Creating a Culture of Safety for Safe Patient Handling
|
|
|
- Lucinda Oliver
- 7 years ago
- Views:
Transcription
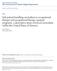
1 Creating a Culture of Safety for Safe Patient Handling Linda Stevens Susan Rees Karen V. Lamb Deborah Dalsing Healthcare workers who handle patients have little guidance to help them identify when to use the existing equipment for moving patients. Manual lifting of patients and healthcare worker injuries continue despite equipment installation and training. The purpose of this project was to decrease the number and severity of healthcare worker injuries by implementing a culture of safety for safe patient handling. A multicomponent safe patient handling program was deployed on one inpatient unit at a Midwest academic acute care hospital. There was a 36% decrease in the number of patient handling injuries, a 71% reduction in the number of lost work days, and a 60% reduction in costs in 1 year related to patient handling injuries. The RN Satisfaction Survey question regarding having enough help to lift/ move on last shift improved from 41% presurvey to 69% postsurvey. Musculoskeletal disorders in healthcare workers are a result of the continual manual lifting of patients (Waters, Collins, Galinsky, & Caruso, 2006). Healthcare workers at the University of Wisconsin Hospital and Clinics (UWHC) who handle patients had little guidance to help them identify when to use the existing equipment for moving patients. Manual lifting of patients continued despite equipment installation and training. As a result, healthcare workers on the inpatient care units continued to be injured from patient handling tasks. UWHC workers compensation claim costs related to patient handling injuries ranged from $114,000 to $814,000 per year from 2006 to 2010 per review of information from the organizations insurance carrier. The UWHC had 203 ceiling lifts installed in inpatient areas as of April In addition, there were seven portable lifts, three sit-to-stand devices, and six frictionreducing lateral transfer devices for 566 inpatient beds. The ceiling lifts were installed in phases beginning in Whereas costs of injuries decreased temporarily with the installation of the ceiling lifts, costs of injuries continued to rise in 2009 and Seventeen of the 23 inpatient units reported not using the ceiling lifts, and only two of the 23 inpatient units required staff to complete an annual checklist to demonstrate the proper use of the equipment as part of 2009 annual review. The environment in which registered nurses work in acute care settings is both physically and cognitively demanding (Kalish & Aebersold, 2010; Trinkoff et al., 2008 ). Musculoskeletal injuries and disorders are costly and prevalent in nursing and healthcare workers (Nelson et al., 2006 ). Research over the years has determined that there is no safe way to manually lift a patient (Marras, Davis, Kirking, & Bertsche, 1999; Waters, 2007 ). Programs developed using manual lifts to mobilize patients have been termed Safe Patient Handling Programs (Nelson, Collins, Siddharthan, Matz, & Waters, 2008). These programs involve analyzing highrisk patient care activities, assessing and planning for patient need for assistance in movement, and using the appropriate equipment to move patients on the basis of the assessment. Attaining and maintaining a culture of safety for safe patient handling are challenging. Providing equipment and training only on the equipment does not ensure that healthcare workers will use the equipment (Pellino, Owen, Knapp, & Noack, 2006). Program outcomes such as healthcare worker injury rates for safe patient handling programs are enhanced when multifaceted approaches are included in program implementation (Collins, Wolf, Bell, & Evanoff, 2004; Evanoff, Wolf, Aton, Canos, & Collings, 2003; Nelson et al., 2006 ; Yassi et al., 2004 ). Multifaceted approaches to program implementation continue to demonstrate a reduced incidence of employee injury, even though self-reporting of compliance with the minimal lift policy 1 year after implementation was 42.8% at the Children's Hospital and Clinics of Minnesota (Haglund, Kyle, & Finkelstein, 2010). Linda Stevens, DNP, RN-BC, CPHQ, CSPHP, Director, Nursing Quality & Safety, University of Wisconsin Hospital and Clinics, Madison. Susan Rees, DNP, RN, CPHQ, CENP, Vice President, Development, Nursing and Patient Care Services, University of Wisconsin Hospital and Clinics, Madison. Karen V. Lamb, DNP, RN, GCNS-BC, Associate Professor, College of Nursing, Rush University Medical Center, Chicago, IL. Deborah Dalsing, MS, RN, Nurse Manager, Acute Medical/Progressive Care Unit, University of Wisconsin Hospital and Clinics, Madison. The authors have disclosed that they have no financial interests to any commercial company related to this educational activity. DOI: /NOR.0b013e318291dbc by National Association of Orthopaedic Nurses Orthopaedic Nursing May/June 2013 Volume 32 Number 3 155
2 Documented components of a culture of safe patient handling include visible support from leadership, accountability for safety, unit-based program champions, focus on system barriers, providing after action event reviews, and using data to analyze effectiveness of the program (Dugan, 2010 ; Hignett, 2003 ). Properties identified in the literature to create and sustain a culture of safety include leadership, teamwork, speaking up on the behalf of patients, learning from mistakes, a just culture that recognizes the contribution of system failures in addition to individual accountability, and focus on patient-centered care (Sammer, Lykens, Singh, Mains, & Lackan, 2010). One general medical unit at the UWHC provided education to unit staff in March 2010 on how to use patient handling equipment. After the education, the unit staff was asked to complete a survey to determine whether equipment was being used and barriers to equipment use. The amount of time to locate the equipment and accessories was the biggest barrier for nurses not to use mechanical lifts (67%), followed by isolation status (60%) and perception of having enough staff to manually lift the patient (40%). The time was right for developing a culture of safety for safe patient handling to change the behaviors of healthcare workers and decrease injuries. The purpose of this