Help Yourself - Physiotherapy for people with respiratory symptoms
|
|
|
- Anissa Marsh
- 9 years ago
- Views:
Transcription
1 Royal Brompton & Harefield NHS Trust Royal Brompton Hospital Sydney Street London SW3 6NP tel: Harefield Hospital Hill End Road Harefield Middlesex UB9 6JH tel: Help Yourself - Physiotherapy for people with respiratory symptoms minicom: website: December 2004
2 Name: Physiotherapist: Contents Sputum production 2 Chest clearance 2 Postural drainage 6 Breathlessness 9 Exercise and activity 13 Further information 15 Introduction This booklet has been designed as a how to help yourself guide, a source of information from which you will benefit if your lung condition gives you symptoms such as: breathlessness sputum production or retention reduced ability to exercise (exercise tolerance). The information provided in this booklet should help you to remember what your physiotherapist has taught you. 1 18
3 Sputum Production Normally, sputum is not a problem as it is produced by the lungs as a defence mechanism. Inhaled particles are transported out of the airways to keep them clean. Sputum can become a problem if your condition involves the production of too much or if your disease affects the ability of your lungs to expel the mucus from your chest. This may involve part of or the whole of the lungs. Sputum may become more of a problem when a range of possible invading bacteria, viruses or fungi cause a chest infection. At this time you may notice the following changes: increasing amount of sputum change in sputum colour increasing frequency of cough possible increase in breathlessness. It is advisable to seek advice from your GP when you have a chest infection. Medication may be provided to help your body defend itself against the infection. You can also help yourself by using chest clearance techniques to expel the sputum from your chest. Chest clearance Why should I use chest clearance techniques? Chest clearance will benefit your lungs by: expelling infected secretions and therefore helping to minimise futher infection reducing damage to the lung tissue caused by retained sputum helping to maintain lung volume and function and reduce breathlessness. 17 2
4 When should I use chest clearance techniques? Chest clearance should be used during chest infections to expel the excess secretions. It should also be used as a preventive treatment so that the risk of infection and lung damage is minimised. Each individual and each condition differs completely in the volume of sputum produced each day. It may vary from as little as a teaspoonful to maybe more than several teacups full. It is for this reason that you will need to ask your physiotherapist how often and for how long you should carry out these sessions. What else can I do to make clearing my chest easier? Make sure that you are well hydrated to make sputum less sticky. Two litres of water each day is recommended, although it is advisable to reduce your caffeine intake by avoiding tea and coffee. If you have been prescribed bronchodilators, (medication which helps open up the airways), you may find it useful to take them about 15 minutes before clearing your chest to maximise the effect of the treatment. Active Cycle of Breathing Technique (ACBT) One technique that physiotherapists teach patients is the Active Cycle of Breathing Technique (ACBT). The diagram opposite will help you to understand this technique. Following the diagram you will find some short summaries which explain how to put the ACBT technique into practice. Notes 3 16
5 Further information Smoking Some chest conditions are related to smoking and may make your breathlessness worse. If you wish to try to help your lungs by giving up smoking, your doctor or physiotherapist may be able to advise on the different options available. Some improvement to your lungs can be made by stopping smoking. A telephone helpline is also available: Chest vibrations and / or clapping (percussion) Start - breathing control 3 or 4 deep breaths breathing control Quitline: am pm Further help Further advice about your condition or on the information given in this booklet can be obtained from your physiotherapist. You can contact Harefield Hospital on tel: Breathing control 1 or 2 huffs breathing control This is literally what it says it is - having control over your breathing. You should make sure you are positioned comfortably during this phase of the cycle to enable maximum support and relaxation and, therefore, minimum work by your muscles. You will now be ready to concentrate your mind on breathing control before starting deep breathing. It is important that you read the Breathlessness section on page 9 to understand more about breathing control. Deep breathing First, take a long, slow, gentle breath in, through the nose if possible, down to the lower chest (your tummy should rise during this phase, but certainly should not be forced to rise). Next, breathe out in a relaxed manner as if sighing out, again not forcing the action. Your chest should be allowed to sag passively. Then continue to try three or four of these breaths before resuming more breathing control. 15 4
