Vascular access flow reduction for arteriovenous fistula salvage in symptomatic patients with central venous occlusion
|
|
|
- Marion Hubbard
- 7 years ago
- Views:
Transcription
1 Department of Surgery, College of Medicine, University of Oklahoma-Tulsa, Tulsa, OK -USA Department of Surgery, College of Medicine, University of Oklahoma-Tulsa, Tulsa, OK -USA J Vasc Access 2012; 13 ( 2): DOI: /jva ORIGINAL ARTICLE Vascular access flow reduction for arteriovenous fistula salvage in symptomatic patients with central venous occlusion William C. Jennings 1, Gregg A. Miller 2, M. Zachary Coburn 1, C. Anthony Howard 1, Michael A. Lawless 3 1 Department of Surgery, College of Medicine, University of Oklahoma-Tulsa, Tulsa, OK - USA 2 Columbia University, New York, NY - USA 3 St. John Medical Center, Tulsa, OK - USA ABSTRACT Purpose: Vascular access patients with central vein (CV) stenosis or occlusion may have significant symptoms. Treatment is generally by balloon angioplasty, with or without stenting. However, CV lesions may not be correctable and when treated, tend to recur. Surgical bypass of CV obstruction is a major procedure and ligation of the access may leave the patient dependent on catheter dialysis. We review a precision inflow banding procedure to limit vascular access flow and pressure for symptomatic patients with CV obstruction while preserving access functionality. Materials and Methods: All individuals with symptomatic CV occlusive disease who underwent an autogenous vascular access inflow restriction procedure by the two senior authors were identified. All had failed attempts to correct CV lesions by angioplasty and stent placement. A precision banding procedure was used for access inflow reduction with the addition of real-time intravascular flow monitoring. Results: Twenty-two patients were identified. Ages were years (mean=43 years). Nine patients (40.9%) were women, and 8 (36.4%) obese. Mean access flow was 1640 ml/minute before banding decreased to 820 ml/minute after banding (P<.01). All patients had access salvage. Swelling resolved promptly in 20 patients and was markedly improved in two individuals. Three patients underwent aneurysm repair with simultaneous inflow banding and decreased intra-access pressure after flow restriction. Two fistulas failed at eight and 13 months. Mean follow-up was 8 months. Conclusions: The symptoms of hemodialysis vascular access patients associated with non-correctable central venous lesions resolved successfully and their access was maintained using a precision inflow banding procedure. Key words: Angioplasty, Arm swelling, Arteriovenous fistula, AVF, Central venous, Hemodialysis, MILLER Banding, Obstruction, Stenosis, Vascular access Accepted: August 25, 2011 JVA-D R1 INTRODUCTION Central vein (CV) stenosis and occlusion are common problems facing patients undergoing renal replacement therapy by hemodialysis (1). These lesions are generally associated with hemodialysis catheters and are more commonly found in patients with multiple catheters, a history of catheter infections, or long-term catheter use (2). Individuals with central venous disease may be asymptomatic and successfully undergo dialysis on a routine basis with venous outflow provided by multiple collateral vessels (3). In cases where the total cross-sectional area of draining collaterals is insufficient to handle arterialized flow, patients may have significant symptoms with swelling and pain in the affected extremity that may extend to the head, neck, and chest wall or breast. These individuals are often treated successfully by CV angioplasty with or without stent placement; however, the lesions tend to recur (2,4,5). Surgical bypass is less commonly utilized as it is often a major procedure in these patients (6-9). In many symptomatic patients physical findings are consistent with a large, well developed, high flow access with little peripheral access pathology. However, diseased central veins and ensuing symptoms may lead to ligation of an otherwise well functioning access for some patients. Since access sites are limited and contralateral central veins are frequently strictured from prior catheter placement, it is often difficult to establish a new permanent access and patients may become catheter dependent for dialysis access. This study reviews our experience with an arteriovenous fistula (AVF) inflow restriction technique (restoring inflow-outflow balance) that limits access blood flow and pressure while preserving functional fistulas in patients where other methods of treatment were not successful or feasible. 157
2 Vascular access flow reduction for patients with central venous occlusion Our aim in these challenging patients was resolution of symptoms with maintenance of a functional vascular access. Patency in this report refers to functional access cannulation with two needles and the prescribed dialysis flow. Access flow data were analyzed by paired t test using Prism 4 software with statistical significance of differences determined at P=.05. This study was approved by our institutional review board. * GraphPad Software, La Jolla, CA. RESULTS Fig. 1 - Ultrasound image of an arteriovenous fistula (AVF) following inflow restriction (banding). MATERIALS AND METHODS We reviewed the separate databases of consecutive vascular access patients of two senior authors (WCJ and GAM), identifying all individuals who underwent an autogenous vascular access inflow restriction procedure because of CV occlusive disease. Each patient had symptoms and physical findings that warranted access abandonment and ligation if no other option was available. Each patient had similar findings leading to the procedures that included multiple attempts to correct CV stenosis or occlusion by angioplasty and stent(s) placement. All patients had 3+ to 4+ pitting edema, significant discomfort related to pain as well as limited mobility of the affected extremity, and lack of surgical opportunities for correction of the CV lesion without thoracotomy or extra-anatomic (extracavitary) bypass. The inflow-limiting technique (MILLER) reported by Goel, et al. for patients with steal syndrome and by Miller et al. for flow reduction was used with the addition of realtime US flow monitoring, or Transonics intravascular flow monitoring (10,11). Most commonly, a four millimeter angioplasty balloon supplied the restrictive configuration and two adjacent polypropylene sutures were tied over the inflated balloon (banding over the balloon served as a sizing dowel). Ultrasound and physical examination were used to locate a small transverse incision site and establish the restriction point close to the anastomosis, just past the AVF surgical scar, as the vein assumes a superficial location. Figure 1 shows a post-operative ultrasound image with the banding in place. MILLER banding procedures were performed with real time flow volume measurements using ultrasound assessment. Patients with enlarging aneurysms requiring simultaneous repair also had intra-access pressure monitoring during the procedure. Twenty-two patients were identified as meeting the above criteria and represented all