How To Treat A Spinal Injury
|
|
|
- Beverly McDaniel
- 5 years ago
- Views:
Transcription
1 Emergency Neurological Life Support Traumatic Spine Injury Protocol Version: 1.1 Last Updated: 7/29/2014 Checklist & Communication
2 Traumatic Spine Injury Table of Contents Emergency Neurological Life Support... 1 Traumatic Spine Injury Protocol... 1 Checklist... 3 Communication... 3 Airway... 4 Who to Intubate... 4 How to Intubate... 4 Breathing... 5 Brief Neurological Examination... 6 As part of initial trauma survey... 6 Circulation... 7 Management of Hypotension: maintain MAP mm Hg for the first 7 days... 7 Clinical clearance... 9 Can the spine be cleared clinically?... 9 Unable to Clear Spine Clinically: May be ligamentous injury... 9 Decision Rules Canadian and NEXUS Rules Canadian C-Spine Rules NEXUS Rules: questions Image the C-Spine with CT CT is most sensitive for bony injury CT Imaging Positive: Reveals a fracture or suspicious Injury CT Shows No Fracture: No fracture or soft tissue swelling Initial Treatment of TSI The question of steroids Maintain Spine Immobilization Focus on stabilization until injury is confirmed absent Neurological Examination Focus on signs related to spinal cord injury Neurological Signs Present? Clinical finding supporting spine injury: Detailed Examination Sensory Examination: Is there a sensory level? Specific Syndromes: Depending on the level and nature of injury ASIA Impairment Scale: Important for prognosis Traumatic Spine Injury Cervical Spine Injury Who should be imaged How to "clear the cervical spine"... 20
3 Traumatic Spine Injury Page 3 Checklist Immobilize C-Spine and maintain precautions Keep SBP > 90 mmhg Administer supplemental O2 Consider early intubation Rule out other causes of hypotension, do not assume neurogenic shock Communication Age Mechanism of injury Basic neurologic exam Other injuries Hemodynamics and treatments administered CT scan and/or MRI results
4 Traumatic Spine Injury Page 4 Airway Who to Intubate Patients with TSI can be at exceptionally high risk of loss of airway due to a combination of: Airway edema Loss of diaphragmatic innervation (C3, C4, and C5 innervate the diaphragm) Failure to ventilate Loss of chest and abdominal wall strength All patients with a complete cervical TSI C1-C4 should be considered for early, elective intubation and mechanical ventilation. Patients with incomplete or lower injuries will have a high degree of variability in their ability to maintain adequate oxygenation and ventilation. General parameters for urgent intubation: Complaint of "shortness of breath", inability to "catch my breath", or breathlessness Vital Capacity < 10 ml/kg or decreasing vital capacity Appearance of "belly breathing" or "quad breathing" (abdomen goes out sharply with inspiration) When in doubt, it is better to intubate a patient with a cervical TSI electively rather than wait until it needs to be done emergently. Patients will typically develop worsening of their primary injury shortly after admission due to cord edema and progressive loss of muscle strength. Patients with very high (above C3) complete TSI will almost invariably suffer a respiratory arrest in the field and, if not intubated by pre hospital providers, typically present in cardiac arrest. How to Intubate Generally, patients with cervical TSI who require intubation should be intubated using an awake, fiberoptic approach by an experienced provider. Video laryngoscopy can be a reasonable alternative to fiberoptic intubations, especially in emergent scenarios, or if fiberoptic equipment is not available. Patients who require urgent or emergent intubation, should be intubated using rapid sequence intubation (see ENLS protocol Airway, Ventilation and Sedation). Special issues related to intubation in TSI: Aspiration precaution should always be taken as for any emergent intubation. Cervical in-line stabilization must be carefully maintained throughout all intubation attempts. No particular RSI regimen is preferred, but these patients will already have loss of vasomotor tone and therefore medications that diminish the catecholamine surge may result in hypotension and bradycardia.
