How To Maintain A Periodontal Or Periimplant
|
|
|
- Alexandrina Shaw
- 5 years ago
- Views:
Transcription
1 Continuing Education 1 Periodontal and Periimplant Maintenance: A Critical Factor in Long-Term Treatment Success Nicholas D. Shumaker, DDS, MS; 1 Brett T. Metcalf, DDS, MS; 2 Nicholas T. Toscano, DDS, MS; 3 and Dan J. Holtzclaw, DDS, MS 4 Abstract: Periodontal maintenance (PM) is a critical factor in the long-term success of both periodontal and dental implant therapy. Studies have shown both modern periodontal and dental implant therapies are effective in maintaining natural teeth and replacing lost teeth, respectively. However, without a regular program of clinical reevaluation, plaque control, oral hygiene instruction, and reassessment of biomechanical factors, the benefits of treatment often are lost and inflammatory disease in the form of recurrent periodontitis or periimplantitis may result. This article reviews the goals, types, and appropriate frequency of PM in periodontal and dental implant therapy, as well as the incidence and etiology of periimplant disease and strategies for management when recurrent disease develops during the maintenance phase of treatment. Learning Objectives After reading this article, the reader should be able to: comprehend the importance of periodontal maintenance for the long-term success of periodontal and dental implant care. use an evidence-based approach to assign the type of maintenance and an appropriate posttreatment maintenance interval to a clinical case. identify during maintenance the signs of recurrent periodontal or periimplant diseases, the appropriate therapy to deliver, and when/how to reevaluate results. The goal of periodontal therapy is the maintenance of the dentition and/or its implant replacements in a state of health, comfort, function, and esthetics for the duration of a patient s life. With the increasing number of patients receiving dental implants and the aging of existing dental implants in service, the prevalence of periimplant inflammatory problems presenting to clinical practices is rising. 1 As well-stated by Newman et al: The periodontal care of the public is primarily the concern of the general dentist, who cannot disregard his or her responsibility to examine, treat, or refer all periodontal problems. The high incidence of periodontal problems and the close relationship between periodontal and restorative dental therapies make this an 1 Department Head for Periodontics, Naval Health Clinic Quantico, Quantico, Virginia 2 Department Head for Periodontics, Naval Hospital Naples, Naples, Italy 3 Department Head for Periodontics, Washington Navy Yard, Washington, DC 4 Department Head for Periodontics, Naval Hospital, Pensacola, Florida 2 Compendium September 2009 Volume 30, Number 7
2 Nicholas D. Shumaker, DDS, MS Brett T. Metcalf, DDS, MS Nicholas T. Toscano, DDS, MS Dan J. Holtzclaw, DDS, MS incontrovertible point. 2 The maintenance phase of treatment most often is conducted in the general practice and, therefore, it is critical for general dentists to understand the importance of monitoring and maintaining not only periodontal health but also periimplant health. 3,4 A clear understanding of the signs of disease recurrence is crucial so that early and definitive action can be taken to prevent further clinical attachment and bone loss around teeth and/or implants, which might otherwise go unnoticed until advanced stages. This article provides a review of periodontal maintenance goals, procedures, and efficacy involving natural teeth and dental implants, as well as makes recommendations on when and how to address signs of recurrent disease activity during periodontal maintenance (PM). A GOALS OF PERIODONTAL AND PERIIMPLANT MAINTENANCE The primary etiology of periodontal and periimplant diseases is pathogenic bacterial plaque in a susceptible patient. Because patient susceptibility currently cannot be altered predictably, PM is aimed at minimizing bacterial plaque to limit the risk of further disease activity that causes continued periodontal and periimplant attachment and bone loss. This therapy usually is delivered at 3-month intervals, but the specific interval is tailored to each patient s presentation and needs. PM also allows for close monitoring of the patient so that if periodontal or periimplant disease recurrence or other oral health problems should occur, early intervention can be provided. B Figure 1 Long-term results of a case involving a 55-year-old woman treated by regenerative periodontal surgery followed by periodontal maintenance every 3 months for 8 years. (A) Radiograph taken in May 2000; and (B) radiograph of the same area taken in July Compendium 3
3 Continuing Education 1 A B Figure 2 (A) Clinical and (B) radiographic views of implants at site Nos. 30 and 31 demonstrating bone loss caused by periimplantitis after 8 years in function. Note gingival inflammation and plaque accumulation around implants. Table 1: Diagnostic Terminology Differences Natural Teeth and Dental Implants 16 Natural Teeth Dental Implants Soft-tissue inflammation (plaque-induced) Gingivitis Periimplant Mucositis without alveolar bone loss (plaque-associated) Soft-tissue inflammation with alveolar bone loss Periodontitis Periimplantitis The goals of PM are: 5 to minimize the recurrence and progression of periodontal diseases in patients who have been treated previously for gingivitis and periodontitis. to reduce the incidence of tooth loss by monitoring the dentition and any prosthetic replacements of the natural teeth (including dental implants). to increase the probability of locating and treating, in a timely manner, other diseases or conditions found within the oral cavity. MAINTENANCE AND PERIODONTITIS Periodontitis is a chronic inflammatory disease of natural teeth that requires lifelong management. Periodontitis presents in several forms, all of which involve loss of supporting bone and periodontal ligament. Long-term studies on the success of periodontal therapy demonstrate that a well-planned and executed periodontal treatment plan (including long-term maintenance) is effective in controlling disease progression and preserving the dentition in most patients. 6,7 After complete management of moderate to severe periodontitis, including scaling and root planing and in some cases periodontal surgery, subsequent regular periodontal maintenance is reported to prevent tooth loss in up to 85% of patients over a long-term follow-up interval of up to 53 years. 6,8 This high success rate of periodontal treatment is comparable to that of dental implants in replacing teeth lost to severe periodontal diseases, highlighting the predictability of maintaining the natural dentition in most patients with periodontal diseases 9,10 (Figure 1A and Figure 1B). It is critical to understand, however, that when periodontal treatment is delivered without a tightly controlled lifelong PM regimen, the benefits of therapy often are lost, allowing the recurrence of disease activity, further loss of periodontal tissues, and tooth mortality. 8,11 Long-term outcome studies on the delivery of periodontal treatment without any posttreatment PM have found that unmaintained patients lose two to three times the number of teeth and have a twofold increased risk for requiring re-treatment in the form of scaling and root planing or periodontal surgery. 8,12 This supports an evidence-based belief that periodontal treatment, in the form of surgical or nonsurgical modalities, is ineffective in the long term without an effective PM regimen. Furthermore, increased emphasis has been placed on the control of periodontal inflammation recently, with 4 Compendium September 2009 Volume 30, Number 7