6 Huffing Huffing is a method of clearing sputum from your chest. It uses less energy than coughing and so will make you feel less short of breath. It will also prevent any chest tightness (wheezing) which sometimes occurs after a bout of coughing. If possible, you should try to suppress your cough until you know that sputum is at the back of your throat and ready to be cleared. In order to perform a huff you should: keep your chin up to allow your airways to be open, but not so far up that your head is tipped backwards take a small half-sized breath in open your mouth wide but relaxed in an O shape breathe out steadily but quickly through your mouth until you move the sputum. The huff should be a similar action to steaming up a mirror or your glasses, but remember to have only a small breath in for this technique. Chest vibrations and clapping (percussion) These are manual techniques which, when combined with the active cycle of breathing technique (ACBT), will help to free secretions inside your chest, thus enabling you to huff them out more efficiently. Your physiotherapist will teach you appropriate techniques which you can use yourself or which a partner can perform for you during the deep breathing phase of the ACBT. However, unless otherwise advised by your doctor or physiotherapist, the techniques should NOT be used if you: notice blood in your sputum feel very short of breath feel wheezy or tight in your chest have or are prone to having broken ribs 5 better posture reduced symptoms of breathlessness and subsequent anxiety improved muscle strength which will require less oxygen and therefore put less demand on your lungs improved self-confidence and well-being: especially in realising your specific capabilities and limitations. Okay, so how do I get started? First of all, do you suffer from any other health problems? If so, you should seek advice from your doctor or physiotherapist before beginning your exercise programme. It is important that the exercise is tailor-made to suit your abilities. Your programme of exercise should focus on the following: the exercises should be progressed gradually - only one step at a time. For example, increase the number of exercise repetitions, the distance you walk or the time spent doing your exercises exercise specific areas of weakness. For example, you may have to strengthen leg muscles to help with any difficulty in climbing stairs gradually increase your self-confidence by learning to use your breathing control and your own capabilities exercise should be tailor-made to a level suitable to you alone. Ask your physiotherapist for advice on how long to carry out each exercise session. A daily, continuing programme designed to bring about steady, gradual improvement is preferable to a once-a-week blitz stop exercising if you experience any ill effects such as palpitations, blackout, excessive shortness of breath or pain during or after your activity. It is important to seek advice on symptoms so that they may be investigated. Advice can then be given to enable you to continue an exercise programme. 14
7 Some people are afraid to ask about your condition whilst others may expect too much of you. It is often difficult for people to understand when you have nothing to show for your breathlessness, such as a leg in plaster or arm in a sling. People need to be put in the picture. Remember that it is OK to rest, as long as you have a moderate amount of daily activity. The two go hand in hand. If you find that regular or even one-off rests make your breathing easier, then don t be ashamed to take them. After all, your breathlessness will make you more tired than other people and sleep is vital for your well-being. Feelings of tension and anxiety may be eased by different relaxation techniques. Some people find that having a partner pat or stoke their back eases their sensation of breathlessness. Exercise and activity Since symptoms such as breathlessness and / or sputum production can make you feel anxious, you may not have considered doing any exercise before. Some people are frightened that exercise will make their breathing worse, especially when they already feel short of breath at rest or with minimal activity. have pain in or around your chest have any areas of skin damage around your chest. Using the ACBT (Active Cycle of Breathing Technique) The cycle should be practised until your chest is clear and you should change position to drain specific areas of your chest. (Please read the following section on Postural Drainage). If you become tired or breathless, you may want to rest and continue the breathing cycle later. In addition, the number of daily treatments should correspond to how much sputum you produce. Certainly, during infection, when there is more sputum, you should try to perform chest clearance regularly. However, even at other times, daily preventive treatments are still important in keeping your airways clear. You may find it easier to build the treatments into your daily routine - perhaps clearing your chest before sleep will ensure a better night s rest. Chest clearance around meal times is not advisable due to the sensation of nausea after food or loss of appetite before food. Postural drainage So what position do I use for the ACBT? It is important to remember that becoming breathless is a normal response to activity or exercise. Everyone will experience this. However, people who already have certain lung conditions will find that they become breathless more easily (i.e. they don t need to do so much in order to bring on the symptoms). Just make sure you use your practised breathing control to enable you to do the activity or exercise you have chosen. Regular exercise brings many benefits at times when you are well. A few examples are: increased independence in daily activities 13 The bronchial tree Postural drainage means that different postures or positions are used to drain sputum from different parts of the lungs. The airways in the lungs are often referred to as the bronchial tree, since the tubes which they contain originate as one large tube which branches out with offshoots in two directions. These offshoots end as small sacs called alveoli. 6
