Patrick Coyne, RN, MSN, CS, CRNH Theresa E. Clor, RN, MS, CS, ANP Laurie Cooksey, PharmD
|
|
|
- Ashlyn Gilmore
- 10 years ago
- Views:
Transcription
1 MEDICAL COLLEGE OF VIRGINIA HOSPITALS VIRGINIA COMMONWEALTH UNIVERSITY DEPARTMENT OF NURSING SERVICES DEPARTMENT OF PHARMACY AND THE DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL Patrick Coyne, RN, MSN, CS, CRNH Theresa E. Clor, RN, MS, CS, ANP Laurie Cooksey, PharmD Previous Contributors: Lori Lush, PharmD Maryanne MacMurren, RN, BSN, CRNI Stephen P. Long, MD John M. Barsanti, MD
2 1995
3 TABLE OF CONTENTS General Procedures for Caring for Patients Receiving Epidural, Intrathecal or Caudal Analgesia or Nerve Blockade via Indwelling Catheters... Page 1 Nursing Procedures for Caring for Patients Receiving Epidural, Intrathecal, or Caudal Analgesia or Nerve Blockade via Indwelling Catheters... Page 3 Nursing Procedures for Caring for Pediatric Patients Receiving Epidural, Intrathecal, or Caudal Analgesia or Nerve Blockade via Indwelling Catheters... Page 7 Analgesia Catheter Disconnect... Page 8 Transporting/Transferring Patients Receiving Analgesia via Epidural, Intrathecal, Caudal or other Indwelling Catheters... Page 9 Removal of Analgesia Catheter...Page 10 Loading the Analgesia Infusion Pump...Page 12 Priming and Programming the Analgesia Infusion Pump...Page 14 Infusion Bag Change...Page 17 Obtaining Patient History from the Analgesia Infusion Pump...Page 19 Bolus Administration via the Analgesia Infusion Pump...Page 21 Analgesia Prescription Change...Page 23 Controlled Substance Recordkeeping...Page 24 Nursing Care of Patients Receiving PCA or Continuous Subcutaneous Opiates...Page 26 Application and Destruction of Fentanyl Transdermal Patches...Page 28 Nursing Care of the Patient Receiving TENS...Page 29 Monitoring Patients with Spinal Cord Stimulation (SCS)...Page 30 Monitoring Patients with a Long Term Implanted Catheter for Infusion of Analgesia...Page 31 Refill Procedure for a Medtronic Synchromed Pump...Page 32 Parameter Changes to Medtronic Synchromed Pump...Page 34
4 APPENDICES Epidural Analgesia...i Pain Management Flowsheet... v Standards of Care for Patients Receiving Epidural, Intrathecal, Caudal Analgesia or Analgesia via other Indwelling Catheters...vi Pain Standard of Care... ix Analgesia Infusion Pump Alarms... xi APS Standing Orders... xii Patient Education Handout for Epidural Analgesia...xv Patient Education Handout for PCA...xvi Opiate Pharmacodynamic/Pharmacokinetic and Equianalgesic Doses... xvii Pediatric Dosing Guidelines... xviii Adjunct Medications... xix TENS Troubleshooting... xx?? ` Hospital Policy of PCA......xx?? Placebo...xx?? Bibliography...xx?? Patient Controlled Analgesia...Appendix 1. MCVH/VCU Policy and Procedure Manual...Appendix 2 MCVH/MCV Associated Physicians Policy and Procedure Manual...Appendix 3 Epidural Caudal Quiz...Appendix 4.
5 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: GENERAL PROCEDURES FOR CARING FOR PATIENTS RECEIVING EPIDURAL, INTRATHECAL OR CAUDAL ORIGINAL DATE: JULY 1991 ANALGESIA OR NERVE BLOCKADE VIA REVIEW/REVISE: SEPTEMBER 2001 INDWELLING CATHETERS EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To outline the general responsibilities surrounding the administration of intermittent, continuous or PCA analgesia infusions with or without local anesthetics into the epidural, intrathecal or caudal space or via other indwelling catheters. II. POLICY Only healthcare professionals verified in analgesia infusion pump operation and inserviced in care of patients with epidural, intrathecal, caudal or other indwelling catheters will care for patients with such catheters. III. SUPPORTIVE DATA A. Epidural catheters may be used for the administration of analgesic agents with or without local anesthetics. B. The Acute Pain Service (APS) is responsible for all analgesic orders for the duration of the catheter placement. No other sedatives, opiates, or hypnotics will be administered without the Acute Pain Service's notification. C. Only preservative-free opiates and/or anesthetics are infused through the epidural catheter. D. The APS will be responsible for changing the epidural tubing and programming the analgesia infusion pump. E. A member of the APS will be available 24 hours a day to assist with problems related to pain control therapy. This patient visit will be documented in the progress notes section of the patient's medical record. F. Naloxone (Narcan ) will be available on all code carts and in individual patient's medication drawers for patients receiving epidural opiates. If a naloxone infusion is initiated, the infusion will be maintained on a pump which is clearly labeled "Narcan infusion". G. Ephedrine injection will be available on nursing units narcotic carts caring for patients receiving local anesthetics. H. Patients will not routinely be monitored with pulse oximeters. Children are the exception to the rule (see Pediatric Policy page 6). I. Rooms of patients receiving epidural opiates will be labeled with a sign clearly identifying he/she is receiving epidural opiates and to administer no sedatives, hypnotics or opiates without notifying the APS. J. Heating pads or cool/cold applications should be used with caution with patients receiving local anesthetics. K. Patients receiving local anesthetics should be on fall precautions. MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL 1
6 SUBJECT: NURSING PROCEDURES FOR CARING FOR PATIENTS RECEIVING EPIDURAL, INTRATHECAL OR CAUDAL ORIGINAL DATE: JULY 1991 ANALGESIA OR NERVE BLOCKADE VIA REVIEW/REVISE: SEPTEMBER 2001 INDWELLING CATHETERS EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To outline nursing responsibilities in administering intermittent, continuous and PCA analgesia with opiate and/or local anesthetic agents via epidural, intrathecal, caudal space or other indwelling catheters. II. POLICY Nurses will properly follow and monitor infusion procedures for patients receiving intermittent, continuous, or PCA analgesia with opiate and/or local anesthetic agents via epidural, intrathecal, caudal or other indwelling catheters. III. SUPPORTIVE DATA A. Licensed nursing personnel who are required to monitor, maintain and care for patients receiving these analgesic modalities will have access to pertinent policies and procedures relating to these therapies. B. Only nurses verified in analgesia infusion pump operation and inserviced in care of patients with epidural, intrathecal, caudal or other indwelling catheters will care for patients with such catheters. C. Nurses without special training will not remove epidural, intrathecal, caudal or other indwelling catheters placed for the purpose of providing analgesia. D. Nurses' responsibilities include: - changing medication bags - changing 9-Volt batteries - reinforcing dressings - reconnecting catheter disconnects at hub - replace hub per policy and procedure - following monitoring procedures IV. ASSESSMENT OF PATIENTS RECEIVING EPIDURAL ANALGESIA A. Ensure that the epidural patient receiving opiates has an order for naloxone and that the drug is available on the nursing unit. B. Ensure patent IV access (can be a saline lock after the first 12 hours) exists for the duration of analgesic therapy. IV access must be maintained for 4-12 hours after the last epidural bolus or from termination of epidural analgesia. C. Ensure that the epidural patient receiving local anesthetics has an order for ephedrine and that the drug is available on the nursing unit. D. Assess and document on the Pain Management Flowsheet: pain ratings, sedation ratings, dermatome levels (if local anesthetic is used), vital signs, analgesia infusion pump function and usage, catheter insertion site and side effects, including motor function blockade per the following procedures. 1. Pain assessment A pain assessment will be conducted q4h while a patient is awake and documented on the Pain Management Flowsheet. A 0-10 verbal scale will be utilized. 2. Sedation assessment 2
7 The following scale will be used to assess the patient's level of sedation. This will be performed q1h x 4 hours for fentanyl (Sublimaze ) infusion and q1h x 12 hours for morphine (Duramorph ) infusion and documented on the Pain Management Flowsheet. 1 = Alert 2 = Intermittently drowsy 3 = Frequently drowsy 4 = Asleep, easy to arouse 5 = Somnolent, difficult to arouse 3. The following is an explanation on how to assess the dermatome level in a patient receiving local anesthetics. A dermatome level will be assessed and documented on the Pain Management Flowsheet q4h if a patient is receiving local anesthetic. T10 - Umbilicus T8 - Lower Rib T4 - Nipple T2 - Inner Aspect of Upper Arm a. Using the assessment scale above, test each general nerve region (S = Sacral, L = lumbar, T = Thoracic, C = Cervical). b. Using an opened, saturated alcohol swab, begin with the feet bilaterally and test all areas upward assessing for changes in sensation. Decreased ability to feel temperature changes or inability to bend at the knees may indicate a need to reduce or stop the local anesthetic infusion. c. Note any new or increased tingling, numbness or absent sensation and notify the Acute Pain Service. d. Document patient's ability to ambulate. e. Note: Patient should be on fall precautions. 4. Assessment of analgesia infusion pump function The function of the analgesia infusion pump as well as the verification of dosage (i.e., medication, concentration, residual volume, given volume, PCA dose, delay, basal rate, 1-hour limit) will be assessed q4h and documented in appropriate columns on the Pain Management Flowsheet. 5. The nurse will document analgesia infusion pump usage via the HIS system every shift. 6. Assessment of catheter insertion site An assessment should be made of the condition of the analgesia catheter insertion site and dressing every shift. If the dressing becomes loose, the dressing should be reinforced and the APS service notified. The Acute Pain Service should also be notified for: a. Signs of leakage b. Skin irritation c. Signs of infections d. Catheter problems 7. Assessment of vital signs Vital signs should be monitored as follows: a. Blood pressure: q4h and prior to ambulation if local anesthetic is used. b. Temperature: as ordered by patient's primary attending. 3
8 c. Pulse: as ordered by patient's primary attending unless local anesthetic is used then every 4 hours. d. Respiratory rate: (counted for 1 full minute) q1h x 12 hours for fentanyl (Sublimaze ) infusion with or without local anesthetic and q1h x 24 hours for morphine (Duramorph ) infusion with or without local anesthetic, then q4h. A nurse may use his/her discretion to avoid waking the patient q1h if respiratory rate is strong, even, regular and of sufficient depth. e. After bolus administration of > 50 µg of fentanyl or with a local anesthetic, a full set of vital signs (except temperature) should be performed q5 minutes x 2; then q15 minutes x 2; then return to the original assessment schedule. f. All vital signs should be documented on the Pain Management Flowsheet unless the patient is in an ICU where vital signs are documented on the ICU flowsheet at the Acute Pain Service ordered intervals. 8. Assessment of side effects Side effects (i.e., nausea, itching, urinary retention or vomiting) will be documented on the Pain Management Flowsheet q4h or whenever the patient complains. 9. Assessment of motor blockade If the patient is receiving local anesthetic via a catheter placed for the purpose of providing analgesia to an extremity, the patient's blocked extremity will be assessed every four hours while awake for signs of motor blockade. E. After the analgesia infusion is discontinued, all standing orders will be discontinued with the exception of those for vital signs, level of sedation and IV access for 4-12 more hours. All other orders will be obtained from the patient's attending physician. F. The following procedures will be utilized in problem solving 1. If unable to infuse the medication: a. Check from catheter insertion site to analgesia infusion pump for kinks. b. Examine the catheter insertion site for fluid leakage. c. Reposition patient. d. Check analgesia infusion pump for malfunctions. e. Notify Acute Pain Service if problem persists. 2. APS will be notified of the following circumstances: a. Altered mental status and/or sedation rating of 5. b. Oral temperature above 102 F x 4 hours. c. Prior to the administration of any sedatives, hypnotics or opiates which have not been approved by the APS. d. Unrelieved pain and/or side effects. e. Pain at the site of epidural insertion, or in the neck, back or head. f. Redness, edema and/or drainage at the epidural site. g. Analgesia infusion pump problem that cannot be resolved. 3. If a local anesthetic is being infused, the APS should be notified immediately if patient complains of the following: a. Shortness of breath b. Muscle tremors c. Increased anxiety d. Hypotension e. Tinnitus 4
9 f. Or any unusual complaint 4. Criteria for stopping analgesia infusion: a. Respiratory rate < 8 breaths/minute. b. Patient does not arouse (sedation rating of 5). c. Patient is mentally confused or disoriented. d. Patient has a dermatome level of above T4. 5. Notify APS whenever an infusion is stopped. 5
