Complete Blood Count in Primary Care
|
|
|
- Lindsey Edwards
- 9 years ago
- Views:
Transcription
1 Complete Blood Count in Primary Care bpac nz better medicine
2 Editorial Team Tony Fraser Professor Murray Tilyard Clinical Advisory Group Dr Dave Colquhoun Michele Cray Dr Rosemary Ikram Dr Peter Jensen Dr Cam Kyle Dr Chris Leathart Dr Lynn McBain Associate Professor Jim Reid Dr David Reith Professor Murray Tilyard bpac nz 10 George Street PO Box 6032, Dunedin phone free fax 0800 bpac nz Programme Development Team Noni Allison Rachael Clarke Rebecca Didham Terry Ehau Peter Ellison Dr Malcolm Kendall-Smith Dr Anne Marie Tangney Dr Trevor Walker Dr Sharyn Willis Dave Woods Report Development Team Justine Broadley Todd Gillies Lana Johnson Web Gordon Smith Design Michael Crawford Management and Administration Kaye Baldwin Tony Fraser Kyla Letman Professor Murray Tilyard Distribution Zane Lindon Lyn Thomlinson Colleen Witchall May 2008 All information is intended for use by competent health care professionals and should be utilised in conjunction with pertinent clinical data.
3 Contents Key points/purpose 2 Introduction 2 Background Haematopoiesis - Cell development 3 Limitations of reference ranges for the CBC 4 Borderline abnormal results must be interpreted in clinical context 4 History and clinical examination 4 White Cells Neutrophils 5 Lymphocytes 9 Monocytes 11 Basophils 12 Eosinophils 12 Platelets 13 Haemoglobin and red cell indices Low haemoglobin 15 Microcytic anaemia 15 Normocytic anaemia 16 Macrocytic anaemia 17 High haemoglobin 17 Other red cell indices 18 Summary Table 19 Glossary 20 This resource is a consensus document, developed with haematology and general practice input. We would like to thank: Dr Liam Fernyhough, Haematologist, Canterbury Health Laboratories Dr Chris Leathart, GP, Christchurch Dr Edward Theakston, Haematologist, Diagnostic Medlab Ltd We would like to acknowledge their advice, expertise and valuable feedback on this document. Complete Blood Count 1
4 Key points/purpose To provide an overview of the use of the complete blood count in primary care and to provide advice on appropriate follow-up for abnormal results. Introduction The complete blood count (CBC) is the most frequently requested blood test in New Zealand. The primary points of interest in the CBC are often whether a patient is anaemic, whether the white count shows evidence of infection and whether the platelets are at a level that may affect haemostasis. GPs have told us they are reasonably comfortable interpreting CBC results with marked abnormalities, but would like guidance when the results show only subtle abnormalities or when the clinical picture is not clear. This is a consensus document This is not a comprehensive document covering all causes of abnormal results; it is a consensus document produced in conjunction with specialist haematologists, providing an overview for some scenarios encountered in primary care. 2 Complete Blood Count
5 Background Haematopoiesis Cell development All blood cells are produced within the bone marrow from a small population of stem cells. Less than one in 5000 of the marrow cells is a stem cell. These cells represent a self-renewing population. The term haematopoiesis refers to the formation and development of the blood cells (Figure 1). In humans the bone marrow is the major site of haematopoiesis for the life of the individual. Initial differentiation of haemopoietic stem cells involves one of two pathways, lymphoid or myeloid. Stem cells then become progenitor cells for each type of mature blood cell and are committed to a given cell lineage. Myeloid stem cells eventually give rise to erythrocytes, megakaryocytes (platelets), neutrophils, monocytes, eosinophils and basophils. Lymphoid stem cells give rise to T and B lymphocytes and plasma cells. Figure 1: Haematopoiesis cell development pathways. Haematopoietic Stem Cell Myeloid Stem Cell Lymphoid Stem Cell Myeloblast Pronormoblast N. Promyelocyte Basophilic Normoblast N. Myelocyte Polychromatic Normoblast Immature Basophil Immature Eosinophil N. Metamyelocyte Immature Monocyte Megakaryocyte Orthochromatic Normoblast N. band Polychromatic Erythrocyte Basophil Eosinophil Neutrophil Monocyte Platelets Erythrocyte Lymphocyte Complete Blood Count 3
6 Limitations of reference ranges for the CBC For most people conventional reference ranges will be adequate for diagnostic purposes, but a number of pitfalls may make interpretation more difficult in some cases. Deriving blood count reference ranges is difficult due to the number of factors that may affect blood count parameters and their frequency in the community. These include iron deficiency, thalassaemias, medication, alcohol and minor infections. In addition there are ethnic differences in some parameters, differences between males and females and differences in pregnancy. Some of these factors are taken into account in published ranges (gender, pregnancy) others are not. Finally, there are differences between different haematology analysers that may affect some blood count parameters. In view of the above, the approach taken to blood count reference intervals has been different to that seen with many biochemical parameters, where reference intervals usually encompass the 2.5th to 97.5th percentiles. Blood count reference intervals have been derived using a mixture of local and published data, together with a degree of pragmatism. This means that many of the reference intervals encompass more than 95% of normal individuals and marginal results must be considered in context. Likewise, a normal blood count does not preclude the possibility of early disease states (e.g. iron deficiency). Borderline abnormalities must be interpreted in clinical context All haematology results need to be interpreted in the context of a thorough history and physical examination, as well as previous results. Follow-up counts are often helpful to assess marginal results as many significant clinical conditions will show progressive abnormalities. The CBC is often included as part of a well-person check, or as part of a series of screening tests for life or health insurance applicants. While a number of organisations are advocating well-person checks, others argue that blood tests are not indicated for well people. In asymptomatic people, the pre-test probability for tests is low, leading to a high rate of false positives. In addition, undertaking investigations in people who do not have a clear clinical need will use resources (time and money) that could be better applied to those with unmet health care needs. History and clinical examination There are a number of features which may be revealed by history and clinical examination. These can provide clues for diagnosis and allow the results of the complete blood count to be interpreted in context. Signs and symptoms relevant to the CBC: Pallor, jaundice Fever, lymphadenopathy Bleeding/bruising Hepatomegaly, splenomegaly Frequency and severity of infections, mouth ulcers, recent viral illness Exposure to drugs and toxins including herbal remedies Fatigue/weight loss 4 Complete Blood Count
7 White Cells Total White blood cell count may be misleading Although the total white count may provide a useful summary, the absolute count of each of the cell types is more useful than the total. The total white count may be misleading; e.g. abnormally low neutrophils with an elevated lymphocyte count may produce a total white count that falls within the reference range. As a result the total white count should not be considered in isolation. Neutrophils For most adults neutrophils account for approximately 70% of all white blood cells. The normal concentration range of neutrophils is /L (range can be different for different labs). The average half-life of a non-activated neutrophil in the circulation is about 4 10 hours. Upon migration, outside the circulation, neutrophils will survive for 1 2 days. Neutropenia (low neutrophil count) Neutropenia is potentially associated with life threatening infection. It is most significant when the total neutrophil count is less than /L, particularly when the neutropenia is due to impaired production (e.g. after chemotherapy). When the neutropenia is due to increased peripheral destruction or margination (e.g. with viral infection), it is less certain what constitutes a significant level. These patients rarely have problems with significant bacterial infection despite quite low neutrophil counts. Neutropenia can be classified as: Classification Neutrophil count Mild /L Moderate /L Severe < /L Neutrophils Low Significant levels < /L (high risk infection) Most common causes Viral (overt or occult) Autoimmune/idiopathic Drugs Red flags Person particularly unwell Severity of neutropenia Rate of change of neutropenia Lymphadenopathy, hepatosplenomegaly Complete Blood Count 5
