Appendix A. Rome III Diagnostic Criteria for Functional Gastrointestinal Disorders
|
|
|
- Antonia Casey
- 8 years ago
- Views:
Transcription
1 Appendix A Rome III Diagnostic Criteria for Functional Gastrointestinal Disorders 885
2 886 Appendix A: Rome III Diagnostic Criteria for FGIDs A. Functional Esophageal Disorders A1. Functional Heartburn 1. Burning retrosternal discomfort or pain 2. Absence of evidence that gastroesophageal acid reflux is the cause of the symptom 3. Absence of histopathology-based esophageal motility disorders A2. Functional Chest Pain of Presumed Esophageal Origin 1. Midline chest pain or discomfort that is not of burning quality 2. Absence of evidence that gastroesophageal reflux is the cause of the symptom 3. Absence of histopathology-based esophageal motility disorders A3. Functional Dysphagia 1. Sense of solid and/or liquid foods sticking, lodging, or passing abnormally through the esophagus 2. Absence of evidence that gastroesophageal reflux is the cause of the symptom 3. Absence of histopathology-based esophageal motility disorders A4. Globus 1. Persistent or intermittent, nonpainful sensation of a lump or foreign body in the throat 2. Occurrence of the sensation between meals 3. Absence of dysphagia or odynophagia 4. Absence of evidence that gastroesophageal reflux is the cause of the symptom 5. Absence of histopathology-based esophageal motility disorders
3 Appendix A: Rome III Diagnostic Criteria for FGIDs 887 B. Functional Gastroduodenal Disorders B1. FUNCTIONAL DYSPEPSIA Diagnostic criteria* Must include: 1. One or more of the following: a. Bothersome postprandial fullness b. Early satiation c. Epigastric pain d. Epigastric burning AND 2. No evidence of structural disease (including at upper endoscopy) that is likely to explain the symptoms B1a. Postprandial Distress Syndrome Diagnostic criteria* Must include one or both of the following: 1. Bothersome postprandial fullness, occurring after ordinary-sized meals, at least several times per week 2. Early satiation that prevents finishing a regular meal, at least several times per week Supportive criteria 1. Upper abdominal bloating or postprandial nausea or excessive belching can be present 2. Epigastric pain syndrome may coexist B1b. Epigastric Pain Syndrome 1. Pain or burning localized to the epigastrium of at least moderate severity, at least once per week 2. The pain is intermittent 3. Not generalized or localized to other abdominal or chest regions 4. Not relieved by defecation or passage of flatus 5. Not fulfilling criteria for gallbladder and sphincter of Oddi disorders Supportive criteria 1. The pain may be of a burning quality, but without a retrosternal component 2. The pain is commonly induced or relieved by ingestion of a meal, but may occur while fasting 3. Postprandial distress syndrome may coexist
4 888 Appendix A: Rome III Diagnostic Criteria for FGIDs B2. BELCHING DISORDERS B2a. Aerophagia 1. Troublesome repetitive belching at least several times a week 2. Air swallowing that is objectively observed or measured * Criteria fulfilled for the last 3 months with symptom onset B2b. Unspecified Excessive Belching 1. Troublesome repetitive belching at least several times a week 2. No evidence that excessive air swallowing underlies the symptom B3. NAUSEA AND VOMITING DISORDERS B3a. Chronic Idiopathic Nausea 1. Bothersome nausea occurring at least several times per week 2. Not usually associated with vomiting 3. Absence of abnormalities at upper endoscopy or metabolic disease that explains the nausea B3b. Functional Vomiting 1. On average one or more episodes of vomiting per week 2. Absence of criteria for an eating disorder, rumination, or major psychiatric disease according to DSM-IV 3. Absence of self-induced vomiting and chronic cannabinoid use and absence of abnormalities in the central nervous system or metabolic diseases to explain the recurrent vomiting
5 Appendix A: Rome III Diagnostic Criteria for FGIDs 889 B3c. Cyclic Vomiting Syndrome Diagnostic criteria Must include all of the following: 1. Stereotypical episodes of vomiting regarding onset (acute) and duration (less than one week) 2. Three or more discrete episodes in the prior year 3. Absence of nausea and vomiting between episodes Supportive criterion History or family history of migraine headaches B4. Rumination Syndrome in Adults Diagnostic criteria Must include both of the following: 1. Persistent or recurrent regurgitation of recently ingested food into the mouth with subsequent spitting or remastication and swallowing 2. Regurgitation is not preceded by retching Supportive criteria 1. Regurgitation events are usually not preceded by nausea 2. Cessation of the process when the regurgitated material becomes acidic 3. Regurgitant contains recognizable food with a pleasant taste C. Functional Bowel Disorders C1. Irritable Bowel Syndrome Diagnostic criterion* Recurrent abdominal pain or discomfort** at least 3 days/month in the last 3 months associated with two or more of the following: 1. Improvement with defecation 2. Onset associated with a change in frequency of stool 3. Onset associated with a change in form (appearance) of stool * Criterion fulfilled for the last 3 months with symptom onset ** Discomfort means an uncomfortable sensation not described as pain. In pathophysiology research and clinical trials, a pain/discomfort frequency of at least 2 days a week during screening evaluation is recommended for subject eligibility. C2. Functional Bloating Diagnostic criteria* Must include both of the following: 1. Recurrent feeling of bloating or visible distension at least 3 days/month in the last 3 months 2. Insufficient criteria for a diagnosis of functional dyspepsia, irritable bowel syndrome, or other functional GI disorder