10 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: NURSING PROCEDURE FOR CARING FOR PEDIATRIC PATIENTS RECEIVING EPIDURAL, INTRATHECAL OR CAUDAL ORIGINAL DATE: JULY 1991 ANALGESIA OR NERVE BLOCKADE VIA REVIEW/REVISE: SEPTEMBER 2001 INDWELLING CATHETERS EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To outline nursing responsibilities in administering intermittent, continuous and PCA analgesia with opiate and/or local anesthetic agents via epidural, intrathecal, caudal space or other indwelling catheters to pediatric patients. II. POLICY Nurses will properly follow and monitor infusion procedures for pediatric patients receiving intermittent, continuous, or PCA analgesia with opiate and/or local anesthetic agents via epidural, intrathecal, caudal or other indwelling catheters. All policies and procedures previously noted for patients receiving these modalities apply to pediatric patients as well. This policy addresses only the exceptions or additions. II. PROCEDURE A. Patients under the age of eight years will be monitored with a pulse oximeter until 12 hours after discontinuation of the epidural or as ordered. B. Patients under the age of 6 months, in addition to a pulse oximeter, will also be monitored with a cardiac monitor until 12 hours after discontinuation of the epidural or as ordered. C. IV access must be maintained after the last analgesic bolus or from termination of analgesic therapy for a specified length of time determined on a case per case basis by the APS Attending Physician. D. Any pain assessment tool which is found to be effective for the child to communicate his/her pain may be utilized. Once a successful pain assessment tool has been identified, it should be utilized consistently for this patient's pain assessments. E. In addition to the previously mentioned criteria for stopping the analgesia infusion, pediatric patients with a respiratory rate below the normal rate (as defined by MD's orders or nurse's assessments) and/or a downward trend in O 2 saturation per pulse oximetry, are also criteria for stopping the patient's analgesic infusion. 6
11 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 ANALGESIA CATHETER DISCONNECT REVIEW/REVISE: SEPTEMBER 2001 EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To decrease the likelihood of infection related to analgesia catheter disconnection and to ensure that analgesia infusion is continued. II. POLICY Nurses will cleanse and reconnect analgesia catheters disconnected from the hub. III. EQUIPMENT A. Betadine swabs B. Sterile epidural catheter hub (obtained from the APS). C. Sterile scissors D. Tubing set - optional E. Sterile 2x2's or sterile needle IV. PROCEDURE A. Remove old hub from analgesia infusion pump tubing. B. Wrap the exposed end of the analgesia infusion pump tubing in a sterile 2x2 or cap with a sterile needle. (Analgesia infusion pump tubing only needs to be changed if it was contaminated.) C. Scrub approximately 2 inches of the exposed end of the epidural catheter with Betadine swabs x 2. Do not use alcohol. D. Allow to air dry. E. Cut approximately 1 1/2-2 inches off the end of the epidural catheter using sterile scissors. F. Replace hub. G. Insert epidural catheter into the hub and secure it by tightening the clamp. H. Attach analgesia infusion pump tubing to luer lock connector of hub and resume infusion. 7
12 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: TRANSPORTING/TRANSFERRING PATIENTS ORIGINAL DATE: JULY 1991 RECEIVING ANALGESIA VIA EPIDURAL, INTRATHECAL, REVIEW/REVISE: SEPTEMBER 2001 CAUDAL OR OTHER INDWELLING CATHETERS EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To safely transport or transfer patients receiving analgesia via epidural, intrathecal, caudal or other indwelling catheters. II. POLICY Nurses will ensure that proper procedures are followed prior to transporting/transferring patients receiving analgesia via epidural, intrathecal, caudal or other indwelling catheters. III. PROCEDURE A. Patients receiving these analgesic modalities may be transported from one location to another within MCV Hospitals without a nurse in attendance unless the following conditions exist: 1. The patient has received a bolus within the last hour. 2. The patient's respiratory rate is less than 12 breaths/min. 3. The patient's level of sedation is a 4 or The patient's dermatome level (if applicable) is T4 or above. 5. The nurse/physician assesses the patient as not stable. B. Prior to transporting/transferring a patient from one location to another, the nurse caring for the patient will: 1. Obtain a full set of vital signs. 2. Assess level of sedation and pain level. 3. Assess dermatome level (if applicable). 4. Ensure analgesia infusion pump is set correctly and functioning properly and has an adequate volume of medication. 5. Document findings on the Pain Management Flowsheet. C. If the patient is being transferred from one unit to another the nurse caring for the patient prior to transfer will give a full report to the accepting nurse. D. If the patient is transferred to a diagnostic testing area, the accepting staff member is to immediately notify the patient's primary nurse in the patient's unit or the Acute Pain Service in the event of patient discomfort, change in vital signs or level of consciousness, and/or analgesia infusion pump malfunction. E. Transferring nurse will remind accepting nurse or staff member of APS parameters. 8
13 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 REMOVAL OF ANALGESIA CATHETER REVIEW/REVISE: SEPTEMBER 2001 EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To safely remove and correctly document the removal of the analgesia catheter after pain management therapy has been discontinued. II. POLICY Acute Pain Service members will remove analgesia catheters. III. EQUIPMENT A. Gloves B. Alcohol Preps C. Band-Aid - optional D. Analgesia Infusion Pump Key E. Pain Management Flowsheet IV. PROCEDURE A. Ensure that the APS has written an order to remove the analgesia catheter. B. If an epidural or intrathecal catheter, ask patient to assume sitting or side-lying position with back exposed and arched out. C. If analgesia infusion pump is infusing, take final volume readings then unlock analgesia infusion pump, press OFF twice within one second to stop infusion, then re-lock analgesia infusion pump. D. Put on gloves. E. Gently remove tape to expose catheter site. F. Apply gentle, steady traction to remove catheter. An epidural or intrathecal catheter will be easier to remove if patient continues to assume the arched back position. Do not pull on catheter vigorously; if resistance is met, stop and notify the APS attending. G. After removal, check the tip of the catheter for the presence of a blue mark indicating that the catheter is intact. If the blue mark is absent, save the catheter and notify the APS attending. H. Epidural catheters are considered hazardous waste. Handle in accordance with established Infection Control Policies and Procedures. I. Cleanse the back of blood and secretions. Cleanse the epidural site with an alcohol prep and cover with a Band- Aid, if needed. 9
14 J. Inform patient of the availability of alternate analgesia upon request. K. Have nurse dispose of opiate as per nursing policy and procedure. L. Documentation: Pain Management Flowsheet: Complete the following information in provided space: Volume of medication given, condition of epidural site, if epidural catheter tip is intact, signature of person removing catheter. M. Notify the Attending Physician of the APS for the following: 1. Difficulty or inability to remove epidural catheter. 2. Patient experiences pain or paresthesia (tingling) during removal. 3. Absence of blue tip on catheter. SAVE THE CATHETER. 4. Epidural site is painful, red, swollen, or draining purulent material. 10
15 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 LOADING THE ANALGESIA INFUSION PUMP REVIEW/REVISE: SEPTEMBER 2001 EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To ensure that infusion tubing and bag containing the ordered drug(s) are loaded correctly and secured for analgesia infusion. II. POLICY A. MCVH currently utilizes the Baxter Ambulatory Pump; therefore, these procedures are specific for this device. B. APS members will perform all activities for epidural catheters that require the authorized analgesia infusion pump security code. C. All medication nurses will be responsible for initiating and maintaining IV PCA per nursing policy and procedure. D. Analgesia infusion pumps containing a Schedule II opiate will remain locked except during initial analgesia infusion pump loading and the changing of the medication bag and/or tubing. E. Pharmacy Services is responsible for delivering opiate analgesic medications to the nursing units. 6. Clinical Engineering is responsible for infusion pumps, 9v battery. 7. All PCA sets will be distributed by materials management via central supply. III. EQUIPMENT A. Analgesia Infusion Pump B. Analgesia Infusion Keys C. Medication D. Epidural - 101" Analgesia infusion pump tubing set - yellow tubing IV PCA - Analgesia infusion Pump air eliminating spike tubing set and anti-reflux Y-set. E. Pain Management Flowsheet IV. PROCEDURE A. Check analgesia infusion bag against the written order for correct drug, drug strength, drug expiration date and bag volume. Note as appropriate, "For Epidural Use Only". B. Turn key counterclockwise and press up on key hole. 11
16 C. Open analgesia infusion pump as you would open a book and lay it on a flat surface. D. To open tubing chamber, locate the small silver tab and push it in the direction of the bag cover. E. Maintaining tubing sterility, place tubing set in tubing chamber by fitting silicone section of tubing into matching grooves in tubing chamber. The tubing should exit the chamber by taking a turn down away from the analgesia infusion pump. The long end of the tubing will go to the patient and the short end to the infusion bag. F. Snap the tubing chamber shut. G. Using aseptic technique, attach the analgesia infusion bag to the short end of the tubing set. H. Place the bag in the bag cover with the medication label facing so that the caregiver can visualize the label with the bag cover closed. I. Close the analgesia infusion pump as you would close a book ensuring the bag and the tubing are not occluded. J. Lock analgesia infusion pump. K. Documentation on Pain Management Flowsheet: 1. Date 2. Time 3. Drug 4. Strength 5. Volume 6. Pain score LOS, vital signs 12
17 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 PRIMING AND PROGRAMMING REVIEW/REVISE: SEPTEMBER 2001 THE ANALGESIA INFUSION PUMP EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To clear air from the infusion tubing prior to connecting to patient and to ensure that the analgesia infusion pump is programmed in accordance with the written order. II. POLICY A. APS members will perform all activities for epidural catheters that require the authorized analgesia infusion pump security code. B. All Epidural infusion prescriptions will be written and programmed in mcg or ml. C. All IV PCA orders will be programmed in MILLIGRAMS, except for fentanyl orders. D. Analgesia infusion pumps containing a Schedule II opiate will remain locked except during initial analgesia infusion pump loading and the changing of the medication bag and/or tubing. III. EQUIPMENT A. Analgesia Infusion Pump B. Analgesia Infusion Pump Key C. Epidural - 101" Analgesia infusion pump tubing set - yellow tubing IV PCA - Analgesia infusion pump air eliminating spike tubing set and anti-reflux Y-set. D. Medication E. Pain Management Flowsheet IV. PROCEDURE - PRIMING *NOTE - NEVER prime tubing while connected to patient. A. Double check analgesia infusion bag against the written order for correct drug, drug strength, drug expiration date and bag volume. Note as appropriate, "For Epidural Use Only". B. Press ON/OFF button once to turn analgesia infusion pump on. C. The pump will read clear of review history, press clear. D. The screen will then show date and time. If correct, press enter. 13
18 *NOTE: Only use security code if also programming analgesia infusion pump. If only changing bag/primary tubing skip to step E. E. Unlock and relock pump.. F. The security code screen will appear in the display (000). G. Press ENTER button once to see prime screen. H. ENSURE PATIENT IS NOT CONNECTED TO TUBING. *NOTE: If using IV PCA, ensure the section of tubing with the anti-reflux valve is connected to the maintenance IV fluid line, NOT the PCA line. I. Press START button once. The analgesia infusion pump will automatically deliver 0.5 ml of fluid, then beep three (3) times and flash the red attention light in the upper left-hand corner of the analgesia infusion pump. Continue to press START in this manner until all tubing is primed. *NOTE: To interrupt priming, press STOP button twice within one second. V. PROCEDURE - PROGRAMMING *NOTE: Only APS team members can program epidural orders. A. After tubing is primed, press ENTER once to see "concentration" screen. This screen should ALWAYS read 0.0 mg/ml. with EPIDURAL analgesia or IV fentanyl PCA. For IV PCA therapy enter appropriate medication concentration in mg/ml. B. Press ENTER to see "dose" screen. Remember: "Dose" is PCA, not Basal! C. Scroll in the "dose" amount. If patient is to receive basal rate only, "dose" amount must read 0.0. If this is the case, press enter key until "basal" screen appears. D. Press ENTER to see "delay" screen. E. Scroll in the number of minutes "delay". F. Press ENTER to see "basal" screen. "Basal" is continuous rate. G. Scroll in the basal rate. If patient is to receive PCA rate only, "basal" must read 0.0. If patient is to receive basal rate only and PCA dose has been set at 0.0, press enter until the "bolus" screen reached. The "one hour limit" will be 0.0. H. Press ENTER to see "one hour limit" screen. I. Scroll in "one hour limit" amount. (1 hour limit = maximum allowed for PCA doses plus the continuous rate). 14
