Evaluation of a Primary Care Dermatology Service: final report
|
|
|
- Randolph Bennett
- 10 years ago
- Views:
Transcription
1 Evaluation of a Primary Care Dermatology Service: final report Report for the National Co-ordinating Centre for NHS Service Delivery and Organisation R&D (NCCSDO) December 2005 prepared by Chris Salisbury* Alison Noble* Sue Horrocks Jo Coast Sian Noble Zoe Crosby Viv Harrison Oya Asim David de Berker Tim Peters* *Academic Unit of Primary Health Care, Department of Community Based Medicine, University of Bristol, Bristol Faculty of Health and Social Care, University of West of England, Bristol Department of Social Medicine, University of Bristol, Bristol Department of Primary Health Care, University of Southampton, Southampton Bristol Royal Infirmary, Bristol Address for correspondence Professor Chris Salisbury, Professor of Primary Health Care, Academic Unit of Primary Health Care, University of Bristol, Cotham House, Cotham Hill, Bristol BS6 6JL, UK Tel: ; [email protected]
2 Executive Summary Introduction The NHS Plan promoted the concept of the general practitioner with special interests (GPSI). There were a number of factors leading to this initiative, in particular the need to increase capacity in the face of rising demand for specialist advice and to reduce excessive waiting lists for hospital outpatient appointments. Many GPSI schemes have been established by Primary Care Trusts (PCTs) in a number of clinical fields, but there is a lack of evidence about the costs and benefits of these schemes. A GPSI service for dermatology was established in Bristol in 2001, and was subject to rigorous evaluation. Dermatology represents one of the most common causes for consultation in primary care and for referral to secondary care. More GPSIs are operating in dermatology than in any other clinical speciality, other than diabetes. Setting and intervention The Bristol Primary Care Dermatology Service (PCDS) is staffed by two GPSIs and a specialist nurse, and is provided from a suburban health centre. It provides care for patients referred by general practitioners in the area served by Bristol South and West PCT. Patients are referred by their general practitioners (GPs) to the outpatient Dermatology Centre at the Bristol Royal Infirmary as usual. Those who appear on the basis of their referral letter to be suitable for management in the PCDS are given an appointment there rather than at the outpatient department. At the time of the trial, suitable patients were adults with non-urgent skin conditions with a provisional diagnosis made by their GP. Aims and objectives Aim The aim of this study was to investigate the effectiveness, costeffectiveness, accessibility and acceptability of a PCDS in comparison with a hospital outpatient clinic for dermatology. Research objectives To determine the proportion of patients referred by general practitioners with dermatological problems which can be managed in a PCDS rather than a specialist dermatology hospital outpatient clinic. NCCSDO
3 To determine whether a PCDS impacts on access to care for patients. To compare the effectiveness and cost-effectiveness of providing care in a PCDS or a hospital outpatient clinic. Costs are assessed from a societal perspective with patient costs and NHS costs clearly distinguished. To determine patients satisfaction with care received in the PCDS compared with a hospital outpatient clinic. Overview of study design A randomised controlled trial comparing patients referred to the PCDS with those receiving usual care at the hospital outpatient clinic. An economic evaluation providing data about the cost-effectiveness of these alternative models of service provision. Analysis of routine data from the study PCT and three neighbouring trusts, providing further information about referral rates and waiting times for appointments. A qualitative study exploring issues that were important to patients in relation to improving access to dermatology services. A discrete-choice modelling study quantifying patients preferences for different aspects of access to dermatology services. and results Randomised controlled trial All adult dermatology referrals from 30 practices in one PCT area over 14 months were triaged according to potential suitability for PCDS, and suitable patients invited to participate. Consenting patients were randomised in a 2:1 ratio to the PCDS or usual outpatient care. Primary outcomes were disease-related quality of life (Dermatology Life Quality Index (DLQI), with higher scores reflecting worse quality of life) and improved patient-perceived access (using a new scale devised for this study, scored out of 100). Secondary outcomes were waiting times, rates of non-attendance (did not attend (DNA) rates), patient satisfaction (Consultation Satisfaction Questionnaire (CSQ), scored out of 100) and patient preference. Outcomes were assessed 9 months after randomisation. Analysis was by intention-to-treat. Process measures included follow-up rates at the PCDS or hospital. Sample-size calculations were based on seeking to establish equivalence between the PCDS and hospital in terms of effectiveness (the DLQI). A sample size of 290 patients in the primary-care arm and 145 patients in the hospital arm would provide 80% power to rule out NCCSDO
4 differences larger than standard deviations in either direction, on the basis of two-sided 95% confidence intervals and assuming no difference between the two groups in terms of (true) effectiveness. Of all referrals, 49% (987/2028) appeared from the referral letter to be suitable for management in the PCDS. After exclusions, of the 768 patients eligible, 556 (72%) were randomised, 354 to PCDS and 202 to outpatients. After 9 months, 422 (76%) were followed up. Patient characteristics in trial arms were similar at baseline. There were no marked differences between the PCDS and hospital care in respect of clinical outcome (median DLQI was 1 in both arms; ratio of geometric means, 0.99; 95% confidence interval (CI), ; P=0.9, adjusting for baseline and stratification). The PCDS was more accessible (the difference between means on the access scale (scored out of 100) was 14; 95% CI, 11 19; P<0.001) and patients had reduced waiting times by a mean of 40 days (95% CI, days; P<0.001). Patients expressed slightly greater satisfaction with PCDS consultations (difference in mean CSQ, 4%; 95% CI, 1 7%; P=0.011) and were more likely to prefer care at PCDS, both at baseline and after 9 months. Fewer PCDS patients (6%) than hospital patients (11%) failed to attend their initial appointment, but overall DNA rates for new and follow-up appointments were similar in both sites (PCDS, 8%; hospital, 11%). Of those patients seen initially at PCDS, 12% were referred to the hospital for one or more follow-up appointments. Economic evaluation Costs were evaluated from the perspective of the NHS, patients, their families and society for the 9 months following randomisation. Costs identified as being important included: the costs of consultation in secondary and primary-care services; investigations, medication and procedures; travel costs; over-the-counter costs; costs of private treatment; and costs of lost production. Resource-use data were collected from a combination of NHS computerised systems and patient questionnaires, and were valued at 2004 prices using data from the hospital, the PCDS and a variety of national sources. Costeffectiveness, using the two primary outcomes of the DLQI and improved patient-perceived access, was assessed in terms of incremental cost-effectiveness ratios and cost-effectiveness acceptability curves. Cost-consequences are presented in relation to all costs and both primary and secondary outcomes from the trial. One sensitivity analysis was conducted to estimate the impact of increasing the number of patients seen in the PCDS. NCCSDO
