Understanding Spinal Cord Injury, Part 2 Recovery and Rehabilitation
|
|
|
- Brian Fowler
- 8 years ago
- Views:
Transcription
1 Understanding Spinal Cord Injury, Part 2 Recovery and Rehabilitation January 2015 This fact sheet is the second in a two-part series in understanding spinal cord injury (SCI). Part one, The Body Before and After Injury, contains terms and information that are discussed in this fact sheet. SCI Fact Sheet Can paralysis caused by spinal cord injury be reversed? Everyone wants to know if there is a cure for spinal cord injury (SCI). There continues to be significant progress made toward this goal, but, despite any claim that there is a cure, there is currently no proven way to reverse paralysis. Will I gain any improvements? There are three areas for potential improvement after SCI. 1. Severity of Injury: At the time of your injury, your injury is graded as either complete or incomplete. Your grade my change. For example, you may be first classified as AIS C and improve to AIS D. 2. Levels of injury: At the time of your injury, you are diagnosed with a neurological level of injury. You may regain levels of injury over time. For example, you may be first classified with a C4 level of injury and improve to a C5 level. This means you gain control of more muscle movement. 3. Functional abilities: These are the activities you are capable of doing as you regain muscle strength and learn to use those muscles after injury. Pushing a wheelchair is one example. How much improvement will I gain? There is almost always hope for at least some improvement after SCI, but there are no guarantees. You have to wait to see what happens in the months after your injury. Here are a few rules of thumb. People with a complete injury often regain 1 or 2 levels of injury. This means you often regain control of 1 or 2 levels of muscle movement. People with an incomplete injury are more likely than people with a complete injury to regain control of more muscle movement, but there is no way to know how much, if any, will return. As long as you are seeing some improvement, like regaining muscle movement, your chances for improvement are better. The longer you go without seeing improvement, your chances for improvement are lower. The Spinal Cord Injury Model System is sponsored by the National Institute on Disability and Rehabilitation Research, Office of Special Education and Rehabilitative Services, U.S. Department of Education. (See model-system-centers for more information). What is Rehabilitation? Your body drastically changes after paralysis. You have medical needs that must be managed. You lose muscle movement and feeling. Plus, you probably have muscle weakness and fatigue after injury in the muscles that you can move. Simply put, you may not be able to do some daily living activities in the same way you did before your injury. Rehabilitation (rehab) is a medical service that can help you reach your full potential after injury. Every injury is different, so rehab is tailored to each person s needs. Skilled specialists provide the necessary services to help you make the most of your abilities. Physiatrists (pronounced fiz-eye-ah-trists) are rehab doctors who lead your treatment team and manage your medical care. Psychologists develop and apply treatment strategies in counseling to help you through your adjustment to life after injury. Nurses usually carry out orders from your doctor, and they often provide the essential education you need on how to manage issues like bowel and bladder management.
2 Physical therapists use a wide variety of techniques to help you regain the strength and stamina to maximize your physical abilities. Occupational therapists use a wide variety of techniques to help you increase and maintain your independence in carrying out your daily living activities. Speech-language pathologists (speech therapists) treat any issues that may develop with swallowing or speaking. Social workers link you and your family to information and resources that help ease your transition from in-patient rehabilitation to home and community living. What is my role in rehab? You have to put all of your effort into rehab to get the most out of it. You will work with your rehab team to set goals that are a realistic expectation of what you should be able to do with the muscle movement you have after injury. To reach your goals, you have to work as hard as you can with your rehab team to help you get stronger and learn the skills you need to manage daily activities and be independent. Some common goals include using a wheelchair, transferring, driving a car, bathing, eating, and dressing. Also, learn as much as you can about how to take care of yourself. Learn how to manage your daily concerns, such as bladder and bowel. Learn how to best prevent health problems like pressure ulcers, urinary tract infections, and pneumonia. Learn what you should do if you develop pain, autonomic dysreflexia, depression, or other medical problems. What advice can be offered from other people with SCI about rehab? People who have been injured and gone through rehab understand what you and your family are experiencing. They have been where you are now, and they can offer some valuable suggestions to help guide you during rehab. They offer the following advice. Trust your rehab team. Rehab professionals are very knowledgeable, and it is in your best interest to follow their advice in setting and reaching your goals. They can also advise you on how to best avoid many of the common setbacks people experience during rehab. For example, pressure ulcers can severely limit your ability to participate in rehab, but most pressure ulcers can be prevented if you do your weight shifts (also known as a pressure relief) as directed by your rehab team. Remember that who you are does not change after injury. You have the love and support of your family, friends, and others in your community. They can be a valuable support network in helping you reach your goals. Approach rehab with a balanced mindset. Everyone hopes they will regain all of their lost movement and feeling. However, the reality is that people are more likely to regain some, but not all, movement and feeling. This makes it very important that you participate in rehab to learn the skills necessary to have the healthiest and happiest life after SCI. Attending education classes will help you learn about SCI And how to take care of yourself. If you do regain everything, you have lost nothing in the process of learning those skills. If you do not regain everything, you will have the valuable knowledge and skills you need for everyday living. Be patient. SCI is a traumatic event that tears your life apart in an instant, and it takes time to rebuild your life after injury. Your body will need time to heal from the trauma of your injury. You will need time to regain the strength and stamina to reach your goals. However, you can do it in time. You will have bad days. It is only natural to feel sad, angry, or afraid at times. There may be times when it is hard to imagine how you can ever be happy after injury. However, most people do find happiness over time as they begin to realize they can live an active, healthy life. Take advantage of peer support. Your rehab team can likely arrange for you to talk with others who have SCI. They have been where you are and learned how to manage day-to-day activities. They can be a valuable source of information. There are also some online support networks. Here are a couple of recommended sites that have a focus in peer support. provides information and resources to meet the needs of people with SCI and their families and friends. is designed to provide Internet-based information and support for people with SCI and their families. The website has more than 1,000 videos of family members answering real-life questions about how they cope with SCI. Ask questions. You will probably have many questions. If you have questions, ask your rehab team. Most questions can be answered, but there may be some questions that cannot be answered. When it comes to regaining movement after injury, for example, sometimes it just takes time to see what happens.