19 J. Press ENTER to see "bolus" screen. K. If a bolus is ordered, scroll in "bolus" amount. "Bolus" will not be given until the START button is pressed. If a bolus is not desired, the screen should read 0.0 and step Q is the next step. Note: Only Pain Service members may bolus epidural patients. L. Programming is complete at this point. Press ENTER as many times as is necessary to review programming for accuracy. M. Connect primed tubing to infusion site using aseptic technique. N. Press START once. If a bolus has been programmed, the "bolus" screen will appear showing the bolus administration as the analgesia infusion pump delivers it. If a bolus has not been programmed, the appropriate mode screen will appear (PCA only will show a large PCA; basal/pca will show a large PCA and a small basal; basal only will show programmed ml or mg/hr). O. To interrupt a bolus, press STOP twice within one second. The remaining amount of the bolus will be erased from the analgesia infusion pump's memory. *NOTE: Remain with patient at all times during bolus administration. Nursing Procedure for bolus must be followed. P. When bolus dose has been given, the analgesia infusion pump will beep three times and flash the red attention light in the upper left-hand corner of the analgesia infusion pump. Q. Press START to start the programmed infusion. The appropriate dose screen will appear (see step N). *NOTE: If patient is receiving PCA therapy, pressing the START button initiates the patient's PCA hour. The patient must wait the programmed delay time before the analgesia infusion pump will administer a PCA dose. R. To stop the infusion at any time, press STOP twice within one second. If the patient would be put at risk if the analgesia infusion pump were accidentally restarted, remove the 9 volt battery (see Battery Change policy and procedure) to stop infusion. The analgesia infusion pump will retain the stored patient history and programming for a set amount of time. S. To restart analgesia infusion pump (if battery was not removed), press START once. T. Check settings with another medication giver by pressing enter through all the screens and document the following on the Pain Management Flowsheet: 1. Concentration 2. PCA dose 3. Delay time 4. Basal infusion 5. 1 hour limit 6. Bolus 7. Pain Score 15
20 8. Vital signs 9. Signature 16
21 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 INFUSION BAG CHANGE REVIEW/REVISE: SEPTEMBER 2001 EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To change epidural/iv PCA analgesia infusion bag. II. POLICY A. RN and LPN medgivers validated in Analgesia Infusion Pump operation may change PCA analgesia bags. Only nurses validated in epidural infusion will change epidural bags. Nurses should insure that an extra bag of ordered medications is always on the patient s unit. B. The Pharmacy Department will supply the epidural analgesia infusion bag to the nursing units. Call the controlled substance vault during the hours of 8:00 a.m.-4:30 p.m. and the Inpatient Pharmacy after 4:30 p.m. for medication bags. III. PROCEDURE A. Unlock analgesia infusion pump with key. Screen should read "UNL" and sound alarm (beeps). NOTE: Whenever pump is unlocked, the PCA delay time resets. B. Press "Silence" one time to silence the alarm. C. Press up on key hole and open analgesia infusion pump as you would open a book. D. Do not open tubing chamber unless tubing needs to be changed. See policy for loading analgesia infusion pump. E. Compare doctor's order to analgesic bag for drug(s) and concentration(s). F. Ensure that the drug has not expired. G. Detach empty bag. H. Attach replacement bag. I. Close analgesia infusion pump as you would close a book. Be sure tubing is not clamped in the door. J. Relock analgesia infusion pump with key. Screen should read "000". K. DO NOT ENTER THE SECURITY CODE. If security code is entered unlock and relock the analgesia infusion pump with the key. Screen should read "000". 17
22 L. Press "ENTER". Screen will read "VOLUME LIMIT". M. Press arrow buttons to enter the amount of the replacement bag (1-250 ml). N. Press "ENTER". Screen should read "PRIME". If priming is needed, press "START". 0.5 ml will be delivered each time the "START" button is pressed. DO NOT PRIME WHILE ATTACHED TO PATIENT. O. Press "ENTER". 1. Screen should read PCA if patient is on PCA with or without basal and rate/hr if patient is on continuous infusion. Analgesia infusion pump is now infusing. P. Document new bag on Pain Management Flowsheet. Q. Have settings checked with second medgiver as per nursing policy. 18
23 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 OBTAINING PATIENT HISTORY FROM REVIEW/REVISE: SEPTEMBER 2001 THE ANALGESIA INFUSION PUMP EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To ensure analgesia infusion pump settings are correct and to determine patient's use of PCA dose in order to make appropriate changes in treatment plan or to reinforce patient teaching if needed. II. POLICY A. Licensed nursing personnel who are validated in analgesia infusion pump operation will obtain and document patient history and analgesia infusion pump programming q4h on the Pain Management Flowsheet. B. For patients receiving basal only, the history consists of the following: residual volume, given volume, and basal rate,. For IV PCA, the rate will be shown as mg/hr (except with IV fentanyl). For epidurals and IV PCA fentanyl, the rate will be shown as ml/hr or mcg/hr. C. For patients receiving basal/pca, the history consists of the following: residual volume, 2 shift totals, given volume, dose, delay, basal rate, 1-hour limit and up to a 24-hour history of doses received and attempted. D. For patients receiving PCA only, the history consists of the following: residual volume, 2 shift totals, given volume, dose, delay, one hour limit and up to 24- hour history of doses received and attempted. E. For patients receiving PCA pain management, the number of doses and attempts will be used to determine ongoing treatment plan. III. PROCEDURE - * NOTE - The key and the security code are not necessary to obtain patient history; however, they are needed to check the programmed drug concentration. A. Do not stop infusion. B. Press the history button repeatedly to see the analgesia infusion pump screen in the following order: 1. Volume limit (residual volume) 2. Shift total (not currently MCV 19
24 3. Volume (given volume) - The analgesia infusion pump will subtract the amount used for priming from the displayed residual volume, but because the priming amount is not actually given to the patient, the analgesia infusion pump will not add it to the displayed given volume. This accounts for the discrepancy in initial bag volume and the final given volume. 4. PCA dose (in PCA or basal/pca modes) 5. Delay (in PCA or basal/pca modes) 6. Basal rate (in basal or basal/pca modes) 7. One hour limit (in PCA or basal/pca modes) 8. Injection/attempt history - reports from the most current hour (or portion of an hour) to the mot distant hour (up to 24 hrs. prior). If the pump is programmed in the continuous mode, this screen will not appear. 9. When all history has been reviewed, the message End of History will be displayed. 10. Press start to restart pump. C. Documentation: 1. The Acute Pain Service will record daily the injections as a previous twelve hour total. 2. Nursing personnel will document analgesia infusion pump settings except injections: attempts on the Pain Management Flowsheet q4h. 20
25 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 BOLUS ADMINISTRATION VIA ANALGESIA INFUSION PUMP EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To safely provide a single dose of analgesia in addition to the amount administered by the programmed prescription. II. POLICY Anesthesiologists or Acute Pain Service members will administer epidural boluses. The Pain Service will notify the patient's nurse that the patient is receiving a bolus. APS personnel will remain with patient during bolus administration and for several minutes thereafter. Only a RN may give a bolus through an analgesia infusion pump delivering intravenous 5q opiates. III. EQUIPMENT A. Analgesia infusion pump Key B. Patient's chart C. Pain Management Flowsheet IV. PROCEDURE A. Obtain physician's order for bolus amount. B. Turn key counterclockwise then clockwise to unlock and relock the analgesia infusion pump. The security code screen will appear (000). C. Scroll in the valid security code. D. Press ENTER as many times as is necessary to see the bolus screen. E. Scroll in bolus amount. F. Press START. Bolus screen will appear showing the bolus administration as the analgesia infusion pump automatically delivers it. Remain with patient during bolus infusion. G. To interrupt a bolus at any time, press STOP twice within one second. The remaining amount of the bolus will be erased from the analgesia infusion pump's memory and will not be given when the START button is pressed to resume infusion. 21
26 H. When the bolus dose has been given, the analgesia infusion pump will emit three (3) beeps and flash red attention light. I. Press START to resume programmed infusion. J. Documentation: Pain Management Flowsheet, Patient's chart 22
27 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1993 ANALGESIA PRESCRIPTION CHANGE REVIEW/REVISE: SEPTEMBER 2001 I. PURPOSE To ensure the infusion of analgesia as ordered in an effort to maximize the patient's experience of comfort and to minimize the patient's experience of side effects. II. POLICY Only Acute Pain Service team members or Anesthesiologists who are knowledgeable in analgesia infusion pump operation will perform prescription changes according to written anesthesiologist's order for epidural analgesia therapy. Staff nurses validated in analgesia infusion pump operation may make prescription changes in IV PCA therapy. The Acute Pain Service is responsible for insuring updated and accurate orders are placed as required in the HIS system. III. EQUIPMENT A. Analgesia infusion pump key B. Pain Management Flowsheet IV. PROCEDURE A. Turn key counterclockwise then clockwise to unlock and relock analgesia infusion pump. B. Scroll in the valid security code. C. Press ENTER as many times as is necessary to see the screen to be changed. *REMEMBER - "Dose" is PCA, not "Basal"! D. Scroll in change according to physician's order. E. Press ENTER until you come to 1-hour limit screen. F. Change according to physician's order. G. Press START to start newly programmed infusion. 23
28 H. Have second medgiver check new program settings. I. Documentation: Pain Management Flowsheet 24
29 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 CONTROLLED SUBSTANCE RECORD KEEPING REVIEW/REVISE: SEPTEMBER 2001 EFFECTIVE DATE: SEPTEMBER 1995 GENERAL POLICIES AND PROCEDURES A. Except during analgesia infusion tubing and bag changes, the analgesia infusion pump containing Schedule II opiates will remain locked. Keys will be kept securely on the nurses' opiate key ring at all times. B. Only physicians, RN's, and RPh's who are knowledgeable in the operation of the analgesia infusion pump will perform the activities that will affect opiate use and waste. C. MCV will use a universal security code for the analgesia infusion pumps. Access to the security code will be limited to health professionals who are knowledgeable in the operation of the analgesia infusion pump. D. Analgesia infusion bags will be prepared in the pharmacy in accordance with the written physician's order and Pharmacy Policies and Procedure. E. All analgesia infusion bags will be labeled with the drug, drug strength, volume, expiration date, and lot #. F. All analgesia infusion bags designated for epidural use will have a yellow label appropriately with "For Epidural Use Only". G. Licensed nursing personnel will order, as needed, standard solution analgesia bags from the pharmacy daily along with the order for other floor stock opiates in accordance with the Pharmacy Controlled Substance Policy. An extra bag of ordered medication should be stocked as well. These bags will be delivered to the floor by a Pharmacy Technician. Licensed nursing personnel will accept and sign the receipt for these bags. The acceptance of these opiates will be added to the Controlled Substance Disposition Log. These bags will be stored in a locked opiate cabinet until needed. H. Replacement bags containing drugs and/or concentrations other than mixtures prepared in bulk quantities by the pharmacy, will be prepared by the pharmacy upon receipt of a written physician's order and will be delivered to the floor by Pharmacy Services where a licensed nursing person will accept, sign a receipt, log the infusion into the Controlled Substance Disposition Log, and store the bag in a locked opiate cabinet in accordance with the Pharmacy Controlled Substance Floater Policy until needed. The signed receipt will serve as documentation of acceptance by nursing personnel of the opiate infusion. 25