6 890 Appendix A: Rome III Diagnostic Criteria for FGIDs C3. Functional Constipation Diagnostic criteria* 1. Must include two or more of the following: a. Straining during at least 25% of defecations b. Lumpy or hard stools in at least 25% of defecations c. Sensation of incomplete evacuation for at least 25% of defecations d. Sensation of anorectal obstruction/blockage for at least 25% of defecations e. Manual maneuvers to facilitate at least 25% of defecations (e.g., digital evacuation, support of the pelvic floor) f. Fewer than three defecations per week 2. Loose stools are rarely present without the use of laxatives 3. Insufficient criteria for irritable bowel syndrome C4. Functional Diarrhea Diagnostic criterion* Loose (mushy) or watery stools without pain occurring in at least 75% of stools * Criterion fulfilled for the last 3 months with symptom onset C5. Unspecified Functional Bowel Disorder Diagnostic criterion* Bowel symptoms not attributable to an organic etiology that do not meet criteria for the previously defined categories * Criterion fulfilled for the last 3 months with symptom onset D. Functional Abdominal Pain Syndrome D. Functional Abdominal Pain Syndrome 1. Continuous or nearly continuous abdominal pain 2. No or only occasional relationship of pain with physiological events (e.g., eating, defecation, or menses) 3. Some loss of daily functioning 4. The pain is not feigned (e.g., malingering) 5. Insufficient symptoms to meet criteria for another functional gastrointestinal disorder that would explain the pain
7 Appendix A: Rome III Diagnostic Criteria for FGIDs 891 E. Functional Gallbladder and Sphincter of Oddi Disorders E. Functional Gallbladder and Sphincter of Oddi Disorders Diagnostic criteria Must include episodes of pain located in the epigastrium and/or right upper quadrant and all of the following: 1. Episodes lasting 30 minutes or longer 2. Recurrent symptoms occurring at different intervals (not daily) 3. The pain builds up to a steady level 4. The pain is moderate to severe enough to interrupt the patient s daily activities or lead to an emergency department visit 5. The pain is not relieved by bowel movements 6. The pain is not relieved by postural change 7. The pain is not relieved by antacids 8. Exclusion of other structural disease that would explain the symptoms Supportive criteria The pain may present with one or more of the following: 1. Associated with nausea and vomiting 2. Radiates to the back and/or right infra subscapular region 3. Awakens from sleep in the middle of the night E1. Functional Gallbladder Disorder Diagnostic criteria Must include all of the following: 1. Criteria for functional gallbladder and sphincter of Oddi disorder 2. Gallbladder is present 3. Normal liver enzymes, conjugated bilirubin, and amylase/lipase E2. Functional Biliary Sphincter of Oddi Disorder Diagnostic criteria Must include both of the following: 1. Criteria for functional gallbladder and sphincter of Oddi disorder 2. Normal amylase/lipase Supportive criterion Elevated serum transaminases, alkaline phosphatase, or conjugated bilirubin temporarily related to at least two pain episodes E3. Functional Pancreatic Sphincter of Oddi Disorder Diagnostic criteria Must include both of the following: 1. Criteria for functional gallbladder and sphincter of Oddi disorder and 2. Elevated amylase/lipase
8 892 Appendix A: Rome III Diagnostic Criteria for FGIDs F. Functional Anorectal Disorders F1. Functional Fecal Incontinence Diagnostic criteria* 1. Recurrent uncontrolled passage of fecal material in an individual with a developmental age of at least 4 years and one or more of the following: a. Abnormal functioning of normally innervated and structurally intact muscles b. Minor abnormalities of sphincter structure and/or innervation c. Normal or disordered bowel habits, (i.e., fecal retention or diarrhea) d. Psychological causes AND 2. Exclusion of all the following: a. Abnormal innervation caused by lesion(s) within the brain (e.g., dementia), spinal cord, or sacral nerve roots, or mixed lesions (e.g., multiple sclerosis), or as part of a generalized peripheral or autonomic neuropathy (e.g., due to diabetes) b. Anal sphincter abnormalities associated with a multisystem disease (e.g., scleroderma) c. Structural or neurogenic abnormalities believed to be the major or primary cause of fecal incontinence * Criteria fulfilled for the last 3 months F2. FUNCTIONAL ANORECTAL PAIN F2a. Chronic Proctalgia 1. Chronic or recurrent rectal pain or aching 2. Episodes last 20 minutes or longer 3. Exclusion of other causes of rectal pain such as ischemia, inflammatory bowel disease, cryptitis, intramuscular abscess, anal fissure, hemorrhoids, prostatitis, and coccygodynia Chronic proctalgia may be further characterized into levator ani syndrome or unspecified anorectal pain based on digital rectal examination. F2a.1. Levator Ani Syndrome Diagnostic criterion Symptom criteria for chronic proctalgia and tenderness during posterior traction on the puborectalis
