generally that s not necessary. Sometimes we'll perform simply a split of this inferior capsule to help get that out of the way and help pass our instruments better. But generally, no further releases are necessary. Now we'll pass our final reamer. I tend to always try to spin these reamers backwards before we spin them forwards in these cases where we're becoming very aggressive and reaming all the way up to size in just one or two passes. These reamers can get hung up on osteophytes, they can certainly get hung up on the tips of retractors that inadvertently are placed interarticularly. And if we'll spin backwards, we can expose all those facts. If we spin forward and actually catch the reamer teeth on instruments or on osteophytes, we can have the reamer jump and do damage we don't want. So this reamer you have in now is what size? This is 58, this is our final reamer. Can we show how much bone was taken out with that acetabular reamer? Because I ream for depth with my first reamer, now I'm simply reaming for size, for diameter. Focused in. So at this point we've got a good bleeding hemisphere of good supportive bone throughout and I'm satisfied that we've got a good bed here. Robert, what we need is a 58 acetabular shell. While he s opening that, can I have the rojure please? And which cup acetabular component are you using? We'll use the Zimmer trabecular metal acetabular component in a modular fashion today. My favorite component. And with a nice largely intact acetabulum, we will use it with a minimum of holes, called the cluster pattern. And in terms of your placement, what s your idea position for this cup? Interestingly enough, with this approach, initially in my experience I operated through a posterior approach where we tended to antevert cups perhaps 15 to 20 degrees. As I learned this operation, we tend to in a normal acetabulum try to antevert the cup and match the acetabulum here. But as we'll put the socket in and line it up, you'll see that it would appear that we're inserting these acceptably in just 5 to 10 degrees of anteversion with approximately 45 degrees of theta. So we're pretty well clean here, guys. Got a cup? Here s our trabecular metal cup. For the tolls, we'll use a dog-leg type of inserter to allow for facilitation for our soft issues. Once again, getting the cup in, we'll simply try to shoehorn the cup inside the wound. 5
6 Yeah, the trabecular metal tends to catch on a lot of different things. Any special tips in getting this in without dragging a bunch of soft tissue in in these minimally invasive incisions? You bet. What we'll try to do to minimize that is we'll try to use our retractors as skids for the widest part of this socket. And at that point we're not tearing up tissue -- give me a little indent -- plus it will help guide us down. We tend to line the cup up in its position instead of sort of the standard toilet plunger technique and we'll tend to just place pressure and just try to deliver this cup straight down to the acetabulum. Sometimes this anterior retractor is what holds us up. But most of the time the cup will -- I'll put you back in here -- deliver down to the acetabulur introitus here. And we've got this cup partially seated but certainly we are able to now control our final theta angle. We're looking for approximately 45 degrees. In this case, we can use our bar for an angle, or we can simply aim our screw port directly toward the ceiling. Alignment of the patient on the table is what we're going to use for to determine our anteversion. Right now the cup is in what I would call neutral. And we'll simply move forward just about 5 degrees off of that. Do you change your position at all for a male versus a female patient? I don't, I don't. We'll drive our cup into a finely seated position, remove our inserter. I'll check for final seating, utilizing the tip of an instrument through the drill hole and see if I'm fully seated, and indeed I am. Can I have the drill. With a trabecular metal component that seats nice and tightly like this, a screw is probably superfluous, however it s become my habit to place a single superiorly placed dome screw in these cups. If the patient has very rigid bone, do you at all over-ream one additional millimeter to get this component to seat, because this is a 2-millimeter press fit, correct? Indeed, at the rim. It s an elliptical cup so that the apex sits aligned to line fit. And yes, indeed out at the rim it gives us an additional millimeter of radius. If I can -- if I pound on the cup and the cup simply bounces on the mouth of the acetabulum or doesn't fully seat, indeed we will ream up. You got a 30 screw please. The screw we're going to use today is not to hold the cup in or provide additional stability, it s simply to provide rotational stability that I think is necessary as we do our final reduction. You certainly can load this, the edge of the