EMERGENCY GUIDELINES FOR EARLY CHILDHOOD PROGRAMS
|
|
|
- Kevin Gallagher
- 10 years ago
- Views:
Transcription
1 EMERGENCY GUIDELINES FOR EARLY CHILDHOOD PROGRAMS Guidelines for helping an ill or injured child when a health consultant is not available. Missouri Department of Health and Senior Services, 2007 Missouri Head Start State Collaboration Office
2 EMERGENCY GUIDELINES FOR EARLY CHILDHOOD PROGRAMS Guidelines for helping an ill or injured child when a health consultant is not available. Allergic Reaction Asthma & Difficulty Breathing Behavioral Emergencies Bites Bleeding Blisters Bruises Burns CPR Child Abuse Choking Communicable Diseases Cuts Diabetes Diarrhea Ear Problems Electric Shock Eye Problems Fainting Fever Fractures & Sprains Frostbite Headache Head Injuries Heat Stroke Hypothermia Mouth & Jaw Injuries Neck & Back Injuries Nose Problems Poisoning & Overdose Puncture Wounds Rashes Seizures Splinters Stabs/Gunshots Stings Stomachaches Teeth Problems Tetanus Ticks Unconsciousness Vomiting Recommended First Aid Equipment & Supplies Emergency Numbers Emergencies Happen Missouri Head Start State Collaboration Office AN EQUAL OPPORTUNITY/AFFIRMATIVE ACTION EMPLOYER Services provided on a nondiscriminatory basis.
3 ABOUT THE GUIDELINES The emergency guidelines in this booklet were originally produced in 1997 by the Ohio Department of Public Safety, Emergency Medical Services for Children (EMSC) program, in cooperation with the Emergency Care Committee of the Ohio Chapter of the American Academy of Pediatrics (AAP). These guidelines have been revised for use in Missouri early childhood programs. The booklet is being made available by the Department of Health and Senior Services, Injury and Violence Prevention Program and the Missouri Head Start-State Collaboration Office at the Center for Family Policy and Research. The emergency guidelines are meant to serve as basic what to do in an emergency information for facility staff without medical/nursing education when a health consultant is not available. It is recommended that staff who are in a position to provide first-aid to children complete an approved first-aid and CPR course. The guidelines have been created as recommended procedures. It is not the intent of the guidelines to supersede or make invalid any laws or rules established by the child care facility, or the state of Missouri. Please check with your health consultant if you have questions regarding the recommendations in these guidelines. Please take some time to familiarize yourself with the format, the background information provided, and the How to Use the Guidelines section prior to an emergency situation.
4 HOW TO USE THE EMERGENCY GUIDELINES The back page of the booklet contains important information about key emergency numbers in your area. It is important to complete this information as soon as you receive the booklet as you will need to have this information ready in an emergency situation. The guidelines are arranged with tabs in alphabetical order for quick access. A colored flow chart format is used to guide you easily through all steps and symptoms from beginning to end. See the KEY TO SHAPES AND COLORS page. If there is any reason to suspect the injury may have been caused by physical abuse, refer to the facility policy for reporting suspected abuse and calling the Child Abuse Hot Line, Take some time to familiarize yourself with the EMERGENCY PROCEDURES FOR AN INJURY OR ILLNESS section. These procedures give a general overview of the recommended steps in an emergency situation and the safeguards that should be taken. In addition to injury and illness information, you will find information about infection control, and planning for children with special health care needs. The DHSS website ( under Health, School Health, Guidelines, has other manuals available on specific issues, including a document, Prevention and Control of Communicable Disease, that contains disease-specific information about symptoms, transmission and exclusion from child care facilities. This edition has been 3-hole punched so that it may be placed in a binder to facilitate addition of information specific for your child care setting and to update pages as appropriate. Please check with your health consultant if you have any questions concerning the recommendations contained in the guidelines.
5 KEY TO SHAPES & COLORS Start here. Provides first-aid instructions. OR A question is being asked. You will have a choice based on the child's condition. Stop here. This is the final instruction. A note to provide background information. This type of box should be read before emergencies occur. Green Shapes = Start Yellow Shapes = Continue Red Shapes = Stop Blue Shapes = Background Information
6 EMERGENCY PROCEDURES FOR INJURY OR ILLNESS Remain calm and assess the situation. Be sure the situation is safe for you to approach. The following dangers will require caution: live electrical wires, gas leaks, chemical spills, building damage, fire, smoke, traffic or violence. A adult should stay at the scene and give basic support until the person designated to handle emergencies arrives (medical or EMS personnel). Send for the person designated to handle emergencies. This person will take charge of the emergency and provide instruction and further first aid as needed. Do T give medications unless there has been prior approval by the parent/ guardian, the child s health care provider and/or according to an individualized emergency action or health care plan. Do T move a severely injured or ill child unless absolutely necessary for immediate safety. If moving is necessary to prevent further injury, follow the guidelines for NECK AND BACK INJURIES section. Call Emergency Medical Services (EMS) and arrange for transportation of the ill or injured child, if necessary. An administrator or a designated employee should notify the parent/guardian of the emergency as soon as possible to determine the appropriate course of action. If the parent/guardian cannot be reached, notify a parent/guardian substitute and call either the physician or the hospital, designated on the Emergency Information Card, so they will know to expect the injured/ill child. A adult should stay with the injured/seriously ill child. An incident report should be completed on all serious injuries, according to facility policy.
7 WHEN TO CALL EMERGENCY MEDICAL SERVICES (EMS) Call EMS if: the child is unconscious, semi-conscious or unusually confused. the child s airway is blocked. the child is not breathing. the child is having difficulty breathing, shortness of breath or is choking. the child has no pulse. the child has bleeding that won t stop. the child is coughing up or vomiting blood. the child has been poisoned. the child has a seizure for the first time, a seizure that lasts more than 5 minutes, or an atypical seizure. the child has injuries to the head, neck or back. the child has sudden, severe pain anywhere in the body. the child s condition is limb-threatening (for example, severe eye injuries, amputations or other injuries that may leave the child permanently disabled unless he/she receives immediate care.) the child s condition could worsen or become life-threatening on the way to the hospital if not transported by EMS. moving the child could cause further injury. the child needs the skills or equipment of paramedics or emergency medical technicians. distance or traffic conditions would cause a delay in getting the child to the hospital. If any of the above conditions exist, or if you are not sure, it is best to call EMS. Sources: American Red Cross & American College of Emergency Physicians
8 INFECTION CONTROL To reduce the spread of infectious diseases (diseases that can be spread from one person to another), it is important to follow Standard Precautions. Standard Precautions is a set of guidelines that assumes that all blood and certain other body fluids are potentially infectious. It is important to follow these precautions when providing care to any child, whether or not the child is known to be infectious. The following list describes Standard Precautions: 1. Wash hands thoroughly with warm running water and a mild, preferably liquid soap for at least 15 seconds, scrubbing between fingers, under fingernails and around the tops and palms of the hands. Handwashing should occur: before and after physical contact with any child (even if gloves have been worn) before and after eating or handling food after contact with a cleaning agent after using the restroom after providing any first-aid after removing gloves 2. Wear gloves when in contact with blood and other body fluids. 3. Wear protective eyewear and clothing when body fluids may come in contact with eyes or clothing (e.g., squirting blood). 4. Wear gloves and wipe up any blood or body fluid spills as soon as possible. Use cleaning materials per the facility exposure control plan for cleaning. 5. Double-bag the trash in a plastic bag or place in a sealable bag and dispose of immediately. 6. Clean the area with an approved disinfectant or a bleach solution (one part bleach to 100 parts of water). 7. Send all soiled clothing (i.e., clothing with blood, stool or vomit) home with the child in a double-bagged plastic bag. 8. Do not eat, or touch your mouth or eyes, while giving any first aid. Guidelines for children: Children should be taught basic handwashing, to wash hands before eating and after toileting, as well as encouraged to wash them any other time when appropriate. Frequent handwashing reduces the spread of illness and infection. Child care facilities are encouraged to provide Body Fluid Spills materials in a convenient kit to any staff for cleaning up spills (i.e., bus drivers, teachers, aides, custodians, etc.). The facility should have an Exposure Control Plan, and any employee that provides care for illness and injury should understand actions to take when exposed to blood or body fluids.
9 PLANNING FOR CHILDREN WITH SPECIAL NEEDS Some children in your facility may have special emergency care needs due to their medical conditions or physical abilities. Medical Conditions: Some children may have special conditions that put them at risk for life-threatening emergencies. For example, students who have: Asthma or other breathing difficulties History of life-threatening or severe allergic reactions Diabetes Seizure disorders Technology-dependent or medically fragile conditions Your health consultant along with the child s parent/guardian and personal physician, should develop an individual emergency action plan for these children upon enrollment. The plans should be made available to appropriate staff at all times. In an emergency for this child, refer to this individualized plan (see individual conditions for resources for plans). The American College of Emergency Physicians and the American Academy of Pediatrics have created an Emergency Information Form for Children with Special Needs that is useful in collecting the information needed to develop individualized emergency and health care plans. The form can be downloaded from or Physical Abilities: Other children in your facility may have special emergency needs due to some physical ability. This would include students who are: Deaf Blind In wheel chairs Unable or have difficulty walking up or down stairs, for any reason Temporarily on crutches These children will need special arrangements in the event of a facility-wide emergency (i.e., fire, tornado, evacuation, etc.). These arrangements should be part of the child s individualized healthcare plan. A person should be designated to assist these children to safety. All appropriate staff should be aware of this plan.