4 Shumaker et al. the discovery of its role as a risk factor for several chronic systemic diseases. Long-term PM provides an opportunity to control systemic low-grade periodontally derived inflammation in a lifelong treatment model. 13 MAINTENANCE AND PERIIMPLANT DISEASE The success of endosseous dental implants has been attributed to their functional ankylosis or bone anchorage, termed osseointegration. 14 While dental implants are a highly successful treatment modality, they are susceptible to periodontal pathogens and a stimulated host inflammatory reaction, which may lead to periimplant soft-tissue inflammation and bone loss. 15 Inflammation limited to soft tissues around a dental implant may result from dental plaque colonization and is termed periimplant mucositis. This is a reversible inflammatory condition limited to the soft tissues around the implant (without any bone loss), analogous to gingivitis around natural teeth. A diagnosis of periimplantitis results when the inflammation spreads apically, causing progressive loss of osseointegrated supporting bone, analogous to periodontitis around natural teeth 16 (Figure 2A and Figure 2B). It is essential for practitioners to be familiar with these diagnostic terms when assessing the long-term success of implants and periimplant health (Table 1). It is also important that the etiology and chronology of bone loss around implants be identified. Periimplant bone loss resulting from surgical trauma or technique, such as pressure necrosis from inadequate osteotomy preparation or coronal bony voids from excessive countersinking, must be differentiated from periimplant bone loss resultant from bacterial plaque-mediated immunoinflammatory bone loss. Implants placed using a subcrestal platform position tend to have deeper baseline probing depths than those placed supracrestally; therefore, it is important to know the baseline probing depth after initial healing to allow monitoring for changes over time. The incidence and prevalence of periimplantitis has been reported in the literature. Berglundh et al 1 found the incidence of periimplantitis was up to 14.4% and appeared to be related to the number of years that the fixtures were in service. Additionally, Roos-Jansåker et al 17 reported that of implant cases not enrolled in a regular posttreatment PM program, 16% demonstrated periimplantitis by 7 to 9 years after implant placement. The incidence of periimplantitis may be underestimated because few studies exist with follow-up longer than 10 years. Considering that chronic periodontitis often takes 30 years or more to develop, the current literature does not evaluate long-term periimplantitis incidence sufficiently. While dental implants have been shown to be successful in patients with severe periodontitis, several researchers have demonstrated the bacterial profile around implants is similar to the patient s natural teeth. 18,19 Dental implants may harbor a complex microbiota with a large proportion of known periodontal pathogens, such as Porphymonas gingivalis, Prevotella intermedia, and Fusobacterium nucleatum, which have been associated with the onset of periimplant mucositis and periimplantitis Additionally, studies examining long-term follow-up dental implants in patients with a history of periodontitis have suggested a higher incidence of soft-tissue inflammation (mucositis) and periimplantitis, as well as a slightly higher failure rate. 23 These findings support the recommendation that patients with dental implants require regular and careful evaluation at selected PM intervals to detect any clinical signs and symptoms of periimplant disease. TYPES OF PERIODONTAL MAINTENANCE PM programs may be prescribed for several scenarios. Patients may enter PM for reduction of disease risk, after completion of nonsurgical or surgical therapy, or for reduction of disease progression when definitive treatment cannot be rendered. For this reason, PM has been divided into four types 24 (Table 2). Selection of the appropriate type of maintenance for each patient allows the therapist to approach every maintenance visit with the appropriate mindset and also gives an idea of the case s direction as a communication tool between patients and providers. 1. Preventive PM: Intended to prevent inception of disease in those who currently do not have periodontal pathology (eg, patients at high risk for development of periodontal or periimplant problems because of systemic disease or dexterity problems that prevent practicing hygiene). 2. Trial PM: Intended to maintain borderline periodontal conditions to assess over time any progression of disease and the need for further treatment (eg, borderline pocket depths or furcation defects, inadequate gingiva Compendium 5
5 Continuing Education 1 around teeth or implants, or gingival architectural defects). 3. Compromise PM: Intended to slow disease progression in patients who would benefit from corrective treatment but are not surgical candidates because of health, economics, inadequate oral hygiene, or other considerations. This type also includes situations in which periodontal or periimplant defects persist after corrective therapy attempts (eg, patients with moderate chronic periodontitis or periimplantitis who cannot undergo treatment because of current gastric cancer treatment). 4. Posttreatment PM: Designed to prevent recurrence of disease after successful corrective therapy. This type of PM is the most commonly prescribed (eg, patients with localized aggressive periodontitis or periimplantitis who have been treated successfully with regenerative surgical therapy). FREQUENCY OF PERIODONTAL MAINTENANCE Soon after the bacterial oral biofilm is disturbed by plaque removal, it begins to reform. Eventually, the plaque becomes increasingly complex and gingival inflammation emerges. 25 Bacterial repopulation to pretreatment levels after scaling and root planing has been studied and, while it is variable between patients, may be seen as early as 42 days. 26 However, in most patients, the return to near-baseline bacterial levels occurs within 3 to 6 months. 27 Based on these studies, an initial PM interval of 3 months is selected for susceptible patients. While a 3-month interval is appropriate for many patients, PM needs to be tailored to each patient s level of disease activity and his or her ability and willingness to perform adequate oral hygiene. Patients who demonstrate persistent gingival inflammation, increasing probing depths, calculus formation, and poor plaque control around natural teeth or dental implants may require more frequent PM visits (ie, every 2 months instead of every 3 months). Conversely, for patients who demonstrate excellent plaque control, healthy gingiva, and stable probing depths, lengthening the PM interval may be appropriate (ie, every 4 months instead of every 3 months). Bleeding on probing has been proposed as one method for determining the PM interval. One study followed patients with treated chronic periodontitis who were on PM for 4 years. 28 It was found that bleeding on probing at more than 16% of sites was associated with increased attachment Table 2: Types of Periodontal/Periimplant Maintenance Type Description Examples Preventive Prevents inception of disease in patient at risk Patients with systemic diseases that Maintenance for periodontal or periimplant pathology predispose them to inflammatory oral oral disease; dexterity problems that complicate oral hygiene practices Trial Maintains borderline conditions Borderline pocket depths or furcation defects; Maintenance and observes for progression inadequate gingiva around teeth or implants; gingival architectural defects Compromise Slows disease progression in a patient who Moderate chronic periodontitis patient; Maintenance would benefit from corrective treatment patient with periimplantitis who cannot but is not a surgical candidate because of undergo surgical corrective therapy because health economics, inadequate oral hygiene, of current cancer/chemotherapy treatment or other considerations Posttreatment Prevents recurrence of disease after successful Localized aggressive periodontitis patient; Maintenance corrective therapy; this type of maintenance periimplantitis patient successfully treated is the most commonly prescribed with regenerative surgical therapy Adapted from Schallhorn RG et al Compendium September 2009 Volume 30, Number 7
