Clinical Recommendations for Treatment of Bipolar Disorder for Hong Kong 2013
|
|
|
- Dinah Osborne
- 10 years ago
- Views:
Transcription
1 Clinical Recommendations for Treatment of Bipolar Disorder for Hong Kong 2013 Version: March 2013
2 Objectives of Treatment Rapid control of symptoms especially agitation, impulsivity, aggression, suicidality and psychotic features Regain pre-morbid functioning Establish maintenance regime and prevention of relapse, rapid cycling or switch NB: The following recommendations are mainly based on the most updated Canadian guidelines, with valuable comments from advisors of SABAD & fellow psychiatrists, though other sources are sometimes referred
3 Specific Issues for Hong Kong When there are a number of choices for 1st-line treatment, 2nd-line or 3rd-line recommendations will usually be omitted These recommendations are tailored for specialists and also primary care doctors with special interests in management of bipolar patients Thus there is a word of caution in the use of some medications with toxic side-effects, especially by nonspecialists The rational choice of medication should also be based also on tolerability, symptomatology, comorbidities & other relevant factors
4 Limitations of Guidelines Not absolute, especially those arrived by consensus May not be applicable in some clinical situations (e.g. with atypical & complicated cases) Individual differences in response May restrict or discourage innovations Conflicts exist between different guidelines Cultural variations e.g. dosage, economic restrictions, etc. should be considered
5 Levels of Evidence Levels of evidence: Level 1: meta-analysis or replicated Double-Blind Randomised Controlled Trial that includes a placebo Level 2: at least 1 DB-RCT with placebo or active comparison Level 3: prospective uncontrolled trial with 10 or more subjects Level 4: anecdotal reports or expert opinion First line Rx: level 1 & level 2 evidence plus clinical support for efficacy & safety Second line Rx: level 3 or higher evidence plus clinical support for efficacy & safety Ref: CANMAT 2007
6 Baseline Assessment History: personal history (s/- of hypomania, substance abuse); family history (bipolar disorders, CVD, DM) Cigarette & alcohol intake Pregnancy & contraception (women of childbearing age) Physical exam: blood pressure, body weight, waist circumference, BMI Laboratory tests: CBC, electrolytes, RFT, LFT, metabolic screening (fasting glucose & fasting lipid profile) & ECG; TFT & pregnancy test if clinically indicated
7 I. Acute Mania Criteria or manic episode: 1 week elevated or irritable mood (with marked impairment of functioning); with or without psychotic features Criteria for hypomania: at least 4 days of elevated, expansive or irritable mood (not sever enough to cause marked impairment of functioning) 3 or more manic symptoms Mixed states Rapid cycling
8 Acute Manic or Mixed Episode 1st line Rx is monotherapy with: Lithium*, sodium valproate (CR or ER), olanzapine, risperidone, quetiapine (IR or XR), aripiprazole, ziprasidone, asenapine, paliperidone ER Lithium* or sodium valproate + risperidone, quetiapine, olanzapine, aripiprazole, asenapine switch to another or combination of two 1st-line agent Parental injections of atypical antipsychotics can be used for very severe mania or agitation* * to be used with caution, especially by non-specialists NB: Monotherapy with gabapentin, topiramate, lamotrigine, verapamil, tiagabine, OR risperidone or olanzapine + carbamazepine not recommended
9 II. Acute Bipolar Depression More disabling than mania Misdiagnosis as unipolar depression Two types: bipolar I & II depression
10 Acute Bipolar I Depression 1st-line Rx Lithium*, OR Lamotrigine; OR Quetiapine (IR or XR); OR Lithium* or sodium valproate + SSRI; OR Olanzapine + SSRI (especially fluoxetine); OR Lithium* + sodium valproate; OR Lithium* or sodium valproate + bupropion Switch to another choice in 1st-line NB: Gabapentin, aripiprazole, ziprasidone monotherapy; adjunctive ziprasidone or levetiracetaim not recommended * to be used with caution, especially by non-specialists
11 Acute Bipolar II Depression 1st-line: Quetiapine (IR or XR) 2nd-line: lithium*; OR lamotrigine; OR sodium valproate; lithium* or sodium valproate + antidepressants; OR lithium* + sodium valproate; OR atypical antipsychotics + antidepressants** * to be used with caution, especially by non-specialists ** careful longitudinal history taken before antidepressant monotherapy
12 III. Maintenance Treatment At least 2 episodes of mania or depression (including current episode) within 2 years (Grof & Angst) 2 major episodes of mania &/or depression, irrespective of frequency (Goodwin & Jamison) Single manic episode or both hypomanic and depressive episode. Also consider past suicidal attempts, psychotic episodes and functional disability associated with episodes (NIMH consensus development panel guidelines) Adopted from Australian & New Zealand Clinical Practice Guideline (2004) NB: There is currently a trend to provide maintenance therapy after one single severe episode.