10 ALLERGIC REACTION Children with life-threatening allergies should be known to all staff. An emergency action plan should be developed for these children.* Children may experience a delayed allergic reaction up to 2 hours following food ingestion, bee sting, etc. Symptoms of a severe allergic reaction include: Hives all over body Flushed face Dizziness Blueness around mouth, eyes Seizures Difficulty breathing Confusion Drooling or difficulty swallowing Weakness Loss of consciousness Paleness Symptoms of a mild allergic reaction include: Red, watery eyes Itchy, sneezing, runny nose Does the child have symptoms of a severe, allergic reaction? Adult(s) supervising child during normal activities should be aware of the child's exposure and should watch for any delayed symptoms of a severe allergic reaction (see above) for up to 2 hours. If child is so uncomfortable that he/she is unable to participate in regular activities, contact authority & parent/guardian. If available, refer to child's emergency action plan. Administer doctor and parent/guardian-approved medication, if available. CALL EMS. authority & parent/guardian. Look, listen and feel for breath. If child stops breathing, see "CPR" *For sample emergency action plan for severe allergic reactions, see
11 ASTHMA/WHEEZING/DIFFICULTY BREATHING Children with a history of breathing difficulties, including asthma/wheezing, should be known to appropriate staff. An asthma action plan should be developed.* Staff in a position to administer approved medications should receive instruction. A child with asthma/wheezing may have breathing difficulties which include: wheezing - high-pitched sound during breathing out. rapid breathing. flaring (widening) of nostrils. increased use of stomach and chest muscles during breathing. tightness in chest. excessive coughing. not speaking in full sentences If available, refer to child's asthma action plan. Does the child have doctor and parent/guardian approved medication? Administer medication as directed in asthma action plan. Encourage the child to sit quietly, breathe slowly and deeply in through the nose and out through the mouth. Did breathing difficulty develop rapidly? Are the lips, tongue or nail beds turning blue? Are symptoms not improving or getting worse? authority & parent/guardian. CALL EMS. *For information regarding Asthma Action Plans and other resources, see Topics A-Z, Asthma, Publications, for Missouri School Asthma Manual.
12 BEHAVIORAL EMERGENCIES Children with a history of behavioral problems, emotional problems or other special needs should be known to appropriate staff. An individualized health care plan should be developed at time of enrollment. Refer to your facility s policy for addressing behavioral emergencies. Behavioral or psychological emergencies may take many forms (e.g. depression, anxiety/panic, phobias, destructive or assaultive behavior, etc.). Intervene only if the situation is safe for you. Does child have visible injuries? See appropriate guideline to provide first aid. CALL EMS if any injuries require immediate care. The cause of unusual behavior may be psychological/emotional or physical (e.g. fever, diabetic emergency, poisoning/overdose, alcohol/drug abuse, head injury, etc.). The child should be seen by a health care provider to determine the cause. authority and parent/ guardian.
13 BITES (HUMAN & ANIMAL) Wear disposable gloves when exposed to blood or other body fluids. Wash the bite area with soap & water. Press firmly with a clean dressing. See "Bleeding". Is child bleeding? Hold under running water for 2-3 minutes. Check child's immunization record for DPT (tetanus). See "Tetanus". Bites from the following animals can carry rabies and may need medical attention: dog opossum bat skunk raccoon fox coyote cat CALL EMS Is bite from an animal or human? ANIMAL If bite is from a snake, hold the bitten area still and below the level of the heart. Call the POISON CONTROL CENTER Is bite large or gaping? Is bleeding uncontrollable? authority & parent/guardian. HUMAN If skin is broken, contact authority & parent/guardian. URGE IMMEDIATE MEDICAL CARE. Parents/guardians of the child who was bitten and the child who was biting should be notified that their child may have been exposed to blood from another child. Report bite to proper authorities, usually the health department, so that the animal can be caught & watched for rabies.
14 BLEEDING Wear disposable gloves when exposed to blood or other body fluids. Check child's immunization record for DPT (tetanus). Is injured part amputated (severed)? CALL EMS Press firmly with a clean bandage to stop bleeding. Elevate bleeding body part gently. If fracture is suspected, gently support part and elevate. Bandage wound firmly without interfering with circulation to the body part. DO T USE A TOURNIQUET. Place detached part in a plastic bag. Tie bag. Put bag in a container of ice water. DO T PUT AMPUTATED PART DIRECTLY ON ICE. Send bag to the hospital with child. Is there continued uncontrollable bleeding? CALL EMS If wound is gaping, child may need stitches. authority & parent/ guardian. URGE MEDICAL CARE. authority & parent/guardian. Have child lie down. Elevate child's feet 8-10 inches unless this causes the child pain/discomfort OR a neck/back injury is suspected. Keep child warm but not hot. Cover child with a light blanket or sheet.
15 BLISTERS (FROM FRICTION) Wear disposable gloves when exposed to blood and other body fluids. Wash area with soap and water. Is blister broken? Apply clean dressing and bandage to prevent further rubbing. DO T BREAK BLISTER. Blisters heal best when kept clean and dry. If infection is suspected, contact authority & parent/guardian.
16 BRUISES If child comes to child care with unexplained, unusual or frequent bruising, consider the possibility of child abuse. See "Child Abuse". Is bruise deep in the muscle? Is there rapid swelling? Is child in great pain? Rest injured part. authority & parent/guardian. Apply cold compress or ice bag, covered with a cloth or paper towel, for half an hour. If skin is broken, treat as a cut. See "Cuts, Scratches, & Scrapes".
17 BURNS If child comes to child care with pattern burns (e.g. iron or cigarette shape) or glove-like burns, consider the possibility of child abuse. See "Child Abuse". Always make sure that the situation is safe for you before helping the child so there are not two victims exposed to the source of the burn. ELECTRICAL What type of burn is it? CHEMICAL All electrical burns need medical attention. (See "Electric Shock"). HEAT Flush the burn with large amounts of cool running water or cover it with a clean, cool, wet cloth for at least 15 minutes. DO T USE ICE. Wear gloves and if possible, goggles. Remove child's clothing & jewelry if exposed to chemical. Rinse chemicals off skin, eyes IMMEDIATELY with large amounts of water. See "Eyes" if necessary. Rinse for minutes. Is burn large or deep? Is burn on face or eye? Is child having difficulty breathing? Is child unconscious? Are there other injuries? CALL THE POISON CONTROL CENTER while flushing burn & ask for instructions. Phone # CALL EMS. Cover/wrap burned part loosely with a clean dressing. Check child's immunization record for DPT (tetanus). (See "Tetanus Immunization"). authority & parent/ guardian.
18 GUIDELINES FOR CARDIOPULMONARY RESUSCITATION (CPR) Every facility should have more than one person certified to provide CPR in the event an individual is not breathing and does not appear to have adequate circulation. The names of individuals with current training in CPR should be posted with the emergency information in the facility and by each phone. Certification to provide CPR must be updated on a regular basis. New guidelines issued by the American Heart Association (AHA) in November 2005, stress the importance of quick action by individuals adequately trained in CPR. The new guidelines attempt to minimize the steps and the differences in CPR across age groups, as well as highlight differences between expectations for lay rescuers and health consultants. The goal is to make CPR easier for all rescuers to learn, remember and perform. The age delineations now used for lay rescuers are: Newborn birth until hospital discharge Infant less than one year Child 1-8 years Adult 8 years and older All age groups are recommended for cycles of 30 chest compressions to 2 breaths. The same techniques for chest compression can be used for children and adults (compress the lower half of sternum [nipple line} one-third to one-half depth of chest. Lay rescuers will no longer be taught to assess for pulse or signs of circulation in an unresponsive victim or to do rescue breathing without chest compressions. If a lay rescuer is alone and finds an unresponsive infant or child, the rescuer should attempt to open the airway and give 2 breaths that are sufficient to make the chest rise. Then the rescuer should provide 5 cycles (30 compressions and 2 breaths = a cycle, about 2 minutes) before leaving the victim to call 911. A child is more likely to suffer from asphyxial (respiratory) arrest than heart irregularities, and is more likely to respond to, or benefit from the initial CPR. If a lay rescuer is alone and finds an unresponsive adult, the rescuer should call 911 first. The rescuer should then return to the victim and begin CPR. Training in CPR is readily available. The goal is to increase the number of people learning safe and effective CPR technique and the number of victims of sudden cardiac arrest who will receive good bystander or lay rescuer CPR, resulting in thousands of lives saved. Skills should be taught and practiced in the presence of a trained instructor. BARRIER DEVICES Barrier devices, to prevent the spread of infections from one person to another, can be used when performing CPR. Several different types (e.g., face shields, pocket masks) exist. It is important to practice using these devices in the presence of a trained CPR instructor before attempting to use them in an emergency situation. The length of rescue breaths and the amount of air that you breathe to make the victim s chest rise can be affected by these devices.
19 CHILD ABUSE & NEGLECT Child abuse is a complicated issue with many potential signs. Anyone in a position to care for children should be trained in the recognition of child abuse/neglect. If child has visible injuries, refer to the appropriate guideline to provide first aid. CALL EMS if any injuries require immediate medical care. Teachers and other facility staff are required to report suspected child abuse and neglect to the State Child Abuse Hotline ( ). Refer to your own facility policy for additional guidance on reporting. Abuse may be physical, sexual or emotional in nature. Some signs of abuse follow. This is T a complete list: Depression, hostility, low self-esteem, poor self-image Evidence of repeated injuries or unusual injuries. Lack of explanation or unlikely explanation for an injury. Pattern bruises or marks (e.g. burns in the shape of a cigarette or iron, bruises or welts in the shape of a hand). "Glove-like" or "sock-like" burns. Unusual knowledge of sex, inappropriate touching or engaging in sexual play with other children. Poor hygiene, underfed appearance. Severe injury or illness without medical care. If a child reveals abuse to you: Try to remain calm. Take the child seriously. Tell the child that he/she did the right thing by telling. Let the child know that you are required to report the abuse to Child Protective Services. Do not make promises that you can not keep. Respect the sensitive nature of the child's situation. Follow appropriate reporting procedures. facility authority.
