Managing Complications of Antireflux and Bariatric Surgery
|
|
|
- Brendan Sherman
- 10 years ago
- Views:
Transcription
1 GASTROENTEROLOGY BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, GROUP PUBLISHER Bruce M. White EDITORIAL DIRECTOR Debra Dreger SENIOR EDITOR Becky Krumm ASSISTANT EDITOR Rita E. Gould EXECUTIVE VICE PRESIDENT Barbara T. White EXECUTIVE DIRECTOR OF OPERATIONS Jean M. Gaul PRODUCTION DIRECTOR Suzanne S. Banish PRODUCTION ASSOCIATE Mary Beth Cunney ADVERTISING/PROJECT MANAGER Patricia Payne Castle SALES & MARKETING MANAGER Deborah D. Chavis NOTE FROM THE PUBLISHER: This publication has been developed without involvement of or review by the American Board of Internal Medicine. Endorsed by the Association for Hospital Medical Education The Association for Hospital Medical Education endorses HOSPITAL PHYSICIAN for the purpose of presenting the latest developments in medical education as they affect residency programs and clinical hospital practice. Managing Complications of Antireflux and Bariatric Surgery Series Editor: Robert M. Craig, MD Professor of Medicine, Division of Gastroenterology, Department of Medicine, The Feinberg School of Medicine, Northwestern University Chicago, IL Contributors: John E. Pandolfino, MD Assistant Professor of Medicine, Division of Gastroenterology, Department of Medicine, The Feinberg School of Medicine, Northwestern University, Chicago, IL Alexander P. Nagle, MD Assistant Professor of Surgery, Division of General Surgery, The Feinberg School of Medicine, Northwestern University, Chicago, IL Table of Contents Introduction Antireflux Surgery Bariatric Surgery References Cover Illustration by Christine Armstrong Copyright 2003, Turner White Communications, Inc., 125 Strafford Avenue, Suite 220, Wayne, PA , All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or by any means, mechanical, electronic, photocopying, recording, or otherwise, without the prior written permission of Turner White Communications, Inc. The editors are solely responsible for selecting content. Although the editors take great care to ensure accuracy, Turner White Communications, Inc., will not be liable for any errors of omission or inaccuracies in this publication. Opinions expressed are those of the authors and do not necessarily reflect those of Turner White Communications, Inc. Gastroenterology Volume 9, Part 4 1
2 GASTROENTEROLOGY BOARD REVIEW MANUAL Managing Complications of Antireflux and Bariatric Surgery John E. Pandolfino, MD, and Alexander P. Nagle, MD INTRODUCTION Over the past decade, the number of laparoscopic procedures performed for 2 very common medical problems gastroesophageal reflux disease (GERD) and obesity has exploded. As a result, the management of postoperative side effects and complications of these surgeries has become an increasingly important aspect of gastroenterology practice. GERD is a disorder that affects 40 million people in the United States, 1 and for patients with chronic GERD, antireflux surgery is an important therapeutic option. Many patients are opting for surgical intervention for GERD in place of lifelong medical therapy. Along similar lines, obesity has reached epidemic proportions in the United States; the National Institutes of Health (NIH) recommends that for patients with severe obesity, gastric restrictive or bypass surgery be considered as a treatment option. 2 This monograph uses a case-based format to review laparoscopic surgical procedures for the treatment of GERD and obesity. Indications for surgery, as well as the potential complications of the procedures, are discussed. ANTIREFLUX SURGERY OVERVIEW OF GERD GERD encompasses all clinical disorders that result from reflux of gastric juice into the esophagus. GERD is a common disorder, with 7% of the US population experiencing daily symptoms and 14% experiencing weekly symptoms. 1 The clinical presentation varies widely, ranging from endoscopy-negative disease with significant reflux symptoms (eg, heartburn, regurgitation, dysphagia, extraesophageal symptoms) to reflux esophagitis and its complications (eg, peptic stricture, Barrett s metaplasia). The pathophysiology of GERD involves a balance between those factors tending to injure the esophageal epithelium and those tending to preserve it. Reflux events are prevented by a competent esophagogastric junction; however, this barrier can be overcome by transient lower esophageal sphincter (LES) relaxations, prolonged episodes of LES hypotension, and anatomic disruption secondary to hiatus hernia. Most cases of GERD can be diagnosed based on symptom assessment and empiric trials with high-dose proton pump inhibitor (PPI) therapy. Endoscopy should be performed if the diagnosis is in doubt or when heartburn is extremely severe or has been chronic. Patients with intermittent mild GERD can be treated with over-the-counter antacids or H 2 -blockers; patients with esophagitis and symptoms more frequently than 3 times weekly typically require PPI therapy. An ideal therapy for GERD would target the pathophysiologic abnormalities, obviating the need for acid suppression. Unfortunately, no medication is currently available that can restore the antireflux barrier. Antireflux surgery was developed to address these pathophysiologic abnormalities and may improve reflux by increasing basal pressure of the high-pressure zone and decreasing the frequency of transient LES relaxations. Some studies report long-term success rates of greater than 90% over 10 to 20 years after open fundoplication; others, however, have described return of esophagitis in 50% of cases within 6 years. 3 Whether surgery is as good or better than medical therapy with PPIs is difficult to ascertain at this time because the data comparing longterm PPI therapy to open and laparoscopic fundoplication is controversial. Antireflux surgery may be considered in the following settings: (1) failed medical therapy with persistent symptomatic esophagitis and stricture; (2) failed medical therapy with persistent symptoms and an abnormal ph study; (3) successful medical therapy in a patient who is young and healthy but is unwilling to take lifelong medication; and (4) severe symptoms caused by regurgitation. Because of the risks inherent to surgery, the decision to pursue medical or surgical therapy must include a careful risk-benefit analysis. 2 Hospital Physician Board Review Manual
