Report of the Welsh Neuroscience External Expert Review Group. Recommendations for Mid and South Wales
|
|
|
- Bethanie McDaniel
- 8 years ago
- Views:
Transcription
1 Report of the Welsh Neuroscience External Expert Review Group Recommendations for Mid and South Wales Main Recommendations 1. A Managed Clinical Network for neurosciences for Mid and South Wales should be established 2. Four medical neurology services, with in-patient capability, should be established in Cardiff, Newport, Swansea and Carmarthen. Complex care will take place in Cardiff and Swansea. 3. Acute Stroke Thrombolysis services should be run by the four medical neurology services until it can be established in the other acute admitting hospitals, where stroke units should be being developed in keeping with the UK guidelines. 4. Two in-patient Neurorehabilitation services should be developed and the spinal rehabilitation service should be close to the Neurosurgical service. This will require an additional WTE consultant at each site. 5. A single Neurosurgical service for South and West Wales, co-located with the Complex spinal and spinal deformity surgical service, the Neurocritical care service, the spinal injury unit and principle Neurorehabilitation service should be urgently developed. 6. Non-complex spinal surgery should be available in Cardiff and Swansea and could be provided by either orthopaedic or neurological surgeons. Rationale Evidence presented to the Review Group by patients, professionals and by benchmarking data shows that the Mid and South Wales population requires enhancement of neurological, neurorehabilitation, neurophysiology, stroke management and diagnostic facilities. Evidence on neurosurgery shows the need for a single service to allow compliance with the European Working Times Directive, to allow subspecialty development, and to provide an effective training environment. A Managed Clinical Network would provide the means by which agreed standards of care, care pathways and service monitoring can be applied. Welsh Assembly Government policy is that services should be developed within Wales whenever it is safe and appropriate to do so.
2 1. Medical Neurology a) Service Provision (viii) (ix) (x) (xi) The current academic medical neurology units should be supported and encouraged. There should be two neurology centres at Cardiff and Swansea with in patient capability for the management of acute and long term neurological conditions. One of these would support the neurosurgical service and the Neurocritical care unit, although general critical care capability would be available at the other centre. Every medical admission unit and critical care area should have a designated named neurologist(s). A 24/7 helpline manned by senior trainees or consultants should be available as a single point of advice for Wales. Initially, the Neurological Service would be out patient only in Newport and Carmarthen, with inpatients being transferred for complex care to Cardiff and Swansea. As soon as possible additional in-patient facilities should be established, in conjunction with the development of a thrombolysis service for stroke. The 4 medical neurology services will be linked through a Managed Clinical Network and provide the services to the other main hospital sites and in Mid Wales selected Community settings. The potential for telemedicine should be further explored to enhance both in-patient and out-patient care. The Network will support Neurophysiological Departments for non complex Electroencephalography (EEG) and Nerve Conduction studies. The centre at Carmarthen would serve Pembrokeshire, Carmarthenshire and Ceredigion and be linked to Swansea for inpatient care and Continuing Professional Development (CPD) requirements. The centre at Newport would serve Gwent and Caerphilly and be linked to Cardiff for in-patient care and CPD. They should at a minimum have access to 24/7 CT imaging linked to the neurosurgical service. All units in the future should plan the availability of 24/7 MRI. The four medical neurology services should also host the local Acquired Brain Injury teams interfacing with the community services. (see recommendation xii below) Modelling would suggest that there is a serious shortfall in the provision of neurology outpatient facilities. There is a need for 54 clinics weekly to see 11,340 new patients per year and a similar number of follow up visits.
3 (xii) (xiii) (xiv) (xv) (xvi) Dedicated outpatient facilities should be made available via the Network at all main hospital sites and as soon as possible in community settings, particularly in Mid Wales. The neurology services will support the local stroke and acquired brain injury teams. There is no bench marked figure for the recommended number of beds per 100,000 population and this will also depend on the pattern of medical admissions. Excluding stroke beds we would recommend 18 beds for Swansea and 24 beds for Cardiff both with expanded rehabilitation services. Patients with an acute neurological disorder admitted to a district hospital should at least have immediate access to an expert neurological opinion and be assessed by a neurologist within 24 hours, possibly via a telemedicine link. There should be rapid access to a designated regional neurosciences centre in which there are adequate numbers of critical care beds for neurological emergencies and access to neurosurgery. b) Workforce Issues On the basis of extant professional recommendations, consultant provision should be 1:80,000 population (Europe has 1:40,000). It is recommended, on a population distribution, 9 WTE consultants for West Wales of which 5 WTE consultants in Swansea. This figure might need to increase to meet an increase in referrals if neurosurgery were to be located elsewhere. In South East Wales, Cardiff should have 7 WTE consultants and Newport 6 WTE consultants. Nurse Specialists should support the medical workforce with a defined case load of no more than 300 patients each, in Epilepsy, Multiple Sclerosis, Parkinson s disease and Neuromuscular Disease. An increase in the number of locally based physiotherapists, occupational therapists and speech and language therapists will be required to meet additional demands. Specialist clinics consisting of multidisciplinary teams should be established to assist in the management of more complex aspects of the commoner neurological conditions (multiple sclerosis, Parkinson s disease, epilepsy, stroke, neuromuscular disorders and stroke) as close to the patients home as is feasible.
4 Patients with acute neurological conditions requiring non elective admission should be under the care of a consultant neurologist and their team. 2. Neurophysiology In addition to providing essential diagnostic services to the neurological patient, neurophysiology also provides essential services to orthopaedics hand clinics and ophthalmology. EEG (diagnosis and management of epilepsy), Electromyography (EMG) and nerve conduction studies should be available at all main hospital sites. They could be provided by a clinical physiologist (neurophysiology) and e- linked to the neurology centres with a quality assurance process monitored by the Network. The current two WTE consultant neurophysiologists in Cardiff with a PMETB accredited training program and its well funded training program for clinical physiologists (neurology) supported by Westminster College in London and funding from the Welsh Assembly Government should be continued and strongly supported. In Swansea, there is one WTE consultant neurophysiologist, supported by a retired neurologist. The service at Carmarthen is no longer active. Both services are well supported by clinical physiologists. Ideally an amalgamation of both services would provide a well balanced and effective resource for local delivery. Complex neurophysiology for epilepsy surgery and for the intra-operative monitoring of cranial and spinal surgery should be available where neurosurgery and spinal deformity surgery is performed. Further development of the interface between functional imaging and neurophysiology should be encouraged. 3. Stroke Management Acute admitting hospitals in Mid and South Wales should continue to develop their stroke units. All hospitals admitting acute stroke patients should have facilities and organisation that conform to the UK stroke guidelines. The development of a stroke thrombolysis service, performing to the United Kingdom thrombolysis guidelines, should be established at the earliest opportunity. This should be a 24/7 service and initially should be centred on the four neurology units with networks extended to the other main hospital sites in a phased process. It will require the integration of consultant rotas, team working and training. Telemedicine networks should be developed to support thrombolysis at geographically remote sites where transfer to a primary stroke centre is impractical.