30 I. Infusion bags will be signed out to a specific patient on the Controlled Substance Disposition Log. The new bag's volume will be recorded on the patient's bedside Pain Management Flowsheet. J. Licensed nursing personnel will monitor and record the patient's current PCA settings and volumes q4h on the Pain Management Flowsheet. K. Bolus amounts will be accounted for on the Pain Management Flowsheet. L. Any alteration in residual and/or given amounts of drugs will be accounted for on the Pain Management Flowsheet. M. Unused drug remaining in bag after therapy has been discontinued or when infusion bag is changed will be destroyed as per Nursing Policy and Procedure. This "destroyed" amount will be documented on the Pain Management Flowsheet and the back of the Controlled Substance Disposition Log. N. The yellow copy of the Pain Management Flowsheet, along with the Controlled Substance Disposition Log, will be returned to the pharmacy for storage in the Controlled Substance Vault in accordance with Federal Controlled Substance Laws. 26
31 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 NURSING CARE OF PATIENTS RECEIVING REVIEW/REVISE: SEPTEMBER 2001 PCA OR CONTINUOUS SUBCUTANEOUS OPIATES EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To properly follow monitoring and infusion procedures for patients receiving subcutaneous infusions with or without patient controlled analgesia (PCA) for pain management. II. POLICY Only health care professionals verified in analgesia infusion pump operations and inserviced in care of patients receiving opiate analgesia will care for patients receiving subcutaneous infusions/pca for pain control. III. EQUIPMENT A. Ordered opiate B. Analgesia infusion pump C. PCA tubing - do not need anti-reflux Y-connector D. Gloves E. Alcohol wipes F. 2x2's G. Tape H. 25 or 27 gauge butterfly needle or specific sub Q infusion set. III. PROCEDURE A. Set up infusion device with ordered medication (see pages 12-23). B. Determine site of SQ infusion/pca which may include: thighs, chest, abdomen, and the upper arms. C. Put on gloves. D. Wipe the insertion site with an alcohol swab and let air dry. 27
32 IV. NOTE E. Insert the butterfly needle (25 or 27 gauge) into subcutaneous tissues, using a degree angle with the bevel down. If using subcutaneous infusion set insert the set at a 90 degree angle. F. Tape the needle securely in place. G. Apply sterile dressing. H. Initiate infusion. I. Change needle q 3 days and as needed. J. Monitor subcutaneous site q shift for signs of infection or discomfort. A. Subcutaneous infusions should be initiated and maintained with the least amount of volume possible to avoid infusing more than 2.5 cc/hr. B. If an infusion of greater than 2.5 cc/hr is required to maintain patient's comfort, change the concentration of the opiate or change the opiate (i.e., from morphine to hydromorphone). C. The PCA dose interval should be increased to minutes as absorption will not be as rapid as IV PCA. 28
33 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 APPLICATION AND DESTRUCTION OF REVIEW/REVISE: SEPTEMBER 2001 FENTANYL TRANSDERMAL PATCHES EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To safely provide transdermal fentanyl administration. II. POLICY Only licensed nursing personnel will apply and/or destroy fentanyl transdermal patches. III. PROCEDURE A. Fentanyl transdermal patches will be applied by a licensed nurse as ordered. B. Fentanyl transdermal patches will be applied to the trunk area (front or back) only. Do not apply to freshly shaved regions; body hair should be clipped, not shaved, if necessary. C. The date of fentanyl patch application will be indicated on/near the patch in a way not to obscure the dosage strength of the patch. D. If an order for a new patch strength is initiated before the old patch was scheduled to be removed, the new strength patch will be applied while removing the old strength patch at the same time. E. Discard fentanyl transdermal patches in the same manner as hazardous waste. F. Nurses will document destruction of fentanyl patches per the Controlled Substance Policy on the back of the Controlled Substance Disposition Log. H. Note: Fentanyl patch has increased absorbtion with fevers and has been shown not to last 72 hours in a small population of patients. 29
34 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: NURSING CARE OF THE PATIENT RECEIVING ORIGINAL DATE: JULY 1991 TENS (TRANSCUTANEOUS ELECTRICAL REVIEW/REVISE: SEPTEMBER 2001 NERVE STIMULATION) EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To assure proper care of patients receiving transcutaneous electrical nerve stimulation (TENS) therapy. II. POLICY Nurses will assist in caring for patients receiving TENS therapy as a form of pain control. III. PROCEDURE A. Assess that the TENS unit leads are connected to the electrodes and stimulator every shift. B. Assess the battery function every shift and replace batteries as needed. The TENS unit's light will blink when functioning properly. C. Assess the patient's pain relief from the TENS unit every shift. D. Notify physical therapy if TENS appears ineffective or if the patient has problems, complaints or concerns as related to this form of therapy. E. Assess the skin condition under the electrodes every twelve hours to determine if irritation or rash is present. This is done by lifting a corner of the electrode and assessing the skin's condition. F. Patients and/or nurses may adjust the TENS unit intensity knobs to obtain an increased level of comfort. G. Nurses may replace electrodes to a similar location on the patients skin if they become detached. Wash and dry skin prior to replacement. H. Review the TENS troubleshooting sheet (in appendix) and the physical therapist's notes in patient's chart as needed for further information. I. The physical therapist should place extra electrodes and batteries in a visible place at the patient's bedside. 30
35 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 MONITORING PATIENTS WITH SPINAL CORD REVIEW/REVISE: SEPTEMBER 2001 STIMULATION (SCS) EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To properly monitor patients with SCS. II. POLICY Only nurses and physicians trained in SCS will make changes to SCS parameters. III. ASSESSMENT OF PATIENTS RECEIVING SCS A. Patients incision sites will be assessed for redness, swelling, drainage and tenderness every shift. B. Call implanting service is fever over 102 F x 4 hours or if the patient complains of severe headache, neck pain, back discomfort and/or loss of bladder or bowel control. C. The patient may turn the SCS on/off and may adjust the rate and amplitude as needed. 31
36 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: JULY 1991 MONITORING PATIENTS WITH A LONG TERM REVIEW/REVISE: SEPTEMBER 2001 IMPLANTED CATHETER FOR ANALGESIA EFFECTIVE DATE: SEPTEMBER 1995 I. PURPOSE To properly monitor patients with a newly implanted port, catheter, or pump. II. POLICY Only nurses and physicians trained in programming pumps will make dosage changes. III. ASSESSMENT OF PATIENTS A. Respiratory rate and level of sedation will be checked q1h x 12 then q4h. B. No opiates, sedatives or hypnotics will be administered without first consulting the implanting service. C. Patient data will be recorded on the appropriate bedside flowsheet. D. If the respiratory rate is < 8 breaths/minute and/or the patient not arousable, call the implanting service and administer naloxone as ordered. E. Record level of analgesia (0-10 verbal pain scale) q4h while awake. F. A running IV is mandatory during the first 12 hours and may then be switched to IV access (i.e., saline/heparin lock) while patient is hospitalized. G. Patients surgical incisions should be assessed q shift for redness, swelling, drainage, or tenderness. Call implanting service with problems. H. Call implanting service is temperature is over 102 F x 4 hours or if patient complains of severe headache, neck pain or back discomfort. I. Call implanting service if patient complains of urinary retention, loss of bowel or bladder control or lower extremity weakness. J. If local anesthetics are being infused, monitor dermatome level q 4 hours or as ordered. 32
37 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: MARCH 1996 REFILL PROCEDURE FOR A MEDTRONIC REVIEW/REVISE: MARCH 2001 SYNCHROMED PUMP EFFECTIVE DATE: MARCH PURPOSE To outline the correct procedure for refilling a Medtronic SynchroMed Pump. II. POLICY Only nurses and physicians trained in filling and programming the group will access the reservoir. III. EQUIPMENT 1. Povidone-iodine swabs 2. Sterile gloves 3. Medtronic SynchroMed Refill Kit 4. Medtronic SynchroMed Programmer 5. Sterile 20ml syringe containing 18ml of the prescribed medication IV. PROCEDURE 1. Wash hands. 2. Perform telemetry to check pump status. 3. Program the appropriate new parameters, i.e., reservoir volume, prescription medication, etc. 4. Verify new parameter settings with a nurse or physician familiar with the SynchroMed pump. 5. Open refill kit. 6. Cleanse the pump area with three (3) povidone-iodine swabs starting from the center of the pump and working outwards. 7. Put on sterile gloves. 8. Place fenestrated drape exposing pump site. 9. Assemble extension tubing set (close pump), non-coring needle and empty 20ml syringe. 33
38 10. Place template over pump aligning the edges of the templates with the edges of the pump. 11. Insert the non-coring needle through the pump s center septum until the needle touches the needle stop. 12. Open the clamp. 13. Withdraw the fluid from the reservoir using gentle negative pressure. Empty the reservoir completely until air bubbles are present in the extension tubing. The amount withdrawn should approximately equal the reservoir volume indicated on the initial pump status. 14. Close the clamp and remove the 20ml syringe. 15. Attach the pressure monitor and filter to the medication syringe. Turn the pressure monitor stopcock to shut off fluid to the monitor tubing. Purge all air from the filter and the monitor. 16. Attach the syring/filter/pressure monitor to the extension tubing. 17. Open clamp and slowly (1ml/3 secs). Inject the fluid into the reservoir. Do not force the injection. 18. When filling is complete, maintain pressure on the syringe plunger and turn the pressure monitor stopcock off the syringe. 19. Release syringe plunger and check the position of the fluid meniscus in the pressure monitor. Top of meniscus must be below the indicated mark. If the meniscus is higher than the mark, the pump must be completely emptied and fill again (steps H through R). 20. Close the tubing pump. 21. Carefully remove the needle from the pump. 22. Apply pressure and dressing to needle site if desired. 23. Using telemetry, update pump with the previously entered parameters. Note: Programmer printouts may fade with time. To ensure long-term legibility, photocopy printouts and include them in the patient s permanent record. 10. Document in the patient s record the following information: 1. Date 2. Time 3. Old parameters 4. Pump s residual volume 34
39 5. New parameters 6. Next refill date 7. How patient tolerated procedure 8. Condition of pump site 35
40 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE POLICY AND PROCEDURE MANUAL SUBJECT: ORIGINAL DATE: MARCH 1996 PARAMETER CHANGES TO MEDTRONIC SYNCHROMED REVIEW/REVISE: MARCH 2001 PUMP EFFECTIVE DATE: MARCH PURPOSE To properly change medication parameters so that the patient receives optimum analgesia. 13. POLICY Only nurses and physicians properly trained in the Medtronic SynchroMed Pump orientation will make changes. 14. EQUIPMENT Medtronic SynchroMed Programmer. 15. PROCEDURE A. Perform telemetry to check pump status. 1. Program the appropriate new parameters, i.e., mode and/or rate of infusion, alarms, etc., per physicians orders. 2. Confirm new parameters with a nurse or physician knowledgeable with the SynchroMed pump. 3. Perform telemetry to update pump. Note: Programmer printouts may fade with time. To ensure long-term legibility, photocopy printouts and include those copies in the patient s record. 4. Document the following in the patient s medical record: 1. Date 2. Time 3. Old parameters 4. New parameters 5. New refill date 36
41 EPIDURAL ANALGESIA Epidural analgesia is a method of pain control where opiates and/or dilute anesthetics are administered into the epidural space. The rationale for using epidural analgesia is to deliver small but adequate amounts of medications near the spinal cord to stop the transmission of pain. Patients will typically experience a greater degree of pain relief and note less sedation with epidural analgesia. Some studies describe earlier hospital discharge due to patients' increased activity because of decreased pain. I. The Epidural Space A. A space located between the ligamentum flavum and the spinal dura mater. It extends from the cranium to the sacrum containing loose connective tissue, fat, arterial and venous plexus, lymphatics, and spinal nerve roots. It is a functional pad around the spinal cord. B. Spinal cord level for epidural analgesia administration is determined by the level of dermatomes and neurotomes involved in the pain sensation. Picture reprinted with Permission: Ostheimer, GW MD Manual of Obstetric Anesthesia, Churchill Livingstone, New York, 1992 II. Mechanisms of Action of Epidural Analgesia A. Epidural opiates inhibits afferent pain conduction at opiate receptors primarily located in the dorsal horn gray matter of the spinal cord. B. With continuous epidural opiates, there is some vascular uptake leading to some systemic effect, especially with lipophilic opiates. C. May affect nerves traversing the epidural space. D. May diffuse across the meninges and anesthetize the cord. III. Drugs Used in Epidural Analgesia A. Fentanyl (Sublimaze ) 1. Opiate analgesic 2. High lipid solubility (quickly absorbed with little migration) 3. Onset of action minutes. 4. Analgesic effect lasts 4-6 hours. i
