Acute Nursing Certification Program
|
|
|
- Franklin Lloyd
- 10 years ago
- Views:
Transcription
1 NEO Stroke Network s Acute Nursing Certification Program Level ONE
2 NEO Stroke Network s Acute Nursing Certification Program Launched at Hôpital régional de Sudbury Regional Hospital in the summer and fall of 2010, this program is a regional initiative made available to medical nursing units in the North East for use as a nursing certification Self Learning Program. The program is currently available as a paper copy in a binder that includes all text, pictures, diagrams, tests, references and appendices. In the future, a paperless, online copy will be available for those nurses who choose to complete this program on a work or personal computer. The program consists of eight Stroke Care Topics that can be completed in any order and are arranged as separate modules, each with its own quiz. Each module should take 45 minutes to 75 minutes to complete depending on the module and the nurse s background/experience. A score of 80% is considered a passing score. Although the answer key will not be posted, it is acceptable that the quizzes be done with an open book. Once initiated, the nurse will be given a set amount of time as determined by the manager to complete all eight modules. The Nurse Clinician of the unit or a designate will be the official monitor and tracker of the certification program, accepting and marking all the quizzes and issuing Certificates of Completion to each nurse. The Nursing Certification Program consists of three distinct levels of certification. Level one is includes eight modules, which are: 1) Neuroanatomy, Pathophysiology and Classification of Stroke 2) Pre-hospital and Emergency Management 3) Diagnostics and Assessments 4) Acute Stroke Management 5) NIHSS Training 6) Swallowing, Feeding and Oral Care 7) Mobility and Positioning for the Stroke Patient (incl the DVD) 8) Secondary Stroke Prevention Level two is highly desired for all nurses working in acute stroke care as it is consistent with best practice. It includes training for and certification in an evidenced-based
3 Swallowing Screen Tool. An example of one is TOR-BSST. Your centre may not have implemented a tool at this time. At Sudbury Regional Hospital, TOR-BSST training is currently organized by the Speech Language Pathologist whereby the nurse participates in a four hour training session and is observed completing two skilled TOR-BSST screens on stroke patients. Level three is completion of Apex Innovation s Hemisphere s Stroke Competency e- learning series. This is a new multi-level; interactive; comprehensive; web based educational series from pre-hospital stroke management to emergency care to acute care. It has been designed to train all levels of users, from students to physicians. It has a very comprehensive module on neuroanatomy and pathophysiology of stroke. Registered users receive a key which acts as a one year license to participate in the online series. Users can take as much time as desired to complete each module as long as all modules are successfully completed at the one year mark. The fee for this key will be reimbursed to the nurse once he/she has shown their Certificate of Completion for the series to the Nurse Clinician or designate. Staying current Each nurse is required to re-certify every two years by completing Level one again and demonstrating a score of 80% or better on each of the module s quizzes. The content in the binder (and electronic version) will be reviewed annually and updated according to current Canadian Best Practice Recommendations for Stroke Care and other evidence-based guidelines relevant to the content.
4 NEO Stroke Network s Acute Nursing Certification Program TABLE OF CONTENTS 1. Acute Nursing Certification Program Description and Process 2. Table of Contents 3. MODULE ONE Pathophysiology of Stroke, Neuroanatomy, Stroke Syndromes i) Classification of Stroke ii) Etiology iii) Brain Anatomy iv) Blood Supply v) Stroke Syndromes vi) References vii) Module One Quiz 4. MODULE TWO Pre-Hospital Care and Emergency Management i) Warning Signs of Stroke ii) Emergency Medical Services iii) Acute Thrombolytic Therapy iv) Adverse Effects of t-pa (Alteplase) v) Stroke Mimics vi) Acute ASA Therapy vii) Reducing Ischemic Damage from Hypertension, Hyperglycemia, Hyperthermia, O2 de-saturation viii) References ix) Module Two Quiz 5. MODULE THREE Diagnostics and Assessments i) Acute Nursing Assessment ii) Standardized Neurological Assessments (CNS, NIHSS, GCS) iii) Other Assessments
5 iv) Investigations v) References vi) Module Three Quiz 6. MODULE FOUR Acute Stroke Management i) Stroke Unit ii) The Team of Professionals iii) Post Stroke Complications iv) Other Effects of Stroke v) Discharge Planning vi) References vii) Module Four Quiz 7. MODULE FIVE NIHSS Training OR CNS Training 8. MODULE SIX Swallowing, Feeding and Oral Care i) Dysphagia Facts ii) Normal Swallow iii) Aspiration iv) Dysphagia Screening v) Dysphagia Diets vi) Feeding Strategies vii) Indications for Enteral Nutrition viii) Oral Care ix) References x) Module Six Quiz 9. MODULE SEVEN Mobility and Positioning Educational DVD (to be available soon) i) Considerations ii) General Principles When Assisting a Stroke Survivor iii) Preventing Injury to the Stroke Survivor and You iv) Hemiplegic Shoulder v) Aids and Equipment vi) Positioning Techniques vii) Mobilizing Techniques Including Transfers viii) DVD: Mobilizing and Positioning a Stroke Survivor ix) References x) Module Seven Quiz
6 10. MODULE EIGHT Secondary Stroke Prevention i) Primary Prevention ii) Lifestyle Modification iii) Medication Management iv) Carotid Intervention v) Transient Ischemic Attack (TIA) vi) Secondary Prevention Clinic vii) Patient Teaching re: Medications v) References v) Module Eight Quiz 11. Hospital - Specific Chart Forms (content will vary for each centre) 12. Other Resources i) Northeastern Ontario Stroke Network (NEOSN) Info sheet ii) EVERYTHING STROKE at your fingertips: an Electronic Toolkit for Health Care Providers (announcement) iii) Stroke Organizations: Lists and Websites iv) NEOSN Professional Education Fund 13. APPENDICES i) How to Obtain Level Two Certification ii) How to Obtain Level Three Certification with Apex Innovations Hemisphere s Stroke Competency Series 14. Acknowledgements 15. Certificate of Completion of LEVEL ONE and Pre and Post Self-Evaluation/Feedback/ Comment Form
7 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE ONE Pathophysiology of Stroke Neuroanatomy Stroke Syndromes Upon completion of this module, nurses will be able to define and/or describe: Types of Stroke Etiology of Stroke General Brain Anatomy Major Blood Vessels of Cerebral Circulation Common Stroke Syndromes Right Sided Clinical Deficits Left Sided Clinical Deficits
8 MODULE ONE The following content is from the Acute Stroke Management Resource, Heart and Stroke Foundation of Ontario, Anatomy and Physiology workshop package. It has been edited and formatted for the NEO Stroke Network Self Learning Package
9 Pathophysiology and Anatomy of Stroke Ischemic stroke 80% of all strokes are caused by blockage of an artery resulting in diminished blood flow Usually the result of a blood clot, either thrombotic or embolic in nature Blockage may also occur because of progressive blood vessel occlusion, due to atherosclerosis, or because of local high pressure collapse of small blood vessels Approximately 50% of ischemic strokes are due to a thrombosis Of that 50%, 30% are related to large-vessel disease, especially of the carotid, middle cerebral, or basilar arteries 20% are related to small vessel disease of the deep penetrating arteries, such as the lenticulostriate, basilar penetrating, and medullary arteries (these are known as lacunar infarcts) The remaining 30% of ischemic strokes are embolic 1
10 Medical Illustration 2010 Nucleus Medical Media, Inc. Clot stops blood supply to an area of the brain Etiology of Ischemic Stroke The cause of ischemic stroke can be further classified as one of the following: 1. Large vessel disease may be classified as: a) Cardioembolism - often a result of atrial fibrillation or left ventricular damage after myocardial infarction b) Atherosclerosis - causes a progressive narrowing of the blood vessel through deposit of plaque on the arterial wall. 2. Small vessel disease, known as lacunar infarct, is thought to be the result of occlusion of single, small perforating arteries, located deep in the subcortical areas of the brain. Hypertension is thought to be a major risk factor associated with lacunar infarcts. 2
11 3. Cryptogenic strokes are strokes with no identified cause or etiology. Cryptogenic strokes are more commonly found in younger population, <45years. (Ionita et al., 2005) The classic risk factors for stroke are usually absent in cryptogenic stroke patients. However, Ionita et al (2005) reported that echocardiography studies in these stroke patients showed an increase incidence of Patent Foramen Ovale (PFO) in up to 45% of cases. Hemorrhagic stroke Caused by arterial rupture Can damage other brain tissue as a result of increased intracranial pressure and compression of brain tissue 20% of all strokes 10% of are due to intracerebral hemorrhage 10% are due to subarachnoid hemorrhage or bleeding from AVM (arteriovenous malformation) Medical Illustration 2010 Nucleus Medical Media, Inc. Hemorrhage/blood leaks into brain tissue 3
12 Etiology of Intracerebral Hemorrhage: 1. PRIMARY hemorrhage Hypertension is responsible for approximately 75% of all cases of primary Intracerebral Hemorrhage (ICH). Cerebral amyloid angiopathy (a disease of small blood vessels in the brain with deposits of amyloid protein which may lead to stroke, brain hemorrhage or dementia) is also a common cause. The use of fibrinolytics and anticoagulants make up approximately 10% of all ICH. (Manno et al, 2005) Drug abuse may cause sudden and severe elevations in blood pressure resulting in ICH. Image courtesy of Alberta Health Services 4
13 2. SECONDARY hemorrhage Underlying vascular abnormalities such as aneurysm, arteriovenous malformation are causes of secondary ICH, which makes up approximately 5 % of all ICH. Hemorrhagic transformation, secondary bleeding into the infarcted site, is considered by some to be a natural evolution of a stroke and some studies suggest that almost all infarcts have some element of petechial hemorrhage. Hemorrhagic transformation may be influenced by the size, location and cause of the stroke. The use of antithrombotics including anticoagulants and thrombolytics increases the likelihood of hemorrhagic transformation. Cerebrum The cerebrum is the largest portion of the brain and contains 2 hemispheres. The left hemisphere controls the right side of the body and the right hemisphere controls the left side of the body. The two hemispheres are joined by the corpus callosum. Permission granted to use image 5
14 In 97% of the population, the left hemisphere is the dominant hemisphere. Cerebral Cortex is divided into 4 lobes: Frontal Parietal Temporal Occipital Two important structures are found in the frontal and parietal lobes. In the posterior portion of the frontal lobe, the primary motor cortex can be found. This is also referred to as the motor strip and is involved in the ability of the body to move various body parts. Damage to parts of the motor strip may result in symptoms such as paralysis of the face, arm or leg or difficulty speaking. In the anterior part of the parietal lobe is the primary sensory cortex or sensory strip. It corresponds directly to the body part locations of the motor strip and is involved in the ability to feel or recognize textures. 6
15 Blood Supply to the Brain Arterial supply is from carotid and vertebral arteries which begin extracranially Internal carotid arteries supply anterior 2/3 of hemispheres Vertebral and basilar arteries supply posterior and medial regions of hemispheres, brainstem, diencephalon, cerebellum; cervical spinal cord Both the carotid (anterior) and vertebral (posterior) blood supply originates outside of the cranium from the internal carotid arteries. The carotid and vertebral arteries enter the cranial cavity via the internal carotid, which come off the common carotids and vertebral arteries which originate from the subclavian arteries. 7
16 The internal carotid arteries and its branches supply 2/3 of the cerebral hemispheres. The anterior circulation s major blood vessels are the anterior cerebral and the middle cerebral arteries. The posterior circulation s major vessels are the vertebral, basilar and posterior cerebral arteries and supply the medial and posterior sections of the hemispheres, the brainstem, deep brain structures such as the diencephalon, the cerebellum and the cervical section of the spinal cord. Circle of Willis An important structure within the cerebral circulation is the Circle of Willis. It is located at the base of the brain. The primary purpose of the Circle of Willis is to provide multiple paths of oxygenated blood to the brain. If any of the major vessels become occluded, the various paths of the Circle of Willis attempt to ensure circulation is maintained. 8
17 The Circle of Willis is comprised of the following vessels: Anterior Cerebral Artery Middle Cerebral Artery Anterior Circulation Anterior Communicating Artery Posterior Cerebral Artery Posterior Communicating Artery Posterior Circulation The Posterior and Anterior Communicating Arteries are responsible for connecting the right and left side blood vessels so that circulation is seamless. Major Cerebral Arteries Image courtesy of Communications, Alberta Health Services 9
18 The Anterior Cerebral Artery (ACA) originates from the internal carotid artery and supplies the anterior portion of the basal ganglia, the corpus callosum, the medial and superior portions of the frontal lobe and the anterior part of the parietal lobe. Region of Anterior Cerebral Artery Permission granted to use image Legend for picture: Anterior Cerebral Artery- blue Middle Cerebral Artery- pink Posterior Cerebral Artery- green The key functional areas that receive blood supply from the anterior cerebral artery are: Primary motor cortex involving the leg and foot areas The centre for micturation found in the frontal lobe The motor planning centre found in the frontal lobe The anterior and middle portions of the corpus callosum A patient who has a stroke involving the anterior cerebral artery may experience weakness in the leg and foot, difficulties with micturation, difficulties with the ability to plan and carry out tasks such as dressing. 10
19 The Middle Cerebral Artery (MCA) arises from the internal carotid artery. Region of Middle Cerebral Artery Permission granted to use image Legend for picture: Anterior cerebral artery-blue Middle cerebral artery- pink Posterior cerebral artery- green The middle cerebral artery is the largest of the major vessels and supplies blood to over 2/3 of the cerebrum. The MCA has 3 branches and passes laterally under the frontal lobe and between the temporal and frontal lobes. The M1 segment is also referred to as lentriculostriate arteries and are located in the deeper sections of the brain called the basal ganglia and most of the internal capsule. 11
20 These lentriculostriate vessels are small vessels located deep in the brain and are also a common site for small vessel or lacunar strokes. The superior branch of the MCA supplies the lateral and inferior frontal lobe and anterior parts of the parietal lobe. The inferior branch of the MCA supplies the lateral temporal lobe, the posterior parietal lobe and the lateral occipital lobe. The Posterior Cerebral Artery (PCA) is responsible for the blood supply for midbrain, hypothalamus and thalamus, posterior medial parietal lobe, corpus callosum, inferior and medial temporal lobe and inferior occipital lobe. Key Functional Areas that receive blood supply from the PCA are: Primary visual cortex in the occipital lobe 3rd cranial nerve in the midbrain Sensory control Hypothalamus-body temperature control, hunger, thirst, hormone release (Antidiuretic hormone) Thalamus-relaying messages to cortex, level of arousal, awareness, pain Communication between the hemispheres Region of Posterior Cerebral Artery Permission granted to use image 12
21 Legend for picture: Anterior Cerebral Artery- blue Middle Cerebral Artery- pink Posterior Cerebral Artery- green Patients who experience a stroke in the Posterior Cerebral Artery may present with symptoms such as problems with recognizing objects, visual disturbances, drooping eyelid, inability to move the eye in, up & out, down & out, difficulty maintaining body temperature, abnormal hormone responses, coma, hyperesthesia Cerebellum The cerebellum has its own major blood vessels which originate from the vertebrobasilar vessels. The 3 cerebellar vessels are: Superior Cerebellar Anterior Inferior Cerebellar Posterior Inferior Cerebellar The major functions of the cerebellum are control of fine motor movement, coordination of muscle groups and maintaining balance and equilibrium. Permission granted to use image 13
22 There are 2 syndromes often seen with cerebellar strokes: 1. Lateral pontine syndrome Involves basilar and anterior inferior cerebellar artery Symptoms: ipsilateral ataxia of arm and leg, contralateral weakness of upper and lower extremities, contralateral hemisensory loss - pain and temperature 2. Lateral Medullary Syndrome (Wallenberg Syndrome) Involves distal and superior medullary artery branches of vertebral artery and the posterior inferior cerebellar artery Symptoms: Ipsilateral sensory loss-face-pain and temperature, ipsilateral ataxia of arm and leg, gait ataxia, nystagmus, nausea and vomiting, vertigo, hoarseness, dysphagia, contrateral hemisensory loss-pain and temperature, horner syndrome (constricted pupil, partial ptosis, loss of hemifacial sweating), hiccoughs Brain Stem The brain stem receives its blood supply from the posterior cerebral artery and the vertebrobasilar vessels. 14
23 The brain stem is divided into 3 major sections: Midbrain: major functions include involvement in vision, hearing, eye movement and body movement Pons: involved in motor control and sensory analysis, level of consciousness, sleep Medulla: responsible for maintaining vital body functions such as breathing and heart rate One of the major structures housed in the brain stem are the cranial nerves. While there are 12 cranial nerves, Cranial nerves 1& ll originate in the frontal lobe and will not be discussed in this section. Cranial nerves lll-xll originate in the brain stem. Patients that experience a stroke in the brain stem will present with symptoms that involve cranial nerve functions such as swallowing, eye movements, facial expression and tongue movements. The brain stem serves an important role as a pathway between the spinal cord and the brain. The afferent and efferent pathways run through the spinal cord and connect with brain centres for interpretation and response to stimuli. The Reticular Activating System originates in the brain stem and is responsible for our wakefulness and attention. It is a very sensitive system that spans the brain and reacts to interruptions in its ability to work. An expanding stroke will interrupt its ability to keep the patient awake, resulting in the patient presenting with a decreased level of consciousness. Patients who experience a brain stem stroke may present with any of the following: Decreased level of consciousness Ipsilateral lower motor neuron facial weakness or sensory loss Contralateral hemiparesis Pupillary changes Hiccoughs, vertigo Bilateral motor findings Diplopia, gaze palsies, intranuclear opthalmoplegia Dysphagia 15
24 Dysarthria Ataxia Collateral Circulation Collateral circulation is an important feature of the brain and for stroke patients. Not all blood vessels have the capability to be able to create collateral circulation. Vessels such as the lenticulostriate vessels are terminal vessels which do not connect with other vessels. Therefore, vessels associated with the lenticulostriate vessels that become occluded will become ischemic. However, there are vessels that can connect or anastomose with other vessels, creating a redundancy that can permit collateral circulation when one vessel is blocked. These vessels include: External and internal carotid via branches of the opthalmic artery Major intracranial vessels via the Circle of Willis Small cortical branches of the anterior cerebral, middle cerebral and posterior cerebral and cerebellar arteries Some stroke may go unnoticed as the collateral circulation has taken over the function of supplying an area of the brain Thanks to the Circle of Willis, by design, the anterior circulation is connected to the posterior circulation 16
25 Ischemic Stroke: Carotid Syndromes The carotid arteries and their branches, the anterior and middle cerebral arteries, form the anterior circulation and the vertebral, basilar, posterior cerebral arteries and their branches form the posterior circulation. Clinical stroke syndromes depend on the area of the cerebral circulation disrupted. Typically, the anterior or carotid circulation stroke syndromes present with symptoms that include sensory or motor deficits aphasia cortical sensory loss apraxia or neglect visual field deficits or retinal ischemia Ischemic Stroke: Vertebrobasilar Syndrome Strokes affecting the posterior circulation or vertebrobasilar system, present with symptoms such as Diplopia Vertigo Coma at onset Crossed sensory loss Bilateral motor signs Isolated field defect Pure motor and sensory deficit Dysarthria Dysphagia Ischemic Stroke: Lacunar Syndromes Makes up 25% of all ischemic strokes Presumed to be occlusion of single small perforating artery Predominantly in the deep white matter, basal ganglia, pons 17
26 Blood vessel: lenticulostriate branches of the Anterior Cerebral and Middle Cerebral Arteries Lacunar infarction results from infarction of one of the lenticulostriate vessels, the penetrating branches of the circle of Willis, the MCA stem, or vertebral or basilar arteries. Type of Syndrome Patient Presentation Pure motor hemiparesis Results from an infarct in the internal capsule or pons Contralateral Hemiparesis of face, arm and leg, dysarthria Contralateral motor hemiparesis with motor aphasia Results from an infarct of the left frontal area with cortical involvement Ataxic hemiparesis Results from an infarct in the pons Hemiparesis of face, arm and leg with inability to speak Paresis of the contralateral leg and side of the face, ataxia of the contralateral leg and arm 18
27 Dysarthria and clumsy hand syndrome Results from an infarct in the pons or internal capsule Pure sensory stroke Results from an infarct in the thalamus Dysarthria, dysphagia, contralateral facial and tongue weakness, paresis and clumsiness of the contralateral arm and hand Contralateral sensory loss to all modalities that usually affect the face, upper and lower extremities May be painful Kistler JP, Ropper AH, Martin JB. Cerebrovascular diseases. In: Isselbacher KJ, Braunwald E, Wilson JD, Martin JB, Fauci AS, Kasper DL, eds. Harrison s Principles of Internal Medicine. 13th ed. New York: McGraw Hill; 1994: Fisher,CM. (1991). Lacunar Syndromes, 1, Ischemic Stroke: Left (dominant) Hemisphere Stroke The CT scan shows a large area of infarction in the territory of the left middle cerebral artery. The MCA is the artery most often occluded in ischemic stroke. 19
28 The associated neurological signs and symptoms form a common pattern of stroke presentation involving the left, or dominant, hemisphere. Aphasia Right field defect Left gaze preference Right upper motor neuron facial weakness Right hemiparesis Right hemisensory loss Ischemic Stroke: Right (non-dominant) Hemisphere Stroke The CT scan shows a large area of infarction in the territory of the right middle cerebral artery. 20
29 The associated neurological signs and symptoms form a common pattern of stroke presentation involving the right, or non-dominant, hemisphere. Left neglect, inattention Left field defect Right gaze preference Left upper motor neuron facial weakness Left hemiparesis Left hemisensory loss, sensory extinction Ischemic Stroke: Cerebellar Infarct The MRI scan shows an area of ischemia in the left cerebellum. This stroke presentation should be considered a neurological emergency because of the possible risk of raised intracranial pressure due to compression of the fourth ventricle. 21
30 The following associated signs and symptoms form a common pattern of stroke presentation involving the cerebellum. Headache, nausea/vomiting Vertigo, imbalance Normal tone, power, reflexes Inability to sit or stand Ataxia or loss of normal coordination Late signs: Decreasing level of consciousness Diplopia, gaze palsy Ipsilateral V, Vll impairment Ischemic Stroke: Brainstem Stroke This MRI scan shows an area of ischemia in the right pons, in the brainstem 22
31 The following associated neurological signs and symptoms form a common pattern of stroke presentation involving the brainstem. Decreased LOC Crossed findings Ipsilateral lower motor neuron facial weakness or sensory loss AND contralateral hemiparesis Pupillary changes Hiccoughs, vertigo Bilateral motor findings Diplopia, gaze palsies, intranuclear opthalmoplegia Dysphagia Dysarthria Ataxia 23
32 The Brain and Function How Stroke Affects Function A stroke is a loss of function that results from the blood supply to the brain being cut off. The following describe how a stroke affects the function of different areas of the brain: Frontal Lobe Arm, opposite side of stroke Leg, opposite side of Frontal stroke Judgment, personality, lobe attention Speaking and writing if stroke is on the dominant side Parietal lobe Parietal Lobe Arm, opposite side of stroke Leg, opposite side of stroke Sensation of touch Visual and sensory perception, if stroke is on the non-dominant side Temporal Lobe Sense of smell Temporal Memory lobe Understanding spoken and written language and math skills if stroke is on the dominant side (part of the Parietal lobe as well) Brain Brainstem Stem Breathing Modulation of temperature and blood pressure Swallowing Cerebellum Cerebellum Coordination Balance Occipital lobe Occipital Lobe Vision Blood Supply and the Brain The Anterior Cerebral Artery supplies blood to the medial (central) parts of the Frontal and Parietal Lobes. The Middle Cerebral Artery supplies blood to the lateral (outer) parts of the Frontal and Parietal Lobes and the Temporal Lobe. The Middle Cerebral Artery is the most common site of stroke. The Posterior Cerebral Artery and Vertebro-Basilar Artery systems supply blood to the Cerebellum, Brain Stem, Occipital Lobe, and the posterior (back) part of the Temporal Lobe. Anterior Cerebral Artery Middle Cerebral Artery Posterior Cerebral Artery Opthalmic Artery Cerebellar Arteries Internal Carotid Artery Basilar Artery Vertebral Artery
33 Module One Pathophysiology of Stroke, Neuroanatomy, Stroke Syndromes REFERENCES The main source for this module was: Acute Stroke Management Resource. (2007). Heart and Stroke Foundation of Ontario, Anatomy and Physiology of Acute Stroke power point presentation. Retrieved from Eng lish.htm That presentation listed the following sources for the content: American Association of Neuroscience Nurses American Stroke Association Brain Attack Coalition Canadian Hypertension Education Program Canadian Stroke Strategy European Stroke Initiative Heart and Stroke Foundation Prof Ed Heart and Stroke Foundation of Canada Internet Stroke Centre National Institute of Neurological Disorders and Stroke
34 Scottish Intercollegiate Guidelines Network StrokeEngine
35 NEO Stroke Network s Nursing Certification Program MODULE ONE Pathophysiology of Stroke Neuroanatomy Stroke Syndromes Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
36 DATE: NAME: 1. The etiology of ischemic stroke can be classified as a. Large vessel b. Small vessel c. Cryptogenic d. all of the above 2. The Cerebrum is made up of all but one of the following structures. Select the structure not part of the cerebrum. a. Temporal lobes b. Occipital lobes c. Parietal lobes d. Superior and inferior cerebellar lobes 3. Hemorrhagic transformation, or secondary bleeding into an infarcted lesion, is often considered to be a natural evolution of an ischemic stroke. It can be serious clinically if there is bleeding beyond the original territory or if mass effect occurs. It is influenced by the a. Size of the stroke b. Location of the stroke c. Etiology of the stroke d. All of the above 4. The three main branches of the Internal Carotid Artery: the Anterior Cerebral Artery (ACA), Middle Cerebral Artery (MCA) and Anterior Communicating Artery together form the a. Posterior circulation b. Circle of Willis c. Anterior circulation d. Cerebellar circulation
37 5. Collateral Circulation can occur because of the: a. Redundancy in our cerebral vasculature b. The Circle of Willis c. Terminal vessels d. Both Answer A and B 6. Small vessel disease causing stroke is thought to be the result of occlusion of single, small penetrating arteries deep in the brain. These strokes are called: a. Cerebellar strokes b. Lacunar strokes c. Cryptogenic strokes d. Arteriovenous malformations 7. Cerebellar infarct may present with all but one of these signs: (Choose the exception) a. Impaired executive functioning; decision making b. Vertigo,imbalance c. Ataxia or loss of normal coordination d. Diplopia 8. The brainstem is responsible for a. Understanding written language b. Perception of the surrounding environment c. Autonomic functions ie. respiration, blood pressure, heart rate d. Thoughts and behaviour TRUE/FALSE Questions (CIRCLE the correct letter) T F 1. The left hemisphere controls the right side of the body AND is most often where the language center is located.
