74 Winter 2014 Volume 29 Number 4
|
|
|
- Timothy Blair
- 9 years ago
- Views:
Transcription
1 74 Winter 2014 Volume 29 Number 4
2 TEAM Japan/Usa Funato/Tonotsuka/Murabe/Hirota/Ogawa A Novel Strategy for Bone Integration and Regeneration: Case Studies Photofunctionalization of Dental Implants and Ti Mesh Akiyoshi Funato, DDS Ryohei Tonotsuka, DDS Hitoshi Murabe, DDS Makoto Hirota, DDS, PhD Takahiro Ogawa, DDS, PhD The digital jcd version features a preview and link to an educational DentalXP video about this article. Abstract Ultraviolet light treatment of dental implants immediately prior to placement, or photofunctionalization, is a novel clinical tool with the potential to improve implant therapy. Photofunctionalization improves the surface properties of titanium surfaces by removing hydrocarbons, regenerating hydrophilicity, and optimizing electrostatic properties. We photofunctionalized dental implants and titanium mesh (Ti mesh) in two complex clinical cases requiring simultaneous guided bone regeneration, sinus elevation, immediate implant placement into the extraction socket, and esthetic consideration. The use of photofunctionalized implants and Ti mesh facilitated more strategic and aggressive treatment planning and resulted in successful treatment outcomes with secure application of immediate and early loading protocols. In vitro, the number of attached osteoblasts and the level of alkaline phosphatase activity were substantially increased on photofunctionalized Ti mesh, providing validation of the enhanced osteoconductive properties of photofunctionalized Ti mesh. An overview of the principles of photofunctionalization and practical guidance on its clinical use are presented. The clinical cases discussed here, along with the suggested technical guidance and research data, suggest that photofunctionalization is a useful and effective tool for improving implant therapy by enabling novel avenues of treatment and overcoming common challenges in current implant dentistry. Key Words: photofunctionalized implants, UV, bone augmentation, Ti mesh, hydrophilic, osseointegration Journal of Cosmetic Dentistry 75
3 Introduction Introduction Ultraviolet (UV) light treatment of dental implants immediately prior to placement, known as photofunctionalization, has drawn considerable interest and attention as a novel and viable clinical tool for improving outcomes in implant therapy. 1-5 A significant number of implant cases require the site-development surgery to secure implant stability, obtain optimal esthetics, and ensure longevity. A common biological event for establishing osseointegration and pre-implant bone augmentation is the interaction between osteogenic cells and titanium materials. This article presents two clinical cases that successfully restored complex situations using photofunctionalized dental implants and titanium mesh (Ti mesh). Also presented are the theoretical and technical rationale for photofunctionalization and clinically relevant in vitro data that show an increased osteoconductivity of photofunctionalized Ti mesh. Photofunctionalization Dental implants are hydrophobic and covered with the hydrocarbons that always accumulate during normal aging (Fig 1). 4-7 Photofunctionalization is the rapid, chairside conditioning of dental implants using UV light that results in the removal of hydrocarbons, regenerates hydrophilicity, and optimizes the electrostatic properties of the implant surfaces (Fig 1). 4,8-10 The improved surface properties have been shown to enhance specific biological events necessary for osseointegration (Fig 2). Photofunctionalization increases the strength of osseointegration threefold during the early stages of healing in animal models and results in an increase in bone-implant contact from 53% to 98.2%, virtually a maximal level of osseointegration. 8 Specifically, photofunctionalization improves implant surfaces by (1) removing surface carbon that unavoidably accumulated on the surface during the biological aging of titanium, (2) regenerating superhydrophilicity that had been lost during the biological aging of titanium, and (3) optimizing the electrostatic status of the surface. Note that the presence of hydrophilicity alone does not improve the osteoconductivity of implants as significantly as when the three prerequisites of osseointegration are met. In humans, a study involving a large number (90%) of complex cases showed that the healing time before functional loading was 3.2 months in photofunctionalized implants and 6.5 months in as-received implants. 1 There was no negative impact of the substantially accelerated loading on the success rate up to the followup period of 2.5 years. The speed of osseointegration, as evaluated by the implant stability quotient (ISQ) increase per month, is 3 to 20 times greater for photofunctionalized implants than as-received implants reported in the literature. 