42 5. Usual MCVH concentration 20 µg/cc. alone, or 5 µg/cc with local anesthetic. B. Morphine Preservative Free (Duramorph ) 1. Opiate analgesic 2. Low lipid solubility (slowly absorbed, spreads within the epidural space). 3. Onset of action minutes after administration. 4. Analgesic effect may last up to 24 hours. 5. Usual MCVH concentration 0.2mg/cc with or without local anesthetic C. Bupivacaine (Marcaine ) 1. Local anesthetic 2. Blocks pain transmission in the spinal nerves. 3. Is often used with an opiate 4. Usual MCVH concentrations are % and 0.125%. IV. Potential Side Effects of Medications Administered Epidurally A. Respiratory depression is the side effect produced by all opiates which raises the greatest concern. The incidence of this effect is less than 1%. 1. Patients at greater risk for respiratory depression are patients who: a. Are above 65 years of age. b. Have an epidural with thoracic or cervical placement. c. Have a history of impaired respiratory function. d. Receive systemic opiates in conjunction with epidural opiates. e. Receive relatively higher doses of epidural opiates. f. Receive opiates or other sedative hypnotic medications after surgery. 2. Phases of Respiratory Depression a. Local anesthetics i. Immediate - secondary to inadvertent spinal injection which could potentially paralyze the diaphragm. ii. Late - Due to slow rostral spread to cervical levels which could impair respiratory effort b. Opiates i. Early - opiates may absorb into the vascular system to travel to the brain and exert a depressive effect on the respiratory center. Also, early respiratory depression may occur due to inadvertent spinal or vascular injection of epidural doses of opiates. ii. Late - due to slow rostral spread of opiates within the CSF to the respiratory centers of the brain. ii
43 3. Monitoring for Respiratory Depression a. Usually, respiratory depression is preceded by increased sedation in adults. Monitoring of the patients' level of sedation is the most reliable measure of the rostral spread of the drug toward the respiratory center. The sedation rating scale: Level of Sedation (LOS) is used to evaluate a patient's course: 1. Alert 2. Intermittently drowsy 3. Frequently drowsy 4. Asleep, easy to arouse 5. Somnolent, difficult to arouse b. If a patient becomes difficult to arouse or has difficulty in remaining awake, notify the Acute Pain Service. Monitor respiratory rate closely. Prompt recognition of increasing sedation can avoid periods of hypoxia for the patient. If you are unable to arouse the patient or the respiratory rate has dropped to 8 breaths per minute or below for adults, or the respiratory rate as specified by physician's orders for children, administer the naloxone as ordered and notify the Acute Pain Service. It is imperative that patients receiving epidural analgesia receive NO other opiate, hypnotic or sedative unless the APS is notified. Patients with an epidural catheter should have signs clearly placed "No opiates, hypnotics or sedatives without contacting APS". B Nausea/vomiting C. Pruritus (itching) D Urinary retention E. Hypotension Bupivacaine is a local anesthetic that blocks the sympathetic nervous system impulses. One side effect of local anesthetics is hypotension, especially postural hypotension. The patient's BP will need to be monitored supine and sitting before assisting the patient out of bed. If a BP reading difference is greater than 20 mmhg systolic, do not allow the patient out of bed and notify the APS. F. Sensory/Motor block Bupivacaine can cause a loss of sensory and/or motor function. Therefore, dermatomes are checked every four hours to determine whether the local anesthetic is spreading and potentially anesthetizing the respiratory muscles. iii
44 To check dermatome level, gently wipe an alcohol swab across the patient's skin. Start with the legs and move up towards the lower ribs. Continue upward until patient notes the change in sensation (cool swab feels warm). Record the dermatome level on the Pain Management Flowsheet. If it is above the nipple line (T-4) promptly notify the APS. Test bilaterally. G. CNS Stimulation Another potential side effect of bupivacaine is CNS stimulation. This stimulation is caused by inadvertent vascular uptake of the drug. Patient complaints of restlessness, anxiety, tremors, or shivering represent possible CNS toxicity and must be promptly reported to APS. H. Bradycardia Bradycardia, while rare, may occur with local anesthetics. If heart rate becomes bradycardic and the patient is receiving epidural local anesthetics, contact the APS. V. Drug Used to Reverse the Adverse Effects of Epidural Analgesics A. Naloxone HCL (Narcan ) 1. Naloxone is a drug that competes for the opiate receptor, therefore, known as an opiate antagonist. This drug displaces an opiate drug, such as fentanyl or morphine, from its receptor site. 2. Naloxone can be given to diminish the effects of opiate overdosage. It may also be used in low doses to decrease or eliminate troublesome side effects such as urinary retention, itching, nausea, and vomiting without decreasing analgesia. This is usually obtained by initiating a low dose continuous infusion of naloxone and titrating to effect. The administration of naloxone may also reverse pain control, depending on the dosage used. 3. When naloxone is utilized for respiratory depression or oversedation, remember it has a short duration of minutes, so a continuous infusion or repeated bolus doses may be required. Naloxone does not reverse the side effects of local anesthetics. 4. Administered IV - may also be given IM or SQ. DO NOT GIVE IN EPIDURAL SPACE. 5. Onset of action is 2-5 minutes when given IV. B. Ephedrine 1. Used for the reversal of hypotension caused by local anesthetics 2. Administered IV 3. Onset of Action 1-2 minutes 4. Given only by Anesthesiologist iv
45 VI. Pain Management Flowsheet There is a flowsheet for patients receiving epidural analgesia. This sheet serves to remind the nurse of the frequency of the required observations and gives a space for recording the nurse's findings. APS orders are to be continued after catheter is discontinued for 4 hours after fentanyl with or without local anesthetic and for 12 hours with morphine with or without local anesthetic. Refer to the following table for charting requirements: Q 1 HOUR Q 4 HOURS Q SHIFT Respiratory Rate x 4 Hours for Fentanyl x 12 Hours for Morphine Level of Sedation x 4 Hours for Fentanyl x 12 Hours for Morphine Respiratory Rate Level of Sedation Pump Setting Verification Pain Ratings (while awake) Side Effects Dermatomes (with local anesthetics only) Blood Pressure (with local anesthetics only) Pulse (with local anesthetics only) Dressing/Site If an opiate (if > 50 µg of fentanyl) or local anesthetic bolus is given : Need to perform full set of vital signs (except temperature): q5 minutes x 2, then q15 minutes x 2, then return to previous schedule v
46 Flowsheet CONTINUOUS, INTERMITTENT ANALGESIA VIA EPIDURAL, INTRATHECAL, CAUDAL OR OTHER INDWELLING CATHETERS STANDARD ROUTINE CARE The rationale for using epidural, intrathecal, or caudal analgesia is to deliver small but adequate amounts of opiates and or other analgesics near the spinal cord to stop the transmission of pain. As all opiates work to relieve pain within the dorsal horn, smaller doses of opiates are needed via this route as it is a more direct delivery method. Patients will typically achieve a greater degree of pain relief and note less sedation with these modalities. NURSING DIAGNOSIS EXPECTED OUTCOME NURSING ACTIONS 1. Potential problems associated with administering local anesthetics epidurally, intrathecally, caudally or via other indwelling catheters. Potential impaired mobility and impaired sensation Early recognition of motor/sensory loss, i.e., patient is able to ambulate. Monitor dermatome level as ordered. Call APS immediately if dermatome level above T4 Check patient's movement and sensation Q4H and report any loss to APS. Place patient on fall precautions. Encourage ambulation with assistance. Potential hypotension Early recognition of hypotension, i.e., BP within expected range After bolus injection, observe patient, recording BP Q5 minutes x2, then Q15 minutes x 2, then return to previous schedule. During infusion, BP as ordered. Call APS when significant drop in BP. Stop infusion. Prepare fluid bolus according to doctor's order. Have vasoconstrictor drug (Ephedrine 10 mg) on hand for doctor to administer. Encourage slow progression to sitting/standing position to avoid postural hypotension. Potential bradycardia Early recognition of bradycardia, i.e., pulse should be over 60 bpm. After bolus injection, check pulse Q 5 minutes x 2, then Q 15 minutes x 2, then return to previous schedule. Call APS if bradycardia occurs. Monitor BP for hypotension. Have Atropine on hand for the doctor to administer if bradycardia severe. 2. Potential problems associated with administering opiates epidurally, intrathecally, caudally or via other indwelling catheters. Early recognition of altered respiratory status. Place sign over head of bed stating patient has analgesia catheter. Notify APS with questions or problems. Maintain patent IV access at all times during epidural, intrathecal or caudal infusion and 4-12 hours after catheter is removed. vi
47 NURSING DIAGNOSIS EXPECTED OUTCOME NURSING ACTIONS Potential impaired gas exchange Respiratory rate within normal limits. Respiratory volume within normal limits Patient will remain at same LOS as prior to these therapies. DO NOT combine epidural, intrathecal or caudal opiates with parenteral opiates. Notify APS if respiratory rate drops below 8 per minute in adults, if patients complains of SOB, if patient's color deteriorates (i.e., dusky, cyanotic), or if patient difficult to arose. Keep naloxone (Narcan ) 400 µg on hand to be given by the doctor in the event of severe respiratory depression. Children under 8 years of age will be placed on pulse oximeter. Children under 6 months of age will be placed on pulse oximeter and cardiac monitor. Monitor respiratory rate/depth as ordered Follow cardiac arrest procedures in the event of respiratory arrest. Place sign at head of bed: "Administer no hypnotics, opiates or sedatives without notifying APS". After bolus injection, (non-pca) observe patient, recording RR, P, LOS, BP q5 x 2 then q15 min x 2, then return to previous assessment schedule. Potential itching related to opiates and/or presence of preservatives in solutions Early recognition of discomfort from itching Reassure patient that this is an effect of the opiate Call APS with severe itching; treat initially with diphenhydramine (Benadryl ) if ordered Anticipate naloxone (Narcan ) low dose infusion Potential fluid volume deficit and/or alterations in nutrition related to nausea and vomiting Early recognition of fluid deficit Follow comfort measure for nausea and vomiting: Antiemetics as ordered K-basin on hand Emotional support Notify APS immediately if nausea and vomiting is persistent and/or patient not tolerating fluids (if ordered) Potential urinary retention related to bladder spasms produced by opiates Early recognition of urinary retention Check urinary output Q4H x 24 then Q shift if urinary catheter is not in place Follow nursing measures to assist patient to void Notify APS if urinary retention persists Monitor intake and output if ordered or if retention is a concern 3. Potential problems with the analgesia catheter Potential inadequate pain control related to: Early recognition of blocked Check for kinks in catheter Document patient comfort level Q4H (use 0-10 verbal pain scale) while awake Check medication bag against physician's order vii
48 NURSING DIAGNOSIS EXPECTED OUTCOME NURSING ACTIONS blocked catheter dislodged catheter leaking around catheter inadequate dose of drug analgesia infusion pump malfunction battery failure empty bag incorrect settings catheter and inadequacy of dose of drug or analgesia infusion pump malfunction Ensure no delay at bag changes, have back-up medication on unit Check analgesia infusion pump history for PCA use Check analgesia infusion pump settings against physician's order Check for low or dead 9-volt battery Notify APS if comfort not achieved Assess patient for change in medical condition Check catheter site Q shift or if alarm on analgesia infusion pump sounds Do not supplement epidural, intrathecal, or caudal analgesia with parenteral opiates, sedatives and hypnotics unless approved by APS Potential pain on injection related to dislodged catheter or meningeal infection Early recognition of dislodged catheter or meningeal infection Notify APS if patient complains of: headache stiff neck pain on bending head forward Notify APS of any pain on injection of PCA dose through catheter or of temperature above 102 o F x 4H Potential infection of the catheter insertion or tunnelling sites possibly related to systemic infection or contamination of catheter or sites Early recognition of redness/swelling or pain at exit or tunnelling sites No increased temperature Notify APS if temp above 102 o F for four hours Maintain aseptic technique when working with analgesia catheter Check site Q shift. Temp Q shift Notify APS of tenderness, redness or purulent drainage at catheter insertion site viii