project was to decrease the number and severity of healthcare worker injuries on one inpatient care unit at the UWHC by implementing a culture of safety for safe patient handling. Literature Review Healthcare workers continue to have one of the higher rates of injury (Bureau of Labor Statistics, 2010). Many of theses injuries are musculoskeletal and result from patient handling. Injuries occur when the load on the tissue exceeds the tissue tolerance (Marras, 2005 ). An increased load or a decrease in tolerance leads to injury. The National Institute for Occupational Safety and Health developed a lifting equation, which recommends lifting no greater than 51 pounds under ideal conditions (Waters, 1993 ). In examining the biomechanical loads for patient handling tasks, it was discovered that the spinal loading was different in patient handling tasks than other manufacturing or warehousing lifting tasks (Nelson, Lloyd, Menzel, & Gross, 2003). Based on this information, the maximum amount of weight for patient handling has been determined to be 35 pounds under ideal conditions (Waters, 2007 ). Because a small percentage of the patient population in healthcare settings weighs less than 35 pounds, different methods other than lifting patients are needed to control the risk for injury. Various approaches have been studied to determine how to continue to keep patients and healthcare workers safe. Nelson and Baptiste (2006) emphasized that high-risk patient handling tasks are different in various environments, and acknowledged the need to group the solutions for controlling risk into engineering, administrative, and behavioral controls. Effective engineering interventions included using patient handling equipment and devices (Nelson & Baptiste, 2006). Many studies have demonstrated that using equipment decreases the spinal load on workers (Dayndar et al., 2001 ; Marras, Knapik, & Ferguson, 2009; Schibye et al., 2003 ; Village et al., 2005 ). But training alone for both equipment and cognitive behavior has not had an effect on musculoskeletal health (Tullar et al., 2010 ). Effective administrative controls to promote safe patient handling include patient care ergonomic assessment protocols, no lift policies, and lift teams (Nelson & Baptiste, 2006). Training on the appropriate use of lifting equipment was reported to be an effective behavioral intervention (Nelson & Baptiste, 2006). Instruction on how to manually lift a patient did not result in any changes in back pain by hospital employees (Fanello, Jousset, Roquelaure, Chotard-Frampas, & Delbos, 2002). Hignett (2003) reviewed the literature from 1960 to 2003 for interventions that would decrease the risk of healthcare workers being injured from patient handling activities and found that training on technique does not change practice or impact injury rates for workers who complete patient handling activities. Some interventions were lacking strong evidence but were reported to be promising. These include the use of patient assessment protocols (administrative control) and unit-based peer leaders (behavioral control) (Nelson & Baptiste, 2006). Hignett (2003) suggested that multifactor interventions should be used to decrease the risk for patient handling. They include state-of-the-art equipment; education and training on risk assessment, patient assessment, and equipment; risk assessment; patient assessment system; policy and procedure; redesigned work environment; and a change in practice (Hignett, 2003 ). Many of these interventions were identified by Nelson and Baptise (2006) as effective or promising. Tullar et al. (2010) completed a systematic review and found 16 studies to answer the question Do occupational safety and health interventions in healthcare settings have an effect on musculoskeletal health status? (p. 199). A moderate level of evidence was found for exercise interventions and multifactor patient handling interventions, which include organizational policy change, lift or transfer equipment, and training on equipment (Tullar et al., 2010 ). Consequently, multifactor interventions should be used to build a culture of safety for safe patient handling. Multifactor interventions for safe patient handling have demonstrated a reduction in workers compensation cost, injury incidence rates, and lost work days in acute care facilities and in nursing homes located in different countries (Alamgir et al., 2008 ; Charney, Simmons, Lary, & Metz, 2006; Collins et al., 2004; Evanoff et al., 2003 ; Haglund et al., 2010 ; Hunter, Branson, & Davenport, 2010; Nelson et al., 2006 ; Silverwood & Haddock, 2006; Stenger, Montgomery, & Briesemeister, 2007). The implementation of programs using patient handling equipment and other interventions has consistently demonstrated significant decreases in workers compensation costs from preintervention periods to postintervention periods (Alamgir et al., 2008 ; Charney et al., 2006 ; Collins et al., 2004 ; Engst, Chhokar, Miller, Tate, & Yassi, 2005; Haglund et al., 2010 ; Hunter et al., 2010 ; Nelson et al., 156 Orthopaedic Nursing May/June 2013 Volume 32 Number by National Association of Orthopaedic Nurses
3 2006 ; Stenger et al., 2007 ). The workers compensation costs reported in these studies have been identified as direct costs of injuries and include medical expenses, program administrative costs, and compensation (Alamgir et al., 2008 ; Engst et al., 2005 ). Calculating cost benefit ratios and return on investment for program analysis is typically reported by measuring only direct costs because indirect costs are difficult to calculate. Indirect costs are estimated to be double or triple that of direct care costs and include costs such as internal employee health costs, benefits, turnover, sick leave, recruitment and retention costs, orientation costs, and employee morale (Alamgir et al., 2008 ; Hunter et al., 2010 ). Several studies that reported reductions in workers compensation costs, lost work days, and/or a reduction in injury rates also collected data on equipment use. Evanoff et al. (2003) acknowledged a self-reported lift usage of 38% in nursing homes and 15% in acute care with significant reductions in injury rates and lost work day injury rates. After 3 months postimplementation, Wardell (2007) reported a 61% reduction in injuries with healthcare