USING NEUROPSYCHOLOGY TO ASSESS TBI
|
|
|
- Shanon Gilbert
- 8 years ago
- Views:
Transcription
1 2015 Trial Lawyers Summit Brain & Traumatic Brain Injury January 20, 2015 USING NEUROPSYCHOLOGY TO ASSESS TBI Kenneth C. Kutner, PhD, ABPP-CN Fellow, National Academy of Neuropsychology Board Certified Neuropsychologist Professional Sports Concussion Care Miami Princeton 80 SW 8th Street 5 Independence Way Miami, FL Princeton, NJ Tel: Tel: DrKutner@proconcussioncare.com
2 USING NEUROPSYCHOLOGY TO ASSESS TBI 2015 Trial Lawyers Summit 1/20/15 Using Neuropsychology to Assess Traumatic Brain Injury (TBI) Abstract Kenneth C. Kutner, PhD, ABPP-CN 1,2 Neuropsychological Assessment provides important evidence for personal injury litigation. In cases of mild traumatic brain injury, Neuropsychological Assessment can reveal brain dysfunction when structural abnormalities cannot be seen on CT or MRI scans. This paper will briefly review neurodiagnostic methods and then focus on the role that Neuropsychological Evaluations play in assessing traumatic brain injury and establishing whether permanent sequelae have developed. Introduction According to the Center for Disease Control (CDC), over 2.5 million traumatic brain injuries occur each year (Faui et al 2010). Diagnostic tools utilized in assessing brain injury include Neuroimaging (CT & MRI), Neurophysiological Tests (EEG & QEEG), Neuropsychological Assessment, as well as experimental methods. These diagnostic methods will be briefly reviewed followed by a more detailed discussion of Neuropsychological Testing. This discussion will focus on the role of Neuropsychological Evaluation in determining whether permanent cognitive impairment has developed and if the resulting deficits will preclude or limit the individual returning to his or her occupation or school/college. Neuroimaging (CT & MRI) Neuroimaging is a well-established method for assessing brain trauma. The introduction of Computerized Tomography (CT) resulted in direct examination of the brain, protective brain coverings (meninges), and brain spaces (ventricles). CT scans provide accurate assessment of brain contusions, hemorrhages, increased cranial pressure, and hydrocephalus. CT scans are utilized to help determine whether effects of a brain injury require neurosurgical intervention (i.e. large subdural hematoma) or indicate conservative treatment (non-surgical). In addition, CT scans also provide accurate assessment of skull fractures and acute hemorrhaging. 1 Department of Neurological Surgery, Weill Cornell Medical College 2 Professional Sports Concussion Care, Miami, FL 2
3 Magnetic Resonance Imaging (MRI) was developed after the introduction of CT scans. MRI scans can detect small or subtle lesions, not discernable by CT scans. Advantages of MRI also include higher detail of brain structures, especially the back of the brain (posterior fossa). Recently, Diffusion Tensor Imaging (DTI) has been introduced, which provides more accurate assessment of damage to white matter in the brain. Functional MRI (fmri) provides mapping of physiology, which helps neuroscientists localize brain functions to specific areas (i.e. speech-left frontal cortex). However, fmri requires further research before it is ready for clinical diagnosis of traumatic brain injury (Edlow & Wu 2012). Other neuroimaging techniques such as Positron Emission Tomography (PET) and Magnetic Resonance Spectroscopy (MRS) are utilized in research, but have not been deemed ready for clinical use (Dimou & Lagopouos 2014). Single Photon Emission Computerized Tomography (SPECT) results have been admitted as evidence in a few states, including Florida (Hammer v. Sentinel Insurance Company). Electrophysiological (EEG & QEEG) Electroencephalograms (EEGs) have a well-established role in the assessment of post-traumatic seizures and epilepsy. However, EEGs are typically noncontributory in determining whether a head injury has occurred. Even in the 10 percent of cases in which EEG is positive following brain trauma, it is only sensitive for the initial 48 hours after injury (Arciniegas 2004). Researchers have been attempting to utilize Quantified Electroencephalograms (QEEGs) in assessment of head trauma for some time. The methodology of these initial studies had significant problems, including not controlling for medication and psychiatric history. With published studies of QEEG being poorly designed, the American Academy of Neurology (AAN) dictated that QEEG remained investigational and should not be utilized in civil or criminal judicial proceedings (Nuwer 1997). However, recent research with improved methodology has been undertaken. Studies measuring electrophysiological recovery after sports-related head injury have shown potential efficacy of QEEG (Prichep et al 2013; Barr et al 2012). In November of 2014, The FDA cleared the approval of a QEEG device (BrainScope Ahead System) as an adjunct to standard clinical practice for patients who sustain a closed head injury within the past 24 hours, present with a mild traumatic brain injury, and are between the ages of Blood Studies (Serum) With the high prevalence of brain trauma sustained in combat-blast injuries, considerable research has been conducted to determine if blood tests can be utilized to determine whether or not a concussion occurred. Neuroscientists have been looking for a protein or protein breakdown marker, which can be utilized for diagnosis of a mild traumatic brain injury. Multiple blood factors including Neuron Specific Enolase (NSE), SB100, and Glial Fibrillary Acidic Protein (GFA) have been 3
4 researched. Isolated studies have found elevations in select blood factors. However, the results to date have not been replicated. At this time, blood studies are not being utilized to clinically diagnose brain damage (Mondello et al 2011). It is likely that a panel of blood markers will be required in order to determine if an injury has taken place. Optic Tracking Optic tracking is another recently developed approach in evaluating traumatic brain injury. This method assesses response time in reacting to specific sensory information (Maruta & Ghajar 2014). While studies have shown optic tracking to be sensitive to concussion, findings are not specific to head injury. Optic tracking does not appear to differentiate head trauma from individuals who have pain or dehydration. Neuropsychological Assessment Neuropsychological Testing is one of the core diagnostic tools utilized to diagnose and quantify effects of brain injury. It has been well established that traumatic brain injury results in cognitive impairment. Research has revealed that brain trauma frequently results in impairment with concentration, processing speed, reasoning, language, memory, and visual-spatial skills. While neuroimaging and EEG studies are quite helpful, they do not measure cognitive functioning. Direct assessment of cognitive functions is required to determine if deficits with attention, memory, and other domains have developed. Neuropsychological Testing will be detailed in the next section. NEUROPSYCHOLOGICAL ASSESSMENT Neuropsychological Assessment provides objective and scientifically-based examination of brain functioning. Specifically, this method assesses cognitive functioning. Neuropsychological Testing can determine whether neurocognitive impairment has occurred and if such impairment is permanent. Currently, Neuropsychological Assessment is utilized in the NFL and NHL, as well as at major teaching medical hospitals. For a clinical method to be scientifically supported and for test results to be deemed admissible, it must be both reliable and valid. In addition, as impaired test scores can result from suboptimal effort, response-bias procedures should be utilized in order to determine whether findings are due to brain damage (neurogenic) or psychological (psychogenic) etiology. These topics will be discussed in the following section. Neuropsychological Evaluation Neuropsychological Evaluation consists of administration of a battery of tests, which measure cognitive domains subserved by the brain. While neuroimaging can reveal brain structure, CT Scans and MRI s cannot measure cognition. The best window 4