socket, for a moment quite eccentrically. So the screw doesn't necessarily have to be terribly long. In this case we'll use a 30-millimeter screw. Just kind of an anti-rotation screw. That's exactly correct. And a nice good bite. You got a 36 neutral? Now are you going to be using the real acetabulum liner or a trial liner? No, we'll move forward with the final liner, owing to the fact that my cup is well positioned. It s the size cup that I actually had planned on in my templating. And this will allow us then to use a pretty standard nonelevated liner. If we need to tweak anteversion or retro version, the nice thing with using the stem that we have today is that we can accomplish that through the stem and don't need to do it here. Come on out. So if, for any reason, you need to accommodate the total anteversion of a total hip replacement, because you're using the connective, you feel that you can do this directly on the femoral side and not need elevated or different liners and can go directly to your original or your planned liner? Quite true. We'll tap our liner into position. And I'll check that our locking mechanism is closed and moves freely and any hitting of the cup is nice and seated. Okay, come on out. At this point with the acetabulum completed, we'll move onto preparation of the femur. You noted that this, once again, will extend the femur and externally rotate it. We'll place the foot in a bag, a sterile bag back here. Initially I'll -- got a little bleeder here that I'm seeing -- we're going to place a standard neck elevator at this point underneath this neck. There you go, Kimmy. 6
7 Any problems with very muscular or very heavy patients? Generally not. The key to this operation seems to be if we can get a nice long femur that we can then extend an AD duct, helps us gain good access to the working on the proximal femur. The downside on some of these, if we have very muscular, very short-thighed people, then it can be difficult to mobilize the leg. So with one retractor now underneath the neck I'll pace a second retractor over the top, over the tip of the greater trochanter. I'll let Denton AD duct for us a bit. Place a very small retractor behind the neck here. Which retractor is that that you're using there, the third one? We call it a little number one. It s just a very tiny vent Hohman type retractor. Can you show us the retractor? There you go. See that? We can clean up here a little bit. Let s see a heavy pickup. Now today I've got pretty good access into this proximal neck at a pretty good angle. If I'm having difficulty getting this leg AD ducted, almost always it s due to a very tight portion of the capsule which inserts on the top of the acetabulum. This is not the adductor, it s simply the capsule. And I can split that. See how that retracts in a pretty aggressive fashion. And indeed, we can continue that release around the posterior trochanter, even onto the posterior neck in theory, as needed. Can you show that to us one more time, point it out to us? We didn't really get a great view when you were releasing it. Yeah, it will be a little difficult to show you here, but I'm working right now on top, directly on top. And this is the last bit of residual femoral neck that s been left behind. And all I'm doing is trying to remove the last bit of tenuous capsule that s been left there. This retractor is actually over the tip of the trochanter. What I'll do now is use a cookie cutter type of osteotome to remove this last bit of neck and gently gain access to the initial portion of my intramedullary canal. I'll then use a blunt type of canal finder -- because I certainly don't want to perforate -- to find my canal in a final fashion. Any special tricks you use to align this with the extremity so that you don't perforate? Well, the nice thing is is that we certainly have a nice view of the femur and we have -- with a nice long instrument, we tend to be able to align that with the femur in both planes quite easily, all right. This blunt retractor should pass very easily. If it doesn't, we'll tend to do a bit more capsule release. We'll tend to reposition our leg until we can very comfortably ascertain that we're in the acetabulum -- I mean, excuse me, in the intermidulary canal. We'll then start rasping. These are the rasps for the new connective system. They're diamond cutting and they cut in both directions with two sets of teeth and are relieved, both medially and laterally, proximately so we don't create a lot of AP channel. I'll tend to start with a very tiny rasp and we'll work our way out. Do you start with the smallest size rasp? The smallest size rasp, I believe, is a number four, which is very tiny. We'll start with the smallest standard rasp. This is a five. This is a six today? What you'll also see is the rasp handles are bent. And the nice thing is that really allows us to get that rasp down on plane. And