Childhood Defecation Disorders: Constipation and Soiling
|
|
|
- Cecily McDaniel
- 8 years ago
- Views:
Transcription
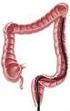
1 Childhood Defecation Disorders: Constipation and Soiling Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New Orleans, Louisiana By: Paul Hyman, M.D., Professor of Pediatrics, Chief, Division of Pediatric Gastroenterology, Louisiana State University Health Sciences Center, New Orleans, Louisiana The purpose of this publication is to describe the characteristics and treatment of four pediatric functional gastrointestinal disorders that prompt parents to bring their child to the doctor for constipation and/or soiling: infant dyschezia, functional constipation, functional fecal retention, and non-retentive fecal soiling. [A functional disorder refers to a condition where the primary abnormality is an altered physiological function (the way the body works) rather than an abnormality that is characterized by tissue damage or inflammation.] In the context of this article, "functional" means that the symptoms occur within the expected range of the body's behavior. (Examples: Shivering after a cold swim is a symptom, but not due to disease; a runner's leg cramp is very painful, but the muscle is healthy.) Genetics, diet, social habits, convenience, cultural beliefs, relationships within the family, and timing of daily activities influence how often a child has a bowel movement. In healthy children, the number of bowel movements (BMs) changes with age and diet. Infants average four BMs each day during the first week of life. There is a decline to about two BMs each day by age two, and one BM each day by age four. Healthy breast-fed infants may have no BMs for weeks. New parents may want to have the symptom checked by a pediatrician, but should be reassured by the absence of alarm symptoms such as vomiting, fever, failure to gain weight, or abdominal distention. Any of these features, along with the infrequent passage of stool, should prompt a visit to the pediatrician. Constipation is defined by a reduced stool frequency, or by painful bowel movements, even when the stool frequency is not reduced. Constipation accounts for 3% of visits to the pediatrician, and about 25% of visits to the pediatric gastroenterologist. Constipation is a problem for about 1 in 6 children at some time. Boys and girls are equally affected.
2 Infant Dyschezia Dyschezia means difficulty coordinating the reflexes necessary to pass a bowel movement. Parents visit the clinician during their infant's first six months of life concerned that their child is constipated. The parents describe a healthy infant, who cries for minutes, screaming, and turning red in the face with effort, until a bowel movement finally takes place. The stools are soft and free of blood. These crying episodes, exhausting for the infant and anxiety provoking for the parents, occur several times daily. This examination includes charting the infant's growth, history (including diet), and a physical examination (including rectal examination). All are normal. For infants, a successful bowel movement requires two coordinated events: relaxation of the pelvic floor muscles (a thick sheath of muscle that spans the underlying surface of the bony pelvis), and an increase in abdominal pressure to squeeze out the stool. Infants with dyschezia have not yet learned to coordinate those two required actions. Crying is how they increase their abdominal pressure. They cry until, by chance, they relax their pelvic floor muscles at the same time and a BM occurs. Reassurance to the parents is all that is needed. No tests or treatments are necessary. The infant is not crying from pain. The infant will learn to have bowel movements more easily in a few days to a few weeks. Suppositories and rectal stimulation interfere with the infant's learning to coordinate the act. They should not be part of the treatment. Functional Constipation Functional constipation is defined by passage of hard, pebble-like stools, or the passage of fewer than two BMs per week for two weeks or more in otherwise healthy infants and children. The transition from breast to formula feedings is a common time for the start of functional constipation. In most cases, laboratory and x-ray examinations are not necessary for the diagnosis of functional constipation. However, if there are worrisome signs like poor weight gain, persistent abdominal distention, unexplained fevers, Down syndrome, bilious vomiting, occult spinal dysraphism [neurological involvement of Spina Bifida], then a thorough evaluation is appropriate. Infants and children who pass soft stools at intervals greater than a week apart, and fail to thrive, will require a diagnostic evaluation for an abnormality in the gastrointestinal anatomy or a metabolic disease. Delayed passage of meconium, the sticky dark, first BM of the newborn is associated with Hirschsprung's disease. [Hirschsprung's disease is a lack of nerve (ganglion) cells in a segment
3 of the bowel. This interferes with the squeezing action called peristalsis, which normally moves stool through the intestines.] Functional constipation is important to treat because it may predispose the child to develop functional fecal retention. Painful passage of hard stool may inhibit the child from relaxing their bottoms when they feel an urge for a BM. A huge BM may accumulate inside. Fruit juices such as prune and pear may increase stool water by virtue of their fructose and sorbitol content, carbohydrates that are poorly absorbed by the small intestine. When dietary intervention alone does not help, non-stimulant laxatives like polyethylene glycol, mineral oil and lactulose can be effective, but only under a doctor's supervision. Functional Fecal Retention Functional fecal retention is defined, in a person from infancy to 16 years old, by the passage of large or enormous bowel movements at intervals less than twice per week, and the attempt to avoid having bowel movements on purpose, by contracting the muscles of the pelvic floor and squeezing the buttocks together. Accompanying symptoms include soiling of the underclothes, irritability, abdominal cramps, and decreased appetite. These symptoms disappear immediately following the passage of a large or enormous bowel movement. Sometimes retentive constipation is associated with bedwetting, and 10% of affected girls get urinary tract infections. Functional fecal retention begins when there is a painful or frightening bowel