Antipsychotic Treatment in OCD. Majed Habib Al Moumen,MD*
|
|
|
- Edwina Caldwell
- 10 years ago
- Views:
Transcription
1 1 Bahrain Medical Bulletin, Vol. 34, No. 2, June 2012 Antipsychotic Treatment in OCD Majed Habib Al Moumen,MD* Due to the phenotypical heterogeneity of Obsessive-Compulsive Disorder (OCD) and its subtypes, and due to the high rate of co-morbid psychopathology, it remains a challenge to treat OCD using medication effectively, behavioral therapy and cognitive therapy.selective serotonin reuptake inhibitors (SSRIs) arefirst-line pharmacotherapy treatments OCD, but up to 50% of patients do not respond to initialtreatment of OCD.Therefore, treatment options for non-respondersinclude augmentation of antidepressantswith antipsychotics and other medications. Bahrain Med Bull 2012; 34(2): After Post Traumatic Stress Disorder, OCD is the highest anxiety disorder, which has initiated more research over the last three decades 1. Meta-analysis has proven that treatment is effective using either pharmacotherapy with SRIs alone or in combination with cognitive behavioral therapy. Unfortunately, 38% of patients are treatment refractory (not experiencing clinically significant benefits) and only 30% of patients were asymptomatic after treatment 1,2. It is well established that there is a need to report the effectiveness of interventions in routine clinical practice as well as the efficacy studies in patients with comorbidities. In addition, we need to study the outcome using varying methods aside from simple significance tests of pre and post symptoms severity comparison. Furthermore, analysis of group means, investigators must assess the responses of each individual patient for reliable and significant change. There are a few published studies concerning the outcome of Cognitive Behavioral Therapy(CBT) in cases of severe OCD 1. Theaim of this review is to define treatment-resistant OCD and to evaluate the effectiveness of treatment of severe OCD. The Etiology of OCD There have been numerous postulations about the cause of OCD. These have evolved from demon possession to melancholia, the result of overt scrupulousness and eventually it was perceived as neurasthenia. Some believed that it stemmed from faulty beliefswoven into a pattern of thought and behavior. While others claimed that dissociative pathology was the cause 2. Freud was finally instrumental in describing OCD as the result of psychological defenses, which protects against unconscious anxiety 3. More scientific theories regarding its origin * Consultant Psychiatrist King Fahd Hospital of the University Saudi Arabia [email protected]
2 2 and careful clinical picture has been described and improved upon in the current DSM-IV. The psychological models of OCD have now been challenged by the relatively recent evidence for a biological basis as progress in genetic research revealed a significant role of hereditary 3,4. Neuroimaging revealed neural pathway disturbances in thebasal ganglia, subcortical areas of the brain and the orbito-frontal cortex. Both dopamine and serotonin disturbances supportthe pathophysiology of OCD 5. Medical conditions, suchas teratoma, endocrine disturbance, neoplasm andtoxin exposures might produce symptoms of OCD; example of this is pediatric autoimmune neuropsychiatricdisorder (PANDAS) and streptococcal infection in veryyoung children.ocd is extremely complex in term of its causative factors. Thereappears to be a combination of genetic and socio-psychological factors.identifying the elements of the disorder is often confounded by thepresence of comorbidities, external environmental influences and thepresence of significant dissociation. The role of diatheses (constitutionalfactors that predispose the body to certain illnesses or conditions)in OCD is inescapable. Some scientists proposed that theetiology of OCD could be viewed best from the framework of a stressdiathesismodel. This integrative model encompasses biological andsocio-psychological factors. They alsothought that OCD should be thought of as a spectrum of manifestationsthat extends from the most biologically determined to the mostpsychologically determined 6. Treatment-resistant OCD OCD is a chronic psychiatric disease characterized by recurrent and persistent thoughts (obsessions) and/or repetitive compulsive behavior (compulsion). These must cause the individual anxiety, are time-consuming and cause a significant socio-occupational dysfunction. Even with pharmacological and behavioral treatments, the outcome is not satisfactory for 40-60% of OCD patients 7. There have been several attempts to define and stage treatment-resistant OCD, see table 1. An estimated 5% of OCD cases have an episodic course, 40-60% of OCD patients fails to improve sufficiently with first line management and considered refractory 4. It is only reasonable to include recovery and remission in the staging terminology. Guy defined Adequacy, Resistance and Refractoriness of treatment 7. A trial is considered Adequate if the patient has been given first-line pharmacotherapy in the form of at least three SSRIs at the maximum recommended dosage for minimum of 12 weeks and the treatment should have included the use of clomipramine and/or behavioral therapy with at least 20 hours of exposure and response prevention (ERP). Failure to respond to the above trial is considered treatment resistance. Resistance is considered failure to respond to one SSRI,i.e. less than 25% reduction on the Yale Brown Obsessive-Compulsive Scale (Y-BOCS) 7,8. It may be argued that it is not absolute since most treatment resistant cases are actually cases of relative resistance to drugs. It might be considered accurate to divide resistance to drug resistance and treatment resistance. Drug Resistance is considered when the patient shows less than 25% reduction on the Y-BOCS after treatment with at least two SSRIs. Treatment Resistance is considered when the patient fails to show response to the above plus 20 hours of compliant ERP 7. Refractoryis failure to respond to two SSRIs.
3 3 Table 1: Stages of Response in Obsessive-CompulsiveDisorder Definition Stage I Recovery/not at all ill Stage II Remission Less than 8 on Yale-BrownObsessive Compulsive Scale (Y-BOCS) Less than 16 on Y-BOCS Stage III Full response 35% or greater reductionof Y-BOCS and CGI 1 or 2 Stage IV Partial response Greater than 25% but lessthan 35% Y-BOCSreduction Stage V Non-response Less than 25% Y-BOCSreduction, CGI 4 Stage VI Relapse Stage VII Refractory Subtypes of OCD Symptoms return (CGI 6 or25% increase in Y-BOCS from remission score) after3+ months No change or worsening,with all available therapies It is now believed that OCD is a heterogenous condition with several subtypes. We can subdivide OCD depending on age of onset (e.g. earlier age with familial form), the presence of tic disorders and comorbid psychiatric disorder, each with a potential implication to treatment. For example, a patient with OCD and comorbid tics is usually has an early onset with a specific range of OCD symptoms and responds very poorly to SRIs 7. In addition, it is believed that psychotic OCD exist, which in the DSM-4 called OCD without insight, usuallyare poor responders 2.Further study of the response to treatment and illness trajectory and outcome may help us further subdivide OCD in the future 8. Epidemiology of OCD OCD is estimated to be 10% of patients in psychiatry clinics. It is the fourth most common psychiatric disorder after phobias, substance related disorders and major depressive disorder. The female to male ratio is equal but the presentation is earlier in males (mean age in males is 19 compared to females 22 years). The first onset of symptoms is before the age 25 for two-thirds of patients, and only 15% of patients present after age 35. The onset could be in childhood or adolescence and the earliest reported case was 2 years of age 9. It is more frequent in single persons, perhaps reflecting the difficulty of maintaining a relationship. It is more often in whites compared to blacks, although this variation could be due to access to healthcare. The prevalence of Obsessive-compulsive personality disorder(ocpd)among patients with OCD is similar to its prevalence among other psychiatric disorders 2,4. Patients with OCD are commonly afflicted by other mental disorders; for instance, the lifetime prevalence for a major depressive episode in these patients is around 67%. Other common comorbid psychiatric diagnoses include alcohol-use disorders, social phobia, specific phobia, panic disorder and eating disorders. The comorbidity of schizophrenia and with tic disorders raises interesting pathophysiological and therapeutic implications. The rate of tic disorders approaches 40% in juvenile OCD and there is an increase in the prevalence of Tourette's syndrome among the relatives of OCD patients 2.
