Prostate Cancer Management and Referral Guidance
|
|
|
- Grant Franklin
- 8 years ago
- Views:
Transcription
1 Prostate Cancer Management and Referral Guidance
2 Prostate Cancer Working Group and Ministry of Health Prostate Cancer Management and Referral Guidance. Wellington: Ministry of Health. Published in September 2015 by the Ministry of Health PO Box 5013, Wellington 6145, New Zealand ISBN: (online) HP 6270 This document is available at: This work is licensed under the Creative Commons Attribution 4.0 International licence. In essence, you are free to: share ie, copy and redistribute the material in any medium or format; adapt ie, remix, transform and build upon the material. You must give appropriate credit, provide a link to the licence and indicate if changes were made.
3 Contents Introduction 1 Algorithm for supporting men with prostate-related concerns 3 Note 1: Preliminary considerations for men considering prostate cancer testing 4 Note 2: Prostate specific antigen (PSA) testing 8 Note 3: Digital rectal examination (DRE) 9 Note 4: Red flags that may indicate advanced or metastatic prostate cancer 10 Note 5: Follow-up options after a normal PSA and DRE 11 Note 6: Referral to a specialist service 12 References 13 Prostate Cancer Management and Referral Guidance iii
4
5 Introduction About this guidance This guidance is to help primary care practitioners provide men and their family and whānau with consistent, culturally appropriate information on prostate cancer testing and treatment. The guidance includes an algorithm to help primary care practitioners have an informed discussion with men who present with prostate-related concerns. Explanatory notes provide more detailed information on each of the steps involved. This guidance has been endorsed by: The Royal New Zealand College of General Practitioners The Prostate Cancer Foundation of New Zealand The Urological Society of Australia and New Zealand The New Zealand Urological Nurses Society The New Zealand Society of Pathologists. Need for this guidance New Zealand men currently receive conflicting advice about prostate cancer testing and treatment. Some men may benefit from early diagnosis and treatment, but have limited opportunity to access appropriate health services. Unlike other cancers, prostate cancer often grows slowly. With routine prostate specific antigen (PSA) testing, many men can be diagnosed with a cancer that is not going to progress during their lifetime. Such a diagnosis may increase men s exposure to unnecessary treatment-related harms. On the other hand, some men will still develop aggressive and potentially life-threatening prostate cancer. These men may benefit from prompt diagnosis and treatment. Development process for this guidance This guidance was developed by the Primary Care Sub-group of the Prostate Cancer Working Group. 1 The Prostate Cancer Working Group supports and advises the Ministry of Health to implement the Prostate Cancer Awareness and Quality Improvement Programme (AQIP), 2 which aims to improve prostate cancer care for New Zealand men by: giving men better and more equitable access to information about prostate cancer testing and treatment supporting primary care practitioners to manage men presenting with prostate-related concerns removing barriers that restrict men s access to diagnostic and treatment services giving men consistent care and equitable outcomes across the entire care pathway. 1 For more information on the Prostate Cancer Working Group, visit: 2 For more information on the AQIP, visit: Prostate Cancer Management and Referral Guidance 1
6 This guidance is largely based on the recommendations of the Prostate Cancer Taskforce. 3 However, other publications were also considered, including the National Institute of Clinical Excellence s guidance on prostate cancer: diagnosis and treatment (Carter et al 2013), the European Randomised Study of Screening for Prostate Cancer (Schröder et al 2014) and the guidance on prostate cancer diagnosis and treatment produced by a number of other jurisdictions. The Primary Care Sub-group acknowledges the evidence around prostate cancer testing and treatment continues to evolve. This guidance will be revised every two years, with subsequent versions published on the Ministry of Health s website ( It was sent out to numerous stakeholders for comment before publication, including: district health boards primary health organisations relevant professional colleges non-governmental organisations, such as the Prostate Cancer Foundation and the Cancer Society. It is part of a suite of resources being developed under the AQIP. Other resources that will be developed over the next two years include: an electronic decision support tool to help men s decision-making around prostate cancer testing and treatment guidance on the use of active surveillance guidance on the pathologic diagnosis and staging of prostate cancer guidance on managing men with advanced or metastatic prostate cancer patient information for men and their family and whānau. Integrating this guidance into routine clinical practice District health boards and primary health organisations are responsible for integrating this guidance into their clinical pathways for prostate cancer in a way that reflects the particular needs of their patients and communities. When using this guidance, primary care practitioners should be conscious of the disparities that exist in prostate cancer outcomes for different men, such as for Māori men or men who live in rural areas. For example, Māori men are less likely to be diagnosed with prostate cancer than non-māori men, but are 37 percent more likely to die from the disease (Ministry of Health 2014). The reasons behind these disparities are not well understood. However, in part, they appear to be related to differences in the access that different groups of men have to appropriate information and diagnostic and treatment services. 3 For more information on the recommendations of the Prostate Cancer Taskforce, visit: 2 Prostate Cancer Management and Referral Guidance
7 Algorithm for supporting men with prostate-related concerns Man presents with prostate-related concerns If aged 50 to 70 years, or over 40 years with a family history of prostate cancer, obtain informed consent before testing by discussing: the benefits and risks of PSA testing and/or DRE the implications of further testing if the PSA or DRE is abnormal. (See Note 1.) Note: Carefully consider each man s individual context when discussing benefits and risks. Normal PSA and DRE PSA test and DRE Abnormal PSA (See Note 2.) Abnormal DRE (See Note 3.) Man decides not to be tested No further action required Are any of the Red Flags present? (See Note 4.) NO Treat urinary tract infection (UTI) or prostatitis if present YES Red Flags Acute neurological symptoms Renal failure Bone pain Macroscopic haematuria (without UTI) Repeat PSA test after 6 12 weeks Is the second PSA result abnormal? NO YES Does the man have a first-degree relative who was diagnosed with prostate cancer under 65 years? NO YES Discuss followup options including no futher testing (See Note 5.) Recommend repeat PSA and DRE every 12 months (See Note 5.) Obtain informed consent and refer to urology service (See Note 6.) Prostate Cancer Management and Referral Guidance 3