workers self-reporting use of equipment 29% of the time. After implementing a multifactor program in a pediatric setting, 42.8% of nurses selfreported using the equipment according to policy with a 71.4% reduction in injury incidence and an average reduction in direct cost of $4,508 per year of injury (Haglund et al., 2010 ). It appears that even a less than 50% self-reported use of equipment results in significant decreases in workers compensation costs and injury incidence with the implementation of multifactor safe patient handling programs. Unfortunately, using equipment for some high-risk tasks, but not all high-risk tasks, highlights that changing the culture to match a minimal lift policy is very difficult. Changing the culture of safety for safe patient handling takes time and continuous attention for sustainability (Hunter et al., 2010 ; Stenger et al., 2007 ). The multifactor interventions need to address engineering, administrative, and behavioral controls for reducing healthcare worker injury and associated costs. In 2003, the American Nurses Association (ANA) began promoting safe patient handling programs through the Handle With Care campaign (ANA, 2004). They continued to promote safe patient handling by launching The ANA Handle with Care Recognition Program in 2009 but withdrew the program nearly a year later (ANA, 2009a). This program provided recognition to facilities who comply with criteria for developing safe patient handling programs. Program criteria were comprehensive and included many of the components identified to create a culture for safe patient handling by addressing engineering, administrative, and behavioral controls (ANA, 2009b). The ANA continues to be an advocate and supports safe patient handling to prevent injuries and protect the well-being of nurses (ANA, 2013). The National Association of Orthopaedic Nursing has made recommendations and offered specific recommendations for orthopaedic nursing practice related to patient handling in a special supplement to Orthopaedic Nursing (Sedlak, Dohey, Nelson & Waters, 2009). Implementation P URPOSE The purpose of this project was to decrease the number and severity of healthcare worker injuries for one inpatient nursing unit at the UWHC by implementing a culture of safety for safe patient handling using an evidence-based program. The project included implementation of a safe patient handling program on one early adopter unit and evaluated program outcomes from this unit. S ETTING The UWHC is an academic medical center with 566 licensed acute care beds, a Level 1 trauma center, and has been designated a Magnet Hospital by the American Nurse Credentialing Center. The early adopter unit is a 29-bed progressive care inpatient unit. Eight of the 29 beds provide an intermediate level of care, whereas the remaining beds are intended for general medical acute care. This unit was selected because of the high volume and cost of injuries in addition to having a nurse manager very interested in and supportive of program implementation. M ARKETING The program was marketed to all levels in the organization. Marketing started by gaining awareness of the problem of patient handling and how injuries to healthcare workers can be career limiting. All workers on the unit were targeted for program awareness, as well as nursing and rehabilitation leaders throughout the organization. A slogan was developed to market the program. The program at the UWHC was marketed as SMART (Safe Movement and Repositioning Techniques). A tip of the week poster was placed in visible areas on the unit with the SMART marketing materials. All program content and tips were made available on the organizations intranet. The program was introduced at various meetings, and regular updates on the project were provided to the nurse executive council, nursing management council, clinical nurse specialist forum, nursing practice council, nursing quality council, and safety resource nurse meetings. Excitement for the program was corroborated when many of the inpatient units requested to also begin the program immediately. P ROJECT IMPLEMENTATION AND EVOLUTION The project was implemented in various phases on the early adopter unit. The phases of the project were awareness, assessment, education, and implementation/ sustainability. The awareness phase occurred from May 2010 until August 2010, in which program planning was completed in addition to heightening staff awareness of the problem. Having a few of the selected peer leaders from the unit conduct observations to assess high-risk patient handling tasks on the unit as part of the unit ergonomic assessment proved to be an eyeopening experience for the staff who participated. The individuals were surprised by how many at-risk patient handling activities they completed and the awkward 2013 by National Association of Orthopaedic Nurses Orthopaedic Nursing May/June 2013 Volume 32 Number 3 157
4 TABLE 1. CREATING A CULTURE OF SAFETY FOR SAFE PATIENT HANDLING PROJECT PHASES AND TASKS Awareness Phase Assessment Phase Education Phase Initiation/Sustainability Phase Develop Safe Patient Handling Coordinator position description Identify unit-based peer leaders Educate peer leaders (4 hours) Educate new healthcare workers who handle patients Develop marketing slogan/campaign Inform physical therapy of unit timeline Educate all staff (10-minute computerbased training and 1-hour equipment training) Educate all unit staff annually Meet with unit clinical nurse manager, clinical nurse specialist, and nursing education specialist and safe patient handling coordinator Discuss initial timeline Assess support for project initiation Review roles and responsibilities Identify unit physical therapist Plan for identifying unit-based peer leaders Complete unit assessment: Healthcare Worker Injury Prevention Survey Observation of patient handling tasks Weight and body mass index data Dependency levels of patients Safety Resource Nurse Data Collection Tool Clinical Nurse Manager Data Collection Tool Unit Assessment Summary Workers compensation cost Lost work days Number of injuries related to patient handling Activity related to patient handling injuries Identify and communicate program initiation date Educate staff who turn over key positions (peer leaders, clinical nurse specialists, nursing