3 ANTIREFLUX PROCEDURES Although many operations have been devised to control reflux, most are of historical significance only. Before laparoscopic techniques were widely available, the 3 most common procedures performed were the Nissen fundoplication, the Belsey Mark IV repair, and the Hill posterior gastropexy. The most commonly performed operations currently are the laparoscopic Nissen fundoplication (360 degree) and the Toupet fundoplication (270 degree). Regardless of which procedure is performed, the surgical goals are the same. The essential features are to mobilize the lower esophagus and reposition the LES back into the abdominal cavity, reduce and repair the hiatal defect (if present), and lengthen and strengthen the high-pressure zone by wrapping the fundus around the esophagus. During the operation, the fundus is first mobilized by taking down the short gastric blood vessels. A 1- to 2-cm plication is made, wrapping the fundus around the distal esophagus, and sutures are placed to secure the wrap to the esophagus and stomach. In addition, the disruption in the crural diaphragm is repaired if present. Figure 1 illustrates the completed operation. A preoperative work-up consisting of at least an upper endoscopy and manometric evaluation is essential to confirm the presence of GERD prior to surgery. Upper endoscopy is performed to document the presence of esophagitis and its complications and also to assess the size of the hiatal hernia (if present) as this may affect surgical outcome. Manometry is performed to rule out other possible etiologies, such as achalasia and other esophageal motor abnormalities, that also may present with heartburn, regurgitation, and chest pain. 4 Evaluation of effective peristaltic function is unnecessary because peristaltic function is not correlated with postoperative symptoms or operative success. 5 For patients presenting with atypical symptoms or symptoms not responding to antisecretory therapy, ambulatory ph monitoring is indicated to provide objective evidence that abnormal acid reflux exists and that the symptoms are associated with reflux. CASE 1 PRESENTATION The patient is a 50-year-old woman with a history of severe heartburn and regurgitation for the past 5 years. Approximately 2 years ago, she had an esophagogastroduodenoscopy (EGD) that revealed a large hiatal hernia (10 cm) and long-segment Barrett s esophagus. She was placed on double-dose PPI therapy and her heartburn improved, but she continued to have severe regurgitation. After failure to improve on quadruple-dose PPI therapy, the patient was referred for laparoscopic Nissen fundoplication, which was performed 2 months Figure 1. Normal results of fundoplication surgery. ago. Postoperatively, she experienced some mild dysphagia that resolved. She was doing well until 4 weeks ago, when severe heartburn and chest pain returned. Over the past 2 weeks she also has noted significant odynophagia and mild dysphagia. She denies any nausea or vomiting; however, her oral intake has decreased secondary to pain and she has lost 10 lb since the surgery. She denies experiencing fever, chills, diaphoresis, or shortness of breath. What is the differential diagnosis for postoperative symptoms? Surgical data reveal that reflux recurs in approximately 3% of patients at 1 year and 8% at 10 years. 4 In addition, a follow-up study on a large Veterans Affairs population randomized to medical or surgical therapy revealed that up to 62% of the surgical patients were taking medications on a regular basis for GERD. 3 Typically, postoperative fundoplication symptoms are either recurrent symptoms or new symptoms related to the procedure itself. Recurrent or continued symptoms may be the result of either surgical failure or incorrect diagnosis. Incorrect diagnosis may occur when patients are referred for symptoms without objective evidence of GERD or a good response to medical therapy. This situation may be prevented by careful patient selection and by performing a preoperative work-up consisting of an upper endoscopy, manometric evaluation, and ambulatory ph monitoring, if indicated. Continued or recurrent symptoms also may be related to disruption or slippage of an intact fundoplication or poor wrap construction. Most patients with a disrupted wrap (Figure 2) respond to antisecretory therapy if a response was noted preoperatively. If these patients symptoms persist, most experts recommend continued PPI therapy because reoperation is associated with Gastroenterology Volume 9, Part 4 3
4 Figure 2. Appearance of a disrupted fundoplication wrap. Figure 3. Appearance of classic (left) and partial (right) slippage of fundoplication. decreased efficacy (70% 80%) and increased mortality (> 1%). 4 Patients with a slipped fundoplication (Figure 3) also present with recurrent symptoms; these patients may present with dysphagia, depending on the position of the wrap. 6 Slippage describes a condition whereby part of the stomach resides above the wrap. It may be the result of intussusception of the stomach through the wrap or incorrect placement of the wrap around the stomach instead of the distal esophagus. The portion of the stomach that has slipped through the wrap may be located above or below the diaphragm. Location below the diaphragm is the classic slipped Nissen. 6 Reflux occurs secondary to partial disruption of the wrap and, when the slipped portion is above the diaphragm, the recurrence of a hiatal hernia. Endoscopically, the squamocolumnar junction (SCJ) is noted to be proximal to the wrap with a hiatus hernia. Retroflexion may demonstrate an intact fundoplication; therefore, a barium esophagram should be obtained to more clearly define the anatomy. A barium esophagram will reveal gastric folds above the wrap and can confirm whether herniation through the crural diaphragm has occurred. Patients at high risk for slippage are those with a large hiatal hernia, peptic stricturing, or esophageal shortening. These patients could require extensive mediastinal mobilization of the esophagus and/or a lengthening procedure such as a Collis gastroplasty. What is the appropriate work-up for this patient? Patients with recurrent symptoms should be referred for either a barium esophagram or upper endoscopy to assess the integrity of the fundoplication. Either procedure is appropriate in most patients; if dysphagia is present, however, barium esophagram should be obtained to rule out a paraesophageal hernia. Findings on esophagram that suggest a disrupted wrap are: (1) hiatal hernia, (2) filling