Prostate Cancer Management Clinical Guidelines
|
|
|
- Kerry Grant
- 9 years ago
- Views:
Transcription
1 Royal College of Surgeons in Ireland Surgery (The Colles Institute) Surgical Clinical Guidelines Surgery (The Colles Institute) Prostate Cancer Management Clinical Guidelines Clinical Guidelines Committee Royal College of Surgeons in Ireland Citation Clinical Guidelines Committee. Prostate Cancer Management Clinical Guidelines. Dublin: Royal College of Surgeons in Ireland, This Report is brought to you for free and open access by the Surgery (The Colles Institute) at It has been accepted for inclusion in Surgery (The Colles Institute) Surgical Clinical Guidelines by an authorized administrator of For more information, please contact
2 Use Licence Attribution-Non-Commercial-ShareAlike 1.0 You are free: to copy, distribute, display, and perform the work. to make derivative works. Under the following conditions: Attribution You must give the original author credit. Non-Commercial You may not use this work for commercial purposes. Share Alike If you alter, transform, or build upon this work, you may distribute the resulting work only under a licence identical to this one. For any reuse or distribution, you must make clear to others the licence terms of this work. Any of these conditions can be waived if you get permission from the author. Your fair use and other rights are in no way affected by the above. This work is licenced under the Creative Commons Attribution-Non-Commercial-ShareAlike License. To view a copy of this licence, visit: URL (human-readable summary): URL (legal code): This report is available at e-publications@rcsi:
3 Prostate Cancer Management Clinical Guidelines Prepared by The Clinical Guidelines Committee Royal College of Surgeons in Ireland February 2002
4 Prostate Cancer Management Clinical Guidelines 1 Foreword FOREWORD Awareness of prostate cancer amongst the general public has risen sharply, due to a number of factors not least of which has been the profiling of prominent sufferers by the media. There is a body of information about prostate cancer available through the Internet, men s and women s magazines, and interest groups. Much of this information is available in a fragmented form, and it is not always possible to synthesise the full picture easily. These guidelines are designed about a series of recommendations, which have been developed from an attempt to gather concisely and accurately the relevant information about prostate cancer. Consequently it is hoped that the recommendations and the supporting information will prove to be an accessible source of knowledge to the medical profession, medical students, the nursing profession and the general public. Considerable effort has gone into publishing the guidelines. We acknowledge that they will have a limited shelf-life and it is our intention to revise them in two or three years so that advances in knowledge can be incorporated, Many people were involved and contributed in a variety of ways to the project. We would like to thank our panel of co-writers and reviewers Dr. John Armstrong, Mr. David Quinlan and Prof. John Fitzpatrick, all of whom contributed to the manuscript. Marjorie White-Flynn at the Urology Department in Tallaght did trojan work, and typed many drafts of the manuscript before it was deemed suitable for publication. We appreciate her patience and good humour. Paula Wilson co-ordinated the project in the Royal College of Surgeons in Ireland and we thank her for putting her organising skills at our disposal. We also wish to thank our publishers who have metamorphosed a rather drab-looking document into a beautiful production. Michael Butler Chairman, Urology Group, Clinical Guidelines Committee Niall O Higgins Chairman, Clinical Guidelines Committee February, 2002.
5 2 Prostate Cancer Management Clinical Guidelines Contents Introduction 3 Purpose of guidelines 3 Keys to level of evidence and grading of recommendations 3 Summary of recommendations 4 Presentation 6 Management of asymptomatic and symptomatic patients 6 Investigation and Diagnosis 9 Tumour markers 9 Obtaining prostatic tissue for histology 9 TNM clinical classification of prostate cancer 11 Histological reporting 12 Imaging 13 Treatment of Prostate Cancer 15 Selection of therapy for localised prostate cancer 15 Management of potentially curable carcinoma of the prostate 15 Surgery of prostate cancer 16 Relapse after prostate surgery: diagnosis, treatment and prognosis 17 The role of adjuvant X-ray therapy 18 XRT for localised prostate cancer 19 Relapse after XRT: diagnosis and treatment 20 Management after failed XRT: cryotherapy and salvage prostatectomy 20 XRT for locally advanced prostate cancer 21 Brachytherapy 21 Conservative Management of Prostate Cancer 23 Surveillance 23 Metastatic Prostate Cancer 24 Hormonal therapy 24 Clinical management of patients with metastatic disease 26 Management of complications of advanced prostate cancer 26 Hormone-refractory prostate cancer 27 Cryotherapy 28 References 29
6 Prostate Cancer Management Clinical Guidelines 3 Introduction PURPOSE OF GUIDELINES Cancer of the prostate is the commonest noncutaneous cancer amongst men in the Republic of Ireland. It represents 11% of all male cancers. The risk of developing prostate cancer before the age of 75 is 5% and has increased by 1.3% since The disease-specific risk of death before 75 is 1.6%. Approximately five hundred and twenty men die of carcinoma of the prostate per annum. 1 The aims of these guidelines are to increase awareness of prostate cancer in the Irish community. The guidelines provide a source of information, the ultimate aim of which is to facilitate and promote optimum care for patients presenting with carcinoma of the prostate. By reference to the guidelines and enactment of the recommendations disease-free intervals and increased survival in patients with prostatic cancer may be achieved. In publishing the guidelines we aspire to inform clinicians about best clinical practice. Promotion of best available standards should lead to the elimination of the unacceptable. The guidelines are not intended to be rigidly dogmatic and are not written as protocols. Clinical freedom is preserved within the limits of good practice. Ultimately it is hoped that the guidelines will lead to better uniform care throughout the country with improvement in survival for all patients with prostate cancer. KEY TO LEVELS OF EVIDENCE AND GRADING OF RECOMMENDATIONS The definitions of the type of evidence of and the grades of recommendations used in these guidelines originated from the United States Agency For Health Care Policy and Research and are set out in the following tables. Level Ia Ib IIa IIb III IV Type of Evidence Evidence obtained from meta-analysis of randomised trials. Evidence obtained from at least one randomised controlled trial Evidence obtained from at least one well-designed controlled study without randomisation. Evidence obtained from at least one other type of well-designed quasiexperimental study. Evidence obtained from welldesigned, non-experimental, descriptive studies such as comparative studies, correlation studies and case series. Evidence obtained from expert committee reports or opinions and/or clinical experience of respected authorities. GRADES OF RECOMMENDATION Grade A requires at least one randomised controlled trial as part of the body of literature of overall good quality and consistency addressing the specific recommendation. (Evidence levels Ia, Ib). requires the availability of well-conducted clinical studies but no randomised clinical trials on the topic of the recommendation. (Evidence levels IIa, IIb, III). requires evidence obtained from expert committees reports or opinions and/or clinical experiences of respected authorities. Indicates the absence of directly applicable clinical studies of good quality. (Evidence level IV).
7 4 Prostate Cancer Management Clinical Guidelines Introduction SUMMARY OF RECOMMENDATIONS Screening 1. Because of a relative increased risk of developing carcinoma in certain subgroups a selective approach to investigation by digital rectal examination (DRE) and prostatic specific antigen (PSA) estimation is warranted. 2. Standardised information should be made available to all asymptomatic patients undergoing PSA examination. Information should include the following: Likelihood that failure to screen will increase the chance of an undetected carcinoma of the prostate in a man s lifetime. Whether PSA screening will lengthen or improve quality of life. The risk of that a raised PSA may result in unnecessary single or serial biopsies. The value of a normal result. 3. In patients with lower urinary tract symptoms PSA should be routinely included in investigations. 4. Currently it is recommended that screening is best achieved by a combination of DRE and PSA on an annual basis to age A screening programme should be introduced in Ireland in the context of a randomised trial for men between 50 and 69 years. Tumour Markers and Histology 6. PSA testing needs further refinement to limit the number of unnecessary biopsies. Ageadjusted total PSA and the ratio of free to total PSA values are the most effective format of reporting PSA results. 7. Histological evidence of prostatic carcinoma in general is essential. Only in exceptional circumstances with overwhelming evidence of advanced cancer should treatment commence without histological confirmation. 8. Systematic sextant transrectal ultrasound (TRUS)-guided biopsy is the preferred method of obtaining biopsies. Positive biopsy rates can be improved by modifying the sextant biopsy technique to include biopsies of the peripheral zone obtained more laterally, and inclusion of some biopsy from the transitional zone in larger prostates. 9. Appropriate antibiotics should always be given when transrectal biopsies are carried out. 10. Repeat biopsy is necessary where there is (a) inadequate tissue sampling, (b) cellular atypia, (c) high-grade (3) prostatic intraepithelial neoplasia (PIN) or (d) a rising PSA after a negative first biopsy. 11. Biopsied specimens should be labelled and orientated according to local protocol. 12. The Gleason system is the grading system of choice. 13. Sampling and reporting protocols should be standardised throughout the country. Imaging 14. Further studies and radiological developments are needed to define the most appropriate modality to stage carcinoma of the prostate pre-operatively. 15. Routine bone scans should be included in patients undergoing radical surgery or X-ray therapy (XRT).
8 Introduction Prostate Cancer Management Clinical Guidelines 5 Selection of Therapy and Pre-operative Assessment 16. As far as is practical, information should be given about best available treatments, individualised to the patient s cancer, health status and life expectancy. 17. Prior to surgery (radical prostatectomy) patients should be informed about major morbidity which includes the risks and incidence of impotence and incontinence of urine. 18. Radical prostatectomy should be performed by surgeons appropriately trained in the procedure, within an institution with medical and nursing personnel trained in the care of such patients. 19. Patients with local recurrence after radical prostatectomy should be given 3D conformal radiotherapy plus hormones. 20. Before radiotherapy patients should be informed of the potential complications of radiation proctitis/cystitis and impotence. 24. Surveillance without specific treatment is an acceptable form of management for some patients with T1a tumours with a poor life expectancy (<10 years) due to the age at which the disease is detected or co-morbid factors. 25. Patients with symptomatic metastatic disease, especially bone disease, should be managed by androgen deprivation therapy. The choice of treatment by LHRH analogues or orchidectomy is determined by many issues including patient preference. 26. Combined androgen blockade should not be used routinely on current evidence. Grade A 27. Spinal cord compression is an indication for urgent referral for radiotherapy or surgery. 28. A multidisciplinary team approach should be available to patients with advanced hormonerefractory prostatic carcinoma. The team should include palliative care specialists, radiotherapists and urologists. Treatment 21. For patients assigned to radiotherapy, 3-dimensional conformal radiotherapy (3D CRT) has become the standard of care because of its advantages in delivering optimal dosage most accurately to the prostate. 22. XRT combined with neoadjuvant hormone ablation should continue to be evaluated by randomised controlled clinical trials. 23. Neoadjuvant or adjuvant hormone therapy should be included in the protocol for high-risk patients with localised prostatic tumours. Grade A
9 6 Prostate Cancer Management Clinical Guidelines Presentation PRESENTATION Historically in Ireland most patients with prostate cancer were referred for specialist consultation by their general practitioner when symptoms of bladder-outlet obstruction had developed. Lower urinary tract symptoms may suggest locally advanced prostatic carcinoma with infiltration into the bladder neck or the urethra. In all patients with bladder-outlet obstructive symptoms a digital rectal examination (DRE) is indicated. The presence of a nodule, induration or irregularity alerts the general practitioner or urologist to the possibility of cancer of the prostate. Patients may present with peripheral limb oedema due to pelvic and abdominal lymphadenopathy. Bone pain due to metastases may be the presenting symptom. Signs of spinal cord compression due to metastases may be the first indication of prostatic cancer. Anaemia occurs with widespread bony metastases. Occasionally uraemia due to bilateral obstruction of the ureters by prostatic carcinoma is the presenting feature. With the widespread introduction of prostatic specific antigen (PSA) testing an increasing number of patients are referred by their general practitioner with elevated PSA for further investigation by transrectal ultrasound (TRUS) and for TRUS-guided biopsies. Many of these patients are asymptomatic and without clinical findings, but are found after investigation to have prostate cancer. This mode of presentation of prostate cancer is increasing and patient numbers in this sub-group have increased significantly in recent years. MANAGEMENT OF ASYMPTOMATIC AND SYMPTOMATIC PATIENTS Asymptomatic Patients In contemporary practice it is common for asymptomatic patients, who are otherwise healthy, to request that a PSA be obtained. PSA is increasingly a standard investigation in preventive health care. A raised PSA increases the likelihood that a patient has prostate cancer. In addition, a raised PSA increases the incidence of clinically important tumours without significantly increasing the detection of clinically insignificant tumours. Treatment outcome data suggests that potential treatments for cure of PSA-detected tumours is available. Currently there are some data confirming that screening by PSA reduces morbidity and mortality. 2 The Surveillance, Epidemiology and End Results (SEER) programme is the basis of most American trends for cancer. The data for prostatic cancer were analysed to determine the effect of screening. No other malignancy has been associated with a greater increase in incidence, and the tumours detected with PSA are mostly clinically significant. Additionally the detection of advanced disease has decreased, that is the incidence of distant disease which influenced mortality rate has decreased with prostate screening of men older than 50 years of age, but the incidence of local and regional disease has increased. The SEER Study 3 showed that in the USA between 1973 and 1992 age-adjusted prostate cancer incidence rates for all males increased dramatically. The rate increase was linear between 1973 and 1976 and exponential between 1976 and Between 1987 and 1992, the age-adjusted incidence increased from to per 100,000 men, an increase of 84%, while the mortality rate fell by 6.3% from 1991 to A contrary view 4 noted that the changes observed in the SEER data cannot be attributed to increased numbers of men undergoing screening, and resulting earlier detection is also consistent with lead-time bias, length bias, and a decline in mortality. These conclusions were that the benefits of screening and early detection are theoretical, but not well supported by the SEER data, whereas the costs and risks are well known. An attempt to estimate the annual cost of screening asymptomatic men for prostatic carcinoma in Canada was carried out by Krahn and associates.
10 Presentation Prostate Cancer Management Clinical Guidelines 7 They provided important information. The conclusions were that PSA screening and attendant down-stream costs consume a very small part of the total direct health care budget, and that prior estimates that PSA screening would ultimately consume 5% of the health care budget are exaggerated. In the end the decision to implement PSA screening depends on the results of clinical trials in this area. If found effective, screening is affordable, and needs support. The converse is equally true no improved trial outcomes, no support. 5 Many factors must be considered by doctors and their patients who contemplate routine PSA for screening for prostate cancer. The results of a refusal to obtain a PSA on patient request could be serious particularly if prostate cancer occurs in the patient at a future date. Because of the implications of the results explicit information should be given to an asymptomatic, healthy patient before PSA estimation is done. Unfortunately PSA is not specific for carcinoma of the prostate. Other factors, particularly benign prostatic hyperplasia (BPH), cause elevation of serum PSA and distinguishing PSA elevations due to carcinoma of the prostate from BPH remains problematical. A raised PSA is more likely to lead to a sequence of further studies such as a TRUS examination of the prostate or TRUS-guided biopsies. A significant problem for patients and urologists is a persistently elevated PSA with negative biopsies. Repeated TRUS examinations and biopsies may be required and may lead on occasions to two or even three biopsy sessions. A healthy, asymptomatic patient will be required to be fully acquainted with the potential sequence of investigative events resulting from obtaining a PSA. Recent editorials have called for standardised, informed consent before ordering a PSA test. 6 Suggested information should attempt to answer questions as to the likelihood that a nonscreened asymptomatic man will be adversely effected by prostate cancer in his lifetime (see table opposite), whether the screening test will lengthen, or improve the quality of life, the chances of having a false positive result and its consequences, the value of a normal result, and perhaps the differing recommendations of various experts. A physician and patient-focused study by Chan et al 7 confirm the lack of consensus on which information is considered appropriate by both. More work is needed to decide pertinent information for men with concerns over PSA testing. The European Randomised Study of Screening for Prostate Cancer (ERSPC), a multi-national collaborative randomised trial of screening for prostate cancer, began in The primary objective was to determine whether screening could cause a specific mortality reduction of 20%. Also under investigation are: the best method of screening, what groups are at risk and would benefit most from a screening programme, evaluation of quality of life (QOL) of the participants and the cost-effectiveness of screening to death. The participating centres are in Belgium, Finland, Italy, The Netherlands and Sweden. Screening includes DRE, PSA and TRUS. Some preliminary results and conclusions are available. False-positive rates for TRUS as a primary screening test are too high and it is to be excluded as a screening test in the near future. The first study results will be available in 2007 and will include results from 180,000 men over a 10 year screening period. There are some discrepancies among countries concerning eligibility criteria and indications for biopsy, but collaboration has resulted in a uniform definition of end-points, trial type, recruitment and methods of assessing disease-related mortality. In four of the five countries randomisation occurs after consent with Sweden opting for randomisation before consent. The importance of this study is the recognition that DRE/PSA screening is desirable but should be conducted in the context of a randomised controlled clinical trial. Based on available data there is a bias that relatively young, healthy, asymptomatic men be encouraged to undergo screening by DRE and PSA. Moreover, screening is encouraged in certain subgroups with a higher risk of disease or higher mortality rates such as those with a significant family history of cancer of the prostate. Present data suggest that screening is best achieved by a combination of DRE and serum PSA. 8, 9 Probability of Prostate Cancer by Age > 40 years 1 : 10, : : 8 Wingo PA et al 10
11 8 Prostate Cancer Management Clinical Guidelines Presentation PSA screening increases the incidence of localised disease and decreases the incidence of metastatic disease. Level of evidence III Estimates of cost of PSA-based screening programmes may be exaggerated and a screening programme is likely to be affordable and costeffective. Level of evidence IIb Recommendation 1 Because of a relative increased risk of developing carcinoma in certain subgroups, a selective approach to examination by DRE and PSA is warranted. Recommendation 2 Standardised information should be made available to all asymptomatic patients undergoing PSA. Information should include the following: Likelihood that failure to screen will increase the chance of an undetected carcinoma of the prostate in a man s lifetime. Whether PSA screening will lengthen or improve quality of life. The risk of that a raised PSA results in unnecessary single or serial biopsies. The value of a normal result. Recommendation 3 In patients with lower urinary tract symptoms PSA should be routinely included in investigations. Recommendation 4 Currently it is recommended that screening is best achieved by a combination of DRE and PSA on an annual basis to age 70. Recommendation 5 A screening programme should be introduced in Ireland in the context of a randomised trial for men between 50 and 69 years.
12 Prostate Cancer Management Clinical Guidelines 9 Investigation and Diagnosis Management of Symptomatic Men Routine evaluation of the prostate is necessary in men presenting with lower urinary tract symptoms. Rectal examination and PSA estimation constitute part of standard clinical evaluation. If an elevated PSA is detected, patients require referral for further studies which are determined by factors such as the age and co-morbidity. These factors will assist in determining whether the patient will benefit from further treatment. PSA (2) errors in calculating prostatic volume may approach 25%. Age-Adjusted Reference Ranges For PSA There is evidence that the rise in PSA with increasing age results from prostatic gland growth due to BPH, and the possible increasing prevalence of microscopic, clinically insignificant prostate cancers. Age-adjusted PSA values for normal men are shown in (see table below). 16 TUMOUR MARKERS Role of Prostatic Specific Antigen Strategies to refine PSA for cancer detection have been explored. The common goal is to increase the sensitivity and specificity and positive predictive value of the test leading to a reduction in unnecessary prostatic biopsies. Refinement of PSA values include PSA velocity, PSA density, age adjusted reference ranges for PSA and estimations of free and bound PSA. PSA Velocity PSA velocity refers to the rate of change of serum PSA over time. A number of studies have shown that men with prostate cancer have a more rapidly rising serum PSA in the years before diagnosis than do men without prostate cancer. Patients whose serum PSA increases by 0.75 ng/ml per year suggests that a cancer may be present. 11 PSA velocity must be interpreted with caution. An elevated PSA velocity should be considered significant only when several assays are carried out by the same laboratory over a period of at least eighteen months. 12 PSA Density The PSA levels are proportional to the volume of BPH tissue. PSA levels are 0.12 ng/ml per gram of BPH tissue. As patients with enlarged glands due to BPH have elevated PSAs estimation of the PSA density can be useful. There are problems utilising the PSA density to determine whether a patient requires prostatic biopsy. Many authors have not 13, 14, 15 found PSA density to be useful. Problems using a PSA density includes the following: (1) epithelial/stroma ratios vary from gland to gland, and only the epithelium produces Age Adjusted Reference Ranges for PSA Age (Years) PSA ng/ml Oesterling JE et al 12 MOLECULAR FORMS OF PSA (THE RATIO OF FREE TO BOUND PSA) A large multicentre study has shown that in men with normal rectal examination and a total PSA level between 4 and 10 ng/ml, a 25% free PSA cut-off would detect 95% of cancers while avoiding 20% of unnecessary biopsies. The cancers associated with greater than 25% free PSA are more likely in older patients and generally are of a lower tumour grade 17, 18 and volume. Recommendation 6 PSA testing needs further refinement to limit the number of unnecessary biopsies. Age-adjusted total PSA and free to total PSA results are the most effective format of reporting PSA results. OBTAINING PROSTATIC TISSUE FOR HISTOLOGICAL DIAGNOSIS As a general rule histological confirmation is essential prior to commencing treatment of prostatic carcinoma. Very exceptionally the clinical evidence of locally advanced disease combined with the presence of unequivocal evidence of multiple metastases on
13 10 Prostate Cancer Management Clinical Guidelines Investigation and Diagnosis bone scan and a significantly raised PSA may lead to commencement of treatment with hormones before histological confirmation is obtained. Transrectal ultrasound examination of the prostate alone is insufficient to define prostatic carcinoma. Despite an array of findings on TRUS indicative of prostatic cancer these are only seen in a quarter of affected patients. In addition, despite new techniques and improved ultrasonography imaging it is important to be realistic in accepting that, at present, biopsy of the prostate is essential. TRUS-guided systematic sextant prostatic biopsies have been the most commonly employed technique for confirming prostatic carcinoma. Initially biopsies were targeted at hypoechoic areas in the peripheral zone. This technique was shown to be less effective in detecting cancer than random systematic sextant biopsies. 19, 20 In sextant biopsies tissue is obtained from the apex, mid-section and base on each side of the prostate in the mid-saggital line, half way between the lateral border and the mid-line. Modification of the systematic biopsy strategy is under study. Laterally directed biopsies of the peripheral zone at the base and mid-sector increase the sensitivity of TRUS-guided biopsies by 14%. In large prostates with a volume in excess of 50 grams the addition of TRUS-guided biopsies of the transition zone increases the sensitivity of cancer detection by 13%. 21 TRUS biopsies have associated risks and complications. Some degree of haematuria may be seen in a third of patients undergoing biopsy. Haematospermia and rectal bleeding are common complications, but usually are limited in duration and in clinical importance. A major risk of transrectal biopsy is septicaemia. Reported papers cite an incidence of up to 2% of patients. A common clinical dilemma is negative biopsies with persistent suspicion of underlying cancer. All current biopsy protocols sample a limited volume of prostatic tissue, and the disease is multifocal. Hence false-negative biopsies occur. Despite the number and site of biopsies taken the possibility of missed cancer exists. The question of repeat biopsies then arises. Repeat biopsies should be considered if inadequate tissue for diagnosis or findings suspicious but inconclusive of cancer are reported. The presence of high grade prostatic intraepithelial neoplasia (PIN) mandates repeat biopsies because it is associated with prostate cancer in 50% of repeat biopsies. 22 A rising PSA velocity after negative first biopsy is associated with a significant incidence of positive biopsy on the second or third sampling. Patients in the group have a re-biopsy cancer rate of 31%. 23 Recommendation 7 Histological evidence of prostatic carcinoma in general is essential. Only in exceptional circumstances with overwhelming evidence of advanced cancer should treatment commence without histological confirmation. Hypoechoic-directed biopsies are less efficacious than systematic biopsies especially when combined with laterally placed peripheral zone biopsies and in bigger prostates, transition zone biopsy sampling. Despite improved biopsy techniques tumours are missed and repeat biopsies are then indicated. Level of evidence III Transrectal ultrasound examination of the prostate alone is insufficient to define prostate carcinoma. TRUS-guided biopsies are essential. Level of evidence IIB Recommendation 8 Systematic sextant TRUS-guided biopsy is the method of choice. Positive biopsy rates can be improved by modifying the sextant biopsy technique to include biopsies of the peripheral zone obtained more laterally, and inclusion of some biopsy from the transitional zone in larger prostates. Recommendation 9 Patients undergoing transrectal biopsies should always be given appropriate antibiotics. Recommendation 10 Repeat biopsy is necessary if tissue samples are inadequate, if cellular atypia is identified, where high-grade (3) PIN is seen or in the presence of a rising PSA after a negative first biopsy. Recommendation 11 Biopsied specimens should be labelled and orientated according to local protocol.
14 Investigation and Diagnosis Prostate Cancer Management Clinical Guidelines 11 TNM CLINICAL CLASSIFICATION OF PROSTATE CANCER T Primary Tumour TX TO T1 Primary tumour cannot be assessed No evidence of primary tumour Clinically inapparent tumour not palpable or visible by imaging T1a Tumour incidental histological finding in 5% or less of tissue resected T1b Tumour incidental histological finding in more than 5% of tissue resected T1c Tumour identified by needle biopsy (e.g., because of elevated PSA) T2 Tumour confined within the prostate 1 T3 T4 T2a Tumour involves one lobe T2b Tumour involves one lobes Tumour extends through the prostatic capsule 2 T3a Extracapsular extension (unilateral or bilateral) T3b Tumour invades seminal vesicle(s) Tumour is fixed or invades adjacent structures other than seminal vesicles: bladder neck, external sphincter, rectum, levator muscles, and/or pelvic wall Notes: 1. Tumour found in one or both lobes by needle biopsy, but not palpable or visible by imaging, is classified as T1c. 2. Invasion into the prostatic apex or into (but not beyond) the prostatic capsule is not classified as T3, but as T2. N Regional Lymph Nodes NX N0 N1 Regional lymph nodes cannot be assessed No regional lymph nodes metastasis Regional lymph nodes metastasis M Distant Metastasis MX M0 M1 Distant metastasis cannot be assessed No distant metastasis Distant metastasis M1a Non-regional lymph node(s) M1b Bone(s) M1c Other site(s) Note: When more than one site of metastasis is present, the most advanced category should be used. PTNM PATHOLOGICAL CLASSIFICATION The pt, pn, and pm categories correspond to the T, N, and M categories. However, there is no pt1 category because there is insufficient tissue to assess the highest pt category. G HISTOPATHOLOGICAL GRADING GX G1 G2 Grade cannot be assessed Well differentiated (slight anaplasia) Moderately differentiated (moderate anaplasia) G3-4 Poorly differentiated/undifferentiated (marked anaplasia) Stage Grouping Stage I T1a N0 M0 G1 Stage II T1a N0 M0 G2,3-4 T1b N0 M0 Any G T1c N0 M0 Any G T1 N0 M0 Any G T2 N0 M0 Any G Stage III T3 N0 M0 Any G Stage IV T4 N0 M0 Any G Any T N1 M0 Any G Any T Any N M1 Any G
15 12 Prostate Cancer Management Clinical Guidelines Investigation and Diagnosis carcinoma, mucinous carcinoma, signet ring carcinoma, neuro-endocrine carcinoma, small cell (oat-cell carcinoma), transitional cell carcinoma, squamous adenocarcinoma, sarcomatous carcinoma. Summary Prostate T1 Not palpable or visible T1a 5% 2. The tumour grade is important. The Gleason system is highly recommended. The system proposes histological grades from 1 to 5 based on the patterns of prostatic glandular formation. Adding together the two most prominent patterns gives a Gleason score which has prognostic significance. 3. Tumour amount in the radical prostatectomy specimen should be reported. The percentage of prostate invaded by carcinoma should be noted in relation to the weight of the whole prostate. In TURP specimens the percentage of chips involved is stated but the number of microscopic foci seen is difficult to apply. Combining percentage volume involved with Gleason grade leads to a pathological stage. Volume of tumour in needle biopsies in millimetres should be recorded along with the measurement of each biopsy core. 4. The presence of PIN (grade 2 and 3) should be reported. Grade 1 PIN is not necessarily reported. 5. Surgical margins in radical prostatectomy specimens should be recorded. All prostatic surfaces are considered surgical margins. Areas of particular importance and common sites of extra-capsular extension are at the apex, especially on the lateral and anterior surfaces, and the bladder margin. Any site of extracapsular penetration is identified and reported. Involvement of seminal vesicle by tumour should be recorded. 6. Reporting of perineural invasion is important and has predictive value. The presence of metastases in lymph nodes with the size and number of nodes is recorded.24, 25 T1b >5% T1c Needle biopsy T2 Confined within prostate T2a One lobe T2b Both lobes T3 Through prostatic capsule T3a Extracapsular T3b Seminal vesicle(s) T4 Fixed or invades adjacent structures: bladder neck, external sphincter, rectum, levator muscles, pelvic wall N1 Regional lymph node(s) M1a Non-regional lymph node(s) M1b Bone(s) M1c Other site(s) RECOMMENDATIONS FOR THE HISTOLOGICAL REPORTING OF PROSTATIC CARCINOMA The Association of Directors of Anatomic and Surgical Pathology (ADASP) has appointed a committee to recommend the format of surgical pathological reports for common malignant tumours. The Association recommends that the following specific features which are generally accepted as of prognostic value in prostatic cancer be included:24 The type of specimen should be specified (prostate, prostate plus seminal vesicles). 7. The procedure to obtain specimens should be stated, that is, radical prostatectomy, transurethral resection of prostate (TURP), needle biopsy or Millin or Freyer prostatectomy. Recommendation 12 The Gleason system is the grading system of choice. Microscopic features specific to carcinoma of the prostate should include the type of prostatic carcinoma. Classification includes: adenocarcinoma of the acinar type, ductal Recommendation 13 Sampling and reporting protocols should be standardised throughout the country. 1.
16 Investigation and Diagnosis Prostate Cancer Management Clinical Guidelines 13 Grading for Prostate Carcinoma Gleason Score 2 to 5 Low-grade cancer 6 to 7 Middle-grade cancer 8 to10 High-grade cancer Gleason Grade based on Acinar Pattern 1 to 2 Mainly well-formed acini 3 to 4 Moderate to poorlyformed acini 5 No visible acinar pattern GLEASON SCORE = sum of the 2 highest grades detected IMAGING Transrectal Ultrasound Transrectal ultrasound is useful for guided prostatic biopsy and affords some, if limited, staging information. Most needle biopsies are TRUSguided, allowing regional sampling of the prostate and lesion-directed biopsies. TRUS provides more accurate staging information than DRE. However, staging by TRUS is not as accurate as initially reported. 26 This is particularly so in less advanced tumours which are now more commonly seen with the use of PSA. Ultrasound has at best an overall accuracy of 60% in staging of suspected localised cancer of the prostate. 27 Magnetic Resonance Imaging (MRI) The reported staging accuracy for localised disease with MRI varies from 51 to 92%. High quality images can be obtained but are dependent on individual operator skills and reporting expertise. A comparative trial comparing TRUS and MRI in evaluating the stage of prostate cancer failed to demonstrate a significant difference between the two modalities. 28 Ongoing trials seeking to identify patients who might benefit from MRI studies are 29, 30, 31 in progress. Axial Imaging by Magnetic Resonance or Computerised Tomography (MRI or CT) Cross-sectional imaging of the pelvis is performed in selected patients to exclude lymph node metastases in high-risk patients being considered for radical local therapy either by surgery or irradiation. The incidence of involved lymph nodes in recent radical prostatectomy series is low (<10%). A review of the literature by Wolfe et al 1995 encompassing 15 series and 1,354 patients revealed an incidence of lymph node metastases of 22%. The sensitivity for CT and MRI in this analysis was 36% and the specificity was 97%. Imaging for lymph nodes is expensive and inaccurate. The likelihood of lymph node metastases can be quantified on the basis of PSA, tumour grade, and local tumour stage. Several nomograms and probability curves exist that aid in predicting 32, 33 pathological stage.
17 14 Prostate Cancer Management Clinical Guidelines Investigation and Diagnosis Staging of prostate cancer by TRUS is inaccurate, particularly in smaller tumours detected by PSA. Imaging is more accurate than staging by DRE. MRI has not been shown to be significantly more efficacious in comparative trials. CT and MRI to detect lymph nodes have a sensitivity of 36% and a specificity of 97%. Imaging for lymph nodes is expensive and inaccurate. Risk of lymph nodes best quantified by combination of PSA, Gleason score and DRE. Level of evidence IV Recommendation 14 Further studies and radiological developments are needed to define the most appropriate modality to stage carcinoma of the prostate pre-operatively. Bone Scan The merits of obtaining a bone scan to stage disease extent prior to radical local therapy is under consideration at present. Oesterling and colleagues conducted studies to assess the ability of PSA to predict bone scan findings (1993). Their results showed that bone scans can be omitted in patients with newly diagnosed, untreated prostatic cancer who are asymptomatic and have PSA less than 20 ng/ml. PSA levels alone were the best predictor of bone scan results.34 There have been recommendations that bone scans may be omitted in patients with PSA between 10 and 20 ng/ml. However, bone scans are readily available and are not associated with serious toxicity, are relatively cheap and have a high sensitivity. Failure to recognise metastases prior to radical therapy subjects patients to significant and unwarranted risks. Bone scans should be included as a standard part of the evaluation of all patients undergoing surgery or XRT.35 Recommendation 15 Routine bone scans should be included in patients undergoing radical surgery or XRT.
18 Prostate Cancer Management Clinical Guidelines 15 Treatment of Prostate Cancer RECOMMENDATIONS FOR SELECTION OF THERAPY FOR LOCALISED PROSTATE CANCER The biological behaviour of prostate cancer can be predicted using clinically available data. The combination of clinical stage, Gleason score, and the level of prostate specific antigen (PSA) can be used to predict the risk category of individual patients. Nomograms have been published which relate these pre-treatment prognostic factors to the pathologic stage. 36 Such information allows identification of categories of patients suitable for local treatment (surgery or radiation) and also those for whom a local treatment alone is inadequate. Screen-detected cancer (T1c stage) Screen-detected cancers are clinically heterogenous. If the patient has T1c clinical stage, PSA less than 10, and Gleason score less than 6 the probability of having organ-confined disease when treated with radical prostatectomy is 67% to 89%. If the patient has T1c clinical stage, PSA in the range of 10.1 to 20, and Gleason score under 5 the probability of having organ-confined disease when treated with radical prostatectomy is 60-75%. The above categories can be treated with radical prostatectomy, external beam radiation, or brachytherapy. For T1c clinical stage, PSA in the range of 10.1 to 20, and Gleason Score of 6 the probability of having organ-confined disease when treated with radical prostatectomy drops to 55%. If the PSA is > 20 or if the Gleason score is 7 or higher the probability of organ-confined disease becomes low and other strategies are appropriate. Identifying non-screen-detected, low risk localised cancers For patients with clinical stage T1 cancers and PSA of 0-20 and Gleason score of 6 or less, the probability of having organ-confined disease when treated with radical prostatectomy is generally approximately 55-84%. If the PSA is close to 20 it is useful to specifically consult the Partin nomograms. These patients can be treated with radical prostatectomy, external beam radiation, or brachytherapy. For patients with clinical stage T2 cancer and PSA of 0-10 and Gleason score of 4 or less, the probability of having organ-confined disease when treated with radical prostatectomy is generally approximately 60%-81%. For T2 tumours with a Gleason score of 5 or higher or a PSA above 10 it is necessary to consult a published nomogram to assess the probability of organconfined disease before embarking on a purely local treatment alone. High-risk localised cancers If the Gleason score reaches 7 or higher, regardless of PSA or clinical stage, the probability of organconfined disease is less than 50%. If the PSA is > 20 regardless of Gleason score or clinical stage it is unusual (<50%) to have organconfined disease. Furthermore, this probability declines dramatically in proportion to the Gleason score and the clinical stage. Historically such patients have been treated with radiation alone with a high resulting rate of PSA detected failure. This is because there is a high risk of relapse by spread to other parts of the body. Similarly all patients with nodal metastases are at extremely high risk of developing further metastatic disease. All such patients should be treated with adjuvant hormonal therapy. In such high-risk patients radiation is the usual locoregional treatment. 37 MANAGEMENT OF POTENTIALLY CURABLE PROSTATIC CARCINOMA (T1-T2, NO,MO) Optimal forms of therapy for all stages of carcinoma of the prostate remains debatable. Dilemmas in the management of T1 and T2 prostate carcinoma persist because of the uncertainty about the relative efficacy of available treatment modalities. There are three viable treatment options; radical prostatectomy, X-ray therapy, and surveillance. Well-designed randomised trials comparing these three treatment options for localised prostate cancer are lacking. Despite the lack of strong data certain agreed practices can be considered as minimum standard of care in early prostatic cancer.
19 16 Prostate Cancer Management Clinical Guidelines Treatment of Prostate Cancer Total assessment of the health status of the patient This factor impinges on the choice of treatment for any individual patient. Life expectancy is an important consideration. The presence of comorbidity is highly relevant, as many patients with carcinoma of the prostate have intercurrent disease processes which represent competing risks for death before and especially after radical treatment. Intercurrent disease reduces the chance that suffering related to advancing prostatic cancer or cancer-specific death will occur. In addition, comorbid conditions weaken the resilience of patients to adverse effects of treatment. In a relatively young man (<60 years of age) the lifetime chances of disease progression is high. A window of opportunity for cure exists and some form of curative therapy should be on offer to such a patient.38, 39 The pathological stage of prostate cancer The stage of cancer is crucial. Small-volume, welldifferentiated tumours in the older patient may be indolent, while large-volume, more poorlydifferentiated (Grade 7 and 8) are aggressive. As a consequence, specific patient and tumour-related factors may determine the treatment of choice. Because of the uncertainty concerning efficacy of treatment patients must be fully informed of available treatment options. After full disclosure of information patient preference must be part of the decision-making process. There is uncertainty about the relative efficacy of available treatment modalities. Well-designed prospective randomised trials comparing radical prostatectomy, XRT and surveillance for localised prostate cancer are lacking. Level of evidence III In the absence of clear advantages of one treatment over another, the treatment decision is based on the stage and grade of tumour, the health status and life expectancy of the patient, efficacy of the recommended treatment to ensure prolonged disease-free survival, the associated complication rate, and patient and surgeon preference. Level of evidence III Recommendation 16 As far as is practical, information should be given about best available treatments for the individual circumstances of the patient s cancer, health status and life expectancy. SURGERY OF PROSTATIC CANCER Radical Prostatectomy Information to the patient must include the advantages and disadvantages of the procedure. There is an opportunity for cure which means lifelong freedom from recurrence of the disease. The peri-operative mortality (up to 30 days) is low at 0.3%, and consistent across most published series.40 Local control of the disease is improved by radical surgery even if the impact on disease-free survival is uncertain. The complications of surgery are significant and may impact more severely on younger, otherwise healthy, patients who are the group most likely to be targeted for surgery. A high risk of impotence remains after radical prostatectomy and relates particularly to the stage of disease and the age of the patient. An anatomical approach using nervesparing techniques has lowered the incidence of erectile dysfunction. There may, however, be some compromise in regard to total excision of the tumour. This may be a particular problem as capsular penetration is often seen in the neuro-vascular groove especially at the apex.41 Urinary incontinence rates have improved with better surgical technique, due to better understanding of the anatomy of the apex of the prostate and the relationship of the dorsal venous complex to the sphincteric mechanism. Total urinary incontinence is rare (<3%) as reported. A variable degree of stress incontinence may occur in up to 20% of patients. In general return of continence after surgery is gradual with 75% of patients dry at 6 months.42, 43 Detailed follow-up after radical prostatectomy is required to assess the patient s quality of life of which continence and erectile function are important dimensions. In a quality surgical programme less than 3 to 5% of patients should need continence appliances or more than 2 pads per day. The rate of artificial sphincter required should be very low. Survival after surgery for organ- confined disease ranged from 70 85% in several series.
20 Prostate Cancer Management Clinical Guidelines 17 Treatment of Prostate Cancer The Results of Radical Surgery Most long-term results come from the U.S., Walsh reporting on nearly 1000 men undergoing surgery found 11.2% to have a raised PSA at 5 years as the only evidence of tumour recurrence. Actuarial likelihood of a stable progression-free PSA at 5 and 10 years was 87 and 77% respectively. An international pool group of 2,975 radical prostatectomies in men with localised prostatic cancer reported 10-year disease-specific survival of 94%, 85% and 77% from men with grade 1, 2, 3 tumours respectively. Since the introduction of PSA testing there has been an increase in the incidence of prostate cancer and a reduction in those presenting with advanced disease. There has been a large rise in the radical prostatectomy rate from 9% of all new cases of prostatic cancer in 1983 to 29% in These changes in practice coincide with the first fall in overall mortality from prostatic cancer in the U.S.A. from 26.5 to 17.3 deaths per 100,000 men between 44, and Quality Standard 1 Less than 3% of patients should be wet to such a degree at one year as to require multiple pads, or implantation of an artificial sphincter. Quality Standard 2 Patients should be followed in a specialised urology department. Data relating to quality of life, detected clinical recurrence rate, recurrence rate by PSA or imaging, survival rates, and complications can thereby be recorded and analysed. Radical prostatectomy improves local control of disease, but its impact on survival remains uncertain. Recently there has been evidence of a fall in mortality which coincides with an increase in detection of earlier disease and a significant rise in the number subjected to radical prostatectomy (between 1990 and 1995). Level of evidence IIB Recommendation 17 Prior to surgery (radical prostatectomy) patients must be informed about major morbidity which includes the risks and incidence of impotence and incontinence of urine. Recommendation 18 Radical prostatectomy should be performed by surgeons appropriately trained in the procedure, within an institution with medical and nursing personnel trained in the care of such patients. DISEASE RELAPSE AFTER PROSTATE SURGERY FOR LOCALISED PROSTATE CANCER A rise in PSA after surgery indicates tumour relapse. Recurrence after radical prostatectomy is related to cancer grade, pathological stage, and degree of capsular penetration. Local recurrence is more common in those with positive margins, seminal vesicle invasion, extra-capsular extension and a high Gleason score. The site of relapse of tumour after radical prostatectomy can be established with reasonable certainty by the interval from surgery to a detectable rise in PSA. Patients with persistent elevated PSA detected immediately or shortly after surgery or those with a rapid doubling of PSA in the post-operative period (6 months) are likely to have systemic spread of the disease. Local recurrence is more likely if the rise in PSA occurs a long time after surgery, and the PSA doubling-rate is prolonged. Average time to detection of a raised PSA is longer 46, 47 in local as opposed to distant relapse. Initially patients with relapse will be detected by a rise in PSA but localised recurrence may be detected by DRE or TRUS or both. Confirmation of relapse by biopsy is useful, but several biopsy sessions may be needed to document a local recurrence, because of the difficulty of obtaining tissue in these circumstances.
21 18 Prostate Cancer Management Clinical Guidelines Treatment of Prostate Cancer Prognosis In men who develop elevated serum PSA after radical prostatectomy, the natural history of progression to distant metastases and death as a result of adenocarcinoma of the prostate is virtually unknown.48, 49 A study was done on 1,997 men with localised prostate cancer after radical prostatectomy. None received neoadjuvant or adjuvant hormones prior to documentation of metastases. Actuarial metastatic free survival was 88% fifteen years after surgery. Of the 1,997 men 15% developed PSA elevation and 34% of these developed metastatic disease within the length of the study (15 years). Median time to metastases was 8 years from time of PSA elevation. After metastases developed, median time to death was 5 years. Patients who relapse may be offered radiotherapy alone or radiotherapy plus hormones. The role of radiotherapy with or without hormones for local recurrence is unclear. There is often a good initial biochemical response but prolonged survival remains to be demonstrated with or without treatment.50 Evidence of local recurrence after radical prostatectomy is a rise in PSA, palpable recurrence of tumour and biopsy-proven recurrence of cancer. The dose of radiation can be increased with XRT techniques as described for primary treatment. Up to 70 Gy (Gray) can be delivered for early recurrent disease with higher doses reserved for patients with bulky local recurrent disease. THE ROLE OF ADJUVANT X-RAY THERAPY FOLLOWING RADICAL PROSTATECTOMY The object of adjuvant XRT is to improve local control by eliminating microscopic residual tumours in the surgical bed and peri-prostatic tissues. Several indications for adjuvant XRT may arise. Despite best practice pre-operative staging of the disease the following situations occur: (a) positive surgical margins, (b) seminal vesicle involvement and (c) extra-capsular extension. The presence of any of these variables is associated with a high probability of local recurrence. Several early studies suggest that adjuvant XRT appears to reduce the incidence of local recurrence in patients with post-surgical positive margins. Studies suggest that those treated may have improved disease-free survival and improved time to distant metastases and a lower incidence of PSA failure.51, 52 However, the impact of adjuvant radiation on survival outcomes remains uncertain. There is a high complication rate with post-operative XRT particularly utilising older treatment techniques. Contemporary series suggest that with more modern planning techniques and equipment the incidence of complications is lower.53 A rise in PSA after surgery indicates tumour recurrence. Detectable rise in PSA soon after surgery (a doubling time in 6 months) is indicative of systemic spread of disease. Level of evidence III Confirmation by TRUS biopsy of local recurrence is useful but difficult to achieve. Level of evidence III Patients with positive margins, capsular involvement or seminal vesicle involvement may benefit from adjuvant X-ray therapy with or without hormones. Impact on survival rates is unknown. Complication rates with 3-dimensional conformal radiotherapy (3D CRT) are reportedly lower than with conventional XRT. Doses up to 70 Gy with low complication rates are reported. Level of evidence III Recommendation 19 Patients with local recurrence after radical prostatectomy should be given 3D conformal radiotherapy plus hormones.
22 Treatment of Prostate Cancer Prostate Cancer Management Clinical Guidelines 19 RADIATION THERAPY EXTERNAL BEAM THERAPY FOR LOCALISED CANCER (T1-T2, N0, M0) Traditional external beam radiotherapy (XRT) enables delivery of 65 to 70 Gy to the prostate. Older X-ray techniques fail to provide adequate dosage of radiation to the target volume in as many as 20-40% of patients. Improved imaging and the use of 3-dimensional treatment planning software can now guarantee that the treatment field is accurately targeted. A higher dose of radiation can be delivered to the prostate without exceeding the tolerance of surrounding tissue, mainly the bladder and rectum. This is achieved by conforming the radiation beam to the shape of the prostate. Conformal radiotherapy is achieved by designing blocks from re-constructed CT images as viewed from the vantage point of the beam source. When viewed from the central axis, they are usually called beam-eye views. Computer assisted beameye views can be generated to design oblique and out-of-plane or non-co-planar beam arrangements. This approach constitutes 3-dimensional conformal radiotherapy. The technique enables dosage to be calculated in 3-dimensions enabling scattered radiation to be accounted for, the ability to generate 3-dimensional dose displays and dose volume histograms. 3-dimensional dose displays allow hot and cold spots (over- and under-dosing) to be recognised while dose-volume histograms allow alteration in technique to be ranked for differential sparing of surrounding tissues. Compared with standard technique 3-dimensional conformal radiotherapy (3 D CRT) is associated with 30% reduction in dose received by 50% of the rectum. 54 Advantages in treatment planning have resulted in 3 D CRT as the new standard of care. 55 The main advantage of 3 D CRT is the increased radiation dosage that can be given which theoretically may lead to improved local control. Data from Memorial Sloan Kettering Cancer Centre and M.D. Anderson Cancer Centre suggest PSA response improves with higher doses of radiation. Early results from these centres suggests that 10% 56, 57 increase in dosage improves local control by 20%. Normal tissue toxicity is the limiting factor. Two prospective randomised trials had demonstrated no difference in acute toxicity in patients with localised prostatic carcinoma treated with 3 D#CRT versus conventional radiotherapy. Of more importance, in the MD Anderson studies higher doses were given to patients receiving 3 D#CRT and the incidence of 58, 59, 60 chronic rectal toxicity was reduced. Conventional XRT fails to provide adequate radiation dosage to the prostate in upwards of 20-40% of patients. Level of evidence IIB With 3D CRT radiation dosage can be increased more safely which theoretically may improve tumour control. Level of evidence IIB Recommendation 20 Before radiotherapy patients should be informed of potential complications of radiation proctitis/cystitis and impotence. Recommendation 21 Where patients are assigned to XRT the advantages in delivery to the prostate makes 3D CRT the new standard of care in XRT treatment of carcinoma of the prostate. In several randomised trials XRT plus hormones (neoadjuvant or adjuvant) has proved superior to XRT alone in certain categories of localised prostatic cancer. Level of evidence IA Recommendation 22 XRT combined with neoadjuvant hormone ablation should continue to be evaluated by randomised controlled clinical trials. Quality Standard 3 Following radical radiotherapy of the prostate, the incidence of severe late complications (beyond 90 days) to bladder and rectum, should be less than 5% at 2 years. Quality Standard 4 Patients undergoing radical radiotherapy should be followed by a specialist unit. Data regarding quality of life, survival, local and distant recurrence, and morbidity can thereby be recorded.
23 20 Prostate Cancer Management Clinical Guidelines Treatment of Prostate Cancer RELAPSE AFTER RADIATION THERAPY DIAGNOSIS AND TREATMENT After X-ray therapy PSA levels may decline slowly and take many months to reach its nadir. The rate of decline is not a reliable prognosticator of outcome, but a rising PSA following definitive XRT is indicative of a cancer relapse as clinical relapse inevitably follows biochemical failure. TRUSguided biopsy of the prostate may identify local recurrence while bone scan and pelvic CT identify distant recurrences. Standards set by the American Society for Therapeutic and Oncological Consensus Panel requires three consecutive increases in PSA obtained at intervals of three to four months in the two years after the completion of radiotherapy. 61 Recurrence of disease (as in failure after surgery) can be judged to be local if the rise in PSA occurs at a long interval after therapy, while early elevation after XRT may indicate metastatic relapse. The site of relapse of cancer is indicated by the PSA doubling-time. Metastatic disease predictably has a doubling-time of less than 6 months, while a longer doubling-time is more consistent with local relapse. MANAGEMENT OF PROSTATE CANCER AFTER FAILED RADIATION THERAPY Cryotherapy and Salvage Prostatectomy Failure of radiation therapy promotes tumour aggressiveness and outcome is poor. In some patients the persistent disease appears to be localised. Use of cryotherapy has been reported as salvage therapy for patients with local recurrence after full dose radiation therapy, with or without hormones. Best results are obtained with a double rather than a single freeze-thaw cycle. Reports on 150 patients from MD Anderson with locally recurrent disease after radiation or other combined therapies are not impressive. 62 One-third of patients had undetectable PSA but 20 to 33% of patients had persistent positive prostatic biopsies. The complication rate is significant, including high rates of incontinence and urinary obstruction. Salvage radical prostatectomy was reported by Scardino and colleagues. 63 The complication rate was high. Contemporary studies suggest that salvage cryotherapy and salvage prostatectomy should be used only in the context of a prospective study in patients with persistent disease after radiotherapy. Salvage therapy by radical prostatectomy or cryotherapy give poor results and a high complication rate. Salvage prostatectomy or cryotherapy should be used as part of a study protocol. Level of evidence IV
24 Prostate Cancer Management Clinical Guidelines Treatment of Prostate Cancer RADIATION THERAPY FOR FOR LOCALLY ADVANCED PROSTATIC CANCER HIGH RISK LOCALISED DISEASE (T3-T4, N0,MO DISEASE) In several randomised trials hormones (neo-adjuvant) plus XRT has proved superior to XRT alone. Pilepich and colleagues65 demonstrated improved disease control and disease-specific survival with neoadjuvant hormone priming and X-ray therapy. Four hundred and fifty-six patients were included in the study. Patients had high volume T2, T3 and T4 disease and were randomised to either XRT with total androgen blockade (two months before and two months during XRT) or to XRT alone. The results of the study showed disease control of 63% versus 51% in favour of the combined therapy. Distant failure occurred in 34% versus 48% and disease-specific survival was 51% versus 43%. There was no evidence of progressive disease in 35% versus 23% in the study arm compared with the control arm of the study. Bolla and his colleagues studied 401 patients with predominantly T3 localised disease. The patients were randomised to receive 3 years of androgen ablation and XRT compared with XRT alone. Improved survival in patients receiving combination therapy was demonstrated. Results showed better local control in 97% of patients versus 77%, diseasefree status in 85% versus 48% for the controls and overall survival 79% versus 62% in the controls.64, 65, 66 Many studies, both prospective and retrospective, confirm the efficacy of radiation therapy in the control of localised prostatic cancer (stage T3). The end point of the studies was based on clinical assessment of local control. In the PSA and TRUS biopsy era clinically judged end points are now known to underestimate the true incidence of local failures because of missed cancers in clinically assessed patients. Many patients clinically free of disease can be shown by PSA or TRUS or both to have persistent disease. The median interval between PSA failure and clinical failure can be as long as 4-5 years67 and a number of strategies to obtain and maintain the lowest possible nadir have been developed. Dose escalation of XRT beyond 70 Gy to 84 Gy by 3-dimensional conformal radiotherapy has been tested and shown to reduce the risk of biochemical failure. Prospective and retrospective studies confirm the efficacy of XRT in the control of localised advanced prostatic cancer (T2b, 3 and 4). Failure rate as determined by PSA decrease when XRT dose is escalated. Level of evidence IB XRT plus neoadjuvant hormones is superior to XRT alone. Patients with T3 and T4 tumours need to be the subject of continuing clinical trials. Level of evidence IA Recommendation 23 Neoadjuvant or adjuvant hormone therapy should be included in the protocol for high risk localised prostatic tumours. Grade A BRACHYTHERAPY The most common form of alternative radiation is brachytherapy. A major theoretical advantage is the ability to deliver high dose-radiation to a localised area and fewer treatment visits. Contemporary series report the use of CT- or TRUS-guided closed techniques. The high failure rates reported in older series suggest that permanent implants without accurate placement were less effective than XRT. Poor placement of radioactive seeds led to suboptimal dosimetry. More recent techniques employing CT- or TRUS-based guidance with site and spacing predetermined by imaging have led to better results. Commonly used isotopes are Iodine 125 or Palladium 130 which are left in place permanently. Permanent implants mean lower dose rates and higher total doses. Brachytherapy can be used alone in early disease (T1/T2) or in combination with XRT. Many comparative studies suggest that brachy therapy alone is a reasonable treatment option for low risk patients with organ confined disease with minimal extra-capsular extension. Because of rapid dose fall-off, when used in high risk patients or those with more extensive local disease it should be combined with XRT. Recently there has been increased interest in temporary or high dose-rate implants. The advantages are decreased exposure risks to hospital personnel and compensatory effects of sub-optimal seed placement. Temporary seed implantation is 21
25 22 Prostate Cancer Management Clinical Guidelines Treatment of Prostate Cancer associated with higher morbidity, and needs inpatient treatment. Iridium-192 is the only widelyused isotope for temporary implantation. Available numbers of patients for meaningful follow-up are small and no firm conclusions about efficacy can be drawn. In summary, results continue to suggest that interstitial therapy appears to be a promising therapy for selected patients with early stage disease. A benefit in more advanced local disease is 68, 69 best achieved in combination with XRT. In older series of patients treated with brachytherapy poor placement of radioactive seeds led to sub-optimal dosimetry. More recent techniques using CT- or TRUS- guidance with site and spacing pre-determined by imaging have led to improved results. Level of evidence IIA Comparative studies suggest that brachytherapy alone is useful in low-risk patients with organconfined disease or minimal extra-capsular extension. Level of evidence IB Rapid dose fall-off makes brachytherapy less suitable for extensive local disease unless combined with XRT. Level of evidence III
26 Conservative Management of Prostatic Cancer Prostate Cancer Management Clinical Guidelines 23 SURVEILLANCE In some patients with localised prostatic cancer a slow rate of progression of the disease occurs and surveillance may be a genuine alternative to proactive treatment by surgery or radiotherapy. Several studies have shown that surveillance alone may be an appropriate form of treatment for selected patients with prostatic carcinoma (see table below). No randomised control trial has been reported on surveillance to date. All reports on the subject consist of a cohort of men selected for a variety of different reasons. The studies suffer from shortcomings due to selection bias, short follow-up, predominant inclusion of older patients, initiation of delayed treatment in many patients and incomplete records as to cause of death. A pooling of data from 4 studies demonstrated that a relatively consistent pattern emerges: (1) At ten years after diagnosis 8-10% of men with low-grade disease will die of carcinoma of the prostate following watchful waiting compared to those treated with surgery or X-ray therapy. (2) The risk of observed metastases is high at 10 years in men on watchful waiting. Eight to ten percent men with low-grade disease and 15-20% with moderately-differentiated disease develop metastases at 10 years. (3) With time prostate cancer progresses in a substantial percentage of patients requiring palliative treatment for pain, urinary obstruction or haematuria. Few of the studies address the quality of life issues which include side-effects of hormones, impact of refractory hormone disease, the need for repeated transurethral resections, bone pain and the need for treatment of bone pain by palliative radiotherapy and pain control clinics. The potential for these events to occur is offset by the fact that a patient may die of an unrelated illness. (4) Competing mortality rates from unrelated disease is significant and is higher than prostatic cancer mortality rates. (5) The disease-specific survival rate at 10 years for patients with well- or moderately- differentiated tumours is 87% and for patients with poorlydifferentiated tumours the disease-specific survival is 34% at 10 years. 70 In summary a policy of surveillance is associated with a significant rate of tumour progression but is often consistent with protracted survival. Comorbidity is a significant cause of mortality. Longterm survival occurs despite the presence of prostate cancer. Expectant treatment, however, will not provide a resolution of prostate cancer problems and better criteria for patient selection and quality 73, 76 of life issues require further definition. Expectant treatment does not provide a resolution of cancer problems, and is associated with a significant rate of tumour progression but is often consistent with protracted survival. Level of evidence IIA Recommendation 24 Surveillance is an acceptable form of treatment in men with T1a tumours with a poor life expectancy (less than 10 years) due to the age at which the disease is detected or co-morbid factors. 71, 72, 74, 75 Results Of Surveillance Studies Study Year Number Follow-up Overall % Disease-specific Disease (years) Mortality Mortality Progression Johansson (1994) % 10% 34 George (1998) % 4% 83 Whitmore, Warner & Thompson (1991) % 15% 69 Adolfsson J (1992) ±3 44% 12%
27 24 Prostate Cancer Management Clinical Guidelines Metastatic Prostate Cancer HORMONAL THERAPY Hormonal therapy is the optimum treatment for locally advanced and distant disease, and is equally effective whether administered by orchidectomy or by LHRH agonists. Response rates in patients treated with hormones is high. Most prostatic cancers are hormone-dependent, and initial therapy decreases or stabilises PSA values and clinical symptoms in approximately 90% of patients. The average duration of response to hormones is 18 to 36 months. Patients with metastatic disease, whether symptomatic or not, should be offered some form of hormonal therapy. The options for first line therapy to induce androgen deprivation are bilateral orchidectomy or LHRH analogue therapy by either monthly or 3 monthly depot injection. The therapeutic efficacy of orchidectomy and LHRH analogues is comparable and all current LHRH analogues are equally effective. 77 LHRH analogues require anti-androgen blockade for 7-10 days prior to administration of LHRH analogue to prevent tumour flare. Orchidectomy can be either total or sub-capsular. Both have equal therapeutic value. Retaining some capsular tissue in the scrotum may improve the patient body image and have a psychological advantage. Timing of Hormone Manipulation Metastases causing bone pain is a clear indication to start hormone therapy. Systemic effects of metastatic disease including weight loss, anaemia, and poor performance status indicate the need for immediate therapy. Cord compression is a serious complication and requires urgent treatment. Hormone manipulation, in conjunction with X-ray therapy and surgery, forms an important component of treatment of cord compression and pathological fracture. Timing of initial endocrine treatment in asymptomatic patients with multiple metastases is a subject of some debate. A randomised study from the Medical Research Council compared early and deferred hormone manipulation in patients with locally advanced or metastatic disease. Therapy was mainly by LHRH agonists but occasionally by orchidectomy. Approximately 50% of the patients were M1 or M0. Within the immediate androgen deprivation arm, there was a statistically significant decrease in morbidity secondary to disease. In addition there was a lower complication rate from cord compression, ureteric obstruction and pathological fractures in patients treated by early endocrine therapy. 78 While early treatment has been demonstrated to have advantages, the main deterrents are the effects on the quality of life (QOL). Decreased libido and erectile dysfunction are inevitable, but insidious morbidity includes muscle wasting, anaemia, depression and osteoporosis. Several treatment strategies are employed to address these problems. Pulse therapy, in which cycles of therapy with LHRH agonists are given at intervals of 3 to 4 months, allows restoration of testosterone levels and rehabilitation from side-effects. This programme of treatment is currently under investigation in an inter-group study in the U.S.A. 79 Another approach involves high doses of non-steroidal anti-androgens to block androgen receptors in the prostate while preserving serum testosterone levels peripherally. A large randomised trial using bicalutamide (Casodex) 150 mgs versus orchidectomy in men with M0 stage Immediate Versus Delayed Hormone Therapy MRC Study (1997) 9 Complication Immediate Hormonal Therapy Delayed Hormonal Therapy Pathological bone fracture 2.3% 4.5% (N/S) Spinal cord compression 1.9% 4.9% (p < 0.025) Ureteric obstruction 7.0% 11.8% (p < 0.025) Extra-skeletal metastases 7.9% 11.8% (p < 0.05) TURP 13.9% 30.3% (p < 0.001)
28 Prostate Cancer Management Clinical Guidelines 25 Metastatic Prostate Cancer disease is under way. A 4-year median follow-up shows significant improvement in QOL and no difference in survival. Oestrogens Oestrogens have a proven record in control of adenocarcinoma of the prostate. They are associated with a significant incidence of thromboembolic complications and aggravation of vascular episodes such as stroke and myocardial infarction. The complications are dose-related and less common in patients receiving doses of 1-2 mgs of stilboestrol daily. Cyproterone Acetate (Androcur) The value of cyproterone acetate is in the management of hot flushes in patients with acutely induced castrate levels of testosterone by orchidectomy or by LHRH analogues. Bicalutamide (Casodex) The most widely used method of androgen deprivation for advanced prostatic cancer is bilateral orchidectomy or medical castration. Orchidectomy or medical castration affect adversely the quality of life and result in loss of libido and cause erectile dysfunction. Bicalutamide, a potent anti-androgen effectively blocks androgen receptors, and could eliminate the need for surgical (which is irreversible) or medical castration. The standard daily dose of bicalutamide is 50 mgs, but higher doses (150 mgs per day) have been shown to reduce the level of PSA more quickly and to a lower level. Monotherapy at higher doses might be as effective as castration with fewer adverse effects. Two open multi-centre randomised trials compared the efficacy, tolerance and quality of life benefits of bicalutamide with castration. Patients included in the study had stage T3/T4 locally advanced (Mo) prostate cancer with PSA levels greater than 20 ng/ml. All patients were untreated for prostate cancer. In a 2:1 ratio, 458 patients were randomised to either bicalutamide 150 mgs per day (N=320) or castration by orchidectomy or goserelin acetate (N=138). Primary end-points were time to death, objective progression, treatment failure and quality of life. Demographic characteristics were similar in both groups. At median follow-up of approximately 4 years the risk of death was similar in both arms. However, bicalutamide demonstrated significant advantages over castration in retention of sexual interest and erectile capacity. There was a higher rate of gynaecomastia and breast pain with bicalutamide. The main advantage of bicalutamide is that it is taken orally, is reversible, and preserves libido and sexual function. This study was expanded to enroll a total of 1,453 patients. All of these patients had confirmed metastatic disease (M1) or T3-T4 non-metastatic disease with raised PSA. At 100 weeks follow-up showed that bicalutamide was less effective than castration in men with M1 disease with a median survival difference of 6 weeks. In symptomatic patients with M1 disease bicalutamide was associated with significant improvement in subjective response compared with castration and was superior to castration in maintenance of sexual interest and capacity. The incidence of hot flushes was significantly lower with bicalutamide. The conclusions of the study were that in men with M1 prostate cancer bicalutamide 150 mgs per day is less effective than castration but leads to a better quality of life and subjective response in symptomatic men with M1 disease and is welltolerated. 80, 81 Monotherapy with bicalutamide at 150mgs per day is an option for men with T3-T4 (M0), or M1 disease for whom surgical or medical castration is not acceptable. Level of evidence IA Complete Androgen Blockade Although testosterone is the major circulating androgen, the adrenal gland secretes dehydroepiandrosterone and androstenedione. Some investigators believe that suppression of both testes and adrenal androgens improves initial and longterm response rates compared to testis blockade alone. Complete androgen blockade (CAB) can be achieved by combining LHRH analogues or orchidectomy with an anti-androgen agent. Patients with good performance status and limited metastatic disease treated by CAB seem to survive longer than those treated by LHRH agonists alone. In patients with advanced disease and poor performance status response to CAB is poor. 82
29 26 Prostate Cancer Management Clinical Guidelines Metastatic Prostate Cancer CLINICAL MANAGEMENT OF PATIENTS WITH METASTATIC DISEASE Patients with metastatic disease require regular follow-up by clinical, biochemical and haematological assessment. Bone scan is required to identify specific metastases which may give rise to localised severe bone pain. These locally painful metastases should be amenable to XRT (regional irradiation). Patients on deferred treatment protocols require careful monitoring. Detection of a rapidly accelerating PSA or increasing bone pain or systemic manifestations of prostate cancer are indications to commence hormone treatment. Response rates to hormone therapy in patients with metastatic prostatic cancer are 90%. Level of evidence III Orchidectomy and LHRH analogue are equally effective in treatment of prostate cancer. Acceptability and QOL factors of orchidectomy require further study. Level of evidence IB Recommendation 25 Patients with symptomatic metastatic disease, especially bone disease, should commence therapy by androgen deprivation. The choice of primary treatment by LHRH analogues or orchidectomy is determined by many issues including patient preference. Current evidence shows no clear treatment advantage in combined androgen blockade, especially in patients with poor performance status and advanced disease. Level of evidence IB Recommendation 26 Combined androgen blockade should not be used routinely on current evidence. Grade A MANAGEMENT OF THE COMPLICATIONS OF ADVANCED PROSTATIC CANCER Spinal Cord Compression Metastases to the subdural space often lead to cord compression. Lower limb weakness, paraesthesia, bladder and bowel dysfunction are consequences of this emergency situation. Prevention of paraplegia is important as restoration of function in established paralysis occurs in less than 10% of patients. Urgent investigation by MRI will identify the site or sites of spinal involvement and the extent of pathological compression of the cord. In ambulatory patients radiation rather than surgery is effective in relieving cord compression. However, paraplegic patients often do not recover function when treated with radiation, steroids or androgen deprivation. In these patients laminectomy with or without radiation may be a suitable alternative. However, surgery should be offered cautiously in those patients as survival averages 3.9 months in this group of patients after laminectomy. When indicated urgent surgery to decompress the spinal cord should be undertaken by a specialist in spinal surgery. Patients should initially be treated with dexamethasone to decrease cord oedema and androgen deprivation.83 Recommendation 27 Spinal cord compression is an indication for urgent referral for radiotherapy or surgery.
30 Metastatic Prostate Cancer Prostate Cancer Management Clinical Guidelines 27 URETERIC OBSTRUCTION Ureteric obstruction occurs from direct invasion by the tumour or compression of the ureters by enlarged lymph nodes. When this occurs despite hormone therapy the prognosis is poor. In the event of an untreated patient presenting with renal failure due to bilateral ureteric obstruction, resolution of the problem may be induced by androgen deprivation. Management usually involves placement of a J stent in both ureters. Cystoscopic placement can be difficult if trigone invasion by the prostate cancer is present. Ureteric orifices are often obscured by disease and bilateral percutaneous nephrostomies may be required followed by J stents placed antegradely into the ureter. These measures are palliative and may offer a variable survival with good quality of life. HORMONE REFRACTORY PROSTATE CANCER (HRPC) Treatment of patients with prostatic cancer in whom hormone therapy has failed is disappointing. Mean survival is approximately one year. Management of the terminal manifestations of the disease require input from palliative care specialists, medical oncologists, radiotherapists and urologists. Depending on the presentation and previous treatment there are a number of possible treatment strategies in patients presenting with a rise in PSA: Patients on LHRH analogues should continue on their therapy and addition of an antiandrogen may induce a temporary response in 10% of patients. Fifteen to 30% of patients on complete androgen blockade will have a fall in their PSA when the anti-androgen is withdrawn. Withdrawal of the androgen should be tried before introducing new treatments. Second-line hormone manoeuvres such as cortisone, adrenal androgen deprivation with ketoconazole may help reduce bone pain. Patients Presenting with Obstructive Symptoms Patients presenting with significant obstructive symptoms or acute urinary retention may be dealt with by transurethral resection of the prostate. Rectal and perineal pain can be controlled by adequate and appropriate analgesia with the direction or advice of palliative care specialists. World guidelines are available. Occasionally radiation to the pelvis may be indicated. Patients Presenting with Bone Pain Bone pain can be very severe. Bone scan is indicated to identify the site of painful metastases. Simple fraction XRT provides pain relief in 80% of patients for about 6 months. Widespread bone pain may require hemi-body radiation on an in-patient basis. Strontium-89 or Rhenium-186 is helpful and is equal to hemi-body radiation in efficacy. Bone marrow depression occurs after Strontium-89 or Rhenium-186 and hemi-body radiation. Evaluation of response in patients with bone involvement alone is difficult. In refractory patients use of PSA has been evaluated and seems a reasonable end-point surrogate of the efficacy of treatment. A sharp fall of 50% is predictive of longer survival of the patient. However, the mean survival in patients with hormone refractory disease is weeks and no single agent or combination of agents has yet been shown to impact on this. HRPC is incurable. Several agents or combinations of agents induce a significant decline in PSA with some objective response in patients, especially those with soft-tissue disease. Pain palliation is often possible in patients unresponsive to narcotics and endocrine therapy. Mitoxantrone, an anthracycline with a relatively broad-spectrum of activity against human tumours, has recently been shown in a randomised trial to relieve bone pain, and to improve the quality of life measurements in patients. Twenty-nine percent of patients treated with a combination of prednisolone and mitoxantrone experienced a valuable degree of pain control compared to 15% receiving prednisolone alone. Toxicity is mild, and while both groups of patients have the same mean survival of one year, activity of mitoxantrone was definable in 84, 85, 86, 87 hormone-relapsed prostate cancer.
31 28 Prostate Cancer Management Clinical Guidelines Metastatic Prostate Cancer Localised bone pain is often severe and can be relieved by simple fraction XRT with pain relief in 80% of patients for about 6-8 months. Level of evidence IB Widespread bone pain can be relieved by Strontium89 or Rhenium-186. Level of evidence IIB Mean survival in patients with hormone-refractory disease averages weeks. Level of evidence III Mitoxantrone submitted to randomised controlled trials relieved bone pain and improved patients quality of life especially when combined with prednisolone. Level of evidence IB Recommendation 28 A multidisciplinary team approach should be made available to patients with advanced hormonerefractory prostatic carcinoma and include palliative care specialists, radiotherapists, medical oncologists and urologists. CRYOTHERAPY (AS MONO THERAPY) A recent report on 66 patients undergoing surgical cryotherapy as monotherapy for localised prostatic carcinoma suggests that cryosurgery does not achieve effective local control of prostatic cancer. In this series most patients died of prostatic cancer and most had local relapse at the time of death. Forty of the 51 patients died of prostatic carcinoma if treated with cryotherapy alone, suggesting that cryotherapy has limited abilities to provide effective local control.88
32 Prostate Cancer Management Clinical Guidelines 29 References 1. The National Cancer Registry Ireland. Cancer in Ireland, Incidence and Mortality Krahn MD, Mahoney JE, Eckman MH, Trachtenberg J, Panker SG, Detsky AS. Screening for prostate cancer: A decision analytic view. J. Amer. Med. Ass, 272 (10): , Smart CR. The results of prostatic carcinoma screening in the U.S.A. as reflected in the surveillance, epidemiology and end results program. Cancer 80: , Brawley OW. Prostate carcinoma incidence and patient mortality: the effects of screening and early detection. Cancer 80: , Krahn MD, Coombs A, Levy IG. Current and projected annual direct costs of screening asymptomatic men for prostatic cancer using prostatic-specific antigen. Can. Med. Assoc J., 160: , Hahn DL, Roberts RG. PSA screening for asymptomatic prostatic cancer: truth in advertising. J. Fam. Pract. 37: 432-6, Chan ECY, Sulmasy DP. What should men know about prostatic-specific antigen screening before giving informed consent. Amer. J. Med. 105: , Von Eschenbach A, Ho R, Murphy GP, Cunningham M, Lins N. American Cancer Society guidelines for the early detection of prostate cancer. Cancer, 80: , Standaert B, Denis L. The European Randomised Study of Screening for Prostate Cancer: an update. Cancer, 80, , Wingo PA, Tong T, Bolden S. Cancer statistics Cancer J. Clin. 45: 8-30, Carter H, Morrell CH, Pearson JD, et al. Estimation of prostatic growth using serial PSA measurements in men with and without prostatic disease. Cancer Research Vol 52: , Carter MB, Pearson JD, Chan DW et al. PSA variability in men without prostatic cancer: Effect of sampling interval on prostatic-specific antigen velocity. Urology, 45: 591, Benson MC, Whang IS, Olsson CA, et al. The use of PSA density to enhance the predictive value of intermediate levels of serum PSA. J. Urol, 147: , Rommel FM, Augusta VE, Presley JA et al. The use of PSA and PSAD in diagnosis of prostate carcinoma in a community based urological practice. J. Urol. 151: , Presti JC Jr, Hovey R, Carroll PR, Shinohara K. Prospective evaluation of prostate specific antigen density in the detection of nonpalpable and stage T1c carcinoma of the prostate. J. Urol., 156: 1685, 1996b. 16. Oesterling JE et al. Serum prostatic specific antigen in a community-based population of healthy men. Establishment of age-specific reference ranges. J. Amer. Med. Ass, 270: 860, Catalona WJ, Partin AW, Slawin KM et al. Use of the percentage of free prostatic specific antigen to enhance differentiation of prostatic carcinoma from benign prostatic disease: A prospective multicentre clinical trial. J. Amer. Med. Ass, 279 (19): , Woodrum DL, Brawer MK, Partin AW et al. Interpretation of free prostatic-specific angigen; clinical research studies for the detection of prostatic carcinoma. J. Urol. 159: 5-12, Hodge KK, Mc Neal JE, Terriss MK, Stamey TA. Random systematic versus ultrasound guided transrectal core biopsies of the prostate. J. Urol. 142: 71-5, Hammerer P, Huland H. Systematic sextant biopsies in 651 patients referred for prostatic evaluation. J. Urol. 151: , Chang JJ, Shinohara K, Hovey RM, Montgomery C, Presti JC Jr. Prospective evaluation of systemic sextant transition zone biopsies in large prostates for cancer detection. Urology, 52: 87-93, Chan TY, Epstein JI. Follow-up of atypical prostate needle biopsies suspicious for cancer. Urology, 53: 351-5, Durkan GC, Greene DR. Elevated serum prostate specific antigen levels in conjunction with an initial prostatic biopsy negative for carcinoma: who should undergo a repeat biopsy? Brit. J. Urol. Int. 83: 34-8, Amin MB, Grignon D, Bostwick D et al. Recommendations for Reporting of Resected Prostate Carcinoma. Association of Directors of Anatomic and Surgical Pathology. Amer. J. Clin. Pathol., 105: , Henson DE, Hutter RV, Farrow GM. Practice protocol for the examination of specimens removed from patients with carcinoma of the prostate gland. A publication of the Cancer Committee College of American Pathologists. Arch. Path. Lab. Med., 118: , Ellis JH, Arbor A, Tempany C, Sarin MS, Gatsonis C, Rifkin MD, McNeil BJ. MR Imaging and sonography of early prostatic cancer: pathologic and imaging features that influence identification and diagnosis. Am. J. Roentgenol. 162: 865-7, Perrapato SD, Carothers GG, Maatman TJ, Soechtig CE. Comparing clinical staging plus transrectal ultrasound with surgical-pathological staging of prostate cancer. Urology, 33: 103-5, 1989.
33 30 Prostate Cancer Management Clinical Guidelines References 28. Presti JC Jr, Hricak H, Narayan P, Shinohara K, White S, Carroll P. Local staging of prostatic carcinoma: comparison of transrectal sonography and endo rectal MR imaging. Am. J. Roentgenol. 166: , Hricak H, White S, Vigernon D, Kurhanewicz J, Kosco A., Levin D, Weiss J, Narayan P, Carroll PR. Carcinoma of the prostate gland: MR imaging with pelvic phased-array coils versus integrated endorectal-pelvic phased-array coils. Radiology, 193: 703-9, Tempany CM, Zhou X, Zerhouni EA, Rifkin MD, Quint LE, Piccoli CW, Ellis JE, McNeil BJ. Staging of prostate cancer: Results of Radiology Diagnostic Oncology Group Project comparison of Three 3 MR imaging techniques. Radiology, 192: 47-54, Schnall M, Imai Y, Tomaszewski J, Pollack HM, Lenkinski RE, Kessel HY. Prostatic cancer: local staging with endorectal surface coil MR imaging. Radiology, 178: , Wolf JS, Cher M, Dall era M, Presti JC Jr., Hricak H, Carroll P. The use and accuracy of cross-sectional imaging and fine needle aspiration cytology for detection of pelvic lymph node metastases before radical prostatectomy. J. Urol, 153: 993-9, Partin AW, Yoo J, Carter HB, Pearson JD, Chan DW, Epstein JI, Walsh PC. The use of prostate specific antigen, clinical stage and Gleason score to predict pathological stage in men with localised prostate cancer. J. Urol, 150: , Oesterling J, Martin SK, Bergstralh EJ, Lowe FC. The use of prostate-specific antigen in staging patients with newly diagnosed prostate cancer. J. Amer. Med. Ass. 269: 57-60, McNeil BJ. Value of bone scanning in neoplastic disease. Semin. Nucl. Med. 14: , Partin AW, Kattan MW, Subong EMP et al. Combination of prostatic specific antigen, clinical stage and Gleason score to predict pathological stage of localised prostate cancer. J. Amer. Med. Ass. 277: , Partin A, and Feneley M. Radical retropubic prostatectomy: limitations in high-risk disease. Proceedings of the American Society of Clinical Oncology. Educational book Albertsen PC, Hanley JA, Gleason DF, Barry MJ. Competing risk analysis of men aged 55 to 74 years at diagnosis managed conservatively for clinically localized prostate cancer. J. Amer. Med. Ass. 280: , Albertsen PC, Fryback DG, Storer BE, Kolon TF, Fine J. Longterm survival among men with conservatively treated localised prostate cancer. J. Amer. Med. Ass. 274: , Eastham JA, Scardino PT, Radical Prostatectomy. Campbell s Urology, Vol 3, p2554, Table th edition Walsh PC, Donker PJ. Impotence following radical prostatectomy: insight into etiology and prevention. J. Urol, 128: 492-7, Steiner MS, Morton RA, Walsh PC. Impact of anatomical radical prostatectomy on urinary incontinence. J. Urol, 145: 512-5, Myers RP, Goellner JR., Cahill DR. Prostate shape, external striated urethral sphincter and radical prostatectomy: the apical dissection. J. Urol; 138: , Mettlin CJ, Murphy GP. Why is prostate cancer death rate declining in the United States? Cancer, 82: , Partin AW, Pound CR, Clements JO, Epstein JI, Walsh PC. Serum PSA after anatomic radical prostatectomy: The Johns Hopkins experience after 10 years. Urol. Clin. Nth Am. 20: 713-5, Partin AW, Pearson JD, Landis PK, Carter HB, Pound CR, Clemens JO, Epstein JI, Walsh PC. Evaluation of serum prostate-specific antigen velocity after radical prostatectomy to distinguish local from distant metastases. Urology, 43: , Trapasso JG, dekernion JB, Smith RB, Dorey F. The incidence and significance of detectable levels of serum prostate specific antigen after radical prostatectomy. J. Urol, 152: , Gerber GS, Thisted RA, Scardino P.et al. Results of radical prostatectomy in men with clinically localised prostatic carcinoma. J. Amer. Med. Ass. 276: 615-9, Pound CR, Partin AW, Eisenberger MA, Chan DW, Pearson JD, Walsh PC Natural history of progression after PSA elevation following radical prostatectomy. J. Amer. Med. Ass. 281: , Connolly JA, Shinohara K, Presti JC Jr, Carroll PR. Local recurrence after radical prostatectomy: characteristics in size, location, and relationship to prostate-specific antigen and surgical margins. Urology, 47: , Anscher MS, Prosnitz LR. Multivariate analysis of factors predicting local relapse after radical prostatectomy - possible indications for post-operative radiotherapy. Int. J. Radiat. Oncol. Biol. Phys. 21: 941-7, Kaplan ID, Bagshaw MA. Serum prostate-specific antigen after post- prostatectomy radiotherapy. Urology, 39: 401-6, Presti JC et al. Effect of adjuvant radiation therapy on urodynamic parameters following radical retropubic prostatectomy. Radiat. Oncol. Invest. 4: 192, Roach M, Pickett B, Phillips, TL. An analysis of the advantages as well as the physical and clinical limitations of 3-dimensional (3-D) based co-planar conformal external beam irradiation in the treatment of localised prostate carcinoma. In: Minet P (editor) 3-Dimensional Treatment Planning. Liege
34 References Prostate Cancer Management Clinical Guidelines Leibel SA, Zelefsky MJ, Kutcher GJ, Burman CM, Kelson S, Fuks Z. 3-dimensional conformal radiation therapy in localised carcinoma of the prostate: Interim report of a phase 1 dose-escalation study. J. Urol, 152: , Sandler HM, Perez-Tamayo C, Ten Haken RK, Lichter AS. Dose escalation for stage C (T3) prostate cancer: minimal rectal toxicity observed using conformal radiotherapy. Radiother-Oncol. 23: 53-4, Hanks GE, Lee WR, Hanlon AL, Hunt M, Kaplan E, Epstein BE, Movsas, Schultheiss TC. Conformal technique dose escalation for prostate cancer: biochemical evidence of improved cancer control with high doses in patients with pretreatment prostate specific antigen >10 or = ng/ml. Int. J. Radiat. Oncol. Biol. Phys. 35: 861-8, Pollack A, Zagars GK. External beam radiotherapy doseresponse of prostate cancer; Int. J. Radiat. Oncol. Bio. Phys. 39: , Zelefsky MJ, Leibel SA, Gaudin PB et al. Dose escalation with 3-dimensional conformal radiation affects the outcome in prostate cancer. Int. J. Radiat. Oncol. Biol. Phys., 41: , Nguyen LN, Pollack A, Zagars GK.; Late effects after radiotherapy for prostate cancer in a randomised dose-response study: results of a self- assessment questionnaire. Urology, 51: 991-7, American Society for Therapeutic Radiology and Oncology Consensus Panel. Consensus : Guideline for PSA following Radiation Therapy in Prostate Cancer. Int. J. Radiat. Oncol. Biol. Phys., 37: , Pisters LL, Von Eschenbach AC, Scott SM et al. The efficacy and complications of salvage cryotherapy of the prostate. J. Urol, 157: 921-5, Rogers E, Ohori M, Kassabian VS, Wheeler TM, Scardino PT. Salvage radical prostatectomy: outcome measured by serum prostatic specific antigen levels. J. Urol. 153: , Bolla M, Gonzalez D, Warde P et al. Improved survival in patients with locally advanced prostate cancer treated with radiotherapy and goserelin. N. Engl. J. Med. 337: , Pilepich MV, Krall JM, Al-Sarraf M et al. Androgen deprivation with radiation therapy compared with radiation therapy alone for localised advanced prostatic carcinoma: a randomised comparative trial of Radiation Therapy Oncology Group. Urology, 45: , Pilepich MV, Caplan R, Byhardt RW et al. Phase III trial of androgen suppression using goserelin in unfavourableprognostic carcinoma of the prostate treated with definitive radiotherapy: report of the Radiation Therapy Oncology Group Protocol J. Clin. Oncol, 15: , Schellhammer PF, El-Mahdi AM, Wright GL Jr., Kolm P, Ragle R. Prostate-specific antigen to determine progression-free survival after radiation therapy for localised carcinoma of the prostate. Urology, 42: 13-20, Ragde H, Blasko JC, Grimm PD et al. Interstitial Iodine-125 radiation without adjuvant therapy in treatment of clinically localised prostatic carcinoma. Cancer, 80: , Brachman DG, Thomas T, Hilbe T, Beyer DC. Failure-free survival following brachytherapy alone or external beam irradiation alone for T1-T2 prostate tumours in 2222 patients: results from a single practice. Int. J. Radiat. Oncol. Biol. Phys., 48: 111-7, Chodak, G.W.: The role of watchful waiting in the management of localized prostate cancer. J. Urol. 152: , Johansson J-E. Expectant management of early stage prostatic cancer: Swedish experience. J. Urol. 152: , George NJR. Natural history of localised prostatic cancer managed by conservative therapy alone. Lancet, i; 494-7, Johansson J-E, Adami H-O, Andersson S-O, Bergstrom R, Holmberg L, Krusemo UB. High 10-year survival rate in patients with early, untreated prostatic cancer. J. Amer. Med. Ass. 267: , Whitmore W.F., Warner JA, Thompson IM: Expectant management of localised prostatic cancer. Cancer; 67: , Adolfsson J, Carstensen J, Lowhagen T. Deferred treatment in localised prostatic cancer. Brit. J. Urol, 69: 183-7, Adolfsson J, Ronstrom L, Lowhagen T, Carstensen J, Hedlund PO. Deferred treatment of clinically localized low grade prostate cancer: the experience from a perspective series at the Karolinska hospital. J. Urol. 152: , Kaisary AV, Tyrrell CJ, Peeling WB, Griffiths K. Comparison of LHRH analogue (zoladex) with orchiectomy in patients with metastatic prostatic carcinoma. Brit. J. Urol, 67: 502-8, Medical Research Council Prostate Cancer Working Party Investigators Group: Immediate versus deferred treatment for advanced prostatic cancer: Initial results of Medical Research Council Trial. Brit. J. Urol, 79: , Goldenberg SL, Bruchovsky N, Gleave ME, Sullivan LD, Akakura K. Intermittent androgen suppression in the treatment of prostate cancer: a preliminary report. Urology, 45: , 1995.
35 32 Prostate Cancer Management Clinical Guidelines References 80. Iversen P, Tyrrell CJ, Kaisary AV et al. Casodex (Bicalutamide) 150 mg monotherapy compared with castration in patients with previously untreated nonmetastatic prostate cancer: results from two multicenter randomised trials at median follow-up of 4 years. Urology, 51: , Tyrrell CJ, Kaisary AV, Iversen P et al. A randomised comparison of Casodex (Bicalutamide) 150 mgs monotherapy versus castration in the treatment of metastatic and locally advanced prostatic cancer. Eur. Urol, 33: , Crawford ED, Eisenberger MA, McLeod DG et al. A controlled trial of leuprolide with and without flutamide in prostatic carcinoma. N. Engl. J. Med. 321: , Smith EM, Hampel N, Ruff RL, Bodner DR, Resnick MI. Spinal cord compression secondary to prostate carcinoma: treatment and prognosis. J. Urol. 149: 330-3, Kelly WK, Scher HI, Mazumdar M, Vlamis V, Schwartz M, Fossa D, Kelly WK. Prostatic specific antigen as a measure of disease outcome in metastatic hormone-refractory prostatic cancer. J. Clin. Oncol, 11: , Small EJ, Carroll PR. Prostate-specific antigen decline after Casodex withdrawal: evidence for anti-androgen withdrawal syndrome. Urology 43: , Tannock IF, Osoba D, Stockler MR et al. Chemotherapy with mitoxantrone plus prednisone or prednisone alone for symptomatic hormone-resistant prostate cancer. A Canadian randomized study with palliative end points. J. Clin. Oncol. 14: , Oh WK, Kantoff P.W. Management of hormone refractory prostate cancer: current standards and future prospective. J. Urol. 160: , Porter MP, Ahaghotu CA, Loening SA, See WA. Disease-free and overall survival after cryosurgical monotherapy for clinical stages B and C carcinoma of the prostate: a 20 year follow-up. J. Urol. 158: , 1997.
36 Royal College of Surgeons in Ireland 123 St. Stephen s Green, Dublin 2, Ireland Tel: Fax: Web:
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Prostate Cancer In-Depth
 Prostate Cancer In-Depth Introduction Prostate cancer is the most common visceral malignancy among American men. In the year 2003, there are expected to be 220,000 new cases and nearly 29,000 deaths in
Prostate Cancer In-Depth Introduction Prostate cancer is the most common visceral malignancy among American men. In the year 2003, there are expected to be 220,000 new cases and nearly 29,000 deaths in
Screening for Prostate Cancer
 Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
For further information on screening and early detection of prostate cancer, see the Section entitled Screening for Prostate Cancer.
 Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
DIAGNOSIS OF PROSTATE CANCER
 DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
PSA Testing 101. Stanley H. Weiss, MD. Professor, UMDNJ-New Jersey Medical School. Director & PI, Essex County Cancer Coalition. weiss@umdnj.
 PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition [email protected] September 23, 2010 Screening: 3 tests for PCa A good screening
PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition [email protected] September 23, 2010 Screening: 3 tests for PCa A good screening
GENERAL CODING. When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis.
 GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
GENERAL CODING When you review old cases that were coded to unknown, make corrections based on guidelines in effect at the time of diagnosis. Exception: You must review and revise EOD coding for prostate
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test
 PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication
PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
Secondary Cancer and Relapse Rates Following Radical Prostatectomy for Prostate-Confined Cancer
 Copyright E 2007 Journal of Insurance Medicine J Insur Med 2007;39:242 250 MORTALITY Secondary Cancer and Relapse Rates Following Radical Prostatectomy for Prostate-Confined Cancer David Wesley, MD; Hugh
Copyright E 2007 Journal of Insurance Medicine J Insur Med 2007;39:242 250 MORTALITY Secondary Cancer and Relapse Rates Following Radical Prostatectomy for Prostate-Confined Cancer David Wesley, MD; Hugh
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
一 本 共 識 依 下 列 參 考 資 料 修 改 版 本 : 1. NCCN Clinical Practice Guidelines in Oncology- Prostate cancer V.2.2014
 一 本 共 識 依 下 列 參 考 資 料 修 改 版 本 : 1. NCCN Clinical Practice in Oncology- Prostate cancer V.2.2014 二 制 訂 人 員 : 泌 尿 外 科 : 鍾 旭 東 醫 師 蔡 宗 佑 醫 師 洪 順 發 醫 師 腫 瘤 內 科 : 蕭 吉 晃 醫 師 放 射 腫 瘤 : 熊 佩 韋 醫 師 解 剖 病 理 : 蔡 建
一 本 共 識 依 下 列 參 考 資 料 修 改 版 本 : 1. NCCN Clinical Practice in Oncology- Prostate cancer V.2.2014 二 制 訂 人 員 : 泌 尿 外 科 : 鍾 旭 東 醫 師 蔡 宗 佑 醫 師 洪 順 發 醫 師 腫 瘤 內 科 : 蕭 吉 晃 醫 師 放 射 腫 瘤 : 熊 佩 韋 醫 師 解 剖 病 理 : 蔡 建
Prostate Cancer & Its Treatment
 Your Health Matters Prostate Cancer & Its Treatment By the UCSF Medical Center Prostate Cancer Advocates Greetings! From our personal experience in dealing with our own prostate cancers, we UCSF Patient
Your Health Matters Prostate Cancer & Its Treatment By the UCSF Medical Center Prostate Cancer Advocates Greetings! From our personal experience in dealing with our own prostate cancers, we UCSF Patient
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Role of MRI in the Diagnosis of Prostate Cancer, A Proposal
 Clinical and Experimental Medical Sciences, Vol. 1, 2013, no. 3, 111 116 HIKARI Ltd, www.m-hikari.com Role of MRI in the Diagnosis of Prostate Cancer, A Proposal W. Akhter Research Fellow Urology, Bartshealth
Clinical and Experimental Medical Sciences, Vol. 1, 2013, no. 3, 111 116 HIKARI Ltd, www.m-hikari.com Role of MRI in the Diagnosis of Prostate Cancer, A Proposal W. Akhter Research Fellow Urology, Bartshealth
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
The PSA Controversy: Defining It, Discussing It, and Coping With It
 The PSA Controversy: Defining It, Discussing It, and Coping With It 11 TH ANNUAL SYMPOSIUM ON MEN S HEALTH June 12, 2013 The PSA Controversy Defining It, Discussing It and Coping With It As of May 2012,
The PSA Controversy: Defining It, Discussing It, and Coping With It 11 TH ANNUAL SYMPOSIUM ON MEN S HEALTH June 12, 2013 The PSA Controversy Defining It, Discussing It and Coping With It As of May 2012,
Beyond the PSA: Genomic Testing in Localized Prostate Cancer
 Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Thomas A. Kollmorgen, M.D. Oregon Urology Institute
 Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Localised prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
PROSTATE CANCER. Diagnosis and Treatment
 Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Clinical Practice Guidelines
 Clinical Practice Guidelines Prostate Cancer Screening CareMore Quality Management CareMore Health System adopts Clinical Practice Guidelines for the purpose of improving health care and reducing unnecessary
Clinical Practice Guidelines Prostate Cancer Screening CareMore Quality Management CareMore Health System adopts Clinical Practice Guidelines for the purpose of improving health care and reducing unnecessary
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Locally advanced prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
Understanding Prostate Cancer. The Urology Group Guide for Newly Diagnosed Patients. Advanced Care. Improving Lives.
 Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Prostate cancer A guide for newly diagnosed men
 Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Prostatectomy, pelvic lymphadenect. Med age 63 years Mean followup 53 months No other cancer related therapy before recurrence. Negative.
 Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Screening for Prostate Cancer
 Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Screening. Dr. J. McCracken, Urologist
 Prostate Cancer Screening Dr. J. McCracken, Urologist USPSTF Lifetime risk for diagnosis currently estimated at 15.9% Llifetime risk of dying of prostate cancer is 2.8% Seventy percent of deaths due to
Prostate Cancer Screening Dr. J. McCracken, Urologist USPSTF Lifetime risk for diagnosis currently estimated at 15.9% Llifetime risk of dying of prostate cancer is 2.8% Seventy percent of deaths due to
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER. Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American
 PROSTATE CANCER 1. Guidelines for Screening Risk Factors Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American High-risk men: Family history of prostate
PROSTATE CANCER 1. Guidelines for Screening Risk Factors Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American High-risk men: Family history of prostate
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa
 PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa Key messages: PSA is present in the benign and malignant prostate There is currently no national screening programme
PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa Key messages: PSA is present in the benign and malignant prostate There is currently no national screening programme
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH
 9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
9. Discuss guidelines for follow-up post-thyroidectomy for cancer (labs/tests) HH Differentiated thyroid cancer expresses the TSH receptor on the cell membrane and responds to TSH stimulation by increasing
Saturation Biopsy for Diagnosis and Staging of Prostate Cancer. Original Policy Date
 MP 7.01.101 Saturation Biopsy for Diagnosis and Staging of Prostate Cancer Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date /12/2013 Return to Medical Policy
MP 7.01.101 Saturation Biopsy for Diagnosis and Staging of Prostate Cancer Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date /12/2013 Return to Medical Policy
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); [email protected] Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
Prostate Cancer Screening in Taiwan: a must
 Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER
 2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
Guidelines for Management of Renal Cancer
 Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Guidelines for Management of Renal Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Section 5 updated bullets 5.3 and 5.4 Section 6 updated
Prostate cancer screening. It s YOUR decision!
 Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
Prostate Cancer. What is cancer?
 What is cancer? Prostate Cancer The body is made up of trillions of living cells. Normal body cells grow, divide into new cells, and die in an orderly way. During the early years of a person s life, normal
What is cancer? Prostate Cancer The body is made up of trillions of living cells. Normal body cells grow, divide into new cells, and die in an orderly way. During the early years of a person s life, normal
Robert Bristow MD PhD FRCPC
 Robert Bristow MD PhD FRCPC Clinician-Scientist and Professor, Radiation Oncology and Medical Biophysics, University of Toronto and Ontario Cancer Institute/ (UHN) Head, PMH-CFCRI Prostate Cancer Research
Robert Bristow MD PhD FRCPC Clinician-Scientist and Professor, Radiation Oncology and Medical Biophysics, University of Toronto and Ontario Cancer Institute/ (UHN) Head, PMH-CFCRI Prostate Cancer Research
PSA screening: Controversies and Guidelines
 PSA screening: Controversies and Guidelines John Phillips, MD, FACS Department of Urology Urology Center of Westchester New York Medical College Historical PerspecGve Cancer of the prostate, although rare,
PSA screening: Controversies and Guidelines John Phillips, MD, FACS Department of Urology Urology Center of Westchester New York Medical College Historical PerspecGve Cancer of the prostate, although rare,
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Science Highlights. To PSA or not to PSA: That is the Question.
 Science Highlights June 2012 by Ann A. Kiessling, PhD at the To PSA or not to PSA: That is the Question. The current raucous debate over the commonly used PSA blood test to screen for prostate cancer,
Science Highlights June 2012 by Ann A. Kiessling, PhD at the To PSA or not to PSA: That is the Question. The current raucous debate over the commonly used PSA blood test to screen for prostate cancer,
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD
 SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
SUNY DOWNSTATE MEDICAL CENTER SURGERY GRAND ROUNDS February 28, 2013 VERENA LIU, MD ROSEANNA LEE, MD Case Presentation 35 year old male referred from PMD with an asymptomatic palpable right neck mass PMH/PSH:
The PSA Test for Prostate Cancer Screening:
 For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
Surgical guidelines for the management of breast cancer
 Available online at www.sciencedirect.com EJSO xx (2009) S1eS22 www.ejso.com Guidelines Surgical guidelines for the management of breast cancer Contents Association of Breast Surgery at BASO 2009 Introduction...
Available online at www.sciencedirect.com EJSO xx (2009) S1eS22 www.ejso.com Guidelines Surgical guidelines for the management of breast cancer Contents Association of Breast Surgery at BASO 2009 Introduction...
Advanced Prostate Cancer Treatments
 Advanced Prostate Cancer Treatments Guest Expert: Kevin, DO Associate Professor of Medical Oncology, Yale Cancer Center www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with
Advanced Prostate Cancer Treatments Guest Expert: Kevin, DO Associate Professor of Medical Oncology, Yale Cancer Center www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
LIvING WITH Prostate Cancer
 Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Guidelines for Cancer Prevention, Early detection & Screening. Prostate Cancer
 Guidelines for Cancer Prevention, Early detection & Screening Prostate Cancer Intervention Comments & Recommendations For primary prevention, it has been suggested that diets low in meat & other fatty
Guidelines for Cancer Prevention, Early detection & Screening Prostate Cancer Intervention Comments & Recommendations For primary prevention, it has been suggested that diets low in meat & other fatty
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer. What is prostate cancer?
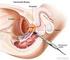 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER
 TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER DILEMMA Thomas J Stormont MD January 2012 http://www.youtube.com/watch?v=8jd 7bAHVp0A&feature=related related INTRODUCTION A government health panel (the
TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER DILEMMA Thomas J Stormont MD January 2012 http://www.youtube.com/watch?v=8jd 7bAHVp0A&feature=related related INTRODUCTION A government health panel (the