education specialist, clinical nurse managers, safe patient handling coordinator) Initiate posting of Tip of the Week for Safe Patient Handling Continue posting Tip of the Week for safe patient handling Continue posting Tip of the Week for safe patient handling Program evaluation: Healthcare Worker Injury Prevention Survey at 6 months Observation of patient handling tasks at 1, 3, and 6 months Develop reporting structure for safe patient handling committees Develop intranet site for safe patient handling Order equipment needed for implementation Documentation assessment: Identify patients who require equipment Identify patients who have equipment documented Calculate compliance of equipment use based on documentation monthly and enter on unit scorecard Identify roles and responsibilities for all stakeholders involved with project Develop competency forms, equipment checklists, and guideline for equipment use Unit scorecard data entry Documentation assessment Health Care Worker Injury Prevention Survey Number of patient handling injuries Number of lost work days Determine equipment needs based on assessment Safe patient handling (SPH) coordinator meets with unit-based peer leader at least once per week for 1 month, then monthly to problem solve SPH barriers and issues Develop patient handling assessment criteria Clinical nurse manager and clinical nurse specialist assist unit-based peer leaders in problem solving SPH barriers Continue posting Tip of the Week for safe patient handling as needed Discuss safe patient handling program monthly at unit council meetings Review data/unit scorecard Identify system barriers Develop plans for improvement as needed Develop and monitor plan for equipment maintenance and replacement 158 Orthopaedic Nursing May/June 2013 Volume 32 Number by National Association of Orthopaedic Nurses
5 FIGURE 1. Project timeline for creating a culture of safety for safe patient handling. positions used to complete the tasks. The increased awareness of the problem led the peer leaders to challenge themselves and others for changing how they moved patients. The assessment phase included identification of additional peer leaders for the program and completing a unit-based ergonomic assessment. Key components of the ergonomic assessment were conducting a survey administered to staff who worked on the unit, collecting data on patient weights and dependency levels, and observing high-risk patient handling tasks. Sixty-five of possible 79 staff members (82%) completed the survey. Preimplementation, the survey was a large component of the unit ergonomic assessment. The ergonomic assessment assisted with projecting the amount and type of equipment needed by the unit for program implementation. The assessment phase took place in June and July Once the assessment phase was completed and equipment needs were determined, the education phase took place from August 2010 to January The education phase began with training the unit peer leaders and ended when all unit staff were educated. The nurse manager, clinical nurse specialist, and nursing education specialist all contributed to educating staff. The project was initiated on January 19, 2011, which began the initiation/sustainability phase. Program evaluation occurred throughout this phase and after action event reviews were conducted after each injury related to patient handling. Project tasks during the phases are identified in Table 1. The specific timeline for the project phases are outlined in Figure 1. One month into the initiation/sustainability phase, early adopter unit leadership meetings were set up to discuss observations and program implementation. Other communication methods were then used to confer about the program with the unit-based peer leaders. These included , communication via the nurse manager, and rounding by the safe patient handling coordinator. Having modern equipment hardware, such as ceiling lifts was identified as a critical component to program implementation. While adequate hardware was in place for the program, accessories were required to move the patient with the hardware. The nurse manager reported that during the first month of implementation, 10 of the 20 washable slings ordered were lost, which limited the ability to utilize equipment. A decision was made to use only single-patient-use accessories for the equipment when the single-patient-use option was available from the manufacturer. Key to implementing the project was deploying a multicomponent safe patient handling program. Program components included state-of-the-art equipment for patient handling; education and training on risk assessment, patient assessment, and equipment; unit-based ergonomic assessment; patient handling assessment criteria; guidelines on safe patient handling; visible support from leadership; unit-based program champions; providing after action event reviews; and using data to analyze the effectiveness of the program. Results/Outcome Analysis Outcome data on injuries, lost days from work, and restricted days were summarized and updated monthly. Costs of patient handling injuries were summarized and updated at 6 months, 9 months, and 1 year postimplementation. A before and after implementation comparison was done, and a percent change was calculated, comparing 1 year preimplementation (calendar year 2010) to postimplementation (calendar year 2011). Process evaluation was completed postimplementation by conducting observations of high-risk handling tasks at 1 and 6 months after program initiation, to measure the extent to which equipment was used for high-risk patient handling tasks. After 1 month of the start of safe patient handling program, four undergraduate industrial engineering students were trained to collect data by observing patient handling tasks. The safe patient handling coordinator spent 1 hour observing tasks simultaneously with each student to ensure reliability of the observations. There were 24 observations of patient handling tasks done by the students. Fourteen of the 24 tasks, or 58%, were completed according to the guideline by National Association of Orthopaedic Nurses Orthopaedic Nursing May/June 2013 Volume 32 Number 3 159
