Shoulder Replacement Surgery Patient Information Manual
|
|
|
- Neil Roberts
- 10 years ago
- Views:
Transcription
1 Shoulder Replacement Surgery Patient Information Manual Maximizing Your New Shoulder UF HEALTH REHAB CENTER SHANDS HOSPITAL UFHealth.org/shands-rehab-center-orthopaedics-and-sports-medicine-institute
2
3 INTRODUCTION Congratulations! You have chosen a premier orthopaedic team to conduct your shoulder replacement! The University of Florida Orthopaedic Surgery program first began in 1960 as a division of the Department of Surgery. In 1975 the Division of Orthopaedic Surgery achieved full departmental status. From our beginning in 1960, the University of Florida Orthopaedics and Rehabilitation program has earned a reputation for excellence in research, teaching and clinical care. Our commitment to patient health care motivates every aspect of our efforts, from the bedside, to the classroom, to the research lab. The foundation of our department is built on two outstanding institutions: the University of Florida, a top 20 public university and UF Health Shands Hospital, one of the Southeast s premier health systems. Your doctor has explained your procedure, and what to expect post surgery. The purpose of this guide is to provide you with more information as to what to expect along the road to recovery, and what you can do to prevent any complications and maximize your outcomes. Although the healthcare team will assist you in your recovery, YOU AND YOUR FAMILY are the most important members of the team. We believe knowledge and preparation as to what to expect pre- and post-operatively will make your recovery easier. If you have questions along the way, be sure to ask them. We are here to help you achieve your goals and want you to be satisfied with your entire experience. Our goal is EXCELLENT service, from start to finish. So, let s begin.
4 TOTAL SHOULDER ARTHROPLASTY When shoulder replacement surgery is performed, the ball is removed from the top if the humerus, or your upper arm bone, and replaced with a metal implant. This is shaped like a half-moon and attached to a stem inserted down the center of the arm bone. The socket portion of the joint, or your glenoid fossa, is shaved clean and replaced with a plastic socket that is cemented into the scapula. The scapula is what you would call your shoulder blade. These implants are shaped so that the shoulder joint will move in a way that is very similar to the way the joint moved when it was healthy. REVERSE TOTAL SHOULDER ARTHROPLASTY With the Reverse Shoulder prosthesis, the anatomy, or structure, of the healthy shoulder is reversed. The implant is designed so that the ball portion is attached to the scapula and the socket is placed at the upper end of the humerus. The reverse shoulder prosthesis is primarily utilized for patients with insufficient rotator cuff musculature.
5 ANATOMY Ball and Socket of Healthy Shoulder Joint Surfaces In a healthy shoulder joint, the surfaces of these bones where the ball and socket rub together are very smooth and covered with a tough protective tissue called cartilage. Arthritis causes damage to the bone surfaces and cartilage. These damaged surfaces become rough and will become painful as they articulate, or rub together, on one another. Arthritic Shoulders Arthritis can be treated in different ways. There are medications for arthritis, exercises, and Physical Therapy and Occupational Therapy that can be done to help conservatively manage your arthritic pain. Surgery is another way to manage arthritis that has become dehabilitating. A total shoulder replacement surgery is one such surgery. Your orthopedic surgeon would help you to determine if this is the right avenue for you to follow. The surgeon will perform a comprehensive exam to include: a complete medical history, x-rays, assess your range of movement and level of daily function, and other tests to show the extent of damage to the joint. Total shoulder joint replacement will be considered if other treatment options will not relieve your pain and disability. It is important to understand the shoulder joint, arthritis, and the surgical procedure. Patients who have tried conservative treatments for shoulder arthritis, but have not been able to find adequate relief, may be a candidate for shoulder replacement surgery. As with any surgical procedure, patients considering the procedure should understand the potential risks of surgery, and understand that the goal of joint replacement is to alleviate arthritic pain. Patients generally find improved motion after surgery, as well as pain relief. When is a Reverse Shoulder Prosthesis Used? The Reverse Shoulder Prosthesis is mainly used for patients with rotator cuff tear, a medical condition in which the muscles around the shoulder joint have degenerated, or weakened to a point where they can no longer hold the shoulder joint intact or allow it to function normally in conjunction with arthritis. Arthritis, a previous shoulder injury such as a shoulder fracture, rotator cuff tear, and/or failed previous shoulder surgeries could all warrant a Reverse Total Shoulder Arthroplasty. There should be no shoulder movement initially following a Reverse Total Shoulder.
