Evaluation of Claims, Medical Records, and Self-report for Measuring Fecal Occult Blood Testing among Medicare Enrollees in Fee for Service
|
|
|
- Jerome Fields
- 8 years ago
- Views:
Transcription
1 799 CEBP Focus: Validating Colorectal Cancer Screening Behaviors Evaluation of Claims, Medical Records, and Self-report for Measuring Fecal Occult Blood Testing among Medicare Enrollees in Fee for Service Anna P. Schenck, 1 Carrie N. Klabunde, 2 Joan L. Warren, 2 Sharon Peacock, 1 William W. Davis, 3 Sarah T. Hawley, 4 Michael Pignone, 5 and David F. Ransohoff 6 1 The Carolinas Center for Medical Excellence, Cary, North Carolina; 2 Health Services and Economics Branch, Applied Research Program, Division of Cancer Control and Population Sciences, National Cancer Institute, Bethesda, Maryland; 3 Statistical Research and Applications Branch, Surveillance Research Program, Division of Cancer Control and Population Sciences, National Cancer Institute, Rockville, Maryland; 4 Division of General Medicine, University of Michigan, Ann Arbor, Michigan; and 5 Department of Medicine and Cecil Sheps Center for Health Services Research and 6 Departments of Medicine and Epidemiology, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina Abstract Background: There is no agreement on the best data source for measuring colorectal cancer (CRC) screening. Medicare claims have been used to measure CRC testing but the validity of using claims to measure fecal occult blood tests (FOBT) has not been established. Methods: We compared ascertainment of FOBTamong three data sources: self-reports, Medicare claims, and medical records. Data were collected on FOBTuse during the study window (1/1/ /31/2002). Our study was conducted with North Carolina Medicare enrollees (N = 561) who had previously responded to a telephone survey on CRC tests. FOBTinformation was abstracted from respondents physician office medical records and compared with self-reported FOBTuse and Medicare claims for FOBT. Data sources were assessed for accuracy and completeness of FOBTreporting using sensitivity, specificity, positive predictive value, negative predictive value, and agreement. Results: Reporting of FOBTuse in the prior year in medical records and Medicare claims agreed 82% of the time [95% confidence interval, 79-85%]. FOBT1-year use rates from self-report agreed with test use found in medical records 70% of the time (95% CI, 66-74%). The lowest agreement was between self-reported 1-year FOBTuse and Medicare claims, which agreed 67% of the time (95% CI, 63-71%). Conclusions: No data source could be established as providing complete and valid information about FOBT use among Medicare enrollees, showing the difficulty of ascertaining test use rates for noninvasive, low-cost procedures conducted in multiple settings. Caution should be used when attempting to measure FOBT use with self-report, Medicare claims, or medical records. (Cancer Epidemiol Biomarkers Prev 2008; 17(4): ) Introduction Colorectal cancer (CRC) screening is widely recommended for persons ages 50 and older (1-3). Although colonoscopy has received more attention recently than other screening modalities, flexible sigmoidoscopy, barium enema, and annual fecal occult blood tests (FOBT) are recognized as equally effective in most screening guidelines. Despite the multiple options for CRC screening, CRC screening is underused (4). Since the Received 9/21/08; revised 12/11/07; accepted 12/28/07. Grant support: The analyses on which this publication is based were done under Contract No NC03 ( Utilization and Quality Control Peer Review Organization for the State of North Carolina ), sponsored by the Centers for Medicare & Medicaid Services and the National Cancer Institute under interagency agreement #Y1-PC Note: The content of this publication does not necessarily reflect the views or policies of Centers for Medicare & Medicaid Services, National Cancer Institute, or The Carolinas Center for Medical Excellence. The opinions expressed in this article are those of the authors. Requests for reprints: Anna P. Schenck, The Carolinas Center for Medical Excellence, 100 Regency Forest, Suite 200, Cary, NC Phone: ; Fax: aschenck@ncqio.sdps.org Copyright D 2008 American Association for Cancer Research. doi: / epi introduction of Medicare coverage for CRC screening tests, test use assessed by Medicare claims has remained virtually stable: f20% of Medicare enrollees receive a CRC test each year and just over half (52%) had any CRC test from 1998 to 2004 (5). To monitor progress toward public health screening goals, it is important to develop methods to evaluate population-based use of CRC screening in the United States. Measuring the level of CRC test use in the population is difficult for two primary reasons. First, the recommended time between tests for average-risk patients varies by test: 10 years between each colonoscopy, 5 years between each sigmoidoscopy or barium enema, and 1 year between each FOBT (1, 2). The optimal mix of how many persons should receive each test in any given year is unknown. Second, there is no uniform source of data to measure CRC test use and no agreement on the best data source to measure CRC test use. Complete ascertainment of CRC test use will vary by the type of procedure and data source. Studies often rely on self-report to assess CRC test use. However, prior studies have found poor agreement between rates for
2 800 Measuring FOBT Use by Medicare Enrollees FOBT based on self-reported test use and claims or medical records (6-10). An alternate source of data to assess CRC testing is Medicare claims. An earlier study on the measurement of colorectal endoscopy (e.g., sigmoidoscopy and colonoscopy) found Medicare claims to be an accurate source for measurement of endoscopy use (11). It is not clear whether FOBT is reported as completely in the Medicare claims as endoscopy. Several characteristics of FOBT distinguish it from endoscopy procedures, leading to the concern that Medicare claims may underrepresent FOBT testing in the Medicare population. Medicare reimbursement for FOBT is low, which may discourage physician billing for FOBT testing, and FOBT test kits are available for purchase and use by consumers without a physician visit. In this article, FOBT use was determined from three data sources: Medicare claims, self-report, and medical records. Although we evaluated all data sources, the primary focus of our analysis was on whether Medicare claims could completely and accurately capture FOBT use. This study was a collaborative effort among the Centers for Medicare & Medicaid Services, the National Cancer Institute, and The Carolinas Center for Medical Excellence, the Quality Improvement Organization for the Medicare program in North and South Carolina. Materials and Methods Details of the study cohort, data, and methods have been previously described (11). Briefly, the study population included African-American and White Medicare feefor-service enrollees between the ages of 50 and 80 years who resided in one of 10 urban counties in North Carolina and had responded to a telephone survey in 2002 on their prior CRC screening (n = 1,001). Primary care providers were identified for survey respondents, making them eligible for medical record abstraction (n = 877). Internal medicine, general practice, family practice, preventive medicine, gerontology, obstetrics/gynecology, nurse practitioners, and physician assistants were included in the definition of primary care providers. The identification of the primary care provider was a two-step process. Respondents were asked the name and address of their primary care provider on the telephone survey. If the respondent did not name a physician, or the physician named by the respondent could not be located, a primary care provider was identified using an algorithm developed by the Medicare Healthcare Quality Improvement Program (12). We examined 3 years of Medicare claims ( ) to identify a primary care provider for study participants identified by the unique physician identifier on the claim. The algorithm ranked physicians based on the number of visits during the 3-year window and selected the primary care provider with the most visits as the likely provider of routine care. If no primary care provider was identified through the survey or algorithm, the physician with the most office visits based on the algorithm, regardless of specialty, was identified as the physician for the medical record accession. A subset of the eligible respondents (n = 694) was targeted for medical record abstraction. This subset included all respondents with a claim or self-report of an endoscopy procedure in the past 2 years (n = 574) and a random sample of respondents without evidence of prior test (n = 120; ref. 11). We obtained medical records from 1998 to 2002 for 88% of the targeted respondents, yielding a study group of 609. Medical records were abstracted between June 2004 and May Analyses were limited to survey respondents with continuous enrollment in Medicare Part A and B and no health maintenance organization enrollment from entry into Medicare until death or the end of the study window (defined as January 1, 1998 to December 31, 2002), yielding a final study group of 561 Medicare enrollees. Data Sources. We merged data from three different sources (Medicare data, telephone survey, and physician office medical records) using a unique Medicare identifier to create a single patient level record for each study participant. Participants records included demographic information and details about their CRC test use. A brief description of each data source follows below. Additional details of the study methods can be found in our earlier report (11). Medicare Data. Medicare claims for study participants were obtained from all settings (inpatient, physician, and hospital outpatient claims) for a 5-year period (January 1, 1998 to December 31, 2002). Claims were analyzed to capture any billing for FOBT tests using both diagnostic and screening codes for FOBT [Current Procedural Terminology (CPT) codes and and Health Care Financing Agency Common Procedure Coding System code G0107; refs. 13, 14]. We obtained demographic and coverage information for study participants from the Medicare enrollment database. Telephone Survey. Questions on the 2002 survey were designed to distinguish the recommended method of FOBT, home test kits, from a FOBT undertaken in the physician s office through a digital rectal exam. Respondents were read the following description of FOBT: A FOBT or stool blood test is a test to check for colon or rectal cancer. It is done at home using a set of three cards. You smear a sample of your fecal matter or stool on a card from three separate bowel movements and return the cards to be tested for blood. After the test description was read, respondents were asked if they had ever completed a stool blood test at home and, if so, the timing of their most recent stool blood test using a home test kit. Respondents were also asked whether the test had been conducted as part of a checkup or because of a problem. The telephone survey also included questions on educational level, marital status, and names and addresses of primary care providers and physicians who conducted respondents most recent CRC tests, if any. A copy of the survey instrument is available from the corresponding author (A.P.S.). Medical Record. A comprehensive record abstraction tool captured CRC test use between the dates January 1, 1998 and December 31, 2002 from medical records. Nurse abstractors visited physicians offices across the state to abstract medical record information directly into an electronic abstraction tool contained on a laptop computer. The following information about the four most recent FOBT tests was abstracted from the medical record: date of test, the type of documentation found about the test (office visit notes, letter, lab result, or