6 FIGURE 2. Self-reported use of ceiling lifts pre- and 6 months postimplementation. Six months after program implementation, the observations were completed by the safe patient handling coordinator, a nursing director, and an ergonomic specialist employed by the hospital. There were 15 patient handling observations completed and 10 of the tasks (67%) were completed per the guideline. In addition to observation, self-reported use of equipment was assessed in the Health Care Worker Injury Prevention Survey. The survey was developed internally by the UWHC Safe Patient Handling task force, which included ergonomic specialists with an expertise in patient handling. No psychometric properties are available for the survey. Preimplementation there were 63 responses to this survey, and 6 months postimplementation there were 32 responses. Self-reported data on the use of equipment were gathered in the Nursing Injury Prevention Survey completed pre- and 6 months postimplementation ( Figure 2 ), by the question When the patient status warrants, how often you use the ceiling lifts? Preimplementation the percent response of often and always was 60%, and this increased to 83% postimplementation, a 38% increase in often and always on self-reported equipment use. Always went from 24% to 21%, but this may be due to the fact that there was no guideline preimplementation to define when to use equipment. Costs of patient handling injuries are obtained from a review of costs provided by the insurance carrier for UWHC workers compensation. The data are reviewed by the organizations ergonomic specialist to determine which injuries and costs are related to patient handling and then identifying the cost center of the injury. The direct cost of the injury is reported and includes medical costs, indemnity, administrative costs, and reserves for anticipated costs related to the injury. Because reserves are an estimated cost, the total figure is subject to change until the case is closed. Injury costs are credited to the month and year the injury occurred, irregardless of the date the expense was incurred. One year preimplementation, calendar year 2010, as of February 8, 2012, the direct cost of injury was $86,326. One year postimplementation, calendar year 2011, the direct cost of injury was $34,165. The direct costs of injuries decreased 60% 1 year preimplementation to 1 year postimplementation. The number of injuries related to patient handling was obtained from workers compensation records. All reported injuries are included, even if the injury did not result in lost time from work or had no costs associated with the injury. A workers compensation specialist reviewed the injury and determined whether the injury is related to patient handling. The data are tracked in a risk management software program and sent to the safe patient handling coordinator monthly, with updated lost work days and restricted work days quarterly. Injuries are summarized by cost center and month of injury. In calendar year 2010, there were 22 injuries related to patient handling reported to workers compensation. Postimplementation, calendar year 2011, there were 14 injuries related to patient handling, a 36% decrease in the number of injuries. Lost work days are obtained from workers compensation records and updated quarterly to reflect days lost that occur after the reporting time. As of January 28, FIGURE 3. The number of injuries by month postimplementation. 160 Orthopaedic Nursing May/June 2013 Volume 32 Number by National Association of Orthopaedic Nurses
7 TABLE 2. REASONS FOR INJURY POSTIMPLEMENTATION Injury Reason Number of Injuries Equipment not used 7 Unable to use equipment on patient 1 Did not use alternate equipment 1 Caught falling patient 1 Data not available 6 Total , the numbers of lost work days 1 year preimplementation (calendar year 2010) was 180. One year postimplementation (calendar year 2011), there were 52 lost work days related to patient handling, a 71% decrease. There were fewer injuries reported in the first 6 months after the program was initiated. The unitbased peer leaders decreased in 1 year, from 19 to 10, thereby leaving only 53% of the unit-based peer leaders to continue to champion the program. Figure 3 displays the number of injuries reported each month related to patient handling. This could be related to the number of unit peer leaders. The after-injury event reviews provided valuable information for program improvement. Most often, it was discovered that staff were not using equipment when they sustained an injury postimplementation related to patient handling. Table 2 provides detailed information on after-injury event reviews. Because of issues with the workers compensation database, not all injuries were available for analysis. Another outcome from the project was realized when the results from the Nursing Database of National Quality Indicators (NDNQI ) RN Satisfaction Survey results became available. One question on the survey inquires about situations on the unit during the last shift. The question asks whether there was enough help to lift or move patients. As displayed in Figure 4, the percentage of yes response increased from 42% in 2010 to 68% in Using equipment for patient handling may have helped with the perception of having enough help to lift and move patients. FIGURE 4. RN satisfaction survey results for enough help to lift/ move on last shift early adopter unit. The survey was administered in November. University of Wisconsin Hospital and Clinics 2011 RN Satisfaction (NDNQI ) Survey Executive Summary. Recommendations Implementing an evidence-based safe patient handling program reduces the costs paid out by workers compensation for patient handling, establishing a necessity to implement the program to all inpatient areas of the UWHC. In addition, the UWHC will explore implementation of the program to other care areas, such as radiology, inpatient hemodialysis, the operating room, ambulatory clinics, and the emergency department. This implementation will assist with the organizational strategic goal of providing the best academic and work environment as a retention strategy. Another contribution toward reaching strategic goals will be met by creating a culture of safety for moving patients, thereby creating an atmosphere of leadership in quality and patient safety. The education component delivered to the unitbased peer leaders was effective in increasing the knowledge of