movement, and the child learns to fear the urge to have a bowel movement. They begin to hold back when they get the urge and a huge stool builds up in their rectum. Often, children are able to hold back the huge stool for weeks, but when they pass gas, small amounts of liquid or solid come out with the gas, soiling the underclothes. Soiling may occur many times a day. Some people refer to soiling as fecal incontinence or encopresis. Functional fecal retention often begins during one of three times: 1) in infants, at the time of weaning from breast milk to formula, with a change in bowel movements from soft to hard pellets, 2) in toddlers during toilet training as they struggle with issues of controlling bowel movements, and 3) in children beginning school, where they must hold back the urge to have a bowel movement (BM) to stay seated in class. A history and a careful physical examination provide reassurance to the clinician and parents that there is no disease, but that there are symptoms caused by a failure to relax the bottom and push out the bowel movement. Often, there is a mass of stool that the physician can feel on either side of the abdominal muscles when examining the belly. When the diagnosis is retentive constipation, no
4 testing is necessary. Diseases of the colon have a different history and physical examination than retentive constipation. (See Table) If there is a history of constipation from birth, no retentive posturing, or no passage of huge bowel movements, then it is important to test for Hirschsprung's disease and other rare colon motility diseases. Remember that 1 in 6 children will have constipation, and Hirschsprung's disease is the most common colon motility disease, with a rate of 1 in 5000 children, so chance of having Hirschsprung's or any other serious disease is small. Differentiating Functional Fecal Retention from Disease* Feature Fecal Retention Disease Starts at Birth Rare Common Fecal Soiling Common Rare Fecal Mass Above Rectum No Common Retentive Posturing (holding back) Common Rare Passage of Very Large Stools Common Rare Painful Bowel Movements Common Rare * This differentiation is not intended to replace the appropriate diagnosis and treatment of your child by a qualified pediatric doctor. Infants and toddlers From a developmental point of view, functional fecal retention is a failure in toilet learning. Normally, when an infant senses a need for a bowel movement, he or she relaxes their bottom and at the same time increases abdominal pressure. Infants have months to practice this behavior before the opportunity to hold back a bowel movement becomes a social choice. Functional fecal retention begins when the child fears passing a bowel movement, most often because BMs are big and hard and hurt as they come out. The child's bottom contracts instead of relaxing, as the child attempts to avoid having a bowel movement. The inside walls of the colon stretch to hold the contents, and the urge to have a bowel movement passes. Over weeks and months the end of the colon stretches out. The infrequent passage of very large stools may cause not only pain, but also tears in the anus, the short canal at the end of the digestive tract. These tears, called anal fissures, bleed, leading to more pain for the child and frightening the parents. Children with retentive constipation sit on the toilet and push, but because they are afraid, they are unable to relax their bottoms, so the bowel movement does not come out. Parents often report that the child tries really hard to push it out. It is true that they do, but at the same time they are not relaxing their bottom. When you are afraid, you cannot relax your bottom.
5 Parents become increasingly distressed by their child's symptoms, and contact a clinician. Some clinicians recommend suppositories or enemas, thinking that as uncomfortable as the procedure is, it will succeed in expelling the big bowel movement. In adults this makes sense, but in children, it is shortsighted. Suppositories and enemas take control away from the child, and may frighten the child even more. These interventions do not help the child relearn how to relax their bottoms and have a bowel movement. The next time there is an urge for a bowel movement, the child may be more frightened, and hold back even more. School-age children Sometimes functional fecal retention lasts only a few weeks, but sometimes it lasts for years. Many affected school-age children develop negative thoughts about themselves, and wrongly believe that they are the only ones with this problem. To cope, they behave with nonchalance concerning soiling and denial about constipation. They claim to be unaware of odors. Some hide soiled underclothing or pieces of stool around the house. Their denial of the problem is a big part of the problem. The child is unable to cooperate with parents, school or clinician because the child denies that there is a problem. These children shrug their shoulders and tell the doctor that they do not know why they are in the doctor's office. They show little interest in treatment, and they frustrate their parents. Parents who follow doctor's instructions find that treatments fail. Treatments fail because regardless of how much stool collects in the colon and how uncomfortable the child may be, the child may refuse to relax the pelvic floor to allow a bowel movement. Treatment succeeds only after the child decides to participate by attending to the sensations that signal a need to have a bowel movement, and behaving by going to the restroom and relaxing his or her bottoms. Treatment It is important to understand the problem as the child understands it. In infants and preschool children, it is all about fear. As soon as they experience a period of painless BMs, their fear goes away and they learn how to relax their bottoms. In school age children, they may be secretive about the problem, and pretend that it does not exist. Before treatment works for them, they must accept responsibility for recognizing the urge to have a BM and cooperate by taking their medicine and relaxing their bottoms. Treatment goals for the clinician are to educate the child and family about the problem, to use medication to assure painless defecation, and to provide continuing availability and interest. Education includes teaching the parent and child that functional fecal retention: 1) is not a disease, but symptoms due to failed toilet learning, 2) always gets better when the child chooses to relearn the correct way to have a bowel
