To Eric, Victor, Lovisa and Gustav.
|
|
|
- Cynthia Powers
- 10 years ago
- Views:
Transcription
1
2
3 To Eric, Victor, Lovisa and Gustav.
4
5 List of Papers This thesis is based on the following papers, which are referred to in the text by their Roman numerals. I Nilsson C, Holmqvist M, Bergkvist L, Hedenfalk I, Lambe M, Fjällskog M-L (2011). Similarities and differences in the characteristics and primary treatment of breast cancer in men and women- a population based study (Sweden). Acta Oncologica, 2011;00:1-6 II Nilsson C, Johansson I, Ahlin C, Thorstenson S, Amini R-M, Holmqvist M, Bergkvist L, Hedenfalk I, Fjällskog M-L. Molecular subtypes of male breast cancer using alternative definitions and its prognostic impact (submitted) III Nilsson C, Koliadi A, Johansson I, Ahlin C, Thorstenson S, Bergkvist L, Hedenfalk I, Fjällskog M-L. High proliferation is associated with inferior outcome in male breast cancer patients (submitted) IV Johansson I, Nilsson C, Berglund P, Lauss M, Ringner M, Olsson H, Luts L, Sim E, Thorstenson S, Fjällskog M-L, Hedenfalk I (2012). Gene expression profiling of primary male breast cancers reveals two unique subgroups and identifies N- acetyltransferase-1 (NAT1) as a novel prognostic biomarker. Breast Cancer Research 2012, 14:R31 V Johansson I, Nilsson C, Berglund P, Strand C, Jönsson G, Staaf J, Ringer M, Nevanlinna H, Barkardottir R B, Borg Å, Olsson H, Luts L, Fjällskog M-L, Hedenfalk I (2011). High-resolution genomic profiling of male breast cancer reveals differences hidden behind the similarities with female breast cancer. Breast Cancer Research and Treatment 2011;129(3): Reprints were made with permission from the respective publishers.
6
7 Contents Background Introduction The male breast Epidemiology Risk factors and genetics Diagnosis Outcome of MBC compared with FBC Treatment Surgery Radiotherapy Endocrine treatment Chemotherapy Prognostic and predictive factors Nodal status and tumor size Histological grade Estrogen and progesterone receptor HER Array-based analysis Proliferation and the cell cycle Proliferation markers in FBC Proliferation markers in MBC Aims of the thesis Materials Paper I Paper II-III Paper IV-V Methods Paper I Paper II-III Construction of TMA block Immunohistochemical staining Evaluation of immunoreactivity scores Paper IV Paper V... 33
8 Statistics Paper I Paper II-III Paper IV-V Results Paper I Paper II Paper III Paper IV Paper V General discussion General conclusions Future perspectives Sammanfattning (Brief summary in Swedish) Delarbete I Delarbete II Delarbete III Delarbete IV Delarbete V Acknowledgements References... 59
9 Abbreviations acgh Array CGH AI Aromatase inhibitor AR Androgen receptor BAC Bacterial artificial chromosome BPH Benign prostate hyperplasia Cdk Cyclin dependent kinase CGH Comparative genomic hybridization CK Cytokeratin kinase CNA Copy number alterations DAVID Database for annotation, visualization, and integrated discovery DMFS Distant metastasis free survival DNA Deoxyribonucleic acid EGFR Epidermal growth factor receptor ER Estrogen receptor FISH Fluorescence in situ hybridization FBC Female breast cancer FGA Fraction of genome altered GEX Gene expression GISTIC Genomic identification of significant targets of cancer HCL Hierarchical clustering HER2 Human epidermal growth factor receptor 2 HLA Human leukocyte antigen HR Hazard ratio IHC Immunohistochemistry MBC Male breast cancer NAT1 N-acetyltransferase-1 NHG Nottingham histological grade PR Progesterone receptor RNA Ribonucleic acid SAM Significance analysis of microarrays SISH Silver in situ hybridization TMA Tissue microarray TNM Tumor size, node, metastasis
10 10
11 Background Introduction Male breast cancer (MBC) is a rare disease accounting for <1% of all breast cancer. Current knowledge about MBC is based mainly on population-based studies or descriptive studies that assess a limited number of patients. The optimal treatment for MBC is presently not known and the general recommendation is to use current guidelines for female breast cancer (FBC). Some differences regarding clinicopathological characteristics have been identified but it has not yet been established whether the prognostic and predictive factors used in FBC have the same impact in MBC. Our aim with this research project was to further examine possible differences in clinicopathological characteristics, treatment modalities and outcome in male and female breast cancer. In addition, we also wished to characterize MBC by using immunohistochemistry and molecular array techniques to identify factors with prognostic and/or predictive value which might be of importance for treatment decisions. The male breast The breast is morphologically similar in boys and girls until puberty and consists of small ductal structures in a fibroblastic stroma. The walls of the ducts consist of two layers of epithelial cells; basal (myo-epithelial cells) and luminal (epithelial) cells 1. In females the breast continues to develop during puberty with the proliferation of end-bud-like structures into terminal duct lobular units, which are the functional units of the breast. After puberty, the female breast continue to undergo developmental changes during the menstrual cycle and pregnancy and this constant remodeling under the influence of hormones and growth factors is thought to make the female breast particularly susceptible to carcinogenic events. In males no further development normally occurs after childhood, leaving the male breast in a rudimentary state. The most common abnormality in the male breast is gynecomastia, defined as an abnormal overgrowth of the breast tissue most often seen during adolescence or in middle-aged men. The condition is benign and often reversible. The histological appearance in gynecomastia is characterized by an increase in the number of ducts together with an increment in stromal cellularity and vascularity. Identified risk factors for gynecomastia 11
12 are different hormonal imbalances, which demonstrate that the male breast like the female breast can proliferate under the influence of hormonal alterations. The male breast does not normally develop lobular units 2. Epidemiology The incidence of MBC varies greatly worldwide, ranging from 5-15% of all breast cancer in certain African countries to less than 1% in North America and Europe. The higher incidence in certain African countries has been explained by infectious diseases that cause liver damage, which in turn leads to higher estrogen levels 3. In the Nordic countries, breast cancer accounts for 0.2% of all invasive cancer in men, with approximately 100 men diagnosed with the disease every year compared with 17, 000 women 4. A slight increase in age-standardized incidence has been reported 5, 6. In MBC, a unimodal age distribution is seen, with a peak incidence in the sixth decade of life 7. The mean age at diagnosis occurs approximately five years later than that for FBC. The mortality rate seems to be stable in MBC, which is in contrast to the decline observed in FBC and due to improved diagnostic procedures and treatment methods 8. Risk factors and genetics In several studies, obesity has been identified as a risk factor for MBC Other factors which have been associated with an increased risk are: physical inactivity, bone fractures after the age of 45, gynecomastia, orchitis/epididymitis, liver cirrhosis and radiation exposure Many of these risk factors are associated with an altered ratio of estrogen/androgen, resulting in a relative excess of estrogen. There are also case reports describing men that have developed breast cancer after treatment with exogenous estrogen, such as in prostate cancer and in transsexuals. An association between benign prostate hyperplasia (BPH) and MBC has also been discussed; however, it is unclear whether similar changes in sex hormone balance could predispose for both conditions or if treatment with finasteride in BPH could increase the risk of breast cancer 12. Genetic predisposition is considered to be of greater importance in MBC, compared with FBC. Approximately 20% of all MBC patients report a firstdegree relative with breast cancer or ovarian cancer 3, 13. BRCA2 mutations have been identified in 4-40% of MBC patients, whereas BRCA1 mutations are infrequent. The estimated risk for male carriers of BRCA 2 of developing breast cancer is 5-10%, whereas the risk for BRCA1 carriers is 1-5% 13, 14. CHEK2, a cell cycle checkpoint kinase, has also been suggested to play a role in the development of MBC 3, 14. The most well-known single condition 12
13 predisposing for MBC is Klinefelter s syndrome (carrier type XXY) with a relative risk of developing breast cancer 15, 16. Diagnosis The most common clinical symptom of MBC is a painless lump in the breast. The tumors are most often located in the retroareolar area and nipple involvement is a relatively early event, with retraction described in 7-9% and discharge in 2-6% of cases 3, 17. The recommended diagnostic work-up is a combination of clinical examination, mammography and/or ultrasonography and histopathological verification with fine-needle aspiration or core biopsy 3. Mammography is a useful tool in the diagnostic procedure with an estimated sensitivity of 92% and a specificity of 90% 18. At diagnosis all breast cancer tumors are described according to the TNM staging system. The system describes tumor size (T), lymph node status (N), and distant metastases (M), and has definitions for clinical and pathological staging. Clinical staging is based on information before surgery, encompassing the clinical examination and radiological imaging. Pathological TNM staging is denoted by the prefix p, for example pt1n0m0, and is based on the histopathologic examination which reveals additional information, especially in describing lymph node status (Table 1). Based on the three parameters in the TNM system, breast tumors are also grouped into different stages 19 (Table 2). Table 1. TNM classification (7 th edition) Tis In situ T1 20 mm T2 >20-50 mm T3 >50mm T4 Chest wall/skin ulceration, skin nodules, inflammatory N1 Movable axillary pn1 1-3 axillary nodes N2 N3 M0 M1 Fixed axillary or internal mammary nodes clinically apparent Supra/infraclavicular nodes or internal mammary together with axillary nodes No distant metastasis Distant metastasis pn2 pn3 4-9 axillary nodes 10 axillary nodes or infraclavicular nodes 13
14 Table 2. Stage classification based on the TNM system Stage T N M Stage 0 Tis N0 M0 Stage I T1 N0 M0 Stage IIA T0-T1 N1 M0 T2 N0 M0 Stage IIB T2 N1 M0 T3 N0 M0 Stage IIIA T0-T2 N2 M0 T3 N1-N2 M0 Stage IIIB T4 N0-N2 M0 Stage IIIC Any N3 M0 Stage IV Any Any M1 MBC has often been reported to be diagnosed at a more advanced stage than FBC, with positive axillary lymph nodes reported in 40-50% and a high proportion of tumors classified as T4 because of skin or nipple involvement. The nipple involvement seen in MBC patients is a result of direct tumor extension to the epidermis and is not comparable to Paget s disease of the nipple, which is most often associated with cancer in situ. Nipple involvement seems to be associated with a high risk of lymph node metastasis 20. It has been hypothesized that the association between tumor size and the presence of lymph node metastases is different in male breast cancer, where the smaller anatomical distances between breast parenchyma and skin and /or chest wall could possibly increase the risk of regional metastases 21, 22. In line with this, studies in MBC have reported a high rate of axillary nodal involvement even in small tumors (pt1) 17, 20. The most common sites for metastases in advanced disease are the skeleton and lungs 17. Invasive breast tumors are classified according to histological appearance. In FBC, the most common histology is ductal carcinoma (75%) followed by lobular carcinoma (5-15%) 23.The predominant histology in MBC tumors is invasive ductal carcinoma which is described in >90 % of cases. Lobular carcinoma is infrequent, probably due to the fact that the male breast tissue only differentiates into lobules when excessive levels of endogenous or exogenous estrogen are present. Isolated in situ cancers account for approximately 5% of MBC tumors 17,
15 Outcome of MBC compared with FBC MBC has in certain studies been described to resemble post-menopausal FBC, with a more indolent tumor behavior 3, 7. Other reports indicate that hormone-receptor-positive MBC tumors are often of higher grade and proliferation, suggesting a more aggressive behavior 8, 25. Comparisons of outcome in cases of male and female breast cancer are contradictory. Several studies report a poorer overall survival for MBC patients when compared with FBC 5, 26. However, this could be attributed to older age and the increased mortality of men in the general population. Disease-specific survival and relative survival have been evaluated in certain studies. In one register study, MBC patients had a statistically significant poorer breast cancer specific survival at longer follow up 22, whereas no difference in disease- specific survival could be seen in other smaller age- and stage matched series 27, 28. A recent population-based multi-institutional study, comparing men and women diagnosed with breast cancer over the last 40 years, concluded that MBC patients had a more advanced disease and higher age at diagnosis. The male patients underwent surgery and/or radiotherapy less often, but there were no differences in the administration of chemotherapy or endocrine treatment between the genders. MBC patients had a poorer overall and relative survival in an overall comparison. After adjusting for multiple parameters including stage, age and treatment, however, the male group had a better relative survival 29. Two other population-based studies could not prove any difference in relative survival between male and female breast cancer patients, although one of them demonstrated a trend towards poorer survival in men 5, 30. Treatment Surgery Surgery is the most important treatment modality in the management of localized breast cancer. In MBC, modified radical mastectomy is considered most feasible in the majority of cases because of the paucity of breast tissue together with the predominantly central location of tumors 13, 14, 22. However, breast conservative surgery followed by radiotherapy is a feasible option 31. Axillary lymph node involvement is a strong prognostic factor and should always be evaluated in invasive breast cancer. Two different procedures are used for determining the axillary nodal status; axillary dissection or sentinel lymph node biopsy. The sentinel node is by definition the first lymph node to receive lymphatic drainage from the tumor, and in FBC, several studies have shown that sentinel node biopsy is reliable in predicting axillary lymph 15
16 node status 32, 33. Sentinel node biopsy decreases the comorbidity related to axillary surgery and is currently the standard procedure in a majority of FBC patients with a clinically normal axilla. Sentinel node biopsy has been evaluated in small series in MBC and appears to be a reliable method. 34, 35. In one of the largest series, 78 men with a clinically negative axilla underwent sentinel node biopsy. Biopsy was successful in 76 of 78 men. In 3 patients (8 %) with a negative SN, a positive non-sn was found. No axillary recurrences were seen after a median follow-up of 28 months. Males are considered to have the same risk of comorbidity after full axillary dissection as females and SN is, therefore, the recommended method 13, 35. Radiotherapy Postoperative radiotherapy after breast-conserving surgery or mastectomy reduces the risk of recurrence and improves overall survival in FBC 36. Radiotherapy is recommended after breast-conserving surgery and in all patients with >3 positive lymph nodes, regardless of the method of surgery 36. Post-mastectomy radiotherapy is recommended in the following situations; tumors >5 cm, uncertain surgical margins and skin involvement. Some studies also demonstrate a benefit from postoperative radiotherapy in patients with 1-3 positive lymph nodes 37. The use of postoperative radiotherapy in MBC has been described in a few retrospective studies. In one of the largest series, 85% of patients received postoperative radiotherapy. A rate of 1.8% chest recurrence and 5.3% nodal recurrence was observed, which is considered low and suggests a benefit from radiotherapy 17. In some earlier studies, a higher risk for local recurrence was reported and it was hypothesized that this could be explained by the smaller anatomical distances between breast tissue and skin/ chest wall 38. Consequently, some authors have suggested post-mastectomy radiotherapy on broader indications in MBC (tumors >1 cm) 39. However, in a study evaluating outcome in MBC patients who had been treated with mastectomy without radiotherapy, the risk of loco-regional recurrence was low and the recommendation was to follow the same indications as in FBC 40. This is supported by a study comparing male and female breast cancer patients treated with mastectomy, where no differences in the loco-regional relapse-free survival rates after radiotherapy was observed 41. Endocrine treatment A majority of MBC tumors express estrogen receptors (ER) and/or progesterone receptors (PR), and endocrine treatment is considered an important part of the treatment. Historically, different endocrine ablative treatments such as orchidectomy were used. Today, tamoxifen is considered 16
17 to be the first choice in the adjuvant and metastatic setting. There are no prospective studies evaluating endocrine treatment in MBC. Some retrospective reports have demonstrated a significantly improved outcome for patients administered adjuvant tamoxifen 17, 42. In metastatic disease, response rates of 32-75% with different endocrine treatments have been described 3. On the other hand, other studies have described an inferior survival in hormone receptor positive MBC cases when compared with FBC patients, despite similar endocrine treatment practices. Furthermore, it has been suggested that ER do not have the same function in MBC as in FBC and that the benefit achieved with tamoxifen is uncertain 43. Knowledge about potential side-effects produced by endocrine treatment in MBC patients is scarce. The role of aromatase inhibitors (AIs) in MBC is unclear. In men, approximately 80% of circulating estrogens are produced from peripheral aromatization of testicular and adrenal androgens with the remaining 20% being derived from direct testicular production. AIs do not affect the estrogen production in the testes and it is, therefore, recommended to combine this treatment with surgical or medical orchidectomy 3, 22. However, some case reports have described objective responses after AI single treatment in the metastatic setting. In line with this, a small study (n=15) examining serum levels of estradiol in men on treatment with AI, reported that some patients with a total and partial response displayed corresponding low levels of estradiol in their serum samples. 44. Chemotherapy To date, only one prospective evaluation of adjuvant chemotherapy in MBC is available. Thirty-one MBC patients with node positive disease were enrolled in a study in which adjuvant CMF (cyclophosphamide, methotrexate, and fluorouracil) was administered. Compared with historical controls, a benefit from the treatment was suggested. However, diseasespecific survival could not be evaluated since the cause of death was not known in in all cases. Furthermore, the chemotherapy regimen administered is not considered to be standard treatment today 45. Some additional small retrospective series suggest a benefit from adjuvant chemotherapy, although no statistically significant results have been demonstrated, which may be explained by the small patient samples 46, 47. The general recommendation today is that male patients should be offered chemotherapy according to the guidelines recommended for FBC patients 14,
