Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay
|
|
|
- Jeffrey Hutchinson
- 6 years ago
- Views:
Transcription
1 Pictorial essay Medical Ultrasonography 2010, Vol. 12, no. 4, Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay Zbigniew Czyrny M.D. Private Practice, Michalow Grabina, Poland Abstract This paper tries to describe reasons, pathophysiological sequence of events, including the sequelae, and location of the traumatic tears of the ossification center of the tibial tuberosity in adolescents. Ultrasonographic features characteristically seen in the traction type of Osgood-Schlatter disease (OSD) are presented in a pictorial. The classification and definitions used is based on the three types of OSD described by Czyrny&Greenspan in Keywords: ultrasonography, Osgood-Schlatter disease, tibial tuberosity Rezumat Acest eseu în imagini incearcă să descrie motivele, secvenţa fiziopatologică a evenimentelor şi localizarea rupturilor traumatice ale centrului de osificare din tuberozitatea tibială la adolescenţi. Modificările ecografice caracteristice ce se pot evidenţia în boala Osgood-Schlatter sunt prezentate pe larg. Clasificarea şi definiţiile utilizate se bazează pe cele trei tipuri de boala Osgood-Schlatter descries de Czyrny&Greenspan în Cuvinte cheie: ecografie, boala Osgood-Schlatter, tuberozitatea tibială Osgood-Schlatter disease (OSD) was first described in 1903 by Robert Osgood of Boston [1] and in 1903 and then 1908 by Carl Schlatter of Zurich [2,3]. Whereas Osgood focused on full avulsion fractures of the tibial tuberosity, with loss of patellar ligament continuity, Schlatter noted a wide variety of reasons for the disease. The main reason was traction trauma to the tibial tuberosity that led to avulsion of a proximal part of the tuberosity or to incomplete fracture. OSD disease occurs in patients between 8 and 15 years of age [1-3]. Features of OSD revealed by US, CT and MRI [4-9] have included pretibial soft tissue swelling, cartilage swelling, fragmentation of the tibial tuberosity s ossification center, thickening at the insertion of the patellar ligament, and inflammation of the deep infrapatellar bursa. Ultrasound has unmatched ability to show the structure of the physeal part of the tibial tuberosity (fig 1). Received Accepted Med Ultrason 2010, Vol. 12, No 4, Address for correspondence: Zbigniew Czyrny, M.D. Private Practice, Michalow Grabina, Poland zbigniew.czyrny@wp.pl Fig 1. Longitudinal US image of the late stage of tibial tuberosity (beak-like process) bone formation with ossification center fusion (long arrow). Arrowheads, patellar ligament; E, epiphysis; M, metaphysis; double arrow, cartilage thickness between the ossification center and the patellar ligament attachment.
2 324 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay to distinguish but after a week of inflammatory process the fibrosis is an inevitable sequelae so the duration of the symptoms may be a key to classification of the image, Hypervascularity of the zone of insertion of the patellar ligament indicating active inflammation/reparative processes defined as the presence of at least two vessels within the distal ligament. In borderline images comparing to the asymptomatic side, if not affected by the disease, is important. The presence of a single vessel at the patellar ligament s tibial insertion does not automatically mean pathology. Fig 2. Magnetic resonance imaging (MRI), STIR, of OSD type I in a 14-year-old boy, 4 months after the first onset of symptoms. PL, patellar ligament edematous at the distal end; asterisk, pretibial soft tissue edema; H, Hoffa s fat pad; black double arrowheads, edema and fibrosis over the tibial wall of the deep infrapatellar bursa; E, epiphysis; M, metaphysis; white double arrowheads, approximate thickness of the delamination zone; arrowheads, margin of the cartilage. Note the diffused edema of the anterior epiphysis and superior metaphysis. Probably second most fitted for the diagnostic accuracy would be MRI. It is much more sensitive in the depiction of the bone/cartilage edema (fig 2) and can even sometimes be a more sensitive tool for exclusion of the disease due to subtle oedematic changes which may appear even before presenting a delamination tear of the ossification center. Definitions Deep infrapatellar bursa effusion defined as even faint amount of fluid but present within the whole width of the bursa or hematoma defined as bright fluid with visible dense material or fibrotic clot movement. Bursal synovial edema defined as layer of more than 1mm thickness of hypo- or hyperechogenic tissue overlying the tibial wall of the bursa. A layer of tissue <1mm thickness overlying the tibial wall of the bursa is frequently seen in asymptomatic bursas. Hypervascularity (increased perfusion) of the bursal tissues defined as presence of even single vessel in Tissue Doppler Mode (Toshiba) set on maximum sensitivity at the synovial tibial bursal lining, Fibrosis within the bursal space defined as layer of more than 1mm thickness of hyperechogenic tissue overlying the tibial wall of the bursa and/or improper bursal fat apron movement between the patellar ligament and tibial bursal wall. It may be difficult at times Anatomy and histology of the tibial tuberosity The anatomic location of the traction injury in OSD is the ossification center of the beak-like process of the tibial epiphysis. It is an endochondral ossification cente a layer of cellular columns responsible for calcium production and the later transformation of calcium into bone [10]. The anterior (cellular) surface of the tuberosity ossification center is a metabolically active zone until the tuberosity terminates it s growth. This zone, a cellular gap between the layers of solid cartilage and cartilage-bone, lacks reinforcing structures such as the collagen fibers present in the surrounding cartilage. As a result, these cellular columns, deprived of collagen reinforcement, constitute the weakest structural link of the tuberosity. Three factors account for the specific location of the traction type of injury in OSD. First, there is a difference in durability between the epiphyseal and metaphyseal parts of the patellar ligament insertion; this can be explained by the type of ossification at the epiphysis (endochondral) versus that at the metaphysis (membranous) [10]. Second, compared with the distal 20 to 25 mm, the proximal mm of the tibial tuberosity has a larger angle between its surface and the longitudinal fibers of the patellar ligament. This approximately mm zone is where traction on the patellar ligament generates most of the delaminating force [11]. Third, the epiphyseal beak-like process, with its ossification center of cellular columns, is the weakest structural link. These three factors prove to be the fatal combination that results in injury to this specific area. The tibial tuberosity development may be divided into three stages: early (fig 3), middle (fig 4, fig 5), and late-stage (fig 6, fig 7) of bone formation of the tibial tuberosity. Fig 8-11 show the normal US aspect of the patellar ligament attachment to the tibial tuberosity Classification and features of Osgood-Schlatter disease (based on Czyrny&Greenspan 2009 [12]).