4 4 Treatment of OCD A combination of a potent serotonergic agent and CBT is considered themost effective treatment. The behavioral component consists of EPR 10. Exposure is helpful in reducing obsessions and response prevention is helpful in reducing compulsive behaviors. Potent 5-HT reuptake inhibitors (SSRIs; clomipramine) are considered the first-line medications for the treatment of OCD. SSRIs are preferred over clomipramine solely because of their lower propensity to cause side effects 11. Medications treatment of OCD should take 8-12 weeks or longer and it requires higher dosage of drugs compared to other neurotic disorders, i.e. generalized anxiety disorder and depression. Medication should be continued for a minimum of 1 year and possibly indefinitely. With adequate treatment, the average reduction in obsessions and compulsions is about 50%, only 5% to 10% of individuals eventually becoming symptom free. If the first-line treatments of SSRIs and clomipramine failed, alternative treatments are required,see table Table 2: Pharmacologic Treatment of OCD OCD Standard Treatment Alternative Treatment Recommended Examples Dose for Adult (mg/day) Citalopram Escitalopram SSRI Fluoxetine Fluvoxamine Paroxetine Sertraline TCA Clomipramine SNRI Venlafaxine NaSSA Mirtazapine MAOI Phenelzine The Yale-Brown Obsessive-Compulsive Scale is commonly used to evaluate patients with OCD and reduction in symptoms of 25-35% is considered the threshold for response. Unfortunately, 40-50% of OCD patients fail to meet these criteria. Before we can say that the patient is treatment resistant, we must first make sure that the diagnosis is correct,the patient is compliant to treatment, the dosage is therapeutic and the trial period is adequate. Other drugs may interfere with efficacy, e.g. metabolic enhancers or inhibitors 13. Psychosocial factors and personality may affect outcome. Depression and substance abuse may complicate OCD. If the patient fails to show response after 8-12 weeks, the medication should be changed. However, if there is partial response, the patient may show improvement after an additional 4-6 weeks of therapy 7. Other strategies evaluated in controlled studies are augmentation of SSRI or clomipramine with atypical (or typical) antipsychotic, seetable 3.There is a positive effect of antipsychotic
5 5 drug augmentation as evaluated by meta-analysis 7. Clomipramine and clonazepam given intravenously has been effective in controlled trials. Other trials evaluated are demonstrated in Table 3. Table 3:Treatment Options of Patients withocd Who Are Unresponsive to Standard Treatment RandomizedControlled Studies Antipsychotic augmentation to SSRI or clomipramine Intravenous clomipramine Clonazepam Open Studies Addition of clomipramine to an SSRI Buspirone Topiramate V-acetylcysteine Addition of gabapentin to an SSRI Addition of l-tryptophan to clomipramine or to SSRIplus pindolol Glutamate antagonist Riluzole NMDA receptor antagonist memantine Combination of citalopram and reboxetine Aripiprazole Psilocybin Gonadotropin-releasing hormone analogue triptorelin Nicotine chewing gum Treatment Strategies for Resistant OCD Patients (Table 4) A practical approach should include the following 7 : 1. Primary physicians should perform early screening to detect juvenile-onset or adolescent OCD. 2. The consideration of different diagnosis if required. 3. The use of antipsychotics to augment the trial if needed. 4. Identifying comorbidities. 5. Considering the psychosocial issues. 6. Making use of non-drug treatments (CBT, group/individual therapy). Table 4: Other Augmenting Agents Drugs Action/ Dose Side Effects Clonazepam Up-regulation of 5-HT1 and 5-HT2 receptor in the frontal cortex Depression, irritability and intoxication Buspirone Partial 5-HT1A receptor agonist at dosage of mg/day Irritability and forgetfulness Lithium Enhancement of 5-HT transmission Neurotoxicity Not approved for use by FDA, Fenfluramine Increases 5-HT neurotransmisson across the considering its cardiac side effects and synaptic cleft risk of pulmonary hypertension Trazodone mg/day Sedation, priapism Inositol Only a few case trials reported Phenelzine OCD with associated panic Hypertensive crisis (or cheese reaction)
6 6 Venlafaxine Sumatriptan Clonidine (1 Open trial and 2 reported case studies have found venlafaxine to have anti-obsessional activity in treatment-resistant OCD 100 mg/day (5-HT1D agonist) Trials only in comorbid tics or Tourette s syndrome at dose of mg/day in three divided doses Hypertension (at higher doses) Postural hypotension, dry mouth, irritability and headache Antipsychotic Treatment in OCD (Table 5) The use of typical neuroleptic to treat anxiety disorders was common in the s, but later, it was abandoned. In recent years, atypical antipsychotics were used to augmentnonresponsive OCD patients 14. Pharmacokinetic Effects The augmentation with quetiapine and SRIs are not fully explained by pharmacokinetic interaction 8. Pharmacodynamic Effects The pharmacodynamics mechanism of action of atypical antipsychotics in OCD has been studied by examining a group and specific agent and their relationship to known receptor binding agents 8. Table 5: Antipsychotic Treatment in OCD OCD Antipsychotic agents for patients with partial response to antidepressants Typical Atypical Examples Haloperidol > = 3 Pimozide 2-12 Risperidone Olanzapine 5-15 Recommended Dose for Adult (mg/day) Mechanism of Action D 2 blockage, H 1, muscarinic, α 1, α 2 -adrenergic & serotonergic receptors D 2 blockage, H 1, muscarinic, α 1, α 2 -adrenergic & serotonergic receptors Antagonist for the 5-HT 2A, 5-HT, D 2, D 3, D 4, H 1, α 1, & α 2 receptors, & weak affinities for the 5-HTT 2C, 5-HT 6, & muscarinic receptors Antagonists for the 5-HT 2A, 5-HT 2C, D 1, D 2, D 4, α 1, H 1, & M 1 & M 2 muscarinic receptors Quetiapine Antagonists for the 5-HT 2A, 5-HT 7, D 2, 5-HT 1A, & α 1 Mechanism of Action of Antipsychotic in OCD 1) Atypical Antipsychotic The serotonin dopamine antagonists (SDAs) are also known as second-generation or atypical antipsychotic drugs. These drugs include risperidone (Risperdal), olanzapine (Zyprexa),