5 The costs to the NHS of the PCDS were considerably greater than the costs of hospital outpatient care (cost per patient over 9 months: PCDS, ; hospital, ). This was mainly due to the higher costs of doctors and nurses time, which were related to the longer consultations at the PCDS, the higher number of consultations received by patients in the PCDS and the higher cost of nurse consultations. The cost to patients of attending the PCDS was less than that of attending the hospital, as was the cost of lost production. This was due to the finding that patients attending the PCDS lost less time from work. Based on analysis with imputation of missing data, costs to patients and companions were 48 at PCDS and 51 at hospital; costs of lost production were 27 at PCDS and 34 at hospital. The incremental cost-effectiveness ratios for PCDS over hospital care were (i) 540 per one-point gain in the DLQI and (ii) 66 per ten-point change in the access scale. Overall, when NHS, patient and lost production costs were combined, the cost of providing care at the PCDS was greater than the cost of providing hospital outpatient care. This overall finding was not influenced by the sensitivity analysis. Analysis of waiting times and referral rates Routine data about referrals to dermatology outpatient departments from GPs in the study PCT and three neighbouring PCTS were obtained from the Avon Information Management and Technology consortium. Descriptive analysis was conducted, as the small number of trusts and the high level of month-to-month variation made statistical comparison inappropriate. Before the study began the acute trust that was the focus of this research had lower waiting times than other trusts. Over the period of the study waiting times in neighbouring trusts improved so that mean waiting times converged at about 65 days in all trusts. Between 2001 and 2004 the number of referrals to dermatology from GPs in the study PCT increased by 22%, compared with smaller increases in the neighbouring PCTs. The total number of patients transferred from the outpatient department in this study to the PCDS represented just 8% of all referrals received. Therefore it is unlikely that the PCDS would have a major impact on waiting times at the acute trust. NCCSDO
6 Qualitative study Twenty patients suitable for the PCDS but not involved in the randomised controlled trial were interviewed using a semi-structured interview schedule. Exploratory analysis using constant comparison and grounded theory techniques was used. Interviews and analysis proceeded iteratively through a series of rounds. The acceptability of a local dermatology service was influenced by four inter-related themes: participants perception of their need (urgency) for diagnosis or treatment, which influenced their willingness to wait for an appointment; their experience of primary-care services; their perception of what constitutes specialist expertise and factors relating to the convenience of the respective services. Discrete-choice modelling The interviews conducted in the qualitative study were also used to identify issues of importance to patients in regard to access to dermatology services and realistic levels for these attributes, in order to inform the design of a questionnaire. Four attributes of time waited, expertise, convenience and individualised care were included in a questionnaire which asked respondents to choose between best and worst scenarios for care. Individuals were sent questionnaires by post. People were randomly sent long or short versions of the questionnaire to answer a methodological question about the impact of questionnaire design on response rates. Of 456 suitable patients, 240 agreed to participate. The response rate to the short version (103/121; 85%) was not markedly greater than to the long version (99/119; 83%). The most important attributes to patients appeared to be the thoroughness of the consultation and the expertise of the doctor, with convenience and waiting times being less important. Discussion and conclusions The PCDS appeared to provide care which was more accessible and preferred by patients, with no evidence of a difference in clinical outcomes. These benefits were obtained at considerably greater cost. Although patients referred to the PCDS had much shorter waiting times than those seen at the hospital outpatient clinic, there was no overall beneficial impact on waiting times at the outpatient clinic. NCCSDO
7 The most important benefit to patients from establishing the PCDS appears to be in terms of accessibility. The location of a GPSI service is therefore crucial in order to maximise accessibility and convenience for as many people as possible. A notable finding from the qualitative research is that accessibility is a complex issue which is not simply based on geographical proximity. The discrete-choice modelling study also showed that improvements in access such as waiting times and convenience were less important to patients than the thoroughness of the consultation and the expertise of the doctor. The benefits identified for the PCDS need to be compared with other ways of increasing service capacity, for example by providing extra resources to support existing hospital services, by managing demand differently within hospitals, or by employing different models of skillmix in primary-care-based services. NCCSDO
8 Disclaimer This report presents independent research commissioned by the National Institute for Health Research (NIHR). The views and opinions expressed therein are those of the authors and do not necessarily reflect those of the NHS, the NIHR, the SDO programme or the Department of Health Addendum This document was published by the National Coordinating Centre for the Service Delivery and Organisation (NCCSDO) research programme, managed by the London School of Hygiene and Tropical Medicine. The management of the Service Delivery and Organisation (SDO) programme has now transferred to the National Institute for Health Research Evaluations, Trials and Studies Coordinating Centre (NETSCC) based at the University of Southampton. Prior to April 2009, NETSCC had no involvement in the commissioning or production of this document and therefore we may not be able to comment on the background or technical detail of this document. Should you have any queries please contact
BriefingPaper. Towards faster treatment: reducing attendance and waits at emergency departments ACCESS TO HEALTH CARE OCTOBER 2005
 ACCESS TO HEALTH CARE OCTOBER 2005 BriefingPaper Towards faster treatment: reducing attendance and waits at emergency departments Key messages based on a literature review which investigated the organisational
ACCESS TO HEALTH CARE OCTOBER 2005 BriefingPaper Towards faster treatment: reducing attendance and waits at emergency departments Key messages based on a literature review which investigated the organisational
BriefingPaper. The access/relationship trade off: how important is continuity of primary care to patients and their carers?