5 Traumatic Spine Injury Page 5 Breathing Patients with TSI are at high risk of inadequate oxygenation and ventilation. This is due to a combination of factors: Loss of diaphragmatic function Loss of ability to cough and deep breathe due to loss of chest wall and abdominal musculature function Aspiration Retention of secretions Atelectasis Concomitant injuries (pulmonary contusions, pneumothorax) Supplemental oxygen should be supplied to all patients with cervical TSI. Hypoxia is extremely detrimental to patients with neurological injury. Noninvasive methods of ventilation should be used with caution as the inability to cough and clear secretions may lead to an increased risk of aspiration.
6 Traumatic Spine Injury Page 6 Brief Neurological Examination As part of initial trauma survey In trauma patients during the primary survey, this can be abbreviated to the patient's Glasgow Coma Scale (GCS), pupil size and reactivity, ability to move all four extremities, and any spinal cord injury level.
7 Traumatic Spine Injury Page 7 Circulation Patients with TSI (above T4) often develop neurogenic shock. The patient suffers a "sympathectomy" resulting in unopposed vagal tone. This leads to a distributive shock with hypotension and bradycardia. Patients are generally hypotensive with warm, dry skin. This is due to the loss of sympathetic tone resulting in an inability to redirect blood flow from the periphery to the core circulation. Bradycardia is a characteristic finding of neurogenic shock and can help to differentiate from other forms of shock. Care should be taken not to "assume" that a patient has neurogenic shock due to a lack of tachycardia, as young healthy people and patients on premorbid beta-blockers, etc. will often not manifest tachycardia in the setting of hemorrhage. As a general rule, the higher and more complete the injury, the more severe and refractory the neurogenic shock. These signs can be expected to last from one to three weeks. Patients may develop manifestations of neurogenic shock hours to days following injury due to progressive edema and ischemia of the spinal cord resulting in "ascension" of their injury. In the patient with traumatic injury, other sources of hypotension (hemorrhage, TBI) MUST be sought and ruled out. o Pitfall: "Spinal shock" has nothing to do with hemodynamics, but rather refers to the loss of deep tendon stretch reflexes because of the spinal injury. Management of Hypotension: maintain MAP mm Hg for the first 7 days First line treatment of neurogenic shock is always fluid resuscitation to maintain euvolemia. The loss of sympathetic tone leads to vasodilation and the need for in increase in the circulating blood volume ("filling the tank") Second line therapy once euvolemia is established includes pressors and/or inotropes. Norepinephrine - has both alpha and some beta activity thereby improving both blood pressure and bradycardia. Norepinephrine is the preferred agent. Phenylephrine - pure alpha agonist. Phenylephrine is commonly used and easily titrated. Lacks beta activity so does not treat bradycardia and may actually worsen it through reflexive mechanisms. Dopamine - need high doses (> 10 microgram/kg/min) for alpha effect, but does have significant beta effects at lower doses. May lead to inadvertent diuresis at lower doses exacerbating relative hypovolemia.
8 Traumatic Spine Injury Page 8 Epinephrine - An alpha and beta agonist. Epinephrine causes vasoconstriction and increased cardiac output. High doses are often required leading to inadvertent mucosal ischemia. Rarely used or needed. Dobutamine - beta agonist (inotrope) that can be useful when the loss of sympathetic tone causes cardiac dysfunction. Caution should be used in patients who are not adequately volume loaded as may cause hypotension. The American Association of Neurological Surgeons and the Congress of Neurological Surgeons' Guidelines for the Management of Acute Cervical Spine and Spinal Cord Injuries recommend as an option "Maintenance of mean arterial blood pressure at mm Hg for the first seven days following acute TSI to improve spinal cord perfusion." This recommendation should be carefully weighed in patients with concomitant injuries, and the potential risks of fluid overload and/or pressors. Institutional collaboration is recommended to develop best practice.