individuals undergoing an AVF inflow-limiting procedure for CV stenosis or occlusion treated by the two authors (WCJ n=12, GAM n=10). All patients in this study had an autogenous access with stable function for more than six months. Ages were years (mean=43). Nine patients (40.9%) were women and eight (36.4%) were obese. The cause of end-stage renal disease was diabetes in seven (31.8%) patients and hypertension in nine (40.9%) individuals. Each patient s AVF was dramatically pulsatile prior to treatment. The AVFs treated had fusiform enlargement, and three had expanding aneurysm formation requiring surgical correction. Twelve patients underwent the MILLER banding procedure in the angiogram suite using a 2 cm transverse incision just proximal to the AV fistula anastomosis (3) and 10 were performed using two lateral 0.5 cm incisions coupled with a blind, blunt dissection (11). The veins were uniformly mature and easily dissected free with passage of two interrupted 3-0 polypropylene sutures secured over a 4 mm balloon angioplasty balloon (a 3 mm diameter balloon was used in some instances). Individual demographic data with pre and post-procedure ultrasound flow monitoring values are shown in Table I. One patient did not have access flows measured. The mean pre-banding access flow was 1640 ml/minute (range cc/min) and mean post-banding access flow was 820 ml/minute (range cc/min) (P<.01). Twenty of the 22 AVFs treated remain functional with follow-up of 3 to 24 months (mean=eight months). The three individuals with enlarging aneurysms were treated in the operating room with aneurysm repair and simultaneous inflow banding. Each of these patients had intra-access pressure monitoring before and after banding in addition to ultrasound flow monitoring. Pre-banding mean access pressures were 98, 74, and 38 mmhg for these patients. After banding mean access pressures fell to 63, 41, and 25 mmhg, respectively, while systemic mean arterial pressures remained stable. Vascular access was initially salvaged in all 22 individuals. Swelling resolved promptly in 20 patients and was markedly improved in two individuals. All AVFs were firm and pulsatile prior to banding and these findings 158
3 Jennings et al resolved immediately following the procedure. There were no wound infections, disruptions, hemorrhage, or other complications associated with these procedures. Five patients had swelling prior to banding that involved the neck, face or breast; in all cases these findings resolved post banding. Four patients later had recurrent swelling with symptoms less severe than pre-treatment levels but warranted repeat fistulagrams and central venous imaging. All had intact banding sites. One of these patients underwent repeat angioplasty of collateral outflow veins with improved symptoms and swelling. Another patient had a closed central venous stent that was eventually recannulated and successfully treated by balloon angioplasty and repeat stenting. Two patients had repeat banding 1 cm proximal to the previous band to create additional resistance and flow reduction. One patient died during the study period from causes unrelated to vascular access with a functional AVF. One patient had access thrombosis eight months after banding and the AVF could not be salvaged. A second individual had extensive and gradual aneurysm formation with concern over bleeding risk that resulted in access ligation 13 months after banding. Both of these patients later had new AVFs established in the contralateral extremity. No aneurysms developed proximal to the flow restriction sites. No deaths were related to the vascular access or banding procedures. One individual required placement of a temporary catheter following repair of an associated aneurysm. All other patients had uninterrupted cannulation of their access for hemodialysis. TABLE I - PATIENT DEMOGRAPHIC INFORMATION AND ULTRASOUND MEASURED FLOW VOLUME BEFORE AND AFTER MILLER BANDING. ONE PATIENT DID NOT HAVE ACCESS FLOWS MEASURED. MEAN PRE-BANDING ACCESS FLOW WAS 1640 ML/MINUTE AND MEAN POST-BANDING ACCESS FLOW WAS 820 ML/MINUTE (P<.01). 159
4 Vascular access flow reduction for patients with central venous occlusion DISCUSSION The incidence of CV stenosis or occlusion in hemodialysis patients is substantial. MacRae et al. found 55 of 235 individuals had significant central venous stenosis in their patient population (1). Although patients will most often have a history of CV catheters, some individuals may have symptomatic CV obstruction without a prior catheter placement and in these cases a combination between anatomic variants and turbulent high flow are likely causative agents (12,21). Swelling with associated pain may progress quickly or slowly worsen over many weeks or months as access flow increases and/or outflow collaterals develop intimal hyperplasia and occlude, worsening the inflow-outflow mismatch. Physical findings include arm, neck, head, or breast swelling often associated with vascular access dysfunction in the form of recirculation and unsuitable dialysis, prolonged cannulation site bleeding, etc (2,5,13). Severe edema may increase the risk of lymphatic congestion and cellulitis. Patients may have asymptomatic CV stenosis with venous outflow provided by multiple collateral veins. Levit, et al. found better outcomes in these individuals followed by observation than those treated by intervention with angioplasty (3). Treatment options are summarized in Table II and include observation for asymptomatic individuals or those with only moderate edema and no pain, inflammation, or threatened tissue ischemia. The most common method of treatment for symptomatic CV stenosis or occlusion is by interventional technique; advancing a guidewire through the stenosis or penetrating a short segment of occlusion followed by balloon dilatation. A retrograde or antegrade approach may be utilized, and in difficult lesions, both techniques may be necessary (14). A stent may be placed primarily during the initial treatment or reserved for recurrent or difficult lesions. Various stents have been developed for this purpose, including bare metal TABLE II - OPTIONS FOR TREATMENT OF CENTRAL VENOUS STE- NOSIS OR OCCLUSION IN VASCULAR ACCESS PATIENTS and covered stents. These therapies have a high initial success rate but recurrence or later failure is common, often requiring retreatment (2,4,5,13,15,16). The NKF-K/ DOQI guidelines state Stent placement combined with angioplasty is indicated in elastic central vein stenosis or if a stenosis recurs within a 3 month period. (17). Yevzlin and Asif et al. reviewed available evidence for stent usage and found no conclusive patency benefit for stent insertion compared with angioplasty alone in central venous stenosis (18). Stent placement is costly. Salman and Asif calculated a cost/benefit ratio for general stent placement for dialysis access and found the total cost per patient benefited amounted to $ when accounting for all stents used in each patient (19). Oquzkhurt et al. reported a patient where flow reduction was utilized in the treatment of arm swelling caused by central venous obstruction (12). In the patient