 CONTINUITY OF CARE SEPTEMBER 2006 BriefingPaper The access/relationship trade off: how important is continuity of primary care to patients and their carers? Key messages Patients want both quick access
CONTINUITY OF CARE SEPTEMBER 2006 BriefingPaper The access/relationship trade off: how important is continuity of primary care to patients and their carers? Key messages Patients want both quick access
PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING
 Introduction PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING Following publication of its new national health research strategy Best Research for Best Health (DH 2006a), the Department
Introduction PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING Following publication of its new national health research strategy Best Research for Best Health (DH 2006a), the Department
Map 1 Statutory specialist services and organisations in England
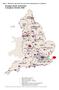 Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
PATIENT INFORMATION SHEET
 PATIENT INFORMATION SHEET Surgical and large bore pleural procedures in Malignant pleural Mesothelioma And Radiotherapy Trial (SMART trial) Stoke Mandeville Hospital Mandeville Road Aylesbury Buckinghamshire
PATIENT INFORMATION SHEET Surgical and large bore pleural procedures in Malignant pleural Mesothelioma And Radiotherapy Trial (SMART trial) Stoke Mandeville Hospital Mandeville Road Aylesbury Buckinghamshire
Improving children s health can nurses, midwives and health visitors make a difference? Key messages
 NURSING AND MIDWIFERY MARCH 2007 ResearchSummary Improving children s health can nurses, midwives and health visitors make a difference? Children s health services in the UK are improving all the time,
NURSING AND MIDWIFERY MARCH 2007 ResearchSummary Improving children s health can nurses, midwives and health visitors make a difference? Children s health services in the UK are improving all the time,
First Look Summary - Patient level information and costing systems (PLICS): Current practice and future potential for the NHS health economy
 First Look Summary - Patient level information and costing systems (PLICS): Current practice and future potential for the NHS health economy Sue Llewellyn*, Professor of Accountability and Management Control,
First Look Summary - Patient level information and costing systems (PLICS): Current practice and future potential for the NHS health economy Sue Llewellyn*, Professor of Accountability and Management Control,
Department of Health/ Royal College of General Practitioners. Implementing a scheme for General Practitioners with Special Interests
 Department of Health/ Royal College of General Practitioners Implementing a scheme for General Practitioners with Special Interests April 2002 Foreword Improved access and consistently high quality services
Department of Health/ Royal College of General Practitioners Implementing a scheme for General Practitioners with Special Interests April 2002 Foreword Improved access and consistently high quality services
Improving Emergency Care in England
 Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Appointment Non-Attendance (Did Not Attend) Procedure
 () Procedure 1. Purpose This Procedure outlines the procedural requirements to be observed by all West Coast District Health Board (WCDHB) staff (excluding Mental Health Service) to ensure all patient
() Procedure 1. Purpose This Procedure outlines the procedural requirements to be observed by all West Coast District Health Board (WCDHB) staff (excluding Mental Health Service) to ensure all patient
Maths Mastery in Primary Schools
 Maths Mastery in Primary Schools Institute of Education, University of London John Jerrim Evaluation Summary Age range Year 7 Number of pupils c. 10,000 Number of schools 50 Design Primary Outcome Randomised
Maths Mastery in Primary Schools Institute of Education, University of London John Jerrim Evaluation Summary Age range Year 7 Number of pupils c. 10,000 Number of schools 50 Design Primary Outcome Randomised
A secondary analysis of primary care survey data to explore differences in response by ethnicity.
