OXYGEN THERAPY Revision 2016 AIRWAY MANAGEMENT
|
|
|
- Bryan Cook
- 7 years ago
- Views:
Transcription
1 Revision 2016 AIRWAY MANAGEMENT After ensuring your own safety at the scene of a sick or injured person, one of the first priorities is the airway. If the victim cannot exchange air, all resuscitation efforts are useless. The basic procedures listed in this booklet, if properly performed, will be a great asset to a wide variety of medical & trauma patients. Airway Management on the part of the rescuer is of paramount importance. Annual recertification with CPR is required to maintain current standards with the Canadian First Aid School, in accordance with Provincial Legislation & International Resuscitation Guidelines. The delivery of oxygen, use of adjunctive airways, pocket masks, etc. all require responsibility on behalf of the rescuer. Oxygen is a medication and, if properly used, is an excellent tool in combating shock. NEVER DELAY RESUSCITATION EFFORTS TO WAIT FOR SPECIAL EQUIPMENT / APPARATUS Airway Anatomy Air enters the nostrils and/or mouth, passes through the nasopharynx, oropharynx, through the vocal cords (glottic opening) into the trachea, bronchi, bronchioles to the alveoli where blood gas exchange takes place (diffusion). Airway Obstruction The UNCONSCIOUS PATIENT The most common cause of airway obstruction is the patient s own tongue. As the patient loses consciousness, the muscles of the tongue relax allowing the tongue to fall back on the throat, thereby obstructing the airway. The tongue is attached to the lower jaw, hence the Jaw Thrust manoeuvre will help open the airway. Placement of an Oropharyngeal Airway (OPA), or Nasopharyngeal Airway (NPA) will help maintain an open airway by holding the tongue upward (anterior).
2 The CONSCIOUS PATIENT The airway can be compromised by several factors: v Anaphylaxis (Severe Allergic Reaction) can cause edema or swelling of the tongue, airway, and epiglottis in addition to severe bronchospasm and increased production of mucous secretions. v Burns Patients who have been involved in a fire or have inhaled superheated smoke and gases are also at risk of airway edema and blistering. v Foreign Body Airway Obstruction Choking on food, liquid, vomitus or small objects can lead to either partial or complete airway obstruction. Choking can cause death if not corrected. Refer to a CPR manual for complete information on choking and the proper application of the abdominal and/or chest thrust manoeuvre. v Gas Inhalation Inhaling certain gases can cause edema and, in some cases, have a corrosive effect on the airway and lungs. In addition to the traumatic effects of gas inhalation, it is important to note that many gases are also Central Nervous System (CNS) depressants. The effects of these central nervous system depressants can decrease respirations, pulse and the level of consciousness. v Trauma Direct trauma to the throat, neck and chest wall can cause obstruction and edema. The PEDIATRIC PATIENT Infants and children are at risk of airway compromise for the same reasons as adults. However, there are special concerns such as a smaller diameter airway and an upper airway which is hypersensitive to abrasions, etc. which can lead to severe edema. Remember, according to current guidelines, when an unconscious child is choking on a foreign body, finger sweeps are performed only when the object is visible. Removal of Foreign Objects The removal of vomitus, blood, mucous, or other liquids can be attained by suction, if available. If necessary, the patient may be log rolled to clear the airway. Ensure that the C-Spine (cervical spine) is stabilized when log rolling a trauma patient. Edema of the Airway Edema of the airway (swelling of the soft tissue along the airway) can be caused by anaphylaxis, blunt trauma, viral infections, etc. A high-pitched squeal or cough may be present. This casualty requires oxygenation and is a very high priority emergency. Arrange for RAPID TRANSPORTATION.