13 Maintenance Therapy for BP I Lithium*; OR Quetiapine; OR Lamotrigine (limited efficacy for preventing manias); OR Valproate; OR Olanzapine; OR Risperidone long-acting injection; OR Aripiprazole Adjunctive lithium or valproate, quetiapine, risperidone long-acting injection (prevent mania), ziprasidone, aripiprazole * to be used with caution, especially by non-specialists NB: Monotherapy with gabapentin, topiramate, antidepressants not recommended
14 Maintenance Treatment for BP II 1st-line: Lithium*; OR lamotrigine; 2nd-line: sodium valproate; OR Lithium* or sodium valproate or atypical antipsychotic + antidepressant; OR Combination of 2 of following: Lithium*, lamotrgine, sodium valproate or atypical antipsychotic * to be used with caution, especially by non-specialists NB: Gabapentin not recommended
15 Maintenance of Rapid Cyclers 1st-line: Lithium*; OR sodium valproate** 2nd line: Lithium* + sodium valproate; OR Lithium* + carbamazepine; OR Lithium* or sodium valproate + lamotrigine; OR Olanzapine NB: Antidepressants not recommended * to be used with caution, especially by non-specialists ** not fully confirmed to-date
16 Maintenance of Mixed States Olanzapine OR Ziprasidone; OR Adjunctive risperidone
17 IV. Special Patient Population (1) Pregnant women No evidence of risk: clozapine Risk cannot be ruled out: gabapentin, topiramate, olanzapine, risperidone, quetiapine, ziprasidone Positive evidence of risk: lithium, sodium valproate, carbamazepine, lamotrigine Electro-convulsive therapy may be considered NB: Omit medications if possible in first trimester because of teratogenic risk; abrupt withdrawal runs the risk of relapse
18 Special Patient Population (2) Breast feeding women With caution: lithium (with monitoring for complete blood picture or CBP, hypotonia, psoriasis, lethargy & cyanosis in infants) Possible: sodium valproate, carbamazepine (monitoring for hepatotoxicity & haematological toxicity especially in infants) Unknown: benzodiazepine, SSRI, antipsychotics, lamotrigine Minimum effective dose is needed, avoid polypharmacy, and breastfeed before taking medications
19 Medications During Breastfeeding Valproate & carbamazepine are usually considered safe (though side-effects in infants have been reported) Lithium should not be prescribed Other anticonvulsants not recommended because of insufficient data
20 Special Population (3) Paediatric patients Lithium; OR Valproate; OR Olanzapine, quetiapine, ziprasidone, risperidone*, aripiprazole Quetiapine + divalproex Oxycarbazepine not effective *FDA for aged 10 or above NB: Evidence based on at least 1 double-blind RCT with placebo or active comparator
21 V. Rx of Psychiatric Comorbidities Panic disorder: Selective Serotonin Reuptake Inhibitors (SSRIs) better than tricyclics antidepressants (TCAs) Obsessive-compulsive disorder (lower prevalence than Major depressive disorder): SSRIs better than clomipramine Body dysmorphic disorder: SSRIs + atypical antipsychotics Substance abuse (poor compliance): Serotonin Reuptake Inhibitors (SRIs +/- atypical antipsychotics
22 Rx of Physical Comorbidities Obesity, metabolic syndrome & diabetes mellitus: avoid those medications which greatly increase body weight Hypertension & cardiac disorder: not contraindicated except for Lithium given diuretics Migraine: may be aggravated by SRIs NB: Beware of drug-drug interactions between psychotropics & medications prescribed for medical diseases