5 Prompt and authoritative radiological reporting will be needed to support this initially (Section 5 radiology). This will require 24/7 local availability of CT scanning and prioritisation of acute stroke patients for CT access. In the foreseeable future MRI scanning is likely to be included. Rapid Access Neurovascular clinics should be established as a preventative measure. These should be One stop clinics enabling clinical assessment, carotid and brain imaging (usually Doppler ultrasound and CT scanning) and the institution of relevant therapy, including onward referral of appropriate cases to a vascular surgeon. Vascular surgical response times should be minimised to conform to UK guidelines. Stroke rehabilitation should follow local clinical pathways for acquired brain injury of whatever cause. A comprehensive stroke centre should be co-located with the neurosurgical and interventional neuroradiological services. Clear links should be established between all Stroke Units and the neurosurgical service for the onward referral of patients to the neurosurgical, unit when required. Guidelines should be in place for decompressive craniectomy and interventional neuroradiology. 4. Rehabilitation Two inpatient Neurological Rehabilitation Centres should be developed in Mid and South Wales, as part of the Managed Clinical Network and based on the resourced facilities at Swansea and Cardiff. This would cater for traumatic acquired brain injury, stroke and other neurological conditions requiring rehabilitation. For a single neurosurgical service to function efficiently and effectively the rehabilitation services will have to be expanded, both in terms of physical resource and personnel. The rehabilitation strategy will be defined and implemented in the acute phase of management and carried through as necessary to the community acquired brain injury team The Neurorehabilitation service in Cardiff is already scheduled for redevelopment. The service in Swansea is also in need of further development. The inpatient facilities should be in a ward /wards dedicated to rehabilitation. It is essential that a major neurological rehabilitation facility is developed in the same city as the neurosurgical service and on a site that enables full medical cover, as it would be anticipated that patients would be transferring into the rehabilitation service earlier than currently. The principle rehabilitation unit should be closely located to the neurosurgical unit. It must be developed on an acute hospital site to ensure
6 appropriate 24/7 medical cover and have the ability to provide a service to the acute phase of the neurological patient. (viii) (ix) (x) (xi) (xii) The co-location of all rehabilitation facilities (cardiac, amputation etc) would be hugely beneficial as would the effective integration with bioengineering and driving assessment centres. A further inpatient rehabilitation facility should be developed on the other principal in-patient neurology site to enable patients with stroke, neurological disability and head injury to be managed nearer home. Both in-patient centres should act as the focus for South East and South West Wales rehabilitation and acquired brain injury services. Acute admitting hospitals should develop integrated facilities for stroke and head injured patients through acquired brain injury teams, to enable their return to the community. There needs to be a liaison rehabilitation team, led by a Rehabilitation Medicine Physician in every hospital to support the other services and to ensure speedy and effective transfer to an in-patient or other rehab facility as needed. The spinal injury unit should have the ability to accept all patients with neurological injury within 24hrs of injury, except for those who require spinal stabilisation procedures who will first be admitted through the complex spinal surgical service. The service providing rehabilitation for spinal injury should work alongside that for neurological rehabilitation to make the most effective use of the resource available for cross cover and educational opportunities. The service should be able to manage ventilated patients and could be further developed to oversee those patients with spinal injury, as well as those with other neurological conditions, who require home ventilation. This would represent a significant opportunity to develop an effective and integrated service in Wales. A minimum of 2 WTE consultants would be required to manage the spinal injury service. Depending on the special interests of the neurological and neurosurgical consultants, a minimum of 2 WTE consultants would be required for each in-patient rehabilitation centre. A full complement of allied health professionals and neuropsychologists would be needed to complete the teams. 5. Neuroradiology and Image Transfer All hospitals accepting acute admissions must have the facility to perform CT scans 24/7. Those hospitals undertaking thrombolysis must be able to perform CT scans within an hour of the patient s admission. To be optimally effective this may need to be extended to include multimodal MRI or CT as soon as is feasible.
7 (viii) With effective and agreed guidelines for the management of acute patients CT scanning should be available without the need for negotiation over access to the scanner. Those clinicians responsible for reporting or making management decisions on scans must be able to do this in an effective time scale. Daytime clinical activities should take this in to account. The ability to review scans at home out of hours should be developed. All images in the future should be available on a single national Welsh PACS which should link with the tertiary centres. Interventional radiology should be developed alongside the neurosurgery service. It needs to be developed to be capable of delivering a 7 day per week service for the management of intracranial aneurysm and arteriovenous malformation, as well as tumour embolisation. There is also potential for it to develop into a 24/7service if the evidence base for aggressive stroke management emerges (intra-arterial clot lysis and mechanical revascularisation). The interventional sessions will need to be fully resourced, with designated anaesthetic sessions and recovery facility. Paediatric neuroradiology would need to be based in relation to paediatric neurology, paediatric neuro-oncology, paediatric neurosurgery and the neurosurgical service. Neuroradiology would be available on the other in-patient neurology site supported by neuroradiologists and image transfer. The availability of a 3 Tesla magnet will enhance the opportunities for research. 6. Neuropathology Neuropathology needs to be supported and developed to provide a sustainable service for the future. The existing consultant WTE is insufficient to maintain an EWTD compliant service. The links with academia need to be promoted to provide the maximum opportunity for research together with education and training. Links with other Neuropathology services need to be developed to enable an effective and compliant 24/7 service.
8 7. Neurosurgery a) Service Provision A single neurosurgery service must be established at the earliest opportunity, co-located with Neurocritical care, complex and spinal deformity surgery, neurology and essentially paediatric neurological care including paediatric neurosurgery, which should be in a collocated in an adjacent child health setting with its own facilities, including paediatric critical care. The neurosurgical service should be supported by a strong on site Neuropathology service. The service must redress the deficiencies of the current two units, not only in terms of resource but also taking account of service redesign and compliance with current and future professional regulation. The Mid and South Wales population of 2.3 million (WAG Census 2006), requires 65 dedicated, ring fenced beds. This excludes adult critical care (levels 3 and 2) and paediatric beds. The bed numbers could be reduced if a non complex spinal assessment and surgery centre were to be maintained in the other neurology centre. (viii) (ix) The adjacent collocation of a further 28 beds is needed to facilitate the management of complex spinal problems. This would also avoid split site working for the spinal orthopaedic surgeons and enable an integrated sustainable emergency spinal 24/7 service This would offer the opportunity for the redesign of pathways of care to ensure effective use of beds. The ability to discharge patients, who no longer require the facilities of the neurosurgical inpatient service, is essential to working with this bed capacity. The operating theatre capacity to support the service would be 18 sessions for elective neurosurgery perhaps incorporating three session days, with either a dedicated third theatre for emergencies or guaranteed immediate 24/7 access to a closely located CEPOD theatre. Recovery beds will also need to recover cases from interventional radiology. Out-patient clinics would be required for individual neurosurgeons, with the capability to run additional multidisciplinary clinics (e.g. neurovascular and neuro-oncology etc). The development of a single service would provide a greater opportunity for sub-specialisation that could include areas such as Deep Brain Stimulation thus enabling repatriation of services to Wales.
9 b) Workforce Issues The population base which currently generates an operative workload of 1, case per year would support 9 WTE consultant neurosurgeons or 10 if two academic positions were created. This would be European Working Time Regulation (EWTR) compliant with the development of neurosurgical teams and also allow development of subspecialty interest and expertise, academic development and opportunity for research. A sustainable accredited training program would be possible and EWTR compliant. Particular attention should be made to accommodate all clinical activity within a three session day, only true emergency activity being undertaken out of hours. This would enable a balance between service needs and training requirements without a large number of additional trainees purely on the basis of rota requirements. There should be a separation of elective and emergency activity to allow a consultant or experienced trainee to be available to respond to requests for emergency opinions. The neurosurgical rota and spinal rota should be constructed to ensure 24/7 cover for spinal emergencies. 8. Neurotrauma Current Trauma Audit and Research Network (TARN) data demonstrates that it currently takes between 4-5 hrs from injury to the neurosurgical operating theatre for the less than 100 craniotomies for traumatic haematomas performed each year. 2-3 hrs of this time is expended in the initial receiving hospital assessing, scanning, resuscitating and stabilising the patient. Significant time is lost in delays in scanning and communication and decision making with the neurosurgical units. Addressing these delays together with ensuring effective transport, including the use of air ambulance, would not only absorb the additional 30mins blue light time to a single centre but should enable a faster admission to the neurosurgical unit. Each receiving unit should clearly designate who is responsible for the inpatient clinical care of non-neurosurgical head injuries and ensure that clinicians have the appropriate training and that a governance system is in place. The SBNS (Society of British Neurological Surgeons) and TARN guidelines, as published in the Lancet (ref), should be adopted immediately. Compliance with national audit such as TARN should be mandatory. Contemporaneous data collection and coding must be in place to monitor outliers and delays, in order to rectify system failures.