of the wrap, and (3) loss of the pseudomass. Endoscopy also can provide information regarding the integrity of the wrap, especially if there is complete disruption and herniation. Typically, the SCJ should reside within the wrap or less than 1 cm proximal to the wrap zone. On retroflexed view, the gastric folds should be parallel to the diaphragm and should create a 2- to 3-cm thickened fundic ring around the scope (Figure 1). In a patient with recurring symptoms whose wrap appears intact on endoscopy or barium esophagram, further testing may be warranted. An empiric trial with a double-dose PPI regimen is often extremely helpful, and many patients responding to medical management will opt to continue rather than undergo additional surgery. If empiric PPI therapy is not successful and reoperation is contemplated, a 24-hour ambulatory ph monitoring study should be performed to provide objective evidence of abnormal acid reflux. CASE 1 RESOLUTION The patient is referred for EGD. The findings reveal a disrupted wrap with recurrence of axial hiatal hernia. In addition, there is recurrence of a Barrett s ulcer at the esophagogastric junction. Given this failure, the patient is referred to a thoracic surgeon for reoperation (fundoplication) and an esophageal lengthening procedure. CASE 2 PRESENTATION The patient is a 40-year-old woman who underwent a laparoscopic Nissen fundoplication 1 year ago for severe regurgitation and heartburn. Her preoperative EGD revealed a small (3 cm) axial hiatal hernia with 4 Hospital Physician Board Review Manual
5 Figure 4. Appearance of a tight fundoplication wrap (left). On endoscopic examination, a tight wrap may resemble pseudoachalasia (right). Figure 5. Appearance of a disrupted fundoplication with a paraesophageal hernia. mild esophagitis. Although her response to PPI therapy was excellent, she was intolerant owing to severe diarrhea despite switching medications several times. She did well postoperatively except for early satiety, which had been chronic, and some mild gas bloat symptoms. She now presents with a 2-day history of severe dysphagia and is unable to tolerate any food. In addition, she complains of severe midepigastric pain. Her physical examination reveals tachycardia with a pulse of 112 bpm, stable blood pressure, and a respiratory rate of 24 breaths/min. She is afebrile and in moderate distress. Her abdominal examination reveals a nondistended abdomen with scars from the previous laparoscopic procedure. Bowel sounds are normal. There is mild tenderness on deep palpation but no organomegaly. Her laboratory evaluation is significant for an elevated leukocyte count of /mm 3 with 12% bands, and a hemoglobin level of 11.2 g/dl. Results of liver function testing are normal. Her plasma amylase level is elevated (230 U/L) and her lipase level is normal. What is the differential diagnosis of dysphagia in postfundoplication patients? Postfundoplication dysphagia is common in the early postoperative period (30% 40%), and patients may require a soft diet for the first 2 to 4 weeks until healing and resolution of edema occurs. 4 The incidence of significant long-term dysphagia has been reported to be as high as 10% in some series. 7 Dysphagia that persists longer than 2 to 4 weeks should be evaluated with a barium esophagram to assess the integrity of the wrap and rule out paraesophageal hernia. Postoperative dysphagia can be caused by a tight wrap, a slipped wrap, a migrated wrap, or a recurrent peptic stricture. A tight wrap is the most common cause of postoperative dysphagia and may result from either a snug wrap or scarring secondary to electrosurgical current. The findings on upper endoscopy and esophagram can mimic achalasia (Figure 4). Some resistance may be encountered when passing the scope through the esophagogastric junction; however, the wrap typically appears normal in the retroflexed view. Treatment for a tight wrap is gradual esophageal dilation with either Savary dilators or through-thescope balloon dilators. A recent study reported a response rate of 67% with dilation in 20 patients who had postfundoplication dysphagia. 8 In this study, 35% required more than 1 dilation, and the mean diameter of dilation was 18.6 mm. Patients not responding to dilation with large dilators (up to 54 Fr, or 18 mm) should be referred for surgical correction. Patients unable or unwilling to tolerate reoperation may be managed safely with pneumatic dilation. 9 A slipped fundoplication also can result in significant dysphagia in addition to recurrent reflux. Dysphagia occurs when compartmentalization occurs and a gastric pouch rests above the wrap, causing partial obstruction. Although somewhat less common than slipped and tight wraps, paraesophageal hernia (Figure 5) and wrap migration deserve special attention because their presentation can be more severe and is sometimes life threatening. Paraesophageal hernia may occur at any time during the postoperative course and appears to be somewhat more common with laparoscopic procedures. Contributing factors may include inadequate crural closure and a shortened esophagus. Presentation can vary from vague intermittent symptoms of mild dysphagia to severe chest and epigastric pain with nausea and retching. Severe symptoms usually are related to ischemia or partial or complete obstruction and may Gastroenterology Volume 9, Part 4 5
6 Figure 6. Herniation of a fundoplication wrap. represent a surgical emergency secondary to incarceration and perforation. The findings of the triad of epigastric pain, inability to vomit, and failure to pass a nasogastric tube may herald impending gangrene and should prompt immediate surgical intervention. Barium esophagrams are almost always diagnostic and is the procedure of choice when a paraesophageal hernia is suspected. Although less sensitive, upper endoscopy also is useful in the evaluation of these patients. A retroflexed view can identify the gastric pouch alongside the esophagogastric junction extending into the chest, and also can document ischemic changes and ulcerations that occur along the crural diaphragm. Given the fact that paraesophageal hernias pose a significant risk and that strangulated incarcerated hernia has an extremely high operative mortality, most authorities recommend that these be treated surgically even if symptoms are not present. 10 However, more recent data suggests that operative mortality of emergent paraesophageal hernia repair has been greatly overestimated and watchful waiting may be a reasonable alternative. 