these nice handles feed the raps into the wound very nicely without putting extra stress on the soft tissue. From our templating, we know that the final shoulder of the rasp we'd like to be approximately 2 to 2-1/4 centimeters down from the tip of the trochanter. The nice thing about this operation is that, as I place these rasps, I can always visualize the shoulder of the rasp. I can always visualize the tip of the greater trochanter. As we advance these rasps, once they advance to the top of the rasp, stop. We don't want to drive the entire handle of things down into the femur and necessitate or give us the possibility of fracture. So if this passes easily, we'll simply move up to the next size. Actually, let s skip. That rasp passed very easily in size 6. My final templated size is a Therefore, we'll skip one rasp here and try to pass a 9 rasp. No? Initially 7
8 these rasps should feed into the intermedulary canal very easily without pounding and only after that -- let s go up on 1 now. I've noticed that when I also use this system, that when you go to a next larger rasp size that if your rasp doesn't feed to within about 3 centimeters, just easily in to the stem, you probably need back down a rasp size. Have you found that also? Absolutely, absolutely. And the nice size about these is that every rasp is effectively the same size, they just grow proportionally so that if I rasp and decide that I should have stopped with the one prior because I can't get this rasp fully seated, I haven't done any damage and I can simply go back down with the stem that s the size of the rasp smaller. And that stem will have the same size. It will simply fit more deeply within the femur. How far would you let this rasp counter-sync into the femoral canal before you sized up? Only to the top line of the rasp here. There s also a hole that they've done and placed in this for extraction. And the nice thing about that hole is -- for our colleagues that do invasive procedures where they can't see the rasp, they re doing them under fluoroscopic control -- that hole is easily visible. Once the rasp plunges far enough that the hole gets in line with your osteotomy, it s time to move up to the next size. Perhaps you heard that rasp start to change tones, which means we're nearing our size because the rasp is starting to get tight. I still think we could move up one more. Now are you adjusting your anteversion at all in this? At this point, I'm following the natural anteversion of the neck, and allowing that rasp to take its most natural course. The nice thing about doing this with the connective system is it allows us to put the largest stem in to the best position, giving good fill here, and then if indeed the anteversion of the neck and the final position of the stem appears to be a little different than what we want, the versatility of this system will allow us to build in anteversion or relative retro version on top of a previously placed stem. Okay, this is now nice and tight. The stem is seating to its full depth but not over-seating. Can you show us that position? We really can't see where it s seating in the -- yeah. See if we can do this a little bit. Okay. The stem is essentially fully seated here. You don't want the collar to get down inside. John, can you put an interior retractor just down at the base of your wound for the camera? Where would you like us to put that? Just at the inferior portion of your wound just to retract it. There you go. Does that help? Yeah. I don't want to pull too much and injure a muscle here. Okay. And with that stem fitting nice and tightly, here s the tip of my trochanter. Here s the shoulder of my prosthesis. And do we have a ruler? Now have you got a scissors? Yeah, just nip off the tip of this ruler so that we go a zero. And I can set the ruler down on the shoulder of this. And at this point, we're at about 2.5 centimeters, which is right approximately where we wanted it. So this is the stem that we'll use. And once again, if the stem feels the progression of our rasp moves along nicely, we end up with a stem size that s largely what we wanted. The stem gets right at an appropriate seating depth. At this point then I'm very comfortable and I will not proceed with trialing off of the rasp. However, with the rasp seated, we can easily leave the rasp in place and build up the trial necks and trial heads to find our final stability and length. What we'll do instead is 8