3 The OROPHARYNGEAL AIRWAY (OPA) & NASOPHARYNGEAL AIRWAY (NPA) The OPA is a soft plastic device used to keep the tongue from the posterior pharynx (back of the throat) and therein prevents obstruction of the airway. Proper sizing, insertion and observation are extremely important. The OPA is only as effective as the rescuer using it. The OPA is to be used only on unconscious patients without gag reflexes, and who may or may not be breathing spontaneously. It is designed primarily to maintain an open airway; it is not an excuse for the rescuer to forget about the airway or respirations. The patient must be assessed constantly to prevent obstruction by vomitus, blood, mucous, etc. If a patient gags upon insertion of the OPA, pull it back out immediately and be prepared for the possibility of vomiting. Do not be discouraged! This indicates that your patient has a moderate level of consciousness. However, continue to assess the airway, respiratory rate, quality, and depth, etc. Also, assist the patient with supplementary or positive pressure oxygen therapy as necessary. Nasopharyngeal airways are inserted through the patient s nostril, and also help keep the airway open. They are better tolerated in patients that are not fully unconscious without a gag reflex. They are the first airway of choice for most basic responders in austere conditions, including military applications. *These will be demonstrated in class* It is generally accepted that any trauma victim with a decreased level of consciousness should receive 100% oxygen using the Bag-Valve mask device. These patients require you to provide positive pressure ventilation for them. Ensure you constantly assess the victim s level of consciousness and other vital signs as well. Trauma victims with a respiratory rate greater than 24 breaths per minute may also be in distress. The victim may have high CO2 levels, or may be hyperventilating from the effects of shock. It is difficult to assess which condition is present, thus monitor the patient closely and administer oxygen as appropriate to the LOC and the ABC s. Positive pressure ventilatory assistance may be necessary. OPA sizes range from pediatric to the largest adult. To find the correct size, you can measure the airway from the middle of the patient s lips to the angle of the lower jaw or from the patient s earlobe to the corner (edge) of his/her mouth. AVERAGE SIZES Adult: Standard #4 #5 #6 Metric #10 #11 #12 Children: Standard #0 #1 #2 #3 #4 Metric #5.5 #6 #7 #8 #10 Insertion of and OPA Insert the OPA upside down until it reaches the posterior pharynx, then rotate it halfway. This allows it to slip behind the tongue. The airway of a child can become damaged by rotation of the OPA. In this case, displace the tongue forward and out of the way to allow the OPA to be inserted directly in place (use a tongue depressor).
4 Methods for Opening the Airway In keeping with current guidelines, the method of head-tilt-chin lift is not acceptable in the trauma patient or any victim whose cause of injury is unknown. ALWAYS SUSPECT A SPINAL INJURY. To open the airway while avoiding further neck injury, use the MODIFIED JAW THRUST manoeuvre. The modified jaw thrust is a one-rescuer method of opening the airway, which also allows the rescuer to stabilize the head and neck. By placing your hands on both sides of the patient s head, you displace the lower mandible upward. This is by far the most acceptable method. Oxygen Flow Rates Supplemental Oxygen Devices The size of the oxygen tank should suit the needs of the response team (i.e. an inner city pool or dental office does not require an M cylinder for their patient). However, an ambulance from a rural area would need a tank capable of running for a longer duration of time. Delivery System O2 Setting/LPM % Oxygen Fi02 Nasal Cannula (prongs) Simple Mask Pocket Mask c/w O2 inlet* Non-Rebreather Mask Bag-Valve-Mask (reservoir) D Tank: Jumbo D Tank: E Tank: M Tank: 360 litres 675 litres 675 litres 2000 litres NOTE: psi is considered normal pressure for most size tanks. *Based on a non-breathing patient receiving positive pressure ventilatory assistance from a rescuer. The pocket mask can also be used for breathing patient if no other delivery system is available. (Follow simple mask settings and remove mucous filter and one-way valve).
5 Nasal Cannula The nasal cannula is the only supplemental device that does not cover the mouth as a mask does. For this reason, the cannula is useful for the following conscious patients: Claustrophobia some patients will not tolerate a mask covering their face. The cannula is usually well tolerated. Vomiting patients who have been vomiting but also require oxygen for their condition will benefit from the cannula. Confined Space Rescue or High Angle Extrication if the patient is strapped down to a spineboard or is secured in a basket stretcher for transport, severe airway distress can occur if the patient vomits with a mask on, and cannot clear their own airway. If the patient is wearing a cannula and vomiting occurs, the stretcher can be rolled and the patient s airway cleared. CONS: The oxygen concentration of the cannula can only reach a maximum of 44%. This does not make it useful for patients requiring high flow oxygen. Some examples of such patients would be for treatment of asthma, severe shock, etc. Simple Mask: The simple mask is not a widely used device. It covers both mouth and nose. It has a head strap to hold it securely to the face, plus a nose clip to ensure a good seal. There are exhalation ports without flap valves on both sides of the mask. CONS: A simple mask is a good medium concentration device for use on conscious patient with spontaneous respirations. The simple mask is capable of oxygen concentrations of 40-60%. This is a generally well-accepted device available in pediatric and adult sizes alike. Oxygen concentrations are at 60% maximum. In addition, it is difficult to assess breathing depth and quality. It is important that the litre flow is set no lower than 10 Lpm for an adult as the exhaled CO2 may not clear the mask and the patient may actually get reduced oxygen concentration as a consequence.