18 Prognostic and predictive factors In FBC, significant improvements in disease-free and overall survival have been achieved by continuous improvements in diagnostic and treatment strategies. A majority of patients who undergo surgery for localized breast cancer are offered adjuvant radiation therapy and/or systemic treatment with the aim of decreasing the risk of breast cancer recurrence. Prognostic and predictive factors are used in order to identify patients with a higher risk for recurrence and to select the most appropriate adjuvant treatment strategy for each patient. Prognostic factors are factors that predict outcome independently of treatment (or with standard treatment), whereas predictive factors predict response to a specific treatment. Established prognostic factors in FBC are age, lymph node status, tumor size, histologic grade, PR and human epidermal growth factor 2 (HER2) status According to some guidelines, Ki-67 is considered to have prognostic value and can also have a role in indicating the potential benefit of chemotherapy 54. The use of molecular gene expression analysis as a prognostic tool in clinical practice is still under debate but is considered to provide additional information in FBC patients with hormone-sensitive, lymph node negative tumors 53. ER and HER2 are also predictive factors, used to identify patients who might benefit from endocrine treatment (tamoxifen and AIs) and agents directed against the HER2 receptor, respectively 52. Due to the rarity of MBC there are only a few previous studies that aim at evaluating these prognostic and predictive factors in MBC, and today it is unclear whether adjuvant treatment strategies recommended for FBC patients are applicable in MBC patients. Nodal status and tumor size In a register study based on 2,537 MBC patients, tumor size >20 and positive lymph node status were independently associated with poorer survival 5. In another analysis on >400 cases of MBC, nodal status but not tumor size were independently associated with increased risk for metastatic disease 17. The prognostic impact of positive nodal status seems to be at least equally negative in male as in FBC 7, 55. Histological grade In a study comparing male and female breast cancer, MBC was more often than FBC classified as low grade, thus indicating a more indolent growth pattern 7. However, in other studies, the contrary has been reported 8, 21. In a recent study, high tumor grade and lymph node status were the only risk factors for metastatic disease in a multivariate analysis 17. Other studies indicate that grade is not an independent prognostic factor 5. 18
19 Estrogen and progesterone receptor Most studies report that MBC tumors express ER and PR to a greater extent than FBC (80-90% versus (vs.) 75% and 73-81% vs. 65%, respectively) 13, 14, 17. Some studies indicate that ER positivity is associated with a better overall survival 24, whereas other series could not find any prognostic value with ER and/ or PR status 5. The predictive and/ or prognostic values of these parameters have not been confirmed in prospective studies. HER2 HER2 is a member of the transmembrane epidermal growth factor family (EGFR) with the corresponding gene on chromosome 17. Overexpression and amplification are seen in 11-30% in FBC and correlate with a poorer prognosis 23, 56. HER2 status can be determined with two different methods; immunohistochemical staining for evaluation of protein expression or in situ hybridization for evaluation of gene copy numbers. Different methods and arrays are used for HER2 testing, but in general, IHC staining 3+ (a uniform and intense membranous positivity in more than 30% of the tumor cells) or amplification with 6 copies of the HER2 gene or a ratio of HER2 gene signals/chromosome 17 signals exceeding 2.2 are all considered as HER2 positive. Different HER2 directed therapies have become a cornerstone in the treatment of HER2 positive patients. Trastuzumab is a monoclonal antibody that binds to the extracellular domain of HER2 and has been demonstrated to improve response rate, time to progression and overall survival when used in combination with chemotherapy or endocrine treatment and is today routinely used in the adjuvant and metastatic setting in HER2 positive patients Additional HER2 targeted therapies have demonstrated improved time to progression in HER2 positive patients with metastatic disease 60, 61. In MBC, the prognostic or predictive value of HER2 is unclear. Studies examining the prevalence of HER2 overexpression in MBC have shown highly varying results, with HER2 expression present in 0-37% and amplification in 0-11% of patients 62, 63. Two of the largest series, with 129 and 99 evaluable patients, demonstrated an overexpression in 4 and 15 % of patients, respectively 63, 64. The prognostic and/or the predictive values of HER2 in MBC have not been examined in the referred studies. Array-based analysis The genome, which is equivalent to the DNA, encompasses the genetic information of the cell. The DNA molecule is built up of nucleotides or bases in two complementary strands, and is densely packed into chromosomes (Figure 1). All cancer arises as a result of accumulated changes, i.e. 19
20 mutations, in the DNA sequence of the genomes in the cancer cells. These mutations range from single nucleotide substitutions to quantitative and structural changes of larger chromosome regions 65. The genome contains segments of DNA which encode different genes. Genes are transferred to messenger RNA (mrna) in a process called transcription. The mrna molecules are thereafter translated to form proteins, the functional molecules and main building blocks of the cells (Figure 2). The difference between various cell types is mainly due to the different subsets of genes expressed in each cell type. Figure 1. DNA structure. Figure 2. Protein synthesis. synthesis 20
21 Gene expression (GEX) profiling is a method of determining which genes are active in a specific cell population. The activity of the genes can be detected by measuring mrna levels. In several cancer entities, tumor subgroups with distinct gene expression patterns have been identified, probably reflecting basic differences in the cell biology of tumors 66, 67. Normal cells contain two copies of each chromosome. By studying alterations of the chromosomal copy number (Copy Number Alterations (CNA)) in cancer cells and comparing these genomic profiles to normal cells, information about the genes involved in cancer development and progression can be achieved. Additionally, the different patterns of DNA alterations can give information about the underlying mechanisms of genomic instability 68. Comparative Genomic Hybridization (CGH) is a method used for analyzing CNA. GEX or CGH can be examined with microarray based technologies, by which thousands of genes or CNAs can be analyzed at the same time. There are different types of microarrays, but typically a microarray is built up of thousands of fragments of DNA molecules or oligonucleotides (spots) printed on a solid substrate, for example a glass slide. One common application is to compare the gene expression levels in two different samples, for example reference sample and tumor sample. From each sample, RNA is extracted and labeled with fluorescent dyes (green for reference sample and red for tumor sample). Samples are thereafter hybridized onto the microarray and, by analyzing the fluorescence intensities and colors for each spot, the relative expression level of the genes in the tumor sample can be estimated. For CGH, overlapping (tiling) bacterial artificial chromosomes (BAC) are often used for the construction of whole genome arrays with a high degree of resolution. Reference and tumor sample are co-hybridized onto the array and by analyzing the fluorescence intensities, the chromosomes in the tumor are compared with normal chromosomes, and gains and losses can be detected. A microarray experiment produces a very large amount of complex raw data that need to be processed by different computational and statistical methods in order to obtain a comprehensive picture of the gene expression patterns. In FBC, it has been found that the classification of tumors based on gene expression patterns is of prognostic importance. In the primary studies, a set of genes was identified which consisted of genes which varied significantly between different tumors but with less variation in paired samples from the same patients, the so-called intrinsic gene set. Based on this gene set, FBC can be classified into 5 different subtypes, viz. luminal A and B, basal-like, HER2-like and normal-like. The diversity between different subtypes is largely driven by the expression of ER- related, proliferation-related and HER2-related genes 69, 70. The subtypes can broadly be characterized as follows: Luminal A type : high expression of ER and ER-related genes 21
22 Luminal type B: expression of ER-related genes together with proliferation-related genes Basal-like : low expression of ER, PR and HER2, together with expression of basal cytokeratins HER2-type : expression of HER2 and related genes Normal-like: expression of genes seen in adipose and other non-epithelial tissue. The most important finding is that ER positive and ER negative breast cancers are fundamentally different diseases on the molecular level, with the greatest separation between luminal and basal-like tumors. Luminal tumors, which are clinically ER positive, are characterized by a high expression of genes expressed by luminal (epithelial) cells, whereas basal-like tumors demonstrate gene patterns seen in basal (myo-epitelial) cells 70. Comparisons between the subtypes have demonstrated significant differences in recurrence free survival and overall survival, with the basal-like and HER2-like groups having the poorest outcome. Significant differences were also seen between the hormone- receptor positive groups, luminal A and B. One of the main challenges in clinical oncology is to distinguish between tumors with high or low risks of recurrence, in order to more specifically identify those patients in need of more intensive treatment and concurrently identify patients in whom it is safe to omit adjuvant systemic treatment with potential harmful side-effects. Gene arrays mirror the heterogeneity of breast cancer tumors and may more accurately describe the tumors clinical behavior compared with the traditional clinicopathological prognostic factors. Gene array profiles have been developed for the prediction of outcome in specified subsets of FBC patients. A majority of these profiles are applicable in patients with hormone receptor positive and lymph node negative disease and have, in this context, demonstrated additional prognostic information when compared with clinicopathological parameters. A unifying characteristic of these profiles is a high expression of proliferation-related genes 71. Two of the most validated, commercially available, gene profiles are the 70 gene profile (Mammaprint) and the 21-gene recurrence score (Oncotype DX). The 70-gene profile was identified in a group of young (<55 years) and primarily node-negative women. The genes included are involved in the cell cycle, invasion and metastasis, angiogenesis and signal transduction 72. The 21-gene recurrence score was developed for prognostication in hormone receptor positive, node- negative patients. Of the 21 genes, 16 are tumor related with the main emphasis on proliferation 73. FBC tumors have also been classified by array CGH (acgh), and different genomic sub-groups have been identified, viz. luminal simple, luminal complex, basal complex, amplifier, 17q12 and mixed. The groups demonstrate different tumor biological features and clinical behavior and four of the subgroups (luminal simple, luminal complex, basal complex, 17q12) demonstrate clear similarities with the gene expression subgroups
23 Today, large-scale subtyping using array-based techniques on paraffin embedded tumor tissue is not feasible due to its high costs. As an alternative, combinations of immunohistochemical (IHC) markers have been identified, broadly matching the different GEX subtypes. One of the most commonly used definition for IHC subtypes are : luminal A (ER+ and/or PR+, HER2-), luminal B (ER+ and/or PR+, HER2+), core basal-like (ER-, PR-, HER2-, CK5/6 positive and/or EGFR+), HER2-like (ER-, PR-, HER2+) and unclassified (negative for all 5 markers) 75, 76. Other definitions use grade or proliferation markers in addition to hormone status and HER2 status to better differentiate between the luminal groups 77, 78. MBC tumors have previously not been classified into subtypes by GEX arrays or high resolution acgh. In one study, gene expression analysis was used to compare male and female breast tumors with similar clinicopathological features. Differences in gene expression were found, possibly indicating different pathways for tumor progression and treatment response in MBC compared with FBC 79. On the contrary, a small study using chromosomal CGH in MBC revealed the same patterns of chromosomal imbalances as in FBC, suggesting similar genetic events behind tumor progression in male and female breast cancer 80. However, chromosomal CGH can only detect larger chromosomal aberrations. Immunohistochemical characterization of MBC tumors indicates that luminal A is the most common subtype (seen in 75-98% of cases) followed by luminal B (0-21%). A very small subset of tumors in performed studies have been classified as basal-like, and the HER2-like subtype seems to be even more infrequent The prognostic relevance of the different subtypes has not been evaluated, due to a lack of outcome data. Proliferation and the cell cycle A key step in tumor growth is the cells capacity to proliferate, i.e. to duplicate and divide. Proliferation is driven by the cell cycle, which consists of a precisely defined set of phases; gap1 (G1); synthesis (S); gap2 (G2); mitosis (M) and the quiescent phase (G0) (Figure 3). In the G1 phase, the cells are prepared for DNA synthesis, which occurs during the S-phase. In G2, cells grow before entering the M-phase, in which mitosis takes place. Nondividing cells remain in G0. The different steps of the cell cycle are executed by cyclin-dependent kinases (CDK) which, in turn are, controlled by changes in the availability and levels of the different cyclins (Figure 4). This complex system is also regulated by CDK inhibitors. In tumor cells, different steps of the cell cycle can be affected leading to a dysregulated cell cycle process and uncontrolled proliferation. 23
24 The prognostic and predictive value of cyclins and other proliferation markers have been investigated by looking at gene alterations and/or the corresponding protein product. Figure 3. The cell cycle. The figure illustrates how each type of cyclin pairs with a specific cyclin-dependent kinase and in which phase the complexes are active. Adapted from The Biology of Cancer, Robert A. Weinberg, Figure 4. Cyclic changes in the availability and levels of the different cyclins Proliferation markers in FBC In recent years, there has arisen a renewed interest in proliferation markers, partly explained by the increasing interest in molecular subtyping. As previously mentioned, proliferation genes are important in the differentiation 24
25 between the molecular subtypes. In the commercially available 21-gene recurrence score, Ki-67 and cyclin B are two of 16 tumor-related genes. However, the utility of gene arrays is limited by high costs and several studies suggest that proliferation factors evaluated by IHC may provide similar prognostic information 84, 85. Protein overexpression of cyclins and the proliferation marker Ki-67 can be evaluated by IHC and several studies have shown that the overexpression of Ki-67, cyclin A, cyclin B and cyclin E is prognostic of a poorer outcome in FBC patients The Ki-67 antibody binds to a nuclear antigen present in all phases of the cell cycle except the quiescent phase (G0) and is, as such, a marker of proliferating cells. Initially, the Ki-67 antibody could only be used on fresh or frozen tissue, which reduced its clinical usefulness. MIB1 is an equivalent antibody developed for the evaluation on paraffin embedded tissue. Studies in FBC have demonstrated an association between high levels of Ki-67 expression and a poorer outcome 92. The expression level defining high proliferating tumor have varied from 5-34%, with 10 and 20% as the most frequently used cut-offs 88. In the St Gallen consensus conference 2011, the recommended cut-off was specified as 14% 93. Cyclin A is a protein which increases in early S-phase and decreases during mitosis. Several studies in FBC have demonstrated that the overexpression of cyclin A can predict recurrence and breast cancer death 87, 89. In a study evaluating Ki-67 and cyclin A in the same patient cohort, it was suggested that cyclin A was a stronger prognostic factor than Ki Furthermore, it has been indicated that cyclin A expression is a stronger prognostic factor in ER positive patients 87. Cyclin B increases at the beginning of the S-phase and reaches its maximum during mitosis. Overexpression of Cyclin B in early FBC is predictive of poorer outcome 90, 94, 95. It has been shown that Cyclin B is associated with tumor grade and HER2, but does not seem to correlate with tumor size 95. Cyclin B overexpression has been demonstrated more often in luminal B and basal-like FBC 86. Cyclin E regulates the progression of the G1 phase and the entry into the S-phase. Overexpression of cyclin E1 protein in FBC has been associated with a poorer outcome in several retrospective studies. There seems to be a correlation between cyclin E and high tumor grade or ER-negativity. High cyclin E expression has also been reported to be predictive of resistance to tamoxifen 96. The D-type cyclins are mainly controlled by extracellular signals and have a role in the G1 /S transition 97. There are at least three different cyclin D proteins, of which cyclin D1 has been most extensively studied but has produced contradictory results. Cyclin D1 is encoded by the gene CCND1 but amplification of the gene does not always seem to correspond with an overexpression of the protein 98. Overexpression of cyclin D1 appears to promote cell proliferation by binding to specific cyclin-dependent kinases. It also 25