8 A good starting position is sitting relaxed in a supportive chair. You can then progress to lying or sitting in different positions which will allow the variety of lung areas to be drained of sputum using gravity. This technique is called Postural Drainage. If necessary, your physiotherapist will advise you on which positions to use. Postural drainage positions lower lobes lingula middle lobe Other tips Remember - if you have been prescribed oxygen, it is there to help you and is not harmful. Using inhalers when you are breathless can be difficult. Ask your doctor about alternative inhalers which allow you to take time to inhale your medication. If your breathlessness limits your ability to carry out normal daily activities such as washing, dressing or cooking, an occupational therapist may be able to help by giving you valuable information and / or equipment for making functional tasks easier to perform. Having a door or window open may ease sensations of being warm or claustrophobic and may even reduce your breathlessness. Try to be as independent as you can within your capabilities. By keeping as active as possible and increasing your level of activity / exercise you will increase your muscle strength and need less oxygen. This will strengthen your ability to fight further infections (see Exercise and activity on page 13). Eating a large meal can seem a daunting task, especially when feeling full afterwards can make you more tired. Try eating little but often or set manageable amounts to eat. Do, however, keep your weight within a normal range. If you are concerned about your nutritional needs, ask to see a dietitian. Try to understand your own limitations and set goals which are achievable. This will help you feel more confident in your abilities and help you to be positive in discussing them with people around you. Pace yourself in each activity. Don t rush or you will feel exhausted at the end. Use breathing control to help pace your activities. Take time to discuss your abilities and disabilities with people close to you. It can be frightening for them too and make them feel helpless. 7 12
9 Breathing control This is controlled breathing which aims to concentrate your mind on your breathing pattern and enables you to feel in control of your breathing, particularly during attacks of breathlessness. First, make sure you are in a comfortable position for practising this technique - try the positioning discussed earlier. This will reduce any unnecessary muscle work, thus reducing the amount of effort you use for breathing. Next, breathe at a rate which is comfortable for you - never deliberately try to slow your breathing down - it should, with breathing control, gradually become easier. Then, try as much as possible to allow your upper chest to relax and feel supported. Feel the muscles around your neck and shoulders ease. lower lobes left lower lobe Now, focus on your breathing pattern. Remember not to hold your breath but to find a pattern or rhythm of breathing in and out that suits you. For example: try (breathe in), one, (breathe out), two, three, four. Progress as you are able to (breathe in) one, two, (breathe out), three, four, five, six etc. Try to keep your upper chest relaxed when breathing in and during this phase allow air to be drawn down to your lower chest and abdomen. Do not force this action, but gently allow your middle to expand. You may want to place a hand on the lower part of your chest (just above your tummy button) to feel this or visualise it by sitting in front of a mirror. upper lobes You can use this counting method either at rest or even during activity - walking, climbing stairs or during attacks of breathlessness for example - to help you achieve the feeling of being in control. By practising breathing control when you are well, you will be able to use it effectively when you are more breathless. 11 8
10 Breathlessness What is breathlessness? Breathlessness can be a distressing sensation for people who have specific lung conditions. Becoming breathless with activity or exercise is a normal and natural body response. However, when the lungs are affected by disease, it causes them to function differently and so breathlessness may occur with minor activity or even at rest. Breathlessness may also become more apparent during infections or so-called flare-ups or exacerbations associated with some conditions. How will the breathlessness make me feel? Feeling breathless is completely individual for each person. No one can tell you how you should feel as only you can know! The following suggestions have been designed to help you gain control of your breathlessness and to identify things you can do yourself in addition to things which have been provided medically, such as oxygen or medication. Positioning There are certain positions which aid the mechanics of breathing in people who are breathless. These positions are adopted during bouts of breathlessness, or during activity, thus easing the symptoms. The following positions have been found to help the diaphragm muscle work more effectively, enabling your neck and shoulders to be less tense. Positions include: high side lying forward lean sitting You may have sensations of being warm, anxious or claustrophobic and may find it easier to breathe by hunching up your shoulders or pursing your lips. All sensations are normal responses, so try not to worry too much about what you should or should not be doing. Instead, try to focus on small things which you know make your breathing easier to manage. Why does my lung condition make me breathless? Many different things can make people feel breathless. Symptoms such as feeling tight or wheezy, having more sputum in your lungs or being tired are just some examples. Try to find out what causes your breathlessness. Ask your physiotherapist. backward lean standing forward lean standing What can I do to manage my breathlessness? Breathlessness is, understandably, a difficult feeling to cope with. For this reason it is valuable for you to feel in control of it. 9 10
Breathing Exercises and Clearing Your Chest