38 T F T F T F T F 2. The cerebellum is responsible for sensation, vision and memory. 3. The middle cerebral artery has a large territory and is most often the artery occluded in stroke. 4. Lacunar syndrome is commonly referred to as a pure motor stroke presenting with contralateral hemiparesis. 5. Tumour or a brain abscess may present like a stroke and is considered to be one of the so-called Stroke Mimics. SCORE: / 13 Stroke Unit/Medical Unit Nurse Clinician/Designate (signature)
39 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE TWO Pre-Hospital and Emergency Management Upon completion of this module, nurses will be able to: State the Warning Signs of Stroke Understand the Role of EMS in Hyperacute Stroke Explain Thrombolytic Therapy - and the importance of quick assessment and administration within the time window Identify Stroke Mimics Understand Acute ASA Therapy Explain the Contributing Factors to Ischemic Damage
40 NEO Stroke Network s Acute Nursing Certification Program MODULE TWO Pre-hospital Care and Emergency Management Self Learning Program NEO Stroke Network Developed April 2010
41 Pre-hospital Care and Emergency Management Warning Signs of Stroke Sudden onset of: Weakness or numbness Speech disturbances Unexplained dizziness Visual changes Sudden severe headache of unknown cause Emergency Medical Services Hyperacute Stroke is defined as the health care activities that take place from the time of first contact between a potential stroke patient and medical care. This period ceases once the patient is either admitted to hospital or discharged back into the community. Patients who show signs and symptoms of hyperacute stroke in the community must be treated as time-sensitive emergency cases and should be transported without delay to the closest institution that provides emergency stroke care. Immediate contact with emergency services by patients or members of the public is strongly recommended because it reduces time to treatment for acute stroke. EMS service dispatchers must triage patients showing signs of hyperacute stroke as a priority dispatch. EMS providers should be using a standardized screening tool. EMS implemented a newly revised Paramedic Prompt Card. The prompt card assists EMS providers in, first, recognizing the signs and symptoms of stroke and second, in decision making around the most appropriate hospital to which to transport the patient. 2
42 Paramedic Bypass Protocols exist in each region whereby the EMS providers will bypass the local community hospital and transport the patient, up to 2 hours in the ambulance, to access a centre equipped to provide optimal acute stroke treatment, and arrive within 3.5 hours from the time of stroke onset. The 2008 Canadian Best Practice Recommendations for Stroke Care also emphasize the need for rapid transport of acute stroke patients to appropriate facilities but unfortunately lack of public awareness of stroke signs and symptoms AND lack of knowledge that stroke is an emergency still exists. PARAMEDIC PROMPT CARD FOR ACUTE STROKE PROTOCOL Indications for Patient Redirect or Transport to a Designated Stroke Centre Redirect or transport to a Designated Stroke Centre will be considered for patients who: Present with a new onset of at least one of the following symptoms suggestive of the onset of an acute ischemic stroke: unilateral arm/leg weakness or drift slurred speech or inappropriate words or mute unilateral facial droop AND Can be transported to arrive at a Designated Stroke Centre within 3.5 hours of a clearly determined time of symptom onset or the time the patient was last seen in a usual state of health. NOTES: 1. A Designated Stroke Centre is a Regional Stroke Centre, District Stroke Centre or Telestroke Centre. 2. Patients will be redirected or transported to the closest Designated Stroke Centre. 3. Patients whose symptoms improve significantly or resolve during transport will continue to a Designated Stroke Centre 4. Out-of-hospital transport will not exceed two hours. Exclusions for Patient Redirect to a Designated Stroke Centre Any of the following conditions exclude a patient from being redirected to a Designated Stroke Centre: CTAS Level 1 and/or uncorrected Airway, Breathing or Circulation problem Patients whose symptoms have resolved prior to paramedic assessment Blood sugar < 3.0mmol/l Seizure at onset of symptoms or observed by paramedic Glasgow Coma Scale <10 CACC will authorize the transport once notified of the patient's need for redirect under the Stroke Protocol. 3
43 Acute Thrombolytic Therapy All patients with disabling acute ischemic stroke who can be treated within 4.5 hours after symptom onset should be evaluated without delay to determine their eligibility for treatment with t-pa (Alteplase). Eligible patients are those who can receive t-pa within 4.5 hours of the onset of stroke symptoms in accordance with criteria adapted from the National Institute of Neurological Disorders and Stroke tpa Stroke Study and Third European Cooperative Acute Stroke Study (ECASS III). The introduction of thrombolytic therapy has provided a proven treatment for acute ischemic stroke patients if given as soon as possible and within the time window. However, it is a high risk treatment that should only be given by personnel trained in its use, in a centre equipped to investigate and monitor patients appropriately. Goal of thrombolytic therapy is to limit irreversible ischemic damage caused by an arterial occlusion. Thrombolysis will promote reperfusion of the viable tissue of the penumbra, improving stroke prognosis and outcome. It is important to note that time is brain and the closer to the time of stroke onset that reperfusion occurs, the better the patient prognosis. What is Tissue Plasminogen Activator (t-pa or Alteplase)? As excerpted from Faaast FAQs for Nurses, page 7, Heart and Stroke Foundation of Ontario (2007)....t-PA (Alteplase) is a thrombotic agent (clot-busting drug) that can destroy an existing blood clot that is approved for use in select patients having an ischemic stroke. It is to be given within the time window of 4.5 hours from last seen normal. Prior to administration of the drug, the patient must undergo specific diagnostic procedures to determine if there is any hemorrhage. This requires immediate access to CT scan imaging and blood work. 4
44 Administration is most often administered intravenously or sometimes intraarterially directly to the site of the clot via catheter, allowing for a greater dose of the drug with fewer potential side effects. What is the usual process prior to a patient receiving t-pa (Alteplase)? Ascertain time of onset (<than 4.5 hours) History and physical symptoms consistent with acute ischemic stroke CT to rule out hemorrhage stroke [or other etiology] CBC, platelets, lytes, glucose, INR, PTT etc Assessment by a Stroke Physician What are the major inclusion criteria for t-pa (Alteplase)? Ischemic stroke Clearly definable time of onset t-pa can be administered within 4.5 hours of symptom onset Symptoms present more than 1 hour without signs of resolution What are some absolute contraindications for t-pa (Alteplase)? TIA or stroke with rapidly improving deficit Hemorrhagic stroke BP>185/110 that does not respond to treatment Major surgery or trauma within 14 days Active internal bleeding or history of hematological abnormality or anticoagulation [this is dependent on INR value which may vary at across centres] Why work quickly to determine if t-pa (Alteplase) is the appropriate treatment? If thrombolysis takes place as soon as possible, the less brain tissue is affected. 5
45 Below you will see the infarcted tissue (ischemic core), the tissue that is still viable but lacking perfusion, therefore, at risk (ischemic penumbra), and the normal brain tissue. Normal brain tissue Brain tissue that is lacking perfusion, at risk of death Infarcted brain tissue NOTE: Our brain requires a constant uninterrupted supply of glucose and oxygen as the brain does not store glucose or oxygen. An interruption in either of these substances can lead to dysfunction. A complete interruption of blood supply to part of the brain for only 30 seconds can alter brain metabolism, for example, neuronal function may cease after 1 minute. After 5 minutes anoxia initiates a chain of events that may lead to death of brain tissue. Penumbra tissue remains viable for several hours after stroke. Penumbra cells are supplied by collateral arteries which contribute to reperfusion and thrombolytic therapy also works to perfuse the penumbra. A stroke patient should receive thrombolytic therapy as soon as possible but within a maximum of 60 minutes of arrival. A rapid and coordinated emergency department response to the arrival of a stroke patient facilitates early diagnosis and treatment. 6
46 The following maximum target times for emergency management of ischemic stroke have been established. Door-to-triage 1 minute Door-to-stroke team notification 5 minutes Door-to-CT scan 25 minutes Door-to-needle 60 minutes (The absolute and relative exclusion criteria for administration of t-pa and the t-pa Order Set are included in the Hospital-Specific Chart Forms section of those packages that are available at District Stroke Centres and Telestroke sites) There are adverse effects of t-pa to be aware of: Hemorrhage a) Superficial Bleeding Observe potential bleeding sites: venous & arterial puncture, lacerations, etc. Avoid invasive procedures during t-pa (Alteplase) and for 24 hours after (incl. N/G and foley catheter) Monitor all secretions for bleeding b) Intracranial hemorrhage Observe for deterioration of neuro status If suspected, stop t-pa (Alteplase) and notify M.D. Obtain CT scan and coagulation workup Angiodema a) Risk assessment Inquire if patient has had angioedema in past Take ACE inhibitor history Although angiotensin II (ATII) receptor antagonists have not been implicated in the angioedema reaction, caution is advised in patients reporting a history of ATII antagonist use 7
47 b) Monitoring Observe for facial, tongue, and/or pharyngeal angioedema 30 minutes, 45 minutes, 60 minutes and 75 minutes after initiation of IV t-pa infusion and periodically for 24 hours afterwards Stroke Mimics Not all cases that appear as a stroke are in fact a stroke. Be aware of the many other conditions that would be part of the differential diagnoses as they can present much like a stroke. Seizure Infection Hypoglycemia Syncope Brain abscess or tumour Drug overdose Head trauma Migraine Bell s palsy Hypertensive encephalopathy Acute ASA Therapy All acute stroke patients should be given at least 160mg of ASA immediately as a one time loading dose after brain imaging has excluded intracranial hemorrhage. [Evidence Level A] (ESO, NZ, RCP, SIGN 13). (Canadian Best practice Recommendations -2008) In patients treated with t-pa (Alteplase), ASA should be delayed until after the 24 hour post-thrombolysis scan has excluded intracranial hemorrhage. ASA ( mg daily) should then be continued indefinitely or until an alternative antithrombotic regime is started. In dysphagic patients, ASA may be given by enteral tube or by rectal suppository The administration of ASA in the hyperacute phase of stroke comes as a result of research that concluded that the administration of ASA within 48 hours of onset of presumed ischemic stroke reduces the risk of early recurrent ischemic stroke without a major risk of early hemorrhagic complications and improves long term outcomes. (Cochrane Database Systematic Review, 2007) 8
48 Goals of Acute Ischemic Stroke Management Reduce or minimize ischemic damage Reduce cerebral edema Prevent secondary complications Determine etiology of stroke Prevent recurrent stroke Facilitate access to rehabilitation and community reintegration Contributing Factors to Ischemic Damage While restoring blood flow to the penumbra is the goal of acute stroke management, there are multiple factors that should be considered and addressed as part of the management plan. Factors that play a role in contributing to potential increase in size of the infarct include: a) Blood pressure b) Blood glucose c) Body temperature d) Oxygen saturation It is important to assess and monitor vital signs to keep this goal at the forefront. from Heart & Stroke: Best Practice Guidelines for Stroke Care Acute Ischemic Stroke receiving t-pa Vital signs (including temperature) should be assessed as follows after beginning t-pa infusion: q 15 minutes for 2 hours q 30 minutes for 2 hours q 1hour for 6 hours q 4 hours for 14 hours 9
49 Acute Ischemic Stroke Non t-pa Vital signs (including temperature) should be assessed as follows: q 1 hour for 24 hours q 4 hours for 24 hours Or as indicated by hospital protocol a) Hypertension (HTN) Acute stroke patients often experience hypertension in the immediate hours after stroke onset. Elevated blood pressure may act as a compensatory mechanism to maintain cerebral perfusion. Normally, cerebral auto regulation maintains cerebral blood flow. However, as cerebral perfusion pressure decreases in the presence of stroke, normal auto regulation is lost and blood flow is dependant on the blood pressure There are many factors that cause hypertension secondary to stroke: full bladder, nausea, pain, pre existing hypertension, anxiety, a physiological response to hypoxia or increased intracranial pressure. The reason for lowering blood pressure is because HTN can increase cerebral edema, increase risk of hemorrhagic transformation, cause further vascular damage and stroke recurrence. There is a concern that reducing blood pressure too quickly and too low may cause neurological damage as a result of reduced perfusion pressure to the ischemic areas. Lowering of the blood pressure can result in serious consequences. Both hypertension and hypotension have been associated with poor patient outcomes. 10
50 For some stroke patients, blood pressure may decline spontaneously within the first few hours as a result of interventions such as moving the patient to a quieter area, emptying the bladder, allowing the patient to rest or controlling pain. Also, the treatment of increased intracranial pressure may result in a lowering of blood pressure. Blood Pressure Reduction BP reduction should be addressed cautiously Measure BP accurately, continuously monitor Clear data is lacking but: 2007 AHA/ASA Guidelines recommend: Initiate treatment if SBP>220mmHg or DBP>120mmHg t-pa candidates: Initiate treatment if SBP>185mmHG or DBP>110mmHG Lower blood pressure by 15-25% within 24 hours Medication selection on case by case basis but consider ability to lower blood pressure quickly but ability for rapid reversal NOTE The HRSRH non-t-pa Order Set adopted these guidelines: Hold antihypertensives x 24 hours unless SBP>220mmHg or DBP>120mmHg *Caution* - avoid rapid lowering of BP. If necessary treat with goal of reduction by ~ 15% within the first 24 hours NOTE Use of sublingual Nifedipine is contraindicated due to its prolonged effect and rapid decline in BP. 11
51 b) Blood Glucose - Hyperglycemia All patients with suspected acute stroke should have their blood glucose concentration checked immediately Blood glucose measurement should be repeated if the first value is abnormal or if the patient is known to have diabetes Markedly elevated blood glucose concentrations should be treated with glucose lowering agents immediately. (CSQCS, Australia) Hyperglycemia is associated with worse stroke outcomes and is also a risk factor for hemorrhagic transformation. It can also have a serious effect on aphasia, hemiparesis, and changes in mental status. It is unclear as to what extent post-stroke hyperglycemia is a normal physiological response or whether hyperglycemia increases cerebral damage. But studies have also shown that hyperglycemia is linked to an increased risk for in-hospital mortality in nondiabetic patients linked to an increased risk of a poor functional recovery Many stroke patients may not have known that they have diabetes (a modifiable risk factor) until admission to hospital. c) Body Temperature - Hyperthermia Increased body temperature (fever) in the setting of acute ischemic stroke is associated with poor neurological outcome (increased risk of morbidity and mortality), possibly secondary to increased metabolic demand, enhanced release of neurotransmitters, and increased free radical production. The source of any fever should be ascertained. The fever may be secondary to a cause of stroke, such as infective endocarditis, or may represent a complication such as pneumonia. (American Stroke Association, 2007) 12
52 d) Oxygen Saturation - Desaturation Ensuring adequate oxygenation of tissues is important in acute stroke management. Oxygen desaturation may exacerbate and worsen ischemic damage. Oxygen saturation should be monitored with the use of pulse oximetry and oxygen applied if oxygen saturation is <92%. (American Heart Association, 2007). Supplemental oxygen given to patients who are not hypoxic may result in the production of oxygen free radicals and contribute to worse outcome. Consideration and assessment of other causes of hypoxia should also be reviewed. These include pneumonia, partial airway obstruction, hypoventilation and atelectasis. Patients who have brain stem infarcts have the greatest risk of airway compromise due to impaired oropharyngeal mobility and loss of reflexes. 13
53 NEO Stroke Network s Acute Nursing Certification Program MODULE TWO Pre-Hospital and Emergency Management QUIZ You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
54 DATE: NAME: 1. List the five warning signs of stroke: 5 points 2. The accepted time window to deliver the drug t-pa to a new stroke patient in our region is: a. 1.5 hours since last seen normal b. 4.5 hours since last seen normal c. 3.5 hours since last seen normal d. Within 24 hours of symptom onset 3. Adverse effects of t-pa to be aware of include: a. Bleeding b. Memory loss c. Angiodema d. Answer A and C 4. List three Stroke Mimics: 3 points 5. The following are contributing factors to ischemic damage except: (Choose the exception) a. blood pressure b. weakness c. oxygen saturation d. body temperature
55 6. All acute stroke patients should be given at least of ASA immediately as a one time loading dose: (fill in the blank) a. 160 mg b. 80 mg c. 325 mg d. 125 mg TRUE/FALSE Questions (CIRCLE the correct letter) T F T F T F 1. There are serious inclusion and exclusion criteria the physician MUST consider before determining if an acute stroke patient qualifies for thrombolytic therapy. 2. Blood Pressure reduction in the acute phase should be addressed cautiously and follow the guidelines of Hold antihypertensives x 24 hours unless SBP>220mmHg or DBP>120mmHg and avoid rapid lowering of BP. 3. Reduction of fever can wait till it has reached 38.5º C or beyond. SCORE: / 15 Stroke Unit/Medical Unit Nurse Clinician/Designate (signature)
56 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE THREE Assessment and Diagnostics Upon completion of this module, nurses will be able to: Describe the Acute Stroke Nursing Assessment Understand why Neurological Assessments are important State the Standardized Neurological Assessments Explain the Relevant Stroke Investigations and why they are being done
57 NEO Stroke Network s Acute Nursing Certification Program MODULE THREE Assessment and Diagnostics Self Learning Program NEO Stroke Network Developed April 2010
58 Acute Care Nursing Assessment Acute stroke patients require skilled and knowledgeable professionals attending to their care. Organized stroke units create the opportunity to develop a critical mass that facilitates the development of expertise of clinicians. Expertise in stroke assessment by clinicians ensures that stroke patients are offered appropriate investigations and receive appropriate and timely care. The nurse is often the first to see changes and early warning signs that may predict a neurological crisis. Familiarity with a stroke nurse assessment promotes the nurse s ability to gather accurate patient information, identify stroke emergencies and promote timely referrals to appropriate specialists and time-dependent investigations (Faaast FAQs, Heart and Stroke Foundation, page 9, 2007) A stroke assessment includes: (Faaast FAQs, page 10, 2007) 1. ABC 2. Health History Begin a general assessment the moment you first encounter the person. Take note any signs of acute distress that are present and assess ABC (airway-breathing-circulation). The purpose of the health history is to collect subjective data and combine it with objective data from the physical examination. The combined data base is then used to make a judgment or diagnosis about the health status of the individual (Jarvis, 2000). 3. Vital Signs Temperature, heart rate, blood pressure, respiration rate, pain assessment and oxygen saturation are all measured/monitored according to Standards of Care for the unit. See frequency as outlined in Module TWO.
59 4. Pupils Record size of the pupils in mm using the pupil scale prior to the application of the light stimulus. Indicate the reaction of pupils as either: + = Brisk Reaction S = Sluggish - = No Reaction If the eyes are closed due to swelling, record C 5. Standardized Neurological Assessment Why do a neuro assessment? Provides a standardized method to rapidly identify emerging stroke complications. Early identification of emerging stroke complications may: lead to early intervention limit the extension of neurological damage impact patient outcomes provide a better patient prognosis (Hachinski & Norris, 1980) The use of standardized and validated stroke assessment tools in both the acute and rehabilitation settings enables sound decision making and care planning. What are you looking for? Symptoms of Change in Neurological Status Restlessness Combativeness Confusion Severe headache Lethargy Decline in motor strength Decrease in coordination Change in balance Change in speech/language (from Faaast FAQS, 2007, HSFO) 3
60 There are three neurological assessment tools that are available for nurses to use: Canadian Neurological Scale, the National Institutes of Health Stroke Scale and the Glasgow Coma Scale (HSFO and RNAO, 2005). Canadian Neurological Scale (CNS): The Canadian Neurological Scale is an assessment tool for evaluating and monitoring the neurological status of acute stoke patients. It has been found to be brief, valid and reliable, and can be administered in approximately 5 minutes. The CNS assesses: level of consciousness orientation speech motor function of the face, arm and legs A limitation of the scale may be that some useful measures are omitted as it does not include assessment of cerebellar or brainstem function. (HSFO and RNAO, 2004) National Institute of Health Stroke Scale (NIHSS): The National Institute of Health Stroke Scale was designed for use in clinical trials and practice to assess stroke severity and degree of recovery. The NIHSS has demonstrated reliability and validity for patients with stroke. It can take up to 20 minutes to administer until you are quite comfortable with each item, then it may be completed in 5-10 minutes. The NIH Stroke Scale (NIHSS) assesses: level of consciousness visual fields motor response sensation language neglect 4
61 It is an 11 item scale that measures various physiological deficits associated with stroke: LOC Limb ataxia Best gaze Sensory Visual field testing Best language Facial paresis Dysarthria Arm & leg motor function Extinction & inattention The NIHSS allows us to: objectively quantify our clinical exam (give it a score) determine if the patients neurological status is improving or deteriorating; provide standardization in assessment (from one nurse to the next the same exam is performed) communicate patient status to staff (nurses and MDs talking the same language) aid in decision making re: t-pa(alteplase) treatment, acute care needs, needs at discharge A limitation of the scale is that it has a low sensitivity to small changes (HSFO and RNAO, 2004). Glascow Coma Scale (GCS): The Glasgow Coma Scale is a standardized and valid neurological assessment tool for assessing level of consciousness or coma. It is a neurological assessment that is widely used by the neurological and neurosurgery community and is found in the curriculum of most undergraduate nursing programs. It lacks specificity and applicability when applied to stroke patients as most do not have impaired LOC. Other Assessments There are many more assessments that are relevant to the stroke inpatient. Some of these assessments are administered by other members of the team. Consult with your Nurse Clinician or Stroke Nurse to learn more about any one of the assessments listed below. 5
62 AlphaFIM (an abbreviated version of the FIM Instrument to assess function and disability in the acute care setting) Pain (Visual Analog Scale) Skin Breakdown (Braden Risk Assessment) Balance (Berg Balance Scale) Cognition (Mini Mental; MoCA) Depression (Beck Depression Inventory) Investigations The following investigations are part of the Acute Ischemic Stroke non t-pa Order Set at Hôpital régional de Sudbury Regional Hospital. Your centre may use a variation of these tests. Check with your Stroke Program s Stroke RN or District Stroke Coordinator. Descriptors for each test were obtained from American Stroke Association s Stroke Tests and Blood tests confirm (or refute) suspicions of specific clinical conditions Levels of cardiac enzymes (including troponin and creatine kinase) can confirm heart muscle damage and extent of damage. Creatinine findings can show reduced renal blood flow, atherosclerosis. Glucose Random Testing indicates blood glucose levels in the blood. PTT/INR Partial Thromboplastin Time indicates the function of all coagulation factors. International Normalized Ratio is a ratio used to monitor the effectiveness of blood thinning drugs such as warfarin (Coumadin). Lipid Profile is a complete fasting lipoprotein profile that will show total blood cholesterol level, HDL, LDL and triglyceride levels. HbA1c is a test that measures the amount of glycated hemoglobin in your blood. Glycated hemoglobin is a substance in red blood cells that is formed when glucose attaches to hemoglobin. It indicates how well blood sugar has been controlled over the previous 2-3 months. HbA1c results can contribute to a diagnosis of diabetes. 6
63 O2 saturation: Monitoring O2 saturation picks up presence of hypoxia which may exacerbate and worsen ischemic damage. If hypoxic, possible causes of respiratory compromise (pneumonia, partial airway obstruction, hypoventilation, and atelectasis) must be considered and managed. Chest XRAY will determine whether the heart is enlarged or if fluid is accumulating in the lungs CT- HEAD is ordered STAT in emergency department to rule out brain hemorrhage or identify other etiologies. The CT Scan may appear normal for several hours after the onset of stroke. In ischemic stroke, a larger infarct may appear as a hypodense area (core) surrounded by area of intermediate density (penumbra). Hypodense area is most commonly seen in hrs. It is necessary to repeat in 2 days. CT Angiogram (Head and Neck) examines blood flow through the arteries in the neck and brain dye is injected into a vein and a series of rapid-image xrays are taken as the dye travels through. Carotid Doppler - ultrasound of carotid arteries to detect blockages. Echocardiogram ECHO - uses ultrasound to show the shape, texture and movement of heart valves, as well as the size of heart chambers and how well they are working. An ECHO may be done to diagnose heart valve problems or identify a cardiac cause of stroke. Electrocardiogram - ECG - is a test to examine a graphic record of the heart's electrical impulses, determining timing and duration of each electrical phase in the heart beat. Result will determine if a heart attack has occurred and monitors for changes in heart rhythm. Holter Hook up (24 and 48 hr) is a 24-hour portable monitor of the electrocardiogram, used to detect heart rhythm abnormalities during daily activities, ruling out atrial fibrillation as a cause of stroke. Optional: TEE Transesophageal echocardiogram an invasive procedure to obtain a more detailed view of the heart structures from the esophagus. EEG Electroencephalogram - Investigates electrical activity in the brain to rule out seizure, using electrodes on the patient s scalp. 7
64 Module Three Diagnostics and Assessments REFERENCES Cote, R., Hachinski, V.C., Shurvell, B.L., Norris, J.W., Wolfson, C., (1986). The Canadian Neurological Scale: A Preliminary Study in Acute Stroke. Stroke, 17(4), DeGraba, TG., Hallenbeck, JM., Pettigrew, KD., Dutka, AJ., & Kelly, BJ. (1999). Progression of Acute Stroke. Value of the initial NIH Stroke Scale Score on Patient Stratification in Future Trials. Stroke, 30, Heart and Stroke Foundation of Ontario, (2003). Heart and Stroke Best Practice Guidelines for Stroke Care. A resource for implementing optimal stroke care. Toronto: Heart and Stroke Foundation of Ontario. Heart and Stroke Foundation of Ontario and Canadian Stroke Network. (2007). Faaast FAQs for Stroke Nurses. Ottawa: Heart and Stroke Foundation of Canada Heart & Stroke Foundation of Canada and Canadian Stroke Network, (2007/2008). Acute Stroke Management Resource. (Power point presentations). Retrieved from Eng lish.htm Lindsay, P., Bayley, M., Hellings, C., Hill, M., Woodbury, E., Phillips, S. (2008). Canadian best practice recommendations for stroke care (Updated 2008). CMAJ, 179 (12 SUPPL): E1-E93. Registered Nurses Association of Ontario, Nursing Best Practice Guidelines. (2005). Stroke Assessment Across the Continuum of Care. Toronto: Registered Nurses Association of Ontario. Schlegel, D., Kolb,SJ., & Kasner, SE. (2003).Utility of the NIH Stroke Scale as a Predictor of Hospital Disposition. Stroke, 34, Web Sources
65 Nationa l_institutes_of_health_stroke_scale_workshop_2008.htm
66 NEO Stroke Network s Acute Nursing Certification Program MODULE THREE Assessment and Diagnostics Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
67 DATE: NAME: 2 points 1. Why is a Neuro exam very important to do on every stroke patient? (Explain) 2. List 4 symptoms that could indicate a change in neurological status. 4 points 3. The GCS assesses: a. Level of consciousness b. Motor recovery c. Balance d. Risk of developing pressure sores 4. The CNS assesses: a. Orientation, speech and motor function b. Orientation, perception c. Cerebellar functioning d. Gait
68 5. NAME 2 other assessments you may use on your stroke inpatient or may hear other team members mention during a Rounds discussion. 2 points 6. Your stroke inpatient s wife Mary has asked you to explain what an Echocardiogram is and why he needs one of those.. Then the daughter Shari asked and what is the Holter Monitor that the doctor said he needs? PICK ONE OF THESE TESTS AND EXPLAIN IT BELOW. 3 points TRUE/FALSE Questions (CIRCLE the correct letter) T F 1. The NIHSS objectively quantifies the clinical exam, giving it a score that can be compared each time one is completed. T F 2. HbA1c is a test that measures levels of cardiac enzymes like troponin. SCORE: / 15 Stroke Unit/Medical Unit Nurse Clinician/designate (signature)
69 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE FOUR Acute Stroke Management Upon completion of this module, nurses will be able to: Understand the Benefits of an Organized Stroke Unit Identify the Professionals within the Acute Team Explain the Common Post-Stroke Complications Identify other Effects of Stroke Understand the Components of Effective Discharge Planning
70 NEO Stroke Network s Acute Nursing Certification Program MODULE FOUR Acute Stroke Management Self Learning Program NEO Stroke Network Developed April 2010
71 Acute Stroke Management Best practice for acute inpatient stroke care is outlined in the 2008 Canadian Best Practice Recommendations for Stroke Care (CMAJ 2008; 179 (12 SUPPL:E1-E93) Recommendation 4.0 Acute inpatient stroke care 4.1 Stroke unit care Patients admitted to hospital because of an acute stroke or transient ischemic attack should be treated in an interdisciplinary stroke unit i) a stroke unit is a specialized, geographically defined hospital unit dedicated to the management of stroke patients ii) the core interdisciplinary team should consist of people with appropriate levels of expertise in medicine, nursing, occupational therapy, physiotherapy, speech language pathology, social work and clinical nutrition additional disciplines may include pharmacy, neuropsychology and recreation therapy Specialized stroke unit care reduces the likelihood of death and disability in men and women with stroke (mild, moderate and severe). Stroke patients are more likely to return home and regain independence than those cared for on traditional hospital wards. ***Evidence suggests that stroke patients treated on acute stroke units have fewer complications, earlier recognition of pneumonia and earlier mobilization and rehabilitation*** Langhorne et al 2002, identified components of stroke unit care to include: Nursing assessments Medical evaluation and diagnostic testing Early assessment of rehabilitation needs Early management policies: early mobilization, prevention of complications, treatment of hypoxia, hyperglycemia, fever and hydration 2
72 Ongoing rehabilitation policies: coordinated interdisciplinary team care, early assessment of needs after discharge excerpt from CMAJ VOL 179(2) Components of acute inpatient care All people admitted to hospital with acute stroke should be assessed by rehab professionals as soon as possible after admission, preferably within the first hours. Rehabilitation is initiated in the acute care setting to enable individuals with impairments, activity limitations and participation restrictions to identify and reach their optimal physical, mental and social functional level. Professionals working within the Acute Care Stroke Team (Excerpted from StrokEngine, roles defined according to Philips et al, 2002) Occupational Therapist: Responsible for the "assessment of personal and domestic care activities; evaluation and treatment of functional impairments related to change in sensorimotor, cognitive and perceptual abilities; prescription of wheelchairs and bathroom appliances; home visits; patient and family education." Physiotherapist: Responsible for the "assessment and treatment of motor functioning, including motor control, strength and physical conditioning; balance, gait and mobility retraining; home and community visits; patient and family education regarding mobility and safety issues." Speech and Language Pathologist: Responsible for the "diagnosis and treatment of acquired communication disturbances; collaborative assessment and management of swallowing disorders; patient and family education. Dietitian: Provides a myriad of services: assessment of nutritional status and requirements; collaborative assessments and management of swallowing disorders, implementation of appropriate diet plans; risk factor modification; patient and family education. Social Worker: Provides services related to "emotional and adjustment counselling for patients and families; assessment of patient, family and community resources 3
73 required to facilitate discharge planning; referral to appropriate community agencies; patient and family education" Pharmacist: Provides "consultation for matters related to drug therapy; patient and family education." Physician: An important member of the interdisciplinary team, the physician provides medical expertise and leadership in the diagnosis and management of the stroke patient and any of their related complications and/or co-morbities. The physician makes decisions around care and as part of the team, determines readiness for discharge. District Stroke Centre/Stroke Program s Stroke Registered Nurse The Stroke Program RN role varies across each District Stroke Centre. In some centres, the Stroke RN facilitates and coordinates the plan of care for all acute stroke and TIA patients that enter the system at the district stroke centre. This includes utilizing recognized stroke assessment tools and ensuring an interdisciplinary team approach is effectively deployed for all patients during their stay. The Stroke RN provides patient and family education with respect to diagnosis, treatment and secondary prevention. The Stroke RN is also involved with staff education regarding implemention of best practices in stroke care. In other centres, the Stroke RN is solely involved in staff orientation on stroke best practice and provides ongoing stroke care education to the district stroke centre staff and the community. All of the Region s Stroke RNs are actively involved in the development and implementation of evidence-based standard orders, algorithms and protocols for acute ischemic stroke and TIA patients. The RN is responsible for identifying and developing solutions for organizational barriers/problems to achieving evidence-based care. The RN is actively involved in committees at both the hospital and community level. There is a Stroke RN working in each of the districts outpatient Secondary Stroke Prevention Clinic triaging all TIA and Stroke patients that come through to assess stroke risk, provide neurological assessments. The nurse works collaboratively with the physician to identify risks and develop risk reduction strategies. 4
74 Post-Stroke Complications (sections excerpted from Faaast FAQs for Stroke Nurses, page 27-44, HSFO, 2007) While frequency and type of complications vary with the severity of neurological and functional deficits, 60% of patients experience some type of complication post-stroke. Hemorrhagic Transformation Hemorrhagic transformation is the bleeding within the infarcted region. It is one of the most serious complications in the immediate time post-admission to acute care. What causes it? Initial vascular obstruction produces ischemia of the distal tissue Affected blood vessels and brain tissue are rendered fragile and injured When the occluding embolus either lyses spontaneously or breaks apart and migrates distally, cerebral blood flow is restored to the "injured or ischemic arterioles and can result in a hemorrhagic or "red infarct" in what had previously been a bloodless field When does it usually occur? 1-2 days after the original infarct What factors are associated with it? Bigger the infarct, the greater the possibility of hemorrhage Richness of collateral circulation Use of anticoagulants and interventional therapy with thrombolytic agents associated with a higher incidence of hemorrhagic transformation What are the signs? Progressive cerebral deterioration including: Headache, vomiting Depressed level of consciousness and neurological signs such as sluggish pupillary response 5
75 Increasing blood pressure Respiratory changes What is the usual treatment? CT scan to diagnose Control blood pressure Avoid use of anticoagulants Surgical removal of clot if possible Cerebral Edema Cerebral edema/pressure, as opposed to hemorrhagic transformation, commonly occurs in large MCA infarcts when profuse quantities of fluid collect in brain tissue due to cellular swelling When is it most likely to occur? 2 3 days after the onset of symptoms What are the signs and symptoms? The earliest sign of an increase in ICP is a change in the patient s level of consciousness (neurological worsening). This can be as subtle as: irritability quietness restlessness change in personality, lethargy headache, dizziness What are the treatments for cerebral edema? Head elevation 30 degrees May require drainage of cerebrospinal fluid Use of Mannitol to reduce increased intracranial pressure (but requires close monitoring, including renal function, urine output, fluid balance, electrolytes) 6
76 Dehydration Patients are at higher risk for dehydration after stroke. The signs to watch for include: Dry mouth/tongue Constipation Hypotension Concentrated urine Weight loss Disorientation Sunken eyes The consequences of dehydration are serious and affect prognosis, overall health and therefore, quality of life: Lethargy Pressure ulcers More falls Bowel obstruction Urinary tract infections Skin breakdown Renal failure Elderly patients in general have a decreased sensation of thirst which will also contribute to potential dehydration. When stroke patients have been placed on a thickened fluids regimen, this adds to the challenge of ensuring adequate hydration is met since often patients refuse or reduce their consumption due to dislike of that consistency or the different taste. The Registered Dietitian on your team should be involved for further management of dehydration and nutrition. Simple ways to help: Have appropriate liquids available to the patient at all times (thin or pre-thickened fluids) Encourage fluid at meals take a sip between bites Offer beverages with snacks Encourage plenty of fluids with medications Follow up with the Speech Language Pathologist to monitor if any texture upgrades are appropriate for those patients on thickened fluids Indications for Enteral Nutrition Support See section on Swallowing, Feeding, Oral Care in this binder 7
77 Seizures What is the risk of seizure post-stroke? Approximately 10% of stroke patients experience a seizure at some time after a stroke In at least 50% of these individuals, seizures do not recur When are seizures most likely to occur? 85% of seizures occur within 72 hours of a stroke. What patients are most at risk? Patients with intracerebral and subarachnoid hemorrhages are at higher risk of seizure Stroke survivors who function independently at 1 month are at very low risk of future seizures Residual motor and sensory deficits make it difficult to detect early symptoms of seizures What are the usual interventions? Standard diagnostic tool is EEG which can demonstrate abnormal focal electric discharge in 30-50% cases after a seizure Anticonvulsants (anti-seizure medication) (ACDs) are generally started in a patient with a typical clinical presentation with or without EEG correlation Patients will need to be re-examined by the Ministry of Transportation to determine driving abilities Deep Venous Thromboembolism (DVT) The concern with a DVT is that it can result in Pulmonary Embolism (PE) development, a blood clot that obstructs blood flow in the pulmonary artery or any of its branches which can be fatal. A high percentage of PE occurs without signs. DVT signs include: Asymmetrical pain, tenderness Swelling Discolouration 8