26 seems to act independent of Cdks by acting as a co-factor for the ER-α. Cyclin D1 protein overexpression has demonstrated variable results in predicting breast cancer outcome and does not seem to be a useful prognostic factor in FBC 99. Tamoxifen exerts its effect by blocking ER-α and certain studies suggest that cyclin D1 can have a predictive role, with overexpression linked to tamoxifen resistance 100, 101. However, many of the referred studies are retrospective and with heterogeneous study populations, thus making the interpretation of data more difficult. In addition, there has been a lack of consensus regarding IHC staining methodology, scoring and cut-off levels. As a consequence, only KI-67 is today recommended for use in routine clinical practice 93, 102. The other proliferation markers have yet to be validated in further studies. Proliferation markers in MBC Ki-67 is the most studied proliferation marker in MBC but results are inconclusive. Some studies indicate an association between high levels of Ki67 expression and a poorer outcome, whereas other studies fail to demonstrate any prognostic importance 25, 103, 104. A few small series have examined the prognostic value of Cyclin D1 in MBC, but results are contradictory 64, 103, 105. The prevalence of CCND1 amplification and cyclin D1 expression was examined by Bärlund et al, and revealed CCND1 amplification in 12% and protein overexpression in 63% of cases. However, due to a lack of outcome data, the prognostic significance of cyclin D1 could not be evaluated 64. To date and to our knowledge, other cyclins have not been investigated in MBC. As previously described, MBC tumors express hormone receptors to a great extent and tamoxifen is often the recommended adjuvant treatment. In line with data presented in FBC, it is of interest to examine whether cyclin D1 could be predictive of tamoxifen resistance in MBC. In summary, information about the molecular biology in MBC comes from small series, with only a few studies having more than 100 cases. Different methodologies have been used as well as different cut- off points, in order to achieve what has been considered a positive result. All in all, this leads to a great inconsistency between studies. Furthermore, in a majority of studies, the prognostic value of different markers has been difficult to assess because of small patient samples and a lack of outcome data. 26
27 Aims of the thesis The aim of this study was to investigate whether MBC differs from FBC. If this is the case, it could have potential implications for the clinical management of male breast cancer. In the first project, male and female breast cancers were compared with regard to treatment and outcome. In the following studies MBC tumors were characterized using IHC and molecular array techniques to evaluate the prognostic impact of clinicopathological factors and to learn more about the tumor biology background. The specific aims were: Paper I: To investigate whether there were any differences in adjuvant treatment and outcome in MBC and FBC patients. Paper II: To evaluate the prevalence and prognostic impact of routinely used immunohistochemical markers in MBC. Furthermore, to classify into molecular subtypes using IHC markers according to alternative definitions and to evaluate their prognostic impact. Paper III: To evaluate the prevalence and prognostic value of proliferation markers in MBC. Paper IV: To characterize MBC tumors on the transcriptional level, to classify into comprehensive subgroups and to compare identified subgroups with established subgroups in FBC. Paper V: To characterize MBC on the genomic level using high resolution acgh, compare with FBC and, furthermore, to investigate whether the genomic subtypes in MBC have prognostic value. 27
28 Materials Paper I All men diagnosed with invasive breast cancer (n=99) in the Uppsala-Örebro region between the years were identified and data retrieved from the Regional Breast Cancer Register. The same register was used for the random sampling of four FBC patients for each MBC patient. The Regional Breast Cancer Register has a high level of completeness and a high level of agreement as regards data on primary treatment retrieved from patients files 106. Paper II-III The National Cancer Register was used to identify male patients diagnosed with breast cancer between the years 1990 and 2007 in two regions of Sweden, encompassing a population of 1.70 (Lund region) and 1.96 million people (Uppsala-Örebro region), respectively. In the Lund region, 131 patients and in Uppsala-Örebro, 131 patients were identified. All patient charts were reviewed and accessible paraffin-embedded tumor blocks collected. Patients with in situ cancer (Uppsala-Örebro n=4, Lund n= 2) and cases with missing patients charts (Uppsala-Örebro n=0, Lund n=2) were excluded. In Lund, patients from the years were excluded since a higher proportion of tumor blocks were missing when data from the National Cancer Register was utilized. Finally, a cohort of 109 patients from Uppsala- Örebro from 1990 to 2007 and 88 patients from Lund from 1990 to 2005 were identified. Updated information about the patients vital status and cause of death were retrieved from the National Population Register. Paper IV-V MBC patients from Skåne University Hospital, Uppsala University Hospital and Örebro University Hospital with available fresh frozen and paraffinembedded tissue were identified. In Paper IV, a total of 66 and in paper V, a total of 56 MBC tumors with sufficient tumor material were identified and could be included in the studies. Medical charts were reviewed for the collection of data on clinicopathological characteristics, treatment and outcome. All tumors were graded according to current pathological standards by a board-certified breast pathologist (ST). ER, PR and HER2 were re-evaluated as described in paper II. 28
29 Methods Paper I In a retrospective setting, cohorts of men and women diagnosed with invasive breast cancer were analyzed. A sampling procedure was conducted in order to achieve comparable groups. To increase the power of the study, each male (n=99) was randomly sampled with four females (n=396). The sampling procedure was performed using age at diagnosis (<49, 50-59, 60-69, 70-79, 80 years of age) and time of diagnosis ( , , ). Data on tumor stage, hormone receptor status, tumor grade and primary treatment were retrieved from the register. In all patients, updated information about vital status was obtained from the National Population Register. Paper II-III The Nottingham histological grade (NHG) was evaluated on hematoxylin and eosin (HE) stained conventional slides while immunohistochemical (IHC) stainings were evaluated on tissue microarrays (TMA). Construction of TMA block Hematoxylin and eosin sections from the original paraffin-embedded tumor blocks were used to determine the most representative areas of invasive tumor. From the tumor blocks, two 1 mm biopsies were punched and brought to recipient paraffin blocks to construct tissue microarrays (TMA). The TMAs were then cut into 4µm thick sections and transferred to glass slides (Figure 3). 29
30 a. b. c. Figure 3. Different steps in TMA construction: a. Paraffin-embedded tumor blocks are collected. b. Representative areas in the tumors are marked. c. Biopsies from the representative areas are punched and brought to recipient paraffin blocks (blocks to the right). TMA blocks are cut and transferred to glass-slides (to the left) Immunohistochemical staining All immunostainings were performed on sections from the TMA blocks. For the preparation of IHC markers used in paper II, a fully automated IHC staining machine (BenchMark Ultra, Ventana) was used for deparaffinization, cell-conditioning and staining.). EGFR was stained using DAKOs EGFRpharmDX. HER2 SISH, a fully automated silver in situ hybridization (SISH) from Ventana, was used for evaluation of HER2 amplification. For the staining of cyclins in paper III another process was implemented. Slides were deparaffinized and rehydrated through a ladder of graded ethanols (absolute ethanol, 95%, 80% and distilled water). For cyclin A and cyclin D1, antigen retrieval was performed in a microwave oven for 10 minutes (750W) + 15 minutes (350W) with the use of a TE-buffer. For Cyclin B, antigen retrieval was carried out in a pressure cooker for four minutes with the use of TRS-buffer. After antigen retrieval, all TMA slides were processed in an automatic immunohistochemistry staining machine according to standard procedures (Autostainer, Dako, Sweden). See Table 3 for antibodies and dilutions. For evaluation of HER2 status, all cases were analyzed by IHC and by SISH. Using IHC, cases were classified as 0, 1+, 2+ or 3+ according to standard procedures. With SISH, cases were scored as no amplification if 5 or fewer copies of the HER2 gene were present per nucleus in more than 50% of the tumor cells. Tumors were classified as HER2 positive when amplified or when HER2 IHC 3+ if amplification was not evaluable. 30
31 Table 3. Summary of antibodies, clones, dilutions and preparations used in paper II-III Marker Clone Vendor Dilution Preparation Paper ER SP1 Ventana Ventanas Ready CC1 Standard II to Use PR 16 Leica 1:25 CC1 Standard II Ki-67 MIB-1 DAKO 1:50 CC1 Mild II CK5/6 D5/16B4 DAKO 1:25 CC1 Standard II EGFR 1494 DAKO EGFR pharmdx II HER2 4B5 Ventana Ventanas Ready CC1 Mild II to Use Cyclin A NCLcyclin Novo Castra 1:100 Microwave oven III A Laboratories and TE-buffer Cyclin B Epitomics Inc 1:200 Pressure cooker III and TRS-buffer Cyclin D1 RM S NeoMarkers 1:75 Microwave oven and TE-buffer III Evaluation of immunoreactivity scores Estrogen receptor status and Ki67 were analyzed by one investigator (CA), Progesterone receptor (PR) status by a second investigator (CN) and EGFR, CK5/6 by a third investigator (IJ) The percentage of positively stained cells was assessed by choosing the high-power field with the largest number of positively stained cells out of the two biopsies, also called hot-spot, and dividing positively stained cells by the entire number of cells from the same high-power field. A minimum of 200 cells per tumor were counted. Cells were counted manually in high-power fields using a light microscope. The method used for scoring has been validated in previous studies 90, 107, 108.ER and PR were considered positive when more than 10% of tumor cells were stained. For Ki-67 a cut-off point of 14% was used 93 and, in the assessment on EGFR and CK5/6, any staining was considered as positive result. Immunohistochemical markers were used to classify tumors into subgroups derived from molecular classification. Three different combinations of IHC markers defining molecular subtypes were used; hereafter called the five biomarker classification, classification/nhg and classification/ki-67. See Table 4 for IHC markers used in the different classifications. 31
32 Table 4 Summary of immunohistochemical criteria for defining breast cancer intrinsic subtypes according to three different classifications Classification Subtype ER and PR HER2 NHG Ki-67 CK5/6 and EGFR Five biomarker Luminal A ER and/ or neg. NA NA any classification PR pos. Luminal B ER and/ or pos. NA NA any PR pos. HER2-like neg. pos. NA NA any Core-basal neg. neg. NA NA CK5/6 and/or EGFR pos. 5NP neg. neg. NA NA neg. Classification /NHG a Luminal A ER and/or PR pos. Luminal B ER and/or PR pos. Classification Luminal A ER and/or /Ki-67 a PR pos. Luminal B ER and/or a Luminal HER2 PR pos. ER and/or PR pos. neg. I-II NA NA HER2 pos. and/ or NHG III NA NA neg. NA low NA neg. NA high NA pos. NA any NA Only receptor-positive subtypes are described. The classification also includes HER2-like subtype (ER and PR negative, HER2 positive) and basal-like (ER, PR negative and HER2 negative). In paper III, cyclin A and D1 were analyzed by one investigator (CN) and cyclin B by a second investigator (AK). The percentage of positive cells was determined using the same criteria as described in paper II. For cyclin A and D1, cells with unequivocal nuclear staining and for cyclin B, nuclear and cytoplasmic stainings were considered positive. Paper IV Only tumors with >70% tumor cell content were included. RNA was extracted from fresh frozen tumor tissue and RNA integrity was assessed. Samples with sufficient RNA quality were finally hybridized to gene arrays (Human HT-12 v3.0 Expression BeadChips) in three batches. BioArray Software Environment (BASE) was used for data normalization and management 109. Normalization is performed with the aim to remove technical variation without removing the biological variation between samples. To be able to adjust for platform related biases, four samples from batch 1 and 2 were re-hybridized in the third batch. A batch effect was detected and adjusted for. Unsupervised hierarchical clustering (HCL) was performed in order to identify GEX subgroups in the MBC cases. HCL, based on Pearson correlation 32
33 distance and complete linkage, identified MBC subgroups which were further analyzed using significance analysis of microarrays (SAM) to identify differentially expressed genes. Up- and down regulated genes were analyzed in the Database for Annotation, Visualization and Integrated Discovery (DAVID), to investigate whether genes with specific biological themes differed between subgroups. The male subgroups were compared with an external FBC GEX data set. Seven GEX modules associated with key biological processes in FBC were used to detect biologically meaningful differences between MBC subgroups and additionally, as a comparison with FBC. The external female data set was also used for analyzing the degree of similarity between the MBC GEX subgroups with FBC GEX subgroups. Vectors of mean values (centroids) representing the MBC and FBC subgroups, respectively, were constructed. Samples were thereafter classified according to the centroid with which they displayed the highest correlation. With the same method, identified subgroups in MBC were validated to an external GEX data set from 37 MBC cases. The protein expression of N-acetyltranseferase-1 (NAT1) and class 1 human leukocyte antigen (HLA), two of the genes which differed significantly between the male subgroups, were evaluated using immunohistochemistry on TMAs in an extended MBC cohort. Paper V Only samples with sufficient tumor cell content were used. DNA was extracted using a modification of a back-extraction protocol from the organic phase of Qiagen Lipid minirna kit. BioAnalyzer was used for the assessment of DNA quality. Tumors of sufficient DNA quality were analyzed by high-resolution tiling BAC acgh. BAC arrays with BAC clones mapped to the UCSC Human Genom build 17 were produced at the SCIBLU Genomics Resource Centre, Lund University. The PopLowess method was used for the normalization of acgh data 110. The Circular Binary Segmentation algorithm was used as a method of dividing the genome into regions of equal copy number 111 and segments containing at least four consecutive probes were used in the following analyses. Gains and losses within the genome were detected and the fraction of genome altered (FGA) was calculated. To identify genomic aberrations in common between cases, a Genomic Identification of Significant Targets in Cancer (GISTIC) analysis was run. GISTIC is an evaluated statistical approach aimed at distinguishing regions of aberration that are more likely to be of importance in cancer pathogenesis. The method identifies regions that are aberrant more often than would be expected by chance 112. An in-house set of 359 FBC samples run on the same acgh platform, and analyzed in a similar way was used for comparison between male and female cancer. GISTIC regions 33
34 derived from the FBC samples were used for hierarchical clustering of the MBC tumors. Using the female tumors as a reference set, the male tumors could be classified into molecular subgroups. In addition, mean values for all GISTIC regions were calculated for all samples in each of the FBC reference CGH groups, and a centroid characterizing each subgroup was constructed. Thereafter, the correlation of each MBC sample to each of the FBC subgroups was calculated using the Pearson correlation. 34
35 Statistics Paper I The differences in proportions between the male and female cohorts were analyzed using the Chi-square test and Fisher s exact test where appropriate. Analyzes were done without regard to the initial sampling procedure. The differences in overall survival between genders were analyzed using Kaplan- Meier with log-rank statistics. Relative survival was used to analyze gender specific differences in survival. Relative survival is a model which estimates the ratio of observed survival to the expected survival of comparable groups in the standard population. The standard population used was Sweden Differences in survival between genders were analyzed using The Poisson model 113. Paper II-III All statistical analyses were performed in SPSS version The study end-point was breast cancer death, other cases were censored. A Cox proportional regression model was used to assess the hazard ratio for the different clinicopathological variables. Correlation between clinicopathological variables were analyzed using Spearman s correlation test. To define the optimal cut-off of the different proliferation markers in MBC, a previously described method was used 114. Briefly, the material was divided into 10 equal groups, so-called deciles, and the cut-off values corresponding to each decile limit were used to separate the material into a higher and a lower proliferating group. For each cut-off, the hazard ratio for breast cancer death was calculated, using Cox proportional hazard model. For comparison of categorical data chi-square statistics were used. Paper IV-V All statistical analyses were performed in R 115.Distant metastasis free survival (DMFS) was used as end-point in all survival analyses. The Wilcoxon test or Students t-test were used for calculation of p-values. 35
36 Results Paper I Current guidelines generally recommend that MBC patients should be managed similarly to FBC patients, but some reports have indicated that MBC patients receive less treatment 30, 116. Many studies have described a poorer overall survival in MBC patients which may partly be explained by reported differences in stage at diagnosis and more advanced age 26, 30. Other explanations could be differences in tumor characteristics or treatment intensity. In the present study, we compared MBC and FBC cohorts which were sampled according to age and time of diagnosis in order to obtain comparable groups. No differences in the distribution of stage at diagnosis were seen between the male and female patients. MBC patients underwent mastectomy more often, and breast conserving surgery less frequently compared with FBC patients. Radiotherapy given after partial (80% vs. 75%, p=1.00) or full mastectomy (44% vs. 39%, p=0.47) did not differ between the groups. No differences in adjuvant chemotherapy (16% vs. 21%; p=0.31) or adjuvant endocrine treatment (59% vs. 52%, p=0.24) could be demonstrated. Not even when analyzing those patients most likely to receive adjuvant chemotherapy (<70 years and node-positive) could any difference in treatment intensity be demonstrated between genders. Overall survival (41% vs. 55%, p=0.001) and relative survival (74% vs. 88%, p=0.015) at five years were significantly inferior in MBC (Fig 6-7). Although no differences in the distribution of stage or treatment strategy was demonstrated, the male group demonstrated a significantly poorer overall survival. However, the observed difference in overall survival may be explained by the fact that men in general have a shorter life expectancy and higher comorbidity burden. With the aim of adjusting for this potential bias, we compared the relative survival between genders and could observe that the MBC patients had significantly poorer relative survival. In conclusion, no differences in stage at diagnosis or primary treatment intensity were seen, but the male group had a significantly poorer survival which might indicate differences in tumor biology. 36