 A secondary analysis of primary care survey data to explore differences in response by ethnicity. A report commissioned by the National Association for Patient Participation Autumn 2006 1.1 Introduction
A secondary analysis of primary care survey data to explore differences in response by ethnicity. A report commissioned by the National Association for Patient Participation Autumn 2006 1.1 Introduction
Delivering Appropriate Emergency Care Services - Protocol Development and Design
 Delivering Appropriate Emergency Care Services - Protocol Development and Design Sherrill Evans, Karen Evans, Peter Huxley, Helen Snooks, Ian Russell et al Mental Health Research Team, College of Human
Delivering Appropriate Emergency Care Services - Protocol Development and Design Sherrill Evans, Karen Evans, Peter Huxley, Helen Snooks, Ian Russell et al Mental Health Research Team, College of Human
Benefits Management: Realising Benefits from your projects. Professor Liz Daniel Associate Dean & Professor in Information Management
 Management: Realising from your projects Professor Liz Daniel Associate Dean & Professor in Information Management BENEFITS MANAGEMENT The process of organising and managing such that the potential benefits
Management: Realising from your projects Professor Liz Daniel Associate Dean & Professor in Information Management BENEFITS MANAGEMENT The process of organising and managing such that the potential benefits
Healthwatch North Somerset. Public Board of Directors Meeting. Local 111 Service (Care UK) Talk. James Head Deputy Clinical Lead
 Healthwatch North Somerset Public Board of Directors Meeting Local 111 Service (Care UK) Talk James Head Deputy Clinical Lead Caroline Pike - Business Relationship Manager Tuesday 14 th April 2015 Nailsea
Healthwatch North Somerset Public Board of Directors Meeting Local 111 Service (Care UK) Talk James Head Deputy Clinical Lead Caroline Pike - Business Relationship Manager Tuesday 14 th April 2015 Nailsea
Outpatient Survey 2011
 THE ROYAL BOURNEMOUTH AND CHRISTCHURCH HOSPITALS NHS FOUNDATION TRUST FINAL REPORT NOVEMBER 0 Copyright 0 Picker Institute Europe. All rights reserved. Trust ID: RDZ UKOUT0/09 Contacting Picker Institute
THE ROYAL BOURNEMOUTH AND CHRISTCHURCH HOSPITALS NHS FOUNDATION TRUST FINAL REPORT NOVEMBER 0 Copyright 0 Picker Institute Europe. All rights reserved. Trust ID: RDZ UKOUT0/09 Contacting Picker Institute
GP-led services for alcohol misuse: the Fresh Start Clinic
 London Journal of Primary Care 2011;4:11 15 # 2011 Royal College of General Practitioners GP Commissioning GP-led services for alcohol misuse: the Fresh Start Clinic Johannes Coetzee GP Principle, Bridge
London Journal of Primary Care 2011;4:11 15 # 2011 Royal College of General Practitioners GP Commissioning GP-led services for alcohol misuse: the Fresh Start Clinic Johannes Coetzee GP Principle, Bridge
Hip replacements: Getting it right first time
 Report by the Comptroller and Auditor General NHS Executive Hip replacements: Getting it right first time Ordered by the House of Commons to be printed 17 April 2000 LONDON: The Stationery Office 0.00
Report by the Comptroller and Auditor General NHS Executive Hip replacements: Getting it right first time Ordered by the House of Commons to be printed 17 April 2000 LONDON: The Stationery Office 0.00
Specialty Selection Test (SST) Pilot INFORMATION PACK
 Specialty Selection Test (SST) Pilot INFORMATION PACK Page 1 of 18 Contents Section 1: Introduction... 2 Section 2: One-page overview... 2 Section 3: FAQs for Applicants... 3 Section 2: FAQs for LETBs/Deaneries/Specialties...
Specialty Selection Test (SST) Pilot INFORMATION PACK Page 1 of 18 Contents Section 1: Introduction... 2 Section 2: One-page overview... 2 Section 3: FAQs for Applicants... 3 Section 2: FAQs for LETBs/Deaneries/Specialties...
Discharge to Assess: South Warwickshire NHS Foundation Trust
 Discharge to Assess: South Warwickshire NHS Foundation Trust The Discharge to Assess (D2A) service enables patients to be discharged earlier from acute inpatient wards by co-ordinating care in alternative
Discharge to Assess: South Warwickshire NHS Foundation Trust The Discharge to Assess (D2A) service enables patients to be discharged earlier from acute inpatient wards by co-ordinating care in alternative
Socio-economic benefits of interoperable electronic health record systems in Europe the evidence -
 Socio-economic benefits of interoperable electronic health record systems in Europe the evidence - Karl A. Stroetmann FRSM PhD MBA with Alexander Dobrev, Tom Jones, Yvonne Vatter empirica Communication
Socio-economic benefits of interoperable electronic health record systems in Europe the evidence - Karl A. Stroetmann FRSM PhD MBA with Alexander Dobrev, Tom Jones, Yvonne Vatter empirica Communication
Evaluating the ENAT : reconciling findings from a mixed methods study
 School of Healthcare FACULTY OF MEDICINE AND HEALTH Evaluating the ENAT : reconciling findings from a mixed methods study Professor Claire A Hale School of Healthcare University of Leeds On behalf of the
School of Healthcare FACULTY OF MEDICINE AND HEALTH Evaluating the ENAT : reconciling findings from a mixed methods study Professor Claire A Hale School of Healthcare University of Leeds On behalf of the
Managing the boundaries of NHS and privately funded healthcare Policy on the separation of private and NHS treatments
 South Central Priorities Committees (Oxfordshire PCT) Policy Statement 67a: Managing the boundaries of NHS and privately-funded healthcare Clinical Executive decision: September 2009 Date of Issue: April
South Central Priorities Committees (Oxfordshire PCT) Policy Statement 67a: Managing the boundaries of NHS and privately-funded healthcare Clinical Executive decision: September 2009 Date of Issue: April
Cervical Screening Programme
 Cervical Screening Programme England 2010-11 1 The NHS Information Centre is England s central, authoritative source of health and social care information. Acting as a hub for high quality, national, comparative
Cervical Screening Programme England 2010-11 1 The NHS Information Centre is England s central, authoritative source of health and social care information. Acting as a hub for high quality, national, comparative
BRITISH DERMATOLOGICAL NURSING GROUP
 Nurse Led systemic monitoring clinics guidance on setting up this service Introduction Nurse led systemic monitoring clinics are an innovative approach to improving care delivery and maintaining both a
Nurse Led systemic monitoring clinics guidance on setting up this service Introduction Nurse led systemic monitoring clinics are an innovative approach to improving care delivery and maintaining both a
Why Service Users Say They Value Specialist Palliative Care Social Work:
 Why Service Users Say They Value Specialist Palliative Care Social Work: and how the medicalisation of palliative care gets in the way Suzy Croft and Peter Beresford Palliative Care Palliative Care is
Why Service Users Say They Value Specialist Palliative Care Social Work: and how the medicalisation of palliative care gets in the way Suzy Croft and Peter Beresford Palliative Care Palliative Care is