3 What are my functional goals? There is a chart on the following pages that outlines common functional goals. These goals are daily activities that most people can manage with the control of muscle movement that they have with a complete injury. You may be able to do addition activities if you have an incomplete injury or if you regain control of more muscle movement. You will work with your rehab team to set your goals and find ways you can reach your goals. Below is a step-by-step guide to using the chart. 1. Find your level of injury in the Level of Injury column. 2. The Physical Abilities column shows what muscle movement is common for anyone with a complete injury at that level. 3. The Functional Goals column outlines how people might manage typical daily activities based at that level of injury. 4. The Equipment Used column suggests various equipment options that might be useful in accomplishing those functional goals. Level of C1 C3 C3 C4 C3 Limited movement of head and neck. Usually has head and neck control. At C4 level, may shrug shoulders. Breathing: Depends on ventilator for breathing. Communication: Talking is sometimes difficult, very limited, or impossible. If the ability to talk is limited, communication can be accomplished independently, with adaptive equipment. Daily tasks: Full assistance from caregiver for turning in bed, transfers, and all self-care (including bowel and bladder management). Assistive technology can allow for independence in such tasks as reading a book or newspaper, using a telephone, and operating lights and appliances. Mobility: Can operate an electric wheelchair by using a head control, mouth stick, sip and puff, or chin control. Can also operate a power tilt wheelchair also for independent pressure relief. Breathing: May initially require a ventilator for breathing; usually adjusts to breathing full time without ventilator assistance. Communication: Normal. Daily Tasks: Individual requires full assistance from a caregiver for turning in bed, transfers, and all self-care (including bowel and bladder management). Individual may be able to use adaptive equipment to eat independently. May also be able to operate an adjustable bed and perform other tasks, such as painting, writing, typing, and using a telephone with assistive technology. Mobility: Can operate a power wheelchair by using head control, a mouth stick, sip and puff, or chin control. Power tilt function on wheelchair allows for independence with pressure relief. Suction equipment to clear secretions, two ventilators with backup generator and battery Mouth stick and assistive technology (e.g., computer, communication board) for speech or typing Mouth stick, environmental control unit (ECU) Power or manual lift, electric or semielectric hospital bed, power wheelchair with pressure-relieving cushion Cough-assist device Eating: Sandwich holder on a gooseneck, feeder, long straw for liquids Other Activities: ECU for operating bed (e.g., head or voice activated, mouth stick controller), hands-free devices, mouth stick for typing, etc. Power or manual lift, electric or semielectric hospital bed, power wheelchair with pressure-relieving cushion
4 Level of C5 C6 Typically has head and neck control, can shrug shoulders, and has some shoulder control. Can bend elbows and turn palms face up. Has movement in head, neck, shoulders, arms, and wrists. Can shrug shoulders, bend elbows, turn palms up and down, and extend wrists. Daily Tasks: Individual can be independent with eating and grooming (e.g., face washing, oral care, shaving, make-up application) after setup from caregiver, with specialized equipment. Individuals will require total assistance from caregiver for bed mobility, transfers, and all other self-care. May be able to assist caregiver with upper body dressing and some bathing, with adaptive equipment. Health Care: Individual will require assistance from caregiver for cough assist. Can perform pressure relief with power tilt in power wheelchair. Mobility: May have strength to push a manual wheelchair for short distances over level surfaces; however, a power wheelchair with hand controls will be required for daily activities. At this level, the individual may be able to drive with specialized hand controls in a modified van with a lift, but still may require attendant to assist with transportation. Bowel and Bladder Management: Individual requires total assistance from caregiver for bowel and bladder management. Individual may have indwelling catheter or the caregiver may perform intermittent catheterization for bladder management. Bowel management can be performed with use of specialized equipment or medication. Daily Tasks: With use of some specialized equipment and setup from a caregiver, an individual can be independent with most feeding, grooming, and upper body dressing. Will still require some assistance for lower body dressing and will be able to assist with upper body during bathing. Can perform sliding board transfers to padded shower commode chair and/or tub bench for toileting and bathing, with some to total assist from caregiver. Can perform some light meal preparation tasks. Health Care: Can independently perform pressure relief with power tilt and may require some to no assist for forward or lateral lean pressure relief. Eating: Universal cuff for attachment of utensils, scoop plate, plate guard, long straw Grooming: Universal cuff for attachment of tooth brush, comb or brush, adapted or electric razor, makeup applicators; wash mitt for face Bathing: Roll-in padded shower and commode chair, or padded transfer tub bench; wash mitt; adapted loofah Cough-assist device Wheelchair: Power or manual lift, electric or semi-electric hospital bed, power wheelchair with pressurerelieving cushion Bed: Bed ladder, thigh straps, and bed rails used for bed mobility Bowel: Roll-in padded shower and commode chair, or padded transfer tub bench Bladder: Leg-bag emptier Feeding: Universal cuff, built-up utensils, scoop plate, long straw, plate guard Grooming: Universal cuff, adapted electric razor, or toothbrush Dressing: Dressing stick, leg lifter, thigh straps, dressing hook splints; adapted or specialized clothing Bathing: Adapted loofah, long-handled sponge with universal cuff Transfers: Power or manual lift, sliding board, padded drop-arm bedside commode, padded tub bench with cutout, padded shower and commode chair