8 Approach to patients with neutropenia Neutrophils < /L: The risk of significant bacterial infection rises as the neutrophil count drops below /L, but is most marked as the count falls below /L. Careful assessment of the patient s condition is critical, and patients who are unwell and/or febrile with a count below /L generally need urgent referral. Patients who are febrile but otherwise well should at least be discussed with a Haematologist. If the patient is well and afebrile, they need to be advised to seek medical attention promptly if their condition deteriorates or they become febrile. Well patients should have follow up blood counts within 48 hours, and if the neutropenia persists at this level or progresses they should be discussed with a Haematologist. Neutrophils /L: If an isolated abnormality follow up blood counts are indicated, with frequency dependent on the severity of the neutropenia but usually within 1-2 weeks. If the neutropenia persists for more than 6 weeks further investigation is indicated. If it is progressive or other abnormalities develop a haematology referral, or discussion with a Haematologist, is indicated. Drug induced neutropenias: There are specific protocols for management of clozapine induced neutropenia. Otherwise, if a drug cause is suspected and the neutropenia is moderate or severe, Haematology referral, or discussion with a Haematologist is indicated. Causes In routine clinical practice the most frequent cause of a low neutrophil count is overt or occult viral infection, including viral hepatitis. Acute changes are often noted within one to two days of infection and may persist for several weeks. The neutrophil count seldom decreases enough to pose a risk of infection. medications, antibiotics, antirheumatics, antipsychotics and anticonvulsants. For a more comprehensive list see Neutropenia, drug induced on Page 20. Many drugs may cause a chronic mild neutropenia e.g. nonsteroidal anti-inflammatory drugs, valproic acid. A low neutrophil count is often discovered in some people as an incidental finding in the CBC result. The patient is generally asymptomatic and the clinical examination is unremarkable. The count is usually stable on follow-up. This is likely to be idiopathic although in some cases a neutropenia may be associated with splenomegaly or an autoimmune disease such as lupus. The presentation of a haematological malignancy with only an isolated neutropenia is a rare finding. Drugs causing neutropenia Although relatively rare, drug therapy may cause an acquired neutropenia in some people. The drugs most likely to be associated with moderate neutropenia are chemotherapy and immunosuppressive drugs, antithyroid Investigations The history and clinical features are important for providing the clues for diagnosis and allowing the results to be interpreted in context. History: frequency and severity of infections, mouth ulcers, recent viral illness, exposure to drugs and toxins, symptoms of malabsorption, symptoms suggesting reduced immunity Drugs (see Neutropenia, drug induced on Page 20). Examination: mouth ulcers, fever, signs of infection, jaundice, lymphadenopathy, hepatomegaly, splenomegaly, signs of autoimmune/connective tissue disorders CBC: is the CBC otherwise normal (particularly haemoglobin and platelets) 6 Complete Blood Count
9 In persistent moderate neutropenia, without an infection or drug related cause, testing might include ANA (anti-nuclear antibodies), B12, folate, SPE (serum protein electrophoresis), HIV, liver enzymes, Hepatitis B and rheumatoid factor. Look for changes on physical examination. Significant red flags Patient unwell Persistence/duration of neutropenia, rate of change Severity Significant findings on physical examination Neutrophilia (high neutrophil count) Neutrophils are the primary white blood cells that respond to a bacterial infection. The most common cause of marked neutrophilia is a bacterial infection. Neutrophils react within an hour of tissue injury and are the hallmark of acute inflammation. An excessive increase in neutrophils (> /L) as a reactive phenomenon is known as a leukaemoid reaction. Neutrophils generally exhibit characteristic changes in response to infection. The neutrophils tend to be more immature, as they are being released earlier. This is called a left shift (Figure 2). In a severe infection the neutrophils may show toxic granulation and other toxic changes such as vacuolation and the presence of Döhle bodies. Neutrophils High Most likely cause Infection/inflammation Necrosis Any stressor/heavy exercise Drugs Pregnancy Smoking CML Red flags Person particularly unwell Severity of neutrophilia Rate of change of neutrophilia Presence of left shift Neutrophils will frequently be increased in any acute inflammation, therefore will often be raised after a heart attack, or other infarct and necrosis. Any stressor, from heavy exercise to cigarette smoking, can elevate the neutrophil count. A number of drugs have been demonstrated to increase the neutrophil count, including steroids, lithium, clozapine and adrenalin. Even nervousness may very slightly raise the neutrophil count because of the effect of steroid release. Pregnancy is associated with a slight increase in total neutrophil count demonstrating a left shift. Most laboratories provide pregnancy specific reference ranges. Complete Blood Count 7
10 Persistent elevation of neutrophils may be a sign of chronic myeloid leukaemia (CML). Characteristic changes are a moderate increase in neutrophil count (usually > /L), with a left shift and a prominence of myelocytes. Basophilia and/or eosinophilia may also be present. Chronic mild neutrophilia without left shift is very unlikely to be due to CML. Follow-up for high neutrophil count For essentially well people: Repeat in 1 2 months, then Continue to follow (3 monthly for 12 months, then occasionally thereafter) Stop monitoring when normal CML occurs in all age groups but most commonly in the middle aged and elderly. The annual incidence is estimated at 1 2 cases per 100,000. Figure 2: Diagram of left shift normal mild moderate left shift severe left shift Increasing Neutrophil Maturity 8 Complete Blood Count
11 Lymphocytes Lymphocytes normally represent 20 40% of circulating white blood cells. The normal concentration of lymphocytes is between /L. There are two broad morphologic categories of lymphocytes which can be distinguished under the light microscope, large granular lymphocytes and small lymphocytes. Functionally distinct subsets of lymphocytes do not correlate with their appearance. lymphocytopenia (low lymphocyte count) Low lymphocyte counts are not usually significant. Characteristic decreases in the lymphocyte count are usually seen late in HIV infection, as T lymphocytes (CD4+ T cells) are destroyed. Steroid administration may reduce lymphocyte counts. More rarely lymphocytopenia may be caused by some types of chemotherapy or malignancies. People exposed to large doses of radiation, such as those involved with situations like Chernobyl, can have severe lymphocytopenia. Lymphocyte Low Not usually clinically significant Lymphocyte High Causes Acute infection (viral, bacterial) Smoking Hyposplenism Acute stress response Autoimmune thyroiditis CLL Lymphocytosis (high lymphocyte count) Increases in the absolute lymphocyte count are usually due to acute infections, such as Epstein-Barr virus infection and viral hepatitis. Less commonly, increased lymphocytes may be the result of pertussis and toxoplasmosis or (rarely) chronic intracellular bacterial infections such as tuberculosis or brucellosis. The lymphocyte count may also be elevated in: Smoking (reactive) Hyposplenism (usually following splenectomy) Complete Blood Count 9
12 Acute stress response usually seen in hospital setting, uncommon in community, usually resolves within 24 hours Acute cardiac event Trauma Autoimmune thyroiditis Chronic lymphocytic leukaemia (CLL) and other lymphoproliferative disorders should be considered in patients with a persistent lymphocytosis. CLL is rarely encountered in people under the age of 40 but increases in incidence with age. It is often discovered as an incidental finding on a blood count, but may be associated with lymphadenopathy, hepatomegaly and splenomegaly. In some cases lymphocyte surface markers may be recommended for differentiating between reactive lymphocytosis and lymphoproliferative disorders. Because they do not affect management of asymptomatic patients with early stage disease, they are usually only indicated when the lymphocyte count is persistently > /L; the lymphocytes demonstrate abnormal features; other blood count parameters are abnormal; or there are signs or symptoms suggestive of lymphoma (fever, sweats, weight loss, lymphadenopathy, hepatosplenomegaly). Inappropriate use should be avoided because the test is particularly expensive around $500. Follow-up Follow-up for clinically unexplained lymphocytosis: In a patient who appears to be essentially well and has no alarming features, check in one to two months. In a patient with mild symptoms of a transient condition, rechecking when the patient is well is appropriate. Patients with persistently elevated lymphocyte count, accompanied by lymphadenopathy, hepatomegaly and splenomegaly should be referred for haematology assessment. 10 Complete Blood Count
13 Monocytes Monocytes constitute between 3 8% of all white cells in the blood. They circulate in the bloodstream for about one to three days and then typically move into tissues (approx 8 12 hours) to sites of infection. The normal concentration of monocytes is between /L. Monocytes which migrate from the bloodstream to other tissues are called macrophages. Macrophages have a role in specific immunity and phagocytosis. Monocytopenia (low monocyte count) An isolated decrease in the total monocyte count is an unusual finding. Occasionally monocytes become depleted in overwhelming bacterial infections, but this is more an incidental finding than a defining clinical indicator. Hairy cell leukaemia, a rare indolent lymphoproliferative disorder, may occasionally be associated with monocytopenia, although other abnormalities (especially neutropenia and lymphocytosis) would generally be present. Monocytes Low Not clinically significant if other cell counts are normal Monocytes High Usually not significant Watch levels > /L more closely, consider chronic infection or inflammation. Monocytosis (high monocyte count) Most often, elevated monocyte counts are associated with infection and inflammatory processes and will be seen in conjunction with other blood count changes. Isolated increases in the monocyte count, not accompanied by other changes in the blood count, are uncommon but may be associated with: Chronic infection including tuberculosis Chronic inflammatory conditions (e.g. Crohn s disease, ulcerative colitis, rheumatoid arthritis, SLE) Dialysis Early sign of chronic myelomonocytic leukaemia (rare) If levels are persistently elevated (i.e. > /L), particularly in association with suspicious symptoms, a haematology referral may be prudent. A mild elevation of monocytes is relatively common and does not usually require follow-up. Complete Blood Count 11