reported, flow was reduced from 2900 ml/minute to 720 ml/minute with maintenance of the access and resolution of symptoms (12). Tellioglu, et al. measured access flow with ultrasonography to guide the degree of surgical restrictive banding in patients with highflow vascular access for treatment of cardiac failure and ischemic steal syndrome (20). Miller and Friedman also reported success with flow reduction procedures in the treatment of recurrent cephalic arch stenosis (21). Other studies found AVF flow restriction banding to resolve high output cardiac failure (11,22). Such an inflow limiting procedure may become increasingly important with concerns over a potential risk of higher flow access in dialysis patients with heart disease (23). Brachytherapy has been utilized in CV lesions as an addition to angioplasty and stenting, hoping to extend initial success following stent placement; however, patency was not improved (24). Extrinsic compression may also play a role in symptomatic CV stenosis or occlusions. Itkin et al. felt extrinsic lesions are more likely to require stent placement for success (25). Ahmad reported salvage of arterial venous fistulas with symptomatic swelling because of central venous stenosis by angioplasty of collateral veins (26). In a small subset of patients we experienced success in restoring inflow-outflow balance and achieved symptomatic relief by dilating collateral veins. Surgical treatment has been utilized when feasible with bypass to outflow options such as a patent and non-obstructed basilic, internal jugular or external jugular vein, gaining uninterrupted flow into the central venous system (8,27). More extensive procedures such as bypass to the contralateral jugular, subclavian or axillary vein have been reported (6,7,28). Intrathoracic procedures or femoral extra-anatomic bypass have been reported for access salvage (9,29,30). Among the surgical bypass procedures, Kalra, et al. reported higher success rates 160
5 Jennings et al using autogenous vein bypass as opposed to PTFE in their access patients (8). Dammers, et al. reviewed patients treated by surgery versus angioplasty. Seventyfive percent of those treated with surgical bypass had a patent access at 12-month follow-up as opposed to a 63% success rate in those treated with angioplasty (27). Occasional patients may have moderate flow within a vascular access associated with symptomatic venous hypertension that requires treatment. If significant symptoms are present, such a patient would likely have a marked elevation in AVF venous outflow pressure that may be because of acute collateral outflow thrombosis complicating a chronic CV occlusion. The sudden loss of outflow collateral veins may result in elevated access pressure in spite of a relatively moderate AVF flow volume. For these individuals with moderate or even lower flow AVFs, a restrictive inflow banding procedure may lower pressure in the access outflow, restoring or improving inflow-outflow balance while maintaining adequate blood flow for dialysis. In our opinion, banding an access with flow volume lower than ml/ minute may not be successful. The lowest access flow in the patients treated in this study was 870 ml/min. Monitoring access flow volume during flow restriction procedures should predict a successful outcome and minimize the risk of lowering access flow to the point of AVF dysfunction or thrombosis. In general, the minimum post-banding access flow for AVFs should be approximately 500 ml/min. All of the accesses in this study were mature AVFs. However, one of the authors (GAM) has used the reported banding technique to treat grafts associated with symptomatic steal syndrome, high access flow, and/or significant arm swelling in a limited number of patients (11). The primary patency of banded graft accesses is lower than that of AVFs. However, banding remains an option to consider, particularly in patients where significant collateral outflow is present and graft ligation would be otherwise necessary. Grafts with noncorrectable occluded CV outflow and few collaterals are likely to have recurrent thrombosis and early failure. These accesses are rarely worth attempts at salvage. Banding a graft when the initial access flow is less than 800 ml/min may be problematic. In addition, banding of any access with chronic CV outflow occlusion is not likely to be successful when venous outflow collaterals are notably absent. For those patients where interventional techniques with balloon angioplasty were not successful and a surgical bypass is not anatomically feasible or carries unwarranted risk, ligation with abandonment of the access remains a final option for resolution of symptoms. The number of fistulas or grafts ligated because of venous outflow disease is unknown but it is likely to be a common problem in the United States. We suggest many of these patients may have access salvage and relief of symptoms using the relatively simple banding procedure utilized in this study. The symptoms of vascular access patients associated with central venous lesions resolved successfully and their access was maintained using a precision inflow banding procedure by treating the primary pathology of these AVFs which is high inflow in relation to limited and non-correctable access outflow. When flow through the central veins is impeded by stenosis, occlusion, or anatomic variants, this banding technique restored inflow-outflow balance and decrease pressure within the venous outflow tract, successfully mitigating symptoms while maintaining access patency. Financial support: There was no outside support for this study. It was funded by the University of Oklahoma-Tulsa, College of Medicine, Department of Surgery. Conflict of interest: None of the authors have any proprietary interest related to this manuscript. Meeting presentation: This manuscript has not been presented at any scientific meeting. Informed consent: Informed consent was not required for this study. A HIPAA waiver of consent was obtained from the Institutional Review Board. Address for correspondence: William C. Jennings Department of Surgery University of Oklahoma-Tulsa, College of Medicine 4502 E. 41 st Street Tulsa, OK 74135, USA William-Jennings@ouhsc.edu 161