78 The gold standard diagnostic test is ultrasound. Prevention is the key! Early mobilization and adequate hydration should be encouraged with all acute stroke patients to help prevent venous thromboembolism (2008 Canadian Best Practice Recommendations, CMAJ, Dec 2, 2008, 179 (2)) Those at high risk for development of DVT (unable to move one or both lower limbs or mobilize independently) should be considered for prophylaxis with low molecular weight heparin (with appropriate prophylactic does per agent). There is weak and inconclusive evidence to support the use of external compression stockings for DVT prophylaxis. The use of these stockings as a preventative measure is not highly recommended at this time. (2008 Canadian Best Practice Recommendations, CMAJ, Dec 2, 2008, 179 (2) ) Emotional Lability Other Effects of Stroke Emotional lability is characterized as inappropriate or prolonged emotional responses to a given situation. This may be characterized by anger outbursts or crying outbursts. Although such patients may comment that they do not know why they are crying, for example, they have no control over their emotions. It is important to explain to the family and the patient that this is a common effect of the stroke and to be supportive. Sometimes, directing their attention away from the triggering topic can change the emotional response. Post-Stroke Depression (PSD) Depression, the most common emotional disorder, may affect up to 40% of all patients with stroke. Depression affects every aspect of one's life, such as their body, 9
79 emotions, thoughts and mood. It is much more complex than simply "feeling blue" and is characterized by a persistent and pervasive feeling of sadness or hopelessness. Stroke survivors are most likely to suffer from depression within the first three months post-stroke. Depression is often accompanied by a change in sleep pattern; weight gain or loss and a change in appetite. Other effects are flat affect; increased sensitivity to pain and discomfort; lack of self care. Depression is serious. It is associated with increased rate of mortality. It is a major barrier to full physical and mental recovery from stroke. It may limit energy to fully participate in rehab and Activities of Daily Living (ADL s). It may increase the severity of cognitive impairment and may increase irritability and the appearance of personality changes. Treatment includes: Antidepressant Medication start low and go slow, especially in geriatric population Psychological therapies to assist the patient and family adjust to the loss of function and compromised self-image and self-esteem. At present, not all stroke survivors are routinely screened. There is often little follow-up once they are discharged from hospital. It is important to differentiate from being emotionally labile. Labile patients may be more tearful with visitors but be able to fill their time when they are alone. Labile patients remain motivated to participate in therapies, set goals and try to achieve them. The 2008 Canadian Best Practice Recommendations state all patients with stroke should be screened for depression using a validated tool. Screening should take place at all transition points and whenever clinical presentation indicates (CMAJ, Dec 2, 2008; 179(2) ) How you can help: Observe & listen Play music as it may improve PSD 10
80 Encourage compliance with medication: especially advising how long medication can take to work Educate survivors and family on services available. Involve the physician and social worker on your team The Social Worker on your team can be a valuable source of information for resources, programs/services, support groups, and/or education sessions that should be part of your patient s recovery from depression. The patient and their family can be referred to him/her as required and consult with them any time their involvement would be of value. The Physician and Pharmacist on your team may be involved in determining the correct medication to treat post-stroke depression. Spasticity Spasticity is involuntary muscle tightness and stiffness that can occur after a stroke. It is characterized by exaggerated deep tendon reflexes that interfere with muscular activity, gait, movement, or speech. Spasticity can increase initially but wane down later on, after stroke. (StrokEngine, 2010) What does it look like in the stroke patient? For stroke patients, degree of spasticity can vary from mild muscle stiffness to severe, painful, and uncontrollable muscle spasm and contracture Can be very painful if joint is pulled into abnormal positions Once established, the chronically shortened muscle may develop physical changes such as shortening and contracture that further contribute to muscle stiffness How can spasticity be treated? Therapeutic positioning as recommended by Physiotherapy and Occupational Therapy Regular stretching exercises prescribed by Physiotherapy Muscle relaxants Serial casting for contractures to allow tendons to stretch Local blocking agent that will deliberately impair the transmission between nerve and muscles when the brain sends these abnormal messages of contraction (botulinum toxin) 11
81 Post-Stroke Pain True incidence unknown but relatively common May be associated with upper limb sensory impairment Can be nociceptive (caused by tissue damage or inflammation) or neuropathic (abnormality of the Peripheral Nervous System or Central Nervous System) Treatment for pain includes anti-inflammatories, applying hot or cold therapy under direction of physiotherapist, support with a sling or use of assistive devices, proper positioning in bed and in chair, gentle passive range of motion under direction of physiotherapist or occupational therapist. Incontinence The 2008 Best Practice Recommendations for Stroke Care (CMAJ 2008) states: Continence All stroke patients should be screened for urinary incontinence and retention (with or without overflow), fecal incontinence and constipation Stroke patients with urinary incontinence should be assessed by trained personnel using a structured functional assessment A bladder training program should be implemented in patients who are incontinent of urine A bowel management program should be implemented in stroke patients with persistent constipation or bowel incontinence The facts: 40-60% of stroke patients have urinary incontinence. 25% of incontinent patients will have urinary incontinence at discharge. 15% will have incontinence at 1 year post stroke. Urinary incontinence within 24 hours of a stroke is a predictor of functional disability. The use of indwelling catheters should be avoided. If used, indwelling catheters should be assessed daily and removed as soon as possible. 12
82 Those patients who have suffered a Frontal Lobe Stroke will have: voluntary control of the external sphincter but uninhibited bladder contraction strong urge to void with short/no warning persistent frequency, nocturia, urge incontinence Those patients who have suffered a Hemispheric Stroke will have: Urinary incontinence secondary to immobility and dependency on others rather than direct effects from the stroke Assessment of Incontinence Incontinence history Fluid intake Medical history Medications Functional ability Post residual volume Urine culture Vaginal examination Rectal examination Strategies for Urinary Incontinence (from Faaast FAQs for Stroke Nurses, page 38, 39, HSFO, 2007) Ensure adequate fluid intake ( mls) Assess post void residuals (normal is mls) Review medications Introduce a regular toileting routine Encourage bladder retraining (urge incontinence) Pelvic muscle exercises Kegal s (as taught by specialized RN or PT) Double voiding, Crede maneuver and intermittent catheterization (overflow incontinence) Limit use of dietary bladder irritants 13
83 Bowel Incontinence Bowel incontinence occurs in 30% of stroke patients and 97% regain control within one year. Incontinence may result due to the following: Altered consciousness Cognitive deficits Impaired communication Neurogenic bowel without sensation or control Bowel function risk factor assessment should include mobility, inactivity, adequate fluid and food intake, polypharmacy, etc. All stroke patients should be screened for fecal incontinence A bowel management program should be implemented in stroke patients with persistent constipation or bowel incontinence Establishing a Bowel Program Encourage appropriate fluids, diet, and activity Choose an appropriate rectal stimulant Provide rectal stimulation initially to trigger defecation daily. Select optimal scheduling and positioning. Select appropriate assistive techniques Evaluate medications that promote or inhibit bowel function. 14
84 Visual Deficits Visual field deficits relate to the location of the stroke. Impairments could be: Homonymous Hemianopsia loss of half of the visual field on the same side of each eye due to lesion of optic tract Diplopia double vision Quadrantanopia partial lesion of the optic radiation involving only a portion of the nerve fibers, resulting in blindness in one quarter of the field of both eyes Cortical Blindness complete or severe loss of vision most commonly caused by bilateral occipital lobe infarctions Decreased visual acuity from aging, diabetes, cataracts, not wearing their glasses Visual field testing, as part of the NIHSS assessment, will determine the deficit, if any, that your stroke patient has. NOTE: Observe an experienced colleague perform Visual Field testing on a stroke patient to appreciate the exact method with which to assess impairments accurately. The Occupational Therapist on your team can provide an eye patch if diplopia is an issue and they can further determine your patient s visual field as part of their objective assessments Skin Breakdown Prevention of pressure ulcer development is crucial. The Braden Scale for Predicting Pressure Sore Risk is a commonly utilized tool. The areas assessed include friction/shear; nutrition; sensation; moisture; activity and 15
85 mobility. Individuals with a score of 18 or less are considered to be at risk of developing pressure ulcers. The lower the score, the higher the risk. ( Risk of Fall Falls are very common post-stroke due to a variety of factors including but not limited to balance disturbance, weakness, sensory impairment, neglect and other perceptual impairments, impulsivity and lack of insight into deficits. A coordinated plan must be in place for the team to follow for fall risk reduction in the acute stroke patient. Post-Stroke Fatigue Fatigue is common after a stroke. It is important to schedule in some rest periods each day. Varying levels of fatigue can and will affect functional abilities, for example, the stroke patient may require more assistance with transfers later in the day or after a therapy session. Activities of Daily Living (ADLs) take longer and require more effort than before the stroke so the stroke patient may be fatigued following what used to be a simple task. Communication Disorders Communication post-stroke may be affected depending on the location of the stroke. It may affect the stroke patient s ability to understand; find the right words; get the words out; speak clearly; read and/or write. Dysarthria Difficulty producing clear speech Weakness or reduced coordination of the muscles needed for speech Slurred speech Hoarseness/breathiness Mumbling quality to the voice 16
86 Changes in vocal quality (sounds nasal or stuffy ) Slow rate of speech Apraxia Difficulty planning the movements for speech The person knows what they want to say, however, the brain has difficulty programming the muscle movements necessary to produce the correct sounds Cognitive-communication impairments Aphasia Difficulty: Organizing thoughts Concentrating Remembering Understanding non-verbal communication or humour/sarcasm a language impairment that results from damage to the language-relevant areas of the frontal, temporal and parietal lobes of the brain The resulting language dysfunctions are roughly classified as expressive (Broca's aphasia) or receptive (Wernicke's aphasia). An individual with Broca's aphasia has a partial or total inability to speak or produce spontaneous speech. They often have no difficulty understanding others, however, thoughts and intentions are difficult to express and may be non-fluent in nature. This form of aphasia can also affect written communication. An individual with Wernicke's aphasia has a partial or total inability to understand spoken and sometimes written language. Expression of language may be fluent in nature, but is not comprehensible. 17
87 The symptoms of global aphasia are those of severe Broca's aphasia and Wernicke's aphasia combined. There is an almost total reduction of all aspects of spoken and written language, in expression as well as comprehension. (exerpted from StrokEngine, 2010) Sadly, aphasia can mask a person's intelligence and ability to communicate feelings, thoughts and emotions. (The Aphasia Institute, Canada) Intelligence is not affected when a person has Aphasia!! How can you help to communicate with an aphasic patient? Use short sentences, simple grammar, common vocabulary Speak S-L-O-W-L-Y Use normal tone and loudness Repeat and/or rephrase Give plenty of time to process what you have said Use facial expressions, gestures, and visual cues Ask if the client understands you Write down key words, draw pictures 18
88 Ask yes/no questions Ask closed ended questions (i.e. orange or apple juice?) Ask the person to write down what they said OR They can point to their answer if given a piece of paper with YES NO? The Speech and Language Pathologist on your team can provide you with more resources to help you better communicate with your stroke patient. Don t hesitate to consult them. Neglect Perception is defined as the way we organize, understand and interpret information. Unilateral Spatial Neglect is the failure to orient to, respond or even be aware of information contra-lateral to the side of brain damage, coming from the body or the environment, or from imagining the body or environment, and not due to primary sensory deficit. Right-sided hemispheric lesions in the parietal lobe often result in varying degrees of perceptual impairment. Moderate to severe neglect can significantly affect one s independence: They may: forget to dress/bath left side be unable to dress left side (Dressing Apraxia) lose things in room, bed, etc. forget to turn water taps off not be able to find temperature setting on stove (e.g., 200 = 00) or place their hand on a hot element on the neglected side be unaware of left side of cupboards, fridge not locate all food on tray/plate be unable to read require assistance with mobility as they may not attend to obstacles on left side which increases fall risk, injury 19
89 be at risk of injury while crossing the street Implications of neglect include: longer length of inpatient rehab higher risk of functional worsening at one year follow-up less independence at home after discharge The Occupational Therapist on your team can provide you with more information and can be consulted for assistance with your stroke patient with neglect. In summary, a nursing assessment of the post-stroke patient should always include monitoring for the common post-stroke complications: Hemorrhagic Transformation Dehydration Cerebral Edema Seizures Deep Vein Thrombosis Urinary or Bowel Incontinence Dysphagia Fatigue Spasticity Falls Skin Breakdown Pain Emotional Lability Visual Deficits Perceptual Impairment Post stroke Depression (from Faaast FAQs, page 44, HSFO 2007) Discharge Planning The 2008 Canadian Best Practice Recommendations state that effective discharge planning is essential for the successful reintegration of individuals with stroke into the community 20
90 Effective discharge planning should include: Family and team meetings Care plans Equipment and service needs assessment General education for all patients with stroke or at risk of stroke, and their families and caregivers Post discharge follow up arrangements Liaison with community providers, link to resources Review of patient and caregiver psychosocial and support needs (CMAJ, Dec 2, 2008, 179 (12) ) 21
91 Module Four Acute Stroke Management REFERENCES Adams, HP., Davis, PH., Leira, EC., Chang, K-C.,Bendixen, BH., Clarke, WR., Woolson, RF., 7 Hansen, MD., (1999). Baseline NIH Stroke Scale score strongly predicts outcome after stroke. A Report of the Trial of Org in Acute Stroke Treatment (TOAST). Neurology, 53 (1), ). Heart and Stroke Foundation of Ontario, (2003). Heart and Stroke Best Practice Guidelines for Stroke Care. A resource for implementing optimal stroke care. Toronto: Heart and Stroke Foundation of Ontario. Heart & Stroke Foundation of Canada and Canadian Stroke Network, (2007/2008). Acute Stroke Management resources. (Power point presentation). Retrieved from Eng lish.htm Heart and Stroke Foundation of Canada, Understanding Transient Ischemic Attack (TIA). Ottawa, Canada. Heart and Stroke Foundation of Ontario and Canadian Stroke Network. (2007). Faaast FAQs for Stroke Nurses. Ottawa: Heart and Stroke Foundation of Canada Hôpital régional de Sudbury Regional Hospital. (2005, updated 2010). Standards of Care, 5 South Medical Unit. Retrieved from %20ACUTE%20STROKE%20PATIENTS-update.pdf Registered Nurses Association of Ontario, Nursing Best Practice Guidelines. (2005). Stroke Assessment Across the Continuum of Care. Toronto: Registered Nurses Association of Ontario. Lindsay, P., Bayley, M., Hellings, C., Hill, M., Woodbury, E., Phillips, S. (2008). Canadian best practice recommendations for stroke care (Updated 2008). CMAJ, 179 (12 SUPPL): E1-E93. Web Sources
92 NEO Stroke Network s Acute Nursing Certification Program MODULE FOUR Acute Stroke Management Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
93 DATE: NAME: 2 points 1. Describe two benefits of having an organized stroke unit within a hospital. 2. The incidence of hemorrhagic transformation is more common: a) In small strokes, immediately following the infarct b) In large strokes, 1-2 days after the original infarct c) In large strokes, during the second week d) When a seizure has taken place at the time of the stroke 3. As cerebral edema persists and ICP progresses, a) LOC will decrease b) Pupil dysfunction is observed c) Restlessness and/or irritability d) Complaints of a worsening headache may be noted e) All of the above may happen 4. DVT signs include all but one of the following: a) Discolouration b) swelling c) spasticity d) pain/tenderness
94 5. List 5 ways you can alter the way you interact with your aphasic stroke patient to better facilitate a two-way conversation: 5 points 6. A visual field deficit(s) that you may discover while assessing your stroke patient is: a) Homonymous Hemianopsia b) Diplopia c) Cortical blindness d) All of the above e) Two of the above 7. Mr. McDonald is complaining of a dry mouth and fatigue. His daughter told you he was confused last night when they talked on the phone. His urine is dark with a small amount of blood present. When you take his BP you notice a drop from his usual. Mr. McDonald is most likely: a) Depressed b) Dysarthric c) Perceptually impaired d) Dehydrated
95 TRUE AND FALSE QUESTIONS: (CIRCLE the correct letter) T F T F T F T F T F T F T F T F 1. Progression of hemorrhagic transformation may vary from patients being asymptomatic in some to causing death in others. 2. Incontinence is a predictor of future functional outcome. 3. Diplopia is double vision. 4. Rehabilitation occurs about 2 months after the diagnosis of stroke, once they have stabilized medically. 5. Emotional Lability and Post-Stroke Depression are synonymous 6. Speaking a lot louder can help the aphasic patient understand a question. 7. Acute stroke patients should be assessed by rehab professionals, starting around two weeks after their inpatient admission. 8. It makes no difference to patient care or patient outcomes if stroke patients are located on different units throughout the hospital. SCORE: / 20 Stroke Unit/Medical Unit Nurse Clinician (signature)
96 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE FIVE National Institute for Health Stroke Scale (NIHSS) Training Upon completion of this module, nurses will be able to: Explain why the NIHSS is a Useful Tool Understand How to Perform NIHSS Demonstrate the Proper Method to Perform a Visual Field Assessment Understand the Scoring Methods for this Assessment Describe How and Where to Document the Scores in the Chart Describe When to Communicate Results of NIHSS Relate NIHSS Scores to Patient Outcomes Access the Online NIHSS Training Program Use their Own Pocket Card for Quick Guide for NIHSS
97 MODULE FIVE NIHSS TRAINING AND CERTIFICATION Read the Self Learning Package enclosed Visit nihss-english.training campus.net to watch a free online training video of the NIHSS and be certified in the administration of this neurological exam Practice the NIHSS on stroke patients NIH Stroke Scale pocket cards are also available to assist you in administering each item of the scale. They are produced by the Canadian Stroke Network and are available to order free of charge from the Heart and Stroke Foundation of Ontario (One has been provided for you in this section of the binder) At Sudbury Regional Hospital, an added process is in place for full NIHSS certification: Be observed performing two NIHSS assessments on stroke patients by a Stroke RN. Two observation opportunities are arranged between the Staff Nurse and the Stroke Program Registered Nurse before full certification is achieved in the use of NIHSS.
98 Use of the NIH Stroke Scale December 2007
99
100 What is the NIHSS and why do we need it? Standardized stroke severity scale to describe neurological deficits in acute stroke patients Allows us to: quantify our clinical exam; determine if the patients neurological status is improving or deteriorating; provide for standardization; and communicate patient status NIHSS is a validated tool that allows clinicians to: Objectively quantify the clinical exam (both for determination of the use of tpa and in the acute phase) determine if the patients neurological status is improving or deteriorating; provide standardization in assessment; (from one person to the next same thorough exam performed) and communicate patient status: (nurses and MDS talking the same language) Elements of the NIH Stroke Scale 11 item scoring system Integrates components of neurological exam Includes testing of LOC, select cranial nerves, motor, sensory, cerebellar function, language,inattention(neglect) Maximum score: 42, minimum score: 0 Not a linear scale
101 NIHSS Guiding Principles 1. The most reproducible response is generally the first response 2. Do not coach patients unless specified in the instructions 3. Some items are scored only if definitely present 4. Record what the patient does not what you think the patient can do Performing and Scoring the NIHSS Instructions Scoring 1a. Level of Consciousness 0 = Alert; keenly responsive The investigator must choose a response. A 3 is scored only if the patient makes no movement (other than reflexive posturing) in response to noxious stimulation. 1 = Not alert, but arousable by minor stimulation to obey, answer, or respond 2 = Not alert, requires repeated stimulation to attend, or is obtunded and requires strong or painful stimulation to make movements 3 = Responds only with reflex motor or autonomic effects or totally unresponsive, flaccid There are two components to this exam: 1. Performing 2. Scoring
102 Scoring: Level of Consciousness (0-3) 0 -Alert, keenly, responsive 1 -Not alert, but arousable by minor stimulation 2 -Not alert, requires repeated stimulation to attend, or painful stimulation to make movements 3 -Responds only with reflex motor or autonomic effects or totally unresponsive If the patient scores 2 or 3,use the Glasgow Coma Scale to assist the neurological examination. Item 1a) LOC is scored from 0 to 3 depending on the patients response Patients scoring a 0 or 1 will NOT be examined using the GCS. The GCS is not an appropriate tool for use with alert, or mildly non-alert patients. You will complete the NIHSS with these patients and any other testing you deem necessary. Patients scoring a 2 or 3 will continue to be examined by nursing staff using the Glasgow Coma Scale and any other relevant neurological tests you are able to use given the patients individual situation. Item 1a. Level of Consciousness Determined through interactions with the patient Auditory stimulation (normal loud voice) Tactile stimulation (light painful) Item 1a) Level of Consciousness: LOC is determined by a three-part assessment (1a, 1b, 1c). Remember not to coach the patient This is determined through interactions with the patient Stimulation should begin with verbal cues, touching or patting lightly Application of pain should only be used if the patient does not respond to verbal stimuli or touch Comment: LOC is the earliest and most sensitive index of change in neurological status Changes in LOC can happen rapidly (minutes), or very slowly, hours, days, or weeks
103 Item 1b. LOC Questions Ask the patient their age wait for a response Ask the patient the current month wait for a response Note: Do not give credit for being close Do not coach or give non verbal cues Item 1b) LOC Questions: If the patient states their date of birth, this is scored as incorrect. The patients response to other questions such as year or place are not used to determine a score on this question. Only the month and pt s age are scored. It is important that only the initial answer be graded and that the examiner not "help" the patient with verbal or non-verbal cues Scoring: LOC Questions (0-2) 0 -Answers both questions correctly 1 -Answers one question correctly 2 -Answers neither question correctly Note: Aphasic patients who do not comprehend the questions will score 2 Patients unable to speak due to endotracheal intubation, orotracheal trauma, severe dysarthria from any cause, language barrier or any other problem not secondary to aphasia are given a 1
104 Item 1c. LOC Commands Ask patient: open & close your eyes and grip and release the nonparetic hand. Give credit if an unequivocal attempt is made but not completed due to weakness If the patient does not respond to command, the task should be demonstrated Item lc) LOC Commands: The patient is asked to: "open your eyes... now close your eyes" and then "Make a fist... now open your hand". (Use the nonparetic hand). Substitute another one step command if the hands cannot be used (i.e. Stick out your tongue or Raise your eyebrows ). Scoring: LOC Commands (0-2) 0 -Performs both tasks correctly 1 -Performs one task correctly 2 -Performs neither task correctly Note: Score only the first attempt
105 Item 2: Best Gaze Ask the patient to "follow my finger" across horizontal eye movements. Aphasic or confused patients: use tracking Unconscious patients: use oculocephalic maneuver OK to coach Item 2: Best Gaze Gaze is the act of focusing the eyes in a particular direction. Observe and score only horizontal eye movements (CNIII, VI). Voluntary or reflexive (oculocephalic) eye movements will be scored but caloric testing is not done. Patients with ocular trauma, bandages, pre-existing blindness or other disorder of visual acuity or fields should be tested with reflexive movements and a choice made by the investigator. This item is an exception to the rules of using the first observable response and not coaching. You can coach the pt, and use the best response as the score. In the patient who fails voluntary gaze, the oculocephalic maneuver and tracking are used to provide stronger testing stimuli. Item 2: Gaze Testing Tracking: establishing eye contact and moving about the patient from side to side and observing if the patients eyes follow The oculocephalic reflex:(doll s eyes) assessed by briskly rotating the patient s head side to side. Note: Normal response: eyes move in the opposite direction to head movement. Abnormal response: the eyes are fixed in one position and follow the direction of passive rotation. When the head is rotated laterally in a patient with intact brainstem function, the eyes should move in a direction opposite to the movement of the head. Absence of the response may indicate brainstem dysfunction. Presence of an intact horizontal oculocephalic reflex verifies intact ocular motor nerves (III, VI) and brain-stem gaze centers. Scoring: Best Gaze (0-2) 0 -Normal horizontal eye movements 1 -Partial gaze palsy abnormality in one or both eyes, but forced deviation is not present 2 - Forced deviation, or total gaze paresis (not overcome with oculocephalic maneuver) If the patient has a conjugate deviation of the eyes that can be overcome by voluntary or reflexive activity, the score will be 1. If a patient has an isolated peripheral nerve paresis (CN III, IV or VI) score a 1. Use voluntary or reflexive stimuli and record a score of 1 if abnormal finding in one or both eyes. Score = 2 reserved for forced eye deviation not overcome by the oculocephalic maneuver
106 Item 3: Visual Fields Stand 2 feet from patient at eye level. Both examiner and patient cover one eye. Ask patient to look directly into your eyes. Test upper and lower visual fields by confrontation (4 quadrants of each eye). Examiner compares this to the norm ( their own vision) To test both fields with eyes open, ask pt to indicate where they see movement (choices: L side, the R side or both) Item 3: Visual Fields Visual fields are tested using finger counting or movement to confrontation and evaluate upper and lower quadrants separately. Each eye is evaluated independently, and 4 quadrants are tested with each eye. You may ask the patient to tell you when they see the moving fingers or the number of fingers they see. Double simultaneous stimulation is performed at this point. Double simultaneous stimulation gives us information about neglect (referred to as extinction and inattention in the NIHSS). Despite the fact that a patient may be able to see the L side of their visual field, they may neglect (or not attend) this area. **You have seen this is patients who do not eat from half of their plate of food. This can be performed as part of the visual field testing or as part of #11 Extinction and Inattention For this test, test both eyes simultaneously and ask the pt to identify if they see your fingers wiggling on the L side, the R side or both. Here, you only need to test upper and lower areas temporally. These test only reveals gross deficits. Ophthalmologists can perform a more detailed screening when deficits are noted.
107 Scoring: Visual (0-3) 0 No visual loss 1 Partial hemianopia (sector or quadrantanopia) 2 Complete hemianopia 3 Bilateral hemianopia (blind) Note: If patient sees the moving fingers, this can be scored as normal If there is unilateral blindness or enucleation, score visual fields in the other eye If there is extinction during double simultaneous stimulation score a 1 and use the results to answer question 11. DEFINITION: Hemi (half) anopia (sightless) Partial: Part of half (sector, quadrant) Complete: All of half (homonymous hemianopia) Bilateral: Both sides of half (blind)
108 Visual Deficits /visual_impairment_effects_vision.asp Visual deficits are common in stroke patients because the visual pathways run through much of the cerebral hemispheres. 1. Blindness R eye seen with lesion of R optic nerve 2. Bitemporal hemianopia (rare in stroke) common with pituitary tumor (lesion at optic chiasm). Pt experiences narrowing peripheral vision. 3. Homonymous hemianopia lesion of optic tract therefore visual loss on the same side (half of each eye) 4. Quadrantic deficit partial lesion of the optic radiation involving only a portion of the nerve fibers Cortical blindness with complete or severe loss of vision is most commonly caused by bilateral occipital lobe infarctions Understanding visual deficits provide important information for safety and perceptual risk assessment. The care plan can be modified to reflect appropriate interventions to accommodate for pt safety concerns and the need for modified care-giving. Ie. Approach pt from the side they can see you coming from, present teaching materials where the pt can see them etc.
109 Item 4: Facial Palsy Ask the patient or use pantomime Show me your teeth, raise your eyebrows and close your eyes tightly Score symmetry of grimace to noxious stimulation in the aphasic or confused patient (tickle each nasal passage one at a time using a cotton-tipped applicator and observe facial movement). Item 4: Facial Palsy Measures facial symmetry Ask, or use pantomime to encourage the patient to "Show me your teeth... now raise your eyebrows... now close your eyes tightly". Lower face: Smile and show your teeth/gums: Observe for flat nasolabial fold or lower facial paralysis (TIP count teeth bilaterally to look for symmetry) Upper face: Lift your eyebrows: Observe wrinkling of forehead Close your eyes tightly: Observe weakness of the eyelid Score symmetry of grimace in response to noxious stimuli in the poorly responsive, confused or non-comprehending patient (tickle each nasal passage one at a time using a cotton-tipped applicator and observe facial movement).
110 Scoring: Facial Palsy (0-3) 0 -Normal symmetrical movement 1 -Minor paralysis: (ie: flattened nasolabial fold, asymmetry on smiling) 2 -Partial paralysis (total or near total paralysis of lower face) 3 -Complete paralysis of one or both sides (absence of facial movement in the upper and lower face) Note: Aphasic or confused patient: Score symmetry of grimace to noxious stimulation Normal function must be clearly demonstrated to obtain the score of 0. Anything in between, including flattened nasolabial fold, is scored a 1. The severely obtunded or comatose patient; patients with bilateral paresis, patients with unilateral upper and lower facial weakness would receive a score of 3. Facial Palsy in Stroke
111 Items 5 & 6: Motor Arm and Leg Test each limb independently Start with non-paretic arm Place the limb in the appropriate position: extend the arm (palm down) 90 sitting/45 supine the leg 30 degrees (supine) Drift =arm falls before 10 sec. or leg before 5 sec. DIP vs DRIFT: Dip: very small change with instantaneous correction. Drift :the limb lowers to any significant degree. Drift is never normal. COUNT OUT LOUD & using your fingers in patients view. Aphasic patient: Use urgency in voice and pantomime to encourage Items 5 & 6: Motor Arm and Leg ARMS: Do NOT test both limbs simultaneously. The limb is placed in the appropriate position: Extend the arm (palm down) 90 degrees (if sitting) or 45 degrees (if supine) *NOTE: For the purpose of the NIHSS, drift is assessed with palms facing down Drift is scored if: the arm falls before 10 seconds or the leg before 5 seconds. Do not coach the patient verbally. LEGS: Extend the leg out at 30 degrees (always tested supine). COUNT OUT LOUD in a strong voice and indicate count using your fingers in full view of the patient. Begin counting the instant you release the limb. You can stop counting when the pts arm or leg touches the bed. The aphasic patient is encouraged using urgency in the voice and pantomime but not noxious stimulation.
112 Scoring: Motor Arm and Leg (0-4,X) 0 -No Drift limb holds steady for full count 10 sec-arm, 5 sec-leg 1 -Drift BUT limb does not hit bed or other support 2 -Drifts towards bed, BUT pt has some effort against gravity 3 -Limb falls, NO effort against gravity. Trace muscular contraction present in limb 4 -No movement X -Amputation, joint fusion The score of 3 is reserved for the patient who exhibits no strength against gravity, but does minimally move the limb on command when it is resting on the bed. A shoulder shrug, hip flexion, or ability to demonstrate muscular contraction are all considered movement. For a score of 4, the pt demonstrates no movement whatsoever. Item 5 & 6: Motor Arm and Leg *Arm tested in pronated position Used with permission from Southeast Toronto Stroke Region Note: arm is tested with the palm downwards, unlike the supine position used for testing pronator drift.
113 Item 7: Limb Ataxia Finger-Nose-Finger & Heel to Shin Item 7: Limb Ataxia This item is aimed at finding evidence of a unilateral cerebellar lesion. There are 2 tests used: Finger-Nose-Finger and Heel to Shin Finger-Nose-Finger: The examiner raises their finger to a distance of 2 ft from the patient (central-midface). It is not necessary for the examiner to move positions (as seen in some of the video footage). The patient is asked With your right hand, touch my finger, then touch your nose; do this as fast as you can. Repeat with the other arm. Heel to Shin: Pt can be lying on their back or sitting. Ask them to slide one heel down the shin of the opposite leg, then repeat the same procedure on the other side. DYSMETRIA is the inability to control accurately the range of movement in muscle action with the resultant overshooting of the mark. Especially of hand movement.
114 Item 7: Limb Ataxia Finger-Nose-Finger & Heel to Shin Finger-Nose-Finger: The examiner raises their finger midline,2 ft from the patient. The patient is asked With your right hand, touch my finger, then touch your nose; do this as fast as you can. Repeat with the other arm. Heel to Shin: Pt can be lying on their back or sitting. Ask pt to slide one heel down the shin of the opposite leg, then repeat the same procedure on the other side. Dysmetria: the inability to accurately control the range of movement in muscle action with the resultant overshooting of the mark. Item 7: Limb Ataxia Detects unilateral cerebellar lesion & limb movement abnormalities in relation to sensory or motor dysfunction Use finger-nose-finger and heel to shin tests Test non-paretic side first Look for smooth, accurate movements Consider limb weakness when looking for dysmetria Non verbal cues are permitted Test all four limbs separately Item 7: Limb Ataxia Test with eyes open. In case of visual defect, ensure testing is done in the intact visual field. Test non-paretic side first. Look for smooth, accurate movements. Consider limb weakness when looking for dysmetria. The finger-nose-finger and heel-shin tests are performed on both sides, and ataxia is scored only if present out of proportion to weakness. The aphasic patient will often perform the test normally if first the limb is passively moved by the examiner. Otherwise the item is scored 0 for absent ataxia. In case of blindness, test by touching nose from extended arm position.
115 Scoring: Limb Ataxia (0-2, X) 0 -Absent 1 -Present in one limb 2 -Present in two limbs Note: Ataxia is only scored if present. In a patient who can not understand the exam or who is paralyzed, a score of 0 (absent) is given. If the patient suffers mild ataxia, and you cannot be certain that it is out of proportion to demonstrated weakness, give a score of 0. Ataxia must be clearly present out of proportion to any weakness. Remember this is scored only when ataxia is present. Score: 0 - Ataxia is absent OR the patient too weak or unable to follow commands and therefore you can not demonstrate it is present. 1 - Present in one limb 2 - Present in two limbs
116 Item 8: Sensory Use a sharp object on face, arms (not hands), trunk, and legs Compare pinprick in same location on both sides. Ask the patient if they can feel the pinprick, if it is different from side to side, and how it is different Record grimace or withdrawal from noxious stimulus in obtunded or aphasic patients Only record sensory loss due to stroke Only record sensory loss if it is clearly demonstrated Item 8: Sensory Test the ability to perceive a pin prick (lightly apply sharp point to the area being tested) You can use a tongue depressor that has been broken lengthwise. Compare sides in the same location on both sides asking the following: pt if they can feel the pinprick. Is it the same or different? If different, How is it different? Only sensory loss attributed to stroke is scored as abnormal. Other sensory loss should have been identified earlier in medical history Only record sensory loss if it is clearly demonstrated Do not test hands and feet as an unrelated neuropathy may be present. Do not test through clothing. Record grimace or withdrawal from noxious stimulus in obtunded or aphasic pts: Use pin prick, If no response, nail bed pressure. Scoring: Sensory (0-2) 0 -Normal, no sensory loss 1 -Mild to moderate sensory loss; patient is aware of being touched but pinprick is less sharp/dull on the affected side 2 -Severe to total sensory loss; patient is not aware of being touched in the face, arm and leg Note: A score of 2 should only be given when severe or total loss of sensation can be clearly demonstrated. Stuporous and aphasic patients will probably score 1 or 0.
117 Item 9: Best Language Incorporates information collected in preceding sections Ask patient to perform the following: name all the objects on the card read all the sentences describe what is happening in the picture Give patient adequate time Patient can write answers If visual loss prevents standard examination: place objects in patient s hand (naming), ask patient to repeat sentences on the card ask patient to produce speech by asking a question Item 9: Best Language A lot of information about comprehension will be obtained during the preceding sections of the examination. You may be tempted to base your score on previous interactions, however it is important to use the attached picture and naming sheet to confirm your impression. It is common to find unexpected difficulties when the formal testing is done, and therefore every patient must be tested with the picture, naming sheet, and sentences. Have the patient name all items on the naming sheet and read all phrases on the two reading sheets. Comprehension is judged from responses as well as to all of the commands in the preceding general neurological exam. **This item is an exception to the rule that the first response is used, since several different tools are used to assess language. For a patient with aphasia or other barrier preventing speech: they should be encouraged to write their responses to the naming items or picture description. Acceptable variations in picture description: leaf/flower for feather, glove/hand, cactus/plant,hammock,. These items are not common in some cultures. Scoring: Best Language (0-3) 0 -No aphasia, normal fluency and comprehension 1 -Mild to mod aphasia some obvious loss of fluency or comprehension, but able to get their ideas across 2 -Severe aphasia all communication limited, examiner must guess what the pt is trying to communicate 3 -Mute, global aphasia- no useable speech, no auditory comprehension. Pt unable to follow any one step commands. Note: To choose between a score of 1 or 2, use all provided materials; it is anticipated that a patient who missed more than two thirds of the naming objects and sentences or who followed only few and simple one step commands would score a 2. If the patient makes one error in naming, or a mild error reading the sentences provided, you may still choose to give them a score of 0 (normal) based on all the other testing you have done. A score of one would be for a patient with obvious loss of fluency or comprehension. A score of 3 should be used only if the patient is mute and follows no one step commands.