 Information for patients Breathing Exercises and Clearing Your Chest Physiotherapy Department Tel: 01473 702073 DMI ref: 1898-08.indd(RP) Issue 1: October 2008 The Ipswich Hospital NHS Trust, 2008. All
Information for patients Breathing Exercises and Clearing Your Chest Physiotherapy Department Tel: 01473 702073 DMI ref: 1898-08.indd(RP) Issue 1: October 2008 The Ipswich Hospital NHS Trust, 2008. All
Physiotherapy for Video Assisted Thoracic Surgery Patients
 Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
Physio for VATS patients Royal Devon and Exeter NHS Foundation Trust Physiotherapy for Video Assisted Thoracic Surgery Patients July 2008 (Review date: July 2011) Physiotherapy Department...01392 402438
Active Cycle of Breathing Technique
 Patient Information Leaflet Physiotherapy Department Active Cycle of Breathing Technique Derriford Hospital Derriford Road Plymouth PL6 8DH Tel: 0845 155 8155 www.plymouthhospitals.nhs.uk Active Cycle
Patient Information Leaflet Physiotherapy Department Active Cycle of Breathing Technique Derriford Hospital Derriford Road Plymouth PL6 8DH Tel: 0845 155 8155 www.plymouthhospitals.nhs.uk Active Cycle
Physiotherapy for COPD. Chronic Obstructive Pulmonary Disease (COPD) Healthcare you can Trust. Pulmonary Rehabilitation
 Pulmonary Rehabilitation Pulmonary rehabilitation is a course of exercise and education designed to help people with COPD get fitter, cope with their symptoms and understand their condition better. Evidence
Pulmonary Rehabilitation Pulmonary rehabilitation is a course of exercise and education designed to help people with COPD get fitter, cope with their symptoms and understand their condition better. Evidence
Help Yourself Breathe. Tender Loving Care for Your Lungs. Department of Physiotherapy. PD 1359 (Rev 06-2009) File: peyles
 Help Yourself Breathe Tender Loving Care for Your Lungs PD 1359 (Rev 06-2009) File: peyles Department of Physiotherapy Why are you breathless? Chronic Airflow Limitation or Obstruction is a decrease in
Help Yourself Breathe Tender Loving Care for Your Lungs PD 1359 (Rev 06-2009) File: peyles Department of Physiotherapy Why are you breathless? Chronic Airflow Limitation or Obstruction is a decrease in
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
MANAGING BREATHLESSNESS
 12 Leaflet issued by: Pulmonary Rehabilitation Service Anglian Community Enterprise (CIC) Kennedy House Kennedy Way, Clacton-on-sea Essex CO15 4AB Tel: 01255 206263 MANAGING BREATHLESSNESS On request,
12 Leaflet issued by: Pulmonary Rehabilitation Service Anglian Community Enterprise (CIC) Kennedy House Kennedy Way, Clacton-on-sea Essex CO15 4AB Tel: 01255 206263 MANAGING BREATHLESSNESS On request,
Managing my Breathlessness
 James Paget University Hospitals NHS Foundation Trust Managing my Breathlessness Patient Information Contents Living with breathlessness 3 Battery life 4 How can I control my breathlessness? 5 Simple breathing
James Paget University Hospitals NHS Foundation Trust Managing my Breathlessness Patient Information Contents Living with breathlessness 3 Battery life 4 How can I control my breathlessness? 5 Simple breathing
Stem cell transplant, you and your rehabilitation Information for patients and their carers
 Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Anxiety and breathing difficulties
 Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Section 2. Breathlessness Management
 Section 2 Breathlessness Management Breathlessness Management Breathing techniques There are various techniques for coping with breathlessness. If you practice these every day when sitting, as you become
Section 2 Breathlessness Management Breathlessness Management Breathing techniques There are various techniques for coping with breathlessness. If you practice these every day when sitting, as you become
Breathlessness. and anxiety. Being anxious can make breathlessness feel worse. Not being able to catch your breath can be very frightening
 Breathlessness and anxiety Being anxious can make breathlessness feel worse Not being able to catch your breath can be very frightening Learning to relax and slow down can help to build your confidence
Breathlessness and anxiety Being anxious can make breathlessness feel worse Not being able to catch your breath can be very frightening Learning to relax and slow down can help to build your confidence
Breathing techniques to help breathlessness 1
 Breathing techniques to help breathlessness 1 Breathing techniques to help breathlessness This information is from the booklet Managing breathlessness. You may find the full booklet helpful. We can send
Breathing techniques to help breathlessness 1 Breathing techniques to help breathlessness This information is from the booklet Managing breathlessness. You may find the full booklet helpful. We can send
WHEN COPD* SYMPTOMS GET WORSE
 WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
Department of Surgery
 Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
These factors increase your chance of developing emphysema. Tell your doctor if you have any of these risk factors:
 Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
Emphysema Pronounced: em-fiss-see-mah by Debra Wood, RN En Español (Spanish Version) Definition Emphysema is a chronic obstructive disease of the lungs. The lungs contain millions of tiny air sacs called
BREATHING TECHNIQUES for BREATHLESS MANAGEMENT in CHRONIC RESPIRATORY CONDITIONS
 BREATHING TECHNIQUES for BREATHLESS MANAGEMENT in CHRONIC RESPIRATORY CONDITIONS AIM To be able to safely and effectively teach and supervise a service user undertaking techniques to minimise breathlessness
BREATHING TECHNIQUES for BREATHLESS MANAGEMENT in CHRONIC RESPIRATORY CONDITIONS AIM To be able to safely and effectively teach and supervise a service user undertaking techniques to minimise breathlessness
Pneumonia. Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid.
 Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
A Stretch-Break Program for Your Workplace! www.healthyworkplaceweek.ca
 www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
Controlling symptoms of mesothelioma
 Controlling symptoms of mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Controlling symptoms of mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
a patient s guide Physiotherapy advice and exercises from four weeks after neck dissection surgery
 Physiotherapy advice and exercises from four weeks after neck dissection surgery Patient Information Series PI 47 East and North Hertfordshire NHS Trust 2 This leaflet has been produced by professionals,
Physiotherapy advice and exercises from four weeks after neck dissection surgery Patient Information Series PI 47 East and North Hertfordshire NHS Trust 2 This leaflet has been produced by professionals,
Living with a lung condition:
 Living with a lung condition: how exercise and eating well can make a difference to your life This information is for people living with a lung condition in the UK and your family and carers. It will help
Living with a lung condition: how exercise and eating well can make a difference to your life This information is for people living with a lung condition in the UK and your family and carers. It will help
Physiotherapy treatment in cystic fibrosis: airway clearance techniques
 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Factsheet March 2013 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Introduction Looking after the chest
Physiotherapy treatment in cystic fibrosis: airway clearance techniques Factsheet March 2013 Physiotherapy treatment in cystic fibrosis: airway clearance techniques Introduction Looking after the chest
CONTENTS. Note to the Reader 00. Acknowledgments 00. About the Author 00. Preface 00. Introduction 00
 Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Natural Therapies for Emphysema By Robert J. Green Jr., N.D. CONTENTS Note to the Reader 00 Acknowledgments 00 About the Author 00 Preface 00 Introduction 00 1 Essential Respiratory Anatomy and Physiology
Chronic Obstructive Pulmonary Disease Patient Guidebook
 Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Chronic Obstructive Pulmonary Disease Patient Guidebook The Respiratory System The respiratory system consists of the lungs and air passages. The lungs are the part of the body where gases are exchanged
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Sensory Sanctuary Staff Occupational Therapy Stress Management Program [email protected]
 Abdominal Breathing Technique How it s done: With one hand on the chest and the other on the belly, take a deep breath in through the nose, ensuring the diaphragm (not the chest) inflates with enough air
Abdominal Breathing Technique How it s done: With one hand on the chest and the other on the belly, take a deep breath in through the nose, ensuring the diaphragm (not the chest) inflates with enough air
Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods. *Includes chronic bronchitis, emphysema, or both.
 DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
Returning to fitness after heart surgery
 Returning to fitness after heart surgery A patient s guide 1 Increasing activity After your operation, your heart function should be improved and so your ability to exercise will also be improved. However,
Returning to fitness after heart surgery A patient s guide 1 Increasing activity After your operation, your heart function should be improved and so your ability to exercise will also be improved. However,
How to Do Chest Physical Therapy (CPT) Babies and Toddlers
 How to Do Chest Physical Therapy (CPT) Babies and Toddlers (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital 1 2 (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital Name of
How to Do Chest Physical Therapy (CPT) Babies and Toddlers (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital 1 2 (2001, 2004, 2009) The Emily Center, Phoenix Children s Hospital Name of
LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS
 LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises
LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises
About lung cancer. Contents. The lungs
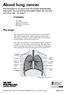 This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
This information is an extract from the booklet Understanding lung cancer. You may find the full booklet helpful. We can send you a free copy see page 7. The lungs Contents The lungs Types of lung cancer
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Lesson 7: Respiratory and Skeletal Systems and Tuberculosis
 Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Objective: Identify effects of stress on everyday issues and strategies to reduce or control stress.
 Lesson Plan: Dealing with Stress Objective: Identify effects of stress on everyday issues and strategies to reduce or control stress. Time: 45-60 minutes Structure: On-line homework before class (Stress
Lesson Plan: Dealing with Stress Objective: Identify effects of stress on everyday issues and strategies to reduce or control stress. Time: 45-60 minutes Structure: On-line homework before class (Stress
Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods. *Includes chronic bronchitis, emphysema, or both.
 DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
A Guide to Controlled Breathing (Pursed Lips Breathing)
 A Guide to Controlled Breathing (Pursed Lips Breathing) Your doctor or nurse may suggest that you learn how to do controlled breathing. This can help to ease shortness of breath (breathlessness) caused
A Guide to Controlled Breathing (Pursed Lips Breathing) Your doctor or nurse may suggest that you learn how to do controlled breathing. This can help to ease shortness of breath (breathlessness) caused
stretches and exercises
 stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
stretches and exercises The enclosed sheets contain stretches and exercises which can be used to delay and minimise the development of contractures and deformities occurring in children with Duchenne muscular
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY
 BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
Things you might want to ask about asthma
 Things you might want to ask about asthma This information is from Asthma UK. We are a charity that helps people with asthma. EasyRead version What is asthma? If you have asthma your airways do not work
Things you might want to ask about asthma This information is from Asthma UK. We are a charity that helps people with asthma. EasyRead version What is asthma? If you have asthma your airways do not work
Managing Side Effects of Palliative Radiation Therapy
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Side Effects of Palliative Radiation Therapy In this booklet you will learn about: Common side effects when you receive palliative radiation therapy Tips on
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Side Effects of Palliative Radiation Therapy In this booklet you will learn about: Common side effects when you receive palliative radiation therapy Tips on
Symptoms of Hodgkin lymphoma
 Produced 28.02.2011 Revision due 28.02.2013 Symptoms of Hodgkin lymphoma Lymphoma is a cancer of cells called lymphocytes. These cells are part of our immune system, which helps us to fight off infections.
Produced 28.02.2011 Revision due 28.02.2013 Symptoms of Hodgkin lymphoma Lymphoma is a cancer of cells called lymphocytes. These cells are part of our immune system, which helps us to fight off infections.
Breathlessness. www.roycastle.org. What is breathlessness? What causes breathlessness?
 What is breathlessness? All of us at some time in our lives have experienced shortness of breath, perhaps from over exertion, the after effects of a chest cold or when feeling particularly anxious or excited.
What is breathlessness? All of us at some time in our lives have experienced shortness of breath, perhaps from over exertion, the after effects of a chest cold or when feeling particularly anxious or excited.
General Home Activity and Exercise Guidelines
 General Home Activity and Exercise Guidelines After a Heart Attack / Angina Angioplasty / Stent Heart Failure Heart Health Risk Reduction Program Vancouver Island Health Authority Created January 2002;
General Home Activity and Exercise Guidelines After a Heart Attack / Angina Angioplasty / Stent Heart Failure Heart Health Risk Reduction Program Vancouver Island Health Authority Created January 2002;
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery
 CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
Asthma and COPD Awareness
 Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Asthma and COPD Awareness Molina Breathe with Ease sm and Chronic Obstructive Pulmonary Disease Molina Healthcare of Michigan Fall 2012 Importance of Controller Medicines Asthma is a disease that causes
Patient Information. and Physical Activity Diary. Wythenshawe Hospital Cardiac Rehabilitation. Name:... The ticker club Registered Charity No.
 Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
There is no cure for COPD Chronic Bronchitis Emphysema
 Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Young Person s Guide to CFS/ME
 Young Person s Guide to CFS/ME The Royal College of Paediatrics and Child Health This leaflet has been developed as part of the Evidence based guideline for management of CFS/ME (Chronic Fatigue Syndrome
Young Person s Guide to CFS/ME The Royal College of Paediatrics and Child Health This leaflet has been developed as part of the Evidence based guideline for management of CFS/ME (Chronic Fatigue Syndrome
Occupational therapy after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
Chronic obstructive pulmonary disease (COPD)
 Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
Chronic obstructive pulmonary disease (COPD) Chronic obstructive pulmonary disease (COPD) is the name for a group of lung diseases including chronic bronchitis, emphysema and chronic obstructive airways
We as COPD ers have to deal with our breathing on so many levels: (1). The psychology of breathing - How anxiety affects our breathing.
 This is from a letter that a member of COPD-International and others, Filcab, developed for publication and sharing with everyone. He would like everyone either who has COPD or works with COPDers to have
This is from a letter that a member of COPD-International and others, Filcab, developed for publication and sharing with everyone. He would like everyone either who has COPD or works with COPDers to have
Enhancing your recovery after cardiac surgery
 Enhancing your recovery after cardiac surgery Steps you can take to get better sooner Patient s name:... Consultant s name:... Admission date:... Planned discharge date:... Type of operation:... Date of
Enhancing your recovery after cardiac surgery Steps you can take to get better sooner Patient s name:... Consultant s name:... Admission date:... Planned discharge date:... Type of operation:... Date of
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD)
 Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Medication and Devices for Chronic Obstructive Pulmonary Disease (COPD) Patients with COPD take a wide variety of medicines to manage their symptoms these include: Inhaled Short Acting Bronchodilators
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Take a few minutes for yourself and incorporate some Office Yoga into your daily routine.