6 movement, 3) is not dangerous it never causes cancer, the colon never bursts, toxins never go back into the bloodstream, no matter how long between bowel movements, and 4) is very common. The child is not alone. To assure painless defecation, non-stimulant stool softeners may be given safely every day for months or even years, under the direction of your child's physician. The goal is to make sure that there will always be soft bowel movements, with a diameter less than that of a quarter. Polyethylene glycol has become the most popular medicine, because it mixes colorless, odorless, and tasteless into the child's favorite drink. Mineral oil is a lubricant and softener with many favorable qualities. There is a commercial form of mineral oil (Kondremull) that mixes easily into infant formula or flavored milk, so that infants and children who are reluctant to take medicine are unaware of the mineral oil. Milk of magnesia, lactulose, and sorbitol (the substance found in prune juice that makes BMs soft) are other choices for softening the BMs. The most appropriate choice and dose of stool softener for your child are determined by the physician. Two problems must be overcome for the child to stop holding back - the large hard stools and the fear. Although the non-stimulant stool softener solves the problem of large hard stools, the fear of a painful BM often takes months to subside. It is important for parents to be consistent about medicating the child every day, because one painful bowel movement will cause more fear, and more holding back. Usually, polyethylene glycol or other stool softeners can be stopped after several months free from pain and soiling. Relapses are common, especially during vacations and times of stress. A successful initial treatment plan serves as the model for relapse treatment. relapses tend to resolve quickly. The clinician should provide continuing availability. The clinician is an empathetic teacher who helps the child relearn how to have a BM without pain, and helps the family understand the nature of the problem. Weekly visits and telephone or e- mail accessibility provide effective reassurance and an opportunity for positive reinforcement for good results. Some patients benefit from other interventions: 1. Star charts or stickers for appropriate behaviors like sitting on the toilet or having a BM in the toilet. 2. Anorectal biofeedback may be helpful for older children seeking a way to relearn faster than trial and error at home. 3. Drugs that stimulate an urge to go may be helpful in training some patients to recognize and respond to the sensation. 4. Collaboration with a mental health professional is helpful when retentive constipation is one of a cluster of behavioral symptoms such as temper tantrums and sleep disorder in toddlers, associated with attention deficit
7 disorder in school children, or the presenting symptom of a distressed family situation. In general, it is not necessary to fuss with diet and fiber. What parent wants to battle their child about diet when they are already struggling over bowel movements? The wise clinician prescribes sufficient stool softener and lifts dietary restrictions. Non-retentive Fecal Soiling Fecal soiling refers to passage of bowel movements into the underclothing, or other inappropriate places. Fecal soiling commonly accompanies functional fecal retention, when liquid BM leaks out as the child attempts to pass gas. Fecal soiling without fecal retention occurs when someone has diarrhea, as the muscles of the bottom fatigue and cannot hold back anymore. Functional non-retentive fecal soiling is diagnosed in children older than 4, who have bowel movements in places and at times that are inappropriate, at least once a week for 3 months, in the absence of a disease to explain it, and without signs of fecal retention. About one in ten children who soils has functional nonretentive fecal soiling. The rest have functional fecal retention. Most children with functional non-retentive fecal soiling have BMs daily during waking hours, and do not complain of constipation. Soiling may be in small amounts, or consist of an entire bowel movement. In contrast to children with functional fecal retention and soiling, children with non-retentive soiling do not hold back their BMs and do not accumulate a big stool. Sometimes functional non-retentive fecal soiling is caused by an emotional disturbance in a school-aged child. Often the soiling episodes have a relationship to a person or time of day, because the soiling acts are triggered by unconscious anger. Treatment goals are to help the parent to understand that there is no medical disease, and to accept a referral to a mental health professional. Parents need guidance to understand that soiling is a symptom of emotional upset, not simply bad behavior.
8 1. The rectum is empty. There is no urge to defecate. 2. Stool enters the rectum and stretches the rectal wall, causing a sensation of fullness. 3. Rectal wall distention causes reflex relaxation of the internal anal sphincter, allowing the stool to descend into the proximal anal canal. This movement causes an awareness that stool passage is imminent. 4. The pelvic floor muscles contract to maintain continence, moving the stool upward and out of the anal canal. 5. If the stool remains in the rectum after the pelvic floor returns to its resting state, then stool will no longer be in contact with the anus. The rectal wall relaxes, reducing the pressure and wall tension, and the urge to defecate abates. 6. Defecation occurs when the pelvic floor relaxes, and the pressure in the rectum is greater than pressure from the external anal sphincter and the pelvic floor. Stool moves from the region of higher pressure to the area of lower pressure. The accompanying increase in intra-abdominal pressure propels stool through the anus. 7. The pelvic floor contracts again when stool is no longer in contact with the anus, and this forces out any remaining stool. 8. If a child repeatedly responds to the urge by withholding (C and D), a fecal mass accumulates. Over time the fecal mass becomes too large and too firm to be extruded without painful stretching of the anus. The mass is too bulky to be shifted out of contact with the anoderm. As pelvic floor muscles fatigue, the anus becomes less competent and retentive fecal soiling with soft or liquid stool occurs. The child resorts to retentive posturing, attempting to preserve continence by vigorous contraction of the gluteal muscles.