the peer leaders and should continue, with a mixture of classroom time and hands-on equipment training. Observations of high-risk tasks at 1 and 6 months postimplementation indicate that the staff had changed behavior and were using equipment at a higher rate than anticipated, lending support that the education provided along with the other program components led to a change in practice for handling patients. After-injury event reviews often identified barriers to equipment use and should continue to be completed after each patient handling injury. Because the number of injuries increased during the second half of the year postimplementation ( Figure 3 ) and there was an identified decrease in the number of unit-based peer leaders, it is recommended to continue with the unit-based peer leaders. A regular count of unit-based peer leaders for safe patient handling should also be performed, and unit-based peer leaders will need to be replaced upon leaving the unit. Based upon the outcomes of this project, other acute care facilities interested in implementing a safe patient handling program should implement an evidence-based multifaceted safe patient handling program. Replication of the program should involve all program components as the benefit of each individual component was not evaluated. S USTAINABILITY Creating a culture of safety for safe patient handling requires continued attention and planning to maintain and sustain the project. Because unit-based peer leaders appear to have a key role in the implementation, sustainability should address maintaining and growing the skills of unit-based peer leaders. Developing an organizational structure for the unit-based peer leaders is a major component for sustainability. A dedicated safe patient handling coordinator is needed to ensure sustainability and continued implementation of the project to other areas of the organization. State-of-the-art equipment is required for the program and requires routine maintenance. Support from key stakeholders to purchase, maintain, and replace equipment will ensure sustainability of the project. Continuing to collect data on program outcomes and 2013 by National Association of Orthopaedic Nurses Orthopaedic Nursing May/June 2013 Volume 32 Number 3 161
8 TABLE 3. LIFT AID EQUIPMENT DETERMINATION GRID VERSION 2 Assessments Interventions Get Up and Go Test Value (Rising From Chair) Bed Mobility Lying to Sitting Reposition or Cares in Bed Vertical Transfer Noncooperative, Poor Upper Body Strength, Nonweight Bearing Vertical Transfer Weight Bearing and Upper Extremity Strength, Cooperative Lateral Transfer Patient Unable to Assist Ambulation Weight Bearing and Upper Extremity Strength, Cooperative 0 Able to Rise in Single Movement None None None None None 1 Pushes Up, Successful in One Attempt Roll/move independently with or without bed rail and/or verbal cues Sit up independently with or without bed rail, head of bed elevated, and/ or verbal cues None None Gait belt None Gait belt 3 Multiple Attempts but Successful Assist with moving upper and/or lower body Sit up and assists with moving legs Ceiling lift Air-assisted FR LT device Reverse trendelenburg if tolerates Ceiling lift with seated sling Gait belt Sit to stand Ceiling lift Air-assisted FR LT device to cardiac chair Sit to stand Ceiling lift with ambulation sling None 4 Unable to Rise Without Assistance Not able to actively assist, no initiation Not able to actively assist, no initiation Ceiling lift Air-assisted FR LT device Ceiling lift Ceiling lift with seated sling Ceiling lift Air-assisted FR LT device Sit to stand Ceiling lift with ambulation sling Unable to Assess Unable to assess Unable to assess Ceiling lift Air-assisted FR LT device Ceiling lift Ceiling lift Ceiling lift Air-assisted FR LT device Not recommended Note : FR friction reducing; LT lateral transfer. 162 Orthopaedic Nursing May/June 2013 Volume 32 Number by National Association of Orthopaedic Nurses
9 reporting on program benefits will need to be employed when requesting funding for equipment. Equipment accessories, such as slings for lifts, are a large component of any safe patient handling initiative. Ensuring availability of accessories for the patient population and different patient handling tasks needs to be monitored so this does not become a barrier to moving patients safely. Ongoing work will need to be done to increase the percentage of high-risk tasks completed by the guideline. Implementing a culture of safety for safe patient handling aims to change the culture of how patients are moved. Culture change takes time (Scott, Mannion, Davies, & Marshall, 2003). Nursing and hospital leadership support will help sustain the program through the use of peer leaders. Peer leaders will problem solve system barriers to assist with the culture change. Feedback will be given to staff on how many patients are moved, and the number of healthcare worker injuries and lost work days each month. The feedback will allow for continuous process improvement, sustaining the culture of safety for safe patient handling. L ESSONS LEARNED Implementing an evidence-based project on an early adopter unit allowed for the opportunity to learn at the local level and improve the project plan before spreading the change throughout the UWHC. The phases of the project provided an excellent structure for implementation. Not having equipment available for the education phase of the project contributed to a delay in the project timeline. Equipment needs to be ordered early once there is an assessed need for it. After approximately 3 months, it was discovered that the patient assessment criteria needed improvement. The assessment criteria were based only on the patient's ability to go from a sitting position to a standing position. Consequently, the patient assessment criteria were not helpful in determining whether equipment was needed for repositioning in bed or assisting a patient from lying to a seated position. A new equipment determination grid was developed by the Safe Patient Handling Task Force and implemented in November 2011 (see Table 3 ). The contribution of the equipment accessories to the project plan should not be overlooked. Accessories included slings for the ceiling lifts and portable lifting equipment in addition to mats for air-assisted lateral