1,3 Clinical and animal studies reported the preservation, and in some cases even a gain, of the marginal bone level after receiving photofunctionalized implants. 2,11,12 The boneimplant interface at the marginal area was more intensively mineralized around photofunctionalized implants, suggesting that the quality of marginal bone was enhanced around photofunctionalized implants. 11 Photofunctionalization is effective for all the titanium surfaces tested, as shown by hydrophobic to hydrophilic surface changes of various dental implants (Fig 1). 13,14 Hemophilicity, as shown by blood spiraling up the implant surface, can be seen around photofunctionalized dental implants as soon as they make contact with the implant site, in contrast to untreated controls (Figs 3a & 3b). Biological Validation of Photofunctionalized Ti Mesh In addition to the acceleration and enhancement of bone-implant integration, the potential effect of photofunctionalization is to improve the interaction of biological cells and tissues with various biomaterials. Given the principle and mechanism behind photofunctionalization (i.e., carbon removable and hydrophilicity regeneration), photofunctionalization should be effective as long as the biomaterial is titanium- or titanium alloy-based. Among titanium-based biomaterials used in conjunction with implant therapy, Ti mesh could be a potential target of improvement because of its large area interfacing with existing and regenerating bone. Probably due to the improved biocompatibility, the anti-inflammatory effect of photofunctionalized Ti mesh is routinely experienced in clinical situations by the reduced manifestation of postoperative swelling and flare reaction, and the accelerated soft tissue wound healing. The percentage of post-implant surgery complications, including the chance of Ti mesh exposure, tissue dehiscence, and infection, can be reduced from 4.95% to 0.59% by applying photofunctionalization. 1 However, the potential effect of photofunctionalization to enhance the osteoconductivity of Ti mesh has not been examined, prompting us to perform the in vitro experimental study discussed in this report. Human mesenchymal stem cell-derived osteoblasts were cultured on Ti mesh with and without photofunctionalization using a previously established experimental protocol. 15 Photofunctionalization was performed for 15 minutes using a photo device (TheraBeam Affiny, Ushio; Tokyo, Japan). After 24 hours of culture, a greater number of osteoblasts attached on photofunctionalized Ti mesh than on untreated Ti mesh. As a result, an approximately five times greater area of Ti mesh was covered by osteoblasts, as seen in confocal microscopy images (Fig 4a). In addition, the behavior of the cells was significantly improved. The cells were immunochemically stained for cytoskeletal actin (red) and adhesion protein, vinculin (green). A histogram showing the area of cell coverage (osteoblasts occupation in % area on Ti mesh) is also presented (Fig 4b). 76 Winter 2014 Volume 29 Number 4
4 Funato/Tonotsuka/Murabe/Hirota/Ogawa As-received Photofunctionalized As-received Photofunctionalized Figure 1: The rapid, chairside conversion from hydrophobic to hydrophilic surfaces on all commercial dental implants by photofunctionalization. Removes carbon Promotes adhesion and spread of cells Regenerates hydrophilicity Provides access for proteins and cells Optimizes electrostatic properties Works as attractants for proteins and cells Figure 2: Photofunctionalization regains the prerequisites for osseointegration that have been lost or substantially compromised during biological aging of titanium. Journal of Cosmetic Dentistry 77
5 Figures 3a & 3b: Typical clinical images depicting hemophilic surfaces of photofunctionalized dental implants. As-received Ti mesh Photofunctionalized Ti mesh 200 µm Figure 4a: Larger area of osteoblast coverage on photofunctionalized Ti mesh. Confocal microscopic image of human osteoblasts cultured on as-received Ti mesh and photofunctionalized Ti mesh 24 hours after seeding. Figure 4b: Histogram showing the area of cell coverage (osteoblasts occupation in % area on Ti mesh). **p < 0.01, statistically significant between as-received and photofunctionalized Ti mesh. A common biological event for establishing osseointegration and pre-implant bone augmentation is the interaction between osteogenic cells and titanium materials. 78 Winter 2014 Volume 29 Number 4