3 Medical Ultrasonography 2010; 12(4): Fig 3. Longitudinal US image of the early stage of bone formation of the tibial tuberosity beginning with the appearance of cloud-like ossified tissue within the anterior tibial cartilage that may be mistaken for fragmentation but in fact merely represent an incomplete fusion of the ossifying cartilage. Short arrows, patellar ligament; long arrows, ossifying cartilage (ossification center is transparent to the US beam at this stage); E, epiphysis; M, metaphysis; double arrow, thickness of the tibial tuberosity cartilage. Fig 4. Longitudinal US image of the middle stage of tibial tuberosity bone formation. The ossified cartilage transforms into mature bone more or less scattered in the area of the tibial tuberosity; this bone is usually not transparent to the ultrasound beam any more and presents as white line that is irregular or discontinued. Arrowheads, patellar ligament; long arrows, ossification center anterior margin (ossified enough to be no longer transparent to the US beam); E, beak-like process of the epiphysis; M, metaphysis; double arrow, cartilage thickness between the ossification center and the patellar ligament attachment; dashed arrow, level of the proximal patellar ligament s attachment. Fig 5. Longitudinal US image of the middle stage of tibial tuberosity bone formation. double arrows, cartilage thickness between the ossification center and the patellar ligament attachment (right), cartilage thickness of the tibial wall of the deep infrapatellar bursa. Asymptomatic patient; note the normal arteries within the patellar ligament insertion (a) and cartilage of the ossification center (b).
4 326 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay Fig 7. Sagittal US image of the normal late-stage formation of the beak-like process of the tibial tuberosity. M, metaphysis; E, epiphysis; dashed line, surface area of the ossification center equal in length to patellar ligament s insertion to the epiphyseal part of the tibial tuberosity (enthesis), where cartilage fracture and delamination can be seen in OSD; double arrow, cartilage covering the beak-like process of the epiphysis; arrows, anterior surface of the patellar ligament. Fig 6. Lateral radiograph of normal late-stage formation of the beak-like process of the epiphyseal part of the tibial tuberosity (*).The epiphyseal part of the tibial tuberosity overlaps the anterior proximal part of the tibial metaphysis anteriorly. The product of this ossification center was named the beak-like process of the tibial tuberosity by Carl Schlatter. E, epiphysis; M, metaphysis; dashed lines, approximate anterior and posterior margins of the patellar ligament. Fig 8. Normal longitudinal US image of the patellar ligament attachment to the tibial tuberosity in an adolescent representing the sagittal crossection of the ligament s footprint. Usually the length and width of the ligament s footprint in ultrasonographical curved line measurements range between 20 and 40 mm and 20 and 30 mm respectively. The type of OSD discussed in this paper is found only within approximately the mm long zone of the proximal tibial insertion of the patellar ligament, which corresponds to the length of the beak-like process. Short arrows, the patellar ligament s margin; long arrow, the proximal border level of the patellar ligament s insertion; dashed long arrow, the level of the cartilage zone between the beak-like process of the epiphysis (E) and the metaphysis (M); curved dotted line, approximate total length of the patellar ligament s tibial insertion.
5 Medical Ultrasonography 2010; 12(4): Fig 9. Longitudinal US image of the tibial tuberosity. The vascularity of this region is, of necessity (supply of nutrients and oxygen to the ossification center) extremely rich. That is why a concept of avascular necrosis in this area seems extremely out of place. There is a common arterial supply to the tuberosity and to the synovium of the deep infrapatellar bursa. This arterial architecture may explain why, even in minor injuries, the inflammatory-reparative process of and around the ossification center may still cause inflammation and later fibrosis in the bursa. Fig 10. The deep infrapatellar bursa is occupying a large space between the posterior margin of the patellar ligament and the anterior margin of the tibial epiphysis, right above the proximal patellar ligament s insertion line. The fat pad of the bursa is a part of Hoffa s fat pad. Because of these particular anatomic characteristics the pathologies of the bursa are a part of the OSD in most cases. Arrows, four walls of the deep infrapatellar bursa bursa; P, patella; H, Hoffa s fat pad; T, tibia; F, femur. Red, the bursae of the extensor apparatus. Fig 11. The deep infrapatellar bursa US images from full extension (a) to full flexion (c) of the knee. A significant part of Hoffa s fat pad is a moving element of the bursa. It does not get compressed between the ligament and the tibial wall in normal nonfibrotic conditions it glides in and out of the space between the ligament and the tibia. In the case of serious bursal fibrosis, the movement of that part during flexion-extension is disturbed and it may become a compressed element of the bursa.
6 328 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay The pathologic features and clinical consequences of the three types of OSD: Type I (fig 12-20) Delamination of the internal ossification center, resulting in an igloo like deformation of the physeal part of the tibial tuberosity, with hump-like anterior displacement of the proximal attachment of the patellar ligament. Deep infrapatellar bursitis and/or fibrosis due to a shared arterial supply with the tibial tuberosity and local inflammation/reparative process. Disseminated inflammation/fibrosis of the patellar ligament secondary to the main injury and deep infrapatellar bursitis. Main character after the acute phase is reparative process. Superficial infrapatellar bursitis secondary to deep infrapatellar bursitis and to changes involving the patellar ligament. Fig 12. Type I OSD, longitudinal US image. A clean delamination tear, with only a thin anterior layer of the ossification center displaced with no calcified material present within the delamination zone. Arrowheads, margins of the patellar ligament; black double arrows, cartilage thickness in the tibial tuberosity over the ossification center (hyperechogenic cartilage edema or/and fibrosis); E, epiphysis; M, metaphysis. Note the clear-cut margins of the delaminated layers of the ossification center (white double arrow) a clear transparent igloo. Dashed line indicates the level of transversal section in the next figure. Fig 13. Type I OSD, transverse US image, patient from previous figure. E, epiphysis; arrowheads, margins of the patellar ligament; dotted double arrow, cartilage thickness in the tibial tuberosity over the ossification center. Note the clear-cut margins of the delaminated layers of the ossification center (white double arrow) a clear transparent igloo. Fig 14. Type I OSD, longitudinal US image. A slightly blurred minimal delamination tear of the ossification center. No displacement of the cartilage at the beginning of the patellar ligament s footprint (long arrow) is observed; Dotted double arrows, cartilage of the ossification center and the tibial wall of the deep infrapatellar bursa; solid double arrows, thickness of the delamination of the ossification center. Fig 15. Type I OSD, transverse US image, patient from previous image. A slightly blurred minimal delamination tear of the ossification center; dotted double arrow, thickness of the delamination of the ossification center; solid double arrows, cartilage of the ossification center and the tibial wall of the deep infrapatellar bursa; arrowheads, patellar ligament margin.