transfer devices. Originally, plans were to use mainly washable accessories and utilize single-patient-use accessories for patients in isolation. After suffering a loss of slings, the decision was made for single patient use. Despite this, the budget for single-patient-use items far exceeded actual usage; therefore, this change did not have a negative impact on the program budget. While the UWHC had an existing database for tracking injuries, the database was converted to a more robust system after program implementation on the early adopter unit. The reports from the new system were discovered to contain errors. Vigilance was required to ensure correct reporting of injuries, especially when converting to new tracking software. Also, the manual abstraction of cost for patient handling injuries could also lead to errors, both pre- and postimplementation. Summary Creating an environment for employees to change behavior for the benefit of themselves and the patients they care for is facilitated by the implementation of an evidence-based multifaceted safe patient handling program. The program did not eliminate all high-risk patient handling tasks, but the change in behavior did result in a decrease in injuries and an even larger decrease in workers compensation costs related to patient handling injuries in a 1-year period of time. Those who would benefit may be resistant to making a change, but we must remember changing culture takes time and continued resources. REFERENCES Alamgir, H., Yu, S., Fast, C., Hennessy, S., Kidd, C., & Yassi, A. ( 2008 ). Efficiency of overhead ceiling lifts in reducing musculoskeletal injury among carers working in long-term care institutions. Injury, 39 ( 5 ), American Nurses Association. ( 2004 ). ANA handle with care. Retrieved from MenuCategories/WorkplaceSafety/SafePatient/hwc. pdf American Nurses Association. ( 2009a ). Handle with care recognition program. Retrieved from world.org/mainmenucategories/occupational andenvironmental/occupationalhealth/handlewith care/recognition-program/handle-with-care- Recognition-Program-Brochure-PDF.aspx American Nurses Association. ( 2009b ). ANA handle with care recognition program criteria. Retrieved from OccupationalandEnvironmental/occupatioalhealth/ handlewithcare/recognition-program/criteria/ana- Handle-with-Care-Recognition-Program-Criteria.aspx American Nurses Association. ( 2013 ). Safe patient handling. Retrieved from MainMenuCategories/WorkplaceSafety/SafePatient Bureau of Labor Statistics. ( 2010 ). U.S. Department of Labor. Retrieved from release/osh.nr0.htm Charney, W., Simmons, B., Lary, M., & Metz, S. ( 2006 ). Zero lift programs in small rural hospitals in Washington State. AAOHN Journal, 54 ( 8 ), Collins, J. W., Wolf, L., Bell, J., & Evanoff, B. ( 2004 ). An evaluation of a best practices musculoskeletal injury prevention program in nursing homes. Injury Prevention, 10 ( 4 ), Dayndar, D., Yassi, A., Cooper, J. E., Tate, R., Norman, R., & Wells, R. ( 2001 ). Biomechanical analysis of peak and cumulative spinal loads during simulated patienthandling activities: A substudy of a randomized controlled trial to prevent lift and transfer of injury of health care workers. Applied Ergonomics, 32, Engst, C., Chhokar, R., Miller, A., Tate, R. B., & Yassi, A. ( 2005 ). Effectiveness of overhead lifting devices in reducing the risk of injury to care staff in extended care facilities. Ergonomics, 48 ( 2 ), Dugan, S. ( 2010, April). Improving safety culture to reduce employee injuries and patient falls. Oral presentation at 2013 by National Association of Orthopaedic Nurses Orthopaedic Nursing May/June 2013 Volume 32 Number 3 163
10 the 10th Annual Safe Patient Handling & Movement Conference, Lake Buena Vista, FL. Evanoff, B., Wolf, L., Anton, E., Canos, J., & Collins, J. ( 2003 ). Reduction in injury rates in nursing personnel through introduction of mechanical lifts in the workplace. American Journal of Industrial Medicine, 44, Fanello, S., Jousset, N., Roquelaure, Y., Chotard-Frampas, V., & Delbos, V. ( 2002 ). Evaluation of a training program for the prevention of lower back pain among hospital employees. Nursing and Health Sciences, 4, Haglund, K., Kyle, J., & Finkelstein, M. ( 2010 ). Pediatric safe patient handling. Journal of Pediatric Nursing, 25 ( 2 ), Hignett, S. ( 2003 ). Intervention strategies to reduce musculoskeletal injuries associated with handling patients: A systematic review. Occupational & Environmental Medicine, 60 ( 9 ), 8. Hunter, B., Branson, M., & Davenport, D. ( 2010 ). Saving costs, saving health care providers backs, and creating a safe patient environment. Nursing Economic$, 28 ( 2 ), Kalish, B. J., & Aebersold, M. ( 2010 ). Interruptions and multitasking in nursing care. The Joint Commission Journal on Quality and Patient Safety, 36 ( 3 ), Marras, W. ( 2005 ). The future of research in understanding and controlling work-related low back disorders. Ergonomics, 48 ( 5 ), Marras, W. S., Davis, K. G., Kirking, B. C., & Bertsche, P. K. ( 1999 ). A comprehensive analysis of low-back disorder risk and spinal loading during the transferring and repositioning of patients using different techniques. Ergonomics, 42 ( 7 ), Marras, W. S., Knapik, G. G., & Ferguson, S. ( 2009 ). Lumbar spine forces during maneuvering of ceilingbased and floor-based patient transfer devices. Ergonomics, 52 ( 3 ), Nelson, A., & Baptiste, A. S. ( 2006 ). Update on evidencebased practices for safe patient handling and movement. Orthopaedic Nursing, 25 ( 6 ), Nelson, A., Collins, J., Siddharthan, K., Matz, M., & Waters, T. ( 2008 ). Link between safe patient handling and patient outcomes in long-term care. Rehabilitation Nursing, 33 ( 1 ), Nelson, A., Lloyd, J. D., Menzel, N., & Gross, C. ( 2003 ). Preventing nursing back injuries: Redesigning patient handling tasks. American Association of Occupational Health Nursing Journal, 51 ( 3 ), Nelson, A., Matz, M., Chen, F., Siddharthan, K., Lloyd, J., & Fragala, G. ( 2006 ). Development and evaluation of a multifaceted ergonomics program to prevent injuries associated with patient handling tasks. International Journal of Nursing Studies, 43 ( 6 ), Pellino, T. A., Owen, B., Knapp, L., & Noak, J. ( 2006 ). The evaluation of mechanical devices for lateral transfers on perceived exertion discomfort and patient comfort. Orthopedic Nursing, 