6 Vascular access flow reduction for patients with central venous occlusion REFERENCES 1. MacRae JM, Ahmed A, Johnson N, Levin A, Kiaii M. Central vein stenosis: a common problem in patients on hemodialysis. ASAIO J. 2005;51(1): Agarwal AK, Patel BM, Haddad NJ. Central vein stenosis: a nephrologist s perspective. Semin Dial. 2007;20(1): Levit RD, Cohen RM, Kwak A, et al. Asymptomatic central venous stenosis in hemodialysis patients. Radiology. 2006;238(3): Epub 2006 Jan Oderich GS, Treiman GS, Schneider P, Bhirangi K. Stent placement for treatment of central and peripheral venous obstruction: a long-term multi-institutional experience. J Vasc Surg. 2000;32(4): Agarwal AK. Central vein stenosis: current concepts. Adv Chronic Kidney Dis. 2009;16(5): Suliman A, Greenburg JI, Angle N. Surgical bypass of symptomatic central venous obstruction for arteriovenous fistula salvage in hemodialysis patients. Ann Vasc Surg. 2008;22(2): Chemla ES, Korrakuti L, Makanjuola D, Chang AR. Vascular access in hemodialysis patients with central venous obstruction or stenosis: one center s experience. Ann Vasc Surg. 2005;19(5): Kalra M, Gloviczki P, Andrews JC, et al. Open surgical and endovascular treatment of superior vena cava syndrome caused by nonmalignant disease. J Vasc Surg. 2003;38(2): Glass C, Maevsky V, Massey T, Illiq K. Subclavian vein to right atrial appendage bypass without sternotomy to maintain arteriovenous access in patients with complete central vein occlusion, a new approach. Ann Vasc Surg. 2009;23(4): Epub 2009 Apr Goel N, Miller GA, Jotwani MC, Licht J, Schur I, Arnold WP. Minimally Invasive Limited Ligation Endoluminal-assisted Revision (MILLER) for treatment of dialysis access-associated steal syndrome. Kidney Int. 2006;70(4): Epub 2006 Jun Miller GA, Goel N, Friedman A, et al. The MILLER banding procedure is an effective method for treating dialysisassociated steal syndrome. Kidney Int. 2010;77(4): Epub 2009 Dec Oguzkurt L, Tercan F, Yildirim S, Torun D. Central venous stenosis in haemodialysis patients without a previous history of catheter placement. Eur J Radiol. 2005;55(2): Epub 2004 Dec Kim YC, Won JY, Choi SY, et al. Percutaneous treatment of central venous stenosis in hemodialysis patients: long-term outcomes. Cardiovasc Intervent Radiol. 2009;32(2): Epub 2009 Feb Altman SD. A practical approach for diagnosis and treatment of central venous stenosis and occlusion. Semin Vasc Surg. 2007;20(3): Aytekin C, Boyvat F, Yagmurdur MC, Moray G, Haberal M. Endovascular stent placement in the treatment of upper extremity central venous obstruction in hemodialysis patients. Eur J Radiol. 2004;49(1): Shoenfeld R, Hermans H, Novick A, et al. Stenting of proximal venous obstructions to maintain hemodialysis access. J Vasc Surg. 1994;19(3): ; discussion National Kidney Foundation-K/DOQI. Clinical Practice Guidelines for Vascular Access: update Am J Kidney Dis. 2001;37(1 Suppl 1):S Yevzlin A, Asif A. Stent placement in hemodialysis access: historical lessons, the state of the art and future directions. Clin J Am Soc Nephrol. 2009;4(5): Epub 2009 Apr Salman L, Asif A. Stent graft for nephrologists: concerns and consensus. Clin J Am Soc Nephrol. 2010;5(7): Epub 2010 May Tellioglu G, Berber I, Kilicoglu G, Seymen P, Kara M, Titiz I. Doppler ultrasonography-guided surgery for high-flow hemodialysis vascular access: preliminary results. Transplant Proc. 2008;40(1): Miller G, Friedman A, Khariton A, Preddie DC, Savransky Y. Access flow reduction and recurrent symptomatic cephalic arch stenosis in brachiocephalic hemodialysis arteriovenous fistulas. J Vasc Access 2010;11(4): Isoda S, Kajiwara H, Kondo J, Matsumoto A. Banding a hemodialysis arteriovenous fistula to decrease blood flow and resolve high output cardiac failure: report of a case. Surg Today. 1994;24(8): Beigi AA, Sadeghi AM, Khosravi AR, Karami M, Masoudpour H. Effects of the arteriovenous fistula on pulmonary artery pressure and cardiac output in patients with chronic renal failure. J Vasc Access 2009;10(3): Kwok PC, Wong KM, Ngan RK, et al. Prevention of recurrent central vein stenosis using endovascular irradiation following stent placement in hemodialysis patients. Cardiovasc Intervent Radiol. 2001;24(6): Epub 2001 Oct Itkin M, Kraus MJ, Trerotola SO. Extrinsic compression of the left innominate vein in hemodialysis patients. J Vasc Interv Radiol. 2004;15(1 Pt 1): Ahmad I. Salvage of arteriovenous fistula by angioplasty of collateral veins establishing a new channel. J Vasc Access. 2007:8(2): Dammers R, de Haan MW, Planken NR, van der Sande FM, Tordoir JH. Central vein obstruction in hemodialysis patients: results of radiological and surgical intervention. Eur J Vasc Endovasc Surg. 2003;26(3): Hernandez DA, Obnial GP, Brown OW, Baciewicz F, Rubin JJ. The use of subclavian-atrial bypass for the treatment of central venous hypertension induced by dialysis access procedures. Abstract: SVS June 12, Boston Mass. 29. Myers JL, Mukherjee D. Bypass graft to the contralateral internal jugular vein for venous outflow obstruction of a functioning hemodialysis access fistula. J Vasc Surg. 2000;32(4): Anaya-Ayala JE, Bellows PH, Ismail N, et al. Surgical management of hemodialysis-related central venous occlusive disease: a treatment algorithm. Ann Vasc Surg. 2011;25(1):
Catheter Reduction Program: Creating the Ideal Vascular Access Culture. Presented by: Diane Peck, RN, CNN
 Catheter Reduction Program: Creating the Ideal Vascular Access Culture Presented by: Diane Peck, RN, CNN Fistula First Initiative The superiority of an AVF over an AVG is an accepted fact. For this reason
Catheter Reduction Program: Creating the Ideal Vascular Access Culture Presented by: Diane Peck, RN, CNN Fistula First Initiative The superiority of an AVF over an AVG is an accepted fact. For this reason
Resection, Reduction, and Revision of Aneurysmal AV Fistulas
 Resection, Reduction, and Revision of Aneurysmal AV Fistulas Patrick R. Cook DO, FACS Timothy G. Canty Jr. MD Robert J. Hye MD, FACS Kaiser Permanente San Diego, CA Aneurysmal AVF Over last decade K-DOQI
Resection, Reduction, and Revision of Aneurysmal AV Fistulas Patrick R. Cook DO, FACS Timothy G. Canty Jr. MD Robert J. Hye MD, FACS Kaiser Permanente San Diego, CA Aneurysmal AVF Over last decade K-DOQI
Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach
 Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach Bao- Thuy D. Hoang, MD 1, Jonathan- Hien Vu, MD 2, Jerry Matteo, MD 3 1 Department of Surgery, University of Florida College of Medicine,
Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach Bao- Thuy D. Hoang, MD 1, Jonathan- Hien Vu, MD 2, Jerry Matteo, MD 3 1 Department of Surgery, University of Florida College of Medicine,
Strategies to Reduce Catheter Use in 2014
 Strategies to Reduce Catheter Use in 2014 Timothy A. Pflederer, MD Chair, Network 10 MRB (I have no commercial affiliations or conflicts of interest to report) Fibrin Sheathing Central Venous Stenosis
Strategies to Reduce Catheter Use in 2014 Timothy A. Pflederer, MD Chair, Network 10 MRB (I have no commercial affiliations or conflicts of interest to report) Fibrin Sheathing Central Venous Stenosis
Tunneled Hemodialysis Catheters: Placement and complications
 Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
James J. Wynn, M.D. Medical College of Georgia
 James J. Wynn, M.D. Medical College of Georgia Early patency Long durability (decades?) Resistance to infection Aesthetically acceptable Early referral to nephrologist Early evaluation to vascular surgeon
James J. Wynn, M.D. Medical College of Georgia Early patency Long durability (decades?) Resistance to infection Aesthetically acceptable Early referral to nephrologist Early evaluation to vascular surgeon
Ultrasound in Vascular Surgery. Torbjørn Dahl
 Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Ultrasound in Vascular Surgery Torbjørn Dahl 1 The field of vascular surgery Veins dilatation and obstruction (varicose veins and valve dysfunction) Arteries dilatation and narrowing (aneurysms and atherosclerosis)
Subclavian Steal Syndrome By Marta Thorup