9 we'll simply place the final stem and then, once again, the versatility of this system will allow us to use trials at the level of the neck and the head to find out final position and stability. Yep. So you are basically very comfortable not only with the fit of the stem after the rasping, but also trialing with the true component in place with your head and neck options? Indeed. We templated for a 12.5, we ended up with a stem that s only one size smaller that that, which is within our range of error on templating. So we're very comfortable with this. Now, once you put your real stem in, your true component, are you going to modify your choice of the head and neck because your stem size is what you actually templated? Perhaps not because my final stem seating height is identical to what I wanted. And ultimately, whether the size of the stem changes or not for fit and fill, the final seating height of that stem is what s most critical in determining whether I need to -- my stem s a little high and I need to shorten my thoughts of the neck length or my stem is a little tall -- excuse me, a little short and I need to add neck in order to fulfill my templating requirements. We have our stem? Here's the connective stem. It s a -- Can we get a close-up of the component? It s a bi-taper design, which is proximally plasma sprayed. The very nice thing about this stem for use in minimally invasive surgery is that I don't have the neck and the trunion already built on so that the stem can very easily be passed into the wound and down the femoral canal. We'll let that stem come to a preseated position and then simply tap it gently until it stops into its final position which corresponds with exactly the same position the broach was in, indicating that we're in good position. As we now begin to trial, I'll always start with certainly a full size smaller, shorter neck line than I presumed that I would use and the fact that I want this reduction to be very easy. I can then determine if I need to go up a size by looking at our tissue tension in the hip. And I generally know that I'm going to go up a size from our templating. What we don't want to do is force a reduction with a neck that is too long and then struggle to get the trial components dislocated once again. So let s have a minus 4 and a neck that, yeah, we can stay right here. That's good. All right. And do we have a head? Now which neck trial did you select for this patient? This is a neutral neck. Can we see that? It s not anteverted within the neck. It is a standard neck as far as neck angle goes. And on top of all of these, we'll simply use a zero head. We won't add neck length or subtrack neck length at the head level at all. We'll try to accomplish that in this system through use of the trial neck. I'll tend to pre-assemble these. I notice this was a gold band, so this has no ante or retroverson built into the neck trial at this time, correct? None whatsoever. And I don't know if you can see what I ve done is assemble the trial within the final stem. Come on out, come on out, everybody. I'll remove our retractors now. I'll simply place my thumb on the head, let this leg come back into a more neutral position and see if we can effect a relatively easy reduction with no other pressure than what I exert with my thumb. Just see here now is our final construct: stem, here's our neck, head and here s our previously placed acetabulum. Now the benefit of this procedure is with the capsule posteriorly and anteriorly intact, we can begin to use a shuck test -- go ahead -- to see if our tissue tension looks reasonable too, okay. There you go. And Dent can just slightly dislocate that hip, sublux that hip, and with just a slight bounce will feel nice and comfortable. But actually this, this reduced neck length, is appropriate for this case. Come on out, Kim. Now what would cause you to choose a greater offset or a greater leg length than what you currently have? 9
10 Generally, I'll try to make those decisions preoperatively. If I can look at my template and tell that I have a very tall Valgus neck or a very short angle, perhaps 125 degree Varus situation, I'll tend to immediately start to make that in my trial construct. Likewise, if I determine that we have very high offset, will tend to immediately try to mimic that in our trial construct. Interoperably, I think it s very difficult to determine whether you need more neck length or a different neck shaft angle and/or determine offset. I think those things have to be determined preoperatively. Now, interoperatively, we an change our relative anteversion by using different necks within this versatile system to affect stability. So here we have a very basic situation. Here we have our hip relocated. You can see that our medius here is completely intact. We come in and these hips tend to be tremendously stable. Always remember through these relative anterior approaches that we need to check our hip at extension and external rotation as well, check for stability. So we're pretty happy with this one. I'll replace this posterior retractor. We got a bone hook? Put a bone hook around the neck. Give mean little tension down. We'll dislocate our hip and we'll disassemble. So this is a 36 millimeter plus zero head. And let s go with a glass head on this gentleman, okay. So your implant trial neck is a what