6 WHAT SHOULD I BRING TO THE HOSPITAL? You should be fitted for your sling prior to your hospital visit. You must have this post-surgery! The therapist or nurse will help you adjust it post-surgery, but you must have it with you. The sling may be bulky, so make sure that you have shirts that are larger and button up in the front, if possible, to make it easier for you to get dressed. You will need good walking shoes, or slippers with backs on them and a rubber sole. You want to do plenty of walking while you are in the hospital. Bring a robe or clothes that button up in the front. Make sure you have a current list of your allergies and medications. If you are having your dominant side operated on, remember that things will be difficult for you to maneuver and you will need some help at home. Also, any personal grooming items that you may want to pack, including hairbrush, toothbrush, deodorant, razor, shaver, eyeglasses/contacts, undergarments (for women, a bra that clasps in front or a tank top that can be cut down the side if needed for reverse TSA) and loose fitting button down the front clothing, items are preferred. If you normally use a cane, bring it with you (please properly label) or have your family bring it the morning after surgery. Before you leave your home Arrange transportation prior to admission since YOU CANNOT DRIVE YOURSELF HOME and your surgeon will let you know when you are able to resume driving again, typically after 4-6 weeks. Think about who will be able to assist you with meal preparation, medication management, self-care and exercise (if indicated by your surgeon) for the next 4-6 weeks. - If you have Medicare for your insurance and there is no skilled need in the home (this means physical therapist or a medical need for a nurse, you likely will not receive homecare). Medicare does not pay for a home health aide to come out and help you without a skilled need in the home. That is why you need to make arrangements prior to your surgery to have family or friends assist you when you get home. - If you have private insurance, most of these do not pay for a home health aide, so please make sure you know your benefits. - Going to a nursing home or rehab facility is usually not an option. There are exceptions but you need to call the doctor s office prior to surgery and talk to someone about the fact you will require placement. - The doctor s office has access to the case manager and confer with him/her regarding nursing home placement and if it will be paid for by insurance (Private, Medicare, Medicaid). Someone will get back to you before your surgery regarding this issue. At that time you can make a decision whether to go on with the surgery as scheduled or postpone until you have someone to take care of you if a nursing home is not an option. It is not the doctor s responsibility or the hospital to make sure you have someone at home to assist you after discharge. Also, remove any throw rugs or objects that may block your path.
7 WHAT SHOULD I BRING TO THE HOSPITAL? (continued) Plan on a family member, caregiver or other support person to be present at the hospital to learn how to perform exercises (if indicated), assist with upper body dressing and learn your precautions post-operatively. ANESTHESIA AND YOU You will see an anesthesiologist and/or an anesthesia nurse practitioner before your surgery. He/she will review your medical history and perform a brief physical exam. The anesthesiologist will discuss with you the options you have for anesthesia during your surgery. Keep in mind your anesthesiologist, based on your history, physical exam, type of surgery and other factors, may suggest one particular anesthetic technique. This is a copy of the pain scale used to help you communicate your pain level. Cervical plexus block and cervical paravertebral block (shoulder and upper neck) The most common nerve block used for shoulder replacement surgeries are the cervical blocks. These blocks have revolutionized early mobility of the shoulder for the Total Shoulder Arthroplasty. These blocks allow for post op day 0 activity of the shoulder when the procedure allows for shoulder activity, and helps keep pain under control to improve your comfort and your ability to rest. The packs are portable and are taken home for continued pain control. There can be side effects, as listed below, but these are temporary. When using the cervical paravertebral approach, the catheter is better anchored because it passes through multiple layers of muscle and vital anterior structures have less risk of being injured.