6 Non-Rebreather Mask: The non-rebreather mask covers the mouth and nose, and is similar in design to the simple mask. However, there is an additional reservoir bag and a one-way valve. All incoming oxygen is directed into the reservoir, which allows inhalation through the valve and into the patient's lungs. The valves on either one or both of the exhalation ports prevents atmospheric air from entering the mask during inhalation thus increasing oxygen concentrations. If one flap valve is used on the exhalation port, 60-90% oxygen concentration is attainable. If two flap valves are covering both exhalation ports, up to 100% oxygen concentration is attainable. However, if both exhalation ports prevent incoming atmospheric air and the oxygen source either runs empty or the tubing becomes kinked during a rescue, there is potential for the patient to suffocate. For this reason, most rescuers prefer non-rebreather masks with only one side flap valve. CONS: While ensuring the same litre flow as the simple mask of lpm, you attain approximately 30-50% better oxygen concentrations. The reservoir bag may be observed during respiration. This allows the rescuer to assess the rate and quality of breathing, in addition to observing chest excursion (expansion). There is a risk of suffocation with the mask models that include two exhalation side flaps valves. However, with close patient monitoring the risk in minimal. Patient Care and Supplemental Devices Nasal Cannula: The cannula should be placed on the patient and looped behind the ears. If the prongs are curved, they should curve inferior (downward) into the nostrils. In addition, the oxygen should NOT be turned on until the cannula is in position. If a cannula is to be used for longer than 30 minutes, humidified oxygen should be considered to prevent drying and possible bleeding of the nasal passages. Simple Mask: Oxygen should be turned on prior to applying the mask to the patient. In addition, please ensure that you take the time to inform your patient of your intentions, and encourage them to continue to breathe normally. Non-Rebreather Mask: As with the simple mask, turn the oxygen on and let the patient know what you are doing. You will need to apply gentle pressure to the one way flap valve over the reservoir bag to facilitate filling of the reservoir prior to placing the mask on the patient. This is referred to as priming the reservoir bag.
7 Resuscitative Oxygen Therapy (Positive Pressure) There are several different delivery systems that may be referred to as Resuscitators. Before we list them however, we should review their use for patient resuscitation. Generally, we resuscitate those patients who breathe <12 breaths/ min., suffer from an altered LOC (level of consciousness) or have experienced a head injury. In addition, virtually any injury or illness causing reduced respiratory rate, volume, and level of consciousness, would benefit from BVM resuscitation using oxygen therapy. In some cases, the need for resuscitation is obvious, as in respiratory or cardio-respiratory arrest situations. Bag-Valve Mask (BVM): Typically silicone, rubber or soft plastic in construction, this device consists of 4 parts: v Reservoir Bag c/w oxygen tubing v Bag v Valve v Mask This method of resuscitation is widely used in hospital and pre-hospital settings alike. It is used with an OPA (oropharyngeal airway) at the basic level of care. The Advanced Life Support community will usually intubate the patient and hook up the BVM directly. Used in conjunction with an OPA, NPA or both, this is one of the best resuscitative methods available to the BLS rescuer. Oxygen flow for adults is set between Lpm and flows into the base of the bag near the reservoir. The oxygen is directed into the reservoir if it is attached. If not, oxygen flows directly into the bag. When the rescuer squeezes the bag, oxygen is forced through the valve, mask, and hopefully, into the patient. It is important to understand the limitations of this device. The BVM should only be used by qualified & trained personnel, who review their skills on a regular basis. Recently we made it a policy that the BVM should only be used with two rescuers. One rescuer can provide better resuscitation using a pocket mask with an oxygen inlet. CONS: The BVM is an excellent device for use on hypoxic and/or apneic patient because it has a high oxygen delivery capability when used with a reservoir bag. BVM s are available for adults, children, infant and neonate sizes, and are either reusable or disposable. The BVM delivers 100% oxygen concentration with a reservoir bag when operated properly. Unless this device is used on a regular basis by a rescuer, it can prove difficult to operate. Constant training and review is recommended. It has been proven that when used by a single rescuer, minimal tidal volumes are delivered due to inexperience, a poor mask seal, and/or squeezing the bag incompletely. It is recommended that this device be used by two rescuers. One person maintains the mask seal, monitors the airway, breathing and circulation constantly and the other person squeezes the bag and monitors oxygen flow rates. The BVM is a large device and should be stored in an appropriate storage case. As well, this device is susceptible to damage during extreme cold weather use.