5 into the brain for assessing cognitive functioning is by direct measurement through Neuropsychological Evaluation. Neuropsychological Tests are administered, which measure cognitive domains subserved by the brain including: attention/concentration, speed of information processing, psychomotor speed, reasoning, language, working memory, memory, and visual-spatial skills. In cases of moderate and severe traumatic brain injury, measurement of academic skills may be performed. Tests are administered in a 1:1 setting. Computerized Neuropsychological Testing with baseline and post-injury is utilized with sportsrelated concussions. However, this approach is only a screening device and does not have the accuracy of a full Neuropsychological Evaluation. Neuropsychological Evaluations include a detailed educational, vocational, and medical history in order to interpret test results. In addition, a neurobehavioral status examination is administered in order to assess for anxiety, depression, and brain injury induced personality changes. Reliability & Validity Tests need to be both reliable and valid. Reliability is necessary, but not sufficient for establishment of validity. Reliability is the consistency of measurement, meaning that repeated administrations of a test need to result in consistent findings. Reliability indicators are frequently characterized as Marginal ( ), Adequate ( ), High ( ), and Very High ( ). It is evident that a test can be reliable with repeated administrations resulting in consistent scores, but that the test is not valid. Validity reflects how well a test examines what it is supposed to be measuring. In Neuropsychological Testing, it means that the test actually measures cognitive functioning. Validity is measured in multiple ways including: Contentrelated, Construct-related, Criterion-related, and Response Processes. (Lezak 2004). Interpretation Pre-injury neuropsychological test results are rarely available for comparison. Similarly, premorbid medical lab findings are typically not available for comparison. For example, few individuals present to the hospital or their physician with a preillness white blood cell count or blood glucose level. Determination of illness is made by comparing the patient s current test results to reference ranges (results from individuals of their age & gender). As in medicine, neurocognitive tests scores are compared to normative data from individuals of their age, gender, culture, and educational level. Interpretation utilizing normative data is critical as education and age are especially important factors. (Smith et al 2008, Hannary & Lezak 2004). Test results are interpreted as either falling within the normal or impaired range. If impaired, the level of impairment is next established. Impairment levels are: Mild, Mild-Moderate, Moderate, Moderate-Severe, and Severe. Research indicates that neurocognitive sequelae in traumatic brain injury are dose-responsive (Rohling et al 2003). In other words, individuals with a Mild Traumatic Brain Injury frequently develop Mild or Mild-Moderate cognitive impairment. However, they would not 5
6 develop severe cognitive impairment. Permanency is established when testing at > 1 year reveals impaired test scores. (Dikmen 1995, Pagulayan, et al 2006) Malingering/Symptom Magnification As there are movement artifacts in radiological studies, test results from Neuropsychological Assessment can contain artifacts. Studies suggest that assessment of motivation and effort is critical when conducting a Neuropsychological Evaluation (Boone 2007). Practice Standards (ACN 2007) in Clinical Neuropsychology indicate that effort measures should be administered in order to determine if test scores are due to brain impairment or psychological causes i.e. symptom enhancement (Bush et al 2005). The advantage of administering these procedures is that impaired test scores in individuals who pass these effort measures can be directly related to the traumatic brain injury. Neuropsychological Role by level of TBI The role Neuropsychological Assessment plays in TBI varies by the level of injury. Traumatic brain injury is classically divided into Mild, Moderate, and Severe levels (Ropper & Samuels 2009). Mild traumatic brain injury (concussion) is defined by a Glasgow Coma Score of 13 15, loss of consciousness (LOC) 0 30 min and Posttraumatic Amnesia of < 24 hrs. In the vast majority of these cases, abnormal findings do not appear on either CT or MRI. Here, Neuropsychological Assessment often provides the best determination that a brain injury has occurred. While defined as mild, many of these patients will be unable to return to their usual occupation, especially if it requires complex cognitive functioning. Moderate traumatic brain injury is defined by a Glasgow Coma Score of 9 12, loss of consciousness ranging from > 30 minutes to < 24 hours and Posttraumatic Amnesia persisting for > 24 hours to < 7 days. Positive findings (hemorrhage, hematoma, contusion) are often evident on neuroimaging. In these cases, Neuropsychologists can determine if neurocognitive impairment has developed and if it precludes the individual from returning to their prior occupation and at times, even any form of competitive employment. In many cases, hemorrhages are absorbed; contusions resolve with subsequent CT and/or MRI studies being unremarkable. Neuropsychological Assessment can establish if neurocognitive impairment persists despite resolution of findings on neuroimaging. Severe traumatic brain injury is defined by a Glasgow Coma Scale of 3 8, loss of consciousness of > 24 hours and Posttraumatic Amnesia of > 7 days. Individuals with this severe level of injury typically have a period of being comatose. In these cases, Neuropsychologists can determine if a patient s brain damage precludes them from any type of competitive employment and if they require 24-hour supervision. 6
7 Training As with any medical expert, Neuropsychologists should complete requisite education and training requirements. Ideally, the Neuropsychologist should complete doctoral training in Neuropsychology, taking courses in neuroanatomy, neurological bases of cognition, and neuropsychometric assessment. Two years of postdoctoral training (residency/fellowship) provides the level of experience required for competent practice. Board Certification by the American Board of Clinical Neuropsychology (ABCN) provides the best format to ensure that the Neuropsychologist has completed requisite courses, training, and acquired the level of experience required to practice at the highest level. Admissibility of Neuropsychological Experts Admissibility of neuropsychological expert testimony is typically governed by the particular rules of evidence on the qualifications needed for the doctor to provide expert testimony. Specifically, the witness should be qualified as an expert by knowledge, education, skills, experience, and training to form his or her opinion. Admissibility of a Neuropsychologist to testify as to the existence of a brain injury is accepted in most jurisdictions. However, the ability of the Neuropsychologist to provide expert testimony as to the cause of the brain injury and prognosis may be limited in a few states i.e. Florida (Jenkins v. United States). In such cases, it may be helpful to have the Neuropsychologist explain the anatomy of the brain, what happens to the brain when it is injured, and what deficits can be expected. After the Neuropsychologist explains impairment found on the testing, the jury can draw their own conclusion whether or not deficits found on cognitive testing were related to the traumatic brain injury (Stern). Summary Neuropsychological Assessment plays an important role in determining that permanent brain damage has resulted from a traumatic brain injury. In cases of mild traumatic brain injury, Neuropsychological Testing can reveal brain dysfunction when structural abnormalities cannot be identified on CT or MRI scans. In cases of moderate traumatic brain injury, Neuropsychological Testing can reveal brain dysfunction even when initial findings on CT and MRI scans resolve on repeat imaging. Research has revealed that Neuropsychological Tests are both reliable and valid. Test results from this clinical diagnostic tool can be utilized to determine if neurocognitive impairment from a brain injury precludes an individual from returning to their usual occupation or school/college and if they are unable to perform competitive employment. 7