 Subclavian Steal Syndrome By Marta Thorup Definition Subclavian steal syndrome (SSS), is a constellation of signs and symptoms that arise from retrograde flow of blood in the vertebral artery, due to proximal
Subclavian Steal Syndrome By Marta Thorup Definition Subclavian steal syndrome (SSS), is a constellation of signs and symptoms that arise from retrograde flow of blood in the vertebral artery, due to proximal
Complications of Femoral Catheterization. Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005
 Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
Complications of Femoral Catheterization Daniel Kaufman, MD University Hospital of Brooklyn December 16, 2005 Case Presentation xx yr old female presents with fever, chills, and painful swelling of R groin
Pediatric Hemodialysis Access
 Pediatric Hemodialysis Access Vincent L. Rowe, M.D., FACS Professor of Surgery Division of Vascular Surgery Keck School of Medicine at University of Southern California NO FINANCIAL DISCLOSURES Outline
Pediatric Hemodialysis Access Vincent L. Rowe, M.D., FACS Professor of Surgery Division of Vascular Surgery Keck School of Medicine at University of Southern California NO FINANCIAL DISCLOSURES Outline
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Renal Vascular Access Having a Fistula For Haemodialysis
 Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Renal Vascular Access Having a Fistula For Haemodialysis Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Patient Information Booklet. Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms
 Patient Information Booklet Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms TABLE OF CONTENTS Introduction 1 Glossary 2 Abdominal Aorta 4 Abdominal Aortic Aneurysm 5 Causes 6 Symptoms
Patient Information Booklet Endovascular Stent Grafts: A Treatment for Abdominal Aortic Aneurysms TABLE OF CONTENTS Introduction 1 Glossary 2 Abdominal Aorta 4 Abdominal Aortic Aneurysm 5 Causes 6 Symptoms
Upper Extremity Vein Mapping for Placement of a Dialysis Access
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Vein Mapping for Placement of a Dialysis Access This Guideline was prepared by the Professional Guidelines Subcommittee of the Society
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Vein Mapping for Placement of a Dialysis Access This Guideline was prepared by the Professional Guidelines Subcommittee of the Society
Stenosis Surveillance 2009
 5 Diamond Patient Safety Program Stenosis Surveillance 2009 *This presentation was collaboratively developed by the Mid-Atlantic Renal Coalition (MARC) and the ESRD Network of New England for the 5-Diamond
5 Diamond Patient Safety Program Stenosis Surveillance 2009 *This presentation was collaboratively developed by the Mid-Atlantic Renal Coalition (MARC) and the ESRD Network of New England for the 5-Diamond
Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC
 Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC 2015 Edition All Reimbursement Amounts are Listed at National Rates and Do Not Include the 2% Sequestration
Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Physician / Hospital / ASC 2015 Edition All Reimbursement Amounts are Listed at National Rates and Do Not Include the 2% Sequestration
The Bioresorbable Vascular Stent Dr Albert Ko
 The Bioresorbable Vascular Stent Dr Albert Ko Dr Albert Ko MB BS, FRACP, FCSANZ Interventional/General Cardiologist Ascot Cardiology Symposium 2013 Treatment Goals for Coronary Artery Disease Relieve of
The Bioresorbable Vascular Stent Dr Albert Ko Dr Albert Ko MB BS, FRACP, FCSANZ Interventional/General Cardiologist Ascot Cardiology Symposium 2013 Treatment Goals for Coronary Artery Disease Relieve of
RADIOLOGY 2014 CPT Codes
 RADIOLOGY 2014 CPT Codes Radiology 2014 CPT Codes CMS has issued 36 new procedure codes (one is a radiation therapy code) for CY 2014 that directly pertain to radiology with 26 of those codes the result
RADIOLOGY 2014 CPT Codes Radiology 2014 CPT Codes CMS has issued 36 new procedure codes (one is a radiation therapy code) for CY 2014 that directly pertain to radiology with 26 of those codes the result
Talent Thoracic Stent Graft with THE Xcelerant Delivery System. Expanding the Indications for TEVAR
 Talent Thoracic with THE Xcelerant Delivery System Expanding the Indications for TEVAR Talent Thoracic Precise placement 1 Broad patient applicability 1 Excellent clinical outcomes 1, a + Xcelerant Delivery
Talent Thoracic with THE Xcelerant Delivery System Expanding the Indications for TEVAR Talent Thoracic Precise placement 1 Broad patient applicability 1 Excellent clinical outcomes 1, a + Xcelerant Delivery
EFSUMB EUROPEAN FEDERATION OF SOCIETIES FOR ULTRASOUND IN MEDICINE AND BIOLOGY Building a European Ultrasound Community
 MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 8: Vascular Ultrasound Level 1 Training and Practice Practical training should involve at least two half day ultrasound
MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 8: Vascular Ultrasound Level 1 Training and Practice Practical training should involve at least two half day ultrasound
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis
 Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Flow in hemodialysis grafts after angioplasty: Do radiologic criteria predict success?
 Kidney International, Vol. 59 (2001), pp. 1974 1978 Flow in hemodialysis grafts after angioplasty: Do radiologic criteria predict success? SHUBHADA N. AHYA, DAVID W. WINDUS, and THOMAS M. VESELY Renal
Kidney International, Vol. 59 (2001), pp. 1974 1978 Flow in hemodialysis grafts after angioplasty: Do radiologic criteria predict success? SHUBHADA N. AHYA, DAVID W. WINDUS, and THOMAS M. VESELY Renal
Renovascular Hypertension
 Renovascular Hypertension Philip Stockwell, MD Assistant Professor of Medicine (Clinical) Warren Alpert School of Medicine Cardiology for the Primary Care Provider September 28, 201 Renovascular Hypertension
Renovascular Hypertension Philip Stockwell, MD Assistant Professor of Medicine (Clinical) Warren Alpert School of Medicine Cardiology for the Primary Care Provider September 28, 201 Renovascular Hypertension
Use of Stents and Stent Grafts to Salvage Angioplasty Failures in Patients with Hemodialysis Grafts
 Use of Stents and Stent Grafts to Salvage Angioplasty Failures in Patients with Hemodialysis Grafts Thomas M. Vesely, Mohammed Zaheer Amin, and Thomas Pilgram St. Louis, Missouri ABSTRACT To determine
Use of Stents and Stent Grafts to Salvage Angioplasty Failures in Patients with Hemodialysis Grafts Thomas M. Vesely, Mohammed Zaheer Amin, and Thomas Pilgram St. Louis, Missouri ABSTRACT To determine
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access
 predialysisaccess.qxp_0616 6/29/16 3:58 PM Page 1 AIUM Practice Parameter for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access Parameter developed in collaboration
predialysisaccess.qxp_0616 6/29/16 3:58 PM Page 1 AIUM Practice Parameter for the Performance of Ultrasound Vascular Mapping for Preoperative Planning of Dialysis Access Parameter developed in collaboration
Section 4: Your Vascular Access. What is vascular access?
 Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty
 Round Table: Antithrombotic therapy beyond ACS Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty M. Matsagkas, MD, PhD, EBSQ-Vasc Associate Professor
Round Table: Antithrombotic therapy beyond ACS Antiplatelet and anticoagulation treatment of patients undergoing carotid and peripheral artery angioplasty M. Matsagkas, MD, PhD, EBSQ-Vasc Associate Professor
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis
 Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Department of Nephrology Care of your Fistula Nephrology Department Lower Lane Liverpool L9 7AL Tel:0151-525-5980 Arterio-Venous Fistula or Arterio-Venous Graft for Haemodialysis Haemodialysis access In
Majestic Trial 12 Month Results
 Majestic Trial 12 Month Results S.Müller-Hülsbeck, MD, EBIR, FCIRSE, FICA ACADEMIC HOSPITALS Flensburg of Kiel University Ev.-Luth. Diakonissenanstalt zu Flensburg Knuthstraße 1, 24939 FLENSBURG Dept.
Majestic Trial 12 Month Results S.Müller-Hülsbeck, MD, EBIR, FCIRSE, FICA ACADEMIC HOSPITALS Flensburg of Kiel University Ev.-Luth. Diakonissenanstalt zu Flensburg Knuthstraße 1, 24939 FLENSBURG Dept.
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Objectives. AV Fistula Maturation, Cannulation, and Protection. What are the KDOQI guideline %s for fistula prevalence
 Objectives AV Fistula Maturation, Cannulation, and Protection Lesley C. Dinwiddie MSN, RN, FNP, CNN The learner will be able to: Define AV fistula maturation Describe the nephrology caregivers role in
Objectives AV Fistula Maturation, Cannulation, and Protection Lesley C. Dinwiddie MSN, RN, FNP, CNN The learner will be able to: Define AV fistula maturation Describe the nephrology caregivers role in
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Vascular Technology (VT) Content Outline Anatomy & physiology 20% Cerebrovascular Cerebrovascular normal anatomy Evaluate the cerebrovascular vessels
 Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
Vascular Technology (VT) Content Outline Anatomy & physiology 20% normal anatomy Evaluate the cerebrovascular vessels hemodynamics Evaluate the cerebrovascular vessels for normal perfusion normal anatomy
Spotlight Series: Interventional Radiology. Varicose Veins and Venous Insufficiency
 Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Understanding Your. Hemodialysis. Access Options
 Understanding Your Hemodialysis Access Options aakp American Association of Kidney Patients 3505 E. Frontage Road, Suite 315 Tampa, FL 33607 Toll-Free: 800-749-2257 Fax: 813-636-8122 www.aakp.org Overview
Understanding Your Hemodialysis Access Options aakp American Association of Kidney Patients 3505 E. Frontage Road, Suite 315 Tampa, FL 33607 Toll-Free: 800-749-2257 Fax: 813-636-8122 www.aakp.org Overview
PATIENT INFORMATION BOOKLET
 PATIENT INFORMATION BOOKLET Wingspan Stent System with Gateway PTA Balloon Catheter TABLE OF CONTENTS Definitions... 2 What is the Purpose of This Booklet?... 3 What is an Intracranial Lesion?... 3 Who
PATIENT INFORMATION BOOKLET Wingspan Stent System with Gateway PTA Balloon Catheter TABLE OF CONTENTS Definitions... 2 What is the Purpose of This Booklet?... 3 What is an Intracranial Lesion?... 3 Who
REPORTING STENT PLACEMENT FOR NONOCCLUSIVE VASCULAR DISEASE IN LOWER EXTREMITIES
 REPORTING STENT PLACEMENT FOR NONOCCLUSIVE VASCULAR DISEASE IN LOWER EXTREMITIES Effective January 1, 2015, there was a change in CPT that affects reporting specific endovascular services provided in the
REPORTING STENT PLACEMENT FOR NONOCCLUSIVE VASCULAR DISEASE IN LOWER EXTREMITIES Effective January 1, 2015, there was a change in CPT that affects reporting specific endovascular services provided in the
Why do we need Dedicated Subspecialists and Interventionalists?
 Optimal Hemodialysis Access Management and The Role of the Interventionalist Vascular Access Education Day May 2, 2009 Interior Health Authority Peter C. Gregory, MD Medical Director Vascular Access Center
Optimal Hemodialysis Access Management and The Role of the Interventionalist Vascular Access Education Day May 2, 2009 Interior Health Authority Peter C. Gregory, MD Medical Director Vascular Access Center
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH
 Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Are venous catheters safe in terms of blood tream infection? What should I know?
 Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
California Health and Safety Code, Section 1256.01
 California Health and Safety Code, Section 1256.01 1256.01. (a) The Elective Percutaneous Coronary Intervention (PCI) Pilot Program is hereby established in the department. The purpose of the pilot program
California Health and Safety Code, Section 1256.01 1256.01. (a) The Elective Percutaneous Coronary Intervention (PCI) Pilot Program is hereby established in the department. The purpose of the pilot program
A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair
 A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair Table of Contents The AFX Endovascular AAA System............................................ 1 What is an Abdominal Aortic Aneurysm
A Patient s Guide to Minimally Invasive Abdominal Aortic Aneurysm Repair Table of Contents The AFX Endovascular AAA System............................................ 1 What is an Abdominal Aortic Aneurysm
Ischemic steal syndrome following arm arteriovenous fistula for hemodialysis
 Ischemic steal syndrome following arm arteriovenous fistula for hemodialysis Payman Zamani Cardiovascular Division, Veterans Affairs Boston Healthcare System and Cardiovascular Division, Brigham and Women
Ischemic steal syndrome following arm arteriovenous fistula for hemodialysis Payman Zamani Cardiovascular Division, Veterans Affairs Boston Healthcare System and Cardiovascular Division, Brigham and Women
Understanding your Renal Stent Procedure. A patient Guide (COVER PAGE) TABLE OF CONTENTS (inside front page)
 Understanding your Renal Stent Procedure. A patient Guide (COVER PAGE) TABLE OF CONTENTS (inside front page) The Kidney and the Renal Arteries... 1 Renal Artery Disease... 2 Diagnosis of Renal.Artery Disease...