6 Funato/Tonotsuka/Murabe/Hirota/Ogawa The cells spread and settled more quickly on photofunctionalized Ti mesh, and there was increased expression of actin (a cytoskeletal protein) and vinculin (an adhesion protein) in cells on photofunctionalized Ti mesh (Fig 5a). The results from cytomorphometry and protein expression densitometry are also presented (Fig 5b). Culture images after alkaline phosphatase (ALP) stain and the result from ALP chemical quantification are shown (Figs 6a & 6b). The expression of ALP, an early marker of osteoblastic function, was considerably greater in cells on photofunctionalized Ti mesh. These results indicated that photofunctionalization of Ti mesh significantly increased the number of osteoblasts attached, enhanced the adhesion and retention of cells on Ti mesh, and expedited the osteogenic function in the cells. Photofunctionalization increases the strength of osseointegration threefold during the early stages of healing in animal models and results in an increase in bone-implant contact from 53% to 98.2%, virtually a maximal level of osseointegration. As-received Ti mesh Photofunctionalized Ti mesh Case Reports Case 1: Fixed Implant Restoration with Simultaneous GBR in the Esthetic Zone Using Photofunctionalized Implants and Ti Mesh Securing three-dimensional shape of bone and soft tissue (e.g., contour, height, and thickness) holds a key to successful implant restoration in esthetic cases A 46-year-old female presented with a dislodged bridge and root fractures in the anterior maxilla. Two months after teeth #7 and #9 were extracted, photofunctionalized implants (4 mm in diameter and 13 mm in length, Osseotite Certain, BIOMET 3i, West Palm Beach, FL) were placed at these sites. Photofunctionalization was performed by treating the implants with UV light for 15 minutes (Fig 7a), using a photo device (TheraBeam Affiny) at chairside immediately prior to implantation (Fig 7b). Simultaneous guided bone regeneration (GBR) was performed Figure 5a: Attachment and spreading behavior of human osteoblasts enhanced on photofunctionalized Ti mesh. High magnification confocal microscopic images are shown with immunochemical stain for cytoskeletal actin (red) and adhesion protein, vinculin (green). Vinculin Figure 5b: The results from cytomorphometry and protein expression densitometry based upon the analyses using the microscopic images. *p < 0.05; **p < 0.01, statistically significant between as-received and photofunctionalized Ti mesh. Journal of Cosmetic Dentistry 79
7 As-received Ti mesh Photofunctionalized Ti mesh Figure 6a: Culture images after ALP stain and the result from ALP chemical quantification. Figure 6b: ALP activity in human osteoblasts compared between as-received and photofunctionalized Ti mesh. **p < 0.01, statistically significant between as-received and photofunctionalized Ti mesh. using Ti mesh, which was also photofunctionalized and confirmed to be highly hydrophilic (Fig 8). After the Ti mesh was fixed with a cover screw, the defect was filled with xenograft bone substitute material (Bio-Oss Cancellous mm particles, Geistlich; Princeton, NJ) and covered with resorbable collagen membrane (Ossix, OraPharma, Warminster, PA). After four months of healing, mature bone formation of sufficient width and height was confirmed clinically and a connective tissue graft procedure performed. Pre- and postoperative clinical images are presented in Figures 9a-9c. The soft tissue healed for two months before the provisional restoration was placed (Fig 10a). 19 Tooth #8 was saved as a submerged root to maintain the surrounding alveolar bone The final fixed restoration was placed, and the esthetics and function have been maintained satisfactorily after a one-year follow-up (Figs 10b & 10c). As-received Ti mesh Photofunctionalized Ti mesh Figure 7a: UV light. Figure 8: Hydrophobic-to-hydrophilic conversion of Ti mesh after photofunctionalization. Figure 7b: A photo device used for photofunctionalization. The device provides an automatic 15- to 20-minute program of conditioning with optimized wavelength and strength of UV light treatment. 80 Winter 2014 Volume 29 Number 4
8 Funato/Tonotsuka/Murabe/Hirota/Ogawa a b c Figures 9a-9c: Case 1, clinical images during (a) implant placement and (b) simultaneous GBR using Ti mesh. The implants and Ti mesh were photofunctionalized. Note the matte Ti mesh surface due to widespread blood, as opposed to a glossy surface typically seen on as-received Ti mesh (b). Mature bone formation of sufficient width and height along with osseointegration were clinically confirmed after four months (c). Figure 10a: Final restoration in place. The use of photofunctionalized implants and Ti mesh enabled more strategic and aggressive treatment planning and resulted in successful treatment outcomes with secure application of immediate and early loading protocols. Figures 10b & 10c: A radiographic image of the final restoration along with the peri-implant x-ray image in Case 1. Journal of Cosmetic Dentistry 81