23 Drugs That Do Not Work (So Far) Bipolar mania Level 1 evidence: lamotrigine, topiramate Level 2 evidence: gabapentin, verapamil, Lithium or sodium valproate + ziprasidone; adjunctive lamotrigine Bipolar depression Level 2 evidence: gabapentin
24 Psychosocial Therapies Often as adjunct to pharmacotherapy Psychoeducation Cognitive behaviour therapy (CBT) Interpersonal psychotherapy (IPT) Interpersonal & Social Rhythm Therapy (ISRT) NB: Beware of burden of care on caregivers
25 Electro-convulsive Therapy 2 nd line for acute mania Otherwise last resort especially for psychotic depression, acute mania with delirium, catatonia or stuporose Fast effect if strong suicidal risk Medications still needed most of the time Pregnancy, when medications are not suitable or contra-indicated NB: Preferably done in hospital, with assistance from an anesthesiologist
26 Monitoring AED (1) Carbamazepine: serum level q3 months (17-50umol/l); liver & renal function tests q3-6 months; complete blood picture q3-6months (then annually); review oral contraceptive efficacy Valproate: serum level q3 months ( umol/l); liver function test q3-6 months; complete blood picture q3-6 months; enquire menstrual changes for women of reproductive age q3months for 1 st year (then annually) NB: 2 levels to establish therapeutic dose (separated by 4 weeks for CPZ)
27 Monitoring AED (2) Lithium: serum level at steady state (>5 days of starting) until 2 within therapeutic range*; at steady state after every dose change; then q3 months & as clinically indicated calcium level, thyroid stimulating hormone & renal function test q6-12 months Weight q6-12 months *NICE: 0.8 mmol/l, less efficacy for NB: If CPZ + lamotrigine: concern over skin eruptions; if CPZ + valproate: advice on bone health
28 Serious Side-effects of AEDs Boxed warning: Lithium: neurotoxicity Valproate*: hepatotoxicity, pancreatitis, teratogenicity Carbamazepine: rash**, blood dyscrasia Lamotrigine: rash** * caution in childbearing women, should provide contraceptive advice ** advise to avoid use of new perfumes, detergents or other household chemicals, etc.
29 Monitoring Atypical Antipsychotics Personal & family history of cardiac & metabolic problems Weight, blood pressure q3m Fasting glucose & lipid profile q3-12m, then annually ECG if indicated (QTc)* Prolactin level if indicated NB: If on clozapine: check CBP regularly; olanzapine can interact with cigarette smoking * normal value: <430 (male); <450 (female)
30 Use of Antidepressants Not useful for BP I or psychotic depression Maybe useful for BP II depression, perhaps as an adjunct to mood stabilizers Risk of rapid cycling Risk of hypo/manic switch still controversial AD of increasing risk: SSRIs < NDRI < SNRIs & TCAs Close monitoring of mood change needed
31 Discontinuation of Long-term Rx Following discontinuation of medicines, the risk of relapse remains, even after years of sustained remission. Discontinuation of any medicine should normally be tapered over at least 2 weeks and preferably longer Relapse to mania is an early risk of abrupt lithium discontinuation. NB: Discontinuation of medicines should not be equated with withdrawal of services.