7 Medical Ultrasonography 2010; 12(4): Fig 16. Type I OSD, longitudinal US image, patient from previous image. Hyperperfusion of the patellar ligament at the insertion. Most likely the cousin of the reparative process at the delaminated ossification center. Fig 17. Type I OSD, longitudinal US image. A blurred delamination of the epiphyseal ossification center which occurs when ossified tissue of the center is torn within and displaced in a scattered manner with only the roof of the igloo being smooth. No fracture and anterior transfer of the proximal part of the tuberosity is present (dashed arrow at the level of the proximal ligament s attachment) which is a key difference from type II. Short arrow, the anterior margin of the patellar ligament; short double arrow, cartilage thickness in the tibial tuberosity; short double dotted arrow, fibrosis within the deep infrapatellar bursa; arrowheads, anterior margin of the delaminated ossification center. Note the uneven distribution of calcified tissue within the delaminated area (long double arrow) a blurred igloo. Fig 18. Type I OSD, longitudinal US image. Patient from previous figure. Effusion (*) and fibrosis (arrows) due to inflammation can be observed within the deep infrapatellar bursa. Arrowheads, patellar ligament; Hoffa s fat pad retracted by fluid; double arrowhead, ossification center cartilage layer. Fig 19. US images of the type I OSD with a blurred igloo. Patellar ligament edematous and hyperperfused (Doppler frame) at the distal end/insertion, most likely representing a reparative process. A lot of vessels enter the ligament from the superficial arterial network but there is no inflammation of the superficial infrapatellar bursa. They seem to reach the depth of the internal arteries of the ossification center. Double arrow, thickness of the intact cartilage overlying the ossification center; double dashed arrow, approximate thickness of the delamination zone.
8 330 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay Fig 20. A, Ossified end-stage after type I OSD delamination tear of the beak-like process of the tuberosity. Bulging of the tuberosity is the basic diagnostic and clinical feature of OSD. Double arrows, cartilage thickness over the ossification center; dashed line on Figure a, normal outline of the ossification center transferred directly (same scale) from Figure b, indicating the difference between the normal outline and the final effect of the ossification center delamination tear; E, epiphysis; M, metaphysis. B, Normal tibial tuberosity, contralateral side. The prognosis is very favorable for this type of disease as it leaves minimal disturbance to the shape of the tuberosity and the state of the patellar ligament. Type II (fig 21-27) Delamination tear/fracture of the epiphyseal part of the tibial tuberosity, with fracture of cartilage overlying ossification center and significant anterior displacement of the proximal attachment of the patellar ligament due to the displacement of the fractured cartilage. Deep infrapatellar bursitis or fibrosis (or both) due to bleeding from the torn cartilage/ossification center. Disseminated inflammation/fibrosis of the patellar ligament secondary to the main injury and deep infrapatellar bursitis. Main character after the acute phase is reparative process. Superficial infrapatellar bursitis secondary to deep infrapatellar bursitis and inflammation/ fibrosis involving enthesis zone of the patellar ligament. The prognosis is moderately favorable for this type of disease as it tends to create significant bursal fibrosis including impairment of dynamic behavior of the fatty apron of the deep infrapatellar bursa/hoffa s fat pad, however doesn t leave significant scarring within the patellar ligament. Fig 21. Longitudinal US image of a delamination tear and cartilage fracture at the patellar ligament s proximal insertion border of the tibial tuberosity ossification center (OSD type II). Arrowheads, patellar ligament; arrow, roof of the clean igloo; double arrow, thickness of the fracture displacement at the line of the proximal patellar ligament insertion - the gate for the blood to pour from the torn ossification center into the deep infrapatellar bursa. P, patella; T, tibia; H, Hoffa s fat pad; HE, hematoma within the deep infrapatellar bursa. Fig 22. Patient from previous figure. OSD type II, a close-up. Arrowheads, patellar ligament; arrow, roof of the clean igloo; double arrow, thickness of the fracture at the line of the proximal patellar ligament insertion the gate for the blood to pour from the torn ossification center into the deep infrapatellar bursa. P, patellal; T, tibia; H, Hoffa s fat pad; HE, hematoma within the deep infrapatellar bursa.
9 Medical Ultrasonography 2010; 12(4): Fig 23. Patient from previous figure. OSD type II, a further close-up. Arrowheads, patellar ligament; double arrow, thickness of the fracture at the line of the proximal patellar ligament insertion - the gate for the blood to pour from the torn ossification center into the deep infrapatellar bursa. P, patellal; T, tibia; H, Hoffa s fat pad; HE, hematoma within the deep infrapatellar bursa; F, fibrotic clot separating the fractured ossification center cartilage from the deep infrapatellar bursa. Fig 26. US transverse type II OSD. Patient from previous image. Double arrowt, maximum delamination distance of the beak-like process; arrowheads, patellar ligament margins. Fig 24. US longitudinal type II OSD. Arrowheads, patellar ligament margin; double black arrow, the thickness of the anteriorly displaced part of the ossification center; double white arrow, distance of anterior displacement of the proximal fractured cartilage; long arrow, proximal, anteriorly transferred, insertion of the patellar ligament. Note the disturbance of tibial wall of the deep infrapatellar bursa filled with bright fibrotic tissue (short arrows). Fig 27. US longitudinal type II OSD. Patient from previous image. b: contralateral side. Fig 25. US longitudinal type II OSD. Patient from previous image. Double arrow right, distance of anterior displacement of the proximal fractured proximal cartilage of the beak-like process; double arrows (two left), fibrotic layers induced by previous hematoma from fractured cartilage and ossification center; long dashed arrow, the route of blood from the fractured ossification center into the deep infrapatellar bursa.
10 332 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay Type III (fig 28-43) Delamination tear of the ossification center resulting in irregular deformation of the tuberosity, cartilage fracture with or without significant anterior displacement of the proximal attachment of the patellar ligament. Cartilage fracture at least in part within the footprint of the patellar ligament insertion. Deep infrapatellar bursitis or fibrosis (or both) due to a shared arterial supply with the tibial tuberosity and bleeding from the torn patellar ligament and fractured cartilage. Disseminated inflammation/reparative process of the patellar ligament secondary to the main injury and deep infrapatellar bursitis. Focal scarring and possible ectopic calcium or bone formation due to a tear (usually a longitudinal delamination tear) in the patellar ligament arising from its torn tibial insertion. Fig 29. Transverse US image at level a from previous figure; type III OSD. Arrows, anterior margin of the patellar ligament; double arrow, cartilage layer over the deformed tibial tuberosity ossification center; arrowheads, ossifying scar of the torn cartilage and patellar ligament the possible start of an ectopic ossified or calcified scar within the patellar ligament. Fig 28. Longitudinal US image of a type III OSD injury to the epiphyseal beak-like area of the tibial tuberosity. Arrows, anterior and posterior margins of the distal patellar ligament; double arrow, cartilage of the tibial tuberosity; arrowheads, line of the cartilage crack and patellar ligament scar in the early ossification phase; a, b levels of the transverse images of this area, shown in next figures. Fig 30. Transverse US image at level b from figure 28; type III OSD. Arrows, anterior and posterior margins of the patellar ligament; arrowheads, calcified area within the scar of the patellar ligament; T, tibia. Fig 31. Normal tibial tuberosity (left) and OSD featuring type III (right). Arrows show margins of the horizontally fractured/torn ossification center. This kind of injury must have torn the insertion of the patellar ligament. Not clearly seen on this image is the fracture and anterior displacement of the proximal beak-like process opening the connection between the ossification center and the deep infrapatellar bursa
11 Medical Ultrasonography 2010; 12(4): Fig 32. OSD type III, patient from the previous image. Arrows show margins of the horizontally fractured/torn ossification center; double arrow, the size of fracture and anterior displacement of the proximal beak-like process opening the connection between the ossification center and the deep infrapatellar bursa; F, fluid in the bursa; FI, fibrosis of bursal walls, due to the hemorrage/ inflammation in the bursa. Fig 33. OSD type III, patient from the previous image. F, fluid in the bursa; FI, fibrosis of bursal walls, due to the hemorrhage/ inflammation in the bursa. Fig 34. Longitudinal US panoramic continuous reconstruction image of the mature ossified type III OSD. P, patella; short arrows, patellar ligament margins; H, Hoffa s fat pad. Subcutaneous tissue edema is seen over the patellar ligament and tibial tuberosity (*). Double dashed arrow, massive local calcium deposits infiltrating the entire thickness of the patellar ligament; long arrow, proximal level of the patellar ligament s insertion. Fig 35. Transverse US image of the patient from previous figure at the level of the patellar ligament s ossification. Arrows, margins of the scarified patellar ligament; double dashed arrow, width of a massive local calcium infiltration of nearly the entire thickness of the patellar ligament; long arrow, blurred outline of the disrupted original anterior margin of the tibial tuberosity. Fig 36. Longitudinal US image of the OSD type III. Patient 1 month after the first symptoms. There was no effusion or fibrosis of the deep infrapatellar bursa, no evidence of the cartilage tear at the proximal border of the patellar ligament s insertion (no communication between the torn/fractured ossification center and the bursa. Double dotted arrow, the size of the ossification center fracture; Double long solid arrow, anterior displacement of the fractured/delaminated part of the ossification center; Small solid double arrows, cartilage thickness of the ossification center and the tibial wall of the deep infrapatellar bursa. Note that cartilage over the ossification center is bright indicating it s oedema. Hyperperfusion within the patellar ligament, cartilage and the floor of the ossification center reparative process.