11 A problem similar to paraesophageal hernia is migration of the wrap through the hiatal canal and into the chest. Depending on the position of the wrap, patients may present with dysphagia if the wrap is partially within the hiatus or with recurrent reflux if it migrates completely into the chest (Figure 6). This condition requires surgical treatment with careful repair of the hiatal defect and possibly an esophageal lengthening procedure such as a Collis gastroplasty. What is the cause of the gas bloat syndrome in fundoplication patients? Given the nature of the operation, it is not surprising that some patients experience upper abdominal bloating postoperatively. Fundoplication restores the competence of the esophagogastric junction and can impair the ability to vent gas (ie, belch). The etiology of gas bloat is unknown; however, some theories suggest that GERD patients have a persisting aerophagia postoperatively that is coupled with an inability to belch. No data exist, however, to support the idea that fundoplication patients have more intestinal air. 12 More likely, gas bloat is a manifestation of the mechanical and physiologic consequences of the operation. The fundoplication acts as a valve preventing gas venting along with acid reflux. Data also suggest that an important component of the belch reflex, transient LES relaxations, are decreased after fundoplication. 13 The incidence of mild symptoms of nausea, abdominal distention, and/or diarrhea following fundoplication is approximately 15%. 14 These symptoms tend to improve over time, but some patients may require alteration of diet, gasbinding agents, or prokinetic agents. Gas bloat also may be related to vagal nerve injury and alteration of gastric motility. Gastroparesis may develop secondary to poor emptying through a functional gastric outlet obstruction, and symptoms can be severe. Patients with severe symptoms require evaluation of gastric emptying. Patients with functional gastric outlet obstruction may respond to pyloric channel dilation or pyloroplasty. Response to dilation of the fundoplication wrap is not consistent. What is the appropriate work-up for this patient? Given the acute changes and the findings of severe epigastric pain and inability to tolerate liquids, suspicion for a complicated paraesophageal hernia is high, and a barium esophagram should be obtained. In patients with mild symptoms without overt obstruction, upper endoscopy is a reasonable alternative. CASE 2 RESOLUTION A barium esophagram is obtained and it appears that there is a paraesophageal hernia (Figure 5). The patient is seen by a thoracic surgeon and is taken to the operating room given the suspicion of an incarcerated hernia. The findings during the procedure are of an incarcerated paraesophageal hernia without evidence of gangrene. The previous fundoplication was taken down and mobilized. The hernia was reduced, and a lengthening procedure was performed. A redofundoplication also was performed. The wrap was secured to the crura and the hiatal defect was repaired. The patient was discharged on postoperative day 7 and is currently asymptomatic. 6 Hospital Physician Board Review Manual
7 BARIATRIC SURGERY INDICATIONS FOR BARIATRIC SURGERY Obesity is a major health problem in the United States and is reaching epidemic proportions, with 6% of women and 2% of men being classified as severely obese. 15 Obesity is an important risk factor for many serious medical diseases that can lead to impaired quality of life and increased mortality. Current guidelines use the body mass index (BMI) classification scheme to identify patients at risk for developing adiposity-related complications. BMI represents the relationship between height and weight and is calculated as weight (kg) divided by height (m 2 ). The NIH proposed guidelines based on BMI to classify patients by risk; patients with a BMI of 25.0 to 29.9 are overweight, and those with a BMI of 30 kg/m 2 or more are obese. Obesity is further classified as high risk (class I, BMI kg/m 2 ), very high risk (class II, BMI kg/m 2 ), and extremely high risk (class III, BMI 40 kg/m 2 or greater). 2 Patients with a BMI of 35 kg/m 2 or greater have a significant increase (relative risk, 2.0) in cardiovascular mortality and have significantly impaired quality of life. 16 Behavior modification, diet, and exercise are the mainstays of treatment for obesity; however, more aggressive treatment may be appropriate for obese subjects at risk for medical complications of obesity. Medical therapy has been limited by side effects and the inability to maintain weight loss over long follow-up periods. Given these limitations, surgery has become an attractive alternative because it represents a long-term solution. In addition, surgery has been shown to be the most effective approach for achieving sustained weight loss in severely obese patients. Therefore, the NIH concluded in 1991 that obesity surgery is a viable option for patients with a BMI of 40 kg/m 2 or greater and those patients with a BMI between 35.0 and 39.9 kg/m 2 who have serious obesity-related medical problems (eg, obstructive sleep apnea, type 2 diabetes mellitus, heart failure, hypertension). 2 BARIATRIC SURGICAL PROCEDURES Surgical procedures for obesity involving the upper gastrointestinal tract are collectively referred to as bariatric surgical procedures. Despite differences in the operative approach, 2 main principles exist in combination or alone: restriction and malabsorption. The restrictive component limits the volume of solid food that can be ingested in a given period of time. Surgical restriction is accomplished by creating a partial obstruction such that overeating results in significant nausea and abdominal discomfort. Gastric restrictive procedures currently performed are the vertical gastroplasty and gastric banding procedures. Vertical gastroplasty entails creating a small gastric pouch by stapling the front of the stomach to the back of the stomach and creating a vertical pouch. The end of the pouch is blocked by either a 1-cm diameter polypropylene band (vertical banded gastroplasty) or a 1-cm silastic ring (vertical ring gastroplasty) (Figure 7). Although these procedures are simple and relatively safe, they are not as effective as gastric bypass operations. The restrictive component (the gastric pouch) does not limit liquid or soft food, and patients may still consume large amounts of high caloric food. In addition, the gastric pouch may eventually dilate, allowing larger volumes of food to be tolerated. The laparoscopic gastric banding procedures involve placing a silastic band below the esophagogastric junction in order to restrict oral intake. Recently, a band that is placed laparoscopically has been developed in which the band diameter can be adjusted by an infusion of saline through a subcutaneous reservoir (Figure 7). The Lap-Band (Inamed Health, Santa Barbara, CA) was approved by the US Food & Drug Administration in 2001 and had been available outside of the United States prior to Good results with the Lap-Band have been reported in Europe 17 ; however, the results in the United States have been less favorable. 