8 PATIENT INSTRUCTIONS: UPPER EXTREMITY CATHETERS You may receive local anesthetic through a small tube located near the nerves that go to your arm or shoulder. This medication will help your pain after surgery. The catheter (tube) has been placed by your anesthesia doctor at the request of your surgeon. About this technique of pain control: The local anesthetic medicine will not usually take away all of your pain, so it is expected that you will use some of the pain pills prescribed by your doctor while you have the catheter in place. Communication is essential to making this therapy work. Your anesthesia doctor will call you on the night you have had your surgery and each day you have your catheter in place. It is important we speak to you each day so that we can make sure that you are doing well and to see if you need any adjustments to your infusion. You will be receiving about a teaspoon of local anesthetic, numbing medicine continuously every hour. You can also give yourself additional medicine by pushing the bolus button located on the front of the pump. You can press the bolus button as often as you want to, but it will only give you the extra medicine once every minutes according to how your doctor has programmed your pump. Therefore, if you still have pain 20 minutes after pressing the bolus button, you may take your oral pain medication as prescribed. Usually about 10 to 15 hours after surgery the intense numbness that you felt initially wears off and you may experience some pain. When this occurs, take some of your pain medication and press the bolus button on the front of your pump. This will give you a small amount of additional local anesthetic medicine. After the dense nerve block goes away, most patients describe their fingers as feeling fat. However, you should be able to move your fingers and have some feeling in them, they just may not feel normal to you while the catheter is in place. The thumb is usually the digit that feels the most numb for the longest time. An example of a portable pain catheter
9 SLING TIPS FROM REHAB Most important tip... BRING IT WITH YOU if you received one at pre-op. After surgery, wear your sling at all times, unless otherwise instructed for exercises and hygiene. During your hospital stay, you will receive information specific to your type of sling, surgery and surgeon. No pushing or pulling with operative arm. Depending on your type of surgery or the surgeon, you will be wearing the sling for 4-6 weeks. GENERAL DISCHARGE INSTRUCTIONS You will receive instructions specific to your surgery postoperatively. Dressing - Move clothing to arm, not arm to clothing - Wear clothing a size or two larger than normal - Often front button down shirts are best or loose v-neck types - Therapist will demo dressing techniques during hospitalization Remember no movement of shoulder! Sleeping - Initially may be more comfortable sleeping in recliner chair - No pushing up from bed or a chair with operated side - Exit/enter bed from non-operated side - Do not place additional pillows behind upper arm Okay to place below lower arm as long as not forced into hike/elevation Swelling - Ice may be used up to 6-8 times a day No more than minutes at a time Do not use until nerve block removed Hygiene - Discuss bathing and your surgical dressing with your surgeon - Sponge bathing recommended for first two weeks to protect shoulder and remain in sling - Avoid water or products (powders or lotions) near incision - Do not shave underarms on operated side before 2 week follow up Assistance - If you live alone or your dominant side shoulder has been operated on, you will need extra help for the first week - Think about who can assist you with transportation, meal preparation and household activities as needed - If you normally use a cane, do not use it with your operated arm - Also, do not use a walker or other two-handed device
10 DISCHARGE INFORMATION KNOW the discharge language... Patients, family caregivers and healthcare providers all play roles in planning for discharge. It is a significant part of the overall care plan that many patients and care givers do not understand. Careful attention to the discharge plan and post hospital care ensures your successful surgery. Many types of post hospital care are not covered under insurance. Here are the basics. Insurance type and medical recommendations both play a role in the type of final discharge plan. Medical staff, Case Managers and Physical Therapists can recommend the appropriate level of care, insurance policies direct care based on coverage and contracts with companies. This can impact your choice of facility and amount of care you are eligible to receive. After joint surgery, patients are discharged to a variety of locations based on their general state of health, how will they recover from surgery, their assistance at home, and their insurance policies. Inpatient Rehab Hospitals are facilities such as UF Health Shands Rehab, or Brooks Rehabilitation in Jacksonville, Florida. To be admitted to these types of facilities, you need a recommendation from physical therapy for intensive therapeutic management of three or more hours per day and have medical needs that require ongoing doctor s supervision. This is most like residing in a hospital. Most orthopedics-planned joint replacements do not discharge to these types of facilities. Medicare, Medicaid and some private insurances cover this type of care. Many private insurances have a very limited benefit for this type of care. Skilled facility, Subacutes, SNF or sometimes skilled nursing facilities or extended care facilities To be admitted to these types of facilities, you need a recommendation from the physical therapist for sub-acute rehab. These facilities have both short-term recovery areas and longterm residential areas where patients receive care. These facilities have physical therapists, occupational therapists, separate therapy gyms to assist with rehabilitation; they also provide nursing care, custodial care, and can accommodate a longer stay for patients. Many orthopedics-planned joint replacements do discharge to these types of facilities. Patients that need additional assistance with walking, more time to recover from surgery, have steps or live in a difficult to reach area, or live alone, often discharge to a sub-acute facility. Is this covered by my insurance? Medicare and private insurances cover this expense; however, most private insurances or Medicare advantage plans require you to go to a facility in their network and a copayment.