37 Figure 6. Overall survival in MBC patients and FBC patients. Figure 7. Relative survival of MBC patients compared with FBC patients Paper II The IHC markers routinely used in clinical practice have not been sufficiently validated in MBC. Previous reports in MBC are contradictory, and in many studies survival data are lacking, thus precluding prognostic evaluation 17, 26, 63, 103, 104. IHC marker combinations broadly matching the molecular subtypes are recommended for clinical use in FBC 93. Previous reports in MBC have demonstrated that there are distinct differences in the prevalence of molecular subtypes compared with FBC, and it is unknown whether 37
38 the subtypes have similar prognostic information In our study, ER- positivity was found in 93% of patients and PR-positivity in 78%. High tumor grade (NHG III) was demonstrated in 41% and HER2 positivity in 11%.Tumor size >20 mm, positive nodal status, ER negativity and PR negativity were significantly associated with an increased risk of breast cancer death in the univariate analysis, whereas no associations could be demonstrated for grade, PR, HER2 status, Ki-67 or age. In a multivariate model; node positivity, tumor size > 20 mm and ER negativity remained as independent prognostic factors (Table 5). The three definitions for molecular subtypes; the five biomarker classification, classification/nhg and classification/ki-67 identified luminal A and luminal B in 81% vs 11%; 48% vs. 44% and 41% vs. 42% of cases, respectively. Two cases of corebasal-like were revealed but no cases of HER2-like. One interesting finding was that luminal A and luminal B were near equally common according to classification/nhg and classification/ki-67, thus differing from data reported in FBC 77, 78, 117. However, no significant difference between Luminal A and B regarding risk for breast cancer death could be demonstrated by any definition (Table 6). The latter finding also differs from FBC, where a majority of studies show a significantly poorer outcome in luminal B cases 77, 78,
39 Table 5. Tumor markers in univariate and multivariate models by Cox Regression. Only variables with significant values in the univariate model were included in the multivariate model. Variable HR a 95% CI p-value HR b 95% CI p-value Tumor size; >20 vs. 20 mm < <0.01 Nodal status; pn1-3 vs. pn < <0.01 Tumor grade; III vs. I-II ER; 10 vs. >10% < <0.01 PR; 10 vs. >10% Ki-67; 14vs. <14% HER2; pos vs. neg Age; 60 vs. > Abbreviations: HR Hazard Ratio; CI, confidence interval a Univariate analysis b Multivariate model including tumor size, nodal status and ER Table 6. Univariate analysis of different classifications of molecular subtypes. Cox proportional regression was used with breast cancer death as an end-point. Classification Subtype Prevalence OR 95% CI p-value n % Five biomarker luminal A (Ref) classification a luminal B Classification/NHG a luminal A (Ref) luminal B Classification/Ki-67 a luminal A (Ref) luminal B luminalher
40 Paper III The clinical utility of proliferation markers in MBC has not yet been fully elucidated. In paper II, we evaluated Ki-67 and NHG in MBC but no prognostic impact could be demonstrated. In this study, we evaluated other proliferation associated variables; cyclin A, B, D1 and mitotic count. Furthermore, Ki-67 was re-evaluated using different cut-off levels. Cyclin A, B, mitotic count and Ki-67 demonstrated strong positive correlation with each other (Spearman correlation coefficient > 0.4) showing that these variables are linked in tumor biology. Cyclin D1 did not demonstrate any correlation with the other cyclins, mitotic count or Ki-67. The 7 th decile cut-off for cyclin A (12%) corresponded well to the previously defined cutoff in FBC (11%). When using these cut-offs, overexpression of cyclin A was associated with a trend to poorer breast cancer survival (p= 0.11 and p= 0.07, respectively). The prognostic impact of cyclin A was enhanced when using cut-offs corresponding to the 8 th (14%) and 9 th decile (17%) with HR 2.1; p=0.05 and HR 3.7; p=0.001, respectively. Overexpression of cyclin B was prognostic of poorer breast cancer survival when using the cut-off corresponding to the 9 th decile (15%), demonstrating HR 2.7; p=0.02. Additionally, high mitotic count (>10 per field of view) was associated with a poorer survival, HR 2.5; p=0.01 (Table 7). Ki-67 did not demonstrate any prognostic value by any cut-off values used in this material. Hence, our results indicate that cyclin A and B may be more reliable markers than Ki-67 for assessment of proliferation. Contrary to the other cyclins, overexpression of cyclin D1 was predictive of better survival (HR 0.3; p=0.001). The prognostic value of cyclin D1 remained in a multivariate model including tumor size and nodal status (HR 0.48; p=0.05). Hormone receptor positive patients were analyzed separately to investigate whether cyclin D1 could have an influence on the response to endocrine treatment. We found that patients undergoing adjuvant endocrine treatment had a significantly poorer breast cancer survival, which may be explained by the fact that endocrine treatment was given more often in higher stage disease. However, adjusting for cyclin D1 did not change the prognostic value of endocrine treatment, which contradicts the hypothesis that cyclin D1 is associated with tamoxifen resistance. 40
41 Table 7. Prognostic impact of proliferation markers compared with other clinicopathological parameters. Univariate analyses using the Cox proportional hazard regression model. Variables Univariate models HR 95 % CI p-value Nodal status pn0 (ref.) 1.0 pn <0.01 Tumor size 20 mm(ref.) 1.0 >20mm <0.01 ER >10% (ref.) % <0.01 PR >10% (ref.) % Cyclin A 17% (ref.) 1.0 >17% <0.01 Cyclin B 15% (ref.) 1.0 >15% Cyclin D1 62% (ref.) 1.0 >62% <0.01 Mitotic count 10 (ref.) 1.0 > Paper IV FBC has been extensively investigated on the transcriptional level, and distinct subgroups providing prognostic information have been identified; luminal A, luminal B, HER2-like, basal-like and normal-like. Whether MBC tumors can be classified into similar subgroups associated with differences in clinicopathological characteristics and survival has previously not been evaluated. In the present study, 66 MBC tumors were characterized using gene expression arrays. An unsupervised hierarchical clustering analysis revealed two stable subgroups of MBC; luminal M1 encompassing 70% of tumors and luminal M2 30% of tumors. There was a tendency for luminal M1 to be associated with a younger age at diagnosis and a poorer survival. No differences in NHG or tumor size between the subgroups could be demonstrated. To further specify differences between the MBC subgroups, the expression of seven GEX modules associated with key biological processes were investigated. In this analysis, five of the modules - ERsignaling, tumor invasion and metastasis, HER2, proliferation and immune response - displayed significant or near significant differences between the subgroups. Luminal M1 was associated with higher scores of invasion and metastasis, proliferation and HER2, indicating a more aggressive tumor behavior. Luminal M2, on the other hand, displayed expression of genes involved in ER-signaling and immune response. Interestingly, ER-signaling 41
42 differed significantly between the subgroups even though the majority of tumors were ER positive at IHC assessment. Similarly low ER-signaling scores have only been seen in ER negative cases in FBC. None of the MBC subgroups displayed GEX module-patterns resembling any of the intrinsic subgroups of FBC. When using centroids based on a FBC GEX dataset, more than half of the MBC tumors remained unclassified. In comparison with the intrinsic subtypes in FBC, luminal M1 displayed higher correlations to HER2-like and basal-like tumors whereas luminal M2 displayed higher correlations to luminal A and luminal B subgroups. To further investigate the clinical relevance of the identified differences between the MBC subgroups, protein expression of NAT1 and HLA which are involved in ER signaling and the immune system, respectively, were investigated. NAT1 positivity was more common in luminal M2 tumors, and was found to be predictive of better DMFS. The prognostic impact of NAT1 was confirmed in a multivariate model including node status, NHG and tumor size (HR 2.8; 95% CI ). High expression of HLA was associated with a better DMFS when compared with a moderate level of expression. Paper V In line with the previously discussed intrinsic subgroups based on gene expression, FBC can also be classified by genomic aberrations, and distinct subgroups with differences in clinical outcome have been demonstrated 74. High resolution acgh in this MBC cohort revealed that MBC is a heterogeneous tumor type. The most common genomic aberrations were similar in MBC and FBC. Although no significant difference in total FGA could be observed between genders, genomic gains were significantly more common whereas genomic losses seem to be less common in MBC tumors. Whole chromosome arm gains were more frequent in MBC. MBC could be classified into two genomic subgroups with distinct genomic patterns; malesimple and male-complex. Twenty percent of cases were classified as malesimple and 77% as male-complex. In the male-simple group, no high-level amplifications or deletions were observed. The male-simple group correlated with significantly smaller tumor size and lower proliferation. Additionally, a higher percentage of male-simple samples were diploid, when compared with the male-complex group. The male-complex group encompassed all PR negative (n=8), all HER2 positive tumors (n=2) and all patients with a known BRCA2 mutation (n=3). When stratifying patients by age, 14 of 15 patients younger than 60 years of age at diagnosis clustered in the malecomplex group. Furthermore, all but one patient with a generalized recurrence clustered into the male-complex subgroup. The observed differences indicate that male-complex is a more aggressive tumor entity. However, no differences in DMFS could be observed, probably due to the small number of patients. The male-complex group displayed evident 42
43 similarities with the female luminal-complex group, whereas the malesimple subgroup did not seem to be comparable with any of the female subgroups. A Kaplan-Meier analysis comparing the male-complex with female-complex cases revealed equally poor DMFS. 43
44 General discussion In this thesis, we present five papers aimed at increasing our understanding of MBC. It is known that MBC patients have a higher median age at diagnosis compared with FBC. Furthermore, it has been described that advanced stage at diagnosis is more common, particular in regions where women are offered regular mammography 13. In contrast, MBC are more often hormone receptor positive, often leading to the interpretation that MBC is a more indolent disease 24. Due to the rarity of MBC, there is a lack of prospective studies evaluating different treatment strategies and the optimal treatment is not known. Today, the general recommendation is to treat male patients according to guidelines in FBC. Breast cancer mortality in women has declined during the last decades due to improvements in diagnostic procedures and treatment but the corresponding observation has not been made in MBC 29. Several reports have indicated that MBC patients do not receive as intensive treatment as FBC patients 30, 116. The older age and higher comorbidity in the male group is one explanation for less treatment, but the lack of evidence for different treatment modalities in MBC may also contribute. In all, the results of our studies indicate that MBC is a unique breast cancer entity, different from FBC. In paper I we demonstrated that MBC is an aggressive disease with poorer disease-specific outcome in comparison with FBC. These findings are in line with some previous reports showing a poorer overall survival 26, 30 or breast cancer specific survival 22 in the male group. On the other hand, a recent population-based study collecting data from registers in six countries concluded that MBC had a better relative survival in comparison with FBC, after adjusting for multiple variables including age, stage and treatment 29. The latter study had larger patient cohorts than our study but the registers from the different countries varied in accessible data and used different definitions for stage and treatment modalities. The access to high-quality, detailed registry data strengthens our results. In papers II-III our aim was to examine MBC tumors as regards the prevalence and prognostic impact of different clinicopathological parameters. Additionally, we wished to classify MBC into molecular subtypes using IHC and evaluate the prognostic values. Previous studies have revealed that lymph node status is an important prognostic factor in MBC, but the knowledge regarding the prognostic value of other clinicopathological 44
45 parameters is scarce and contradictory 5, 17, In recent years, the classification into intrinsic subtypes by gene expression has become more important in FBC. These molecular signatures are considered to mirror the heterogeneity of tumors in a better way and have proven to make certain conventional clinicopathological parameters redundant by identifying a higher proportion of low-risk patients not necessarily in need of adjuvant systemic treatment 69, 70. One important finding in FBC is that proliferation is the most important parameter in the classification of hormone receptor positive tumors into luminal A and B, where the latter subgroup is associated with a poorer prognosis 70. Based on these findings, commercial gene arrays have been developed most importantly to improve the risk-assessment of hormone receptor positive tumors 72, 73. However, gene arrays are expensive and not always accessible; therefore, combinations of immunohistochemical markers broadly matching the intrinsic gene expression subtypes have been identified and may be more feasible in clinical routine Today, IHC based molecular subtyping is recommended by several guidelines for the prognostication and treatment decision-making in FBC 93, 118. In paper II, we could conclude that node status, tumor size and ER status are independent prognostic factors in MBC. A large subset of cases was assessed as highly proliferating according to NHG or Ki-67, but we could not demonstrate that this was of any prognostic value. HER2 did not reveal any prognostic information but interestingly, the interpretation of HER2 assessment by IHC seem to differ from that in FBC. Of all HER2 amplified cases, only a few had a corresponding strong (3+) IHC expression. Three commonly used models for classification into subtypes were evaluated and, in all models, the vast majority of patients were classified into the hormone receptor positive luminal subgroups. Interestingly, luminal A and B were almost equally common in the two models adding tumor grade or Ki-67 for classification into luminal subtypes, which differs from reports in FBC 77, 78, 119. Furthermore, the molecular subtyping did not by any classification seem to give similar prognostic information to that reported in FBC. Recently, two papers have been published describing molecular subtypes assessed by IHC in MBC. Shaaban et al used HER2 status to separate the luminal subtypes. The male cohort was compared with a matched female cohort and no survival difference between the male and female luminal A was seen; however, in the same paper, tumor biological differences were discussed indicating that luminal A in MBC is not comparable with luminal A in FBC. Furthermore, international praxis on evaluation of HER2 status was not adhered to: no FISH testing was performed and only IHC 3+ was considered HER2 positive. None of the tumors had IHC 3+ and consequently, no tumors were classified as luminal B 83. In the second paper, a classification including proliferation and HER2 was used but the prognostic 45
46 relevance of the different subtypes was not evaluated due to lack of outcome data 82. To date, our study is the first to correlate molecular subtypes with breast cancer survival. Non-significant results should be interpreted with caution due to the moderate level of power but the results imply that the molecular subtypes validated in FBC are not applicable in MBC, and molecular classifications specific for MBC tumors need to be identified. In papers IV-V, the molecular background of MBC was investigated. In paper IV global GEX analyses in MBC tumors were performed and compared with a previous data set of FBC tumors. Two subgroups among MBC tumors were identified; luminal M1 and luminal M2. When evaluating the degree of similarity to the intrinsic subtypes in FBC tumors, more than half of the MBC tumors were left unclassified. To enlighten the differences between the MBC subtypes, tumors were analyzed for seven different GEX modules representing key biological processes; proliferation, tumor invasion, immune response, angiogenesis, apoptosis, ER-signaling and HER The larger subtype (luminal M1), encompassing 70% of patients, displayed higher scores in proliferation, tumor invasion and HER2 modules, whereas luminal M2 tumors were characterized by a higher expression of genes related to the immune system and ER-signaling. The observed differences in GEX modules indicate that luminal M1 displays a more aggressive tumor behavior, which was further supported by a survival analysis suggesting poorer DMFS in this group. The observed significant difference in ER-related gene signaling between the groups is different from FBC, where only tumors ER-negative by IHC display similar reduced ER-signaling. One of the genes correlating to ER-signaling, NAT1, was significantly higher expressed in luminal M2 tumors. The protein expression of NAT1 was investigated in an extended MBC cohort. Half of the patients were assessed as NAT 1 negative, which in FBC has been found to be associated with an inferior response of tamoxifen 121. In our material, NAT1 displayed independent prognostic information, but unfortunately, there were too few cases to evaluate the association of NAT1 to tamoxifen response. In paper V, MBC tumors were evaluated on the DNA level by CGH, revealing differences compared with FBC. As in the GEX analyses, two subgroups were identified and a majority of patients were classified into the subgroup with more aggressive tumor behavior. One unique MBC subgroup, not resembling any of the FBC subgroups, was identified. Hence, both studies on the molecular level indicate that there are distinct differences in key biological processes between male and female breast cancer and that MBC has unique molecular subtypes with probable prognostic importance. Furthermore, the findings demonstrate that MBC is a heterogeneous tumor entity. 46