letter? It s an E. And you're going to actually implant a -- The same one. Same one. We're going to stick with this same one. I was very pleased with this construct with respect to tissue tension, final height of our stem and stability. Now this trial does not have the bump, correct? This one actually does have a bump -- does he. But the stem s the same either direction on this one. Okay. In most of these it s very important, especially if we're using one that has any changes whether it s a higher neck, a more Valgus neck, a more Varus neck or it s anteverted or retro version that when we trial, we trial with this little bump that s present on one side but not the other so that when we put in our finals, we're not putting things in exactly opposite of what we intended, right. Because one could see perhaps in this neck that this neck could be used to take perhaps 150 degree neck shaft angle, but if we turn it over we turn it in the exactly opposite situation and perhaps just 125 degrees. So it s critical that every one of these that you trial with the nubbin up so that, as you put your final components back together, you're getting exactly what you trailed and not something completely different. Okay, let s have that neck. And what we do with these is try to assemble the entire construct -- give me a bone hook, ah so -- and then we'll impact and finally seat it all at once. Let s have an impacter. So technique-wise, you don't impact these separately, you just do -- assemble and do one basically impaction to assemble neck as well as head. Indeed, indeed. Take one final check of our acetabulum, make sure that s clear and let s reduce that. Okay. Here s our final reduction. In this case, we've used a Biolex ceramic femoral head against a standard polyethylene in the fact that this is young, active heavy 60-year-old gentleman. Okay. So you're using a large head with very slim tapered head and neck combination, so you feel that your impingement and levering should be actually -- Very low. 10
11 Very low. Once again, once we've accomplished this, I'll replace this posterior retractor not one layer shallower, indeed now extra-articularly. And you'll see that the flaps that we created with our initial capsulotomy are still intact both anteriorly and posteriorly. We don't need this capsule for stability but simply to make sure that the flaps stay where they belong, we'll put in a single heavy Tycron stitch -- got a pickup -- and tie those flaps back together again. Generally when I repair the capsule, I find that if I ve misgauged my leg length or my stability in my anteversion, my capsule will not close nicely. I think that that s a very good indicator. Sometimes in these with thick, heavy capsule, sometimes if the capsule gets in the way of the operation too much, I'll excise pieces of the capsule or do a complete capsulectomy here of these two flaps. As I don't think that superiorly here they contribute to our anteversion at all. We've now closed the capsule. Once again, we'll simply allow the muscles to reoppose themselves. Do we have a dreg? Very little trauma to your medius there. Exactly. And generally a minimum of bleeding in these cases. I'll simply place a drain underneath and through the lateralis and we'll just place a drain right on top of the capsule here. We'll plan to remove that first thing tomorrow morning. Post-op rehab for this patient, immediate weight-bearing? Absolutely -- let s have a sponge. He -- if we can get a little cooperation out of our therapy department, he ll spend two hours in the recovery room and then head upstairs and immediately begin his therapy in a weight-bearing as-tolerated fashion. When will he go home? Come on over. Depending on how he feels and the reports from therapy, he ll either go home tomorrow, or if they feel he needs another session, I have no problem keeping him that second night and sending him home the following morning. So your patients generally are going home, not to rehab, and within a day or two of surgery. Absolutely. Normally our rehab placements, quite frankly, are much more social placements for some of our older patients who live alone and really have no place to go other than that. All right, now we'll simply close our rent in the tensor. What about your post-operative limp? Excuse me? Do you have a postoperative limp? When a case goes like this and there s -- I don't see really that we've involved any of those branches of the superior gluteal nerve, and when we have virtually no embarrassment of all at the gluteus medius, I would anticipate that this fellow will not limp honestly at all. He ll certainly be sore in this incisional area, but generally he ll walk right away from this. Well, John, I think we're just about done here. I'd like to thank you for letting us join you in the operating room. And that s really about it from here from Tucson, Arizona. And thank you for joining us for the Webcast. 11