9 Appendix A: Rome III Diagnostic Criteria for FGIDs 893 F2a.2. Unspecified Functional Anorectal Pain Diagnostic criterion Symptom criteria for chronic proctalgia but no tenderness during posterior traction on the puborectalis F2b. Proctalgia Fugax Diagnostic criteria Must include all of the following: 1. Recurrent episodes of pain localized to the anus or lower rectum 2. Episodes last from seconds to minutes 3. There is no anorectal pain between episodes For research purposes criteria must be fulfilled for 3 months; however, clinical diagnosis and evaluation may be made prior to 3 months. F3. Functional Defecation Disorders Diagnostic criteria* 1. The patient must satisfy diagnostic criteria for functional constipation** 2. During repeated attempts to defecate must have at least two of the following: a. Evidence of impaired evacuation, based on balloon expulsion test or imaging b. Inappropriate contraction of the pelvic floor muscles (i.e., anal sphincter or puborectalis) or less than 20% relaxation of basal resting sphincter pressure by manometry, imaging, or EMG c. Inadequate propulsive forces assessed by manometry or imaging ** Diagnostic criteria for functional constipation: (1) Must include two or more of the following: (a) Straining during at least 25% of defecations, (b) Lumpy or hard stools in at least 25% of defecations, (c) Sensation of incomplete evacuation for at least 25% of defecations, (d) Sensation of anorectal obstruction/blockage for at least 25% of defecations, (e) Manual maneuvers to facilitate at least 25% of defecations (e.g., digital evacuation, support of the pelvic floor), (f ) Fewer than three defecations per week. (2) Loose stools are rarely present without the use of laxatives. (3) Insufficient criteria for irritable bowel syndrome. F3a. Dyssynergic Defecation Diagnostic criterion Inappropriate contraction of the pelvic floor or less than 20% relaxation of basal resting sphincter pressure with adequate propulsive forces during attempted defecation F3b. Inadequate Defecatory Propulsion Diagnostic criterion Inadequate propulsive forces with or without inappropriate contraction or less than 20% relaxation of the anal sphincter during attempted defecation
10 894 Appendix A: Rome III Diagnostic Criteria for FGIDs G. Childhood Functional GI Disorders: Infant/Toddler G1. Infant Regurgitation Diagnostic criteria Must include both of the following in otherwise healthy infants 3 weeks to 12 months of age: 1. Regurgitation two or more times per day for 3 or more weeks 2. No retching, hematemesis, aspiration, apnea, failure to thrive, feeding or swallowing difficulties, or abnormal posturing G2. Infant Rumination Syndrome Diagnostic criteria Must include all of the following for at least 3 months: 1. Repetitive contractions of the abdominal muscles, diaphragm, and tongue 2. Regurgitation of gastric content into the mouth, which is either expectorated or rechewed and reswallowed 3. Three or more of the following: a. Onset between 3 and 8 months b. Does not respond to management for gastroesophageal reflux disease, or to anticholinergic drugs, hand restraints, formula changes, and gavage or gastrostomy feedings c. Unaccompanied by signs of nausea or distress d. Does not occur during sleep and when the infant is interacting with individuals in the environment G3. Cyclic Vomiting Syndrome Diagnostic criteria Must include both of the following: 1. Two or more periods of intense nausea and unremitting vomiting or retching lasting hours to days 2. Return to usual state of health lasting weeks to months G4. Infant Colic Diagnostic criteria Must include all of the following in infants from birth to 4 months of age: 1. Paroxysms of irritability, fussing or crying that starts and stops without obvious cause 2. Episodes lasting 3 or more hours/day and occurring at least 3 days/wk for at least 1 week 3. No failure to thrive G5. Functional Diarrhea Diagnostic criteria Must include all of the following: 1. Daily painless, recurrent passage of three or more large, unformed stools 2. Symptoms that last more than 4 weeks 3. Onset of symptoms that begins between 6 and 36 months of age 4. Passage of stools that occurs during waking hours 5. There is no failure-to-thrive if caloric intake is adequate
11 Appendix A: Rome III Diagnostic Criteria for FGIDs 895 G6. Infant Dyschezia Diagnostic criteria Must include both of the following in an infant less than 6 months of age 1. At least 10 minutes of straining and crying before successful passage of soft stools 2. No other health problems G7. Functional Constipation Diagnostic criteria Must include one month of at least two of the following in infants up to 4 years of age: 1. Two or fewer defecations per week 2. At least one episode/week of incontinence after the acquisition of toileting skills 3. History of excessive stool retention 4. History of painful or hard bowel movements 5. Presence of a large fecal mass in the rectum 6. History of large diameter stools which may obstruct the toilet Accompanying symptoms may include irritability, decreased appetite, and/or early satiety. The accompanying symptoms disappear immediately following passage of a large stool. H. Childhood Functional GI Disorders: Child/Adolescent H1. VOMITING AND AEROPHAGIA H1a. Adolescent Rumination Syndrome 1. Repeated painless regurgitation and rechewing or expulsion of food that a. begin soon after ingestion of a meal b. do not occur during sleep c. do not respond to standard treatment for gastroesophageal reflux 2. No retching 3. No evidence of an inflammatory, anatomic, metabolic, or neoplastic process that explains the subject s symptoms H1b. Cyclic Vomiting Syndrome Diagnostic criteria Must include both of the following: 1. Two or more periods of intense nausea and unremitting vomiting or retching lasting hours to days 2. Return to usual state of health lasting weeks to months H1c. Aerophagia Diagnostic criteria* Must include at least two of the following: 1. Air swallowing 2. Abdominal distention due to intraluminal air 3. Repetitive belching and/or increased flatus * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis
12 896 Appendix A: Rome III Diagnostic Criteria for FGIDs H2. ABDOMINAL PAIN-RELATED FUNCTIONAL GI DISORDERS H2a. Functional Dyspepsia 1. Persistent or recurrent pain or discomfort centered in the upper abdomen (above the umbilicus) 2. Not relieved by defecation or associated with the onset of a change in stool frequency or stool form (i.e., not irritable bowel syndrome) 3. No evidence of an inflammatory, anatomic, metabolic or neoplastic process that explains the subject s symptoms * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis H2b. Irritable Bowel Syndrome Diagnostic criteria* Must include both of the following: 1. Abdominal discomfort** or pain associated with two or more of the following at least 25% of the time: a. Improvement with defecation b. Onset associated with a change in frequency of stool c. Onset associated with a change in form (appearance) of stool 2. No evidence of an inflammatory, anatomic, metabolic, or neoplastic process that explains the subject s symptoms * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis ** Discomfort means an uncomfortable sensation not described as pain. H2c. Abdominal Migraine 1. Paroxysmal episodes of intense, acute periumbilical pain that lasts for 1 hour or more 2. Intervening periods of usual health lasting weeks to months 3. The pain interferes with normal activities 4. The pain is associated with 2 of the following: a. Anorexia b. Nausea c. Vomiting d. Headache e. Photophobia f. Pallor 5. No evidence of an inflammatory, anatomic, metabolic, or neoplastic process considered that explains the subject s symptoms * Criteria fulfilled two or more times in the preceding 12 months
13 Appendix A: Rome III Diagnostic Criteria for FGIDs 897 H2d. Childhood Functional Abdominal Pain 1. Episodic or continuous abdominal pain 2. Insufficient criteria for other FGIDs 3. No evidence of an inflammatory, anatomic, metabolic, or neoplastic process that explains the subject s symptoms * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis H2d1. Childhood Functional Abdominal Pain Syndrome Diagnostic criteria* Must satisfy criteria for childhood functional abdominal pain and have at least 25% of the time one or more of the following: 1. Some loss of daily functioning 2. Additional somatic symptoms such as headache, limb pain, or difficulty sleeping * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis H3. CONSTIPATION AND INCONTINENCE H3a. Functional Constipation Diagnostic criteria* Must include two or more of the following in a child with a developmental age of at least 4 years with insufficient criteria for diagnosis of IBS: 1. Two or fewer defecations in the toilet per week 2. At least one episode of fecal incontinence per week 3. History of retentive posturing or excessive volitional stool retention 4. History of painful or hard bowel movements 5. Presence of a large fecal mass in the rectum 6. History of large diameter stools which may obstruct the toilet * Criteria fulfilled at least once per week for at least 2 months prior to diagnosis H3b. Nonretentive Fecal Incontinence Diagnostic criteria* Must include all of the following in a child with a developmental age at least 4 years: 1. Defecation into places inappropriate to the social context at least once per month 2. No evidence of an inflammatory, anatomic, metabolic, or neoplastic process that explains the subject s symptoms 3. No evidence of fecal retention * Criteria fulfilled for at least 2 months prior to diagnosis
14
CHOC CHILDREN SUROLOGY CENTER. Constipation
 Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
It s A Gut Feeling: Abdominal Pain in Children. David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians
 It s A Gut Feeling: Abdominal Pain in Children David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians Introduction Common Symptom Affects 10-15% of school-aged children Definition (Dr.
It s A Gut Feeling: Abdominal Pain in Children David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians Introduction Common Symptom Affects 10-15% of school-aged children Definition (Dr.
Normal Gastrointestinal Motility and Function
 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily to describe the contraction of the muscles in the gastrointestinal tract. Because the
Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily to describe the contraction of the muscles in the gastrointestinal tract. Because the
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Reporter s Guide to Functional Gastrointestinal Disorders
 Reporter s Guide to Functional Gastrointestinal Disorders Setting the Record Straight Functional GI disorders are among the most common chronic medical conditions and the least understood. Dear Reporter
Reporter s Guide to Functional Gastrointestinal Disorders Setting the Record Straight Functional GI disorders are among the most common chronic medical conditions and the least understood. Dear Reporter
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN
 NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
IBS:Constipation. Richard N. Redinger, M.D. Professor of Medicine
 IBS:Constipation Richard N. Redinger, M.D. Professor of Medicine Functional Bowel Disorders Functional bowel disorders are best understood as a biopsychosocial model of the pathophysiology of illness or
IBS:Constipation Richard N. Redinger, M.D. Professor of Medicine Functional Bowel Disorders Functional bowel disorders are best understood as a biopsychosocial model of the pathophysiology of illness or
Childhood functional gastrointestinal disorders
 II60 Gut 1999;45(Suppl II):II60 II68 Childhood functional gastrointestinal disorders A Rasquin-Weber, P E Hyman, S Cucchiara, D R Fleisher, J S Hyams, P J Milla, A Staiano Co-Chair, Committee on Childhood
II60 Gut 1999;45(Suppl II):II60 II68 Childhood functional gastrointestinal disorders A Rasquin-Weber, P E Hyman, S Cucchiara, D R Fleisher, J S Hyams, P J Milla, A Staiano Co-Chair, Committee on Childhood
Fecal incontinence (Encopresis) It is the fecal incontinence condition observed in children with chronic constipation over 1-2 years.
 WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
Chronic abdominal pain of childhood
 Chronic abdominal pain of childhood Sandra I. Escalera, M.D. ProHealth Physicians Associate Clinical Professor Department of Pediatrics Yale University School of Medicine Objectives Brief overview of approach
Chronic abdominal pain of childhood Sandra I. Escalera, M.D. ProHealth Physicians Associate Clinical Professor Department of Pediatrics Yale University School of Medicine Objectives Brief overview of approach
Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal
 www.complexchild.com Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal A surprisingly large number of children with motility disorders experience the same progression of events
www.complexchild.com Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal A surprisingly large number of children with motility disorders experience the same progression of events
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Chapter 6 Gastrointestinal Impairment
 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Childhood Defecation Disorders: Constipation and Soiling
 Childhood Defecation Disorders: Constipation and Soiling Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New
Childhood Defecation Disorders: Constipation and Soiling Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New
FUNCTIONAL BOWEL DISORDERS
 FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
A 33 year old woman is referred to a gastroenterologist by her primary care physician(pcp) because of a long
 Figure 1: Constant or frequently recurring abdominal pain 1 patient with constant or frequently recurring abdominal pain for at least 6 months: not associated with known systemic disease with loss of daily
Figure 1: Constant or frequently recurring abdominal pain 1 patient with constant or frequently recurring abdominal pain for at least 6 months: not associated with known systemic disease with loss of daily
Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606
 October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
Peptic Ulcer Disease and Dyspepsia. John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital
 Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
Peptic Ulcer Disease and Dyspepsia John M. Inadomi, MD Professor of Medicine UCSF Chief, Clinical Gastroenterology San Francisco General Hospital Case History 49 y/o woman complains of several months of
I can t empty my rectum without pressing my fingers in or near my vagina
 Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Original Article: http://www.mayoclinic.com/health/esophageal-spasms/ds00763
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
Gastrointestinal problems in children with Down's syndrome
 Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Figure 2: Recurrent chest pain of suspected esophageal origin
 Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
Learning Objectives. Introduction to Medical Careers. Vocabulary: Chapter 16 FACTS. Functions. Organs. Digestive System Chapter 16
 Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Constipation in the older child
 Constipation in the older child Definition Constipation in children is a common problem. Constipation in children is often characterized by infrequent bowl movements or hard, dry stools. Various factors
Constipation in the older child Definition Constipation in children is a common problem. Constipation in children is often characterized by infrequent bowl movements or hard, dry stools. Various factors
Why are antidepressants used to treat IBS? Some medicines can have more than one action (benefit) in treating medical problems.
 The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD What are functional GI disorders? There are more
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD What are functional GI disorders? There are more
CLINICAL UPDATE. Irritable Bowel Syndrome IBS
 CLINICAL UPDATE Irritable Bowel Syndrome IBS 2nd Edition 2003, Reprinted 2006 Digestive Health Foundation 2006 Table of Contents 1 Digestive Health Foundation 2 What Is Irritable Bowel Syndrome? 2 How
CLINICAL UPDATE Irritable Bowel Syndrome IBS 2nd Edition 2003, Reprinted 2006 Digestive Health Foundation 2006 Table of Contents 1 Digestive Health Foundation 2 What Is Irritable Bowel Syndrome? 2 How
Abdominal symptoms in relation to perceived health in adults with Familial Adenomatous Polyposis (FAP)
 Abdominal symptoms in relation to perceived health in adults with Familial Adenomatous Polyposis (FAP) Kaisa Fritzell, RN, MSc, Phd student Department of Neurobiology, Care Sciences and Society, Division
Abdominal symptoms in relation to perceived health in adults with Familial Adenomatous Polyposis (FAP) Kaisa Fritzell, RN, MSc, Phd student Department of Neurobiology, Care Sciences and Society, Division
Figure 3: Dysphagia. 14 meets. esophageal. esophageal manometry +/- +/- impedance measurement. structural lesion? no. 19 yes
 Figure 3: Dysphagia 1 patient with dysphagia 2 history and physical exam. suggestive of nesophageal etiology? 3 evaluate and treat as as indicated 4 upper GI GI endoscopy with biopsies 15 achalasia, absent
Figure 3: Dysphagia 1 patient with dysphagia 2 history and physical exam. suggestive of nesophageal etiology? 3 evaluate and treat as as indicated 4 upper GI GI endoscopy with biopsies 15 achalasia, absent
Functional Fecal Retention With Encopresis in Childhood
 Journal of Pediatric Gastroenterology and Nutrition 38:79 84 January 2004 Lippincott Williams & Wilkins, Inc., Philadelphia Functional Fecal Retention With Encopresis in Childhood Vera Loening-Baucke Department
Journal of Pediatric Gastroenterology and Nutrition 38:79 84 January 2004 Lippincott Williams & Wilkins, Inc., Philadelphia Functional Fecal Retention With Encopresis in Childhood Vera Loening-Baucke Department
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel and Bladder Dysfunction in MS. Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center. Bladder Dysfunction
 Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Abdominal Wall Pain. What is Abdominal Wall Pain?
 Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
SOD (Sphincter of Oddi Dysfunction)
 SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
SOD (Sphincter of Oddi Dysfunction) SOD refers to the mechanical malfunctioning of the Sphincter of Oddi, which is the valve muscle that regulates the flow of bile and pancreatic juice into the duodenum.