47 In both studies on the molecular level, proliferation was one important tumor biological feature that differed between the MBC subgroups. In paper II, however, we could not show that NHG or Ki-67, two parameters highly associated with proliferation and today used in clinical routine, had any prognostic value. In paper III, other proliferation-related markers were assessed. We found that the overexpression of cyclin A and B were near significantly or significantly associated with a poorer outcome in the subset of patients with the highest expression. In addition, we could demonstrate that high mitotic count was associated with an increased risk of breast cancer death, which further strengthens the conclusion that proliferation is of prognostic importance in MBC. These findings are in line with some previous reports 17, 103, 122 but contrary to others 5, 17, 103, 104, 122. Ki-67 was re-evaluated using different cutoffs, but no prognostic value was demonstrated in this cohort. This is in accordance with studies in FBC indicating that Ki-67 may be a weaker prognostic factor than cyclin A and B 87, 90, and, consequently, a larger cohort may be needed to be able to confirm its prognostic impact. Another issue with potential influence on our results is that a subset of our patients had received adjuvant and /or palliative chemotherapy treatment which is known to diminish the prognostic impact of proliferation markers. 114, 123. To summarize, our observations indicate that cyclins A and B and mitotic count may be more reliable markers than Ki-67 for assessment of proliferation, but additionally studies are warranted to establish the optimal marker and cutoff. In line with previous reports in MBC, overexpression of Cyclin D1 was independently predictive of better breast cancer survival 103, 105. The reason for cyclin D1 overexpression seeming to be associated with a better outcome despite its proliferation-activating potential is not fully understood. One hypothesis is that there might be an interaction between key biological processes in the process of metastasis. This is supported by in vitro studies where a lower expression of cyclin D1 was linked to an enhanced infiltrative potential in the tumor. The explanation for the latter finding was that cells in the quiescent phase had a greater migratory capacity 124. Previous studies in FBC have suggested that Cyclin D1 has dual roles, in addition to its the cell cycle related actions, it has been suggested that it can stimulate the ER α receptor in a ligand-independent manner and thereby have the ability to reverse the ER blocking effect of tamoxifen, leading to tamoxifen resistance 101. In our study, patients undergoing adjuvant endocrine treatment had a poorer breast cancer survival, possibly explained by the fact that treatment was given more often in higher stage disease. However, cyclin D1 did not seem to influence the response of endocrine treatment. One reason for this could be that ER-signaling is different in MBC, as postulated in paper IV. This notion is supported by other studies, suggesting a reduced ER functionality in MBC. Further studies regarding this issue are needed 43,
48 A number of limitations concerning this thesis need to be discussed. In Paper I, we used registry data for information on clinicopathological parameters, treatment data and vital status. An alternate method is to collect corresponding data from patient files which may give more accurate information. However, the Regional Breast Cancer Register has been validated and a very high level of agreement on data regarding primary treatment has been demonstrated. Furthermore, the Regional Breast Cancer Registry has shown a high level of completeness with >95% of diagnosed breast cancer cases registered. One limitation in this study was the absence of data on breast cancer deaths, preventing us from analyzing breast cancer specific survival. Instead we used relative survival, a method which estimates the ratio of the observed survival of patients in a cohort to the expected survival of a comparable group from the general population. In this model, commonly used in population-based studies, the cause of death is not required but the excess mortality related to the cancer diagnosis can be estimated 113. In Papers II-III, MBC tumors were characterized by IHC markers on TMA. Hot-spots were chosen for evaluation and a minimum of 200 cells per tumor were counted. The TMA technique enables rapid screening of a large number of tumors on a single microscopic slide. One drawback with the technique is that only a small amount of tumor is analyzed which leads to the question of how representative the TMA core is, and how much tumor heterogeneity could affect the results. However, several studies have shown that even though the result from an individual TMA core in comparison with a conventional histological slide may vary, the correlation to histopathological variables and prognostic implications are in agreement when a large number of tumors are studied It could also be questioned why we did not validate the scoring results with two or more investigators but this was not considered necessary as previous studies have demonstrated good reproducibility between different investigators with the scoring method used in our studies 90, 107. One known disadvantage with the TMA technique is that tissue cores can be lost or damaged during sectioning, which was also a problem in our studies, leading to loss of tumor marker information in 2-6% of cases. In papers IV V, two distinct male subgroups were identified both on the transcriptional level (luminal M1 and luminal M2) and on the genomic level (male complex and male simple). In FBC, at least five subgroups with clinical relevance have been identified and it cannot be excluded that additional subgroups can exist in MBC. Although our material with fresh frozen tissue from MBC cases is the largest reported to date, the small number of patients included may prevent as accurate sub classification as that performed in FBC. However, the results were validated in an external GEX data 48
49 set from MBC tumors and comparable subgroups and a similar distribution of subgroups was observed. For the comparison between MBC and FBC GEX groups, an external FBC data set was used. Even though the FBC data set was derived from GEX analysis performed in a similar way, methodological differences between analyzes may influence the comparison between genders. Another concern which needs to be enlightened is the issue of patient selection. It is today not routine practice to save fresh frozen tissue from all patients diagnosed with breast cancer, which is reflected in the small subset of patients where frozen tissue was available. We collected all accessible fresh frozen tumor samples but there is a risk that this patient material may not be entirely applicable to the entire MBC population. Our patient materials are comprehensive in comparison with previous studies in MBC. However, the problem of achieving sufficiently large patient materials is a matter that concerns all papers presented in this thesis. As a consequence, the power of the studies is moderate which makes interpretation of non-significant results difficult. In conclusion, MBC is a unique breast cancer entity. Positive nodal status, larger tumor size, ER-negativity, low expression of cyclin D1 and low expression of NAT1 are independent predictors of poorer breast cancer survival. The established molecular subtypes used in FBC are not applicable in MBC. Two MBC subtypes were identified on both the transcriptional and genomic levels, but additional subtypes of clinical importance may exist. Molecular subtypes are today used in clinical routine, but we have yet to discover which IHC markers to use to define the MBC subtypes. Furthermore, MBC tumors ER positive by IHC do not seem to correspond to ER-signaling as highly as in FBC. This could imply that MBC tumors respond differently to endocrine treatment. 49
50 General conclusions Paper I: When comparing cohorts of MBC and FBC patients, sampled according to age and year of diagnosis, no differences in primary treatment intensity could be demonstrated. At time of diagnosis, MBC and FBC patients presented with a similar distribution of disease stage. Although no differences in treatment intensity or stage was observed, the male group had significantly poorer overall and relative survival. Paper II: In this study we demonstrated that ER-negativity, tumor size >20 mm and positive lymph nodes are independent risk factors for breast cancer death in MBC. Age, HER2, grade or Ki-67 did not reveal any prognostic impact, but the moderate power of this study must be taken into account. The classification using IHC markers into molecular subtypes does not seem to provide similar prognostic information as in FBC and prognostic profiles specific for MBC need to be identified. Paper III: In this paper we showed that proliferation is important in MBC. Overexpression of cyclin A, cyclin B and high mitotic count is predictive of poorer survival in MBC and seems to provide more reliable prognostic information compared with Ki-67. Contrary to the other cyclins, overexpression of cyclin D1 is associated with better breast cancer survival. The prognostic information of cyclin D1 adds independent prognostic information to the other cyclins. However, further studies are warranted to be able to establish the optimal markers and what cut-offs to use. Paper IV: In this MBC material two unique and stable gene expression subgroups were identified; luminal M1 and luminal M2. The subgroups displayed differences in tumor characteristics and outcome. The MBC subgroups differed from the acknowledged intrinsic subgroups in FBC. The findings may indicate that MBC patients may need specific treatment strategies, and further studies are warranted. NAT1 protein expression was identified as a prognostic factor, with overexpression associated with better outcome. Paper V: With high-resolution genomic profiling, differences between male and female breast cancer could be demonstrated. MBC could be divided into two different sub-groups, male simple and male complex, which may have prognostic value. The male simple group seems to represent a new subgroup, unique for MBC patients. 50
51 Future perspectives The present study emphasizes the need of further investigations into different fields of MBC. Regarding the molecular subtyping of MBC, several questions need to be answered. Our colleagues in Lund are planning to perform a GEX analysis with MBC tumors together with FBC tumors. In paper IV, the GEX patterns of MBC patients were compared with previous data from a FBC tumor data set analyzed in a similar way. The reason for the comparison with historical data was mainly due to the high costs of GEX arrays. A GEX analysis with male and female tumors analyzed together will hopefully validate the MBC subtypes but will also give a clearer picture of the differences in subtypes between genders. Another important issue is to identify IHC marker combinations defining the MBC molecular subtypes. It would in that case be logical to focus on the GEX modules that differed significantly between the MBC subtypes and identify additional corresponding protein products which could be used for IHC classification. Further GEX analyzes on larger MBC cohorts are warranted for the evaluation of the prognostic significance of the MBC subtypes. The findings in papers II-III also need to be validated in, preferably, larger studies. Due to the rarity of the disease, multi-institutional collaboration is crucial in order to achieve larger patient materials. Different research collaborations have been discussed 13 and we have been asked to participate in a research project involving a number of countries in Europe. In this project, two different studies are being considered. Firstly, a retrospective part assembling clinical data and tumor tissue from MBC patients diagnosed during the last 20 years is planned, with the goal of assembling more than 1000 cases. Paraffin-embedded tumor tissue will be collected for analyses of tumor biology. A central pathology review is planned with the aim of overcoming the problem of lack of harmonization in techniques and cut-off definitions. Clinical data and histopathological parameters will be correlated to outcome data for the evaluation of prognostic impact. Additionally, GEX analyses will be performed on fresh frozen tissue. The second part will be a prospective registration of all new cases diagnosed during two years. The registration will include information on risk factors, clinicopathological variables, treatment and follow-up data. If the collaboration succeeds, it will open up the possibility of launching randomized, controlled trials for the male group. Most importantly, the value of different endocrine treatments needs to be evaluated. It is also important to 51
52 allow the inclusion of MBC patients in all future larger clinical trials in the breast cancer field. Many clinical trials today collect blood samples and frozen tissue to identify molecular profiles predictive of treatment response, and this could prove valuable for male patients. Another way of learning more about factors behind tumor development and progression or the interaction between different treatments and molecular pathways, would be to use animal models. A method for the induction of mammary tumors in male transgenic mice has been developed 128. In the future, we will have an excellent resource for research in MBC. Research centers in Sweden plan or have already started projects where fresh tissue and blood samples from all patients diagnosed with breast cancer are collected 129, 130. Molecular analyses will be conducted using high resolution genomic techniques and the molecular information will be linked to clinicopathological, treatment and outcome data from our comprehensive breast cancer registries mandatory for all patients diagnosed with breast cancer. This will probably give us the possibility to better answer the question regarding the optimal treatment and the optimal prognostic tools for MBC. 52
53 Sammanfattning (Brief summary in Swedish) Manlig bröstcancer är en mycket ovanlig sjukdom som står för ca 0,6 % av all bröstcancer, vilket innebär att ca män drabbas av sjukdomen i Sverige varje år 4. Vid kvinnlig bröstcancer har man de senaste decennierna sett en minskad dödlighet till följd av tidigare diagnostik samt effektivare behandlingar, vilket dock inte har kunnat visas vid manlig bröstcancer. Idag finns mycket lite kunskap om hur vi på bästa sätt ska behandla män med bröstcancer. Eftersom sjukdomen är så ovanlig har det inte gått att utvärdera effekten av olika behandlingar vid manlig bröstcancer och idag behandlas männen enligt de riktlinjer som gäller vid kvinnlig bröstcancer. Vid kvinnlig bröstcancer används olika prognostiska samt prediktiva faktorer för att välja den bästa behandlingen för varje enskild patient. En prognostisk faktor förutsäger sjukdomens naturalförlopp medan en prediktiv faktor beskriver känslighet för en viss behandling. Idag är tumörstorlek, körtelstatus, tumörgrad, Ki-67, progesteronreceptoruttryck samt HER2 (human epidermal growth factor receptor 2) de viktigaste prognostiska faktorerna 52. Under senare år har det även varit en ökad användning av olika genprofiler som hjälp i den prognostiska bedömningen 70, 72, 73. Vi vet dock inte om det kan finnas avgörande skillnader i den tumörbiologiska bakgrunden mellan manlig och kvinnlig bröstcancer som i så fall också kan innebära att de idag använda prognostiska och prediktiva faktorer inte har samma betydelse vid manlig bröstcancer. Delarbete I I delarbete I undersöktes skillnader i behandlingsintensitet och överlevnad mellan manliga och kvinnliga patienter med invasiv bröstcancer. Samtliga män som fick diagnosen bröstcancer mellan år identifierades i det Regionala bröstcancer registret i Uppsala-Örebro. I syfte att öka studiens styrka samt för att få jämförbara grupper matchades varje manlig patient (n=99) mot fyra slumpvis utvalda kvinnliga patienter (n=396). Patienterna matchades avseende ålder vid diagnos samt diagnosår. Vi kunde visa att det inte var någon säker skillnad i fördelningen mellan olika tumörstadier vid diagnos mellan den manliga och den kvinnliga gruppen. Det fanns en skillnad i valet av operationsmetod vilket förklaras av den mindre bröstvolymen hos männen som gör att bröstbevarande kirurgi är mindre angeläget. Vi 53
54 kunde dock inte se några skillnader i andelen patienter som planerades för postoperativ strålbehandling efter mastektomi, dvs. borttagande av hela bröstet. Vi kunde inte heller se någon skillnad i andelen patienter som erbjöds adjuvant cytostatika eller endokrin behandling. Trots att manliga och kvinnliga patienter hade jämförbart sjukdomsstadium vid diagnos och planerades för lika intensiv behandling, hade manliga bröstcancerpatienter en sämre överlevnad vilket kan tala för en mer aggressiv sjukdom. Delarbete II I delstudie II utvärderades den prognostiska betydelsen av olika tumörkarakteristika som idag används för att styra patienternas behandling. Vi undersökte också värdet av 3 olika modeller där immunhistokemiska markörer användes för uppdelning i molekylära subtyper. Molekylär subtypning har visats ha prognostisk betydelse vid kvinnlig bröstcancer och baseras ursprungligen på skillnader i genuttryck mellan olika bröstcancertumörer. Immunhistokemiska färgningar samt tumörgradering utfördes på tumörer från 197 manliga bröstcancerpatienter. Vi kunde visa att tumörstorlek, körtelstatus samt uttryck av östrogenreceptorer var oberoende prognostiska faktorer men vi kunde inte visa något prognostiskt värde av tumörgrad, Ki-67 eller HER2. Vi kunde inte heller visa någon statistisk säkerställd skillnad i prognos mellan olika molekylära subtyper, oavsett vilken definition som användes. Delarbete III I delarbete III utvärderades olika proliferationsassocierade markörer. Proliferation har visats vara en av de viktigaste tumörbiologiska processerna i uppdelningen av molekylära subtyper vid kvinnlig bröstcancer. Proliferationsgener är också av stor betydelse i olika kommersiella genprofiler som används för att identifiera bröstcancerpatienter med högre risk för återfall. I delarbete II kunde vi dock inte visa någon prognostisk betydelse av tumörgrad eller Ki-67, markörer som är starkt korrelerade till proliferation. I det här arbetet användes samma patientmaterial som i delarbete II för att utvärdera cyclin A, cyclin B, cyclin D1 samt antal mitoser, vilka samtliga är proliferationsassocierade markörer. Dessa markörer har tidigare inte undersökts vid manlig bröstcancer och det var därför oklart vilken cut-off som skulle användas för att dela upp tumörerna i hög- respektive lågproliferativa. Vi använde oss av en tidigare beskriven metod där patientmaterialet delades upp i 10 lika stora delar, s.k. deciler. Gränsen för varje decil användes för uppdelning av tumörer i hög- eller lågproliferativa. För varje decilvärde beräknades riskökningen för bröstcancerdöd och det värde som gav den högsta risken ansågs vara det bästa cut-off värdet. Vi kunde visa att 54