9 Opinions expressed are an author's own and not necessarily those of the International Foundation for Functional Gastrointestinal Disorders (IFFGD). IFFGD does not guarantee nor endorse any product in this publication nor any claim made by an author and disclaims all liability relating thereto. This article is in no way intended to replace the knowledge or diagnosis of your doctor. We advise seeing a physician whenever a health problem arises requiring an expert's care. IFFGD is a nonprofit education and research organization. Our mission is to inform, assist, and support people affected by gastrointestinal disorders. For more information, or permission to reprint this article, write to IFFGD, PO Box , Milwaukee, WI Toll free: Visit our websites at: or IFFGD. All rights reserved. Used with permission.
CHOC CHILDREN SUROLOGY CENTER. Constipation
 Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation in the older child
 Constipation in the older child Definition Constipation in children is a common problem. Constipation in children is often characterized by infrequent bowl movements or hard, dry stools. Various factors
Constipation in the older child Definition Constipation in children is a common problem. Constipation in children is often characterized by infrequent bowl movements or hard, dry stools. Various factors
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Fecal incontinence (Encopresis) It is the fecal incontinence condition observed in children with chronic constipation over 1-2 years.
 WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
WHAT IS DYSFUNCTIONAL URINATION (URINATION FUNCTION DISORDER)? It stands for the urination phase disorders, which appear due to wrongly acquired urination habits during the toilet training of some neurologically
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN
 NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
Successful Toilet Training and Beyond
 Successful Toilet Training and Beyond Anna Edwards, Ph.D., Clinical Child Psychologist Kristen Michener, Ph.D., Clinical Child Psychologist Made For Kids, Inc. www.made4kids.org Intro Most children have
Successful Toilet Training and Beyond Anna Edwards, Ph.D., Clinical Child Psychologist Kristen Michener, Ph.D., Clinical Child Psychologist Made For Kids, Inc. www.made4kids.org Intro Most children have
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
I can t empty my rectum without pressing my fingers in or near my vagina
 Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
FUNCTIONAL BOWEL DISORDERS
 FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
FUNCTIONAL BOWEL DISORDERS Contributed by the International Foundation for Functional Gastrointestinal Disorders (IFFGD) and edited by the Patient Care Committee of the ACG. INTRODUCTION Doctors use the
It s A Gut Feeling: Abdominal Pain in Children. David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians
 It s A Gut Feeling: Abdominal Pain in Children David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians Introduction Common Symptom Affects 10-15% of school-aged children Definition (Dr.
It s A Gut Feeling: Abdominal Pain in Children David Deutsch, MD Pediatric Gastroenterology Rockford Health Physicians Introduction Common Symptom Affects 10-15% of school-aged children Definition (Dr.
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Functional Fecal Retention With Encopresis in Childhood
 Journal of Pediatric Gastroenterology and Nutrition 38:79 84 January 2004 Lippincott Williams & Wilkins, Inc., Philadelphia Functional Fecal Retention With Encopresis in Childhood Vera Loening-Baucke Department
Journal of Pediatric Gastroenterology and Nutrition 38:79 84 January 2004 Lippincott Williams & Wilkins, Inc., Philadelphia Functional Fecal Retention With Encopresis in Childhood Vera Loening-Baucke Department
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is flexible sigmoidoscopy? Flexible sigmoidoscopy
Flexible Sigmoidoscopy National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is flexible sigmoidoscopy? Flexible sigmoidoscopy
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Understanding and managing your bowel program
 Understanding and managing your bowel program A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care
Understanding and managing your bowel program A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
A guide for adults with. Intestinal. Dysmotility
 A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
Pediatric Incontinence
 Alberta Aids to Daily Living P R O G R A M Pediatric Incontinence PROGRAM MANDATE: The Alberta Aids to Daily Living (AADL) program helps Albertans with a long-term disability, chronic illness or terminal
Alberta Aids to Daily Living P R O G R A M Pediatric Incontinence PROGRAM MANDATE: The Alberta Aids to Daily Living (AADL) program helps Albertans with a long-term disability, chronic illness or terminal
Irritable Bowel Syndrome
 What I need to know about Irritable Bowel Syndrome NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services What I need to know
What I need to know about Irritable Bowel Syndrome NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services What I need to know
Bladder and Bowel Problems Associated with Multiple Sclerosis
 Bladder and Bowel Problems Associated with Multiple Sclerosis Bladder Dysfunction Bladder dysfunction is one of the most common symptoms associated with Multiple Sclerosis Surveys have indicated that 60-90%
Bladder and Bowel Problems Associated with Multiple Sclerosis Bladder Dysfunction Bladder dysfunction is one of the most common symptoms associated with Multiple Sclerosis Surveys have indicated that 60-90%
Approach to Constipation. Dr. S. Budree (Paed GIT Fellow) Dr. L. Goddard (HOD PaedGIT) Dr. R. De Lacy (Snr Consultant Paed GIT)
 Approach to Constipation Dr. S. Budree (Paed GIT Fellow) Dr. L. Goddard (HOD PaedGIT) Dr. R. De Lacy (Snr Consultant Paed GIT) Definition: Constipation No standardized or comparable definition Constipation
Approach to Constipation Dr. S. Budree (Paed GIT Fellow) Dr. L. Goddard (HOD PaedGIT) Dr. R. De Lacy (Snr Consultant Paed GIT) Definition: Constipation No standardized or comparable definition Constipation
However, if your child is learning how to use the toilet without problems, there is no need to stop because of these situations.