5 Level of C7 T1 T2 T12 Has movement similar to C6 level, with the added ability to straighten elbows. At the C8 T1 level, has added strength and precision of hands and fingers. Has normal motor function in head, neck, shoulders, arms, hands, and fingers. Has increased use of rib and chest muscles, or trunk control. At the T10 T12 level, more improvements in trunk control due to increase in abdominal strength. Mobility: An individual may require some to no assist for turning in bed, with use of special equipment. May be able to perform sliding board transfers on level surfaces with some to no assistance from caregiver. Can use a ultra-lightweight manual wheelchair for mobility, but some may use a power wheelchair for greater ease over uneven terrain. Can be independent driving a vehicle from power or manual wheelchair with specialized equipment. Bowel and Bladder Management: Some to total assist with adaptive equipment for management of bowel and bladder. Daily Tasks: Independent with all feeding, grooming, and upper body dressing, with equipment. Individuals may require some to no assistance with lower body dressing and bathing with equipment. Can perform sliding board transfers with some to no assistance to padded shower commode chair and/or tub bench for toileting and bathing. Health Care: Independent with wheelchair pushup or lateral lean for pressure relief. Mobility: Independent with manual wheelchair propulsion and level surface sliding board transfers. Some assistance may be required from caregiver for uphill transfers. Can be independent with driving if able to load and unload wheelchair. Bowel and Bladder Management: Depending on hand function, some to total assist for bowel management, with use of adaptive equipment or medication. Can be independent or need some assist for bladder management with ICP or condom catheter. Daily Tasks: Independent with all self-care, including bowel and bladder management, with adaptive equipment if necessary. Health Care: Independent with wheelchair pushup for pressure relief. Bed: Bed ladder, thigh straps, bed rails Wheelchair: Wheelchair pegs, specialized wheelchair gloves, and rubber tubing on wheels. Also, powerassist wheels can be used for independence with manual wheelchair propulsion. Transportation: Modified van with lift, specialized hand controls, tie-downs Bowel: Digital stimulation splint device, enema insertion device Bladder: Catheter inserter, penis positioner, thigh spreader with mirror Feeding: Universal cuff, built-up handles, curved utensils, long straw, plate guard, adapted techniques for grasp Grooming: Universal cuff, splint material to adapt devices Dressing: Leg lifter, dressing stick, zipper pull, hooks on shoes Bathing: Adapted loofah, long-handled sponge with universal cuff Transfers: Sliding board, padded droparm bedside commode, padded tub bench with cutout, padded shower and commode chair Wheelchair: Rigid or folding lightweight wheelchair, wheelchair pegs, wheelchair gloves Transportation: Hand controls, modified van if unable to perform transfer or load unload chair Bowel: Digital stimulation splint device, enema insertion device, toileting aid Bladder: Catheter inserter house hold (for men), thigh spreader with mirror (for women) Dressing: Thigh straps, reacher, dressing stick, sock aid Bathing: Long-handled sponge Transfers: Sliding board, padded droparm bedside commode, padded tub bench with cutout, padded shower/commode chair Bowel/Bladder: Mirror
6 Level of L1 L5 S1 S5 Has additional return of motor movement in the hips and knees. Depending on level of injury, various degrees of return of voluntary bladder, bowel, and sexual function. Mobility: Independent with all bed mobility and transfers, with or without use of equipment. Independent with wheelchair propulsion on uneven and even surfaces and up and down curbs. Able to load and unload wheelchair independently for driving with hand controls. Mobility: Independent with all bed mobility and transfers with or without use of equipment. Independent with wheelchair propulsion on uneven and even surfaces and up and down curbs. Ambulation possible with use of specialized leg braces and walking devices. Functionality of ambulation depends on strength and movement in legs. Individuals ability to ambulate depends primarily on their level household distances. Individuals may use a wheelchair for community mobility. Able to load and unload wheelchair independently for driving with hand controls. Mobility: Increased ability to walk with fewer to no bracing or assistive devices. Wheelchair: Ultra-lightweight wheelchair Transfers: Sliding board, leg straps Transportation: Hand controls Wheelchair: Ultra-lightweight wheelchair if necessary. Walking: Leg braces that extend to the hip, the knee, or just the ankle/foot and varying assistive devices Transportation: Hand controls Walking: Braces that support the ankle/foot Authorship Understanding Spinal Cord Injury: Part 2 Recovery and Rehabilitation was developed by Phil Klebine, M.A.; Olivia Smitherman, M.O.T.R./L.; and Laney