55 överuttryck av cyclin A och B samt ett högt antal mitoser talar för en ökad risk för bröstcancerdöd. Överuttryck av cyclin D1 var istället associerat till minskad risk för bröstcancerdöd, där en möjlig förklaring kan vara att cyclin D1 utöver proliferation också har associerats till processer som styr tumörinvasivitet och metastasering. Ki-67 analyserades på nytt med den beskrivna metoden, men visade inget prognostiskt värde oavsett cut-off. Delarbete IV Kvinnliga bröstcancertumörer kan baserat på genuttryck delas upp i 5 olika molekylära subtyper; luminal A, luminal B, basal-typ, HER2-typ samt normal-typ. Subtyperna har visats ha prognostisk betydelse 69, 70. I delarbete IV användes frusen tumörvävnad från 66 manliga bröstcancerpatienter för att undersöka genuttrycksprofiler. RNA extraherades och hybridiserades till gen-arrayer. Två subtyper identifierades; luminal M1 samt luminal M2. Trettio procent av tumörerna klassades som luminal M2, en subtyp som kännetecknades av ett högt uttryck av gener associerade till immunologiska processer samt till östrogenreceptorsignalering. Resterande tumörer klassades som luminal M1 vilka istället karakteriserades av ett lågt uttryck av gener associerade till östrogenreceptorsignalering trots att en majoritet av tumörerna hade ett starkt östrogenreceptoruttryck vid immunhistokemisk bedömning. Luminal M1 tumörerna var associerade till karakteristika som talade för en mer aggressiv tumörtyp och hade också en tendens till sämre prognos. Vid jämförelse mot data från kvinnliga bröstcancertumörer kunde mindre än hälften av manliga tumörer klassas enligt de undergrupper som är validerade vid kvinnlig bröstcancer. Proteinuttrycket av två gener som visade stor skillnad i uttryck mellan de manliga grupperna; N- acetyltransferase-1 (NAT-1) samt klass 1 humant leukocyt antigen, undersöktes senare med immunhistokemisk metod och NAT-1 visade sig vara en prognostisk faktor med överuttryck associerat till bättre överlevnad. Sammanfattningsvis identifierades två undergrupper vid manlig bröstcancer med tydliga skillnader i tumör-karakteristika och prognos. De manliga undergrupperna överensstämmer inte med någon av de ofta omnämnda kvinnliga undergrupperna. Delarbete V Vid kvinnlig bröstcancer har omfattande forskning bedrivits på molekylär nivå. Molekylära subtyper med prognostisk betydelse har identifierats både vid analyser av genuttryck samt vid analyser av förändringar i genomet (DNA). Genom att studera förändringar av genomet kan man också få information om vilka mekanismer som ligger bakom cancercellernas genomiska instabilitet. I delarbete V analyserades frusen vävnad från 55
56 56 manliga bröstcancertumörer med högupplöst BAC-array teknik för att undersöka avvikelser på DNA-nivå och se om undergrupper med prognostisk betydelse kunde identifieras. Resultaten jämfördes sedan med 396 kvinnliga bröstcancertumörer som hade analyserats med samma teknik. Analysmetoden Genomic Identification of Significant Targets in Cancer (GISTIC) användes för att identifiera signifikanta DNA-avvikelser som var ofta förekommande i tumörerna. Med utgång från de GISTIC regioner som hade identifierats i de kvinnliga bröstcancertumörerna utfördes en hierarkisk klustring av de manliga bröstcancertumörerna. Hierarkisk klustring är en analys metod som syftar till indelning i undergrupper med likartat mönster av DNA-avvikelser. Vi kunde inte visa någon signifikant skillnad i den totala mängden DNAavvikelser mellan manliga och kvinnliga bröstcancer tumörer, men vi såg skillnader i mönstret av DNA-avvikelser. Vid klusteranalysen identifierades två undergrupper av manlig bröstcancer; male complex och male simple. Grupperna skiljde sig från identifierade undergrupper vid kvinnlig bröstcancer. En majoritet av manliga bröstcancertumörer tillhörde male complex, den tumörtyp som var associerad med karakteristika som talade för en mer aggressiv tumör. Sammanfattningsvis visade studien att det finns tydliga skillnader mellan manlig och kvinnlig bröstcancer på DNAnivå. 56
57 Acknowledgements I should wish to express my deepest appreciation and gratitude to those who have helped and supported me during the work presented in this thesis: Marie-Louise Fjällskog, my main supervisor. I could not have asked for a better supervisor! Always encouraging and helpful, teaching me nearly everything I know in the area of research. I am aware that you have spent a lot of time during vacations and weekends on supporting me in this thesis, offering valuable time which should have been spent with your wonderful family, Gunnar, Lovisa and Tora, all of whom I should give my thanks. Leif Bergkvist, my co-supervisor, for your support, good advice, and for always rapidly reviewing and commenting the manuscripts. Ingrid Hedenfalk and Ida Johansson, Department of Oncology, Clinical Sciences and CREATE Health Strategic Center for Translational Cancer Research, Lund University. Thank you for allowing me the opportunity of obtaining insight into the world of molecular biology. Marit Holmqvist, for guidance in statistical matters. Cecilia Ahlin, Anthoula Koliadi and Claudia Lundgren, colleagues in Örebro and Uppsala, for your encouragement and support. All other co-authors who have contributed to my papers and consequently, also to this thesis. Jerzy Leppert, former head of the Centre for Clinical Research and Mats Enlund, current head of the Centre for Clinical Research, for providing time and necessary resources for the completion of this project. Henry Letocha, my mentor, colleague and friend. For good advice, encouragement, linguistic revision and last, but not least all good moments of laughter at work. 57
58 My colleagues at the Department of Oncology, just for being such great colleagues! A special thanks to Inger Andreasson, the head of the Department of Oncology in Västerås, for providing the time for my research work. All the personnel and researchers at the Centre for Clinical Research, with special thanks to Maria, Michaela, Katarina, Tony, Annika and Marja-Leena. Nic Löving, for all your help. Ulf and Eva, my parents, for believing in me and for always being there for me and my family. Christina and Stig-Roland, my parents-in-law. Without your help this would never have been possible. Ulrika and Fredrik, my brother and sister, for being such good friends! Victor, Lovisa and Gustav, my wonderful children. I love you! Eric, my true love and best friend. Thank you for all your support during these years, even in times when I did not deserve it. 58
59 References 1. Ronnov-Jessen L, Petersen OW, Bissell MJ. Cellular changes involved in conversion of normal to malignant breast: importance of the stromal reaction. Physiol Rev 1996; 76(1): Howard BA, Gusterson BA. Human breast development. J Mammary Gland Biol Neoplasia 2000; 5(2): Fentiman IS, Fourquet A, Hortobagyi GN. Male breast cancer. Lancet 2006; 367(9510): NORDCAN. Cancer Incidence, Mortality, Prevalence and Prediction in the Nordic Countries Giordano SH, Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN. Breast carcinoma in men: a population-based study. Cancer 2004; 101(1): Stang A, Thomssen C. Decline in breast cancer incidence in the United States: what about male breast cancer? Breast Cancer Res Treat 2008; 112(3): Anderson WF, Althuis MD, Brinton LA, Devesa SS. Is male breast cancer similar or different than female breast cancer? Breast Cancer Res Treat 2004; 83(1): Nahleh ZA. Hormonal therapy for male breast cancer: A different approach for a different disease. Cancer Treat Rev 2006; 32(2): Brinton LA, Carreon JD, Gierach GL, McGlynn KA, Gridley G. Etiologic factors for male breast cancer in the U.S. Veterans Affairs medical care system database. Breast Cancer Res Treat 2010; 119(1): Brinton LA, Richesson DA, Gierach GL, et al. Prospective evaluation of risk factors for male breast cancer. J Natl Cancer Inst 2008; 100(20): Liukkonen S, Saarto T, Maenpaa H, Sjostrom-Mattson J. Male breast cancer: a survey at the Helsinki University Central Hospital during Acta Oncol 2010; 49(3): McConnell JD, Roehrborn CG, Bautista OM, et al. The long-term effect of doxazosin, finasteride, and combination therapy on the clinical progression of benign prostatic hyperplasia. N Engl J Med 2003; 349(25): Korde LA, Zujewski JA, Kamin L, et al. Multidisciplinary Meeting on Male Breast Cancer: Summary and Research Recommendations. J Clin Oncol Ottini L, Palli D, Rizzo S, et al. Male breast cancer. Crit Rev Oncol Hematol 2010; 73(2): Hultborn R, Hanson C, Kopf I, et al. Prevalence of Klinefelter's syndrome in male breast cancer patients. Anticancer Res 1997; 17(6D): Swerdlow AJ, Schoemaker MJ, Higgins CD, Wright AF, Jacobs PA. Cancer incidence and mortality in men with Klinefelter syndrome: a cohort study. J Natl Cancer Inst 2005; 97(16): Cutuli B, Le-Nir CC, Serin D, et al. Male breast cancer. Evolution of treatment and prognostic factors. Analysis of 489 cases. Crit Rev Oncol Hematol 2010; 73(3):
60 18. Stewart RA, Howlett DC, Hearn FJ. Pictorial review: the imaging features of male breast disease. Clin Radiol 1997; 52(10): Sobin LH G, MK WC (eds). International Union Against Cancer (UICC). TNM Classification of malignant Tumours. Wiley-Blackwell. 20. Joshi MG, Lee AK, Loda M, et al. Male breast carcinoma: an evaluation of prognostic factors contributing to a poorer outcome. Cancer 1996; 77(3): Cutuli B. Strategies in treating male breast cancer. Expert Opin Pharmacother 2007; 8(2): Czene K, Bergqvist J, Hall P, Bergh J. How to treat male breast cancer. Breast 2007; 16 Suppl 2:S Uppsala-Örebro Regional Oncologic Center U, Sweden. Register for breast cancer. edn, Vol., Donegan WL, Redlich PN, Lang PJ, Gall MT. Carcinoma of the breast in males: a multiinstitutional survey. Cancer 1998; 83(3): Munoz de Toro MM, Maffini MV, Kass L, Luque EH. Proliferative activity and steroid hormone receptor status in male breast carcinoma. J Steroid Biochem Mol Biol 1998; 67(4): Nahleh ZA, Srikantiah R, Safa M, et al. Male breast cancer in the veterans affairs population: a comparative analysis. Cancer 2007; 109(8): Marchal F, Salou M, Marchal C, Lesur A, Desandes E. Men with breast cancer have same disease-specific and event-free survival as women. Ann Surg Oncol 2009; 16(4): Willsher PC, Leach IH, Ellis IO, et al. A comparison outcome of male breast cancer with female breast cancer. Am J Surg 1997; 173(3): Miao H, Verkooijen HM, Chia KS, et al. Incidence and Outcome of Male Breast Cancer: An International Population-Based Study. J Clin Oncol Scott-Conner CE, Jochimsen PR, Menck HR, Winchester DJ. An analysis of male and female breast cancer treatment and survival among demographically identical pairs of patients. Surgery 1999; 126(4):775-80; discussion Golshan M, Rusby J, Dominguez F, Smith BL. Breast conservation for male breast carcinoma. Breast 2007; 16(6): Bergkvist L, de Boniface J, Jonsson PE, et al. Axillary recurrence rate after negative sentinel node biopsy in breast cancer: three-year follow-up of the Swedish Multicenter Cohort Study. Ann Surg 2008; 247(1): Kell MR, Burke JP, Barry M, Morrow M. Outcome of axillary staging in early breast cancer: a meta-analysis. Breast Cancer Res Treat 2010; 120(2): Flynn LW, Park J, Patil SM, Cody HS, 3rd, Port ER. Sentinel lymph node biopsy is successful and accurate in male breast carcinoma. J Am Coll Surg 2008; 206(4): Gentilini O, Chagas E, Zurrida S, et al. Sentinel lymph node biopsy in male patients with early breast cancer. Oncologist 2007; 12(5): Recht A, Edge SB, Solin LJ, et al. Postmastectomy radiotherapy: clinical practice guidelines of the American Society of Clinical Oncology. J Clin Oncol 2001; 19(5): Overgaard M, Hansen PS, Overgaard J, et al. Postoperative radiotherapy in high-risk premenopausal women with breast cancer who receive adjuvant chemotherapy. Danish Breast Cancer Cooperative Group 82b Trial. N Engl J Med 1997; 337(14): Hultborn R, Friberg S, Hultborn KA, Peterson LE, Ragnhult I. Male breast carcinoma. II. A study of the total material reported to the Swedish Cancer Registry with respect to treatment, prognostic factors and survival. Acta Oncol 1987; 26(5):
61 39. Gennari R, Curigliano G, Jereczek-Fossa BA, et al. Male breast cancer: a special therapeutic problem. Anything new? (Review). Int J Oncol 2004; 24(3): Chakravarthy A, Kim CR. Post-mastectomy radiation in male breast cancer. Radiother Oncol 2002; 65(2): Macdonald G, Paltiel C, Olivotto IA, Tyldesley S. A comparative analysis of radiotherapy use and patient outcome in males and females with breast cancer. Ann Oncol 2005; 16(9): Giordano SH. A review of the diagnosis and management of male breast cancer. Oncologist 2005; 10(7): Weber-Chappuis K, Bieri-Burger S, Hurlimann J. Comparison of prognostic markers detected by immunohistochemistry in male and female breast carcinomas. Eur J Cancer 1996; 32A(10): Doyen J, Italiano A, Largillier R, et al. Aromatase inhibition in male breast cancer patients: biological and clinical implications. Ann Oncol 2010; 21(6): Walshe JM, Berman AW, Vatas U, et al. A prospective study of adjuvant CMF in males with node positive breast cancer: 20-year follow-up. Breast Cancer Res Treat 2007; 103(2): Giordano SH, Perkins GH, Broglio K, et al. Adjuvant systemic therapy for male breast carcinoma. Cancer 2005; 104(11): Yildirim E, Berberoglu U. Male breast cancer: a 22-year experience. Eur J Surg Oncol 1998; 24(6): Bloom HJ, Richardson WW. Histological grading and prognosis in breast cancer; a study of 1409 cases of which 359 have been followed for 15 years. Br J Cancer 1957; 11(3): Russo J, Frederick J, Ownby HE, et al. Predictors of recurrence and survival of patients with breast cancer. Am J Clin Pathol 1987; 88(2): Carter CL, Allen C, Henson DE. Relation of tumor size, lymph node status, and survival in 24,740 breast cancer cases. Cancer 1989; 63(1): Cianfrocca M, Goldstein LJ. Prognostic and predictive factors in early-stage breast cancer. Oncologist 2004; 9(6): Harris L, Fritsche H, Mennel R, et al. American Society of Clinical Oncology 2007 update of recommendations for the use of tumor markers in breast cancer. J Clin Oncol 2007; 25(33): Beckmann MW, Blohmer JU, Costa SD, et al. Zurich Consensus: German Expert Opinion on the St. Gallen Votes on 15 March 2009 (11th International Conference at St. Gallen: Primary Therapy of Early Breast Cancer). Breast Care (Basel) 2009; 4(2): Goldhirsch A, Ingle JN, Gelber RD, et al. Thresholds for therapies: highlights of the St Gallen International Expert Consensus on the primary therapy of early breast cancer Ann Oncol 2009; 20(8): Borgen PI, Senie RT, McKinnon WM, Rosen PP. Carcinoma of the male breast: analysis of prognosis compared with matched female patients. Ann Surg Oncol 1997; 4(5): Slamon DJ, Clark GM, Wong SG, et al. Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science 1987; 235(4785): Piccart-Gebhart MJ, Procter M, Leyland-Jones B, et al. Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. N Engl J Med 2005; 353(16):
62 58. Romond EH, Perez EA, Bryant J, et al. Trastuzumab plus adjuvant chemotherapy for operable HER2-positive breast cancer. N Engl J Med 2005; 353(16): Viani GA, Afonso SL, Stefano EJ, De Fendi LI, Soares FV. Adjuvant trastuzumab in the treatment of her-2-positive early breast cancer: a metaanalysis of published randomized trials. BMC Cancer 2007;7: Baselga J, Cortes J, Kim SB, et al. Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N Engl J Med 2012; 366(2): Cameron D, Casey M, Oliva C, et al. Lapatinib plus capecitabine in women with HER-2-positive advanced breast cancer: final survival analysis of a phase III randomized trial. Oncologist 2010; 15(9): Giordano SH, Buzdar AU, Hortobagyi GN. Breast cancer in men. Ann Intern Med 2002; 137(8): Rudlowski C, Friedrichs N, Faridi A, et al. Her-2/neu gene amplification and protein expression in primary male breast cancer. Breast Cancer Res Treat 2004; 84(3): Barlund M, Kuukasjarvi T, Syrjakoski K, Auvinen A, Kallioniemi A. Frequent amplification and overexpression of CCND1 in male breast cancer. Int J Cancer 2004; 111(6): Stratton MR, Campbell PJ, Futreal PA. The cancer genome. Nature 2009; 458(7239): Alizadeh AA, Eisen MB, Davis RE, et al. Distinct types of diffuse large B-cell lymphoma identified by gene expression profiling. Nature 2000; 403(6769): Nielsen TO, West RB, Linn SC, et al. Molecular characterisation of soft tissue tumours: a gene expression study. Lancet 2002; 359(9314): Kwei KA, Kung Y, Salari K, Holcomb IN, Pollack JR. Genomic instability in breast cancer: pathogenesis and clinical implications. Mol Oncol 2010; 4(3): Perou CM, Jeffrey SS, van de Rijn M, et al. Distinctive gene expression patterns in human mammary epithelial cells and breast cancers. Proc Natl Acad Sci U S A 1999; 96(16): Sorlie T, Tibshirani R, Parker J, et al. Repeated observation of breast tumor subtypes in independent gene expression data sets. Proc Natl Acad Sci U S A 2003; 100(14): Reis-Filho JS, Pusztai L. Gene expression profiling in breast cancer: classification, prognostication, and prediction. Lancet 2011; 378(9805): van 't Veer LJ, Dai H, van de Vijver MJ, et al. Gene expression profiling predicts clinical outcome of breast cancer. Nature 2002; 415(6871): Paik S, Shak S, Tang G, et al. A multigene assay to predict recurrence of tamoxifen-treated, node-negative breast cancer. N Engl J Med 2004; 351(27): Jonsson G, Staaf J, Vallon-Christersson J, et al. Genomic subtypes of breast cancer identified by array-comparative genomic hybridization display distinct molecular and clinical characteristics. Breast Cancer Res 2010; 12(3):R Carey LA, Perou CM, Livasy CA, et al. Race, breast cancer subtypes, and survival in the Carolina Breast Cancer Study. JAMA 2006; 295(21): Nielsen TO, Hsu FD, Jensen K, et al. Immunohistochemical and clinical characterization of the basal-like subtype of invasive breast carcinoma. Clin Cancer Res 2004; 10(16):