10 Each receiving unit should have clear policies for the evaluation of potential spinal injury with clear clinical responsibility. Spinal injury with neurological deficit and or evidence of orthopaedic instability (SBNS/TARN, British Orthopaedic Association BOA Guidelines), should be admitted within 24hrs of injury with onward referral on completion of stabilisation to the Spinal Rehabilitation service if appropriate. 9. Neurocritical Care a) Service Provision Both short and long term capacity targets argue strongly for a single neurocritical care service in Mid and South Wales: to ensure the necessary critical mass for the delivery of efficient and high quality clinical care, to allow the peaks and troughs of demand to be managed most effectively and to provide the only workable solution to sustainable workforce planning. It is clear that there is considerable unmet need for neurocritical care throughout Wales. At the moment this is probably at least 50% of current provision and possible more. When likely changes in practice are taken into account (e.g. transfer of all severe Traumatic Brain Injury (TBI), poor grade Sub Arachnoid Haemorrhage (SAH) and increased numbers of stroke patients), the unmet need is likely to rise to 100% of current capacity. Neuroscience critical care capacity in Wales should be planned to ensure adequate numbers of staffed level 2 and level 3 beds to allow access for all patients within appropriate clinical timescales. In general terms, capacity should be managed to allow: Patients requiring life-saving neurosurgery for an expanding intracranial mass lesion to be transferred to the neuroscience centre within 4 hours of acceptance for treatment. All other patients with severe head injury to be transferred to a neuroscience critical care bed, irrespective of whether neurosurgical intervention is required, and ideally within 24 hours. Other patients who require intensive care management in a neuroscience unit but who are stable on a general ICU should be transferred within 48 hours of referral. The Society of British Neurological Surgeons recommends that there should be 10 dedicated level 2 and 3 critical care beds per million population to support emergency and elective neurosurgical services. The Association of British Neurologists additionally estimates that between 5
11 and 7 dedicated neurocritical care beds per million population are required to support the care of neurology patients. (viii) (ix) Using these estimates there should be neurocritical care beds for the population of Mid and South Wales. However, some believe that these estimates are excessive and that a responsive neurocritical care service can be delivered with fewer numbers of beds so long as flexibility between level 2 and level 3 capacity is maintained. There is also local evidence from English units serving similar populations that an excellent service can be delivered, under current referral arrangements, with fewer beds. Using such units as exemplars the minimum capacity available for the population of South Wales should be neurocritical care beds. Future plans should look beyond this minimum and incorporate sufficient capacity to accommodate the changes in practice that will occur over the next five years. These include, but are not limited to, admission of all patients with severe TBI to neuroscience units, increasing intervention in patients with poor grade SAH and the increased numbers of patients with ischaemic stroke, who will require neurocritical care. If neuroscience critical care beds are integrated into a general critical care facility, appropriate policies should be in place to maintain access for neuroscience patients with consideration given to ring-fencing a cohort of beds. The workforce, medical staffing, nurse and allied health professionals should be as identified in the Neuroscience Critical Care Report: progress in developing services and in guidance published by the Intensive Care Society. In addition to the general facilities available to all critically ill patients, facilities for intracranial pressure monitoring should be routinely available. Facilities for other intracranial monitoring (e.g. cerebral oxygenation, cerebral microdialysis, cerebral blood flow, continuous EEG) should be available where appropriate. There should be 24/7 immediate access to CT, and to MRI, diagnostic angiography and interventional neuroradiology within clinically appropriate timescales. Access to transcranial Doppler ultrasonography and diagnostic electrophysiological services should also be available within clinically appropriate timescales. The rehabilitation process should start in the acute phase and allied health professionals and rehabilitation medicine specialists play a pivotal role in this aspect of care. Their specialist skills contribute to ensuring the best possible outcome for patients. There should be a culture of data collection and performance review.
12 Data should be collected to allow local and national activity planning, facilitate clinical audit, including the provision of comparative outcome data, and to inform financial flows. (ix) (x) (xi) (xii) The Critical Care Minimum Dataset (CCMDS) should be collected for all neuroscience critical care activity and in addition, membership of the Intensive Care National Audit Research Centre (ICNARC) Case mix Programme is mandatory. NccNet, a collaboration of neuroscience critical care units, has recently been established and is working towards the development of a national database for neuroscience critical care. Contribution to this database should be mandatory when established. Local strategies should be developed to identify all critically ill neuroscience patients across the whole hospital, including those that require level 1 care. There are particular problems identifying neurosurgical patients receiving level 2 care when this care is delivered within neurosurgical wards. It is crucial that mechanisms are developed to capture this activity via the Critical Care Minimum Dataset. Neuroscience units often experience difficulties in discharging patients from critical care units when the period of specialist care has ended. Network guidelines should be agreed to facilitate the transfer/repatriation of patients to appropriate facilities in a timely manner. b) Critical Care Outreach The concept of existing critical care outreach services should be applied to neuroscience patients in ward areas in the neuroscience unit. In addition, the concept of neuroscience outreach should be adapted to support neuroscience patients along their complete care pathway, including the district general hospital and community. When a critically ill patient with neurological disease is being managed in a DGH intensive care unit, a named consultant from the neuroscience unit (usually the consultant neurologist covering that DGH) should be identified as the primary liaison between DGH and neuroscience unit. c) Long term ventilation Neuroscience patients that require long term ventilatory support often remain for long periods, and inappropriately, in an acute environment. The plans for the development of a step-down facility for the management of those patients who require long term ventilatory support in Mid and South Wales, should be expedited and consideration should be given to the provision of a similar facility in North Wales.
13 Such a facility will require 24/7 medical cover and should preferably be located on an acute hospital site. 10. Spinal Surgery Co-location of the complex/scoliosis orthopaedic spinal service and neurosurgical service would enable the provision of a 24/7 emergency service for acute spinal conditions and an advice service to the peripheral hospitals for the interpretation of scans for acute lumbar, thoracic and cervical discs, metastatic disease and infection. The scoliosis service requires access to both adult and paediatric intensive care facilities. A non complex spinal service could be provided in either Swansea or Cardiff to minimise patient travel either from east or west respectively. Protocols and guidelines should be developed for the assessment of back pain and sciatica, cauda equina compression and when available from NICE, metastatic cord compression, to enable local evaluation and to minimise the need to travel. The service must be able to deliver the findings of NICE guidelines for metastatic cord compression. The fluctuations in bed requirements would be best managed with a combined resource. Spinal assessment teams based on advanced nurse and allied health practitioners could provide support at district general hospitals and be based for CPD and quality assurance within the two spinal services The spinal service should have accessibility to interventional radiology for image guided biopsy, vertebroplasty and the neurovascular management of spinal vascular anomalies. Training opportunities for both neurosurgeons and orthopaedic neurosurgeons would be enhanced. 11. Mid Wales In addition to the recommendations and conclusions above it is recognised that Mid Wales has unique requirements caused by its geography and existing service provision. The centre of Wales has particular problems of access to hospital care. The increased provision of neurologists will allow access to neurological care in Community settings. However there will be patients with neurotrauma and other neurological emergencies whose nearest access will be in England; this will need to continue for the foreseeable future.
ADULT HEALTH AND WELLBEING LONG-TERM NEUROLOGICAL CONDITIONS
 ADULT HEALTH AND WELLBEING LONG-TERM NEUROLOGICAL CONDITIONS i. Summary The National Service Framework for long-term neurological conditions categorises neurological conditions as: Sudden-onset conditions
ADULT HEALTH AND WELLBEING LONG-TERM NEUROLOGICAL CONDITIONS i. Summary The National Service Framework for long-term neurological conditions categorises neurological conditions as: Sudden-onset conditions
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD
 REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services
REHABILITATION MEDICINE by PROFESSOR ANTHONY WARD What is Rehabilitation Medicine? Rehabilitation Medicine (RM) is the medical specialty with rehabilitation as its primary strategy. It provides services
Reconfiguration of Surgical, Accident and Emergency and Trauma Services in the UK
 Reconfiguration of Surgical, Accident and Emergency and Trauma Services in the UK K Reconfiguration of Surgical, Accident and Emergency and Trauma Services in the UK Summary Our aim is to provide an excellent
Reconfiguration of Surgical, Accident and Emergency and Trauma Services in the UK K Reconfiguration of Surgical, Accident and Emergency and Trauma Services in the UK Summary Our aim is to provide an excellent
The new Stroke Nurse Practitioner candidate position at Austin Health
 The new Stroke Nurse Practitioner candidate position at Austin Health The new Stroke Nurse Practitioner (NP) candidate position offered by Austin Health provides an exciting opportunity for a senior nurse
The new Stroke Nurse Practitioner candidate position at Austin Health The new Stroke Nurse Practitioner (NP) candidate position offered by Austin Health provides an exciting opportunity for a senior nurse
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 27th February 2014
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Regional Trauma Network Trauma Centre Trauma Service RMTN Network Organisation Measures (T13-1C-1) - 2013/14 Peer Review Visit Date 27th February 2014
Strategic Planning for Stroke Center Accreditation/Certification. Suzanne Borgos, MBA/MHA VP, Planning
 Strategic Planning for Stroke Center Accreditation/Certification Suzanne Borgos, MBA/MHA VP, Planning Disclosures I have no pertinent relationships to disclose. 2 Stroke Care at Capital Health Regional
Strategic Planning for Stroke Center Accreditation/Certification Suzanne Borgos, MBA/MHA VP, Planning Disclosures I have no pertinent relationships to disclose. 2 Stroke Care at Capital Health Regional
CHILDREN S NEUROSCIENCE CENTER
 CHILDREN S NEUROSCIENCE CENTER W hen families come to Children s Memorial Hermann Hospital, they expect to find the technological advances and healing expertise of a university-affiliated, academic hospital.