18 There have been reports regarding reduced effectiveness compared to gastric bypass 18 as well as complications such as band stenosis, band erosion, band slippage, gastric pouch dilation, and esophageal dilation. 19 Given the limitations that have been described for restrictive procedures, a natural progression in bariatric surgery was to combine a restrictive procedure with a diversionary operation. Although the mechanism for weight loss is unclear, bypass operations potentially induce weight loss by causing malabsorption of calories, inducing a dumping syndrome, and altering appetite through alterations in gastrointestinal peptides (eg, ghrelin). Similar to vertical banded gastroplasty, a small pouch is created by either stapling or transecting the proximal stomach (Figure 7). The pouch is then connected to and empties into a Roux-en-Y limb of the jejunum, which is approximately 50 to 100 cm in length. Randomized trials comparing gastric bypass to vertical banded gastroplasty have reported greater weight loss in patients who underwent gastric bypass surgery. 16 In addition, long-term evaluations confirm that weight loss is maintained for up to 14 years after gastric bypass Gastroenterology Volume 9, Part 4 7
8 Gastric pouch (20 30 ml) Silastic band Gastric remnant Gastric pouch (30 ml) Anastomosis Adjustable silastic band Jejunojejunostomy Vertical banded gastroplasty Banded gastroplasty Roux-en-Y gastric bypass Figure 7. Types of bariatric surgical procedures. surgery, 20 whereas patients who underwent vertical banded gastroplasty had poor sustained weight loss at 10 or more years post-procedure. 21 Therefore, the current gold standard for obesity surgery is the Roux-en-Y gastric bypass. 16 CASE 3 PRESENTATION The patient is a 37-year-old woman who underwent a Roux-en-Y gastric bypass operation approximately 4 weeks prior to admission. She was referred for gastric bypass surgery because of class III obesity and obstructive sleep apnea. She had an uncomplicated postoperative course until her current presentation. She is now complaining of nausea, vomiting, and epigastric pain related to food for the past 5 days. She has been unable to tolerate either liquids or solids, and she experiences significant pain with eating. She denies hematemesis, melena, or hematochezia. She also denies experiencing fever, chills, or diaphoresis. She has lost 20 lb in the 4 weeks since her surgery. On physical examination, she appears to be in mild distress and is afebrile. She is tachycardic (pulse, 100 bpm), and her blood pressure is 110/60 mm Hg. She exhibits orthostatic hypotension, with a pulse elevation of 24 bpm upon standing. Results of her cardiopulmonary examination are normal, and her abdomen is soft and nontender with a healing incision scar from her gastric bypass surgery. Her complete blood count (CBC) is normal. Her blood urea nitrogen level is slightly elevated (30 mg/dl) and her creatinine level is 0.8 mg/dl. What are the gastrointestinal complications of bariatric surgery? Complications of bariatric surgery can be separated into complications associated with the operation and complications associated with the anatomic changes related to the procedure. POSTOPERATIVE SYMPTOMS RELATED TO ANATOMIC CHANGES Given the alteration in upper gastrointestinal anatomy, certain side effects of bariatric surgery are to be expected and can be ameliorated through patient education and postoperative treatment. The most common adverse effects from the procedure are nausea, vomiting, and diarrhea (Table 1). These symptoms typically are associated with inappropriate diet and noncompliance with a gastroplasty diet. Patients who have undergone gastric bypass surgery may develop symptoms related to increased transit of ingested food directly into the small bowel (dumping syndrome). Dumping syndrome symptoms increased with the ingestion of food with a high sugar content and high osmotic activity. Symptoms of nausea, bloating, abdominal pain, and lightheadedness in these patients generally improve with fasting and are a deterrent to overeating. If diarrhea or other symptoms suggestive of dumping syndrome do not improve with fasting, an alternate diagnosis of bacterial overgrowth should be considered and an empiric trial of antibiotics may be warranted. All patients with gastric bypass surgery also should be monitored for nutritional deficiencies and should take a multivitamin containing Vitamin B 12 and folate along with a calcium supplement Hospital Physician Board Review Manual
9 COMPLICATIONS OF SURGERY Perioperative mortality of bariatric surgery is less than 1% 16,22 and is usually associated with anastomotic leaks leading to peritonitis (75%) or pulmonary embolism (25%). 16 Symptoms of an anastomotic leak can be overt with frank peritoneal signs or vague with symptoms of mild abdominal pain, shoulder pain, back pain, unexplained tachycardia, or alteration in urination and bowel frequency. Given the devastating outcome of anastomotic leaks, there should be a low threshold for evaluation with water-soluble contrast agents and surgical exploration. An early complication of gastric bypass surgery is acute gastric distention secondary to edema and obstruction at the enteroenterostomy. This complication may lead to staple line dehiscence or gastroenterostomy leaks. Acute gastric distention can be treated with radiographically guided percutaneous gastrostomy or reoperation with tube gastrostomy. Nausea and vomiting following bariatric surgery typically are associated with noncompliance with a gastroplasty diet. If these symptoms are associated with epigastric pain, significant dehydration, or are not explained by dietary indiscretions, an alternative diagnosis must be explored. One of the most common causes of nausea and vomiting in gastric bypass patients is anastomotic ulcers with or without stomal stenosis (Figure 8). Ulceration or stenosis at the gastrojejunostomy of the bypass has a reported incidence of 3% to 20% The etiology of these ulcers is unclear and has been theorized to be secondary to staple-line dehiscence or excessive acid secretion. Evidence suggests that little acid is secreted in the gastric bypass pouch; however, staple line dehiscence may lead to excessive acid bathing of the anastomosis. Treatment for both marginal ulcers and stomal ulcers in bypass patients should include antisecretory therapy with PPIs and/or sucralfate and avoidance of nonsteroidal anti-inflammatory drugs (NSAIDs). Stomal stenosis may respond to endoscopic dilation with through-the-scope balloon dilators and may obviate the need for surgical revision. 