9 Figure 11: Case 2, panoramic x-ray image. Case 2: Effective Application of Immediate and Early Loading Protocols on Photofunctionalized Implants A 64-year-old female wearing upper and lower removable dentures presented for possible replacement with implant restorations (Fig 11). A boneanchored bridge with pink porcelain was planned for both the maxilla and mandible, and the application of early and immediate loading protocols was planned for the maxilla and mandible, respectively. A two-stage extraction was planned for the six maxillary hopeless teeth; three teeth were extracted on the day of implant placement, while the other three were extracted when the provisional restoration was placed onto the implants (Fig 12a). After the three maxillary teeth were extracted, six photofunctionalized implants (4 mm in diameter and 13 mm in length, Osseotite Certain) were placed; two implants were placed in fresh extraction sockets at the bilateral a c b Figures 12a-12c: Intraoral images of the maxilla before (a) and during (b) implant surgery. Six photofunctionalized implants were placed in either fresh extraction sockets, native bone, or sinus elevation sites. Two months after implant placement, a provisional restoration was put in place on the implants (c). 82 Winter 2014 Volume 29 Number 4
10
11 lateral incisor areas, while two implants were placed in the bilateral premolar areas with native bone support (Fig 12b). Another two implants were placed in the posterior maxilla with simultaneous sinus elevation, using the lateral window technique. A temporary prosthesis was placed using the three natural teeth as anchors while the implants were kept unloaded. After two months, the implants were uncovered and the provisional restoration was screwed onto the six implants at the time of extraction of the remaining three teeth (Fig 12c). Two months later, all remaining teeth in the mandible were extracted and four photofunctionalized implants were placed (all were 4 mm in diameter and 13 mm in length, except for the one at the lower right anterior position, which was 5 mm in diameter and 13 mm in length) (Fig 13a). The implants were immediately loaded with a full-arch acrylic temporary prosthesis (Fig 13b). After confirming successful osseointegration and soft tissue healing (Fig 14), a computer-aided design/computer-aided manufacturing (CAD/CAM)-assisted final restoration was fabricated and placed (Fig 15). Seven Tips for Photofunctionalization The results of the previous studies and the outcomes of the two cases discussed here show that photofunctionalization is a novel and effective tool that has the potential to improve multiple aspects of current implant therapy. The ability to overcome biological aging, a simple chairside procedure, and its versatile application are additional benefits of the technology. Its use need not be limited to expediting and enhancing osseointegration, but can also be extended to enhancing bone formation around Ti mesh. Here are seven practical tips for the effective use of photofunctionalization: Figures 13a & 13b: Mandibular images before (a) and after (b) implant placement. Four photofunctionalized implants were placed and immediately loaded with full-arch acrylic provisional (b). Figure 14: Panoramic x-ray image confirming successful osseointegration. 84 Winter 2014 Volume 29 Number 4
12 Funato/Tonotsuka/Murabe/Hirota/Ogawa 1. Photofunctionalization requires adequate conditioning (15 to 20 minutes for TheraBeam Affiny). Therefore, implants of appropriate diameter and length need to be selected prior to commencing surgery. 2. The use of one-step shorter implants (e.g., 10 mm instead of 11.5 mm) may be considered to make surgery less invasive due to improved osseointegration of the photofunctionalized implants. 3. When there is uncertainty about the size and length of implants to be used in the surgery, multiple potential implants should be photofunctionalized in preparation for the final decision. 4. The same number of implant drivers as implants need to be ready, to allow the implants to stand in the photo device (Fig 16). Figure 15: Presentation of the final prosthesis. 5. After photofunctionalization is complete, the implant and implant driver need to be handled and set in the handpiece with caution, and care should be taken not to drop the implant or make contact with unsterilized instruments or materials. 6. After photofunctionalization, the implants should be placed immediately (and certainly within 30 minutes) for maximal surface bioactivity. If the implants were stored without opening the photo device, the bioactivity appears to be maintained up to two hours. Therefore, if multiple implants are to be placed, the timing and sequence of implant placement and concomitant surgery need to be planned in advance. For example, if implants are to be placed in the maxilla and mandible with simultaneous GBR, photofunctionalization should be performed separately for the maxillary and mandibular implants. 