7 7 quetiapine (Seroquel), clozapine (Clozaril) and ziprasidone (Geodon). They are called SDAs because they have a higher ratio of serotonin type 2 (5-HT2) to D2 dopamine receptor blockades than the typical or conventional, dopamine receptor antagonists (DRAs) that previously were the mainstay of treatment 16,17. All SDAs share the following characteristics: 1) low D2 receptor blocking effects compared with DRAs, which have high D2 receptor blockades; 2) reduced risk of extrapyramidal side effects compared with older agents, reduced risk that probably extends to theoccurrence of tardive dyskinesia as well; 3) proved efficacy as treatments for schizophrenia; and 4) proved efficacy as treatments for acute mania 2,3,5. Patients who do not respond to SSRIs may have additional abnormalities in dopamine function and thus require augmentation with dopamine blockers. It is believed to work via antagonism of both D2 and 5HS receptors. In psychosis, augmentation with risperidone 2-6mg/day and olanzapine 5-20 mg/day are effective in low doses 18. A trial of 4 weeks at the maximum dose is sufficient. At present, there is no justification for the use of Clozapine due to its relative toxicity. There was a single placebo-controlled trial using Quetiapine but it was limited by small sample size. The indications were comorbid tic, delusional disorder, obsessions bordering on delusions. Quetiapine was limited by side effects including sedation, weight gain and EPS 7. 2) Typical Antipsychotic The typical antipsychotic drugs vary in their in vitro and in vivo affinities for receptors such as the dopamine D 1, histamine H 1, muscarinic, α 1,α 2 -adrenergic and serotonergic receptors, which modulate their effects on arousal, extrapyramidal, cognitive, cardiovascular, gastrointestinal and genitourinary function. Pimozide is a relatively potent antimuscarinic agent. Most of the low-potency antipsychotic agents are potent α 1 and H 1 antagonists 2,3,5. In OCD patients with comorbid tic disorder or Trichotillomania, typical antipsychotics, i.e. haloperidol and pimozide, were used to augment OCD treatmentsuccessfully. This was not the case in treatment-resistant OCD. Neuroleptic agents like typical antipsychotics are used to augment SSRIs but carry the risk of inducing EPS and tardive dyskinesia 7. CONCLUSION In most cases, a combination of drug treatment and CBT may control symptoms and improve the quality of life for OCD patients. Studies have confirmed that augmentation of SSRIs with antipsychotics helps in SRI-refractory cases. Further controlled studies are needed to examine the efficacy of various atypical agents that may be used in augmentation, their dosage, duration of treatment and predictors of response. Additional research is needed to study the complexities and the exact mechanism of action and to divide OCD into subtypes according to psychobiology and phenomenology. It is important to identify the patients with refractory OCD and switch them to a more effective pharmacological and/or psychological agent. Those patients who did not
8 8 respond after switching them to another pharmacological or psychological treatment may still have a chance to improve using intensive specialist treatment regimen. Author contribution: All authors share equal effort contribution towards (1) substantial contributions to conception and design, acquisition, analysis and interpretation of data; (2) drafting the article and revising it critically for important intellectual content; and (3) final approval of the manuscript version to be published. Yes Potential conflicts of interest: No Competing interest: None Sponsorship: None Submission date: 3 February 2012Acceptance date: 30 April 2012 Ethical approval: Faculty Research Committee, University of Dammam. REFERENCES 1. Savas HA, Yumru M, Ozen ME. Quetiapine and Ziprasidone as Adjuncts in Treatment-Resistant Obsessive-Compulsive Disorder: A Retrospective Comparative Study. Clin Drug Invest 2008; 28(7): Sadock BJ, Sadock AV. Kaplan & Sadock s Synopsis of Psychiatry: Behavioral Sciences / Clinical Psychiatry. 10 th ed. Philadelphia: Lippincott Williams & Wilkins, 2007; ; Gelder MG, Lopez-Ibor J, Andreasen N. New Oxford Textbook of Psychiatry. 2 nd ed. Oxford University, 2009; Pallanti S, Bemardi S, Antonini S,et al. Ondansetron Augmentation in Treatment- Resistant Obsessive-Compulsive Disorder: A Preliminary, Single-Blind, Prospective Study. CNS Drugs 2009; 23(12): Strahl NR. Clinical Study Guide for the Oral Boards in Psychiatry. 4 th ed. Arlington, VA: American Psychiatric Publishing, 2011;36-75; Frederick C. Hypnotically Facilitated Treatment of Obsessive-Compulsive Disorder: Can It be Evidence-Based? Intl Journal of Clinical and Experimental Hypnosis 2007; 55(2): Mishra Bi, Sahoo S, Mishra BA. Management of Treatment-resistant Obsessive- Compulsive Disorder: An Update on Therapeutic Strategies. Ann Indian Acad Neurol 2007; 10(3): Abudy A, Juven-Wetzler A, Zohar J. Pharmacological Management of Treatment- Resistant Obsessive-Compulsive Disorder. CNS Drugs 2011; 25(7): Butwicka A, Gmitrowicz A. Symptom Clusters in Obsessive compulsive Disorder (OCD): Influence of Age and Age of Onset. Eur Child Adolesc Psychiatry 2010; 19(4): Marazzit D, Golia F, Consoli G, et al. Effectiveness of Long-Term Augmentation with Citalopram to Clomipramine in Treatment-Resistant OCD Patients. CNS Spectr 2008; 13(11):
9 11. Boschen MJ, Drummond LM, Pillay A. Treatment of Severe, Treatment- Refractory Obsessive-Compulsive Disorder: A Study of Inpatient and Community Treatment. CNS Spectr 2008; 13(12): Kellner M. Drug Treatment of Obsessive-Compulsive Disorder. Dialogues Clin Neurosci 2010; 12(2): Komossa K, Depping AM, Meyer M, et al. Second-Generation Antipsychotics for Obsessive Compulsive Disorder.Cochrane Database Syst Rev 2010; (12):CD Bandelow B. The Medical Treatment of Obsessive-Compulsive Disorder and Anxiety. CNS Spectr 2008; 13(9 Suppl 14): Dell'Osso B, Mundo E, Altamura AC. Quetiapine Augmentation of Selective Serotonin Reuptake Inhibitors in Treatment-Resistant Obsessive-Compulsive Disorder: A Six-Month Follow-Up Case Series. CNS Spect 2006; 11(11): Maina G, Pessina E, Albert U, et al. 8-Week, Single-Blind, Randomized Trial Comparing Risperidone versus Olanzapine Augmentation of Serotonin Reuptake Inhibitors in Treatment-Resistant Obsessive-Compulsive Disorder. Eur Neuropsychopharmacol 2008; 18(5): Khullar A, Chue P, Tibbo P. Quetiapine and Obsessive-Compulsive Symptoms (OCS): Case Report and Review of Atypical antipsychotic-induced OCS. Journal of Psychiatry & Neuroscience 2011; 26(1): Komossa K, Depping AM, Meyer M, et al. Second-generation Antipsychotic Drugs for Obsessive Compulsive Disorder. Cochrane Database Syst Rev 2010; (12): CD
OCD & Anxiety: Helen Blair Simpson, M.D., Ph.D.