14 Basophils Basophils are the least common of the white cells, representing about % of all white blood cells. The normal concentration of basophils is /L The function of basophils is not fully understood, but it is known that they are capable of phagocytosis and producing histamine. Basopenia (low basophil count) Basopenia is difficult to demonstrate as the normal basophil count is so low. Basophils Low Difficult to demonstrate Basophils High Associated with: Myeloproliferative disorders Other rare causes Basophilia (high basophil count) The basophil count will only very rarely be significantly raised. When present, it may indicate a myeloproliferative disorder, or other more obscure causes. A repeat CBC a week or two later may help. Eosinophils In most people eosinophils make up about 1 6% of white blood cells. The normal concentration of eosinophils is /L. Eosinophils persist in the circulation for 8 12 hours, and can survive in tissue for an additional 8 12 days in the absence of stimulation. Eosinopenia (Low eosinophil count) Eosinopenia is difficult to demonstrate in practice because of the low frequency of eosinophils in most healthy people. As a result a low eosinophil count should not be a cause for concern. Eosinophilia (high eosinophil count) In developed countries the most common causes are allergic diseases such as asthma and hay fever, but Eosinophils Low No real cause for concern Eosinophils High Most common causes: Allergy/atopy: asthma/hayfever Parasites (less common in developed countries) Rarer causes: Hodgkins disease Myeloproliferative disorders Churg-Strauss syndrome 12 Complete Blood Count
15 worldwide the main cause of increased eosinophils is parasitic infection. Follow-up Haematology assessment is appropriate for patients with persistent (more than six months) moderate eosinophilia, or marked or increasing eosinophilia. Total eosinophil count Follow-up < /L Trivial, ignore Up to /L Probably, ignore > /L Consider possible causes Platelets Platelets are produced by budding off from megakaryocytes in the bone marrow. Each megakaryocyte produces between 5,000 to 10,000 platelets. Platelets circulate for approximately one to two weeks and are destroyed by the spleen and liver. A normal platelet count ranges from /L. thrombocytopenia (LOW Platelet COUNT) Interpretation of a low platelet count involves consideration of the clinical context. Severe thrombocytopenia is associated with an increased risk of bleeding and requires urgent assessment. It is particularly significant if accompanied by other changes in the CBC or the platelet count is falling. Bleeding is unusual at platelet counts of > /L unless there is an associated platelet function defect (which is uncommon). Platelets Low Significant levels < /L Most common causes Viral infection Idiopathic thrombocytopenic purpura Liver disease Medications Hypersplenism Autoimmune disease Pregnancy Red flags Bruising Petechiae Signs of bleeding Causes Thrombocytopenia may be artefactual due to a variety of causes, which are worth excluding before looking for clinical causes, including: Partially clotted sample. Platelet clumping in the blood collection tube. The laboratory will usually look for evidence of these, but if the platelet count is not consistent with the clinical picture, a repeat sample may be warranted. Complete Blood Count 13
16 Causes of isolated thrombocytopenia include: Viral infection Idiopathic thrombocytopenic purpura (ITP) Medications Liver disease Autoimmune disease Hypersplenism HIV infection Pregnancy Bone marrow causes Thrombocytopenia may also occur in conjunction with microangiopathic haemolysis (usually apparent on blood film examination) in haemolytic uraemic syndrome (HUS), thrombotic thrombocytopenic purpura (TTP) and chronic or acute disseminated intravascular coagulation (DIC). TTP should be considered if the patient is febrile, unwell or has neurological symptoms. Follow-up Low platelets are reasonably common, but it is important that results be interpreted in context, looking for clues to help. Further testing that should be considered in patients with persistently low platelets includes a blood film, ANA (anti-nuclear antibodies), HIV, Hepatitis B and C and liver enzymes. In some cases of chronic thrombocytopenia, Helicobacter pylori serology and anticardiolipin antibodies may be indicated. Splenomegaly and lymph nodes should be checked on examination. Recommended follow up for thrombocytopenia: Platelet count Referral < /L Requires urgent referral /L Judgment depending on context. Urgent referral if bleeding. Needs further investigation if persistent/ progressive. Refer if no cause found /L Follow up counts. Investigate if persistent. Refer if progressive without obvious cause. thrombocytosis (high Platelet COUNT) Elevated platelet levels may be a reactive change and will not necessarily signal any clinical problem. Generally, a reactive thrombocytosis is not associated with an increased thrombotic risk. Rarely will a thrombocytosis reflect a myeloproliferative disorder such as essential thrombocythaemia or myelofibrosis. These should particularly be considered if there is a chronic persistent elevation in platelet counts (more than six months) or a very high platelet count without an obvious reactive cause. They may also be associated with splenomegaly and the platelet count is usually > /L (and often much higher). Platelets High Significant levels > /L Most likely causes Reactive conditions e.g. infection, inflammation Pregnancy Iron deficiency Post splenectomy Essential thrombocythaemia 14 Complete Blood Count
17 Haemoglobin and red cell indices Low haemoglobin Low haemoglobin levels are generally indicative of anaemia. Most laboratories report a haemoglobin level of less than 130 g/l for men as low. The lower limit of the reference range for women is usually presented as 115 g/l but some laboratories use a value of 120 g/l. Anaemia requires careful consideration. The wide differential diagnosis can be narrowed considerably by checking the mean cell volume (MCV) and the reticulocyte count and initially classifying the anaemia as: Microcytic, MCV < 80 fl Normocytic, MCV fl Macrocytic, MCV > 100 fl Microcytic Anaemia The three most common causes for microcytic anaemia are: Iron deficiency Thalassaemia Anaemia of Chronic disease A suggested approach to laboratory testing is shown in Figure 3. Iron deficiency is the most common cause of microcytic anaemia, therefore measurement of serum ferritin is the appropriate first step. A low ferritin in the presence of a microcytic anaemia is diagnostic of iron deficiency. Patients with low normal ferritin levels (<30 μg/l) may well have a latent iron deficient state. Iron deficiency can not be excluded in a person with concurrent inflammation, despite a normal ferritin, and requesting a CRP may be useful to exclude inflammation. Microcytic anaemia not related to iron deficiency When microcytic anaemia is not due to iron deficiency it is most likely related to thalassaemia or an underlying chronic disease. Thalassaemias are associated with chronic microcytosis with no or mild anaemia. They are seen with high frequency in a number of ethnic groups, including Māori and Pacific Peoples, Asians and those of Mediterranean or Middle Eastern origin. Appropriate investigation includes ferritin and a haemoglobinopathy screen. For some patients with milder forms of alpha thalassaemia the haemoglobinopathy screen may be negative. Microcytic anaemia of chronic disease is most frequently associated with: Chronic inflammation Chronic infection The microcytosis is usually only mild and many patients with anaemia of chronic disease are normocytic. Complete Blood Count 15
18 Figure 3: A suggested approach to laboratory testing for microcytic anemia. Microcytic anaemia Check serum ferritin Low Normal or elevated Iron deficiency anaemia Check for inflammation clinical and/or CRP Inflammation present No inflammation Consider anaemia of chronic disease. Consider thalassaemia Check full iron studies to ensure not iron deficient Normocytic anaemia The causes of normocytic anaemia include: Bleeding Early nutritional anaemia (iron, B12, folate deficiencies) Anaemia of renal insufficiency Anaemia of chronic disease/chronic inflammation Haemolysis Primary bone marrow disorder Initial investigation in primary care generally focuses on the tests listed below. These will depend on history and examination, potential sources of bleeding, diet and general health status. Testing may include: Ferritin, B12, folate Creatinine Reticulocyte count CRP Liver enzymes Serum Protein Electrophoresis If the reticulocyte count is elevated the differential is small and includes blood loss, haemolysis and hypersplenism. If the clinical features and results of these tests are inconclusive a haematological opinion may be appropriate. 16 Complete Blood Count