8 References American Academy of Neuropsychology-Board Directors. Practice Guidelines for Neuropsychological Assessment and Consultation. The Clin Neuropsych, 2007, 21: Arciniegas D., Anderson, C., Rojas, D. Electrophysiological Techniques. In: Silver JM, McAllister TW, Yudofsky SC, editors. Textbook of traumatic brain injury. Washington. American Psychiatric Publ; Barr, W., Prichep, L., Chabot, R., Powell, M., & McCrea, M. Brain Injury. 2012, vol 26. Boone, K. Assessment of Feigned Cognitive Impairment. Guilford Press, Bush, S., Ruff, R., Troster, A., Barth, J., Koffler, S., Pliskin, N., Reynold, C. & Silver, C NAN Position Paper: Symptom validity assessment: Practice issues and medical necessity. Arch of Clin Neuropsych 2005, 20: Edlow, B. & Wu, O. Advanced Neuroimaging in Traumatic Brain Injury. Seminars in Neurology. 2012: 32(4), Dikmen, S., Machamer, J., Winn, H. & Temkin, N. Neuropsychological Outcome at 1- year post head injury. Neuropsychology, 1995, 9, Dimou, S., & Lagopoulos, J. Toward Objective Markers of Concussion in Sport: A Review of White Matter and Neurometabolic Changes in the Brain after Sports- Related Concussion. J of Neurotrauma, 2014, 31: Faui, M, Xu L, Wald, M, Coronado, VG. Traumatic brain injury in the United States: emergency department visits, hospitalizations, and deaths. Atlanta (GA): Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; Hannay, J. & Lezak, M. The Neuropsychological Examination: Interpretation In: Lezak, M., Howieson, D., & Loring, D. Neuropsychological Assessment, 4 th Ed. Oxford Maruta, J. & Ghajar, J. Detecting eye movement abnormalities from concussion. Prog Neurol Surg. 2014, 28: Montello, S., Muller, U., Jeromin, A., Streeter, J., Hayes, R., & Wang, K. Expert Rev Mol Diag. 2011; 11(1) Nuwer, M. Assessment of digital EEG, quantitative EEG and EEG brain mapping: Report of the American Academy of Neurology and the American Clinical Neurophysiology Society. Neurology, 1997; 49: ) 8
9 Pagulayan, K., Temkin, N., Machamer, J. & Dikmen, S. A longitudinal study of healthrelated quality of life after traumatic brain injury. Arch Phys Med Rehab: 2007, 87(5) Prichep, L., McCrea, M., Barr, W., Powell, M., & Chabot, R. Journal of Head Trauma Rehabilitation vol 28. Rohling, M., Meyers, J., & Millis S. Neuropsychological impairment following traumatic brain injury: a dose responsive analysis, The Clinical Neuropsychologist, 2003, 17(s): Ropper, A. & Samuels, M. Adams and Victor s Principles of Neurology, McGraw Hill, Smith, G., Ivnik, R., and Lucas, J. Assessment techniques: Tests, Test batteries, norms and methodological approaches In: Morgan, J. & Ricker, J. Textbook of Clinical Neuropsychology, Taylor & Francis, Stern, B. Admissibility of Neuropsychological Testimony. Stark & Stark (injury.starkstark.com/lawyer-attorney html). 9
V OCATIONAL E CONOMICS, I NC.
 V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm Volume 2,
V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm Volume 2,
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Brain Injury Litigation. Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com
 Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
CREATIVE DEMONSTRATIVE EVIDENCE: ADDING THE MIDAS TOUCH. We all know that the use of demonstrative evidence can be crucial to the jury s ability to
 CREATIVE DEMONSTRATIVE EVIDENCE: ADDING THE MIDAS TOUCH A. Introduction We all know that the use of demonstrative evidence can be crucial to the jury s ability to understand complex issues at trial. There
CREATIVE DEMONSTRATIVE EVIDENCE: ADDING THE MIDAS TOUCH A. Introduction We all know that the use of demonstrative evidence can be crucial to the jury s ability to understand complex issues at trial. There
1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136. Days and Hours: Monday Friday 8:30a.m. 6:00p.m. (305) 355 9028 (JMH, Downtown)
 UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY
 J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
USE OF DEMONSTRATIVE EVIDENCE IN THE TRIAL OF A MILD TRAUMATIC BRAIN INJURY CASE. Your client, who sustained a closed head injury in an
 USE OF DEMONSTRATIVE EVIDENCE IN THE TRIAL OF A MILD TRAUMATIC BRAIN INJURY CASE Your client, who sustained a closed head injury in an automobile crash one year ago, appears perfectly fine as his trial
USE OF DEMONSTRATIVE EVIDENCE IN THE TRIAL OF A MILD TRAUMATIC BRAIN INJURY CASE Your client, who sustained a closed head injury in an automobile crash one year ago, appears perfectly fine as his trial
The Indiana Trial Lawyer Association s Lifetime Achievement Seminar. Honoring Peter L. Obremsky. May 23-24, 2005
 The Indiana Trial Lawyer Association s Lifetime Achievement Seminar Honoring Peter L. Obremsky May 23-24, 2005 The Use of Medical Literature in the Brain Injury Case Thomas C. Doehrman Doehrman-Chamberlain
The Indiana Trial Lawyer Association s Lifetime Achievement Seminar Honoring Peter L. Obremsky May 23-24, 2005 The Use of Medical Literature in the Brain Injury Case Thomas C. Doehrman Doehrman-Chamberlain
Psychological and Neuropsychological Testing
 2015 Level of Care Guidelines Psych & Neuropsych Testing Psychological and Neuropsychological Testing Introduction: The Psychological and Neuropsychological Testing Guidelines provide objective and evidencebased
2015 Level of Care Guidelines Psych & Neuropsych Testing Psychological and Neuropsychological Testing Introduction: The Psychological and Neuropsychological Testing Guidelines provide objective and evidencebased
Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle
 Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
Practice Guideline. Neuropsychological Evaluations
 Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
Practice Guideline Neuropsychological Evaluations Adapted from the practice guideline of the same name by the Arizona Department of Health Services Division of Behavioral Health Services Effective: 06/30/2006
20 Questions (and answers) about Traumatic Brain Injury
 20 Questions (and answers) about Traumatic Brain Injury for insurance claims adjusters, case managers, attorneys, and health-care providers by Dennis P. Swiercinsky, Ph.D. 1. What is traumatic brain injury
20 Questions (and answers) about Traumatic Brain Injury for insurance claims adjusters, case managers, attorneys, and health-care providers by Dennis P. Swiercinsky, Ph.D. 1. What is traumatic brain injury
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
EYE-TRAC Advance. A research study funded by the Department of Defense
 EYE-TRAC Advance A research study funded by the Department of Defense BROCHURE CONTENTS About BTF..................................................... 1 Eye-Trac Advance Overview....................................1
EYE-TRAC Advance A research study funded by the Department of Defense BROCHURE CONTENTS About BTF..................................................... 1 Eye-Trac Advance Overview....................................1
Concussion Rates per Sport
 PSE4U UNIT 1: SPORTS-RELATED HEAD INJURIES DUE DATE: LATE PENALTY (-5% PER WEEK): K/U T/I C A FINAL MARK 10 10 10 32 62 PART A: BRAINSTORMING [T/I /10] [C /10] 1.) Construct a mind-map: research the amount
PSE4U UNIT 1: SPORTS-RELATED HEAD INJURIES DUE DATE: LATE PENALTY (-5% PER WEEK): K/U T/I C A FINAL MARK 10 10 10 32 62 PART A: BRAINSTORMING [T/I /10] [C /10] 1.) Construct a mind-map: research the amount
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi.
 Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
Cognitive Rehabilitation of Blast Traumatic Brain Injury
 Cognitive Rehabilitation of Blast Traumatic Brain Injury Yelena Bogdanova, PhD VA Boston Healthcare System Rehabilitation Research & Development Boston University School of Medicine IOM Committee on Cognitive
Cognitive Rehabilitation of Blast Traumatic Brain Injury Yelena Bogdanova, PhD VA Boston Healthcare System Rehabilitation Research & Development Boston University School of Medicine IOM Committee on Cognitive
Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle
 Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
PE finding: Left side extremities mild weakness No traumatic wound No bloody otorrhea, nor rhinorrhea
 Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Case report A 82-year-old man was suffered from sudden onset spasm of extremities then he fell down to the ground with loss of consciousness. He recovered his consciousness 7-8 mins later but his conscious
Sequence of Evidence and Witnesses in a Traumatic Brain Injury Case
 Sequence of Evidence and Witnesses in a Traumatic Brain Injury Case Sequence of Evidence and Witnesses in a Traumatic Brain Injury Case Who's on First? Princeton, New Jersey Trial Diplomacy Journal, Vol.
Sequence of Evidence and Witnesses in a Traumatic Brain Injury Case Sequence of Evidence and Witnesses in a Traumatic Brain Injury Case Who's on First? Princeton, New Jersey Trial Diplomacy Journal, Vol.
Psychological and Neuropsychological Testing
 Psychological and Neuropsychological Testing I. Policy University Health Alliance (UHA) will reimburse for Psychological and Neuropsychological Testing (PT/NPT) when it is determined to be medically necessary
Psychological and Neuropsychological Testing I. Policy University Health Alliance (UHA) will reimburse for Psychological and Neuropsychological Testing (PT/NPT) when it is determined to be medically necessary
TCHP Behavioral Health Psychological/Neuropsychological Testing Child/Adolescent Guidelines
 TCHP Behavioral Health Psychological/Neuropsychological Testing Child/Adolescent Guidelines Psychological testing involves the culturally and linguistically competent administration and interpretation
TCHP Behavioral Health Psychological/Neuropsychological Testing Child/Adolescent Guidelines Psychological testing involves the culturally and linguistically competent administration and interpretation
Sports Neuropsychology: Definition, Qualifications, and Training Guidelines
 Sports Neuropsychology: Definition, Qualifications, and Training Guidelines An Official Position of the Sports Neuropsychology Society Preamble Clinical neuropsychology has a long history, and clinical
Sports Neuropsychology: Definition, Qualifications, and Training Guidelines An Official Position of the Sports Neuropsychology Society Preamble Clinical neuropsychology has a long history, and clinical
Traumatic brain injury (TBI), caused either by blunt force or acceleration/
 Traumatic Brain Injury (TBI) Carol A. Waldmann, MD Traumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons
Traumatic Brain Injury (TBI) Carol A. Waldmann, MD Traumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons
HANDLING NON-CATASTROPHIC BRAIN INJURY CASES
 HANDLING NON-CATASTROPHIC BRAIN INJURY CASES WE VE LEARNED THAT THE BRAIN IS MORE PLASTIC THAN WE ONCE THOUGHT AND THAT DAMAGE CAN COM FROM ITS MOVEMENT WITHIN THE SKULL AFTER A BLOW TO THE HEAD OR TO
HANDLING NON-CATASTROPHIC BRAIN INJURY CASES WE VE LEARNED THAT THE BRAIN IS MORE PLASTIC THAN WE ONCE THOUGHT AND THAT DAMAGE CAN COM FROM ITS MOVEMENT WITHIN THE SKULL AFTER A BLOW TO THE HEAD OR TO
Early Response Concussion Recovery
 Early Response Concussion Recovery KRISTA MAILEY, BSW RSW, CONCUSSION RECOVERY CONSULTANT CAREY MINTZ, PH.D., C. PSYCH., PRACTICE IN CLINICAL NEUROPSYCHOLOGY FOR REFERRAL: Contact Krista Mailey at (204)
Early Response Concussion Recovery KRISTA MAILEY, BSW RSW, CONCUSSION RECOVERY CONSULTANT CAREY MINTZ, PH.D., C. PSYCH., PRACTICE IN CLINICAL NEUROPSYCHOLOGY FOR REFERRAL: Contact Krista Mailey at (204)
A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1
 A PEEK INSIDE A CLOSED HEAD INJURY CLAIM By: Douglas Fletcher Fernando Fred Arias Dr. Jim Hom April 11, 2014 CONTENTS A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1 SYMPTOMATOLOGY... 2 CRITICAL INFORMATION...
A PEEK INSIDE A CLOSED HEAD INJURY CLAIM By: Douglas Fletcher Fernando Fred Arias Dr. Jim Hom April 11, 2014 CONTENTS A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1 SYMPTOMATOLOGY... 2 CRITICAL INFORMATION...
Behavioral Health Psychological/Neuropsychological Testing Guidelines
 Behavioral Health Psychological/Neuropsychological Testing Guidelines Psychological testing (procedural code 96101) and Neuropsychological Testing (procedural code 96118) involve the culturally and linguistically
Behavioral Health Psychological/Neuropsychological Testing Guidelines Psychological testing (procedural code 96101) and Neuropsychological Testing (procedural code 96118) involve the culturally and linguistically
brain injury take care of yourself. we ll take care of the rest.