 OCD & Anxiety: Symptoms, Treatment, & How to Cope Helen Blair Simpson, M.D., Ph.D. Professor of Clinical Psychiatry, Columbia University Director of the Anxiety Disorders Clinic, New York State Psychiatric
OCD & Anxiety: Symptoms, Treatment, & How to Cope Helen Blair Simpson, M.D., Ph.D. Professor of Clinical Psychiatry, Columbia University Director of the Anxiety Disorders Clinic, New York State Psychiatric
Psychopharmacotherapy for Children and Adolescents
 TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
TREATMENT GUIDELINES Psychopharmacotherapy for Children and Adolescents Guideline 7 Psychopharmacotherapy for Children and Adolescents Description There are few controlled trials to guide practitioners
TREATMENT-RESISTANT DEPRESSION AND ANXIETY
 University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
University of Washington 2012 TREATMENT-RESISTANT DEPRESSION AND ANXIETY Catherine Howe, MD, PhD University of Washington School of Medicine Definition of treatment resistance Failure to remit after 2
Psychopharmacology. Psychopharmacology. Hamish McAllister-Williams Reader in Clinical. Department of Psychiatry, RVI
 Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Regional Affective Disorders Service Psychopharmacology Northumberland, Tyne and Wear NHS Trust Hamish McAllister-Williams Reader in Clinical Psychopharmacology Department of Psychiatry, RVI Intro NOT
Update on guidelines on biological treatment of depressive disorder. Dr. Henry CHEUNG Psychiatrist in private practice
 Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
Update on guidelines on biological treatment of depressive disorder Dr. Henry CHEUNG Psychiatrist in private practice 2013 update International Task Force of World Federation of Societies of Biological
TREATING MAJOR DEPRESSIVE DISORDER
 TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
TREATING MAJOR DEPRESSIVE DISORDER A Quick Reference Guide Based on Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Second Edition, originally published in April 2000.
Recognizing and Treating Depression in Children and Adolescents.
 Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
Recognizing and Treating Depression in Children and Adolescents. KAREN KANDO, MD Division of Child and Adolescent Psychiatry Center for Neuroscience and Behavioral Medicine Phoenix Children s Hospital
ATYPICALS ANTIPSYCHOTIC MEDICATIONS
 The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
The atypical antipsychotics are a class of drugs that are used to treat a number of behavioral health disorders, including schizophrenia, other psychotic disorders, mood disorders, and behavioral agitation
NICE Clinical guideline 23
 NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
NICE Clinical guideline 23 Depression Management of depression in primary and secondary care Consultation on amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised
Obsessive Compulsive Disorder: a pharmacological treatment approach
 Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Obsessive Compulsive Disorder: a pharmacological treatment approach Professor Alasdair Vance Head, Academic Child Psychiatry Department of Paediatrics University of Melbourne Royal Children s Hospital
Bipolar Disorder. Mania is the word that describes the activated phase of bipolar disorder. The symptoms of mania may include:
 Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Bipolar Disorder What is bipolar disorder? Bipolar disorder, or manic depression, is a medical illness that causes extreme shifts in mood, energy, and functioning. These changes may be subtle or dramatic
Conjoint Professor Brian Draper
 Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Chronic Serious Mental Illness and Dementia Optimising Quality Care Psychiatry Conjoint Professor Brian Draper Academic Dept. for Old Age Psychiatry, Prince of Wales Hospital, Randwick Cognitive Course
Emergency Room Treatment of Psychosis
 OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
OVERVIEW The term Lewy body dementias (LBD) represents two clinical entities dementia with Lewy bodies (DLB) and Parkinson s disease dementia (PDD). While the temporal sequence of symptoms is different
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION
 MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
MOH CLINICAL PRACTICE GUIDELINES 6/2011 DEPRESSION Executive summary of recommendations Details of recommendations can be found in the main text at the pages indicated. Clinical evaluation D The basic
Overview of Mental Health Medication Trends
 America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
America s State of Mind Report is a Medco Health Solutions, Inc. analysis examining trends in the utilization of mental health related medications among the insured population. The research reviewed prescription
Psychotic Disorder. Psychosis. Psychoses may be caused by: Examples of Hallucinations and Delusions 12/12/2012
 Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: [email protected] Web: www.psywellness.com.sg A condition
Psychosis Psychotic Disorder Dr Lim Boon Leng Psychiatrist and Medical Director Dr BL Lim Centre For Psychological Wellness Tel: 64796456 Email: [email protected] Web: www.psywellness.com.sg A condition
Comorbid Conditions in Autism Spectrum Illness. David Ermer MD June 13, 2014
 Comorbid Conditions in Autism Spectrum Illness David Ermer MD June 13, 2014 Overview Diagnosing comorbidities in autism spectrum illnesses Treatment issues specific to autism spectrum illnesses Treatment
Comorbid Conditions in Autism Spectrum Illness David Ermer MD June 13, 2014 Overview Diagnosing comorbidities in autism spectrum illnesses Treatment issues specific to autism spectrum illnesses Treatment
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS. Juanaelena Garcia, MD Psychiatry Director Institute for Family Health
 PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
PSYCHOPHARMACOLOGY AND WORKING WITH PSYCHIATRY PROVIDERS Juanaelena Garcia, MD Psychiatry Director Institute for Family Health Learning Objectives Learn basics about the various types of medications that
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 The European Medicines Agency Evaluation of Medicines for Human Use London, 20 January 2005 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL INVESTIGATION OF MEDICINAL PRODUCTS
The European Medicines Agency Evaluation of Medicines for Human Use London, 20 January 2005 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL INVESTIGATION OF MEDICINAL PRODUCTS
Antidepressant treatment in adults
 Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Antidepressant treatment in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive and
Questions & Answers About OCD In Children and Adolescents
 Questions & Answers About OCD In Children and Adolescents What is Obsessive Compulsive Disorder? Obsessive Compulsive Disorder (OCD) i s one o f the m ost comm on psychiatric illnesses affecting young
Questions & Answers About OCD In Children and Adolescents What is Obsessive Compulsive Disorder? Obsessive Compulsive Disorder (OCD) i s one o f the m ost comm on psychiatric illnesses affecting young
MEDICATIONS AND TOURETTE S DISORDER: COMBINED PHARMACOTHERAPY AND DRUG INTERACTIONS. Barbara Coffey, M.D., Cheston Berlin, M.D., Alan Naarden, M.D.