11 Home Care DISCHARGE INFORMATION (continued) Home care is a visit by a medical professional including a visit by a nurse to assess, physical therapist or occupational therapist. All planned joint replacements receive some type of homecare to assist with mobility. You will be asked to choose a Home Care agency. Medicare and private insurances cover this expense, there are restrictions on the company that your insurance allows you to choose from, and you will be provided with a list of companies that are available within your network. DME This stands for durable medical equipment and includes walkers, wheelchairs, crutches, bedside commodes, and other items to assist with your mobility and care. Most insurances cover the above items, however, they do not carry specialty items such as shower chairs, slide boards or hand rails. Outpatient Rehab This is therapy that you will receive in an outpatient clinic. Most insurances cover this service, although you may have a limited choice or area that you must choose from.
12 SUMMARY OF ACTIVITY POD 0 or day of surgery Mobility Goals: Get out of bed to the chair Walk with assistance Use the bathroom with assistance You should expect to be out of bed once you are awake and alert enough to do so. You are encouraged to walk with therapy or nursing and eat your meals out of the bed. You will have a regular diet Your sling will be checked for fit and comfort A pillow can be placed under lower arm to prevent your shoulder from overstretching You should have restrictions to shoulder movement, so follow these instructions carefully POD 1 Mobility Goals: Get dressed, up for meals, walk in hallway and get ready for home You should be getting dressed, up walking, and getting ready for discharge home You will be having a PT/OT come in to review precautions, restrictions, and any exercises you are allowed to do, depending on what type of surgery you had done Thank you for choosing UF Health for your elective surgery. We appreciate your business, and wish you years of comfortable mobility!
13 NOTES /QUESTIONS
14 NOTES /QUESTIONS
15
16 Rev. 12/5/13 PS118587
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Admission to Inpatient Rehabilitation (Rehab) Services
 Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
Family Caregiver Guide Admission to Inpatient Rehabilitation (Rehab) Services What Is Rehab? Your family member may have been referred to rehab after being in a hospital due to acute (current) illness,
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
.org. Shoulder Joint Replacement. Anatomy
 Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
Shoulder Joint Replacement Page ( 1 ) Although shoulder joint replacement is less common than knee or hip replacement, it is just as successful in relieving joint pain. Shoulder replacement surgery was
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Medical Rehabilitation. Rehabilitation Unit
 Medical Rehabilitation Rehabilitation Unit Medical Rehabilitation The purpose of this handout is to give you information about University Hospital s Rehabilitation Unit (2 North or 2N). It will explain:
Medical Rehabilitation Rehabilitation Unit Medical Rehabilitation The purpose of this handout is to give you information about University Hospital s Rehabilitation Unit (2 North or 2N). It will explain:
Endovascular Abdominal Aortic Aneurysm Repair Surgery
 Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
 Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
SLAP repair. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Total Shoulder Arthroplasty
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
Lumbar Spine Surgery What to Expect
 Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
Rebuilding your INDEPENDENCE. The Joint Center. This is your hospital.