7. Pay particular attention to the details of the fundamentals and principles of implant surgery. In particular, make sure that the implant site is filled with blood so that the photofunctionalized implant absorbs blood effectively and efficiently. Be sure to avoid contact of implants with saliva or contaminated tissues and fluids, which might dilute blood or cause biological and chemical contamination. Summary Ultraviolet light treatment of dental implants immediately prior to placement, or photofunctionalization, is a novel clinical tool with the potential to improve implant therapy. Photofunctionalization improves the surface properties of implant surfaces by removing hydrocarbons, regenerating hydrophilicity, and optimizing electrostatic properties. We first tested the effect of photofunctionalization to potentially enhance the Figure 16: Dental implants with an implant driver set on a removable metallic stand. The stand will be placed in the photo device for photofunctionalization. osteoconductivity of Ti mesh in an in vitro culture study using human osteoblasts. The results showed that the attachment, spreading behavior, adhesion, and function of osteoblasts were remarkably increased on photofunctionalized Ti mesh compared to untreated ones, suggesting the considerable enhancement of osteoconductivity by photofunctionalization. We then applied photofunctionalization to dental implants and Ti mesh in two complex clinical cases requiring simultaneous GBR, sinus elevation, immediate implant placement into the extraction socket, and esthetic consideration. The use of photofunctionalized implants and Ti mesh enabled more strategic and aggressive treatment planning and resulted in successful treatment outcomes with secure application of immediate and early loading protocols. The cases discussed here, in combination with the results from human cell study, help to show that photofunctionalization is a useful and effective tool for improving implant therapy and that, with the advent of this technology, novel avenues of treatment can be pursued and some clinical challenges overcome. Long-term controlled trials and/or histologic studies are warranted to verify that photofunctionalization is a clinically significant and beneficial therapy. Journal of Cosmetic Dentistry 85
13 References 1. Funato A, Yamada M, Ogawa T. Success rate, healing time, and implant stability of photofunctionalized dental implants. Int J Oral Maxillofacial Implants Sep-Oct;28(5): Funato A, Ogawa T. Photofunctionalized dental implants: a case series in compromised bone. Int J Oral and Maxillofacial Implants Nov-Dec;28(6): Suzuki S, Kobayashi H, Ogawa T. Implant stability change and osseointegration speed of immediately loaded photofunctionalized implants. Implant Dent Oct;22(5): Att W, Ogawa T. Biological aging of implant surfaces and their restoration with ultraviolet light treatment: a novel understanding of osseointegration. Int J Oral Maxillofacial Implants Jul- Aug;27(4): Lee JH, Ogawa T. The biological aging of titanium implants. Implant Dent Oct;21(5): Suzuki T, Hori N, Att W, Kubo K, Iwasa F, Ueno T, Maeda H, Ogawa T. Ultraviolet treatment overcomes time-related degrading bioactivity of titanium. Tissue Eng Part A Dec;15(12): Ikeda T, Hagiwara Y, Hirota M, Tabuchi M, Yamada M, Sugita Y, Igawa T. Effect of photofunctionalization on fluoride-treated nanofeatured titanium. J Biomater Appl Aug 28. [Epub ahead of print]. 15. Aita H, Att W, Ueno T, Yamada M, Hori N, Iwasa F, Tsukimura N, Ogawa T. Ultraviolet light-mediated photofunctionalization of titanium to promote human mesenchymal stem cell migration, attachment, proliferation and differentiation. Acta Biomater Oct;5(8): Ishikawa T, Salama M, Funato A, Kitajima H, Moroi H, Salama H, Garber D. Threedimensional bone and soft tissue requirements for optimizing esthetic results in compromised cases with multiple implants. Int J Periodontics Restorative Dent Oct;30(5): Funato A, Salama MA, Ishikawa T, Garber DA, Salama H. Timing, positioning, and sequential staging in esthetic implant therapy: a four-dimensional perspective. Int J Periodontics Restorative Dent Aug;27(4): Att W, Hori N, Takeuchi M, Ouyang J, Yang Y, Anpo M, Ogawa T. Time-dependent degradation of titanium osteoconductivity: an implication of biological aging of implant materials. Biomaterials Oct;30(29): Hori N, Att W, Ueno T, Sato N, Yamada M, Saruwatari L, Suzuki T, Ogawa T. Age-dependent degradation of the protein adsorption capacity of titanium. J Dent Res Jul;88(7): Aita H, Hori N, Takeuchi M, Suzuki T, Yamada M, Anpo M, Ogawa T. The effect of ultraviolet functionalization of titanium on integration with bone. Biomaterials Feb;30(6): Iwasa F, Hori N, Ueno T, Minamikawa H, Yamada M, Ogawa T. Enhancement of osteoblast adhesion to UV-photofunctionalized titanium via an electrostatic mechanism. Biomaterials Apr;31(10): Hori N, Ueno T, Suzuki T, Yamada M, Att W, Okada S, Ohno A, Aita H, Kimoto K, Ogawa T. Ultraviolet light treatment for the restoration of age-related degradation of titanium bioactivity. Int J Oral Maxillofacial Implants Jan;25(1): Pyo SW, Park YB, Moon HS, Lee JH, Ogawa T. Photofunctionalization enhances bone-implant contact, dynamics of interfacial osteogenesis, marginal bone seal, and removable torque value of implants: a dog jawbone study. Implant