CHILDREN S NEUROSCIENCE CENTER W hen families come to Children s Memorial Hermann Hospital, they expect to find the technological advances and healing expertise of a university-affiliated, academic hospital.
ACUTE STROKE PATHWAY
 ACUTE STROKE PATHWAY THERE IS A NEED FOR STATEWIDE STROKE SYSTEM OF CARE ALL MISSISSIPPIANS SHOULD BE ABLE TO ACCESS NEW PROTOCOLS FOR STROKE TREATMENT JOINT EFFORT WITH EMS, PHYSICIANS, HOSPITALS AND
ACUTE STROKE PATHWAY THERE IS A NEED FOR STATEWIDE STROKE SYSTEM OF CARE ALL MISSISSIPPIANS SHOULD BE ABLE TO ACCESS NEW PROTOCOLS FOR STROKE TREATMENT JOINT EFFORT WITH EMS, PHYSICIANS, HOSPITALS AND
1 1-1 1-1 All trauma centers must participate in the state and/or regional trauma system planning, development, or operation.
 American College of Surgeons Consultation/Verification Program Reference Guide of Suggested Classification Level II Chapter CD Requirement by Chapter http://www.facs.org/trauma/verifivisitoutcomes.html
American College of Surgeons Consultation/Verification Program Reference Guide of Suggested Classification Level II Chapter CD Requirement by Chapter http://www.facs.org/trauma/verifivisitoutcomes.html
Aims. Background. The aims of this report are to:
 COMMENTARY Aims The aims of this report are to: establish current practice in the provision of services for the management of patients with head injuries in the United Kingdom and the Republic of Ireland;
COMMENTARY Aims The aims of this report are to: establish current practice in the provision of services for the management of patients with head injuries in the United Kingdom and the Republic of Ireland;
National Clinical Programmes
 National Clinical Programmes Section 3 Background information on the National Clinical Programmes Mission, Vision and Objectives July 2011 V0. 6_ 4 th July, 2011 1 National Clinical Programmes: Mission
National Clinical Programmes Section 3 Background information on the National Clinical Programmes Mission, Vision and Objectives July 2011 V0. 6_ 4 th July, 2011 1 National Clinical Programmes: Mission
Anaesthetics, Pain Relief & Critical Care Services Follow-Up Study REGIONAL REPORT. Performance Review Unit
 Anaesthetics, Pain Relief & Critical Care Services Follow-Up Study REGIONAL REPORT Performance Review Unit CONTENTS page I INTRODUCTION... 2 II PRE-OPERATIVEASSESSMENT... 4 III ANAESTHETIC STAFFING AND
Anaesthetics, Pain Relief & Critical Care Services Follow-Up Study REGIONAL REPORT Performance Review Unit CONTENTS page I INTRODUCTION... 2 II PRE-OPERATIVEASSESSMENT... 4 III ANAESTHETIC STAFFING AND
Neurocritical Care Program Requirements
 Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
Neurocritical Care Program Requirements Approved October 17, 2014 Page 1 Table of Contents I. Introduction 3 II. Institutional Support 3 A. Sponsoring Institution 4 B. Primary Institution 4 C. Participating
STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS
 STATEMENT Document No: S12 Approved: Jul-97 Last Revised: Nov-12 Version No: 05 STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS 1. PURPOSE This document defines the minimum requirement for a health
STATEMENT Document No: S12 Approved: Jul-97 Last Revised: Nov-12 Version No: 05 STATEMENT ON THE DELINEATION OF EMERGENCY DEPARTMENTS 1. PURPOSE This document defines the minimum requirement for a health
Proposed co-location of stroke services
 Proposed co-location of stroke services Contents Contents... 2 Executive summary... 3 Introduction... 4 How stroke services are currently provided... 6 The case for change... 8 What is our proposed service
Proposed co-location of stroke services Contents Contents... 2 Executive summary... 3 Introduction... 4 How stroke services are currently provided... 6 The case for change... 8 What is our proposed service
Manifesto for Acquired Brain Injury Rehabilitation
 Manifesto for Acquired Brain Injury Rehabilitation For further information please contact: Chloë Hayward UKABIF Executive Director PO Box 355 Plymouth PL3 4WD Tel: 01752 601318 Email: ukabif@btconnect.com
Manifesto for Acquired Brain Injury Rehabilitation For further information please contact: Chloë Hayward UKABIF Executive Director PO Box 355 Plymouth PL3 4WD Tel: 01752 601318 Email: ukabif@btconnect.com
AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Verificatoin Criterea EFFECTIVE JANUARY 1, 2015. Criterion. Level (1 or 2) Number
 Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Good Samaritan Inpatient Rehabilitation Program
 Good Samaritan Inpatient Rehabilitation Program Living at your full potential. Welcome When people are sick or injured, our goal is their maximum recovery. We help people live to their full potential.
Good Samaritan Inpatient Rehabilitation Program Living at your full potential. Welcome When people are sick or injured, our goal is their maximum recovery. We help people live to their full potential.
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. CP57 Version: V3
 GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
GP workshop. Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre
 GP workshop Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre Stroke: the Facts Stroke: the Facts Every 5 minutes someone in the UK has a stroke 1 in 4 men and 1 in 5 women will have a stroke
GP workshop Maria Fitzpatrick Nurse Consultant Kings College Stroke Centre Stroke: the Facts Stroke: the Facts Every 5 minutes someone in the UK has a stroke 1 in 4 men and 1 in 5 women will have a stroke
SCHEDULE 2 THE SERVICES. Paediatric Critical Care Transport
 SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E07/S/d Paediatric Critical Care Transport 12 Months 1. Population
SCHEDULE 2 THE SERVICES A. Service Specifications Service Specification No. Service Commissioner Lead Provider Lead Period Date of Review E07/S/d Paediatric Critical Care Transport 12 Months 1. Population
Rehabilitation Where You Recover. Inpatient Rehabilitation Services at Albany Medical Center
 Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Background paper 9: Rehabilitation services
 Background paper 9: Rehabilitation services Current services Townsville Health Service District (HSD) provides all rehabilitation services for the District. Within the District, a number of Institutes
Background paper 9: Rehabilitation services Current services Townsville Health Service District (HSD) provides all rehabilitation services for the District. Within the District, a number of Institutes
D04/ODN/a NHS STANDARD CONTRACT FOR NEUROMUSCULAR OPERATIONAL DELIVERY NETWORKS SCHEDULE 2- THE SERVICES A. SERVICE SPECIFICATIONS
 D04/ODN/a NHS STANDARD CONTRACT FOR NEUROMUSCULAR OPERATIONAL DELIVERY NETWORKS SCHEDULE 2- THE SERVICES A. SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period
D04/ODN/a NHS STANDARD CONTRACT FOR NEUROMUSCULAR OPERATIONAL DELIVERY NETWORKS SCHEDULE 2- THE SERVICES A. SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider Lead Period
STANDARDS. for the provision of. Inpatient Adult Rehabilitation Medicine Services. Public and Private Hospitals
 Australasian Faculty of Rehabilitation Medicine STANDARDS for the provision of Inpatient Adult Rehabilitation Medicine Services in Public and Private Hospitals 2011 Telephone (02) 9256 5420 145 Macquarie
Australasian Faculty of Rehabilitation Medicine STANDARDS for the provision of Inpatient Adult Rehabilitation Medicine Services in Public and Private Hospitals 2011 Telephone (02) 9256 5420 145 Macquarie
All Wales Neurosciences Standards for Children and Young People s Specialised Healthcare Services
 All Wales Neurosciences Standards for Children and Young People s Specialised Healthcare Services CMK-22-12-160 E1240910 ISBN: 978 0 7504 5215 1 Crown Copyright July 2009 Foreword It gives me great pleasure
All Wales Neurosciences Standards for Children and Young People s Specialised Healthcare Services CMK-22-12-160 E1240910 ISBN: 978 0 7504 5215 1 Crown Copyright July 2009 Foreword It gives me great pleasure
Stakeholder s Report. 2525 SW 75 th Ave Miami, Florida 33155 305.262.6800 www.westgablesrehabhospital.com
 212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
212 Stakeholder s Report 2525 SW 75 th Ave Miami, Florida 33155 35.262.68 www.westgablesrehabhospital.com PROFILE REPORT For more than 25 years, West Gables Rehabilitation Hospital has made a mission of
Specialist brain injury services. Rehabilitation Transitional medical care Community support Special education
 Specialist brain injury services Rehabilitation Transitional medical care Community support Special education I don t know where we d be without the support we ve had from the staff at The Children s Trust.