6 Shumaker et al. loss, while bleeding on probing at < 10% of sites was not. Based on these findings, the researchers suggested the PM interval can be shortened or lengthened, depending on the percentage of bleeding sites found at each PM visit (Table 3). However, because bacterial repopulation occurs by 6 months in all patients, this interval should not exceed 6 months. Around dental implants, it appears that bleeding on probing provides similar predictability as an indicator of disease as with natural teeth. 29 These findings facilitate an evidence-based approach for clinicians to determine recall intervals for PM patients around both natural teeth and dental implants. MAINTENANCE VISITS PM visits should include an update of the medical and dental history; thorough extraoral and intraoral examinations that include oral cancer screening; periodontal and implant reevaluation; radiographic review; check of occlusion; removal of supra- and subgingival bacterial plaque and calculus; selective root planing; implant debridement if indicated; polishing if necessary; and a review of the patient s oral hygiene efficacy. 5,24 A typical appointment should take no more than 60 minutes, with at least 25% of this time devoted to mechanical debridement. 24 If signs of persistent disease activity are evident at the PM visit, such as persistent gingival or periimplant inflammation, bleeding on probing, implant mobility, and/or increasing probing depths, steps should be taken to address these findings to maintain health. If active treatment is performed during maintenance, a subsequent reevaluation should be scheduled at a 4- to 6- week interval to ensure any intervention was successful in controlling periodontal or periimplant diseases and whether further treatment is necessary. 30 This interval is recommended based on classic studies by Proye et al as well as Morrison et al, which have demonstrated posttreatment periodontal healing (around natural teeth) requires at least 4 weeks for reductions in pocket depth and gains in clinical attachment levels to fully occur. 30,31 There appears to be a paucity of specific studies on similar posttreatment response around ailing dental implants. However, most current studies suggest periimplant wound-healing processes are similar to natural teeth, and therefore a similar interval of 4 to 6 weeks is empirically suggested for reevaluation after treatment of inflammation around dental implants. 16,29 Table 3: Determining the Frequency of Maintenance Using Bleeding on Probing 28 Bleeding on Probing Frequency > 16% Sites Increase frequency of maintenance by 1 month (ie, every 4 months increased to every 3 months) < 10% Sites Decrease frequency of maintenance by 1 month (ie, every 2 months decreased to every 3 months) MANAGEMENT OF RECURRENT DISEASE DURING MAINTENANCE: NATURAL TEETH Signs of disease activity around natural teeth are indicated by the presence of bleeding on probing, visible soft-tissue inflammation, increasing probing depth, suppuration, radiographic bone loss, and/or increasing mobility that presents during maintenance. A combination of bleeding on probing at successive PM visits and increasing probing depth of > 1 mm has been found to be 87% predictive of periodontal bone and attachment loss. 32 When such findings are encountered during PM, early action should be taken to ensure management. The first step in addressing disease activity is local debridement of the site. For natural teeth, this involves high-quality scaling and root planing, using a combination of ultrasonic instruments and sharp hand curettes to ensure effective removal of plaque and calculus. Human clinical studies have demonstrated ultrasonic instruments have a tremendous advantage over hand instrumentation alone for several reasons. First, accessing the challenging anatomic features of multirooted teeth with furcation involvement is better achieved with ultrasonics Second, ultrasonics have been found to be more efficient and equally effective compared to hand instruments when applied to single rooted teeth. 33,36 Third, a combination of sonic and hand curette instruments for nonsurgical therapy has been shown to be more effective in calculus removal than either modality used alone. 37 Often, a single intervention of nonsurgical therapy is successful in controlling disease activity during the PM phase. Long-term studies have shown that after periodontal surgery, recurrent disease developing during PM responds favorably to nonsurgical therapy in 88% of cases. 38 The use of adjunctive treatments, such as introduction of additional oral hygiene aids, use of locally delivered antibiotics (such as minocycline microspheres [Arestin, OraPharma Compendium 7
7 Continuing Education 1 A B Figure 3 A patient in posttreatment periodontal maintenance program returned with (A) isolated bleeding on probing; and (B) a 5-mm probing depth noted at a maintenance visit. C D Figure 3C The site was treated by localized scaling and root planing, followed by use of Arestin (minocycline microspheres). Figure 3D The resolution of inflammation and bleeding on probing on the reevaluation appointment 6 weeks later. Inc, Warminster, PA]), host modulation therapy (low-dose doxycycline [Periostat]), subgingival irrigation, or prescription mouth rinses may be helpful in controlling signs of persistent disease. Locally delivered, controlled-release agents are a popular treatment adjunct and serve to augment scaling and root planing to help improve outcomes. Clinical studies have shown that use of such agents can provide an average of 0.5-mm additional pocket depth reduction over scaling and root planing alone, so the practitioner must weigh the cost-benefit ratio of using these products in each patient situation. 39,40 A guideline for the appropriate use of locally delivered antimicrobials has been provided by the American Academy of Periodontology. 41 These materials are contraindicated in patients with (1) multiple 5-mm pocket depths in one quadrant; (2) anatomic defects caused by periodontal diseases (intrabony defects); and (3) when the previous use of locally delivered agents has failed to control disease. As noted before, a follow-up reevaluation always should be completed to evaluate the success of any therapeutic intervention, generally at 4 to 6 weeks after treatment has been rendered 30,31 (Figure 3A through Figure 3D). If adjunctive treatments have been unsuccessful in controlling signs of disease, providers should re-treat the patient within their clinical competency and experience level or refer the patient to a specialist in periodontics for comanagement of the case. For recommendations on risk assessment and when to refer a patient to a periodontist, it is suggested that practitioners refer to the 2006 American Academy of Periodontology position paper, entitled Guidelines for the Management of Patients with Periodontal Diseases, which is at pdf. 42 These guidelines, while initially controversial, are intended to assist the general practitioner in quickly identifying only patients who are at the greatest risk and most appropriately suited for specialty care. These guidelines are not intended to serve as a medico-legal standard of care and do not replace the knowledge, skill, and abilities of the practitioner. 42 Ultimately, it is the patient who will benefit from thorough risk assessment and appropriate source of care. 8 Compendium September 2009 Volume 30, Number 7
8 Shumaker et al. MANAGEMENT OF RECURRENT DISEASE DURING MAINTENANCE: DENTAL IMPLANTS Signs of inflammatory disease activity around dental implants appear to be similar to those noted above for natural teeth, including bleeding on probing, visual inflammation, radiographic bone loss, and implant mobility. 29 Following implant restoration, patients should be reevaluated regularly (ie, every 3 to 4 months) during the first year. After the first year, the periimplant-tissue response should be evaluated and then the required customized frequency of PM should be determined, as discussed earlier in this article. Initial bone loss during the first year can be expected to be near the level of the first thread or may be less in systems that include platform switching. 43 Additional bone loss of approximately 0.1 mm per year for the first 5 years (up to a total of 1.5 mm) is considered normal. 44 Complete seating of the associated parts (abutment and/or restoration), occlusal overloading, absence of restorative overhangs, and the removal of all restorative cements also should be verified from the radiograph because these problems can predispose to longterm complications. 45 Conventional periodontal therapy should be instituted if inflammation develops around an implant. Therapy should include efforts to improve patient oral hygiene, using similar methods as around natural teeth (Figure 4A and Figure 4B). Lang et al suggested a novel, systematic stepwise approach for the prevention and treatment of periimplant diseases referred to as the cumulative interceptive supportive therapy (CIST) protocol 46 (Table 4). This system is based on periodic monitoring with implementation of treatment as thresholds for a particular condition are met. The first step is protocol (A), then (B) and, if conditions A continue to worsen, the case may require more advanced treatment, which may include comanagement with a specialist who has implant training to execute protocol (C), and finally (D). 