19 Figure 4: A suggested approach to laboratory testing for macrocytic anemia. Macrocytic anaemia Consider drugs and alcohol B12, folate Low result Normal Investigate/Treat Check Liver function, thyroid function, reticulocytes, SPE No diagnosis Not significantly anaemic Anaemic Consider alcohol. If other CBC parameters are normal then observe. Consider haematology referral for bone marrow Macrocytic anaemia Common causes of macrocytosis include alcohol, liver disease, B12 or folate deficiency, thyroid disease and some drugs (especially hydroxyurea). Macrocytosis may be present without anaemia. A reticulocytosis may also elevate the MCV and a reticulocyte count should be checked. Severe hypothyroidism may cause a macrocytosis, but is usually clinically apparent. Investigation in primary care includes history and examination, and laboratory testing. A suggested diagnostic approach to macrocytosis is shown in Figure 4. The frequently requested tests include: B12 and folate A blood film Reticulocyte count Liver enzymes TSH RAPS4 Alcohol Screening Test for dependent drinking may be useful (see over page). When these investigations are normal, and the anaemia is significant, bone marrow disorders may need to be excluded. High haemoglobin Elevated haemoglobin and PCV (packed cell volume or haemocrit ) levels can reflect decreased plasma Complete Blood Count 17
20 volume (due to dehydration, alcohol, cigarette smoking, diuretics) or increased red cell mass (polycythaemia). Polycythaemia may be secondary (usually to chronic hypoxia, but occasionally to erythropoietin-secreting tumours, especially renal tumours, fibroids) or primary (polycythaemia vera). Unless the haemoglobin/pcv is very high it is usually advisable to repeat the blood count ensuring adequate hydration. A PCV of > 0.52 in men and > 0.47 in women needs to be confirmed in a specimen taken without venous occlusion. A confirmed PCV above these levels, in the absence of an obvious secondary cause, is an indication for a haematological opinion because of the high risk of stroke and other adverse events for people with polycythaemia vera. Other Red cell indices (Red cell count, RDW, MCH, MCHC) These red cell indices are useful for building a picture of many patterns suggested by the haemoglobin. There are limited situations in which isolated abnormalities of these indices are useful and not all of the indices are reported by all laboratories. The RAPS4 Alcohol Screening Test for dependent drinking Ask the patient the following four questions: During the last year have you had a feeling of guilt or remorse after drinking? During the last year has a friend or a family member ever told you about things you said or did while you were drinking that you could not remember? During the last year have you failed to do what was normally expected from you because of drinking? Do you sometime take a drink when you first get up in the morning? A positive response to any of these questions warrants further investigation. From: Cherpitel, C. J. (2000) A brief screening instrument for problem drinking in the emergency room: the RAPS4. Journal of Studies on Alcohol 61, Complete Blood Count
21 SUMMARY TABLE Cell High Low Neutrophil Lymphocyte Eosinophils Monocytes Basophils Platelets Most common causes: Infection/inflammation Necrosis Any stressor/heavy exercise Drugs Pregnancy CML Smoking Malignancy Red flags: Person particularly unwell Severity of neutrophilia Rate of change of neutrophilia Presence of left shift Causes: Acute infection (viral, bacterial) Smoking Hyposplenism Acute stress response Autoimmune thyroiditis CLL Most common causes: Allergy/atopy, asthma/hayfever Parasites (less common in developed countries) Rarer causes: Hodgkins Myeloproliferative disorders Churg-Strauss syndrome Usually not significant Watch levels > /L more closely Associated with: Myeloproliferative disorders Other rare causes Significant levels: > /L Most likely causes: Reactive conditions e.g. infection, inflammation Pregnancy Iron deficiency Post splenectomy Essential thrombocythaemia Significant levels: < /L (high risk infection) Most common causes: Viral (overt or occult) Autoimmune/idiopathic Medications Red flags: Person particularly unwell Severity of neutropenia Rate of change of neutropenia Lymphadenopathy, hepatosplenomegaly Not usually clinically significant No real cause for concern Not clinically significant Difficult to demonstrate Significant levels: < /L Most common causes: Viral infection Idiopathic thrombocytopenic purpura Liver disease Drugs Hypersplenism Autoimmune disease Pregnancy Red flags: bruising petechiae signs of bleeding Complete Blood Count 19
22 Glossary cellular abnormalities seen on the peripheral blood film Acanthocytes are irregularly spiculated (spikey) red cells. Found in liver disease, hyposplenism, anorexia, myelodysplasia and abetalipoproteinaemia (very rare). Anisocytosis is variation in red cell size. May occur in many different situations and is a non-specific finding. Variant Lymphocytes (reactive lymphocytes) are lymphocytes that, as a result of antigen stimulation, have become larger than usual. Usually the result of infection, especially viral. Basophilic stippling the presence of small granular bodies within the red cell cytoplasm. This occurs when there is accelerated red cell production and cells with immature cytoplasm are released into the circulation or else with dyserythropoiesis (abnormal production of red cells). May be found in lead poisoning, thalassaemia or other causes of significant anaemia. Blast cells are very immature precursor cells which are not usually seen outside the bone marrow. Their presence in the peripheral blood most commonly indicates acute leukaemia, myelodysplasia or myelofibrosis. Burr cells (echinocyte or crenated cell) are irregularly shaped red cells that may be found in patients with uraemia or as an artefact in older samples. Dimorphic picture/appearance describes heterogeneity in the size of red blood cells, usually with two distinct populations. It can be found in partially treated iron deficiency, mixed deficiency anaemias (e.g. folate/b12 and iron together), following transfusion, or in cases of sideroblastic anaemia. Döhle bodies appear as a small, light blue-grey staining area in the cytoplasm of the neutrophil. They are most commonly found in severe infections, but may also be seen with poisoning, burns and following chemotherapy. Elliptocytes are red blood cells that are oval or cigarshaped. They may be found in various anaemias, but are found in large numbers in hereditary elliptocytosis. Which is a reasonably common but usually clinically insignificant red cell membrane disorder. Howell-Jolly bodies are nuclear remnants found in red cells after splenectomy, in cases of megaloblastic anaemia and occasionally in cases of myelodysplasia. Hypersegmented neutrophils. See Right shift Hypochromia is reduced staining of red cells seen commonly in iron deficiency anaemia and also in thalassaemia and sideroblastic anaemias. Usually associated with microcytosis. Left shift describes immature white blood cells that are released from the marrow when there is a cause of marrow outpouring, typically due to infection. Leucoerythroblastic anaemia/picture describes a combination of nucleated red cells and a left shift of granulocytes. It may be seen with severe infection, blood loss, hypoxia, haemolysis or else with bone marrow infiltration, fibrosis or dysplasia. Leukaemoid reaction is an excessive marked reactive leucocytosis, usually consisting of granulocytes. It is seen after burns, in cases of severe infection, following an acute haemolysis or prolonged hypoxia. Macrocytosis is the presence of abnormally large red cells found when erythropoiesis is disordered or when red cells are released prematurely from the marrow. See Page 17 for causes. Microcytosis is the presence of abnormally small red cells often found in association with hypochromia. See Page 15 for causes. Metamyelocytes, myelocytes and promyelocytes are increasingly immature white cells with a left shift. Neutropenia, drug induced. Many drugs have been implicated including: Analgesics and anti-inflammatory agents include phenylbutazone, indomethacin, ibuprofen, acetylsalicylic acid, barbiturates, mesalazine, and quinine. Antimicrobials include penicillin, cephalosporins, vancomycin, chloramphenicol, gentamicin, clindamycin, doxycycline, flucytosine, nitrofurantoin, minocycline, metronidazole, rifampin, isoniazid, streptomycin, 20 Complete Blood Count