20 CHOKING (FOR CONSCIOUS VICTIMS) Call 911 or activate EMS after starting rescue efforts. INFANTS UNDER ONE YEAR Begin the following if the infant is choking and is unable to breathe. However, if the infant is coughing or crying, DO T do any of the following, but call EMS, try to calm the child and watch for worsening of symptoms. If cough becomes ineffective (loss of sound), begin step 1 below. CHILDREN OVER ONE YEAR OF AGE & ADULTS Begin the following if the child is choking and unable to breathe. However, if the child is coughing, crying or speaking, DO T do any of the following, but call EMS, try to calm the child and watch for worsening of symptoms. If cough becomes ineffective (loss of sound), begin step 1 below. 1. Position the infant, with head slightly lower than chest, face down on your arm and support the head (support jaw; do T compress throat). 2. Give up to 5 back blows with the heel of hand between infant s shoulder blades. 3. If object is not coughed up, position infant face up on your forearm with head slightly lower than rest of body. 4. With 2 or 3 fingers, give up to 5 chest thrusts near center of breastbone, about one finger width below the nipple line. 5. Open mouth and look. If foreign object is seen, sweep it out with finger. 6. Tilt head back and lift chin up and out to open the airway. Try to give 2 breaths. 7. Repeat steps 1-6 until object is coughed up, infant starts to breathe or infant becomes unconscious. 1. Stand or kneel behind child with arms encircling child. 2. Place thumbside of fist against middle of abdomen just above the navel. Do T place your hand over the very bottom of the breastbone. Grasp fist with other hand. 3. Give up to 5 quick inward and upward thrusts. 4. Repeat steps 1-2 until object is coughed up, child starts to breathe or child becomes unconscious. IF CHILD BECOMES UNCONSCIOUS, PLACE ON BACK AND GO TO STEP 6 OF CHILD OR ADULT CPR IN RIGHT COLUMN. FOR OBESE OR PREGNANT PERSONS: Stand behind person and place your arms under the armpits to encircle the chest. Press with quick backward thrusts. IF INFANT BECOMES UNCONSCIOUS, GO TO STEP 6 OF INFANT CPR IN RIGHT COLUMN.
21 COMMUNICABLE DISEASES For more information on protecting yourself from communicable diseases, see "Infection Control". Chicken pox, head lice, pink eye, strep throat and influenza (flu) are just a few of the common communicable diseases that affect children. There are many more. In general, there will be little that you can do for a child who has a communicable disease. Following, are some general guidelines. *Refer to your facility s exclusion policy for ill students. A communicable disease is a disease that can be spread from one person to another. Germs (bacteria, virus, fungus, parasite) cause communicable diseases. SIGNS OF LIFE-THREATENING ILLNESS: Difficulty breathing or swallowing, rapid breathing. Severe coughing, high pitched whistling sound. Blueness in the face. Fever greater than F in combination with lethargy, loss of consciousness, extreme sleepiness, abnormal activity. CALL EMS. authority and parent/guardian. SIGNS OF PROBABLE ILLNESS: Sore throat Redness, swelling, drainage of eye Unusual spots/rash with fever or itching Crusty, bright yellow, gummy skin sores Diarrhea (more than two loose stools a day) Vomiting Yellow skin or yellow "white of eye" Fever greater than F Extreme tiredness or lethargy Unusual behavior authority and parent/ guardian. URGE MEDICAL CARE. SIGNS OF POSSIBLE ILLNESS: Earache Headache Itching of scalp Fussiness Runny nose Mild cough Monitor child for worsening of symptoms. parent/guardian and discuss. *State recommendations for exclusion: Health, School Health, Guidelines, Prevention and Control of Communicable Disease
22 CUTS (small), SCRATCHES & SCRAPES (including rope and floor burns) Wear disposable gloves when exposed to blood or other body fluids. Use wet gauze to wash the wound gently with clean water and soap in order to remove dirt. Is the wound: large? deep? bleeding freely? See "Bleeding". Rinse under running water. Pat dry with clean gauze or paper towel. Apply clean gauze dressing (non-adhering/non-sticking type for scrapes) and bandage. Check child's immunization record for DPT. (See "Tetanus") authority & parent/guardian.
23 DIABETES A child with diabetes should be known to appropriate school staff. A history should be obtained and an emergency action plan* should be developed at time of enrollment. A child with diabetes could have the following symptoms: Irritability and feeling upset Seizure Change in personality Listlessness Sweating and feeling "shaky" Cramping Loss of consciousness Dizziness Confusion or strange behavior Paleness Rapid, deep breathing Rapid pulse If available, refer to child s emergency action plan. Does child have a blood sugar monitor available? Check blood sugar. Is blood sugar less than 60 or LOW according to emergency action plan? OR, Is blood sugar HIGH according to emergency action plan? LOW. Is the child: Unconscious or losing consciousness? Having a seizure? Unable to speak? Having rapid, deep breathing? Follow child s emergency action plan, if available, OR Give the child "SUGAR" such as: Fruit juice or soda pop (not diet) 6-8 ounces Hard candy (6-7 lifesavers or 1/2 candy bar) Sugar (2 packets or 2 teaspoons) Cake decorating gel (1/2 tube) or icing Instant glucose The child should begin to improve within 10 minutes. Continue to watch the child in a quiet place. Re-check blood sugar. Is child improving? HIGH authority & parent/guardian. CALL EMS. If child is unconscious, see "Unconsciousness". *For Diabetes Emergency Action Plans and other resources, see Topics A-Z, Diabetes, Publications, for Diabetes Management in the School setting.
24 DIARRHEA Wear disposable gloves when exposed to blood or other body fluids. A child may be sent to the office because of repeated diarrhea, or after an "accident" in the bathroom. Allow the child to rest if experiencing any stomach pain. Give the child water to drink. authority & parent/guardian and urge medical care if: the child has continued diarrhea (2 or more times). the child has a fever. (See "Fever".) blood is present in the stool. the child is dizzy and pale. the child has severe stomach pain. If the child's clothing is soiled, wear disposable gloves and double-bag the clothing to be sent home. Wash hands thoroughly.
25 EARS DRAINAGE FROM EAR Do T try to clean out ear. authority & parent/ guardian. URGE MEDICAL CARE. EARACHE school authority & parent/guardian. URGE MEDICAL CARE. OBJECT IN EAR CANAL Ask child if he/she knows what is in the ear. If there is no pain, the child may return to class. Notify the parent/guardian. Do you suspect a live insect is in the ear? Gently tilt head toward the affected side. Did object come out on its own? OR T SURE DO T ATTEMPT TO REMOVE. authority & parent/ guardian. URGE MEDICAL CARE. DO T ATTEMPT TO REMOVE OBJECT.
26 ELECTRIC SHOCK If no one else is available to call EMS, perform CPR first for two minutes, and then call EMS yourself. TURN OFF POWER SOURCE, IF POSSIBLE. DO T TOUCH CHILD UNTIL POWER SOURCE IS SHUT OFF. Once power is off and situation is safe, approach. the child and ask, "Are you okay?" Is child unconscious or unresponsive? Send someone to CALL EMS. Treat any burns. See "Burns". Keep airway clear. Look, listen & feel for breath. If child is not breathing, see "CPR". authority & parent/guardian. URGE MEDICAL CARE. authority & parent/guardian.
27 E EYE INJURY: Keep the child lying flat and quiet. Is injury severe? Is there a change in vision? Has object penetrated eye? If an object has penetrated the eye, DO T REMOVE OBJECT. authority & parent/ guardian. URGE IMMEDIATE MEDICAL CARE. Cover eye with a paper cup or similar object to keep child from rubbing, BUT DO T TOUCH EYE OR PUT ANY PRESSURE ON EYE. CALL EMS. authority and parent/guardian. ("E" continued on next page.)
28 E (continued from previous page) PARTICLE IN EYE: Keep child from rubbing eye. If necessary, lay child down, & tip head toward affected side. Gently pour tap water over the open eye to flush out the particle. If particle does not flush out of eye or if eye pain continues, contact authority and parent/ guardian. URGE MEDICAL CARE. CHEMICALS IN EYE Wear gloves and if possible, goggles. Immediately flush the eye with large amounts of clean water for 20 to 30 minutes. Tip the head so that the affected eye is below the unaffected eye and water washes eye from nose out to side of the face. CALL NEAREST POISON CONTROL CENTER while flushing eye. Phone # Follow instructions. authority and parent/guardian. If eye has been burned by chemical, CALL EMS.
29 FAINTING If you observe any of the following signs of fainting, have the child lie down to prevent injury from falling: Extreme weakness or fatigue Dizziness or light-headedness Extreme sleepiness Pale, sweaty skin Nausea Fainting may have many causes including: injuries, blood loss, poisoning, severe allergic or diabetic reaction, heat exhaustion, illness, fatigue, stress, not eating, standing still for too long, etc. If you know the cause of the fainting, see the appropriate guideline. Most children who faint will recover quickly when lying down. If the child does not regain consciousness immediately, see "Unconsciousness". OR T SURE Is fainting due to injury? Did child injure self when he/she fainted? Treat as possible neck injury. See "Neck & Back Pain". DO T MOVE CHILD. Keep child in flat position. Elevate feet. Loosen clothing around neck and waist. Keep airway clear and monitor breathing. Keep child warm, but not hot. Control bleeding if needed (wear disposable gloves). Give nothing by mouth. Keep child lying down. authority & parent/guardian. URGE MEDICAL CARE. authority & parent/ guardian. Are symptoms (dizziness, light-headedness, weakness, fatigue, etc.) still present? If child feels better, and there is no danger of neck injury, he/she may be moved to a quiet, private area.