9 Traumatic Spine Injury Page 9 Clinical clearance Can the spine be cleared clinically? Depending on the patient's level of consciousness, one may be able to clear the patient s cervical spine clinically, if the patient has had either a negative CT scan, or did not meet NEXUS or Canadian Decision Rules criteria that recommend CT imaging. If the patient has a normal neurologic exam, and is alert and without pain, the cervical spine can be clinically cleared. This is done by removing the cervical collar and having the patient rotate their head 45 degrees to each side. If they are able to do this without significant pain, the C-Spine can be cleared. If there is significant pain or the patient cannot perform the entire movement, replace the cervical collar. If the patient has altered mental status that is expected to be transient (e.g. alcohol or drug intoxication), maintain cervical spine immobilization until reliable examination is possible (NEXUS or Canadian C-Spine Rules) and proceed through this algorithm from the beginning. Unable to Clear Spine Clinically: May be ligamentous injury If the action of self-imposed neck rotation 45 degrees to either side proves too painful to complete, ligamentous injury is a possibility. The cervical collar should be left in place and advanced imaging pursued (See section on Imaging). MRI may be of value to investigate ligamentous injury if the patient cannot be clinically cleared within the first few days of injury. The patient can also remain in a soft cervical immobilization collar for 1-2 weeks until a repeat exam or flexion-extension films can be performed.
10 Traumatic Spine Injury Page 10 Decision Rules Canadian and NEXUS Rules CT of the spine should be performed if any of the following are present: Significant associated injuries: Multiple trauma patient needs CT of head, chest, or abdomen/pelvis Intubated Depressed level of consciousness Neurological deficit referable to the spine, or complaints of bilateral parathesias Strong clinical suspicion of any spinal fracture Multiple fractures Pelvis fracture Significant head or facial trauma CT of the spine should be considered for significant mechanism of injury: Motor vehicle collision with speed exceeding 35 mph Ejection from vehicle Pedestrian, bicyclist, or motorcyclist struck and thrown Axial load injury (vehicle roll-over or diving injury) Fall in excess of 10 ft. Death at accident scene Patient Factors Age > 65 yr. DJD, ankylosing spondylitis, rheumatoid arthritis Depressed level of consciousness Known cervical spine injury If the mechanism is worrisome (clear history of neck injury or circumstances that have a reasonable likelihood of causing spinal trauma) one can consider using two validated clinical scales. These are the NEXUS Rules and the Canadian C-spine Rules. Each of these systems allows you to either move toward clinical clearance of the C-spine or escalate evaluation to spine imaging. Canadian C- Spine Rules These rules help one decide if spine imaging is indicated. First, consider any high-risk features; if none, examine any low risk features. If after considering all of the features, and
11 Traumatic Spine Injury Page 11 none apply, the patient can be cleared clinically and the cervical spine immobilization can be discontinued. Canadian High-risk Features Are there any high-risk factor that mandates radiography? Age > 65 yrs. or dangerous mechanism (fall from elevation over 3 ft. or 5 stairs)? An axial load to the head (e.g. diving)? A motor vehicle collision exceeding 100 km/hr. or with roll-over or ejection, or a collision involving a motorized recreational vehicle, or a bicycle collision? IF YES to ANY of the above, consider CT criteria for imaging next. If NO to ALL of the above, move on to Canadian Low Risk features below. Canadian Low-risk Features Do any of the following low risk features exist? Simple rear-end motor vehicle collision Sitting position in the emergency department Ambulatory at any time Delayed (not immediate) onset of neck pain Absence of midline cervical-spine tenderness If YES to ANY of the above, then proceed to testing of neck rotation. If NO to ALL of the above, then consider CT criteria for clearance. NEXUS Rules: 5 questions NEXUS Rules: These "rules" apply 5 criteria that used alone can help you clinically clear the cervical spine. These include the presence of spinal tenderness and presence of focal neurological deficit among other things. Use of the NEXUS rules is a reasonable protocol to clear the cervical spine; although we encourage you to look at the Canadian Rules as well. The NEXUS rules are: No posterior midline cervical-spine tenderness. No evidence of intoxication. A normal level of alertness. No focal neurological deficit. No painful distracting injuries.
12 Traumatic Spine Injury Page 12 If all of the above are true then you can clinically clear the cervical spine and remove the immobilization device. If any one or more is true, move on to the next step regarding spine imaging.