12 334 Zbigniew Czyrny et al Osgood-Schlatter disease in ultrasound diagnostics a pictorial essay Fig 37. Longitudinal US image of the OSD type III. Patient from previous image. Solid double arrow, cartilage thickness of the ossification center and the tibial wall of the deep infrapatellar bursa. Note that cartilage over the ossification center is bright indicating it s oedema; Curved dotted arrow, line of the cartilage/patellar ligament tear over the fractured ossification center; Arrowheads, patellar ligament margins Fig 38. Transverse US image of the OSD type III. Patient from previous image. The image shows that the ossification center is fractured not only in the transverse plain but also has a longitudinal component from the medial side double arrow shows the size of that medial longitudinal component of the fracture. Curved dotted arrow, the tear of the cartilage and the patellar ligament, the potential portal for calcification and ectopic bone formation within the ligament; Arrowheads, patellar ligament margins Fig 39. Transverse US image of the OSD type III. Patient from previous image, the same location. Image shows accumulation of hypervascularity at the medial cartilage/ligament tear site indicating most prominent reparative process Superficial infrapatellar bursitis secondary to deep infrapatellar bursitis and to a tear and later scar formation involving the patellar ligament. For this type of disease, the prognosis is unfavorable, with a high probability of chronic symptoms due to fibrosis of the deep infrapatellar bursa and ectopic bone or calcium formation within the patellar ligament s scar. Fig 40. Lateral radiograph of an adult male patient with a history of OSD, type III. Dashed lines, approximate anterior and posterior margins of the patellar ligament; short arrow, ectopic ossification formed within the patellar ligament s scar; short dotted arrow, possible past fracture line between the ectopic ossification and the main part of the tibial tuberosity; long solid arrow, distorted shape of the tibial tuberosity within the epiphyseal footprint of the patellar ligament; long dashed arrow, distorted shape of the tibial wall of the deep infrapatellar bursa, proximal to the patellar ligament insertion, indicating a past serious disruption in the ossification center and multidirectional cartilage fracture.
13 References Medical Ultrasonography 2010; 12(4): Fig 41. US longitudinal image of the type III OSD with an ectopic ossification. Arrowheads, anterior and posterior margins of the patellar ligament; long arrows, ectopic ossifications formed within patellar ligament s scar; dashed arrow, distal segment of the possible fracture line between the ectopic ossification and the main part of the tibial tuberosity; dashed curved line, theoretical anterior margin of the tuberosity, partly obscured by the ossification. H, Hoffa s fat pad; T, tibia. Fig 42. US longitudinal image of the type III OSD at the border of an ectopic ossification (patient from previous image) shows rebuilt scar of the patellar ligament at the border of the intraligamentous ossification. Deformed anterior margin of the tuberosity. 1. Osgood RB. Lesions of the tibial tubercle occurring during adolescence. Boston Medicine and Surg Journal 1903; 148: Schlatter C. Verletzungen des schnabelformigen Fortsatzes der oberen Tibiaepiphyse. Bruns Beitr Klein Chir Schlatter C. Unvollstandige Abrissfrakturen der Tuberositas tibiae oder Wachstumsanomalien. Bruns Beitr Klein Chir Blankstein A, Cohen I, Heim M, et al. Ultrasonography as a diagnostic modality in Osgood-Schlatter disease. A clinical study and review of the literature. Arch Orthop Trauma Surg 2001; 121: Peace KAL, Lee JC, Healy J. Imaging the infrapatellar tendon in the elite athlete. Clinical Radiol 2006; 61: De Flaviis L, Nessi R, Scaglione P, Balconi G, Albisetti W, Derchi LE. Ultrasonic diagnosis of Osgood-Schlatter and Sinding-Larsen-Johansson diseases of the knee. Skeletal Radiol 1989; 18: Lanning P, Heikkinen E. Ultrasonic features of the Osgood- Schlatter lesion. J Pediatr Orthop 1991; 11: Bergami G, Barbuti D, Pezzoli F. Ultrasonographic findings in Osgood-Schlatter disease. Radiol Med (Torino) 1994; 88: Rosenberg ZS, Kawelblum M, Cheung YY, Beltran J, Lehman WB, Grant AD. Osgood-Schlatter lesion: fracture or tendinitis? Scintigraphic, CT, and MR imaging features. Radiology 1992; 185: Gray H, Standring S, Ellis H, Berkovitz BKB. Gray s Anatomy, 39 th edition. New York, Elsevier, Churchill Livingstone, 2005: I.A.Kapandji, The Physiology of the Joints: Lower Limb, Volume 2, 5 th edition, Churchill Livingstone, Czyrny Z, Greenspan A. Osgood-Schlatter Disease: a new perspective and classification based on ultrasonography. Ultrasonografia 2009; 38: Fig 43. US transverse of the type III OSD over an ectopic ossification (arrow) (patient from previous image).