118 Item 10: Dysarthria An adequate sample of speech must be obtained by asking patient to read or repeat words from the attached list even if patient is thought to be normal. If the patient has aphasia, the clarity of articulation of spontaneous speech can be rated. Even if the patient is thought to have normal articulation, an adequate sample of speech must be obtained by asking patient to read or repeat words from the attached list. Do not tell the pt that you are testing clarity of speech. It is common to find slurring of one or more words in patients one might otherwise score as normal. Scoring: Dysarthria (0-2, X) 0 -Normal 1 -Mild to moderate; patient slurs some words but can be understood 2 -Severe; patient s speech is so slurred/unintelligible in the absence of or out of proportion to any dysphasia, or is mute. X -Intubated or other physical barrier
119 Item 11: Extinction & Inattention (Neglect) Sufficient information to identify neglect may be obtained during prior testing. If the patient has a severe visual loss preventing visual double simultaneous stimulation, and the cutaneous stimuli are normal, the score is normal. If the patient has aphasia but does appear to attend to both sides, the score is normal. The presence of visual spatial neglect or anosognosia may also be taken as evidence of abnormality. Since the abnormality is scored only if present, the item is never untestable. Item 11: Extinction and inattention DEMONSTRATE BILATERAL CUTANEOUS AND VISUAL STIMULATION Sufficient information may be obtained during the prior testing. (From the picture description and double simultaneous stimulation of both cutaneous and visual senses). when you asked the patient to describe what is going on in the standard picture, did they exclude any portion? Examined by pt s ability to recognize simultaneous cutaneous sensory and visual stimuli from R & L sides Encourage pt to scan both sides of the picture Test bilateral simultaneous visual fields by asking pt to say if L, R, or both of examiners fingers are moving when doing visual exam Test recognition of bilateral simultaneous touch to upper and lower limbs (pt s eyes closed) If the patient has a severe visual loss preventing visual double simultaneous stimulation, and the cutaneous stimuli are normal, the score is normal. If the patient has aphasia but does appear to attend to both sides, the score is normal. The presence of visual spatial neglect or anosognosia may also be taken as evidence of abnormality. Since the abnormality is scored only if present, the item is never untestable.
120 Scoring: Extinction & Inattention (Neglect) (0-2) 0 -No abnormality 1 -Visual, tactile, auditory, spatial, or personal inattention or extinction to bilateral simultaneous stimulation in one of the sensory modalities. 2 -Profound hemi-inattention or hemi-inattention to more than one modality. Does not recognize own hand or orients to only one side of space Anosognosia is the inability to recognize, denial of, or unawareness of a defect in physical function It involves denial, lack of insight, understanding, concern, or awareness Patient may fail to use or look at the involved side of the body without being reminded Patient may not recognize own hand
121 NIHSS and Patient Outcomes Total scores range from 0-42 with higher values representing more severe infarcts. >25 Very severe neurological impairment Severe impairment 5-14 Moderately severe impairment <5 Mild impairment Adams, HP, et al. (1999). Neurology: 53: A 2-point (or greater) increase on the NIHSS administered serially indicates stroke progression. It is advisable to report this increase. While a 2 point or greater increase on the NIHSS administered serially was used to indicate stroke progression in this study, smaller changes can be equally significant. Some of the literature suggests a 2 point increase and also a 3 point increase as a measure to indicate stroke progression. A change of 1 point in Motor Arm or Leg assessment can be very concerning. A change in score of 1 where the patient previously scored 0 may indicate a NEW deficit. Likewise, subtle changes in LOC may lead you to discover other changes. Always use your own judgment! Communicating NIHSS results The total NIHSS score is an important piece of information to relate patient status but it is important include the score with a full assessment of the patient. Communicate the following which neurological area has changed, how it has changed, and any other new findings (vital signs, pupils, cranial nerve deficits, mental status etc) Document your assessment, interventions plans, and follow-up. Communication of the NIHSS score results is essential and should include the total score and changes identifying neurological status. When using the NIHSS as part of an assessment, the total score is important to communicate but so are the areas in which we see the changes.
122 Possible points: Summary LOC 7 Cranial Nerves (Portions of CN II,III,V,VI,VII) 8 Motor 8x2 = 16 Ataxia 2 Sensory 2 Language 5 Inattention 2 NIHSS total =42 Adapted from presentation by Dr. Edward Sloan The majority of points come from the top 4 items listed here. Not surprisingly, many incidences of neurological decline are first recognized by decreases in LOC, motor strength, or Cranial Nerve palsies. Examiners need to keep in mind the area of neurological involvement based on the affected cerebral vessel or lesion. NIHSS and Patient Outcomes Total scores range from 0-42 with higher values representing more severe infarcts. >25 Very severe neurological impairment Severe impairment 5-14 Moderately severe impairment <5 Mild impairment Adams, HP, et al. (1999). Neurology: 53: A 2-point (or greater) increase on the NIHSS administered serially indicates stroke progression. It is advisable to report this increase. These NIHSS score results from 3 studies found the following results that correlated to patient outcomes. DeGraba et al, 1999, found that a score greater than 7 demonstrated a worsening of patient status of up to 65.9% Schlegel et al, 2003, found that patients with scores less than 5 were likely to be able to be discharged home, scores of 6-13 were strongly associated with patients being able to go to rehabilitation and scores greater than 13 were associated with a greater likelihood of the patient being discharged to a nursing home. Adams et al, 2003, found that patients with an NIHSS score greater than 20 had a 17% likelihood of experiencing an intracranial hemorrhage, whereas a patient with an NIHSS score of less than 20, had only a 3% likelihood of experiencing an intracranial hemorrhage.
123 When to communicate NIHSS results Neurological decline NEW focal deficit Advancing neurological deficit Other concern Early changes in the LOC are sensed by the RAS and can be demonstrated by such behaviors as : restlessness, agitation, subtle behavioral changes. These are usually picked up by family of staff who have gotten to know the patient well and note he is just different. To ensure we do not miss a decline in the Reticular Activating System (RAS), particularly as a result of an evolving stroke or new stroke, it is important to listen to subtle changes as noted by other team members of family.i.e.: he s just not right.different from last night when I saw him. Important Points: If patient is not co-operative: explanation must be clearly written on the form. NIHSS items are rarely untestable.
124 Documentation NIHSS Flowsheet As indicated the full assessment is required: 1) To be done q4h x 48 hours after admission for stroke, then q shift x 3 days 2) With any decline in neurological status 3) When the patient is received from ER, ICU, or other in patient units 4) Prior to discharge. TOTAL SCORE is always calculated for the full assessment On-Line NIHSS Certification On-line NIHSS Certification is available free through the American Stroke Association. The on-line program provides detailed instructions and demonstration scenarios for practice in scoring the NIHSS. Certification is completed by scoring different patient scenarios.
125
126 National Institutes of Health Stroke Scale Workshop The Stroke Survivor with Aphasia There are several places throughout the NIH Stroke Scale booklet, where exceptions to the general rules or creative adaptations are made to the assessment of patients with problems expressing or receiving information. This document was designed to place all this information on one page for ease of understanding when using the NIHSS with the stroke survivor with aphasia. The differences in the overall NIHSS are highlighted below: Item 1a: Level of Consciousness No difference in the exam. 1b. LOC Questions Aphasic and stuporous patients who do not comprehend the questions will score 2 (answers neither question correctly). Patients may write their response. 1c. LOC Commands If the patient does not respond to command, the task should be demonstrated to them (pantomime). Item 2: Best Gaze Gaze is testable in all aphasic patients. Establish eye contact and move about the bed with patients who are aphasic or confused. Can coach and use best response as score. In the patient who fails voluntary gaze, use oculocephalic maneuver and tracking of examiner s face to provide stronger testing stimuli. Item 3: Visual If introducing your finger into visual quadrants as usual, the aphasic patient can be asked: Point towards my hand when you see my fingers move. If patient looks at the side of the moving fingers appropriately, this can be scored as normal.
127 If using visual threat: Test each eye independently x 4 quadrants (Upper and lower nasal side & temporal side). Use a single finger briskly introduced into the visual field to see if a blink response is elicited (Using an entire hand may result in a breeze that may cause reflexive blinking). Item 4: Facial Palsy Ask and use pantomime to encourage. "Show me your teeth... now raise your eyebrows... now close your eyes tightly". Score symmetry of grimace to noxious stimulation (such as tickling each nasal passage with a cotton applicator tip) in the aphasic or confused patient. Items 5 & 6: Motor Arm and Leg Place the patient s arm or leg in the desired starting position. Encourage the patient using urgency in the voice and pantomime but not noxious stimulation. Count OUT LOUD in a strong voice and indicate count using your fingers in full view of the patient. Item 7: Limb Ataxia Non verbal cues are permitted. The patient will often perform the test normally if first the limb is passively moved by the examiner. Ataxia is only scored if present. In a patient who cannot understand the exam or who is paralyzed, a score of 0 (absent) is given. If the weak patient suffers mild ataxia and you cannot be certain that it is out of proportion to the weakness, give a score of 0. Remember this is scored positive only when ataxia is present. Item 8: Sensory If the patient has some ability to express themselves, for example, Yes/No, shaking or nodding head, or pointing to the limb touched: Ask: Can you feel the pin prick Is it the same or different? Which side is different? etc. Record grimace or withdrawal from noxious stimulus in patients who are obtunded or have aphasia (only if no response is demonstrated with the safety pin). Only record sensory loss if it is clearly demonstrated. Patients with aphasia often score 0 or 1 (since clearly demonstrating severe or total sensory loss may be very difficult). NIHSS and Aphasia,
128 Item 9: Best Language This portion of the exam is complimented by information collected in preceding sections. Encourage patient to write their responses to the naming items or picture description. Score Tips : 0 = No aphasia, normal fluency and comprehension 1 = Mild to moderate aphasia some obvious loss of fluency or comprehension, but the patient is able to get their ideas across in general 2 = Severe aphasia all communication very limited, examiner must guess what the patient is trying to communicate 3 = Mute, global aphasia NO useable speech, NO auditory comprehension. (Pt unable to follow any one step commands) To choose between a score of 1 or 2 use all the provided materials. It is anticipated that a patient who missed more than two thirds of the naming objects and sentences or who followed only very few and simple one step commands would score a 2. Item 10: Dysarthria Ask the patient to repeat the listed words after you read them out loud. Score patients based on listening to the speech that they do produce. Determine if any slurring of speech is present using the above information and score the patient accordingly. If no intelligible speech is produced or the patient is mute: Score a 2 (severe dysarthria). Item 11: Extinction & Inattention (Neglect) Test bilateral simultaneous visual fields by asking patient to point to L, R, or both of examiners fingers when doing visual exam. Test recognition of bilateral simultaneous touch to upper and lower limbs (patient s eyes closed) by asking patient to point to side(s) being touched (L, R, or both). If the patient has aphasia but does appear to attend to both sides, the score is normal. Abnormality is scored only if present, so this item is never untestable. NIHSS and Aphasia,
129 Module Five NIHSS Training REFERENCES Module Five CONTENT from: NIHSS Workshop 2008 (power point presentation) Retrieved from Nationa l_institutes_of_health_stroke_scale_workshop_2008.htm
130 NEO Stroke Network s Acute Nursing Certification Program MODULE FIVE NIHSS TRAINING Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or Designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
131 DATE: NAME: 1. Skilled and consistent use of a Standardized Nursing Assessment such as NIHSS may: a. Positively impact patient outcomes. b. Lead to early intervention. c. Provide a better prognosis. d. Limit the extension of neurological damage. e. All of the above 2. Performing an NIHSS on a patient, once the nurse is familiar with it, a. Should take 10 minutes or so to complete. b. Should take about an hour if the patient cooperates. c. Only needs to be done upon admission and again on discharge. d. Will show poor sensitivity to neurological change and Glasgow Coma Scale should be used instead. 3. Communicate NIHSS results when: a. You notice a neurological decline b. A new deficit has arisen. c. An already present deficit has gotten worse. d. You have a concern as the nurse that your patient is not quite right, compared to last night. e. All of the above 4. If you forget something about the NIHSS, you can: a. Look it up in this binder. b. Refer to your pocket card. c. Ask the Stroke Nurse or Nurse Clinician. d. Go to nihss-english..trainingcampus.net e. All of the above
132 TRUE/FALSE Questions (CIRCLE the correct letter) T F T F T F T F T F T F 1. The NIH Stroke Scale is designed to assess level of consciousness or coma and measures best response in arousal and orientation. 2. The lower the NIHSS overall total score, the more severe the stroke was. 3. It is important not to help the patient answer the LOC questions. 4. Only the upper quadrant is important when assessing the visual field. 5. Mild paralyis such as asymmetry with a smile would score a 1 on the Facial Palsy question. 6. Repeating words from the Standardized List on the NIHSS pocket card is the proper method to assess clarity of speech and detect presence of dysarthria. SCORE: / 10 Stroke Unit/Medical Unit Nurse Clinician/Designate (signature)
133 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE FIVE Canadian Neurological Scale (CNS) Upon completion of this module, nurses will be able to: Explain why the CNS is a Useful Tool Understand How to Perform CNS Understand the Scoring Methods for this Assessment Describe How and Where to Document the Scores in the Chart Describe When to Communicate Results of CNS Use their Own Pocket Card for Quick Guide for CNS
134 Canadian Neurological Scale 1 Canadian Neurological Scale (CNS) Performing ongoing neurological assessment provides a standardized method to detect neurological deterioration that can lead to early intervention Canadian Neurological Scale is a tool that has been recommended by the HSFO Best Practice Guidelines for Stroke Care, 2003 as a valid and reliable standardized measure for assessment of neurological deficits in the acute stroke period Developed in 1985 in Montreal Focuses on assessment of patients with acute stroke Measures impairment 2 Canadian Neurological Scale, cont Glasgow Coma Scale assesses patients with acute neurological nervous system dysfunction resulting in coma CNS provides a complementary scale to assess conscious and aphasic patients Well tested for reliability and validity Suitable for prognostic stratification in trials and planning rehabilitative measures for patients Higher CNS scores (>11) tended to be associated with favourable outcome lower risk of poor outcome at 6 months Lower CNS scores (<9) tended to be associated with increased death, morbidity Heart and Stroke Foundation of Ontario,
135 Canadian Neurological Scale 3 Advantages of the CNS Standardized Reliability and validity well described Sensitive to relevant changes in patients Can be done repeatedly at bedside for acute patients Uses simple and non-ambiguous definitions for each modality tested Uses a minimum number of grades per modality Addresses issue of aphasia 4 Frequency of Neurological Assessment Using CNS The Heart and Stroke Best Practice Guidelines for Stroke Care outlines the frequency of assessing neurological status based on different clinical situations to assist organizations to set individual protocols based on specific patient needs: Individuals with acute ischemic stroke receiving t-pa (pg 76, ) Monitor vital signs and CNS q15 minutes during drug administration Post infusion care (24 hours) Monitor CNS q1hour for 24hours OR More frequently as ordered, e.g. q15 minutes for 2 hours, q30 minutes for 6 hours, q1hour for 16 hours Heart and Stroke Foundation of Ontario,
136 Canadian Neurological Scale 5 Frequency of Assessment Using CNS cont Based on Heart and Stroke Best Practice Guidelines for Stroke Care: Individuals with acute ischemic stroke not receiving t-pa (pg 78) Monitor vital signs and CNS q1hour for 24 hours or more frequently if ordered Definitive or Suspected TIA Care Pathway and Plan (pg 114) Monitor vital signs and CNS q2hours and prn Acute Care Guides: First 24 hours (pg 82) Follow t-pa protocol if indicated Assess vital signs and CNS q4hours 6 Frequency of Assessment Using CNS cont Based on Heart and Stroke Best Practice Guidelines for Stroke Care: Acute Care Guide: Day 2 (pg 84) Assess vital signs and CNS q4hours Acute Care Guide: Day 3 (pg 86), Day 4-6 (pg 88) Assess vital signs and CNS as required due to patient status These care guides that are meant to provide recommendations based on the best evidence, however, always follow physician orders or clinical pathway guidelines for your organization Heart and Stroke Foundation of Ontario,
137 Canadian Neurological Scale 7 Canadian Neurological Scale 11.5 point scale that has three components: Section A Section A1 Section A2 Mentation (LOC, Orientation, Speech) Motor function -- no comprehension deficit Motor function -- with comprehension deficit 8 Getting Started Assess Pupils Size and light reaction Vital Signs (BP, T, P, R, Oximetry) Assess Level of Consciousness Alert or drowsy CNS Stuporous/comatose GCS Assess Orientation Assess Speech Assess Motor No receptive deficit With receptive deficit Heart and Stroke Foundation of Ontario,
138 Canadian Neurological Scale 9 Definition of Terms Alert: awake and alert, normal level of consciousness Drowsy: rouses when stimulated verbally, remains awake and alert for short periods but tends to doze Stuporous: responds to loud verbal stimuli and/or strong touch; may vocalize, but does not completely wake up Comatose: responds to deep pain: purposeful movement, non-purposeful movement, no response 10 Section A: Mentation Level of Consciousness Alert or drowsy: If patient is Alert score 3.0 If patient is Drowsy score 1.5 Orientation Where are you (city and hospital)? What is the month and year? Patient can write answers to questions of orientation If the patient cannot state both place and time score Disoriented or not applicable score Heart and Stroke Foundation of Ontario,
139 Canadian Neurological Scale 11 Section A: Speech Assess for Receptive Deficit Ask patient to close eyes Point to ceiling Does a stone sink in water? If patient does not complete all three, score receptive deficit 0.0, do not assess Expressive Deficit and go to Section A2: Motor Response Receptive Deficit Present If no receptive deficit Assess for Expressive Deficit 12 Section A: Speech If no receptive deficit Assess for Expressive Deficit Assess for Expressive Deficit Name 3 objects and the use of each: key, pencil, watch If cannot name all 3 objects and the use of each Score Expressive Deficit 0.5 If the patient writes the responses, this is NOT acceptable as speech is being assessed If the patient is slurred but intelligible, that is acceptable for normal speech. Indicate SL when scoring normal speech If no Expressive Deficit, score Normal Speech 1.0 If the patient has an Expressive Deficit or Normal Speech go to Section A1 - Motor Response (No Receptive Deficit) Heart and Stroke Foundation of Ontario,
140 Canadian Neurological Scale 13 Section A1: Motor Response (No Receptive Deficit) Complete this section if patient has an Expressive Speech Deficit or Normal Speech Face: Ask patient to smile or show teeth or gums Note asymmetry of mouth and nasal labial folds Scores for Face: No weakness score None 0.5 Weakness score Present 0.0 Note: Record the side exhibiting the WORST deficit, using R or L 14 Section A1, Proximal Arms Note: Submit both arms to the same testing. Record the side exhibiting the WORST deficit, using R or L Arm (proximal) If patient is sitting: lift arms to shoulder level (90º) and apply resistance just above elbows bilaterally If patient is in lying in bed: elevate arms to 90º and apply resistance above elbows bilaterally Heart and Stroke Foundation of Ontario,
141 Canadian Neurological Scale 15 Section A1, Proximal Arms Scores for Arms (proximal) None Mild = no weakness = movement to 90º, unable to oppose pressure Significant = movement <90º Total = absence of motion 16 Section A1, Distal Arms Arms (distal): Patient sitting or lying Submit both arms to the same testing. Record the side exhibiting the WORST deficit, using R or L Arms outstretched with wrists cocked-back (dorsiflex hands) Support patient s arms while applying pressure between wrist and knuckles Heart and Stroke Foundation of Ontario,
142 Canadian Neurological Scale 17 Section A1, Distal Arms Scores for Arms (distal) None Mild Significant Total = no weakness = can cock-back wrist, unable to oppose pressure = some movement of fingers = absence of movement 18 Section A1, Proximal Legs Legs (proximal): Patient lying in bed Submit both arms to the same testing. Record the side exhibiting the WORST deficit, using R or L Thighs brought toward body Keeping knees flexed to 90º Push down on each thigh one at a time Scores for Legs (proximal) None Mild Significant = no weakness = can lift leg, unable to oppose pressure = lateral movement but no power to lift leg Total = absence of movement Heart and Stroke Foundation of Ontario,
143 Canadian Neurological Scale 19 Section A1, Distal Legs Legs (distal): Patient lying in bed Submit both arms to the same testing. Record the side exhibiting the WORST deficit, using R or L Toes and feet pointed upward Push down on each foot, one at a time Scores for Legs (distal) None Mild Significant =1.5 - no weakness =1.0 - can point foot & toes upward, unable to oppose pressure =0.5 - some movement of toes, but cannot lift toes or foot Total =0.0 - absence of movement 20 Section A2: Motor Response (Receptive Deficit Present) Complete this section if patient has a Receptive Speech Deficit only Face: Have patient mimic your own grin, show his teeth or gums Note asymmetry of mouth and nasal labial folds If patient is unable to cooperate, observe facial response when pressure is applied to sternum Note: Record the side exhibiting the WORST deficit, using R or L Scores for Face Symmetrical = 0.5 Asymmetrical = Heart and Stroke Foundation of Ontario,
144 Canadian Neurological Scale 21 Section A2, Arms Arms: Demonstrate and/or place patient s arms outstretched in front of patient at 90º If patient is unable to cooperate, apply finger nail bed pressure bilaterally and compare response Note: Submit both limbs to the same testing. Record the side exhibiting the WORST deficit, using R or L Scores for Arms Equal Unequal = equal motor response = unequal motor response 22 Section A2, Legs Legs: thighs toward trunk with knees flexed to 90º If patient is unable to cooperate, apply toenail bed pressure bilaterally and compare response Note: Submit both limbs to the same testing. Record the side exhibiting the WORST deficit, using R or L Scores for Legs Equal Unequal = maintain position or withdraw equally = cannot maintain position or unequal withdrawing Heart and Stroke Foundation of Ontario,
145 Canadian Neurological Scale 23 Scoring the CNS Score Mentation Section -Section A for all patients Score Section A1 OR Section A2 Do not score both A1 & A2 Add Section A + A1 OR A + A2 Maximum Score = 11.5 Decrease of more than 1 point from previous CNS scores is indicative of a change in patient status and requires notification of the physician. Changes in vitals signs and pupil size and reaction would also warrant a change in status and also require notification of the physician Thanks The Heart and Stroke Foundation of Ontario gratefully acknowledges the contribution of Rhonda McNicoll, R.N., BSc.N., CNN(c), Hamilton Health Sciences, in the development of this presentation. Heart and Stroke Foundation of Ontario,
146 Organization Name Procedure for Use of the Canadian Neurological Scale Observation Record Initial Issue Date: Document Number: Last Revision Date: Approved By: Applies To: Purpose To describe the procedure for the assessment of acute stroke patients using the Canadian Neurological Scale. Definitions Canadian Neurological Scale (CNS): The Canadian Neurological Scale was designed to assess neurological function in conscious stroke patients. It includes an assessment of level of consciousness, orientation, aphasia, and motor strength. Each domain is assigned a score, and a total score from 1.5 to 11.5 is calculated. Alert: Patient is awake and alert and has a normal level of consciousness. Drowsy: Patient rouses when stimulated verbally and remains awake and alert for short periods but tends to doze. Stuporous: Patient responds to loud verbal stimuli and/or strong touch; may vocalize but does not completely wake up. Comatose: Patient responds to deep pain with purposeful movement, non-purposeful movement or no response. Expressive Speech Deficit: Patient can understand verbal speech, but is unable to say the word, or cannot think of the right word. Receptive Speech Deficit: Patient is unable to understand both spoken and written words. U 1
147 Equipment Keys, Watch, Pencil/Pen, Blood Pressure Machine and Thermometer General Guidelines The Heart and Stroke Foundation's Best Practice Guidelines for Stroke Care outlines the frequency for assessing neurological status using the Canadian Neurological Scale based on different clinical situations or phase of care in the sample care guides. These care guides are based on best evidence and can serve as a reference for staff. However, it is essential that clincians follow the physician orders or clinical pathway guidelines for frequency for assessing neurological status using the Canadian Neurological Scale within their organization. The patient s identification must be stamped on the top corner of each side of the Canadian Neurological Scale Observation Record. Write all information in blue/black ink unless otherwise directed. Initials, signature and designation must appear in the signature section. Significant findings are indicated by an asterisk * and documentation made in the patient s chart. Specific Guidelines CARDIOVASCULAR Graph all vital signs, temperature, blood pressure, pulse and respirations as ordered. Indicate time of the assessment in the box provided. When recording blood pressure, identify whether the measurement was obtained by cuff, noninvasive blood pressure cuff, arterial line or Doppler. As appropriate, identify right versus left arm and sitting versus lying. Re-label only when the measurement has been obtained by an alternate method of limb. Document respiratory rate, percentage of oxygen in use and oximetry as per order and organization policy. Organizations or clinicians can use the additional lines to add additional monitoring of acute stroke patients e.g. angioedema or bleeding for the patient who has received tpa. PUPILS Record size of the pupils in mm using the pupil scale prior to the application of the light stimulus. Indicate the reaction of pupils as either: + = Brisk Reaction, S = Sluggish Reaction or - = No Reaction. If the eyes are closed due to swelling record "C". Use of the Canadian Neurological Scale,
148 Procedure Note: The CNS Scale is to be used for alert or drowsy patients. If patient is comatose or stuporous, use the Glasgow Coma Scale. SECTION A: MENTATION Mentation involves assessing Level of Consciousness, Orientation, and Speech. ASSESS LEVEL OF CONSCIOUSNESS Score "3" for Alert if the patient is alert, alert and has a normal level of consciousness. Score "1.5" for Drowsy if the patient rouses when stimulated verbally and remains awake and alert for short periods but tends to doze. If the patient is stuporous or comatose use the Glasgow Coma Scale for assessing neurological function. ASSESS ORIENTATION Score "1.0" for Oriented if the patient is able to tell the examiner the place, i.e., city or hospital and time, i.e., correct month and year. If early in month (i.e., first three days) previous month is acceptable. Speech may be mispronounced or slurred but intelligible. If the patient is able to write the place and time, this is also an acceptable response. Score "0.0" for Disoriented or Non Applicable if for any reason the patient cannot answer the questions about place and time (i.e., does not know the answer, gives the wrong answer, answers only partially, cannot express self because of unintelligible speech or ignores the question). If the patient s first language is not English and an interpreter is used to complete the assessment, initially complete the assessment without the interpreter as a baseline and then with the interpreter. If an interpreter is used, indicate that on the documentation tool. ASSESS SPEECH Assess Receptive Language Ask patient to "Close your eyes", "Point to the ceiling" and "Does a stone sink in water?" Repeat question twice if necessary. Do not mimic commands. NOTE: For the purpose of this procedure the original protocol as described in the research articles is followed. Some organizations may not ask the question Does a stone sink in water? Follow the Receptive Language testing used within your organization. If the patient obeys the 3 commands, continue to assess expressive language. If the patient obeys 2 or less commands, score "0" for receptive deficit, do not assess expressive language and move to assess Motor Function Section A2: Receptive Deficit. Assess Expressive Language Objects needed: pencil/pen, key, watch. Use of the Canadian Neurological Scale,
149 Show patient each item and ask patient to name: pencil, key and watch. Allow patient time to respond. Again show the patient each item and ask the patient to state the use of the pencil, key and watch. One word telegraphic answers are acceptable. NOTE: If the patient writes the answer to any of the above questions, this is NOT acceptable as expressive speech is being assessed. Grading: Patient is scored according to the worst speech deficit. If patient is unable to name all the 3 objects and their use, score the patient as having an Expressive Deficit and scored "0.5". If the patient names all three objects and the use of the 3 objects, score "1.0" for Normal Speech. If the patient s speech is slurred, indicate SL beside the appropriate speech grading for the patient. If the patient is scored as having normal speech or expressive speech deficit, assess Motor Function using Section A1: No Receptive Deficit. MOTOR FUNCTION: SECTION A1 OR A2 If patient is able to follow directions and cooperate, complete section Motor Function A1 - No Receptive Deficit. If patient is scored as a receptive deficit, complete section Motor function A2 - Receptive Deficit. Complete one section only on each patient, i.e. A1 or A2 not both. When evaluating strength and range of motion in limbs always test both sides of the body, record the worst deficit identified and the side of the body the deficit is in. If weakness is present, identify which side has the weakness with "R" or "L" in the slot with the grade, e.g.: R The Canadian Neurological Scale is meant to identify changes in motor function in the acute stroke patient. If on admission it is identified that the patient has a pre-existing permanent deficits related to a previous stroke or other medical condition, e.g. right sided significant deficit or right sided amputation etc, that is not on the side of the new stroke motor deficit indicate this on the Canadian Neurological Scale form and score the deficit related to the new motor deficit. NOTE: For the purpose of this procedure, the original motor grading terms as described in the research articles were used. Some regions may use different terms to describe each level, e.g. Moderate or Severe may be used instead of Significant, and Complete may be used instead of Total. Follow the motor grading scale used within your organization. Use of the Canadian Neurological Scale,
150 Motor Function Section A 1 (No Receptive Deficit) Complete only if patient is able to obey commands and follow directions and was assessed in Speech section to have an expressive speech deficit or normal speech. Complete one section only on each patient, i.e. A1 or A2 not both. Face Observe the patient s face; ask them to smile or show their teeth or gums and note symmetry of mouth and nasal labial folds. Grading: Assess both sides but score the side of the face with the worst deficit and identify the side with the weakness by using either "R" or "L" in the grading slot. No weakness, score "0.5": Symmetrical grin, no asymmetry in smile. Weakness Present "0.0": Facial asymmetrical, i.e., one corner of mouth lower than other, either at rest or while showing teeth. Upper Limb (Proximal) Patient should be tested in sitting position if possible. Have patient abduct their arms 90 degrees to the side (flap like a bird). If patient is lying in bed, have patient elevate arms in front of patient. Apply resistance midway between the shoulders and elbows. Grading: Assess both arms but score the arm with the worst motor deficit and identify the side with the weakness with either "R" or "L" in grading slot. None, score"1.5": No weakness of the proximal arm. Mild, score "1.0": Mild weakness of the proximal arm. Normal range of motion against gravity but succumbs to resistance by observer either partially or totally. Movement to 90 degrees but unable to oppose pressure. Significant, score "0.5": The patient cannot overcome gravity in range of motion, i.e., movement or arms in abduction less than 90 degrees. Total, score "0.0": No movement of the proximal arm. Upper Limb (Distal) Patient is tested sitting or lying position. Have patient raise arms in front of him with wrists cocked back (dorsiflexed hands). Apply resistance to wrists while stabilizing the patient s arm. Grading: Assess both arms but score the arm with the worst motor deficit and identify the side with the weakness with either "R" or "L" in grading slot. None, score "1.5": No weakness in wrist. Use of the Canadian Neurological Scale,
151 Mild, score "1.0": Mild weakness, normal range of motion, i.e., can "cock-back" wrist but unable to oppose pressure of examiner. Significant, score "0.5": Some movement of fingers but cannot completely overcome gravity in full range of motion, i.e., cannot cock-back wrists. Total, score "0.0": Absence of movement of wrists. Proximal Legs Patient is tested lying in bed. Have patient flex thighs toward trunk with knees flexed at 90 degrees. Push down on each thigh one at a time. Grading: Assess both legs but score the leg with the worst motor deficit and identify the side with the weakness with either "R" or "L" in grading slot. None, score "1.5": No weakness of the proximal leg. Mild, score "1.0: Mild weakness, can lift leg to 90 degrees, but unable to oppose pressure either partially or total. Significant, score "0.5": Severe weakness of the proximal leg, the patient cannot flex hip to 90 degrees, partial movement against gravity. Total, score "0.0": No movement of the proximal leg or only contraction of muscle without actual movement of limb. Distal Legs Patient is tested lying in bed. Ask the patient to point toes and foot upward. Apply resistance alternately to each foot after full movement has been completed. Grading: Assess both legs but score the leg with the worst motor deficit and identify the side with the weakness with either "R" or "L" in grading slot. None, score "1.5": No weakness of the distal leg. Mild, score "1.0": Mild weakness of the distal leg, can point foot and toes upward but unable to oppose pressure. Significant, score "0.5": Severe weakness of the distal leg, some movement of toes but cannot lift toes or foot. Total, score "0.0": No movement of the distal leg. Motor Function Section A 2 (Receptive Deficit Present) Complete this section only if patient cannot follow instructions and has been assessed as having a receptive deficit in the Speech section. Complete one section only on each patient, i.e. A1 or A2 not both. Use of the Canadian Neurological Scale,
152 When evaluating strength and range of motion in limbs always submit both limbs to same testing and record the side with the worst deficit. If weakness is present, identify which side has the weakness with "R" or "L" in the slot with the grade, e.g.: R Face Have patient try to mimic your grin and note symmetry of mouth and nasal labial folds. If patient is unable to follow commands, observe facial response when pressure is applied to sternum. Grading: Assess both side of the face but score the worst deficit and identify the side with the weakness with either "R" or "L" in grading slot. Symmetrical, score "0.5": Symmetrical grin, no asymmetry in smile. Asymmetrical, score "0.0": Facial asymmetrical, facial weakness on one side, facial droop. Arms Elevate the patient s arms outstretched at 90 degrees in front of patient. Observe if patient can maintain it for 3-5 seconds, note asymmetry. If unable to elevate arms, test by applying nail bed pressure bilaterally and compare response. Grading: Assess both arms but score the arm with the worst deficit and identify the side with the weakness with either "R" or "L" in grading slot. Equal, score "1.5": Equal motor response in both arms. Unequal, score"0.0": Unequal motor response. Legs Elevate one leg at a time to 90 degrees Observe if maintained for 3-5 seconds, note asymmetry. If patient unable to cooperate, test by applying pressure to toenail beds bilaterally and compare response. Grading: Assess both legs but score the leg with the worst motor deficit and identify the side with the weakness with either "R" or "L" in grading slot. Equal, score "1.5": Able to maintain position or withdraw equally. Unequal, score"0.0": Cannot maintain position or unequal withdrawing. Documentation Document the scores on the Canadian Neurological Scale form. Each domain is assigned a score, and the total score is calculated. Minimum score is 1.5 and the maximum score is Add scores in Section A: Mentation and Motor Function Section A1 or Motor Function Section A2 to obtain the total Canadian Neurological Scale Score. Use of the Canadian Neurological Scale,
153 A decrease of more than 1 point from previous Canadian Neurological Scale may indicate deterioration in the patient s condition and requires notification of the physician. If the patient experiences change in pupil size and reaction to light or vital signs this may indicate deterioration in the patient s condition and require notification of the physician. References Cote R, Hachinski V, Shurvell B, Norris J, & Wolfson C. The Canadian Neurological Scale: A Preliminary Study in Acute Stroke. Stroke 1986;17: Cote R, Battista R, Wolfson C, Boucher J, Adam J, & Hachinski V. The Canadian Neurological Scale: Validation and Reliability Assessment. Neurology 1989;39: Heart and Stroke Foundation of Ontario. Best Practice Guidelines for Stroke Care. Author:2003. The Institute for Clinical Evaluative Sciences and the Canadian Stroke Network. Operations Manual, The Registry of the Canadian Stroke Network. Author:2002. The Toronto Hospital. Canadian Neurological Scale. Developed By CNS Working Group, Neurosciences Program, Hamilton Health Sciences, Hamilton, Ontario. Use of the Canadian Neurological Scale,
154 INSERT LOGO CANADIAN NEUROLOGICAL SCALE OBSERVATION RECORD YEAR BLOOD PRESSURE STANDING = Systolic = Diastolic LYING V = Systolic Λ = Diastolic = PULSE DATE: M/D TIME 200 _ 190 _ 180 _ 170 _ 160 _ 150 _ 140 _ 130 _ 120 _ 110 _ 100 _ 90 _ 80 _ 70 _ 60 _ 50 _ 40 _ TEMPERATURE =X _ 41 _ 40.5 _ 40 _ 39.5 _ 39 _ 38.5 _ 38 _ 37.5 _ 37 _ 36.5 _ 36 _ 35.5 _ 35 _ 34.5 _ 34 _ 33.5 _ 33 PUPIL SCALE mm Respirations Oxygen (Litre /min or %) Oxygen Saturation (%) PUPILS MENTATION SECTION A1 NO COMPREHENSION DEFICIT Record Right (R) and Left (L) to indicate side of deficit SECTION A2 COMPREHENSION DEFICIT Right Eye Left Eye SIGNATURE AND DISCIPLINE Size Reaction Size Reaction Level of Consciousness: Alert 3.0 Drowsy 1.5 Orientation: Oriented 1.0 Disoriented or non applicable 0.0 Speech: Normal 1.0 Expressive deficit 0.5 Receptive deficit 0.0 MOTOR FUNCTIONING WEAKNESS Face: None 0.5 Present 0.0 Arm: Proximal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Arm: Distal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Leg: Proximal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Leg: Distal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 MOTOR RESPONSE Face: Symmetrical 0.5 Asymmetrical 0.0 Arms: Equal 1.5 Unequal 0.0 Legs Equal 1.5 Unequal 0.0 TOTAL SCORE + = Reaction = No Reaction C = Eyes Closed due to swelling Record Worst Deficit LEGEND R.A. - Room Air CNS OBSERVATION RECORD
155 M E N T A T I O N Section A1 No Comprehension Deficit Level of Consciousness Alert 3.0 Drowsy 1.5 Orientation Oriented 1.0 Canadian Neurological Scale (CNS) Cheat Sheet Alert or Drowsy CNS Stuporous or Comatose Glasgow Coma Scale Disoriented 0.0 Speech Receptive deficit 0.0 Expressive deficit 0.5 Normal Speech 1.0 Face None 0.5 Present 0.0 Arm: Proximal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Arm: Distal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Leg: Proximal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Leg: Distal None 1.5 Mild 1.0 Significant 0.5 Total 0.0 Spontaneous eye opening, normal level of consciousness When stimulated verbally patient remains awake and alert but tends to doze 1. Where are you? (City and Hospital) 2. What is the month and year? Speech can be slurred but must be intelligible. Patient cannot state both place and time or cannot express answers in words or intelligible speech. It is acceptable for patient to write answer to questions of orientation Receptive deficit: Ask pt. 1) to close eyes; 2) Point to ceiling; 3) Does a stone sink in water? If pt. does not complete the above 3, go to Section A2. Ask pt. to smile: No weakness 0.5 Weakness 0.0 (Record L or R) Ask pt. to lift arms to shoulder level and apply resistance above elbows bilaterally No weakness 1.5 Movement to 90, unable to oppose pressure 1.0 Movement < Absence of motion 0.0 Ask pt. to bend wrist back. Apply pressure on back of the hand. No weakness 1.5 Can bend wrist, unable to oppose pressure 1.0 Some movement of fingers 0.5 Absence of movement 0.0 Ask pt. to flex knee to 90. Push down on each thigh one at a time. No weakness 1.5 Can lift leg, unable to oppose pressure 1.0 Lateral movement but no power to lift leg 0.5 Absence of movement 0.0 Ask pt. to point toes and feet upward. Push down on each foot one at a time. No weakness 1.5 Can point foot & toes upward, unable to oppose pressure 1.0 Some movement of toes, but cannot lift toes or foot 0.5 Absence of movement 0.0
156 Section A2 Comprehension Deficit Face: Symmetrical 0.5 Asymmetrical 0.0 Arms: Equal 1.5 Unequal 0.0 Legs: Equal 1.5 Unequal 0.0 Ask pt. to mimic your grin (if unable, apply pressure to sternum). Symmetrical 0.5 Asymmetrical 0.0 Demonstrate/place pt. arms in front of pt. at 90 (if unable, apply finger nail bed pressure bilaterally and compare response) Equal motor response 1.5 Unequal motor response 0.0 (record L or R) Thighs flexed to 90 (if unable, apply toenail bed pressure bilaterally and compare response) Maintain position or withdraw equally 1.5 Cannot maintain position or unequal withdrawing 0.0 (record L or R) Developed by Moire Brown and Jun Li, HHS
157 NEO Stroke Network s Acute Nursing Certification Program MODULE FIVE CNS TRAINING Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or Designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
158 DATE: NAME: 1. Skilled and consistent use of a Standardized Nursing Assessment such as CNS may: a. Positively impact patient outcomes. b. Lead to early intervention by detecting neurological deterioration. c. Provide a better prognosis. d. Limit the extension of neurological damage. e. All of the above 2. You will choose to assess Motor Response using either the A1 OR the A2 component of the CNS. You will select A2 when: a. Your stroke patient has a Receptive Speech Deficit, that is, they do not comprehend the questions you are verbally asking them. b. Your stroke patient is drowsy or asleep. c. Your stroke patient has an Expressive Speech Deficit, that is, they can not produce speech properly. d. You are finished both A and A1 components of the test. 3. Communicate CNS results when: a. You notice a neurological decline in your patient. b. The new score differs by 1 point from the last CNS score. c. An already present deficit has gotten worse. d. You have a concern as the nurse that your patient is not quite right, compared to last night. e. All of the above 4. If you forget something about the CNS, you can: a. Look it up in this binder. b. Refer to your pocket card. c. Ask the Stroke Nurse or Nurse Clinician.