63 77. Dawood S, Hu R, Homes MD, et al. Defining breast cancer prognosis based on molecular phenotypes: results from a large cohort study. Breast Cancer Res Treat 2011; 126(1): Voduc KD, Cheang MC, Tyldesley S, et al. Breast cancer subtypes and the risk of local and regional relapse. J Clin Oncol 2010; 28(10): Callari M, Cappelletti V, De Cecco L, et al. Gene expression analysis reveals a different transcriptomic landscape in female and male breast cancer. Breast Cancer Res Treat Rudlowski C, Schulten HJ, Golas MM, et al. Comparative genomic hybridization analysis on male breast cancer. Int J Cancer 2006; 118(10): Ge Y, Sneige N, Eltorky MA, et al. Immunohistochemical characterization of subtypes of male breast carcinoma. Breast Cancer Res 2009; 11(3):R Kornegoor R, Verschuur-Maes AH, Buerger H, et al. Molecular subtyping of male breast cancer by immunohistochemistry. Mod Pathol Shaaban AM, Ball GR, Brannan RA, et al. A comparative biomarker study of 514 matched cases of male and female breast cancer reveals gender-specific biological differences. Breast Cancer Res Treat Allison KH, Kandalaft PL, Sitlani CM, Dintzis SM, Gown AM. Routine pathologic parameters can predict Oncotype DX recurrence scores in subsets of ER positive patients: who does not always need testing? Breast Cancer Res Treat 2012; 131(2): Williams DJ, Cohen C, Darrow M, et al. Proliferation (Ki-67 and phosphohistone H3) and oncotype DX recurrence score in estrogen receptorpositive breast cancer. Appl Immunohistochem Mol Morphol 2011; 19(5): Agarwal R, Gonzalez-Angulo AM, Myhre S, et al. Integrative analysis of cyclin protein levels identifies cyclin b1 as a classifier and predictor of outcomes in breast cancer. Clin Cancer Res 2009; 15(11): Ahlin C, Zhou W, Holmqvist M, et al. Cyclin A is a proliferative marker with good prognostic value in node-negative breast cancer. Cancer Epidemiol Biomarkers prev 2009; 18(9): Luporsi E, Andre F, Spyratos F, et al. Ki-67: level of evidence and methodological considerations for its role in the clinical management of breast cancer: analytical and critical review. Breast Cancer Res Treat Michalides R, van Tinteren H, Balkenende A, et al. Cyclin A is a prognostic indicator in early stage breast cancer with and without tamoxifen treatment. Br J Cancer 2002; 86(3): Nimeus-Malmstrom E, Koliadi A, Ahlin C, et al. Cyclin B1 is a prognostic proliferation marker with a high reproducibility in a population-based lymph node negative breast cancer cohort. Int J Cancer 2010; 127(4): Rudolph P, Kuhling H, Alm P, et al. Differential prognostic impact of the cyclins E and B in premenopausal and postmenopausal women with lymph node-negative breast cancer. Int J Cancer 2003; 105(5): de Azambuja E, Cardoso F, de Castro G, Jr., et al. Ki-67 as prognostic marker in early breast cancer: a meta-analysis of published studies involving 12,155 patients. Br J Cancer 2007; 96(10): Goldhirsch A, Wood WC, Coates AS, et al. Strategies for subtypes--dealing with the diversity of breast cancer: highlights of the St. Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer Ann Oncol 2011; 22(8):
64 94. Koliadi A, Nilsson C, Holmqvist M, et al. Cyclin B is an immunohistochemical proliferation marker which can predict for breast cancer death in low-risk node negative breast cancer. Acta Oncol. 95. Kuhling H, Alm P, Olsson H, et al. Expression of cyclins E, A, and B, and prognosis in lymph node-negative breast cancer. J Pathol 2003; 199(4): Span PN, Tjan-Heijnen VC, Manders P, Beex LV, Sweep CG. Cyclin-E is a strong predictor of endocrine therapy failure in human breast cancer. Oncogene 2003; 22(31): Sherr CJ. The Pezcoller lecture: cancer cell cycles revisited. Cancer Res 2000; 60(14): Cho EY, Choi YL, Han JJ, Kim KM, Oh YL. Expression and amplification of Her2, EGFR and cyclin D1 in breast cancer: immunohistochemistry and chromogenic in situ hybridization. Pathol Int 2008; 58(1): Colozza M, Azambuja E, Cardoso F, et al. Proliferative markers as prognostic and predictive tools in early breast cancer: where are we now? Ann Oncol 2005; 16(11): Rudas M, Lehnert M, Huynh A, et al. Cyclin D1 expression in breast cancer patients receiving adjuvant tamoxifen-based therapy. Clin Cancer Res 2008; 14(6): Stendahl M, Kronblad A, Ryden L, et al. Cyclin D1 overexpression is a negative predictive factor for tamoxifen response in postmenopausal breast cancer patients. Br J Cancer 2004; 90(10): Swedish Breast Cancer Group Rayson D, Erlichman C, Suman VJ, et al. Molecular markers in male breast carcinoma. Cancer 1998; 83(9): Wang-Rodriguez J, Cross K, Gallagher S, et al. Male breast carcinoma: correlation of ER, PR, Ki-67, Her2-Neu, and p53 with treatment and survival, a study of 65 cases. Mod Pathol 2002; 15(8): Kanthan R, Fried I, Rueckl T, Senger JL, Kanthan SC. Expression of cell cycle proteins in male breast carcinoma. World J Surg Oncol 2010; 8: Eaker S, Dickman PW, Hellstrom V, et al. Regional differences in breast cancer survival despite common guidelines. Cancer Epidemiol Biomarkers prev 2005; 14(12): Aaltonen K, Ahlin C, Amini RM, et al. Reliability of cyclin A assessment on tissue microarrays in breast cancer compared to conventional histological slides. Br J Cancer 2006; 94(11): Kyndi M, Sorensen FB, Knudsen H, et al. Tissue microarrays compared with whole sections and biochemical analyses. A subgroup analysis of DBCG 82 b&c. Acta Oncol 2008; 47(4): Vallon-Christersson J, Nordborg N, Svensson M, Hakkinen J. BASE--2nd generation software for microarray data management and analysis. BMC Bioinformatics 2009; 10: Staaf J, Jonsson G, Ringner M, Vallon-Christersson J. Normalization of array- CGH data: influence of copy number imbalances. BMC Genomics 2007; 8: Venkatraman ES, Olshen AB. A faster circular binary segmentation algorithm for the analysis of array CGH data. Bioinformatics 2007; 23(6): Beroukhim R, Getz G, Nghiemphu L, et al. Assessing the significance of chromosomal aberrations in cancer: methodology and application to glioma. Proc Natl Acad Sci U S A 2007; 104(50): Dickman PW, Sloggett A, Hills M, Hakulinen T. Regression models for relative survival. Stat Med 2004; 23(1):
65 114. Ahlin C, Aaltonen K, Amini RM, et al. Ki67 and cyclin A as prognostic factors in early breast cancer. What are the optimal cut-off values? Histopathology 2007; 51(4): The R Project for Statistical Computing [ Wang J, Kollias J, Marsh C, Maddern G. Are males with early breast cancer treated differently from females with early breast cancer in Australia and New Zealand? Breast 2009; 18(6): Cheang MC, Voduc D, Bajdik C, et al. Basal-like breast cancer defined by five biomarkers has superior prognostic value than triple-negative phenotype. Clin Cancer Res 2008; 14(5): Guidelines for breast cancer treatment in the region of Uppsala-Örebro; Cheang MC, Chia SK, Voduc D, et al. Ki67 index, HER2 status, and prognosis of patients with luminal B breast cancer. J Natl Cancer Inst 2009; 101(10): Desmedt C, Haibe-Kains B, Wirapati P, et al. Biological processes associated with breast cancer clinical outcome depend on the molecular subtypes. Clin Cancer Res 2008; 14(16): Bieche I, Girault I, Urbain E, Tozlu S, Lidereau R. Relationship between intratumoral expression of genes coding for xenobiotic-metabolizing enzymes and benefit from adjuvant tamoxifen in estrogen receptor alpha-positive postmenopausal breast carcinoma. Breast Cancer Res 2004; 6(3):R Pich A, Margaria E, Chiusa L. Proliferative activity is a significant prognostic factor in male breast carcinoma. Am J Pathol 1994; 145(2): Miglietta L, Vanella P, Canobbio L, et al. Prognostic value of estrogen receptor and Ki-67 index after neoadjuvant chemotherapy in locally advanced breast cancer expressing high levels of proliferation at diagnosis. Oncology 2010; 79(3-4): Lehn S, Tobin NP, Berglund P, et al. Down-regulation of the oncogene cyclin D1 increases migratory capacity in breast cancer and is linked to unfavorable prognostic features. Am J Pathol 2010; 177(6): Camp RL, Charette LA, Rimm DL. Validation of tissue microarray technology in breast carcinoma. Lab Invest 2000; 80(12): Gillett CE, Springall RJ, Barnes DM, Hanby AM. Multiple tissue core arrays in histopathology research: a validation study. J Pathol 2000; 192(4): Kononen J, Bubendorf L, Kallioniemi A, et al. Tissue microarrays for highthroughput molecular profiling of tumor specimens. Nat Med 1998; 4(7): Arendt LM, Schuler LA. Prolactin drives estrogen receptor-alpha-dependent ductal expansion and synergizes with transforming growth factor-alpha to induce mammary tumors in males. Am J Pathol 2008; 172(1): [ South Sweden Cancerome Analysis Network [ Uppsala-Umeå Comprehensive Cancer Consortium. 65
66
Your Guide to the Breast Cancer Pathology Report
 Your Guide to the Breast Cancer Pathology Report Developed for you by Breastcancer.org is a nonprofit organization dedicated to providing education and information on breast health and breast cancer. The
Your Guide to the Breast Cancer Pathology Report Developed for you by Breastcancer.org is a nonprofit organization dedicated to providing education and information on breast health and breast cancer. The
Male breast cancer - Wikipedia, the free encyclopedia
 pagina 1 van 5 Male breast cancer From Wikipedia, the free encyclopedia Male breast cancer is a relatively rare cancer in men that originates from the breast. As it presents a similar pathology as female
pagina 1 van 5 Male breast cancer From Wikipedia, the free encyclopedia Male breast cancer is a relatively rare cancer in men that originates from the breast. As it presents a similar pathology as female
Breast Cancer. The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer.
 Breast Cancer What Does the Pathology Report Say Normal Cells The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer. Non-Invasive
Breast Cancer What Does the Pathology Report Say Normal Cells The Pathology report gives an outline on direction of treatment. It tells multiple stories to help us understand the patient s cancer. Non-Invasive
www.downstatesurgery.org
 Male Breast Cancer Rabih Nemr MD Kings County Hospital August 2008 ACGME Core Competencies 1 Patient t Care Medical Knowledge 2 g 3 4 Practice Based Learning/Improvement Interpersonal Communication Skills
Male Breast Cancer Rabih Nemr MD Kings County Hospital August 2008 ACGME Core Competencies 1 Patient t Care Medical Knowledge 2 g 3 4 Practice Based Learning/Improvement Interpersonal Communication Skills
Breast Cancer: from bedside and grossing room to diagnoses and beyond. Adriana Corben, M.D.
 Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
Breast Cancer: from bedside and grossing room to diagnoses and beyond Adriana Corben, M.D. About breast anatomy Breasts are special organs that develop in women during puberty when female hormones are
Description of Procedure or Service. assays_of_genetic_expression_to_determine_prognosis_of_breast_cancer 11/2004 3/2015 3/2016 3/2015
 Corporate Medical Policy Assays of Genetic Expression to Determine Prognosis of Breast File Name: Origination: Last CAP Review: Next CAP Review: Last Review: assays_of_genetic_expression_to_determine_prognosis_of_breast_cancer
Corporate Medical Policy Assays of Genetic Expression to Determine Prognosis of Breast File Name: Origination: Last CAP Review: Next CAP Review: Last Review: assays_of_genetic_expression_to_determine_prognosis_of_breast_cancer
Your Guide to the Breast Cancer Pathology Report
 Your Guide to the Breast Cancer Pathology Report Developed for you by Breastcancer.org is a nonprofit organization dedicated to providing education and information on breast health and breast cancer. The
Your Guide to the Breast Cancer Pathology Report Developed for you by Breastcancer.org is a nonprofit organization dedicated to providing education and information on breast health and breast cancer. The
BREAST CANCER PATHOLOGY
 BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
BREAST CANCER PATHOLOGY FACT SHEET Version 4, Aug 2013 This fact sheet was produced by Breast Cancer Network Australia with input from The Royal College of Pathologists of Australasia I m a nurse and know
Outline. Workup for metastatic breast cancer. Metastatic breast cancer
 Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
Metastatic breast cancer Immunostain Update: Diagnosis of metastatic breast carcinoma, emphasizing distinction from GYN primary 1/3 of breast cancer patients will show metastasis 1 st presentation or 20-30
How To Use A Breast Cancer Test To Help You Choose Chemotherapy
 Gene expression profiling and expanded immunohistochemistry tests for guiding adjuvant chemotherapy decisions in early breast cancer management: MammaPrint, Oncotype DX, IHC4 and Mammostrat Issued: September
Gene expression profiling and expanded immunohistochemistry tests for guiding adjuvant chemotherapy decisions in early breast cancer management: MammaPrint, Oncotype DX, IHC4 and Mammostrat Issued: September
Chapter 2 Staging of Breast Cancer
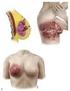 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Breast Cancer Treatment Guidelines
 Breast Cancer Treatment Guidelines DCIS Stage 0 TisN0M0 Tamoxifen for 5 years for patients with ER positive tumors treated with: -Breast conservative therapy (lumpectomy) and radiation therapy -Excision
Breast Cancer Treatment Guidelines DCIS Stage 0 TisN0M0 Tamoxifen for 5 years for patients with ER positive tumors treated with: -Breast conservative therapy (lumpectomy) and radiation therapy -Excision
Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy
 Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy W. Fraser Symmans, M.D. Associate Professor of Pathology UT M.D. Anderson Cancer Center Pathologic Complete Response (pcr) Proof
Pathologic Assessment Of The Breast And Axilla After Preoperative Therapy W. Fraser Symmans, M.D. Associate Professor of Pathology UT M.D. Anderson Cancer Center Pathologic Complete Response (pcr) Proof
Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too.
 Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Robert Bristow MD PhD FRCPC
 Robert Bristow MD PhD FRCPC Clinician-Scientist and Professor, Radiation Oncology and Medical Biophysics, University of Toronto and Ontario Cancer Institute/ (UHN) Head, PMH-CFCRI Prostate Cancer Research
Robert Bristow MD PhD FRCPC Clinician-Scientist and Professor, Radiation Oncology and Medical Biophysics, University of Toronto and Ontario Cancer Institute/ (UHN) Head, PMH-CFCRI Prostate Cancer Research
Changes in Breast Cancer Reports After Second Opinion. Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain
 Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Changes in Breast Cancer Reports After Second Opinion Dr. Vicente Marco Department of Pathology Hospital Quiron Barcelona. Spain Second Opinion in Breast Pathology Usually requested when a patient is referred
Prognostic and Predictive Factors in Oncology. Mustafa Benekli, M.D.
 Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
Understanding your pathology report
 Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Understanding your pathology report 2 Contents Contents Introduction 3 What is a pathology report? 3 Waiting for your results 4 What s in a pathology report? 4 Information about your breast cancer 5 What
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer
 Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer J.-L. Zhang, Q. Yao, J.-H. Chen,Y. Wang, H. Wang, Q. Fan, R. Ling, J. Yi and L. Wang Xijing Hospital Vascular Endocrine
Effects of Herceptin on circulating tumor cells in HER2 positive early breast cancer J.-L. Zhang, Q. Yao, J.-H. Chen,Y. Wang, H. Wang, Q. Fan, R. Ling, J. Yi and L. Wang Xijing Hospital Vascular Endocrine
HER2 Testing in Breast Cancer
 HER2 Testing in Breast Cancer GAIL H. VANCE, M.D. AGT MEETING JUNE 13, 2014 LOUISVILLE, KENTUCKY No Conflict of Interest to Report Human Epidermal Growth Factor Receptor 2-HER2 Human epidermal growth factor
HER2 Testing in Breast Cancer GAIL H. VANCE, M.D. AGT MEETING JUNE 13, 2014 LOUISVILLE, KENTUCKY No Conflict of Interest to Report Human Epidermal Growth Factor Receptor 2-HER2 Human epidermal growth factor
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
SAMO FoROMe Post-ESMO 2013 Breast Cancer
 SAMO FoROMe Post-ESMO 2013 Breast Cancer Dr. med. Manuela Rabaglio Klinik und Poliklinik für Medizinische Onkologie Breast Cancer Track 300 Abstracts 142 Poster 11 Proffered paper 4 late breaking news
SAMO FoROMe Post-ESMO 2013 Breast Cancer Dr. med. Manuela Rabaglio Klinik und Poliklinik für Medizinische Onkologie Breast Cancer Track 300 Abstracts 142 Poster 11 Proffered paper 4 late breaking news
Breast Cancer Educational Program. June 5-6, 2015
 Breast Cancer Educational Program June 5-6, 2015 Adjuvant Systemic Therapy For Early Breast Cancer: Who, What and for How Long? Debjani Grenier MD, FRCPC Medical Oncologist Disclosures Advisory Board Member:
Breast Cancer Educational Program June 5-6, 2015 Adjuvant Systemic Therapy For Early Breast Cancer: Who, What and for How Long? Debjani Grenier MD, FRCPC Medical Oncologist Disclosures Advisory Board Member:
HER2 Status: What is the Difference Between Breast and Gastric Cancer?
 Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
PROGNOSIS AND PREDICTIVE FACTORS IN HUMAN BREAST CANCER DURING TUMOR PROGRESSION. Eva Karlsson
 From THE DEPARTMENT OF ONCOLOGY-PATHOLOGY Karolinska Institutet, Stockholm, Sweden PROGNOSIS AND PREDICTIVE FACTORS IN HUMAN BREAST CANCER DURING TUMOR PROGRESSION Eva Karlsson Stockholm 2014 . Published
From THE DEPARTMENT OF ONCOLOGY-PATHOLOGY Karolinska Institutet, Stockholm, Sweden PROGNOSIS AND PREDICTIVE FACTORS IN HUMAN BREAST CANCER DURING TUMOR PROGRESSION Eva Karlsson Stockholm 2014 . Published
Male Breast Cancer Edward Yu, MD PhD, FRCPC. Department of Oncology, Western University, London, Ontario, Canada
 1 Male Breast Cancer Edward Yu, MD PhD, FRCPC. Department of Oncology, Western University, London, Ontario, Canada Epidemiology Male breast cancer (MBC) is a rare disease worldwide. MBC accounts for approximately
1 Male Breast Cancer Edward Yu, MD PhD, FRCPC. Department of Oncology, Western University, London, Ontario, Canada Epidemiology Male breast cancer (MBC) is a rare disease worldwide. MBC accounts for approximately
Cellular, Molecular, and Biochemical Targets in Breast Cancer
 Cellular, Molecular, and Biochemical Targets in Breast Cancer Kristy Kummerow Ingrid Meszoely December 12, 2012 VUMC Resident Bonus Conference One size fits all surgical treatment of breast cancer Wilhelm
Cellular, Molecular, and Biochemical Targets in Breast Cancer Kristy Kummerow Ingrid Meszoely December 12, 2012 VUMC Resident Bonus Conference One size fits all surgical treatment of breast cancer Wilhelm
HAVE YOU BEEN NEWLY DIAGNOSED with DCIS?
 HAVE YOU BEEN NEWLY DIAGNOSED with DCIS? Jen D. Mother and volunteer. Diagnosed with DCIS breast cancer in 2012. An educational guide prepared by Genomic Health This guide is designed to educate women
HAVE YOU BEEN NEWLY DIAGNOSED with DCIS? Jen D. Mother and volunteer. Diagnosed with DCIS breast cancer in 2012. An educational guide prepared by Genomic Health This guide is designed to educate women
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Effect of Chemotherapy for Luminal A Breast Cancer
 Yonago Acta medica 2013;56:51 56 Original Article Effect of Chemotherapy for Luminal A Breast Cancer Naotaka Uchida,* Takako Suda and Kiyosuke Ishiguro *Clinic of Surgery, Tottori Prefectural Kosei Hospital,
Yonago Acta medica 2013;56:51 56 Original Article Effect of Chemotherapy for Luminal A Breast Cancer Naotaka Uchida,* Takako Suda and Kiyosuke Ishiguro *Clinic of Surgery, Tottori Prefectural Kosei Hospital,
Early-stage Breast Cancer Treatment: A Patient and Doctor Dialogue
 page 1 Early-stage Breast Cancer Treatment: A Patient and Doctor Dialogue Q: What is breast cancer, and what type do I have? A: Cancer is a disease in which cells become abnormal and form more cells in
page 1 Early-stage Breast Cancer Treatment: A Patient and Doctor Dialogue Q: What is breast cancer, and what type do I have? A: Cancer is a disease in which cells become abnormal and form more cells in
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Proportion of patients with invasive breast cancer in whom ER, PR and/or
 1.1.a. Proportion of patients with invasive breast cancer in whom ER, PR and/or HER2 status assessment were performed 1.1.b. Proportion of patients with invasive breast cancer in whom systemic treatment
1.1.a. Proportion of patients with invasive breast cancer in whom ER, PR and/or HER2 status assessment were performed 1.1.b. Proportion of patients with invasive breast cancer in whom systemic treatment
SECOND PRIMARY BREAST CANCERS FOLLOWING HAEMATOLOGIC MALIGNANCIES A CASE SERIES STUDY FARAH TANVEER PGY 3 DR.MEIR WETZLER DR.