Dent Dec;22(6): Ohyama T, Uchida T, Shibuya N, Nakabayashi S, Ishigami T, Ogawa T. High bone-implant contact achieved by photofunctionalization to reduce periimplant stress: a three-dimensional finite element analysis. Implant Dent Feb;22(1): Funato A, Ishikawa T. 4D implant therapy: esthetic considerations for soft-tissue management. Tokyo: Quintessence Pub.; Salama M, Ishikawa T, Salama H, Funato A, Garber D. Advantages of the root submergence technique for pontic site development in esthetic implant therapy. Int J Periodontics Restorative Dent Dec;27(6): jcd Dr. Funato maintains a private practice in Kanazawa, Ishikawa, Japan. Dr. Tonotsuka maintains a private practice in Tokyo, Japan. Dr. Murabe maintains a private practice in Hitachinaka, Japan. Dr. Hirota is an associate professor, Department of Oral and Maxillofacial Surgery, Yokohama City University School of Medicine, Yokohama, Japan, where he also practices. Dr. Ogawa is a professor at The Weintraub Center for Reconstructive Biotechnology, Division of Advanced Prosthodontics, UCLA School of Dentistry, Los Angeles, California, where he also practices. Disclosures: The authors did not report any disclosures. 86 Winter 2014 Volume 29 Number 4
Photofunctionalization
 Photofunctionalization One and only technology to overcome the biological aging of titanium Scientific brochure of photofunctionalization Volume 1, Issue 1, 2013 published by Global Network for Photofunctionalized
Photofunctionalization One and only technology to overcome the biological aging of titanium Scientific brochure of photofunctionalization Volume 1, Issue 1, 2013 published by Global Network for Photofunctionalized
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
P hotofunctionalization of titanium
 IMPLANT DENTISTRY / VOLUME 22, NUMBER 5 2013 481 Implant Stability Change and Osseointegration Speed of Immediately Loaded Photofunctionalized Implants Senichi Suzuki, DDS, PhD,* Hiroyuki Kobayashi, MD,
IMPLANT DENTISTRY / VOLUME 22, NUMBER 5 2013 481 Implant Stability Change and Osseointegration Speed of Immediately Loaded Photofunctionalized Implants Senichi Suzuki, DDS, PhD,* Hiroyuki Kobayashi, MD,
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
MAIN LINE DENTAL IMPLANT CENTER
 1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
1257 Lancaster Ave Berwyn, PA 19312 Tel: 610-722-5542 CHIUN-LIN (STEVEN), LIU D.D.S., D.M.D. School of Dental Medicine CURRICULUM VITAE Summer, 2012 Education: 1987-1993 D.D.S. Kaohsiung Medical University
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
E. Richard Hughes, D.D.S.
 E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 [email protected] Diplomate,
E. Richard Hughes, D.D.S. Docket No. FDA-2012-N-0677 Blade Form Endosseous Dental Implants E. Richard Hughes, D.D.S. 46440 Benedict Dr.,# 201 Sterling, Va. 20164 USA 703-444-1152 [email protected] Diplomate,
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Foundation Revolutionary Bone Augmentation Material. Thinking ahead. Focused on life. Regional Partner
 Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
Foundation Revolutionary Bone Augmentation Material Thinking ahead. Focused on life. Regional Partner Stimulates New Bone Growth Foundation is a collagen-based, bone filling augmentation material for use
vitality meets bone volume around dental implants Straumann BoneCeramic
 vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
vitality meets bone volume around dental implants Straumann BoneCeramic The vitality you need around your implants Bone volume restoration and preservation for the desired esthetic outcome Image by PD
Ultraviolet (UV) light treatment of titanium implants. Success Rate, Healing Time, and Implant Stability of Photofunctionalized Dental Implants
 Success Rate, Healing Time, and Implant Stability of Photofunctionalized Dental Implants Akiyoshi Funato /Masahiro Yamada /Takahiro Ogawa Purpose: This is the first study to report the clinical outcomes
Success Rate, Healing Time, and Implant Stability of Photofunctionalized Dental Implants Akiyoshi Funato /Masahiro Yamada /Takahiro Ogawa Purpose: This is the first study to report the clinical outcomes
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
A Comprehensive Explanation
 Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
CAD/CAM technology supporting successful implant therapy
 CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
BICON DENTAL IMPLANTS
 BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide
 Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
Strong bone for beautiful teeth Patient Information I Bone reconstruction with Geistlich Bio-Oss and Geistlich Bio-Gide Contents Smiling is the most beautiful way to show your teeth 3 What are the causes
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Osseo-integrated Dental Implant Policy and Guidelines
 Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
What is a dental implant?