3 801 CEBP Focus: Validating Colorectal Cancer Screening Behaviors documentation on a flow sheet), type of test (three cards sent to lab, digital rectal exam done in office; immunochemical FOBT or not specified), the reason for the test (screening, symptoms, surveillance, or not specified), and the results of the test (positive, negative, or not specified). In addition, the medical record abstraction also collected the date of the last visit and most recent well checkup, patient medical conditions, and information about the medical practice (type of practice, number of physicians in the practice, and whether the practice used electronic medical records). Definitions of FOBTUse. The recommended interval for CRC testing by FOBT is 1 year (1-3). The national goal for CRC screening by FOBT, as published in Healthy People 2010, sets a target of 50% of adults ages 50 years or older having a FOBT within the past 2 years (15). For this study, we measured the frequency of FOBT use in two ways. First, consistent with the recommended test use interval, we classified people as having had a FOBT if there was evidence they had it in the preceding 1 year. To allow for comparisons with the Healthy People 2010 target, and because analyses of self-reports have shown telescoping, where procedures are recalled to have occurred more recently than their actual date, we expanded our test use window to analyze FOBT use during the preceding 2 years. Both measures of FOBT use were calculated separately for each data source. We captured any FOBT mentioned in the medical records occurring during the study window. However, in the assessment of the data sources, FOBTs that were identified in the medical record as having been conducted by digital rectal exam were not included. Tests found in the medical record for which the abstractor was unable to tell the type of FOBT test were included, although we evaluated the effect of excluding those tests. As classification of the FOBT tests of undetermined type in the medical record made very little difference in our findings, the results we report include these tests in the definition of FOBTs found in the medical record. Analytic Approach. Analysis of data sources on FOBT testing included three different comparisons: claim with medical record, survey with medical record, and survey with claim. In comparisons using the medical record, the medical record was designated as the criterion standard. For the survey-with-claim comparison, the claim was designated as the criterion standard. Assessment of the completeness and accuracy of FOBT reporting was measured with five statistics: sensitivity, specificity, positive predictive value, negative predictive value, and agreement (see Table 3 for formulas; refs. 16, 17). We calculated each statistic twice (for 1-year use and for 2-year use). Ninety-five percent confidence intervals were calculated around the statistics using standard methods (17). Although the statistics are interrelated, each provides a slightly different measure of validity of the data sources. Using the claim-with-medical record comparisons as an example, sensitivity provides a measure of the extent to which claims for FOBT can completely capture the universe of people who had the test (in this case, measured by medical record). Specificity provides a measure of the extent to which claims for FOBT can be used to identify accurately persons who did not undergo the test. Positive predictive value indicates the proportion of people who actually had a FOBT, given that there is a claim. Negative predictive value indicates the probability that a person has not had a FOBT, given that there is not a claim. Agreement indicates the percentage of people for whom the claims and the medical record agree on FOBT use. Vernon et al. (18) have recommended the use of the report-to-records ratio to quantify the bias in cancer screening rates based on self-report. Report-to-records ratios greater than 1 indicate over-reporting and values less than 1 indicate underreporting. We calculated the report-to-records ratio for the two comparisons: selfreport compared with medical records and self-report compared with claims. The report-to-records ratio was calculated by dividing the number of person who reported having a FOBT by the number of persons who had a FOBT in the data source used as the gold standard (either the medical record or the claim). Results Records were abstracted from 269 physician offices. The majority of offices were single-specialty primary care providers (68%), 14% were multispecialty offices, 10% were gastroenterology offices, and 7% were other specialties. Although many FOBTs were identified in the medical records during the 5-year abstraction window (n = 953), documentation in the medical records of the type of FOBT was poor. Examining the most recent FOBT found in the medical records, 31% of study participants had a test with insufficient documentation to determine the type of FOBT (Table 1). One hundred seventy-six (31%) of the study group had a FOBT based on a digital rectal exam as their most recent FOBT, which is not recommended for CRC screening. Estimates of FOBT use in the previous 1- and 2-year windows varied by data source and by demographic characteristic of the study participant (Table 2). The highest 1-year rates observed were based on self-report (28.7%). Claims-based 1-year test rates were 21.1%. The lowest rates were from medical records (19.4%). Across all demographic groups, 1-year rates based on self-report were higher than those from claims or medical records. Test use rates captured by claims were higher than those ascertained from the medical record except for those ages 50 to 64 years. However, similar patterns were observed, with the highest rates based on self-report and lowest rates from medical records. Table 3 shows the results from comparison of different data sources for reporting of FOBT. For the 1-year period, the sensitivity of the data sources ranged from 40% (self-report with claims) to 58% (claims with medical record). The highest positive predictive value was 53% (claims with medical records for both time windows). Agreement measure of FOBT use among the data sources was moderate (Table 3). The highest measures of agreement were observed in the comparison of medical records and Medicare claims for FOBT use in the previous 1 year (agreement, 82%; 95% CI, 79-85). The worst agreement for FOBT in the previous 1 year was between self-report and Medicare claims (agreement, 67%; 95% CI, 63-71). Across all three
4 802 Measuring FOBT Use by Medicare Enrollees Table 1. Evidence of most recent FOBT found in review of 5 y of medical records (N = 561), No. (N = 561) Percentage Home kit Office-based digital rectal exam Unable to determine type of FOBT No evidence of FOBT in medical record comparisons, the 1-year window had better agreement than the 2-year window. The report-to-records ratio of FOBT use in the past year, for the comparison of survey to medical record, was 1.5. The report-to-records ratio, for FOBT use in the past year for survey compared with Medicare claim, was 1.4. Both estimates indicate over-reporting. Given the limited agreement between the data sources on FOBT testing, we conducted several sensitivity analyses. First, we attempted to identify, in the Medicare claims, those tests that were conducted during office visits, assuming such tests would be more likely to be based on single cards rather than the three cards done as part of a home test kit. Using the CPT codes to designate office visits, we created a flag to indicate when FOBT occurred in the claims files on the same date as an office visit claim, labeling those FOBTs as presumptively single-card tests. We then excluded those claims and compared FOBTs not linked to office visits to the FOBTs identified in the medical record as having been done using the three-card approach. The concordance measures were virtually unchanged (data not shown). Second, we included all FOBTs found in the medical record, thereby including digital rectal exams done in the office. We examined the concordance of this revised definition of medical record FOBT with FOBTs identified using all Medicare claims, with similar results (data not shown). Finally, we examined the potential of using more than one data source as the gold standard. We created variables to characterize FOBT testing in either of two data sources (claim or medical record, medical record or survey, and claim or survey) and used the two-source test use measure as the gold standard against which to compare the third data source. We created two versions of the two-source test use measures, accommodating definitions for claims and medical records to include or exclude office-based tests. None of the comparisons, with any of the modifications or combinations attempted, showed sufficient concordance to instill confidence in the use of any of the data sources (data not shown). Discussion We found that no data source could be established as providing complete and valid information about FOBT use among Medicare enrollees in fee for service. Our primary purpose for conducting these analyses was to determine whether Medicare claims could be used to accurately measure FOBT. Other investigators have used Medicare claims to assess use of FOBT (19-24). Our results provide strong evidence that these claims are not a reliable source for measuring FOBT. However, the limitations of the data are not restricted to Medicare claims; all three data sources examined in this study were imperfect sources of information about FOBT use. Table 2. Evidence of FOBT use in past 1 and 2 y, by participant characteristic and data source, Total study population (N = 561) FOBT in past 1 y Percentage of study group with FOBT FOBT in past 2 y Self-report Claim Medical record Self-report Claim Medical record Overall Age (y) Race African-American White Sex Female Male Education Less than high school High school High school plus Marital status Married Divorced, separated, single Widowed Low income No state buy in State buy in Region Eastern NC Central NC Western NC NOTE: Study population numbers and percentages within characteristic may not sum to total population due to missing information.