32 Consult or Refer Consult or refer to senior colleague or specialist when there is No clinical improvement, frequent relapses, or worsening of mental condition after adequate trial of 1 (or at most 2) 1st-line medications: adequate dosage for an adequate period of time (4 to 8 weeks) Danger to self or to others (include offences) Complicated by substance abuse, personality disorders, eating disorders, etc. Unmanageable physical comorbidity
33 Conclusion The above recommendations are for guidance only Clinical judgment (with reasons) remains the key element in management Not to be distributed without prior approval from SABAD The present version would be updated from time to time & is available at the SABAD s website: Feedback from users of these clinical guidelines are welcome
34 Highlights of UK NICE Guidelines (2006) Caution in diagnosis of mania in prepubertal children Concerns about use of valproate in women of reproductive potential (risk of polycystic ovary) Highlights diabetes/metabolic problems with olanzapine But recommends lithium, olanzapine & valproate for maintenance Ref:
35 Key References Yatham LN, Kennedy SH, Schaffer A et al (2013) Canadian Network for Mood & Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update 2013, Bipolar Disorders, 15, 1-44 Ng, F, Mammen, K, Wilting, I et al (2009) the ISBD consensus guidelines for the safety monitoring of bipolar disorder treatments. Bipolar Disorders, 11, Royal Australian & New Zealand College of Psychiatrists Clinical Practice Guidelines Team for Bipolar Disorder. Australian & New Zealand Journal Psychiatry, 2004, 38,
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Medications for bipolar disorder
 Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Bipolar Disorder Practice Guidelines for Adults
 Bipolar Disorder Practice Guidelines for Adults Introduction PerformCare s condensed guidelines for the treatment of Bipolar Disorder are derived from the American Psychiatric Association (APA) Guidelines
Bipolar Disorder Practice Guidelines for Adults Introduction PerformCare s condensed guidelines for the treatment of Bipolar Disorder are derived from the American Psychiatric Association (APA) Guidelines
Improving the Recognition and Treatment of Bipolar Depression
 Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
CLINICIAN INTERVIEW COMPLEXITIES OF BIPOLAR DISORDER. Interview with Charles B. Nemeroff, MD, PhD
 COMPLEXITIES OF BIPOLAR DISORDER Interview with Charles B. Nemeroff, MD, PhD Dr Nemeroff is the Reunette W. Harris Professor and Chairman of the Department of Psychiatry and Behavioral Sciences at Emory
COMPLEXITIES OF BIPOLAR DISORDER Interview with Charles B. Nemeroff, MD, PhD Dr Nemeroff is the Reunette W. Harris Professor and Chairman of the Department of Psychiatry and Behavioral Sciences at Emory
Psychopharmacology. Psychopharmacology. Hamish McAllister-Williams Reader in Clinical. Department of Psychiatry, RVI
 Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Suicide in Bipolar Disorder. Julie Anderson, MD Oregon State Hospital Psychiatrist OHSU Assistant Professor September 25, 2012
 Suicide in Bipolar Disorder Julie Anderson, MD Oregon State Hospital Psychiatrist OHSU Assistant Professor September 25, 2012 Disclosure Statement I have no significant financial relationships to disclose...
Suicide in Bipolar Disorder Julie Anderson, MD Oregon State Hospital Psychiatrist OHSU Assistant Professor September 25, 2012 Disclosure Statement I have no significant financial relationships to disclose...
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Bipolar Disorder. MOH Clinical Practice Guidelines 5/2011. Singapore Medical Association. Academy of Medicine, Singapore
 Bipolar Disorder MOH Clinical Practice Guidelines 5/2011 College of Family Physicians, Singapore Academy of Medicine, Singapore Singapore Medical Association November 2011 Levels of evidence and grades
Bipolar Disorder MOH Clinical Practice Guidelines 5/2011 College of Family Physicians, Singapore Academy of Medicine, Singapore Singapore Medical Association November 2011 Levels of evidence and grades
TREATING BIPOLAR DISORDER
 TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. 1 For Continuing Medical
TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. 1 For Continuing Medical
Bipolar disorder. Understanding NICE guidance
 Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Understanding NICE guidance Information for people who use NHS services Bipolar disorder NICE clinical guidelines advise the NHS on caring for people with specific conditions or diseases and the treatments
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Bipolar disorder. The management of bipolar disorder in adults, children and adolescents, in primary and secondary care
 Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
Issue date: July 2006 Bipolar disorder The management of bipolar disorder in adults, children and adolescents, in primary and secondary care NICE clinical guideline 38 Developed by the National Collaborating
A Manic Episode is defined by a distinct period during which there is an abnormally and persistently elevated, expansive, or irritable mood.
 Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Bipolar disorder Bipolar (manic-depressive illness) is a recurrent mode disorder. The patient may feel stable at baseline level but experience recurrent shifts to an emotional high (mania or hypomania)
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
TREATMENT-RESISTANT DEPRESSION AND ANXIETY
 University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS. Juanaelena Garcia, MD Psychiatry Director Institute for Family Health
 PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
New Treatments. For Bipolar Disorder. Po W. Wang, MD Clinical Associate Professor Bipolar Disorders Clinic Stanford University School of Medicine
 New Treatments For Bipolar Disorder Po W. Wang, MD Clinical Associate Professor Bipolar Disorders Clinic Stanford University School of Medicine Abbott Laboratories AstraZeneca Bristol-Myers Squibb Corcept
New Treatments For Bipolar Disorder Po W. Wang, MD Clinical Associate Professor Bipolar Disorders Clinic Stanford University School of Medicine Abbott Laboratories AstraZeneca Bristol-Myers Squibb Corcept
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS
 BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
BIPOLAR DISORDER A GUIDE FOR INDIVIDUALS AND FAMILIES FOR THE TREATMENT OF BIPOLAR DISORDER IN ADULTS A publication of the Massachusetts Department of Mental Health and the Massachusetts Division of Medical
TREATING BIPOLAR DISORDER
 TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. A guideline watch,
TREATING BIPOLAR DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition, originally published in April 2002. A guideline watch,
Psychopharmacotherapy for Children and Adolescents
 TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
Treatment of Patients With Bipolar Disorder Second Edition
 PRACTICE GUIDELINE FOR THE Treatment of Patients With Bipolar Disorder Second Edition WORK GROUP ON BIPOLAR DISORDER Robert M.A. Hirschfeld, M.D., Chair Charles L. Bowden, M.D. Michael J. Gitlin, M.D.
PRACTICE GUIDELINE FOR THE Treatment of Patients With Bipolar Disorder Second Edition WORK GROUP ON BIPOLAR DISORDER Robert M.A. Hirschfeld, M.D., Chair Charles L. Bowden, M.D. Michael J. Gitlin, M.D.
PSYCHOTROPIC MEDICATIONS
 PSYCHOTROPIC MEDICATIONS 644.3 Bipolar Disorder This Instructor s Guide contains: Brief Description, Objectives, Discussion Questions, Pretest, Post-test, Answer Keys and Glossary for this program, Psychotropic
PSYCHOTROPIC MEDICATIONS 644.3 Bipolar Disorder This Instructor s Guide contains: Brief Description, Objectives, Discussion Questions, Pretest, Post-test, Answer Keys and Glossary for this program, Psychotropic
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource
 E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
E-Resource March, 2015 DEPRESSION Depression Assessment PHQ-9 Screening tool Depression treatment Treatment flow chart Medications Patient Resource Depression affects approximately 20% of the general population
Antipsychotic Medications and the Risk of Diabetes and Cardiovascular Disease
 Antipsychotic Medications and the Risk of Diabetes and Cardiovascular Disease Professional Tool #1: Screening and Monitoring in a High-Risk Population: Questions and Answers Overview of Cardiometabolic
Antipsychotic Medications and the Risk of Diabetes and Cardiovascular Disease Professional Tool #1: Screening and Monitoring in a High-Risk Population: Questions and Answers Overview of Cardiometabolic
North of Tyne Area Prescribing Committee
 North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
North of Tyne Area Prescribing Committee ANTIPSYCHOTICS IN PSYCHOSIS, BIPOLAR DISORDER AND AUGMENTATION THERAPY IN TREATMENT RESISTANT DEPRESSION Information for Primary Care Updated November 2013 This
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Preconception Clinical Care for Women Medical Conditions
 Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Preconception Clinical Care for Women All women of reproductive age are candidates for preconception care; however, preconception care must be tailored to meet the needs of the individual. Given that preconception
Best Practices Patient Monitoring Parameters for Mood Stabilizers*
 Best Practices Patient Monitoring Parameters for Mood Stabilizers* All Mood Stabilizers Baseline 6 months Annually As Clinically General Physical Assessment (blood pressure, heart rate, height, weight,
Best Practices Patient Monitoring Parameters for Mood Stabilizers* All Mood Stabilizers Baseline 6 months Annually As Clinically General Physical Assessment (blood pressure, heart rate, height, weight,
American Psychiatric Association
 Practice Guideline for the Treatment of Patients With Bipolar Disorder (Revision) American Psychiatric Association Originally published in April 2002. A guideline watch, summarizing significant developments
Practice Guideline for the Treatment of Patients With Bipolar Disorder (Revision) American Psychiatric Association Originally published in April 2002. A guideline watch, summarizing significant developments
Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole)
 EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
EMA/303592/2015 Summary of the risk management plan (RMP) for Aripiprazole Pharmathen (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Pharmathen, which details the measures
ATYPICALS ANTIPSYCHOTIC MEDICATIONS
 The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
There are four groups of medications most likely to be used for depression: Antidepressants Antipsychotics Mood stabilisers Augmenting agents.