159 d. All of the above TRUE/FALSE Questions (CIRCLE the correct letter) T F T F 1. The CNS complements the GCS and is a reliable and valid tool for acute stroke patients. 2. The CNS is a 11.5 point scale measuring Mentation and Motor Function. T F 3. Higher CNS scores tend to imply a poor outcome. T F 4. It is not necessary to notify the physician of a change in CNS score unless the score has decreased by 3 or more points from previous CNS scores. T F T F 5. Presence of aphasia is taken into account with the CNS. 6. When assessing motor function in the upper limbs, record the side with the WORST deficit, using R or L. SCORE: / 10 Stroke Unit/Medical Unit Nurse Clinician/Designate (signature)
160 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE SIX Swallowing, Feeding and Oral Care Upon completion of this module, nurses will be able to: Define Dysphagia List the Complications Associated with Dysphagia Understand the Mechanics of a Normal Swallow List Signs of Swallowing Problems Define Silent Aspiration Identify a Screening Tool for Dysphagia Understand the Purpose and Goals of Dysphagia Management Explain the Indications, Risks and Benefits Related to Enteral Nutrition Understand Proper Feeding Strategies Understand the Importance and Methods for Oral Care
161 NEO Stroke Network s Acute Nursing Certification Program MODULE SIX Swallowing, Feeding and Oral Care Self Learning Program NEO Stroke Network Developed April 2010
162 Swallowing Post Stroke Optimal stroke care includes identifying and managing dysphagia. Studies indicate that almost 50% of acute stroke patients have some degree of dysphagia within the first 72 hours after the stroke. (Kidd D et al., 1995) *NOTE the difference between these two terms: Dysphasia/Aphasia - is a language disorder in which there is an impairment of the comprehension and expression of language. Dysphagia - is a medical term defined as "difficulty swallowing." Dysphagia: the loss or the impaired ability to chew and/or swallow characterized by a disturbance in the swallowing mechanism difficulties include choking, coughing, excess drooling, and the inability to manage secretions presentation is varied and difficulty can occur in one or more of the swallowing phases risk increases with the elderly population Stroke can affect one s ability to eat or swallow when: 1. Muscles involved in feeding, swallowing, or breathing are affected 2. Alertness and attention to eating are affected 3. Independence for eating is taken away 2
163 Here are some facts: In total, more than 200,000 people suffer from dysphagia in Canada at any given time 1/3 of hospitalized patients have dysphagia (Groher and Bukatman, 1986) Visible signs of swallowing difficulty exist in 80% of the institutionalized elderly The cost of treating pneumonia in Canada has been estimated at $1,000 per day of hospitalization (Steele et al, 199 Swallowing Problems Related to Aging Decreased peristalsis in the esophagus Decreased lung function Decreased muscle strength Problems with dentition Decreased saliva Complications Associated with Dysphagia Having dysphagia can have a serious impact on one s health, leading to other serious conditions such as: a. Airway obstruction b. Aspiration pneumonia c. Malnutrition d. Dehydration e. Reduced quality of life Malnutrition Inadequate energy and protein intake is highly prevalent in stroke. The majority of stroke patients do not consume their estimated energy and protein requirements. Therefore, it is very important to be aware of a stroke patient s intake. Identifying malnutrition in stroke patients is critical as 16% of acute stroke patients admitted to hospital are malnourished. Malnutrition increases the risk of pneumonia and other infections. 3
164 Malnutrition after stroke is associated with poor long-term outcome (ie.decreased functional status, physical decline, increased length in hospital etc.) It is critical to begin appropriate nutrition as soon as possible. Hydration Stroke patients on thickened flds are at increased risk of inadequate fluid intake, which leads to dehydration; UTI s etc. This is due to the reduced level of free water content in the thickened fluids and overall reduced total fluid intake. Stroke patients need to be encouraged to consume the thickened fluids on their meal trays. If there is a concern on the amount of fluids your patient is consuming, consult the dietitian. What is a Normal Swallow? Swallowing is a semi-automatic motor action involving the movement of food from mouth to stomach. The average adult swallows 1500 times per day. While awake, we swallow once every seconds. A normal swallow has four phases: 1. Oral Preparatory Phase 2. Oral Transport Phase 3. Pharyngeal Phase 4. Esophageal Phase 1. Oral Preparatory Phase This is the initial stage whereby food and drink are brought to the mouth, lips and jaw close to seal the mouth and saliva is produced to add moisture Under voluntary control Food is chewed and mixed with saliva to form a bolus (ball of food) 4
165 2. Oral Transport Phase Bolus is delivered by voluntary tongue movement to the back of the mouth, into the pharynx 3. Pharyngeal Phase Involuntary/reflexive phase lasts 800 milliseconds Triggered when food passes towards the esophagus and the soft palate closes Pharynx and the larynx move up to protect the airway and direct the bolus to the esophagus 5
166 3. Esophageal Phase Involuntary/reflexive Relaxation of the upper part of the esophagus Peristalsis pushes the bolus down into the stomach Gravity also assists with bolus transportation
167 Signs of Swallowing Problems It is important to notice these crucial signs that may indicate your stroke patient is having difficulty swallowing: Drooling Slow eating, prolonged chewing Food left in mouth after eating (e.g. residue or pocketing) Pain associated with swallow Effortful swallow Delayed initiation of swallow Coughing or choking during and/or after swallowing Throat clearing after swallowing Voice changes (i.e. wet/gurgly voice) Refusal to eat Recurrent chest infections Unexplained weight loss Gagging Nasal regurgitation Few Words about Reflexes Absence of a gag reflex does not predict dysphagia Presence of a gag reflex does not protect against aspiration The cough reflex can be impaired or absent, so silent aspiration may occur Aspiration is the entry of food or liquid into the airway below the muscles that produce sound, that is the vocal folds. (Rosenbek JC et al., 1996) Bacteria in saliva, foods and liquids, or refluxed material from the stomach can enter the airway. It can lead to choking or breathing problems. If this material enters the lungs, it can cause an infection -typically aspiration pneumonia. Incidence of aspiration in stroke 50% aspirate immediately after the brain insult 25% die of aspiration pneumonia within the 1st year of rehabilitation (American Academy of Otolaryngology Head and Neck Surgery, 2006) 7
168 Silent Aspiration Coughing is a physiologic response to aspiration in normal healthy individuals. (Logemann) But aspiration is not always accompanied by coughing. Silent Aspiration is when there are no clinical signs of aspiration (no coughing or throat clearing). It is very common in fact, lack of coughing is prevalent in 40% of aspirators (Logemann). When silent aspiration is occurring, it is not until respiratory complications occur that we realize the patient has been aspirating. How do you detect silent aspiration? a) When a stroke patient presents with high risk of aspiration we closely monitor temperature, fever, WBC, and chest to detect any new infection. b) If the patient is silently aspirating, they will not cough or clear their throat at bedside. Remember the Chest X-ray key terms: Consolidation Infiltrate Atelectasis Pleural effusion It is important to evaluate overall respiratory status and consider the patient s likelihood of being able to protect themselves from further infection when evaluating feeding options. Goals of Dysphagia Management Maximize nutrition Protect airway from obstruction Protect airway from aspiration Manage reflux Control oral bacteria 8
169 Monitor medication intake Monitor and maintain fluid intake for hydration Dysphagia management is the key to preventing aspiration and aspiration pneumonia! SCREENING The TOR-BSST is a screen that can accurately and reliably detect the presence of dysphagia (Martino, 2000). It must be done by a trained health care professional who administers and interprets the results of the test. The TOR-BSST comprises 5 clinical tests (50 ml water test, impaired pharyngeal sensation, impaired tongue movements, dysphonia and general muscle weakness) which contribute to making a prediction of dysphagia. If the patient passes the screening, they are initiated on oral feeding (Diet as Tolerated DAT soft). These individuals should be monitored during their first few meals to ensure safe and efficient swallowing. Should swallowing difficulties occur, they should be referred to the Speech and Language Pathologist for assessment. Those who fail the screening are referred to the SLP for a full assessment. The individual should remain NPO until after a full clinical bedside assessment can be performed. During this time, good oral hygiene practices are to continue. They are to have nothing by mouth, not even ice chips. A referral is also made to the Registered Dietician. There are other evidence-based swallowing screening tools such as STAND which may be implemented in the region in the future. 9
170 Dysphagia DIETS Solid Textures Regular: Any food Soft: Meat cooked soft, no raw vegetables, seeds, nuts Diced: Food that is cut into bite-size pieces Minced: Food that is the consistency of ground meat (incl. scrambled eggs, and salad sandwiches) Purée: Food that has been blended Fluid Textures Thin: Any fluid, includes anything that turns into a thin fluid once in the mouth (i.e.. ice cream, Jell-o, milkshakes, etc.) Nectar Thick: This is the consistency of tomato juice or buttermilk. Honey Thick: This is the thickest consistency, almost the consistency of liquid honey Mixed Consistencies A liquid and a solid in the same food. Examples: cold cereal in milk, vegetable soup, fruit in juice. Patients have difficulty coordinating musculature to safely swallow mixed consistencies. If a patient is receiving thickened fluids they are not allowed mixed consistencies. Cream or thickened soups will be provided. Fruit in juice must be strained. 10
171 Diet Textures Solids Easiest Hardest Puree Minced Diced Regular Fluids Easiest Hardest Honey Nectar Thin (in most cases but not all) Indications for Enteral Nutrition Support If stroke patients are anticipated to be left NPO for several days before a bedside swallowing assessment can be completed ; then consider enteral feeding via nasogastric (NG) tube to provide both nutrition and medications and await the Speech Language Pathologist s swallowing assessment. The potential need for a NG feeding tube is even more important for those stroke patients at higher risk for malnutrition and complications due to other comorbidities and/or previous malnourished state (i.e. emaciated / cachectic). An NG feeding tube may also be needed for those stroke patients who are on oral diets, but are unable to meet basic nutritional needs with oral intake alone (supplemental tube feeding). Early gastrostomy tube feeding is proving to be superior to NG tube feeding in acute dysphagic stroke). 11
172 PEG FeedingTube (percutaneous endoscopic gastrostomy tube) Used for longer term nutrition support (>4-6 weeks). Can be done endoscopically,radiologically, CT-guided or surgically. Consider PEG placement for enteral feeding lasting longer than 28 days, as this time frame has been associated with fewer complications. Nasogastric (NG) Feeding Tube Used for short term nutrition support. Average use is < 4 weeks. The nares should be checked periodically for breakdown and soreness. Common benefits: Provides immediate route to provide nutrition, water & medications Allows patient to be nourished & hydrated when some recovery of swallowing ability is expected within a short time period (1-3 weeks) Common risks: Patient may pull NG out, as it is easily accessible Hands may need to be restrained if repeatedly pulled out Smaller tubes clog more easily May cause: reflux, possible aspiration pneumonia May cause an increase in secretions & sinusitis If no progress in 1-3 weeks, PEG should be considered for longer-term tube feeds. 12
173 Feeding your stroke patient To ensure patient safety one needs to consider Positioning for feeding Safe feeding techniques & strategies Mouth Care Dysphagia diets Thickened fluids How Should the Patient Be Positioned? While Eating and Drinking: Sit fully upright Slight chin tuck 13
174 How Should the Feeder Be Positioned? Eye-level with the patient Across from the patient Feeder should be comfortable Do not feed from above the mouth Positioning to Feed the Patient. (Retrieved from Tips and Tools for Caregivers, Heart and Stroke Foundation of Ontario, 2002, page 54, figure 16) 14
175 Feeding Considerations Feeding is a skill that requires knowledge and experience!! Stroke survivors should be encouraged and assisted to feed themselves it is actually safer than being fed. Patients who are fed by others are at an increased risk of dysphagia. Safe/low-risk feeding practices should be used with all patients but are especially important with patients requiring full feeding assistance to prevent serious health problems and improve the quality of the experience for the patient. Feeding Strategies Check the tray to ensure the correct diet has been provided! Feed at a relaxed pace Ensure patient has swallowed before giving the next bite, watch/feel the swallow Present one teaspoon at a time Do not engage in conversation with patient when there is food or liquid in their mouth It is permissible to engage in conversation once their mouth is empty as this is a way to check vocal quality Use hand-over-hand support with dysphagic patients who cannot self-feed Cue patients to feed on the strong side of their mouth (eg. present utensil or cup to non-affected side) Reduce distractions Provide 1 pill at a time (crush if necessary) Patient should remain upright for at least 30 minutes after meal Complete mouth care after each meal 15
176 The Heart and Stroke Foundation of Ontario s Improving Recognition and Management of Dysphagia in Acute Stroke, A Vision for Ontario 2005 published the following piece. Dangerous Practices Did you know??? The following practices may have significant clinical consequences, including aspiration or dehydration, for individuals with dysphagia: Feeding someone who is not alert Syringe feeding Feeding in a fully or partially recumbent position Giving pills with water to individuals on a no thin fluids diet Unnecessarily restricting diet to thickened fluids and puree Feeding with a tablespoon rather than a teaspoon Giving anything not approved in the diet: tell the family, other staff members and visitors to check if specific food items are allowed before bringing them Oral Care The objective of proper mouth care is to maintain the mouth in a comfortable, clean, moist and infection-free state. (Diagram retrieved from Management of Dysphagia in Acute Stroke, 2006, Heart and Stroke Foundation of Ontario, page 26, figure 7) To be effective, ORAL CARE MUST INCLUDE cleaning the: Entire oral mucosa Tongue Teeth Sulci (spaces between the cheeks and gums) 16
177 Thorough and effective mouth care is required to maintain a healthy oral environment on all patients, especially if they are: Unconscious NPO (nothing per oral) Eating and drinking minimally Have impaired oral sensation For patients that are NPO mouth care should be performed a minimum of bid (twice daily) ** For patients receiving thickened fluids: If patient has prescribed mouth care agent (e.g. nystatin) ensure it is swabbed on due to risk of aspiration.. patient cannot swish and swallow but may be able to swish and spit Consider consulting dentistry, occupational therapy, speech language pathologists, and/or a dental hygienist to develop an oral care protocol (National Stroke Nursing Council, 2010) Weight It is important that all stroke patients are weighed upon their admission to the medical floor. This will serve as a baseline weight so that the Dietitian can determine that any weight loss is occurring during their hospital stay. Weights can be recorded in the care trends section of the patient s chart. Intake Records Food intake records can be ordered by the Physician and/or Dietitian for a set number of days to better determine if a stroke patient s oral intake is meeting their estimated nutritional needs. Please use the menu tickets, if available, on a patient s meal tray to mark the approximate amount of each food consumed. In some centres, these menu tickets are kept on the front of the patient s chart for the Dietitian to view. 17
178 Module Six Swallowing, Feeding and Oral Care REFERENCES Campbell-Taylor I. (2008). Oropharyngeal Dysphagia in long-term care: Misperceptions of treatment efficacy. J Am Med Dir Assoc., 9: College of Audiologists and Speech-Language Pathologists of Ontario, (2008). Practice Standards and Guidelines for Speech Language Pathology Practice in the area of Dysphagia. Retrieved from Heart and Stroke Foundation of Ontario. (2002). Tips and Tools for Everyday Living: A guide for stroke caregivers. Toronto, ON. Feagan BG, Marrie TJ, Lau CY et al.(2000). Treatment and Outcomes of Community- Acquired Pneumonia at Canadian Hspitals. CMAJ, 162(10), Franceschini T. (2006). Dysphagia Practice: Taking Services to the Next Level of Evidenced Based Practice. Northern Speech Service. Toronto ON. Groher ME. (1997). Dysphagia: Diagnosis and Management. Tampa, FL: Butterworth- Heinmann. Groher ME, Bukatman R. (1986). The prevalence of swallowing disorders in two teaching hospitals. Dysphagia 1: 3 6. Heart and Stroke Foundation of Ontario and Canadian Stroke Network. (2007). Faaast FAQs for Stroke Nurses. Ottawa: Heart and Stroke Foundation of Canada Heart and Stroke Foundation of Ontario. (2006). Management of Dysphagia in Acute Stroke. Toronto, ON: Heart and Stroke Foundation of Ontario. Heart and Stroke Foundation of Ontario. (2002). Improving Recognition and Management of Dysphagia in Acute Stroke: A Vision for Ontario. Toronto, ON Hôpital régional de Sudbury Regional Hospital. (2005, updated 2010). Standards of Care, 5 South Medical Unit. Retrieved from %20ACUTE%20STROKE%20PATIENTS-update.pdf Kidd D, Lawson J, Nesbitt R & MacMahon J. (1995). The natural history and clinical consequences of aspiration in acute stroke. Quarterly J Med; 88:
179 Langmore SE, Terpenning MS, Schork A, et. al. (1998). Predictors of aspiration pneumonia: How important is dysphagia? Dysphagia, 13: Lindsay, P., Bayley, M., Hellings, C., Hill, M., Woodbury, E., Phillips, S. (2008). Canadian best practice recommendations for stroke care (Updated 2008). CMAJ, 179 (12 SUPPL): E1-E93. Logemann, J. (1983). Evaluation and Treatment of Swallowing Disorders. San Diego, CA: College-Hill Press. Lundy, D. (2006). Swallowing: Patient Safety and Medicinal Therapy for Ear, Nose, and Throat Disorders. Head and Neck Surgery, American Academy of Otolaryngology, Marik PE. (2001). Aspiration Pneumonitis and Pneumonia: A clinical review. N Engl J Med; 344: Marik PE & Kaplan D. (2003). Aspiration pneumonia and dysphagia in the elderly. Chest, 124: Martino R & French B. (2007). TOR-BSST(C) Training for the SLP Dysphagia Expert, (Videoconference), Toronto Western Hospital: Toronto, ON. Martino R, Foley N, Bhogal S, Diamant N, Speechley M & Teasel R.(1995). Dysphagia After Stroke: Incidence, Diagnosis, and Pulmonary Complications. Stroke, 36: Martino R, Pron G & Diamant NE. (2000). Screening for Oropharyngeal Dysphagia in Stroke: Insufficient Evidence for Guidelines. Dysphagia, Millns B. et al. (2003). Acute Stroke Predisposes to Oral Gram-negative Bacilli-A Cause of Aspiration Pneumonia, Gerontology, 49: Naidoo R & Nella M. (2004). Dysphagia and Stroke, Thunder Bay Health Sciences Centre. Platt J. (2001). The Art of Dysphagia Management (Workshop Handout), Jerrilynn Platt Clinical & Educational Services: Hamilton. Platt J. (2001). Dysphagia Management for Long-Term Care: A Manual for Nurses and Other Healthcare Professionals. Clinical and Educational Services: Hamilton, ON. Platt J. (2006). Self directed program for feeding certification. Sloan H. (2005). Assessment and Treatment Strategies for the Management of Dysphagia in Stroke Patients, West GTA Stroke Network: Toronto, ON.
180 Sloan H & Haber-Lazar J. (2004). Assessment and Treatment Strategies for the Management of Aphasia and Dysphagia in Stroke Patients. West GTA Stroke Network: Toronto, ON. Steele C. & Coyle J. (2008). Oropharyngeal Dysphagia Assessment and Treatment Efficacy: Setting the record straight. (Response to Campbell-Taylor). University of Toronto: Toronto, ON Steele C. (2004). Best Practices in Videofluoroscopic Assessment and Rehabilitative Intervention for Acquired Neurogenic Oropharyngeal Dysphagia: an Advanced Course for Speech-Language Pathologists. Glenrose Rehabilitation Hospital: Edmonton, AB Teasel R, Foley N, Martino R, Bhogal S & Speechley M. (2008). Evidence-Based Review of Stroke Rehabilitation: Dysphagia. Heart and Stroke Foundation of Ontario.
181 NEO Stroke Network s Acute Nursing Certification Program MODULE SIX Swallowing, Feeding and Oral Care QUIZ You may use your binder as a reference to answer these questions Submit your completed quiz to the Nurse Clinician or designate for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
182 DATE: NAME: 1. What percentage of acute stroke patients have some degree of dyphagia within 72 hours after a stroke? a. 25% b. 50% c. 60% d. 80% 2. Acute stroke patients are to remain NPO until swallowing ability has been determined. These patients: a. May have ice chips b. May have po meds with sips of water c. May have nothing by mouth d. Require regular mouth care I) A and B II) A, B and C III) C and D IV) B and D 3. Dysphagia is the a. Loss or impaired ability to chew and/or swallow. b. Inability to comprehend spoken language. c. Loss of expressive oral ability. d. Motor planning impairment about the mouth. 4. Complications associated with dysphagia may include: a. Malnutrition and dehydration. b. Reduced quality of life. c. Aspiration pneumonia and airway obstruction. e. All of the above
183 5. During a normal swallow, the food is chewed and mixed to form a bolus during the: a. Pharyngeal phase b. Esophageal phase c. Oral phase d. Peristalsis phase 6. During a normal swallow, the pharyngeal phase is a. Voluntary b. Involuntary/reflexive c. A physiological response to aspiration d. Often accompanied by coughing 7. List 5 common signs that your stroke patient is having difficulty swallowing points Briefly explain Silent Aspiration: 1 point 9. What may not occur when a patient aspirates silently?