Specialist brain injury services Rehabilitation Transitional medical care Community support Special education I don t know where we d be without the support we ve had from the staff at The Children s Trust.
South Eastern Health and Social Care Trust
 South Eastern Health and Social Care Trust JOB DESCRIPTION TITLE OF POST: Consultant General Surgeon LOCATION: This post is part of the South Eastern Trust and will be based at the Ulster Hospital. However,
South Eastern Health and Social Care Trust JOB DESCRIPTION TITLE OF POST: Consultant General Surgeon LOCATION: This post is part of the South Eastern Trust and will be based at the Ulster Hospital. However,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE CENTRE FOR CLINICAL PRACTICE QUALITY STANDARDS PROGRAMME standard topic: Specialist neonatal care Output: standard advice to the Secretary of State
Main Specialty/Treatment Function Codes. Human Behavioural Guidance
 Human Behavioural Guidance Version No: 0.1 Purpose of this document This document comprises the Human Behavioural Guidance for NHS Organisations in relation to the changes to the Main Specialty and Treatment
Human Behavioural Guidance Version No: 0.1 Purpose of this document This document comprises the Human Behavioural Guidance for NHS Organisations in relation to the changes to the Main Specialty and Treatment
DRAFT note of meeting
 Neurosurgery Managed Service Network Operational Management Group 20 September 2010, 10 a.m. Conference Room A, St Andrew s House, Edinburgh DRAFT note of meeting Present: Apologies: Mr Eric Ballantyne,
Neurosurgery Managed Service Network Operational Management Group 20 September 2010, 10 a.m. Conference Room A, St Andrew s House, Edinburgh DRAFT note of meeting Present: Apologies: Mr Eric Ballantyne,
Rehabilitation. Day Programs
 Rehabilitation Day Programs Healthe Care is the hospital division of Healthe. As the largest privately owned network of private hospitals in Australia, we take pride in delivering premium care to our valued
Rehabilitation Day Programs Healthe Care is the hospital division of Healthe. As the largest privately owned network of private hospitals in Australia, we take pride in delivering premium care to our valued
Guidelines for the Operation of Burn Centers
 C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
C h a p t e r 1 4 Guidelines for the Operation of Burn Centers............................................................. Each year in the United States, burn injuries result in more than 500,000 hospital
Child & Adolescent Rehabilitation Services (CARS)
 Child & Adolescent Rehabilitation Services (CARS) Operational Guidelines To be read in conjunction with the CARS contract June 2013 This is a living document and will be updated as required Contents Child
Child & Adolescent Rehabilitation Services (CARS) Operational Guidelines To be read in conjunction with the CARS contract June 2013 This is a living document and will be updated as required Contents Child
Future hospital: Caring for medical patients. Extract: Recommendations
 Future hospital: Caring for medical patients Extract: Recommendations Future hospital: caring for medical patients Achieving the future hospital vision 50 recommendations The recommendations from Future
Future hospital: Caring for medical patients Extract: Recommendations Future hospital: caring for medical patients Achieving the future hospital vision 50 recommendations The recommendations from Future
A systematic review of focused topics for the management of spinal cord injury and impairment
 A systematic review of focused topics for the management of spinal cord injury and impairment icahe, University of South Australia For the NZ Spinal Cord Impairment Strategy Introduction This was the third
A systematic review of focused topics for the management of spinal cord injury and impairment icahe, University of South Australia For the NZ Spinal Cord Impairment Strategy Introduction This was the third
CONSULTANT PAEDIATRIC ALLERGIST FULL TIME JOB DESCRIPTION
 1. THE TRUST CONSULTANT PAEDIATRIC ALLERGIST FULL TIME JOB DESCRIPTION Alder Hey Children s NHS Foundation Trust is a major teaching hospital of the University of Liverpool. It serves not only the children
1. THE TRUST CONSULTANT PAEDIATRIC ALLERGIST FULL TIME JOB DESCRIPTION Alder Hey Children s NHS Foundation Trust is a major teaching hospital of the University of Liverpool. It serves not only the children
Rehabilitation Services within Essex Cancer Network for people with Brain & CNS tumours
 Rehabilitation Services within Essex Cancer Network for people with Brain & CNS tumours The NICE IOG for people with Brain & other CNS tumours (2006) states that patients with such tumours should have
Rehabilitation Services within Essex Cancer Network for people with Brain & CNS tumours The NICE IOG for people with Brain & other CNS tumours (2006) states that patients with such tumours should have
The SheYeld experiment: the evects of centralising accident and emergency services in a large urban setting
 Emerg Med J 2001;18:193 197 193 The SheYeld experiment: the evects of centralising accident and emergency services in a large urban setting A N Simpson, J Wardrope, D Burke Northern General Hospital, Herries
Emerg Med J 2001;18:193 197 193 The SheYeld experiment: the evects of centralising accident and emergency services in a large urban setting A N Simpson, J Wardrope, D Burke Northern General Hospital, Herries
Transfer of Care Guideline for Stroke Patients Stroke Reperfusion Workgroup
 Transfer of Care Guideline for Stroke Patients Stroke Reperfusion Workgroup Contact: Mark Longworth, Stroke Network Manager, ACI, Mob 0417 680 482, Tel 02 8644 2188 Mark.Longworth@aci.health.nsw.gov.au
Transfer of Care Guideline for Stroke Patients Stroke Reperfusion Workgroup Contact: Mark Longworth, Stroke Network Manager, ACI, Mob 0417 680 482, Tel 02 8644 2188 Mark.Longworth@aci.health.nsw.gov.au
The shape of things to come
 The shape of things to come Whole pathway assurance rehabilitation Major trauma Appendix 6f 2 Contents Contents...3 1 Introduction...4 2 Executive summary...4 3 Scope and context...4 4 Part A Assurance...5
The shape of things to come Whole pathway assurance rehabilitation Major trauma Appendix 6f 2 Contents Contents...3 1 Introduction...4 2 Executive summary...4 3 Scope and context...4 4 Part A Assurance...5
STEREOTACTIC RADIOSURGERY COMMISSIONING POLICY
 STEREOTACTIC RADIOSURGERY COMMISSIONING POLICY Release Version 3.1 Date: 21 st September 2006 Author: Owner: Client: Ian Langfield, Service Group Commissioner, HCW Ian Langfield, Service Group Commissioner,
STEREOTACTIC RADIOSURGERY COMMISSIONING POLICY Release Version 3.1 Date: 21 st September 2006 Author: Owner: Client: Ian Langfield, Service Group Commissioner, HCW Ian Langfield, Service Group Commissioner,
The Acute Neurological Rehabilitation Unit
 The Acute Neurological Rehabilitation Unit Welcome The Wellington Hospital s Acute Neurological Rehabilitation Unit is the largest private unit in the UK, with 60 rooms specifically designed for neurological
The Acute Neurological Rehabilitation Unit Welcome The Wellington Hospital s Acute Neurological Rehabilitation Unit is the largest private unit in the UK, with 60 rooms specifically designed for neurological
Quality and Safety Programme Inter-hospital transfers - adults
 Quality and Safety Programme Inter-hospital transfers - adults London quality standards October 2014 Introduction A lack of robust inter-hospital transfer and acceptance standards is a current issue for
Quality and Safety Programme Inter-hospital transfers - adults London quality standards October 2014 Introduction A lack of robust inter-hospital transfer and acceptance standards is a current issue for
Baptist Health Rehabilitation Institute. Clinical Outcomes
 Baptist Health Rehabilitation Institute Clinical Outcomes Baptist Health Rehabilitation Institute (BHRI), located on chaplain services offer a range of individualized evaluations and the campus of Baptist