49 STANDARDS OF CARE FOR THE PATIENT IN PAIN Patrick J. Coyne, RN, CS, MSN, CRNH NURSING DIAGNOSIS: Alteration in Comfort: Pain Pain is perceived as a potential or actual problem by the patient and/or his/her significant other(s). Expected Outcomes * The patient/significant other(s) will understand the current or proposed pain relief plan and assessment technique. * The patient/significant other(s) will readily discuss concerns, questions, or problems as related to pain management. Nursing Actions * Instruct patient/significant other(s) in the current pain control regimen. * Involve/include patient/significant other(s) in discussions related to pain relief options/interventions such as: IV PCA, oral, epidural analgesia, imagery, relaxation, etc. * Answer patients' questions honestly. * Supply educational materials to the patient/significant other(s) as applicable regarding pain relief information. * The patient's complaint of pain will be believed. Accept patient's complaint of pain as valid. * Assess for presence of pain upon admission. If pain is determined to be actual or potential problem, perform a pain assessment every 4 hours or prn. * Record in a consistent manner the pain assessment and pain scores on appropriate flow sheets. * Assess with a standardized measurement tool (0-10 scale or slide algometer). (Various other assessment tools may be utilized if the patient is unable to master the standard tools. * Assess the nature of the patient's pain, a minimum of daily, to include: the quality, quantity, and location. * Patient will obtain/maintain an optimal level of comfort as noted by pain scores and patient's verbalizations as related to pain. * Notify patient's physician if pain relief techniques fail to maintain a pain level below and agreed upon tolerable level. (0-10/slide algometer) * Medications will be changed as appropriate. * Administer analgesic medications as ordered/needed. * Provide appropriate pain medication in a timely manner. * Monitor and evaluate the effectiveness of analgesics and/or interventions. * Medicate patient as appropriate in advance of painful procedures. ix
50 Expected Outcomes * Patient's pain tolerance will be maintained and/or improved as demonstrated by pain scores. Nursing Actions * Assume the patient is in pain if a physiologic etiology exists and patient is unable to communicate his/her complaint. Ask significant others' input regarding their assessment as to whether patient is in pain. * Incorporate adjunct pain relief techniques into the patient's plan of care as applicable (distraction, imagery, heat/cold, relaxation, positioning for comfort, TENS unit, etc.). * Consult appropriate resources as required (dietary, physical therapy, chaplain, clinical nurse specialist). * Insure adequate periods of rest. * Maintain nutritional status. * Maintain safe, relaxing environment. * Maintain adequate analgesia. for * Patient will perform ADLs at optimal level. * Increase patient's activity as ordered/possible to insure adequate pain relief with the activities of daily living. * Instruct and encourage patient to initiate and maintain a pain log or diary if pain is anticipated to persist for an extended duration. * Patient will experience minimal side effects of analgesic therapy. * Monitor for side effects of analgesic therapy such as increased level of sedation, constipation, nausea, vomiting, pruritus, and respiratory depression. * Initiate appropriate interventions to decrease and/or eliminate side effects. * Notify patient's physician of active side effects of analgesic therapy and obtain required interventions. Contact information: Patrick J. Coyne, RN, MSN, CS, CRNH Medical College of Virginia Hospitals P.O. Box Richmond, Virginia (804) x
51 INFUSION PUMP ALARMS OCC = Occlusion: To silence: To clear: EOB = End of Bag: To silence: To clear: UNL = Unlock: To silence: To clear: There is resistance to flow along infusion line. Press "STOP" once. Correct the occlusion (kinked tubing, clamped bag, etc.). Press "START". If occlusion alarms, try: unlocking and opening pump, opening tubing chamber, checking tubing in chamber, closing and locking pump. Press "START". Infusion bag is empty and must be changed. Press "STOP" once. Change infusion bag. Security code is not necessary. Press "ENTER" to pass code screen. Reset volume limit. Press "ENTER". Press "ENTER" to pass priming screen. Pump is now infusing. Infusion pump is unlocked. Press "STOP" once. Lock pump. Press "START". LOBAT = Low Battery: 9-volt battery needs to be changed. To silence: Alarm will sound every 5 minutes for 1 hour. If battery is not changed by that time, alarm will sound continuously and infusion will stop. To clear: Change battery. Press "ON". Press "START". UEA = Unauthorized Entry Attempt: Three incorrect security codes were entered. To silence: Press "STOP" once. To clear: Use key to unlock and lock. Enter correct security code or press "ENTER" to pass code, volume limit, and priming screens. Pump is now infusing. OP = Open: To silence: To clear: ONE HOUR LIMIT: To silence: To clear: Tubing chamber is not properly closed or no tubing is in pump. Press "STOP" once. Unlock and open pump. Open and close tubing chamber door. Lock pump. Press "ENTER" to pass code, volume limit, and prime screens. Pump is now infusing. Patient Demand has exceeded the set ONE HOUR LIMIT. Press "STOP" once. Program in a higher one hour limit or wait out the PCA hour. At the end of the PCA hour, the alarm will sound and basal rate (if programmed) will resume and/or patient may activate the PCA button again. E6: PCA button or patient remote button has been pressed and held down too long. To clear: Press "ON/OFF" once. Press "ON/OFF" again. Press "START" after pump goes through test patterns and screen shows "000". E3, E7, E8, E9, EB, EE, and EU - All should be handled as E6 and patient history, prescription and security code information are retained. No programming is needed. E0, E1, E2, E5, EA, and EP - Patient history, prescription, and security code are not retained. Pump must be reprogrammed by Acute Pain Service if epidural, intrathecal, caudal or other indwelling catheter or by nurse if IV or SQ. Replacement pump may be needed from Inpatient Pharmacy. xi
52 ACUTE PAIN SERVICE - STANDING ORDERS - ADULT Fentanyl Duramorp h Fentanyl or Duramorph with Bupivacaine Pt has epidural catheter. Please call Acute Pain Service (APS) for any questions Please administer no narcotics, sedatives, or hypnotics without first consulting APS, and discontinue all standing such orders. Record all Pt data on appropriate bedside flow sheet Record Resp Q1HR x and then Q HR. Call APS for resp <8/min Q1 x 4 then Q4 Q1 x 12 then Q4 Q1 x 4 then Q4 Q1 x 12 then Q4 If Resp /Min and/or Pt not arousable, call pain on call resident pager and administer Naloxone Record level of consciousness Q1H (If Pt asleep with unchanged resp, nurse may use discretion and not awaken patient) x HR and then Q4H. Call Pain Resident on Call if Pt not arousable x12 x24 x12 x24 Record Degree of analgesia (0-10 visual analogue scale) Q4H while awake If local anesthetics are infused, record level of sensation Q4H. Call APS if above T4 Dermatome level A running, IV is mandatory during first 12 hours and may then be switched to patent IV access (I.E. Saline Lock) while epidural catheter in place Notify APS if temperature > 102 x 4H Check urinary output Q4H x 24H and then Qshift if urinary catheter is not in place. If unable to void after 12H call APS Resident Before ambulating, check for orthostatic hypotension and record BP and pulse. Do not ambulate if >20% decrease in systolic BP or if severe dizziness occurs. If local anesthetic infused, after bolus injection record pulse, BP, level of sedation, and consciousness Q1-2min for 5 min and then Q15min x 2, and then Q4H. If narcotic bolus given, observe Pt for 5 min and record BP & Resp Q1-2min & then, record BP, Resp, & level of consciousness Q15min x 1H and then per normal APS vital sign order All APS orders must be recorded for HR after discontinuing epidural catheter/spinal narcotics. Narcotics, sedatives, or hypnotics must be used with caution during this time. Check with APS for questions Place preprinted epidural catheter sign at head of bed Any problems with epidural catheter or dressing should be addressed to APS nurse pager between 8am and 5pm- other hours call APS resident Patient has received spinal narcotics. Call APS for questions at beeper Only if patient is truly receiving spinal narcotics Only if patient is truly receiving spinal narcotics Only if patient is truly receiving spinal narcotics xii
53 ACUTE PAIN SERVICE - STANDING ORDERS - PEDS Fentanyl Duramorp h Fentanyl or Duramorph with Bupivacaine Pt has epidural catheter. Please call Acute Pain Service (APS) for any questions Please administer no narcotics, sedatives, or hypnotics without first consulting APS, and discontinue all standing such orders. Record all Pt data on appropriate bedside flow sheet Call APS (Digital) if patient appears in pain Place patient on pulse oximeter when receiving epidural/caudal analgesia if 8 years old or younger. Place patient on cardiac monitor and pulse oximeter when receiving epidural/caudal analgesia if 6 months old or younger If RR < /min and or Pt unarousable, call pain resident STAT (Digital) and administer Narcan (Naloxone) MG IV push Should be used on any child 8 Should be used on all children. Use appropriate charts for RR and Narcan dose A running patent IV is mandatory during first 12 hours and may then be switched to patent IV access (I.E. Saline Lock) while epidural catheter is in place All above orders must be recorded for hours after discontinuing epidural catheter, narcotics, sedatives, or hypnotics must be used with caution during this time. Check with APS if questions Place labels at head of bed reading: Patient has epidural catheter. Call APS for questions Problems with pump, batteries, or disposable should be referred to Clinical Engineering. Only if patient has a pump Only if patient has a pump Only if patient has a pump Any problems with epidural catheter or dressing should be addressed to APS nurse pager between 8am and 5pm- other hours call APS resident THE STANDING ORDERS SCREEN FOR ADULTS HAS TO BE USED TO ACCESS THE FOLLOWING TWO ORDERS: Record resp Q1HR x HR and then Q HR. Call APS for resp < 8/min x 4 then Q4 x 12 then Q4 x 4 then Q4 x 12 then Q4 Record level of consciousness Q1H (If Pt asleep with unchanged resp, nurse may use discretion and not awaken patient) x HR and then Q4H. Call Pain Resident on Call if Pt not arousable x 4 x 12 x 4 x 12 xiii
54 ACUTE PAIN SERVICE - AUXILIARY MED ORDERS Naloxone HCL inj (0.mg/ml), 0.2mg, IV push, prn for respirations less than 6/min or Pt unarousable, may repeat x 2 Q15min, if needed. Page anesthesia resident on call STAT (Beeper 1475) Metoclopramide Inj, (10mg/2ml), 10 MG, IV, now, & then Q6H, x 4 doses Metoclopramide 10mg IV piggyback, 0.9% saline, 100 ml, infuse over minutes, now, & the Q6H, x 4 doses Diphenhydramine HCL inj (50mg/ml),, IV, Q6H prn pruritus agitation Diphenhydramine HCL Inj, mg, IV piggyback, in 5% Dextrose, 50ml, infuse over minutes, Q6H prn pruritus, agitations Promethazine HCL inj (25mg/ml),. mg, IV, Q4H, prn N/V Promethazine Inj. mg, IV piggyback, in 5% Dextrose, 50 ml, infuse over minutes, Q4H, prn N/V/ Ketoralac Inj, 30 mg IV piggyback, in 5% Dextrose, 50 ml, infuse over minutes, now and then Q6H x days Ketoralac Inj, 15 mg IV piggyback, in 5% Dextrose, 50 ml, infuse over minutes, now and then Q6H x days Ephedrine Sulf Inj (50mg/ml), 50mg, IV prn severe hypotension, hold on floor for APS Admin only All patients have Narcan ordered You may use your choice of drugs for N/V. Benadryl, 25 mg, is usually ordered for itching. The ICUs use IV, the floors use piggyback. Use appropriate charts for pediatric doses Order if appropriate. ( 55 kgs, 30 mg) Order if appropriate. ( 55 kgs, 15 mg) All patients with bupivacaine have ephedrine ordered Promethazine HCL rectal supp 25mg, 1, rect, Q4-6H, prn N/V 1st select IV line IV line #1 IV line #2 IV line #3 IV line #4 IV line #5 IV line #6 2nd select solution Start Dextrose 5% & water, 250ml Start Sodium Chloride 0.9%, 250ml 3rd Select rate Naloxone 2.5 mg, in each bag/bottle, cont til DC/D used to relieve side effects, ie itching, urinary retention, N/V. drowsiness not relieved by other drugs Prochlorperazine Inj (5mg/ml), 10mg IV, Q4-6, prn N/V Prochlorperazine Inj (5mg/ml), 10mg IV, piggyback, in 5% Dextrose, 50 ml, infuse over 30 minutes, Q4-6, prn N/V Morphine Sulfate, controlled release tab 30 mg,, PO Q8H 30 mg,, PO Q12H Morphine Sulfate, controlled release tab 15 mg,, PO Q8H 15 mg,, PO Q12H Fentanyl Transdermal Patch, (25, 50, 75, 100) mcg/hr apply 1 patch now and then Q3D xiv