 Rebuilding your INDEPENDENCE The Joint Center This is your hospital. Providing you with high-tech orthopedic care inahealingenvironment. Every year, thousands of Americans suffer from severe pain in their
Rebuilding your INDEPENDENCE The Joint Center This is your hospital. Providing you with high-tech orthopedic care inahealingenvironment. Every year, thousands of Americans suffer from severe pain in their
Managing at home with your arm in a polysling following shoulder surgery
 Managing at home with your arm in a polysling following shoulder surgery Exceptional healthcare, personally delivered Contents Page Introduction...04 Restrictions in movement following shoulder surgery...04
Managing at home with your arm in a polysling following shoulder surgery Exceptional healthcare, personally delivered Contents Page Introduction...04 Restrictions in movement following shoulder surgery...04
Treatment Options for Rotator Cuff Tears A Guide for Adults
 Treatment Options for Rotator Cuff Tears A Guide for Adults Is This Guide for Me? YES, if your doctor has told you that you have a rotator cuff tear, which is an injury to one or more of the muscles and
Treatment Options for Rotator Cuff Tears A Guide for Adults Is This Guide for Me? YES, if your doctor has told you that you have a rotator cuff tear, which is an injury to one or more of the muscles and
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
CAREGIVER GUIDE. A doctor. He or she authorizes (approves) the rehab discharge.
 Guide for Discharge to Home From Inpatient Rehab Who Is on the Discharge Team? Many people help plan a rehab discharge, and they are often referred to as a team. The team members include: A doctor. He
Guide for Discharge to Home From Inpatient Rehab Who Is on the Discharge Team? Many people help plan a rehab discharge, and they are often referred to as a team. The team members include: A doctor. He
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
Patient s Handbook. Provincial Rehabilitation Unit ONE ISLAND HEALTH SYSTEM ONE ISLAND FUTURE 11HPE41-30364
 Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Chapter 7: Inpatient & Outpatient Hospital Care
 7 Inpatient & Outpatient Hospital Care ACUTE INPATIENT ADMISSIONS All elective and emergent admissions require prior authorization and/or notification for all Health Choice Generations Members admissions.
7 Inpatient & Outpatient Hospital Care ACUTE INPATIENT ADMISSIONS All elective and emergent admissions require prior authorization and/or notification for all Health Choice Generations Members admissions.
MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty
 Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
PALM BEACH ORTHOPAEDIC INSTITUTE, P.A. FAQ: OUT-PATIENT SURGERY
 DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
TRANSFERRING TO A NURSING FACILITY FOR KAISER MEMBERS
 SAN DIEGO CONTINUING CARE SERVICES DEPARTMENT TRANSFERRING TO A NURSING FACILITY FOR KAISER MEMBERS You are going to a skilled nursing facility for further care. This booklet gives you information about
SAN DIEGO CONTINUING CARE SERVICES DEPARTMENT TRANSFERRING TO A NURSING FACILITY FOR KAISER MEMBERS You are going to a skilled nursing facility for further care. This booklet gives you information about
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
Orthopaedic Stem Cell Treatment
 Orthopaedic Stem Cell Treatment Stem Cell Injections Surgically Implanted Stem Cells Learn about the treatment option that is best for you. Emory Healthcare patients can benefit from surgical implantation
Orthopaedic Stem Cell Treatment Stem Cell Injections Surgically Implanted Stem Cells Learn about the treatment option that is best for you. Emory Healthcare patients can benefit from surgical implantation
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
Total Hip or Knee Joint Replacement
 Preparing for your Total Hip or Knee Joint Replacement Pre-operative education for patients St. Clair Hospital Center for Orthopedics Copyright 2011 by St. Clair Hospital The Orthopedic Team Physicians
Preparing for your Total Hip or Knee Joint Replacement Pre-operative education for patients St. Clair Hospital Center for Orthopedics Copyright 2011 by St. Clair Hospital The Orthopedic Team Physicians
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Having Surgery? What you need to know. Questions to ask your doctor and your surgeon
 Having Surgery? What you need to know Questions to ask your doctor and your surgeon Agency for Healthcare Research and Quality Advancing Excellence in Health Care www.ahrq.gov This booklet was developed
Having Surgery? What you need to know Questions to ask your doctor and your surgeon Agency for Healthcare Research and Quality Advancing Excellence in Health Care www.ahrq.gov This booklet was developed
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
How To Plan For A Hospital Discharge
 Family Caregiver Guide Rehab-to-Home Discharge Guide In Rehab: Planning for Discharge The best time to start planning for discharge is just after your family member is admitted. While it may seem too soon
Family Caregiver Guide Rehab-to-Home Discharge Guide In Rehab: Planning for Discharge The best time to start planning for discharge is just after your family member is admitted. While it may seem too soon
Shoulder Replacement Surgery
 In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Provincial Rehabilitation Unit. Patient Handbook
 Provincial Rehabilitation Unit Patient Handbook ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM Welcome to Unit 7, the Provincial Rehabilitation Unit. This specialized 20 bed unit is staffed by an interdisciplinary
Provincial Rehabilitation Unit Patient Handbook ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM Welcome to Unit 7, the Provincial Rehabilitation Unit. This specialized 20 bed unit is staffed by an interdisciplinary
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
This information is provided by SRC for Medicare Information. (The costs that are used in these examples are from 2006.)