184 10. A Minced Diet means the food is: a. Cooked soft b. Nectar thick c. The consistency of ground meat d. Blended like a purée 11. Proper oral care MUST INCLUDE: a. Entire mucosa b. Sulci (spaces between the cheeks and gums) c. Teeth and tongue d. All of the above TRUE/FALSE Questions (CIRCLE the correct letter) T F T F T F T F T F 1. Oral medication or ice chips can still be given even if a Dysphagia Screening tool (such as TOR-BSST or STAND) has been deemed a fail. 2. Thickened fluids are one way to prevent dehydration when dysphagia is present in a stroke survivor. 3. Feeding a patient while they are lying down is okay as long as they are comfortable. 4. All stroke survivors should be screened for dysphagia as soon as they are awake and alert and before ANY oral intake is allowed. 5. Presence of a gag reflex does not protect against aspiration. SCORE: / 20 Stroke Unit/Medical Unit Nurse Clinician/designate (signature)
185 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE SEVEN Mobility and Positioning Upon completion of this module, nurses will have reviewed: What They Need to Know about Stroke Survivors before Starting to Mobilize them General Principles to Follow when Assisting the Stroke Survivor Key Principles of Body Mechanics for Positioning, Mobilizing and Transferring Stroke Survivors The Hemiplegic Shoulder and How to Prevent Injury Positioning Techniques Bed Mobility Techniques Transfer Techniques Ambulation Assistance
186 NEO Stroke Network s Acute Nursing Certification Program MODULE SEVEN Positioning, Mobility and Transfers Self Learning Program NEO Stroke Network Developed April
187 Positioning, Mobility and Transfers The goal of assisting the stroke survivor is to maximize functional recovery and promote independence of movement in a safe manner. Who Are You Working With? You are working with a population with a unique set of impairments that influence every aspect of their lives. Some may require a high level of assistance in their care, others less so. Communicating with your stroke survivor and observing how they respond and move will help you see how the impairments affect their ability to participate. How you Position, Mobilize and Transfer a Stroke Survivor is KEY in: preventing pain or injury encouraging safe active participation contributing to normal movement increasing independence 2
188 General Principles of What You Can Do? Therapy is an ongoing activity and you are a key member of the team participating in the recovery process. Here are some general principles to follow when assisting your stroke survivor. Use a personalized approach for each stroke survivor. Each survivor will be affected differently. Take your time to observe what they are doing and how you could assist them. Use a problem solving approach, there is no set recipe to follow. Interact with the stroke survivor and use simple, clear instructions. You may need to demonstrate the action. Check to see they have understood. The survivor s brain needs time to think and plan what is about to happen. Do not rush! Moving slowly and gently, give time to prepare, this will allow the stroke survivor to participate more successfully. A calm and supportive approach will help to keep muscle tone down and the survivor from fatiguing due to anxiety. Assist only as needed; coordinate your efforts with the survivors to maximize success. Knowing your survivor s abilities and limitations this will assist you in knowing whether verbal coaching, guidance or assistance is needed. Recognize that the stroke survivor s energy levels can change throughout the day. Do not attempt to assist a person alone if you are unsure of what they can do. Ask for standby assist or someone to assist with the task. When a second caregiver is required coordinate your efforts, to ensure safety. Communicate with the team, you are all working together to achieve the stroke survivors goals. Ensure that you are aware of equipment required, amount of assistance to provide for mobility. Communicate with the family about what they can safely do to assist with their family member, provide education about activity and rest. The shoulder can easily be injured, handle very carefully, use a sling if indicated. 3
189 Maintain good posture: crucial for being in control of the manouver, protects your back, ensures the correct muscles are involved in the manouver. Engage your core muscles: excellent support for your back Good base of support: you will be in better control and balanced. Reduce distance between you and the load : get close, don t reach, the forces on you will be lighter if the lever arm is short Communicate clearly: 1,2,3 GO Prepare environment: move bedside table, set up chair position, lower side rails The Hemiplegic Shoulder Before we review positioning, mobility and transfers for stroke survivors, it is important to learn about the hemiplegic shoulder. The Normal Shoulder: Contributes to functional movement, affecting transfers, balance, ADL s and hand function Has a large range of motion which contributes to speed, power, coordination and fine motor control Is vulnerable to injury as the sacrifice for this increased range of motion is decreased stability 4
190 The shoulder or glenohumeral (GH) joint: is a joint between the rounded humeral head and shallow saucer like surface of the glenoid fossa. The humerus is supported by muscles, ligaments and a capsule. There are no bony attachments. This is why it is so versatile in function yet so vulnerable to injury. Rotator cuff muscles are attached to and act on the head of the humerus. Rotator cuff muscles guide the humeral head through rolls and glides to allow normal movement of the shoulder through all of its range of motion. 5
191 Stability The shoulder is protected by muscles and the capsule. Alignment Correct alignment is also required for normal movement. Proper alignment of the humeral head is dependent on normal activity of scapular, rotator cuff, trunk muscles which keep the bones in their proper positions in order to move correctly. Rotator cuff muscles provide dynamic stability; these muscles move the arm but also provide stability to the joint through their actions. The capsule is a tough band of tissue that surrounds the shoulder joint. It does not move the arm so it provides static stability. So What Does all this Mean? Normal Shoulder Movement requires: muscles, ligaments and capsule to all be functioning correctly Proper alignment of bones, joints and muscles Stability of the joints Movement of muscles and joints to be occurring properly 6
192 In the Hemiplegic shoulder there are changes that put the shoulder at risk of injury. Up to 72% stroke survivors report an incidence of shoulder pain within the first year of their stroke. It can start as early as 2 weeks post stroke to 2-3 months later. Shoulder pain c an affect the functional recovery of the arm and hand, sleeping and contribute to depression. In the Hemiplegic Shoulder Changes in muscle tone Tone is the resting state of the muscle Affects all the muscles on the affected side that contribute to movement. If these muscles are floppy or very tight it changes the positioning of the bones = change in alignment A decrease in tone leads to a flaccid or floppy state (arm will feel heavy and has l ittle or no muscle activit y) If the muscle is floppy the weight of the arm can stretch the soft tissues = loss of stability, risk for tissue injury An increase in tone leads to a spastic or excited state it will feel stiff ( it will be more difficult to move the joint through its range) If the arm is tight, it can lead to loss of range of motion and development of contractures The can be a loss of the normal joint spaces available for movement in the shoulder. This could lead to pinching of tissues causing irritation and inflammation with forced movement = pain Change in posture Trunk muscles can also be weakened affecting posture. Trunk alignment is important as many of the muscles that act on the scapula and humerus are attached to the spine and ribcage Change in trunk alignment affects the position of the scapula and glenoid fossa =change in alignment and biomechanics Poor alignment can lead to pain with forced movement 7
193 Weakness Muscle weakness can affect Lack of muscle activity or muscle all muscles on one side of pump can lead to edema in the arm the body. or hand. There may be varying amounts of weakness in different limbs. Edema contributes to stiffness of the joints and pain with movement. There may be good strength in the leg but no movement in the arm. Can lead to lack of stability and loss of protection of the joint. Affects alignment in shoulder girdle affecting movement patterns can cause tissues to be pinched Causes the weight of the arm to pull down and lead to tissues being stretched, torn, inflamed Can lead to subluxation, which is the dropping of the head of the humerus down the glenoid fossa. This can be a painful condition. Loss of awareness This is called inattention or They may not see things placed on neglect whereby the person their affected side is not aware of the affected side of the body or The arm and hand can be left in positions where: environment on that side of circulation is compromised the body tissues are put on prolonged stretch skin can be burned, caught between objects or injured in other ways 8
194 With these changes in the hemiplegic shoulder it is important to know Stretched capsular tissue, ligaments and muscles are not correctable conditions. These tissues remain in a lengthened state. Subluxation is not correctable. Pain is difficult to treat and leads to further loss of movement and potential functional recovery As Primary Caregivers PREVENTION IS KEY..We Can: Prevent tissue damage Prevent pain Maintain good joint alignment and muscle length Good handling Good positioning Use of appropriate aids and equipment Use Good Handling Techniques Prepare the person for transitional movements or handling of the arm Tell them what you are going to do to promote awareness of the arm Involve them in protecting the arm by bringing their attention to the arm activity Support the arm at both the upper arm and wrist. Never lift the arm by the hand, it does not take any weight off of the shoulder joint and will cause stretching of soft tissues. and 9
195 Never lift through the axilla or pull on the arm. You are asking an unprotected joint to support body weight which will cause injury. During bathing and dressing support the arm and move the joints gently. The body will respond to how you handle it. Quick movements will increase tone and can cause pain. Keeping movements slow and gentle can reduce tone and stimulate activity. Range of motion exercises should not be done unless you have been instructed by a therapist on proper technique. Use Appropriate Aids and Equipment Use a sling when transferring or standing a person, to support the weight of the arm After the support is in place at the hemiplegic elbow (1), slide the sling around the back, and up to the opposite shoulder, coming over in front of the chest and down to the hemiplegic wrist to secure the second support cuff (2)
196 When the person is sitting, support the arm on a lap tray, arm trough, pillow or table Positioning Proper seating assists with achieving good trunk alignment and position of the shoulder and arm This helps maintain muscle length, limit changes in tone and reduce contractures in the shoulder and arm Elevate the hand to reduce edema. This can be achieved in supine or sitting 11
197 The shoulder girdle is a complex system but being aware of potential complications and utilizing good positioning and careful handling techniques, can minimize problems too often seen with the hemiplegic shoulder. Positioning the Stroke Survivor Positioning of your stroke survivor is important to prevent many secondary problems and maximize recovery. Goals of positioning are: Support the affected limbs Prevent and manage pain Support muscles and prevent abnormal tone patterns Maintain skin integrity Increase awareness of the affected side Promote body symmetry and alignment Comfort Prevent joint and muscle stiffness 12
198 Positioning Stroke Survivor on Their Back When you position your stroke survivor, the key principles are to: support limbs, maintain good alignment and provide comfort. The head should be aligned in neutral position, not tipped or turned but in line with the body. You can use a small towel under the pillow to support good alignment of the head. No less than 30 º HOB The affected arm should be positioned away from the body, with the elbow straight and the elbow crease facing up The affected hand is elevated to reduce/prevent swelling. Separate the fingers. The affected leg should be level at the pelvis with the unaffected leg. You can level the hips with a towel or flat pillow under the affected hip. To reduce pressure on the heels, the knees can be bent and supported with a folded pillow but only for a short time so as to not encourage knee flexion stiffness. Caution: ensure that pillows or towels are not cutting off circulation or increasing pressure on the skin. Ensure that there are no wrinkles in the sheets to prevent skin breakdown. 13
199 Lying on the affected side: The head aligned in neutral position. Do not have the stroke survivor lie directly on top of the affected shoulder. Draw the shoulder complex out by gently bringing the shoulder blade slightly forward. Support the arm on a pillow with the elbow bent and resting away from the body or with the arm out straight (as in the photo below). For the legs, have both knees bent with the bottom leg slightly forward, pillow between knees to provide good alignment and prevent pressure points on bony areas. Support the trunk with a pillow lengthwise behind the back. Lying on the unaffected side: Head aligned in neutral position Do not lay the patient directly on the shoulder. Place the bottom shoulder in a slightly forward position. Support the affected arm on 2 pillows to keep the arm from dropping down and pulling on the shoulder. Elevate the hand as needed with fingers spread. 14
200 Keep the bottom leg straight, the top affected leg bent and supported on a pillow slightly forward Support the trunk with a pillow tucked in lengthwise behind the back Once you have positioned your stroke survivor, it is important to check on them regularly, to reposition every 2 hours or more frequently if needed if they are not able to move themselves, in order to reduce the risk of pressure sores. Mobilizing Mobilizing involves moving in bed, sitting up, standing and walking. Mobilizing your stroke survivor is a key component of best practice stroke care. Stroke survivors should be assisted to move as early and as frequently as possible. If bed rest is ordered, ensure this is reassessed after 24 hours. Once bed rest is discontinued, patients must be mobilized. 15
201 It is the nurse s responsibility to initiate the mobilization of the acute stroke patient. Don t wait for the physiotherapist or occupational therapist to begin mobilizing the survivor into a dangle position or a transfer to the bedside chair. It is important to remember, however, that two people are required to initially mobilize the stroke patient. An RN or RPN should be present during this first transfer. Within 48 hours, the physiotherapist or occupational therapist should assess the stroke survivor s ability to mobilize and will direct the type of transfer to be used by all staff and the amount of assistance required. Throughout the patient s inpatient stay, consult with other members of the team as available if you have questions or concerns about the stroke survivor s mobility. When mobilizing the stroke survivor, always keep in mind: Safety and comfort Encouragement or assistance is aimed at enhancing normal movement. Promotion of independence Mobility is Important for: Prevention of secondary complications of DVT Skin integrity Maintaining or improving function Preventing contractures Decreasing pain Improving mood 16
202 Survivors may not be able to learn to use the affected side normally due to spasticity or difficulties with motor control. What assistance you provide is specific to each survivor based on their needs and abilities. Bed Mobility Moving and repositioning the stroke survivor in bed or in their chair is essential to: good skin care assisting with awareness of the body maintaining good alignment of the body early mobilization. Rolling to the Affected Side When rolling to affected side, ensure that affected arm is slightly forward so to prevent rolling onto the shoulder Stand on weak side of patient and remove side rail Tell patient to bend their stronger leg and use it to help roll. To roll, assist the stroke survivor by helping at the back of the shoulder and hip as needed. Encourage them to roll themselves as much as possible by turning their head and reaching over with the unaffected arm 17
203 Rolling to the Unaffected Side When rolling to the unaffected side, ensure the affected arm is supported, the stroke survivor can support their arm and bring it across their body Remove side rail and stand on good side. The good leg remains straight Help the patient bend the affected leg Assist the stroke survivor to roll by helping at the back of the shoulder and hip as needed. Encourage them to roll themselves as much as possible by turning their head, pushing with the leg and drawing their affected arm across their body To Reposition the Stroke Survivor in the Bed Remove pillows, lower bed rails, adjust height of bed and lower head of bed Ensure the wheelchair brakes are applied Stroke survivor can tuck chin and may be able to help if their legs are bent (may need help getting their affected leg into this position) Remember that a draw sheet or slider sheet can help You should not be lifting shift your weight toward the direction you are moving, your feet should be apart, with back straight and knees bent - count GO with your partner Use a mechanical lift if the stroke survivor cannot assist with the repositioning Sitting up from Side Lying Depending on the patient s ability, a second nurse or PSW may be needed to assist with either the legs or the trunk. From side lying, bend the hips and knees, let the legs come over the edge of the bed, scoop under the shoulder and ask the stroke survivor to lift their head and push up with their arms 18
204 (The head of bed can be raised to get a head start) You can assist by applying a bit of pressure to the top of the pelvis to help lever them up Don t forget to use good body mechanics, lift with your legs and keep your core muscles engaged Finally, lower the bed to ensure the stroke survivor s feet touch the floor to assist with sitting balance Assess their ability to sit unsupported without leaning or falling, as this will dictate whether you can proceed with a 1or 2 man transfer or need a mechanical lift Sit to Stand Feet should be flat on floor with balls of feet under knees Apply transfer belt snugly Support a flaccid arm with a hemi-sling Cue the stroke survivor to bring shoulders forward over knees with back straight and head up Always count together or communicate in some way so that you will both start moving at the same time You provide supervision/cueing, minimal guidance or assistance using the transfer belt as required to complete the stand Transfers Transfers are important to start early mobilization of the stroke survivor out of bed and into a chair, onto a commode or onto the toilet. How you transfer the stroke survivor depends on a few key points. 19
205 What to consider before mobilizing: Is the stroke survivor able to move themselves in the bed i.e. roll to side or shift their hips? Is the stroke survivor able to maintain sitting up independently or are they constantly falling to the side or backwards? Are they able to stand? Are they able to understand and follow directions? Are they aware of the affected side of the body and the environment on the affected side i.e. do they turn their head to both sides, do they look at you when you speak to them from the affected side, are they aware of where the affected arm is are they supporting it or is it caught behind or underneath them? What is their fatigue level? Mechanical Lift Transfer Consider if the stroke survivor: Is unable to maintain sitting without moderate to maximal support. Has significant dizziness or poor sitting balance Cannot follow directions to assist with a safe transfer Does not move well in bed 20
206 Two Man Transfer Consider if the stroke survivor: Is able to sit with minimal support Has been up to a chair already Is ambulatory with the therapists Is able to follow instructions to participate in the transfer but will need physical help Is able to move themselves in bed i.e. roll, bridge which shows they have some recovery to assist in a transfer The stroke survivor will require two people to assist if one person is needed to assist them to a stand position using a transfer belt while a second person is required to assist with turning the hips to the chair, preventing the trunk from falling back and guiding them back into the chair safely. Transfer to the Stronger Side Put the stroke survivor s shoulder sling on if they are unable to use the arm to assist Ensure wheelchair is positioned at a slight angle to the bed so that the corner of the chair touches the bed on the survivor s stronger side Ensure the wheelchair s armrest and foot rests are removed (if applicable) and the brakes are on Ensure the stroke survivor is sitting with the balls of his/her feet under their knees, turn the stroke survivors heels in the direction you want to go Put transfer belt on snugly, ensure it is on snug so that is does not slide up. If a feeding tube is present, apply the belt above the tube to prevent dislodging the tube. Ask the stroke survivor to bring shoulders forward over their knees but still keeping their back straight and head up 21
207 Ask the stroke survivor to push up from the bed and you assist as needed to stand and guide the turn to transfer A second person behind can guide the hips to the chair and make sure they don t lean or fall backward The stroke survivor can then wiggle hips back into the chair Transfer to the Weak Side (more difficult) A stroke survivor who transfers with the assistance of two people, will find moving to the weak side very difficult so this should be avoided whenever possible In some cases like transferring on or off the toilet in a small washroom, it can not be avoided Be sure the stroke survivor is strong enough and stable enough to perform a transfer to the weak side Be prepared to offer more assistance to initiate the turn and the descent to a sitting position The sit-to-stand component is the same as other transfer One Man Transfer Consider if the stroke survivor: Is able to move themselves in bed and sit themselves up on the side of the bed Is able to stand with minimal assist Is able to follow instructions to transfer safely Once seated at the side of the bed, apply the transfer belt Ask the stroke survivor to bring shoulders forward over their knees but still keep their back straight and head up 22
208 As in the other transfers, the balls of the feet must be under the knees, feet flat on floor and ready to accept weight Their hand(s) start out placed on the bed to assist by pushing off the bed THEN reaching toward the arm rest of the chair. You may need to help moderately or minimally depending on their ability, be in front of them and be ready to offer moderate help as needed. If the patient performs poorly and moderate help will not be sufficient to safely complete the transfer, sit the stroke survivor back down and get help from a colleague to perform a two man transfer. Walking Before walking the stroke survivor, check if the stroke survivor is: able to follow instructions moving well in bed able to sit up and transfer with minimal assist able to take weight on their affected leg Stand on the affected side clearing the floor with their affected foot already walking with therapists Use a transfer belt for support as needed (do not hold onto the affected arm) Have the appropriate walking aid ready (consult with therapists if not known) Put on good footwear (sloppy slippers provide no stability and can cause falls) Use a sling if necessary to support the hemiplegic arm 23
209 Before walking ensure balance is stable while standing with weight distributed over both feet, not leaning to one side Ensure they are standing with the hip, knee and ankle inline in order to weight bear and balance effectively Look forward so you have good posture Check if the foot clears the floor during each step and is flat on the floor when standing and not rolling over Encourage attention to safety when walking in room or hallway Provide any needed verbal cueing for safety i.e. to slow down, be careful of foot placement, keep head up, not to place the walking aid too far ahead etc. 24
210 Module Seven Positioning, Mobilizing and Transferring a Stroke Patient REFERENCES Hôpital régional de Sudbury Regional Hospital. Using Proper Body Mechanics %20Injury.pdf Hôpital régional de Sudbury Regional Hospital (2008). Occupational Health and Safety Educational videos. Retrieved from isordermsdprevention/tabid/2138/default.aspx Hopital regional de Sudbury Regional Hospital (2008). MSD Prevention Policy and Procedure, Occupational Health and Safety. Retrieved from Occupational Health Clinics for Ontario Workers Inc Health Care Workers Patient Handling. Retrieved from Taipalus, L. (2009). Lecture: Nurse s Best Practice Workshop. Hemiplegic Shoulder (Power point presentation). Taipalus, L. (2009). Lecture: Nurse s Best Practice Workshop. Key Principles of Body Mechanics and Transfers. (Power point presentation). The South East Toronto Stroke Network. Positioning, Transfer and Mobility of the Stroke Survivor DVD: Facilitator s Guide. Toronto, ON.
211 NEO Stroke Network s Nursing Certification Program MODULE SEVEN Mobility and Positioning Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the designated Nurse for marking Your test will be returned to you to keep in your binder NEO Stroke Network Developed April 2010
212 DATE: NAME: 1. The goal of assisting the stroke survivor is to functional recovery and independence of movement in a safe manner. (fill in blanks) 2. You can put your stroke survivor at risk of injury when a) You use the appropriate equipment b) You rush the stroke survivor during the task c) You are not familiar with the stroke survivors limitations d) You provide clear instructions and ensure that they are understood Choose answer: i) a) and b) ii) c) and d) iii) b) and c) iv) all of the above 3. Taking the time to become familiar with the stroke survivor s impairments and how to best assist them a) will decrease the risk of injury to the stroke survivor and yourself b) contributes to ongoing therapy c) can reduce any anxiety or stress the stroke survivor has during movement d) allows you to complete tasks quickly without having to communicate with the client
213 Choose Answer: i. a) b) d) ii. b) c) d) iii. a) b) c) 4. Which of the following are key principles of body mechanics? a) Using your core muscles can help to protect you from injury when mobilizing stroke survivors b) Move quickly to decrease stress on muscles and joints c) Decrease your lever arm and have a good base of support d) Prepare the stroke survivor and your environment for activity Choose Answer: i. all of the above ii. a), b), d) iii. a), c), d) iv) b), c), d) 5. Which statement is most accurate when it comes to Key Principles of good body mechanics and patient safety in rolling a patient to their side? a) It is good practice to keep your back straight lean over the bed rail as you roll your patient towards you. b) It is good practice to raise the bed, lower the bed rail and pull your patient towards you. c) It is good practice to raise the bed, lower the bed rail and communicate with your patient what you would like to do and instruct them in how to assist in rolling to their side. d) It is good practice to raise the bed, lower the bed rail and communicate with your patient what you would like to do and instruct them in how to assist in rolling to their side. You assist by pulling on their affected arm to help roll them. e) None of the above
214 6. The shoulder can be injured by: a) The weight of the unsupported arm pulling down when sitting up in a wheelchair b) Improper technique when doing range of motion c) Pulling on the arm to roll someone in bed d) Transferring by lifting under the axilla of the affected arm Choose answer: i. a), c), d) ii. b), c), d) iii. a), b), c) iv. all of the above 7. When positioning the stroke survivor it is important to: a) Promote good alignment b) Support the affected limbs c) Ensure comfort d) Check on them regularly to ensure the above e) All of the above 8. When assisting the stroke survivor to sit up from side-lying: a) Adjust the height of the bed b) Ensure you have a good base of support c) Bend forward at the hips d) Stay close to the stroke survivor e) Bend your knees and shift your weight in the direction you are moving Choose answer: i. All of the above ii. a) b) c) d) iii. a) b) d) e)
215 iv. b) c) d) e) 9. Asking the stroke survivor to assist with rolling promotes a) body awareness b) early mobilization for standing and transfers c) increased risk of injury to staff d) increased independence in bed mobility e) all except c) 10. When assisting the stroke survivor to walk, it is best to: a) Stand on the unaffected side and hold onto their arm b) Stand behind the stroke survivor by holding onto the transfer belt c) Stand on the affected side and hold onto the affected arm d) Stand on the affected side and use the transfer belt for support as needed 11. What key things do you consider before deciding on which transfer to use? a) Ability to understand instructions b) Ability to sit up c) Size and weight of the stroke survivor d) Ability to weight bear e) All of the above 12. Mr. Smith is unable to speak but can understand instructions. He is able to sit up independently and maintain sitting at the side of the bed. He has had good recovery in his right leg but very little in his right arm. He would be suitable for a: a) 2 person transfer b) 1 person transfer 13. What equipment would you use to transfer Mr. Smith? a) Lift b) Transfer belt
216 c) Walker d) Hemi arm sling e) Sliding board Choose answer: i. a) and d) ii. b) and c) iii. b) and e) iv) b) and d) 14. Mrs. Jones has had a severe stroke and presents with neglect of the left side, flaccid left arm and leg. She tries to pull herself over to her right side when asked to roll to the left. How would you transfer her? a) Mechanical lift b) 2 person transfer TRUE AND FALSE QUESTIONS: Circle the correct word. 15. True or False A stroke survivor may not be aware of their deficits. 16. True or False A stroke survivor s ability to transfer can change throughout the day due to fatigue. 17. True or False The hemiplegic shoulder sling goes under the affected arm and over the opposite shoulder 18. True or False It is good practice to ask the stroke survivor to assist in moving or supporting the affected arm during ADLs. 19. True or False The stroke survivor should never lie on the affected side. 20. True or False Early mobilization is important for skin, circulation and recovery, once the stroke survivor is medically stable. SCORE: / 20 Stroke Unit/Medical Unit Nurse Clinician/Designate (signature)
217 NEO Stroke Network s Acute Nursing Certification Program LEARNING OBJECTIVES MODULE EIGHT Secondary Stroke Prevention Upon completion of this module, nurses will be able to: Explain Modifiable and Non-Modifiable Risk Factors Identify Key Aspects of Secondary Stroke Prevention (including the role of diet, sodium, exercise, weight, smoking, alcohol, hypertension and hyperlipidemia) Identify Best Practices for Carotid Stenosis Interventions Identify Commonly Prescribed Medications for Stroke and Stroke Prevention Understand TIA Explain the Role of the Secondary Prevention Clinic Learn Key Points for Teaching Stroke Patients about their Medications
218 NEO Stroke Network s Acute Nursing Certification Program MODULE EIGHT Secondary Stroke Prevention Self Learning Program NEO Stroke Network Developed April 2010
219 PRIMARY STROKE PREVENTION is an individually-based clinical approach to disease prevention. It targets otherwise healthy individuals with modifiable risk factors to prevent the initial occurrence of a disease. It is typically implemented in the primary care setting. SECONDARY STROKE PREVENTION is an individually based clinical approach to reduce the risk of further vascular events in: 1) An individual who has experienced a stroke or transient ischemic attack (TIA) 2) An individual who is at high risk of stroke due to underlying medical conditions or risk factors Heart & Stroke Foundation of Canada, 2008 In the 2008 Canadian Best Practice Recommendations for Stroke Care, Prevention of Stroke is Recommendation #2. The section covers: 2.1 Lifestyle and Risk Factor Management 2.2 Blood Pressure Management 2.3 Lipid Management 2.4 Diabetes Management 2.5 Antiplatelet Therapy 2.6 Antithrombotic Therapy for Atrial Fibrillation 2.7 Carotid Intervention 2.1 Lifestyle and Risk Factor Management Persons at risk of stroke and patients who have had a stroke should be assessed for vascular disease risk factors and lifestyle management issues They should receive information and counselling about possible strategies to modify their lifestyle and risk factors (CMAJ 2008; 179, E1-E93) 2
220 STROKE RISK FACTORS that are NON-MODIFIABLE Age (note: After age 55 the risk of stroke doubles in each successive decade) Gender (note: prior to menopause, stroke is more prevalent in men) Race/Ethnicity (note: More prevalent in Black Americans, Hispanic, Japanese and Chinese) Family History (2 times more likely to have a stroke if you have a family history) Previous TIA or Stroke STROKE RISK FACTORS that are MODIFIABLE Hypertension Smoking Diabetes Hyperlipidemia Atrial Fibrillation Cardiac Disease Obesity Physical inactivity Excessive alcohol intake Stress Hormone Replacement Therapy TIA (if history of TIA, management of the above risk factors could prevent another one) Modifiable risk factors are those over which an individual has some control; factors he/she can modify in order to reduce the risk of stroke. 8 out of 10 individuals have at least one of the following risk factors: smoking, physical inactivity, obesity, hypertension or diabetes. 1 out of 10 has three or more. Preventative measures aimed at reducing these risk factors will not only prevent strokes but will also prevent other chronic diseases which share similar risk factors. 3
221 Lifestyle and Risk Factor Management i) Diet and Sodium ii) Physical Activity iii) Smoking iv) Alcohol i) A healthy balanced diet should be in accordance with Canada s Food Guide to Healthy Eating and limit sodium intake from all sources according to the amount considered adequate by age consider the adequate sodium intake for most adults is 1500 mg per day Gender Men Women Average Daily Sodium Intake 3575 mg 2680 mg Source: Blood Pressure Canada 2007 the average daily sodium intake is well beyond the upper limit daily intake shouldn t exceed 2300mg (This is only 1 teaspoon!) Simply getting rid of the salt shaker is not enough! Most of our sodium intake is hidden in processed foods, therefore we need to eat much less than a teaspoon of added table salt a day. Becoming familiar with reading nutrition labels will help make healthy food choices: More information is available at sodium101.ca 4
222 ii) Physical Activity should include Daily moderate exercise (brisk walking, jogging, cycling, swimming) Accumulation of 30 to 60 minutes daily, four to seven days of the week (in addition to activities of daily living) Medically supervised programs recommended for high risk patients (e.g. those with cardiac disease) Benefits of Physical Activity include better lipid values, especially HDL and TG, better blood glucose control, a lower BP, more energy, lower stress level, weight control, and improved immune system. Weight Management Maintain goal of a body mass index (BMI) of 18.5 to 24.9 kg/m2 (BMI is weight divided by height squared) Overweight defined as a BMI between Obesity BMI >30 BMI > 40 defines severe or extreme obesity Maintain goal of a waist circumference of less than 88 cm for women less than 102 cm for men Waist circumference is an index of the absolute amount of abdominal fat. Abdominal obesity should be measured as it plays a critical role in the etiology of metabolic syndrome (increased waist circumference, raised triglycerides, decreased HDL, increased BP and raised fasting glucose) Clear evidence exists that obese individuals are at increased risk of health problems, including stroke, heart disease, type 2 diabetes, osteoarthritis and certain cancers. (2006 Canadian Clinical Practice Guidelines on the Management and Prevention of Obesity in Adults and Children) 5
223 iii) Smoking Recommendations include smoking cessation programs and smoke-free environments Initiate nicotine replacement therapy and behavioural therapy Cigarette smoking causes more deaths in Canada from heart disease and stroke than cancer (HSFO, 2000) Smoking doubles the risk of ischemic stroke and is associated with a 2-4 fold increase in hemorrhagic stroke (Goldstein et al, 2006) Those who smoke heavily (more than 40/day) have 2 times the relative risk of stroke than those who are light smokers (less than 10/day) (Thom et al, 2006) Integrating Smoking Cessation into Daily Nursing Practice (Nursing Best Practice Guidelines, visit Window of opportunity in the hospital setting to intervene or at least introduce the notion of not resuming tobacco on discharge Nurses could implement minimal tobacco use intervention using the Ask, Advise, Assist, Arrange protocol with all clients 5 A s Model for Treating Tobacco Use and Dependence (Clinical Practice Guidelines for Treating Tobacco Use and Dependence: 2008 Update) Ask about tobacco use Advise to quit Assess willingness to make a quit attempt Assist in quit attempt Identify and document tobacco use status for every patient at every visit In a clear strong, and personalized manner, urge every tobacco user to quit Is the tobacco user willing to make quit attempt at this time? For the patient willing to make a quit attempt, offer medication and provide or refer for counselling or additional treatment to help the patient quit. 6