Osseous Tissue & Structure. The skeletal system includes: Storage of minerals: calcium salts
 Chapter 15 Lecture The Skeletal System: Osseous Tissue & Skeletal Structure The Skeletal System The skeletal system includes: Bones, cartilages, ligaments Bone tissue = osseous tissue Includes living cells
Chapter 15 Lecture The Skeletal System: Osseous Tissue & Skeletal Structure The Skeletal System The skeletal system includes: Bones, cartilages, ligaments Bone tissue = osseous tissue Includes living cells
Running Head: Salter Harris Fractures 1
 Running Head: Salter Harris Fractures 1 Salter Harris Classification of Growth Plate Fractures November 15 th, 2011 Salter Harris Fractures 2 Abstract Salter-Harris Classifications are a straightforward
Running Head: Salter Harris Fractures 1 Salter Harris Classification of Growth Plate Fractures November 15 th, 2011 Salter Harris Fractures 2 Abstract Salter-Harris Classifications are a straightforward
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Common Foot & Ankle Sports Injuries
 Common Foot & Ankle Sports Injuries Symptoms Related to Abnormal Foot Biomechanics & their Differential Diagnosis Daniel Pang BSc (Hon) P&O, Cped Certified Pedorthist (USA) Only 10% of foot having structure
Common Foot & Ankle Sports Injuries Symptoms Related to Abnormal Foot Biomechanics & their Differential Diagnosis Daniel Pang BSc (Hon) P&O, Cped Certified Pedorthist (USA) Only 10% of foot having structure
Imaging of the Knee Extensor Mechanism
 Imaging of the Knee Extensor Mechanism Kirkland W. Davis, MD University of Wisconsin School of Medicine and Public Health Madison, Wisconsin Introduction: This handout accompanies a presentation at the
Imaging of the Knee Extensor Mechanism Kirkland W. Davis, MD University of Wisconsin School of Medicine and Public Health Madison, Wisconsin Introduction: This handout accompanies a presentation at the
Rotator cuff tears Acute or chronic? Mary Obele ANZSOM September 2012 Acknowledgement: ACC
 Rotator cuff tears Acute or chronic? Mary Obele ANZSOM September 2012 Acknowledgement: ACC Anatomy Epidemiology Asymptomatic rotator cuff tears: prevalence is 35% (5) 15% full thickness and 20% partial
Rotator cuff tears Acute or chronic? Mary Obele ANZSOM September 2012 Acknowledgement: ACC Anatomy Epidemiology Asymptomatic rotator cuff tears: prevalence is 35% (5) 15% full thickness and 20% partial
Sonography of Partial-Thickness Quadriceps Tendon Tears With Surgical Correlation
 Article Sonography of Partial-Thickness Quadriceps Tendon Tears With Surgical Correlation Samuel La, MD, David P. Fessell, MD, John E. Femino, MD, Jon A. Jacobson, MD, David Jamadar, MB, BS, Curtis Hayes,
Article Sonography of Partial-Thickness Quadriceps Tendon Tears With Surgical Correlation Samuel La, MD, David P. Fessell, MD, John E. Femino, MD, Jon A. Jacobson, MD, David Jamadar, MB, BS, Curtis Hayes,
Is Your Horse Off Behind?? Hindlimb Facts. Common Hindlimb Lameness. Diagnostic Techniques. Gait Analysis 3/21/2012
 Is Your Horse Off Behind?? Nathaniel A. White II DVM MS DACVS Jean Ellen Shehan Professor and Director Common Hindlimb Lameness Sacroiliac joint pain Hip Lameness Stifle Lameness Stress Fractures Hock
Is Your Horse Off Behind?? Nathaniel A. White II DVM MS DACVS Jean Ellen Shehan Professor and Director Common Hindlimb Lameness Sacroiliac joint pain Hip Lameness Stifle Lameness Stress Fractures Hock
DIAGNOSING SCAPHOID FRACTURES. Anthony Hewitt
 DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
DIAGNOSING SCAPHOID FRACTURES Anthony Hewitt Introduction Anatomy of the scaphoid Resembles a deformed peanut Articular cartilage covers 80% of the surface It rests in a plane 45 degrees to the longitudinal
MRI of Bone Marrow Radiologic-Pathologic Correlation
 MRI of Bone Marrow Radiologic-Pathologic Correlation Marilyn J. Siegel, M.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, MO and Visiting Scientist, AFIP, Washington,
MRI of Bone Marrow Radiologic-Pathologic Correlation Marilyn J. Siegel, M.D. Mallinckrodt Institute of Radiology Washington University School of Medicine St. Louis, MO and Visiting Scientist, AFIP, Washington,
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
Ulnar sided Wrist Pain
 Ulnar sided Wrist Pain 1 Susan Cross, 1 Anshul Rastogi, 2 Brian Cohen, 1 Rosy Jalan 1 Dept of Radiology, Barts Health NHS Trust, London, UK 2 London Orthopaedic Centre Contact: susan.cross@bartshealth.nhs.uk
Ulnar sided Wrist Pain 1 Susan Cross, 1 Anshul Rastogi, 2 Brian Cohen, 1 Rosy Jalan 1 Dept of Radiology, Barts Health NHS Trust, London, UK 2 London Orthopaedic Centre Contact: susan.cross@bartshealth.nhs.uk
The Land of Os: Accessory Ossicles of the Foot
 The Land of Os: Accessory Ossicles of the Foot Susan Cross, Anshul Rastogi, Rosy Jalan; Dept of Radiology, Barts Health NHS Trust, London, UK Contact: susan.cross@bartshealth.nhs.uk Pictorial review Abstract
The Land of Os: Accessory Ossicles of the Foot Susan Cross, Anshul Rastogi, Rosy Jalan; Dept of Radiology, Barts Health NHS Trust, London, UK Contact: susan.cross@bartshealth.nhs.uk Pictorial review Abstract
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Ultrasound Tissue Characterization an innovative method to visualize and monitor Patellar Tendinopathy
 Ultrasound Tissue Characterization an innovative method to visualize and monitor Patellar Tendinopathy Hans T.M. van Schie DVM, PhD UTC Imaging, Netherlands Scoring with Patellar Tendinopathy? no one size
Ultrasound Tissue Characterization an innovative method to visualize and monitor Patellar Tendinopathy Hans T.M. van Schie DVM, PhD UTC Imaging, Netherlands Scoring with Patellar Tendinopathy? no one size
How To Know If You Can Recover From A Knee Injury
 David R. Cooper, M.D. www.thekneecenter.com Wilkes-Barre, Pa. Knee Joint- Anatomy Is not a pure hinge Ligaments are balanced Mechanism of injury determines what structures get damaged Medial meniscus tears
David R. Cooper, M.D. www.thekneecenter.com Wilkes-Barre, Pa. Knee Joint- Anatomy Is not a pure hinge Ligaments are balanced Mechanism of injury determines what structures get damaged Medial meniscus tears
Hole s Human Anatomy and Physiology Eleventh Edition. Mrs. Hummer Hanover Area Jr./Sr. High School. Chapter 1 Introduction to Anatomy and Physiology
 Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Hanover Area Jr./Sr. High School Chapter 1 Introduction to Anatomy and Physiology 1 Chapter 1 Introduction to Human Anatomy and Physiology
Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Hanover Area Jr./Sr. High School Chapter 1 Introduction to Anatomy and Physiology 1 Chapter 1 Introduction to Human Anatomy and Physiology
Hamstring Apophyseal Injuries in Adolescent Athletes
 Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
Hamstring Apophyseal Injuries in Adolescent Athletes Kyle Nagle, MD MPH University of Colorado Department of Orthopedics Children s Hospital Colorado Orthopedics Institute June 14, 2014 Disclosures I have
Evaluating Knee Pain
 Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Commonly Missed Fractures in the Emergency Department
 Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Imaging of Lisfranc Injury
 November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
Biomechanics of Joints, Ligaments and Tendons.