20 Protocol (A) is used to control inflammation in periimplant mucositis, that is, implants with minimal increase in pocket depth, slight (+) bleeding on probing, marginal erythema, plaque, and/or calculus. The therapeutic endpoint is to resolve inflammation with cautious mechanical debridement (using plastic curettes and rubber cup prophylaxis), twice-daily swabbing with 0.12% chlorhexidine, and a review of home care and patient motivation. Protocol (B) is initiated for conditions that exhibit similar mucositis features but with deeper pocket depths (4 mm to 5 mm); however, there is still no loss of supporting bone. The treatment should include the therapies of protocol (A), plus locally delivered antibiotic (minocycline microspheres, doxycycline gel) at the infected implant site(s). Recent studies have shown the use of minocycline microspheres may be beneficial in treatment of periimplant mucositis and periimplantitis. 46 Management of early periimplantitis, protocol (C), requires a more robust approach and is used in conditions with evidence of osseointegrated bone loss of < 2 mm and pocket depths > 5 mm. The strategy should comprise the modalities for protocols (A) and (B) with the addition of systemic antibiotic therapy (metronidazole 250 mg t.i.d. for 7 days or amoxicillin 500 mg t.i.d. for 10 days). Furthermore, periodontal surgical access for surface decontamination (citric acid 1 to 2 minutes or tetracycline 250 mg, 5 ml for 5 minutes) should be considered. Protocol (D) is initiated in circumstances of frank periimplantitis that reveal probing depths (> 5 mm), (+) bleeding on probing, plaque/calculus, and periimplant bone loss of > 2 mm. This strategy requires periodontal surgical intervention B Figure 4A and 4B Use of a proxi-brush and large-diameter floss to perform plaque control around an implant-supported/retained prosthesis. Compendium 9
9 Continuing Education 1 Table 4: Summary of the CIST protocol for management of periimplant mucositis and periimplantitis in a clinical setting. 47 (PD = pocket depth; BOP = bleeding on probing.) Absence of Plaque BOP Negative No Treatment PD >3mm Presence of Plaque Protocol A Mechanical Debridement + Polishing PD 4-5 mm PD > 5 mm BOP+ No Bone Loss BOP+ Bone Loss < 2mm BOP+ Bone Loss >2mm + Protocol B + Protocol C + Protocol D Antiseptic Cleansing Local or Systemic Antibiotic Therapy Refer to Specialist Regenerative or Resective Surgery Refer to Specialist for chemical disinfection, osseous resection, and/or guided bone regeneration (GBR). GBR will attempt to salvage the implant through bone regeneration techniques with the use of resorbable or nonresorbable semipermeable membranes and a bone replacement graft (such as freeze-dried bone allograft or anorganic bovine bone). In clinical practice, CIST is aimed at early detection and methodical stepwise treatment, which may rescue and reverse the fate of the ailing or failing endosseous dental implant. 47 COMPLIANCE WITH PERIODONTAL MAINTENANCE Compliance with prescribed PM is often a challenge. Wilson conducted a survey of compliance rates in a private practice setting and found only 16% of patients were totally compliant with PM, 32% of patients never returned for PM, and the remaining 52% were erratic with compliance. 48 These numbers appear to be consistent with the medical literature on compliance. While the outlook on compliance may seem grim, Wilson et al found in a later study that compliance could be improved twofold by several methods, including sending reminder cards to patients and scheduling patients far in advance. 49 Additionally, compliance seems to increase with growing complexity of treatment, which may result in improved PM compliance among patients who have undergone significant periodontal surgery and/or dental implant therapy. Because compliance with PM is so critical to the longterm success of periodontal and dental implant therapy, the importance of PM must be emphasized with patients from the onset of treatment by all dental providers and at each follow-up maintenance visit. Patients must understand that the success of periodontal therapy rendered depends on compliance with PM and dental implants are not impervious to later inflammatory complications. MAINTENANCE AND PERIODONTAL MEDICINE Recent studies support the connection of periodontal diseases to several systemic diseases and conditions through chronic inflammatory mediators. 50 These include cardiovascular disease, stroke, chronic obstructive pulmonary disease, preterm low-birth-weight, and type 2 diabetes mellitus (dependent on level of blood glucose control). Many of these diseases and conditions are chronic and develop as a result of constant circulation of low-grade inflammatory cytokines and acute-phase proteins, such as interleukin-1, tumor necrosis factor-, and C-reactive protein, which have been shown to be increased by periodontal inflammation. 51 While at first glance, it may appear that short-term periodontal treatment may affect these disease relationships, in general, it is doubtful that a single session of scaling and root planing will reverse, for example, 30 years of atherosclerosis. Therefore, the role of the dental practitioner 10 Compendium September 2009 Volume 30, Number 7
10 Shumaker et al. in periodontal medicine best fits into a PM model. Lifelong PM is important not only in achieving periodontal health but also in minimizing the circulation of inflammatory cytokines for many years to mitigate the periodontally derived inflammatory risk factors for systemic diseases. CONCLUSION Periodontal treatment success, including both nonsurgical and surgical therapy, is dependent on appropriate maintenance. PM therapy also applies to dental implants, as they have been shown to be susceptible to periimplant disease. In addition, long-term control of periodontal inflammation may reduce the risk of several systemic diseases and conditions. It is the general practitioner s responsibility to evaluate each patient s dental history and prescribe appropriate periodontal and periimplant maintenance care, as well as to identify when conventional treatment is failing and to execute a prompt and appropriate solution, which includes use of adjunctive agents, surgery, or referral to a periodontist. The keys to success include consistent reminders sent to the patients on the importance of longterm maintenance in preventing periodontal or periimplant disease progression, as well as early identification and treatment of inflammatory and biomechanical problems to minimize their impact. This will maximize the likelihood of maintenance of natural teeth and dental implants in health, comfort, function, and esthetics for the duration of the patient s life. REFERENCES 1. Berglundh T, Persson L, Klinge B. A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. J Clin Periodontol. 2002;29(suppl 3): Newman MG, Takei HH, Carranza FA. Clinical Periodontology. 9th ed. Philadelphia, PA: Saunders; Lang NP, Nyman SR. Supportive maintenance care for patients with implants and advanced restorative therapy. Periodontol ;4: Preshaw PM, Heasman PA. Periodontal maintenance in a specialist periodontal clinic and in general dental practice. J Clin Periodontol. 2005;32(3): Cohen RE, Research, Science and Therapy Committee, American Academy of Periodontology. Position paper: periodontal maintenance. J Periodontol. 2003;74(9): Hirschfeld L, Wasserman B. A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol. 1978;49(5): Axelsson P, Nyström B, Lindhe J. The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J Clin Periodontol. 2004;31(9): Becker W, Becker BE, Berg LE. Periodontal treatment without maintenance. A retrospective study in 44 patients. J Periodontol. 1984;55(9): Lekholm U, Gunne J, Henry P, et al. Survival of the Brånemark implant in the partially edentulous jaws: a 10-year prospective multicenter study. Int J Oral Maxillofac Implants. 1999;14(5): Testori T, Del Fabbro M, Feldman S, et al. A multicenter prospective evaluation of 2-months loaded Osseotite implants placed in the posterior jaws: 3-year follow-up results. Clin Oral Implants Res. 2002;13(2): Nyman S, Lindhe J, Rosling B. Periodontal surgery in plaqueinfected dentitions. J Clin Periodontol. 