Problems of the Digestive System
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The Digestive System
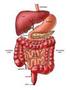 School of Social Work The Digestive System Undergraduate researcher: Nancy D. Bergerson (2010). 1 The Digestive System breaks down and absorbs food. When food is eaten, it is not in a form the body can
School of Social Work The Digestive System Undergraduate researcher: Nancy D. Bergerson (2010). 1 The Digestive System breaks down and absorbs food. When food is eaten, it is not in a form the body can
Symptoms of constipation are extremely common; the
 GASTROENTEROLOGY 2000;119:1761 1778 AMERICAN GASTROENTEROLOGICAL ASSOCIATION American Gastroenterological Association Medical Position Statement: Guidelines on Constipation This document presents the official
GASTROENTEROLOGY 2000;119:1761 1778 AMERICAN GASTROENTEROLOGICAL ASSOCIATION American Gastroenterological Association Medical Position Statement: Guidelines on Constipation This document presents the official
Care and Problems of the Digestive System. Chapter 18 Lesson 2
 Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
Laparoscopic Antireflux Surgery Information Sheet
 Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
IRRITABLE BOWEL SYNDROME
 IRRITABLE BOWEL SYNDROME What is Irritable Bowel Syndrome (IBS)? IBS is one of more than twenty functional gastrointestinal disorders (FGID). These are disorders in which the gastrointestinal (GI) tract
IRRITABLE BOWEL SYNDROME What is Irritable Bowel Syndrome (IBS)? IBS is one of more than twenty functional gastrointestinal disorders (FGID). These are disorders in which the gastrointestinal (GI) tract
COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP)
 The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 19 March 2003 CPMP/EWP/785/97 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) POINTS TO CONSIDER
The European Agency for the Evaluation of Medicinal Products Evaluation of Medicines for Human Use London, 19 March 2003 CPMP/EWP/785/97 COMMITTEE FOR PROPRIETARY MEDICINAL PRODUCTS (CPMP) POINTS TO CONSIDER
IBS. Understanding Constipation. A patient s guide to living with irritable bowel syndrome. a program of
 IBS Understanding Constipation A patient s guide to living with irritable bowel syndrome a program of Constipation Basics } Constipation has different definitions, and individuals define it based on family
IBS Understanding Constipation A patient s guide to living with irritable bowel syndrome a program of Constipation Basics } Constipation has different definitions, and individuals define it based on family
Nash Heartburn Treatment Center
 Nash Heartburn Treatment Center a division of Nash Health Care NHCS Mission Statement: To provide superior quality health care services and to help improve the health of the community in a caring, efficient
Nash Heartburn Treatment Center a division of Nash Health Care NHCS Mission Statement: To provide superior quality health care services and to help improve the health of the community in a caring, efficient
IBS. A patient s guide to living with irritable bowel syndrome. a program of the aga institute
 IBS A patient s guide to living with irritable bowel syndrome a program of the aga institute IBS Basics Irritable bowel syndrome (IBS) is a common disorder of the intestines with symptoms that include
IBS A patient s guide to living with irritable bowel syndrome a program of the aga institute IBS Basics Irritable bowel syndrome (IBS) is a common disorder of the intestines with symptoms that include
FUSSY INFANTS. Boosba Vivatvakin. Department of Pediatric, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand
 FUSSY INFANTS Boosba Vivatvakin Department of Pediatric, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand In the first 3 months of life, crying is a tool that a baby uses to communicate
FUSSY INFANTS Boosba Vivatvakin Department of Pediatric, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand In the first 3 months of life, crying is a tool that a baby uses to communicate
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
NAUSEA AND VOMITING. Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St.
 NAUSEA AND VOMITING Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St. Louis, MO What is nausea and vomiting? Nausea is the unpleasant urge to
NAUSEA AND VOMITING Ryan F. Porter, M.D. and C. Prakash Gyawali, M.D., MRCP Division of Gastroenterology Washington University St. Louis, MO What is nausea and vomiting? Nausea is the unpleasant urge to
IRRITABLE BOWEL SYNDROME - a patient's guide. What is it? What is the cause? Dr Ishy Maharaj - Gastroenterologist
 IRRITABLE BOWEL SYNDROME - a patient's guide Dr Ishy Maharaj - Gastroenterologist What is it? The irritable bowel syndrome is the most common gastrointestinal disease in clinical practice. It is a condition
IRRITABLE BOWEL SYNDROME - a patient's guide Dr Ishy Maharaj - Gastroenterologist What is it? The irritable bowel syndrome is the most common gastrointestinal disease in clinical practice. It is a condition
GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
SECTION H: BLADDER AND BOWEL. H0100: Appliances. Item Rationale Health-related Quality of Life. Planning for Care
 SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
IRRITABLE BOWEL SYNDROME
 IRRITABLE BOWEL SYNDROME CONTENTS Digestive Health Foundation What Is? How Big is the Problem? What Causes? Diagnosis of Other Gut Symptoms in Non Gut Symptoms in Differential Diagnosis of How To Manage
IRRITABLE BOWEL SYNDROME CONTENTS Digestive Health Foundation What Is? How Big is the Problem? What Causes? Diagnosis of Other Gut Symptoms in Non Gut Symptoms in Differential Diagnosis of How To Manage
A guide for adults with. Intestinal. Dysmotility
 A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
Scleroderma Education Program. Chapter 4. Gastrointestinal Tract
 Scleroderma Education Program Chapter 4 Gastrointestinal Tract Chapter 4-1 Chapter Highlights 1. Learn about how the GI tract works. 2. What happens when things go wrong? -Appetite loss -Difficulty chewing
Scleroderma Education Program Chapter 4 Gastrointestinal Tract Chapter 4-1 Chapter Highlights 1. Learn about how the GI tract works. 2. What happens when things go wrong? -Appetite loss -Difficulty chewing
CMS Limitations Guide - Laboratory Services
 CMS Limitations Guide - Laboratory Services Starting October 1, 2015, CMS will update their exisiting medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitattions
CMS Limitations Guide - Laboratory Services Starting October 1, 2015, CMS will update their exisiting medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitattions
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
QS114. NICE quality standard for irritable bowel syndrome in adults (QS114)
 NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
G E R D. (Gastroesophageal Reflux Disease)
 G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
Marginal Ulcers. Marginal Ulcers. Gastric Remnant Ulcers. Double Balloon Enteroscopy. Marginal Ulcer. Gastrojejunal Stricture.
 Upper Abdominal Pain in the Bariatric Surgery Patient Martin L. Freeman, M.D., FASGE,FACG Professor of Medicine Director, Pancreaticobiliary Endoscopy Fellowship Interim Director, Division of GI, Hepatology
Upper Abdominal Pain in the Bariatric Surgery Patient Martin L. Freeman, M.D., FASGE,FACG Professor of Medicine Director, Pancreaticobiliary Endoscopy Fellowship Interim Director, Division of GI, Hepatology
Chemotherapy Side Effects Worksheet
 Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
KEYHOLE HERNIA SURGERY
 Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Tone Up Your Pelvic Floor. A regular pelvic floor exercise ( Kegel ) routine can prevent symptoms before, during, and after childbirth.
 Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Borland-Groover Clinic PATIENT GENERATED MEDICAL HISTORY Name: DOB: Email: Primary Care Physician: Pharmacy: Pharmacy Phone #:
 PATIENT GENERATED MEDICAL HISTORY Name: DOB: Email: Primary Care Physician: Referring: Pharmacy: Pharmacy Phone #: Place Sticker Here Directions: Please circle any of the following you have personally
PATIENT GENERATED MEDICAL HISTORY Name: DOB: Email: Primary Care Physician: Referring: Pharmacy: Pharmacy Phone #: Place Sticker Here Directions: Please circle any of the following you have personally
This document presents the official recommendations of
 GASTROENTEROLOGY 2013;144:211 217 American Gastroenterological Association Medical Position Statement on Constipation The Institute Medical Position Panel consisted of the lead technical review author
GASTROENTEROLOGY 2013;144:211 217 American Gastroenterological Association Medical Position Statement on Constipation The Institute Medical Position Panel consisted of the lead technical review author
The eating problems that children suffer from are very different to those experienced by
 one one types of problem The problems that children suffer from are very different to those experienced by adolescents and adults. There are a larger number of different problems found in children, which
one one types of problem The problems that children suffer from are very different to those experienced by adolescents and adults. There are a larger number of different problems found in children, which
MEDICAL HISTORY AND SCREENING FORM
 MEDICAL HISTORY AND SCREENING FORM The purpose of preventive exams is to screen for potential health problems and provide education to promote optimal health. It is best practice for chronic health problems
MEDICAL HISTORY AND SCREENING FORM The purpose of preventive exams is to screen for potential health problems and provide education to promote optimal health. It is best practice for chronic health problems
Irritable bowel syndrome (IBS)
 Irritable bowel syndrome (IBS) Kok-Ann Gwee, Uday C Ghoshal* Associate Professor, National University of Singapore, and *Associate Professor, Dept. of Gastroenterology, SGPGI, Lucknow, India Story of a
Irritable bowel syndrome (IBS) Kok-Ann Gwee, Uday C Ghoshal* Associate Professor, National University of Singapore, and *Associate Professor, Dept. of Gastroenterology, SGPGI, Lucknow, India Story of a
University of California, Berkeley 2222 Bancroft Way Berkeley, CA 94720 Appointments 510/642-2000 Online Appointment www.uhs.berkeley.
 Constipation Why Am I Constipated? Constipation is passage of small amounts of hard, dry bowel movements, usually fewer than three times a week. People who are constipated may find it difficult and painful
Constipation Why Am I Constipated? Constipation is passage of small amounts of hard, dry bowel movements, usually fewer than three times a week. People who are constipated may find it difficult and painful
PEDIATRIC GASTROENTEROLOGY
 May 05 CLINICAL REFERENCE PEDIATRIC GASTROENTEROLOGY INTRODUCTION Introduction Alberta Referral Pathways for Pediatric GI Services has been a collaborative project. The referral guidelines have considered
May 05 CLINICAL REFERENCE PEDIATRIC GASTROENTEROLOGY INTRODUCTION Introduction Alberta Referral Pathways for Pediatric GI Services has been a collaborative project. The referral guidelines have considered
1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE
 in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
in association with 1 ST JAMAICAN PAEDIATRIC NEPHROLOGY CONFERENCE Jamaica Conference Centre Kingston, Jamaica October 4 th 2014 VOIDING DISORDERS IN CHILDREN Dr. Colin Abel Paediatric Urologist Bustamante
Normal bladder function. Aging of the bladder and urethra
 SECTION 10 Bladder and bowel control (continence) Section overview This section looks at: Normal bladder function Stroke and loss of bladder control (incontinence) Normal bowel function Stroke and bowel
SECTION 10 Bladder and bowel control (continence) Section overview This section looks at: Normal bladder function Stroke and loss of bladder control (incontinence) Normal bowel function Stroke and bowel
Millions of Americans suffer from abdominal pain, bloating, constipation and diarrhea. Now new treatments can relieve your pain and discomfort.