 take care of yourself. we ll take care of the rest. common injuries While injuries to the head do not always result in damage to the brain, it s important to note the most common forms of head trauma that
take care of yourself. we ll take care of the rest. common injuries While injuries to the head do not always result in damage to the brain, it s important to note the most common forms of head trauma that
Clinical Policy: Neuroimaging and Decisionmaking in Adult Mild Traumatic Brain Injury in the Acute Setting
 TRAUMA/CLINICAL POLICY : Neuroimaging and Decisionmaking in Adult Mild Traumatic Brain Injury in the Acute Setting From the American College of Emergency Physicians (ACEP)/Centers for Disease Control and
TRAUMA/CLINICAL POLICY : Neuroimaging and Decisionmaking in Adult Mild Traumatic Brain Injury in the Acute Setting From the American College of Emergency Physicians (ACEP)/Centers for Disease Control and
Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI
 Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI Reviewer Emma Scheib Date Report Completed November 2011 Important Note: This report is not intended to replace clinical judgement,
Pragmatic Evidence Based Review Substance Abuse in moderate to severe TBI Reviewer Emma Scheib Date Report Completed November 2011 Important Note: This report is not intended to replace clinical judgement,
Attention & Memory Deficits in TBI Patients. An Overview
 Attention & Memory Deficits in TBI Patients An Overview References Chan, R., et.al.. (2003). Are there sub-types of attentional deficits in patients with persisting post- concussive symptoms? A cluster
Attention & Memory Deficits in TBI Patients An Overview References Chan, R., et.al.. (2003). Are there sub-types of attentional deficits in patients with persisting post- concussive symptoms? A cluster
Concussion Management Program for Red Bank Catholic High School Athletic Department
 Concussion Management Program for Red Bank Catholic High School Athletic Department *This document should be used as a framework for a successful concussion management program but is not intended to replace
Concussion Management Program for Red Bank Catholic High School Athletic Department *This document should be used as a framework for a successful concussion management program but is not intended to replace
A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee
 A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee The following is a guideline for parents to use when choosing a sports
A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee The following is a guideline for parents to use when choosing a sports
Top 10 Things a Workers Compensation Care Manager needs to know about Brain Injury
 Top 10 Things a Workers Compensation Care Manager needs to know about Brain Injury Dixie Eastridge, MA, BCBA, CBIS Clinical Director/Behavior Analyst Learning Services Neurobehavioral Institute-West Original
Top 10 Things a Workers Compensation Care Manager needs to know about Brain Injury Dixie Eastridge, MA, BCBA, CBIS Clinical Director/Behavior Analyst Learning Services Neurobehavioral Institute-West Original
What is Neuropsychology and What s the (Power)Point?
 What is Neuropsychology and What s the (Power)Point? Geoffrey Kanter, Ph.D., ABN, ABPdN Board-Certified, American Board of Professional Neuropsychology Board-Certified, American Board of Pediatric Neuropsychology
What is Neuropsychology and What s the (Power)Point? Geoffrey Kanter, Ph.D., ABN, ABPdN Board-Certified, American Board of Professional Neuropsychology Board-Certified, American Board of Pediatric Neuropsychology
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve
 Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve University The opinions or assertions contained herein are
Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve University The opinions or assertions contained herein are
Neuropsychological assessment of children and adults with traumatic brain injury
 Neuropsychological assessment of children and adults with traumatic brain injury Guidelines for the NSW Compulsory Third Party Scheme and Lifetime Care and Support Scheme 2013 Motor Accidents Authority
Neuropsychological assessment of children and adults with traumatic brain injury Guidelines for the NSW Compulsory Third Party Scheme and Lifetime Care and Support Scheme 2013 Motor Accidents Authority
SPORTS CONCUSSION INSTITUTE Excellence in Concussion Management Centinela Freeman Regional Medical Center, Marina Campus
 SPORTS CONCUSSION INSTITUTE Excellence in Concussion Management Centinela Freeman Regional Medical Center, Marina Campus An estimated ten percent of all athletes participating in contact sports suffer
SPORTS CONCUSSION INSTITUTE Excellence in Concussion Management Centinela Freeman Regional Medical Center, Marina Campus An estimated ten percent of all athletes participating in contact sports suffer
The Role of Neuropsychological Testing in Guiding Decision- Making Related to Dementia
 The Role of Neuropsychological Testing in Guiding Decision- Making Related to Dementia By Scott Knight, Director, SLR Diagnostics & Assessments, a division of Sibley & Associates Inc., and Konstantine
The Role of Neuropsychological Testing in Guiding Decision- Making Related to Dementia By Scott Knight, Director, SLR Diagnostics & Assessments, a division of Sibley & Associates Inc., and Konstantine
Brain Injury Litigation Today
 MILD TRAUMATIC BRAIN INJURY PAPER 3.1 Brain Injury Litigation Today These materials were prepared by Joseph E. Murphy, QC, of Murphy Battista LLP, Vancouver, BC, for the Continuing Legal Education Society
MILD TRAUMATIC BRAIN INJURY PAPER 3.1 Brain Injury Litigation Today These materials were prepared by Joseph E. Murphy, QC, of Murphy Battista LLP, Vancouver, BC, for the Continuing Legal Education Society
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion
 NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
CLINICAL NEUROPSYCHOLOGY Course Syllabus, Summer 2010
 CLINICAL NEUROPSYCHOLOGY Course Syllabus, Summer 2010 Instructor: E mett McCaskill, PhD Office: 415-O Milbank Hall, Barnard College Email: emccaski@barnard.edu Phone: 212-85408601 Course Description This
CLINICAL NEUROPSYCHOLOGY Course Syllabus, Summer 2010 Instructor: E mett McCaskill, PhD Office: 415-O Milbank Hall, Barnard College Email: emccaski@barnard.edu Phone: 212-85408601 Course Description This
Memory Development and Frontal Lobe Insult
 University Press Scholarship Online You are looking at 1-10 of 11 items for: keywords : traumatic brain injury Memory Development and Frontal Lobe Insult Gerri Hanten and Harvey S. Levin in Origins and
University Press Scholarship Online You are looking at 1-10 of 11 items for: keywords : traumatic brain injury Memory Development and Frontal Lobe Insult Gerri Hanten and Harvey S. Levin in Origins and
NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases
 NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases Carl F. Mariano Barry H. Uhrman Introduction to Neuropsychology As many of you are aware, clinical
NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases Carl F. Mariano Barry H. Uhrman Introduction to Neuropsychology As many of you are aware, clinical
Clinical Medical Policy Cognitive Rehabilitation
 Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Covered Benefit for
Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Covered Benefit for
Curriculum Vitae. Psychology Atlanta, GA Psy.D., 2011 Concentration: Clinical Neuropsychology
 Curriculum Vitae Education: September, 2006-November, 2011 September, 2006-August, 2008 September, 2001-May, 2005 Georgia School of Professional Psychology Atlanta, GA Psy.D., 2011 Concentration: Clinical
Curriculum Vitae Education: September, 2006-November, 2011 September, 2006-August, 2008 September, 2001-May, 2005 Georgia School of Professional Psychology Atlanta, GA Psy.D., 2011 Concentration: Clinical
Introduction to Neuropsychological Assessment
 Definitions and Learning Objectives Introduction to Neuropsychological Assessment Alan Sunderland Reader in Clinical Neuropsychology Neuropsychological assessment seeks to define cognitive disability in
Definitions and Learning Objectives Introduction to Neuropsychological Assessment Alan Sunderland Reader in Clinical Neuropsychology Neuropsychological assessment seeks to define cognitive disability in
Practice Protocol. Neuropsychological Evaluations
 Practice Protocol Neuropsychological Evaluations Jointly Developed by the Arizona Department of Health Services/Division of Behavioral Health Services and AHCCCS/Health Plans Effective June 30, 2006 Revised
Practice Protocol Neuropsychological Evaluations Jointly Developed by the Arizona Department of Health Services/Division of Behavioral Health Services and AHCCCS/Health Plans Effective June 30, 2006 Revised
Types of Brain Injury
 Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Types of Brain Injury The bones of your skull are hard and they protect your brain. Your brain is soft, like firm Jell-O. When your head moves, your brain moves inside your skull. When your head is hit
Traumatic Brain Injury for VR Counselors Margaret A. Struchen, Ph.D. and Laura M. Ritter, Ph.D., M.P.H.