8 Note 1: Preliminary considerations for men considering prostate cancer testing 1.1. Age If men are considering being tested, they need to know there is no clear evidence on what age men should begin prostate cancer testing. The best recommendation is for primary care practitioners to discuss the benefits and risks of prostate cancer testing with men aged between 50 and 70 years and men aged over 40 years who have a family history of prostate cancer, as they are the most likely to benefit (Andriole et al 2009; Schröder et al 2009). There is no strong evidence to suggest that testing men over the age of 70 years reduces mortality from prostate cancer in this age group. Generally men aged over 70 years, who have a normal-feeling prostate on digital rectal examination (DRE) and who have had normal PSA tests in the past, should be advised they are not likely to benefit from any further PSA testing. Some men aged over 70 years who have a family history of prostate cancer or who have had a previously raised PSA level may benefit from further monitoring if they are otherwise well and have a life expectancy of more than 10 years (Hugosson et al 2010) Family history A man is defined as having a family history of prostate cancer if he has at least one first-degree relative (father or brother) who was diagnosed with prostate cancer. Men with a family history of prostate cancer are twice as likely to develop the disease than men without a family history. If a man has two or more first-degree relatives who were diagnosed with prostate cancer under the age of 65 years, then his risk increases by 5 11 times (Steinberg et al 1990). A small group of men with prostate cancer (about 9 percent) will have the true hereditary form of the disease, which is defined as three or more affected relatives or at least two relatives who have developed prostate cancer before the age of 55 years (Steinberg et al 1990; Bratt 2002). Patients with hereditary prostate cancer usually develop the disease six to seven years earlier than other men, but have about the same chance of developing a more aggressive form of the disease (Carter et al 1992; Grönberg et al 1996) Ethnicity Inequalities in prostate cancer outcomes are significant in New Zealand. The most notable inequalities are between Māori and non-māori men. In 2011, Māori men were about 18 percent less likely to be diagnosed with prostate cancer than non-māori men, but were 37 percent more likely to die from the disease once diagnosed (taking age and stage into account) (Ministry of Health 2014). The reasons behind these inequalities are not yet well understood (Lamb et al 2008). However, they appear to be related to differences in Māori men s access to appropriate information and to diagnostic and treatment services. Primary care practitioners should work to understand any barriers that exist for Māori men in terms of accessing such services (for example, difficulty getting to a laboratory or outpatient appointment due to work commitments, family needs or transport difficulties). Where possible, primary care practitioners should try to address any individual or system-level barriers, so their patients fully understand why they may need further diagnostic work. 4 Prostate Cancer Management and Referral Guidance
9 1.4. Other demographic and lifestyle factors Men who live in rural or low-decile communities may have restricted access to diagnostic or treatment services, meaning that they may be more likely to have poorer prostate cancer outcomes than men who do not live in such communities. Research shows a disparity in PSA testing across New Zealand, with a higher proportion of men being tested in decile 1 communities compared with decile 10 (Gray et al 2005). It is not known if this higher rate of testing results in better outcomes, or not. However, it suggests a significant disparity in access to health services between men who live in low-decile communities and those in higher-decile communities. There is conflicting evidence whether obesity, smoking, diet, prostatitis or sexually transmitted infections can increase a man s risk of developing prostate cancer (Health Science Center San Antonio 2006; Cancer Research UK 2014; American Cancer Society 2015a, 2015b). In general, these men should be managed in the same way as any other man presenting to their primary care practitioner with prostate-related concerns Obtaining informed consent for prostate cancer testing Primary care practitioners must obtain informed consent (which can be verbal consent) before doing a PSA test and/or DRE. The decision to have a PSA test and/or DRE is entirely the man s, but it is the primary care practitioner s responsibility to make sure the man understands the benefits and risks before he makes his decision. This includes making sure the man understands the benefits and risks of the PSA test and DRE, and the benefits and risks of the procedures he could undergo if he has an abnormal PSA or DRE or is diagnosed with prostate cancer (see Figure 1). Figure 1: Prostate cancer care pathway following referral to a urology service Referral to urology service for assessment Prostate biopsy Biopsy result No prostate biopsy Man followed up according to his prostate cancer risk and preference Prostate cancer diagnosis No cancer detetcted Man followed up according to his prostate cancer risk and preference Active surveillance Curative treatment Non-curative treatment Watchful waiting Treatment of localised disease Treatment of advanced/metastatic disease Surgery and/or radiation therapy Radiation therapy, androgen deprivation therapy, chemotherapy and/or palliative care Prostate Cancer Management and Referral Guidance 5
10 How primary care practitioners present this information will vary depending on each man s needs and level of health literacy. The information that they should provide is included in section 1.6. Men should be invited to bring a support person with them to their appointment with their primary care practitioner. This person could be their partner, a close friend or a member of their extended family or whānau The benefits and risks of prostate cancer testing and treatment The role of primary care practitioners is to provide men and their family and whānau with clear and balanced information about the benefits and risks of prostate cancer testing, so that they can make an informed decision on whether or not to proceed. The information that men need to make an informed decision is included in sections to below. How primary care practitioners provide this information may need to change depending on each man s individual needs Benefits of prostate cancer testing Men and their family and whānau can be reassured that prostate cancer is unlikely to be present if the man s PSA and DRE are normal. If testing indicates that prostate cancer is present, it is likely to be early stage, meaning that the chance of cure is greater (Albertson et al 2005; Cooperberg et al 2010). If a man is found to have localised, low-risk prostate cancer, he has the option of entering an active surveillance programme. 4 This will allow him to delay or avoid potential treatment-related harms Risks of prostate cancer testing PSA testing and DRE can produce false positives due to calcifications in the prostate, prostatitis, urinary tract infection, benign prostatic hypertrophy, recent ejaculation or cycling. PSA testing can also produce false negatives when the prostate cancer releases no or little PSA Risks of prostate biopsy An abnormal PSA test does not confirm that a man has prostate cancer. However, it does indicate the need for further diagnostic testing; usually a prostate biopsy. Risks associated with prostate biopsy include: false negatives (where the biopsy misses the prostate cancer) infection / systemic sepsis (Loeb et al 2013) transient haematuria transient haemospermia transient rectal bleeding. 4 For more information on active surveillance, visit: 6 Prostate Cancer Management and Referral Guidance