12 Absolutely, certainly our pleasure to have you all today. We'll put this last stitch in the tensor and then we'll let Kim finish with the subcutaneous tissue. We'll use some small staples in the skin, a light dressing and we'll let the patient head back to the recovery area. Thank you for attending and hopefully you will see the benefits and the advantages of the new Zimmer Kinectiv System. Thank you. Thank you for watching this "OR Live" Webcast presentation brought to you by Zimmer. "OR Live" makes it easy for you to learn more. Just click on the Request Information button on your Webcast screen and open the door to informed medical care. "OR Live," the vision of improving health. 12
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
MINIMALLY INVASIVE TOTAL HIP REPLACEMENT VANDERBILT UNIVERSITY MEDICAL CENTER, NASHVILLE, TN Broadcast April 13 2005
 NARRATOR MINIMALLY INVASIVE TOTAL HIP REPLACEMENT VANDERBILT UNIVERSITY MEDICAL CENTER, NASHVILLE, TN Broadcast April 13 2005 For the more than 200,000 people who undergo hip replacement surgery every
NARRATOR MINIMALLY INVASIVE TOTAL HIP REPLACEMENT VANDERBILT UNIVERSITY MEDICAL CENTER, NASHVILLE, TN Broadcast April 13 2005 For the more than 200,000 people who undergo hip replacement surgery every
Design surgeon list. Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team:
 Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
MIS Direct Anterior Approach Surgical Protocol
 Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Hip Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Zimmer M/L Taper Hip Prosthesis. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Introduction
 ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
P REPLACEMENT SURGERY
 P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Exeter X3 RimFit. Acetabular Cup Surgical Protocol
 Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Total hip arthroplasty (THA) through the anterior approach
 Primary Total Hip Arthroplasty with a Minimally Invasive Anterior Approach Jonathan G. Yerasimides, MD, and Joel M. Matta, MD Total hip arthroplasty (THA) through the anterior approach is a minimally invasive
Primary Total Hip Arthroplasty with a Minimally Invasive Anterior Approach Jonathan G. Yerasimides, MD, and Joel M. Matta, MD Total hip arthroplasty (THA) through the anterior approach is a minimally invasive
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
When is Hip Arthroscopy recommended?
 HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
HIP ARTHROSCOPY Hip arthroscopy is a minimally invasive surgical procedure that uses a camera inserted through very small incisions to examine and treat problems in the hip joint. The camera displays pictures
Why an Exactech Hip is Right for You
 Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
PINNACLE. Polyethylene Surgical Technique. Surgical Technique
 PINNACLE Hip Solutions Polyethylene Surgical Technique Surgical Technique Table of Contents Surgical technique Introduction 4 Templating and Pre-Operative Planning 6 Surgical Approach Anterolateral 8
PINNACLE Hip Solutions Polyethylene Surgical Technique Surgical Technique Table of Contents Surgical technique Introduction 4 Templating and Pre-Operative Planning 6 Surgical Approach Anterolateral 8
NETWORK FITNESS FACTS THE HIP
 NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
Surgical Approaches to Total Hip Arthroplasty
 Surgical Approaches to Total Hip Arthroplasty Daniel Kelmanovich, 1 Michael L. Parks, MD, 2 Raj Sinha, MD, PhD, 3 and William Macaulay, MD 4 Surgical exposure of the hip for trauma, infection, or reconstruction
Surgical Approaches to Total Hip Arthroplasty Daniel Kelmanovich, 1 Michael L. Parks, MD, 2 Raj Sinha, MD, PhD, 3 and William Macaulay, MD 4 Surgical exposure of the hip for trauma, infection, or reconstruction
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer MOST Options System
 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Aesculap Orthopaedics Metha
 Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Introduction to the Bertram Hip Spacer
 Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e
 the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e REVO The following techniques are described by Stephen J. Snyder, M.D., Van Nuys, CA. Arthroscopic repair of the rotator
the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e REVO The following techniques are described by Stephen J. Snyder, M.D., Van Nuys, CA. Arthroscopic repair of the rotator
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Femoral head and neck ostectomy (FHO) is a commonly
 P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
P ro c e d u re s P ro O R T H O P E D I C S Peer Reviewed Laura E. Peycke, DVM, MS, Diplomate CVS Texas &M University Femoral Head & Neck Ostectomy Femoral head and neck ostectomy (FHO) is a commonly