25 Patients with restrictive procedures (eg, vertical band gastroplasty) also may develop nausea and vomiting secondary to stomal stenosis, erosion of the restrictive band or ring, or increased gastroesophageal reflux. Treatment is dependent on the etiology. Stomal stenosis is treated similarly to stenosis in gastric bypass surgery. Erosion of the restrictive band or ring may require surgery. Severe GERD associated with the purely restrictive surgical procedures may respond to PPI therapy or require conversion to a gastric bypass. Another cause of mechanical obstruction in gastric bypass patients is internal hernia. These hernias may Table 1. Adverse Effects and Complications of Bariatric Surgery Adverse effects Cholelithiasis Diarrhea Dumping syndrome Nausea Nutrient deficiency Vomiting Complications Acute gastric distention Anastomotic leak Internal hernia Staple line disruption Stomal stenosis Stomal ulceration occur where the Roux limb passes through the transverse mesocolon or at the mesenteric defect at the jejunojenunal anastomosis. This problem is extremely difficult to diagnose as symptoms are nonspecific (cramping, periumbilical pain with or without nausea, vomiting) and diagnostic radiographic studies can be normal. 26 If symptoms persist or become severe, surgical exploration is indicated to rule out internal hernia. Gastrointestinal bleeding in patients with who have undergone either a restrictive gastroplasty or gastric bypass should be evaluated similarly to patients who have not. The distal stomach and proximal duodenum may not be accessible to endoscopy; however, bleeding from these areas is rare, possibly owing to low acid secretory states secondary to vagal interruption and lack of antral distention and contact with food. Patients are still susceptible to NSAID-related complications and should avoid these medications. If bleeding from the distal stomach or proximal small bowel is suspected, a pediatric colonoscope or enteroscope may be used to evaluate this area. In addition, interventional angiography may be able to both locate and treat bleeding lesions in this area. Colonoscopy is unchanged in obesity surgery patients; however, the preparation should be performed carefully because these patients are unable to tolerate large volumes orally. 25 What is the most appropriate work-up for patient 3? Because the patient s symptoms are severe and are associated with dehydration and epigastric pain, she Gastroenterology Volume 9, Part 4 9
10 A B Figure 8. Anastomotic ulcer stenosis. (A) Anastomotic ulcer with patent gastrojejunostomy. (B) Upper gastrointestinal radiograph revealing anastomotic stricture. (C) Endoscopic view of stricture. (D) Dilation with a through-the-scope balloon dilator. C D should be evaluated with upper endoscopy after resuscitation with intravenous fluids. Before proceeding with endoscopy, it is extremely important to discuss the case with the surgeon who performed the bariatric procedure and confirm the type of operation performed so the patient s anatomy is clearly understood prior to endoscopy. In addition, the surgeon should be consulted regarding the stability of the anastomosis, especially if dilation is contemplated. If an anastomotic leak is suspected, a water-soluble contrast study is indicated before performing endoscopy. CASE 3 RESOLUTION After consultation with the bariatric surgeon, an upper endoscopy is performed and reveals a stomal stenosis of the gastric pouch jejunal anastomosis (Figure 8). Dilation is performed with a through-the-scope balloon dilator. Dilation starts at 6 mm and proceeds sequentially to 10 mm. The patient s diet is slowly advanced and she is placed on PPI therapy. CASE 4 PRESENTATION The patient is a 35-year-old man who had a laparoscopic Roux-en-Y gastric bypass 2 years prior to admission at different hospital. The patient presents now with the acute onset of severe epigastric pain after eating. He has not been experiencing nausea or vomiting. The pain is constant but worsens with eating. He denies fever, chills, diaphoresis, and changes in his bowel habits. He had an uneventful postoperative course 2 years ago and has lost 140 lb since his operation. (His current weight is 162 lb.) On examination, he is in mild distress and his vital signs are normal, with a pulse of 88 bpm, a blood pressure of 132/78 mm Hg, and a temperature of 98.9 F. Results of his cardiopulmonary examination are normal and examination of his abdomen reveals laparoscopic surgical scars. Active bowels sounds are normal and the abdomen is not distended. Mid-epigastric abdominal tenderness is evident on deep palpation, but there are no rebound or peritoneal signs. His laboratory evaluation reveals a normal CBC with a hemoglobin level of 11.8 gm/dl and a leukocyte count of /mm 3. The patient is placed on NPO status and is admitted to the surgical service. Given the concern for a possible anastomotic leak, an abdominal computed tomography scan with oral contrast is performed and reveals normal postoperative changes consistent with a previous Roux-en-Y gastric bypass. There is no leak or evidence of obstruction. The surgical team requests an upper endoscopy, which reveals a normal pouch, no stomal ulcer or stenosis, and a normal jejunojejunal anastomosis. The patient s symptoms improve slightly following the endoscopy, and his diet is advanced to clear liquids. Shortly after his 10 Hospital Physician Board Review Manual