30 FEVER & T FEELING WELL Fever may be first sign of a communicable disease. Look for other signs of illness. Take the child s temperature, if possible. Note temperature over F as fever. Have the child lie down in a room which affords privacy. Give no medication, unless previously authorized. Exclude from facility per health policy. authority and parent/ guardian.
31 FRACTURES, DISLOCATIONS, SPRAINS, OR STRAINS child Leave child in a position Can child move or put weight on authority and parent/guardian. child to return to classroom. authority & parent/guardian.
32 FROSTBITE Frostbite can result in the same type of tissue damage as a burn. It is a serious condition and requires medical attention. Exposure to cold even for short periods of time may cause "HYPOTHERMIA" in children (See Hypothermia). The nose, ears, chin, cheeks, fingers and toes are the parts most often affected by frostbite. Frostbitten skin may: Look discolored (flushed, grayish-yellow, pale, white). Feel cold to the touch. Feel numb to the child. Deeply frostbitten skin may Look white or waxy Feel firm - hard (frozen) Take the child to a warm place. Remove cold or wet clothing and give child warm, dry clothes. Protect cold part from further injury. Do T rub or massage the cold part OR apply heat such as a water bottle or hot running water. Cover part loosely with nonstick, sterile dressings or dry blanket. Does extremity/part: Look discolored - grayish, white or waxy? Feel firm-hard (frozen)? Have a loss of sensation? CALL EMS. Keep child warm and affected part covered. Keep child and affected body part warm. authority & parent/ guardian. Encourage medical care.
33 HEADACHE Have child lie down for a short time in a room which affords privacy. Has a head injury occurred? See "Head Injuries" Give no medication unless previously authorized. Apply a cold cloth or compress to the child's head. Is headache severe? Are other symptoms, such as vomiting, fever (See "Fever"), blurred vision or dizziness present? If headache persists, contact parent/ guardian. parent/ guardian. URGE MEDICAL CARE.
34 HEAD INJURIES Many head injuries that happen in early childhood are minor. Head wounds may bleed easily and form large bumps. Bumps to the head may not be serious. Head injuries from falls, activities and violence may be serious. If head is bleeding, see "Bleeding". Have child rest, lying flat. Keep child quiet & warm. If child only bumped head and does not have any other complaints or symptoms, see "Bruises". With a head injury (other than head bump), always suspect neck injury as well. Do T move or twist the spine or neck. See "Neck & Back Injuries" for more information. Is child vomiting? Turn the head and body together to the side, keeping the head and neck in a straight line with the trunk. Watch child closely. DO T LEAVE CHILD ALONE. CALL EMS. Look, listen & feel for breathing. If child stops breathing, see "CPR". Give nothing by mouth. authority & parent/ guardian. Are any of the following symptoms present: Unconsciousness? Seizure? Neck pain? Child is unable to respond to simple commands? Blood or watery fluid in the ears? Child is unable to move or feel arms or legs? Blood is flowing freely from the head? Child is sleepy or confused? Abnormal speech or behavior? Even if child was only briefly confused & seems fully recovered, contact authority & parent/ guardian. URGE MEDICAL CARE. Watch for delayed symptoms.
35 HEAT STROKE/HEAT EXHAUSTION Heat emergencies are caused by spending too much time in the heat. Heat emergencies can be life-threatening situations. Strenuous activity in the heat may cause heat-related illness. Symptoms may include: red, hot, dry skin weakness and fatigue cool, clammy hands vomiting loss of consciousness profuse sweating headache nausea confusion muscle cramping Remove child from the heat to a cooler place. Have the child lie down. Is child unconscious or losing consciousness? Are any of the following happening: hot, dry red skin? vomiting? confusion? Quickly remove child from heat to a to a cooler place. Put child on his/her side to protect the airway. Look, listen and feel for breathing. If child is not breathing, see "CPR". Give clear fluids such as water, 7-up or Gatorade frequently in small amounts if child is fully awake and alert. Cool rapidly by completely wetting clothing with room temperature water. DO T USE ICE WATER. authority & parent/guardian. CALL EMS. authority & parent/guardian.
36 HYPOTHERMIA (EXPOSURE TO COLD) Hypothermia happens after exposure to cold when the body is no longer capable of warming itself. Young children are particularly susceptible to hypothermia. It can be a life-threatening condition if left untreated for too long. Hypothermia can occur after a child has been outside in the cold or in cold water. Symptoms may include: confusion shivering weakness sleepiness blurry vision white or grayish skin color slurred speech impaired judgment Take the child to a warm place. Remove cold or wet clothing and wrap child in a warm, dry blanket. Continue to warm child with blankets. If child is fully awake and alert, offer warm (T HOT) fluids, but no food. Does child have: Loss of consciousness? Slowed breathing? Confused or slurred speech? White, grayish or blue skin? authority & parent/guardian. Encourage medical care. CALL EMS. Give nothing by mouth. Continue to warm child with blankets. If child is sleepy or losing consciousness, place the child on his/her side to protect the airway. Look, listen and feel for breathing. If child stops breathing, see CPR.
37 NECK & BACK INJURIES Suspect a neck/back injury if pain results from: Falls over 10 feet or falling on head Being thrown from a moving object Sports Violence Being struck by a car or other fast moving object Has an injury occurred? A stiff or sore neck from sleeping in a "funny" position is different than neck pain from a sudden injury. Non-injured stiff necks may be uncomfortable but they are not emergencies. Did child walk in or was child found lying down? LYING DOWN DO T MOVE CHILD unless there is IMMEDIATE danger of further physical harm. If child MUST be moved, support head and neck and move child in the direction of the head without bending the spine forward. Do T drag the child sideways. WALKING If child is so uncomfortable that he or she is unable to participate in normal activities, contact authority & parent/ guardian. Have child lie down on his/her back. Support head by holding it in a "face forward" position. TRY T TO MOVE NECK OR HEAD. Keep child quiet and warm Hold the head still by gently placing one of your hands on each side of the head OR Place rolled up towels/clothing on both sides of head so it will not move CALL EMS. authority & parent/guardian.
38 SE SEBLEED See "Head Injuries" if you suspect a head injury other than a nose bleed or broken nose. Wear disposable gloves when exposed to blood or other body fluids. Place child sitting comfortably with head slightly forward or lying on side with head raised on pillow. Encourage mouth breathing and discourage nose blowing, repeated wiping or rubbing. If blood is flowing freely from the nose, provide constant uninterrupted pressure by pressing the nostrils firmly together for about 15 minutes. Apply ice to nose. If blood is still flowing freely after applying pressure and ice, contact authority & parent/guardian. BROKEN SE Care for nose as in "Nosebleed" above. authority and parent/ guardian. URGE MEDICAL CARE. ("SE" continued on next page.)
39 SE (continued from previous page) OBJECT IN SE Is object: large? puncturing nose? deeply imbedded? OR T SURE DO T ATTEMPT TO REMOVE. See "Puncture Wounds" if object has punctured nose. Have child hold the clear nostril closed while gently blowing nose. Did object come out on own? authority & parent/ guardian. URGE MEDICAL CARE. If there is no pain, child may return to classroom. Notify parent/ guardian. If object cannot be removed easily, DO T ATTEMPT TO REMOVE.
40 POISONING & OVERDOSE substance in child s mouth Check child s mouth. child. What the child swallowed or If child becomes unconscious, authority & parent/guardian. the child.
41 PUNCTURE WOUNDS Wear disposable gloves when exposed to blood or other body fluids. Has eye been wounded? See "Eyes - Eye Injuries" DO T TOUCH EYE. Is object still stuck in wound? DO T REMOVE OBJECT. Wrap bulky dressing around object to support it. Try to calm the child. DO T TRY TO PROBE OR SQUEEZE. Wash the wound gently with soap and water. Check to make sure the object left nothing in the wound (e.g. pencil lead). Cover with a clean bandage. If wound is deep or bleeding freely, treat as bleeding. (See "Bleeding") Is object large? Is wound deep? Is wound bleeding freely or squirting blood? Check child's immunization record for DPT (tetanus). See "Tetanus Immunization". CALL EMS. If wound is deep or bleeding freely, treat as bleeding. (See "Bleeding") authority & parent/guardian.
42 RASHES Rashes may have many causes, including heat, infection, illness, reaction to medications, allergic reactions, insect bites, dry skin or skin irritations. Some rashes may be contagious (pass from one person to another). Wear disposable gloves to protect self when in contact with any rash. Rashes include such things as: Hives Red spots (large or small, flat or raised) Purple spots Small blisters CALL EMS. authority and parent/ guardian. See "Allergic Reaction" and "Communicable Disease" for more information. Other symptoms may indicate whether the child needs medical care. Does child have: Loss of consciousness? Difficulty breathing or swallowing? Purple spots? If the following symptoms are present, contact authority & parent/ guardian. URGE MEDICAL CARE. Fever (See "Fever"). Headache Diarrhea Sore throat Vomiting Rash is bright red and sore to the touch. Rash (hives) is all over body. Child is so uncomfortable (e.g. itchy, sore, feels ill) that he/she is not able to participate in regular activities.