Immune Cell Studies in Type 1 Diabetes (ISTID) INFORMATION SHEET FOR ADULTS WITH NEWLY- DIAGNOSED DIABETES. Sponsored by Cardiff University
 Immune Cell Studies in Type 1 Diabetes (ISTID) INFORMATION SHEET FOR ADULTS WITH NEWLY- DIAGNOSED DIABETES Sponsored by Cardiff University Chief Investigator Wales: Professor Colin Dayan Address: Centre
Immune Cell Studies in Type 1 Diabetes (ISTID) INFORMATION SHEET FOR ADULTS WITH NEWLY- DIAGNOSED DIABETES Sponsored by Cardiff University Chief Investigator Wales: Professor Colin Dayan Address: Centre
To achieve this aim the specific objectives of this PhD will include:
 PhD Project Proposal - Living well with dementia: a PhD programme to develop a complex intervention that integrates healthcare for people with dementia 1. Background to the study There are 800,000 people
PhD Project Proposal - Living well with dementia: a PhD programme to develop a complex intervention that integrates healthcare for people with dementia 1. Background to the study There are 800,000 people
The RADICALS trial Radiotherapy Timing Randomisation (RADICALS-RT) Clinical trial of treatment after surgery for prostate cancer
 Stoke Mandeville Hospital Mandeville Road Aylesbury Buckinghamshire HP21 8AL Tel: 01296 315 908 www.buckshealthcare.nhs.uk The RADICALS trial Radiotherapy Timing Randomisation (RADICALS-RT) Clinical trial
Stoke Mandeville Hospital Mandeville Road Aylesbury Buckinghamshire HP21 8AL Tel: 01296 315 908 www.buckshealthcare.nhs.uk The RADICALS trial Radiotherapy Timing Randomisation (RADICALS-RT) Clinical trial
The Family Nurse Partnership Programme
 The Family Nurse Partnership Programme Information leaflet DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development Finance Planning
The Family Nurse Partnership Programme Information leaflet DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development Finance Planning
DMRI Drug Misuse Research Initiative
 DMRI Drug Misuse Research Initiative Executive Summary Dexamphetamine Substitution as a Treatment of Amphetamine Dependence: a Two-Centre Randomised Controlled Trial Final Report submitted to the Department
DMRI Drug Misuse Research Initiative Executive Summary Dexamphetamine Substitution as a Treatment of Amphetamine Dependence: a Two-Centre Randomised Controlled Trial Final Report submitted to the Department
Rehabilitation services for long term neurological conditions: what works and what is available?
 EVALUATING MODELS OF SERVICE DELIVERY AUGUST 2008 ResearchSummary Rehabilitation services for long term neurological conditions: what works and what is available? Over a million people are treated for
EVALUATING MODELS OF SERVICE DELIVERY AUGUST 2008 ResearchSummary Rehabilitation services for long term neurological conditions: what works and what is available? Over a million people are treated for
Time to Act Urgent Care and A&E: the patient perspective
 Time to Act Urgent Care and A&E: the patient perspective May 2015 Executive Summary The NHS aims to put patients at the centre of everything that it does. Indeed, the NHS Constitution provides rights to
Time to Act Urgent Care and A&E: the patient perspective May 2015 Executive Summary The NHS aims to put patients at the centre of everything that it does. Indeed, the NHS Constitution provides rights to
Big Chat 4. Strategy into action. NHS Southport and Formby CCG
 Big Chat 4 Strategy into action NHS Southport and Formby CCG Royal Clifton Hotel, Southport, 19 November 2014 Contents What is the Big Chat? 3 About Big Chat 4 4 How the event worked 4 Presentations 5
Big Chat 4 Strategy into action NHS Southport and Formby CCG Royal Clifton Hotel, Southport, 19 November 2014 Contents What is the Big Chat? 3 About Big Chat 4 4 How the event worked 4 Presentations 5
Attributing the costs of health and social care Research & Development (AcoRD)
 Frequently Asked Questions Annex B Q1. Why have you revised the guidance on attributing Research Costs, Support Costs and Treatments Cost in the NHS? A. The definitions of Research Costs, NHS Support Costs
Frequently Asked Questions Annex B Q1. Why have you revised the guidance on attributing Research Costs, Support Costs and Treatments Cost in the NHS? A. The definitions of Research Costs, NHS Support Costs
NIHR Research Design Service London Dr Peter Lovell Deputy Director
 NIHR Research Design Service London Dr Peter Lovell Deputy Director Research Design Service (RDS) A national network of support services; Supporting those who are putting together REGIONAL RDS North East
NIHR Research Design Service London Dr Peter Lovell Deputy Director Research Design Service (RDS) A national network of support services; Supporting those who are putting together REGIONAL RDS North East
Do nurse practitioners working in primary care provide equivalent care to doctors?
 August 2008 SUPPORT Summary of a systematic review Do nurse practitioners working in primary care provide equivalent care to doctors? Nurse practitioners are nurses who have undergone further training,
August 2008 SUPPORT Summary of a systematic review Do nurse practitioners working in primary care provide equivalent care to doctors? Nurse practitioners are nurses who have undergone further training,
!!!!!!!!!!!! Liaison Psychiatry Services - Guidance
 Liaison Psychiatry Services - Guidance 1st edition, February 2014 Title: Edition: 1st edition Date: February 2014 URL: Liaison Psychiatry Services - Guidance http://mentalhealthpartnerships.com/resource/liaison-psychiatry-servicesguidance/
Liaison Psychiatry Services - Guidance 1st edition, February 2014 Title: Edition: 1st edition Date: February 2014 URL: Liaison Psychiatry Services - Guidance http://mentalhealthpartnerships.com/resource/liaison-psychiatry-servicesguidance/
Decision Support Tool for NHS Continuing Healthcare User Notes
 Decision Support Tool for NHS Continuing Healthcare User Notes July 2009 1 Decision Support Tool for NHS Continuing Healthcare We have developed the Decision Support Tool (DST) to support practitioners
Decision Support Tool for NHS Continuing Healthcare User Notes July 2009 1 Decision Support Tool for NHS Continuing Healthcare We have developed the Decision Support Tool (DST) to support practitioners
Second English National Memory Clinics Audit Report
 Second English National Memory Clinics Audit Report December 2015 Funded by: Department of Health Conducted by: Royal College of Psychiatrists Authors: Sophie Hodge & Emma Hailey Correspondence: Sophie
Second English National Memory Clinics Audit Report December 2015 Funded by: Department of Health Conducted by: Royal College of Psychiatrists Authors: Sophie Hodge & Emma Hailey Correspondence: Sophie
GP Patient Survey Your doctor, your experience, your say
 GP Patient Survey Your doctor, your experience, your say Guidance 2007/08 for strategic health authorities, primary care trusts and GP practices Introduction 1. This document provides guidance on this
GP Patient Survey Your doctor, your experience, your say Guidance 2007/08 for strategic health authorities, primary care trusts and GP practices Introduction 1. This document provides guidance on this
Information Governance. A Clinician s Guide to Record Standards Part 1: Why standardise the structure and content of medical records?