5 803 CEBP Focus: Validating Colorectal Cancer Screening Behaviors Table 3. Assessment of accuracy and completeness of FOBT by medicare claim, medical record, and self-report, Data sources compared* Type of test Test was found in: Measures of concordance Both sources (A) Source 1 only (B) Source 2 only (C) Neither source (D) Sensitivity Specificity PPV NPV Agreement Claim to medical In past 1 y (48-67) 88 (85-91) 53 (44-62) 90 (87-92) 82 (79-85) record In past 2 y (55-70) 77 (73-81) 53 (46-60) 83 (79-87) 73 (69-77) Self-report to In past 1 y (37-56) 76 (72-80) 32 (24-39) 86 (82-89) 70 (66-74) medical record In past 2 y (54-68) 63 (58-68) 40 (34-47) 80 (75-84) 62 (58-66) Self-report to claim In past 1 y (31-48) 74 (70-78) 29 (22-36) 82 (78-86) 67 (63-71) In past 2 y (43-57) 59 (54-64) 39 (33-45) 69 (64-75) 56 (52-60) NOTE: Formulas for assessment statistics: sensitivity = [A / (A + C)] 100; specificity = [D / (B + D)] 100; positive predictive value = [A / (A + B)] 100; negative predictive value = [D / (C + D)] 100; agreement = [(A + D) / (A + B + C + D)] 100. Abbreviations: PPV, positive predictive value; NPV, negative predictive value. * Comparisons are made using the second source listed (source 2) as the criterion standard. Our study results are in contrast to those of Baier et al. (25). In a study of managed care enrollees, these investigators compared self-reported FOBT use with test use based on laboratory evidence of FOBT cards and found high sensitivity and specificity (96% and 86%, respectively). One probable reason for the disparate results is that our study was conducted in a community setting where patients can, and do, visit multiple providers and thus have multiple medical records. In contrast, the study by Baier et al. was conducted in a health care system that used a single laboratory; this minimized the potential for missing a FOBT test by looking in the wrong medical record. Although most studies, including ours, have found FOBT self-reported use to be higher than claims or medical record documented levels, one study found the opposite pattern (26). In an intervention study, Lipkus et al. compared self-reported recall of FOBT use with laboratory records indicating that a FOBT kit had been returned to the study group. The finding of lower self-report in that study is likely due to two factors: more complete ascertainment of laboratory information and better ascertainment of self-report. In the study by Lipkus et al., FOBT kits were mailed to a central location, creating a more accurate gold standard. In addition, in their telephone survey, Lipkus et al. asked about completion of a FOBT in the previous 10 months, a shorter window than used in our study, thereby minimizing problems with recall. Our study underscores the difficulty of ascertaining test use rates for noninvasive, low-cost procedures conducted in multiple settings. Each data source has different reasons for its possibly inaccurate ascertainment of FOBT. Self-reported FOBT use may be higher than that found in claims or the medical record due to inaccurate or telescoped recall. On the other hand, selfreported FOBT use may be more accurate than claims because it can capture tests where no insurance was billed. Medicare claims, as the primary payer for Medicare enrollees, can, at least in theory, capture procedures done by multiple providers in multiple settings. However, lack of agreement between claims and medical records for procedures conducted in the physician office has been observed previously (27, 28). Adding to the confusion is the fact that, historically, the Medicare CPT-4 code for FOBT has provided reimbursement for one to three cards, making it impossible to distinguish claims for a FOBT based on a single card obtained by a digital rectal exam done by a physician and a FOBT based on three cards from a home test kit. Medical records can capture tests done regardless of payment source, but many people have more than one physician, especially over time. Thus, outside of an integrated health care system, a medical record from a single office can be incomplete. Even when a short time window was of interest, we found a substantial number of FOBT tests in the medical record with insufficient documentation to determine the type of test that had been conducted (i.e., digital rectal exam versus home test kit). Further complicating the measurement of FOBT, we found substantial documentation in medical records of FOBT having been done by digital rectal exam, which is not a recommended approach for CRC screening. It is unknown whether physicians discuss the office-based digital rectal exam with patients as a cancer screening approach, but it is possible that patients think they have been screened when they receive a digital rectal exam, thus adding to problems with self-report. The gap between the recommended use of a three-card home FOBT and the prevalence of physician use of office-based FOBT underscores the need for better understanding of how to incorporate screening guidelines into standard care. These findings have implications for health care providers and researchers interested in CRC screening. The poor concordance across FOBT data sources observed in this study shows that there is no single data source capable of accurately measuring FOBT use. An increasing interest in electronic medical records has fostered the expectation that their application will improve our ability to track preventive services use. However, for FOBT, documentation of the type of test (digital rectal exam versus home test kit) must be included before electronic medical records will improve our ability to monitor FOBT use through medical records. Effective January 1, 2007, Centers for Medicare & Medicaid Services implemented a new CPT code to help distinguish tests based on a single card obtained in the physician s office and tests based on three cards completed at home (29). This new code may improve the future ability of Medicare claims to capture
6 804 Measuring FOBT Use by Medicare Enrollees CRC screening with FOBT. Increasing use of immunochemical FOBT, which is reimbursed at a higher rate than guaiac FOBT, may also result in improved documentation of FOBT in claims and medical records. Future validation studies of FOBT should focus on assessing the effect of these recent changes. Acknowledgments We thank Jim Coan (Centers for Medicare & Medicaid Services) for project management support and Karen Bell (The Carolinas Center for Medical Excellence) for her assistance with coding questions. References 1. U.S. Preventive Services Task Force. Screening for colorectal cancer: recommendations and rationale. Ann Intern Med 2002;137: Winawer S, Fletcher R, Rex D, et al.; Gastrointestinal Consortium Panel. Colorectal cancer screening and surveillance: clinical guidelines and rationale update based on new evidence. Gastroenterology 2003;124: Smith RA, Cokkinides V, Eyre HJ. American Cancer Society guidelines for the early detection of cancer, CA Cancer J Clin 2003;53: Hiatt RA, Klabunde C, Breen N, Swan J, Ballard-Barbash R. Cancer screening practices from National Health Interview Surveys: past present and future. J Natl Cancer Inst 2002;94: Colorectal cancer test use in the Medicare population [report on the internet]. Cary (NC): The Carolinas Center for Medical Excellence [cited 2007 July 24]. Available from: thecarolinascenter.org/crcreport. 6. Hall IH, Van Den Eeden SK, Tolsma DD, et al. Testing for prostate and colorectal cancer: comparison of self-report and medical record audit. Prev Med 2004;39: Hiatt RA, Perez-Stable EJ, Quesenberry C, Sabogal F, Otero-Sabogal R, McPhee S. Agreement between self-reported early cancer detection practices and medical audits among Hispanic and non- Hispanic white health plan members in northern California. Prev Med 1995;24: Mandelson MT, LaCroix AZ, Anderson LA, Nadel MR, Lee NC. Comparison of self-reported fecal occult blood testing with automated laboratory records among older women in a health maintenance organization. Am J Epidemiol 1999;150: Lipkus IM, Rimer BK, Lyna PR, Pradhan AA, Conway M, Woods-Powell CT. Colorectal screening patterns and perceptions of risk among African-American users of a community health center. J Community Health 1996;21: Gordon NP, Hiatt RA, Lampert DI. Concordance of self-reported data and medical record audit for six cancer screening procedures. J Natl Cancer Inst 1993;85: Schenck AP, Klabunde CN, Warren JL, et al. Data sources for measuring colorectal endoscopy use among Medicare enrollees. Cancer Epidemiol Biomarkers Prev 2007;16: Outpatient Data Reports: October 2003 Diabetes and Breast Cancer Screening Performance and Provider Profiles. Technical Documentation, Appendix A. Outpatient Data QIOSC, Iowa Foundation for Medical Care, October American Medical Association. Current Procedural Terminology th ed. Chicago (IL): American Medical Association; HCPCS 1998: Medicare s National Level II Codes. Salt Lake City (UT): Medicode, Inc.; U.S. Department of Health and Human Services. Healthy People 2010: understanding and improving health. 2nd ed. Washington (DC): U.S. Government Printing Office; Hennekens CH, Buring JE. Epidemiology in medicine. Boston: Little, Brown and Company; Fleiss JL. Statistical methods for rates and proportions. 2nd ed. Wiley Series in probability and mathematical statistics. New York (NY): John Wiley & Sons, Inc.; Vernon SW, Briss PA, Trio JA, Warnecke RB. Some methodologic lessons learned from cancer screening research. Cancer 2004;101: Lurie JD, Welch HG. Diagnostic testing following fecal occult blood screening in the elderly. J Natl Cancer Inst 1999;91: Engelman KK, Ellerbeck EF, Ahluwalia JS, Nazir N, Velasco A. Fecal occult blood test use by Kansas Medicare beneficiaries. Prev Med 2001;33: Cooper GS, Koroukian SM. Racial disparities in the use of and indications for colorectal procedures in Medicare beneficiaries. Cancer 2004;100: Cooper GS, Koroukian SM. Geographic variation among Medicare beneficiaries in the use of colorectal carcinoma screening procedures. Am J Gastroenterol 2004;99: Cooper GS, Payes JD. Receipt of colorectal testing prior to colorectal carcinoma diagnosis. Cancer 2005;103: Koroukian SM, Litaker D, Dor A, Cooper GS. Use of preventive services by Medicare fee-for-service beneficiaries: does spillover from managed care matter? Med Care 2005;43: Baier M, Calonge N, Cutter G, et al. Validity of self-reported colorectal cancer screening behavior. Cancer Epidemiol Biomarkers Prev 2000;9: Lipkus IM, Samsa GP, Dement J, et al. Accuracy of self-reports of fecal occult blood tests and test results among individuals in the carpentry trade. Prev Med 2003;37: Koroukian SM, Xu F, Dor A, Cooper GS. Colorectal cancer screening in the elderly population: disparities by dual Medicare-Medicaid enrollment status. Health Serv Res 2006;41: Fowles JB, Lawthers AG, Weiner JP, Garnick DW, Petrie DS, Palmer HR. Agreement between physicians office records and Medicare Part B claims data. Health Care Financ Rev 1995;16: Medicare Learning Network Matters SE0710 [newsletter on the internet], Baltimore (MD): Centers for Medicare & Medicaid Services [cited 2007 September 17]. Available from: cms.hhs.gov/mlnmattersarticles/downloads/se0710.pdf.