 SECOND PRIMARY BREAST CANCERS FOLLOWING HAEMATOLOGIC MALIGNANCIES A CASE SERIES STUDY FARAH TANVEER PGY 3 DR.MEIR WETZLER DR. TRACEY O CONNOR RESEARCH QUESTON Patients with previously diagnosed hematologic
SECOND PRIMARY BREAST CANCERS FOLLOWING HAEMATOLOGIC MALIGNANCIES A CASE SERIES STUDY FARAH TANVEER PGY 3 DR.MEIR WETZLER DR. TRACEY O CONNOR RESEARCH QUESTON Patients with previously diagnosed hematologic
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Appendix One. HER2-positive early breast cancer, its treatment and prognosis
 Appendix One. HER2-positive early breast cancer, its treatment and prognosis Breast cancer and HER2/neu over-expression Health need is one of PHARMAC s nine decision criteria (http://www.pharmac.govt.nz/pdf/231205.pdf
Appendix One. HER2-positive early breast cancer, its treatment and prognosis Breast cancer and HER2/neu over-expression Health need is one of PHARMAC s nine decision criteria (http://www.pharmac.govt.nz/pdf/231205.pdf
Hereditary Multifocal Breast Cancer. Farin Amersi M.D., F.A.C.S Division of Surgical Oncology Department of Surgery Cedar Sinai Medical Center
 Hereditary Multifocal Breast Cancer Farin Amersi M.D., F.A.C.S Division of Surgical Oncology Department of Surgery Cedar Sinai Medical Center CASE STUDY 30 year old Ashkenazi Jewish woman Nulliparous Felt
Hereditary Multifocal Breast Cancer Farin Amersi M.D., F.A.C.S Division of Surgical Oncology Department of Surgery Cedar Sinai Medical Center CASE STUDY 30 year old Ashkenazi Jewish woman Nulliparous Felt
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Receptor conversion in distant breast cancer metastases. Breast cancer metastases: A spitting image of their primary?
 Receptor conversion in distant breast cancer metastases Breast cancer metastases: A spitting image of their primary? Introduction Breast cancer is the leading cause of female cancer death worldwide (13,000
Receptor conversion in distant breast cancer metastases Breast cancer metastases: A spitting image of their primary? Introduction Breast cancer is the leading cause of female cancer death worldwide (13,000
Impact of radiation therapy on survival in patients with triple negative breast cancer
 548 Impact of radiation therapy on survival in patients with triple negative breast cancer LAUREN T. STEWARD 1, FENG GAO 2, MARIE A. TAYLOR 3 and JULIE A. MARGENTHALER 1 1 Department of Surgery; 2 Division
548 Impact of radiation therapy on survival in patients with triple negative breast cancer LAUREN T. STEWARD 1, FENG GAO 2, MARIE A. TAYLOR 3 and JULIE A. MARGENTHALER 1 1 Department of Surgery; 2 Division
Patient Guide to Breast Cancer Surgery and Treatment
 Patient Guide to Breast Cancer Surgery and Treatment Coree H. Flight attendant and mother of 3. Diagnosed with invasive breast cancer in 2009. An educational guide prepared by Genomic Health This Is Your
Patient Guide to Breast Cancer Surgery and Treatment Coree H. Flight attendant and mother of 3. Diagnosed with invasive breast cancer in 2009. An educational guide prepared by Genomic Health This Is Your
Modern Staging in Primary Breast Cancer
 Bulletin No. 143 from Department of Surgery, Clinical Sciences Lund, Lund University, Sweden, 2013 Modern Staging in Primary Breast Cancer Aspects of micrometastatic disease in bone marrow and molecular
Bulletin No. 143 from Department of Surgery, Clinical Sciences Lund, Lund University, Sweden, 2013 Modern Staging in Primary Breast Cancer Aspects of micrometastatic disease in bone marrow and molecular
Genomic Medicine The Future of Cancer Care. Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America
 Genomic Medicine The Future of Cancer Care Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America Personalized Medicine Personalized health care is a broad term for interventions
Genomic Medicine The Future of Cancer Care Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America Personalized Medicine Personalized health care is a broad term for interventions
Breast cancer: Diagnosis and complex treatment. Ibolya Czegle MD PhD Semmelweis University 3rd Department of Internal Medicine
 Breast cancer: Diagnosis and complex treatment Ibolya Czegle MD PhD Semmelweis University 3rd Department of Internal Medicine Epidemiology Worldwide, breast cancer is the most frequently diagnosed life-threatening
Breast cancer: Diagnosis and complex treatment Ibolya Czegle MD PhD Semmelweis University 3rd Department of Internal Medicine Epidemiology Worldwide, breast cancer is the most frequently diagnosed life-threatening
One of the most mature trials that examined PROCEEDINGS. Hormone Therapy in Postmenopausal Women With Breast Cancer * William J.
 Hormone Therapy in Postmenopausal Women With Breast Cancer * William J. Gradishar, MD ABSTRACT *Based on a presentation given by Dr Gradishar at a roundtable symposium held in Baltimore on June 28, 25.
Hormone Therapy in Postmenopausal Women With Breast Cancer * William J. Gradishar, MD ABSTRACT *Based on a presentation given by Dr Gradishar at a roundtable symposium held in Baltimore on June 28, 25.
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
BioPATH: A Study of Biomarker Profiles in Asia Pacific HER2 Breast Cancer Patients Treated with Lapatinib and Other Anti-HER2 Therapy
 BioPATH: A Study of Biomarker Profiles in Asia Pacific HER2 Breast Cancer Patients Treated with Lapatinib and Other Anti-HER2 Therapy Soonmyung Paik 1 ; Gyungyub Gong 2 ; Yap Yoon Sim 3 ; Tae- You Kim
BioPATH: A Study of Biomarker Profiles in Asia Pacific HER2 Breast Cancer Patients Treated with Lapatinib and Other Anti-HER2 Therapy Soonmyung Paik 1 ; Gyungyub Gong 2 ; Yap Yoon Sim 3 ; Tae- You Kim
Chemotherapy or Not? Anthracycline or Not? Taxane or Not? Does Density Matter? Chemotherapy in Luminal Breast Cancer: Choice of Regimen.
 Chemotherapy in Luminal Breast Cancer: Choice of Regimen Andrew D. Seidman, MD Attending Physician Breast Cancer Medicine Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Cornell
Chemotherapy in Luminal Breast Cancer: Choice of Regimen Andrew D. Seidman, MD Attending Physician Breast Cancer Medicine Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Cornell
Breast Cancer. Presentation by Dr Mafunga
 Breast Cancer Presentation by Dr Mafunga Breast cancer in the UK Breast cancer is the second most common cancer in women. Around 1 in 9 women will develop breast cancer It most commonly affects women over
Breast Cancer Presentation by Dr Mafunga Breast cancer in the UK Breast cancer is the second most common cancer in women. Around 1 in 9 women will develop breast cancer It most commonly affects women over
Adjuvant Therapy for Breast Cancer: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Adjuvant Therapy for Breast
MALE BREAST CANCER - CASE REPORT AND BRIEF REVIEW
 Middle East Journal of Family Medicine, 2004; Vol. 6 (6) MALE BREAST CANCER - CASE REPORT AND BRIEF REVIEW Elias A Sarru', MD, MS, AAFP, ABFP Family Physician, Al Hasa Primary Care Services Division Faysal
Middle East Journal of Family Medicine, 2004; Vol. 6 (6) MALE BREAST CANCER - CASE REPORT AND BRIEF REVIEW Elias A Sarru', MD, MS, AAFP, ABFP Family Physician, Al Hasa Primary Care Services Division Faysal
Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis?
 Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis? Erin I. Lewis, BUSM 2010 Cheri Nguyen, BUSM 2008 Priscilla Slanetz, M.D., MPH Al Ozonoff, Ph.d.
Breast cancer close to the nipple: Does this carry a higher risk ofaxillary node metastasesupon diagnosis? Erin I. Lewis, BUSM 2010 Cheri Nguyen, BUSM 2008 Priscilla Slanetz, M.D., MPH Al Ozonoff, Ph.d.
Tumour Markers. What are Tumour Markers? How Are Tumour Markers Used?
 Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
Dr. Anthony C.H. YING What are? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer cells or
What is Cancer? Cancer is a genetic disease: Cancer typically involves a change in gene expression/function:
 Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Cancer is a genetic disease: Inherited cancer Sporadic cancer What is Cancer? Cancer typically involves a change in gene expression/function: Qualitative change Quantitative change Any cancer causing genetic
Loco-regional Recurrence
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer AGO AGO e. e. V. V. Loco-regional Recurrence Loco-regional Recurrence Version 2002: Brunnert / Simon Versions 2003 2012: Audretsch
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer AGO AGO e. e. V. V. Loco-regional Recurrence Loco-regional Recurrence Version 2002: Brunnert / Simon Versions 2003 2012: Audretsch
Breast Cancer in Men. What is cancer?
 What is cancer? Breast Cancer in Men The body is made up of trillions of living cells. Normal body cells grow, divide into new cells, and die in an orderly way. During the early years of a person's life,
What is cancer? Breast Cancer in Men The body is made up of trillions of living cells. Normal body cells grow, divide into new cells, and die in an orderly way. During the early years of a person's life,
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs. Case Study. Surgery. Lumpectomy and Radiation
 Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
Current Status and Perspectives of Radiation Therapy for Breast Cancer
 Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
Breast Cancer Current Status and Perspectives of Radiation Therapy for Breast Cancer JMAJ 45(10): 434 439, 2002 Masahiro HIRAOKA, Masaki KOKUBO, Chikako YAMAMOTO and Michihide MITSUMORI Department of Therapeutic
micrornas Non protein coding, endogenous RNAs of 21-22nt length Evolutionarily conserved
 microrna 2 micrornas Non protein coding, endogenous RNAs of 21-22nt length Evolutionarily conserved Regulate gene expression by binding complementary regions at 3 regions of target mrnas Act as negative
microrna 2 micrornas Non protein coding, endogenous RNAs of 21-22nt length Evolutionarily conserved Regulate gene expression by binding complementary regions at 3 regions of target mrnas Act as negative
Breakthrough Treatment Options for Breast Cancer
 Breakthrough Treatment Options for Breast Cancer Guest Expert: Lyndsay, MD Associate Professor of Medical Oncology, Yale Cancer Center www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center
Breakthrough Treatment Options for Breast Cancer Guest Expert: Lyndsay, MD Associate Professor of Medical Oncology, Yale Cancer Center www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center
Breast Cancer. CSC Cancer Experience Registry Member, breast cancer
 ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
ESSENTIALS Breast Cancer Take things one step at a time. Try not to be overwhelmed by the tidal wave of technical information coming your way. Finally you know your body best; you have to be your own advocate.
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER
 GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER Author: Dr Susan O Reilly On behalf of the Breast CNG Written: December 2008 Agreed at CNG: June 2009 & June 2010 Review due: June 2011 Guidelines Adjuvant Systemic
GUIDELINES ADJUVANT SYSTEMIC BREAST CANCER Author: Dr Susan O Reilly On behalf of the Breast CNG Written: December 2008 Agreed at CNG: June 2009 & June 2010 Review due: June 2011 Guidelines Adjuvant Systemic
BREAST CANCER AWARENESS FOR WOMEN AND MEN by Samar Ali A. Kader. Two years ago, I was working as a bedside nurse. One of my colleagues felt
 Ali A. Kader, S. (2010). Breast cancer awareness for women and men. UCQ Nursing Journal of Academic Writing, Winter 2010, 70 76. BREAST CANCER AWARENESS FOR WOMEN AND MEN by Samar Ali A. Kader Two years
Ali A. Kader, S. (2010). Breast cancer awareness for women and men. UCQ Nursing Journal of Academic Writing, Winter 2010, 70 76. BREAST CANCER AWARENESS FOR WOMEN AND MEN by Samar Ali A. Kader Two years
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 [email protected] Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials)
 ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Guide to Understanding Breast Cancer
 An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
CHROMOSOMES Dr. Fern Tsien, Dept. of Genetics, LSUHSC, NO, LA
 CHROMOSOMES Dr. Fern Tsien, Dept. of Genetics, LSUHSC, NO, LA Cytogenetics is the study of chromosomes and their structure, inheritance, and abnormalities. Chromosome abnormalities occur in approximately:
CHROMOSOMES Dr. Fern Tsien, Dept. of Genetics, LSUHSC, NO, LA Cytogenetics is the study of chromosomes and their structure, inheritance, and abnormalities. Chromosome abnormalities occur in approximately:
Breast Cancer & Treatment in ACT and Surrounding Regions QUALITY ASSURANCE PROJECT. Five-year report
 Breast Cancer & Treatment in ACT and Surrounding Regions QUALITY ASSURANCE PROJECT Five-year report Community Health Pathology Southern Area Health Service ACT Health General Practitioners Nurses Social
Breast Cancer & Treatment in ACT and Surrounding Regions QUALITY ASSURANCE PROJECT Five-year report Community Health Pathology Southern Area Health Service ACT Health General Practitioners Nurses Social
Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns
 July 2013 Edition Vol. 7, Issue 7 Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns By Julie Katz, MPH, MPhil Biomarkers played a prominent role in the research presented in
July 2013 Edition Vol. 7, Issue 7 Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns By Julie Katz, MPH, MPhil Biomarkers played a prominent role in the research presented in
Prognostic and Predictive Factors in Breast Cancer Kyle T. Bradley, MD, MS CAP Cancer Committee
 Prognostic and Predictive Factors in Breast Cancer Kyle T. Bradley, MD, MS CAP Cancer Committee Breast cancer is the most common malignant tumor in American women and is second only to lung cancer as a
Prognostic and Predictive Factors in Breast Cancer Kyle T. Bradley, MD, MS CAP Cancer Committee Breast cancer is the most common malignant tumor in American women and is second only to lung cancer as a
Understanding Your Surgical Options For Breast Cancer
 RADIATION THERAPY SYMPTOM MANAGEMENT CANCER INFORMATION Understanding Your Surgical Options For Breast Cancer In this booklet you will learn about: Role of surgery in breast cancer diagnosis and treatment
RADIATION THERAPY SYMPTOM MANAGEMENT CANCER INFORMATION Understanding Your Surgical Options For Breast Cancer In this booklet you will learn about: Role of surgery in breast cancer diagnosis and treatment
Helen Joseph Breast Care Clinic - Johannesburg, South Africa
 - Johannesburg, South Africa General Information New breast cancer cases treated per year 360 Breast multidisciplinarity team members 12 Radiologists, surgeons, pathologists, medical oncologists, radiotherapists
- Johannesburg, South Africa General Information New breast cancer cases treated per year 360 Breast multidisciplinarity team members 12 Radiologists, surgeons, pathologists, medical oncologists, radiotherapists
Nancy E. Davidson, MD Johns Hopkins University. Breast Cancer
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
CHAPTER 2: UNDERSTANDING CANCER
 CHAPTER 2: UNDERSTANDING CANCER INTRODUCTION We are witnessing an era of great discovery in the field of cancer research. New insights into the causes and development of cancer are emerging. These discoveries
CHAPTER 2: UNDERSTANDING CANCER INTRODUCTION We are witnessing an era of great discovery in the field of cancer research. New insights into the causes and development of cancer are emerging. These discoveries
Breast Cancer. Treatment Guidelines for Patients
 Breast Cancer Treatment Guidelines for Patients Version IX/ July 2007 Current ACS-NCCN Treatment Guidelines for Patients Advanced Cancer and Palliative Care Treatment Guidelines for Patients (English and
Breast Cancer Treatment Guidelines for Patients Version IX/ July 2007 Current ACS-NCCN Treatment Guidelines for Patients Advanced Cancer and Palliative Care Treatment Guidelines for Patients (English and
Breast Cancer Awareness Month
 Aon Kenya Insurance Brokers Ltd Aon Hewitt Healthcare Division Breast Cancer Awareness Month Issue 12 October 2015 In this Issue 2 Cancer Statistics in Kenya 3 What is Breast Cancer? 4 Symptoms of Breast
Aon Kenya Insurance Brokers Ltd Aon Hewitt Healthcare Division Breast Cancer Awareness Month Issue 12 October 2015 In this Issue 2 Cancer Statistics in Kenya 3 What is Breast Cancer? 4 Symptoms of Breast
Invasive lobular breast cancer
 Invasive lobular breast cancer This booklet is about invasive lobular breast cancer. It describes what invasive lobular breast cancer is, the symptoms, how it s diagnosed and possible treatments. Diagnosed
Invasive lobular breast cancer This booklet is about invasive lobular breast cancer. It describes what invasive lobular breast cancer is, the symptoms, how it s diagnosed and possible treatments. Diagnosed
http://www.springer.com/3-540-22006-2
 http://www.springer.com/3-540-22006-2 1 Molecular Pathology Laboratory of the Future Christopher A. Moskaluk 1.1 The Past The integration of laboratory analysis with human medicine has traditionally been
http://www.springer.com/3-540-22006-2 1 Molecular Pathology Laboratory of the Future Christopher A. Moskaluk 1.1 The Past The integration of laboratory analysis with human medicine has traditionally been
Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma
 The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
The Use of Kinase Inhibitors: Translational Lab Results Targeting Specific Cell Signaling Pathways for the Treatment of Malignant Peritoneal Mesothelioma Sheelu Varghese, Ph.D. H. Richard Alexander, M.D.
Breast Imaging Made Brief and Simple. Jane Clayton MD Associate Professor Department of Radiology LSUHSC New Orleans, LA
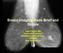 Breast Imaging Made Brief and Simple Jane Clayton MD Associate Professor Department of Radiology LSUHSC New Orleans, LA What women are referred for breast imaging? Two groups of women are referred for
Breast Imaging Made Brief and Simple Jane Clayton MD Associate Professor Department of Radiology LSUHSC New Orleans, LA What women are referred for breast imaging? Two groups of women are referred for