13 Traumatic Spine Injury Page 13 Image the C- Spine with CT CT is most sensitive for bony injury The patient meets criteria for CT imaging of the spine. Maintain C-spine immobilization throughout the imaging and transportation. CT Imaging Positive: Reveals a fracture or suspicious Injury The CT reveals a finding that is definitive (vertebral fracture) or suspicious (soft tissue swelling). Maintain C-spine immobilization Consult Spine surgeon (Neurosurgery or Orthopedic Surgery) Obtain MRI as indicated If neurological examination is compatible with spinal cord injury (myelopathy) or the patient complains of bilateral parathesias If the patient is alert with continued midline cervical spine tenderness or if the patient is expected to require prolonged cervical spinal immobilization (e.g. severe closed head injury), consider MRI for the possibility of anterior-posterior spinal ligamentous injury Perform MRI of the known or suspected areas of spinal cord injury CT Shows No Fracture: No fracture or soft tissue swelling The CT shows intact vertebrae and no evidence for soft tissue swelling around the spine. At this point it is okay to move toward clinical clearance of the cervical spine if possible.
14 Traumatic Spine Injury Page 14 Initial Treatment of TSI The question of steroids The mainstay of treatment for SCIs is decompression of the spinal cord to minimize additional injury from cord compression surgical stabilization of unstable ligamentous and bony injury minimizing the effect of secondary complications, such as venous thromboembolic disease, pressure ulcer prevention, respiratory failure, and infections. Place Foley catheter GI prophylaxis Steroids: The use of steroids following acute traumatic cervical spinal injury is likely ineffective and they are no longer used for the majority of TSI patients in most highvolume institutions. If steroids are to be used, the recommended regimen is methylprednisolone 30 mg/kg as a bolus, then 5.4 mg/kg/hr for 23 or 47 hours. Steroids are most often used in a patient with an incomplete injury and minimal risk factors for complications.
15 Traumatic Spine Injury Page 15 Maintain Spine Immobilization Focus on stabilization until injury is confirmed absent Appropriate care must be taken to provide spinal immobilization on scene. The spinal column should be immobilized until an unstable injury can be excluded. In the prehospital setting, patients are typically fitted with a cervical collar to provide cervical spinal column immobilization, and patients are subsequently transferred to the hospital on a backboard. If the patient is intoxicated and uncooperative with medical evaluation, chemical sedation may be indicated to assure proper protection of the spinal column and, more importantly, the spinal cord. As a general rule, the diagnosis and treatment of the majority of spine injuries can be deferred to address other life-threatening injuries, such as hemorrhage or intracranial mass lesions, as long as spine immobilization is maintained.
16 Traumatic Spine Injury Page 16 Neurological Examination Focus on signs related to spinal cord injury The neurological examination should focus on motor, sensory and rectal tone findings. If the patient has abnormality in any of these, the goal is to localize the lesion to the highest spinal level where you see dysfunction. Neurological Signs Present? Clinical finding supporting spine injury: Based on a neurological examination, there are findings consistent with a spinal cord injury. The include: weakness below the level of the spine injury sensory loss below the level of spine injury loss of rectal tone hyperreflexia or areflexia If present, one should image the spine with CT and maintain spine immobilization. Detailed Examination Here are a few motor and sensory "levels" as a guide (these refer to the myotome and dermatome respectively for these regions of dysfunction): Ten key muscles that should be tested and documented (grade each as grade 0-5*): C5- Biceps C6 - Extensor carpi radialis longus C7 - Triceps C8 - Flexor digitorum profundus T1 - Adductor digiti minimi L2 - Iliopsoas L3 - Quadriceps L4 - Tibialis anterior L5 - Extensor hallucis longus S1 - Gastrocnemius, soleus Sacral: voluntary anal contraction (present/absent) *Motor Strength Grading: 0 = no active movement 1 = muscle contraction 2 = movement thru ROM w/o gravity 3 = movement thru ROM against gravity
17 Traumatic Spine Injury Page 17 4 = movement against some resistance 5 = movement against full resistance Detailed examinations recommended by the American Spinal Injury Association can be found on their website. Sensory: C4 - deltoid T4 - nipple T10 - umbilicus Decreased rectal tone: may be the only sign of a spinal cord injury. Sensory Examination: Is there a sensory level? With light touch and/or pin, touch each dermatome beginning with C1 (posterior scalp) and move caudally to see if the patient has normal, diminished or absent sensory function at a particular level and below. Light touch and pain may be separated by 1-2 dermatomes; select the highest (cephalad) level as the sensory level. Test sacral sensory function with a pin; score it as normal, diminished or absent. Score deep anal sensation as present or absent. Specific Syndromes: Depending on the level and nature of injury There are several spinal cord injury syndromes that if present help indicate the extent and nature of the injury. Anterior Cord Syndrome - Loss of pain/temperature and motor but not light touch; due to contusion of the anterior cord or occlusion of the anterior spinal artery. It is associated with burst fractures of the spinal column with fragment retropulsion by the axial compression. Central Cord Syndrome - loss of cervical motor function with relative sparing of lower extremity strength. This is typically due to hyperextension injury in elderly patients with cervical stenosis. It is often not associated with a fracture; rather, buckling of the ligamentum flavum contuses the cord causing bleeding with the center of the cord. The amount of damage to the corticospinal tracts (which lie laterally) is variable and determines the amount of lower extremity weakness. Brown-Sequard Syndrome - hemiplegia, loss of ipsilateral light touch, and loss of contralateral pain/temperature sensation due to hemisection of the cord. Indicates a penetrating cord injury often from missile or knife, or a lateral mass fracture of the spine.