11 Risks of active surveillance Men on active surveillance are more likely to die from another cause than from their prostate cancer, but some men on active surveillance will still develop more aggressive disease and may require curative treatment. Men on active surveillance require regular monitoring. This mostly relies on the findings of repeat prostate biopsies, PSA tests, DREs and occasionally MRIs. Some men find active surveillance psychologically stressful. Around percent of men on active surveillance decide to exit the programme in favour of curative treatment or watchful waiting Benefits of curative treatment Curative treatment is successful: in most men with early and moderately advanced disease (70 85 percent relapse-free survival at 10 or more years after treatment) in many men with locally advanced disease (50 60 percent relapse-free survival at 10 or more years after treatment). Outcomes from curative treatment are also affected by co-morbidities, such as diabetes, obesity, cardiovascular disease and respiratory problems Risks of curative treatment Curative treatment of any cancer carries a risk of adverse events, including failure to stop the spread of the disease. The curative options for prostate cancer radical prostatectomy, external beam radiation therapy, high dose rate brachytherapy and low dose rate brachytherapy (seeds) differ in their adverse effect profiles. Some radiation oncology and urology services do not offer high dose rate brachytherapy and low dose rate brachytherapy. All curative treatments have a risk of erectile dysfunction, although erectile dysfunction is not uncommon in men aged over 50 years without prostate cancer (Weber et al 2013). Radical prostatectomy carries the additional risk of urinary incontinence Risks of radical prostatectomy Early risks associated with a surgical procedure, such as wound infections. Later risks include urinary incontinence and erectile dysfunction (Wilt et al 2012; Wallis et al 2015). Wound infections generally resolve themselves quickly with antibiotic treatment, but urinary incontinence and erectile dysfunction may continue indefinitely Risks of radiation therapy Early risks during and for up to several months after radiation therapy include fatigue, acute prostatitis, urethritis, cystitis, and proctitis. The later risks of radiation therapy include erectile dysfunction, rectal bleeding and lower urinary tract symptoms. Prostate Cancer Management and Referral Guidance 7
12 Note 2: Prostate specific antigen (PSA) testing 2.1. General information about PSA PSA is produced by the epithelial cells of the prostate. PSA is organ-specific rather than cancerspecific, meaning that PSA levels may be elevated in the presence of non-malignant prostate conditions, such as benign prostatic hypertrophy or prostatitis (Stamey et al 1987). Other factors may also produce a temporary increase in men s PSA levels. For this reason, men should ideally not have a PSA test within two days of having a DRE or within three days of ejaculation or cycling (National Health and Medical Research Council 2013). If a man consents to having a PSA test as well as a DRE, the PSA test should always be done first The relationship between age, PSA level and prostate cancer Generally the higher a man s PSA level, the more likely it is that he has prostate cancer (Heidenreich 2008). However, some men will have prostate cancer even in the absence of a raised PSA (Thompson et al 2004). Increased PSA levels can be transient, which is why men should always have a repeat PSA test after 6 12 weeks to confirm the result. The exceptions to this are if a man has a raised PSA level and an abnormal DRE or if a man has a raised PSA level and one of the red flags shown in the algorithm on page 3 (see Note 4 for more information on the red flags). Whether a man s PSA result is considered clinically significant or not depends on his age. This is because the benefits of early diagnosis reduce with increasing age. At 70 years old, a man diagnosed with prostate cancer has a 50 percent chance of his prostate cancer becoming symptomatic during his lifetime, but by the time he reaches 75 years of age this risk reduces to 33 percent (Lamb et al 2007). Table 1 identifies what an abnormal PSA level is, by age. If a man s PSA level is between 4.0 µg/l and 10.0 µg/l, there is a 40 percent chance of detecting prostate cancer on prostate biopsy (Leinert et al 2009). If a man s PSA level is between 10.0 µg/l and 20.0 µg/l, there is a 67 percent chance of detecting prostate cancer. A PSA level of more than 20.0 µg/l means that prostate cancer is highly likely to be present and metastases can sometimes be seen on bone or computed tomography (CT) scans. Values over 10 µg/l are rarely the result of benign prostatic hypertrophy, but prostatitis can cause significant and rapid rises in PSA levels. Table 1: Definitions for an abnormal PSA level, by age Age group Abnormal PSA level (µg/l) Men aged 70 years 4.0 Men aged years 10.0 Men aged 76 years Prostate Cancer Management and Referral Guidance
13 Note 3: Digital rectal examination (DRE) Most prostate cancers are located in the peripheral zone of the prostate gland and some can be detected on DRE (Horwich et al 2001). Prostate cancer may present as a hard, discrete nodule or with asymmetry of the prostate gland. An enlarged prostate gland is not a good indicator for prostate cancer if the man s PSA result is normal, as the prostate gland generally increases in size as men age. A man with an abnormal DRE should be referred to a urology service. An abnormal DRE indicates the need for a prostate biopsy, as it can be predictive of more aggressive prostate cancer (Katie et al 2007; Gosselaar et al 2008). Some men may be reluctant to have a DRE. For Māori and Pasifika men, there may also be a cultural barrier to the procedure. Primary care practitioners should inform these men that not every prostate cancer increases PSA and there is a chance that they will still have prostate cancer even if their PSA result is normal. Around 20 percent of prostate cancers are diagnosed from an abnormal DRE when the PSA level is normal. If a man declines a DRE, even after he has been given the above information, it is acceptable to refer him to a urology service based on two clearly abnormal PSA results. Prostate Cancer Management and Referral Guidance 9