 Training Session 1c: Understanding Recovery Courses and Outcomes after TBI What is the typical recovery course after a mild or moderate/severe TBI? What are the effects of personal and environmental factors,
Training Session 1c: Understanding Recovery Courses and Outcomes after TBI What is the typical recovery course after a mild or moderate/severe TBI? What are the effects of personal and environmental factors,
Clinical Medical Policy Cognitive Rehabilitation
 Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Cognitive rehabilitation
Benefit Coverage Outpatient cognitive rehabilitation is considered to be the most appropriate setting for members who have sustained a traumatic brain injury or an acute brain insult. Cognitive rehabilitation
Cognitive Neuroscience. Questions. Multiple Methods. Electrophysiology. Multiple Methods. Approaches to Thinking about the Mind
 Cognitive Neuroscience Approaches to Thinking about the Mind Cognitive Neuroscience Evolutionary Approach Sept 20-22, 2004 Interdisciplinary approach Rapidly changing How does the brain enable cognition?
Cognitive Neuroscience Approaches to Thinking about the Mind Cognitive Neuroscience Evolutionary Approach Sept 20-22, 2004 Interdisciplinary approach Rapidly changing How does the brain enable cognition?
Traumatic Brain Injury Lawsuit
 Traumatic Brain Injury Lawsuit D Legal Guide Simple Step-By-Step Guide to Your Brain & Traumatic Brain Injury (TBI) [Type text] Distributed By: www.downtownlalw.com A Simple Step-by-Step Guide to your
Traumatic Brain Injury Lawsuit D Legal Guide Simple Step-By-Step Guide to Your Brain & Traumatic Brain Injury (TBI) [Type text] Distributed By: www.downtownlalw.com A Simple Step-by-Step Guide to your
MYBRAINTEST. Computerized Concussion Testing
 MYBRAINTEST Computerized Concussion Testing Best Practices for Sports Teams and School Athletic Departments A Guide for Coaches, Athletic Trainers, Physicians, and Parents Table of Contents About This
MYBRAINTEST Computerized Concussion Testing Best Practices for Sports Teams and School Athletic Departments A Guide for Coaches, Athletic Trainers, Physicians, and Parents Table of Contents About This
Revised 10-4-10 Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes
 Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes If the Certified Athletic Trainer of Bethel Park School District has a concern that a student-athlete
Bethel Park s Sports Concussion and Closed Head Injury Protocol and Procedures for Student-Athletes If the Certified Athletic Trainer of Bethel Park School District has a concern that a student-athlete
CHILDREN S NEUROSCIENCE CENTER
 CHILDREN S NEUROSCIENCE CENTER W hen families come to Children s Memorial Hermann Hospital, they expect to find the technological advances and healing expertise of a university-affiliated, academic hospital.
CHILDREN S NEUROSCIENCE CENTER W hen families come to Children s Memorial Hermann Hospital, they expect to find the technological advances and healing expertise of a university-affiliated, academic hospital.
Traumatic Brain Injury: Separating the Wheat from the Chaff
 Traumatic Brain Injury: Separating the Wheat from the Chaff Les Kertay, Ph.D., ABPP American Academy of Disability Examining Physicians 27 th Annual ScienAfic Session & Business MeeAng San Antonio, Texas
Traumatic Brain Injury: Separating the Wheat from the Chaff Les Kertay, Ph.D., ABPP American Academy of Disability Examining Physicians 27 th Annual ScienAfic Session & Business MeeAng San Antonio, Texas
B U R T & D A V I E S PERSONAL INJURY LAWYERS
 TRANSPORT ACCIDENT LAW - TRAUMATIC BRAIN INJURY Traumatic Brain Injury ( TBI ) is a common injury in transport accidents. TBI s are probably the most commonly undiagnosed injuries in a hospital setting.
TRANSPORT ACCIDENT LAW - TRAUMATIC BRAIN INJURY Traumatic Brain Injury ( TBI ) is a common injury in transport accidents. TBI s are probably the most commonly undiagnosed injuries in a hospital setting.
Department of Defense INSTRUCTION. DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting
 Department of Defense INSTRUCTION NUMBER 6490.11 September 18, 2012 USD(P&R) SUBJECT: DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting References: See
Department of Defense INSTRUCTION NUMBER 6490.11 September 18, 2012 USD(P&R) SUBJECT: DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting References: See
Chemobrain. Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015
 Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
Chemobrain Halle C.F. Moore, MD The Cleveland Clinic October 3, 2015 Terminology Chemotherapy-associated cognitive dysfunction Post-chemotherapy cognitive impairment Cancer treatment-associated cognitive
MANUEL DAVID TOBIAS, Ph.D. 9255 Town Centre Dr. Suite 875 San Diego, California 92121 Phone 858-362-8779 Fax-858-455-5556
 MANUEL DAVID TOBIAS, Ph.D. 9255 Town Centre Dr. Suite 875 San Diego, California 92121 Phone 858-362-8779 Fax-858-455-5556 PROFESSIONAL EXPERIENCE Qualified Medical Examiner- State of California, Division
MANUEL DAVID TOBIAS, Ph.D. 9255 Town Centre Dr. Suite 875 San Diego, California 92121 Phone 858-362-8779 Fax-858-455-5556 PROFESSIONAL EXPERIENCE Qualified Medical Examiner- State of California, Division
Clinician Portal: Enabling a Continuity of Concussion Care
 Clinician Portal: Enabling a Continuity of Concussion Care www.concussionvitalsigns.com Clinician Portal: Enabling a Continuity of Concussion CARE The Clinician Portal advances sports concussion care by
Clinician Portal: Enabling a Continuity of Concussion Care www.concussionvitalsigns.com Clinician Portal: Enabling a Continuity of Concussion CARE The Clinician Portal advances sports concussion care by
BINSA Information on Mild Traumatic Brain Injury
 Mild traumatic brain injuries (MTBI) occur through sporting, car and workplace accidents. Mild brain injury is not easily diagnosed. This fact sheet explains how it may be recognised and assessed, and
Mild traumatic brain injuries (MTBI) occur through sporting, car and workplace accidents. Mild brain injury is not easily diagnosed. This fact sheet explains how it may be recognised and assessed, and
Recovering from a Mild Traumatic Brain Injury (MTBI)
 Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
A Step by Step Guide to Understanding and Managing Traumatic Brain Injury Cases for Attorneys and Risk Managers. Sam Goldstein, Ph.D.