11 meal, the patient once again develops severe midepigastric pain and nausea. What is the most appropriate step at this point? Given the severity of the patient s symptoms and his failure to improve, some surgeons would proceed directly to reoperation. In this case, it is also reasonable to obtain an upper gastrointestinal series with watersoluble contrast for the purpose of identifying anastomotic leaks and internal hernias (Figure 9). However, as the upper gastrointestinal series can be normal with both of these diagnoses, surgical exploration is indicated if the patient does not improve. CASE 4 RESOLUTION An upper gastrointestinal series with Gastrografin contrast is obtained and is read as no overt obstruction; however, there is mild dilation of the Roux limb. Given the suspicion for internal hernia, the patient is brought to the operating room the following day. Surgical exploration reveals 2 internal hernias in mesenteric defects at the gastrojejunostomy and jejunojejunal anastomosis. The bowel is viable and the hernias are reduced and the defects repaired. The patient s diet is slowly advanced on postoperative day 2, and he is discharged on postoperative day 5 tolerating a full general diet. REFERENCES Gastric pouch Herniated Roux limb Figure 9. Internal hernia of Roux limb through the mesocolon. Note where contrast ends abruptly. 1. Nebel OT, Fornes MF, Castell DO. Symptomatic gastroesophageal reflux: incidence and precipitating factors. Am J Dig Dis 1976;21: NIH conference. Gastrointestinal surgery for severe obesity. Consensus Development Conference Panel. Ann Intern Med 1991;115: Spechler SJ. Medical or invasive therapy for GERD: an acidulous analysis. Clini Gastroenterol Hepatol l2003;1: Waring JP. Management of postfundoplication complications. Semin Gastrointest Dis 1999;10: Rydberg L, Ruth M, Abrahamsson H, Lundell L. Tailoring antireflux surgery: a randomized clinical trial. World J Surg 1999;23: Hinder RA, Klingler PJ, Perdikis G, Smith SL. Management of the failed antireflux operation. Surg Clin North Am 1997;77: Johnson DA, Younes Z, Hogan WJ. Endoscopic assessment of hiatal hernia repair. Gastrointest Endosc 2000; 52: Malhi-Chowla N, Gorecki P, Bammer T, et al. Dilation after fundoplication: timing, frequency, indications, and outcome. Gastrointest Endosc 2002;55: Hui JM, Hunt DR, de Carle DJ, et al. Esophageal pneumatic dilation for postfundoplication dysphagia: safety, efficacy, and predictors of outcome. Am J Gastroenterol 2002;97: Hill LD. Incarcerated paraesophageal hernia. A surgical emergency. Am J Surg 1973;126: Stylopoulos N, Gazelle GS, Rattner DW. Paraesophageal hernias: operation or observation? Ann Surg 2002;236: ; discussion Low DE. Management of the problem patient after antireflux surgery. Gastroenterol Clin North Am 1994;23: Straathof JW, Ringers J, Lamers CB, Masclee AA. Provocation of transient lower esophageal sphincter relaxations by gastric distension with air. Am J Gastroenterol 2001;96: Hunter JG, Trus TL, Branum GD, et al. A physiologic approach to laparoscopic fundoplication for gastroesophageal reflux disease. Ann Surg 1996;223:673 85; discussion Martin LF, Hunter SM, Lauve RM, O Leary JP. Severe obesity: expensive to society, frustrating to treat, but important to confront. South Med J 1995;88: Klein S, Wadden T, Sugerman HJ. AGA technical review on obesity. Gastroenterology 2002;123: Belachew M, Belva PH, Desaive C. Long-term results of laparoscopic adjustable gastric banding for the treatment of morbid obesity. Obes Surg 2002;12: Gastroenterology Volume 9, Part 4 11
12 18. DeMaria EJ, Sugerman HJ, Meador JG, et al. High failure rate after laparoscopic adjustable silicone gastric banding for treatment of morbid obesity. Ann Surg 2001;233: Hauri P, Steffen R, Ricklin T, et al. Treatment of morbid obesity with the Swedish adjustable gastric band (SAGB): complication rate during a 12-month follow-up period. Surgery 2000;127: Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg 1995;222:339 50; discussion Balsiger BM, Poggio JL, Mai J, et al. Ten and more years after vertical banded gastroplasty as primary operation for morbid obesity. J Gastrointest Surg 2000;4: Schauer PR, Ikramuddin S, Gourash W, et al. Outcomes after laparoscopic Roux-en-Y gastric bypass for morbid obesity. Ann Surg 2000;232: Sanyal AJ, Sugerman HJ, Kellum JM, et al. Stomal complications of gastric bypass: incidence and outcome of therapy. Am J Gastroenterol 1992;87: Pope GD, Goodney PP, Burchard KW, et al. Peptic ulcer/ stricture after gastric bypass: a comparison of technique and acid suppression variables. Obes Surg 2002;12: Stellato TA, Crouse C, Hallowell PT. Bariatric surgery: creating new challenges for the endoscopist. Gastrointest Endosc 2003;57: Blachar A, Federle MP, Pealer KM, et al. Gastrointestinal complications of laparoscopic Roux-en-Y gastric bypass surgery: clinical and imaging findings. Radiology 2002;223: Copyright 2003 by Turner White Communications Inc., Wayne, PA. All rights reserved. 12 Hospital Physician Board Review Manual
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Dept. of Medical Imaging University of Ottawa
 ED Visits Related to Bariatric Surgery: Review of Normal Post-Surgical Anatomy as Well as Complications Dept. of Medical Imaging University of Ottawa Disclosures Background Roux-en-Y Gastric Bypass Surgery
ED Visits Related to Bariatric Surgery: Review of Normal Post-Surgical Anatomy as Well as Complications Dept. of Medical Imaging University of Ottawa Disclosures Background Roux-en-Y Gastric Bypass Surgery
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of
 Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
GASTROESOPHAGEAL REFLUX DISEASE (GERD) Gastroesophageal reflux disease is a clinical scenario where the gastric or duodenal contents reflux back up into the esophagus. Reflux esophagitis, however, is a
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Obesity When to Recommend Surgery. Lily Chang, MD September 27, 2013
 Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Chapter 6 Gastrointestinal Impairment
 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Gastroesophageal Reflux
 Gastroesophageal Reflux What is Gastroesophageal Reflux? Gastroesophageal reflux (GER) is involuntary regurgitation of stomach contents into the esophagus. Reflux causes a number of problems: 1. Chemical
Gastroesophageal Reflux What is Gastroesophageal Reflux? Gastroesophageal reflux (GER) is involuntary regurgitation of stomach contents into the esophagus. Reflux causes a number of problems: 1. Chemical
What is the Sleeve Gastrectomy?