14 Note 4: Red flags that may indicate advanced or metastatic prostate cancer If a man has a clearly abnormal PSA result and any of the conditions described in Table 2, he does not need to have a second PSA test before being referred to a urology or radiation oncology service. An abnormal PSA result in the presence of any of these conditions may indicate that the man has advanced or metastatic prostate cancer. For information on the level of urgency required in referring a man with a red flag present to a urology or radiation oncology service, see Note 6. Table 2: Red flags that may indicate advanced or metastatic prostate cancer Red flag Acute neurological symptoms (ie, spinal cord compression) Renal failure Bone pain Macroscopic haematuria (without urinary tract infection) Description Acute neurological symptoms consistent with spinal cord compression or cauda equina compression. The most common is spinal cord compression, which occurs in up to 12 percent of men with metastatic prostate cancer. Spinal cord compression is an emergency. It frequently presents as increasingly severe back pain and subsequent neurological symptoms including weakness, unsteadiness, numbness, urinary retention, urinary incontinence or faecal incontinence. Spinal cord compression less commonly presents as bladder or bowel incontinence or retention/ constipation. Men who present with a clearly abnormal PSA and acute neurological symptoms should be immediately referred to a radiation oncology service or, where no radiation oncology service is available, to a urology service. Delays in referral and diagnosis may influence functional outcome. Early diagnosis and rapid treatment of spinal cord compression are crucial for neurological recovery. Prostate cancer resulting in renal failure is usually evident as locally advanced disease on DRE. Symptoms of renal failure include tiredness, lack of energy, nausea, peripheral oedema and poor appetite. Metastatic prostate cancer may initially present as new-onset, progressive and severe bone pain, often with local tenderness. Men with a clearly abnormal PSA and bone pain should be discussed with a urologist and considered for prostate biopsy and androgen deprivation therapy. If the bone pain is severe, admission to hospital should also be considered for symptom control. Haematuria is rarely associated with prostate cancer but, when it is, it is usually a late sign of locally advanced disease. DRE is often grossly abnormal. Patients with haematuria and a markedly raised PSA level (in the absence of infection) should be discussed with a urologist. 10 Prostate Cancer Management and Referral Guidance
15 Note 5: Follow-up options after a normal PSA and DRE 5.1. Follow-up options for men with a family history of prostate cancer As noted in section 1.2 a man is defined as having a family history of prostate cancer if he has at least one first-degree relative (father or brother) who was diagnosed with prostate cancer. Although there is no strong evidence to support how often to test men with a family history of prostate cancer, best practice suggests that these men should be offered a PSA test and DRE every 12 months from the age of years Follow-up options for men without a family history of prostate cancer To date, there has been no clear evidence to indicate that regularly testing men without a family history of prostate cancer will reduce their risk of prostate cancer mortality. These men, particularly those aged over 70 years, can therefore be reassured further prostate cancer testing is not likely to be of any benefit. However some men will want further testing regardless. If a man with a normal PSA and DRE, or a single abnormal PSA, requests further testing, he should be offered repeat PSA tests and DREs every two to four years, depending on his personal preference (Catalona et al 2011; Basch et al 2012). If his situation changes, use the algorithm on page 3 to guide the decision on whether to refer him to a urology service. Prostate Cancer Management and Referral Guidance 11
16 Note 6: Referral to a specialist service Table 3 identifies how urgently men should be seen by a urology or radiation oncology service, depending on their particular signs and symptoms. These referral criteria aim to ensure that priority is given to: a. men who have progressive or new onset symptoms that may indicate metastatic or advanced prostate cancer (see note 4 for more detail on which acute neurological, renal, bone pain and haematuria symptoms are considered red flags) b. men who are likely to have more advanced localised prostate cancer and who would benefit from early assessment and treatment. For more information on PSA testing and DRE, see Notes 2 and 3. Table 3: Criteria for referral to a urology or radiation oncology service Type of referral Immediate referral (should be seen within 24 hours) Urgent referral (should be seen within 14 days) Routine referral (should be seen within 6 8 weeks) Criteria PSA is 10 µg/l AND severe back pain AND acute neurological symptoms consistent with spinal cord compression or cauda equina compression (Note: Where available, refer to a radiation oncology service in the first instance by phone consult with on-call radiation oncologist) PSA is 10 µg/l AND renal failure is present (Note: Phone consult with an on-call urologist is recommended) PSA is 10 µg/l AND bone pain (new onset, progressive and severe) is present (Note: Phone consult with an oncall urologist is recommended) PSA is 10 µg/l AND macroscopic haematuria is present (Note: Phone consult with an on-call urologist is recommended) PSA is 10 µg/l AND prostate feels hard and/or irregular on DRE PSA is between 4 and 10 µg/l AND macroscopic haematuria is present (in the absence of infection) PSA is < 10 µg/l AND prostate feels hard and/or irregular on DRE Two clearly abnormal PSA results 6 12 weeks apart (see Table 1 on page 8 for definitions of a clearly abnormal PSA) The Government s Faster Cancer Treatment (FCT) programme 5 aims to reduce waiting times for appointments, tests and treatment and standardise care pathways for all patients wherever they live. The rationale for implementing the FCT programme is that prompt treatment is more likely to ensure better outcomes for cancer patients. Men who meet any of the criteria set out in Table 3 are considered to have a high suspicion of cancer. However, only men who require immediate or urgent referral to a urology or radiation oncology service should be included in the cohort for the FCT 62 day health target. 5 For more information on the Faster Cancer Treatment health target, visit: 12 Prostate Cancer Management and Referral Guidance
17 References Albertson PC, Hanley JA, Fine J year outcomes following conservative management of clinically localized prostate cancer. Journal of the American Medical Association 293: American Cancer Society. 2015a. Do we know what causes prostate cancer? URL: prostatecancer/detailedguide/prostate-cancer-what-causes (accessed 24 June 2015). American Cancer Society. 2015b. Prostate cancer risk factors. URL: detailedguide/prostate-cancer-risk-factors (accessed 24 June 2015). Andriole GL, Crawford ED, Grubb RL 3rd, et al Mortality results from a randomized prostate-cancer screening trial. New England Journal of Medicine 360: Basch E, Oliver TK, Vickers A, et al Screening for prostate cancer with prostate-specific antigen testing: American Society of Clinical Oncology provisional clinical opinion. Journal of Clinical Oncology 30: Bratt O Hereditary prostate cancer: Clinical aspects. Journal of Urology 168(3): Cancer Research UK Prostate cancer risk factors overview. URL: cancerstats/types/prostate/riskfactors/prostate-cancer-risk-factors (accessed 01 June 2015). Carter HB, Albertsen PC, Barry MJ, et al Early detection of prostate cancer: AUA Guideline. Journal of Urology 190: Carter BS, Beaty TH, Steinberg GD, Childs B, Walsh PC Mendelian inheritance of familial prostate cancer. Proceedings of the National Academy of Science 89(8): Catalona WJ, Partin AW, Sanda MG, et al A multicenter study of [ 2] pro-prostate specific antigen combined with prostate specific antigen and free prostate specific antigen for prostate cancer detection in the 2.0 to 10.0 ng/ml prostate specific antigen range. Journal of Urology 185: Cooperberg MR, Broering JM, Carroll PR Time trends and local variation in primary treatment of localised prostate cancer. Journal of Clinical Oncology 28: Gosselaar C, Roobol MJ, Roemeling S, et al The role of the digital rectal examination in