23 mebendazole, pyrimethamine, levamisole, sulfonamides, chloroquine, hydroxychloroquine, dapsone, ciprofloxacin, trimethoprim, imipenem/ cilastatin, zidovudine, acyclovir and terbinafine. Antipsychotics, antidepressants and neuropharmacologics include phenothiazines (chlorpromazine, thioridazine, prochlorperazine, trifluoperazine, trimeprazine), clozapine, risperidone, imipramine, desipramine, diazepam, chlordiazepoxide, thiothixene and haloperidol. Anticonvulsants include valproic acid, phenytoin and carbamazepine. Antithyroid drugs include thiouracil, propylthiouracil, methimazole and carbimazole. Cardiovascular system drugs include procainamide, captopril, propranolol, methyldopa, quinidine, nifedipine and ticlopidine. Other drugs include cimetidine, ranitidine, allopurinol, colchicine, famotidine, bezafibrate, flutamide, tamoxifen, penicillamine, retinoic acid, metoclopramide, ethanol, chlorpropamide, tolbutamide, thiazides, spironolactone, acetazolamide, IVIG and levodopa. Some herbal remedies. Nucleated red blood cells are immature red blood cells. These are usually seen in newborn infants and in patients with severe bone marrow stress. Other causes are similar to those for a leucoerythroblastic blood picture (see above). Pappenheimer bodies are the granules seen in siderocytes found after splenectomy and in association with iron overload and dyserythropoiesis. Poikilocytosis is the variation in cell shape usually seen in iron deficiency anaemia. Polychromasia is the heterogeneous staining of RBCs of different ages, and reflects an increase in younger cells (reticulocytes), which appear blue. It may occur after haemorrhage, haemolysis, dyserythropoiesis and treatment with haematinics such as iron and vitamin B12. Reticulocytosis is the presence of >0.8 2% of total red cell count in the form of reticulocytes. They are young, oversized red cells that are present when the marrow is actively producing red cells. They are increased after haemorrhage, haemolysis or following treatment of deficient patients with haematinics. Right shift is characterised by the presence of hypersegmented neutrophils (five or more lobes to their nucleus), seen most commonly in B12 and folate deficiency. Other rarer causes include infection, uraemia, and myelodysplastic syndrome. Confusingly a right shift can also be seen in iron deficiency. Rouleaux are stacked/clumped groups of red cells caused by the presence of high levels of circulating acute-phase proteins which increase red cell stickiness. They are often an indicator that a patient has a high ESR and are seen in infections, autoimmune conditions and myeloma. Schistocytes are red cells fragmented by their passage through intravascular strands of fibrin, found in cases of microangiopathic haemolysis. Spherocytes are overly-round or spheroid red cells that usually indicate active haemolysis. They are seen more rarely in cases of hereditary spherocytosis. Stomatocytes are red blood cells with an oval or rectangular area of central pallor, sometimes referred to as a mouth. These cells have lost the indentation on one side and may be found in liver disease, electrolyte imbalance and hereditary stomatocytosis. Target cells are red cells with a central area of increased staining, surrounded by a ring of lighter staining and then a further ring of dense staining at the edge of the cell, giving an appearance similar to an archery target. They may be found in liver disease, thalassaemia, and other haemoglobinopathies. They occur occasionally in small numbers in iron deficiency anaemia. Teardrop cells (dacrocytes) are teardrop shaped red blood cells found in: iron deficiency, megaloblastic anaemia, thalassaemia, some haemolytic anaemias, marrow infiltration and myelofibrosis and other myeloproliferative disorders. Complete Blood Count 21
24 bpac nz better medicine
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
NEW YORK STATE CYTOHEMATOLOGY PROFICIENCY TESTING PROGRAM Glass Slide Critique ~ November 2010
 NEW YORK STATE CYTOHEMATOLOGY PROFICIENCY TESTING PROGRAM Glass Slide Critique ~ November 2010 Slide 081 Available data: 72 year-old female Diagnosis: MDS to AML WBC 51.0 x 10 9 /L RBC 3.39 x 10 12 /L
NEW YORK STATE CYTOHEMATOLOGY PROFICIENCY TESTING PROGRAM Glass Slide Critique ~ November 2010 Slide 081 Available data: 72 year-old female Diagnosis: MDS to AML WBC 51.0 x 10 9 /L RBC 3.39 x 10 12 /L
Hematology Morphology Critique
 Survey Slide: History: 60-year-old female presenting with pneumonia Further Laboratory Data: Hgb : 90 g/l RBC : 2.92 10 12 /L Hct : 0.25 L/L MCV : 87 fl MCH : 30.8 pg MCHC : 355 g/l RDW : 17.7 % WBC :
Survey Slide: History: 60-year-old female presenting with pneumonia Further Laboratory Data: Hgb : 90 g/l RBC : 2.92 10 12 /L Hct : 0.25 L/L MCV : 87 fl MCH : 30.8 pg MCHC : 355 g/l RDW : 17.7 % WBC :
Young fetus: site of hematopoiesis together with the liver and bone marrow. Hgb WBC >----------< Plt Hct. Retic =
 Learning Objectives At the completion of this program, the participants will be able to: 1. Identify the components of the CBC and Differential and their clinical implications. 2. Identify normal pediatric
Learning Objectives At the completion of this program, the participants will be able to: 1. Identify the components of the CBC and Differential and their clinical implications. 2. Identify normal pediatric
General Practice Referral Guidelines Haematology Department Southend University Hospital NHS Foundation Trust March 2014
 General Practice Referral Guidelines Haematology Department Southend University Hospital NHS Foundation Trust March 2014 Dear Colleague The attached protocols have been designed with the aim of streamlining
General Practice Referral Guidelines Haematology Department Southend University Hospital NHS Foundation Trust March 2014 Dear Colleague The attached protocols have been designed with the aim of streamlining
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Interpretation of the full blood count in systemic disease a guide for the physician
 CME http://dx.doi.org/10.4997/jrcpe.2014.109 2014 Royal College of Physicians of Edinburgh Interpretation of the full blood count in systemic disease a guide for the physician M Leach Consultant Haematologist
CME http://dx.doi.org/10.4997/jrcpe.2014.109 2014 Royal College of Physicians of Edinburgh Interpretation of the full blood count in systemic disease a guide for the physician M Leach Consultant Haematologist
Laboratory Studies in the Diagnosis of Iron Deficiency, Latent Iron Deficiency and Iron Deficient Erythropoiesis
 Laboratory Studies in the Diagnosis of Iron Deficiency, Latent Iron Deficiency and Iron Deficient Erythropoiesis General Comments The laboratory studies listed below are helpful in the diagnosis and management
Laboratory Studies in the Diagnosis of Iron Deficiency, Latent Iron Deficiency and Iron Deficient Erythropoiesis General Comments The laboratory studies listed below are helpful in the diagnosis and management
Estimated New Cases of Leukemia, Lymphoma, Myeloma 2014
 ABOUT BLOOD CANCERS Leukemia, Hodgkin lymphoma (HL), non-hodgkin lymphoma (NHL), myeloma, myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPNs) are types of cancer that can affect the
ABOUT BLOOD CANCERS Leukemia, Hodgkin lymphoma (HL), non-hodgkin lymphoma (NHL), myeloma, myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPNs) are types of cancer that can affect the
RDW-- Interpreting the Full Blood Count
 RDW-- Interpreting the Full Blood Count The most important components of a Full Blood Count report are, of course, the Haemoglobin, the White Cell Count and Differential and the Platelet Count. However,
RDW-- Interpreting the Full Blood Count The most important components of a Full Blood Count report are, of course, the Haemoglobin, the White Cell Count and Differential and the Platelet Count. However,
STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY
 9 STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY 9.1 INTRODUCTION A peripheral blood smear (peripheral blood film) is a glass microscope slide coated on one side with a thin
9 STAINING OF PBF AND INTERPRETATION OF NORMAL AND ABNORMAL RED CELL MORPHOLOGY 9.1 INTRODUCTION A peripheral blood smear (peripheral blood film) is a glass microscope slide coated on one side with a thin
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2
 Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran ABNORMAL MORPHOLOGY OF BLOOD CELLS
 Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran ABNORMAL MORPHOLOGY OF BLOOD CELLS April - 2012 ABNORMAL MORPHOLOGY OF RED BLOOD CELL When a blood smear is inspected for abnormal
Hematology-Immunology System Faculty of Medicine Universitas Padjadjaran ABNORMAL MORPHOLOGY OF BLOOD CELLS April - 2012 ABNORMAL MORPHOLOGY OF RED BLOOD CELL When a blood smear is inspected for abnormal
White Blood Cells (WBCs) or Leukocytes
 Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
Lec.5 Z.H.Al-Zubaydi Medical Physiology White Blood Cells (WBCs) or Leukocytes Although leukocytes are far less numerous than red blood cells, they are important to body defense against disease. On average,
Haematology what does your blood test mean?
 Haematology what does your blood test mean? This document provides some reading material to be used in preparation for the Haematology what does your blood test mean? workshop at RMIT s Experience Health
Haematology what does your blood test mean? This document provides some reading material to be used in preparation for the Haematology what does your blood test mean? workshop at RMIT s Experience Health
An overview of CLL care and treatment. Dr Dean Smith Haematology Consultant City Hospital Nottingham
 An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
What Does My Bone Marrow Do?
 What Does My Bone Marrow Do? the myelodysplastic syndromes foundation, inc. Illustrations by Kirk Moldoff Published by The Myelodysplastic Syndromes Foundation, Inc. First Edition, 2009. 2012. Table of
What Does My Bone Marrow Do? the myelodysplastic syndromes foundation, inc. Illustrations by Kirk Moldoff Published by The Myelodysplastic Syndromes Foundation, Inc. First Edition, 2009. 2012. Table of
Atlas of Hematology and Analysis of Peripheral Blood Smears
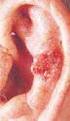 CHAPTER e17 Atlas of Hematology and Analysis of Peripheral Blood Smears Dan L. Longo Some of the relevant findings in peripheral blood, enlarged lymph nodes, and bone marrow are illustrated in this chapter.
CHAPTER e17 Atlas of Hematology and Analysis of Peripheral Blood Smears Dan L. Longo Some of the relevant findings in peripheral blood, enlarged lymph nodes, and bone marrow are illustrated in this chapter.
Introduction. About 10,500 new cases of acute myelogenous leukemia are diagnosed each
 Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
KEY CHAPTER 14: BLOOD OBJECTIVES. 1. Describe blood according to its tissue type and major functions.
 KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
KEY CHAPTER 14: BLOOD OBJECTIVES 1. Describe blood according to its tissue type and major functions. TISSUE TYPE? MAJOR FUNCTIONS connective Transport Maintenance of body temperature 2. Define the term
CLL. Handheld record. Stockport NHS foundation trust
 CLL 2015 Handheld record Contains- Patient information booklet, details of haematology clinic assessment and ongoing clinical assessment at GP surgery Stockport NHS foundation trust You have been diagnosed
CLL 2015 Handheld record Contains- Patient information booklet, details of haematology clinic assessment and ongoing clinical assessment at GP surgery Stockport NHS foundation trust You have been diagnosed
chronic leukemia lymphoma myeloma differentiated 14 September 1999 Pre- Transformed Ig Surface Surface Secreted Myeloma Major malignant counterpart
 Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Appendix D- Monoclonal Gammopathy of Undetermined Significance (MGUS)
 Local Enhanced Service: Primary care management of stable haematological patients Monoclonal Gammopathy of Undetermined Significance (MGUS) 1. Introduction Monoclonal Gammopathy of Undetermined Significance
Local Enhanced Service: Primary care management of stable haematological patients Monoclonal Gammopathy of Undetermined Significance (MGUS) 1. Introduction Monoclonal Gammopathy of Undetermined Significance
Exercise 9: Blood. Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826.
 Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Exercise 9: Blood Readings: Silverthorn 5 th ed, 547 558, 804 805; 6 th ed, 545 557, 825 826. Blood Typing The membranes of human red blood cells (RBCs) contain a variety of cell surface proteins called
Hepatitis C. Laboratory Tests and Hepatitis C
 Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
Hepatitis C Laboratory Tests and Hepatitis C If you have hepatitis C, your doctor will use laboratory tests to check your health. This handout will help you understand what the major tests are and what
Granulocytes vs. Agranulocytes
 Leukocytes are white blood cells (AKA colorless (non-pigmented) blood cells). (Much) smaller in number than RBCs. Unlike RBCs, there are several different types of WBCs. All contain a visible nucleus.
Leukocytes are white blood cells (AKA colorless (non-pigmented) blood cells). (Much) smaller in number than RBCs. Unlike RBCs, there are several different types of WBCs. All contain a visible nucleus.
BLOOD-Chp. Chp.. 6 What are the functions of blood? What is the composition of blood? 3 major types of plasma proteins
 6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
6.1 Blood: An overview BLOOD-Chp Chp.. 6 What are the functions of blood? Transportation: oxygen, nutrients, wastes, carbon dioxide and hormones Defense: against invasion by pathogens Regulatory functions:
Thibodeau: Anatomy and Physiology, 5/e. Chapter 17: Blood
 Thibodeau: Anatomy and Physiology, 5/e Chapter 17: Blood This chapter begins a new unit. In this unit, the first four chapters deal with transportation one of the body's vital functions. It is important
Thibodeau: Anatomy and Physiology, 5/e Chapter 17: Blood This chapter begins a new unit. In this unit, the first four chapters deal with transportation one of the body's vital functions. It is important
EDUCATIONAL COMMENTARY - GRANULOCYTE FORMATION AND CHRONIC MYELOCYTIC LEUKEMIA
 LEUKEMIA Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education
LEUKEMIA Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn CE Credits under Continuing Education
Blood Testing Protocols. Disclaimer
 Blood Testing Protocols / Page 2 Blood Testing Protocols Here are the specific test protocols recommend by Dr. J.E. Williams. You may request these from your doctor or visit www.readyourbloodtest.com to
Blood Testing Protocols / Page 2 Blood Testing Protocols Here are the specific test protocols recommend by Dr. J.E. Williams. You may request these from your doctor or visit www.readyourbloodtest.com to
Blood. Functions of Blood. Components of Blood. Transporting. Distributing body heat. A type of connective tissue. Formed elements.
 Blood Functions of Blood Transporting nutrients respiratory gases waste products Distributing body heat Components of Blood A type of connective tissue Formed elements Living blood cells Plasma Nonliving
Blood Functions of Blood Transporting nutrients respiratory gases waste products Distributing body heat Components of Blood A type of connective tissue Formed elements Living blood cells Plasma Nonliving
Myelodysplasia. Dr John Barry
 Myelodysplasia Dr John Barry Myelodysplasia Group of heterogenouus bone marrow disorders that are due to a defect in stem cells. Increasing bone marrow failure leading to quan>ta>ve and qualita>ve abnormali>es
Myelodysplasia Dr John Barry Myelodysplasia Group of heterogenouus bone marrow disorders that are due to a defect in stem cells. Increasing bone marrow failure leading to quan>ta>ve and qualita>ve abnormali>es
Anemia and Leukocytosis Answers
 Case #1 RBC abnormalities Anemia and Leukocytosis Answers History: A 19-year-old woman with anemia presents with a two day history of fever, joint pain, and left upper quadrant discomfort. She reports
Case #1 RBC abnormalities Anemia and Leukocytosis Answers History: A 19-year-old woman with anemia presents with a two day history of fever, joint pain, and left upper quadrant discomfort. She reports
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI
 Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
Yvette Marie Miller, M.D. Executive Medical Officer American Red Cross October 20, 2012 45 th Annual Great Lakes Cancer Nursing Conference Troy, MI Overview of Hematology, http://www.nu.edu.sa/userfiles/mhmorsy/h
Technical University of Mombasa Faculty of Applied and Health Sciences
 Technical University of Mombasa Faculty of Applied and Health Sciences DEPARTMENT OF MEDICAL SCIENCES UNIVERSITY EXAMINATION FOR THE DEGREE OF BACHELOR OF MEDICAL LABORATORY SCIENCES BMLS 12S Mid AML 4321
Technical University of Mombasa Faculty of Applied and Health Sciences DEPARTMENT OF MEDICAL SCIENCES UNIVERSITY EXAMINATION FOR THE DEGREE OF BACHELOR OF MEDICAL LABORATORY SCIENCES BMLS 12S Mid AML 4321
ACUTE MYELOID LEUKEMIA (AML),
 1 ACUTE MYELOID LEUKEMIA (AML), ALSO KNOWN AS ACUTE MYELOGENOUS LEUKEMIA WHAT IS CANCER? The body is made up of hundreds of millions of living cells. Normal body cells grow, divide, and die in an orderly
1 ACUTE MYELOID LEUKEMIA (AML), ALSO KNOWN AS ACUTE MYELOGENOUS LEUKEMIA WHAT IS CANCER? The body is made up of hundreds of millions of living cells. Normal body cells grow, divide, and die in an orderly
Pathology No: SHS-CASE No. Date of Procedure: Client Name Address
 TEL #: (650) 725-5604 FAX #: (650) 725-7409 Med. Rec. No.: Date of Procedure: Sex: A ge: Date Received: Date of Birth: Account No.: Physician(s): Client Name Address SPECIMEN SUBMITTED: LEFT PIC BONE MARROW,
TEL #: (650) 725-5604 FAX #: (650) 725-7409 Med. Rec. No.: Date of Procedure: Sex: A ge: Date Received: Date of Birth: Account No.: Physician(s): Client Name Address SPECIMEN SUBMITTED: LEFT PIC BONE MARROW,
BLOOD COUNT INTERPRETATION. J. Bačovský
 BLOOD COUNT INTERPRETATION J. Bačovský Sysmex XE 5000 + software + staining ) CellaVision DM 96 (automatic digitál morphology of peripheral blood smears Hematology Cell Counter Counts cells by electronic
BLOOD COUNT INTERPRETATION J. Bačovský Sysmex XE 5000 + software + staining ) CellaVision DM 96 (automatic digitál morphology of peripheral blood smears Hematology Cell Counter Counts cells by electronic
Summary of the risk management plan (RMP) for Accofil (filgrastim)
 EMA/475472/2014 Summary of the risk management plan (RMP) for Accofil (filgrastim) This is a summary of the risk management plan (RMP) for Accofil, which details the measures to be taken in order to ensure
EMA/475472/2014 Summary of the risk management plan (RMP) for Accofil (filgrastim) This is a summary of the risk management plan (RMP) for Accofil, which details the measures to be taken in order to ensure
Additional Blood Tests
 Additional Blood Tests CBC W/Auto Diff The CBC is used as a broad screening test to check for such disorders as anemia, infection, and many other diseases. It is actually panel of tests that examines different
Additional Blood Tests CBC W/Auto Diff The CBC is used as a broad screening test to check for such disorders as anemia, infection, and many other diseases. It is actually panel of tests that examines different
Blood & Marrow Transplant Glossary. Pediatric Blood and Marrow Transplant Program Patient Guide
 Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Acute myeloid leukaemia (AML) in children
 1 61.02 Acute myeloid leukaemia (AML) in children AML can affect children of any age, and girls and boys are equally affected. Leukaemia Acute myeloid leukaemia (AML) FAB classification of AML Causes of
1 61.02 Acute myeloid leukaemia (AML) in children AML can affect children of any age, and girls and boys are equally affected. Leukaemia Acute myeloid leukaemia (AML) FAB classification of AML Causes of
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
Prof. of Tropical Medicine Faculty of Medicine Alexandria University
 prof. Dr. Ali El-Kady (MD) Prof. of Tropical Medicine Faculty of Medicine Alexandria University DRUGS THAT MAY CAUSE LIVER DYSFUNCTION DAMAGE The liver is the principal organ that is capable of converting
prof. Dr. Ali El-Kady (MD) Prof. of Tropical Medicine Faculty of Medicine Alexandria University DRUGS THAT MAY CAUSE LIVER DYSFUNCTION DAMAGE The liver is the principal organ that is capable of converting