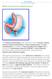 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Laparoscopic Antireflux Surgery Information Sheet
 Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Laparoscopic Antireflux Surgery Information Sheet What is Laparoscopic Antireflux Surgery? Antireflux surgery (also known as fundoplication) is the standard surgical method of treating gastro-oesophageal
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Gastric Bypass and Other Bariatric Surgical Procedures*
 Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
5. Conversion Procedures that change from an index procedure to a different type of procedure.
 Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Nash Heartburn Treatment Center
 Nash Heartburn Treatment Center a division of Nash Health Care NHCS Mission Statement: To provide superior quality health care services and to help improve the health of the community in a caring, efficient
Nash Heartburn Treatment Center a division of Nash Health Care NHCS Mission Statement: To provide superior quality health care services and to help improve the health of the community in a caring, efficient
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
5/9/2012. What is Morbid Obesity? Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person)
 Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
When, Why, and How to Revise a Failed Sleeve Gastrectomy
 When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery
 Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
G E R D. (Gastroesophageal Reflux Disease)
 G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE)
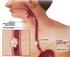 Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
Gastroesophageal Reflux Disease (GERD) and Barrett s Esophagus (BE) Hashem El-Serag, M.D., M.P.H. Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Baylor College of Medicine Houston,
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Weight Loss Surgery Information Session. WFBH Bariatric Surgery Program
 Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
Complications of Bariatric Surgery
 47 Complications of Bariatric Surgery Robert F. Poirier KEY POINTS Laparoscopic Roux-en-Y gastric bypass is the most commonly performed bariatric procedure in the United States. Pulmonary embolism (30%
47 Complications of Bariatric Surgery Robert F. Poirier KEY POINTS Laparoscopic Roux-en-Y gastric bypass is the most commonly performed bariatric procedure in the United States. Pulmonary embolism (30%
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Endoluminal Bariatric Revision. Todd David Wilson, MD
 Endoluminal Bariatric Revision Todd David Wilson, MD Surgical Endoscopy and the Bariatric Surgeon Preoperative Endoscopy Postoperative Endoscopy Revisional Endoscopy Primary Endoluminal Bariatrics Preoperative
Endoluminal Bariatric Revision Todd David Wilson, MD Surgical Endoscopy and the Bariatric Surgeon Preoperative Endoscopy Postoperative Endoscopy Revisional Endoscopy Primary Endoluminal Bariatrics Preoperative
LAPAROSCOPIC HELLER MYOTOMY FOR TREATMENT OF ACHALASIA
 LAPAROSCOPIC HELLER MYOTOMY FOR TREATMENT OF ACHALASIA JL Holihan, LR Hafen, MK Liang, University of Texas Health Science Center at Houston, Houston, TX Background: Achalasia is a rare esophageal dismotility
LAPAROSCOPIC HELLER MYOTOMY FOR TREATMENT OF ACHALASIA JL Holihan, LR Hafen, MK Liang, University of Texas Health Science Center at Houston, Houston, TX Background: Achalasia is a rare esophageal dismotility
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY
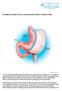 INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
INFORMATION SHEET FOR A LAPAROSCOPIC SLEEVE GASTRECTOMY You are considering undergoing a laparoscopic sleeve gastrectomy for weight loss. The purpose of this information sheet is to provide you with the
Weight Loss Surgery Advisory
 PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
PATIENT NAME: D.O.B.: / / INSTRUCTIONS: As you consider surgical treatment for morbid obesity, it is very important that you fully understand (1) the nature of your condition, (2) the types of surgical
IEHP UM Subcommittee Approved Authorization Guidelines Bariatric Surgery for Morbid Obesity
 According to the National Institutes of Health (NIH) Consensus Development Conference on Gastrointestinal Surgery for Severe Obesity, the risk for morbidity and mortality accompanying obesity increases
According to the National Institutes of Health (NIH) Consensus Development Conference on Gastrointestinal Surgery for Severe Obesity, the risk for morbidity and mortality accompanying obesity increases
Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy
 CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery
 Obesity Surgery, 14, 224-229 Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery Roy Shen, MD; Christine J. Ren, MD Department of Surgery, NYU School of Delivered Medicine, by
Obesity Surgery, 14, 224-229 Removal of Peri-Gastric Fat Prevents Acute Obstruction after Lap-Band Surgery Roy Shen, MD; Christine J. Ren, MD Department of Surgery, NYU School of Delivered Medicine, by
Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it
 CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Figure 2: Recurrent chest pain of suspected esophageal origin
 Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
Figure 2: Recurrent chest pain of suspected esophageal origin 1 patient with chest pain of suspected esophageal origin 2 history and physical exam. suggestive of n-esophageal etiology? 3 evaluate and treat
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach
 Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Dealing with weight regain after Rouxen-Y gastric bypass: surgical approach Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida Disclosures PI Enteromedics
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
BARIATRIC SURGERY PATIENT GUIDE
 You the patient play a critical role in the long term success of surgery. You will need to: Commit to improving your health. Discuss your health history with your surgeon. Discuss any questions or concerns
You the patient play a critical role in the long term success of surgery. You will need to: Commit to improving your health. Discuss your health history with your surgeon. Discuss any questions or concerns
Why a loop and new approach makes sense!
 IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
KEYHOLE HERNIA SURGERY
 Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
University College Hospital. Laparoscopic Fundoplication. Gastrointestinal Services Division
 University College Hospital Laparoscopic Fundoplication Gastrointestinal Services Division 2 3 If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
University College Hospital Laparoscopic Fundoplication Gastrointestinal Services Division 2 3 If you need a large print, audio or translated copy of the document, please contact us on 020 3447 9202. We
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE
 INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
INFORMED CONSENT FOR LAPAROSCOPIC GASTRIC SLEEVE SURGICAL PROCEDURE It is very important to [insert physician, practice name] that you understand and consent to the treatment your doctor is rendering and
Roux-en-Y Gastric Bypass
 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Bariatric Surgery Guide Dr. Stewart s Weight Loss Specialists of North Texas
 Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
Welcome. This resource is created for you by Dr. Stewart and our bariatric surgery team with input from people who have found success through weight loss surgery. It is not intended to replace consultation
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Laparoscopic Fundoplication for Reflux
 Laparoscopic Fundoplication for Reflux Exceptional healthcare, personally delivered Understanding Reflux General Reflux happens when acid from the stomach washes up into the gullet (oesophagus) from the
Laparoscopic Fundoplication for Reflux Exceptional healthcare, personally delivered Understanding Reflux General Reflux happens when acid from the stomach washes up into the gullet (oesophagus) from the
Gastroesophageal Reflux Disease:
 Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