Clinic Readiness Survey Leadership
 Clinic Readiness Survey Leadership Date of interview: Organizational interview ID#: Interviewer: Interview modality: 1 phone 2 in-person STOP CRC is a program about colon health. As part of STOP CRC, we
Clinic Readiness Survey Leadership Date of interview: Organizational interview ID#: Interviewer: Interview modality: 1 phone 2 in-person STOP CRC is a program about colon health. As part of STOP CRC, we
Inequalities in Colon Cancer
 Inequalities in Colon Cancer Chyke Doubeni, MD, FRCS, MPH Chair and The Presidential Associate Professor Department of Family Medicine and Community Health Perelman School of Medicine Senior Scholar, Center
Inequalities in Colon Cancer Chyke Doubeni, MD, FRCS, MPH Chair and The Presidential Associate Professor Department of Family Medicine and Community Health Perelman School of Medicine Senior Scholar, Center
Rethrowing Health Care Disadvantages in North Carolina
 PEER-REVIEWED ARTICLE Racial/Ethnic Differences in Quality of Care for North Carolina Medicaid Recipients C. Annette DuBard, MD, MPH; Angie Yow, RN; Susan Bostrom, RN; Emad Attiah, MSc; Brad Griffith,
PEER-REVIEWED ARTICLE Racial/Ethnic Differences in Quality of Care for North Carolina Medicaid Recipients C. Annette DuBard, MD, MPH; Angie Yow, RN; Susan Bostrom, RN; Emad Attiah, MSc; Brad Griffith,
Health care accounts for a large and increasing share of the. Administrative and Claims Records as Sources of Health Care Cost Data
 CONDUCTING THE COST ANALYSIS Administrative and Claims Records as Sources of Health Care Cost Data Gerald F. Riley, MSPH Background: Many economic studies of disease require cost data at the person level
CONDUCTING THE COST ANALYSIS Administrative and Claims Records as Sources of Health Care Cost Data Gerald F. Riley, MSPH Background: Many economic studies of disease require cost data at the person level
1992 2001 Aggregate data available; release of county or case-based data requires approval by the DHMH Institutional Review Board
 50 Table 2.4 Maryland Cancer-Related base Summary: bases That Can Be Used for Cancer Surveillance base/system and/or of MD Cancer Registry Administration, Center for Cancer Surveillance and Control 410-767-5521
50 Table 2.4 Maryland Cancer-Related base Summary: bases That Can Be Used for Cancer Surveillance base/system and/or of MD Cancer Registry Administration, Center for Cancer Surveillance and Control 410-767-5521
CANCER AND MEDICARE A CHARTBOOK
 CANCER AND MEDICARE A CHARTBOOK February 2009 PREPARED BY: Lisa Potetz Health Policy Alternatives, Inc. Leticia Flores DeWilde American Cancer Society Cancer Action Network (ACS CAN) ACKNOWLEDGEMENTS We
CANCER AND MEDICARE A CHARTBOOK February 2009 PREPARED BY: Lisa Potetz Health Policy Alternatives, Inc. Leticia Flores DeWilde American Cancer Society Cancer Action Network (ACS CAN) ACKNOWLEDGEMENTS We
Colorectal Cancer Screening Behaviors among American Indians in the Midwest
 JOURNAL OF HD RP Journal of Health Disparities Research and Practice Volume 4, Number 2, Fall 2010, pp. 35 40 2010 Center for Health Disparities Research School of Community Health Sciences University
JOURNAL OF HD RP Journal of Health Disparities Research and Practice Volume 4, Number 2, Fall 2010, pp. 35 40 2010 Center for Health Disparities Research School of Community Health Sciences University
This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement.
 This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement. Suggested Citation Centers for Disease Control and Prevention.
This publication was developed and produced with funding from the Centers for Disease Control and Prevention under a cooperative agreement. Suggested Citation Centers for Disease Control and Prevention.
COLORECTAL CANCER SCREENING
 COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
Medical Care Costs for Diabetes Associated with Health Disparities Among Adults Enrolled in Medicaid in North Carolina
 No. 160 August 2009 Among Adults Enrolled in Medicaid in North Carolina by Paul A. Buescher, Ph.D. J. Timothy Whitmire, Ph.D. Barbara Pullen-Smith, M.P.H. A Joint Report from the and the Office of Minority
No. 160 August 2009 Among Adults Enrolled in Medicaid in North Carolina by Paul A. Buescher, Ph.D. J. Timothy Whitmire, Ph.D. Barbara Pullen-Smith, M.P.H. A Joint Report from the and the Office of Minority
Colorado Cancer Coalition Priorities: 2016 2018
 Option 3 of 10: Screening & Early Detection: Screening Rates Presenter: Toni Panetta, MA, Director of Mission Programs, Susan G. Komen Colorado Goal 5: Objective 5.1: Objective 5.2 Focus Area: Focus Area:
Option 3 of 10: Screening & Early Detection: Screening Rates Presenter: Toni Panetta, MA, Director of Mission Programs, Susan G. Komen Colorado Goal 5: Objective 5.1: Objective 5.2 Focus Area: Focus Area:
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health
MEDICARE PAYMENTS FOR DIAGNOSTIC RADIOLOGY SERVICES IN EMERGENCY DEPARTMENTS
 Department of Health and Human Services OFFICE OF INSPECTOR GENERAL MEDICARE PAYMENTS FOR DIAGNOSTIC RADIOLOGY SERVICES IN EMERGENCY DEPARTMENTS Daniel R. Levinson Inspector General April 2011 OEI-07-09-00450
Department of Health and Human Services OFFICE OF INSPECTOR GENERAL MEDICARE PAYMENTS FOR DIAGNOSTIC RADIOLOGY SERVICES IN EMERGENCY DEPARTMENTS Daniel R. Levinson Inspector General April 2011 OEI-07-09-00450
National Findings on Access to Health Care and Service Use for Non-elderly Adults Enrolled in Medicaid
 National Findings on Access to Health Care and Service Use for Non-elderly Adults Enrolled in Medicaid By Sharon K. Long Karen Stockley Elaine Grimm Christine Coyer Urban Institute MACPAC Contractor Report
National Findings on Access to Health Care and Service Use for Non-elderly Adults Enrolled in Medicaid By Sharon K. Long Karen Stockley Elaine Grimm Christine Coyer Urban Institute MACPAC Contractor Report
Coverage Analysis: The Cornerstone of Clinical Research Billing Presented by: Mary L. Veazie, CPA, MBA, CHC, CHRC Executive Director, Clinical
 Coverage Analysis: The Cornerstone of Clinical Research Billing Presented by: Mary L. Veazie, CPA, MBA, CHC, CHRC Executive Director, Clinical Research Finance The University of Texas MD Anderson Cancer
Coverage Analysis: The Cornerstone of Clinical Research Billing Presented by: Mary L. Veazie, CPA, MBA, CHC, CHRC Executive Director, Clinical Research Finance The University of Texas MD Anderson Cancer
Cancer Screening. Robert L. Robinson, MD, MS. Ambulatory Conference SIU School of Medicine Department of Internal Medicine.