 3888-IBS Consumer Bro 5/8/03 10:38 AM Page 1 TAKE THE IBS TEST Do you have recurrent abdominal pain or discomfort? YES NO UNDERSTANDING IRRITABLE BOWEL SYNDROME A Consumer Education Brochure Do you often
3888-IBS Consumer Bro 5/8/03 10:38 AM Page 1 TAKE THE IBS TEST Do you have recurrent abdominal pain or discomfort? YES NO UNDERSTANDING IRRITABLE BOWEL SYNDROME A Consumer Education Brochure Do you often
4.5 Specialist Health Expertise Guidelines
 4.9 Specialist Health Expertise Guidelines 4.5.9 Faecal incontinence (Encopresis) Background Encopresis may be defined as the voluntary or involuntary passage of formed, semiformed, or liquid stool into
4.9 Specialist Health Expertise Guidelines 4.5.9 Faecal incontinence (Encopresis) Background Encopresis may be defined as the voluntary or involuntary passage of formed, semiformed, or liquid stool into
Pi-Wei System Related Diseases. Introduction
 1 A. Review of Pi-Wei System: I. Functions of Spleen Pi-Wei System Related Diseases Introduction By H. Shen The spleen is situated in the middle jiao and its meridian connects with the stomach with which
1 A. Review of Pi-Wei System: I. Functions of Spleen Pi-Wei System Related Diseases Introduction By H. Shen The spleen is situated in the middle jiao and its meridian connects with the stomach with which
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Upper Gastrointestinal Tract KNH 406
 Upper Gastrointestinal Tract KNH 406 Upper GI A&P GI tract long tube ~ 15 ft. Upper GI mouth, pharynx, esophagus, stomach Accessory organs pancreas, biliary system, liver Four basic functions: motility,
Upper Gastrointestinal Tract KNH 406 Upper GI A&P GI tract long tube ~ 15 ft. Upper GI mouth, pharynx, esophagus, stomach Accessory organs pancreas, biliary system, liver Four basic functions: motility,
Abdominal pain in functional GI disorders
 Abdominal pain in functional GI disorders Hubert LOUIS Service de Gastroentérologie, Hôpital Erasme Hubert.louis@erasme.ulb.ac.be Outline Functional GI disorders: from a clinician view Common Is it really
Abdominal pain in functional GI disorders Hubert LOUIS Service de Gastroentérologie, Hôpital Erasme Hubert.louis@erasme.ulb.ac.be Outline Functional GI disorders: from a clinician view Common Is it really
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Irritable Bowel Syndrome
 Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is irritable bowel syndrome (IBS)? Irritable
Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is irritable bowel syndrome (IBS)? Irritable
THE PRIMARY CARE MANAGEMENT OF CHRONIC CONSTIPATION. Dr Richard Stevens GP in Oxford and editor-in-chief of the Digest and Eurodigest
 THE PRIMARY CARE MANAGEMENT OF CHRONIC CONSTIPATION Dr Richard Stevens GP in Oxford and editor-in-chief of the Digest and Eurodigest Introduction Bowel functions are private. When bowels misfunction, privacy
THE PRIMARY CARE MANAGEMENT OF CHRONIC CONSTIPATION Dr Richard Stevens GP in Oxford and editor-in-chief of the Digest and Eurodigest Introduction Bowel functions are private. When bowels misfunction, privacy
Eating, pooping, and peeing THE DIGESTIVE SYSTEM
 THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
THE DIGESTIVE SYSTEM Ingested food is not technically in the body until it is absorbed so it needs to be: Mechanically and chemically reduced Transported by the blood to the cells Large portions are not
CHPN Review Course Pain Management Part 1 Hospice and Palliative Nurses Association
 CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
CHPN Review Course Pain Management Part 1 Disclosures Bonnie Morgan has no real or perceived conflicts of interest that relate to this presentation. Copyright 2015 by the. HPNA has the exclusive rights
1 Common Symptoms and Signs in Gastroenterology
 1 Common Symptoms and Signs in Gastroenterology C. Dubé With sections authored by: R.F. Bursey, M.C. Champion, J.M. Fardy, S. Grégoire, D.G. MacIntosh, D.G. Patel, A. Rostom, N. Saloojee, L.J. Scully,
1 Common Symptoms and Signs in Gastroenterology C. Dubé With sections authored by: R.F. Bursey, M.C. Champion, J.M. Fardy, S. Grégoire, D.G. MacIntosh, D.G. Patel, A. Rostom, N. Saloojee, L.J. Scully,
2015 Clinical Education Course Catalog
 2015 Clinical Education Course Catalog 1 Table of Contents and Course Objectives The objective of Sandhill University is to provide clinical users with the knowledge and skills necessary to effectively
2015 Clinical Education Course Catalog 1 Table of Contents and Course Objectives The objective of Sandhill University is to provide clinical users with the knowledge and skills necessary to effectively
Dallas Neurosurgical and Spine Associates, P.A Patient Health History
 Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Dallas Neurosurgical and Spine Associates, P.A Patient Health History DOB: Date: Reason for your visit (Chief complaint): Past Medical History Please check corresponding box if you have ever had any of
Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly. Prapa Pattrapornpisut 7 June 2012
 1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
Urinary Incontinence in Women. Susan Hingle, M.D. Department of Medicine
 Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
NEW PATIENT CONSULTATION FORM. Social Security Number - - Date of Birth Age. Home Address. Home phone Cell phone. Work phone Email address
 NEW PATIENT CONSULTATION FORM Welcome to our office. Please fill out the first four pages. Date Name Social Security Number - - Date of Birth Age Home Address Home phone Cell phone Work phone Email address
NEW PATIENT CONSULTATION FORM Welcome to our office. Please fill out the first four pages. Date Name Social Security Number - - Date of Birth Age Home Address Home phone Cell phone Work phone Email address
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Basics on Bladder and Bowel
 Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Women s Continence and Pelvic Health Center
 Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
CHOP Chemotherapy Regimen for Lymphoma Information for Patients
 CHOP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cytoxan (cyclophosphamide) H: Adriamycin (hydroxy doxorubicin) O: vincristine (Oncovin ) P: Prednisone How Is This
CHOP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cytoxan (cyclophosphamide) H: Adriamycin (hydroxy doxorubicin) O: vincristine (Oncovin ) P: Prednisone How Is This
7 Reasons You Can t Eat the Foods You Love!
 Dr. Susan Plank s Report: 7 Reasons You Can t Eat the Foods You Love! Betsy Coltrain sat feeling miserable on the couch. She had just finished eating dinner and began to feel the uncomfortable fullness,
Dr. Susan Plank s Report: 7 Reasons You Can t Eat the Foods You Love! Betsy Coltrain sat feeling miserable on the couch. She had just finished eating dinner and began to feel the uncomfortable fullness,

 More details >>> HERE
More details >>> HERE  Full version is >>> HERE
Full version is >>> HERE  More information >>> HERE
More information >>> HERE