 A Step by Step Guide to Understanding and Managing Traumatic Brain Injury Cases for Attorneys and Risk Managers Sam Goldstein, Ph.D. Neurology, Learning and Behavior Center 230 South 500 East, Suite 100
A Step by Step Guide to Understanding and Managing Traumatic Brain Injury Cases for Attorneys and Risk Managers Sam Goldstein, Ph.D. Neurology, Learning and Behavior Center 230 South 500 East, Suite 100
Mild head injury: How mild is it?
 Mild head injury: How mild is it? Carly Dutton; Gemma Foster & Stephen Spoors Sunderland and Gateshead Community Acquired Brain Injury Service (CABIS), Northumberland, Tyne and Wear NHS Foundation Trust
Mild head injury: How mild is it? Carly Dutton; Gemma Foster & Stephen Spoors Sunderland and Gateshead Community Acquired Brain Injury Service (CABIS), Northumberland, Tyne and Wear NHS Foundation Trust
Injury Law Center HEAD INJURY. Head injuries can be caused by car crashes, sports injuries, falls, workplace injuries and assaults.
 Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. Description
Injury Law Center Note: This information is provided to give you a basic understanding of the injury. It is not intended as medical advice. You should consult a qualified medical provider. Description
Mild Traumatic Brain Injury.
 Mild Traumatic Brain Injury. Review of the literature and A look at the WCB of BC data By WCB Evidence Based Practice Group Dr. Craig W. Martin, Senior Medical Advisor August 7, 2003 Compensation and Rehabilitation
Mild Traumatic Brain Injury. Review of the literature and A look at the WCB of BC data By WCB Evidence Based Practice Group Dr. Craig W. Martin, Senior Medical Advisor August 7, 2003 Compensation and Rehabilitation
Cycling-related Traumatic Brain Injury 2011
 Cycling-related Traumatic Brain Injury 2011 The Chinese University of Hong Kong Division of Neurosurgery, Department of Surgery Accident & Emergency Medicine Academic Unit Jockey Club School of Public
Cycling-related Traumatic Brain Injury 2011 The Chinese University of Hong Kong Division of Neurosurgery, Department of Surgery Accident & Emergency Medicine Academic Unit Jockey Club School of Public
PSYCHOLOGICAL AND NEUROPSYCHOLOGICAL TESTING
 Status Active Medical and Behavioral Health Policy Section: Behavioral Health Policy Number: X-45 Effective Date: 01/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members
Status Active Medical and Behavioral Health Policy Section: Behavioral Health Policy Number: X-45 Effective Date: 01/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members
What is a concussion? What are the symptoms of a concussion? What happens to the brain during a concussion?
 What is a concussion? The working definition used today for concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces (developed by the consensus
What is a concussion? The working definition used today for concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces (developed by the consensus
Compassionate Allowance Outreach Hearing on Brain Injuries. Social Security Administration. November 18, 2008. Statement of
 Compassionate Allowance Outreach Hearing on Brain Injuries Social Security Administration November 18, 2008 Statement of Jerome E. Herbers, Jr., M.D. Office of Healthcare Inspections Office of Inspector
Compassionate Allowance Outreach Hearing on Brain Injuries Social Security Administration November 18, 2008 Statement of Jerome E. Herbers, Jr., M.D. Office of Healthcare Inspections Office of Inspector
TESTING GUIDELINES PerformCare: HealthChoices. Guidelines for Psychological Testing
 TESTING GUIDELINES PerformCare: HealthChoices Guidelines for Psychological Testing Testing of personality characteristics, symptom levels, intellectual level or functional capacity is sometimes medically
TESTING GUIDELINES PerformCare: HealthChoices Guidelines for Psychological Testing Testing of personality characteristics, symptom levels, intellectual level or functional capacity is sometimes medically
HEAD INJURIES V S U H E A L T H C E N T E R V A L D O S T A S T A T E U N I V E R S I T Y F A L L 2 0 1 2
 HEAD INJURIES V S U H E A L T H C E N T E R V A L D O S T A S T A T E U N I V E R S I T Y F A L L 2 0 1 2 LET S TALK ABOUT BRAIN INJURIES! Traumatic head injury affects more than 1.7 million people in
HEAD INJURIES V S U H E A L T H C E N T E R V A L D O S T A S T A T E U N I V E R S I T Y F A L L 2 0 1 2 LET S TALK ABOUT BRAIN INJURIES! Traumatic head injury affects more than 1.7 million people in
Traumatic brain injury (TBI)
 Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
V OCATIONAL E CONOMICS, I NC.
 V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm DEFINING VOCATIONAL
V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm DEFINING VOCATIONAL
DEBUNKING THE TOP 10 MYTHS OF TRAUMATIC BRAIN INJURY: EFFECTIVE CROSS EXAMINATION OF THE DEFENSE NEUROPSYCHOLOGIST
 DEBUNKING THE TOP 10 MYTHS OF TRAUMATIC BRAIN INJURY: EFFECTIVE CROSS EXAMINATION OF THE DEFENSE NEUROPSYCHOLOGIST By Richard A. Ruohonen The following article was published in the Minnesota Association
DEBUNKING THE TOP 10 MYTHS OF TRAUMATIC BRAIN INJURY: EFFECTIVE CROSS EXAMINATION OF THE DEFENSE NEUROPSYCHOLOGIST By Richard A. Ruohonen The following article was published in the Minnesota Association
General Disclaimer (learned from Dr. Melhorn)
 Mild Traumatic Brain Injury: Postconcussion Syndrome, Persistent Posttraumatic Headache, etc. Robert J. Barth, Ph.D. Chattanooga, TN and Birmingham, AL General Disclaimer (learned from Dr. Melhorn) All
Mild Traumatic Brain Injury: Postconcussion Syndrome, Persistent Posttraumatic Headache, etc. Robert J. Barth, Ph.D. Chattanooga, TN and Birmingham, AL General Disclaimer (learned from Dr. Melhorn) All
COURSE APPROVAL GUIDELINES APS COLLEGE OF CLINICAL NEUROPSYCHOLOGISTS
 Page 1 COURSE APPROVAL GUIDELINES APS COLLEGE OF CLINICAL NEUROPSYCHOLOGISTS Updated October 2000 Page 2 1. General Introduction and Principles Clinical neuropsychology is a division of psychology concerned
Page 1 COURSE APPROVAL GUIDELINES APS COLLEGE OF CLINICAL NEUROPSYCHOLOGISTS Updated October 2000 Page 2 1. General Introduction and Principles Clinical neuropsychology is a division of psychology concerned
How To Know If You Can Get Better From A Brain Injury
 Assessment of the Brain Injured Client: Neuropsychological, Psychiatric and Adjustment Issues Ann Marie McLaughlin, Ph.D. Clinical Director, ReMed s Community Outpatient Services Objectives 1. Brief review
Assessment of the Brain Injured Client: Neuropsychological, Psychiatric and Adjustment Issues Ann Marie McLaughlin, Ph.D. Clinical Director, ReMed s Community Outpatient Services Objectives 1. Brief review