 MEDICATIONS AND TOURETTE S DISORDER: COMBINED PHARMACOTHERAPY AND DRUG INTERACTIONS Barbara Coffey, M.D., Cheston Berlin, M.D., Alan Naarden, M.D. Introduction Tourette Syndrome (TS) or Tourette s Disorder
MEDICATIONS AND TOURETTE S DISORDER: COMBINED PHARMACOTHERAPY AND DRUG INTERACTIONS Barbara Coffey, M.D., Cheston Berlin, M.D., Alan Naarden, M.D. Introduction Tourette Syndrome (TS) or Tourette s Disorder
Medication Management of Depressive Disorders in Children and Adolescents. Satya Tata, M.D. Kansas University Medical Center
 Medication Management of Depressive Disorders in Children and Adolescents Satya Tata, M.D. Kansas University Medical Center First Line Medications SSRIs Prozac (Fluoxetine): 5-605 mg Zoloft (Sertraline):
Medication Management of Depressive Disorders in Children and Adolescents Satya Tata, M.D. Kansas University Medical Center First Line Medications SSRIs Prozac (Fluoxetine): 5-605 mg Zoloft (Sertraline):
I. The Positive Symptoms...Page 2. The Negative Symptoms...Page 2. Primary Psychiatric Conditions...Page 2
 SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
SUTTER PHYSICIANS ALLIANCE (SPA) 2800 L Street, 7 th Floor Sacramento, CA 95816 SPA PCP Treatment & Referral Guideline Assessment & Treatment of Psychosis Developed March 1, 2003 Revised September 21,
What are the best treatments?
 What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
What are the best treatments? Description of Condition Depression is a common medical condition with a lifetime prevalence in the United States of 15% among adults. Symptoms include feelings of sadness,
CLINICIAN INTERVIEW COMPLEXITIES OF BIPOLAR DISORDER. Interview with Charles B. Nemeroff, MD, PhD
 COMPLEXITIES OF BIPOLAR DISORDER Interview with Charles B. Nemeroff, MD, PhD Dr Nemeroff is the Reunette W. Harris Professor and Chairman of the Department of Psychiatry and Behavioral Sciences at Emory
COMPLEXITIES OF BIPOLAR DISORDER Interview with Charles B. Nemeroff, MD, PhD Dr Nemeroff is the Reunette W. Harris Professor and Chairman of the Department of Psychiatry and Behavioral Sciences at Emory
Algorithm for Initiating Antidepressant Therapy in Depression
 Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
Algorithm for Initiating Antidepressant Therapy in Depression Refer for psychotherapy if patient preference or add cognitive behavioural office skills to antidepressant medication Moderate to Severe depression
DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D.
 DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D. GOALS Learn DSM 5 criteria for DMDD Understand the theoretical background of DMDD Discuss background, pathophysiology and treatment
DSM 5 AND DISRUPTIVE MOOD DYSREGULATION DISORDER Gail Fernandez, M.D. GOALS Learn DSM 5 criteria for DMDD Understand the theoretical background of DMDD Discuss background, pathophysiology and treatment
TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines
 TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines DATE: 01 December 2009 CONTEXT AND POLICY ISSUES: Post-traumatic stress disorder
TITLE: Cannabinoids for the Treatment of Post-Traumatic Stress Disorder: A Review of the Clinical Effectiveness and Guidelines DATE: 01 December 2009 CONTEXT AND POLICY ISSUES: Post-traumatic stress disorder
Step 4: Complex and severe depression in adults
 Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Step 4: Complex and severe depression in adults A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Treatments for Major Depression. Drug Treatments The two (2) classes of drugs that are typical antidepressants are:
 Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
Treatments for Major Depression Drug Treatments The two (2) classes of drugs that are typical antidepressants are: 1. 2. These 2 classes of drugs increase the amount of monoamine neurotransmitters through
BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS
 BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
BRIEF NOTES ON THE MENTAL HEALTH OF CHILDREN AND ADOLESCENTS The future of our country depends on the mental health and strength of our young people. However, many children have mental health problems
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice Parameter for the Assessment and Treatment of Children and Adolescents With Bipolar Disorder,
Neuroscience An extra bit. Dr Sasha Gartside Institute of Neuroscience Newcastle University
 Neuroscience An extra bit Dr Sasha Gartside Institute of Neuroscience Newcastle University Drugs, receptors, and transporters Most psychoactive drugs interfere with neurotransmission The main targets are
Neuroscience An extra bit Dr Sasha Gartside Institute of Neuroscience Newcastle University Drugs, receptors, and transporters Most psychoactive drugs interfere with neurotransmission The main targets are
Understanding Antipsychotic Medications
 Understanding Antipsychotic Medications NARSAD RESEARCH National Alliance for Research on Schizophrenia and Depression 60 Cutter Mill Road, Suite 404 Great Neck, NY 11021 516-829-0091 1-800-829-8289 516-487-6930
Understanding Antipsychotic Medications NARSAD RESEARCH National Alliance for Research on Schizophrenia and Depression 60 Cutter Mill Road, Suite 404 Great Neck, NY 11021 516-829-0091 1-800-829-8289 516-487-6930
NICE clinical guideline 90
 Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Depression in adults The treatment and management of depression in adults Issued: October 2009 NICE clinical guideline 90 guidance.nice.org.uk/cg90 NHS Evidence has accredited the process used by the Centre
Anxiety Disorders Drug Treatment Guidelines
 Western Australian Psychotropic Drugs Committee Anxiety Disorders Drug Treatment Guidelines August 2008 www.watag.org.au Table of Contents Executive Summary... 4 Psychological or pharmacological treatment?...
Western Australian Psychotropic Drugs Committee Anxiety Disorders Drug Treatment Guidelines August 2008 www.watag.org.au Table of Contents Executive Summary... 4 Psychological or pharmacological treatment?...