8 OXYGEN THERAPY Pocket Mask: v Made out of durable plastic v Comes with a one way valve & a mucous filter v Also available with a head strap & oxygen inlet The pocket mask has popular benefits including size, versatility, low cost and ease of use. Its use is taught in many CPR and first aid courses. CONS: Because pocket masks are made of plastic, they are susceptible to breakage in extremely cold weather. It should always be stored in a warm environment or close to the body in a holder. This unit should also be taken out of its holder every month and inspected visually for cracks, tears, etc. It is difficult to criticize the pocket mask because its quality is exceptional, and use is relatively easy. Pulse Oximetry The saturation of oxygen in the body can be measured with a portable pulse Oximeter. This device is usually attached to the clean fingertip, and in some cases like pediatric patients, it is attached to the foot or earlobe. It sends an infrared light wave through the tissues, and receives the signal on the other side of the probe. This tells the team the percentage of 02 bound to the hemoglobin in the patient s bloodstream. Current thinking and evidence suggests that a value of 94% or greater is considered normal in most cases. Because the pulse Oximeter provides us with an actual value, we refer to it as a quantifiable means of measuring 02 therapy we may be delivering to the patient. The portable devices are often less than $40.00 and are considered a basic and fundamental means of measuring blood 02 levels as we provide care, and possibly 02 therapy. They do have limitations such as dirty fingers, dark nail polish, and have been shown to deliver false-positive results in the case of carbon monoxide inhalation. ILCOR recommends not giving supplemental 02 to potential cardiac patients if their room air saturation is already greater than 94%. Talk with your instructor about this important situation, as current evidence suggests 02 may worsen an ongoing heart attack.
9 Oxygen Tank Safety Considerations It is important to remember that Oxygen tanks are compressed cylinders, and as such, carry risks in operational mode and storage. Here is a brief safety list: v Do not store O2 cylinders around open flames. O2 as a gas is not flammable, but does support combustion aggressively. v Do not use compressed 02 around oil or grease. In particular, do not attempt to lube sticky cylinders or regulators. Always contact an approved service technician for maintenance problems. v When O2 tanks are stored, they should be secured and prevented from the risk of falling, or being struck. v Protect the regulator from bumps and falls. Many commercial O2 tank kits and bags are designed to protect the regulator and cylinder. v Have the tank maintained and filled by an approved technician. They will ensure that the cylinder is safe, free from defects, and receives periodic hydrostatic testing on a scheduled basis. v Ensure that O2 tanks and regulators are not used underwater. They are not designed for the atmospheric pressures exerted in such environments. Conclusion The Canadian College of Emergency Medical Services endeavours to provide the most current and up-to-date information and training when it comes to Airway management and 02 therapy. It s important that you follow the advice, medical control guidelines and most current science when providing this medication. Feel free to contact us at any time should you have questions, concerns, or recommendations for our programmes. Sincerely, Canadian College of Emergency Medical Services John (Gregory) Clarkes EMT-P, NRP, MICP Education Coordinator info@ccofems.org
ADMINISTERING EMERGENCY OXYGEN
 FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
Emergency Medical Responder Mid-Course Knowledge Evaluation
 Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services
 State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
Difficult Pre-hospital Airway Management
 Difficult Pre-hospital Airway Management Frans L. Rutten, MD, FDSA Elisabeth Hospital Tilburg, The Netherlands In management of patients with an emergency, airway management and ventilatory care are the
Difficult Pre-hospital Airway Management Frans L. Rutten, MD, FDSA Elisabeth Hospital Tilburg, The Netherlands In management of patients with an emergency, airway management and ventilatory care are the
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
PROCEDURE FOR USING A NASAL CANNULA
 PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT
 Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
PROCEDURE FOR USING A NASAL CANNULA
 FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING
 TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when
 Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
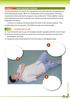 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum
 100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum consist of not less than fifteen (15) hours in first aid and
100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum consist of not less than fifteen (15) hours in first aid and
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Objectives. Burn Assessment and Management. Questions Regarding the Case Study. Case Study. Patient Assessment. Patient Assessment
 Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
CHAPTER 21 QUIZ. Handout 21-1. Write the letter of the best answer in the space provided.