 Toilet Training Readiness When do I start? Bowel and bladder control is a necessary skill. Teaching your child to use the toilet takes time, understanding, and patience. The important thing to remember
Toilet Training Readiness When do I start? Bowel and bladder control is a necessary skill. Teaching your child to use the toilet takes time, understanding, and patience. The important thing to remember
4.5 Specialist Health Expertise Guidelines
 4.9 Specialist Health Expertise Guidelines 4.5.9 Faecal incontinence (Encopresis) Background Encopresis may be defined as the voluntary or involuntary passage of formed, semiformed, or liquid stool into
4.9 Specialist Health Expertise Guidelines 4.5.9 Faecal incontinence (Encopresis) Background Encopresis may be defined as the voluntary or involuntary passage of formed, semiformed, or liquid stool into
Maintaining Proper Bowel Elimination
 Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the nursing assistant should be able to: 1. Describe the normal
Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the nursing assistant should be able to: 1. Describe the normal
FAILURE TO THRIVE What Is Failure to Thrive?
 FAILURE TO THRIVE The first few years of life are a time when most children gain weight and grow much more rapidly than they will later on. Sometimes, however, babies and children don't meet expected standards
FAILURE TO THRIVE The first few years of life are a time when most children gain weight and grow much more rapidly than they will later on. Sometimes, however, babies and children don't meet expected standards
URINARY PROBLEMS IN PARKINSON'S DISEASE Julie H.Carter, R.N., M.S., A.N.P.
 URINARY PROBLEMS IN PARKINSON'S DISEASE Julie H.Carter, R.N., M.S., A.N.P. Urinary incontinence (involuntary loss of urine), is a common symptom in Parkinson's disease. A person's embarrassment about this
URINARY PROBLEMS IN PARKINSON'S DISEASE Julie H.Carter, R.N., M.S., A.N.P. Urinary incontinence (involuntary loss of urine), is a common symptom in Parkinson's disease. A person's embarrassment about this
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
AAP Section on Developmental and Behavioral Pediatrics Newsletter, Fall 2013. continued on page 11
 Managing Encopresis in the Pediatric Setting By Edward R. Christophersen, PhD, FAAP (Hon) and Matthew Wassom, PhD Children s Mercy Hospitals and Clinics, Kansas City, Missouri Encopresis is defined as
Managing Encopresis in the Pediatric Setting By Edward R. Christophersen, PhD, FAAP (Hon) and Matthew Wassom, PhD Children s Mercy Hospitals and Clinics, Kansas City, Missouri Encopresis is defined as
Gastrointestinal problems in children with Down's syndrome
 Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Geriatric Medicine. Advice on. Constipation and Laxatives
 Geriatric Medicine Advice on Constipation and Laxatives 1 Constipation Constipation is defined as having bowel movements less than three times a week. Stools are usually hard, dry, small in size and difficult
Geriatric Medicine Advice on Constipation and Laxatives 1 Constipation Constipation is defined as having bowel movements less than three times a week. Stools are usually hard, dry, small in size and difficult
Daily Habits and Urinary Incontinence
 Effects of Daily Habits on the Bladder Many aspects of our daily life influence bladder and bowel function. Sometimes our daily habits may not be in the best interest of the bladder. A number of surprisingly
Effects of Daily Habits on the Bladder Many aspects of our daily life influence bladder and bowel function. Sometimes our daily habits may not be in the best interest of the bladder. A number of surprisingly
Recovery After Stroke: Bladder & Bowel Function. Treatments
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
IBS. Understanding Constipation. A patient s guide to living with irritable bowel syndrome. a program of
 IBS Understanding Constipation A patient s guide to living with irritable bowel syndrome a program of Constipation Basics } Constipation has different definitions, and individuals define it based on family
IBS Understanding Constipation A patient s guide to living with irritable bowel syndrome a program of Constipation Basics } Constipation has different definitions, and individuals define it based on family
Staying Dry: Good bladder habits for your child
 Staying Dry: Good bladder habits for your child Developed by the health care professionals of Urology Department with assistance from the Department of Learning and Development. All rights reserved. No
Staying Dry: Good bladder habits for your child Developed by the health care professionals of Urology Department with assistance from the Department of Learning and Development. All rights reserved. No
University of California, Berkeley 2222 Bancroft Way Berkeley, CA 94720 Appointments 510/642-2000 Online Appointment www.uhs.berkeley.