224 For patients unwilling to quit at the time, provide interventions designed to increase future quit attempt. Arrange follow-up For the patient willing to make a quit attempt, arrange for followup contacts, beginning within the first week after the quit date For patients unwilling to make a quit attempt at the time, address tobacco dependence and willingness to quit at the next visit Smoking Cessation Interventions: Nicotine Replacement Therapy (NRT) (patch, gum, inhaler, lozenges, nasal spray) Nicotine Receptor Partial Agonists (Varenicline - Champix) Bupropion SR Counselling Smoker s Helpline (visit Withdrawal symptoms include: initially anger, impatience, restlessness, difficulty concentrating, insomnia, increased appetite and anxiety and depressed mood. Symptoms can begin a few hours after last cigarette and peak 2-3 days later and continue over a period of several weeks or months. (JAMA 1999, Hughes) NRT goal is to assist in the transition from smoking to abstinence by decreasing withdrawal symptoms and motivation to smoke (Stead et al, 2009-Cochrane Review) iv) Alcohol Consumption Recommendations include two or fewer standard drinks per day Fewer than 14 drinks per week for men Fewer than 9 drinks per week for women 7
225 A standard drink is 5oz of wine, 12oz of beer or 1.5oz of spirits Heavy drinking (more than 5 drinks per day) has been associated with the risk of hemorrhagic stroke. Irregular and binge drinking (more than 5 drinks at one time) has been associated with an increase risk of hemorrhagic stroke 2.2 Blood Pressure Management Hypertension is the single most important risk factor for stroke Blood pressure should be monitored in all persons at risk for stroke Canadian Hypertension Education Program (CHEP) states that about 25% of adult Canadians are hypertensive and with current lifestyles over 90% will develop hypertension Blood pressure increases with age Blood pressure should be checked with each encounter with the health care system CHEP guidelines should be followed for a comprehensive treatment plan that includes identification of other risk factors, lifestyle modification, pharmacotherapy and ongoing monitoring CHEP 2008 Recommendations for the Management of Blood Pressure Condition Prevention of first stroke in general population Recommendation Target: 140/90mmHg Patients who have had a stroke/tia Target: <140/90mmHg Patient with diabetes for prevention of first stroke/tia Target: 130/80mmHg Non-diabetic chronic kidney disease Target: <130/80mmHg 8
226 Ideally the targets should be even lower and studies are underway to better define the appropriate lower target rate for stroke patients. Nursing Best Practice Guidelines (revised 2009) Manual includes: The detection and diagnosis of hypertension Using correct cuff size Education for clients about home BP monitoring Education for clients on their target BP and importance of achieving this target Assessment and Development of a Treatment Plan 1) Lifestyle interventions help to identify lifestyle factors which may influence hypertension management 2) Diet-instruct DASH diet (Dietary Approaches to Stop Hypertension) 3) Healthy weight-weighing clients, calculating BMI and measuring waist circumference 4) Exercise guidelines 5) Alcohol consumption 6) Smoking cessation 7) Stress reduction Pharmacological Treatment of Hypertension Thiazide-like diuretic such as Lasix and Hydrochlorothiazide ACE (Angiotensin Converting Enzyme) such as Altace and Prinivil ARB (Angiotensin ll Receptor Blocker) such as Diovan or Avapro Long-acting CCB (Calcium Channel Blocker) such as Cardizen and Norvase Beta-Blocker such as Labetalol or Atenolol These have all shown to reduce recurrent stroke and other vascular events. Most patients with stroke or TIA will benefit from treatment with a blood pressure lowering agent, regardless of the presence of hypertension. There is less evidence on the role of beta blockers and calcium channel blockers in the secondary prevention of stroke but there may be some benefit. 9
227 For secondary prevention, aggressive treatment of blood pressure is of greater benefit than more modest reductions. For patients with non-disabling stroke or TIA not requiring hospitalization, it is recommended that blood pressure lowering treatment be initiated or modified at the time of the first medical assessment. ****As stated in a previous module, there is lack of randomized controlled trials that define the optimal time to initiate blood pressure lowering therapy after acute stroke or TIA and each case must be assessed individually. *** 2.3 Lipid Management Best practice indicates that lipid levels should be monitored in all persons at risk for stroke. Dyslipidemia is a modifiable risk factor for atherosclerosis in which screening is imperative in order to identify risk and institute appropriate therapy for both primary and secondary prevention of CAD, PAD and stroke (Adams et al, 2008) Lipid Assessment Fasting lipid levels (TC, TG, LDL-C, HDL-C) should be measured every 1-3 years for all men 40 years or older and post menopausal women and/or 50 years or older, and more frequent with abnormal values or it treatment is initiated. Adults at any age should have their blood lipid levels measured if they have a history of diabetes, smoking, hypertension, obesity, ischemic heart disease, renal vascular disease, peripheral vascular disease, ischemic stroke, TIA or symptomatic carotid stenosis. (from Canadian Cardiovascular Society position statement-recommendations for the Diagnosis and Treatment of Dyslipidemia and Prevention of Cardiovascular Disease) Considered in the High Risk category is any patient with a diagnosis of CAD, PVD or cerebrovascular disease and most adult patients with type 1 or type 2 diabetes mellitus. It is important to implement the healthy Lifestyle Modifications outlined earlier to lower overall risk of stroke. 10
228 Ischemic stroke patients with LDL-C >2.0mmol/L should be managed with lifestyle modification, dietary guidelines. Pharmacological Treatment of Dyslipidemia Statins Atorvastatin (lipitor), Fluvastatin (lescol), Lovastatin (mevacor) Rosuvastatin (crestor), Simvastatin (zocor), Pravastatin (pravachol) Statin agents should be prescribed for most patients who have had an ischemic stroke or transient ischemic attack to achieve current recommended lipid levels. Possible effects of statins include the following: Anti-inflammatory properties may help to stabilize the lining of the blood vessels. Statins may help relax blood vessels thus contributing to lower blood pressure Statins may have a blood thinning effect thus reducing the risk of blood clots. Bile acid and/or Cholesterol Absorption Inhibitors Cholestyramine, Colestipol (colestid), Ezetimibe (ezetrol) Fibrates Bezafibrate (Bezalip), Fenofibrate (Lipidil Micro/Lipidil Supra/Lipidil EZ), Gemfibrozil(lopid) Niacins Nicotinic Acid 11
229 2.4 Diabetes Management Best practice indicates that All individuals in the general population should be evaluated annually for type 2 diabetes risk on the basis of demographic and clinical criteria. A fasting plasma glucose (FPG) should be performed every three years in individuals >40 years of age to screen for diabetes. (CMAJ 2008, Canadian Best Practice Recommendations for Stroke Care) Diabetes is a major risk factor for stroke and most adults with type 1 or 2 diabetes should be considered at high risk for vascular disease. Diabetes is a particularly strong risk factor in younger patients. Diabetes increases the risk of ischemic stroke more than hemorrhagic stroke. Many patients may exhibit metabolic syndrome and additional risk factors such as hypertension, hyperdyslipidemia which further increase the risk of TIA/Stroke. Reducing risk factors to target levels is essential and involves a multi-issue approach including lifestyle modifications, tight glycemic control, antiplatelet drugs (aspirin), control of lipid levels and blood pressure control. According to the Canadian Diabetes Association 2008, Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada, the recommended target for Glycemic Control is: A1C (Glycated Hemoglobin) < or = to 7.0 % FPG/AC (Fasting Plasma Glucose) = mmol/l 2 HR PG (Plasma Glucose) = mmol/l OR mmol/l if A1C targets not being met Diagnosis of Diabetes FPG greater than or equal to 7.0 Casual PG-equal to or greater than 11.0 mmol/l plus symptoms of diabetes (polyuria, polydipsia and unexplained weight loss) 12
230 Stroke Prevention for Diabetics Adults at high risk of a vascular event should be treated with a statin to achieve an LDL-Cholesterol 2.0 mmol/l. Unless contraindicated, low dose ASA therapy (80-325mg/day) is recommended in all patients with diabetes with evidence of cardiovascular disease and those with atherosclerotic risk factors. 2.5 Antiplatelet Therapy All patients with ischemic stroke or transient ischemic attack should be prescribed antiplatelet therapy for secondary prevention of recurrent stroke unless there is an indication for anticoagulation. (Stroke Best Practice Recommendations Update 2010) There is a 25% relative risk reduction in recurrent stroke for patients treated with ASA. (Antithrombotic Trialists Collaboration. BMJ 2002) There is also some evidence to support the use of alternative antiplatelet agents including extended-release dipyridamole plus ASA or clopidogrel. Long term use of combinations of aspirin and clopidogrel are not recommended Aspirin (ASA), combined ASA and extended release dypyridamole (Aggrenox), or clopidogrel (Plavix) may be used depending on the clinical circumstances. For adult patients on ASA, the usual maintenance dosage is mg/day. 2.6 Antithrombotic Therapy in Atrial Fibrillation Patients with atrial fibrillation at very low risk (CHADS2 = 1) should receive aspirin (ASA) ( mg/day). Patients with atrial fibrillation at low risk should receive either warfarin or dabigatran. ASA is a reasonable alternative for some low risk patients, depending on the individual and their case. Patients with atrial fibrillation at moderate to high risk of stroke (CHADS2 >=2) should receive warfarin or dabigatran. 13
231 Patients with non-valvular atrial fibrillation who are treated with warfarin should have a target INR of 2.5, range 2.0 to 3.0. For patients with AF and mechanical heart valves, the target INR is 3.0, range 2.5 to 3.5). For those patients treated with Dabigatran, a dose of 150 mg twice daily is appropriate for most individuals. (A dose of 110 mg is recommended for patients aged 80 and over or those at risk of bleeding). (Canadian Best Practice Recommendations for Stroke Care, Update 2010) NOTE: For more information on CHADS risk stratification tool, visit OR Carotid Intervention (CMAJ 2008, Canadian Best Practice Recommendations for Stroke Care) A. Symptomatic Carotid Stenosis Patients with transient ischemic attack or nondisabling stroke and ipsilateral 70-99% internal carotid artery stenosis should be offered carotid endarterectomy within 2 weeks of the incident transient ischemic attack or stroke unless contraindicated Carotid endarterectomy is contraindicated for patients with mild (<50%) stenosis. Carotid endarterectomy recommended for selected patients with moderate (50 to 69% symptomatic stenosis), should be evaluated by a physician with expertise in stroke management Patients with severe stenosis (70-99%) benefit most from surgery performed within 2 weeks of the event Carotid endarterectomy for asymptomatic patients is controversial and not recommended. The benefit of endarterectomy depends not only on the degree of stenosis but also on the timing of the surgery after the event. 14
232 Carotid stenting may be offered open-label to those patients who are not operative candidates for technical, anatomical or medical reasons. B. Asymptomatic Carotid Stenosis Carotid endarterectomy may be considered for selected patients with asymptomatic 60-99% carotid stenosis. Transient Ischemic Attack (TIA) Transient ischemic attack (TIA) is defined as a transient episode of neurologic dysfunction caused by focal brain, spinal cord, or retinal ischemia, without acute infarction. This new definition was endorsed by American Heart Association and American Stroke Association (AHA/ASA) in TIA was originally defined as a sudden onset of a focal neurologic symptom and/or sign lasting less than 24 hours, presumably brought on by a transient decrease in blood supply, which rendered the brain ischemic in the area producing the symptom. (Easton et al. Stroke, 2009) The classic definition of TIA, regarding 24 hrs was inadequate for several reasons. Most notably, there is risk of permanent tissue injury (ie, infarction) even when focal transient neurologic symptoms last less than one hour. Thus, the benign connotation of "TIA" has been replaced by an understanding that even relatively brief ischemia can cause permanent brain injury. Symptoms of a TIA may include: Unilateral motor weakness affecting the face, arm or leg Speech (dysarthria) or language (aphasia) difficulties Visual disturbance (amaurosis fugax, hemianopia or diplopia) Unilateral sensory disturbance (paresthesias) affecting the face, arm or leg Vertigo and/or ataxia Symptoms depend on which arterial supply is compromised. 15
233 Some facts: Recovery is complete Can be called a stroke warning event TIA precedes 15% of strokes (Gladstone et al, 2004) The 90 day risk of stroke after TIA is 10.5% ½ of the risk occurs within the first 2 days (Johnson et al, 2000) TRIAGING a TIA patient: The ABCD2 tool identifies Risk Factors for Stroke Within 90 Days of a TIA. The ABCD2 Score is a 7-point tool that includes clinical features: Age >60: 1 point for age 60 years or greater Blood pressure: 1 point for SBP >140 or DBP >90 at the acute evaluation Clinical features: 2 points for focal weakness, 1 point for speech disturbance without focal weakness Duration of symptoms: 1 point for minutes, 2 points for 60 minutes or greater Diabetes: 1 point for presence of diabetes Medication Management for TIA Anticoagulant therapy: to prevent the formation of blood clots in patients with heart disease atrial fibrillation (Coumadin, EC ASA if Coumadin contraindicated) Antiplatelet therapy: to decrease further development of thrombi (EC ASA, Plavix, Aggrenox) Antihypertensive therapy: control systolic blood pressure to reduce the risk of cerebrovascular events Lipid management: to prevent the formation of atherosclerotic plaque Lifestyle modification: includes management of hypertension, hyperlipidemia and diabetes, low-fat / salt diet, increased physical activity, smoking cessation, medication compliance, etc Role of the Secondary Prevention Clinic evaluate and triage all TIA and minor stroke patients.treated surgically and medically avoid an inpatient admission to hospital facilitate timely investigations to determine etiology 16
234 initiate appropriate medications provide access to timely carotid intervention when indicated counsel on risk reduction, lifestyle modification Teaching Your Stroke Patients About Their Medication D85B2D02EE71%7D/2P%20Piece%2010%20Acute%20Inteventions%20final.ppt Blood Pressure Medication Angiotensin Converting Enzyme (ACE) Inhibitor Take same time every day Contraindicated in patients with renal stenosis May increase creatinine, urea and potassium May have a persistent, dry cough Can cause angioedema (1/500) Other S/E: Dizziness, feeling faint Swelling of feet Diarrhea Taste disturbance Headache MORE DETAILS: ACE Inhibitors dilate arterial and venous vessels by blocking the conversion of Angiotensin I to Angiotensin II In order for the medication to be effective advise your patient to take medication at the same time every day It is important to know that the ACE Inhibitor can cause Bradykinin release which can cause a persistent dry cough and angioedema (swelling of the mouth, face) (1/500 people) Other side effects also include low blood pressure, less commonly swelling of the feet, diarrhea, headache, taste disturbance, or feeling dizzy or faint, and possibly sexual dysfunction Remember to advise the patient to have their creatinine checked 1 week after starting ACE Inhibitor 17
235 Angiotensin II Receptor Blockers Well tolerated Contraindicated in patients with renal stenosis May increase creatinine, urea and potassium MORE DETAILS: ARBs permit dilatation of arteries by preventing angiotensin from binding (allows blood vessels to relax and widen a bit causing a lower BP) Well tolerated Orthostatic hypotension may be seen due to vasodilatation Contraindicated in patients with renal stenosis Need to monitor creatinine, urea and potassium These medication names for these medications end in tans Lipid Medication Statins Take once a day with largest meal in evening May be prescribed when cholesterol levels are normal Blood work required for follow-up May interact with antidepressants, antibiotics & immunosuppressants Avoid grapefruit/grapefruit juice Possible side effects: Mild nausea, diarrhea, constipation Some muscle pain/weakness is normal (2-10%) Extreme muscle pain/weakness (serious but rare) MORE DETAILS: To be effective, take your statin once a day. It is usually best to take your statin with the largest meal of the day, but it can also be taken at bedtime Even if cholesterol level is normal, a statin helps stabilise plaque and it also helps decrease inflammation and keep the vessels healthy A baseline liver function test is needed before starting a statin Patients will be asked to have cholesterol profile redrawn in 6-8 weeks after starting statin to ensure decrease in LDL 18
236 A repeat liver function test is done semi-annually during the 1st year or until 1 year after last dose increase. If LFTs are more than 3 times upper limit of normal the statin should be discontinued Advise your patient that statins may interact with other medications including antidepressants, antibiotics and immunosuppressants Avoid grapefruit juice as it may increase the risk of side effects Side effects are usually mild and improve on their own over time. If you experience side effects consult your physician. The most common complaint is gas, stomach pain, indigestion and constipation. After starting a statin, be aware of any NEW muscle pain, or weakness as this could be a sign of a rare, but serious side effect (rhabdomyolysis) Antiplatelet Therapy Aspirin Take one pill, once a day, everyday More is not better Most common side effects include GI upset (take with meals, use EC-ASA) bruise easier bleed longer Consult a doctor immediately if you have unusual or excessive bleeding Aggrenox Do not chew or crush 1/5 people will have a headache in first 5 days Always have a plan B If by the 5th day HA is intolerable, call the physician and resume ASA Other side effects: GI upset (take with food or water) Bleeding Combination of two meds in one pill (ASA (25 mg) & Extended release dipyridamole (200mg) Offer patient Tylenol plain to control headache Clopidrogel Take once a day, every day Best to take with meals 19
237 Side effects: usually mild and improve on their own GI upset Bleeding Skin rash Anticoagulation Therapy Warfarin (Coumadin) Take once a day, every day Best to take with meals Side effects: Usually mild & improve on their own GI upset Bleeding Skin rash MORE DETAILS: Initially, the patient may need daily or several blood tests every week to determine the appropriate dose of Coumadin Some patients require as little as 2mg per day to achieve an INR between 2-3, others require as much as 15mg or more. The dosage required reflects the amount of vitamin K in the diet and the metabolism of Coumadin. A higher dose does not put the patient at a greater risk of side effects. It is the INR that matters, not the dose. Advise your patient to always take Coumadin at the same time every day If your patient forgets a dose, instruct them to take it as soon as he remembers that same day, but do not double up the next day to catch up. Advise your patients not to make drastic changes in their diet, or eating habits without consulting their physician first. Vitamin K plays a role in the clotting process, so it s important to keep levels of vitamin K consistent in their diet. Examples of food containing vit. K is: asparagus, broccoli, brussel sprouts, and cucumber with peel, endives, lettuce, spinach, turnip greens, pistachio nuts, parsley, and watercress. There is no correct amount of Vitamin K to consume- consistency is the best way to go. Alcohol may affect the action of Coumadin therapy, and should only be consumed in moderation.( 1drink/day), a change in routine can change their INR 20
238 Avoid all body contact sports and other activities in which injuries are common. Advise your patient to always wear a helmet when cycling. Things your patients should report immediately to a physician Any falls or injuries to their head or back Fever and chills for more than 1-2 days Vomiting, nausea or diarrhea for more than 1-2 days Repeated or persistent severe chest pain Persistent swelling of feet and lower legs ( for more than 1-2 days), especially if painful Yellow discoloration of eyes and skin or changes to their general health Dabigatran etexilate Available in capsule in doses of 75 and 150 mg Physician will prescribe the optimal dose considering the patient case May be taken with or without food; swallow whole Not to be sprinkled onto food or in liquids, cannot be broken or chewed Take at the same time each day about 12 hours apart Watch for signs of bleeding Never double a dose if a dose is missed Circulation.2011; 124:e209-e21, American Heart Association 21
239 Module Eight Secondary Stroke Prevention REFERENCES Adams, P., Bayley, M., Hellings, C., Hill, M., Woodbury, E., Phillis, S., et al.(2008). Canadian best practice recommendations for stroke care-section 2. Prevention of Stroke (Updated 2008). Canadian Medical Association Journal, 179(12), E15-30 Cahill, K., Stead, LF., & Lancaster, T. (2009). Nicotine receptor partial agonists for smoking cessation. Cochrane Database of Systemic Reviews , DOI: / CD pub3 Canadian Diabetes Association: Clinical Practice Guidelines Expert Committee. (2008). Clinical practice guidelines for the prevention and management of diabetes in Canada. Can J Diabetes, 32(1), S1-S201. Canadian Hypertension Education Program (2009). CHEP Recommendations Part1: Recommendation for hypertension diagnosis, assessment and follow-up (Public Education Slide Kit). Retrieved from Canadian Hypertension Education Program (2009). Dietary Sodium and Blood Pressure Public Education Task Force (Slide Kit). Retrieved from Canadian Stroke Network and Heart & Stroke Foundation of Canada (2008). Canadian Best Practice Recommendations for Stroke Care: Recommendation 2 Prevention of Stroke (Toolkit power point presentation). Retrieved from Stro ke_secondary_prevention.htm Eliasziw M, Kennedy J, Hill J, et al. (2004). Early risk of stroke after a transient ischemic attack in patients with internal carotid artery disease. CMAJ; 170: Hôpital régional de Sudbury Regional Hospital. (2005, updated 2010). Standards of Care, 5 South Medical Unit. Retrieved from %20ACUTE%20STROKE%20PATIENTS-update.pdf Lau, D., Douketis, J., Morrison, K., Hramicak,I., Sharma, A., Ur, E., (2007) Canadian Clinical Practice Guidelines on the Management and Prevention of Obesity in Adults and Children. Canadian Medical Association Journal, 176(8), 1-118
240 Lancaster, T., & Stead, LF., (2005). Individual behavioral counseling for smoking cessation (review). Cochrane Database of Systematic Reviews 2, DOI: / CD pub2 McPherson, R., Frohlich, J., Fodor, G., Genest, J., (2006). Canadian Cardiovascular Society position statement-recommendation for the diagnosis and treatment of dyslipidemia and prevention of cardiovascular disease. Canadian Journal of Cardiology, 22(11), Registered Nurses Association of Ontario (2007). Integrating Smoking Cessation into Daily Nursing Practice. Toronto, Canada: Registered Nurses Association of Ontario Rigotti, N., (2002) Treatment of tobacco use and dependence. The New England Journal of Medicine, 346 (7), Rothwell, PM, Eliasziw M, Gutnikov SA, et al. (2004). Endarterectomy for symptomatic carotid stenosis in relation to clinical subgroups and timing of surgery. Lancet; 363: Sorace, P. (2006). Exercise, physical activity, and dyslipidemia. Strength and Conditioning Journal, 28(4), Stead, LF., Perera, R., Ballen, C., Mant, D., & Lancaster, T. (2009). Nicotine Replacement Therapy for Smoking Cessation (Review). Cochrane Database of Systematic Reviews , DOI: / CD00146.pub3 Stead, LF., Perera, R., Lancaster, T., (2006). Telephone counselling for smoking Cessation (Review). Cochrane Database of Systematic Reviews 3, DOI: / CD pub 2. Thom, T., Haase, N., Rosamond, W., Howard, V., Rumsfeld, J., Manolio, T. et al (2006). Heart Disease and Stroke Statistics 2006 Update: A Report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 113, e85-e151. Heart and Stroke Foundation of Ontario. (2009). Triage and Management of Transient Ischemic patients: A TIA treatment triage and management algorithm, (power point presentation). Retrieved from D85B2D02EE71%7D/2P%20Piece%2010%20Acute%20Inteventions%20final.ppt World Health Organization. (2008). WHO Report on the Global Tobacco Epidemic, The MPOWER package: Geneva.
241 Web Sources
242 NEO Stroke Network s Acute Nursing Certification Program MODULE EIGHT Secondary Stroke Prevention Quiz You may use your binder as a reference to answer these questions Submit your completed quiz to the designated Nurse for marking Your test will be returned to you to keep in your binder NEO Stroke Network May 2010
243 DATE: NAME: 1. The purpose of a Secondary Stroke Prevention Clinic is to: a. Evaluate and triage all TIA and minor stroke patients.treated surgically and medically b. Facilitate timely investigations to determine etiology c. Provide access to timely carotid intervention when indicated d. Counsel on risk reduction, lifestyle modification e. All of the above 2. is the most significant modifiable risk factor for stroke. (Choose one to fill in blank) a. Diabetes b. High LDL Cholesterol c. Hypertension d. Alcoholism 3. In non-diabetic individuals, the Canadian Hypertension Education Program (CHEP 2010) states to treat to a target blood pressure of a. 120/80 mmhg b. 130/80 mmhg c. 135/85 mmhg d. 140/90 mmhg
244 4. Statins act as the first line agents in the treatment of dyslipidemia. Possible effects include: a. Anti-inflammatory properties that may help to stabilize the lining of the blood vessels. b. Statins may help relax blood vessels thus contributing to lower blood pressure. c. Statins may have a blood thinning effect thus reducing the risk of blood clots. d. All of the above TRUE or FALSE QUESTIONS (CIRCLE the correct letter) T F T F T F T F T F T F 1. All patients with ischemic stroke or transient ischemic attack should be prescribed antiplatelet therapy for secondary prevention of recurrent stroke unless there is an indication for anticoagulation. 2. Medication management in stroke prevention usually involves a combination of medications, often including an antihypertensive, a statin and an antithrombotic. 3. TIA is not a medical emergency. As long as the CT Scan is negative, the patient will be fine. 4. An accumulation of 30 to 60 min of brisk walking or other dynamic exercise 4-7 days each week is recommended to reduce stroke risk. 5. Smoking doubles the risk of ischemic stroke. 6. Patients with stroke and atrial fibrillation should be treated with warfarin at a target INR of 4.5, range SCORE: / 10 Stroke Unit/Medical Unit Nurse Clinician or designate (signature)
245 NEO Stroke Network s Acute Nursing Certification Program Hospital - Specific Chart Forms
246 NEO Stroke Network s Acute Nursing Certification Program HRSRH-Specific Chart Forms 1. Telestroke Inclusion/Exclusion Guidelines 2. t-pa Stroke Protocol 3. Standards of Care 5 South, HRSRH for Acute Stroke Patients 4. Non t-pa Order Set 5. TIA Order Set 6. Inpatient Stroke Protocol: Inpatient Policy and Procedure and Algorithm 7. NIHSS Observation Record and Comment Score Sheet 8. Some Guidelines and Tips for the TOR-BSST 9. Secondary Stroke Prevention Clinic Referral Form
247 NEO Stroke Network s Acute Nursing Certification Program Other Resources 1. Northeastern Ontario Stroke Network (NEOSN) Info sheet 2. EVERYTHING STROKE at your fingertips: an Electronic Toolkit for Health Care Providers (announcement) 3. Stroke Organizations: Lists and Websites 4. NEOSN Professional Education Fund information
248 EVERYTHING STROKE.at your fingertips THE NORTHEASTERN ONTARIO STROKE NETWORK Part of the Ontario Stroke System since 2003, the Northeastern Ontario Stroke Network includes District Stroke Centres in North Bay, Timmins and Sault Ste. Marie in addition to an Enhanced District Stroke Centre in Sudbury. These centres along with their partners across the stroke care continuum (prehospital, emergency care, acute care, rehabilitation, community, primary and secondary prevention, health promotion) are tasked with implementing best practice stroke care across the region. Our website will inform you about Upcoming Educational Events and Conferences, Community Initiatives, Rehabilitation News, our Secondary Stroke Prevention Clinic, and includes a tab for the PUBLIC. Contacting the Regional Team Regional Program Director/ Administrative Assistant (705) ext 3138 / ext 1586 Regional Education Coordinator (705) ext 1668 Regional Rehabilitation Coordinator (705) ext 1718 Community and Long Term Care Specialist (705) ext 1585
249 ELECTRONIC TOOLKIT Have you ever tried to find: A copy of the Stroke Best Practice Recommendations? Information on a certain Outcome Measure? Ordering process for patient education pamphlets on stroke? Information on acute swallowing screening? How to put on a hemiplegic sling? The phone number of the CCAC office in your community? ATTENTION Stroke Care Providers! EVERYTHING STROKE.at your fingertips!!!! Visit our website Click on For Professionals Under the Professional Education section, Click EVERYTHING STROKE...at your fingertips A toolkit for stroke care providers working in hospitals View the Table of Contents to find your area of interest Click on that folder to see more topics Contact Susan Bursey, Regional Educ. Coord. (705) ext 1668 [email protected] to find out more about this online resource.
250 EVERYTHING STROKE.at your fingertips Stroke Organizations: LIST AND LINKS Heart and Stroke Centre for Stroke Recovery The Heart and Stroke Foundation Centre for Stroke Recovery is a virtual organization, made up of some of Canada's foremost healthcare centres: The Ottawa Health Research Institute, the University of Ottawa; Sunnybrook Health Sciences Centre and Baycrest, the Rotman Research Institute and the Kunin-Lunenfeld Applied Research Unit. The organization was formed to allow experts in stroke, working in different locations, to share knowledge and collaborate on research initiatives. Heart and Stroke Foundation of Canada The Heart and Stroke Foundation, a volunteer-based health charity, leads in eliminating heart disease and stroke and reducing their impact through the advancement of research and its application, the promotion of healthy living and advocacy. The Heart and Stroke Foundation of Canada is a federation of 10 provincial Foundations, led and supported by a force of more than 140,000 volunteers. Heart and Stroke Foundation of Ontario, Professional Education The Heart and Stroke Foundation of Ontario Profesional Education website's aim is to assist all healthcare providers by providing: sound scientific cardio/cerebrovascular-related information best practice guidelines educational programs resources that can be ordered or accessed to help you to help your patients Canadian Stroke Consortium Created, owned and operated by its members, the Canadian Stroke Consortium (CSC) is the nation's premiere neurologist network. It is an academic alliance committed to the pursuit of anti-stroke therapies by designing and/or conducting research projects and clinical trials. Canadian Stroke Network The Canadian Stroke Network's mission is to reduce the impact of stroke on Canadians through collaborations that create valuable new knowledge in stroke; to ensure the best knowledge is applied; and to build Canadian capacity in stroke.
251 American Stroke Association EVERYTHING STROKE.at your fingertips The American Stroke Association is the division of the American Heart Association that's solely focused on reducing disability and death from stroke through research, education, fundraising and advocacy. Resources include Stroke Journal, Guidelines, Scientific statements, patient resources. Internet Stroke Center The Internet Stroke Center is a non-profit, educational service of the Stroke Center at Barnes-Jewish Hospital, Washington University Medical Center and the Cerebrovascular Diseases Section of the Department of Neurology at Washington University School of Medicine in St. Louis. A comprehensive site for health care professionals, patients and families. National Stroke Association National Stroke Association achieves its mission to lower the incidence and impact of stroke by developing compelling community outreach programs, calling for continued improvement in the quality of stroke patient care, and educating both healthcare professionals and the general public about stroke. Resources for both consumers and health care professionals The Brain Attack Coalition The Brain Attack Coalition is a group of professional, voluntary and governmental entities dedicated to reducing the occurrence, disabilities and death associated with stroke. The goal of the Coalition is to strengthen and promote the relationships among its member organizations in order to help stroke patients or those who are at risk for a stroke. Resources include stroke scales, pre-hospital stroke scales, guidelines - including children's intervention and treatment guidelines, standing orders and care paths. National Institute of Neurological Disorders and Stroke (NINDS) The National Institute of Neurological Disorders and Stroke (NINDS) conducts and supports research on brain and nervous system disorders. Created by the U.S. Congress in 1950, NINDS is one of the more than two dozen research institutes and centers that comprise the National Institutes of Health (NIH). The NIH, located in Bethesda, Maryland, is an agency of the Public Health Service within the U.S. Department of Health and Human Services. European Stroke Initiative The European Stroke Initiative's aim is to improve and optimise stroke management in Europe through educational programmes, both for healthcare professionals and the general public.
252 Northeastern Ontario Stroke Network Professional Education Fund Application Process The Northeastern Ontario Stroke Network (NEOSN) Professional Educational Fund was established with funding provided by the Ministry of Health and Long-Term Care for the Ontario Stroke System. The purpose of the fund is to assist clinicians working in stroke care across the continuum to incorporate best practices through learning opportunities focused on evidence based practices in stroke care. An example of a learning opportunity is a stroke-related professional development conference where your acquired knowledge is shared with your organization and/or region upon your return from the conference. The intent of the fund is to provide financial assistance to enable a variety of stroke clinicians working in Northeastern Ontario to attend stroke-related educational opportunities that are not provided through alternate funding resources (i.e.global hospital budget, RNAO education fund). The maximum amount of funding per submission is anticipated to be $ Special exceptions may be considered. This opportunity is open to health care providers, including physicians, nurses and allied health, working in stroke care across the continuum and whose work is done in collaboration with the NEOSN. The application/request for funding must include a description of: the rationale for attendance at the learning opportunity the benefits to your organization, the region, or for the stroke survivor and their family the plan for information dissemination within your team, your organization and the region must be clearly outlined The committee granting the funding will consist of the following representatives from the NEO Stroke Network: Chair of the NEO Stroke Network Steering Committee Regional Program Manager Regional Stroke Education Coordinator Regional Long-Term Care and Community Specialist Regional Stroke Rehabilitation Coordinator District Stroke Coordinators If there are numerous applications for one event or if the cost associated with attending a particular educational activity is high, the committee may grant partial funding based on equity throughout the region, relevancy and available funding.
253 PROCESS FOR COMPLETING APPLICATION 1. Complete the Stroke-Related Learning Opportunity application form and submit electronically to: Susan Jayne Bursey BSc. P.T., NEO Regional Stroke Education Coordinator, Note: This funding is available for educational opportunities offered from April 1, of the current year March 31, next year. Travel expense forms and receipts for costs incurred must be submitted within two weeks of attending the educational activity. Helpful Hints for Completion of the Application Please write clearly and legibly. Applications should be sent 6-8 weeks prior to the registration deadline of the educational opportunity. However, applications not received within this allotted time frame may still be given consideration. Incomplete applications will be returned to the sender with a welcome to resubmit it within the allotted time frame. The NEOSN Professional Educational Fund does not provide for wage replacement. If the application for educational funding is accepted, a memorandum of understanding will be completed between the applicant and the region. The memorandum of understanding will outline the deliverables including submission of a final report, monitoring of deliverables, deadlines, evaluation of learning opportunity and budget. Applicants are to follow the steps outlined in the acceptance letter. It clearly lists what is involved to receive the funding. Within two weeks following the educational event, the travel expense sheet AND Plan for Dissemination are required. Once those are received, pending any delays for missing information, the expense sheet is forwarded to the finance department for processing. The Final Learning Report is still expected and will complete the process. If required, 75% of the approved funding allotment can be provided in advance of the event. The remaining 25% of the funds would be allocated following attendance at the educational event. The final report must include learning opportunity and description, learning objectives, achievements, sustainability and budget.
254 The memorandum of understanding and final report are shared with the NEOSN and the possibly the applicant s manager(s). Note: The participant is to assume responsibility for all conference arrangements once the education request is approved. **Group applications for funding are discouraged. If two or more individuals wish to participate in the same learning opportunity, they are to submit their individual Application for Learning Opportunity forms; individual Memorandum of Understanding forms; individual Travel Expense Statements. They can, however, submit one Plan for Dissemination of Acquired Knowledge form and clearly state the role of each applicant in the plan. In other words, the two or more individuals can prepare one plan describing how they will share the information/learned material with their colleagues to prepare and deliver a joint in-service/teleconference/ videoconference/written summary.