Attention, memory and learning and acquired brain injury. Vicki Anderson. Jamie M. Attention & learning: an information processing model
 Attention, memory and learning and acquired brain injury Vicki Anderson Jamie M. Childhood acquired amnesia Attention & learning: an information processing model MANAGEMENT Organising, problem solving
Attention, memory and learning and acquired brain injury Vicki Anderson Jamie M. Childhood acquired amnesia Attention & learning: an information processing model MANAGEMENT Organising, problem solving
Introduction to the DSM-IV and Psychological Testing
 Introduction to the DSM-IV and Psychological Testing Significance of Mental Illness In any given year, how many Americans will suffer with a diagnosable mental illness? How many will suffer with a serious
Introduction to the DSM-IV and Psychological Testing Significance of Mental Illness In any given year, how many Americans will suffer with a diagnosable mental illness? How many will suffer with a serious
The Clinical Evaluation of the Comatose Patient in the Emergency Department
 The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
The Clinical Evaluation of the Comatose Patient in the Emergency Department patients with altered mental status (AMS) and coma. treat patients who present to the Emergency Department with altered mental
How To Prevent Mild Traumatic Brain Injury In The United States
 Report to Congress on Mild Traumatic Brain Injury in the United States: Steps to Prevent a Serious Public Health Problem September 2003 The Report to Congress on Mild Traumatic Brain Injury in the United
Report to Congress on Mild Traumatic Brain Injury in the United States: Steps to Prevent a Serious Public Health Problem September 2003 The Report to Congress on Mild Traumatic Brain Injury in the United
FUNCTIONAL EEG ANALYZE IN AUTISM. Dr. Plamen Dimitrov
 FUNCTIONAL EEG ANALYZE IN AUTISM Dr. Plamen Dimitrov Preamble Autism or Autistic Spectrum Disorders (ASD) is a mental developmental disorder, manifested in the early childhood and is characterized by qualitative
FUNCTIONAL EEG ANALYZE IN AUTISM Dr. Plamen Dimitrov Preamble Autism or Autistic Spectrum Disorders (ASD) is a mental developmental disorder, manifested in the early childhood and is characterized by qualitative
Anoxic Brain Injury and Neural Damage: Three Case Reports
 Anoxic Brain Injury and Neural Damage: Three Case Reports Abstract Anoxic brain injury (ABI) is common and can occur in a wide variety of disorders. This neural injury is associated with significant and
Anoxic Brain Injury and Neural Damage: Three Case Reports Abstract Anoxic brain injury (ABI) is common and can occur in a wide variety of disorders. This neural injury is associated with significant and
Integrated Neuropsychological Assessment
 Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Magnetic Resonance Imaging
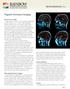 Magnetic Resonance Imaging What are the uses of MRI? To begin, not only are there a variety of scanning methodologies available, but there are also a variety of MRI methodologies available which provide
Magnetic Resonance Imaging What are the uses of MRI? To begin, not only are there a variety of scanning methodologies available, but there are also a variety of MRI methodologies available which provide
EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY
 Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
Michael J. Sileo, MD. Orthopedic Associates of Long Island (OALI)
 Michael J. Sileo, MD Orthopedic Associates of Long Island (OALI) ! Jeremy Thode, AD! Center Moriches BOE ! Safety of our student-athletes is our Number 1 concern! NYS is now forcing our hand " Referees
Michael J. Sileo, MD Orthopedic Associates of Long Island (OALI) ! Jeremy Thode, AD! Center Moriches BOE ! Safety of our student-athletes is our Number 1 concern! NYS is now forcing our hand " Referees
Traumatic Brain Injury (TBI) Examination Comprehensive Version
 Traumatic Brain Injury (TBI) Examination Comprehensive Version Name: Date of Exam: SSN: C-number: Place of Exam: Narrative: The potential residuals of traumatic brain injury necessitate a comprehensive
Traumatic Brain Injury (TBI) Examination Comprehensive Version Name: Date of Exam: SSN: C-number: Place of Exam: Narrative: The potential residuals of traumatic brain injury necessitate a comprehensive
CURRICULUM VITAE. Bachelor of Science in Physical Therapy, 1989. University of New England College of Osteopathic Medicine (UNECOM)
 Kristin Brousseau, D.O., PLLC Boulder Neuropsychiatry 2501 Walnut Street, Suite 201 Boulder, CO 80302 CURRICULUM VITAE Education: Undergraduate Boston University Bachelor of Science in Physical Therapy,
Kristin Brousseau, D.O., PLLC Boulder Neuropsychiatry 2501 Walnut Street, Suite 201 Boulder, CO 80302 CURRICULUM VITAE Education: Undergraduate Boston University Bachelor of Science in Physical Therapy,
New Onset Seizure Clinic
 New Onset Seizure Clinic Timely Care from the Region s Experts The New Onset Seizure Clinic at UH Rainbow Babies & Children s Hospital provides expert diagnostic services, referrals, treatment and follow-up
New Onset Seizure Clinic Timely Care from the Region s Experts The New Onset Seizure Clinic at UH Rainbow Babies & Children s Hospital provides expert diagnostic services, referrals, treatment and follow-up
Traumatic Brain Injury and Incarceration. Objectives. Traumatic Brain Injury. Which came first, the injury or the behavior?
 Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Thomas R. Wodushek, Ph.D., ABPP-CN
 Curriculum Vitae Personal contact information: 2450 Windrow Dr. #E-201 wodushek@hotmail.com Fort Collins, CO 80525 970-689-2152 Practice Location:, P.C. Fort Collins, CO 80524 BOARD CERTIFICATION IN CLINICAL
Curriculum Vitae Personal contact information: 2450 Windrow Dr. #E-201 wodushek@hotmail.com Fort Collins, CO 80525 970-689-2152 Practice Location:, P.C. Fort Collins, CO 80524 BOARD CERTIFICATION IN CLINICAL
Neuropsychological Testing
 Last Review Date: March 17, 2015 Number: MG.MM.ME.18dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: March 17, 2015 Number: MG.MM.ME.18dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
TBI Global Synapse Town Hall: Your TBI Information Connection
 Today s webinar is: TBI Global Synapse Town Hall: Your TBI Information Connection Nov. 20, 2013, 2:30-4 p.m. (EST) Moderator: Alison Cernich, Ph.D., ABPP Deputy Director Defense Centers of Excellence for
Today s webinar is: TBI Global Synapse Town Hall: Your TBI Information Connection Nov. 20, 2013, 2:30-4 p.m. (EST) Moderator: Alison Cernich, Ph.D., ABPP Deputy Director Defense Centers of Excellence for