18 Traumatic Spine Injury Page 18 ASIA Impairment Scale: Important for prognosis The American Spinal Injury Association (ASIA) defined a 5-element scale that is prognostic of neurological recovery: A - Complete: No motor or sensory function in the lowest sacral segment. B - Incomplete: Sensory but not motor function is preserved in the lowest sacral segment. C - Incomplete: Less the one-half of the key muscles below the neurological spinal level have grade 3 or better strength. D - Incomplete: at least one-half of the key muscles below the neurological level have grade 3 or better strength. E - Sensory and motor function are normal. Complete injury (no sensory or motor function below a spinal level) has a worse prognosis; however, spinal shock can present this way. Incomplete injuries have better prognosis.
19 Traumatic Spine Injury Page 19 Traumatic Spine Injury Cervical Spine Injury Traumatic Spine Injury (TSI): This topic covers TSI as it relates to the cervical spine; many of the concepts apply to less common thoracic or lumbar spine trauma. One should suspect cervical spine injury when there is A worrisome mechanism Midline cervical spine tenderness Neurological findings consistent with acute spinal cord injury Initial management should include: Airway Breathing Circulation Immobilization Detailed examination Imaging, if necessary Treatment Notes: You may put the patient in reverse Trendelenburg if at risk for aspiration. Back boards should be used for transport only because of the risk of skin breakdown. Thoracic and lumbar immobilization can be accomplished in an ED stretcher or hospital bed. Topic Co-Chairs: William Knight, MD Deborah Stein, MD
20 Traumatic Spine Injury Page 20 Who should be imaged How to "clear the cervical spine" Point tenderness over a spinous process may indicate instability of the respective vertebral bone. Examine the entire spine by palpation or percussion; focal spine injury often produces highly focal tenderness. If focal tenderness is present, the patient may need a CT of the spine There are two recommended systems that help you determine who you can "clinically clear" from significant spine injury without imaging, and who you should perform CT/MRI to detect fractures or spine misalignment. These are the NEXUS and Canadian Rules.
Traumatic injuries SPINAL CORD. Causes of Traumatic SCI SYMPTOMS. Spinal Cord trauma can be caused by:
 Traumatic injuries SPINAL CORD Jennie Trkulja RN, BScN, ENC (c) Causes of Traumatic SCI Spinal Cord trauma can be caused by: MVC (most injuries) Gunshots Falls Stabbings Assaults Industrial accidents Sports
Traumatic injuries SPINAL CORD Jennie Trkulja RN, BScN, ENC (c) Causes of Traumatic SCI Spinal Cord trauma can be caused by: MVC (most injuries) Gunshots Falls Stabbings Assaults Industrial accidents Sports
Spine and Spinal Cord Injuries. William Schecter, MD
 Spine and Spinal Cord Injuries William Schecter, MD Anatomy of the Spine http://education.yahoo.com/reference/gray/fig/387.html Anatomy of the spine 7 cervical vertebrae 12 thoracic vertebrae 5 lumbar
Spine and Spinal Cord Injuries William Schecter, MD Anatomy of the Spine http://education.yahoo.com/reference/gray/fig/387.html Anatomy of the spine 7 cervical vertebrae 12 thoracic vertebrae 5 lumbar
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Field Evaluation of Cervical Spinal Injuries NCEMSF Conference 2010. Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS
 Field Evaluation of Cervical Spinal Injuries NCEMSF Conference 2010 Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Cervical Spinal Immobilization Standard of care for patients
Field Evaluation of Cervical Spinal Injuries NCEMSF Conference 2010 Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Cervical Spinal Immobilization Standard of care for patients
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Nursing. Management of Spinal Trauma. Content. Objectives. Objectives
 7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
CHAPTER 32 QUIZ. Handout 32-1. Write the letter of the best answer in the space provided.
 Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Sign up to receive ATOTW weekly - email [email protected]
 THE UNSTABLE CERVICAL SPINE ANAESTHESIA TUTORIAL OF THE WEEK 292 9 TH SEPTEMBER 2013 Dr Patrick Cowie and Professor Peter Andrews Western General Hospital Edinburgh, UK Correspondence to [email protected]
THE UNSTABLE CERVICAL SPINE ANAESTHESIA TUTORIAL OF THE WEEK 292 9 TH SEPTEMBER 2013 Dr Patrick Cowie and Professor Peter Andrews Western General Hospital Edinburgh, UK Correspondence to [email protected]
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine & Nervous System Trauma
 Spine & Nervous System Trauma Andrea L. Williams PhD, RN Emergency Education Specialist Clinical Associate Professor University of Wisconsin School of Nursing http://www.youtube.com/watch?v=g2tdp_7q3n4
Spine & Nervous System Trauma Andrea L. Williams PhD, RN Emergency Education Specialist Clinical Associate Professor University of Wisconsin School of Nursing http://www.youtube.com/watch?v=g2tdp_7q3n4
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng41
 Spinal injury: assessment and initial management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng41 NICE 2016. All rights reserved. Contents Recommendations... 3 1.1 Assessment and management
Spinal injury: assessment and initial management NICE guideline Published: 17 February 2016 nice.org.uk/guidance/ng41 NICE 2016. All rights reserved. Contents Recommendations... 3 1.1 Assessment and management
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
NEW YORK STATE IN-HOSPITAL CERVICAL SPINE CLEARANCE GUIDELINES IN BLUNT TRAUMA
 Page 1 of 5 NEW YORK STATE IN-HOSPITAL CERVICAL SPINE CLEARANCE GUIDELINES IN BLUNT TRAUMA STAC Evaluation Subcommittee Authors: Jamie S. Ullman, MD FACS, Matthew Bank, MD, FACS, Nelson Rosen, MD, FACS,
Page 1 of 5 NEW YORK STATE IN-HOSPITAL CERVICAL SPINE CLEARANCE GUIDELINES IN BLUNT TRAUMA STAC Evaluation Subcommittee Authors: Jamie S. Ullman, MD FACS, Matthew Bank, MD, FACS, Nelson Rosen, MD, FACS,
Michael J. Reihart, MD Chair Medical Advisory Committee Pennsylvania Emergency Health Services Council
 Douglas F. Kupas, MD, EMT-P Commonwealth EMS Medical Director Bureau of Emergency Medical Services PA Department of Health Michael J. Reihart, MD Chair Medical Advisory Committee Pennsylvania Emergency
Douglas F. Kupas, MD, EMT-P Commonwealth EMS Medical Director Bureau of Emergency Medical Services PA Department of Health Michael J. Reihart, MD Chair Medical Advisory Committee Pennsylvania Emergency
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
Objectives. Spinal Fractures: Classification Diagnosis and Treatment. Level of Fracture. Neuro exam Muscle Grading
 Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
LOW BACK PAIN EXAMINATION
 LOW BACK PAIN EXAMINATION John Petty, M.D. Medical Director Department of Physical Medicine & Rehabilitation Kettering Medical Center February 8, 2014 PRE-TEST QUESTION What part of the low back physical
LOW BACK PAIN EXAMINATION John Petty, M.D. Medical Director Department of Physical Medicine & Rehabilitation Kettering Medical Center February 8, 2014 PRE-TEST QUESTION What part of the low back physical
Guidelines for the Management of Acute Spinal Cord Injury Revised August 2004
 Guidelines for the Management of Acute Spinal Cord Injury Revised August 2004 University Mississippi Medical Center Section of Neurotrauma Department of Neurosurgery I. Introduction i. Trauma is the leading
Guidelines for the Management of Acute Spinal Cord Injury Revised August 2004 University Mississippi Medical Center Section of Neurotrauma Department of Neurosurgery I. Introduction i. Trauma is the leading
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
Emergency Neurological Life Support. Spinal Cord Compression. Version: 1.0 Last Updated: 8/3/2014. Checklist & Communication
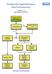 Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
Emergency Neurological Life Support 18 Spinal Cord Compression Version: 1.0 Last Updated: 8/3/2014 17 5 10 12 9 7 13 6 15 4 Checklist & Communication Spinal Cord Compression Page 2 Checklist Quadriplegia?