 Handout 21-1 QUIZ Write the letter of the best answer in the space provided. 1. A severe form of allergic reaction is called A. an allergen. C. epinephrine. B. anaphylaxis. D. an immune reaction. 2. Harmless
Handout 21-1 QUIZ Write the letter of the best answer in the space provided. 1. A severe form of allergic reaction is called A. an allergen. C. epinephrine. B. anaphylaxis. D. an immune reaction. 2. Harmless
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
The EMT Instructional Guidelines in this section include all the topics and material at the EMR level PLUS the following material:
 Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
State of Indiana EMR Psychomotor Skills Examination
 SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
Emergency Action Plans
 Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION. Airway must be open so oxygen can enter the body.
 CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
CASAID THE AIMS OF FIRST AID, INCIDENT ACTION PLAN, INITIAL ASSESSMENT AND THE RECOVERY POSITION The Aims of First Aid The aims of first aid (the three Ps) are to: Preserve the casualty s life. Prevent
1st Responder to Emergency Medical Responder Transition Course
 1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
National Registry Skill Sheets
 Airway, Oxygen and Ventilation Skills/Upper Airway Adjuncts and Suction Bag-Valve-Mask/Apneic Patient Bleeding Control/Shock Management Cardiac Arrest Management/AED Immobilization Skills/Joint Injury
Airway, Oxygen and Ventilation Skills/Upper Airway Adjuncts and Suction Bag-Valve-Mask/Apneic Patient Bleeding Control/Shock Management Cardiac Arrest Management/AED Immobilization Skills/Joint Injury
Frontline First Aid EMR Scenario Examples
 Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Enables MDA Medical Teams to categorize victims in mass casualty scenarios, in order to be able to triage and treat casualties
 MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
How you can help save lives
 How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015
 2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015 Introduction This document provides the statewide
2012 Mississippi EMT Transitional Refresher Curriculum EMT Refresher Training- Curriculum Transition: EMT-Basic EMT Timeline: February 2012-March 2015 Introduction This document provides the statewide
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
TN Emergency Medical Services
 TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING.
 LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS
 Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
SUBJECT: BASIC LIFE SUPPORT AMBULANCE EQUIPMENT REFERENCE NO. 710
 SUBJECT: BASIC LIFE SUPPORT AMBULANCE EQUIPMENT REFERENCE NO. 70 POLICY: NOTE: Ambulances dedicated for infant transportation or when staffed and equipped for use in conjunction with newborn intensive
SUBJECT: BASIC LIFE SUPPORT AMBULANCE EQUIPMENT REFERENCE NO. 70 POLICY: NOTE: Ambulances dedicated for infant transportation or when staffed and equipped for use in conjunction with newborn intensive
Heart information. CPR cardiopulmonary resuscitation
 Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
First Aid as a Life Skill. Training Requirements for Quality Provision of Unit Standard-based First Aid Training
 First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
Airway and Breathing Skills Levels Interpretive Guidelines
 Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Basic ATLS. The Primary Survey. Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon
 Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Vacuum mattress, Bariatric Transfer, Monitoring Documents Lisa Curatolo / Pete Davis Reviewer Stephen Hearns / Alistair Kennedy
 Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Packaging Version 9 Related Vacuum mattress, Bariatric Transfer, Monitoring Documents
Emergency Medical Retrieval Service (EMRS) www.emrs.scot.nhs.uk Standard Operating Procedure Public Distribution Title Packaging Version 9 Related Vacuum mattress, Bariatric Transfer, Monitoring Documents
First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder.