 Constipation Why Am I Constipated? Constipation is passage of small amounts of hard, dry bowel movements, usually fewer than three times a week. People who are constipated may find it difficult and painful
Constipation Why Am I Constipated? Constipation is passage of small amounts of hard, dry bowel movements, usually fewer than three times a week. People who are constipated may find it difficult and painful
A Parent s Guide to Understanding Congenital Hypothyroidism. Children s of Alabama Department of Pediatric Endocrinology
 A Parent s Guide to Understanding Congenital Hypothyroidism Children s of Alabama Department of Pediatric Endocrinology How did you get here? Every baby born in the state of Alabama is required by law
A Parent s Guide to Understanding Congenital Hypothyroidism Children s of Alabama Department of Pediatric Endocrinology How did you get here? Every baby born in the state of Alabama is required by law
Centre for Community Child Health and Department of General Medicine. Training Diary
 Centre for Community Child Health and Department of General Training Diary Training Diary This diary belongs to This training diary is based on original work by Professor Terry Nolan, published in 1991
Centre for Community Child Health and Department of General Training Diary Training Diary This diary belongs to This training diary is based on original work by Professor Terry Nolan, published in 1991
Bowel cancer: should I be screened?
 Patient information from the BMJ Group Bowel cancer: should I be screened? Bowel cancer is a serious condition, but there are good treatments. Treatment works best if it's started early.to pick up early
Patient information from the BMJ Group Bowel cancer: should I be screened? Bowel cancer is a serious condition, but there are good treatments. Treatment works best if it's started early.to pick up early
Millions of Americans suffer from abdominal pain, bloating, constipation and diarrhea. Now new treatments can relieve your pain and discomfort.
 3888-IBS Consumer Bro 5/8/03 10:38 AM Page 1 TAKE THE IBS TEST Do you have recurrent abdominal pain or discomfort? YES NO UNDERSTANDING IRRITABLE BOWEL SYNDROME A Consumer Education Brochure Do you often
3888-IBS Consumer Bro 5/8/03 10:38 AM Page 1 TAKE THE IBS TEST Do you have recurrent abdominal pain or discomfort? YES NO UNDERSTANDING IRRITABLE BOWEL SYNDROME A Consumer Education Brochure Do you often
Irritable Bowel Syndrome
 Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is irritable bowel syndrome (IBS)? Irritable
Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is irritable bowel syndrome (IBS)? Irritable
Colon and Rectal Cancer
 Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Childhood Constipation Toddler/Children
 Childhood Constipation Toddler/Children Public Health Nursing and Community Nutrition Services Interior Health Authority February 2013 Feedback welcome to Nutrition.earlyyears@interiorhealth.ca 1 Developed
Childhood Constipation Toddler/Children Public Health Nursing and Community Nutrition Services Interior Health Authority February 2013 Feedback welcome to Nutrition.earlyyears@interiorhealth.ca 1 Developed
Children s Cancer Pain Can Be Relieved A Guide for Parents and Families
 Children s Cancer Pain Can Be Relieved A Guide for Parents and Families This booklet is dedicated to Shaney Banks and all other children with cancer. Wisconsin Cancer Pain Initiative 1989 This booklet
Children s Cancer Pain Can Be Relieved A Guide for Parents and Families This booklet is dedicated to Shaney Banks and all other children with cancer. Wisconsin Cancer Pain Initiative 1989 This booklet
Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence
 Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY
 BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
Urinary Incontinence Definitions
 (AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
(AADL) Program Urge Stress Overflow Functional Mixed DHIC (Detrussor hyperreflexia with impaired contractility) Reflex Incontinence Leakage of urine (usually larger volumes) because of inability to delay
Dietary Fiber. Soluble fiber is fiber that partially dissolves in water. Insoluble fiber does not dissolve in water.
 Dietary Fiber Introduction Fiber is a substance in plants. Dietary fiber is the kind of fiber you get from the foods you eat. Fiber is an important part of a healthy diet. Fiber helps get rid of excess
Dietary Fiber Introduction Fiber is a substance in plants. Dietary fiber is the kind of fiber you get from the foods you eat. Fiber is an important part of a healthy diet. Fiber helps get rid of excess
Common Bowel Problems
 Bowel Problems the ba sic fac t s multiple sclerosis The bowel: what it is, what it does The bowel, also known as the colon or large intestine, makes up the lower portion of the digestive system. This
Bowel Problems the ba sic fac t s multiple sclerosis The bowel: what it is, what it does The bowel, also known as the colon or large intestine, makes up the lower portion of the digestive system. This
Overactive bladder syndrome (OAB)
 Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or desire to pass
When Bed-Wetting Becomes A Problem. A Guide for Patients and their Families
 When Bed-Wetting Becomes A Problem A Guide for Patients and their Families Bed-wetting loss of urine during sleep can be a major problem for children. Bed-wetting is almost never done on purpose or due
When Bed-Wetting Becomes A Problem A Guide for Patients and their Families Bed-wetting loss of urine during sleep can be a major problem for children. Bed-wetting is almost never done on purpose or due
Patients who fail to bring a driver/someone to stay with them for the night will have their procedure cancelled immediately.
 Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Preparing for your Colonoscopy You must have someone and/or a driver accompany you and stay with you for 24 hours after your procedure. Patients who fail to bring a driver/someone to stay with them for
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear
 Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
Caring for your perineum and pelvic floor after a 3rd or 4th degree tear Most women, up to nine in ten (90%), tear to some extent during childbirth. Most tears occur in the perineum, the area between the
Bowel and Bladder Dysfunction in MS. Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center. Bladder Dysfunction
 Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
MANAGING CHRONIC CONSTIPATION A PATIENT G U IDE
 MANAGING CHRONIC CONSTIPATION A PATIENT G U IDE Do you have Fewer than three bowel movements per week? The need to strain during bowel movements at least 25 percent of the time? A feeling of not being
MANAGING CHRONIC CONSTIPATION A PATIENT G U IDE Do you have Fewer than three bowel movements per week? The need to strain during bowel movements at least 25 percent of the time? A feeling of not being
WHAT IS INCONTINENCE?
 CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
X-Plain Hypoglycemia Reference Summary
 X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
X-Plain Hypoglycemia Reference Summary Introduction Hypoglycemia is a condition that causes blood sugar level to drop dangerously low. It mostly shows up in diabetic patients who take insulin. When recognized
INFORMATION FOR YOU. Lower Back Pain
 INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
The Well Woman Centre. Adult Urinary Incontinence
 The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
STROKE CARE PLAN: BLADDER & BOWEL CONTINENCE
 Urinary incontinence related to loss of ability to identify and respond to need to urinate; involuntary bladder contractions, increased nightly urine production, difficulty communication need to urinate
Urinary incontinence related to loss of ability to identify and respond to need to urinate; involuntary bladder contractions, increased nightly urine production, difficulty communication need to urinate
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Chronic Diarrhea in Children
 Chronic Diarrhea in Children National Digestive Diseases Information Clearinghouse What is chronic diarrhea? Diarrhea is loose, watery stools. Chronic, or long lasting, diarrhea typically lasts for more
Chronic Diarrhea in Children National Digestive Diseases Information Clearinghouse What is chronic diarrhea? Diarrhea is loose, watery stools. Chronic, or long lasting, diarrhea typically lasts for more
15 things you might not know about back pain
 15 things you might not know about back pain Mary O Keeffe (University of Limerick), Dr Kieran O Sullivan (University of Limerick), Dr Derek Griffin (Tralee Physiotherapy Clinic) Managing back pain costs
15 things you might not know about back pain Mary O Keeffe (University of Limerick), Dr Kieran O Sullivan (University of Limerick), Dr Derek Griffin (Tralee Physiotherapy Clinic) Managing back pain costs
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Bowel problems in Congenital Myotonic Dystrophy. by Tim Kerr, Stephanie Robb & Graham Clayden.
 Bowel problems in Congenital Myotonic Dystrophy by Tim Kerr, Stephanie Robb & Graham Clayden. Congenital Myotonic Dystrophy is not only associated with problems of the limb muscles but with the smooth
Bowel problems in Congenital Myotonic Dystrophy by Tim Kerr, Stephanie Robb & Graham Clayden. Congenital Myotonic Dystrophy is not only associated with problems of the limb muscles but with the smooth
Problems of the Digestive System
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
Constipation and Urologic Problems
 Child and Family Instructional Information Constipation and Urologic Problems In order to understand constipation, one must first understand normal bowel function. Stool is formed as a result of digestion
Child and Family Instructional Information Constipation and Urologic Problems In order to understand constipation, one must first understand normal bowel function. Stool is formed as a result of digestion
Care and Problems of the Digestive System. Chapter 18 Lesson 2
 Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
Care and Problems of the Digestive System Chapter 18 Lesson 2 Care of the Digestive System Good eating habits are the best way to avoid or minimize digestive system problems. Eat a variety of foods Avoid
Women s Continence and Pelvic Health Center
 Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
Care Manager Resources: Common Questions & Answers about Treatments for Depression
 Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
Care Manager Resources: Common Questions & Answers about Treatments for Depression Questions about Medications 1. How do antidepressants work? Antidepressants help restore the correct balance of certain
IBS. A patient s guide to living with irritable bowel syndrome. a program of the aga institute
 IBS A patient s guide to living with irritable bowel syndrome a program of the aga institute IBS Basics Irritable bowel syndrome (IBS) is a common disorder of the intestines with symptoms that include
IBS A patient s guide to living with irritable bowel syndrome a program of the aga institute IBS Basics Irritable bowel syndrome (IBS) is a common disorder of the intestines with symptoms that include
Night frequency None 1 2 3 4 5 6 7 8 9 10. Not enough warning before needing to urinate. none mild moderate severe
 {Patient Label} SYMPTOMS SURVEY: FREQUENCY: How many times do you urinate during the day and get up from sleep to urinate at night? Day frequency 3 4 5 6 7 8 9 10 11 12 13 14 15 More Night frequency None
{Patient Label} SYMPTOMS SURVEY: FREQUENCY: How many times do you urinate during the day and get up from sleep to urinate at night? Day frequency 3 4 5 6 7 8 9 10 11 12 13 14 15 More Night frequency None
Beating the Toilet Monster
 Beating the Toilet Monster Introduction I was toilet trained at 18months He is doing it to wind me up Two comments that many parents of special needs children have either heard or have said themselves.
Beating the Toilet Monster Introduction I was toilet trained at 18months He is doing it to wind me up Two comments that many parents of special needs children have either heard or have said themselves.