43 SEIZURES Seizures may be any of the following: Episodes of staring with loss of eye contact. Staring involving twitching of the arm and leg muscles. Generalized jerking movements of the arms and legs. Unusual behavior for that person. (e.g. running, belligerence, making strange sounds, etc.) If available, refer to child s emergency action plan.* A child with a history of seizures should be known to appropriate staff. An emergency action plan should be developed containing a description of the onset, type, duration and aftereffects of the seizures. If child seems off balance, place him/her on the floor (on a mat) for observation & safety. DO T RESTRAIN MOVEMENTS. Move surrounding objects to avoid injury. DO T PLACE ANYTHING BETWEEN THE TEETH or give anything by mouth. Observe details of the seizure for parent/guardian, emergency personnel or physician. Note: Duration Kind of movement or behavior Body parts involved Loss of consciousness, etc. After seizure, keep airway clear by placing child on his/her side. A pillow should not be used. Seizures are often followed by sleep. The child may also be confused. This may last from 15 minutes to an hour or more. After the sleeping period, the child should be encouraged to participate in all normal classroom activities. Is child having a seizure lasting longer than 5 minutes? Is child having seizures following one another at short intervals? Is child without a known history of seizures, having a seizure? Is child having any breathing difficulties after the seizure? CALL EMS. authority & parent/ guardian. *For resources regarding emergency action plans for a child with a seizure disorder, go to then click on Programs, then School Nurse Training, then Seizure Action Plans.
44 SPLINTERS OR IMBEDDED PENCIL LEAD Wear disposable gloves when exposed to blood or other body fluids. Check child's immunization record for DPT (tetanus). See "Tetanus Immunization". Gently wash area with clean water and soap. Is splinter or lead: protruding above the surface of the skin? small? shallow? Leave in place. DO T PROBE UNDER SKIN. Remove with tweezers unless this causes the child pain. DO T PROBE UNDER SKIN. authority & parent/ guardian. ENCOURAGE MEDICAL CARE. Were you successful in removing the entire splinter/pencil lead? Wash again. Apply clean dressing.
45 STABBING & GUNSHOT INJURIES Refer to your facility's policy for handling violent incidents. CALL EMS for injured person. Call the police. Intervene only if the situation is safe for you to approach. Wear disposable gloves when exposed to blood or other body fluids. Open the person s airway and look, listen and feel for breathing. (see "CPR"). Is the person: losing consciousness? having difficulty breathing? bleeding uncontrollably? Lie person down if he/she is not already doing so. Elevate feet 8-10 inches. Press wound firmly with a clean bandage to stop bleeding. Elevate injured part gently if possible. Cover with a blanket or sheet. authority & parent/ guardian.
46 STINGS Children with a history of allergy to stings should be known to all staff. An emergency action plan should be developed.* If available, follow child's emergency action plan. * Does child have: difficulty breathing? a rapidly expanding area of swelling, especially of the lips, mouth or tongue? a history of allergy to stings? A child may have a delayed allergic reaction up to 2 hours after the sting. Adult(s) supervising child during normal activities should be aware of the sting and should watch for any delayed reaction. If available, administer doctor and parent/guardian-approved medications. To remove stinger (if present) scrape area with a card. DO T SQUEEZE. Wash area with soap and water. Apply cold compress. Look, listen and feel for breathing. If child stops breathing, see "CPR". CALL EMS. authority & parent/ guardian. See "Allergic Reaction". *For sample emergency action plan, see
47 STOMACHACHES/PAIN Stomachaches may have many causes including: Illness Food Poisoning Hunger Psychological Issues Overeating Constipation Diarrhea Gas Pain Have the child lie down in a room which affords privacy. Has an injury occurred? authority and parent/guardian. URGE MEDICAL CARE. Take the child's temperature. Note temperature over F as fever. (See "Fever".) Does child have: Fever? Severe stomach pains? Vomiting? Allow child to rest minutes. Allow child to return to classroom. Does child feel better? If stomachache persists or becomes worse, contact authority & parent/ guardian.
48 TEETH BLEEDING GUMS Generally related to chronic infection. Presents some threat to child's general health. No first aid measure will be of any significant value. Urge parent/ guardian to obtain dental care. TOOTHACHE OR GUM BOIL For tongue, cheek, lip, jaw or other mouth injury not involving the teeth, refer to "Mouth & Jaw". These conditions can be direct threats to a child's general health, not just local tooth problems! No first aid measure will be of any significant value. Relief of pain in the child care setting often postpones dental care. Do T place pain relievers (e.g. Aspirin, Tylenol) on the gum tissue of the aching tooth. THEY CAN BURN TISSUE! authority and parent/guardian. URGE DENTAL CARE. ("TEETH" continued on next page)
49 TEETH (continued from previous page) DISPLACED TOOTH Do T try to move tooth into correct position. authority and parent/guardian. OBTAIN EMERGENCY DENTAL CARE. KCKED-OUT OR BROKEN PERMANENT TOOTH Find tooth. Do T handle tooth by the root. If tooth is dirty, clean gently by rinsing with water. DO T SCRUB THE KCKED-OUT TOOTH. The following steps are listed in order of preference. If permanent tooth (within minutes): 1. place gently back in socket and have child hold it in place; OR. 2. place in glass of skim or low fat milk. OR 3. place in normal saline. OR 4. have child spit in cup and place tooth in it. OR 5. place in glass of water. TOOTH MUST T DRY OUT. authority & parent/ guardian. OBTAIN EMERGENCY DENTAL CARE. THE CHILD SHOULD BE SEEN BY A DENTIST WITHIN 60 MINUTES. Apply a cold compress to face to minimize swelling.
50 TETANUS IMMUNIZATION Protection against tetanus should be considered with any wound, even a minor one. After any wound, check the child's immunization record for DPT (tetanus) and notify parent/guardian. It is helpful to provide EMS personnel with the dates of the child s DPT immunizations.
51 TICKS Children should be inspected for ticks after time in woods or brush. Ticks may carry serious infections and must be completely removed. Do T handle ticks with bare hands. Refer to your facility's policy regarding the removal of ticks. Wear disposable gloves when exposed to blood and other body fluids. Wash the tick area gently with soap and water before attempting removal. Using a tweezer, grasp the tick as close to the skin surface as possible and pull upward with steady, even pressure. Do T twist or jerk the tick as this may cause the mouth parts to break off. It is important to remove the ENTIRE tick. Take care not to squeeze, crush, or puncture the body of the tick as its fluids may carry infection. After removal, wash the tick area thoroughly with soap and water. Wash your hands. Apply a sterile adhesive or Band-Aid type dressing. Ticks can be safely thrown away by placing them in container of alcohol or flushing them down the toilet. parent/guardian.
52 UNCONSCIOUSNESS If child stops breathing, and no one else is available to call EMS, provide two minutes of initial CPR before leaving student to call EMS. Unconsciousness may have many causes including: injuries, blood loss, poisoning, severe allergic reaction, diabetic reaction, heat exhaustion, illness, fatigue, stress, not eating, etc. If you know the cause of the unconsciousness, see the appropriate guideline. See "Fainting". Did child regain consciousness immediately? OR T SURE Is unconsciousness due to injury? Treat as possible neck injury. See "Neck & Back Injuries Guideline. DO T MOVE CHILD. Keep child in flat position. Elevate feet. Loosen clothing around neck and waist. Open AIRWAY with head tilt/chin lift or jaw thrust. Look, listen and feel for BREATHING. Is child BREATHING? CALL EMS. Keep child warm, but not hot. Control bleeding if needed (always wear gloves). Give nothing by mouth. Examine child from head-to-toe and give firstaid for specific conditions. authority and parent/guardian. See "CPR" CALL EMS.
53 VOMITING If a number of children or staff become ill with the same symptoms, suspect food poisoning. CALL THE POISON CONTROL CENTER & ask for instructions. (See "Poisoning".) Notify public health officials (usually the health department). Vomiting may have many causes including: Illness Injury Food poisoning Heat exhaustion Over exertion If you know the cause of the vomiting, see the appropriate guideline. Wear disposable gloves when exposed to blood and other body fluids. Apply a cool, damp cloth to child's face or forehead. Have a bucket available. Have child lie down on his/her side in a room which affords privacy. Give no food or medications. Offer ice chips or small sips of clear fluids containing sugar (such as 7-Up or Gatorade),. if the child is thirsty. authority and parent/guardian. URGE MEDICAL CARE.