 Cancer Screening Robert L. Robinson, MD, MS Ambulatory Conference SIU School of Medicine Department of Internal Medicine March 13, 2003 Why screen for cancer? Early diagnosis often has a favorable prognosis
Cancer Screening Robert L. Robinson, MD, MS Ambulatory Conference SIU School of Medicine Department of Internal Medicine March 13, 2003 Why screen for cancer? Early diagnosis often has a favorable prognosis
Leveraging Electronic Health Records to Increase Colorectal Cancer Screening
 Leveraging Electronic Health Records to Increase Colorectal Cancer Screening Purpose of this presentation: Part 1: To present the results of a large EHR leveraged randomized trial performed in an integrated
Leveraging Electronic Health Records to Increase Colorectal Cancer Screening Purpose of this presentation: Part 1: To present the results of a large EHR leveraged randomized trial performed in an integrated
C-CoP (1B1b) Results, Procedure-Based Report for Colorectal Cancer Screening by Jurisdiction
 Appendix J: Explanation of Colorectal Cancer Reports C-CoP (1B1b) Results, Procedure-Based Report for Colorectal Cancer Screening by Jurisdiction Purpose: The purpose of this report is to give a summary
Appendix J: Explanation of Colorectal Cancer Reports C-CoP (1B1b) Results, Procedure-Based Report for Colorectal Cancer Screening by Jurisdiction Purpose: The purpose of this report is to give a summary
Site of Service Cost Differences for Medicare Patients Receiving Chemotherapy
 Site of Service Cost Differences for Medicare Patients Receiving Chemotherapy October, 2011 Prepared by: Kate Fitch, RN, MEd Principal and Healthcare Management Consultant Bruce Pyenson, FSA, MAAA Principal
Site of Service Cost Differences for Medicare Patients Receiving Chemotherapy October, 2011 Prepared by: Kate Fitch, RN, MEd Principal and Healthcare Management Consultant Bruce Pyenson, FSA, MAAA Principal
Economic Assessment of Providing Mental Health Services in Rural Health Clinics
 Economic Assessment of Providing Mental Health Services in Rural Health Clinics Fred C. Eilrich Assistant State Extension Specialist Email: eilrich@okstate.edu Cheryl F. St. Clair Associate State Extension
Economic Assessment of Providing Mental Health Services in Rural Health Clinics Fred C. Eilrich Assistant State Extension Specialist Email: eilrich@okstate.edu Cheryl F. St. Clair Associate State Extension
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2012
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2012 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health Interview Statistics,
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2012 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health Interview Statistics,
Increasing Quality Colorectal An Action Guide for Working
 Increasing Quality Colorectal An Action Guide for Working Cancer Screening: with Health Systems U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. This publication
Increasing Quality Colorectal An Action Guide for Working Cancer Screening: with Health Systems U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. This publication
Health Insurance Coverage of Children Under Age 19: 2008 and 2009
 Health Insurance Coverage of Children Under Age 19: 2008 and 2009 American Community Survey Briefs Issued September 2010 ACSBR/09-11 IntroductIon Health insurance, whether private or public, improves children
Health Insurance Coverage of Children Under Age 19: 2008 and 2009 American Community Survey Briefs Issued September 2010 ACSBR/09-11 IntroductIon Health insurance, whether private or public, improves children
Medicare Supplemental Coverage in Minnesota
 Medicare Supplemental Coverage in Minnesota December 2002 h ealth e conomics p rogram Health Policy and Systems Compliance Division Minnesota Department of Health Medicare Supplemental Coverage in Minnesota
Medicare Supplemental Coverage in Minnesota December 2002 h ealth e conomics p rogram Health Policy and Systems Compliance Division Minnesota Department of Health Medicare Supplemental Coverage in Minnesota
MEDICARE PHYSICAL THERAPY. Self-Referring Providers Generally Referred More Beneficiaries but Fewer Services per Beneficiary
 United States Government Accountability Office Report to Congressional Requesters April 2014 MEDICARE PHYSICAL THERAPY Self-Referring Providers Generally Referred More Beneficiaries but Fewer Services
United States Government Accountability Office Report to Congressional Requesters April 2014 MEDICARE PHYSICAL THERAPY Self-Referring Providers Generally Referred More Beneficiaries but Fewer Services
Preventive Health Care Services Provided to the New Hampshire Medicaid Adult Population with Comparisons to the Commercially Insured Population
 Preventive Health Care Services Provided to the New Hampshire Medicaid Adult Population with Comparisons to the Commercially Insured Population A report prepared for the New Hampshire Department of Health
Preventive Health Care Services Provided to the New Hampshire Medicaid Adult Population with Comparisons to the Commercially Insured Population A report prepared for the New Hampshire Department of Health
Epi procolon The Blood Test for Colorectal Cancer Screening
 Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
a GAO-04-713 GAO PRIVATE HEALTH INSURANCE Coverage of Key Colorectal Cancer Screening Tests Is Common but Not Universal
 GAO United States General Accounting Office Report to the Ranking Minority Member, Committee on Health, Education, Labor, and Pensions, U.S. Senate June 2004 PRIVATE HEALTH INSURANCE Coverage of Key Colorectal
GAO United States General Accounting Office Report to the Ranking Minority Member, Committee on Health, Education, Labor, and Pensions, U.S. Senate June 2004 PRIVATE HEALTH INSURANCE Coverage of Key Colorectal
Evaluation of Diagnostic and Screening Tests: Validity and Reliability. Sukon Kanchanaraksa, PhD Johns Hopkins University
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Observation Coding and Billing
 How do you get paid? Observation Coding and Billing Michael Ross MD FACEP President, Society of Chest Pain Centers Medical Director, Chest Pain Center and Observation Medicine Associate Professor, Department
How do you get paid? Observation Coding and Billing Michael Ross MD FACEP President, Society of Chest Pain Centers Medical Director, Chest Pain Center and Observation Medicine Associate Professor, Department
Colorectal Cancer: Preventable, Beatable, Treatable. American Cancer Society
 Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2013 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2013 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Access to Health Services
 Ah Access to Health Services Access to Health Services HP 2020 Goal Improve access to comprehensive, quality health care services. HP 2020 Objectives Increase the proportion of persons with a usual primary
Ah Access to Health Services Access to Health Services HP 2020 Goal Improve access to comprehensive, quality health care services. HP 2020 Objectives Increase the proportion of persons with a usual primary
An Action Guide for Engaging Employers and Professional Medical Organizations
 Increasing Quality Colorectal Cancer Screening and Promoting Screen Quality: An Action Guide for Engaging Employers and Professional Medical Organizations U.S. Department of Health and Human Services,
Increasing Quality Colorectal Cancer Screening and Promoting Screen Quality: An Action Guide for Engaging Employers and Professional Medical Organizations U.S. Department of Health and Human Services,
kaiser medicaid commission on and the uninsured May 2009 Community Care of North Carolina: Putting Health Reform Ideas into Practice in Medicaid
 P O L I C Y B R I E F kaiser commission on medicaid SUMMARY and the uninsured Community Care of North Carolina: Putting Health Reform Ideas into Practice in Medicaid May 2009 Why is Community Care of North
P O L I C Y B R I E F kaiser commission on medicaid SUMMARY and the uninsured Community Care of North Carolina: Putting Health Reform Ideas into Practice in Medicaid May 2009 Why is Community Care of North
Comparative effectiveness of two pharmacy-based colorectal cancer screening interventions during an annual influenza. vaccination campaign.
 Research Comparative effectiveness of two pharmacy-based colorectal cancer screening interventions during an annual influenza vaccination campaign Michael B. Potter, Ginny Gildengorin, Yinan Wang, May
Research Comparative effectiveness of two pharmacy-based colorectal cancer screening interventions during an annual influenza vaccination campaign Michael B. Potter, Ginny Gildengorin, Yinan Wang, May
Custodial Mothers and Fathers and Their Child Support: 2011
 Custodial Mothers and Fathers and Their Child Support: 2011 Current Population Reports By Timothy Grall Issued October 2013 P60-246 IntroductIon This report focuses on the child support income that custodial
Custodial Mothers and Fathers and Their Child Support: 2011 Current Population Reports By Timothy Grall Issued October 2013 P60-246 IntroductIon This report focuses on the child support income that custodial
EQR PROTOCOL 4 VALIDATION OF ENCOUNTER DATA REPORTED BY THE MCO
 OMB Approval No. 0938-0786 EQR PROTOCOL 4 VALIDATION OF ENCOUNTER DATA REPORTED BY THE MCO A Voluntary Protocol for External Quality Review (EQR) Protocol 1: Assessment of Compliance with Medicaid Managed
OMB Approval No. 0938-0786 EQR PROTOCOL 4 VALIDATION OF ENCOUNTER DATA REPORTED BY THE MCO A Voluntary Protocol for External Quality Review (EQR) Protocol 1: Assessment of Compliance with Medicaid Managed
A Health Profile of Older North Carolinians
 A Health Profile of Older North Carolinians A Joint Publication of the State Center for Health Statistics and Older Adult Health Branch North Carolina Division of Public Health and North Carolina Division
A Health Profile of Older North Carolinians A Joint Publication of the State Center for Health Statistics and Older Adult Health Branch North Carolina Division of Public Health and North Carolina Division
Screening for Cancer in Light of New Guidelines and Controversies. Christopher Celio, MD St. Jude Heritage Medical Group
 Screening for Cancer in Light of New Guidelines and Controversies Christopher Celio, MD St. Jude Heritage Medical Group Screening Tests The 2 major objectives of a good screening program are: (1) detection
Screening for Cancer in Light of New Guidelines and Controversies Christopher Celio, MD St. Jude Heritage Medical Group Screening Tests The 2 major objectives of a good screening program are: (1) detection
Ontario Health Insurance Plan (OHIP) Billing Codes Information and Procedures for Claiming the Cumulative Preventative Care Bonus
 Ontario Health Insurance Plan (OHIP) Billing Codes Information and Procedures for Claiming the Cumulative Preventative Care Bonus Eligible Patient Enrolment Model (PEM) physicians may receive Cumulative
Ontario Health Insurance Plan (OHIP) Billing Codes Information and Procedures for Claiming the Cumulative Preventative Care Bonus Eligible Patient Enrolment Model (PEM) physicians may receive Cumulative
colon cancer Talk to your doctor about getting tested for colon cancer. They know how to prevent and you can, too. Take a look inside.