Depression Flow Chart
 Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression Flow Chart SCREEN FOR DEPRESSION ANNUALLY Assess for depression annually with the PHQ-9. Maintain a high index of suspicion in high risk older adults. Consider suicide risk and contributing
Depression in adults with a chronic physical health problem
 Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Depression in adults with a chronic physical health problem Treatment and management Issued: October 2009 NICE clinical guideline 91 guidance.nice.org.uk/cg91 NICE has accredited the process used by the
Treatment and management of depression in adults, including adults with a chronic physical health problem
 Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Issue date: October 2009 Depression Treatment and management of depression in adults, including adults with a chronic physical health problem This is an update of NICE clinical guideline 23 Developed by
Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of
 Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of antipsychotic agents Identify common adverse effects
Chapter 18 Drugs Used for Psychoses Learning Objectives Identify signs and symptoms of psychotic behavior Describe major indications for the use of antipsychotic agents Identify common adverse effects
Depression: management of depression in primary and secondary care
 Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Issue date: December 2004 Quick reference guide Depression: management of depression in primary and secondary care Clinical Guideline 23 Developed by the National Collaborating Centre for Mental Health
Maintenance treatment for obsessivecompulsive disorder: Findings from a naturalistic setting
 ANNALS OF CLINICAL PSYCHIATRY ANNALS OF CLINICAL PSYCHIATRY 2015;27(1):25-32 RESEARCH ARTICLE Maintenance treatment for obsessivecompulsive disorder: Findings from a naturalistic setting Eric D. Peselow,
ANNALS OF CLINICAL PSYCHIATRY ANNALS OF CLINICAL PSYCHIATRY 2015;27(1):25-32 RESEARCH ARTICLE Maintenance treatment for obsessivecompulsive disorder: Findings from a naturalistic setting Eric D. Peselow,
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 [email protected] www.bpsweb.
 BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 [email protected] www.bpsweb.org Content Outline for the PSYCHIATRIC PHARMACY SPECIALTY
BOARD OF PHARMACY SPECIALITIES 2215 Constitution Avenue, NW Washington, DC 20037-2985 202-429-7591 FAX 202-429-6304 [email protected] www.bpsweb.org Content Outline for the PSYCHIATRIC PHARMACY SPECIALTY
Improving the Recognition and Treatment of Bipolar Depression
 Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
Handout for the Neuroscience Education Institute (NEI) online activity: Improving the Recognition and Treatment of Bipolar Depression Learning Objectives Apply evidence-based tools that aid in differentiating
SESSION K2. When SSRIs Are Not Enough, What Then?
 37th Annual Advanced Practice in Primary and Acute Care Conference: October 9-11, 2014 SESSION K2 3:55 When SSRIs Are Not Enough, What Then? Scott MacHaffie, MN, ARNP S E S S I O N Session Description:
37th Annual Advanced Practice in Primary and Acute Care Conference: October 9-11, 2014 SESSION K2 3:55 When SSRIs Are Not Enough, What Then? Scott MacHaffie, MN, ARNP S E S S I O N Session Description:
Amendments to recommendations concerning venlafaxine
 Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Amendments to recommendations concerning venlafaxine On 31 May 2006 the MHRA issued revised prescribing advice for venlafaxine*. This amendment brings the guideline into line with the new advice but does
Medications Used in the Management of Disruptive Behavior Disorders
 The following medication chart is provided as a brief guide to some of the medications used in the management of various behavior disorders, along with their potential benefits and possible side effects.
The following medication chart is provided as a brief guide to some of the medications used in the management of various behavior disorders, along with their potential benefits and possible side effects.
Best Practices Treatment Guideline for Major Depression
 Best Practices Treatment Guideline for Major Depression Special Report on New Depression Treatment Technology Based on 2010 APA Practice Guidelines Best Practices Guideline for the Treatment of Patients
Best Practices Treatment Guideline for Major Depression Special Report on New Depression Treatment Technology Based on 2010 APA Practice Guidelines Best Practices Guideline for the Treatment of Patients
Depressive disorders among older residents in a Chinese rural community. Risk for Depression by Age and Sex. Risk for Depression by Age and Sex
 Risk for Depression by Age and Sex Risk for Depression by Age and Sex Depressive disorders among older residents in a Chinese rural community. Liu CY, et al: Psychological Medicine 1997:27: 943-949 Male
Risk for Depression by Age and Sex Risk for Depression by Age and Sex Depressive disorders among older residents in a Chinese rural community. Liu CY, et al: Psychological Medicine 1997:27: 943-949 Male
ESCITALOPRAM IN THE TREATMENT OF OBSESSIVE-COMPULSIVE DISORDER: A DOUBLE BLIND PLACEBO CONTROL TRIAL
 ESCITALOPRAM IN THE TREATMENT OF OBSESSIVE-COMPULSIVE DISORDER: A DOUBLE BLIND PLACEBO CONTROL TRIAL M. Nasar Sayeed Khan, Usman Amin Hotiana, Salman Ahmad Department of Psychiatry, SIMS & Services Hospital,
ESCITALOPRAM IN THE TREATMENT OF OBSESSIVE-COMPULSIVE DISORDER: A DOUBLE BLIND PLACEBO CONTROL TRIAL M. Nasar Sayeed Khan, Usman Amin Hotiana, Salman Ahmad Department of Psychiatry, SIMS & Services Hospital,
1. Which of the following SSRIs requires up to a 5-week washout period because of the
 1 Chapter 38. Major Depressive Disorders, Self-Assessment Questions 1. Which of the following SSRIs requires up to a 5-week washout period because of the long half-life of its potent active metabolite?
1 Chapter 38. Major Depressive Disorders, Self-Assessment Questions 1. Which of the following SSRIs requires up to a 5-week washout period because of the long half-life of its potent active metabolite?
Social phobia following maprotiline: The first case report. Mazandaran University of Medical Sciences, Sari, Mazandaran, Iran
 Social phobia following maprotiline: The first case report Seyed Hamzeh Hosseini (MD) 1*, Ebraheim Salehifar (PharmD) 2 1* Associate professor of Psychiatry, Department of Psychiatry, Faculty of Medicine,
Social phobia following maprotiline: The first case report Seyed Hamzeh Hosseini (MD) 1*, Ebraheim Salehifar (PharmD) 2 1* Associate professor of Psychiatry, Department of Psychiatry, Faculty of Medicine,
Obsessive-Compulsive Disorder
 continuing education Obsessive-Compulsive Disorder: An Overview for Pharmacists By Jennifer P. Askew, BS, PharmD, CPP and Emily L. Heil U pon successful completion of this article, the pharmacist should
continuing education Obsessive-Compulsive Disorder: An Overview for Pharmacists By Jennifer P. Askew, BS, PharmD, CPP and Emily L. Heil U pon successful completion of this article, the pharmacist should
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services
 Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
Clinical Guideline / Formulary Document Pharmacy Department Medicines Management Services DEPRESSION Pharmacological Treatment of Depression NICE guidelines suggest the following stepped care model also
These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes.
 This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
This is a new guideline. These guidelines are intended to support General Practitioners in the care of their patients with dementia both in the community and in care homes. It incorporates NICE clinical
Chronic mental illness in LTCF. Chronic mental illness. Other psychiatric disorders.