 OFFICE YOGA Working in an office or at a computer for prolonged periods of time can put strain on the neck, shoulder and back muscles which in turn can lead to tension and stiffness. This tension can cause
OFFICE YOGA Working in an office or at a computer for prolonged periods of time can put strain on the neck, shoulder and back muscles which in turn can lead to tension and stiffness. This tension can cause
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
COPD - Education for Patients and Carers Integrated Care Pathway
 Patient NHS COPD - Education for Patients and Carers Integrated Care Pathway Date ICP completed:. Is the patient following another Integrated Care Pathway[s].. / If yes, record which other Integrated Care
Patient NHS COPD - Education for Patients and Carers Integrated Care Pathway Date ICP completed:. Is the patient following another Integrated Care Pathway[s].. / If yes, record which other Integrated Care
The Doctor-Patient Relationship
 The Doctor-Patient Relationship It s important to feel at ease with your doctor. How well you are able to talk with your doctor is a key part of getting the care that s best for you. It s also important
The Doctor-Patient Relationship It s important to feel at ease with your doctor. How well you are able to talk with your doctor is a key part of getting the care that s best for you. It s also important
Axillary Lymph Node Dissection: Instructions/Exercises
 Axillary Lymph Node Dissection: Instructions/Exercises The following activities have been approved by your physician to help you increase the motion and strength of your shoulder and improve your posture
Axillary Lymph Node Dissection: Instructions/Exercises The following activities have been approved by your physician to help you increase the motion and strength of your shoulder and improve your posture
The advanced back rehabilitation programme
 Physiotherapy Department The advanced back rehabilitation programme This booklet explains what happens during the advanced back rehabilitation programme and how the exercises may help your condition. We
Physiotherapy Department The advanced back rehabilitation programme This booklet explains what happens during the advanced back rehabilitation programme and how the exercises may help your condition. We
Anxiety. Providing services we would be happy for our own families to use
 Anxiety Providing services we would be happy for our own families to use An information guide for Anxiety This booklet aim to: Give you an understanding of Anxiety, it s causes and symptoms Provide information
Anxiety Providing services we would be happy for our own families to use An information guide for Anxiety This booklet aim to: Give you an understanding of Anxiety, it s causes and symptoms Provide information
Manage cancer related fatigue:
 Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Operating Instructions
 Operating Instructions Table of Contents IMPORTANT INFORMATION 1-2 1 The backrack TM 3-6 Introduction 3 What does it do? 4 How do I use it? 5 How often should I use it? 6 2 Getting On 7-10 3 Basic Exercises
Operating Instructions Table of Contents IMPORTANT INFORMATION 1-2 1 The backrack TM 3-6 Introduction 3 What does it do? 4 How do I use it? 5 How often should I use it? 6 2 Getting On 7-10 3 Basic Exercises
What is Separation of the Abdominal Muscles after Childbirth (also known as Divarication of Rectus Abdominis)?
 What is Separation of the Abdominal Muscles after Childbirth (also known as Divarication of Rectus Abdominis)? Following your pregnancy and the birth of your baby your abdominal (tummy) muscles may have
What is Separation of the Abdominal Muscles after Childbirth (also known as Divarication of Rectus Abdominis)? Following your pregnancy and the birth of your baby your abdominal (tummy) muscles may have
BREATHE BETTER SWIM FASTER
 BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
BREATHE BETTER SWIM FASTER Breath control is fundamental to efficient swimming. Like singers, swimmers need to train their breathing for effective performance. Controlled breathing is the main factor contributing
Otago Exercise Program
 Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Caring for your body. Antenatal exercises
 Caring for your body Antenatal exercises Antenatal Exercises FROM EARLY PREGNANCY TO DELIVERY INTRODUCTION.................................................3 DEEP BREATHING & FOOT AND ANKLE EXERCISES..................4
Caring for your body Antenatal exercises Antenatal Exercises FROM EARLY PREGNANCY TO DELIVERY INTRODUCTION.................................................3 DEEP BREATHING & FOOT AND ANKLE EXERCISES..................4
Stress management for presentations and interviews
 Learning Development Stress management for presentations and interviews This guide aims to help you recognise and understand anxiety and nervousness which may arise during presentations or interviews.
Learning Development Stress management for presentations and interviews This guide aims to help you recognise and understand anxiety and nervousness which may arise during presentations or interviews.