 Information Governance A Clinician s Guide to Record Standards Part 1: Why standardise the structure and content of medical records? Contents Page 3 A guide for clinicians Pages 4 and 5 Why have standards
Information Governance A Clinician s Guide to Record Standards Part 1: Why standardise the structure and content of medical records? Contents Page 3 A guide for clinicians Pages 4 and 5 Why have standards
Homelessness and Health Information Sheet
 Homelessness and Health Information Sheet Number 3: Dental Services Homelessness and Health Homeless people can face major barriers in accessing dental services while their life circumstances can often
Homelessness and Health Information Sheet Number 3: Dental Services Homelessness and Health Homeless people can face major barriers in accessing dental services while their life circumstances can often
JSNA Factsheet Template Tower Hamlets Joint Strategic Needs Assessment 2010 2011
 JSNA Factsheet Template Tower Hamlets Joint Strategic Needs Assessment 2010 2011. Executive Summary This fact sheet considers breast cancer, with a particular emphasis on breast screening and raising awareness
JSNA Factsheet Template Tower Hamlets Joint Strategic Needs Assessment 2010 2011. Executive Summary This fact sheet considers breast cancer, with a particular emphasis on breast screening and raising awareness
Xerox Custom Healthcare Solution
 Xerox Custom Healthcare Solution Xerox HR Services has undertaken a comprehensive review of the employee benefits market, assessing all of the major providers, in order to develop our Xerox Custom Healthcare
Xerox Custom Healthcare Solution Xerox HR Services has undertaken a comprehensive review of the employee benefits market, assessing all of the major providers, in order to develop our Xerox Custom Healthcare
Improving data quality in the NHS Executive summary
 Improving data quality in the NHS Executive summary Health 2010 The Audit Commission is an independent watchdog, driving economy, efficiency and effectiveness in local public services to deliver better
Improving data quality in the NHS Executive summary Health 2010 The Audit Commission is an independent watchdog, driving economy, efficiency and effectiveness in local public services to deliver better
Service delivery interventions
 Service delivery interventions S A S H A S H E P P E R D D E P A R T M E N T O F P U B L I C H E A L T H, U N I V E R S I T Y O F O X F O R D CO- C O O R D I N A T I N G E D I T O R C O C H R A N E E P
Service delivery interventions S A S H A S H E P P E R D D E P A R T M E N T O F P U B L I C H E A L T H, U N I V E R S I T Y O F O X F O R D CO- C O O R D I N A T I N G E D I T O R C O C H R A N E E P
State of medical education and practice in the UK: 2013. Name: Dr. Judith Hulf Senior Medical Adviser to the GMC
 State of medical education and practice in the UK: 2013 Name: Dr. Judith Hulf Senior Medical Adviser to the GMC What is the General Medical Council - GMC? An independent public body A charity The independent
State of medical education and practice in the UK: 2013 Name: Dr. Judith Hulf Senior Medical Adviser to the GMC What is the General Medical Council - GMC? An independent public body A charity The independent
Intensive Positive Behaviour Support Service (ipbs)
 Community Children s Healthcare Partnership Intensive Positive Behaviour Support Service (ipbs) In partnership with Exceptional healthcare, personally delivered What is the Intensive Positive Behaviour
Community Children s Healthcare Partnership Intensive Positive Behaviour Support Service (ipbs) In partnership with Exceptional healthcare, personally delivered What is the Intensive Positive Behaviour
Mesothelioma Priority Setting Partnership. PROTOCOL November 2013
 Mesothelioma Priority Setting Partnership PROTOCOL November 2013 Purpose The purpose of this protocol is to set out the aims, objectives and commitments of the Mesothelioma Priority Setting Partnership
Mesothelioma Priority Setting Partnership PROTOCOL November 2013 Purpose The purpose of this protocol is to set out the aims, objectives and commitments of the Mesothelioma Priority Setting Partnership
2014 National NHS staff survey. Results from London Ambulance Service NHS Trust
 2014 National NHS staff survey Results from London Ambulance Service NHS Trust Table of Contents 1: Introduction to this report 3 2: Overall indicator of staff engagement for London Ambulance Service NHS
2014 National NHS staff survey Results from London Ambulance Service NHS Trust Table of Contents 1: Introduction to this report 3 2: Overall indicator of staff engagement for London Ambulance Service NHS
GP Patient Survey Your Doctor, Your Experience, Your Say
 To: GP Practices Chief Executives of Primary Care Trusts Dear Colleague GP Patient Survey Your Doctor, Your Experience, Your Say This letter confirms arrangements for delivery of the 2008 GP Patient Survey.