255 LEVEL TWO Acute Stroke Nursing Certification Program Dysphagia Screening Tool Certification *****CONTACT the NEO Stroke Network or your District Stroke Coordinator to find out about a dysphagia screening tool that may be available at your centre. ******
256 LEVEL THREE Acute Stroke Nursing Certification Program HEMISPHERE S STROKE COMPETENCY SERIES E-learning program One year license per participant TOPICS include: Brain Anatomy Stroke Pathophysiology Pre-Hospital & ED Stroke Hemorrhagic Stroke Ischemic Stroke Stroke Prevention NIHSS training & certification is available in this program as well Includes TESTS and Certificate of Completion *****CONTACT your nurse clinician to participate in this interesting & challenging program******
257 NEO Stroke Network s Acute Nursing Certification Program Acknowledgements The NEO Stroke Network would like to acknowledge the contributions of the following individuals towards the development and completion of this program. Susan Bursey PT, Regional Education Coordinator Lisa Taipalus PT, Best Practice Consultant, Physiotherapy Elaine Noble RN, Stroke Program Michelle Brush RN, Stroke Program Cathy Corrigan-Lauzon RN, Secondary Prevention Clinic Corinne Savignac RN, Nurse Clinician Wendy Archambault SLP, Rehab Unit Hillary Young SLP, Medical Unit Lisa Zeman RN, Manager 5 South Medical Unit, HRSRH Sue Verrilli RT, Community and Long Term Care Specialist Betty Rowley RN, District Stroke Coordinator, North Bay Lorraine Durepos RN, District Stroke Coordinator, Timmins Pam Mancuso RN, District Stroke Coordinator, Sault Ste Marie Jenn Fearn, PT, Regional Rehabilitation Coordinator Darren Jermyn, MBA, Regional Program Manager, NEO Stroke Network
258 Acute Stroke Nurse Certification is hereby granted to: for successful completion of Acute Stroke Nursing Certification Program, LEVEL ONE Susan Bursey, Regional Education Coordinator Date
259 NEO STROKE NETWORK S PRE - ACUTE NURSING CERTIFICATION PROGRAM 2010 FEEDBACK/COMMENT FORM Indicate your discipline/position: Educator Admin RN RPN Other: Please rate your level of confidence for each of the questions BEFORE beginning LEVEL ONE of the Acute Nursing Certification Program. (Mark the most applicable place on the 10 mm line using a short vertical line to indicate your confidence level for each question) A) Knowledge of Medications involved in the management of stroke and the prevention of a recurrent stroke: Lacking Extremely Confidence Confident B) Knowledge of Cerebral Circulation and the related clinical presentations of stroke: Lacking Extremely Confidence Confident C) Knowledge and Skill to Position and Mobilize an acute stroke patient: Lacking Extremely Confidence Confident
260 NEO STROKE NETWORK S POST - ACUTE NURSING CERTIFICATION PROGRAM 2010 FEEDBACK/COMMENT FORM Indicate your discipline/position: Educator Admin RN RPN Other: Indicate what point of the continuum of care best describes where you work: Stroke Prevention Stroke Recognition & Prevention Pre-Hospital Care Emergency Mgmt. Acute Care Transition Mgmt. Rehabilitation Community Reengagement Long Term Care Other: Indicate years in practice: Indicate years of experience providing stroke care: Was the time frame of three months adequate to complete the entire Acute Nursing Certification Program? YES NO, it should be 2. Do you feel the length of time it took to complete each module was reasonable? YES NO Please elaborate 3. Generally speaking, did you find the QUIZ questions to be at the right level of difficulty? 4. Did completing this Acute Nursing Certification Program make you feel like you accomplished something significant and relevant to your work as a nurse working with stroke patients? YES, especially NO, I ll explain
261 5. Please rate your level of confidence NOW after having completed LEVEL ONE. (Mark the most applicable place on the 10 mm line using a short vertical line to indicate your confidence level for each question) A) Knowledge of Medications involved in the management of stroke and the prevention of a recurrent stroke: Lacking Extremely Confidence Confident B) Knowledge of Cerebral Circulation and the related clinical presentations of stroke: Lacking Extremely Confidence Confident C) Knowledge and Skill to Position and Mobilize an acute stroke patient: Lacking Extremely Confidence Confident 6. Do you feel you can apply the Stroke Knowledge you gained to your everyday work with stroke patients? NO YES, in particular,
262 7. List any suggestions you may have for improving this Self Learning Acute Nursing Certification Program: 8. If given the choice, would you choose the BINDER version with the paper quizzes or an ELECTRONIC version with all content and quizzes online?
APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION
 APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION ICD-9-CM codes for cerebrovascular diseases is not user friendly. This presentation is designed to assist
APPENDIX A NEUROLOGIST S GUIDE TO USING ICD-9-CM CODES FOR CEREBROVASCULAR DISEASES INTRODUCTION ICD-9-CM codes for cerebrovascular diseases is not user friendly. This presentation is designed to assist
DIAGNOSTIC CRITERIA OF STROKE
 DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
DIAGNOSTIC CRITERIA OF STROKE Diagnostic criteria are used to validate clinical diagnoses. Here below MONICA diagnostic criteria are reported. MONICA - MONItoring trends and determinants of CArdiovascular
Basic Stroke for the New Recruit
 Basic Stroke for the New Recruit Authors Erin Conahan MSN, RN, ACNS-BC, CNRN, SCRN Julie FussnerBSN, RN, CPHQ, SCRN The authors have nothing to disclose. 1 Objectives List causes of small vessel stroke
Basic Stroke for the New Recruit Authors Erin Conahan MSN, RN, ACNS-BC, CNRN, SCRN Julie FussnerBSN, RN, CPHQ, SCRN The authors have nothing to disclose. 1 Objectives List causes of small vessel stroke
Level III Stroke Center Data Collection Requirements
 Who? Level III Stroke Center Data Collection Requirements All LERN Level III Stroke Centers. LERN Level I and II Stroke Centers have reporting requirements to The Joint Commission or other Board approved
Who? Level III Stroke Center Data Collection Requirements All LERN Level III Stroke Centers. LERN Level I and II Stroke Centers have reporting requirements to The Joint Commission or other Board approved
E x p l a i n i n g Stroke
 Explaining Stroke Introduction Explaining Stroke is a practical step-by-step booklet that explains how a stroke happens, different types of stroke and how to prevent a stroke. Many people think a stroke
Explaining Stroke Introduction Explaining Stroke is a practical step-by-step booklet that explains how a stroke happens, different types of stroke and how to prevent a stroke. Many people think a stroke
Vertebrobasilar Disease
 The Vascular Surgery team at the University of Michigan is dedicated to providing exceptional treatments for in the U-M Cardiovascular Center (CVC), our new state-of-the-art clinical facility. Treatment
The Vascular Surgery team at the University of Michigan is dedicated to providing exceptional treatments for in the U-M Cardiovascular Center (CVC), our new state-of-the-art clinical facility. Treatment
JHS Stroke Program. 2016 JHS Annual Mandatory Education
 JHS Stroke Program 2016 JHS Annual Mandatory Education Learner Objectives At the conclusion of this module learners will be able to: State the definition of stroke Discuss the pathophysiology of stroke
JHS Stroke Program 2016 JHS Annual Mandatory Education Learner Objectives At the conclusion of this module learners will be able to: State the definition of stroke Discuss the pathophysiology of stroke
Acute Myocardial Infarction (the formulary thrombolytic for AMI at AAMC is TNK, please see the TNK monograph in this manual for information)
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Alteplase (Tissue Plasminogen Activator (t-pa)), Activase in the Treatment
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Slumping, Slurring and Slipping Away: Stroke Assessment. Laurie A. Romig, MD, FACEP Medical Director Pinellas County (FL) EMS
 Slumping, Slurring and Slipping Away: Stroke Assessment Laurie A. Romig, MD, FACEP Medical Director Pinellas County (FL) EMS Caution! This discussion relates only to nontraumatic neurological problems!
Slumping, Slurring and Slipping Away: Stroke Assessment Laurie A. Romig, MD, FACEP Medical Director Pinellas County (FL) EMS Caution! This discussion relates only to nontraumatic neurological problems!
Is this pt s brain dysfunction due to ischemia? Onset & progression of sx; location of deficit
 CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
CEREBROVASCULAR ACCIDENTS & TIA s Maggie Kelly History: Onset of symptoms exact time Previous sxs suggestive of TIA s Progression of symptoms Headache? Medications Past history of CVA, clotting events
STATEMENT OF STANDARD
 OHSU HEALTH CARE SYSTEM PRACTICE STANDARD Acute Stroke Practice Standard for the Emergency Department (includes ischemic stroke, TIAs, intracerebral hemorrhage, and non-subarachnoid hemorrhage), PS 01.11
OHSU HEALTH CARE SYSTEM PRACTICE STANDARD Acute Stroke Practice Standard for the Emergency Department (includes ischemic stroke, TIAs, intracerebral hemorrhage, and non-subarachnoid hemorrhage), PS 01.11
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd.
 About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd. Brain Anatomy Definitions Brainstem: The lower extension of the brain where it connects to the
About Brain Injury: A Guide to Brain Anatomy Information from http://www.waiting.com, 1997-2002, Becca, Ltd. Brain Anatomy Definitions Brainstem: The lower extension of the brain where it connects to the
Developing a Dynamic Team Approach to Stroke Care. Emergency Medical Services 2015
 Developing a Dynamic Team Approach to Stroke Care Emergency Medical Services 2015 Why Stroke, Why now? A recent study showed that 80 percent of people in the United States live within an hour s drive of
Developing a Dynamic Team Approach to Stroke Care Emergency Medical Services 2015 Why Stroke, Why now? A recent study showed that 80 percent of people in the United States live within an hour s drive of
EMS Management of Stroke. Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D.
 EMS Management of Stroke Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D. Financial Disclosure: No relevant financial relationship exists Working Together to End Stroke Formed in 2013 Identified
EMS Management of Stroke Deaver Shattuck, M.D. Brian Wiseman, M.D. Keith Woodward, M.D. Financial Disclosure: No relevant financial relationship exists Working Together to End Stroke Formed in 2013 Identified
Global Objectives. Use of the NIH Stroke Scale (NIHSS) in Emergency Department Patients with Acute Stroke. Why Do This Exercise? Session Objectives
 1 Use of the NIH Scale (NIHSS) in Emergency Department Patients with Acute Professor Department of Emergency Medicine University of Illinois College of Medicine Chicago, IL Global Objectives Improve pt
1 Use of the NIH Scale (NIHSS) in Emergency Department Patients with Acute Professor Department of Emergency Medicine University of Illinois College of Medicine Chicago, IL Global Objectives Improve pt
Parts of the Brain. Chapter 1
 Chapter 1 Parts of the Brain Living creatures are made up of cells. Groups of cells, similar in appearance and with the same function, form tissue. The brain is a soft mass of supportive tissues and nerve
Chapter 1 Parts of the Brain Living creatures are made up of cells. Groups of cells, similar in appearance and with the same function, form tissue. The brain is a soft mass of supportive tissues and nerve
Stroke Thrombolysis Awareness. Initial patient assessment. Using F.A.S.T., Rosier, & NIHSS Tools
 Stroke Thrombolysis Awareness Initial patient assessment Using F.A.S.T., Rosier, & NIHSS Tools Adapted from 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities Aims Improve recognition
Stroke Thrombolysis Awareness Initial patient assessment Using F.A.S.T., Rosier, & NIHSS Tools Adapted from 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities Aims Improve recognition
STROKE OCCURRENCE SYMPTOMS OF STROKE
 STROKE OCCURRENCE SYMPTOMS OF STROKE The symptoms of stroke depend on what part of the brain is affected and how large an area is involved. A stroke is a sudden event accompanied by one or more of the
STROKE OCCURRENCE SYMPTOMS OF STROKE The symptoms of stroke depend on what part of the brain is affected and how large an area is involved. A stroke is a sudden event accompanied by one or more of the
Stroke affects approximately 795,000 persons in the
 CLINICAL ASSESSMENT OF STROKE: AREVIEW FOR ED NURSES Authors: Karen Bergman, RN, PhDc, Dean Kindler, MD, and Lindsy Pfau, RN, Kalamazoo, MI Stroke affects approximately 795,000 persons in the United States
CLINICAL ASSESSMENT OF STROKE: AREVIEW FOR ED NURSES Authors: Karen Bergman, RN, PhDc, Dean Kindler, MD, and Lindsy Pfau, RN, Kalamazoo, MI Stroke affects approximately 795,000 persons in the United States
Subclavian Steal Syndrome By Marta Thorup
 Subclavian Steal Syndrome By Marta Thorup Definition Subclavian steal syndrome (SSS), is a constellation of signs and symptoms that arise from retrograde flow of blood in the vertebral artery, due to proximal
Subclavian Steal Syndrome By Marta Thorup Definition Subclavian steal syndrome (SSS), is a constellation of signs and symptoms that arise from retrograde flow of blood in the vertebral artery, due to proximal
REGIONAL SUSPECTED STROKE PROTOCOL
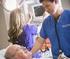 1. Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed. Strokes should be treated emergently. During a stroke, up to 2 million
1. Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed. Strokes should be treated emergently. During a stroke, up to 2 million
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE
 STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
STROKE PREVENTION AND TREATMENT MARK FISHER, MD PROFESSOR OF NEUROLOGY UC IRVINE CASE REPORT: ACUTE STROKE MANAGEMENT 90 YEAR OLD WOMAN, PREVIOUSLY ACTIVE AND INDEPENDENT, CHRONIC ATRIAL FIBRILLATION,
Chapter 7: The Nervous System
 Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
STROKE TRAINING FOR EMS PROFESSIONALS
 1 STROKE TRAINING FOR EMS PROFESSIONALS COURSE OBJECTIVES About Stroke Stroke Policy Recommendations Stroke Protocols and Stroke Hospital Care Stroke Assessment Tools Pre-Notification Stroke Treatment
1 STROKE TRAINING FOR EMS PROFESSIONALS COURSE OBJECTIVES About Stroke Stroke Policy Recommendations Stroke Protocols and Stroke Hospital Care Stroke Assessment Tools Pre-Notification Stroke Treatment
3) Cerebral Cortex & Functions of the 4 LOBES. 5) Cranial Nerves (Nerves In the Cranium, i.e., Head)
 Lecture 5 (Oct 8 th ): ANATOMY and FUNCTION OF THE NERVOUS SYSTEM Lecture Outline 1) Basic Divisions (CNS vs. PNS, Somatic vs. Autonomic) and Directional Terms 2) The Brain (Hindbrain/ Midbrain/ Forebrain)
Lecture 5 (Oct 8 th ): ANATOMY and FUNCTION OF THE NERVOUS SYSTEM Lecture Outline 1) Basic Divisions (CNS vs. PNS, Somatic vs. Autonomic) and Directional Terms 2) The Brain (Hindbrain/ Midbrain/ Forebrain)
Brain Tumor 101. Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center
 Brain Tumor 101 Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center Objectives Identify the different parts of the brain Describe how each part of the brain works Connect each part
Brain Tumor 101 Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center Objectives Identify the different parts of the brain Describe how each part of the brain works Connect each part
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Let s talk about: Stroke
 Let s talk about: Stroke February 20 th 2013 Laura Wilson Christine Stables Questions 1. Why is knowing about stroke important? 2. What exactly is a stroke and what are the symptoms? 3. What should I do
Let s talk about: Stroke February 20 th 2013 Laura Wilson Christine Stables Questions 1. Why is knowing about stroke important? 2. What exactly is a stroke and what are the symptoms? 3. What should I do
Homework Help Stroke
 The Brain & Strokes Your brain is the most complex organ in your body. It is the command centre for everything you do, think, sense and say! It has over 100 billion special nerve cells called neurons.
The Brain & Strokes Your brain is the most complex organ in your body. It is the command centre for everything you do, think, sense and say! It has over 100 billion special nerve cells called neurons.
Appendix L: HQO Year 1 Implementation Priorities
 Appendix L: HQO Year 1 Implementation Priorities Chronic Obstructive Pulmonary Disease (Source: COPD Chairs) Non-Invasive Positive Pressure Ventilation Early Ambulation If possible, seek patient preferences
Appendix L: HQO Year 1 Implementation Priorities Chronic Obstructive Pulmonary Disease (Source: COPD Chairs) Non-Invasive Positive Pressure Ventilation Early Ambulation If possible, seek patient preferences
Stroke And Multiple Sclerosis. 2013 ACOI Internal Medicine Review Course Scott Spradlin D.O. FACOI
 Stroke And Multiple Sclerosis 2013 ACOI Internal Medicine Review Course Scott Spradlin D.O. FACOI Stroke 3 rd Leading cause of Death Acute brain injury due to a vascular cause Sudden onset Persist at least
Stroke And Multiple Sclerosis 2013 ACOI Internal Medicine Review Course Scott Spradlin D.O. FACOI Stroke 3 rd Leading cause of Death Acute brain injury due to a vascular cause Sudden onset Persist at least
REMINDER: Please ensure all stroke and TIA patients admitted to hospital are designated as "Stroke Service" in Cerner.
 ACUTE STROKE CLINICAL PATHWAY QEH/HH PCH KCMH Souris Western Stewart Memorial O'Leary PATIENT ID INCLUSION CRITERIA* All patients admitted to hosptial with a suspected diagnosis of acute ischemic stroke
ACUTE STROKE CLINICAL PATHWAY QEH/HH PCH KCMH Souris Western Stewart Memorial O'Leary PATIENT ID INCLUSION CRITERIA* All patients admitted to hosptial with a suspected diagnosis of acute ischemic stroke
The Normal Neurological Examination
 Normal Neurological Examination 1 of 10 The Normal Neurological Examination Introduction One of the most daunting aspects of the medical examination for the Emergency Physician and the primary care provider
Normal Neurological Examination 1 of 10 The Normal Neurological Examination Introduction One of the most daunting aspects of the medical examination for the Emergency Physician and the primary care provider
ALBERTA PROVINCIAL STROKE STRATEGY (APSS)
 ALBERTA PROVINCIAL STROKE STRATEGY (APSS) Stroke Systems of Care Key Components APSS Pillar Recommendations March 28, 2007 1 The following is a summary of the key components and APSS Pillar recommendations
ALBERTA PROVINCIAL STROKE STRATEGY (APSS) Stroke Systems of Care Key Components APSS Pillar Recommendations March 28, 2007 1 The following is a summary of the key components and APSS Pillar recommendations
Ischaemic stroke 85% (85 in every 100 strokes)
 UNDERSTANDING STROKE DUE TO INTRACEREBRAL HAEMORRHAGE This factsheet provides information for people who have had a stroke due to an intracerebral (bleed in the brain) and for their families and carers.
UNDERSTANDING STROKE DUE TO INTRACEREBRAL HAEMORRHAGE This factsheet provides information for people who have had a stroke due to an intracerebral (bleed in the brain) and for their families and carers.
Therapeutic Management Options for. Acute Ischemic Stroke Anna Rosenbaum, MD
 Therapeutic Management Options for Acute Ischemic Stroke Anna Rosenbaum, MD Epidemiology Epidemiology 4 th leading cause of death in the United States 1 Leading cause of disability Increase in projected
Therapeutic Management Options for Acute Ischemic Stroke Anna Rosenbaum, MD Epidemiology Epidemiology 4 th leading cause of death in the United States 1 Leading cause of disability Increase in projected
WMAS Clinical Guidelines CLN PRO - 027 I Version - 4
 WMAS Clinical Guidelines CLN PRO - 027 I Version - 4 Guideline ID CLN PRO - 027 Version Version 4 Title WMAS Stroke Guidelines Approved by Clinical Steering Group Date Issued 4 May 2016 Review Date May
WMAS Clinical Guidelines CLN PRO - 027 I Version - 4 Guideline ID CLN PRO - 027 Version Version 4 Title WMAS Stroke Guidelines Approved by Clinical Steering Group Date Issued 4 May 2016 Review Date May
Background on Brain Injury
 CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Traumatic Brain Injury and Incarceration. Objectives. Traumatic Brain Injury. Which came first, the injury or the behavior?
 Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
STROKE INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. A commonly used term for stroke is cerebrovascular accident, typically shortened
STROKE INTRODUCTION Stroke is the medical term for a specific type of neurological event that causes damage to the brain. A commonly used term for stroke is cerebrovascular accident, typically shortened
GP workshop. Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre
 GP workshop Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre Stroke: the Facts Stroke: the Facts Every 5 minutes someone in the UK has a stroke 1 in 4 men and 1 in 5 women will have a stroke
GP workshop Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre Stroke: the Facts Stroke: the Facts Every 5 minutes someone in the UK has a stroke 1 in 4 men and 1 in 5 women will have a stroke
S9 Administer thrombolytic treatment in acute ischaemic stroke
 S9 Administer thrombolytic treatment in acute ischaemic Screening and initiating treatment, overseeing competency of treatment About this workforce competence This competence is about the emergency administration
S9 Administer thrombolytic treatment in acute ischaemic Screening and initiating treatment, overseeing competency of treatment About this workforce competence This competence is about the emergency administration
Day Rehab ICD-10 documentation
 Day Rehab documentation Seven key impacts to documentation 1. Disease or disorder site 2. Acuity and/or encounter status of treatment 3. Etiology, causative agent, or disease type and injury/ poisoning
Day Rehab documentation Seven key impacts to documentation 1. Disease or disorder site 2. Acuity and/or encounter status of treatment 3. Etiology, causative agent, or disease type and injury/ poisoning
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Substandard Underwriting Structured Settlements
 Substandard Underwriting Structured Settlements Structures 101-Back to Basics February 20-22, 2013 Las Vegas, Nevada Rosemary Brindamour BSN CSSC Chief Medical Underwriter Structured Settlement Underwriting
Substandard Underwriting Structured Settlements Structures 101-Back to Basics February 20-22, 2013 Las Vegas, Nevada Rosemary Brindamour BSN CSSC Chief Medical Underwriter Structured Settlement Underwriting
Acute Stroke Diagnosis and Management
 Acute Stroke Diagnosis and Management Dr Gemma Smith (Specialty Trainee in Elderly Care and Stroke Medicine) Correspondence - Gemma Smith: [email protected] ABSTRACT Stroke (noun): a sudden disabling
Acute Stroke Diagnosis and Management Dr Gemma Smith (Specialty Trainee in Elderly Care and Stroke Medicine) Correspondence - Gemma Smith: [email protected] ABSTRACT Stroke (noun): a sudden disabling
Vocabulary & General Concepts of Brain Organization
 Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
Student Academic Learning Services Page 1 of 8 Nervous System Quiz
 Student Academic Learning Services Page 1 of 8 Nervous System Quiz 1. The term central nervous system refers to the: A) autonomic and peripheral nervous systems B) brain, spinal cord, and cranial nerves
Student Academic Learning Services Page 1 of 8 Nervous System Quiz 1. The term central nervous system refers to the: A) autonomic and peripheral nervous systems B) brain, spinal cord, and cranial nerves
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium
 Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
Stroke Coding Issues Presentation to: NorthEast Cerebrovascular Consortium October 30, 2008 Barry Libman, RHIA, CCS, CCS-P President, Barry Libman Inc. Stroke Coding Issues Outline Medical record documentation
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Nervous System Pathology
 Nervous System Pathology Nervous System Central Nervous System CNS Brain & Spinal cord Nervous System Peripheral Nervous System PNS Spinal and cranial nerves CNS Close relationship with endocrine system
Nervous System Pathology Nervous System Central Nervous System CNS Brain & Spinal cord Nervous System Peripheral Nervous System PNS Spinal and cranial nerves CNS Close relationship with endocrine system
The Clinical Evaluation of the Comatose Patient in the Emergency Department
 The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
Module 1: The Brain and the Central Nervous System (CNS)
 Module 1: The Brain and the Central Nervous System (CNS) By the end of this unit, the learner will be able to: Describe the anatomy of the brain and the central nervous system Identify regions of the brain
Module 1: The Brain and the Central Nervous System (CNS) By the end of this unit, the learner will be able to: Describe the anatomy of the brain and the central nervous system Identify regions of the brain
Diagram 2(i): Structure of the Neuron
 Diagram 2(i): Structure of the Neuron Generally speaking, we can divide the nervous system into different parts, according to location and function. So far we have mentioned the central nervous system
Diagram 2(i): Structure of the Neuron Generally speaking, we can divide the nervous system into different parts, according to location and function. So far we have mentioned the central nervous system
Glossary. Activities of Daily Living (ADL): routine daily self care skills, including dressing, bathing, toileting, and feeding.
 Glossary Acoustic nerve: the nerve that is responsible for hearing. Activities of Daily Living (ADL): routine daily self care skills, including dressing, bathing, toileting, and feeding. Adaptive physical
Glossary Acoustic nerve: the nerve that is responsible for hearing. Activities of Daily Living (ADL): routine daily self care skills, including dressing, bathing, toileting, and feeding. Adaptive physical
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Lifecheque Basic Critical Illness Insurance
 Lifecheque Basic Critical Illness Insurance Strong. Reliable. Trustworthy. Forward-thinking. Extra help on the road to recovery Surviving a critical illness can be very challenging financially Few of us
Lifecheque Basic Critical Illness Insurance Strong. Reliable. Trustworthy. Forward-thinking. Extra help on the road to recovery Surviving a critical illness can be very challenging financially Few of us
NEUROLOCALIZATION MADE EASY
 NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99)
 CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
Stroke Care First week
 Stroke Care First week Florence Nightingale (1820 1910) Stroke Unit Dedicated personnel trained in stroke management Stepwise guidelines supported by explicit checklists Continuous monitoring available
Stroke Care First week Florence Nightingale (1820 1910) Stroke Unit Dedicated personnel trained in stroke management Stepwise guidelines supported by explicit checklists Continuous monitoring available
A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation
 Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation PATIENT EDUCATION GUIDE What is atrial fibrillation? Atrial fibrillation
Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation A Patient s Guide to Antithrombotic Therapy in Atrial Fibrillation PATIENT EDUCATION GUIDE What is atrial fibrillation? Atrial fibrillation
TIME LOST IS BRAIN LOST. TARGET: STROKE CAMPAIGN MANUAL
 TIME LOST IS BRAIN LOST. TARGET: STROKE CAMPAIGN MANUAL 2010, American Heart Association TARGET: STROKE CAMPAIGN MANUAL 01 INTRODUCTION Welcome to the Target: Stroke. The purpose of this manual is to provide
TIME LOST IS BRAIN LOST. TARGET: STROKE CAMPAIGN MANUAL 2010, American Heart Association TARGET: STROKE CAMPAIGN MANUAL 01 INTRODUCTION Welcome to the Target: Stroke. The purpose of this manual is to provide
STROKE REHABILITATION RESOURCE GUIDE
 STROKE REHABILITATION RESOURCE GUIDE INTRODUCTION The intent of the Stroke Rehabilitation Resource Guide is to enable stroke care providers seeking information related to the rehabilitation of the stroke
STROKE REHABILITATION RESOURCE GUIDE INTRODUCTION The intent of the Stroke Rehabilitation Resource Guide is to enable stroke care providers seeking information related to the rehabilitation of the stroke
Spontaneous Vertebral Artery Dissection. William Barsan, MD, FACEP
 The patient was a 29-year-old woman with a history of migraine headaches who has otherwise been in good health. She stated that earlier today she was walking in her house and talking on the phone when
The patient was a 29-year-old woman with a history of migraine headaches who has otherwise been in good health. She stated that earlier today she was walking in her house and talking on the phone when
Making the Case for CPG s Jean Luciano, MSN, RN, CNRN, SCRN, CRNP, FAHA Claranne Mathiesen, MSN, RN, CNRN, SCRN, FAHA
 Making the Case for CPG s Jean Luciano, MSN, RN, CNRN, SCRN, CRNP, FAHA Claranne Mathiesen, MSN, RN, CNRN, SCRN, FAHA Disclosures Jeanie Luciano Genentech speakers bureau Claranne Mathiesen - none 1 Objective
Making the Case for CPG s Jean Luciano, MSN, RN, CNRN, SCRN, CRNP, FAHA Claranne Mathiesen, MSN, RN, CNRN, SCRN, FAHA Disclosures Jeanie Luciano Genentech speakers bureau Claranne Mathiesen - none 1 Objective
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
2401 : Anatomy/Physiology
 Dr. Chris Doumen Week 7 2401 : Anatomy/Physiology The Brain Central Nervous System TextBook Readings Pages 431 through 435 and 463-467 Make use of the figures in your textbook ; a picture is worth a thousand
Dr. Chris Doumen Week 7 2401 : Anatomy/Physiology The Brain Central Nervous System TextBook Readings Pages 431 through 435 and 463-467 Make use of the figures in your textbook ; a picture is worth a thousand
BIOLOGY STUDY PACKET THE BRAIN
 BIOLOGY STUDY PACKET THE BRAIN SC.912.L.14.26 AA Spring 2012 The intent of this packet is to supplement regular classroom instruction, not to replace it. This also supposes that the students have access
BIOLOGY STUDY PACKET THE BRAIN SC.912.L.14.26 AA Spring 2012 The intent of this packet is to supplement regular classroom instruction, not to replace it. This also supposes that the students have access
Basic Brain Information
 Basic Brain Information Brain facts Your brain weighs about 3lbs, or just under 1.5Kg It has the texture of blancmange Your brain is connected to your spinal cord by the brain stem Behind your brain stem
Basic Brain Information Brain facts Your brain weighs about 3lbs, or just under 1.5Kg It has the texture of blancmange Your brain is connected to your spinal cord by the brain stem Behind your brain stem
Dallas Neurosurgical and Spine Associates, P.A Patient Health History
 Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Stroke: Major Public Health Burden. Stroke: Major Public Health Burden. Stroke: Major Public Health Burden 5/21/2012
 Faculty Prevention Sharon Ewer, RN, BSN, CNRN Stroke Program Coordinator Baptist Health Montgomery, Alabama Satellite Conference and Live Webcast Monday, May 21, 2012 2:00 4:00 p.m. Central Time Produced
Faculty Prevention Sharon Ewer, RN, BSN, CNRN Stroke Program Coordinator Baptist Health Montgomery, Alabama Satellite Conference and Live Webcast Monday, May 21, 2012 2:00 4:00 p.m. Central Time Produced
Rehabilitation Nurses: Champions for Optimizing Stroke Rehabilitation Across the Continuum of Care
 Rehabilitation Nurses: Champions for Optimizing Stroke Rehabilitation Across the Continuum of Care Presenters Sandra Melchiorre RN, MN, ACNP, CNN (c) Regional Stroke Acute Care Advanced Practice Nurse,
Rehabilitation Nurses: Champions for Optimizing Stroke Rehabilitation Across the Continuum of Care Presenters Sandra Melchiorre RN, MN, ACNP, CNN (c) Regional Stroke Acute Care Advanced Practice Nurse,
Medical Management of Ischemic Stroke: An Update. Siddharth Sehgal, MD Medical Director, TMH Neuroscience Center
 Medical Management of Ischemic Stroke: An Update Siddharth Sehgal, MD Medical Director, TMH Neuroscience Center Objectives Diagnostic evaluation and management of acute ischemic stroke. Inpatient management
Medical Management of Ischemic Stroke: An Update Siddharth Sehgal, MD Medical Director, TMH Neuroscience Center Objectives Diagnostic evaluation and management of acute ischemic stroke. Inpatient management
Imaging of Acute Stroke. Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group
 Imaging of Acute Stroke Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group Modalities Non Contrast CT (NCCT) Contrast CT Angiography MRI MR Angiography Perfusion
Imaging of Acute Stroke Noam Eshkar, M.D New Jersey Neuroscience Institute JFK Medical Center Edison Radiology Group Modalities Non Contrast CT (NCCT) Contrast CT Angiography MRI MR Angiography Perfusion
Treatment of Ischemic Stroke in the Neuro-ICU
 Treatment of Ischemic Stroke in the Neuro-ICU Gary L. Bernardini, MD, PhD Professor of Neurology Director, Stroke and Neurocritical Care Departments of Neurology and Neurosurgery Albany Medical Center
Treatment of Ischemic Stroke in the Neuro-ICU Gary L. Bernardini, MD, PhD Professor of Neurology Director, Stroke and Neurocritical Care Departments of Neurology and Neurosurgery Albany Medical Center
Emerging therapies for Intracerebral Hemorrhage
 Emerging therapies for Intracerebral Hemorrhage Chitra Venkat, MBBS, MD, MSc. Associate Professor of Neurology and Neurological Sciences Stroke and Neurocritical Care. Stanford University Learning objectives
Emerging therapies for Intracerebral Hemorrhage Chitra Venkat, MBBS, MD, MSc. Associate Professor of Neurology and Neurological Sciences Stroke and Neurocritical Care. Stanford University Learning objectives
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
ICD-9-CM coding for patients with Traumatic Brain Injury*
 ICD-9-CM coding for patients with Traumatic Brain Injury* The diagnostic code for sequelae of traumatic brain injury is: 907.0 Late effect of intracranial injury without mention of skull fracture (Late
ICD-9-CM coding for patients with Traumatic Brain Injury* The diagnostic code for sequelae of traumatic brain injury is: 907.0 Late effect of intracranial injury without mention of skull fracture (Late
CSE511 Brain & Memory Modeling. Lect04: Brain & Spine Neuroanatomy
 CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
THE BRAIN AND CRANIAL NERVES
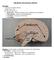 THE BRAIN AND CRANIAL NERVES The Brain - made up of a trillion neurons - weighs about 3 lbs - has four principle parts 1. Brain stem - medulla oblongata, pons, midbrain (mesencephalon) 2. Diencephalon
THE BRAIN AND CRANIAL NERVES The Brain - made up of a trillion neurons - weighs about 3 lbs - has four principle parts 1. Brain stem - medulla oblongata, pons, midbrain (mesencephalon) 2. Diencephalon
Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence
 Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
Antoinne C. Able, M.D., MSCI Vanderbilt University Medical Center Department of Physical Medicine and Rehabilitation Nashville, TN
 Antoinne C. Able, M.D., MSCI Vanderbilt University Medical Center Department of Physical Medicine and Rehabilitation Nashville, TN 16 th Annual Harold Jobe Bernard Stroke and Neurosciences Symposium November
Antoinne C. Able, M.D., MSCI Vanderbilt University Medical Center Department of Physical Medicine and Rehabilitation Nashville, TN 16 th Annual Harold Jobe Bernard Stroke and Neurosciences Symposium November
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Types of Brain Injury
 Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Chapter 15. Autonomic Nervous System (ANS) and Visceral Reflexes. general properties Anatomy. Autonomic effects on target organs
 Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Hospital-based SNF Coding Tip Sheet: Top 25 codes and ICD-10 Chapter Overview
 Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Hospital-based SNF Coding Tip Sheet: Top 25 codes and Chapter Overview Chapter 5 - Mental, Behavioral and Neurodevelopmental Disorders (F00-F99) Classification improvements (different categories) expansions:
Anatomy: The sella is a depression in the sphenoid bone that makes up part of the skull base located behind the eye sockets.
 Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
Pituitary Tumor Your doctor thinks you may have a pituitary tumor. Pituitary tumors are benign (non-cancerous) overgrowth of cells that make up the pituitary gland (the master gland that regulates other