 2006, American Cancer Society, Inc. No. 243900 Rev.01/08 The American Cancer Society is the nationwide community-based voluntary health organization dedicated to eliminating cancer as a major health problem
2006, American Cancer Society, Inc. No. 243900 Rev.01/08 The American Cancer Society is the nationwide community-based voluntary health organization dedicated to eliminating cancer as a major health problem
THE U.S. HEALTH WORKFORCE CHARTBOOK. Part III: Technologists & Technicians and Aides & Assistants
 THE U.S. HEALTH WORKFORCE CHARTBOOK Part III: Technologists & Technicians and Aides & Assistants U.S. Department of Health and Human Services Health Resources and Services Administration National Center
THE U.S. HEALTH WORKFORCE CHARTBOOK Part III: Technologists & Technicians and Aides & Assistants U.S. Department of Health and Human Services Health Resources and Services Administration National Center
PLAN DESIGN AND BENEFITS HMO Open Access Plan 912
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
PLAN DESIGN AND BENEFITS POS Open Access Plan 1944
 PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
PharmaSUG2011 Paper HS03
 PharmaSUG2011 Paper HS03 Using SAS Predictive Modeling to Investigate the Asthma s Patient Future Hospitalization Risk Yehia H. Khalil, University of Louisville, Louisville, KY, US ABSTRACT The focus of
PharmaSUG2011 Paper HS03 Using SAS Predictive Modeling to Investigate the Asthma s Patient Future Hospitalization Risk Yehia H. Khalil, University of Louisville, Louisville, KY, US ABSTRACT The focus of
Total Cost of Cancer Care by Site of Service: Physician Office vs Outpatient Hospital
 Total Cost of Cancer Care by Site of Service: Physician Office vs Outpatient Hospital Prepared by Avalere Health, LLC Page 2 Executive Summary Avalere Health analyzed three years of commercial health plan
Total Cost of Cancer Care by Site of Service: Physician Office vs Outpatient Hospital Prepared by Avalere Health, LLC Page 2 Executive Summary Avalere Health analyzed three years of commercial health plan
Trends in Medigap Enrollment and Coverage Options, 2013
 November 2014 Trends in Medigap Enrollment and Coverage Options, 2013 www.ahipresearch.org LIST OF TABLES AND FIGURES TABLE 1. TABLE 2. TABLE 3. TABLE 4. Distribution of Medigap Companies with Standardized
November 2014 Trends in Medigap Enrollment and Coverage Options, 2013 www.ahipresearch.org LIST OF TABLES AND FIGURES TABLE 1. TABLE 2. TABLE 3. TABLE 4. Distribution of Medigap Companies with Standardized
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2013
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2013 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health Interview Statistics,
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, 2013 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health Interview Statistics,
QUALITY OF LAST DOCTOR VISIT REPORTS: A COMPARISON OF MEDICAL RECORD AND SURVEY DATA
 QUALITY OF LAST DOCTOR VISIT REPORTS: A COMPARISON OF MEDICAL RECORD AND SURVEY DATA Gina M. Jay, Robert F. Belli, & James M. Lepkowski, Research Center Gina M. Jay, Research Center, University of Michigan,
QUALITY OF LAST DOCTOR VISIT REPORTS: A COMPARISON OF MEDICAL RECORD AND SURVEY DATA Gina M. Jay, Robert F. Belli, & James M. Lepkowski, Research Center Gina M. Jay, Research Center, University of Michigan,
Cancer screening: cost-effectiveness. Endoscopic polypectomy: : CRC mortality. Endoscopic polypectomy: : CRC incidence
 Cribado del cáncer (colorrectal): las pruebas de detección precoz salvan vidas Dr. Antoni Castells Servicio de Gastroenterología Hospital Clínic nic,, Barcelona (castells@clinic.cat) Conditions for a population-based
Cribado del cáncer (colorrectal): las pruebas de detección precoz salvan vidas Dr. Antoni Castells Servicio de Gastroenterología Hospital Clínic nic,, Barcelona (castells@clinic.cat) Conditions for a population-based
Early Detection of Colorectal Cancer Made Easy with a Blood Test
 INFORMATION FOR PHYSICIANS Early Detection of Colorectal Cancer Made Easy with a Blood Test Epi pro Colon 2.0 : 2 nd Generation Septin 9 Test CRC SCREENING SAVES LIVES Colorectal cancer is a major health
INFORMATION FOR PHYSICIANS Early Detection of Colorectal Cancer Made Easy with a Blood Test Epi pro Colon 2.0 : 2 nd Generation Septin 9 Test CRC SCREENING SAVES LIVES Colorectal cancer is a major health
Twenty-first century radiology requires rapid and. Radiology by Nonradiologists: Is Report Documentation Adequate? CLINICAL. Shelley Nan Weiner, MD
 CLINICAL Radiology by Nonradiologists: Is Report Documentation Adequate? Shelley Nan Weiner, MD Objective: To determine if the quality of medical imaging reports differs significantly between radiologists
CLINICAL Radiology by Nonradiologists: Is Report Documentation Adequate? Shelley Nan Weiner, MD Objective: To determine if the quality of medical imaging reports differs significantly between radiologists
Health Care Utilization and Costs of Full-Pay and Subsidized Enrollees in the Florida KidCare Program: MediKids
 Health Care Utilization and Costs of Full-Pay and Subsidized Enrollees in the Florida KidCare Program: MediKids Prepared for the Florida Healthy Kids Corporation Prepared by Jill Boylston Herndon, Ph.D.
Health Care Utilization and Costs of Full-Pay and Subsidized Enrollees in the Florida KidCare Program: MediKids Prepared for the Florida Healthy Kids Corporation Prepared by Jill Boylston Herndon, Ph.D.
Despite the acknowledged effectiveness of colorectal cancer (CRC)
 Primary Care, Economic Barriers to Health Care, and Use of Colorectal Cancer Screening Tests Among Medicare Enrollees Over Time Chyke A. Doubeni, MD, MPH 1,2 Adeyinka O. Laiyemo, MD, MPH 3 Angela C. Young,
Primary Care, Economic Barriers to Health Care, and Use of Colorectal Cancer Screening Tests Among Medicare Enrollees Over Time Chyke A. Doubeni, MD, MPH 1,2 Adeyinka O. Laiyemo, MD, MPH 3 Angela C. Young,
The Collaborative Models of Mental Health Care for Older Iowans. Model Administration. Collaborative Models of Mental Health Care for Older Iowans 97
 6 The Collaborative Models of Mental Health Care for Older Iowans Model Administration Collaborative Models of Mental Health Care for Older Iowans 97 Collaborative Models of Mental Health Care for Older
6 The Collaborative Models of Mental Health Care for Older Iowans Model Administration Collaborative Models of Mental Health Care for Older Iowans 97 Collaborative Models of Mental Health Care for Older
Colon Cancer. What Is Colon Cancer? What Are the Screening Methods?