55 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE EPIDURAL ANALGESIA WHAT DOES IT MEAN? Epidural analgesia is a common form of pain control that is used nationwide for decreasing and even eliminating the pain that usually follows surgery or other types of chronic pain conditions. Presently, this method of pain relief offers many benefits to you. You deserve as pleasant a recovery period or quality of life as possible, and pain reduction or elimination should be something you expect! WHY HAVE AN EPIDURAL FOR PAIN CONTROL? The vast majority of patients receiving epidural pain control report good satisfaction with this technique. Recent research has shown that some surgical patients with this form of pain control technique actually recover faster, are able to take care of themselves better in the hospital, and go home sooner. When receiving your pain medicine in this manner, you will be more alert because you will receive less opiate medication while experiencing better pain relief. WHAT IS THE EPIDURAL CATHETER? The epidural catheter can be placed in the lower area of your back just in front of your spine. The epidural catheter does not enter your spine. A small amount of opiate (pain medicine) will be infused through this catheter by a small machine and will help decrease the pain that you experience. This form of pain control allows you to receive excellent pain control with less medication. The physician, and anesthesiologist, will place the epidural catheter prior to your surgery. The area on your back will be numbed with some local anesthetic so that all you fell when the catheter is inserted is a little pressure. The physician will make sure that the catheter is positioned correctly, and then it will be taped in place. You will most likely not even realize that you have a catheter in your epidural space. You will be able to walk, bathe, and perform normal activities even with the catheter in place. Normally, the catheter remains in place 3-5 days, or until you can tolerate taking pain medications by mouth. HOW WILL I RECEIVE PAIN MEDICINE? Your physician on the Pain Team will determine the right dose of medicine just for you. The medicine will typically be continuously infusing. If you need more pain medicine, there will be a button available for you to push which will deliver an extra dose of medicine to ensure your comfort. This avoids any delay in receiving the pain medication and possible extra discomfort to you. You control your own pain. All patients who receive epidural analgesia are followed by the Acute Pain Service here at the Medical College of Virginia Hospitals. The Acute Pain Service consists of anesthesiologist, nurses, pharmacists, and physical therapists. A chaplain is also available should you request such a service. The Acute Pain service is available 24 hours a day to ensure your comfort. Your anesthesiologist will explain all the risks and benefits of epidural analgesia. We will be happy to answer any questions you might have concerning this type of pain control. If you have any questions, ask your anesthesiologist or call the Acute Pain Service between 8:00 a.m. and 4:30 p.m. xv
56 MEDICAL COLLEGE OF VIRGINIA HOSPITALS DEPARTMENT OF ANESTHESIOLOGY ACUTE PAIN SERVICE PATIENT CONTROLLED ANALGESIA (PCA) WHAT DOES IT MEAN? When you are sick or have an operation, you may hurt or have pain. Sometimes it hurts to move; sometimes it hurts to breath. While you are in the hospital, we will try our best to help you feel better. Sometimes you may hurt a little and sometimes you may hurt a lot. We will ask you questions so you can tell us how much you hurt. WHAT IS PCA? PCA or Patient Controlled Analgesia is a way of delivering pain medicine. You decide when to take medicine and then push a button. Once you push the button, you will receive a safe dose of pain medicine. WHAT ARE THE BENEFITS OF PCA? Pain medicine given by PCA is quick acting and fully absorbed. This means you need less medicine than if you get pain medicine through shots or injections. You may go home sooner and have fewer problems with PCA. HOW MUCH MEDICINE WILL I GET? Your doctor will decide the right dose for you. The nurses will set a machine for that dose. When you feel pain or discomfort, just push, then let go of the button. The medicine starts working in a few minutes. CAN I GIVE MYSELF TOO MUCH MEDICINE? Built-in timers in the machine prevent you from giving yourself too much. Also, you must let go of the button before you can receive medicine. Remember, since you are the only one who feels the pain, only you may press the button. WILL I GET "HOOKED" ON THE PAIN MEDICINE? Don't worry about getting hooked on the pain medicine. Research studies show that this is very rare -- unless you already have a problem with drug abuse. WHAT DO I DO IF I START FEELING SLEEPY? Pain medicine often makes people feel sleepy. You may want to wait a little longer before your next dose when you feel too drowsy. You will find the right balance between feeling sleepy and relieving pain. WHAT DO I DO IF THE PAIN DOESN'T GO AWAY? If you feel your pain medicine isn't working well enough, tell the nurse. Your nurse will help you get more comfortable and see if there is any problem with your pump and lines. If you notice a problem, let the nurse know. HOW DO I GET PCA? Talk to your doctor or nurse to see if PCA is right for you. Other options are available. However, you receive your pain medicine, the nurses and doctors will make every effort to make you as comfortable as possible. If you have any questions, please ask! You can write your questions below: 1. xvi
57 OPIATE ANALGESIC PHARMACODYNAMICS/PHARMACOKINETICS AND EQUIANALGESIC CONVERSIONS Agent Onset Peak Duration t½ IM / IV PO (min) (min) (hrs) (hrs) (mg) (mg) Codeine Fentanyl (Sublimaze ) 5-15 < N/A Hydromorphone (Dilaudid ) Meperidine 1 (Demerol ) Methadone 2 (Dolophine ) Morphine up to Oxycodone (Percocet ) Sufentanil (Sufenta ) N/A Hydrocodone ND ND N/A ND Dosage frequency for most narcotic analgesics is q3-4h. Doses are based on acute management of severe pain., i.e., postoperative pain. Always use the lowest dose initially to determine patient response and minimize side-effects. Titrate to patient's needs. ND= No Data. 1 2 Consider factors that may predispose patient to seizures from accumulation from normeperidine: doses greater than 1000 mg per day for longer than 24 hours, renal impairment, and history of seizure disorder. Methadone has a long half-life and accumulates over time. Methadone should not be given more frequently than q6h for management of acute pain. Upon accumulation, the dosing interval can be increased to q8h. q12h, or qd. Note: Recent studies demonstrate that methadone may be much more potent than documented above. COMMONLY USED DRUGS WITH ORAL DOSES EQUIANALGESIC TO 650 MG ORAL ASPIRIN OR ACETAMINOPHEN* Pentazocine (Talwin ) 30 mg Codeine 32 mg Meperidine (Demerol ) 50 mg Propoxyphene (Darvon ) 65 mg * From: Hill CS. The NSAIDs: When and why to use then for pain control. Primary Care Handbook: Pain Management, May xvii
58 PEDIATRIC DOSING GUIDELINES Promethazine injection: mg/kg IV every 4-6 hours prn N/V Diphenhydramine injection: 1.25 mg/kg IV q 6 hours prn pruritus/agitation 300 mg max daily dose Naloxone injection: 10 mcg/kg IV for severe respiratory depression If using infusion for side effects of epidural fentanyl: Initial dose of 0.2 mcg/kg/hr & titrate frequently to effect for morphine epidural, 1.0 mcg/kg/hr & titrate to effect Fentanyl Epidural PCA: 0.4 mcg/kg PCA dose 0.5 mcg/kg/hr basal infusion Fentanyl Intermittent Caudal Dosing: 1 mcg/kg (with or in between morphine doses) Morphine Preservative Free for Caudal Dosing: 50 mcg/kg no more frequently than every 8 hr xviii
59 ADJUNCT MEDICATIONS Problem Bone pain Intracranial Pressure Postherpetic neuralgia Nerve compression Intermittent stabbing Gastric/bladder tenesmus Muscle spasm Lymphedema Superficial dysesthesia Nerve Destruction (Deafferentation) Gastric distention Pain & depression Pain & anxiety Intestinal colic Agitation Skin ulceration Stomatitis/mucositis Sedation appetite Trigeminal neuralgia Refractory neuropathic pain Nocturnal leg pain in diabetes Postmastectomy pain Diabetic neuropathy Intractable cancer pain Headache Migraine Headache Dental pain Uterine cramps Treatment options NSAIDs, corticosteroids, pamidronate, strontium-89 Corticosteroids Tricyclic antidepressants, anticonvulsants, topical capsaicin, topical lidocaine, clonidine Corticosteroids, anticonvulsants Anticonvulsants Chlorpromazine Benzodiazepines, baclofen Diuretics, corticosteroids Tricyclic antidepressants, anticonvulsants, capsaicin, corticosteroids Tricyclic antidepressants, anticonvulsants Metoclopramide Tricyclic antidepressants, pemoline Benzodiazepines, phenothiazines Loperamide, scopolamine Benzodiazepines, chlorpromazine NSAIDs, antibiotics, nitrous oxide inhalation or lidocaine aerosol spray for dressing changes Lidocaine viscous or jelly, artificial saliva Methylphenidate, dextroamphetamine Corticosteroids, tricyclic antidepressants, megestrol Anticonvulsants, tricyclic antidepressants, baclofen Clonidine Clonidine Topical capsaicin Topical capsaicin, anticonvulsants, tricyclic antidepressants Epidural bupivacaine, epidural clonidine Acetaminophen, NSAIDs, caffeine Sumatriptan, ergot alkaloids NSAIDs, caffeine NSAIDs, caffeine xix
60 This list is not all inclusive. Dosages for pain management are often varied from the normal doses. xx
61 BIBLIOGRAPHY Acute Pain Management Guideline Panel. Acute Pain Management: Operative or Medical Procedures and Trauma Clinical Practice Guideline. AHCPR Pub. No , Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, U.S. Department of Health and Human Services, Feb American Pain Society: Principles of analgesic use in the treatment of acute pain and cancer pain. 4th Edition. Skokie, IL, American Pain Society, American Pain Society. Sickle Cell Pain Management Guideline 1. Skokie, Ill. American Pain Society, Billings JA. Neuropathic pain. J Palliat Care 1994;10: Breitbart W. Psychiatric management of cancer pain. Cancer 1989;63(11) suppl: Cahill-Wright, Cas. Managing Postoperative Pain. Nursing 1991;91: Coyle N, Adelhardt J, Foley K, and Portenoy R. Character of terminal illness in the advanced cancer patient: Pain and other symptoms during the last four weeks of life. J Pain Symptom Manage 1990;5(2): Coyne P and Ropka M. Pain in Ropka, M. and Williams, A. (eds). HIV: Nursing and Symptoms Management. Philadelphia, PA: Jones and Bartlett, Dalton J and Feurerstein M. Biobehavioral factors in cancer pain. Pain 1988;33(2): Doyle D. Have we looked beyond the physical and psychosocial? J Pain Symptom Manage 1992;7(5): Edwards W. Optimizing opioid treatment of postoperative pain. J Pain Symptom Manage 1990;5(1) suppl:s Foley K and Payne R. Current therapy of pain. Philadelphia: B.C. Decker, Inc Fulk C and Hadley J. Something of pain: New trends in epidural analgesia. J Post Anesth Nurs 1990;5(4): Greenland S. Pain management: a review of the uses of epidural analgesia. Nurs Stand 1995;9: Hegarty A, Portenoy RK. Pharmacotherpy of neuropathic pain. Semin Neurol 1994;14: Jacox A, Carr DB, Payne R, et al. Management of Cancer Pain. Clinical Practice Guideline No. 9. AHCPR Publication No Rockville, MD Agency for Health Care Policy and Research, U.S. Department of Health and Human Services, Public Health Service, March, Littrell RA. Epidural analgesia. Am J Hosp Pharm 1991;48: MacMurren M and Coyne P. Acute Pain Management Service. In McKisson, J. (ed). Manuals of Operating Room Management. Gaithersburg, MD: Aspen Publishers, Chapter 31, p 1-10, Magni G. The use of antidepressants in the treatment of chronic pain. A review of the current evidence. Drugs 1991;42: McCaffey M and Pasero C. Pain: Clinical Manual. St. Louis, MO: The C.V. Mosby Company, McGuire D. Comprehensive and multidimensional assessment and measurement of pain. J Pain Symptom Manage 1992;7(5): McGuire D and Yarbro C (eds). Cancer Pain Management. Orlando, FL:Grune and Stratton, Inc;1987. xxi
62 Melzack R. The tragedy of needless pain. Sci Am 1990;262(2):2-8. Paice J. Unraveling the mystery of pain. Oncol Nurs Forum 1991;18(5): Payne R and Foley K. Cancer Pain. Med Clin North Am 1987;71(2). Spross J. Cancer pain and suffering: Lessons from life, literature and legend. Oncol Nurs Forum 1985;12(4): Spross J, McGuire D, and Schmitt R. Oncology Nursing Society Position Paper on Cancer Pain. Part I. Oncol Nurs Forum 1985;17(4): Spross J, Curtiss C, Coyne P, McGuise and Fink R. Oncology Nursing Security Position: Cancer Pain Management. Oncology Nursing Forum 2 S(S) , Varga C, Graff-Radford S, and Seto B. Management of pain associated with mucositis following bone marrow transplantation. Clin J Pain 1987;3: Wall P. The Prevention of postoperative pain. Pain 1988;33: xxii
A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS
 SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
POSSIBLE NURSING DIAGNOSIS: Pain Potential for Infection / Infection Fluid volume deficit
 1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
1 Procedure for Subcutaneous Over-the-needle Cannula Insertion, Removal, Medication Administration, and Fluid Administration for the Individual in the Home PURPOSE: To provide medication via the subcutaneous
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC
 Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
CADD-legacy PCA pump Model 6300-100ml Cassette
 HOW TO START THE CADD PUMP Press and hold the stop/start button CADD-legacy PCA pump Model 6300-100ml Cassette Three dashes will count down under the STARTING message STOPPED HOW TO STOP THE CADD PUMP
HOW TO START THE CADD PUMP Press and hold the stop/start button CADD-legacy PCA pump Model 6300-100ml Cassette Three dashes will count down under the STARTING message STOPPED HOW TO STOP THE CADD PUMP
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Epidural Management. Policy/Purpose. Scope
 Fluid & Medications Management Policy/Purpose... 1 Scope... 1 Associated documents... 2 General... 2 Epidural Indications... 2 Contra-indications:... 2 Educational requirements... 3 Procedural Considerations...