1977;4(4): Fardal O, Linden GJ. Re-treatment profiles during long-term maintenance therapy in a periodontal practice in Norway. J Clin Periodontol. 2005;32(7): Scannapieco FA. Systemic effects of periodontal diseases. Dent Clin North Am. 2005;49(3): Brånemark PI. Introduction to osseointegration. In: Brånemark PI, Zarb G, Albrektsson T. Tissue Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago, IL: Quintessence; 1985: Hultin M, Gustafsson A, Hallström H, et al. Microbiological findings and host response in patients with peri-implantitis. Clin Oral Implants Res. 2002;13(4): Esposito M, Hirsch J, Lekholm U, et al. Differential diagnosis and treatment strategies for biologic complications and failing oral implants: a review of the literature. Int J Oral Maxillofac Implants. 1999;14(4): Roos-Jansåker AM, Lindahl C, Renvert H, et al. Nine- to fourteen-year follow-up of implant treatment. Part II: presence of peri-implant lesions. J Clin Periodontol. 2006;33(4): Quirynen M, Listgarten MA. Distribution of bacterial morphotypes around natural teeth and titanium implants ad modum Brånemark. Clin Oral Implants Res. 1990;1(1): Mombelli A, Marxer M, Gaberthüel T, et al. The microbiota of osseointegrated implants in patients with a history of periodontal disease. J Clin Periodontol. 1995;22(2): Compendium 11
11 Continuing Education 1 20.Weyant RJ, Burt BA. An assessment of survival rates and within-patient clustering of failures for endosseous oral implants. J Dent Res. 1993;72(1): Tonetti MS, Schmid J. Pathogenesis of implant failures. Periodontology ;4: Pontoriero R, Tonelli MP, Carnevale G, et al. Experimentally induced peri-implant mucositis. A clinical study in humans. Clin Oral Implants Res. 1994;5(4): Roos-Jansåker AM, Renvert H, Lindahl C, et al. Nine- to fourteen-year follow-up of implant treatment. Part III: factors associated with peri-implant lesions. J Clin Periodontol. 2006; 33(4): Schallhorn RG, Snider LE. Periodontal maintenance therapy. J Am Dent Assoc. 1981;103(2): Löe H, Theilade E, Jensen SB. Experimental gingivitis in man. J Periodontol. 1965;36: Mosquès T, Listgarten MA, Phillips RW. Effect of scaling and root planing on the composition of the human subgingival microbial flora. J Periodontal Res. 1980;15(2): Slots J, Mashimo P, Levine MJ, et al. Periodontal therapy in humans. I. Microbiological and clinical effects of a single course of periodontal scaling and root planing, and of adjunctive tetracycline therapy. J Periodontol. 1979;50(10): Lang NP, Joss A, Orsanic T, et al. Bleeding on probing. A predictor for the progression of periodontal disease. J Clin Periodontol. 1986;13(6): Salvi GE, Lang NP. Diagnostic parameters for monitoring periimplant conditions. Int J Oral Maxillofac Implants. 2004;19 (suppl): Proye M, Caton J, Polson A. Initial healing of periodontal pockets after a single episode of root planing monitored by controlled probing forces. J Periodontol. 1982;53(5): Morrison EC, Ramfjord SP, Hill R. Short-term effects of initial, nonsurgical periodontal treatment (hygienic phase). J Clin Periodontol. 1980;7(3): Claffey N, Egelberg J. Clinical indicators of probing attachment loss following initial periodontal treatment in advanced periodontitis patients. J Clin Periodontol. 1995;22(9): Matia JI, Bissada NF, Maybury JE, et al. Efficiency of scaling of the molar furcation area with and without surgical access. Int J Periodontics Restorative Dent. 1986;6(6): Wylam JM, Mealey BL, Mills MP, et al. The clinical effectiveness of open versus closed scaling and root planing on multirooted teeth. J Periodontol. 1993;64(11): Bower RC. Furcation morphology relative to periodontal treatment. Furcation entrance architecture. J Periodontol. 1979;50 (1): Badersten A, Nilveus R, Egelberg J. Effect of nonsurgical periodontal therapy. III. Single versus repeated instrumentation. J Clin Periodontol. 1984;11(2): Gellin RG, Miller MC, Javed T, et al. The effectiveness of the Titan-S sonic scaler versus curettes in the removal of subgingival calculus. A human surgical evaluation. J Periodontol. 1986; 57(11): Kaldahl WB, Kalkwarf KL, Patil KD, et al. Long-term evaluation of periodontal therapy: II. Incidence of sites breaking down. J Periodontol. 1996;67(2): Hanes PJ, Purvis JP. Local anti-infective therapy: pharmacological agents. A systematic review. Ann Periodontol. 2003;8 (1): Bonito AJ, Lux L, Lohr KN. Impact of local adjuncts to scaling and root planing in periodontal disease therapy: a systematic review. J Periodontol. 2005;76(8): Academy Report: American Academy of Periodontology statement on local delivery of sustained or controlled release antimicrobials as adjunctive therapy in the treatment of periodontitis. J Periodontol. 2006;77(8): Academy Report. Guidelines for the management of patients with periodontal diseases. J Periodontol. 2006;77(9): Canullo L, Rasperini G. Preservation of peri-implant soft and hard tissues using platform switching of implants placed in immediate extraction sockets: a proof-of-concept study with 12- to 36-month follow-up. Int J Oral Maxillofac Implants. 2007;22(6): Albrektsson T, Zarb G, Worthington P, et al. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986; 1(1): Lang B, Worthington P, LaVelle W. Osseointegration in Dentistry: An Introduction. Chicago, IL: Quintessence; 1994: Salvi GE, Persson GR, Heitz-Mayfield LJ, et al. Adjunctive local antibiotic therapy in the treatment of peri-implantitis II: clinical and radiographic outcomes. Clin Oral Implants Res. 2007;18(3): Lang NP, Berglundh T, Heitz-Mayfield LJ, et al. Consensus statements and recommended clinical procedures regarding implant survival and complications. Int J Oral Maxillofac Implants. 2004;19(suppl): Wilson TG Jr. Compliance. A review of the literature with possible applications to periodontics. J Periodontol. 1987;58(10): Wilson TG Jr, Hale S, Temple R. The results of efforts to improve compliance with supportive periodontal treatment in a private practice. J Periodontol. 1993;64(4): Scannapieco FA. Systemic effects of periodontal diseases. Dent Clin North Am. 2005;49(3): Loos BG. Systemic markers of inflammation in periodontitis. J Periodontol. 2005;76(11 suppl): Compendium September 2009 Volume 30, Number 7
12 Continuing Education 1 Quiz 1 1. Patient susceptibility currently: a. is modified with immunoglobulin. b. is tested for using RT-PCR. c. cannot be altered predictably. d. follows the y chromosome. 2. Subsequent regular periodontal maintenance is reported to prevent tooth loss in up to what percent of patients over a long-term follow-up interval of up to 53 years? a. 15% b. 35% c. 85% d. 95% 3. Long-term outcome studies on the delivery of periodontal treatment without any posttreatment PM have found that unmaintained patients lose how many times the number of teeth? a. one to two b. two to three c. three to four d. four to five 4. Inflammation limited to soft tissues around a dental implant may result from dental plaque colonization and is termed: a. periimplantitis. b. periimplant mucositis. c. periodontitis. d. gingivitis. 5. Patients may enter PM to: a. reduce disease risk. b. after completion of nonsurgical or surgical therapy. c. to reduce disease progression when definitive treatment cannot be rendered. d. all of the above 6. Bacterial repopulation to pretreatment levels after scaling and root planing has been studied and, while it is variable between patients, may be seen as early as: a. 24 to 48 hours. b. 7 to 10 days. c. 42 days. d. 3 to 6 months. 7. It was found that bleeding on probing at more than what percent of sites was associated with increased attachment loss? a. 16% b. 37% c. 48% d. 58% 8. Posttreatment periodontal healing (around natural teeth) requires at least how long for reductions in pocket depth and gains in clinical attachment levels to fully occur? a. 1 week b. 4 weeks c. 3 months d. 6 months 9. Additional bone loss of approximately 0.1 mm per year for the first 5 years (up to a total of how many mm) is considered normal? a. 0.5 mm b. 1 mm c. 1.5 mm d. 2 mm 10. Lifelong PM is important not only in achieving periodontal health but also in: a. preventing occlusal wear. b. minimizing the circulation of inflammatory cytokines. c. decreasing host immunity. d. altering the genetic response to bacterial attack. Please see tester form on page xx. This article provides 2 hours of CE credit from AEGIS Communications. Record your answers on the enclosed answer sheet or submit them on a separate sheet of paper. You may also phone your answers in to (888) or fax them to (703) or log on to and click on Continuing Education. Be sure to include your name, address, telephone number, and last 4 digits of your Social Security number. Compendium 13
SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW
 Review Article International Journal of Dental and Health Sciences Volume 02,Issue 06 SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW Deepak Kumar 1, Manvi Chandra agarwal 2, Ellora
Review Article International Journal of Dental and Health Sciences Volume 02,Issue 06 SUPPORTIVE PERIODONTAL THERAPY AND PATIENT S COMPLIANCE: AN OVERVIEW Deepak Kumar 1, Manvi Chandra agarwal 2, Ellora
The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis
 [ continuing [ education 1 ] 1 ] The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis Paul S. Rosen, DMD, MS Abstract Practitioners who are knowledgeable
[ continuing [ education 1 ] 1 ] The Team Approach to Managing Dental Implant Complications: Strategies for Treating Peri-implantitis Paul S. Rosen, DMD, MS Abstract Practitioners who are knowledgeable
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Scottish Dental Clinical Effectiveness Programme SDcep. Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief
 Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
Scottish Dental Clinical Effectiveness Programme SDcep Prevention and Treatment of Periodontal Diseases in Primary Care Guidance in Brief June 2014 Scottish Dental Clinical Effectiveness Programme SDcep
Guideline for Periodontal Therapy
 Guideline for Periodontal Therapy Originating Group American Academy of Periodontology Endorsed by the American Academy of Pediatric Dentistry 2003 Research has provided evidence that chronic inflammatory
Guideline for Periodontal Therapy Originating Group American Academy of Periodontology Endorsed by the American Academy of Pediatric Dentistry 2003 Research has provided evidence that chronic inflammatory
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION
 MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
Periodontal Screening and Recording: Early Detection of Periodontal Diseases
 Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Periodontal Screening and Recording: Early Detection of Periodontal Diseases Tanya Villalpando Mitchell, RDH, MS Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce53/ce53.aspx
Manage Patients in Peri - Implant Health
 Matilde N Hernandez Gonzalez, DDS, MS, MBA Manage Patients in Peri - Implant Health Upon completion of reading these articles, the clinician will be able to: 1. Use adjunctive therapies to enhance dental
Matilde N Hernandez Gonzalez, DDS, MS, MBA Manage Patients in Peri - Implant Health Upon completion of reading these articles, the clinician will be able to: 1. Use adjunctive therapies to enhance dental
Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan
 Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Treatment of Peri-implantitis Lesions with Laser-assisted Therapy and a Minimally Invasive Approach: A Case Report
 Treatment of Peri-implantitis Lesions with Laser-assisted Therapy and a Minimally Invasive Approach: A Case Report Elvan Efeoglu a, Gulin T. Eyyupoglu b Publication a Professor, Dr, Department of Periodontology,
Treatment of Peri-implantitis Lesions with Laser-assisted Therapy and a Minimally Invasive Approach: A Case Report Elvan Efeoglu a, Gulin T. Eyyupoglu b Publication a Professor, Dr, Department of Periodontology,
Periodontal Surgery. What Can I Expect? The word "periodontal" literally means around the tooth. Many factors, such as oral hygiene habits, genetics,
 The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Periodontology JOURNAL OF CONTENTS. Parameters of Care. Foreword...i. Overview...ii. Parameter on Comprehensive Periodontal Examination...
 Volume 71 Number 5 May 2000 (Supplement) JOURNAL OF Periodontology CONTENTS Parameters of Care Foreword...i Overview...ii Parameter on Comprehensive Periodontal Examination...847 Parameter on Periodontal
Volume 71 Number 5 May 2000 (Supplement) JOURNAL OF Periodontology CONTENTS Parameters of Care Foreword...i Overview...ii Parameter on Comprehensive Periodontal Examination...847 Parameter on Periodontal
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Periodontal (Gum) Disease: Causes, Symptoms, and Treatments
 Periodontal (Gum) Disease: Causes, Symptoms, and Treatments Introduction If you have been told you have periodontal (gum) disease, you're not alone. An estimated 80 percent of American adults currently
Periodontal (Gum) Disease: Causes, Symptoms, and Treatments Introduction If you have been told you have periodontal (gum) disease, you're not alone. An estimated 80 percent of American adults currently
CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT. Philosophical Basis of the Patient Care System. Patient Care Goals
 University of Washington School of Dentistry CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT Philosophical Basis of the Patient Care System The overall mission of the patient care system in the School
University of Washington School of Dentistry CLINICAL GOALS OF PATIENT CARE AND CLINIC MANAGEMENT Philosophical Basis of the Patient Care System The overall mission of the patient care system in the School
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
Peri-implant diseases are characterized by. Clinical Review
 Clinical Review Prognosis in Implant Dentistry: A System for Classifying the Degree of Peri-Implant Mucosal Inflammation Getulio Nogueira-Filho, DDS, MDent, PhD; Anthony M. Iacopino, DMD, PhD; Howard C.
Clinical Review Prognosis in Implant Dentistry: A System for Classifying the Degree of Peri-Implant Mucosal Inflammation Getulio Nogueira-Filho, DDS, MDent, PhD; Anthony M. Iacopino, DMD, PhD; Howard C.
NONSURGICAL PERIODONTAL THERAPY Instructed by Kelli R. Illyes, R.D.H, M.D.H.
 NONSURGICAL PERIODONTAL THERAPY Instructed by Kelli R. Illyes, R.D.H, M.D.H. INSTRUCTIONS: Read and study the narrative. Complete the quiz and registration form, and mail (along with registration fee)
NONSURGICAL PERIODONTAL THERAPY Instructed by Kelli R. Illyes, R.D.H, M.D.H. INSTRUCTIONS: Read and study the narrative. Complete the quiz and registration form, and mail (along with registration fee)
Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.210 Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review Kyoung-Kyu Kim*, DDS, MSD, Hun-Mo
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.4.210 Outcomes of dental implant treatment in patients with generalized aggressive periodontitis: a systematic review Kyoung-Kyu Kim*, DDS, MSD, Hun-Mo
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW
 Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW Presented by: Dr. Syeda Mahvash Hussain Resident Operative Dentistry Aga Khan University Hospital Karachi Contributors: Drs. Maham
Amount of tooth substance gained by crown lengthening: A SYSTEMATIC REVIEW Presented by: Dr. Syeda Mahvash Hussain Resident Operative Dentistry Aga Khan University Hospital Karachi Contributors: Drs. Maham
Complications with excess cement & dental implants: Diagnosis, recommendations & treatment of 7 clinical cases.
 Robert A. Levine DDS, FCPP, Diplomate, American Board of Periodontology Clinical Professor, Temple University Kornberg School of Dentistry Fellow International Team for Implantology Pennsylvania Center
Robert A. Levine DDS, FCPP, Diplomate, American Board of Periodontology Clinical Professor, Temple University Kornberg School of Dentistry Fellow International Team for Implantology Pennsylvania Center
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Figure 1. Comparison of crestal gingival fiber orientation.
 70 Test 75.2 IMPLANTS Oral Hygiene and Maintenance of Dental Implants Lee H. Silverstein, DDS, MS Gregori M. Kurtzman, DDS Figure 1. Comparison of crestal gingival fiber orientation. In more recent years,
70 Test 75.2 IMPLANTS Oral Hygiene and Maintenance of Dental Implants Lee H. Silverstein, DDS, MS Gregori M. Kurtzman, DDS Figure 1. Comparison of crestal gingival fiber orientation. In more recent years,
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Teeth and Dental Implants: When to save, and when to extract.
 Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Teeth and Dental Implants: When to save, and when to extract. One of the most difficult decisions a restorative dentist has to make is when to refer a patient for extraction and placement of dental implants.