To: GP Practices Chief Executives of Primary Care Trusts Dear Colleague GP Patient Survey Your Doctor, Your Experience, Your Say This letter confirms arrangements for delivery of the 2008 GP Patient Survey.
GP-led health centres. Background Briefing
 GP-led health centres Background Briefing Equitable Access to Primary Medical Care Lord Darzi is an eminent surgeon who is currently serving as a junior health minister. In June 2007 the Secretary of State
GP-led health centres Background Briefing Equitable Access to Primary Medical Care Lord Darzi is an eminent surgeon who is currently serving as a junior health minister. In June 2007 the Secretary of State
Rehabilitation Network Strategy 2014 2017. Final Version 30 th June 2014
 Rehabilitation Network Strategy 2014 2017 Final Version 30 th June 2014 Contents Foreword 3 Introduction Our Strategy 4 Overview of the Cheshire and Merseyside Rehabilitation Network 6 Analysis of our
Rehabilitation Network Strategy 2014 2017 Final Version 30 th June 2014 Contents Foreword 3 Introduction Our Strategy 4 Overview of the Cheshire and Merseyside Rehabilitation Network 6 Analysis of our
Private treatment. Which treatments are available privately? Can I have private and NHS treatment together?
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Private treatment Because the NHS only offers limited access to some therapies after stroke, you might choose to explore the option of private treatment.
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Private treatment Because the NHS only offers limited access to some therapies after stroke, you might choose to explore the option of private treatment.
Stour Access System: a new way to manage GP appointments Better for GPs, better for patients, better all-round
 12:56 Page 1 Stour Access System: a new way to manage GP appointments Better for GPs, better for patients, better all-round Take control of your time, improve the flow of patients, improve access and whats
12:56 Page 1 Stour Access System: a new way to manage GP appointments Better for GPs, better for patients, better all-round Take control of your time, improve the flow of patients, improve access and whats
HSF Assist Providing support and advice when it is most needed
 HSF Assist Providing support and advice when it is most needed Welcome to your new HSF Assist service - part of your health cash plan cover. HSF Assist provides you with unlimited access to a variety of
HSF Assist Providing support and advice when it is most needed Welcome to your new HSF Assist service - part of your health cash plan cover. HSF Assist provides you with unlimited access to a variety of
Quality Assurance of Medical Appraisers
 Quality Assurance of Medical Appraisers Recruitment, training, support and review of medical appraisers in England www.revalidationsupport.nhs.uk Contents 1. Introduction 3 2. Purpose and overview 4 3.
Quality Assurance of Medical Appraisers Recruitment, training, support and review of medical appraisers in England www.revalidationsupport.nhs.uk Contents 1. Introduction 3 2. Purpose and overview 4 3.
COST OF SKIN CANCER IN ENGLAND MORRIS, S., COX, B., AND BOSANQUET, N.
 ISSN 1744-6783 COST OF SKIN CANCER IN ENGLAND MORRIS, S., COX, B., AND BOSANQUET, N. Tanaka Business School Discussion Papers: TBS/DP05/39 London: Tanaka Business School, 2005 1 Cost of skin cancer in
ISSN 1744-6783 COST OF SKIN CANCER IN ENGLAND MORRIS, S., COX, B., AND BOSANQUET, N. Tanaka Business School Discussion Papers: TBS/DP05/39 London: Tanaka Business School, 2005 1 Cost of skin cancer in
Improving Urgent and Emergency care through better use of pharmacists. Introduction. Recommendations. Shaping pharmacy for the future
 Improving Urgent and Emergency care through better use of pharmacists The Royal Pharmaceutical Society (RPS) believes that pharmacists are an underutilised resource in the delivery of better urgent and
Improving Urgent and Emergency care through better use of pharmacists The Royal Pharmaceutical Society (RPS) believes that pharmacists are an underutilised resource in the delivery of better urgent and
Case study: Pennine MSK Partnership
 Case study: Pennine MSK Partnership Dr Alan Nye is a GP in Oldham, GPSI in Rheumatology, Director of Pennine MSK Partnership, Associate Medical Director of NHS Direct and Associate Medical Director of
Case study: Pennine MSK Partnership Dr Alan Nye is a GP in Oldham, GPSI in Rheumatology, Director of Pennine MSK Partnership, Associate Medical Director of NHS Direct and Associate Medical Director of
PATIENT ACCESS POLICY
 PATIENT ACCESS POLICY Completed Review Date: June 2015 Date for Review June 2016 1 NHS LANARKSHIRE PATIENT ACCESS POLICY 1. BACKGROUND NHS Lanarkshire is required by Scottish Government to deliver a consistent,
PATIENT ACCESS POLICY Completed Review Date: June 2015 Date for Review June 2016 1 NHS LANARKSHIRE PATIENT ACCESS POLICY 1. BACKGROUND NHS Lanarkshire is required by Scottish Government to deliver a consistent,
EASTER ROSS ORTHOPAEDIC TRIAGE PILOT
 EASTER ROSS ORTHOPAEDIC TRIAGE PILOT SUE KING EXTENDED SCOPE PRACTITIONER PHYSIOTHERAPIST COUNTY COMMUNITY HOSPITAL INVERGORDON AUGUST 2009 INTRODUCTION A 12 month pilot project to test out a model of
EASTER ROSS ORTHOPAEDIC TRIAGE PILOT SUE KING EXTENDED SCOPE PRACTITIONER PHYSIOTHERAPIST COUNTY COMMUNITY HOSPITAL INVERGORDON AUGUST 2009 INTRODUCTION A 12 month pilot project to test out a model of
Family Focused Therapy for Bipolar Disorder (Clinical Case Series) Participant Information Sheet