ABO-Rh Blood Typing Using Neo/BLOOD
 ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
ABO-Rh Blood Typing Using Neo/BLOOD Objectives Determine the ABO and Rh blood type of unknown simulated blood samples. Prepare a simulated blood smear. Examine a prepared blood smear under the microscope
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org
 Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
Selective IgA deficiency (slgad) [email protected] 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
INITIATING ORAL AUBAGIO (teriflunomide) THERAPY
 FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
FOR YOUR PATIENTS WITH RELAPSING FORMS OF MS INITIATING ORAL AUBAGIO (teriflunomide) THERAPY WARNING: HEPATOTOXICITY AND RISK OF TERATOGENICITY Severe liver injury including fatal liver failure has been
Acute myeloid leukemia (AML)
 Acute myeloid leukemia (AML) Adult acute myeloid leukemia (AML) is a type of cancer in which the bone marrow makes abnormal myeloblasts (a type of white blood cell), red blood cells, or platelets. Adult
Acute myeloid leukemia (AML) Adult acute myeloid leukemia (AML) is a type of cancer in which the bone marrow makes abnormal myeloblasts (a type of white blood cell), red blood cells, or platelets. Adult
IRON METABOLISM DISORDERS
 IRON METABOLISM DISORDERS ANEMIA Definition Decrease in the number of circulating red blood cells Most common hematologic disorder by Most common hematologic disorder by far 1 Blood loss ANEMIA Causes
IRON METABOLISM DISORDERS ANEMIA Definition Decrease in the number of circulating red blood cells Most common hematologic disorder by Most common hematologic disorder by far 1 Blood loss ANEMIA Causes
Guidelines for the Investigation and Management of Vitamin B12 and Folate Deficiency
 Hull and East Riding Prescribing Committee Guidelines for the Investigation and Management of Vitamin B12 and Folate Deficiency Developed by:, Hull & East Yorkshire Hospital NHS Trust Hull and East Riding
Hull and East Riding Prescribing Committee Guidelines for the Investigation and Management of Vitamin B12 and Folate Deficiency Developed by:, Hull & East Yorkshire Hospital NHS Trust Hull and East Riding
Arthritis in Children: Juvenile Rheumatoid Arthritis By Kerry V. Cooke
 Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
Reading Comprehension Read the following essay on juvenile rheumatoid arthritis. Then use the information in the text to answer the questions that follow. Arthritis in Children: Juvenile Rheumatoid Arthritis
Chapter 3. Immunity and how vaccines work
 Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Chapter 3 Immunity and how vaccines work 3.1 Objectives: To understand and describe the immune system and how vaccines produce immunity To understand the differences between Passive and Active immunity
Oncology Best Practice Documentation
 Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
Oncology Best Practice Documentation Click on the desired Diagnoses link or press Enter to view all information. Diagnoses: Solid Tumors Lymphomas Leukemias Myelodysplastic Syndrome Pathology Findings
1.5 Function of analyte For albumin, see separate entry. The immunoglobulins are components of the humoral arm of the immune system.
 Total protein (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Total protein 1.2 Alternative names None 1.3 NMLC code 1.4 Description of analyte This is a quantitative measurement
Total protein (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Total protein 1.2 Alternative names None 1.3 NMLC code 1.4 Description of analyte This is a quantitative measurement
Testing for RA. The Ideal Lab Test. William M. Wason, MD, PhD 9/24/2010. Confusion Abounds
 Confusion Abounds Rheumatoid arthritis: ulnar deviation and muscle artrophy, hands Poor sensitivity and specificity Hepatitis C causes lots of false + tests Changing technology in how tests are done Historic
Confusion Abounds Rheumatoid arthritis: ulnar deviation and muscle artrophy, hands Poor sensitivity and specificity Hepatitis C causes lots of false + tests Changing technology in how tests are done Historic
Albumin. Prothrombin time. Total protein
 Hepatitis C Fact Sheet February 2016 www.hepatitis.va.gov Laboratory Tests and Hepatitis If you have hepatitis C, your doctor will use laboratory tests to about learn more about your individual hepatitis
Hepatitis C Fact Sheet February 2016 www.hepatitis.va.gov Laboratory Tests and Hepatitis If you have hepatitis C, your doctor will use laboratory tests to about learn more about your individual hepatitis
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL VOLUME I RESPONSE ASSESSMENT LEUKEMIA CHAPTER 11A REVISED: OCTOBER 2015
 LEUKEMIA Response in Acute Myeloid Leukemia (AML) Response criteria in Acute Myeloid Leukemia for SWOG protocols is based on the review article Diagnosis and management of acute myeloid leukemia in adults:
LEUKEMIA Response in Acute Myeloid Leukemia (AML) Response criteria in Acute Myeloid Leukemia for SWOG protocols is based on the review article Diagnosis and management of acute myeloid leukemia in adults:
What is chronic lymphocytic leukaemia?
 Revised October 2011 What is chronic lymphocytic leukaemia? The diagnosis of a blood cancer can be a devastating event for patients, families and friends. It is therefore vital for everyone to have access
Revised October 2011 What is chronic lymphocytic leukaemia? The diagnosis of a blood cancer can be a devastating event for patients, families and friends. It is therefore vital for everyone to have access
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
NHS FORTH VALLEY B12 and Folate: A Practical Guide
 NHS FORTH VALLEY B12 and Folate: A Practical Guide Date of First Issue 27/05/2011 Approved 28/06/2011 Current Issue Date 24/06/2013 Review Date 24/06/2015 Version 1.0 EQIA 27/05/2011 Author / Contact Group
NHS FORTH VALLEY B12 and Folate: A Practical Guide Date of First Issue 27/05/2011 Approved 28/06/2011 Current Issue Date 24/06/2013 Review Date 24/06/2015 Version 1.0 EQIA 27/05/2011 Author / Contact Group
Inflammation and Healing. Review of Normal Defenses. Review of Normal Capillary Exchange. BIO 375 Pathophysiology
 Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
Inflammation and Healing BIO 375 Pathophysiology Review of Normal Defenses Review of Normal Capillary Exchange 1 Inflammation Inflammation is a biochemical and cellular process that occurs in vascularized
MALE AND FEMALE PANEL CHARTS
 MALE AND FEMALE PANEL CHARTS Complete Blood Count (CBC) Test What this test measures What test results may indicate Red blood cell count Total number of red blood cells Blood loss High altitude per volume
MALE AND FEMALE PANEL CHARTS Complete Blood Count (CBC) Test What this test measures What test results may indicate Red blood cell count Total number of red blood cells Blood loss High altitude per volume
INTRODUCTION Thrombophilia deep vein thrombosis DVT pulmonary embolism PE inherited thrombophilia
 INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
INTRODUCTION Thrombophilia (Hypercoagulability) is a condition in which a person forms blood clots more than normal. Blood clots may occur in the arms or legs (e.g., deep vein thrombosis DVT), the lungs
2015 RN.ORG, S.A., RN.ORG, LLC
 The Complete Blood Count and Associated Tests WWW.RN.ORG Reviewed December, 2015, Expires December, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
The Complete Blood Count and Associated Tests WWW.RN.ORG Reviewed December, 2015, Expires December, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Summary of the risk management plan (RMP) for Otezla (apremilast)
 EMA/741412/2014 Summary of the risk management plan (RMP) for Otezla (apremilast) This is a summary of the risk management plan (RMP) for Otezla, which details the measures to be taken in order to ensure
EMA/741412/2014 Summary of the risk management plan (RMP) for Otezla (apremilast) This is a summary of the risk management plan (RMP) for Otezla, which details the measures to be taken in order to ensure
Careers in Haematology
 Careers in Haematology A Guide for Medical Students and Junior Doctors Haematology is the medical speciality concerned with blood disorders. Your non-medical friends however will always think that you
Careers in Haematology A Guide for Medical Students and Junior Doctors Haematology is the medical speciality concerned with blood disorders. Your non-medical friends however will always think that you
Laboratory 12 Blood Cells
 Laboratory 12 Blood Cells Objectives: Identify microscopically each of the following: erythrocytes (red blood cells or RBCs), the five types of leukocytes (white blood cells or WBCs), and thrombocytes
Laboratory 12 Blood Cells Objectives: Identify microscopically each of the following: erythrocytes (red blood cells or RBCs), the five types of leukocytes (white blood cells or WBCs), and thrombocytes
ABO-Rh Blood Typing With Synthetic Blood
 70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
70-0101 ABO-Rh Blood Typing With Synthetic Blood Teacher s Manual World-Class Support for Science & Math The ability to type blood is an invaluable tool in the fields of medicine and criminology. Using
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Functions of Blood. Collects O 2 from lungs, nutrients from digestive tract, and waste products from tissues Helps maintain homeostasis
 Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
Blood Objectives Describe the functions of blood Describe blood plasma Explain the functions of red blood cells, white blood cells, and platelets Summarize the process of blood clotting What is Blood?
Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding.
 Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding. Bleeding may be spontaneous in the form of small haemorrhages into the
Bleeding disorders or haemorrhagic diatheses are a group of disorders characterised by defective haemostasis with abnormal bleeding. Bleeding may be spontaneous in the form of small haemorrhages into the
Protein electrophoresis is used to categorize globulins into the following four categories:
 Globulin Globulin is one of the two types of serum proteins, the other being albumin. This generic term encompasses a heterogeneous series of families of proteins, with larger molecules and less soluble
Globulin Globulin is one of the two types of serum proteins, the other being albumin. This generic term encompasses a heterogeneous series of families of proteins, with larger molecules and less soluble
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Lupus in Children and Teenagers. Arielle Hay, MD Pediatric Rheumatologist Nicklaus Children s Hospital
 Lupus in Children and Teenagers Arielle Hay, MD Pediatric Rheumatologist Nicklaus Children s Hospital Systemic Lupus Erythematosus (SLE) Chronic Illness What is lupus? Autoimmune Multisystem Antinuclear
Lupus in Children and Teenagers Arielle Hay, MD Pediatric Rheumatologist Nicklaus Children s Hospital Systemic Lupus Erythematosus (SLE) Chronic Illness What is lupus? Autoimmune Multisystem Antinuclear
Rheumatology Labs for Primary Care Providers. Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine
 Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
MORPHOLOGIC ABNORMALITIES OF THE ERYTHROCYTE
 MORPHOLOGIC ABNORMALITIES OF THE ERYTHROCYTE 68 Assignment: VIEW the RBC Morphology Slides located on Blackboard as you read/refer to the following pages 67-73 regarding Morphologic Abnormalities of the
MORPHOLOGIC ABNORMALITIES OF THE ERYTHROCYTE 68 Assignment: VIEW the RBC Morphology Slides located on Blackboard as you read/refer to the following pages 67-73 regarding Morphologic Abnormalities of the
Proteins. Protein Trivia. Optimizing electrophoresis
 Proteins ELECTROPHORESIS Separation of a charged particle in an electric field Michael A. Pesce, Ph.D Department of Pathology New York-Presbyterian Hospital Columbia University Medical Center Rate of migration
Proteins ELECTROPHORESIS Separation of a charged particle in an electric field Michael A. Pesce, Ph.D Department of Pathology New York-Presbyterian Hospital Columbia University Medical Center Rate of migration
3. The Circulatory System
 3. The Circulatory System A. Introduction B. Blood 1. Circulatory system transports water, electrolytes, hormones, enzymes, antibodies, cell, gases and nutrients to all cells and carries away metabolic
3. The Circulatory System A. Introduction B. Blood 1. Circulatory system transports water, electrolytes, hormones, enzymes, antibodies, cell, gases and nutrients to all cells and carries away metabolic
Evaluation of Cell Morphology and Introduction to Platelet and White Blood Cell Morphology
 Evaluation of Cell Morphology and Introduction to Platelet and White Blood Cell Morphology Kathy W. Jones, MS, MT(ASCP), CLS(NCA) Chapter 5 Introduction Examination of the Peripheral Blood Smear The Normal
Evaluation of Cell Morphology and Introduction to Platelet and White Blood Cell Morphology Kathy W. Jones, MS, MT(ASCP), CLS(NCA) Chapter 5 Introduction Examination of the Peripheral Blood Smear The Normal
More details >>> HERE <<<
 More details >>> HERE http://urlzz.org/conitp/pdx/cc8648/ Tags:
More details >>> HERE http://urlzz.org/conitp/pdx/cc8648/ Tags:
Side effect of drugs, such as amphetamines, tranquilizers, bulk-type laxatives containing psyllium and certain antibiotics
 Eosinophils Eosinophils are a type of white blood cell. A normal eosinophil count is less than 350 cells per microliter of blood. The exact role of eosinophils in your body is unclear, but eosinophils
Eosinophils Eosinophils are a type of white blood cell. A normal eosinophil count is less than 350 cells per microliter of blood. The exact role of eosinophils in your body is unclear, but eosinophils
Symptoms of Hodgkin lymphoma
 Produced 28.02.2011 Revision due 28.02.2013 Symptoms of Hodgkin lymphoma Lymphoma is a cancer of cells called lymphocytes. These cells are part of our immune system, which helps us to fight off infections.
Produced 28.02.2011 Revision due 28.02.2013 Symptoms of Hodgkin lymphoma Lymphoma is a cancer of cells called lymphocytes. These cells are part of our immune system, which helps us to fight off infections.
Morphology of infant blood films not as scary as it looks
 Morphology of infant blood films not as scary as it looks Dr Bronwyn Williams Haematologist QHPS Central Babies not quite the same as us Look like us BUT Not just little adults Still changing /developing
Morphology of infant blood films not as scary as it looks Dr Bronwyn Williams Haematologist QHPS Central Babies not quite the same as us Look like us BUT Not just little adults Still changing /developing
Other treatments for chronic myeloid leukaemia
 Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
Other treatments for chronic myeloid leukaemia This information is an extract from the booklet Understanding chronic myeloid leukaemia. You may find the full booklet helpful. We can send you a copy free
EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE
 EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE Textbook: Skills: None 10 points Objectives: 1. State the principle of the Erythrocytes Sedimentation Rate - ESR. 2. List two factors which may
EXERCISE 5: ERYTHROCYTES SEDIMENTATION RATE - ESR, SED RATE Textbook: Skills: None 10 points Objectives: 1. State the principle of the Erythrocytes Sedimentation Rate - ESR. 2. List two factors which may
Cardiovascular System. Blood Components
 Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Cardiovascular System Blood Components 1 Components of Blood Formed elements: erythrocytes, leukocytes, platelets Plasma: water, proteins, other solutes The components of blood can be divided into two
Platelet Review July 2012. Thomas S. Kickler M.D. Johns Hopkins University School of Medicine
 Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
Platelet Review July 2012 Thomas S. Kickler M.D. Johns Hopkins University School of Medicine Hemostasis Hemostasis is the process that leads to the stopping of bleeding Hemostasis involves blood vessels,
LCD for Viral Hepatitis Serology Tests
 LCD for Viral Hepatitis Serology Tests Applicable CPT Code(s): 86692 Antibody; Hepatitis, Delta Agent 86704 Hepatitis B Core Antibody (HBcAb); Total 86705 Hepatitis B Core Antibody (HBcAb); IgM Antibody
LCD for Viral Hepatitis Serology Tests Applicable CPT Code(s): 86692 Antibody; Hepatitis, Delta Agent 86704 Hepatitis B Core Antibody (HBcAb); Total 86705 Hepatitis B Core Antibody (HBcAb); IgM Antibody
Interpretation of Laboratory Values
 Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Interpretation of Laboratory Values Konrad J. Dias PT, DPT, CCS Overview Electrolyte imbalances Renal Function Tests Complete Blood Count Coagulation Profile Fluid imbalance Sodium Electrolyte Imbalances
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Evaluation of a Child with Elevated Transaminases. Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium
 Evaluation of a Child with Elevated Transaminases Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium Disclosures I do not have a financial interest, arrangement or affiliation
Evaluation of a Child with Elevated Transaminases Linda V. Muir, M.D. April 11, 2008 Northwest Pediatric Liver Disease Symposium Disclosures I do not have a financial interest, arrangement or affiliation
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer
 Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Blood, Lymphatic and Immune Systems
 Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
Component 3-Terminology in Healthcare and Public Health Settings Unit 4-Blood, Lymphatic and Immune Systems This material was developed by The University of Alabama at Birmingham, funded by the Department
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