Understanding your Renal Stent Procedure. A patient Guide (COVER PAGE) TABLE OF CONTENTS (inside front page) The Kidney and the Renal Arteries... 1 Renal Artery Disease... 2 Diagnosis of Renal.Artery Disease...
Heart transplantation
 Heart transplantation A patient s guide 1 Heart transplantation Heart transplantation has the potential to significantly improve the length and quality of life for patients with severe heart failure.
Heart transplantation A patient s guide 1 Heart transplantation Heart transplantation has the potential to significantly improve the length and quality of life for patients with severe heart failure.
Renovascular Disease. Renal Artery and Arteriosclerosis
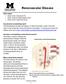 Other names: Renal Artery Stenosis (RAS) Renal Vascular Hypertension (RVH) Renal Artery Aneurysm (RAA) How does the normal kidney work? The blood passes through the kidneys to remove the body s waste.
Other names: Renal Artery Stenosis (RAS) Renal Vascular Hypertension (RVH) Renal Artery Aneurysm (RAA) How does the normal kidney work? The blood passes through the kidneys to remove the body s waste.
Hemodialysis, and therefore patent hemodialysis access, is of great
 Diagn Interv Radiol DOI 10.5152/dir.2014.14348 Turkish Society of Radiology 2014 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Technical success of percutaneous transluminal balloon angioplasty and factors
Diagn Interv Radiol DOI 10.5152/dir.2014.14348 Turkish Society of Radiology 2014 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Technical success of percutaneous transluminal balloon angioplasty and factors
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
Cilostazol versus Clopidogrel after Coronary Stenting
 Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
Cilostazol versus Clopidogrel after Coronary Stenting Seong-Wook Park, MD, PhD, FACC Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine Seoul, Korea AMC, 2004 Background
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
VFI Technology to Change the Way You Work
 Technology to Change the Way You Work Vascular Ultrasound Made Easier Vector Flow Imaging VFI VFI is a ground-breaking technology that can revolutionize the workflow for many Doppler ultrasound applications.
Technology to Change the Way You Work Vascular Ultrasound Made Easier Vector Flow Imaging VFI VFI is a ground-breaking technology that can revolutionize the workflow for many Doppler ultrasound applications.
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Components of CVC Care Bundle. selection
 Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Dialysis Access Procedures
 2 Dialysis Access Procedures Khalid O. Khwaja Hemodialysis Introduction Surgical Procedures a) Radiocephalic Fistula b) Brachiocephalic Fistula c) Basilic Vein Transposition d) Forearm Loop Arteriovenous
2 Dialysis Access Procedures Khalid O. Khwaja Hemodialysis Introduction Surgical Procedures a) Radiocephalic Fistula b) Brachiocephalic Fistula c) Basilic Vein Transposition d) Forearm Loop Arteriovenous
The Fatal Pulmonary Artery Involvement in Behçet s Disease
 The Fatal Pulmonary Artery Involvement in Behçet s Disease Dr. Vedat Hamuryudan Div. Rheumatology, Dept. Internal Medicine Cerrahpasa Medical Faculty, University of Istanbul 33 years old man Sept 2011:
The Fatal Pulmonary Artery Involvement in Behçet s Disease Dr. Vedat Hamuryudan Div. Rheumatology, Dept. Internal Medicine Cerrahpasa Medical Faculty, University of Istanbul 33 years old man Sept 2011:
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Non-surgical treatment of severe varicose veins
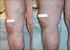 Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
renal transplantation: A single-center comparative study
 Impact of posterior urethral valves on pediatric renal transplantation: A single-center comparative study BY Mohamed Kamal Gheith, MD Oberarzt die Urologie, Universitätsmedizin Mainz Ass. Prof. of Urology,
Impact of posterior urethral valves on pediatric renal transplantation: A single-center comparative study BY Mohamed Kamal Gheith, MD Oberarzt die Urologie, Universitätsmedizin Mainz Ass. Prof. of Urology,
Hemodialysis Catheter Reduction. Janice Handley, RN, CNN, M.Ed Quality Support Specialist Fresenius Medical Care Kentucky Region
 Hemodialysis Catheter Reduction Janice Handley, RN, CNN, M.Ed Quality Support Specialist Fresenius Medical Care Kentucky Region Catheter patients initiating HD 65.3% in 1995 82% in 2006 Mortality Risk
Hemodialysis Catheter Reduction Janice Handley, RN, CNN, M.Ed Quality Support Specialist Fresenius Medical Care Kentucky Region Catheter patients initiating HD 65.3% in 1995 82% in 2006 Mortality Risk
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Duration of Dual Antiplatelet Therapy After Coronary Stenting
 Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Duration of Dual Antiplatelet Therapy After Coronary Stenting C. DEAN KATSAMAKIS, DO, FACC, FSCAI INTERVENTIONAL CARDIOLOGIST ADVOCATE LUTHERAN GENERAL HOSPITAL INTRODUCTION Coronary artery stents are
Thoracoabdominal aortic aneurysm
 Thoracoabdominal aortic aneurysm Patient (1) - 69 PMH: 2013 - MVP, aortic root replacement with biological valve (Perimount) and subtotal aortic arch replacement Analysis for oppressive chest complaints
Thoracoabdominal aortic aneurysm Patient (1) - 69 PMH: 2013 - MVP, aortic root replacement with biological valve (Perimount) and subtotal aortic arch replacement Analysis for oppressive chest complaints
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
MEDICAL COVERAGE POLICY. SERVICE: Varicose Veins of the Lower Extremities. PRIOR AUTHORIZATION: Required.
 Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
EMBOLIZATION OF CRANIOFACIAL ARTERIOVENOUS MALFORMATIONS. Dinah Hernandez MSN ED, PHN, RN Kaiser Permanente Los Angeles Medical Center
 EMBOLIZATION OF CRANIOFACIAL ARTERIOVENOUS MALFORMATIONS Dinah Hernandez MSN ED, PHN, RN Kaiser Permanente Los Angeles Medical Center Background Arteriovenous malformations (AVMs) are pathological direct
EMBOLIZATION OF CRANIOFACIAL ARTERIOVENOUS MALFORMATIONS Dinah Hernandez MSN ED, PHN, RN Kaiser Permanente Los Angeles Medical Center Background Arteriovenous malformations (AVMs) are pathological direct
Abdominal Aortic Aneurysm (AAA) General Information. Patient information Leaflet
 Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 1 st July 2016 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the heart
Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 1 st July 2016 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the heart
ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease. Erich Minar Medical University Vienna
 ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease Erich Minar Medical University Vienna for the Task Force on the Diagnosis and Treatment of Peripheral
ESC Guidelines on the diagnosis and treatment of peripheral artery diseases Lower extremity artery disease Erich Minar Medical University Vienna for the Task Force on the Diagnosis and Treatment of Peripheral
Catheter Embolization and YOU
 Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Catheter Embolization and YOU What is catheter embolization? Embolization therapy is a minimally invasive (non-surgical) treatment that occludes or blocks one or more blood vessels or vascular channels
Clinical Review Criteria
 Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
Effective Date: March 2, 2016
 Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Hemodialysis Access: What You Need to Know
 Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Hemodialysis Access: What You Need to Know Hemodialysis Access: What You Need To Know Whether you already get hemodialysis treatment, or you will need to start dialysis soon, this booklet will help you
Upper Extremity Arterial Duplex Evaluation
 VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Arterial Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
VASCULAR TECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Arterial Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
Imaging of Thoracic Endovascular Stent-Grafts
 Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
INTRODUCTION TO EECP THERAPY
 INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
INTRODUCTION TO EECP THERAPY is an FDA cleared, Medicare approved, non-invasive medical therapy for the treatment of stable and unstable angina, congestive heart failure, acute myocardial infarction, and
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Central Venous Catheters and Upper Extremity DVT: Update, Diagnosis and Management
 Central Venous Catheters and Upper Extremity DVT: Update, Diagnosis and Management David Hahn, MD Interventional Radiology NorthShore University HealthSystem Objectives Discuss the epidemiology and clinical
Central Venous Catheters and Upper Extremity DVT: Update, Diagnosis and Management David Hahn, MD Interventional Radiology NorthShore University HealthSystem Objectives Discuss the epidemiology and clinical
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Renal artery stenting: are there any indications left?
 there any indications left? Luís Mendes Pedro, MD. PhD, FEBVS Lisbon Academic Medical Centre (University of Lisbon and Hospital Santa Maria) Instituto Cardiovascular de Lisboa Disclosures Speaker name:
there any indications left? Luís Mendes Pedro, MD. PhD, FEBVS Lisbon Academic Medical Centre (University of Lisbon and Hospital Santa Maria) Instituto Cardiovascular de Lisboa Disclosures Speaker name:
FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE
 FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE The following describes the open surgical preparation and implantation technique for the Freedom Inguinal Hernia Repair System. 1) Anesthesia can be
FREEDOM INGUINAL Hernia Repair System TECHNIQUE GUIDE The following describes the open surgical preparation and implantation technique for the Freedom Inguinal Hernia Repair System. 1) Anesthesia can be
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS
 Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS What is a vascular access? A vascular access is a place on your body close to a vein and artery. This place
Understanding Your Hemodialysis Access Options UNDERSTANDING YOUR HEMODIALYSIS ACCESS OPTIONS What is a vascular access? A vascular access is a place on your body close to a vein and artery. This place
Complete coverage. Unbeatable value.
 Quest Travel Insurance Complete coverage. Unbeatable value. Quest with confidence, anytime, anywhere! Quest protects you when nothing else can, with: Future stability coverage: Stable now? Not sure you
Quest Travel Insurance Complete coverage. Unbeatable value. Quest with confidence, anytime, anywhere! Quest protects you when nothing else can, with: Future stability coverage: Stable now? Not sure you
ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY. Dr. Mahesh Vakamudi. Professor and Head
 ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY Dr. Mahesh Vakamudi Professor and Head Department of Anesthesiology, Critical Care and Pain Medicine Sri Ramachandra University INTRODUCTION
ANESTHESIA FOR PATIENTS WITH CORONARY STENTS FOR NON CARDIAC SURGERY Dr. Mahesh Vakamudi Professor and Head Department of Anesthesiology, Critical Care and Pain Medicine Sri Ramachandra University INTRODUCTION
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Raymond J. Holmes, M.D.
 CURRENT POSITION The Cardiovascular Care Group Vascular & Endovascular Surgery 5 Franklin Ave, Suite 310 Belleville, NJ 07109 (973) 759-9000 November 2004 to Present PREVIOUS POSITION Assistant Attending
CURRENT POSITION The Cardiovascular Care Group Vascular & Endovascular Surgery 5 Franklin Ave, Suite 310 Belleville, NJ 07109 (973) 759-9000 November 2004 to Present PREVIOUS POSITION Assistant Attending
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
NCD for Lipids Testing
 Applicable CPT Code(s): NCD for Lipids Testing 80061 Lipid panel 82465 Cholesterol, serum or whole blood, total 83700 Lipoprotein, blood; electrophoretic separation and quantitation 83701 Lipoprotein blood;
Applicable CPT Code(s): NCD for Lipids Testing 80061 Lipid panel 82465 Cholesterol, serum or whole blood, total 83700 Lipoprotein, blood; electrophoretic separation and quantitation 83701 Lipoprotein blood;
Provided by the American Venous Forum: veinforum.org
 CHAPTER 19 VASCULAR MALFORMATIONS Original authors: David H. Deaton, Byung Boong Lee, James Loredo, Richard F. Neville, William H. Pearce, and Heron E. Rodriguez Abstracted by Raghu Motaganahalli Introduction
CHAPTER 19 VASCULAR MALFORMATIONS Original authors: David H. Deaton, Byung Boong Lee, James Loredo, Richard F. Neville, William H. Pearce, and Heron E. Rodriguez Abstracted by Raghu Motaganahalli Introduction
Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery
 Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery Position Statement There is currently insufficient data for the (AOFAS) to recommend for or against routine VTED prophylaxis for
Position Statement: The Use of VTED Prophylaxis in Foot and Ankle Surgery Position Statement There is currently insufficient data for the (AOFAS) to recommend for or against routine VTED prophylaxis for
Listen to your heart: Good Cardiovascular Health for Life
 Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