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Dental implants: Maintenance, care and treatment of peri-implant infection
 MS 1023 REVIEW Australian Dental Journal 2003;48:(4):212-220 Dental implants: Maintenance, care and treatment of peri-implant infection S Chen,* I Darby, Abstract Osseointegration is becoming increasingly
MS 1023 REVIEW Australian Dental Journal 2003;48:(4):212-220 Dental implants: Maintenance, care and treatment of peri-implant infection S Chen,* I Darby, Abstract Osseointegration is becoming increasingly
Insurance Coding: Teaching Our Periodontics Residents
 Charleston, SC Insurance Coding: Teaching Our Periodontics Residents Joe W. Krayer, D.D.S., M.S. Associate Professor & Director Post-Doctoral Periodontics Program Robert G. Gellin, D.M.D., M.H.S. Professor
Charleston, SC Insurance Coding: Teaching Our Periodontics Residents Joe W. Krayer, D.D.S., M.S. Associate Professor & Director Post-Doctoral Periodontics Program Robert G. Gellin, D.M.D., M.H.S. Professor
TREATMENT REFUSAL FORMS
 TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Implant therapy using osseointegrated implants has
 Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
MDA New Dental Health Care Worker Dental Scaling Assistant
 MDA New Dental Health Care Worker Dental Scaling Assistant Registered Dental Therapist -1 Proposed additional functions delegable to dental assistants (only under the direct supervision of a dentist):
MDA New Dental Health Care Worker Dental Scaling Assistant Registered Dental Therapist -1 Proposed additional functions delegable to dental assistants (only under the direct supervision of a dentist):
ACADEMY OF LASER DENTISTRY COMMITTEE ON REGULATORY AFFAIRS TABLE OF CONTENTS
 ACADEMY OF LASER DENTISTRY COMMITTEE ON REGULATORY AFFAIRS INFORMATION PACKET FOR STATE BOARDS OF DENTISTRY May 2014 TABLE OF CONTENTS 1. Mission Statement of the Academy... 1 2. Position Statement on
ACADEMY OF LASER DENTISTRY COMMITTEE ON REGULATORY AFFAIRS INFORMATION PACKET FOR STATE BOARDS OF DENTISTRY May 2014 TABLE OF CONTENTS 1. Mission Statement of the Academy... 1 2. Position Statement on
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
3. Entry Requirements
 1. Introduction The EFP has previously published its recommendations concerning undergraduate and specialist education in periodontology. The aim of this document is to give guidance to those authorities
1. Introduction The EFP has previously published its recommendations concerning undergraduate and specialist education in periodontology. The aim of this document is to give guidance to those authorities
Legal Ethical Dilemma
 Legal Ethical Dilemma Jen Sandstrom, Marta Rewako, Michelle Vu, and Lindsey Cetani Foothill College Spring 2014 Introduction Throughout our career as dental hygienists, we will face many legal and ethical
Legal Ethical Dilemma Jen Sandstrom, Marta Rewako, Michelle Vu, and Lindsey Cetani Foothill College Spring 2014 Introduction Throughout our career as dental hygienists, we will face many legal and ethical
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
SCOPE OF PRACTICE GENERAL DENTAL COUNCIL
 www.gdc-uk.org SCOPE OF PRACTICE Effective from 30 September 2013 2 SCOPE OF PRACTICE The scope of your practice is a way of describing what you are trained and competent to do. It describes the areas
www.gdc-uk.org SCOPE OF PRACTICE Effective from 30 September 2013 2 SCOPE OF PRACTICE The scope of your practice is a way of describing what you are trained and competent to do. It describes the areas
into the for Entry Following Entry into care team the Allied Dental Assisting guidelines. professions. programs.
 ADEA Competencies for Entry into the Allied Dental Professionss (As approved by the 2011 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association of Dental
ADEA Competencies for Entry into the Allied Dental Professionss (As approved by the 2011 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association of Dental
Eastman Dental Hospital. Dental implants - general information for patients. Department of Restorative Dentistry
 Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
HEALTH SERVICES POLICY & PROCEDURE MANUAL. SUBJECT: Types of Dental Treatments Provided EFFECTIVE DATE: July 2014 SUPERCEDES DATE: January 2014
 PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
The management of traumatic tooth loss with dental implants: Part 2. Severe trauma
 The management of traumatic tooth loss with dental implants: Part 2. Severe trauma D. W. Seymour,* 1 M. Patel, 2 L. Carter 3 and M. Chan 2 IN BRIEF Discusses the challenges associated with the provision
The management of traumatic tooth loss with dental implants: Part 2. Severe trauma D. W. Seymour,* 1 M. Patel, 2 L. Carter 3 and M. Chan 2 IN BRIEF Discusses the challenges associated with the provision
PARTIAL CURRICULUM VITAE. Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012
 PARTIAL CURRICULUM VITAE Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012 Professional Education: D.D.S. Marquette University 1952-1956 Certificate
PARTIAL CURRICULUM VITAE Robert G. Schallhorn, D.D.S., M.S. Business Address: 11200 E. Mississippi Avenue Aurora, Colorado 80012 Professional Education: D.D.S. Marquette University 1952-1956 Certificate
(a) The performance of intraoral tasks by dental hygienists or assistants shall be under the direct supervision of the employer-dentist;
 5-1-8. Expanded duties of dental hygienists and dental assistants. 8.1. General. Licensed dentists may assign to their employed dental hygienists or assistants intraoral tasks as set out in this section
5-1-8. Expanded duties of dental hygienists and dental assistants. 8.1. General. Licensed dentists may assign to their employed dental hygienists or assistants intraoral tasks as set out in this section
TRAINING STANDARDS IN IMPLANT DENTISTRY
 TRAINING STANDARDS IN IMPLANT DENTISTRY Introduction 2012 1 Dental implants are used to replace one or more missing teeth. Their insertion involves various surgical and restorative dental procedures and
TRAINING STANDARDS IN IMPLANT DENTISTRY Introduction 2012 1 Dental implants are used to replace one or more missing teeth. Their insertion involves various surgical and restorative dental procedures and
Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates)
 Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association
Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association
Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies
 Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies Jason M. Mailhot, DMD, MS, FACD; Spencer L. Fried, DDS, MS Continuing
Periodontics: Oral Health and Wellness I. Understanding Periodontal Health, Recognizing Disease States and Choices in Treatment Strategies Jason M. Mailhot, DMD, MS, FACD; Spencer L. Fried, DDS, MS Continuing
OVERVIEW The MetLife Dental Plan for Retirees
 OVERVIEW The MetLife Dental Plan for Retirees IN NETWORK: Staying in network saves you money. 1 Participating dentists have agreed to MetLife s negotiated fees which are typically 15% to 45% below the
OVERVIEW The MetLife Dental Plan for Retirees IN NETWORK: Staying in network saves you money. 1 Participating dentists have agreed to MetLife s negotiated fees which are typically 15% to 45% below the
Semester I Dental Anatomy (Basic Orofacial Anatomy)
 Dental Assisting Curriculum Example The dentalcare.com CE library offers over 150 courses that can be used in conjunction with your dental assisting curriculum. The guide below recommends courses to assign,
Dental Assisting Curriculum Example The dentalcare.com CE library offers over 150 courses that can be used in conjunction with your dental assisting curriculum. The guide below recommends courses to assign,
IMPLANT MENTOR PROGRAM
 THE BRIGHTON INSTITUTE FOR DENTAL IMPLANTS IMPLANT MENTOR PROGRAM WITH DR BRUNO SILVA www.brightonimplantclinic.com www.thebrightonimplantinsitute.com Foreword Osseointegrated implants are enabling dentists
THE BRIGHTON INSTITUTE FOR DENTAL IMPLANTS IMPLANT MENTOR PROGRAM WITH DR BRUNO SILVA www.brightonimplantclinic.com www.thebrightonimplantinsitute.com Foreword Osseointegrated implants are enabling dentists
Dental Services. Dental Centre. HKSH Healthcare Medical Centre Dental Centre. For enquiries and appointments, please contact us
 Dental Services For enquiries and appointments, please contact us HKSH Healthcare Medical Centre Dental Centre Level 22, One Pacific Place 88 Queensway, Hong Kong (852) 2855 6666 (852) 2892 7589 [email protected]
Dental Services For enquiries and appointments, please contact us HKSH Healthcare Medical Centre Dental Centre Level 22, One Pacific Place 88 Queensway, Hong Kong (852) 2855 6666 (852) 2892 7589 [email protected]
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
The success of osseointegrated dental implants
 REVIEW ARTICLE Current Status of Dental Implants: A Periodontal Perspective Perry R. Klokkevold 1 /Michael G. Newman, DDS 2 The success of osseointegrated dental implants has revolutionized dentistry.