Baptist Health Rehabilitation Institute Clinical Outcomes Baptist Health Rehabilitation Institute (BHRI), located on chaplain services offer a range of individualized evaluations and the campus of Baptist
NHS Midlands and East Stroke Services Specification
 NHS Midlands and East Stroke Services Specification Version Control Version No. Date Authors/ Editors To be reviewed by Status v1.0 01 June 2012 Tim Lawrence, Laura Dendy External Expert Advisory Group
NHS Midlands and East Stroke Services Specification Version Control Version No. Date Authors/ Editors To be reviewed by Status v1.0 01 June 2012 Tim Lawrence, Laura Dendy External Expert Advisory Group
Improving Our Services for Older People in Cardiff and the Vale of Glamorgan. The Development of Clinical Gerontology Services
 Improving Our Services for Older People in Cardiff and the Vale of Glamorgan The Development of Clinical Gerontology Services What s this document about? Cardiff and Vale University Health Board (UHB)
Improving Our Services for Older People in Cardiff and the Vale of Glamorgan The Development of Clinical Gerontology Services What s this document about? Cardiff and Vale University Health Board (UHB)
Pre-budget Submission 2016. Joint Committee on Finance, Public Expenditure and Reform
 Pre-budget Submission 2016 Joint Committee on Finance, Public Expenditure and Reform July 2015 SUMMARY POINTS Acquired Brain Injury Ireland (ABI Ireland) is asking the Government to support people living
Pre-budget Submission 2016 Joint Committee on Finance, Public Expenditure and Reform July 2015 SUMMARY POINTS Acquired Brain Injury Ireland (ABI Ireland) is asking the Government to support people living
FRESNO/KINGS/MADERA EMERGENCY MEDICAL SERVICES
 FRESNO/KINGS/MADERA EMERGENCY MEDICAL SERVICES HEALTH SERVICES AGENCY POLICIES AND PROCEDURES Manual Subject References Emergency Medical Services Administrative Policies and Procedures Pediatric Critical
FRESNO/KINGS/MADERA EMERGENCY MEDICAL SERVICES HEALTH SERVICES AGENCY POLICIES AND PROCEDURES Manual Subject References Emergency Medical Services Administrative Policies and Procedures Pediatric Critical
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
Improving Emergency Care in England
 Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Stroke Telemedicine Services: A Guide to the Commissioning and Provision
 Stroke Telemedicine Services: A Guide to the Commissioning and Provision Author: Professor Tony Rudd, National Clinical Director for Stroke Date: December 2014 First produced in August 2010 by Dr Damian
Stroke Telemedicine Services: A Guide to the Commissioning and Provision Author: Professor Tony Rudd, National Clinical Director for Stroke Date: December 2014 First produced in August 2010 by Dr Damian
British Cardiovascular Society: Guidance on appropriate workload for consultant cardiologists
 Page 1 of 9 British Cardiovascular Society: Guidance on appropriate workload for consultant cardiologists David Hackett Vice-President, Clinical Standards Division March 2010 Introduction: The British
Page 1 of 9 British Cardiovascular Society: Guidance on appropriate workload for consultant cardiologists David Hackett Vice-President, Clinical Standards Division March 2010 Introduction: The British
Chapter 23. New Criteria Quick Reference Guide Changes are noted in Orange
 Chapter 23 New Criteria Quick Reference Guide Changes are noted in Orange The preceding chapters of Resources for Optimal Care of the Injured Patient are designed to clearly define the criteria to verify
Chapter 23 New Criteria Quick Reference Guide Changes are noted in Orange The preceding chapters of Resources for Optimal Care of the Injured Patient are designed to clearly define the criteria to verify
www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862
 Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Effective Approaches in Urgent and Emergency Care. Priorities within Acute Hospitals
 Effective Approaches in Urgent and Emergency Care Paper 1 Priorities within Acute Hospitals When people are taken to hospital as an emergency, they want prompt, safe and effective treatment that alleviates
Effective Approaches in Urgent and Emergency Care Paper 1 Priorities within Acute Hospitals When people are taken to hospital as an emergency, they want prompt, safe and effective treatment that alleviates
Rehabilitation Network Strategy 2014 2017. Final Version 30 th June 2014
 Rehabilitation Network Strategy 2014 2017 Final Version 30 th June 2014 Contents Foreword 3 Introduction Our Strategy 4 Overview of the Cheshire and Merseyside Rehabilitation Network 6 Analysis of our
Rehabilitation Network Strategy 2014 2017 Final Version 30 th June 2014 Contents Foreword 3 Introduction Our Strategy 4 Overview of the Cheshire and Merseyside Rehabilitation Network 6 Analysis of our
ROYAL NATIONAL ORTHOPAEDIC HOSPITAL NHS TRUST CONSULTANT SPINAL SURGEON JOB DESCRIPTION
 ROYAL NATIONAL ORTHOPAEDIC HOSPITAL NHS TRUST CONSULTANT SPINAL SURGEON JOB DESCRIPTION TRUST PROFILE The Royal National Orthopaedic Hospital was founded in 1907 with the amalgamation of London s three
ROYAL NATIONAL ORTHOPAEDIC HOSPITAL NHS TRUST CONSULTANT SPINAL SURGEON JOB DESCRIPTION TRUST PROFILE The Royal National Orthopaedic Hospital was founded in 1907 with the amalgamation of London s three
Information for Adults with Physical Disabilities and Long Term Neurological Conditions
 Information for Adults with Physical Disabilities and Long Term Neurological Conditions Rehabilitation Medicine Service Community & Therapy Services Directorate of Operations This leaflet has been designed
Information for Adults with Physical Disabilities and Long Term Neurological Conditions Rehabilitation Medicine Service Community & Therapy Services Directorate of Operations This leaflet has been designed
How To Become A Physio And Rehabilitation Medicine Specialist
 EUROPEAN BOARD OF PHYSICAL AND REHABILITATION MEDICINE LOGBOOK EUROPEAN UNION OF MEDICAL SPECIALISTS UEMS IDENTIFICATION... 2 INSTRUCTIONS FOR USE... 3 THE TRAINING COURSE... 3 TRAINING PROGRAMME... 4
EUROPEAN BOARD OF PHYSICAL AND REHABILITATION MEDICINE LOGBOOK EUROPEAN UNION OF MEDICAL SPECIALISTS UEMS IDENTIFICATION... 2 INSTRUCTIONS FOR USE... 3 THE TRAINING COURSE... 3 TRAINING PROGRAMME... 4
4.2 Spinal Cord Compression
 4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
4.2 Spinal Cord Compression AO Protocol Name: Metastatic Spinal Cord Compression (MSCC) AO Type: Type I (New Cancer), Type III (Cancer Complication) Author: ST Introduction: MSCC can cause irreversible
Welcome to the Children s Epilepsy Surgery Service
 Welcome to the Children s Epilepsy Surgery Service Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Contents Introduction 3 My Team 4 The Epilepsy Team 5 Data collection
Welcome to the Children s Epilepsy Surgery Service Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Contents Introduction 3 My Team 4 The Epilepsy Team 5 Data collection
Physicians at-a-glance
 Ohio Physicians Neurosurgery Office UC Physicians Office - Clifton Expertise traumatic brain injury, intracerebral hemorrhage, stroke, carotid artery disease, moyamoya disease, brain tumors; spine surgery,
Ohio Physicians Neurosurgery Office UC Physicians Office - Clifton Expertise traumatic brain injury, intracerebral hemorrhage, stroke, carotid artery disease, moyamoya disease, brain tumors; spine surgery,
CARDIFF HEALTH SOCIAL CARE AND WELL BEING STRATEGY NEEDS ASSESSMENT COMMUNITY SERVICES/INTERMEDIATE CARE (6.6.2)
 CARDIFF HEALTH SOCIAL CARE AND WELL BEING STRATEGY NEEDS ASSESSMENT COMMUNITY SERVICES/INTERMEDIATE CARE (6.6.2) COMMUNITY SERVICES Cardiff and Vale NHS Trust, with its partners is reviewing Community
CARDIFF HEALTH SOCIAL CARE AND WELL BEING STRATEGY NEEDS ASSESSMENT COMMUNITY SERVICES/INTERMEDIATE CARE (6.6.2) COMMUNITY SERVICES Cardiff and Vale NHS Trust, with its partners is reviewing Community
CONTENTS Error! Bookmark not defined.