Gernenz, P.T. in collaboration with the Model Systems Knowledge Translation Center. Source: Portions of this document were adapted from materials developed by the UAB SCI Model System, Northwest Regional SCI System, Southeastern Regional Spinal Cord Injury Care System, Rocky Mountain Regional Spinal Injury System, and Paralyzed Veterans of America Consortium for Spinal Cord Medicine. Disclaimer: This information is not meant to replace the advice of a medical professional. You should consult your health care provider regarding specific medical concerns or treatment. The contents of this fact sheet were developed under a grant from the Department of Education, NIDRR grant number H133A However, those contents do not necessarily represent the policy of the Department of Education, and you should not assume endorsement by the federal government. Copyright 2015 Model Systems Knowledge Translation Center (MSKTC). May be reproduced and distributed freely with appropriate attribution. Prior permission must be obtained for inclusion in fee-based materials. More in the Understanding Spinal Cord Injury series: Part 1: The Body Before and After Spinal Cord Injury
FIM ITEM SCORING EXERCISE SHEETS 2015
 FIM EXERCISE - EATING The helper applies the universal cuff on to the patient s hand before she eats. The patient then brings food to her mouth, chews & swallows by herself. The helper scoops all food
FIM EXERCISE - EATING The helper applies the universal cuff on to the patient s hand before she eats. The patient then brings food to her mouth, chews & swallows by herself. The helper scoops all food
Patient s Handbook. Provincial Rehabilitation Unit ONE ISLAND HEALTH SYSTEM ONE ISLAND FUTURE 11HPE41-30364
 Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY
 SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY SELF CARE & ACTIVITIES OF DAILY LIVING Frazier Rehab and Neuroscience Center 220 Abraham Flexner Way Louisville, Kentucky Copyright 2007 (866) 540-7719
SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY SELF CARE & ACTIVITIES OF DAILY LIVING Frazier Rehab and Neuroscience Center 220 Abraham Flexner Way Louisville, Kentucky Copyright 2007 (866) 540-7719
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
Medical Rehabilitation. Rehabilitation Unit
 Medical Rehabilitation Rehabilitation Unit Medical Rehabilitation The purpose of this handout is to give you information about University Hospital s Rehabilitation Unit (2 North or 2N). It will explain:
Medical Rehabilitation Rehabilitation Unit Medical Rehabilitation The purpose of this handout is to give you information about University Hospital s Rehabilitation Unit (2 North or 2N). It will explain:
Adaptive Equipment: An Illustrated Guide
 Page 1 of 6 About Us Mission and Vision Statements Services Services Offered at NRHN Locations Directions to Hospital and Clinics Testimonials Messages from Other Patients Education Articles, Links and
Page 1 of 6 About Us Mission and Vision Statements Services Services Offered at NRHN Locations Directions to Hospital and Clinics Testimonials Messages from Other Patients Education Articles, Links and
Spinal Cord Injury Rehabilitation Program
 Workbook Spinal Cord Injury Rehabilitation Program Table of Contents Page Before coming to Rehab... 1 Tests before starting your Rehabilitation Program... 2 SCI Personal Goal Tracking Tool... 3 To do
Workbook Spinal Cord Injury Rehabilitation Program Table of Contents Page Before coming to Rehab... 1 Tests before starting your Rehabilitation Program... 2 SCI Personal Goal Tracking Tool... 3 To do
HELPFUL HINTS FOR A HEALTHY BACK
 HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
Physiotherapy Database Exercises for people with Spinal Cord Injury
 Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Indications for a PMD as Reasonable and Necessary and Types of PMD Categories Available
 Appendix K The face-to-face examination provides the clinical information needed to determine if a patient needs a Power Mobility Device (PMD) and what type of PMD may be needed. This information needs
Appendix K The face-to-face examination provides the clinical information needed to determine if a patient needs a Power Mobility Device (PMD) and what type of PMD may be needed. This information needs
my personal joint profile Your own personal profile of how rheumatoid arthritis is affecting your joints.
 my personal joint profile Your own personal profile of how rheumatoid arthritis is affecting your joints. What you and your rheumatologist can learn from your joint profile. It seems like a simple question:
my personal joint profile Your own personal profile of how rheumatoid arthritis is affecting your joints. What you and your rheumatologist can learn from your joint profile. It seems like a simple question:
Provincial Rehabilitation Unit. Patient Handbook
 Provincial Rehabilitation Unit Patient Handbook ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM Welcome to Unit 7, the Provincial Rehabilitation Unit. This specialized 20 bed unit is staffed by an interdisciplinary
Provincial Rehabilitation Unit Patient Handbook ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM Welcome to Unit 7, the Provincial Rehabilitation Unit. This specialized 20 bed unit is staffed by an interdisciplinary
Mobility After Stroke
 Mobility After Stroke Issues facing stroke survivors and their families Regaining Mobility Moving around safely and easily is not something you may think about, until you have had a stroke. Each year more
Mobility After Stroke Issues facing stroke survivors and their families Regaining Mobility Moving around safely and easily is not something you may think about, until you have had a stroke. Each year more
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