Symptoms of constipation are extremely common; the
 GASTROENTEROLOGY 2000;119:1761 1778 AMERICAN GASTROENTEROLOGICAL ASSOCIATION American Gastroenterological Association Medical Position Statement: Guidelines on Constipation This document presents the official
GASTROENTEROLOGY 2000;119:1761 1778 AMERICAN GASTROENTEROLOGICAL ASSOCIATION American Gastroenterological Association Medical Position Statement: Guidelines on Constipation This document presents the official
Abdominal Wall Pain. What is Abdominal Wall Pain?
 Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Normal Gastrointestinal Motility and Function
 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily to describe the contraction of the muscles in the gastrointestinal tract. Because the
Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily to describe the contraction of the muscles in the gastrointestinal tract. Because the
Urinary Incontinence. Causes of Incontinence. What s Happening?
 National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
National Institute on Aging AgePage Urinary Incontinence Sarah loves to spend time with her friends talking about her grandchildren and going to exercise classes with neighbors. But she s started to have
How to Improve Bladder After Bowler Cancer
 Bladder changes after bowel cancer treatment This information is from the booklet Managing the late effects of bowel cancer treatment. You may find the full booklet helpful. We can send you a free copy
Bladder changes after bowel cancer treatment This information is from the booklet Managing the late effects of bowel cancer treatment. You may find the full booklet helpful. We can send you a free copy
Spina Bifida Occulta. Lo-Call 1890 20 22 60. Occulta Means Hidden
 Occulta Means Hidden Spina Bifida Occulta is not easily detected because skin covers the area, such as the spinal cord, spinal bone or nerve roots, which may be affected. Spina Bifida Occulta can affect
Occulta Means Hidden Spina Bifida Occulta is not easily detected because skin covers the area, such as the spinal cord, spinal bone or nerve roots, which may be affected. Spina Bifida Occulta can affect
es of Urinary Incontinence:
 Reversible Cause Urinary incontinence is a loss of control over the passing of urine. Urine loss can occur in very small amounts (enough only to dampen underwear) to very large amounts (requiring a change
Reversible Cause Urinary incontinence is a loss of control over the passing of urine. Urine loss can occur in very small amounts (enough only to dampen underwear) to very large amounts (requiring a change
Basics on Bladder and Bowel
 Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Basics on Bladder and Bowel A quick journey through some of our recent new insights on the nervous system, the lower urinary tract and gastrointestinal tract Basics on Bladder and Bowel Basics on bladder
Irritable Bowel Syndrome
 Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health and
Irritable Bowel Syndrome National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health and
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Urinary Incontinence. Patient Information Sheet
 Urinary Incontinence Patient Information Sheet What is urinary incontinence (UI)? UI happens when you are not able to control when you urinate and you wet yourself. How common is urinary incontinence?
Urinary Incontinence Patient Information Sheet What is urinary incontinence (UI)? UI happens when you are not able to control when you urinate and you wet yourself. How common is urinary incontinence?
Learning Objectives. Introduction to Medical Careers. Vocabulary: Chapter 16 FACTS. Functions. Organs. Digestive System Chapter 16
 Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
THE ANSWERS SERIES ENCOPRESIS
 COMMUNITY PSYCHIATRIC CENTERS A Partnership of Dr. Robert A. Lowenstein, M.D. & John Carosso, Psy..D. THE ANSWERS SERIES ENCOPRESIS Page 2 of 16 What is soiling (encopresis)? A child with encopresis passes
COMMUNITY PSYCHIATRIC CENTERS A Partnership of Dr. Robert A. Lowenstein, M.D. & John Carosso, Psy..D. THE ANSWERS SERIES ENCOPRESIS Page 2 of 16 What is soiling (encopresis)? A child with encopresis passes
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Why are antidepressants used to treat IBS? Some medicines can have more than one action (benefit) in treating medical problems.
 The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD What are functional GI disorders? There are more
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD What are functional GI disorders? There are more
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Colon Polyps. What I need to know about. National Digestive Diseases Information Clearinghouse NATIONAL INSTITUTES OF HEALTH
 What I need to know about Colon Polyps U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse What I need to know about Colon
What I need to know about Colon Polyps U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse What I need to know about Colon
Probiotics for the Treatment of Adult Gastrointestinal Disorders
 Probiotics for the Treatment of Adult Gastrointestinal Disorders Darren M. Brenner, M.D. Division of Gastroenterology Northwestern University, Feinberg School of Medicine Chicago, Illinois What are Probiotics?
Probiotics for the Treatment of Adult Gastrointestinal Disorders Darren M. Brenner, M.D. Division of Gastroenterology Northwestern University, Feinberg School of Medicine Chicago, Illinois What are Probiotics?
Constipation in Adults
 Information about Constipation in Adults What are the commonest causes? What are the unusual causes? Constipation in Adults Will I need to have tests? What does constipation mean? What research is needed?
Information about Constipation in Adults What are the commonest causes? What are the unusual causes? Constipation in Adults Will I need to have tests? What does constipation mean? What research is needed?
COLORECTAL CANCER SCREENING
 COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