 GREATER MANCHESTER INTEGRATED STROKE SERVICE ESTABLISHING THE GOVERNANCE FRAMEWORK TO SUPPORT INTEGRATED ACUTE STROKE CARE 1 CONTENTS 1.0 INTRODUCTION...3 2.0 SERVICE AIMS...4 2.3 Comprehensive Stroke
GREATER MANCHESTER INTEGRATED STROKE SERVICE ESTABLISHING THE GOVERNANCE FRAMEWORK TO SUPPORT INTEGRATED ACUTE STROKE CARE 1 CONTENTS 1.0 INTRODUCTION...3 2.0 SERVICE AIMS...4 2.3 Comprehensive Stroke
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Assessment Blueprint for Stroke Medicine. Mini- DOPS MSF SESR CBD TP A R area
 Assessment Blueprint for troke Medicine DOP MF ER CBD TP A R 1. ACUTE TROE OBJECTIVE - TO PROVIDE THE TRAINEE WITH THE NOWLEDGE AND ILL TO CONTRIBUTE TO A COMPREHENIVE PECIALIT ERVICE FOR PATIENT WITH
Assessment Blueprint for troke Medicine DOP MF ER CBD TP A R 1. ACUTE TROE OBJECTIVE - TO PROVIDE THE TRAINEE WITH THE NOWLEDGE AND ILL TO CONTRIBUTE TO A COMPREHENIVE PECIALIT ERVICE FOR PATIENT WITH
Board of Directors. 28 January 2015
 Executive Summary Purpose: Board of Directors 28 January 2015 Briefing on the requirements for the Trust to comply with Hard Truths Commitments Regarding the Publishing of Staffing Data Director of Nursing
Executive Summary Purpose: Board of Directors 28 January 2015 Briefing on the requirements for the Trust to comply with Hard Truths Commitments Regarding the Publishing of Staffing Data Director of Nursing
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Managed Clinical Neuromuscular Networks
 Managed Clinical Neuromuscular Networks Registered Charity No. 205395 and Scottish Registered Charity No. SC039445 The case for Managed Clinical Neuromuscular Networks 1. Executive summary Muscular Dystrophy
Managed Clinical Neuromuscular Networks Registered Charity No. 205395 and Scottish Registered Charity No. SC039445 The case for Managed Clinical Neuromuscular Networks 1. Executive summary Muscular Dystrophy
Map 1 Statutory specialist services and organisations in England
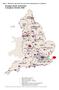 Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
POSITION DESCRIPTION
 POSITION DESCRIPTION POSITION TITLE REPORTS TO Exercise Physiologist Senior Clinician (Spinal Rehabilitation) AWARD/AGREEMENT/CONTRACT POSITION TYPE e.g. Registered Nurse Div 1, Occupational Therapist
POSITION DESCRIPTION POSITION TITLE REPORTS TO Exercise Physiologist Senior Clinician (Spinal Rehabilitation) AWARD/AGREEMENT/CONTRACT POSITION TYPE e.g. Registered Nurse Div 1, Occupational Therapist
Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required]
![Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required]](/thumbs/25/4903617.jpg) Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Medical Policy: MP-ME-05-09 Original Effective Date: February 18, 2009 Reviewed: April 22, 2011 Revised: This policy applies to products
Inpatient Rehabilitation Facilities (IRFs) [Preauthorization Required] Medical Policy: MP-ME-05-09 Original Effective Date: February 18, 2009 Reviewed: April 22, 2011 Revised: This policy applies to products
Patient Information Guide. Getting you Back to Better. 859.426.2400 www.vrhgateway.com
 Patient Information Guide Getting you Back to Better 859.426.2400 www.vrhgateway.com The Gateway Difference Gateway Rehabilitation Hospital provides expert care to help patients get back to better after
Patient Information Guide Getting you Back to Better 859.426.2400 www.vrhgateway.com The Gateway Difference Gateway Rehabilitation Hospital provides expert care to help patients get back to better after
CALVARY HEALTH CARE SYDNEY DAY REHABILITATION UNIT (DRU) JEREMEY HORNE
 CALVARY HEALTH CARE SYDNEY DAY REHABILITATION UNIT (DRU) JEREMEY HORNE DAY REHABILITATION UNIT OVERVIEW What is a DRU Minimum requirements Calvary Day Rehabilitation Admission Criteria Type of Patients
CALVARY HEALTH CARE SYDNEY DAY REHABILITATION UNIT (DRU) JEREMEY HORNE DAY REHABILITATION UNIT OVERVIEW What is a DRU Minimum requirements Calvary Day Rehabilitation Admission Criteria Type of Patients
Progress on the System Sustainability Programme. Submitted to: NHS West Norfolk CCG Governing Body, 31 July 2014
 Agenda Item: 9.1 Subject: Presented by: Progress on the System Sustainability Programme Dr Sue Crossman, Chief Officer Submitted to: NHS West Norfolk CCG Governing Body, 31 July 2014 Purpose of Paper:
Agenda Item: 9.1 Subject: Presented by: Progress on the System Sustainability Programme Dr Sue Crossman, Chief Officer Submitted to: NHS West Norfolk CCG Governing Body, 31 July 2014 Purpose of Paper:
Helen Fry Manager, Publications and Education Resources Joint Commission Resources
 July 2012 Dear Valued Customer: The Joint Commission developed a new Disease-Specific Care Advanced Certification Program for Comprehensive Stroke Centers (CSC) in collaboration with the American Heart
July 2012 Dear Valued Customer: The Joint Commission developed a new Disease-Specific Care Advanced Certification Program for Comprehensive Stroke Centers (CSC) in collaboration with the American Heart
Rehabilitation Medicine Service for Adults with Physical Disabilities
 Rehabilitation Medicine Service for Adults with Physical Disabilities Information for Professionals Rehabilitation Medicine Service Community & Therapy Services Group This leaflet has been designed to
Rehabilitation Medicine Service for Adults with Physical Disabilities Information for Professionals Rehabilitation Medicine Service Community & Therapy Services Group This leaflet has been designed to
REHABILITATION. begins right here
 REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
REHABILITATION begins right here Select Rehabilitation Hospital of Denton offers you a new direction in medical rehabilitation. Our 44-bed, state-of-the-science hospital offers unparalleled treatment to
Rehabilitation Following Major Trauma in Greater Manchester
 Rehabilitation Following Major Trauma in Greater Manchester Dr Krystyna Walton Consultant in Neurorehabilitation Director Greater Manchester Major Trauma Rehabilitation Major Trauma Rehabilitation in the
Rehabilitation Following Major Trauma in Greater Manchester Dr Krystyna Walton Consultant in Neurorehabilitation Director Greater Manchester Major Trauma Rehabilitation Major Trauma Rehabilitation in the
IMPROVING YOUR EXPERIENCE
 Comments trom the Aberdeen City Joint Futures Brain Injury Group The Aberdeen City Joint Futures Brain Injury Group is made up of representatives from health (acute services, rehabilitation and community),
Comments trom the Aberdeen City Joint Futures Brain Injury Group The Aberdeen City Joint Futures Brain Injury Group is made up of representatives from health (acute services, rehabilitation and community),
Acute care toolkit 2
 Acute care toolkit 2 High-quality acute care October 2011 Consultant physicians are at the forefront of delivering care to patients presenting to hospital with medical emergencies. Delivering this care
Acute care toolkit 2 High-quality acute care October 2011 Consultant physicians are at the forefront of delivering care to patients presenting to hospital with medical emergencies. Delivering this care
New Technologies and Their Role in Enhancing Neurological Recovery
 REHABILITATION CARE 2014: under the ACA Patient Centered Medical Home for Persons with Disability: Acute Neurology, Medicine, Surgery services seamlessly blending into Acute inpatient Rehabilitation Ambulatory