Fluid & Medications Management Policy/Purpose... 1 Scope... 1 Associated documents... 2 General... 2 Epidural Indications... 2 Contra-indications:... 2 Educational requirements... 3 Procedural Considerations...
VA SAN DIEGO HEALTHCARE SYSTEM MEMORANDUM 118-28 SAN DIEGO, CA
 GUIDELINES FOR PATIENT-CONTROLLED ANALGESIA (PCA) AND PATIENT- CONTROLLED EPIDURAL ANALGESIA (PCEA) FOR ACUTE PAIN MANAGEMENT 1. PURPOSE: To assure the safe and effective use of patient controlled analgesia
GUIDELINES FOR PATIENT-CONTROLLED ANALGESIA (PCA) AND PATIENT- CONTROLLED EPIDURAL ANALGESIA (PCEA) FOR ACUTE PAIN MANAGEMENT 1. PURPOSE: To assure the safe and effective use of patient controlled analgesia
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Procedure for Inotrope Administration in the home
 Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol
 Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol Who Division 1 Registered Nursing staff for the purposes of administering and monitoring of infusion Division 2
Using a Graseby MS26 Syringe Driver for Continuous Subcutaneous Infusions (CSCI) Protocol Who Division 1 Registered Nursing staff for the purposes of administering and monitoring of infusion Division 2
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Cytotoxic and Biotherapies Credentialing Programme Module 6
 Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
Pain Relief during Labour and Delivery: What Are My Options?
 Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Baxter Elastomeric Pumps CLINICIAN GUIDE
 Baxter Elastomeric Pumps CLINICIAN GUIDE Portfolio Overview: Baxter Elastomeric Pumps are non-electronic medication pumps designed to provide ambulatory infusion therapy. Medication is delivered to the
Baxter Elastomeric Pumps CLINICIAN GUIDE Portfolio Overview: Baxter Elastomeric Pumps are non-electronic medication pumps designed to provide ambulatory infusion therapy. Medication is delivered to the
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS
 PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
STANDARDIZED PROCEDURE BONE MARROW ASPIRATION
 I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
SARASOTA MEMORIAL HOSPITAL
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE MANAGEMENT OF PATIENT S OWN INSULIN PUMP/CONTINUOUS SUBCUTANEOUS INSULIN INFUSION PUMP (dia13) DATE: REVIEWED: PAGES: 08/84 10/15 1 of 7 PS1094 ISSUED
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE MANAGEMENT OF PATIENT S OWN INSULIN PUMP/CONTINUOUS SUBCUTANEOUS INSULIN INFUSION PUMP (dia13) DATE: REVIEWED: PAGES: 08/84 10/15 1 of 7 PS1094 ISSUED
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER
 URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
Achieving Independence
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
ATI Skills Modules Checklist for Urinary Catheter Care
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS
 SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
SASKATOON DISTRICT HEALTH Department of Nursing Affairs ADMINISTRATION OF INTRAVENOUS PUSH/DIRECT MEDICATIONS SPECIAL NURSING PROCEDURE LEARNING PACKAGE This package provides the basic information necessary
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
INJECTION TECHNIQUE. IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole
 IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Dehydration and Fluid Therapy Guide
 Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
Dehydration and Fluid Therapy Guide Background: Dehydration occurs when the loss of body fluids (mainly water) exceeds the amount taken in. Fluid loss can be caused by numerous factors such as: fever,
DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358. www.nj.gov/health
 CHRIS CHRISTIE Governor KIM GUADAGNO Lt. Governor Dear Administrator: DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358 www.nj.gov/health January, 2013 MARY E. O DOWD, M.P.H. Commissioner Since
CHRIS CHRISTIE Governor KIM GUADAGNO Lt. Governor Dear Administrator: DEPARTMENT OF HEALTH PO BOX 358 TRENTON, N.J. 08625-0358 www.nj.gov/health January, 2013 MARY E. O DOWD, M.P.H. Commissioner Since
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and
 Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
Carla Duff, CPNP MSN CCRP Clinical Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology Intravenous Subcutaneous IVIg SCIg What should you
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Pain Relief Options for Labor. Providing You with Quality Care, Information and Support
 Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Electronic Medication Administration Record (emar) (For Cerner Sites Only)
 POLICY NO. 1009 Approved: 12/05 Effective: 12/05 Reviewed: 9/10; 5/12 1. Purpose: Electronic Medication Administration Record (emar) (For Cerner Sites Only) To provide direction for the transcription and
POLICY NO. 1009 Approved: 12/05 Effective: 12/05 Reviewed: 9/10; 5/12 1. Purpose: Electronic Medication Administration Record (emar) (For Cerner Sites Only) To provide direction for the transcription and
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
Patient Information. PORT-A-CATH Implantable Venous Access Systems
 Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Patient Information PORT-A-CATH Implantable Venous Access Systems Your doctor has prescribed treatment that requires the frequent administration of medications or other fluids directly into your bloodstream
Appendix L: Accessing/Deaccessing Implanted Central Venous Access Port
 Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
Effective Date: 03/01/2008 Page 1 of 5 Recommendations for Use Insertion Considerations Implanted Port Dressing Access/ Reaccess An implanted port is strongly recommended for patients in whom more than
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Clinical Guideline for: Aseptic Technique
 Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Clinical Guideline for: Technique Summary This guideline provides the principles of, Non Touch, and Clean Techniques to be implemented in the hospital environment. Key Points The essential elements of
Location: Clinical Practice Manual
 Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Purpose: To provide guidelines for the safe administration, proper documentation and auditing of controlled substances by nursing personnel.
 University of Kentucky / UK HealthCare Policy and Procedure Policy # ND14-03 Title/Description: Administration, Documentation, and Auditing of Controlled Substances Purpose: To provide guidelines for the
University of Kentucky / UK HealthCare Policy and Procedure Policy # ND14-03 Title/Description: Administration, Documentation, and Auditing of Controlled Substances Purpose: To provide guidelines for the
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
Your Nerve Block &Home Pump For Arm/Hand Surgery
 Your Nerve Block &Home Pump For Arm/Hand Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 5/10 Why? To Help Control Postoperative Pain at Home A pump connected
Your Nerve Block &Home Pump For Arm/Hand Surgery Department of Anesthesiology and Perioperative Medicine www.happypatient.org Updated 5/10 Why? To Help Control Postoperative Pain at Home A pump connected
To outline nursing management of patients receiving epidural anesthesia during labor (Includes walking epidurals and combined spinal-epidurals).
 HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
Transcutaneous Electrical Nerve Stimulation Device LUMI-TENS
 Transcutaneous Electrical Nerve Stimulation Device LUMI-TENS Operation Manual Read Before Using LUMI-TENS-INS-LAB-RevA08 TABLE OF CONTENTS INTRODUCTION TO TENS INDICATIONS AND CONTRAINDICATIONS WARNINGS
Transcutaneous Electrical Nerve Stimulation Device LUMI-TENS Operation Manual Read Before Using LUMI-TENS-INS-LAB-RevA08 TABLE OF CONTENTS INTRODUCTION TO TENS INDICATIONS AND CONTRAINDICATIONS WARNINGS
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Promoting safer use of injectable medicines
 Promoting safer use of injectable medicines A template standard operating procedure for: prescribing, preparing and administering injectable medicines in clinical areas Introduction The use of injectable
Promoting safer use of injectable medicines A template standard operating procedure for: prescribing, preparing and administering injectable medicines in clinical areas Introduction The use of injectable
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
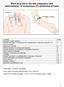 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Caring for Your PleurX Pleural Catheter
 Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
PATIENT URINARY CATHETER PASSPORT
 n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
n PATIENT URINARY CATHETER PASSPORT A guide on how to look after your Catheter NHS Hertfordshire Patient Experience Team Charter House Parkway Welwyn Garden City Hertfordshire AL8 6JL Telephone: 01707
How many hours a day do you need to use the therapy? Introduction. How long will it take to improve your wound? What does PICO do? Will it be painful?
 Patient Information Introduction This patient handbook will provide you with important information while you are receiving negative pressure wound therapy (NPWT) from Smith & Nephew s PICO system. The
Patient Information Introduction This patient handbook will provide you with important information while you are receiving negative pressure wound therapy (NPWT) from Smith & Nephew s PICO system. The
The OmniPod Insulin Management System
 Caregiver GUIDE The OmniPod Insulin Management System The OmniPod is an easy-to-use, two-part insulin delivery system. If you are a school nurse, daycare provider, or other secondary caregiver for someone
Caregiver GUIDE The OmniPod Insulin Management System The OmniPod is an easy-to-use, two-part insulin delivery system. If you are a school nurse, daycare provider, or other secondary caregiver for someone
Pain Management after Surgery Patient Information Booklet
 Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Achieving Independence. A Guide to Self-Catheterization with the Bard Touchless Plus Intermittent Catheter System
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization with the Bard Touchless Plus Intermittent Catheter System Achieving Independence Introducing the Bard Touchless Plus Catheter One
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization with the Bard Touchless Plus Intermittent Catheter System Achieving Independence Introducing the Bard Touchless Plus Catheter One
Patient Instruction Manual
 Patient Instruction Manual Preventice Services, LLC and Preventice Technologies, Inc., are independent, wholly owned subsidiaries of Preventice Solutions, Inc. Welcome to BodyGuardian Verité Your physician
Patient Instruction Manual Preventice Services, LLC and Preventice Technologies, Inc., are independent, wholly owned subsidiaries of Preventice Solutions, Inc. Welcome to BodyGuardian Verité Your physician
IVF CLASS. IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, nicole.l.sobers.ctr@health.
 IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, [email protected] PLEASE NOTE: If you do not have medications for the next
IVF CLASS IVF NURSE CONTACT INFORMATION: Darshana 301-400-2151, [email protected] Nicole 301-400-2146, [email protected] PLEASE NOTE: If you do not have medications for the next
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Emergency Care for Patients of The James
 PATIENT EDUCATION patienteducation.osumc.edu Emergency Care for Patients of The James Emergency Care During and After Treatment Here are guidelines about when and how to report problems that you may have
PATIENT EDUCATION patienteducation.osumc.edu Emergency Care for Patients of The James Emergency Care During and After Treatment Here are guidelines about when and how to report problems that you may have
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
INSULIN INJECTION KNOW-HOW
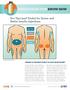 0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Fact Sheet. Caring for and Changing your Supra-Pubic Catheter (SPC) Queensland Spinal Cord Injuries Service
 and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES
 ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