 Medicare Information Source This information is provided by SRC for Medicare Information. (The costs that are used in these examples are from 2006.) The Senior Resource Center for Medicare Information
Medicare Information Source This information is provided by SRC for Medicare Information. (The costs that are used in these examples are from 2006.) The Senior Resource Center for Medicare Information
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
A Patient's Guide to Arthritis of the Finger Joints
 Introduction A Patient's Guide to Arthritis of the Finger Joints When you stop to think about how much you use your hands, it's easy to see why the joints of the fingers are so important. Arthritis of
Introduction A Patient's Guide to Arthritis of the Finger Joints When you stop to think about how much you use your hands, it's easy to see why the joints of the fingers are so important. Arthritis of
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Rhode Island Hospital Inpatient Rehab Unit (IRU)
 Rhode Island Hospital Inpatient Rehab Unit (IRU) We are located on the 7 th floor of the Main Building. The unit phone number is (401) 444-2217 Within this packet, you will find answers to some commonly
Rhode Island Hospital Inpatient Rehab Unit (IRU) We are located on the 7 th floor of the Main Building. The unit phone number is (401) 444-2217 Within this packet, you will find answers to some commonly
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM
 ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
ROTATOR CUFF TEARS SMALL
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Dr. Benjamin Hewitt. Subacramial Decompression & Rotator Cuff Repair
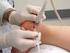 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Subacramial Decompression & Rotator Cuff Repair The Rotator Cuff consists of four
AFTER TOTAL KNEE REPLACEMENT. Living with Your New Knee
 AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
AFTER TOTAL KNEE REPLACEMENT Living with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Movements that you once took for granted
Spine and Orthopedic Surgery Unit Hamilton General Hospital. Information for patients and their families
 Spine and Orthopedic Surgery Unit Hamilton General Hospital Information for patients and their families Curing - Caring - Comforting 905-527-4322, ext. 46650 Table of contents Page About 6 West... 1 Health
Spine and Orthopedic Surgery Unit Hamilton General Hospital Information for patients and their families Curing - Caring - Comforting 905-527-4322, ext. 46650 Table of contents Page About 6 West... 1 Health
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program
 Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery
 Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Why an Exactech Hip is Right for You
 Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Why an Exactech Hip is Right for You Why do I need a total hip replacement? Which surgical approach is best for me? How long will it last? Which implant is right for me? Founded in 1985 by an orthopaedic
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Shoulder Dislocation or Instability Surgery: A Guide to Recovery After Surgery
 What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion
 Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen,
Anterior Cervical Decompression and Fusion or Anterior Cervical Corpectomy and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen,
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Rehabilitation Center
 Rehabilitation Center PATIENT INFORMATION Welcome to Ministry Saint Joseph s Hospital At Ministry Health Care, we earn trust by working together as One Ministry to keep PATIENTS FIRST in everything we
Rehabilitation Center PATIENT INFORMATION Welcome to Ministry Saint Joseph s Hospital At Ministry Health Care, we earn trust by working together as One Ministry to keep PATIENTS FIRST in everything we
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
INPATIENT REHABILITATION SERVICES
 MOVE. GROW. LIVE. INPATIENT REHABILITATION SERVICES THE IMPORTANCE OF CHOOSING THE RIGHT RECOVERY PARTNER. You do have a choice when it comes to inpatient rehabilitation, and the decision you make can
MOVE. GROW. LIVE. INPATIENT REHABILITATION SERVICES THE IMPORTANCE OF CHOOSING THE RIGHT RECOVERY PARTNER. You do have a choice when it comes to inpatient rehabilitation, and the decision you make can
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
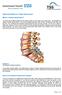 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