 Chicago Implants - Dr Ivan Valcarenghi - Dental Implants In our office, getting one or more dental implants involves two phases: the surgical and restorative phases. Most often, the surgical phase is performed
Chicago Implants - Dr Ivan Valcarenghi - Dental Implants In our office, getting one or more dental implants involves two phases: the surgical and restorative phases. Most often, the surgical phase is performed
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
Eastman Dental Hospital. Dental implants - general information for patients. Department of Restorative Dentistry
 Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Rehabilitation of a complex case with zirconium dental implants
 Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
Abutment fracture in a bridge supported by natural teeth and implants
 Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
Dr. Little received his doctorate degree in dentistry from UT Health at San Antonio Dental
 Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
Implant Solutions for the Implant Patient: Diagnosis and Treatment Planning for Predictable Results David Little, DDS 6961 U.S. Highway 87 East San Antonio, TX 78263 Phone: (210)648-4411 Fax: (210) 648-6498
A New Beginning with Dental Implants. A Guide to Understanding Your Treatment Options
 A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
Retrospective study on the survival rate of IBS implant
 Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Dental Bone Grafting Options. A review of bone grafting options for patients needing more bone to place dental implants
 Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
BioHorizons Education Programme 2015
 BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
DENTAL IMPLANT THERAPY
 DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
Treatment planning for the class 0, 1A, 1B dental arches
 Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
Single anterior tooth replacement: clinical approaches
 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software
 Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software XCPT Patient Engagement System was developed and engineered to combine scientific research relating to the brain s ability
Optimizing Referral Team Collaboration Using Dynamic Visual Communication Software XCPT Patient Engagement System was developed and engineered to combine scientific research relating to the brain s ability
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE
 IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
dental implants for tooth replacement be a confident you
 dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
dental implants for tooth replacement be a confident you smile big Anyone missing one or more teeth understands how tooth loss can make you feel uncomfortable about smiling or eating in public. You may
All-on-4 treatment concept with NobelSpeedy Groovy
 All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
In the Spring of 2010, the American Academy of Cosmetic
 Greetings to the members of the American Academy of Cosmetic Dentistry (AACD). As you know, a sisterhood agreement was concluded between the AACD and the Japan Academy of Esthetic Dentistry (JAED) at a
Greetings to the members of the American Academy of Cosmetic Dentistry (AACD). As you know, a sisterhood agreement was concluded between the AACD and the Japan Academy of Esthetic Dentistry (JAED) at a
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
INFUSE Bone Graft (rhbmp-2/acs)
 1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Dental Implant Restoration
 Dental Implant Restoration Principles and Procedures Stuart H. Jacobs Brian C. O Connell London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo,
Dental Implant Restoration Principles and Procedures Stuart H. Jacobs Brian C. O Connell London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo,
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration
 Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Retention of maxillary implant overdenture bars of different designs
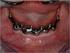 Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
forrest avenue d e n t a l c e n t r e
 Implant Treatment FAQ IMPLANT TREATMENT: FREQUENTLY ASKED QUESTIONS WHAT ARE DENTAL IMPLANTS? Dental implants are titanium rods that are surgically placed in your jaw bone which will subsequently support
Implant Treatment FAQ IMPLANT TREATMENT: FREQUENTLY ASKED QUESTIONS WHAT ARE DENTAL IMPLANTS? Dental implants are titanium rods that are surgically placed in your jaw bone which will subsequently support
USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016
 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 About the Program Implants
USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 USC Comprehensive Surgical and Restorative Implant Training Program in Hong Kong 2015-2016 About the Program Implants
The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment
 Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Renaissance of One-Piece Implants
 2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation
 Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
IMPLANTS IN FOCUS. Endosseous dental implant restorations PLANNING FOR IMPLANT RESTORATIONS
 IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
it will set at body temperature, and it will grow. UNIQUE FORMULATIONS
 BETTER BONE GRAFT FORMULATION. SUPERIOR BONE GRAFT HANDLING. When choosing a Demineralized Bone Matrix, remember that not all products are created equal. For excellent clinical performance and patient
BETTER BONE GRAFT FORMULATION. SUPERIOR BONE GRAFT HANDLING. When choosing a Demineralized Bone Matrix, remember that not all products are created equal. For excellent clinical performance and patient
Dental Implants and Esthetics
 Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Boston College, BS in Biology 1980-1984. University of Southern California, Doctor of Dental Surgery, DDS, 1990.
 CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION
 MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
While the prosthetic rehabilitation of
 Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
Restoring Mandibular Single Teeth with the Inclusive Tooth Replacement Solution Go online for in-depth content by Bradley C. Bockhorst, DMD While the prosthetic rehabilitation of full-arch cases provides
Ando A., Nakamura Y., Kanbara R., Kumano H., Miyata T., Masuda T., Ohno Y. and Tanaka Y.
 11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
BEST DENTAL ASSOCIATES / DRSTONEDDS.COM THE DENTAL IMPLANT GUIDE
 THE DENTAL IMPLANT GUIDE We specialize in the most advanced technologies in dental restoration, reconstruction and replacement. We d love to help you to improve your comfort, lifestyle, & confidence with
THE DENTAL IMPLANT GUIDE We specialize in the most advanced technologies in dental restoration, reconstruction and replacement. We d love to help you to improve your comfort, lifestyle, & confidence with
Removing fixed prostheses using the ATD automatic crown and bridge remover
 Removing fixed prostheses using the ATD automatic crown and bridge remover By Dr. Ian E. Shuman, Baltimore, MD. Information provided by J. Morita USA When removing cemented provisionals and final fixed
Removing fixed prostheses using the ATD automatic crown and bridge remover By Dr. Ian E. Shuman, Baltimore, MD. Information provided by J. Morita USA When removing cemented provisionals and final fixed
INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures
 INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures Dental Products Advisory Panel Committee Ed Chin, DPh Group Director, Regulatory Affairs Medtronic Spinal and Biologics 1 INFUSE Bone Graft
INFUSE Bone Graft Oral Maxillofacial Bone Grafting Procedures Dental Products Advisory Panel Committee Ed Chin, DPh Group Director, Regulatory Affairs Medtronic Spinal and Biologics 1 INFUSE Bone Graft
More than an implant. A sense of trust. Straumann Dental Implant System
 More than an implant. A sense of trust. Straumann Dental Implant System More than an implant. A sense of trust. Patients today are more aware of their options when it comes to tooth replacement. Partner
More than an implant. A sense of trust. Straumann Dental Implant System More than an implant. A sense of trust. Patients today are more aware of their options when it comes to tooth replacement. Partner
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
Smile Confidently With DIEM 2. Immediate Full Arch Rehabilitation
 Smile Confidently With DIEM 2 Immediate Full Arch Rehabilitation Immediate Full Arch Rehabilitation * Edentulism and failing dentition continue to be major health challenges affecting millions of people
Smile Confidently With DIEM 2 Immediate Full Arch Rehabilitation Immediate Full Arch Rehabilitation * Edentulism and failing dentition continue to be major health challenges affecting millions of people
Full Mouth Restoration with Screw-Retained Zirconia Bridges
 Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Full Mouth Restoration with Screw-Retained Zirconia Bridges A DENTIST-LAB RELATIONSHIP THAT WORKS Dentist: Steven P. Stern, DMD Windsor Dental Center New Windsor, NY Dental Laboratory: InnoDDS Dental Laboratory
Immediate Molar Implant Placement: A Private Practice Clinical Investigation. Abstract
 Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
Immediate Molar Implant Placement: A Private Practice Clinical Investigation Gargiulo et al Alphonse Gargiulo, DDS, MS 1 Thomas Manos, DDS, MS 2 Mark Kolozenski, DDS, MS 3 Alex Tzanos, DDS, MSD 3 Michael
Oral Plastic Surgery
 20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
20/20 TM Oral Plastic Surgery Hands-On Courses EDWARD P. ALLEN, DDS, PhD 20/20 Oral Plastic Surgery Advanced Techniques for Predictable Results Advanced surgical techniques in oral plastic surgery are
Periodontal Surgery. What Can I Expect? The word "periodontal" literally means around the tooth. Many factors, such as oral hygiene habits, genetics,
 The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
The word "periodontal" literally means around the tooth. Periodontal disease, also known as "gum disease," is a chronic bacterial infection that damages the gums and bone supporting the teeth. Left untreated,
Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report
 Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
Technology Breakthrough in Spinal Implants (Technical Insights)
 Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
Technology Breakthrough in Spinal Implants (Technical Insights) Biomaterial innovations is a growth factor for spinal implant market June 2014 Table of Contents Section Page Number Executive Summary 4