COLLABORATIVE NURSING DOCUMENTATION
 COLLABORATIVE NURSING DOCUMENTATION The following section is designed to assist the clinician in providing information to the nursing staff in effort to facilitate collaborative nursing documentation regarding
COLLABORATIVE NURSING DOCUMENTATION The following section is designed to assist the clinician in providing information to the nursing staff in effort to facilitate collaborative nursing documentation regarding
INPATIENT REHABILITATION SERVICES
 MOVE. GROW. LIVE. INPATIENT REHABILITATION SERVICES THE IMPORTANCE OF CHOOSING THE RIGHT RECOVERY PARTNER. You do have a choice when it comes to inpatient rehabilitation, and the decision you make can
MOVE. GROW. LIVE. INPATIENT REHABILITATION SERVICES THE IMPORTANCE OF CHOOSING THE RIGHT RECOVERY PARTNER. You do have a choice when it comes to inpatient rehabilitation, and the decision you make can
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Project Ready Occupational Therapy
 Project Ready Occupational Therapy What is Occupational Therapy? The goal of occupational therapy is to help patients with physical and/or mental disabilities to become as independent as possible with
Project Ready Occupational Therapy What is Occupational Therapy? The goal of occupational therapy is to help patients with physical and/or mental disabilities to become as independent as possible with
Types of Home Health Care Services You Need
 Types of Home Health Care Services You Need You may receive one type or many depending on your needs. Care may be provided by one source or by several sources. Work with your physician, clinic staff, or
Types of Home Health Care Services You Need You may receive one type or many depending on your needs. Care may be provided by one source or by several sources. Work with your physician, clinic staff, or
Cardiac Rehab Program: Stretching Exercises
 Cardiac Rehab Program: Stretching Exercises Walk around the room, step side to side, ride a bike or walk on a treadmill for at least 5 minutes to warm up before doing these stretches. Stretch warm muscles
Cardiac Rehab Program: Stretching Exercises Walk around the room, step side to side, ride a bike or walk on a treadmill for at least 5 minutes to warm up before doing these stretches. Stretch warm muscles
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Expected Outcomes: What You Should Know
 C6 CONSUMER GUIDE: EXPECTED OUTCOMES SPINAL CORD MEDICINE Expected Outcomes: What You Should Know A Guide for People with C6 Spinal Cord Injury Administrative and financial support provided by Paralyzed
C6 CONSUMER GUIDE: EXPECTED OUTCOMES SPINAL CORD MEDICINE Expected Outcomes: What You Should Know A Guide for People with C6 Spinal Cord Injury Administrative and financial support provided by Paralyzed
Strengthening Exercises - Below Knee Amputation
 Strengthening Exercises - Below Knee Amputation These exercises will help you strengthen your muscles to best use your prosthetic leg. Do these exercises as directed by your therapist or doctor. Do the
Strengthening Exercises - Below Knee Amputation These exercises will help you strengthen your muscles to best use your prosthetic leg. Do these exercises as directed by your therapist or doctor. Do the
Brachial Plexus Palsy
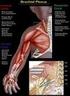 Patient and Family Education Brachial Plexus Palsy A Therapy Guide for Your Baby Brachial Plexus Palsy is caused by trauma to the nerves of the arm. This trauma may have caused muscle weakness, lack of
Patient and Family Education Brachial Plexus Palsy A Therapy Guide for Your Baby Brachial Plexus Palsy is caused by trauma to the nerves of the arm. This trauma may have caused muscle weakness, lack of
Good Samaritan Inpatient Rehabilitation Program
 Good Samaritan Inpatient Rehabilitation Program Living at your full potential. Welcome When people are sick or injured, our goal is their maximum recovery. We help people live to their full potential.
Good Samaritan Inpatient Rehabilitation Program Living at your full potential. Welcome When people are sick or injured, our goal is their maximum recovery. We help people live to their full potential.
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY
 SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY Frazier Rehab and Neuroscience Center 220 Abraham Flexner Way Louisville, Kentucky Copyright 2007 (866) 540-7719 (Toll Free) (502) 582-7495 www.spinalcordmedicine.com
SPINAL CORD MEDICINE HANDBOOK FOR PATIENT AND FAMILY Frazier Rehab and Neuroscience Center 220 Abraham Flexner Way Louisville, Kentucky Copyright 2007 (866) 540-7719 (Toll Free) (502) 582-7495 www.spinalcordmedicine.com
Shoulder Replacement Surgery Patient Information Manual
 Shoulder Replacement Surgery Patient Information Manual Maximizing Your New Shoulder UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute www.rehabcenters.ufhealth.org
Shoulder Replacement Surgery Patient Information Manual Maximizing Your New Shoulder UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute www.rehabcenters.ufhealth.org
Welcome to your LOW BACK PAIN treatment guide
 Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Spinal Cord Injury Program
 Spinal Cord Injury Information Series PATIENT & FAMILY GUIDE Spinal Cord Injury Program A Service of Santa Clara Valley Medical Center Rehabilitation and 1-Center What You Should Know What is 1-Center?
Spinal Cord Injury Information Series PATIENT & FAMILY GUIDE Spinal Cord Injury Program A Service of Santa Clara Valley Medical Center Rehabilitation and 1-Center What You Should Know What is 1-Center?
Spinal Cord Injury: Basic Facts... 1. Spinal Column Anatomy: The Basics... 3. ASIA/ISCoS Exam and Grade... 8. Glossary of Terms You May Hear...