 Family Focused Therapy for Bipolar Disorder (Clinical Case Series) Participant Information Sheet Study Title: Family Focused Therapy for Bipolar Disorder: A Clinical Case Series) We would like to invite
Family Focused Therapy for Bipolar Disorder (Clinical Case Series) Participant Information Sheet Study Title: Family Focused Therapy for Bipolar Disorder: A Clinical Case Series) We would like to invite
NATIONAL STROKE NURSING FORUM NURSE STAFFING OF STROKE SERVICES POSITION STATEMENT FOR NATIONAL STROKE STRATEGY
 NATIONAL STROKE NURSING FORUM NURSE STAFFING OF STROKE SERVICES POSITION STATEMENT FOR NATIONAL STROKE STRATEGY Preamble The National Stroke Nursing Forum is pleased to be able to contribute to the development
NATIONAL STROKE NURSING FORUM NURSE STAFFING OF STROKE SERVICES POSITION STATEMENT FOR NATIONAL STROKE STRATEGY Preamble The National Stroke Nursing Forum is pleased to be able to contribute to the development
Patient Access Policy
 Patient Access Policy NON-CLINICAL POLICY ACE 522 Version Number: 2 Policy Owner: Lead Director: Assistant Director of Operations Director of Operations Date Approved: Approved By: Management Executive
Patient Access Policy NON-CLINICAL POLICY ACE 522 Version Number: 2 Policy Owner: Lead Director: Assistant Director of Operations Director of Operations Date Approved: Approved By: Management Executive
Questions often asked by patients and answers from the Randolph Surgery
 Questions often asked by patients and answers from the Randolph Surgery 1. Why does the Randolph Surgery insist that everyone over 40 (or anyone who requires prescribed medication under 40) has a comprehensive
Questions often asked by patients and answers from the Randolph Surgery 1. Why does the Randolph Surgery insist that everyone over 40 (or anyone who requires prescribed medication under 40) has a comprehensive
PATIENT ONLINE SUPPORT AND RESOURCES. Contact the Patient Online team:[email protected]
 PATIENT ONLINE SUPPORT AND RESOURCES Contact the Patient Online team:[email protected] #Patientonline WHO IS THIS GUIDE FOR? This guide is intended for GPs, general practice staff, clinical
PATIENT ONLINE SUPPORT AND RESOURCES Contact the Patient Online team:[email protected] #Patientonline WHO IS THIS GUIDE FOR? This guide is intended for GPs, general practice staff, clinical
Sensitivity of Hospital Clinic queues to patient non-attendance. Neville J. Ford, Paul D. Crofts, and Richard H. T. Edwards
 ISSN 1360-1725 UMIST Sensitivity of Hospital Clinic queues to patient non-attendance Neville J. Ford, Paul D. Crofts, and Richard H. T. Edwards Numerical Analysis Report No. 383 A report in association
ISSN 1360-1725 UMIST Sensitivity of Hospital Clinic queues to patient non-attendance Neville J. Ford, Paul D. Crofts, and Richard H. T. Edwards Numerical Analysis Report No. 383 A report in association
Patient Access Policy
 Patient Access Policy SECTION 1 - INTRODUCTION AND OVERVIEW 1.1. Introduction The principles and definitions of the 18 week target count the referral to treatment (RTT) waiting times in totality. Spire
Patient Access Policy SECTION 1 - INTRODUCTION AND OVERVIEW 1.1. Introduction The principles and definitions of the 18 week target count the referral to treatment (RTT) waiting times in totality. Spire
PATIENT ACCESS POLICY
 PATIENT ACCESS POLICY Document Type Policy Document Number Version Number 1.0 Approved by NHS Borders Board on 18 October 2012 Issue date Nov 2012 Review date Nov 2013 Distribution Prepared by Developed
PATIENT ACCESS POLICY Document Type Policy Document Number Version Number 1.0 Approved by NHS Borders Board on 18 October 2012 Issue date Nov 2012 Review date Nov 2013 Distribution Prepared by Developed
Strengthening And stretching for Rheumatoid Arthritis of the Hand (SARAH). A randomised controlled trial and economic evaluation
 Strengthening And stretching for Rheumatoid Arthritis of the Hand (SARAH). A randomised controlled trial and economic evaluation Mark A Williams, 1* Esther M Williamson, 1 Peter J Heine, 1 Vivien Nichols,
Strengthening And stretching for Rheumatoid Arthritis of the Hand (SARAH). A randomised controlled trial and economic evaluation Mark A Williams, 1* Esther M Williamson, 1 Peter J Heine, 1 Vivien Nichols,
Improving access to insulin pump therapy: The role of the Insulin Pump Network
 Article Improving access to insulin pump therapy: The role of the Insulin Pump Network Peter Hammond Citation: Hammond, P (2013) Improving access to insulin pump therapy: The role of the Insulin Pump Network.
Article Improving access to insulin pump therapy: The role of the Insulin Pump Network Peter Hammond Citation: Hammond, P (2013) Improving access to insulin pump therapy: The role of the Insulin Pump Network.
Pharmacists improving care in care homes
 The Royal Pharmaceutical Society believes that better utilisation of pharmacists skills in care homes will bring significant benefits to care home residents, care homes providers and the NHS. Introduction
The Royal Pharmaceutical Society believes that better utilisation of pharmacists skills in care homes will bring significant benefits to care home residents, care homes providers and the NHS. Introduction
NHS inpatient elective admission events and outpatient referrals and attendances
 NHS inpatient elective admission events and outpatient referrals and attendances Quarter Ending December 2013 Commentary o Key Points o Time Series Graphs Statistical Notes o National Statistics o Quarterly
NHS inpatient elective admission events and outpatient referrals and attendances Quarter Ending December 2013 Commentary o Key Points o Time Series Graphs Statistical Notes o National Statistics o Quarterly