 What this fact sheet covers: Physical treatments (medication, ECT and TMS) Psychological treatments Self-help & alternative therapies Key points to remember Where to get more information. Introduction
What this fact sheet covers: Physical treatments (medication, ECT and TMS) Psychological treatments Self-help & alternative therapies Key points to remember Where to get more information. Introduction
GMMMG Interface Prescribing Subgroup. Shared Care Template
 GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
GMMMG Interface Prescribing Subgroup Shared Care Template Shared Care Guideline for Selective Serotonin Reuptake Inhibitors (SSRIs) for the treatment of Obsessive Compulsive Disorder (OCD) and Body Dysmorphic
Barriers to Healthcare Services for People with Mental Disorders. Cardiovascular disorders and diabetes in people with severe mental illness
 Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
Barriers to Healthcare Services for People with Mental Disorders Cardiovascular disorders and diabetes in people with severe mental illness Dr. med. J. Cordes LVR- Klinikum Düsseldorf Kliniken der Heinrich-Heine-Universität
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Antidepressants in Pregnancy D R S N E H A P A R G H I
 Antidepressants in Pregnancy D R S N E H A P A R G H I Overview Depression and its effects Antidepressants and their effects Birth defects Miscarriage Neonatal withdrawal Longterm consequences Breastfeeding
Antidepressants in Pregnancy D R S N E H A P A R G H I Overview Depression and its effects Antidepressants and their effects Birth defects Miscarriage Neonatal withdrawal Longterm consequences Breastfeeding
Treatments for Major Depression. Drug Treatments The two (2) classes of drugs that are typical antidepressants are:
 Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
FACT SHEET 4. Bipolar Disorder. What Is Bipolar Disorder?
 FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
FACT SHEET 4 What Is? Bipolar disorder, also known as manic depression, affects about 1 percent of the general population. Bipolar disorder is a psychiatric disorder that causes extreme mood swings that
Practice guideline for the treatment of patients with bipolar disorder (revision).
 Brief Summary GUIDELINE TITLE Practice guideline for the treatment of patients with bipolar disorder (revision). BIBLIOGRAPHIC SOURCE(S) Practice guideline for the treatment of patients with bipolar disorder
Brief Summary GUIDELINE TITLE Practice guideline for the treatment of patients with bipolar disorder (revision). BIBLIOGRAPHIC SOURCE(S) Practice guideline for the treatment of patients with bipolar disorder
DEMENTIA EDUCATION & TRAINING PROGRAM
 The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
The pharmacological management of aggression in the nursing home requires careful assessment and methodical treatment to assure maximum safety for patients, nursing home residents and staff. Aggressive
Overview of Mental Health Medication Trends
 America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Symptoms of mania can include: 3
 Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
Bipolar Disorder This factsheet gives information on bipolar disorder. It explains the symptoms of bipolar disorder, treatments and ways to manage symptoms. It also covers what treatment the National Institute
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA
 COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
COMPREHENSIVE MANAGEMENT OF THE ELDERLY PATIENT WITH MANIA Manic depressive illness is a biological brain disorder that produces significant alterations of mood and psychosis. Mania in the elderly occurs
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services
 Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D.
 DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D. GOALS Learn DSM 5 criteria for DMDD Understand the theoretical background of DMDD Discuss background, pathophysiology and treatment
DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D. GOALS Learn DSM 5 criteria for DMDD Understand the theoretical background of DMDD Discuss background, pathophysiology and treatment
Canadian Network for Mood and Anxiety Treatments (CANMAT) guidelines for the management of patients with bipolar disorder: consensus and controversies
 Bipolar Disorders 2005: 7(Suppl. 3): 5 69 Copyright ª Blackwell Munksgaard 2005 BIPOLAR DISORDERS Canadian Network for Mood and Anxiety Treatments (CANMAT) guidelines for the management of patients with
Bipolar Disorders 2005: 7(Suppl. 3): 5 69 Copyright ª Blackwell Munksgaard 2005 BIPOLAR DISORDERS Canadian Network for Mood and Anxiety Treatments (CANMAT) guidelines for the management of patients with
Medical marijuana for pain and anxiety: A primer for methadone physicians. Meldon Kahan MD CPSO Methadone Prescribers Conference November 6, 2015
 Medical marijuana for pain and anxiety: A primer for methadone physicians Meldon Kahan MD CPSO Methadone Prescribers Conference November 6, 2015 Conflict of interest statement No conflict of interest to
Medical marijuana for pain and anxiety: A primer for methadone physicians Meldon Kahan MD CPSO Methadone Prescribers Conference November 6, 2015 Conflict of interest statement No conflict of interest to
Recognizing and Treating Depression in Children and Adolescents.
 Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
Chronic mental illness in LTCF. Chronic mental illness. Other psychiatric disorders.
 Chronic mental illness in LTCF Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Chronic mental illness 1. Schizophrenia and Schizoaffective disorder. 2. Bipolar disorder (Type 1 and
Chronic mental illness in LTCF Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Chronic mental illness 1. Schizophrenia and Schizoaffective disorder. 2. Bipolar disorder (Type 1 and
Steven Bander, DO, FACOFP Bander Family Medical Center Wylie, Texas
 Bipolar Disorder: Lessons for Rural Physicians: Adjunctive Interventions for Maintaining Remission Steven Bander, DO, FACOFP Bander Family Medical Center Wylie, Texas Disclosure Nothing to disclose Objectives
Bipolar Disorder: Lessons for Rural Physicians: Adjunctive Interventions for Maintaining Remission Steven Bander, DO, FACOFP Bander Family Medical Center Wylie, Texas Disclosure Nothing to disclose Objectives
The following is a sample of psychotropic drug warnings that drug regulatory agencies
 Chronology of International Drug Regulatory Agency Warnings about Psychotropic Drugs The following is a sample of psychotropic drug warnings that drug regulatory agencies around the world have issued.
Chronology of International Drug Regulatory Agency Warnings about Psychotropic Drugs The following is a sample of psychotropic drug warnings that drug regulatory agencies around the world have issued.
Major Depressive Disorder:
 Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Depre r s e sio i n o i n i a dults Yousuf Al Farsi
 Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Depression in adults Yousuf Al Farsi Objectives 1. Aetiology 2. Classification 3. Major depression 4. Screening 5. Differential diagnosis 6. Treatment approach 7. When to refer 8. Complication 9. Prognosis
Shared Care Protocol for Atypical Antipsychotics
 Shared Care Protocol for Atypical Antipsychotics Version Number: 2 Name of originator/author: Chief Pharmacist, 07813 783165 (with thanks to GMW) Name of responsible committee: Clinical Governance Committee
Shared Care Protocol for Atypical Antipsychotics Version Number: 2 Name of originator/author: Chief Pharmacist, 07813 783165 (with thanks to GMW) Name of responsible committee: Clinical Governance Committee
A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES
 INTRODUCTION A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES Individuals with intellectual disabilities are not uncommonly prescribed psychotropic medications.
INTRODUCTION A BRIEF OVERVIEW OF PSYCHOTROPIC MEDICATION USE FOR PERSONS WITH INTELLECTUAL DISABILITIES Individuals with intellectual disabilities are not uncommonly prescribed psychotropic medications.
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Bipolar Disorder: Advances in Psychotherapy
 Bipolar Disorder: Advances in Psychotherapy Questions from chapter 1 1) Which is characterized by one or more major depressive episodes with at least one hypomanic episode in which the patient s functioning
Bipolar Disorder: Advances in Psychotherapy Questions from chapter 1 1) Which is characterized by one or more major depressive episodes with at least one hypomanic episode in which the patient s functioning
Irritability and DSM-5 Disruptive Mood Dysregulation Disorder (DMDD): Correlates, predictors, and outcome in children
 Irritability and DSM-5 Disruptive Mood Dysregulation Disorder (DMDD): Correlates, predictors, and outcome in children Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders National Institute
Irritability and DSM-5 Disruptive Mood Dysregulation Disorder (DMDD): Correlates, predictors, and outcome in children Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders National Institute
Psychotic Disorder. Psychosis. Psychoses may be caused by: Examples of Hallucinations and Delusions 12/12/2012
 Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: [email protected] Web: www.psywellness.com.sg A condition
Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: [email protected] Web: www.psywellness.com.sg A condition
Major Depression. What is major depression?
 Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
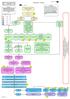 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR. 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014
 COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
COUNTY OF LOS ANGELES - DEPARTMENT OF MENTAL HEALTH OFFICE OF THE MEDICAL DIRECTOR 3.4 PARAMETERS FOR THE USE OF ANXIOLYTIC MEDICATIONS October 2014 I. GENERAL CONSIDERATIONS A. Definition: Anxiolytic
TEXAS MEDICATION ALGORITHM PROJECT PROCEDURAL MANUAL
 TEXAS MEDICATION ALGORITHM PROJECT PROCEDURAL MANUAL BIPOLAR DISORDER ALGORITHMS M. Lynn Crismon, PharmD, BCPP Tami R. Argo, PharmD, MS, BCPP Sherrie D. Bendele, BS Trisha Suppes, MD, PhD 2007, Texas Department
TEXAS MEDICATION ALGORITHM PROJECT PROCEDURAL MANUAL BIPOLAR DISORDER ALGORITHMS M. Lynn Crismon, PharmD, BCPP Tami R. Argo, PharmD, MS, BCPP Sherrie D. Bendele, BS Trisha Suppes, MD, PhD 2007, Texas Department
Feeling Moody? Major Depressive. Disorder. Is it just a bad mood or is it a disorder? Mood Disorders. www.seclairer.com S Eclairer 724-468-3999
 Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Feeling Moody? Is it just a bad mood or is it a disorder? Major Depressive Disorder Prevalence: 7%; 18-29 years old; Female>Male DDx: Manic episodes with irritable mood or mixed episodes, mood disorder
Eating Disorder Treatment Protocol
 Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
PTSD Evidence Based Practice Recommendations
 PTSD Evidence ased Practice Recommendations Jason's ox est Practice Group Dr. Sam Moreno, Michelle Schnack Compilation & consolidation of the research and recommendations located in: The VA/DoD Clinical
PTSD Evidence ased Practice Recommendations Jason's ox est Practice Group Dr. Sam Moreno, Michelle Schnack Compilation & consolidation of the research and recommendations located in: The VA/DoD Clinical
Obsessive Compulsive Disorder: a pharmacological treatment approach
 Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
BIPOLAR DISORDER IN PRIMARY CARE
 E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
E-Resource January, 2014 BIPOLAR DISORDER IN PRIMARY CARE Mood Disorder Questionnaire Common Comorbidities Evaluation of Patients with BPD Management of BPD in Primary Care Patient resource Patients with
Depression. The treatment and management of depression in adults. This is a partial update of NICE clinical guideline 23
 Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
Issue date: October 2009 Depression The treatment and management of depression in adults This is a partial update of NICE clinical guideline 23 NICE clinical guideline 90 Developed by the National Collaborating
I. The Positive Symptoms...Page 2. The Negative Symptoms...Page 2. Primary Psychiatric Conditions...Page 2
 SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Bipolar Disorder: What s the Difference & What s New?
 Bipolar Disorder: What s the Difference & What s New? Rex S. Lott, Pharm.D., BCPP Professor, Idaho State University College of Pharmacy Mental Health Clinical Pharmacist, Boise VA Medical Center Clinical
Bipolar Disorder: What s the Difference & What s New? Rex S. Lott, Pharm.D., BCPP Professor, Idaho State University College of Pharmacy Mental Health Clinical Pharmacist, Boise VA Medical Center Clinical
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Treating Children with Anxiety and Bipolar Disorder. Ellen Leibenluft, M.D.
 Treating Children with Anxiety and Bipolar Disorder Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders Emotion and Development Branch National Institute of Mental Health National Institutes
Treating Children with Anxiety and Bipolar Disorder Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders Emotion and Development Branch National Institute of Mental Health National Institutes
What is Bipolar Disorder?
 What is Bipolar Disorder? We all get excited by new ideas, pursue our goals with passion, have times when we want to party with our friends and enjoy life to its fullest. There will also be times when
What is Bipolar Disorder? We all get excited by new ideas, pursue our goals with passion, have times when we want to party with our friends and enjoy life to its fullest. There will also be times when
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Eating Disorders: Anorexia Nervosa and Bulimia Nervosa Preferred Practice Guideline
 Introduction Eating Disorders are described as severe disturbances in eating behavior which manifest as refusal to maintain a minimally normal body weight (Anorexia Nervosa) or repeated episodes of binge
Introduction Eating Disorders are described as severe disturbances in eating behavior which manifest as refusal to maintain a minimally normal body weight (Anorexia Nervosa) or repeated episodes of binge