 Cancer of the colon or rectum (colorectal cancer) is the second most common cancer in the U.S. In fact, of all people born, 1 in 40 will die of the disease. What Is Colon Cancer? Colon cancer begins with
Cancer of the colon or rectum (colorectal cancer) is the second most common cancer in the U.S. In fact, of all people born, 1 in 40 will die of the disease. What Is Colon Cancer? Colon cancer begins with
GAO HEALTH INSURANCE. Report to the Committee on Health, Education, Labor, and Pensions, U.S. Senate. United States Government Accountability Office
 GAO United States Government Accountability Office Report to the Committee on Health, Education, Labor, and Pensions, U.S. Senate March 2008 HEALTH INSURANCE Most College Students Are Covered through Employer-Sponsored
GAO United States Government Accountability Office Report to the Committee on Health, Education, Labor, and Pensions, U.S. Senate March 2008 HEALTH INSURANCE Most College Students Are Covered through Employer-Sponsored
Medicare Advantage special needs plans
 O n l i n e A p p e n d i x e s14 Medicare Advantage special needs plans 14-A O n l i n e A p p e n d i x Additional data on Medicare Advantage special needs plans and information on quality TABLE 14 A1
O n l i n e A p p e n d i x e s14 Medicare Advantage special needs plans 14-A O n l i n e A p p e n d i x Additional data on Medicare Advantage special needs plans and information on quality TABLE 14 A1
Explanation of care coordination payments as described in Section 223.000 of the PCMH provider manual
 Explanation of care coordination payments as described in Section 223.000 of the PCMH provider manual Determination of beneficiary risk Per beneficiary amounts Per beneficiary amounts 1 For the first year
Explanation of care coordination payments as described in Section 223.000 of the PCMH provider manual Determination of beneficiary risk Per beneficiary amounts Per beneficiary amounts 1 For the first year
Aetna Life Insurance Company Hartford, Connecticut 06156
 Aetna Life Insurance Company Hartford, Connecticut 06156 Extraterritorial Certificate Rider (GR-9N-CR1) Policyholder: The TLC Companies Group Policy No.: GP-811431 Rider: West Virginia ET Medical Issue
Aetna Life Insurance Company Hartford, Connecticut 06156 Extraterritorial Certificate Rider (GR-9N-CR1) Policyholder: The TLC Companies Group Policy No.: GP-811431 Rider: West Virginia ET Medical Issue
!"#$%&%'()&*+'"(,+"''*-*.
 /0'"0-'1!"#$%&%'()&*+'"(,+"''*-*.!"#$%&%'()&*)'"(+$(%,'($')#*-(.'&-+*/()&0$'(#1()&*)'"2"'.&%'-(-'&%,(+*(3'*(&*-(&4#0%(56(7'")'*%(#1(&..( -+&/*#$'-(7"#$%&%'()&*)'"$(&"'(1#0*-(+*(3'*(&/'(58(#"(#.-'"9 : (;'-+)&"'(7"#
/0'"0-'1!"#$%&%'()&*+'"(,+"''*-*.!"#$%&%'()&*)'"(+$(%,'($')#*-(.'&-+*/()&0$'(#1()&*)'"2"'.&%'-(-'&%,(+*(3'*(&*-(&4#0%(56(7'")'*%(#1(&..( -+&/*#$'-(7"#$%&%'()&*)'"$(&"'(1#0*-(+*(3'*(&/'(58(#"(#.-'"9 : (;'-+)&"'(7"#
Case Study Dr. Damian Folch, Chelmsford, MA. Practice Improvement. Leadership in Patient Safety
 Proactive Reduction in Outpatient Malpractice: Improving Safety and Efficiency and Satisfaction (PROMISES) Case Study Dr. Damian Folch, Chelmsford, MA Practice Improvement Leadership in Patient Safety
Proactive Reduction in Outpatient Malpractice: Improving Safety and Efficiency and Satisfaction (PROMISES) Case Study Dr. Damian Folch, Chelmsford, MA Practice Improvement Leadership in Patient Safety
Clinical Indicator Ages 19-29 Ages 30-39 Ages 40-49 Ages 50-64 Ages 65+ Frequency of visit as recommended by PCP
 SCREENING EXAMINATION & COUNSELING UPMC Health Plan Clinical Indicator Ages 19-29 Ages 30-39 Ages 40-49 Ages 50-64 Ages 65+ Annually Physical Exam and Counseling 1 Blood Pressure 2 At each visit. At least
SCREENING EXAMINATION & COUNSELING UPMC Health Plan Clinical Indicator Ages 19-29 Ages 30-39 Ages 40-49 Ages 50-64 Ages 65+ Annually Physical Exam and Counseling 1 Blood Pressure 2 At each visit. At least
Cancer Screening 22M 36% 56% Only 56% of uninsured women aged 50 74 are up-to-date with mammography screening. Colorectal Cancer Breast Cancer
 July 2010 22M 22 million adults aged 50 75 need to be screened for colorectal cancer, and 7 million women aged 50 74 need to be screened for breast cancer. Cancer Screening Colorectal Cancer Breast Cancer
July 2010 22M 22 million adults aged 50 75 need to be screened for colorectal cancer, and 7 million women aged 50 74 need to be screened for breast cancer. Cancer Screening Colorectal Cancer Breast Cancer
New Hampshire Accountable Care Project: Analytic Report User Guide
 New Hampshire Accountable Care Project: Analytic Report User Guide November 2015 Contents OVERVIEW... 2 Introduction... 2 User Guide Purpose... 2 USING THE ANALYTIC REPORT... 3 Report Access... 3 Report
New Hampshire Accountable Care Project: Analytic Report User Guide November 2015 Contents OVERVIEW... 2 Introduction... 2 User Guide Purpose... 2 USING THE ANALYTIC REPORT... 3 Report Access... 3 Report
inflammation of the pancreas and damage to the an increased risk of hypertension, stroke and Table 7.1: Classification of alcohol consumption
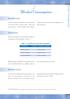 H E A LT H SURVEY Alcohol Consumption 7 Alcohol Consumption N AT I O N A L Introduction Excessive alcohol consumption is associated with inflammation of the pancreas and damage to the an increased risk
H E A LT H SURVEY Alcohol Consumption 7 Alcohol Consumption N AT I O N A L Introduction Excessive alcohol consumption is associated with inflammation of the pancreas and damage to the an increased risk
Colorectal Cancer: Preventable, Beatable, Treatable. American Cancer Society
 Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2016 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2016 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Disparities in Stage at Diagnosis, Survival, and Quality of Cancer Care in California by Source of Health Insurance
 Disparities in Stage at Diagnosis, Survival, and Quality of Cancer Care in California by Source of Health Insurance Acknowledgements and Disclaimer The collection of cancer incidence data used in this
Disparities in Stage at Diagnosis, Survival, and Quality of Cancer Care in California by Source of Health Insurance Acknowledgements and Disclaimer The collection of cancer incidence data used in this
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2014
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 04 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health Interview
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 04 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health Interview
Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety
 Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Measure #130 (NQF 0419): Documentation of Current Medications in the Medical Record National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY DESCRIPTION:
Preventive Medicine and Screening Policy
 REIMBURSEMENT POLICY Policy Number 2015R0013C Preventive Medicine and Screening Policy Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
REIMBURSEMENT POLICY Policy Number 2015R0013C Preventive Medicine and Screening Policy Annual Approval Date 3/11/2015 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT THIS REIMBURSEMENT
New York Small Group Indemnity Aetna Life Insurance Company Plan Effective Date: 10/01/2010. PLAN DESIGN AND BENEFITS - NY Indemnity 1-10/10*
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $7,500 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services,
PLAN DESIGN AND BENEFITS Basic HMO Copay Plan 1-10
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
Evaluating Mode Effects in the Medicare CAHPS Fee-For-Service Survey
 Evaluating Mode Effects in the Medicare Fee-For-Service Survey Norma Pugh, MS, Vincent Iannacchione, MS, Trang Lance, MPH, Linda Dimitropoulos, PhD RTI International, Research Triangle Park, NC 27709 Key
Evaluating Mode Effects in the Medicare Fee-For-Service Survey Norma Pugh, MS, Vincent Iannacchione, MS, Trang Lance, MPH, Linda Dimitropoulos, PhD RTI International, Research Triangle Park, NC 27709 Key
The Role of Insurance in Providing Access to Cardiac Care in Maryland. Samuel L. Brown, Ph.D. University of Baltimore College of Public Affairs
 The Role of Insurance in Providing Access to Cardiac Care in Maryland Samuel L. Brown, Ph.D. University of Baltimore College of Public Affairs Heart Disease Heart Disease is the leading cause of death
The Role of Insurance in Providing Access to Cardiac Care in Maryland Samuel L. Brown, Ph.D. University of Baltimore College of Public Affairs Heart Disease Heart Disease is the leading cause of death
White Paper. Medicare Part D Improves the Economic Well-Being of Low Income Seniors
 White Paper Medicare Part D Improves the Economic Well-Being of Low Income Seniors Kathleen Foley, PhD Barbara H. Johnson, MA February 2012 Table of Contents Executive Summary....................... 1
White Paper Medicare Part D Improves the Economic Well-Being of Low Income Seniors Kathleen Foley, PhD Barbara H. Johnson, MA February 2012 Table of Contents Executive Summary....................... 1
Health Care Access to Vulnerable Populations
 Health Care Access to Vulnerable Populations Closing the Gap: Reducing Racial and Ethnic Disparities in Florida Rosebud L. Foster, ED.D. Access to Health Care The timely use of personal health services
Health Care Access to Vulnerable Populations Closing the Gap: Reducing Racial and Ethnic Disparities in Florida Rosebud L. Foster, ED.D. Access to Health Care The timely use of personal health services
As Reported by the Senate Health, Human Services and Aging Committee. 127th General Assembly Regular Session Sub. S. B. No. 278 2007-2008 A B I L L