REVIEW ARTICLE Current Status of Dental Implants: A Periodontal Perspective Perry R. Klokkevold 1 /Michael G. Newman, DDS 2 The success of osseointegrated dental implants has revolutionized dentistry.
Spedding Dental Clinic. 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk
 DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
Updated: February 2014. 1986-1990 Highland General Hospital, Certificate of Completion Oral & Maxillofacial Surgery Residency
 Edmond Bedrossian DDS, FACD, FACOMS, FAO Diplomate, American Board of Oral & Maxillofacial Surgery Director, Implant Surgery, Alameda Medical Center & UOP School of Dentistry Professor, Department of Oral
Edmond Bedrossian DDS, FACD, FACOMS, FAO Diplomate, American Board of Oral & Maxillofacial Surgery Director, Implant Surgery, Alameda Medical Center & UOP School of Dentistry Professor, Department of Oral
POWER SCALING AIR-FLOW AIR POLISHING SOLUTIONS
 POWER SCALING AIR-FLOW AIR POLISHING SOLUTIONS ADVANCING PROPHYLAXIS PROTOCOL Introducing THE AIR-FLOW TECHNOLOGY AIR-FLOW PERIO units reach into periodontal pockets to remove biofilm. The new PERIO-FLOW
POWER SCALING AIR-FLOW AIR POLISHING SOLUTIONS ADVANCING PROPHYLAXIS PROTOCOL Introducing THE AIR-FLOW TECHNOLOGY AIR-FLOW PERIO units reach into periodontal pockets to remove biofilm. The new PERIO-FLOW
Immediate Molar Implant Placement: A Private Practice Clinical Investigation. Abstract
 Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
DENTAL COUNCIL. Statutory Examination
 DENTAL COUNCIL Statutory Examination The Dentists Act 1985 requires that in order to practice dentistry in the Republic of Ireland a dentist must be registered with the Dental Council of Ireland. Registration
DENTAL COUNCIL Statutory Examination The Dentists Act 1985 requires that in order to practice dentistry in the Republic of Ireland a dentist must be registered with the Dental Council of Ireland. Registration
[PAGE HEADLINE] Improve your Health and Change Your Smile with Complete Dental Services in One [CITYNAME] Location
![[PAGE HEADLINE] Improve your Health and Change Your Smile with Complete Dental Services in One [CITYNAME] Location [PAGE HEADLINE] Improve your Health and Change Your Smile with Complete Dental Services in One [CITYNAME] Location](/thumbs/31/14971568.jpg) Eddie Stephens//Copywriter Sample: Website copy/internal Dental Services Pages [PAGE HEADLINE] Improve your Health and Change Your Smile with Complete Dental Services in One [CITYNAME] Location [LEAD SENTENCE/PARAGRAPH]
Eddie Stephens//Copywriter Sample: Website copy/internal Dental Services Pages [PAGE HEADLINE] Improve your Health and Change Your Smile with Complete Dental Services in One [CITYNAME] Location [LEAD SENTENCE/PARAGRAPH]
MAIN LINE DENTAL IMPLANT CENTER
 1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
2007 Insurance Benefits Guide. Dental and Dental Plus. Dental and. Dental Plus. www.eip.sc.gov Employee Insurance Program 91
 Dental and www.eip.sc.gov Employee Insurance Program 91 Table of Contents Introduction...93 Your Dental Benefits at a Glance...94 Claim Examples (using Class III procedure claims)...95 How to File a Dental
Dental and www.eip.sc.gov Employee Insurance Program 91 Table of Contents Introduction...93 Your Dental Benefits at a Glance...94 Claim Examples (using Class III procedure claims)...95 How to File a Dental
C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY
 C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY I. TREATMENT PLANNING GUIDELINES As part of informed consent, the clinician should carefully explain the risks and benefits of oral and maxillofacial surgery
C HAPTER 4 O RAL AND M AXILLOFACIAL S URGERY I. TREATMENT PLANNING GUIDELINES As part of informed consent, the clinician should carefully explain the risks and benefits of oral and maxillofacial surgery
POWER SCALING CLINICAL EVIDENCE FOR AIR-FLOW PERIO ON NATURAL TEETH AND IMPLANTS SCIENTIFIC LITERATURE IN PERIODONTOLOGY
 POWER SCALING CLINICAL EVIDENCE FOR AIR-FLOW PERIO ON NATURAL TEETH AND IMPLANTS SCIENTIFIC LITERATURE IN PERIODONTOLOGY TABLE OF CONTENTS EDITORIAL... 4 AIR-FLOW increasingly significant in modern prophylaxis
POWER SCALING CLINICAL EVIDENCE FOR AIR-FLOW PERIO ON NATURAL TEETH AND IMPLANTS SCIENTIFIC LITERATURE IN PERIODONTOLOGY TABLE OF CONTENTS EDITORIAL... 4 AIR-FLOW increasingly significant in modern prophylaxis
Encode Impression System. Optimization By Design
 The Encode Impression System Optimization By Design Optimization Is Key To Aesthetics The BellaTek Encode Impression System provides optimized solutions to clinicians by eliminating the need for implant
The Encode Impression System Optimization By Design Optimization Is Key To Aesthetics The BellaTek Encode Impression System provides optimized solutions to clinicians by eliminating the need for implant
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
Oral Plastic Surgery
 20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
Differential Diagnosis and Treatment Strategies for Biologic Complications and Failing Oral Implants: A Review of the Literature
 Differential Diagnosis and Treatment Strategies for Biologic Complications and Failing Oral Implants: A Review of the Literature Marco Esposito, DDS*/Jan Hirsch, DDS, PhD**/Ulf Lekholm, DDS, PhD***/ Peter
Differential Diagnosis and Treatment Strategies for Biologic Complications and Failing Oral Implants: A Review of the Literature Marco Esposito, DDS*/Jan Hirsch, DDS, PhD**/Ulf Lekholm, DDS, PhD***/ Peter
dental implants for tooth replacement be a confident you
 dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
IMPLANTS IN FOCUS. Endosseous dental implant restorations PLANNING FOR IMPLANT RESTORATIONS
 IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on Periodontology
 J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
J Clin Periodontol 2008; 35 (Suppl. 8): 168 172 doi: 10.1111/j.1600-051X.2008.01268.x Advances in bone augmentation to enable dental implant placement: Consensus Report of the Sixth European Workshop on
Position Classification Standard for Dental Officer Series, GS-0680
 Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment.
 Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment. Dr. med. dent. David McFadden, Dallas County, USA Initial situation (single X-ray) Tooth 16
Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment. Dr. med. dent. David McFadden, Dallas County, USA Initial situation (single X-ray) Tooth 16
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
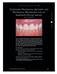 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial.
 Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
States That Allow Hygienists to Authorizing rule, Law, or Policy
 States That Allow Hygienists to Use Lasers: 31 Authorizing rule, Law, or Policy Alaska If the statutes and regulations are silent on a procedure or do not prohibit a procedure, the interpretation is a
States That Allow Hygienists to Use Lasers: 31 Authorizing rule, Law, or Policy Alaska If the statutes and regulations are silent on a procedure or do not prohibit a procedure, the interpretation is a