subsequent screening visits in the European randomized study of screening for prostate cancer (ERSPC), Rotterdam. European Urology 54(3): Gray MA, Borman B, Crampton P, et al Elevated serum prostate-specific antigen levels and public health issues in three New Zealand ethnic groups: European, Maori and Pacific Islands men. New Zealand Medical Journal 118: Grönberg H, Damber L, Damber JE Familial prostate cancer in Sweden: A nationwide register cohort study. Cancer 77(1): Health Science Center San Antonio Prostate Cancer Prevention Trial Risk Calculator Version 2.0. URL: www. myprostatecancerrisk.com (accessed 24 June 2015). Heidenreich A Identification of high-risk prostate cancer: role of prostate-specific antigen, PSA doubling time, and PSA velocity. European Urology 54(5): 976 7; discussion Horwich A, Waxman J, Abel P, et al Tumours of the prostate. In Souhami R, Tannock I, Hohenberger P, Horiot J-C (eds). The Oxford Textbook of Oncology (2nd edn). Oxford: Oxford University Press. Hugosson J, Carlsson S, Aus G, et al Mortality results from the Göteborg randomized population based prostate cancer screening trial. Lancet Oncology 11(8): Katie OT, Roehl KA, Han M, et al Characteristics of prostate cancer detected by digital rectal examination only. Urology 70(6): Lamb DS, Bupha-Intr O, Bethwaite P, et al Prostate cancer: are ethnic minorities disadvantaged? Anticancer Research 28: Lamb DS, Slaney D, Smart R, et al Prostate cancer: the new evidence base for diagnosis and treatment. Pathology 39(6): Leinert AR, Davidson PJ, Wells JE The outcomes of transrectal ultrasound guided biopsy of the prostate in a New Zealand population. New Zealand Medical Journal 122(1288): Prostate Cancer Management and Referral Guidance 13
18 Loeb S, Vellekoop A, Ahmed HU, et al Systematic review of complications of prostate biopsy. European Urology 64: Ministry of Health Cancer: New Registrations and Deaths Wellington: Ministry of Health. National Health and Medical Research Council Prostate-Specific Antigen (PSA) Testing in Asymptomatic Men: Evidence evaluation report. Commonwealth of Australia. URL: (accessed 24 June 2015). Schröder FH, Hugosson J, Roobol MJ, et al Screening and prostate-cancer mortality in a randomized European study. New England Journal of Medicine 360: Schröder FH, Hugosson J, Roobol MJ et al Screening and prostate cancer mortality: Results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet 384: Stamey TA, Yang N, Hay AR, et al Prostate-specific antigen as a serum marker for adenocarcinoma of the prostate. New England Journal of Medicine 317(15): Steinberg GD, Carter BS, Beaty TH, et al Family history and the risk of prostate cancer. Prostate 17(4): Thompson IM, Pauler DK, Goodman PJ, et al Prevalence of prostate cancer among men with a prostate-specific antigen level < or =4.0 ng per milliliter. New England Journal of Medicine 350(22): Wallis CJD, Herschorn S, Saskin R, et al Complications after radical prostatectomy or radiotherapy for prostate cancer: results of a population-based, propensity score-matched analysis. Urology 85: Weber MF, Smith DP, O Connell DL, et al Risk factors for erectile dysfunction in a cohort of men. Medical Journal of Australia 199: Wilt TJ, Brawer MK, Jones KM, et al Radical prostatectomy versus observation for localized prostate cancer. New England Journal of Medicine 367: Prostate Cancer Management and Referral Guidance
Prostate Cancer Management and Referral Guidance
 Prostate Cancer Management and Referral Guidance The Prostate Cancer Management and Referral Guidance has been developed to help primary care health professionals manage men with symptoms suggestive of
Prostate Cancer Management and Referral Guidance The Prostate Cancer Management and Referral Guidance has been developed to help primary care health professionals manage men with symptoms suggestive of
PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa
 PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa Key messages: PSA is present in the benign and malignant prostate There is currently no national screening programme
PSA screening in asymptomatic men the debate continues www.bpac.org.nz keyword: psa Key messages: PSA is present in the benign and malignant prostate There is currently no national screening programme
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Cancer research in the Midland Region the prostate and bowel cancer projects
 Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
Cancer research in the Midland Region the prostate and bowel cancer projects Ross Lawrenson Waikato Clinical School University of Auckland MoH/HRC Cancer Research agenda Lung cancer Palliative care Prostate
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Screening for Prostate Cancer
 Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
Official reprint from UpToDate www.uptodate.com 2013 UpToDate
 Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
Official reprint from UpToDate www.uptodate.com 2013 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment. Always seek
The PSA Test for Prostate Cancer Screening:
 For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
Role of MRI in the Diagnosis of Prostate Cancer, A Proposal
 Clinical and Experimental Medical Sciences, Vol. 1, 2013, no. 3, 111 116 HIKARI Ltd, www.m-hikari.com Role of MRI in the Diagnosis of Prostate Cancer, A Proposal W. Akhter Research Fellow Urology, Bartshealth
Clinical and Experimental Medical Sciences, Vol. 1, 2013, no. 3, 111 116 HIKARI Ltd, www.m-hikari.com Role of MRI in the Diagnosis of Prostate Cancer, A Proposal W. Akhter Research Fellow Urology, Bartshealth
Key Messages for Healthcare Providers
 Cancer Care Ontario: Prostate Cancer Screening with the Prostate- Specific Antigen (PSA) Test Key Messages for Healthcare Providers Considerations for men at average risk Avoid prostate-specific antigen
Cancer Care Ontario: Prostate Cancer Screening with the Prostate- Specific Antigen (PSA) Test Key Messages for Healthcare Providers Considerations for men at average risk Avoid prostate-specific antigen
PSA Testing 101. Stanley H. Weiss, MD. Professor, UMDNJ-New Jersey Medical School. Director & PI, Essex County Cancer Coalition. weiss@umdnj.
 PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition weiss@umdnj.edu September 23, 2010 Screening: 3 tests for PCa A good screening
PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition weiss@umdnj.edu September 23, 2010 Screening: 3 tests for PCa A good screening
Screening for Prostate Cancer
 Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Cancer Expert Working Group on Cancer Prevention and Screening Screening for Prostate Cancer Information for men and their families 1 What is the prostate? 2 What is prostate cancer? prostate The prostate
Diagnosis and Management of Prostate Cancer in New Zealand Men. Recommendations from the Prostate Cancer Taskforce
 Diagnosis and Management of Prostate Cancer in New Zealand Men Recommendations from the Prostate Cancer Taskforce Citation: Prostate Cancer Taskforce. 2012. Diagnosis and Management of Prostate Cancer
Diagnosis and Management of Prostate Cancer in New Zealand Men Recommendations from the Prostate Cancer Taskforce Citation: Prostate Cancer Taskforce. 2012. Diagnosis and Management of Prostate Cancer
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test
 PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication
PSA Testing for Prostate Cancer An information sheet for men considering a PSA Test What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15.
 Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
Virtual Mentor American Medical Association Journal of Ethics January 2011, Volume 13, Number 1: 10-15. CLINICAL CASE The Debate Over Prostate Cancer Screening Guidelines Commentary by Karen E. Hoffman,
PSA: Prostate Cancer Screening
 PSA: Prostate Cancer Screening 42 nd Annual Convention of the Philippines College of Physicians May 7, 2012, SMX Convention Center Jose Albert Cruz Reyes III, MD, FPCS, FPUA, DPBU Institute of Urology
PSA: Prostate Cancer Screening 42 nd Annual Convention of the Philippines College of Physicians May 7, 2012, SMX Convention Center Jose Albert Cruz Reyes III, MD, FPCS, FPUA, DPBU Institute of Urology
The Centers for Medicare & Medicaid Services (CMS) seeks stakeholder comments on the following clinical quality measure under development:
 The Centers for Medicare & Medicaid Services (CMS) seeks stakeholder comments on the following clinical quality measure under development: Title: Non-Recommended PSA-Based Screening Description: The percentage
The Centers for Medicare & Medicaid Services (CMS) seeks stakeholder comments on the following clinical quality measure under development: Title: Non-Recommended PSA-Based Screening Description: The percentage
DECISION AID TOOL PROSTATE CANCER SCREENING WITH PSA TESTING
 DECISION AID TOOL PROSTATE CANCER SCREENING WITH PSA TESTING This booklet is what is often called a decision aid. The goals of a decision aid are to help people better understand their medical choices
DECISION AID TOOL PROSTATE CANCER SCREENING WITH PSA TESTING This booklet is what is often called a decision aid. The goals of a decision aid are to help people better understand their medical choices
Prostate cancer screening. It s YOUR decision!
 Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate Cancer Information and Facts
 Prostate Cancer Information and Facts Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnutsized structure that makes up part of a man's reproductive system.
Prostate Cancer Information and Facts Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnutsized structure that makes up part of a man's reproductive system.
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
Screening for Prostate Cancer
 Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
Screening for Prostate Cancer Review against programme appraisal criteria for the UK National Screening Committee (UK NSC) Version 1: This document summarises the work of ScHARR 1 2 and places it against
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
Prostate cancer is the most common cause of death from cancer in men over age 75. Prostate cancer is rarely found in men younger than 40.
 A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
A.D.A.M. Medical Encyclopedia. Prostate cancer Cancer - prostate; Biopsy - prostate; Prostate biopsy; Gleason score Last reviewed: October 2, 2013. Prostate cancer is cancer that starts in the prostate
Prostate Cancer Screening in Taiwan: a must
 Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Position Statement on Testing for Prostate Cancer
 1 Position Statement on Testing for Prostate Cancer 2 Key Messages There is still no clear evidence to recommend a national screening programme for prostate cancer. General practitioners (GP s) and other
1 Position Statement on Testing for Prostate Cancer 2 Key Messages There is still no clear evidence to recommend a national screening programme for prostate cancer. General practitioners (GP s) and other
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Prostate Cancer Screening Guideline
 Prostate Cancer Screening Guideline Contents Prevention 2 Screening Recommendations 2 Shared Decision Making 2 Test Recommendations 3 Follow-up/Referral 3 Treatment Overview 4 Evidence Summary 4 References
Prostate Cancer Screening Guideline Contents Prevention 2 Screening Recommendations 2 Shared Decision Making 2 Test Recommendations 3 Follow-up/Referral 3 Treatment Overview 4 Evidence Summary 4 References
Guidelines for Cancer Prevention, Early detection & Screening. Prostate Cancer
 Guidelines for Cancer Prevention, Early detection & Screening Prostate Cancer Intervention Comments & Recommendations For primary prevention, it has been suggested that diets low in meat & other fatty
Guidelines for Cancer Prevention, Early detection & Screening Prostate Cancer Intervention Comments & Recommendations For primary prevention, it has been suggested that diets low in meat & other fatty
Prostate-Specific Antigen Based Screening: Controversy and Guidelines
 Prostate-Specific Antigen Based Screening: Controversy and Guidelines Eric H. Kim and Gerald L. Andriole Institutional Address: Washington University School of Medicine 4960 Children's Place Campus Box
Prostate-Specific Antigen Based Screening: Controversy and Guidelines Eric H. Kim and Gerald L. Andriole Institutional Address: Washington University School of Medicine 4960 Children's Place Campus Box
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER
 TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER DILEMMA Thomas J Stormont MD January 2012 http://www.youtube.com/watch?v=8jd 7bAHVp0A&feature=related related INTRODUCTION A government health panel (the
TO SCREEN OR NOT TO SCREEN: THE PROSTATE CANCER DILEMMA Thomas J Stormont MD January 2012 http://www.youtube.com/watch?v=8jd 7bAHVp0A&feature=related related INTRODUCTION A government health panel (the
Getting checked for Prostate Cancer
 Getting checked for Prostate Cancer Quick guide for men and their families and whanau Stay well for your family and whanau. doctor, nurse or health professional about prostate cancer. You should do this
Getting checked for Prostate Cancer Quick guide for men and their families and whanau Stay well for your family and whanau. doctor, nurse or health professional about prostate cancer. You should do this
Prostate Cancer Screening
 Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
PROSTATE CANCER. Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American
 PROSTATE CANCER 1. Guidelines for Screening Risk Factors Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American High-risk men: Family history of prostate
PROSTATE CANCER 1. Guidelines for Screening Risk Factors Normal-risk men: No family history of prostate cancer No history of prior screening Not African-American High-risk men: Family history of prostate
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Update on Prostate Cancer Screening Guidelines
 www.medscape.com Update on Prostate Cancer Screening Guidelines Christine Gonzalez, PharmD, CHHC US Pharmacist Abstract and Introduction Introduction In the United States, prostate cancer is the most common
www.medscape.com Update on Prostate Cancer Screening Guidelines Christine Gonzalez, PharmD, CHHC US Pharmacist Abstract and Introduction Introduction In the United States, prostate cancer is the most common
4/8/13. Pre-test Audience Response. Prostate Cancer 2012. Screening and Treatment of Prostate Cancer: The 2013 Perspective
 Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Pre-test Audience Response Screening and Treatment of Prostate Cancer: The 2013 Perspective 1. I do not offer routine PSA screening, and the USPSTF D recommendation will not change my practice. 2. In light
Clinical Practice Guidelines
 Clinical Practice Guidelines Prostate Cancer Screening CareMore Quality Management CareMore Health System adopts Clinical Practice Guidelines for the purpose of improving health care and reducing unnecessary
Clinical Practice Guidelines Prostate Cancer Screening CareMore Quality Management CareMore Health System adopts Clinical Practice Guidelines for the purpose of improving health care and reducing unnecessary
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT
 MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
The PSA Controversy: Defining It, Discussing It, and Coping With It
 The PSA Controversy: Defining It, Discussing It, and Coping With It 11 TH ANNUAL SYMPOSIUM ON MEN S HEALTH June 12, 2013 The PSA Controversy Defining It, Discussing It and Coping With It As of May 2012,
The PSA Controversy: Defining It, Discussing It, and Coping With It 11 TH ANNUAL SYMPOSIUM ON MEN S HEALTH June 12, 2013 The PSA Controversy Defining It, Discussing It and Coping With It As of May 2012,
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Advice to patients about the PSA (prostate-specific antigen) blood test: frequently-asked questions
 Advice to patients about the PSA (prostate-specific antigen) blood test: frequently-asked questions What is the PSA blood test? If you want more information before deciding to have this test, it is important
Advice to patients about the PSA (prostate-specific antigen) blood test: frequently-asked questions What is the PSA blood test? If you want more information before deciding to have this test, it is important
For further information on screening and early detection of prostate cancer, see the Section entitled Screening for Prostate Cancer.
 Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
There are many different types of cancer and sometimes cancer is diagnosed when in fact you are not suffering from the disease at all.
 About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
Prostate cancer A guide for newly diagnosed men
 Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Prostate cancer A guide for newly diagnosed men 2 Prostate cancer A guide for newly diagnosed men About this booklet This booklet is for men who have recently been diagnosed with prostate cancer. It is
Thomas A. Kollmorgen, M.D. Oregon Urology Institute
 Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Cancer in Primary Care: Prostate Cancer Screening. How and How often? Should we and in which patients?
 Cancer in Primary Care: Prostate Cancer Screening How and How often? Should we and in which patients? PLCO trial (Prostate, Lung, Colorectal and Ovarian) Results In the screening group, rates of compliance
Cancer in Primary Care: Prostate Cancer Screening How and How often? Should we and in which patients? PLCO trial (Prostate, Lung, Colorectal and Ovarian) Results In the screening group, rates of compliance
PCA3 DETECTION TEST FOR PROSTATE CANCER DO YOU KNOW YOUR RISK OF HAVING CANCER?
 PCA3 DETECTION TEST FOR PROSTATE CANCER DO YOU KNOW YOUR RISK OF HAVING CANCER? PCA3 DETECTION TEST FOR PROSTATE CANCER There is a range of methods available to your healthcare professional to verify the
PCA3 DETECTION TEST FOR PROSTATE CANCER DO YOU KNOW YOUR RISK OF HAVING CANCER? PCA3 DETECTION TEST FOR PROSTATE CANCER There is a range of methods available to your healthcare professional to verify the
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Questions to ask my doctor: About prostate cancer
 Questions to ask my doctor: About prostate cancer Being diagnosed with prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it
Questions to ask my doctor: About prostate cancer Being diagnosed with prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it
Draft Clinical Practice Guidelines. PSA Testing and Early Management of Test-Detected Prostate Cancer
 Draft Clinical Practice Guidelines PSA Testing and Early Management of Test-Detected Prostate Cancer Draft November 2014 Prostate Cancer Foundation of Australia and Cancer Council Australia ISBN: This
Draft Clinical Practice Guidelines PSA Testing and Early Management of Test-Detected Prostate Cancer Draft November 2014 Prostate Cancer Foundation of Australia and Cancer Council Australia ISBN: This
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
In 2014, about 233,000 American men. Prostate Cancer Screening
 ELIE MULHEM, MD, Oakland University William Beaumont School of Medicine, Sterling Heights, Michigan NIKOLAUS FULBRIGHT, MD, Providence Hospital, South Lyon, Michigan NORAH DUNCAN, MD, Oakland University
ELIE MULHEM, MD, Oakland University William Beaumont School of Medicine, Sterling Heights, Michigan NIKOLAUS FULBRIGHT, MD, Providence Hospital, South Lyon, Michigan NORAH DUNCAN, MD, Oakland University
Beyond the PSA: Genomic Testing in Localized Prostate Cancer
 Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Beyond the PSA: Genomic Testing in Localized Prostate Cancer Kelvin A. Moses, MD, PhD Vanderbilt University Medical Center Wednesday, December 2, 2015 5:00 p.m. ET/2:00 p.m. PT About ZERO ZERO s mission
Summary 1. KEY FINDINGS The Office of Technology Assessment (OTA) concludes that research has not yet been completed to determine CHAPTER
 CHAPTER 1 Summary 1 rostate cancer is a common and serious malignancy among Medicare-age men. 1 In 1995, 244,000 new cases and 40,400 deaths are anticipated from this disease; men age 65 and older bear
CHAPTER 1 Summary 1 rostate cancer is a common and serious malignancy among Medicare-age men. 1 In 1995, 244,000 new cases and 40,400 deaths are anticipated from this disease; men age 65 and older bear
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
Linköping University Post Print. Randomised prostate cancer screening trial: 20 year follow-up
 Linköping University Post Print Randomised prostate cancer screening trial: 20 year follow-up Gabriel Sandblom, Eberhard Varenhorst, Johan Rosell, Owe Lofman and Per Carlsson N.B.: When citing this work,
Linköping University Post Print Randomised prostate cancer screening trial: 20 year follow-up Gabriel Sandblom, Eberhard Varenhorst, Johan Rosell, Owe Lofman and Per Carlsson N.B.: When citing this work,
Treatment Routes in Prostate Cancer Urological Cancers SSCRG
 1 Treatment Routes in Prostate Cancer Urological Cancers SSCRG Introduction To better understand outcome measures, it is necessary to analyse what treatment pathway a patient has followed after diagnosis.
1 Treatment Routes in Prostate Cancer Urological Cancers SSCRG Introduction To better understand outcome measures, it is necessary to analyse what treatment pathway a patient has followed after diagnosis.
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Focus on PSA Screening for Prostate Cancer Vol. 28 Supplement, February 2012. Prostate Cancer: Should We Be Screening?