 Table of Contents Spinal Cord Injury: Basic Facts... 1 Spinal Column Anatomy: The Basics... 3 Levels of Injury... 4 ASIA/ISCoS Exam and Grade... 8 Glossary of Terms You May Hear... 9 Questions Families
Table of Contents Spinal Cord Injury: Basic Facts... 1 Spinal Column Anatomy: The Basics... 3 Levels of Injury... 4 ASIA/ISCoS Exam and Grade... 8 Glossary of Terms You May Hear... 9 Questions Families
Inpatient Rehabilitation
 Inpatient Rehabilitation Patient Handbook 2601 Electric Avenue, Port Huron, MI 48060 810-985-1500 mymercy.us SJMPH 12-12 300 My Rehabilitation Team Physician Nurse Case Manager Physical Therapist Occupational
Inpatient Rehabilitation Patient Handbook 2601 Electric Avenue, Port Huron, MI 48060 810-985-1500 mymercy.us SJMPH 12-12 300 My Rehabilitation Team Physician Nurse Case Manager Physical Therapist Occupational
Shoulder Extension Exercise Using Theraband
 Shoulder Extension Exercise Using Theraband Loop the theraband around the stable surface at chest height Lift your chest and pull your arm behind you Keep your neck long and relaxed Make sure you keep
Shoulder Extension Exercise Using Theraband Loop the theraband around the stable surface at chest height Lift your chest and pull your arm behind you Keep your neck long and relaxed Make sure you keep
Stem cell transplant, you and your rehabilitation Information for patients and their carers
 Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
APPENDIX A. Sets = the completion of one consecutive grouping of repetitions of an exercise.
 Exercise Instruction Sheet Instructions: APPENDIX A Exercises are to be performed 3 times per week. Allow one rest day between each exercise day. You may divide the exercises into groups and perform them
Exercise Instruction Sheet Instructions: APPENDIX A Exercises are to be performed 3 times per week. Allow one rest day between each exercise day. You may divide the exercises into groups and perform them
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
UW MEDICINE PATIENT EDUCATION. Your Care Team. Helpful information
 UW MEDICINE PATIENT EDUCATION Your Care Team Helpful information In this section: You: The Patient Medical Staff Nursing Staff Allied Health Professionals Support Staff Peer Mentors for People with Spinal
UW MEDICINE PATIENT EDUCATION Your Care Team Helpful information In this section: You: The Patient Medical Staff Nursing Staff Allied Health Professionals Support Staff Peer Mentors for People with Spinal
Do s and Don ts with Low Back Pain
 Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
Occupational therapy after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
HOPE EXERCISE RECOVERY RESOURCES RELATIONSHIPS INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RELATIONSHIPS MOVEMENT. A Stroke Recovery Guide
 INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
Otago Exercise Program
 Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Sue Schuerman, PT, GCS, PhD UNLVPT
 Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Basic Training Exercise Book
 Basic Training Exercise Book Basic Training Exercise Book Instructions The exercises are designed to challenge the major muscles groups every day, approximately every 2 to 3 hours., for a total of 6 times
Basic Training Exercise Book Basic Training Exercise Book Instructions The exercises are designed to challenge the major muscles groups every day, approximately every 2 to 3 hours., for a total of 6 times
MVA Accident Information
 In this Report MVA Accident Information... 1 Vehicle Information... 3 Vehicular and Patient Relationship.. 4 Facts about the Patient before the MVA Accident... 4 Facts about the Patient during this MVA
In this Report MVA Accident Information... 1 Vehicle Information... 3 Vehicular and Patient Relationship.. 4 Facts about the Patient before the MVA Accident... 4 Facts about the Patient during this MVA
Rehabilitation and Choosing a Rehab Center
 The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453457/k.a4cb/overview How_to_Pick_a_Rehab.htm
The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453457/k.a4cb/overview How_to_Pick_a_Rehab.htm
Physical Capability Strength Test: One Component of the Selection Process
 Physical Capability Strength Test: One Component of the Selection Process One aspect of the Power Systems Institute selection process is to successfully complete and achieve a passing score on a physical
Physical Capability Strength Test: One Component of the Selection Process One aspect of the Power Systems Institute selection process is to successfully complete and achieve a passing score on a physical
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Pre-operative Instructions for MIS Total Knee Stephen J Kelly, M.D.
 Pre-operative Instructions for MIS Total Knee Stephen J Kelly, M.D. 33 Sewall Street Portland, ME 04102 207.828.2100 800.439.0274 www.orthoassociates.com Pre-operative Pain Protocol Two days before surgery:
Pre-operative Instructions for MIS Total Knee Stephen J Kelly, M.D. 33 Sewall Street Portland, ME 04102 207.828.2100 800.439.0274 www.orthoassociates.com Pre-operative Pain Protocol Two days before surgery:
Rehabilitation Center
 Rehabilitation Center PATIENT INFORMATION Welcome to Ministry Saint Joseph s Hospital At Ministry Health Care, we earn trust by working together as One Ministry to keep PATIENTS FIRST in everything we
Rehabilitation Center PATIENT INFORMATION Welcome to Ministry Saint Joseph s Hospital At Ministry Health Care, we earn trust by working together as One Ministry to keep PATIENTS FIRST in everything we
Rehabilitation Medicine Clinic. New Patient Questionnaire
 Rehabilitation Medicine Clinic (Please complete this 5-page form and bring to your appointment.) Date Appt. Date Age Date of Birth Name Male Female Hand dominance: R L Home Address Home Phone ( ) Work
Rehabilitation Medicine Clinic (Please complete this 5-page form and bring to your appointment.) Date Appt. Date Age Date of Birth Name Male Female Hand dominance: R L Home Address Home Phone ( ) Work
Info. from the nurses of the Medical Service. LOWER BACK PAIN Exercise guide
 Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Otago Exercise Program Activity Booklet
 Head Movements Stand up tall and look ahead. Slowly turn your head as far as you can to the right. Slowly turn your head as far as you can to the left. Repeat five times to each side. 44 Neck Movements
Head Movements Stand up tall and look ahead. Slowly turn your head as far as you can to the right. Slowly turn your head as far as you can to the left. Repeat five times to each side. 44 Neck Movements