 Hippocrates (460-377 B.C.) Biomechanics of Joints, s and Tendons. Course Text: Hamill & Knutzen (some in chapter 2 and 3, but ligament and tendon mechanics is not well covered in the text) Nordin & Frankel
Hippocrates (460-377 B.C.) Biomechanics of Joints, s and Tendons. Course Text: Hamill & Knutzen (some in chapter 2 and 3, but ligament and tendon mechanics is not well covered in the text) Nordin & Frankel
Clients w/ Orthopedic, Injury and Rehabilitation Concerns. Chapter 21
 Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Musculoskeletal Ultrasound Technical Guidelines. V. Knee
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines V. Knee Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines V. Knee Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Module F SKELETAL SYSTEM & ARTICULATIONS
 Module F SKELETAL SYSTEM & ARTICULATIONS Topic from General functions of bone & the skeletal system Structural components microscopic anatomy Structural components gross anatomy Physiology of embryonic
Module F SKELETAL SYSTEM & ARTICULATIONS Topic from General functions of bone & the skeletal system Structural components microscopic anatomy Structural components gross anatomy Physiology of embryonic
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Juvenile Dermatomyositis Joseph Junewick, MD FACR
 Juvenile Dermatomyositis Joseph Junewick, MD FACR 10/11/2015 History Child with several month history of weakness, arthralgias and palpable abnormalities at the knee Diagnosis Juvenile Dermatomyositis
Juvenile Dermatomyositis Joseph Junewick, MD FACR 10/11/2015 History Child with several month history of weakness, arthralgias and palpable abnormalities at the knee Diagnosis Juvenile Dermatomyositis
NURS 821 Alterations in the Musculoskeletal System. Rheumatoid Arthritis. Type III Hypersensitivity Response
 NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
Upper Limb QUESTIONS UPPER LIMB: QUESTIONS
 1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
Approach to Lower Extremity Osteomyelitis. A radiologic tour of a patient encounter
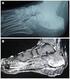 Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation
 167 Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation Richard F. Costello, DO a, *, Douglas P. Beall, MD a,b MAGNETIC RESONANCE IMAGING CLINICS Magn Reson Imaging Clin N
167 Nomenclature and Standard Reporting Terminology of Intervertebral Disk Herniation Richard F. Costello, DO a, *, Douglas P. Beall, MD a,b MAGNETIC RESONANCE IMAGING CLINICS Magn Reson Imaging Clin N
A Patient s Guide to Shoulder Pain
 A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
Dr Dan Gill Department of Radiology Windsor Regional Hospital Oxford Medical Imaging Erie St Clair Radiology
 Dr Dan Gill Department of Radiology Windsor Regional Hospital Oxford Medical Imaging Erie St Clair Radiology -5000 Olympic athletes and team officials -1350 Paralympic athletes and team officials -82
Dr Dan Gill Department of Radiology Windsor Regional Hospital Oxford Medical Imaging Erie St Clair Radiology -5000 Olympic athletes and team officials -1350 Paralympic athletes and team officials -82
Unit 4: Skeletal System Test Review Test Review
 Name: Period: Unit 4: Skeletal System Test Review Test Review 1. List four functions of the skeletal system: a. b. c. d. 2. Define ossification and identify the roles of the osteoblasts, osteocytes, and
Name: Period: Unit 4: Skeletal System Test Review Test Review 1. List four functions of the skeletal system: a. b. c. d. 2. Define ossification and identify the roles of the osteoblasts, osteocytes, and
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
(in: Skeletal Radiology - Vol. 30, n. 3 - March 2001)
 ACUTE AVULSION FRACTURES OF THE PELVIS IN ADOLESCENT COMPETITIVE ATHLETES: PREVALENCE, LOCATION AND SPORTS DISTRIBUTION OF 203 CASES COLLECTED Folco Rossi - Stefano Dragoni (in: Skeletal Radiology - Vol.
ACUTE AVULSION FRACTURES OF THE PELVIS IN ADOLESCENT COMPETITIVE ATHLETES: PREVALENCE, LOCATION AND SPORTS DISTRIBUTION OF 203 CASES COLLECTED Folco Rossi - Stefano Dragoni (in: Skeletal Radiology - Vol.
Structure & Function of the Knee. One of the most complex simple structures in the human body. The middle child of the lower extremity.
 Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Structure & Function of the Knee One of the most complex simple structures in the human body. The middle child of the lower extremity. Osteology of the Knee Distal femur (ADDuctor tubercle) Right Femur
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon to have a clear view of the
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Practical Aspects of Ultrasonography Assessment in Rheumatoid Arthritis
 Practical Aspects of Ultrasonography Assessment in Rheumatoid Arthritis Dr. Andrew K. Brown Senior Lecturer & Consultant Rheumatologist Content Practical RA Assessment Advantages of ultrasonography Potential
Practical Aspects of Ultrasonography Assessment in Rheumatoid Arthritis Dr. Andrew K. Brown Senior Lecturer & Consultant Rheumatologist Content Practical RA Assessment Advantages of ultrasonography Potential
Sports Radiology : Making a diagnosis or solving a problem
 Sports Radiology : Making a diagnosis or solving a problem Professor Dr John George University of Malaya Research Imaging Centre University of Malaya Medical Centre Kuala Lumpur, Malaysia. Abstract: Aim:
Sports Radiology : Making a diagnosis or solving a problem Professor Dr John George University of Malaya Research Imaging Centre University of Malaya Medical Centre Kuala Lumpur, Malaysia. Abstract: Aim:
Rehabilitation Guidelines for Meniscal Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW Health Sports Rehabilitation Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
RADIOGRAPHIC EVALUATION
 Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
Jeff Husband MD Objectives Evaluate, diagnose and manage common wrist injuries due to high energy trauma in athletes Appropriately use radiographs, CT scans and MRI Know when to refer patients for additional
CHS 06-07 BONES AND SKELETAL TISSUES
 CHS 06-07 BONES AND SKELETAL TISSUES This chapter provides a review of bone and skeletal tissue. The human skeleton is composed primarily of two connective tissues: (1) cartilage and (2) bone. CHARACTERISTICS
CHS 06-07 BONES AND SKELETAL TISSUES This chapter provides a review of bone and skeletal tissue. The human skeleton is composed primarily of two connective tissues: (1) cartilage and (2) bone. CHARACTERISTICS
Common Pediatric Fractures. Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014
 Common Pediatric Fractures Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014 Pediatric fractures 20% of injured kids found to have fracture on evaluation Between birth and
Common Pediatric Fractures Quoc-Phong Tran, MD UNSOM Primary Care Sports Medicine Fellow November 6, 2014 Pediatric fractures 20% of injured kids found to have fracture on evaluation Between birth and
Anterior Knee Pain: Patellofemoral Pain a review
 Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
Anterior Knee Pain: Patellofemoral Pain a review Overview Anatomy review A brief understanding of biomechanics The differential for anterior knee pain Pertinent history and physical Imaging which one and
Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understa
 Plantar Fasciitis Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understand why it occurs. Recognize the injury
Plantar Fasciitis Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understand why it occurs. Recognize the injury
Synopsis of Causation
 Ministry of Defence Synopsis of Causation Anterior Knee Pain Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Mr Jignesh Patel, University College Hospital, London September 2008
Ministry of Defence Synopsis of Causation Anterior Knee Pain Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Mr Jignesh Patel, University College Hospital, London September 2008
Aggressive vs. nonaggressive bone lesions. Anthony Pease, DVM, MS, DACVR
 Aggressive vs. nonaggressive bone lesions Anthony Pease, DVM, MS, DACVR The evaluation of the musculoskeletal system is difficult due to the numerous soft tissues as well as the bone structures involved.