 APPROVED SCOPE 2/8/08 BOARD MTG First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder. Emergency Medical Responder (EMR) Description of the Profession The
APPROVED SCOPE 2/8/08 BOARD MTG First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder. Emergency Medical Responder (EMR) Description of the Profession The
Infant CPR. What You Need to Know. How to Do Infant CPR
 Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
How To Treat A Pregnant Woman With A Miscarriage
 Special Patient Populations Obstetrics EMR Education Standard Recognizes and manages life threats based on simple assessment findings for a patient with special needs while awaiting additional emergency
Special Patient Populations Obstetrics EMR Education Standard Recognizes and manages life threats based on simple assessment findings for a patient with special needs while awaiting additional emergency
EMR Instructional Guidelines. Preparatory
 EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
!!!!!! Blood Pressure Measurement Palpation... 1 Blood Pressure Measurement Auscultation... 2 Conscious, Choking Adult or Child...
 !!!!!! Blood Pressure Measurement Palpation... 1 Blood Pressure Measurement Auscultation... 2 Conscious, Choking Adult or Child... 3 Conscious, Choking Baby... 4 Unconscious, Choking Adult, Child, or Baby...
!!!!!! Blood Pressure Measurement Palpation... 1 Blood Pressure Measurement Auscultation... 2 Conscious, Choking Adult or Child... 3 Conscious, Choking Baby... 4 Unconscious, Choking Adult, Child, or Baby...
American Heart Association. BLS Instructor Course. Written Examination. July 2003
 American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
American Heart Association BLS Instructor Course Written Examination July 2003 Basic Life Support Instructor Exam Part I Please do not mark on this examination. Record the best answer on the separate answer
(ISBN:9781449604103) Preferred Package Digital Supplement
 College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: gregl@tcdupage.org Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: gregl@tcdupage.org Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
Emergency Medical Technician Basic. Practical Skills Examination Sheets
 New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
Comhairle Fó-Thuinn DIVER MEDIC. Student Handouts
 Comhairle Fó-Thuinn DIVER MEDIC Student Handouts Irish Underwater Council 1999 Diver Medic Training Programme STUDENT HANDOUT Course Introduction Introduction This course, CFT Diver Medic, is designed
Comhairle Fó-Thuinn DIVER MEDIC Student Handouts Irish Underwater Council 1999 Diver Medic Training Programme STUDENT HANDOUT Course Introduction Introduction This course, CFT Diver Medic, is designed
(Organization s Name)
 2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
2 1 6 W A K E M A N P L A C E B R O O K L Y N, N E W Y O R K 1 1 2 2 0 W W W. A F O R U M F O R L I F E. O R G P H O N E 7 1 8 7 5 9 9 0 1 3 F A X 4 3 7 4 9 7 4 0 2 9 In association with the PROPOSAL FIRST
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
12/5/2012. Introduction. Head, Neck, and Spine Injuries. Recognizing and Caring for Serious Head, Neck and Back Injuries
 Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
Head, Neck, and Spine Injuries Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries. List the signals of head,
Patient Assessment/Management Trauma
 Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
On the Go with Oxygen
 On the Go with Oxygen Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into
On the Go with Oxygen Oxygen is in the air we breathe and is necessary to live. When we breathe in, oxygen enters the lungs and it goes into the blood. When the lungs cannot transfer enough oxygen into
EMR EMERGENCY MEDICAL RESPONDER Course Syllabus
 6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum
 EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
The Alberta College of Paramedics
 The Alberta College of Paramedics Alberta Occupational Competency Profile (AOCP) Upgrade Gap Training Program Emergency Medical Responder (EMR) Airway Management Module Study Guide Table of Contents Acknowledgements
The Alberta College of Paramedics Alberta Occupational Competency Profile (AOCP) Upgrade Gap Training Program Emergency Medical Responder (EMR) Airway Management Module Study Guide Table of Contents Acknowledgements
Epinephrine Auto Injector Interim Policy (Amended March 12, 2008)
 Epinephrine Auto Injector Interim Policy (Amended March 12, 2008) Pursuant to the authority conferred by N.J.S.A. 26:2K-47.1, et seq., the Department of Health and Senior Services (the Department) shall
Epinephrine Auto Injector Interim Policy (Amended March 12, 2008) Pursuant to the authority conferred by N.J.S.A. 26:2K-47.1, et seq., the Department of Health and Senior Services (the Department) shall