Injury Prevention for the Back and Neck
 Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Rehabilitation Where You Recover. Inpatient Rehabilitation Services at Albany Medical Center
 Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
back care TIPS FOR DAILY ACTIVITIES
 back care TIPS FOR DAILY ACTIVITIES TIPS FOR DAILY ACTIVITIES INTRODUCTION When your back hurts, the way you hold and move your body is important. Your muscles can become more tense and painful depending
back care TIPS FOR DAILY ACTIVITIES TIPS FOR DAILY ACTIVITIES INTRODUCTION When your back hurts, the way you hold and move your body is important. Your muscles can become more tense and painful depending
Rotator Cuff and Shoulder Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Rehabilitation. Among the professions you can expect to find on a rehabilitation team:
 The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453457/k.a4cb/overview How_to_Pick_a_Rehab.htm
The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453457/k.a4cb/overview How_to_Pick_a_Rehab.htm
Rehabilitation Exercises for Shoulder Injuries Pendulum Exercise: Wal Walk: Back Scratcher:
 Rehabilitation Exercises for Shoulder Injuries Begin these exercises when your pain has decreased about 25% from the time when your injury was most painful. Pendulum Exercise: Lean over with your uninjured
Rehabilitation Exercises for Shoulder Injuries Begin these exercises when your pain has decreased about 25% from the time when your injury was most painful. Pendulum Exercise: Lean over with your uninjured
How To Improve Drainage
 Rehabilitation Home Program Edema Exercises To Improve Drainage You will improve your lymph flow by doing a few exercises each day. These exercises are an important part of your home program. They may
Rehabilitation Home Program Edema Exercises To Improve Drainage You will improve your lymph flow by doing a few exercises each day. These exercises are an important part of your home program. They may
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
General Guidelines. Neck Stretch: Side. Neck Stretch: Forward. Shoulder Rolls. Side Stretch
 Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Fact sheet Exercises for older adults undergoing rehabilitation
 Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Lifting & Moving Patients. Lesson Goal. Lesson Objectives 9/10/2012
 Lifting & Moving Patients Lesson Goal Learn the correct techniques, equipment, & positioning for moving patients safely and effectively in a variety of situations &locations Lesson Objectives Define body
Lifting & Moving Patients Lesson Goal Learn the correct techniques, equipment, & positioning for moving patients safely and effectively in a variety of situations &locations Lesson Objectives Define body
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY / PROCEDURE:
 PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
PARTNERSHIP HEALTHPLAN OF CALIFORNIA POLICY/PROCEDURE Policy Number: MCUP3003 (previously UP100303) Reviewing Entities: Credentialing IQI P & T QUAC Approving Entities: BOARD CEO COMPLIANCE FINANCE PAC
Inpatient Rehabilitation Guidebook
 Inpatient Rehabilitation Guidebook Welcome to Alta Bates Summit Medical Center s Regional Rehabilitation Program Our experienced and caring team will provide you with outstanding care as you begin your
Inpatient Rehabilitation Guidebook Welcome to Alta Bates Summit Medical Center s Regional Rehabilitation Program Our experienced and caring team will provide you with outstanding care as you begin your
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
Sun Retirement Health Assist
 Sun Retirement Health Assist product FEATURE SHEET Sun Retirement Health Assist provides an income-style benefit if you become unable to care for yourself due to aging, an accident, illness or deteriorated
Sun Retirement Health Assist product FEATURE SHEET Sun Retirement Health Assist provides an income-style benefit if you become unable to care for yourself due to aging, an accident, illness or deteriorated
Patient handling techniques to prevent MSDs in health care
 28 Introduction Patient handling techniques Work-related musculoskeletal disorders (MSDs) are a serious problem among hospital personnel, and in particular the nursing staff. Of primary concern are back
28 Introduction Patient handling techniques Work-related musculoskeletal disorders (MSDs) are a serious problem among hospital personnel, and in particular the nursing staff. Of primary concern are back
AFTER TOTAL KNEE REPLACEMENT. Living with Your New Knee
 AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS:
 LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
LESSON TOPIC: AVERAGE TIME: BACK INJURY PREVENTION 30 Minutes INSTRUCTIONAL MATERIALS: REFERENCES: a. PAEC School Safety Manual b. Any locally produced Back Injury pamphlet TRAINING AIDS: a. Handout #1
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
SCI Rehab. Stages of Pressure Sores. Prevention of Pressure Sores Develop due to pressure on skin, lack of blood supply, tissue death.
 SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
Lateral pterygoid muscle Medial pterygoid muscle
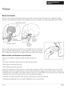 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
Parkinson s Disease. Signs. Your Care
 Parkinson s Disease Parkinson s disease affects the part of the brain that controls muscle movement. The exact cause of this disease is not known, but there is a decrease in a chemical called dopamine
Parkinson s Disease Parkinson s disease affects the part of the brain that controls muscle movement. The exact cause of this disease is not known, but there is a decrease in a chemical called dopamine
GRASP. Graded Repetitive Arm Supplementary Program. Exercise manual. Level. This research project is funded by UBC and the Heart and Stroke Foundation
 GRASP Graded Repetitive Arm Supplementary Program Exercise manual Level 1 This research project is funded by UBC and the Heart and Stroke Foundation 1 Welcome to the Grasp study! Thank you for volunteering
GRASP Graded Repetitive Arm Supplementary Program Exercise manual Level 1 This research project is funded by UBC and the Heart and Stroke Foundation 1 Welcome to the Grasp study! Thank you for volunteering
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Exercise 1: Knee to Chest. Exercise 2: Pelvic Tilt. Exercise 3: Hip Rolling. Starting Position: Lie on your back on a table or firm surface.