REHABILITATION CARE 2014: under the ACA Patient Centered Medical Home for Persons with Disability: Acute Neurology, Medicine, Surgery services seamlessly blending into Acute inpatient Rehabilitation Ambulatory
OhioHealth Neuroscience
 SEPTEMBER/OCTOBER 2013 OhioHealth Neuroscience CLINICAL UPDATE IN THIS ISSUE: NEW SERVICES OhioHealth advancing many of its programs across the neuroscience continuum of care NEW FACILITY OhioHealth Rehabilitaton
SEPTEMBER/OCTOBER 2013 OhioHealth Neuroscience CLINICAL UPDATE IN THIS ISSUE: NEW SERVICES OhioHealth advancing many of its programs across the neuroscience continuum of care NEW FACILITY OhioHealth Rehabilitaton
BSRM Standards for Rehabilitation Services Mapped on to the National Service Framework for Long-Term Conditions
 BSRM Standards for Rehabilitation Services Mapped on to the National Service Framework for Long-Term Conditions British Society of Rehabilitation Medicine C/o Royal College of Physicians, 11 St Andrews
BSRM Standards for Rehabilitation Services Mapped on to the National Service Framework for Long-Term Conditions British Society of Rehabilitation Medicine C/o Royal College of Physicians, 11 St Andrews
GENERAL ADMISSION CRITERIA INPATIENT REHABILITATION PROGRAMS
 Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
Originator: Case Management Original Date: 9/94 Review/Revision: 6/96, 2/98, 1/01, 4/02, 8/04, 3/06, 03/10, 3/11, 3/13 Stakeholders: Case Management, Medical Staff, Nursing, Inpatient Therapy GENERAL ADMISSION
Guidance for commissioners: service provision for Section 136 of the Mental Health Act 1983
 Guidance for commissioners: service provision for Section 136 of the Mental Health Act 1983 Position Statement PS2/2013 April 2013 London Approved by the multi-agency Mental Health Act group chaired by
Guidance for commissioners: service provision for Section 136 of the Mental Health Act 1983 Position Statement PS2/2013 April 2013 London Approved by the multi-agency Mental Health Act group chaired by
Requirements for Provision of Outreach Paediatric Cardiology Service
 Requirements for Provision of Outreach Paediatric Cardiology Service Dr Shakeel A Qureshi, Consultant Paediatric Cardiologist, Evelina Children s Hospital, London, UK On behalf of British Congenital Cardiac
Requirements for Provision of Outreach Paediatric Cardiology Service Dr Shakeel A Qureshi, Consultant Paediatric Cardiologist, Evelina Children s Hospital, London, UK On behalf of British Congenital Cardiac
Accreditation and Certification Guidelines
 Accreditation and Certification Guidelines MARTIN GIZZI, MD, PHD, FAHA CHAIR, NJ NEUROSCIENCE INSTITUTE AT JFK CHAIR, NORTH EAST CEREBROVASCULAR CONSORTIUM (NECC) CHAIR, STROKE ADVISORY PANEL, NJDOH MEMBER,
Accreditation and Certification Guidelines MARTIN GIZZI, MD, PHD, FAHA CHAIR, NJ NEUROSCIENCE INSTITUTE AT JFK CHAIR, NORTH EAST CEREBROVASCULAR CONSORTIUM (NECC) CHAIR, STROKE ADVISORY PANEL, NJDOH MEMBER,
Managed Service Network for Neurosurgery
 Managed Service Network for Neurosurgery Business Plan 2012-2015 MSN Business Plan diana.beard@nhslothian.scot.nhs.uk Contents 1. Vision of the MSN for Neurosurgery 2. Key Customers / Stakeholders 3. Aims
Managed Service Network for Neurosurgery Business Plan 2012-2015 MSN Business Plan diana.beard@nhslothian.scot.nhs.uk Contents 1. Vision of the MSN for Neurosurgery 2. Key Customers / Stakeholders 3. Aims
The case for a dedicated Paediatric Emergency and Trauma department at Southampton Children s Hospital
 The case for a dedicated Paediatric Emergency and Trauma department at Southampton Children s Hospital Part of University Hospital Southampton NHS Foundation Trust Overview We re seeking 2m capital cost
The case for a dedicated Paediatric Emergency and Trauma department at Southampton Children s Hospital Part of University Hospital Southampton NHS Foundation Trust Overview We re seeking 2m capital cost
Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation
 Health Informatics Unit Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation April 2011 Funded by: Acknowledgements This project was funded by the Academy of
Health Informatics Unit Evidence on the quality of medical note keeping: Guidance for use at appraisal and revalidation April 2011 Funded by: Acknowledgements This project was funded by the Academy of
BRIEFING PAPER STROKE SERVICES REDESIGN
 1. Introduction BRIEFING PAPER STROKE SERVICES REDESIGN Agenda Item 3 Stroke is the leading cause of adult disability in Wales, and the third most common cause of death, after cancer and heart disease.
1. Introduction BRIEFING PAPER STROKE SERVICES REDESIGN Agenda Item 3 Stroke is the leading cause of adult disability in Wales, and the third most common cause of death, after cancer and heart disease.
How To Become A Royal Perth Hospital Graduate Nurse
 www.nursingwa.com.au > graduate info 1...the Career of a Lifetime > Graduate Nurse Programs > graduate info AT RPH, WE OFFER OUR NURSES EXCEPTIONAL CAREER OPPORTUNITIES ACROSS A COMPREHENSIVE RANGE OF
www.nursingwa.com.au > graduate info 1...the Career of a Lifetime > Graduate Nurse Programs > graduate info AT RPH, WE OFFER OUR NURSES EXCEPTIONAL CAREER OPPORTUNITIES ACROSS A COMPREHENSIVE RANGE OF
The Regulation and Quality Improvement Authority. Review of Brain Injury Services in Northern Ireland
 The Regulation and Quality Improvement Authority Review of Brain Injury Services in Northern Ireland September 2015 Assurance, Challenge and Improvement in Health and Social Care www.rqia.org.uk The Regulation
The Regulation and Quality Improvement Authority Review of Brain Injury Services in Northern Ireland September 2015 Assurance, Challenge and Improvement in Health and Social Care www.rqia.org.uk The Regulation
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, post-polio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Stroke rehabilitation
 Costing report Stroke rehabilitation Published: June 2013 http://guidance.nice.org.uk/cg162 This costing report accompanies the clinical guideline: Stroke rehabilitation (available online at http://guidance.nice.org.uk/cg162).
Costing report Stroke rehabilitation Published: June 2013 http://guidance.nice.org.uk/cg162 This costing report accompanies the clinical guideline: Stroke rehabilitation (available online at http://guidance.nice.org.uk/cg162).
Profile: Kessler Patients
 Profile: Kessler Patients 65 Breakthrough Years Kessler Institute has pioneered the course of medical rehabilitation since 1948. Today, as the nation s largest single rehabilitation hospital, we continue
Profile: Kessler Patients 65 Breakthrough Years Kessler Institute has pioneered the course of medical rehabilitation since 1948. Today, as the nation s largest single rehabilitation hospital, we continue
University Rehabilitation Institute Republic of Slovenia. Helena Burger, Metka Teržan University Rehabilitation Institute, Ljubljana, Slovenia
 University Rehabilitation Institute Republic of Slovenia Helena Burger, Metka Teržan University Rehabilitation Institute, Ljubljana, Slovenia 2 3 Introduction * Primary level PT only * Secondary level:
University Rehabilitation Institute Republic of Slovenia Helena Burger, Metka Teržan University Rehabilitation Institute, Ljubljana, Slovenia 2 3 Introduction * Primary level PT only * Secondary level:
