Clinical Rotation 3: PHYS 705 Fall 2015 (Aug. 25, 2015 to Feb. 25, 2016) COURSE INFORMATION
|
|
|
- Rudolf Hines
- 9 years ago
- Views:
Transcription
1 Clinical Rotation 3: PHYS 705 Fall 2015 (Aug. 25, 2015 to Feb. 25, 2016) COURSE INFORMATION Days: Monday-Friday Times: Full Time Location: One of the participating cancer clinics Program Director: George Mardirossian, Ph.D., DABR (T) Contact Information: Office Hours Days: Friday Genesis Healthcare Partners 3366 First Ave San Diego, CA Office: Fax: Associate Program Directors at Participating Sites: San Diego State University M. Tambasco, Ph.D., MCCPM 5500 Campanile Drive San Diego, CA Office: Fax: Naval Medical Center Richard LaFontaine, Ph.D., DABR (T) Bob Wilson Drive, STE 14 San Diego, CA Office: Cell: Sharp Grossmont Hospital Patrick Guo, Ph.D., DABR(T) Lead Medical Physicist Radiaton Therapy/Cancer Center 5555 Grosssmont Center Dr. La Mesa, CA Tel: Course Overview Description from the Official Course Catalog: On-site, full-day clinical training in the principles of computed tomography (CT) simulator, associated radiation protection/design considerations, CT protocols. Understand the physics of imaging modalities, image guided radiotherapy, image archiving and communication systems, and perform quality assurance on CT, MRI, ultrasound and PET as related to radiation therapy. On board imaging procedures are also covered. Description of the Purpose and Course Content: This course is a clinical rotation that comprises an integral part of the residency training for radiation oncology physics. It is designed to be in accordance with American Association of Physicists in Medicine (AAPM) Task Group 249, 'Essential and Guidelines for Hospital based Medical Physics Residency Training Programs', and the Commission on Accreditation of Medical
2 Physics Educational Programs (CAMPEP). The course will also include didactic coverage of the topics during biweekly resident sessions at SDSU. This clinical rotation course extends over the third six-months of the certificate program and consists of rotations through areas of computed tomography (CT) simulation, associated radiation protection/design considerations, CT protocols, image guided radiotherapy, image archiving and communication systems, some treatment planning, and quality assurance on CT, MRI, ultrasound, PET as related to radiation therapy. Objectives are established at the commencement of the course. The student s performance is evaluated by direct observation, a project/progress report, and bimonthly oral examinations administered by the supervising Medical Physicist including a final oral examination by the Advisory Committee. The work at the clinic, including self-study of reading material and contact hours of the Resident with the clinic team (i.e., Medical Physicists, Dosimetrists, Radiation Oncologists, Radiation Therapists) and chart rounds/tumor board meetings will be full time. Note: The proposed course requires access to external beam radiotherapy equipment, simulation equipment, imaging equipment, treatment planning equipment, and quality assurance equipment that are only available at community/academic cancer centers. Arrangements will be made to have board certified Clinical Medical Physicists at the hospitals train the residence in all aspects of the physics of external beam radiation therapy including equipment usage and quality assurance. Once trained, the Resident will be expected to perform routine quality control of the equipment available at the assigned cancer center under the supervision of a qualified Medical Physicist. In addition to the clinical activities below, the resident is expected to attend one medical physics conference per year and the following activities at SDSU: Biweekly didactic resident sessions covering the clinical topics below and resident progress/concerns (~2 hours/session) Medical physics seminars (~ 4 per rotation). I. CT Simulator-Total 8 weeks A. Selection (1 week) 1. Performance specification 2. Feature comparison 3. Mechanical/architectural considerations 4. Performance test design B. Protection/design/architectural (2 weeks) 1. Walls/ceiling/floor 2. Control area 3. Darkroom 4. Room survey 5. Regulations: federal, state, local C. Acceptance testing (2 weeks) 1. Diagnostic image quality tests 2. Dose calculations 3. Geometry tests (digitally reconstructed radiographs [DRRs], etc.) 4. Networking tests D. Quality assurance (2 weeks) 1. Geometric accuracy 2. Imaging 3. Networking E. CT protocols (1 week) II. Imaging-Total 9 weeks A. CT (2 weeks) 1. Scanning systems and techniques 2. Geometric accuracy 3. Density tables 4. 4-D CT (four-dimensional CT) B. MRI (2 weeks)
3 1. Scanning systems and techniques 2. Geometric accuracy 3. MRI-CT image registration C. Ultrasound (1 week) 1. Scanning systems and techniques 2. Tumor positioning D. PET (2 weeks) 1. Scanning systems and techniques 2. Tumor localization 3. Image registration E. Picture archiving and communication system (PACS)/Informatics (2 weeks) 1. Digital Imaging and Communications in Medicine (DICOM) 2. DICOM RT (DICOM in Radiation Therapy) 3. PACS systems and their integration 4. DICOM standards 5. Information acquisition from PACS/images 6. Quality/maintenance of imaging workstations 7. Evaluation of viewing conditions 8. Quantitative analysis 9. Network integration/management, and roles of physics and information technology staff III. On Board MV & kv Imaging & Associated QA (1.5 weeks) 1. General 2. 2D Imaging techniques and 3D (e.g., CBCT) IV. Proton Therapy (1.5 weeks) 2. Student Learning Outcomes & Competency Evaluation Metrics All of the outcomes listed in Appendix 1 of Clinical Rotation 3 below will be assessed by measurable competencies in clinical measurements and practice, oral evaluations, written reports and a final oral exam. Many of the objectives, learning outcomes, and competency evaluation metrics given in Appendix 1 of this syllabus have been adapted from AAPM Report Task Group 249. Real Life Relevance: This clinical rotation course provides practical hands on clinical training in radiation oncology physics. Relation to Other Courses: This is the third clinical rotation course in the Advanced Certificate of Medical Physics Residency Program. The topics covered in this and the other clinical rotations are core requirements for the Commission on Accreditation of Medical Physics Education Programs (CAMPEP). 3. Enrollment Information Prerequisites: Clinical Rotation 2 (PHYS- 703) Adding/Dropping Procedures: The course must be added before the end of the second week of the semester. Dropping procedures will follow the Physics Department guidelines. Note: Dropping a clinical rotation course is effectively equivalent to withdrawing from the residency program. 4. Course Materials
4 Required & Recommended Materials: The following task group publications available at from the American Association of Physicists in Medicine (AAPM) and books and will be the references for the course: 1. Radiation Oncology Physics: A Handbook for Teachers and Students, by E. B. Podgorsak. Radiation Oncology Physics: A Handbook for Teachers and Students, by E. B. Podgorsak. International Atomic Energy Agency, Vienna, Austria. Date Published: PDF available for free download at: 2. The Modern Technology of Radiation Oncology: A Compendium for Medical Physicists and Radiation Oncologists, Volume 1, Editor: Jacob Van Dyk, Medical Physics Publishing Corporation, The Modern Technology of Radiation Oncology: A Compendium for Medical Physicists and Radiation Oncologists, Volume 2, Editor: Jacob Van Dyk, Medical Physics Publishing Corporation, AAPM REPORT NO. 74 Quality Control in Diagnostic Radiology, Report of Task Group #12, Diagnostic X-ray Imaging Committee, Medical Physics Publishing, Quality assurance for computed-tomography simulators and the computed tomography- simulation process: Report of the AAPM Radiation Therapy Committee Task Group No. 66. Medical Physics, Vol. 30, Issue 10, The Measurement, Reporting, and Management of Radiation Dose in CT: Report of the AAPM Task Group 23, American Association of Physicists in Medicine, The management of imaging dose during image-guided radiotherapy: Report of the AAPM Task Group 75, Medical Physics, Vol 34, Issue 10, Quality assurance for image-guided radiation therapy utilizing CT-based technologies: A report of the AAPM TG-179 Medical Physics, Vol 39, Issue 4, AAPM TG-53. Quality Assurance for Clinical Radiotherapy Treatment Planning, Medical Physics 25(10): , IAEA TRS 430. Commissioning and Quality Assurance of Computerized Planning Systems for Radiation Treatment of Cancer. Technical Reports Series (TRS) No Vienna, Austria: International Atomic Energy Agency, Bushberg et al., The Essential Physics of Medical Imaging, 3 rd Ed Huda, Review of Radiologic Physics, 3 rd Ed NCCN guidelines for treatment of cancer by site: 5. Course Structure and Conduct Style of the Clinical Rotation: Residents will be trained by the Certified Clinical Medical Physicist to perform hands on clinical duties in the cancer center. Once trained the residents will gain practice by preforming routine clinical duties. Residents will be responsible for learning the recommended reference materials on their own. 6. Course Assessment and Grading
5 Grading Scale: The Resident s performance will be evaluated by direct observation, project/progress reports, and three oral evaluations (approximately bimonthly) administered by the supervising Medical Physicist. Note: The final oral examination is cumulative and will be administered by the Advisory Committee. One of the writing components of this course will include a report by the resident that describes all of the clinical activities/projects in which they participated. The report will include the objectives and relevance, description, methods, and discussion/conclusions of each major clinical activity/project. Special assigned clinical project reports may also be included. The final assessment breaks down as follows: 1. Observation of clinical measurements and practice by supervising Medical Physicist: 10% 2. Bimonthly oral evaluations based on the clinical rotation topics (Approximately ranging from 20 minutes to 1 hour long): 40% 3. Project/progress and reports: 20% 4. Final presentation and oral exam (1 hour): 30% The following evaluation scheme from 1 to 5 will be used: 1. Unsatisfactory Performance and/or consistency is below standard in most/all areas covered by evaluation Immediate and consistent improvement to Meets Expectations rating is required in next evaluation and final oral exam 2. Needs Improvement Performance and/or consistency is below standards in certain areas and improvement is needed 3. Meets Expectations Competent level of performance that consistently meets high standards 4. Above Expectations Examination results exceed expectations Performance is consistently high quality 5. Outstanding Knowledge of evaluation material is exceptional and consistently superior The resident will be assigned a pass/fail for the course. An overall score of 3 or greater constitutes a pass. If the resident fails one section of the rotation, they will be given one chance to prepare and re-take the oral exam for that section two weeks later. A copy of all evaluations will be sent to the Program Director. Excused Absence Make-up Policies: Students should have an extraordinary reason (e.g., illness, death in the family, etc.), with proof, to miss the oral examination or final oral examination. A make-up for such a case will be arranged with the Advisory Committee 7. Other Course Policies The residents are expected to: Engage with supervising Medical Physicist for training. Record daily activities and time spent in the clinic. This will be reviewed by regularly the supervising Medical Physicist and quarterly by the Advisory Committee. Report for duties at the clinic and meetings on time. Perform assigned readings, presentations, lectures, and clinical duties in a timely manner. Attend medical physics seminars (approximately 4 per semester) at SDSU. Attend all of the biweekly resident sessions at SDSU. Attend one Medical Physics Conference each year (e.g., the AAPM, ASTRO, or COMP Annual Meeting). Report any QC results that are out of tolerance to the supervising or other qualified Medical Physicist at the clinic as soon as possible. Hand in project and progress reports by assigned deadline. Dress appropriately in the clinic (e.g., dress shirt and dress pants). Interact respectfully with all staff members and patients in the clinic.
6 Advise the supervising Medical Physicist and Program Director of planned absences (e.g., vacation time or sick leave). A record of vacation days absent shall be kept by the Associate/Program Director and should not exceed the allotted two weeks per six-month semester. In addition, the holidays allotted to Medical Physicists at the center are applicable to the resident. The resident may also take up to 1.5 days of personal leave per six-month rotation. Note: A senior resident will be chosen to be part of the Advisory Committee to provide input on resident issues and concerns. If you are a student with a disability and believe you will need accommodations for this class, it is your responsibility to contact Student Disability Services at (619) To avoid any delay in the receipt of your accommodations, you should contact Student Disability Services as soon as possible. Please note that accommodations are not retroactive, and that I cannot provide accommodations based upon disability until I have received an accommodation letter from Student Disability Services. Your cooperation is appreciated.
7 Appendix 1 of Clinical Rotation 3 Resident s Name: RADIATION ONCOLOGY RESIDENCY PROGRAM Competency Evaluation of Resident Rotation: PHYS 705: Clinical Rotation 3 Inclusive dates of rotation: Director or Associate Director: Competency Assessment Scheme: 1. Unsatisfactory Performance/Knowledge is below standard 2. Needs Improvement Performance/Knowledge is below standards in certain areas and improvement is needed 3. Meets Expectations Performance/knowledge that consistently meets high standards of competency 4. Above Expectations Performance/Knowledge exceeds expectations Performance/Knowledge is consistently high quality 5. Outstanding Performance/Knowledge is exceptional and consistently superior Evaluation criteria Computed Tomography (CT) Simulators - General a. Demonstrates understanding of the nuances of CT simulators with those of diagnostic CT scanners (e.g., in terms of lasers, table top indexing, localization software, bore size) b. Demonstrates an understanding of the theory of CT imaging reconstruction and of the operation of a CT simulator c. Demonstrates an understanding of the major subsystems and components of a CT simulator d. Demonstrates an understanding of the room shielding and other radiation protection requirements of a CT simulator Computed Tomography (CT) Simulators - Selection a. Reviews the steps required to select a new CT simulator, including performance Competency (from 1 5) Explanatory Notes & Mentor Signature
8 specification and feature comparison b. Reviews and understands the mechanical/architectural considerations relevant to installing a new CT simulator in both new and existing rooms Computed Tomography (CT) Simulators Acceptance Testing & Quality Control a. Demonstrates an understanding of the mechanical tests performed during a CT simulator acceptance procedure b. Demonstrates an understanding of the tests of image quality and characteristics for a CT image and DRR for a CT simulator c. Demonstrates an understanding of the measurement of dose and the computed tomography dose index (CTDI) from a CT simulator for different body sites d. Demonstrates an understanding of the measurement of CT number as opposed to density calibration with kvp and CT number used in treatment planning systems e. Demonstrates an understanding of the alignment of internal and external laser systems in a CT simulator f. Demonstrates an understanding of network connectivity tests between other systems used in the radiation oncology process (e.g., treatment planning systems, treatment verification systems, PAC system) g. Demonstrates an understanding of the validation tests related to the transfer of CTimaged objects to treatment planning systems Computed Tomography (CT) Simulators Radiation Safety a. Demonstrates an understanding of state/provincial licensing of x-ray producing devices b. Explains the principles behind a radiation protection program, including the rationale for the dose limits for radiation workers and members of the public c. Describes the key parameters necessary to perform a shielding calculation d. Describes the significance of an isodose distribution plot for a CT simulator e. Demonstrates an understanding of structural shielding designs for a CT simulator and performs a shielding calculation (walls, ceilings, floor, and control area)
9 f. Demonstrates an understanding of film processing and darkroom design Computed Tomography (CT) Simulators Dose Calculations a. Understands the physical basis for the use of CT-simulator images in treatment planning as the current standard for dose calculations b. Understands the calibration of these CTsimulator images for computing radiation dose deposition in different tissues Computed Tomography (CT) Simulators Quality Assurance a. Competently performs routine QA test processes for CT simulators and understands the QA test processes relationship to acceptance testing and commissioning measurements b. Understands the bases of recommended measurements for CT-simulators and the measurements tolerances specified by the AAPM, ACR, and other professional bodies c. Understands and competently determines the geometric accuracy of laser alignment, couch motion, gantry motion, and CT-simulator images for both static and moving objects d. Understands and competently assesses the quality of images produced by CT-simulators in any mode of operation and image reconstruction, and is able to discuss the impact of image artifacts and distortion on treatment planning e. Understands the connectivity requirements of a CT simulator to other computer systems that form part of a modern radiation therapy treatment process, including being familiar with Internet and DICOM-RT image data transfer protocols Computed Tomography (CT) Simulators CT Protocols a. Demonstrates an understanding of the following parameters, their typical values, and how they are combined in CT protocols: slice thickness, pitch, kv, mas, FOV, and scan length b. Demonstrates an understanding of how CT protocols consider multi-slice capabilities, tube heating, and maximum scan time c. Demonstrates an understanding of the relationship between image quality and patient dose from examination
10 d. Demonstrates an understanding of the need to define dose-optimized imaging protocols for various body parts and sizes of patient e. Demonstrates an understanding of image artifacts that may arise in CT images, while being able to identify their causes and assess or mitigate their impact on radiation treatment planning f. Understands the different imaging protocols used in tumor motion management (e.g., voluntary breath hold, active breathing control, shallow breathing by compression, free breathing helical CT, 4D-CT) g. Understands the different CT image acquisition modes available with a modern CT simulator (e.g., prospective, retrospective, cine, helical, 4D, and image sorting based on breathing phase and breathing amplitude) Magnetic Resonance Imaging (MRI) - General a. Demonstrates an understanding of the basic imaging principles behind MRI b. Compares the treatment planning-related advantages and limitations of MRI with those of CT c. Demonstrates an understanding of the role of MRI for radiation therapy applications, providing examples Magnetic Resonance Imaging (MRI) - QA a. Demonstrates an understanding of the quality assurance processes and frequencies of checks for MR simulators (e.g., image quality, image integrity, safety and mechanical checks, network connectivity) Ultrasound (US) - General a. Demonstrates an understanding of the basic imaging principles behind US imaging b. Demonstrates an understanding of the role of US in external beam and brachytherapy treatments using trans-rectal as opposed to trans-abdominal probes, providing examples Ultrasound (US) - QA a. Describes methods for QA of US imaging probes prior to clinical uses in procedures such
11 as prostate implants and prostate external beam therapy Positron Emission Tomography (PET) - General b. Demonstrates an understanding of the basic imaging principles behind PET c. Compares the advantages and limitations of PET with those of CT for treatment planning d. Demonstrates an understanding of the role of PET for radiation therapy applications, providing examples Positron Emission Tomography (PET) - QA a. Demonstrates an understanding of the quality assurance processes and frequencies of checks for PET-CT simulators (e.g., image quality, image integrity, safety and mechanical checks, network connectivity) SPECT - General a. Demonstrates an understanding of the basic imaging principles behind SPECT b. Describes the comparative advantages and limitations for treatment planning of SPECT and CT c. Demonstrates an understanding of the role of SPECT for external beam and radiopharmaceutical therapy applications, providing examples Informatics a. Uses information technology to retrieve and store patient demographic, examination, and image information b. Understands how image processing is used to create radiographic images for display presentation and depict 3D structures in CT and MR c. Uses information technology to investigate clinical, technical, and regulatory questions d. Uses and understands common information systems used in radiation oncology (e.g., record and verify, electronic medical records, image handling) e. Demonstrates an understanding of the various methods of data transfer, storage, and security, including:
12 i. PACS ii. DICOM iii. DICOM in radiation therapy (DICOM-RT) iv. Health Level 7 (HL7) v. Integrating the Healthcare Enterprise (IHE) vi. IHE Radiation Oncology (IHE-RO) f. Understands the roles of physics and information technology staff, including their work in network integration and maintenance Image Registration/Fusion a. Describes the rationale behind and the advantages/challenges of image registration and image fusion b. Defines the image features on which registration can be based (e.g., landmarks, segments, intensities) c. Defines the different forms of registration (e.g., rigid, affine, deformable) and Describes their advantages and limitations d. Defines similarity metrics used to assess quality of registration (e.g., squared intensity differences, cross-correlation, mutual information) e. Describes how to commission imaging modalities such as MRI, PET-CT, and diagnostic CT for the purpose of image registration to a radiation oncology planning CT f. Describes issues associated with the transfer of images (e.g., connectivity, image dataset integrity) g. Describes issues associated with patient positioning (e.g., bore size, couch top, lasers, compatibility of immobilization devices, differences in patient position/ organ filling, motion) h. Describes issues associated with the choice of image acquisition technique (e.g., length of scan, slice thickness, FOV, kv, mas) Imaging Tests a. Describes the tests that would be performed to ensure that the imported image data are
13 correct b. Demonstrates that images can be imported from CT, MR, and PET or PET/CT scanners c. Demonstrates that the above imaging sets can be accurately fused with the primary treatment planning image set d. Describes the different image fusion algorithms available on a treatment-planning system (e.g., CT-CT, CT-MR, CT-PET) On-Board MV and kv Imaging - General a. Describes the different detector technologies that have been used for on-board MV and kv imaging b. Describes the imaging dose associated with on-board MV and kv imaging technologies c. Understands and performs the different measures of radiographic image quality as part of the routine duties On-Board MV and kv Imaging - QA a. Understands the QA processes and frequencies of checks for on-board MV and kv imaging, including cone-beam CT (e.g., image quality, image integrity, safety and mechanical checks, network connectivity, imaging dose, and localization software, isocenter calibration) b. Performs the above QA checks as part of the routine duties Proton Therapy - Basics a. Demonstrates an understanding of the theory of operation of proton accelerators currently used in radiation oncology treatment (e.g., synchrotrons and cyclotrons) and their limitations b. Demonstrates an understanding of proton percent depth dose in tissue and other media and proton ranges for different energies, e.g., stopping and scattering power and range c. Demonstrates an understanding of potential dose deposition uncertainties in proton therapy Proton Therapy Radiobiology
14 a. Demonstrates an understanding of the impact of the proton beam quality (e.g., linear energy transfer [LET]) on the relative biological effectiveness (RBE)
1. Provide clinical training in radiation oncology physics within a structured clinical environment.
 Medical Physics Residency Program Overview Our Physics Residency Training is a 2 year program typically beginning July 1 each year. The first year resident will work closely with medical physicists responsible
Medical Physics Residency Program Overview Our Physics Residency Training is a 2 year program typically beginning July 1 each year. The first year resident will work closely with medical physicists responsible
MEDICAL DOSIMETRY. COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: therapy.
 Graduate Catalog 2012-2013 Medical Dosimetry / 339 MEDICAL DOSIMETRY COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: Collins, Kevin Scott, Associate Professor, Ph.D., Jensen, Steve, Emeritus Professor,
Graduate Catalog 2012-2013 Medical Dosimetry / 339 MEDICAL DOSIMETRY COLLEGE OF APPLIED SCIENCES AND ARTS Graduate Faculty: Collins, Kevin Scott, Associate Professor, Ph.D., Jensen, Steve, Emeritus Professor,
Accreditation Is Coming
 Accreditation Is Coming Accreditation Is Coming Accreditation Is Coming Yes, It Is! Currently, Accreditation is Voluntary However, Some of the Accrediting Organizations Are Lobbying the Congress to Adopt
Accreditation Is Coming Accreditation Is Coming Accreditation Is Coming Yes, It Is! Currently, Accreditation is Voluntary However, Some of the Accrediting Organizations Are Lobbying the Congress to Adopt
IGRT. IGRT can increase the accuracy by locating the target volume before and during the treatment.
 DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
DERYA ÇÖNE RADIOTHERAPY THERAPIST ACIBADEM KOZYATAGI HOSPITAL RADIATION ONCOLOGY DEPARTMENT IGRT IGRT (image-guided radiation therapy) is a technique that reduces geometric uncertainties by considering
RADIATION THERAPY FACULTY TOBJECTIVES. Post-Baccalaureate Certificate. Marissa Johnson, M.S.R.S., R.T. (T)
 R A D I A T I O N T H E R A P Y c l i n i c a l n u t r i t i o n e m e r g e n c y m e d i c i n e e d u c a t i o n h e a l t h c a r e s c i e n c e s p h y s i c a l t h e r a p y p h y s i c i a n
R A D I A T I O N T H E R A P Y c l i n i c a l n u t r i t i o n e m e r g e n c y m e d i c i n e e d u c a t i o n h e a l t h c a r e s c i e n c e s p h y s i c a l t h e r a p y p h y s i c i a n
IBA Proton Therapy. Biomed days 2015. Vincent Bossier. System Architect [email protected]. Protect, Enhance and Save Lives
 Vincent Bossier System Architect [email protected] IBA Proton Therapy Biomed days 2015 Protect, Enhance and Save Lives 1 Agenda AN INTRODUCTION TO IBA WHY PROTON THERAPY CLINICAL WORKFLOW TREATMENT
Vincent Bossier System Architect [email protected] IBA Proton Therapy Biomed days 2015 Protect, Enhance and Save Lives 1 Agenda AN INTRODUCTION TO IBA WHY PROTON THERAPY CLINICAL WORKFLOW TREATMENT
First Three Years After Project Proton Therapy Facility:
 39. Project Related Utilization and Financial Information. Proton Therapy Facility: Unit of Service Delivery Projected Utilization FY2017 FY2018 FY2019 Estimated Patients 448 670 808 Average Revenue Per
39. Project Related Utilization and Financial Information. Proton Therapy Facility: Unit of Service Delivery Projected Utilization FY2017 FY2018 FY2019 Estimated Patients 448 670 808 Average Revenue Per
RADIATION THERAPY guide. Guiding you through your treatment
 RADIATION THERAPY guide Guiding you through your treatment 2013_RADIATION_GUIDE_6PG.indd 1 Before Treatment Consultation with the Radiation Oncologist During your first visit with the radiation oncologist,
RADIATION THERAPY guide Guiding you through your treatment 2013_RADIATION_GUIDE_6PG.indd 1 Before Treatment Consultation with the Radiation Oncologist During your first visit with the radiation oncologist,
Key words: treatment planning, quality assurance, 3D treatment planning
 American Association of Physicists in Medicine Radiation Therapy Committee Task Group 53: Quality assurance for clinical radiotherapy treatment planning Benedick Fraass a) University of Michigan Medical
American Association of Physicists in Medicine Radiation Therapy Committee Task Group 53: Quality assurance for clinical radiotherapy treatment planning Benedick Fraass a) University of Michigan Medical
Quality Assurance of Radiotherapy Equipment
 Clinical Implementation of Technology & Quality Assurance in Radiation Oncology For the course: Survey of Clinical Radiation Oncology 1 Quality Assurance of Radiotherapy Equipment Outline: A. Criteria
Clinical Implementation of Technology & Quality Assurance in Radiation Oncology For the course: Survey of Clinical Radiation Oncology 1 Quality Assurance of Radiotherapy Equipment Outline: A. Criteria
C A M P E P. Standards for Accreditation of Graduate Educational Programs in Medical Physics
 Standards for Accreditation of Graduate Educational Programs in Medical Physics Preamble Revised July 2015 Medical Physics is a branch of physics that applies the concepts and principles of physics to
Standards for Accreditation of Graduate Educational Programs in Medical Physics Preamble Revised July 2015 Medical Physics is a branch of physics that applies the concepts and principles of physics to
Proton Therapy. What is proton therapy and how is it used?
 Scan for mobile link. Proton Therapy Proton therapy delivers radiation to tumor tissue in a much more confined way than conventional photon therapy thus allowing the radiation oncologist to use a greater
Scan for mobile link. Proton Therapy Proton therapy delivers radiation to tumor tissue in a much more confined way than conventional photon therapy thus allowing the radiation oncologist to use a greater
Prepublication Requirements
 Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Issued Prepublication Requirements The Joint Commission has approved the following revisions for prepublication. While revised requirements are published in the semiannual updates to the print manuals
Department of Radiation Oncology
 Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Department of Radiation Oncology Welcome to Radiation Oncology at Emory Clinic Every member of Emory Clinic Department of Radiation Oncology strives to provide the highest quality of care for you as our
Albany Medical Center Chief Medical Physicist Radiation Oncology Imaging and Related Services
 Albany Medical Center Chief Medical Physicist Radiation Oncology Imaging and Related Services POSITION SUMMARY: The Medical Physicist is responsible for assuring the high quality radiation therapy through
Albany Medical Center Chief Medical Physicist Radiation Oncology Imaging and Related Services POSITION SUMMARY: The Medical Physicist is responsible for assuring the high quality radiation therapy through
Professional Doctorate Program in Medical Physics (DMP) University of Cincinnati. Program Assessment. August 2014
 Professional Doctorate Program in Medical Physics (DMP) University of Cincinnati Program Assessment August 2014 Program Director Howard R. Elson, Ph.D. Barrett Cancer Center 513-584-9092 [email protected]
Professional Doctorate Program in Medical Physics (DMP) University of Cincinnati Program Assessment August 2014 Program Director Howard R. Elson, Ph.D. Barrett Cancer Center 513-584-9092 [email protected]
Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy
 Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy Set of 232 slides based on the chapter authored by W. Parker, H. Patrocinio of the IAEA publication (ISBN 92-0-107304-6): Review
Chapter 7: Clinical Treatment Planning in External Photon Beam Radiotherapy Set of 232 slides based on the chapter authored by W. Parker, H. Patrocinio of the IAEA publication (ISBN 92-0-107304-6): Review
American Association of Physicists in Medicine
 [email protected] American Association of Physicists in Medicine One Physics Ellipse College Park, MD 20740-3846 (301) 209-3350 Fax (301) 209-0862 http://www.aapm.org September 2, 2015 Andrew Slavitt Acting
[email protected] American Association of Physicists in Medicine One Physics Ellipse College Park, MD 20740-3846 (301) 209-3350 Fax (301) 209-0862 http://www.aapm.org September 2, 2015 Andrew Slavitt Acting
MDCT Technology. Kalpana M. Kanal, Ph.D., DABR Assistant Professor Department of Radiology University of Washington Seattle, Washington
 MDCT Technology Kalpana M. Kanal, Ph.D., DABR Assistant Professor Department of Radiology University of Washington Seattle, Washington ACMP Annual Meeting 2008 - Seattle, WA Educational Objectives Historical
MDCT Technology Kalpana M. Kanal, Ph.D., DABR Assistant Professor Department of Radiology University of Washington Seattle, Washington ACMP Annual Meeting 2008 - Seattle, WA Educational Objectives Historical
MSBS/Medical Physics Clinical Radiation Oncology Degree Requirements
 MSBS/ MEDICAL PHYSICS- CLINICAL RADIATION ONCOLOGY DEGREE REQUIREMENTS Admission Requirements T he purpose of the MSBS/Medical Physics with concentration in Clinical Radiation Oncology (MSCRO) is to train
MSBS/ MEDICAL PHYSICS- CLINICAL RADIATION ONCOLOGY DEGREE REQUIREMENTS Admission Requirements T he purpose of the MSBS/Medical Physics with concentration in Clinical Radiation Oncology (MSCRO) is to train
Clinic. ED Trauma Trauma Stroke. OR Neuro/Spine. Critical Care. Neuro ENT. Diagnostic. Pediatric. Radiology. Plastics Thoracic. Neuro.
 www.neurologica.com Critical Care Clinic Operating Room Radiology ED Trauma OR Neuro/Spine Pediatric Plastics Thoracic General Interventional Radiology ENT ED Trauma Trauma Stroke Critical Care Neuro Pediatric
www.neurologica.com Critical Care Clinic Operating Room Radiology ED Trauma OR Neuro/Spine Pediatric Plastics Thoracic General Interventional Radiology ENT ED Trauma Trauma Stroke Critical Care Neuro Pediatric
NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF ENVIRONMENTAL RADIATION PROTECTION EXTERNAL BEAM & BRACHYTHERAPY QUALITY ASSURANCE PROGRAM AUDIT FORM
 NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF ENVIRONMENTAL RADIATION PROTECTION EXTERNAL BEAM & BRACHYTHERAPY QUALITY ASSURANCE PROGRAM AUDIT FORM Purpose: To provide licensees and registrants with a
NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF ENVIRONMENTAL RADIATION PROTECTION EXTERNAL BEAM & BRACHYTHERAPY QUALITY ASSURANCE PROGRAM AUDIT FORM Purpose: To provide licensees and registrants with a
CT RADIATION DOSE REPORT FROM DICOM. Frank Dong, PhD, DABR Diagnostic Physicist Imaging Institute Cleveland Clinic Foundation Cleveland, OH
 CT RADIATION DOSE REPORT FROM DICOM Frank Dong, PhD, DABR Diagnostic Physicist Imaging Institute Cleveland Clinic Foundation Cleveland, OH CT Patient comes out... Patient goes in... Big Black Box Radiology
CT RADIATION DOSE REPORT FROM DICOM Frank Dong, PhD, DABR Diagnostic Physicist Imaging Institute Cleveland Clinic Foundation Cleveland, OH CT Patient comes out... Patient goes in... Big Black Box Radiology
WHERE IN THE WORLD JILL LIPOTI?
 WHERE IN THE WORLD IS JILL LIPOTI? HELLO FROM NEW JERSEY CRCPD - National Symposium on Fusion Imaging and Multimodalities February 18-20, 2004 Kansas City, Missouri New Jersey s Requirements As They Pertain
WHERE IN THE WORLD IS JILL LIPOTI? HELLO FROM NEW JERSEY CRCPD - National Symposium on Fusion Imaging and Multimodalities February 18-20, 2004 Kansas City, Missouri New Jersey s Requirements As They Pertain
AMERICAN BOARD OF MEDICAL PHYSICS
 AMERICAN BOARD OF MEDICAL PHYSICS INFORMATION BOOKLET American Board of Medical Physics, Inc. P.O. Box 780518 San Antonio, TX 78258 Phone: (210) 901-9052 Email: [email protected] ABMP_Information_Booklet_Revised_5/2015_TP
AMERICAN BOARD OF MEDICAL PHYSICS INFORMATION BOOKLET American Board of Medical Physics, Inc. P.O. Box 780518 San Antonio, TX 78258 Phone: (210) 901-9052 Email: [email protected] ABMP_Information_Booklet_Revised_5/2015_TP
SOP #: Revision #: Current Version Implementation Date: Page #: Page 1 of 10 Last Reviewed/Update Date: Expiration
 Implementation Page #: Page 1 of 10 Last Reviewed/Update 1. Purpose and Scope The purpose of this document is to describe the Medical Physics and Radiation Safety program at Boston University (BU) and
Implementation Page #: Page 1 of 10 Last Reviewed/Update 1. Purpose and Scope The purpose of this document is to describe the Medical Physics and Radiation Safety program at Boston University (BU) and
Emory University RT to Bachelor of Medical Science Degree Medical Imaging
 Emory University RT to Bachelor of Medical Science Degree Medical Imaging Courses: All RT-BMSc students must complete all of the program s core courses and the courses specific to their selected minor
Emory University RT to Bachelor of Medical Science Degree Medical Imaging Courses: All RT-BMSc students must complete all of the program s core courses and the courses specific to their selected minor
Gated Radiotherapy for Lung Cancer
 Gated Radiotherapy for Lung Cancer Steve B. Jiang, Ph.D. Depart Of Radiation Oncology University of California San Diego [email protected] radonc.ucsd.edu/research/cart Two Types of Gating Internal gating
Gated Radiotherapy for Lung Cancer Steve B. Jiang, Ph.D. Depart Of Radiation Oncology University of California San Diego [email protected] radonc.ucsd.edu/research/cart Two Types of Gating Internal gating
Radiologic Technology (RAD, CLE) courses are open only to Radiologic Technology majors.
 RADIOLOGIC TECHNOLOGY (A.A.S Degree) Director: Prof. Virginia Mishkin, M.S., R.T. (R) (M) (QM) A radiologic technologist is a skilled professional who provides a specialized health care service. This rewarding
RADIOLOGIC TECHNOLOGY (A.A.S Degree) Director: Prof. Virginia Mishkin, M.S., R.T. (R) (M) (QM) A radiologic technologist is a skilled professional who provides a specialized health care service. This rewarding
Moving Forward What does this mean for the Medical Physicist and the Imaging Community?
 Moving Forward What does this mean for the Medical Physicist and the Imaging Community? John M. Boone, Ph.D., FAAPM, FACR Professor and Vice Chairman of Radiology University of California Davis Medical
Moving Forward What does this mean for the Medical Physicist and the Imaging Community? John M. Boone, Ph.D., FAAPM, FACR Professor and Vice Chairman of Radiology University of California Davis Medical
Health. NYC Quality Assurance Guidelines for. Primary Diagnostic Monitors
 Health NYC Quality Assurance Guidelines for Primary Diagnostic Monitors June 2015 Content I. Overview... 1 II. Definitions... 1 III. Acceptance Testing Requirements... 4 IV. Bi-weekly PDM Testing... 4
Health NYC Quality Assurance Guidelines for Primary Diagnostic Monitors June 2015 Content I. Overview... 1 II. Definitions... 1 III. Acceptance Testing Requirements... 4 IV. Bi-weekly PDM Testing... 4
Our Department: structure and organization
 EORTC meeting for Radiation Therapy Technologists: RTT s role in the modernization of radiotherapy 10th October 2014, Villejuif (Grand Paris), France Elekta Stereotactic Body Frame: transmission modelled
EORTC meeting for Radiation Therapy Technologists: RTT s role in the modernization of radiotherapy 10th October 2014, Villejuif (Grand Paris), France Elekta Stereotactic Body Frame: transmission modelled
European Academy of DentoMaxilloFacial Radiology
 European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
Understanding Digital Modalities: System Integration and Use
 Understanding Digital Modalities: System Integration and Use Donald J. Peck, PhD Henry Ford Health System Detroit, MI [email protected] Dicom Digital Imaging and Communications in Medicine Part 3: Information
Understanding Digital Modalities: System Integration and Use Donald J. Peck, PhD Henry Ford Health System Detroit, MI [email protected] Dicom Digital Imaging and Communications in Medicine Part 3: Information
INTRODUCTION. A. Purpose
 New York State Department of Health Bureau of Environmental Radiation Protection Guide for Radiation Safety/Quality Assurance Programs Computed Radiography INTRODUCTION A. Purpose This guide describes
New York State Department of Health Bureau of Environmental Radiation Protection Guide for Radiation Safety/Quality Assurance Programs Computed Radiography INTRODUCTION A. Purpose This guide describes
Data Flow and Management in Radiation Therapy
 Data Flow and Management in Radiation Therapy Issues in Data Flow and Data Management in Radiation Oncology DICOM- an Overview with an Emphasis on Therapy - R. Siochi Issues in Data Flow Management in
Data Flow and Management in Radiation Therapy Issues in Data Flow and Data Management in Radiation Oncology DICOM- an Overview with an Emphasis on Therapy - R. Siochi Issues in Data Flow Management in
33-10-06-03. General requirements. 1. Administrative Controls.
 33-10-06-03. General requirements. 1. Administrative Controls. a. Registrant. The registrant shall be responsible for directing the operation of the x-ray systems which have been registered with the department.
33-10-06-03. General requirements. 1. Administrative Controls. a. Registrant. The registrant shall be responsible for directing the operation of the x-ray systems which have been registered with the department.
SWABIK Project. Software Tools for DICOM Media Exchange in Clinical Research: the. SWABIK Project
 Software Tools for DICOM Media Exchange in Clinical Research: the SWABIK Project Software Tools for DICOM Media Exchange in Clinical Research: the SWABIK Project O. ElGazzar 1, M. Onken 1, M. Eichelberg
Software Tools for DICOM Media Exchange in Clinical Research: the SWABIK Project Software Tools for DICOM Media Exchange in Clinical Research: the SWABIK Project O. ElGazzar 1, M. Onken 1, M. Eichelberg
King Fahd University of Petroleum & Minerals. Graduate Bulletin
 King Fahd University of Petroleum & Minerals Graduate Bulletin 2009-2011 King Fahd University of Petroleum & Minerals GRADUATE BULLETIN 2009-2011 Dhahran 31261, Saudi Arabia GRADUATE BULLETIN 2009-2011
King Fahd University of Petroleum & Minerals Graduate Bulletin 2009-2011 King Fahd University of Petroleum & Minerals GRADUATE BULLETIN 2009-2011 Dhahran 31261, Saudi Arabia GRADUATE BULLETIN 2009-2011
Implementation of Cone-beam CT imaging for Radiotherapy treatment localisation.
 Implementation of Cone-beam CT imaging for Radiotherapy treatment localisation. Andrew Bridges Clinical Scientist Diagnostic Radiology & Radiation Protection Physics Overview What is CBCT? Use of CBCT
Implementation of Cone-beam CT imaging for Radiotherapy treatment localisation. Andrew Bridges Clinical Scientist Diagnostic Radiology & Radiation Protection Physics Overview What is CBCT? Use of CBCT
Intensity-Modulated Radiation Therapy (IMRT)
 Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
Scan for mobile link. Intensity-Modulated Radiation Therapy (IMRT) Intensity-modulated radiotherapy (IMRT) uses linear accelerators to safely and painlessly deliver precise radiation doses to a tumor while
Radiation Protection in Radiotherapy
 Radiation Protection in Radiotherapy Albert Lisbona Medical Physics Department CLCC Nantes Atlantique 44805 Saint-Herblain France [email protected] Radiation therapy The lecture is oriented to
Radiation Protection in Radiotherapy Albert Lisbona Medical Physics Department CLCC Nantes Atlantique 44805 Saint-Herblain France [email protected] Radiation therapy The lecture is oriented to
Bon Secours St. Mary s Hospital School of Medical Imaging Course Descriptions by Semester 18 Month Program
 Bon Secours St. Mary s Hospital School of Medical Imaging Course Descriptions by Semester 18 Month Program First Semester RAD 1101 Patient Care, Ethics, Law and Diversity Credits This 16 week course prepares
Bon Secours St. Mary s Hospital School of Medical Imaging Course Descriptions by Semester 18 Month Program First Semester RAD 1101 Patient Care, Ethics, Law and Diversity Credits This 16 week course prepares
Proton beam. Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia
 Proton beam Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia Egyptian Candidates Proton therapy It can do more!!! Effectiveness of the proton therapy in targeting and curing
Proton beam Medical Technical Complex Joint Institute for Nuclear Research, Dubna, Russia Egyptian Candidates Proton therapy It can do more!!! Effectiveness of the proton therapy in targeting and curing
Radiation Oncology Department Solution
 Radiation Oncology Department Solution Radiation Oncology Department Solution Why MIM? Leading radiation oncology centers around the world are switching to MIM to maximize efficiency and take advantage
Radiation Oncology Department Solution Radiation Oncology Department Solution Why MIM? Leading radiation oncology centers around the world are switching to MIM to maximize efficiency and take advantage
Image Area. View Point. Medical Imaging. Advanced Imaging Solutions for Diagnosis, Localization, Treatment Planning and Monitoring. www.infosys.
 Image Area View Point Medical Imaging Advanced Imaging Solutions for Diagnosis, Localization, Treatment Planning and Monitoring www.infosys.com Over the years, medical imaging has become vital in the early
Image Area View Point Medical Imaging Advanced Imaging Solutions for Diagnosis, Localization, Treatment Planning and Monitoring www.infosys.com Over the years, medical imaging has become vital in the early
GE Healthcare. pet/ct for simulation. Precision in motion.
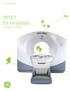 GE Healthcare pet/ct for simulation. Precision in motion. Patient profile H: 5 10 W: 370 lbs BMI: 53 Each cancer patient is just as unique as his or her cancer. Approaches to cancer treatment are changing
GE Healthcare pet/ct for simulation. Precision in motion. Patient profile H: 5 10 W: 370 lbs BMI: 53 Each cancer patient is just as unique as his or her cancer. Approaches to cancer treatment are changing
5/3/2011. DMP: Two Year Experience Outline. Professional Doctorate in Medical Physics (DMP) Two Year Experience. CAMPEP Accreditation
 DMP: Two Year Experience Outline Professional Doctorate in Medical Physics (DMP) Two Year Experience Charles W. Coffey Vanderbilt University Medical Center Nashville, TN Brief History of the Vanderbilt
DMP: Two Year Experience Outline Professional Doctorate in Medical Physics (DMP) Two Year Experience Charles W. Coffey Vanderbilt University Medical Center Nashville, TN Brief History of the Vanderbilt
Centralizing image and data management in radiation oncology with MOSAIQ Data Director
 White Paper Centralizing image and data management in radiation oncology with MOSAIQ Data Director Authors: Laura Francis, Global Product Marketing, Elekta Software, UK and Erdal Sipahi, Information Technology,
White Paper Centralizing image and data management in radiation oncology with MOSAIQ Data Director Authors: Laura Francis, Global Product Marketing, Elekta Software, UK and Erdal Sipahi, Information Technology,
PET and PET/CT in Clinical Trials
 PET and PET/CT in Clinical Trials Nathan C. Hall, M.D., Ph.D. The Ohio State University Medical Center CALGB Imaging Core Lab CALGB Imaging Committee Outline Introduction to PET Positron Emitter Physics
PET and PET/CT in Clinical Trials Nathan C. Hall, M.D., Ph.D. The Ohio State University Medical Center CALGB Imaging Core Lab CALGB Imaging Committee Outline Introduction to PET Positron Emitter Physics
There must be an appropriate administrative structure for each residency program.
 Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Cancer Care Delivered Locally by Physicians You Know and Trust
 West Florida Physician Office Building Johnson Ave. University Pkwy. Olive Road N. Davis Hwy. For more information on West Florida Cancer Center: 850-494-5404 2130 East Johnson Avenue Pensacola, Florida
West Florida Physician Office Building Johnson Ave. University Pkwy. Olive Road N. Davis Hwy. For more information on West Florida Cancer Center: 850-494-5404 2130 East Johnson Avenue Pensacola, Florida
2012 LACC Clinical Obligations & Grading System. Attendance Requirement
 2012 LACC Clinical Obligations & Grading System Attendance Requirement The Radiology program has a Monday through Friday schedule during the fall, winter, spring and summer semesters. Students are required
2012 LACC Clinical Obligations & Grading System Attendance Requirement The Radiology program has a Monday through Friday schedule during the fall, winter, spring and summer semesters. Students are required
Radiation Oncology Practice Accreditation Program Requirements
 Radiation Oncology Practice Accreditation Program Requirements Contents Introduction... 3 Application for Accreditation... 3 Preliminary Self-Assessment (ROPA Website Toolkit)... 3 Checklist for Site Survey...
Radiation Oncology Practice Accreditation Program Requirements Contents Introduction... 3 Application for Accreditation... 3 Preliminary Self-Assessment (ROPA Website Toolkit)... 3 Checklist for Site Survey...
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
The First Non-University Based CAMPEP Accredited dresidency Program
 The First Non-University Based CAMPEP Accredited dresidency Program Brian Wichman, MS, DABR Kansas City Cancer Center ABR 2012/2014 Eligibility Changes You know the changes you know the dilemma. However,
The First Non-University Based CAMPEP Accredited dresidency Program Brian Wichman, MS, DABR Kansas City Cancer Center ABR 2012/2014 Eligibility Changes You know the changes you know the dilemma. However,
Imaging Technology. Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist
 Imaging Technology Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist Diagnostic Medical Sonographer, Dosimetrist Diagnostic Medical
Imaging Technology Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist Diagnostic Medical Sonographer, Dosimetrist Diagnostic Medical
Tumor. An Brief Introduction to 4D CT Scanning. Outline. Three Types of Motion Artifacts. CT Artifacts in Free Breathing 3D Scan
 An Brief Introduction to 4D CT Scanning Steve B. Jiang, Ph.D. Dept of Radiation Oncology Univ of California San Diego Outline Problems with free breathing 3D scanning What is 4D CT? How does it work? Acknowledgements
An Brief Introduction to 4D CT Scanning Steve B. Jiang, Ph.D. Dept of Radiation Oncology Univ of California San Diego Outline Problems with free breathing 3D scanning What is 4D CT? How does it work? Acknowledgements
Patient Dose Tracking for Imaging Studies. David E. Hintenlang, Ph.D., DABR University of Florida
 Patient Dose Tracking for Imaging Studies David E. Hintenlang, Ph.D., DABR University of Florida Conflict of Interest Statement No affiliation or financial interests in any of the commercial products or
Patient Dose Tracking for Imaging Studies David E. Hintenlang, Ph.D., DABR University of Florida Conflict of Interest Statement No affiliation or financial interests in any of the commercial products or
kv-& MV-CBCT Imaging for Daily Localization: Commissioning, QA, Clinical Use, & Limitations
 kv-& MV-CBCT Imaging for Daily Localization: Commissioning, QA, Clinical Use, & Limitations Moyed Miften, PhD Dept of Radiation Oncology University of Colorado Denver Questions Disease Stage (local, regional,
kv-& MV-CBCT Imaging for Daily Localization: Commissioning, QA, Clinical Use, & Limitations Moyed Miften, PhD Dept of Radiation Oncology University of Colorado Denver Questions Disease Stage (local, regional,
REGULATION: QUALITY ASSURANCE PROGRAMS FOR MEDICAL DIAGNOSTIC X-RAY INSTALLATIONS N.J.A.C. 7:28-22
 REGULATION: QUALITY ASSURANCE PROGRAMS FOR MEDICAL DIAGNOSTIC X-RAY INSTALLATIONS N.J.A.C. 7:28-22 New Jersey Department of Environmental Protection Bureau of Radiological Health PO Box 415 Trenton NJ
REGULATION: QUALITY ASSURANCE PROGRAMS FOR MEDICAL DIAGNOSTIC X-RAY INSTALLATIONS N.J.A.C. 7:28-22 New Jersey Department of Environmental Protection Bureau of Radiological Health PO Box 415 Trenton NJ
CHAPTER 7. CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY
 Review of Radiation Oncology Physics: A Handbook for Teachers and Students CHAPTER 7. CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY WILLIAM PARKER Department of Medical Physics McGill
Review of Radiation Oncology Physics: A Handbook for Teachers and Students CHAPTER 7. CLINICAL TREATMENT PLANNING IN EXTERNAL PHOTON BEAM RADIOTHERAPY WILLIAM PARKER Department of Medical Physics McGill
NIA RADIATION ONCOLOGY CODING STANDARD. Dosimetry Planning
 NIA RADIATION ONCOLOGY CODING STANDARD Dosimetry Planning CPT Codes: 77295, 77300, 77301, 77306, 77307, 77321, 77316, 77317, 77318, 77331, 77399 Original Date: April, 2011 Last Reviewed Date: November,
NIA RADIATION ONCOLOGY CODING STANDARD Dosimetry Planning CPT Codes: 77295, 77300, 77301, 77306, 77307, 77321, 77316, 77317, 77318, 77331, 77399 Original Date: April, 2011 Last Reviewed Date: November,
International Conference on Clinical PET CT and Molecular Imaging: PET CT in the Era of Multimodality Imaging and Image Guided Therapy (IPET-2015)
 International Conference on Clinical PET CT and Molecular Imaging: PET CT in the Era of Multimodality Imaging and Image Guided Therapy (IPET-2015) IAEA Headquarters Vienna, Austria 5 9 October 2015 Ref.
International Conference on Clinical PET CT and Molecular Imaging: PET CT in the Era of Multimodality Imaging and Image Guided Therapy (IPET-2015) IAEA Headquarters Vienna, Austria 5 9 October 2015 Ref.
Education, Training, and Certification of Medical Physicist in Korea
 Education, Training, and Certification of Medical Physicist in Korea Rena Lee, Education Committee, KSMP Tae-Suk Suh, President, KSMP The 7th Asia-Oceania Congress of Medical Physics IOMP Symposium on
Education, Training, and Certification of Medical Physicist in Korea Rena Lee, Education Committee, KSMP Tae-Suk Suh, President, KSMP The 7th Asia-Oceania Congress of Medical Physics IOMP Symposium on
GE Healthcare. DoseWatch. Gathering Radiation Dose Data
 GE Healthcare DoseWatch Gathering Radiation Dose Data Gathering Radiation Dose Data After your organization crosses the bridge of Why? for patient radiation dose management either due to regulation, risk
GE Healthcare DoseWatch Gathering Radiation Dose Data Gathering Radiation Dose Data After your organization crosses the bridge of Why? for patient radiation dose management either due to regulation, risk
Monitoring Patient Radiation Dose in VA. Charles M. Anderson MD, PhD Chief Consultant for Diagnostic Services Veterans Health Administration
 Monitoring Patient Radiation Dose in VA Charles M. Anderson MD, PhD Chief Consultant for Diagnostic Services Veterans Health Administration TWENTY ONE/NOVEMBER 2011 Computed Tomography (CT), Magnetic Resonance
Monitoring Patient Radiation Dose in VA Charles M. Anderson MD, PhD Chief Consultant for Diagnostic Services Veterans Health Administration TWENTY ONE/NOVEMBER 2011 Computed Tomography (CT), Magnetic Resonance
Design and Scheduling of Proton Therapy Treatment Centers
 Design and Scheduling of Proton Therapy Treatment Centers Stuart Price, University of Maryland Bruce Golden, University of Maryland Edward Wasil, American University Howard Zhang, University of Maryland
Design and Scheduling of Proton Therapy Treatment Centers Stuart Price, University of Maryland Bruce Golden, University of Maryland Edward Wasil, American University Howard Zhang, University of Maryland
Quality Reports With. PlanIQ. *Export only. 510(k) pending. Patent pending. Your Most Valuable QA and Dosimetry Tools
 Quality Reports With PlanIQ * *Export only. 510(k) pending. Patent pending. Your Most Valuable QA and Dosimetry Tools Objective Plan Assessment? How good are my treatment plans? Quality assurance of radiation
Quality Reports With PlanIQ * *Export only. 510(k) pending. Patent pending. Your Most Valuable QA and Dosimetry Tools Objective Plan Assessment? How good are my treatment plans? Quality assurance of radiation
4D Scanning. Image Guided Radiation Therapy. Outline. A Simplified View of the RT Process. Outline. Steve B. Jiang, Ph.D.
 4D Scanning Steve B. Jiang, Ph.D. Department of Radiation Oncology [email protected] http://gray.mgh.harvard.edu/ Outline Problems with free breathing 3D scanning What is 4D CT? How does it work?
4D Scanning Steve B. Jiang, Ph.D. Department of Radiation Oncology [email protected] http://gray.mgh.harvard.edu/ Outline Problems with free breathing 3D scanning What is 4D CT? How does it work?
NEW JERSEY RADIOLOGIC TECHNOLOGY BOARD OF EXAMINERS (BOARD) ACCREDITATION STANDARDS FOR SCHOOLS OF DENTAL RADIOLOGIC TECHNOLOGY
 NEW JERSEY RADIOLOGIC TECHNOLOGY BOARD OF EXAMINERS (BOARD) ACCREDITATION STANDARDS FOR SCHOOLS OF DENTAL RADIOLOGIC TECHNOLOGY This document contains the Board s accreditation standards for schools of
NEW JERSEY RADIOLOGIC TECHNOLOGY BOARD OF EXAMINERS (BOARD) ACCREDITATION STANDARDS FOR SCHOOLS OF DENTAL RADIOLOGIC TECHNOLOGY This document contains the Board s accreditation standards for schools of
QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET
 Centers for Quantitative Imaging Excellence (CQIE) LEARNING MODULE QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET American College of Radiology Clinical Research Center v.1 Centers for Quantitative
Centers for Quantitative Imaging Excellence (CQIE) LEARNING MODULE QUANTITATIVE IMAGING IN MULTICENTER CLINICAL TRIALS: PET American College of Radiology Clinical Research Center v.1 Centers for Quantitative
Failure Modes and Effects Analysis (FMEA)
 Failure Modes and Effects Analysis (FMEA) Sasa Mutic Washington University School of Medicine St. Louis Missouri Failure Modes and Effects Analysis Objectives: To motivate the use of FMEA and to provide
Failure Modes and Effects Analysis (FMEA) Sasa Mutic Washington University School of Medicine St. Louis Missouri Failure Modes and Effects Analysis Objectives: To motivate the use of FMEA and to provide
Diagnostic Exposure Tracking in the Medical Record
 Diagnostic Exposure Tracking in the Medical Record J.A. Seibert, Ph.D. Department of Radiology Sacramento, California USA Vancouver. British Columbia Relevant disclosures None Learning objectives Understand
Diagnostic Exposure Tracking in the Medical Record J.A. Seibert, Ph.D. Department of Radiology Sacramento, California USA Vancouver. British Columbia Relevant disclosures None Learning objectives Understand
U.S. Bureau of Labor Statistics. Radiology Tech
 From the: U.S. Bureau of Labor Statistics Radiology Tech What They Do Radiologic technologists (RTs) perform diagnostic imaging examinations, such as x rays, on patients. Duties RTs typically do the following:
From the: U.S. Bureau of Labor Statistics Radiology Tech What They Do Radiologic technologists (RTs) perform diagnostic imaging examinations, such as x rays, on patients. Duties RTs typically do the following:
Oncentra Brachy Comprehensive treatment planning for brachytherapy. Time to focus on what counts
 Oncentra Brachy Comprehensive treatment planning for brachytherapy Time to focus on what counts Time to focus on what counts In contemporary brachytherapy, the medical physicist needs to process an increasing
Oncentra Brachy Comprehensive treatment planning for brachytherapy Time to focus on what counts Time to focus on what counts In contemporary brachytherapy, the medical physicist needs to process an increasing
Presentation Objective: Benefits to New Employee. Goal for Participants. Benefits to the Administration
 Imaging Department Quick Step How to Create and Implement a Rapid Integration Orientation New Employee Orientation builds a bridge between the old job and the new job for better quality in health care
Imaging Department Quick Step How to Create and Implement a Rapid Integration Orientation New Employee Orientation builds a bridge between the old job and the new job for better quality in health care
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS
 INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
Preface to Practice Standards
 0 0 0 0 Preface to Practice Standards A profession s practice standards serve as a guide for appropriate practice. The practice standards define the practice and establish general criteria to determine
0 0 0 0 Preface to Practice Standards A profession s practice standards serve as a guide for appropriate practice. The practice standards define the practice and establish general criteria to determine
Medical Radiologic Technology
 Medical Radiologic Technology 220 Medical Radiologic Technology Location: Trenholm Campus - Bldg. H Program Information The Medical Radiologic Technology program at Trenholm State provides students with
Medical Radiologic Technology 220 Medical Radiologic Technology Location: Trenholm Campus - Bldg. H Program Information The Medical Radiologic Technology program at Trenholm State provides students with
COURSE OUTLINE Course Title: Quality Assurance and Radiography Seminar
 Course Number: RAD220 Lecture Hours: 3 Laboratory Hours: 2 COURSE OUTLINE Course Title: Quality Assurance and Radiography Seminar Prerequisites: RAD216 Co-Requisites: RAD224, RAD240 Credits: 4 Catalog
Course Number: RAD220 Lecture Hours: 3 Laboratory Hours: 2 COURSE OUTLINE Course Title: Quality Assurance and Radiography Seminar Prerequisites: RAD216 Co-Requisites: RAD224, RAD240 Credits: 4 Catalog
HDR Brachytherapy 1: Overview of QA. Disclosures: Learning Objectives 7/23/2014
 HDR Brachytherapy 1: Overview of QA Bruce Libby Department of Radiation Oncology University of Virginia Health System Disclosures: Nondisclosure agreement with Varian Brachytherapy Shareholder- Varian,
HDR Brachytherapy 1: Overview of QA Bruce Libby Department of Radiation Oncology University of Virginia Health System Disclosures: Nondisclosure agreement with Varian Brachytherapy Shareholder- Varian,
The role, responsibilities and status of the clinical medical physicist in AFOMP
 Australasian Physical & Engineering Sciences in Medicine Volume 32 Number 4, 2009 AFOMP POLICY STATEMENT N O 1 The role, responsibilities and status of the clinical medical physicist in AFOMP K. H. Ng*
Australasian Physical & Engineering Sciences in Medicine Volume 32 Number 4, 2009 AFOMP POLICY STATEMENT N O 1 The role, responsibilities and status of the clinical medical physicist in AFOMP K. H. Ng*
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Radiation Oncology Centers Participating in MassHealth. Daniel Tsai, Assistant Secretary and Director of MassHealth
 Executive Office of Health and Human s Office of Medicaid www.mass.gov/masshealth May 2015 TO: FROM: RE: Radiation Oncology Centers Participating in Daniel Tsai, Assistant Secretary and Director of (2015
Executive Office of Health and Human s Office of Medicaid www.mass.gov/masshealth May 2015 TO: FROM: RE: Radiation Oncology Centers Participating in Daniel Tsai, Assistant Secretary and Director of (2015
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
M D Anderson Cancer Center Orlando TomoTherapy s Implementation of Image-guided Adaptive Radiation Therapy
 M D Anderson Cancer Center Orlando TomoTherapy s Implementation of Image-guided Adaptive Radiation Therapy Katja Langen, PhD Research supported by TomoTherapy Inc. Today s Lecture Introduction to helical
M D Anderson Cancer Center Orlando TomoTherapy s Implementation of Image-guided Adaptive Radiation Therapy Katja Langen, PhD Research supported by TomoTherapy Inc. Today s Lecture Introduction to helical
Quality Control and Maintenance Programs
 Quality Control and Maintenance Programs Cari Borrás, D.Sc., FACR, FAAPM Visiting Professor DOIN-DEN / UFPE Recife, Pernambuco, Brazil Co-Chair, IUPESM Health Technology Task Group 1 Medical Imaging Equipment
Quality Control and Maintenance Programs Cari Borrás, D.Sc., FACR, FAAPM Visiting Professor DOIN-DEN / UFPE Recife, Pernambuco, Brazil Co-Chair, IUPESM Health Technology Task Group 1 Medical Imaging Equipment
Total Solutions. Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA phone 412 312 6700 800 70 NOMOS www.nomos.com
 Serial Tomotherapy IGRT Total Solutions Treatment Planning Brachytherapy Imaging Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA BMI.v.08.2010 Best NOMOS Your Single Source Oncology Solutions Provider
Serial Tomotherapy IGRT Total Solutions Treatment Planning Brachytherapy Imaging Best NOMOS One Best Drive, Pittsburgh, PA 15202 USA BMI.v.08.2010 Best NOMOS Your Single Source Oncology Solutions Provider
Consultation. Review of the scopes of practice for registration in the profession of medical radiation technology
 Consultation Review of the scopes of practice for registration in the profession of medical radiation technology CONTENTS Page Consultation Information... 3 Context of the Consultation... 4-7 Legislative
Consultation Review of the scopes of practice for registration in the profession of medical radiation technology CONTENTS Page Consultation Information... 3 Context of the Consultation... 4-7 Legislative
Establishing a Patient Safety Program in Radiation Oncology
 Establishing a Patient Safety Program in Radiation Oncology : John E. Bayouth, PhD Professor and Chief of Physics Department of Human Oncology University of Wisconsin ! none Disclosures Introduction! Modern
Establishing a Patient Safety Program in Radiation Oncology : John E. Bayouth, PhD Professor and Chief of Physics Department of Human Oncology University of Wisconsin ! none Disclosures Introduction! Modern
RADIOLOGIC TECHNOLOGY PROGRAM ASSOCIATE of SCIENCE DEGREE
 Mt. San Antonio College Technology and Health Division 1100 N. Grand Ave Walnut, CA 91789 TEL: 909-594-5611, EX. 4750 FAX: 909-468-3938 RADIOLOGIC TECHNOLOGY PROGRAM ASSOCIATE of SCIENCE DEGREE The course
Mt. San Antonio College Technology and Health Division 1100 N. Grand Ave Walnut, CA 91789 TEL: 909-594-5611, EX. 4750 FAX: 909-468-3938 RADIOLOGIC TECHNOLOGY PROGRAM ASSOCIATE of SCIENCE DEGREE The course
IAEA-TECDOC-1540. Specification and Acceptance Testing of Radiotherapy Treatment Planning Systems
 IAEA-TECDOC-1540 Specification and Acceptance Testing of Radiotherapy Treatment Planning Systems April 2007 IAEA-TECDOC-1540 Specification and Acceptance Testing of Radiotherapy Treatment Planning Systems
IAEA-TECDOC-1540 Specification and Acceptance Testing of Radiotherapy Treatment Planning Systems April 2007 IAEA-TECDOC-1540 Specification and Acceptance Testing of Radiotherapy Treatment Planning Systems
Innovative RT SBRT. The variables with REQ in superscript are required.
 The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
The variables with REQ in superscript are required. The variables with a are single-select variables; only one answer can be selected. The variables with a are multi-select variables; multiple answers
SEAAPM Symposium The Practice of Quality Assurance in an Era of Change
 SEAAPM Symposium The Practice of Quality Assurance in an Era of Change Directors: Dan Bourland and Ingrid Marshall Vendors, breaks, and food next door Thank you to SEAAPM EXCOM, Commercial Partners, Faculty,
SEAAPM Symposium The Practice of Quality Assurance in an Era of Change Directors: Dan Bourland and Ingrid Marshall Vendors, breaks, and food next door Thank you to SEAAPM EXCOM, Commercial Partners, Faculty,