54 RECOMMENDED FIRST AID EQUIPMENT AND SUPPLIES Current American Red Cross First Aid Manual or equivalent guidelines Covered waste receptacle with disposable liners Sink with running water Cot with waterproof cover Washable blankets, pillows, pillow cases (disposable covers are available) Wash cloths, hand towels, portable basin, emesis basins Bandage scissors, tweezers Digital or electronic thermometers with disposable thermometer covers or single-use thermometers Hot water bottle (heating pads not recommended) Disposable supplies: Sterile cotton tipped applicators, individually packaged Sterile adhesive bandages, individually packaged Cotton balls Sterile gauze squares (2 x 2 ; 3 x 3 ), individually packaged Adhesive tape (1 tape), paper tape recommended Gauze roller bandage (1 and 2 widths) Cold packs or compresses Triangular bandage for sling Tongue blades, individually wrapped 70% Isopropyl alcohol for use with thermometer Safety pins Liquid soap Paper towels Disposable facial tissues Eye wash bottle Disposable gloves (latex or vinyl, if latex allergy is possible) Bleach for cleaning solutions and sprays (mix 1:100 with water) Splints, long and short Pocket mask/fact shield for CPR Flashlight with spare bulb and batteries One ounce emergency supply of Ipecac (dated) to be used only under the direction of the Poison Control Center
55 EMERGENCY PHONE NUMBERS Complete this page as soon as possible and update as needed. Copy and post near all phones. Each building/facility should update this information at least annually. EMERGENCY PHONE NUMBERS: 911 or Name of Emergency Medical Service: Average emergency response time to your building/facility: Directions to your building/facility: BE PREPARED TO GIVE THE FOLLOWING INFORMATION & DO T HANG UP BEFORE THE OTHER PERSON HANGS UP! Name and facility name Nature of emergency Facility telephone number Address and easy directions, including best entrance to use Exact location of injured person (e.g., behind building in parking lot) Type of injury/condition suspected (e.g., head or neck injury, shock, etc.) Help already given to victim (e.g., epinephrine, CPR, etc.) Ways to find the entrance easily (someone standing out front, flag pole, etc.) OTHER IMPORTANT PHONE NUMBERS Health Consultant Responsible Administrator Poison Control Center Emergency/Disease Reporting Fire Department 911 or Police 911 or Hospital or Nearest Emergency Facility County Family Services Division/Child Protective Services Local Health Agency Child Abuse Hotline Sexual Assault Hotline Domestic Violence Hotline Other
56 1. Create a plan EMERGENCIES HAPPEN Being Prepared Saves Lives 3 Steps to Prepare for an Emergency Families may not be together when emergencies strike. Make sure to have current contact information on file for parents or guardians of individuals in your care. Be sure to obtain doctor s names, health insurance and any special medical information. It is also a good idea to collect contact information of a nearest relative in the event the parent or guardian is unavailable. Families should plan how they will stay in contact if they are separated by a disaster. They should choose two meeting places, a reunion location should be a safe distance from their home and an alternative location should be a place outside their neighborhood. They should also choose an out-of-town friend or family member as a contact for everyone to call. Designating a safe room in their home if they must stay for several days is also recommended. Families should also designate a place where their family will be able to stay for a few days in case they are asked to evacuate. Family members should know and discuss these plans. 2. Prepare an emergency kit The following items should be part of an emergency kit and kept in a container that can be easily carried. Consider placing an emergency kit in each room of your facility. Prescription medicine Clean clothes and sturdy shoes Extra credit card Extra money Sturdy trash bags Formula and baby food if there is an infant in your home Flashlight Bottled water (One gallon of water per person per day, to last three days.) Canned or dried food (A three-day supply of non-perishable food items for each person. Remember a manual can opener.) Battery-powered radio Extra batteries for radio and flashlight First-aid kit 3. Listen for information Listen for information about what to do and where to go during an emergency. City, county, and state officials have developed emergency plans. During an emergency, it is important to follow their instructions and advice.
EMERGENCY GUIDELINES FOR SCHOOLS AND CHILD CARE FACILITIES
 EMERGENCY GUIDELINES FOR SCHOOLS AND CHILD CARE FACILITIES Guidelines for helping an ill or injured child when a health professional is not available. Missouri Department of Health and Senior Services,
EMERGENCY GUIDELINES FOR SCHOOLS AND CHILD CARE FACILITIES Guidelines for helping an ill or injured child when a health professional is not available. Missouri Department of Health and Senior Services,
5420-R STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods
 STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods EMERGENCY PROCEDURES Contact parents and cooperate with them in
STUDENT HEALTH SERVICES REGULATION NORTH COLONIE CENTRAL SCHOOLS NEWTONVILLE, NEW YORK Emergency Procedures and Approved First Aid Methods EMERGENCY PROCEDURES Contact parents and cooperate with them in
Emergency Healthcare Guidelines For School Districts
 Emergency Healthcare Guidelines For School Districts EMERGENCY HEALTHCARE GUIDELINES FOR SCHOOL DISTRICTS Special Recognition: Ohio Department of Public Safety, Division of EMS, EMS for Children Program
Emergency Healthcare Guidelines For School Districts EMERGENCY HEALTHCARE GUIDELINES FOR SCHOOL DISTRICTS Special Recognition: Ohio Department of Public Safety, Division of EMS, EMS for Children Program
First Aid Multiple Choice Test
 First Aid Multiple Choice Test Answer all 25 questions by circling the correct answer. This is an open-book test. Answers are contained in The Boy Scout Handbook. Patrol Troop 1. When making a 911 call,
First Aid Multiple Choice Test Answer all 25 questions by circling the correct answer. This is an open-book test. Answers are contained in The Boy Scout Handbook. Patrol Troop 1. When making a 911 call,
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Pesticide Harmful Effects And Emergency Response
 Pesticide Harmful Effects And Emergency Response Most pesticides are designed to harm or kill pests. Because some pests have systems similar to the human system, some pesticides also can harm or kill humans.
Pesticide Harmful Effects And Emergency Response Most pesticides are designed to harm or kill pests. Because some pests have systems similar to the human system, some pesticides also can harm or kill humans.
NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF EMERGENCY MEDICAL SERVICES
 NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF EMERGENCY MEDICAL SERVICES TRAINING PROGRAM OUTLINE FOR UNLICENSED OR UNCERTIFIED PERSONNEL TO ADMINISTER EPINEPHRINE BY AUTO-INJECTOR IN LIFE-THREATENING
NEW YORK STATE DEPARTMENT OF HEALTH BUREAU OF EMERGENCY MEDICAL SERVICES TRAINING PROGRAM OUTLINE FOR UNLICENSED OR UNCERTIFIED PERSONNEL TO ADMINISTER EPINEPHRINE BY AUTO-INJECTOR IN LIFE-THREATENING
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector
 OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK TO WRIST
 GRIT IN EYE BROKEN LEG BONE WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK HEART ATTACK SUFFERING FROM SHOCK CHOKING SEVERE BLEEDING TO WRIST HYPOTHERMIA ANGINA Localised
GRIT IN EYE BROKEN LEG BONE WET, COUGHING AND COLD NEAR RIVER BANK STUNG BY BEE CAUSING ANAPHYLACTIC SHOCK HEART ATTACK SUFFERING FROM SHOCK CHOKING SEVERE BLEEDING TO WRIST HYPOTHERMIA ANGINA Localised
LEGAL PROTECTION. Good Samaritan Law RCW 4.24.300
 GOALS This course is designed to instruct coach very basic first aid techniques to protect the players under your guidance. This presentation only provides a brief overview of the issues that you may face
GOALS This course is designed to instruct coach very basic first aid techniques to protect the players under your guidance. This presentation only provides a brief overview of the issues that you may face
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
EMERGENCY NURSING SERVICES GUIDELINES
 MONONA GROVE SCHOOL DISTRICT Board Rule 453.1 EMERGENCY NURSING SERVICES GUIDELINES A. School Nurse Certification and Duties 1. The name and educational preparation of the School Nurse shall be provided
MONONA GROVE SCHOOL DISTRICT Board Rule 453.1 EMERGENCY NURSING SERVICES GUIDELINES A. School Nurse Certification and Duties 1. The name and educational preparation of the School Nurse shall be provided
12/5/2012. Introduction. Head, Neck, and Spine Injuries. Recognizing and Caring for Serious Head, Neck and Back Injuries
 Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
MRSA. Living with. Acknowledgements. (Methicillin-Resistant Staphylococcus aureus)
 How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
Guide for Emergency Care in Maryland Schools
 Guide for Emergency Care in Maryland Schools The Guide for Emergency Care in Maryland Schools was developed by the guidelines committee of the Maryland State School Health Council. It reflects input from
Guide for Emergency Care in Maryland Schools The Guide for Emergency Care in Maryland Schools was developed by the guidelines committee of the Maryland State School Health Council. It reflects input from
MRC Medical Jeopardy Feud List of Treatments for Possible Injuries/Conditions
 List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
List of Treatments for Possible Injuries/Conditions A. Apply cold compresses to affected area; elevate the area to reduce swelling and possible bleeding B. Apply direct pressure to wound area with sterile
What Is. Norovirus? Learning how to control the spread of norovirus. Web Sites
 Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
EMERGENCY TREATMENT OF ANAPHYLAXIS EPINEPHRINE AUTO-INJECTOR
 I. GENERAL GUIDELINES EMERGENCY TREATMENT OF ANAPHYLAXIS EPINEPHRINE AUTO-INJECTOR A. PURPOSE To counteract a severe allergic reaction (anaphylaxis) to a foreign substance as prescribed by the licensed
I. GENERAL GUIDELINES EMERGENCY TREATMENT OF ANAPHYLAXIS EPINEPHRINE AUTO-INJECTOR A. PURPOSE To counteract a severe allergic reaction (anaphylaxis) to a foreign substance as prescribed by the licensed
How To Care For A Sick Person
 39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. Medicines are often not necessary. But good care is always important. The
39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. Medicines are often not necessary. But good care is always important. The
BROCKTON AREA MULTI-SERVICES, INC. MEDICAL PROCEDURE GUIDE. Date(s) Reviewed/Revised:
 Page 1 of 5 PROCEDURE FOR: MAP-certified staff and RN/LPN MAP-certified staff are to be trained in the use of epinephrine administration via pre-filled autoinjector devices(s) annually. Certified staff
Page 1 of 5 PROCEDURE FOR: MAP-certified staff and RN/LPN MAP-certified staff are to be trained in the use of epinephrine administration via pre-filled autoinjector devices(s) annually. Certified staff
American Red Cross First Aid EXAMPLE ANSWER SHEET
 American Red Cross First Aid Exam A IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed
American Red Cross First Aid Exam A IMPORTANT: Read all instructions before beginning the exam. INSTRUCTIONS: Do not write on this exam. Mark all answers in pencil on the separate answer sheet as directed
FIRST AID FOR BASEBALL COACHES
 FIRST AID FOR BASEBALL COACHES Liability Issues. Do the right thing State provides qualified immunity Chapter 258 C, Section 13. Good Samaritan Law: No person who, in good faith, provides or obtains, or
FIRST AID FOR BASEBALL COACHES Liability Issues. Do the right thing State provides qualified immunity Chapter 258 C, Section 13. Good Samaritan Law: No person who, in good faith, provides or obtains, or
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Basic First Aid for the Community and Workplace
 A M E R I C A N S A F E T Y & H E A LT H I N S T I T U T E Basic First Aid for the Community and Workplace Student Handbook This handbook serves as a reference guide for basic first aid. For the purpose
A M E R I C A N S A F E T Y & H E A LT H I N S T I T U T E Basic First Aid for the Community and Workplace Student Handbook This handbook serves as a reference guide for basic first aid. For the purpose
Living with MRSA. Things to remember about living with MRSA: This is really serious. I need to do something about this now!
 Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Taking Out a Tooth. Before You Begin: Ask Questions! CHAPTER11
 159 CHAPTER11 Taking Out a Tooth Not every painful tooth needs to come out. You must decide how serious the problem is, and then decide if you can treat and save the tooth. Some problems such as root canal
159 CHAPTER11 Taking Out a Tooth Not every painful tooth needs to come out. You must decide how serious the problem is, and then decide if you can treat and save the tooth. Some problems such as root canal
How to Respond: Injury and Illness at School. DOH Pub #: 130-021
 P r i n t i n g S p e c i f i c a t i o n s Publication: How to Respond: Injury and Illness at School DOH Pub #: 130-021 Printing instructions: To print this publication as a booklet from a desktop printer,
P r i n t i n g S p e c i f i c a t i o n s Publication: How to Respond: Injury and Illness at School DOH Pub #: 130-021 Printing instructions: To print this publication as a booklet from a desktop printer,
Guidelines for Hand Foot and Mouth Disease HFMD
 Guidelines for Hand Foot and Mouth Disease HFMD Hand, foot, and mouth disease, or HFMD, is a contagious illness caused by different viruses. Infants and children younger than 5 years are more likely to
Guidelines for Hand Foot and Mouth Disease HFMD Hand, foot, and mouth disease, or HFMD, is a contagious illness caused by different viruses. Infants and children younger than 5 years are more likely to
& WHEN SHOULD I WORRY?
 WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
Facial Sports Injuries
 Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Facial Sports Injuries Playing catch, shooting hoops, bicycling on a scenic path or just kicking around a soccer ball have more in common than you may think. On the up side, these activities are good exercise
Learning About MRSA. 6 How is MRSA treated? 7 When should I seek medical care?
 IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
FIRST AID TEST. 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988. www.schoolbusing.com. Revised April 21, 2008 - 1 -
 FIRST AID TEST 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988 www.schoolbusing.com Revised April 21, 2008-1 - West County Transportation Agency This test was developed to help school bus driver
FIRST AID TEST 367 West Robles Ave Santa Rosa, CA 95407 707-206-9988 www.schoolbusing.com Revised April 21, 2008-1 - West County Transportation Agency This test was developed to help school bus driver
EXTREME HEAT/HUMIDEX ADVISORY FACT SHEET
 EXTREME HEAT/HUMIDEX ADVISORY FACT SHEET While it is important to enjoy the outdoors during Canadian summers, it is also essential to keep in mind that periods of extreme heat and humidex events may cause
EXTREME HEAT/HUMIDEX ADVISORY FACT SHEET While it is important to enjoy the outdoors during Canadian summers, it is also essential to keep in mind that periods of extreme heat and humidex events may cause
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
A Trip to the. Emergency Room. Help Us Help You
 A Trip to the Emergency Room Help Us Help You No one plans to have a medical emergency however there are things that you can do ahead of time to help make the process easier and faster once you arrive
A Trip to the Emergency Room Help Us Help You No one plans to have a medical emergency however there are things that you can do ahead of time to help make the process easier and faster once you arrive
American Red Cross Advisory Council on First Aid, Aquatics, Safety and Preparedness
 Copyright 2008 by The American National Red Cross All rights reserved. No part of this publication may be reproduced; stored in a retrieval system; or transmitted, in any form or by any means, electronic,
Copyright 2008 by The American National Red Cross All rights reserved. No part of this publication may be reproduced; stored in a retrieval system; or transmitted, in any form or by any means, electronic,
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
TakE Care in Hot & Cold Weather
 www.coned.com TakE Care in Hot & Cold Weather Preventing Hyperthermia and Hypothermia When it s Too Hot! Beating the heat is as much a part of summer as baseball and hot dogs. City residents are particularly
www.coned.com TakE Care in Hot & Cold Weather Preventing Hyperthermia and Hypothermia When it s Too Hot! Beating the heat is as much a part of summer as baseball and hot dogs. City residents are particularly
Types of electrical injuries
 Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
For the Patient: Dasatinib Other names: SPRYCEL
 For the Patient: Dasatinib Other names: SPRYCEL Dasatinib (da sa' ti nib) is a drug that is used to treat many types of cancer. It is a tablet that you take by mouth. Tell your doctor if you have ever
For the Patient: Dasatinib Other names: SPRYCEL Dasatinib (da sa' ti nib) is a drug that is used to treat many types of cancer. It is a tablet that you take by mouth. Tell your doctor if you have ever
2 CHECKING AN INJURED OR ILL ATHLETE
 American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
Emergency Care for Patients of The James
 PATIENT EDUCATION patienteducation.osumc.edu Emergency Care for Patients of The James Emergency Care During and After Treatment Here are guidelines about when and how to report problems that you may have
PATIENT EDUCATION patienteducation.osumc.edu Emergency Care for Patients of The James Emergency Care During and After Treatment Here are guidelines about when and how to report problems that you may have
HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS
 HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS TABLE OF CONTENTS 1.0 Purpose... 1 2.0 Heat Illness Prevention... 2 2.1 Heat Stroke... 2 2.2 Heat Exhaustion... 2 2.3 Heat Cramps...
HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS TABLE OF CONTENTS 1.0 Purpose... 1 2.0 Heat Illness Prevention... 2 2.1 Heat Stroke... 2 2.2 Heat Exhaustion... 2 2.3 Heat Cramps...
Emergency procedures instructions to farm staff
 Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
Emergency procedures instructions to farm staff The first priority in the event of an emergency is for the safety of all people present. Emergency phone numbers Dial 111 for Fire/Police/Ambulance 1. Tell
ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE
 ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE NAME: DATE: ADDRESS: AGE: TELEPHONE#: RELIGION: OCCUPATION: REFERRED BY WHOM: NEAREST FRIEND/RELATIVE: TELEPHONE#: ADDRESS: PLEASE EXPLAIN WHY YOU HAVE COME TO SEE
ORTHOPAEDIC SPINE PAIN QUESTIONNAIRE NAME: DATE: ADDRESS: AGE: TELEPHONE#: RELIGION: OCCUPATION: REFERRED BY WHOM: NEAREST FRIEND/RELATIVE: TELEPHONE#: ADDRESS: PLEASE EXPLAIN WHY YOU HAVE COME TO SEE
Women s Continence and Pelvic Health Center
 Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
Women s Continence and Pelvic Health Center Committed to Caring 580-590 Court Street Keene, New Hampshire 03431 (603) 354-5454 Ext. 6643 URINARY INCONTINENCE QUESTIONNAIRE The purpose of this questionnaire
Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome
 Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome All Health Care Providers are required by law to make a referral to the Department of Children s Services (DCS) Child
Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome All Health Care Providers are required by law to make a referral to the Department of Children s Services (DCS) Child
Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery.
 JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Accident/Injury Reporting, Investigation, & Basic First Aid Plan
 Accident/Injury Reporting, Investigation, & Basic First Aid Plan Environmental Health, Safety, and Risk Management Department Box 6113, SFA Station Nacogdoches, Texas 75962-6113 Revised: January 2011 Purpose
Accident/Injury Reporting, Investigation, & Basic First Aid Plan Environmental Health, Safety, and Risk Management Department Box 6113, SFA Station Nacogdoches, Texas 75962-6113 Revised: January 2011 Purpose
For the Patient: GDP Other names: LYGDP
 1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
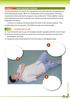 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
JAC-CEN-DEL COMMUNITY SCHOOLS BLOODBORNE PATHOGENS UNIVERSAL PRECAUTIONS A BACK TO SCHOOL TRADITION
 JAC-CEN-DEL COMMUNITY SCHOOLS BLOODBORNE PATHOGENS UNIVERSAL PRECAUTIONS A BACK TO SCHOOL TRADITION UNIVERSAL PRECAUTIONS AGAINST BLOODBORNE PATHOGENS Employees working in a school system are potentially
JAC-CEN-DEL COMMUNITY SCHOOLS BLOODBORNE PATHOGENS UNIVERSAL PRECAUTIONS A BACK TO SCHOOL TRADITION UNIVERSAL PRECAUTIONS AGAINST BLOODBORNE PATHOGENS Employees working in a school system are potentially
Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress.
 Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress. Overview Workers who are exposed to extreme heat or work in hot environments may be at risk of heat stress. Exposure to extreme heat can result
Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress. Overview Workers who are exposed to extreme heat or work in hot environments may be at risk of heat stress. Exposure to extreme heat can result
Student Health 2015/2016. Welcome Back!