Aggressive vs. nonaggressive bone lesions Anthony Pease, DVM, MS, DACVR The evaluation of the musculoskeletal system is difficult due to the numerous soft tissues as well as the bone structures involved.
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Syndesmosis Injuries
 Syndesmosis Injuries Dr. Alex Rabinovich Outline Anatomy Injury types and classification Treatment options Nonoperative vs. Operative Indications for operative Operative technique Postoperative management
Syndesmosis Injuries Dr. Alex Rabinovich Outline Anatomy Injury types and classification Treatment options Nonoperative vs. Operative Indications for operative Operative technique Postoperative management
Chapter 4 Physiological Therapeutics. 3 Therapeutic Ultrasound
 Chapter 4 Physiological Therapeutics 3 Therapeutic Ultrasound Therapeutic Ultrasound PHYSIOLOGIC EFFECTS OF ULTRASOUND 1. Increased collagen extensibility 5. Increased nerve conduction velocities 2. Increased
Chapter 4 Physiological Therapeutics 3 Therapeutic Ultrasound Therapeutic Ultrasound PHYSIOLOGIC EFFECTS OF ULTRASOUND 1. Increased collagen extensibility 5. Increased nerve conduction velocities 2. Increased
REHABILITATION OF TENDON AND LIGAMENT INJURIES
 REHABILITATION OF TENDON AND LIGAMENT INJURIES Carol Gillis, DVM, PhD, DACVSMR Equine Ultrasound & Rehabilitation carolgillis@earthlink.net www.equineultrasound.com 803-522-1700 The first step to healing
REHABILITATION OF TENDON AND LIGAMENT INJURIES Carol Gillis, DVM, PhD, DACVSMR Equine Ultrasound & Rehabilitation carolgillis@earthlink.net www.equineultrasound.com 803-522-1700 The first step to healing
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Musculoskeletal Ultrasound Technical Guidelines. II. Elbow
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines II. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines II. Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
HEEL PAIN. Differential diagnosis. 1. Insertional Plantar fascitis. 2. Enthesis. 3. Heel pad atrophy. 4. Tarsal tunnel syndrome
 HEEL PAIN Differential diagnosis 1. Insertional Plantar fascitis 2. Enthesis 3. Heel pad atrophy 4. Tarsal tunnel syndrome 5. Calcaneal stress fracture 6. Haglund s syndrome 7. Posterior ankle impingement
HEEL PAIN Differential diagnosis 1. Insertional Plantar fascitis 2. Enthesis 3. Heel pad atrophy 4. Tarsal tunnel syndrome 5. Calcaneal stress fracture 6. Haglund s syndrome 7. Posterior ankle impingement
Function of Bones. Bone Tissue and Bones BONE CLASSIFICATION. Long Bones Gross Anatomy. Lab Activity 1 - Gross Anatomy of a Long Bone
 Function of Bones Bone Tissue and Bones Bones form the framework of the skeleton. Anatomy and Physiology Text and Laboratory Workbook, Stephen G. Davenport, Copyright 2006, All Rights Reserved, no part
Function of Bones Bone Tissue and Bones Bones form the framework of the skeleton. Anatomy and Physiology Text and Laboratory Workbook, Stephen G. Davenport, Copyright 2006, All Rights Reserved, no part
Chapter 5. Objectives. Normal Ankle Range of Motion. Lateral Ankle Sprains. Lateral Ankle Sprains. Assessment of Lateral Ankle Sprains
 Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Cervical Spine: Postmortem Assessment of Accident Injuries Comparison of Radiographic, MR Imaging, Anatomic, and Pathologic Findings
 Cervical Spine: Postmortem Assessment of Accident Injuries Comparison of Radiographic, MR Imaging, Anatomic, and Pathologic Findings 1 Radiology, November, 2001;221:340-346. Axel Stäbler, MD, Jurik Eck,
Cervical Spine: Postmortem Assessment of Accident Injuries Comparison of Radiographic, MR Imaging, Anatomic, and Pathologic Findings 1 Radiology, November, 2001;221:340-346. Axel Stäbler, MD, Jurik Eck,
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013
 Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
Ankle Injury/Sprains in Youth Soccer Players Elite Soccer Community Organization (ESCO) November 14, 2013 Jeffrey R. Baker, DPM, FACFAS Weil Foot and Ankle Institute Des Plaines, IL Ankle Injury/Sprains
Skeletal system. 2012 Pearson Education, Inc.
 NURS1004 Week 6 Part I Prepared by Didy Button Skeletal system An Introduction to the Skeletal System The Skeletal System Includes: Bones of the skeleton Cartilages, ligaments, and connective tissues 6-1
NURS1004 Week 6 Part I Prepared by Didy Button Skeletal system An Introduction to the Skeletal System The Skeletal System Includes: Bones of the skeleton Cartilages, ligaments, and connective tissues 6-1
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Distal Radius Fractures. Lee W Hash, MD Affinity Orthopedics and Sports Medicine
 Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
Distal Radius Fractures Lee W Hash, MD Affinity Orthopedics and Sports Medicine The Problem of Distal Radius Fractures Common injury: >450,000/yr. in USA High potential for functional impairment and frequent
MR Imaging of the Anatomy of and Injuries to the Lateral and Posterolateral Aspects of the Knee
 Downloaded from www.ajronline.org by 37.44.192.158 on 07/15/16 from IP address 37.44.192.158. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
Downloaded from www.ajronline.org by 37.44.192.158 on 07/15/16 from IP address 37.44.192.158. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
Kne. Kne og Ultralyd. Kne og Ultralyd. Anatomi/Sonoanatomi
 Kne Modul 1 Oslo feb 2013 Frode Garmannvik- Ultralyd Trøndelag Kne og Ultralyd Diagnostisk Ultralyd på kne er ikke en foretrukket billeddiagnostisk metode for full oversikt over strukturer. Ligamenter,
Kne Modul 1 Oslo feb 2013 Frode Garmannvik- Ultralyd Trøndelag Kne og Ultralyd Diagnostisk Ultralyd på kne er ikke en foretrukket billeddiagnostisk metode for full oversikt over strukturer. Ligamenter,
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Wound and Skin Assessment. Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center
 Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Indications for Treatment: Indications for treatment include pain, swelling, instability, loss of mobility and function.