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Arthroscopic Shoulder Procedures. David C. Neuschwander MD. Shoulder Instability. Allegheny Health Network Orthopedic Associates of Pittsburgh
 Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
The Anterior Approach for Total Hip Replacement. Background and Operative Technique
 The Anterior Approach for Total Hip Replacement Background and Operative Technique Joel M. Matta, MD Hip and Pelvis Institute at Saint John s Health Center, Director Santa Monica, California RECOVERY FUNCTION
The Anterior Approach for Total Hip Replacement Background and Operative Technique Joel M. Matta, MD Hip and Pelvis Institute at Saint John s Health Center, Director Santa Monica, California RECOVERY FUNCTION
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Hips designed to fit the unique anatomies of men and women Independent control for a natural fit Simple, practical solutions for optimal restoration
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Lower Body Exercise One: Glute Bridge
 Lower Body Exercise One: Glute Bridge Lying on your back hands by your side, head on the floor. Position your feet shoulder width apart close to your glutes, feet facing forwards. Place a theraband/mini
Lower Body Exercise One: Glute Bridge Lying on your back hands by your side, head on the floor. Position your feet shoulder width apart close to your glutes, feet facing forwards. Place a theraband/mini
Exeter. Surgical Technique. V40 Stem Cement-in-Cement. Orthopaedics
 Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Metasul LDH Large Diameter Head
 Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
MDMTM. Surgical Technique. Modular Dual Mobility TM Acetabular System. Orthopaedics
 MDMTM X3 Modular Dual Mobility TM Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint
MDMTM X3 Modular Dual Mobility TM Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint
Double Bone Plug Meniscus Reconstruction Surgical Technique
 Double Bone Plug Meniscus Reconstruction Surgical Technique Double Bone Plug Meniscus Low Profile Reamer 2-0 FiberWire Meniscus Repair Needles Collared Pin & Coring Reamer Set RetroConstruction Drill Guide
Double Bone Plug Meniscus Reconstruction Surgical Technique Double Bone Plug Meniscus Low Profile Reamer 2-0 FiberWire Meniscus Repair Needles Collared Pin & Coring Reamer Set RetroConstruction Drill Guide
Technique Guide. Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Blender Notes. Introduction to Digital Modelling and Animation in Design Blender Tutorial - week 9 The Game Engine
 Blender Notes Introduction to Digital Modelling and Animation in Design Blender Tutorial - week 9 The Game Engine The Blender Game Engine This week we will have an introduction to the Game Engine build
Blender Notes Introduction to Digital Modelling and Animation in Design Blender Tutorial - week 9 The Game Engine The Blender Game Engine This week we will have an introduction to the Game Engine build
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MDM. Surgical Technique. Modular Dual Mobility Acetabular System. Orthopaedics
 MDM X3 Modular Dual Mobility Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint disease
MDM X3 Modular Dual Mobility Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint disease
Primary V40 Surgical Protocol. Exeter. total hip system
 Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Knotilus TM. Anchor Instability Repair. Technique Guide
 Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Don t. Hamstrings. Calf Muscles. both legs 2-3 times. stretch is felt in the back of the calf. Repeat with both legs 2-3 times.
 Remember to: Warm-up your muscles first before stretching (e.g. stretch after walking). Stretch until you feel mild discomfort, not pain. Never bounce or force a stretch. Hold the stretch for 10-30 seconds
Remember to: Warm-up your muscles first before stretching (e.g. stretch after walking). Stretch until you feel mild discomfort, not pain. Never bounce or force a stretch. Hold the stretch for 10-30 seconds
Self-Myofascial Release Foam Roller Massage
 How it works. Self-Myofascial Release Foam Roller Massage Traditional stretching techniques simply cause increases in muscle length and can actually increase your chances of injury. Self-myofascial release
How it works. Self-Myofascial Release Foam Roller Massage Traditional stretching techniques simply cause increases in muscle length and can actually increase your chances of injury. Self-myofascial release
Surgical technique. Sagitta EVL
 Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
MOON SHOULDER GROUP. Rotator Cuff Home Exercise Program. MOON Shoulder Group
 MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
Zimmer Natural Nail System. Cephalomedullary Nail Surgical Technique STANDARD
 Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
A: We really embarrassed ourselves last night at that business function.