 Chronic mental illness in LTCF Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Chronic mental illness 1. Schizophrenia and Schizoaffective disorder. 2. Bipolar disorder (Type 1 and
Chronic mental illness in LTCF Abhilash K. Desai MD Medical Director Alzheimer s Center of Excellence Chronic mental illness 1. Schizophrenia and Schizoaffective disorder. 2. Bipolar disorder (Type 1 and
Eating Disorder Treatment Protocol
 Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
Eating Disorder Treatment Protocol All Team Members: Patient Self-Management Education & Support Eating Disorders are incredibly debilitating and are associated with significant medical and psychosocial
[KQ 804] FEBRUARY 2007 Sub. Code: 9105
![[KQ 804] FEBRUARY 2007 Sub. Code: 9105 [KQ 804] FEBRUARY 2007 Sub. Code: 9105](/thumbs/26/8053833.jpg) [KQ 804] FEBRUARY 2007 Sub. Code: 9105 (Revised Regulations) Theory : Two hours and forty minutes Q.P. Code: 419105 Maximum : 100 marks Theory : 80 marks M.C.Q. : Twenty minutes M.C.Q. : 20 marks 1. A
[KQ 804] FEBRUARY 2007 Sub. Code: 9105 (Revised Regulations) Theory : Two hours and forty minutes Q.P. Code: 419105 Maximum : 100 marks Theory : 80 marks M.C.Q. : Twenty minutes M.C.Q. : 20 marks 1. A
Medications for Huntington s Disease Vicki Wheelock, M.D.
 Medications for Huntington s Disease Vicki Wheelock, M.D. Director, HDSA Center of Excellence at UC Davis June 4, 2013 Outline Introduction and disclaimers Medications for cognitive symptoms Medications
Medications for Huntington s Disease Vicki Wheelock, M.D. Director, HDSA Center of Excellence at UC Davis June 4, 2013 Outline Introduction and disclaimers Medications for cognitive symptoms Medications
IMR ISSUES, DECISIONS AND RATIONALES The Final Determination was based on decisions for the disputed items/services set forth below:
 Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
Case Number: CM13-0018009 Date Assigned: 10/11/2013 Date of Injury: 06/11/2004 Decision Date: 01/13/2014 UR Denial Date: 08/16/2013 Priority: Standard Application Received: 08/29/2013 HOW THE IMR FINAL
ADHD PRACTISE PARAMETER. IRSHAAD SHAFFEEULLAH, M.D. A diplomate American Board of CHILD AND ADOLESCENT PSYCHIATRY
 ADHD PRACTISE PARAMETER IRSHAAD SHAFFEEULLAH, M.D. A diplomate American Board of CHILD AND ADOLESCENT PSYCHIATRY Similar type of idea Similar document Similar document AACAP document Neurobiological condition
ADHD PRACTISE PARAMETER IRSHAAD SHAFFEEULLAH, M.D. A diplomate American Board of CHILD AND ADOLESCENT PSYCHIATRY Similar type of idea Similar document Similar document AACAP document Neurobiological condition
Major Depressive Disorder:
 Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Major Depressive Disorder: An Actuarial Commercial Claim Data Analysis July 2013 Prepared by: Milliman, Inc. NY Kate Fitch RN, MEd Kosuke Iwasaki FIAJ, MAAA, MBA This report was commissioned by Takeda
Clinical Practice Guidelines: Attention Deficit/Hyperactivity Disorder
 Clinical Practice Guidelines: Attention Deficit/Hyperactivity Disorder AACAP Official Action: OUTLINE OF PRACTICE PARAMETERS FOR THE ASSESSMENT AND TREATMENT OF CHILDREN, ADOLESCENTS, AND ADULTS WITH ADHD
Clinical Practice Guidelines: Attention Deficit/Hyperactivity Disorder AACAP Official Action: OUTLINE OF PRACTICE PARAMETERS FOR THE ASSESSMENT AND TREATMENT OF CHILDREN, ADOLESCENTS, AND ADULTS WITH ADHD
Current Pharmacological Treatments for Obsessive-Compulsive Disorder
 F E A T U R E A R T I C L E Current Pharmacological Treatments for Obsessive-Compulsive Disorder Alexander Bystritsky, MD Dr. Bystritsky is Professor of Psychiatry and Biobehavioral Sciences and Director
F E A T U R E A R T I C L E Current Pharmacological Treatments for Obsessive-Compulsive Disorder Alexander Bystritsky, MD Dr. Bystritsky is Professor of Psychiatry and Biobehavioral Sciences and Director
Rogers Memorial Hospital (Wisconsin).
 Bradley C. Riemann, Ph.D. Clinical Director, OCD Center and CBT Services Rogers Memorial Hospital The Use of Exposure and Ritual Prevention with OCD: Key Concepts and New Directions OCD Center Rogers Memorial
Bradley C. Riemann, Ph.D. Clinical Director, OCD Center and CBT Services Rogers Memorial Hospital The Use of Exposure and Ritual Prevention with OCD: Key Concepts and New Directions OCD Center Rogers Memorial
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller
 Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Elizabeth A. Crocco, MD Assistant Clinical Professor Chief, Division of Geriatric Psychiatry Department of Psychiatry and Behavioral Sciences Miller School of Medicine/University of Miami Question 1 You
Depression Pathway. Patient Education Box 4. Guided self help Box 18. pg 11
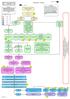 LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
LCFT localised Map pathway June 2009 Depression Pathway Instructions: Throughout this pathway if you click on the Bookmarks tab to the left of the screen and then click on the various documents you will
MOH CLINICAL PRACTICE GUIDELINES 2/2008 Prescribing of Benzodiazepines
 MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
MOH CLINICL PRCTICE GUIELINES 2/2008 Prescribing of Benzodiazepines College of Family Physicians, Singapore cademy of Medicine, Singapore Executive summary of recommendations etails of recommendations
The Pharmacological Management of Depression in the Adult Person with Mental Retardation and Developmental Disabilities (MR/DD)
 The Pharmacological Management of Depression in the Adult Person with Mental Retardation and (MR/DD) 1. Overview Multiple classes of medications are available for treatment of depression in the patient
The Pharmacological Management of Depression in the Adult Person with Mental Retardation and (MR/DD) 1. Overview Multiple classes of medications are available for treatment of depression in the patient
and body dysmorphic disorder (BDD) in adults, children and young people Issue date: November 2005
 Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Issue date: November 2005 Treating obsessivecompulsive disorder (OCD) and body dysmorphic disorder (BDD) in adults, children and young people Understanding NICE guidance information for people with OCD
Second-generation antipsychotics for obsessive compulsive disorder (Review)
 Second-generation antipsychotics for obsessive compulsive disorder (Review) Komossa K, Depping AM, Meyer M, Kissling W, Leucht S This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Second-generation antipsychotics for obsessive compulsive disorder (Review) Komossa K, Depping AM, Meyer M, Kissling W, Leucht S This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
PTSD Evidence Based Practice Recommendations
 PTSD Evidence ased Practice Recommendations Jason's ox est Practice Group Dr. Sam Moreno, Michelle Schnack Compilation & consolidation of the research and recommendations located in: The VA/DoD Clinical
PTSD Evidence ased Practice Recommendations Jason's ox est Practice Group Dr. Sam Moreno, Michelle Schnack Compilation & consolidation of the research and recommendations located in: The VA/DoD Clinical
Major Depression. What is major depression?
 Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Major Depression What is major depression? Major depression is a serious medical illness affecting 9.9 million American adults, or approximately 5 percent of the adult population in a given year. Unlike
Psychotic Disorders. Goals. Goals continued. Goals continued. What is Psychosis? Where does it occur? Provide a working definition for psychosis
 Psychotic Disorders Robert W. Marvin, MD Assistant Professor Acting Residency Training Director Department of Psychiatry [email protected] 1 Goals Provide a working definition for psychosis Understand the
Psychotic Disorders Robert W. Marvin, MD Assistant Professor Acting Residency Training Director Department of Psychiatry [email protected] 1 Goals Provide a working definition for psychosis Understand the
2013/14 NHS STANDARD CONTRACT FOR SEVERE OBSESSIVE COMPULSIVE DISORDER AND BODY DYSMORPHIC DISORDER SERVICE (ADULTS AND ADOLESCENTS)
 C09/S(HSS)/a 2013/14 NHS STANDARD CONTRACT FOR SEVERE OBSESSIVE COMPULSIVE DISORDER AND BODY DYSMORPHIC DISORDER SERVICE (ADULTS AND ADOLESCENTS) PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATION
C09/S(HSS)/a 2013/14 NHS STANDARD CONTRACT FOR SEVERE OBSESSIVE COMPULSIVE DISORDER AND BODY DYSMORPHIC DISORDER SERVICE (ADULTS AND ADOLESCENTS) PARTICULARS, SCHEDULE 2 THE SERVICES, A - SERVICE SPECIFICATION
Post-traumatic stress disorder overview
 Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
Post-traumatic stress disorder overview A NICE pathway brings together all NICE guidance, quality standards and materials to support implementation on a specific topic area. The pathways are interactive
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå. aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí=
 `çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
`çããçå=jéåí~ä= aáëçêçéêëw=^åñáéíó=~åç= aééêéëëáçå aêk=`=f=lâçåü~ jéçáå~ä=aáêéåíçê lñäé~ë=kep=cçìåç~íáçå=qêìëí= Overview: Common Mental What are they? Disorders Why are they important? How do they affect
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over
 Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
Depression is a common biological brain disorder and occurs in 7-12% of all individuals over the age of 65. Specific groups have a much higher rate of depression including the seriously medically ill (20-40%),
DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE
 1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
1 DEPRESSION CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for depression and any history of depression? 2. Did staff
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD
 Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Post Traumatic Stress Disorder (PTSD) Karen Elmore MD Robert K. Schneider MD Revised 5-11-2001 by Robert K. Schneider MD Definition and Criteria PTSD is unlike any other anxiety disorder. It requires that
Obsessive Compulsive Disorder What you need to know to help your patients
 Obsessive Compulsive Disorder What you need to know to help your patients By Renae M. Reinardy, PsyD, LP, and Jon E. Grant, MD Obsessive compulsive disorder (OCD) is a condition that affects millions of
Obsessive Compulsive Disorder What you need to know to help your patients By Renae M. Reinardy, PsyD, LP, and Jon E. Grant, MD Obsessive compulsive disorder (OCD) is a condition that affects millions of
Antidepressants in Pregnancy D R S N E H A P A R G H I
 Antidepressants in Pregnancy D R S N E H A P A R G H I Overview Depression and its effects Antidepressants and their effects Birth defects Miscarriage Neonatal withdrawal Longterm consequences Breastfeeding
Antidepressants in Pregnancy D R S N E H A P A R G H I Overview Depression and its effects Antidepressants and their effects Birth defects Miscarriage Neonatal withdrawal Longterm consequences Breastfeeding
Antipsychotic drugs are the cornerstone of treatment
 Article Effectiveness of Olanzapine, Quetiapine, Risperidone, and Ziprasidone in Patients With Chronic Schizophrenia Following Discontinuation of a Previous Atypical Antipsychotic T. Scott Stroup, M.D.,
Article Effectiveness of Olanzapine, Quetiapine, Risperidone, and Ziprasidone in Patients With Chronic Schizophrenia Following Discontinuation of a Previous Atypical Antipsychotic T. Scott Stroup, M.D.,
Depression in Older Persons
 Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Depression in Older Persons How common is depression in later life? Depression affects more than 6.5 million of the 35 million Americans aged 65 or older. Most people in this stage of life with depression
Autism Spectrum Disorders and Comorbid Behavioral Health Symptoms
 Autism Spectrum Disorders and Comorbid Behavioral Health Symptoms Cynthia King, MD Child and Adolescent Psychiatrist Associate Professor of Psychiatry UNMSOM Psychopharmacologic and Alternative Medicine
Autism Spectrum Disorders and Comorbid Behavioral Health Symptoms Cynthia King, MD Child and Adolescent Psychiatrist Associate Professor of Psychiatry UNMSOM Psychopharmacologic and Alternative Medicine
Abnormal Psychology PSY-350-TE
 Abnormal Psychology PSY-350-TE This TECEP tests the material usually taught in a one-semester course in abnormal psychology. It focuses on the causes of abnormality, the different forms of abnormal behavior,
Abnormal Psychology PSY-350-TE This TECEP tests the material usually taught in a one-semester course in abnormal psychology. It focuses on the causes of abnormality, the different forms of abnormal behavior,
Medications for bipolar disorder
 Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Medications for bipolar disorder Findings from Australian National Survey of Mental Health and Wellbeing (Mitchell et al, 2004) In 12 months, only one-third saw a mental health professional 40% received
Off-Label Use of Second Generation Antipsychotics in Anxiety Disorders and Obsessive Compulsive Disorder
 Activitas Nervosa Superior Rediviva Volume 52 No. 4 2010 REVIEW ARTICLE Off-Label Use of Second Generation Antipsychotics in Anxiety Disorders and Obsessive Compulsive Disorder Jan Praško 1,2,3, Klára
Activitas Nervosa Superior Rediviva Volume 52 No. 4 2010 REVIEW ARTICLE Off-Label Use of Second Generation Antipsychotics in Anxiety Disorders and Obsessive Compulsive Disorder Jan Praško 1,2,3, Klára