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy ICD 9 Codes: 844.1 Case Type / Diagnosis: The anatomy of the medial knee has been divided into 3 layers, consisting of
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy ICD 9 Codes: 844.1 Case Type / Diagnosis: The anatomy of the medial knee has been divided into 3 layers, consisting of
Animal Systems: The Musculoskeletal System
 Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
Animal Systems: The Musculoskeletal System Tissues, Organs, and Systems of Living Things Cells, Cell Division, and Animal Systems and Plant Systems Cell Specialization Human Systems The Digestive The Circulatory
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
Imaging of Sports Injuries
 Imaging of Sports Injuries Capable of tremendous mobility Paradox Must be loose enough to function but stable enough to prevent symptoms Shoulder injuries occur when the balance between stability & mobility
Imaging of Sports Injuries Capable of tremendous mobility Paradox Must be loose enough to function but stable enough to prevent symptoms Shoulder injuries occur when the balance between stability & mobility
Normal osseous anatomy. Hip is ball and socket joint stabilized by its intrinsic anatomy
 MRI of the HIP Normal osseous anatomy Hip is ball and socket joint stabilized by its intrinsic anatomy Normal osseous anatomy Acetabular labrum: ring closed by transverse ligament Ligaments Yellow / fatty
MRI of the HIP Normal osseous anatomy Hip is ball and socket joint stabilized by its intrinsic anatomy Normal osseous anatomy Acetabular labrum: ring closed by transverse ligament Ligaments Yellow / fatty
Head Position and Impact Direction in Whiplash Injuries: Associations with MRI-Verified Lesions of Ligaments and Membranes in the Upper Cervical Spine
 Head Position and Impact Direction in Whiplash Injuries: Associations with MRI-Verified Lesions of Ligaments and Membranes in the Upper Cervical Spine 1 Journal of Neurotrauma Volume 22, Number 11, November
Head Position and Impact Direction in Whiplash Injuries: Associations with MRI-Verified Lesions of Ligaments and Membranes in the Upper Cervical Spine 1 Journal of Neurotrauma Volume 22, Number 11, November
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
OS TRIGONUM SYNDROME. Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4.
 OS TRIGONUM SYNDROME Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4. Mechanism of Injury: Os trigonum syndrome occurs due to repetitive,
OS TRIGONUM SYNDROME Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4. Mechanism of Injury: Os trigonum syndrome occurs due to repetitive,
Definition: A joint or articulation is a place in the body where two bones come together.
 Definition: A joint or articulation is a place in the body where two bones come together. CLASSES OF JOINTS. 1. Joints are classified according to how the bones are held together. 2. The three types of
Definition: A joint or articulation is a place in the body where two bones come together. CLASSES OF JOINTS. 1. Joints are classified according to how the bones are held together. 2. The three types of
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY
 George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
Musculoskeletal Ultrasound Technical Guidelines. I. Shoulder
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines I. Shoulder Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines I. Shoulder Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
Thyroid Eye Disease. Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
DEVELOPMENT AND GROWTH OF THE MANDIBLE
 2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
Upper limb injuries. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries Traumatology RHS 231 Dr. Einas Al-Eisa Pain in the limbs: May be classified under 4 headings: 1. Joint pain 2. Soft tissue pain 3. Neurogenic pain 4. Orthopaedic causes (fractures,
Upper limb injuries Traumatology RHS 231 Dr. Einas Al-Eisa Pain in the limbs: May be classified under 4 headings: 1. Joint pain 2. Soft tissue pain 3. Neurogenic pain 4. Orthopaedic causes (fractures,
Youth Thrower s Elbow
 Youth Thrower s Elbow Description Youth Thrower s elbow is an inflammatory condition involving the growth plate of the humerus, near the inner elbow at the medial epicondyle.(figure 1) This condition is
Youth Thrower s Elbow Description Youth Thrower s elbow is an inflammatory condition involving the growth plate of the humerus, near the inner elbow at the medial epicondyle.(figure 1) This condition is
Section B: Epithelial Tissue 1. Where are epithelial tissues found within the body? 2. What are the functions of the epithelial tissues?
 Tissue worksheet Name Section A: Intro to Histology Cells are the smallest units of life. In complex organisms, cells group together with one another based on similar structure and function to form tissues.
Tissue worksheet Name Section A: Intro to Histology Cells are the smallest units of life. In complex organisms, cells group together with one another based on similar structure and function to form tissues.
Shoulder MRI for Rotator Cuff Tears. Conor Kleweno,, Harvard Medical School Year III Gillian Lieberman, MD
 Shoulder MRI for Rotator Cuff Tears Conor Kleweno,, Harvard Medical School Year III Goals of Presentation Shoulder anatomy Function of rotator cuff MRI approach to diagnose cuff tear Anatomy on MRI images
Shoulder MRI for Rotator Cuff Tears Conor Kleweno,, Harvard Medical School Year III Goals of Presentation Shoulder anatomy Function of rotator cuff MRI approach to diagnose cuff tear Anatomy on MRI images
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
7. Skeletal System: Bone Structure and Function
 7. Skeletal System: Bone Structure and Function For the next two chapters (7 and 9) we will study the skeletal system. Although the major feature of this system is the bones, the skeletal system also consists
7. Skeletal System: Bone Structure and Function For the next two chapters (7 and 9) we will study the skeletal system. Although the major feature of this system is the bones, the skeletal system also consists
Knee Injuries in the Adolescent Population. Joshua Johnson, MD Sports Medicine Physician Knoxville Orthopedic Clinic
 Knee Injuries in the Adolescent Population Joshua Johnson, MD ports Medicine Physician Knoxville Orthopedic Clinic Knee Anatomy Knee Anatomy A proper working knowledge of knee anatomy is essential to diagnose
Knee Injuries in the Adolescent Population Joshua Johnson, MD ports Medicine Physician Knoxville Orthopedic Clinic Knee Anatomy Knee Anatomy A proper working knowledge of knee anatomy is essential to diagnose
A Guide to Heel Pain
 The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
The Knee: Problems and Solutions
 The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
CHARACTERSTIC RADIOGRAPHIC APPEARANCE
 OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
Imaging of Thoracic Endovascular Stent-Grafts
 Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