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
1) Understand best practices of spinal immobilization. 3) Open the conversation with your local medical director
 April 23, 2016 1) Understand best practices of spinal immobilization 2) Updated indications for use of backboard and C- collar 3) Open the conversation with your local medical director Disclaimer: This
April 23, 2016 1) Understand best practices of spinal immobilization 2) Updated indications for use of backboard and C- collar 3) Open the conversation with your local medical director Disclaimer: This
Management pathway: whiplash-associated disorders (WAD)
 Management pathway: whiplash-associated disorders (WAD) This management tool is a guide intended to assist general practitioners and health professionals delivering primary care to adults with acute or
Management pathway: whiplash-associated disorders (WAD) This management tool is a guide intended to assist general practitioners and health professionals delivering primary care to adults with acute or
Cervical Spine Imaging
 March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Medical Direction and Practices Board WHITE PAPER
 Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Medical Direction and Practices Board WHITE PAPER Use of Pressors in Pre-Hospital Medicine: Proper Indication and State of the Science Regarding Proper Choice of Pressor BACKGROUND Shock is caused by a
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Clearing the C Spine
 1. Introduction 2. Clinical Presentation 3. History 4. Physical Exam 5. Diagnosis 6. Investigations 7. Evaluation 8. Management 9. Reference 10. Acknowledgents Clearing the C Spine 1. Introduction: Injury
1. Introduction 2. Clinical Presentation 3. History 4. Physical Exam 5. Diagnosis 6. Investigations 7. Evaluation 8. Management 9. Reference 10. Acknowledgents Clearing the C Spine 1. Introduction: Injury
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
CERVICAL DISC HERNIATION
 CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
CERVICAL DISC HERNIATION Most frequent at C 5/6 level but also occur at C 6 7 & to a lesser extent at C4 5 & other levels In relatively younger persons soft disk protrusion is more common than hard disk
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. CP57 Version: V3
 GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
GUIDELINES FOR ASSESSMENT OF SPINAL STABILITY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: CP57 Version: V3 Dr V. Misra Accountable Committee: Acute Oncology Group Network
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Gilbert Varela, M.D., Inc 5232 E. Beverly Boulevard Los Angeles, California 90022 Phone: (323) 724-6911 Fax: (323) 724-6915
 Gilbert Varela, M.D., Inc 5232 E. Beverly Boulevard Los Angeles, California 90022 Phone: (323) 724-6911 Fax: (323) 724-6915 September 10, 2007 Law offices of xxxxxxxxx Santa Monica, CA 90405 REGARDING:
Gilbert Varela, M.D., Inc 5232 E. Beverly Boulevard Los Angeles, California 90022 Phone: (323) 724-6911 Fax: (323) 724-6915 September 10, 2007 Law offices of xxxxxxxxx Santa Monica, CA 90405 REGARDING:
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care. Clinical Management Guideline: Standard Trauma Resuscitation
 Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
C-Spine Injuries. Trauma Rounds
 C-Spine Injuries Trauma Rounds OUTLINE Introduction: Incidence, Importance Normal C-spine Anatomy Clinical Criteria for C-Spine X-rays Imaging Evaluation & Interpretation Fractures: Mechanism, Types, Management
C-Spine Injuries Trauma Rounds OUTLINE Introduction: Incidence, Importance Normal C-spine Anatomy Clinical Criteria for C-Spine X-rays Imaging Evaluation & Interpretation Fractures: Mechanism, Types, Management
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY
 THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY THE SPINAL CORD. A part of the Central Nervous System The nervous system is a vast network of cells, which carry information in the form
THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY THE SPINAL CORD. A part of the Central Nervous System The nervous system is a vast network of cells, which carry information in the form
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
International Standards for the Classification of Spinal Cord Injury Motor Exam Guide
 C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
Vasopressors. Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco
 Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
Vasopressors Judith Hellman, M.D. Associate Professor Anesthesia and Perioperative Care University of California, San Francisco Overview Define shock states Review drugs commonly used to treat hypotension
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Electrical Burns 新 光 急 診 張 志 華
 Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Weakness More diffuse More focal Atrophy Mild, general Severe, focal Atrophy versus weakness
 Spinal Cord Disorders (Dr. Merchut) Clinical signs and symptoms in spinal cord lesions 1. Motor signs and symptoms Lower motor neuron (LMN) signs (Table 1) are found in a limb if some of its muscles are
Spinal Cord Disorders (Dr. Merchut) Clinical signs and symptoms in spinal cord lesions 1. Motor signs and symptoms Lower motor neuron (LMN) signs (Table 1) are found in a limb if some of its muscles are
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
OVERVIEW. NEUROSURGICAL ASSESSMENT CERVICAL PROBLEMS Dirk G. Franzen, M.D. WHAT IS THE MOST IMPORTANT PART OF THE PHYSICAL EXAM?
 NEUROSURGICAL ASSESSMENT CERVICAL PROBLEMS Dirk G. Franzen, M.D. Neurological Surgery Bluegrass Orthopaedics and Hand Care OVERVIEW SCOPE OF THE PROBLEM PREVALENCE PATHOLOGY ANATOMIC CONSIDERATIONS ASSESSMENT
NEUROSURGICAL ASSESSMENT CERVICAL PROBLEMS Dirk G. Franzen, M.D. Neurological Surgery Bluegrass Orthopaedics and Hand Care OVERVIEW SCOPE OF THE PROBLEM PREVALENCE PATHOLOGY ANATOMIC CONSIDERATIONS ASSESSMENT
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
BACK PAIN PATHWAY DEFINTIONS
 BACK PAIN PATHWAY DEFINTIONS Cauda Equina Syndrome (CES) Current or imminent compression of the sacral nerve roots resulting in neurogenic bladder and bowel dysfunction. Symptoms typically include: severe
BACK PAIN PATHWAY DEFINTIONS Cauda Equina Syndrome (CES) Current or imminent compression of the sacral nerve roots resulting in neurogenic bladder and bowel dysfunction. Symptoms typically include: severe
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
The Anatomy of Spinal Cord Injury (SCI)
 The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Septic Shock: Pharmacologic Agents for Hemodynamic Support. Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident
 Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
Septic Shock: Pharmacologic Agents for Hemodynamic Support Nathan E Cope, PharmD PGY2 Critical Care Pharmacy Resident Objectives Define septic shock and briefly review pathophysiology Outline receptor
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
CERVICAL SPINE CLEARANCE
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
Head & Spinal Trauma. Lesson Goal. Lesson Objectives 9/10/2012
 Head & Spinal Trauma Lesson Goal Learn assessment of patients with head or spinal injuries and how to treat those injuries Lesson Objectives State nervous system components List central nervous system
Head & Spinal Trauma Lesson Goal Learn assessment of patients with head or spinal injuries and how to treat those injuries Lesson Objectives State nervous system components List central nervous system
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Thoracolumbar Spine Fractures. Outline. Outline. Holmes Criteria. Disclosure:
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION. ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements
 TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
ITLS & PHTLS: A Comparison
 ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
Do you have Back Pain? Associated with:
 Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