 Dialog: VIP LESSON 049 - Future of Business A: We really embarrassed ourselves last night at that business function. B: What are you talking about? A: We didn't even have business cards to hand out. We
Dialog: VIP LESSON 049 - Future of Business A: We really embarrassed ourselves last night at that business function. B: What are you talking about? A: We didn't even have business cards to hand out. We
Scaphoid Fracture of the Wrist
 Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Page 1 of 6 Scaphoid Fracture of the Wrist Doctors commonly diagnose a sprained wrist after a patient falls on an outstretched hand. However, if pain and swelling don't go away, doctors become suspicious
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP
 Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Rotator Cuff Home Exercise Program MOON SHOULDER GROUP Introduction The MOON Shoulder group is a Multi-center Orthopaedic Outcomes Network. In other words, it is a group of doctors from around the country
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Titanium Wire with Barb and Needle. For canthal tendon procedures.
 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Rejuvenate Total Hip System Surgical Protocol. Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility
 Rejuvenate Total Hip System Surgical Protocol Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility Rejuvenate Total Hip System Surgical Protocol Table of Contents
Rejuvenate Total Hip System Surgical Protocol Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility Rejuvenate Total Hip System Surgical Protocol Table of Contents
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Assisting Students Who Use Wheelchairs:
 Quick-Guide Extra Assisting Students Who Use Wheelchairs: Guidelines for School Personnel Michael F. Giangreco, Irene McEwen, Timothy Fox, and Deborah Lisi-Baker Quick-Guides to Inclusion 3: Ideas for
Quick-Guide Extra Assisting Students Who Use Wheelchairs: Guidelines for School Personnel Michael F. Giangreco, Irene McEwen, Timothy Fox, and Deborah Lisi-Baker Quick-Guides to Inclusion 3: Ideas for
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique
 Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
Okay, good. He's gonna release the computers for you and allow you to log into NSLDS.
 Welcome to the NSLDS hands-on session. My name is Larry Parker. I'm from the Department of Education NSLDS. Today, I have with me a whole host of folks, so we're gonna make sure that if you have any questions
Welcome to the NSLDS hands-on session. My name is Larry Parker. I'm from the Department of Education NSLDS. Today, I have with me a whole host of folks, so we're gonna make sure that if you have any questions
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Shoulder Restoration System
 Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Technique Guide. Orthopaedic Cable System. Cerclage solutions for general surgery.
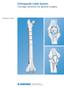 Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
9 exercises to rehab a torn ACL without surgery
 MENU Search foxnews.com Health Home Men's Health Women's Health Children's Health Alternative Medicine Diabetes Heart Health Allergies HEALTH 9 exercises to rehab a torn ACL without surgery By Julie Wilcox
MENU Search foxnews.com Health Home Men's Health Women's Health Children's Health Alternative Medicine Diabetes Heart Health Allergies HEALTH 9 exercises to rehab a torn ACL without surgery By Julie Wilcox
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Baby Hip Health A guide to hip development
 steps We don t take walking for granted steps We don t take walking for granted Baby Hip Health A guide to hip development Where can I find out more information about DDH? You should contact your medical
steps We don t take walking for granted steps We don t take walking for granted Baby Hip Health A guide to hip development Where can I find out more information about DDH? You should contact your medical
Rotator Cuff and Shoulder Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
MET: Posterior (backward) Rotation of the Innominate Bone.
 MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique. Table of Contents
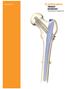 Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