 As Reported by the Senate Health, Human Services and Aging Committee 127th General Assembly Regular Session Sub. S. B. No. 278 2007-2008 Senator Coughlin Cosponsors: Senators Stivers, Mumper, Spada, Miller,
As Reported by the Senate Health, Human Services and Aging Committee 127th General Assembly Regular Session Sub. S. B. No. 278 2007-2008 Senator Coughlin Cosponsors: Senators Stivers, Mumper, Spada, Miller,
Survey of Nurses 2013
 Survey of Nurses 2013 Survey of Nurses Report Summary Since 2004, the Michigan Center for Nursing has conducted an annual survey of Michigan nurses in conjunction with the licensure renewal process for
Survey of Nurses 2013 Survey of Nurses Report Summary Since 2004, the Michigan Center for Nursing has conducted an annual survey of Michigan nurses in conjunction with the licensure renewal process for
Standing for Equity Eliminating Disparities and Promoting Wellness
 The 2014 Culturally Competent Healthcare Event DiversityInc October 22, 2014 Standing for Equity Eliminating Disparities and Promoting Wellness Winston Wong, MD Medical Director, Community Benefit Director,
The 2014 Culturally Competent Healthcare Event DiversityInc October 22, 2014 Standing for Equity Eliminating Disparities and Promoting Wellness Winston Wong, MD Medical Director, Community Benefit Director,
Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico
 Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico Ruth Ríos-Motta, PhD, José A. Capriles-Quirós, MD, MPH, MHSA, Mario
Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico Ruth Ríos-Motta, PhD, José A. Capriles-Quirós, MD, MPH, MHSA, Mario
How To Calculate Health Insurance Coverage In The United States
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January March 2014 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January March 2014 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., M.H.S.A. Division of Health
Health Insurance Coverage: Estimates from the National Health Interview Survey, 2004
 Health Insurance Coverage: Estimates from the National Health Interview Survey, 2004 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., Division of Health Interview Statistics, National Center
Health Insurance Coverage: Estimates from the National Health Interview Survey, 2004 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., Division of Health Interview Statistics, National Center
Essential Hospitals VITAL DATA. Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012
 Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012 Published: July 2014 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Survey, FY 2012 Published: July 2014 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
United States General Accounting Office. Testimony MEDICARE
 GAO United States General Accounting Office Testimony Before the Committee on Finance, U.S. Senate For Release on Delivery Expected at 10:00 a.m. In Bozeman, Montana Tuesday, May 28, 2002 MEDICARE Using
GAO United States General Accounting Office Testimony Before the Committee on Finance, U.S. Senate For Release on Delivery Expected at 10:00 a.m. In Bozeman, Montana Tuesday, May 28, 2002 MEDICARE Using
Methodological Comparison of Estimates of Ambulatory Health Care Use from the Medical Expenditure Panel Survey and Other Data Sources
 Methodological Comparison of Estimates of Ambulatory Health Care Use from the Medical Expenditure Panel Survey and Other Data Sources Jeffrey A. Rhoades, Joel W. Cohen, and Steven R. Machlin Agency for
Methodological Comparison of Estimates of Ambulatory Health Care Use from the Medical Expenditure Panel Survey and Other Data Sources Jeffrey A. Rhoades, Joel W. Cohen, and Steven R. Machlin Agency for
Butler Memorial Hospital Community Health Needs Assessment 2013
 Butler Memorial Hospital Community Health Needs Assessment 2013 Butler County best represents the community that Butler Memorial Hospital serves. Butler Memorial Hospital (BMH) has conducted community
Butler Memorial Hospital Community Health Needs Assessment 2013 Butler County best represents the community that Butler Memorial Hospital serves. Butler Memorial Hospital (BMH) has conducted community
Essential Hospitals VITAL DATA. Results of America s Essential Hospitals Annual Hospital Characteristics Report, FY 2013
 Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Report, FY 2013 Published: March 2015 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
Essential Hospitals VITAL DATA Results of America s Essential Hospitals Annual Hospital Characteristics Report, FY 2013 Published: March 2015 1 ABOUT AMERICA S ESSENTIAL HOSPITALS METHODOLOGY America s
Colorectal Cancer Screening (FOBT)
 Colorectal Cancer Screening (FOBT) Rates of colorectal cancer screening are slowly increasing but remain very low in Ontario. In response, Cancer Care Ontario and the Ministry of Health and Long-Term Care
Colorectal Cancer Screening (FOBT) Rates of colorectal cancer screening are slowly increasing but remain very low in Ontario. In response, Cancer Care Ontario and the Ministry of Health and Long-Term Care
Health Insurance Coverage: Estimates from the National Health Interview Survey, 2005
 Health Insurance Coverage: Estimates from the National Health Interview Survey, 2005 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., Division of Health Interview Statistics, National Center
Health Insurance Coverage: Estimates from the National Health Interview Survey, 2005 by Robin A. Cohen, Ph.D., and Michael E. Martinez, M.P.H., Division of Health Interview Statistics, National Center
On the Road to Meaningful Use of EHRs:
 On the Road to Meaningful Use of EHRs: A Survey of California Physicians June 2012 On the Road to Meaningful Use of EHRs: A Survey of California Physicians Prepared for California HealthCare Foundation
On the Road to Meaningful Use of EHRs: A Survey of California Physicians June 2012 On the Road to Meaningful Use of EHRs: A Survey of California Physicians Prepared for California HealthCare Foundation
Computer-assisted Coding Software Improves Documentation, Coding, Compliance, and Revenue
 Computer-assisted Coding Software Improves Documentation, Coding, Compliance, and Revenue 1 Computer-assisted Coding Software Improves Documentation, Coding, Compliance, and Revenue by Sean Benson Abstract
Computer-assisted Coding Software Improves Documentation, Coding, Compliance, and Revenue 1 Computer-assisted Coding Software Improves Documentation, Coding, Compliance, and Revenue by Sean Benson Abstract
The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions. What is the Forzani MacPhail Colon Cancer Screening Centre?
 The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions What is the Forzani MacPhail Colon Cancer Screening Centre? The Forzani and MacPhail Colon Cancer Screening Centre (CCSC) is
The Forzani MacPhail Colon Cancer Screening Centre Frequently Asked Questions What is the Forzani MacPhail Colon Cancer Screening Centre? The Forzani and MacPhail Colon Cancer Screening Centre (CCSC) is
In the mid-1960s, the need for greater patient access to primary care. Physician Assistants in Primary Care: Trends and Characteristics
 Physician Assistants in Primary Care: Trends and Characteristics Bettie Coplan, MPAS, PA-C 1 James Cawley, MPH, PA-C 2 James Stoehr, PhD 1 1 Physician Assistant Program, College of Health Sciences, Midwestern
Physician Assistants in Primary Care: Trends and Characteristics Bettie Coplan, MPAS, PA-C 1 James Cawley, MPH, PA-C 2 James Stoehr, PhD 1 1 Physician Assistant Program, College of Health Sciences, Midwestern
Lost in Translation: The use of in-person interpretation vs. telephone interpretation services in the clinic setting with Spanish speaking patients
 Kellie Hawkins, MD, MPH CRC IRB Proposal November 2011 Lost in Translation: The use of in-person interpretation vs. telephone interpretation services in the clinic setting with Spanish speaking patients
Kellie Hawkins, MD, MPH CRC IRB Proposal November 2011 Lost in Translation: The use of in-person interpretation vs. telephone interpretation services in the clinic setting with Spanish speaking patients
Merrile Sing. Agency for Healthcare Research and Quality Working Paper No. 08011. December 2008
 Benchmarking Medicare Managed Care Plan Enrollment Estimates from the Medical Expenditure Panel Survey and Administrative Enrollment Files from the Centers for Medicare & Medicaid Services Merrile Sing
Benchmarking Medicare Managed Care Plan Enrollment Estimates from the Medical Expenditure Panel Survey and Administrative Enrollment Files from the Centers for Medicare & Medicaid Services Merrile Sing
STATISTICAL BRIEF #173
 Medical Expenditure Panel Survey STATISTICAL BRIEF #173 Agency for Healthcare Research and Quality June 27 Use of the Pap Test as a Cancer Screening Tool among Women Age 18 64, U.S. Noninstitutionalized
Medical Expenditure Panel Survey STATISTICAL BRIEF #173 Agency for Healthcare Research and Quality June 27 Use of the Pap Test as a Cancer Screening Tool among Women Age 18 64, U.S. Noninstitutionalized
The State of Multiple Myeloma Care. An Evaluation of Access to Medical Care
 The State of Multiple Myeloma Care An Evaluation of Access to Medical Care executive summary An access to care research survey of 239 multiple myeloma (MM) patients showed that a large majority (70%) of
The State of Multiple Myeloma Care An Evaluation of Access to Medical Care executive summary An access to care research survey of 239 multiple myeloma (MM) patients showed that a large majority (70%) of
SMALL GROUP PLAN DESIGN AND BENEFITS OPEN CHOICE OUT-OF-STATE PPO PLAN - $1,000
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