& WHEN SHOULD I WORRY?
 WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
WHEN SHOULD I WORRY? - Your guide to Coughs, Colds, Earache & Sore Throats Information For:- Who is this booklet for? Having an ill child can be a very scary experience for parents. If you understand more
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
CorCap Cardiac Support Device Patient Information Booklet
 What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
What is Heart Failure? CorCap Cardiac Support Device Patient Information Booklet Heart failure is a condition in which the heart is unable to pump enough blood to meet the needs of the body. To compensate
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Info. from the nurses of the Medical Service. LOWER BACK PAIN Exercise guide
 Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
COPD What Is It? Why is it so hard to catch my breath? What does COPD feel like? What causes COPD? What is an exacerbation (ig-zas-er-bay-shun)?
 Attitudes and Beliefs 4 COPD What Is It? Why is it so hard to catch my breath? COPD is a disease that damages the lungs. In a healthy lung, the airways are open and the air sacs fill up with air. Then
Attitudes and Beliefs 4 COPD What Is It? Why is it so hard to catch my breath? COPD is a disease that damages the lungs. In a healthy lung, the airways are open and the air sacs fill up with air. Then
Exercises and advice for patients recovering from thyroid surgery
 Exercises and advice for patients recovering from thyroid surgery Information for patients who have had surgery for conditions affecting their thyroid gland Following your thyroid surgery, the position
Exercises and advice for patients recovering from thyroid surgery Information for patients who have had surgery for conditions affecting their thyroid gland Following your thyroid surgery, the position
The Well Woman Centre. Adult Urinary Incontinence
 The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
The Well Woman Centre Adult Urinary Incontinence 1 Adult Urinary Incontinence... 3 Stress Incontinence Symptoms... 3 Urge Incontinence Symptoms... 4 Mixed Incontinence Symptoms... 5 Where to Start?...
FROZEN SHOULDER OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU. Frozen Shoulder FROZEN SHOULDER
 OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..?
 Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..? Staying healthy at work is easier than you might think: Try building the following desk based exercises into your
Do you sit at a desk all day? Does your 9 to 5 leave no time for structured exercise..? Staying healthy at work is easier than you might think: Try building the following desk based exercises into your
Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre
 Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre Introduction...2 Patient Education and Information...2&3 Treatment Planning...3&4 Your Appointments...5 Radiation
Radiation Therapy for Palliative Treatment at The Carlo Fidani Peel Regional Cancer Centre Introduction...2 Patient Education and Information...2&3 Treatment Planning...3&4 Your Appointments...5 Radiation
Epilepsy and stress / anxiety
 Epilepsy and stress / anxiety Stress is a term used to describe emotional strain and tension. When we experience stress we also can become anxious. Although stress and anxiety do not cause epilepsy, for
Epilepsy and stress / anxiety Stress is a term used to describe emotional strain and tension. When we experience stress we also can become anxious. Although stress and anxiety do not cause epilepsy, for
COPD. Information brochure for chronic obstructive pulmonary disease.
 COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
COPD Information brochure for chronic obstructive pulmonary disease. CONTENTS What does COPD mean?...04 What are the symptoms of COPD?...06 What causes COPD?...09 Treating COPD...10 Valve therapy in COPD...12
St. George s Respiratory Questionnaire PART 1
 ST. GEORGE S RESPIRATORY QUESTIONNAIRE ORIGINAL ENGLISH VERSION ST. GEORGE S RESPIRATORY QUESTIONNAIRE (SGRQ) This questionnaire is designed to help us learn much more about how your breathing is troubling
ST. GEORGE S RESPIRATORY QUESTIONNAIRE ORIGINAL ENGLISH VERSION ST. GEORGE S RESPIRATORY QUESTIONNAIRE (SGRQ) This questionnaire is designed to help us learn much more about how your breathing is troubling
National Hospital for Neurology and Neurosurgery. Migraine associated dizziness Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
Fatigue Beyond Tiredness
 Fatigue Beyond Tiredness The development and printing of this booklet was sponsored by Roche Products Ltd and Chugai Pharma UK Ltd. Editorial control remains with NRAS. Have you ever: Got all dressed up
Fatigue Beyond Tiredness The development and printing of this booklet was sponsored by Roche Products Ltd and Chugai Pharma UK Ltd. Editorial control remains with NRAS. Have you ever: Got all dressed up
How to Do Self Lymphatic Massage on your Upper Body
 How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
How to Do Self Lymphatic Massage on your Upper Body UHN For patients who were treated for breast cancer on one side of their body. For example: Lumpectomy Mastectomy Lymph node removal from an underarm