 Student Health 2015/2016 Welcome Back! Back-to-School Highlights Bloodborne Pathogens Organisms in blood and other body fluids that can cause disease Examples: HBV HCV HIV AIDS Protect yourself! Observe
Student Health 2015/2016 Welcome Back! Back-to-School Highlights Bloodborne Pathogens Organisms in blood and other body fluids that can cause disease Examples: HBV HCV HIV AIDS Protect yourself! Observe
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
For the Patient: Paclitaxel injection Other names: TAXOL
 For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
BLOOD BORNE PATHOGENS
 BLOOD BORNE PATHOGENS AIDS and other blood-borne pathogens such as Hepatitis B and C are deadly diseases that are present in today s society. All blood-borne pathogens are transmitted in blood and other
BLOOD BORNE PATHOGENS AIDS and other blood-borne pathogens such as Hepatitis B and C are deadly diseases that are present in today s society. All blood-borne pathogens are transmitted in blood and other
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
Accident Prevention. and Crisis Management. Learning Objectives
 13 1 1 Accident Prevention 2 and Crisis Management Learning Objectives How can you prevent accidents? What should you do when a food recall or food crisis occurs? What should you do if the establishment
13 1 1 Accident Prevention 2 and Crisis Management Learning Objectives How can you prevent accidents? What should you do when a food recall or food crisis occurs? What should you do if the establishment
Staying on Track with TUBERCULOSIS. Medicine
 Staying on Track with TB TUBERCULOSIS Medicine What s Inside: Read this brochure to learn about TB and what you can do to get healthy. Put it in a familiar place to pull out and read when you have questions.
Staying on Track with TB TUBERCULOSIS Medicine What s Inside: Read this brochure to learn about TB and what you can do to get healthy. Put it in a familiar place to pull out and read when you have questions.
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Section 400: Code # 453.4R
 Section 400: Code # 453.4R Administering Medication Conditions for Administering Prescription Drugs Except as otherwise specifically provided by law, a school bus driver, employee, or volunteer that has
Section 400: Code # 453.4R Administering Medication Conditions for Administering Prescription Drugs Except as otherwise specifically provided by law, a school bus driver, employee, or volunteer that has
MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES
 Department of Health and Mental Hygiene Maryland State Department of Education Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Emergency Management Guidelines for
Department of Health and Mental Hygiene Maryland State Department of Education Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Emergency Management Guidelines for
let s talk bleeds a bleed checklist for haemophilia patients
 let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
What Medical Emergencies Should a Dental Office be Prepared to Handle?
 What Medical Emergencies Should a Dental Office be Prepared to Handle? Gary Cuttrell, DDS, JD, University of NM Division of Dental Services Santiago Macias, MD, First Choice Community Healthcare Dentists
What Medical Emergencies Should a Dental Office be Prepared to Handle? Gary Cuttrell, DDS, JD, University of NM Division of Dental Services Santiago Macias, MD, First Choice Community Healthcare Dentists
Diabetes Hypoglycemia/Hyperglycemia Reaction
 Diabetes Hypoglycemia/Hyperglycemia Reaction Hypoglycemic Reaction (Insulin Shock) A. Hypoglycemic reactions (insulin reactions) should be treated according to current nursing and medical recommendations.
Diabetes Hypoglycemia/Hyperglycemia Reaction Hypoglycemic Reaction (Insulin Shock) A. Hypoglycemic reactions (insulin reactions) should be treated according to current nursing and medical recommendations.
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
POINCIANA INTERNAL MEDICINE PA. Patient Name: Social Security Number: Date of Birth: / / Sex: M/F (Circle One) Married/Single/Divorced/Widow Address:
 Patient Name: Social Security Number: Date of Birth: / / Sex: M/F (Circle One) Married/Single/Divorced/Widow Address: (Street) (City/State/Zip) Home Phone: ( ) E Mail Address: Would you be interested in
Patient Name: Social Security Number: Date of Birth: / / Sex: M/F (Circle One) Married/Single/Divorced/Widow Address: (Street) (City/State/Zip) Home Phone: ( ) E Mail Address: Would you be interested in
Moving to a hospital or skilled nursing facility
 H Moving to a hospital or skilled nursing facility What to expect when you have MRSA (Methicillin-resistant Staphylococcus aureus) A booklet for patients, residents, family members, and caregivers About
H Moving to a hospital or skilled nursing facility What to expect when you have MRSA (Methicillin-resistant Staphylococcus aureus) A booklet for patients, residents, family members, and caregivers About
Sanitary Food Preparation & Safe Food Handling
 70 Feeding Infants 10 Sanitary Food Preparation & Safe Food Handling Babies are more susceptible to bacteria than older children, and unsanitary food conditions can cause serious infections. General cleanliness,
70 Feeding Infants 10 Sanitary Food Preparation & Safe Food Handling Babies are more susceptible to bacteria than older children, and unsanitary food conditions can cause serious infections. General cleanliness,
3/24/2014. Waubonsee Community College Safety Day 2014. Why do we need a First Aid Program?
 Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
2. When temperature and wind chill falls below 35 degrees including the wind chill, students, are kept indoors.
 Weather /Environmental Guidelines Time spent outdoors is an important part of the school day. It is difficult to set guidelines that fit every circumstance and condition in regards to outside activities.
Weather /Environmental Guidelines Time spent outdoors is an important part of the school day. It is difficult to set guidelines that fit every circumstance and condition in regards to outside activities.
INFLUENZA (FLU) Flu and You
 Influenza (Flu) What is the flu? The flu is an illness caused by flu viruses. The flu may make people cough and have a sore throat and fever. They may also have a runny or stuffy nose, feel tired, have
Influenza (Flu) What is the flu? The flu is an illness caused by flu viruses. The flu may make people cough and have a sore throat and fever. They may also have a runny or stuffy nose, feel tired, have
Cataract Information for Patients
 Cataract Information for Patients http://www.gov.pe.ca/health and click on Wait Times tab Page 1 What is a Cataract? A cataract is a clouding of the eye s naturally clear lens. When the lens becomes cloudy,
Cataract Information for Patients http://www.gov.pe.ca/health and click on Wait Times tab Page 1 What is a Cataract? A cataract is a clouding of the eye s naturally clear lens. When the lens becomes cloudy,
Okolona Fire Department Standard Operating Procedure
 Page 1 of 6 October 1, 2011 New Operational Purpose: This policy will govern the type of training, the environment, gear to be used for training, and outside non-emergency activities for the Okolona Fire
Page 1 of 6 October 1, 2011 New Operational Purpose: This policy will govern the type of training, the environment, gear to be used for training, and outside non-emergency activities for the Okolona Fire
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
MEDICAL AND HEALTH EMERGENCIES
 IX.041 MEDICAL AND HEALTH EMERGENCIES POLICY The Board shall provide medically appropriate, immediate, quality emergency care in the event of an accident or illness that may compromise the well-being of
IX.041 MEDICAL AND HEALTH EMERGENCIES POLICY The Board shall provide medically appropriate, immediate, quality emergency care in the event of an accident or illness that may compromise the well-being of
How can you protect yourself from infections?
 How can you protect yourself from infections? Your Infection Prevention Guide www.esrdncc.org Table of Contents Preventing an infection is an important part of your kidney care...3 Things you can do...4
How can you protect yourself from infections? Your Infection Prevention Guide www.esrdncc.org Table of Contents Preventing an infection is an important part of your kidney care...3 Things you can do...4
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
How to treat your injured neck
 How to treat your injured neck Exceptional healthcare, personally delivered Your neck is made up of a number of bones bound together by strong discs and ligaments. It is also protected by strong muscles.
How to treat your injured neck Exceptional healthcare, personally delivered Your neck is made up of a number of bones bound together by strong discs and ligaments. It is also protected by strong muscles.
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
What You And Your Family Can Do About Asthma
 GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
MOTOR VEHICLE ACCIDENT QUESTIONNAIRE
 MOTOR VEHICLE ACCIDENT QUESTIONNAIRE Thank you in advance for taking the time to complete this form, this will help us to better assess all of your pain concerns and provide you with the best treatment.
MOTOR VEHICLE ACCIDENT QUESTIONNAIRE Thank you in advance for taking the time to complete this form, this will help us to better assess all of your pain concerns and provide you with the best treatment.
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Cervical Spine. New Patient Form
 Cervical Spine New Patient Form Please mark the painful areas on the pictures below Use the following marks: stabbing pain ooo burning pain +++ aching pain pins and needles = = = numbness Right Right Right
Cervical Spine New Patient Form Please mark the painful areas on the pictures below Use the following marks: stabbing pain ooo burning pain +++ aching pain pins and needles = = = numbness Right Right Right
Get Trained. A Program for School Nurses to Train School Staff in Epinephrine Administration
 A Program for School Nurses to Train School Staff in Epinephrine Administration The Get Trained School Nursing Program was created through an unrestricted grant from Mylan Specialty. The Program is intended
A Program for School Nurses to Train School Staff in Epinephrine Administration The Get Trained School Nursing Program was created through an unrestricted grant from Mylan Specialty. The Program is intended
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g.
 How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
How to safely collect blood samples from persons suspected to be infected with highly infectious blood-borne pathogens (e.g. Ebola) Step 1: Before entering patient room, assemble all equipment (1 st part)
Chemotherapy Side Effects Worksheet
 Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
Page 1 of 6 Chemotherapy Side Effects Worksheet Medicines or drugs that destroy cancer cells are called cancer chemotherapy. It is sometimes the first choice for treating many cancers. Chemotherapy differs