 Exercise 1: Knee to Chest Starting Position: Lie on your back on a table or firm surface. Action: Clasp your hands behind the thigh and pull it towards your chest. Keep the opposite leg flat on the surface
Exercise 1: Knee to Chest Starting Position: Lie on your back on a table or firm surface. Action: Clasp your hands behind the thigh and pull it towards your chest. Keep the opposite leg flat on the surface
Admission to Inpatient Rehabilitation (Rehab) Services
 Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Why Back Safety is Important
 Back Safety Why Back Safety is Important Back injuries are considered by OSHA (the Occupational Safety and Health Administration) as the nation's #1 workplace safety problem. Back Injuries are often: Very
Back Safety Why Back Safety is Important Back injuries are considered by OSHA (the Occupational Safety and Health Administration) as the nation's #1 workplace safety problem. Back Injuries are often: Very
How To Manage A Catastrophic Injury
 Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
Guidelines for levels of attendant care for people with spinal cord injury
 Guidelines for levels of attendant care for people with spinal cord injury FOR USE IN THE NSW MOTOR ACCIDENTS SCHEME,AND LIFETIME CARE & SUPPORT SCHEME CONTENTS Introduction 2 Background 2 Using these
Guidelines for levels of attendant care for people with spinal cord injury FOR USE IN THE NSW MOTOR ACCIDENTS SCHEME,AND LIFETIME CARE & SUPPORT SCHEME CONTENTS Introduction 2 Background 2 Using these
Guidelines for levels of attendant care for people who have spinal cord injury and can claim under the New South Wales Motor Accidents Scheme
 Guidelines for levels of attendant care for people who have spinal cord injury and can claim under the New South Wales Motor Accidents Scheme March 2002 ISBN 1 876958 09 X Published by Motor Accidents
Guidelines for levels of attendant care for people who have spinal cord injury and can claim under the New South Wales Motor Accidents Scheme March 2002 ISBN 1 876958 09 X Published by Motor Accidents
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Rehabilitation Center
 WELCOME TO OUR PATIENTS AND FAMILIES Rehabilitation Center NEIGHBORS HELPING NEIGHBORS IN THE COMMUNITY Location: REHABILITATION CENTER AT EL CAMINO HOSPITAL LOS GATOS 355 Dardanelli Lane (off Knowles
WELCOME TO OUR PATIENTS AND FAMILIES Rehabilitation Center NEIGHBORS HELPING NEIGHBORS IN THE COMMUNITY Location: REHABILITATION CENTER AT EL CAMINO HOSPITAL LOS GATOS 355 Dardanelli Lane (off Knowles
Activities of Daily Living
 Activities of Daily Living About this domain ADLs To identify the need for support in completing basic daily activities including eating, bathing, dressing, personal hygiene/grooming, toileting, mobility,
Activities of Daily Living About this domain ADLs To identify the need for support in completing basic daily activities including eating, bathing, dressing, personal hygiene/grooming, toileting, mobility,
Australian Centre for Agricultural Health and Safety. Farming with Back Pain
 Australian Centre for Agricultural Health and Safety Farming with Back Pain 2008 Australian Centre for Agricultural Health and Safety All rights reserved Title: Farming with Back Pain Authors: Boughton
Australian Centre for Agricultural Health and Safety Farming with Back Pain 2008 Australian Centre for Agricultural Health and Safety All rights reserved Title: Farming with Back Pain Authors: Boughton
Aquatic Exercises: Upper Body Strengthening
 Aquatic Exercises: Upper Body Strengthening These exercises will strengthen your muscles in your arms, shoulders, chest and neck. Exercising in water allows you to have less stress on your joints. When
Aquatic Exercises: Upper Body Strengthening These exercises will strengthen your muscles in your arms, shoulders, chest and neck. Exercising in water allows you to have less stress on your joints. When
Instruction Guide to Sterile Self-Catheterization for Women Using the Cure Catheter Closed System
 Cure Medical donates 10% of net income to medical research in pursuit of a cure for spinal cord injuries and central nervous system disorders. For information on scientific advancements, visit www.curemedical.com.
Cure Medical donates 10% of net income to medical research in pursuit of a cure for spinal cord injuries and central nervous system disorders. For information on scientific advancements, visit www.curemedical.com.
Chapter. Some days I m so stiff. But even then, your firm yet gentle guidance always helps me move more easily. MOVING AND POSITIONING
 15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
NHS Continuing Healthcare
 NHS Continuing Healthcare Questionnaire In association with Questionnaire 1. Full name of patient 2. Home address (prior to transfer into care home if applicable) 3. Patient s Date of Birth 4. Patient
NHS Continuing Healthcare Questionnaire In association with Questionnaire 1. Full name of patient 2. Home address (prior to transfer into care home if applicable) 3. Patient s Date of Birth 4. Patient
Splinting for individuals with Spinal Cord Injury
 Splinting for individuals with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This information is developed to direct
Splinting for individuals with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This information is developed to direct