POLICIES & PROCEDURES. ID Number: 1115
 POLICIES & PROCEDURES Title: OXYGEN ADMINISTRATION ID Number: 1115 Authorization [X] SHR Nursing Practice Committee Source: Nursing, Respiratory Therapy, Physiotherapy Date Revised: March 2015 Date of
POLICIES & PROCEDURES Title: OXYGEN ADMINISTRATION ID Number: 1115 Authorization [X] SHR Nursing Practice Committee Source: Nursing, Respiratory Therapy, Physiotherapy Date Revised: March 2015 Date of
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector
 OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
OPTIONAL LESSON Anaphylaxis and Epinephrine Auto-Injector Lesson Length: 54 minutes GUIDANCE FOR THE INSTRUCTOR To complete this lesson and meet the lesson objectives, you must: Discuss all points in the
Procedure 17: Cardiopulmonary Resuscitation
 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Chapter 26. Assisting With Oxygen Needs. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Emergency Medical Response INSTRUCTOR S MANUAL
 Emergency Medical Response INSTRUCTOR S MANUAL Contents Acknowledgments 3 SECTION A: ADMINISTRATION Chapter 1: Introduction 9 Course Purpose Course Objectives Course Participants Instructor Responsibilities
Emergency Medical Response INSTRUCTOR S MANUAL Contents Acknowledgments 3 SECTION A: ADMINISTRATION Chapter 1: Introduction 9 Course Purpose Course Objectives Course Participants Instructor Responsibilities
Basic life support (BLS) Techniques
 module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
module Basic life support (BLS) Techniques 1 01 04. Basic Cardio Pulmonary Resuscitation (CPR) 08. Adult basic life support sequence, according to European Resuscitation Guidelines 12. Recognition of cardiorespiratory
Oxygen Therapy. A guide for the patient. Please bring to any outpatient appointments. Patients name. Exceptional healthcare, personally delivered
 A guide for the patient Please bring to any outpatient appointments Patients name Exceptional healthcare, personally delivered Introduction This leaflet has been written for patients starting, or who have
A guide for the patient Please bring to any outpatient appointments Patients name Exceptional healthcare, personally delivered Introduction This leaflet has been written for patients starting, or who have
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Skills Summaries. Legend. Wear personal protective equipment. Communicate with patient or other responders. Record/document findings
 Legend Wear personal protective equipment Communicate with patient or other responders Record/document findings Follow your local protocol Treat for shock Link to another skill Six Rights of Medication
Legend Wear personal protective equipment Communicate with patient or other responders Record/document findings Follow your local protocol Treat for shock Link to another skill Six Rights of Medication
EMT B Practice Test. Practice Questions:
 EMT B Practice Test Practice Questions: Questions 1 to 3 pertain to the following scenario: You and your partner are called to the home of a 75-year-old man complaining of severe pain in the chest and
EMT B Practice Test Practice Questions: Questions 1 to 3 pertain to the following scenario: You and your partner are called to the home of a 75-year-old man complaining of severe pain in the chest and
Canine Tactical Combat Casualty Care
 Canine Tactical Combat Casualty Care The following C-TCC guidelines are based on human C-TCCC guidelines and the limited data available on combat injuries and field treatment of working dogs. These guideline
Canine Tactical Combat Casualty Care The following C-TCC guidelines are based on human C-TCCC guidelines and the limited data available on combat injuries and field treatment of working dogs. These guideline
CPR /AED for Professional Rescuers
 CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
CPR /AED for Professional Rescuers In-Depth Instructor Resource Contents C-A-B (Compression-Airway-Breathing) 1,3... 3 CPR Barriers... 10 Adult CPR 1,3,4... 15 Child CPR 2... 17 Infant CPR 2... 19 Special
Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014
 Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014 General Information: Q: What is Heartsaver Pediatric First Aid CPR AED Online Part
Heartsaver Pediatric First Aid CPR AED Online Part 1 (90-1434) Frequently Asked Questions (FAQs) As of March 25, 2014 General Information: Q: What is Heartsaver Pediatric First Aid CPR AED Online Part
Chapter Review Questions
 1 Chapter Review Questions Chapter 1 1. True or false: As an Emergency Medical Responder, your first priority when responding to any emergency scene is patient care. 2. True or false: The first step in
1 Chapter Review Questions Chapter 1 1. True or false: As an Emergency Medical Responder, your first priority when responding to any emergency scene is patient care. 2. True or false: The first step in