 Focus on PSA Screening for Prostate Cancer Vol. 28 Supplement, February 2012 Prostate Cancer: Should We Be Screening? INSIDE THIS ISSUE 2 Why the Controversy? 3 Active Surveillance 4 The Radical Prostatectomy
Focus on PSA Screening for Prostate Cancer Vol. 28 Supplement, February 2012 Prostate Cancer: Should We Be Screening? INSIDE THIS ISSUE 2 Why the Controversy? 3 Active Surveillance 4 The Radical Prostatectomy
Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine
 Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine Case #1 A 55 yo white man with well-controlled hypertension presents for his annual
Prostate Cancer Screening: Are We There Yet? March 2010 Andrew M.D. Wolf, MD University of Virginia School of Medicine Case #1 A 55 yo white man with well-controlled hypertension presents for his annual
The PLCO Trial Not a comparison of Screening vs no Screening
 PSA Screening: Science, Politics and Uncertainty David F. Penson, MD, MPH Hamilton and Howd Chair of Urologic Oncology Professor and Chair, Department of Urologic Surgery Director, Center for Surgical
PSA Screening: Science, Politics and Uncertainty David F. Penson, MD, MPH Hamilton and Howd Chair of Urologic Oncology Professor and Chair, Department of Urologic Surgery Director, Center for Surgical
Questions to Ask My Doctor About Prostate Cancer
 Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Urology Nurse Practitioner Urology Research Nurse Australian Prostate Cancer Research Centre Epworth November 18, 2011
 Urology Nurse Practitioner Helen Crowe Urology Nurse Practitioner Urology Research Nurse Australian Prostate Cancer Research Centre Epworth November 18, 2011 Nurse Practitioner Registered nurse who has
Urology Nurse Practitioner Helen Crowe Urology Nurse Practitioner Urology Research Nurse Australian Prostate Cancer Research Centre Epworth November 18, 2011 Nurse Practitioner Registered nurse who has
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Prostate Cancer Screening Clinical Practice Guideline. Approved by the National Guideline Directors November, 2013
 Prostate Cancer Screening Clinical Practice Guideline This guideline is informational only. It is not intended or designed as a substitute for the reasonable exercise of independent clinical judgment by
Prostate Cancer Screening Clinical Practice Guideline This guideline is informational only. It is not intended or designed as a substitute for the reasonable exercise of independent clinical judgment by
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER
 2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
2010 SITE REPORT St. Joseph Hospital PROSTATE CANCER Humboldt County is located on the Redwood Coast of Northern California. U.S census data for 2010 reports county population at 134,623, an increase of
Prostate Cancer. What is prostate cancer?
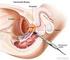 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
DIAGNOSIS OF PROSTATE CANCER
 DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
Understanding the. Controversies of. testosterone replacement. therapy in hypogonadal men with prostate cancer. controversies surrounding
 Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
to Know About Your Partner s
 What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
Prostate Specific Antigen (PSA) Blood Test
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Prostate Specific Antigen (PSA) Blood Test An information guide Prostate Specific Antigen (PSA) Blood Test Prostate Specific Antigen (PSA)
How prostate cancer is diagnosed
 How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
How prostate cancer is diagnosed This information is an extract from the booklet Having tests for prostate cancer. You may find the full booklet helpful. We can send you a free copy see page 7. Contents
CONTENTS: WHAT S IN THIS BOOKLET
 Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Prostate cancer. Christopher Eden. The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing.
 Prostate cancer Christopher Eden The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing. Screening Screening men for PCa (prostate cancer) using PSA (Prostate Specific Antigen blood
Prostate cancer Christopher Eden The Royal Surrey County Hospital, Guildford & The Hampshire Clinic, Old Basing. Screening Screening men for PCa (prostate cancer) using PSA (Prostate Specific Antigen blood
U.S. Preventive Services Task Force
 U.S. Preventive Services Task Force Screening for Prostate Cancer: Recommendation Statement See related Putting Prevention into Practice on page 283. This summary is one in a series excerpted from the
U.S. Preventive Services Task Force Screening for Prostate Cancer: Recommendation Statement See related Putting Prevention into Practice on page 283. This summary is one in a series excerpted from the
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Understanding Prostate Cancer. The Urology Group Guide for Newly Diagnosed Patients. Advanced Care. Improving Lives.
 Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
November 25, 2015. Albert L Siu, MD, MSPH Chair, US Preventive Services Task Force 5600 Fishers Lane, Mail Stop 06E53A Rockville, MD 20857
 November 25, 2015 Men's Health Network P. O. Box 75972 Washington, D.C. 20013 202-543-MHN-1 (6461) Fax 202-543-2727 Albert L Siu, MD, MSPH Chair, US Preventive Services Task Force 5600 Fishers Lane, Mail
November 25, 2015 Men's Health Network P. O. Box 75972 Washington, D.C. 20013 202-543-MHN-1 (6461) Fax 202-543-2727 Albert L Siu, MD, MSPH Chair, US Preventive Services Task Force 5600 Fishers Lane, Mail
PROSTATE CANCER CONTENTS. December 2013 MICA (P) 035/05/2012
 December 2013 MICA (P) 035/05/2012 PROSTATE CANCER What is Prostate Cancer? Prostate cancer generally affects men over 50 and is rare in younger men. It is the uncontrolled spread or malignant growth of
December 2013 MICA (P) 035/05/2012 PROSTATE CANCER What is Prostate Cancer? Prostate cancer generally affects men over 50 and is rare in younger men. It is the uncontrolled spread or malignant growth of
CLINICAL PRACTICE. Clinical Practice. The PSA Test
 Clinical Practice This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review of formal guidelines,
Clinical Practice This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review of formal guidelines,
Clinical guideline Published: 8 January 2014 nice.org.uk/guidance/cg175
 Prostate cancer: diagnosis and management Clinical guideline Published: 8 January 2014 nice.org.uk/guidance/cg175 NICE 2014. All rights reserved. Contents Introduction... 4 Drug recommendations... 5 Patient-centred
Prostate cancer: diagnosis and management Clinical guideline Published: 8 January 2014 nice.org.uk/guidance/cg175 NICE 2014. All rights reserved. Contents Introduction... 4 Drug recommendations... 5 Patient-centred
PSA Screening and the USPSTF Understanding the Controversy
 PSA Screening and the USPSTF Understanding the Controversy Peter C. Albertsen Division of Urology University of Connecticut Farmington, CT, USA USPSTF Final Report 1 Four Key Questions 1. Does PSA based
PSA Screening and the USPSTF Understanding the Controversy Peter C. Albertsen Division of Urology University of Connecticut Farmington, CT, USA USPSTF Final Report 1 Four Key Questions 1. Does PSA based
An Empirical Evaluation of Guidelines on Prostate-specific Antigen Velocity in Prostate Cancer Detection
 DOI: 10.1093/jnci/djr028 ARTICLE JNCI djr028 MA JOURNAL NAME Art. No. CE Code The Author 2011. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
DOI: 10.1093/jnci/djr028 ARTICLE JNCI djr028 MA JOURNAL NAME Art. No. CE Code The Author 2011. Published by Oxford University Press. All rights reserved. For Permissions, please e-mail: journals.permissions@oup.com.