35 ( 1 ), Sammer, C. E., Lykens, K., Singh, K. P., Mains, D. A., & Lackan, N. A. ( 2010 ). What is patient safety culture? A review of the literature. Journal of Nursing Scholarship, 42 ( 2 ), Schibye, B., Faber Hansen, S., Hye-Knudsen, C. T., Essendrop, M., Mocher, M., & Skotte, J. ( 2003 ). Biomechanical analysis of the effect of changing patient handling technique. Applied Ergonomics, 34, Scott, T., Mannion, R., Davies, H., & Marshall, M. ( 2003 ). Implementing culture change in health care: Theory and practice. International Journal for Quality in Health Care, 15 ( 2 ), Sedlak, C., Doheny, M., Nelson, A., & Waters, T. ( 2009 ). Development of the National Association of Orthopaedic Nurses guidance statement on safe patient handling and movement in the orthopaedic setting. Orthopaedic Nursing, 28 ( 2S ), S2 S8. Silverwood, S., & Haddock, M. ( 2006 ). Reduction of musculoskeletal injuries in intensive care nurses using ceiling-mounted patient lifts. Dynamics, 17 ( 3 ), Stenger, K., Montgomery, L., & Briesemeister, E. ( 2007 ). Creating a culture of change through implementation of a safe patient handling program [corrected] [published erratum appears in Crit Care Nurs Clin North Am. 2009;21(4):595]. Critical Care Nursing Clinics of North America, 19 ( 2 ), Trinkoff, A. M., Geiger-Brown, J. M., Caruso, C. C., Lopscomb, J. A., Johantgen, M., Nelson, A. L., Selby, V. L. ( 2008 ). Personal safety for nurses. In Hughes, R. G. (Ed.), Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville, MD : Agency for Healthcare Research and Quality. pp Tullar, J., Brewer, S., Amick, B., Irvin, E., Mahood, Q., Pompeii, L., Evanoff, B. ( 2010 ). Occupational safety and health interventions to reduce musculoskeletal symptoms in the health care sector. Journal of Occupational Rehabilitation, 20 ( 2 ), doi: /s y Village, J., Frazer, M., Cohen, M., Leyland, A., Park, I., & Yassi, A. ( 2005 ). Electromyography as a measure of peak and cumulative workload in intermediate care and its relationship to musculoskeletal injury: An exploratory ergonomic study. Applied Ergonomics, 36, Wardell, H. ( 2007 ). Reduction of injuries associated with patient handling. AAOHN Journal, 55 ( 10 ), Waters, T. R. ( 2007 ). When is it safe to manually lift a patient? American Journal of Nursing, 107 ( 8 ), Waters, T. ( 1993 ). Revised NIOSH equation for the design and evaluation of manual lifting tasks. Ergonomics, 36 ( 7 ), Waters, T., Collins, J., Galinsky, T., & Caruso, C. ( 2006 ). NIOSH research efforts to prevent musculoskeletal disorders in the healthcare industry. Orthopaedic Nursing, 25 ( 6 ), Yassi, A., Cohen, M., Cvitkovich, Y., Park, I. H., Ratner, P. A., Ostry, A. S., Pollak, N. ( 2004 ). Factors associated with staff injuries in intermediate care facilities in British Columbia, Canada. Nursing Research, 53 ( 2 ), Orthopaedic Nursing May/June 2013 Volume 32 Number by National Association of Orthopaedic Nurses
Evaluation of Z-Slider for Lateral Patient Transfers, Repositioning, and Staff Musculoskeletal Injuries (Abstract) Laurie J. Bacastow RN, MSN, CNRN
 Evaluation of Z-Slider 1 Evaluation of Z-Slider for Lateral Patient Transfers, Repositioning, and Staff Musculoskeletal Injuries (Abstract) Laurie J. Bacastow RN, MSN, CNRN Stanford Hospital and Clinics
Evaluation of Z-Slider 1 Evaluation of Z-Slider for Lateral Patient Transfers, Repositioning, and Staff Musculoskeletal Injuries (Abstract) Laurie J. Bacastow RN, MSN, CNRN Stanford Hospital and Clinics
SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN
 Department of Veterans Affairs VHA DIRECTIVE 2010-032 Veterans Health Administration Washington, DC 20420 SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN 1. PURPOSE: This Veterans Health Administration
Department of Veterans Affairs VHA DIRECTIVE 2010-032 Veterans Health Administration Washington, DC 20420 SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN 1. PURPOSE: This Veterans Health Administration
HEALTH FACILITIES EVALUATION AND LICENSING DIVISION. Authorized by: Poonam Alaigh, MD, MSHCPM, FACP,
 HEALTH AND SENIOR SERVICES SENIOR SERVICES AND HEALTH SYSTEMS BRANCH HEALTH FACILITIES EVALUATION AND LICENSING DIVISION OFFICE OF CERTIFICATE OF NEED AND HEALTHCARE FACILITY LICENSURE Safe Patient Handling
HEALTH AND SENIOR SERVICES SENIOR SERVICES AND HEALTH SYSTEMS BRANCH HEALTH FACILITIES EVALUATION AND LICENSING DIVISION OFFICE OF CERTIFICATE OF NEED AND HEALTHCARE FACILITY LICENSURE Safe Patient Handling
Policy & Procedure. Safe Patient Handling (No Lift Policy)
 Effective date signifies approval of this MHS policy by the Performance Improvement Leadership Oversight Team (PILOT) (see minutes). Policy. Policy & Procedure Safe Patient Handling ( Lift Policy) Effective
Effective date signifies approval of this MHS policy by the Performance Improvement Leadership Oversight Team (PILOT) (see minutes). Policy. Policy & Procedure Safe Patient Handling ( Lift Policy) Effective
Using patient handling equipment to manage mobility in and around a bed.
 Loughborough University Institutional Repository Using patient handling equipment to manage mobility in and around a bed. This item was submitted to Loughborough University's Institutional Repository by
Loughborough University Institutional Repository Using patient handling equipment to manage mobility in and around a bed. This item was submitted to Loughborough University's Institutional Repository by
Evidence Based Decision Making in Occupational Health and Safety
 Evidence Based Decision Making in Occupational Health and Safety Hasanat Alamgir, MPharm, MBA, PhD Director, Statistics and Evaluation Occupational Health and Safety Agency for Healthcare (OHSAH) Presentation
Evidence Based Decision Making in Occupational Health and Safety Hasanat Alamgir, MPharm, MBA, PhD Director, Statistics and Evaluation Occupational Health and Safety Agency for Healthcare (OHSAH) Presentation
Presented by Kelly Moed, MSN, RN-BC Nursing Logic LLC
 Presented by Kelly Moed, MSN, RN-BC Nursing Logic LLC November 10,2011 Quality Care Community Conference Transforming Nursing Homes for Generations---Let s Make It Happen Identify healthcare workers who
Presented by Kelly Moed, MSN, RN-BC Nursing Logic LLC November 10,2011 Quality Care Community Conference Transforming Nursing Homes for Generations---Let s Make It Happen Identify healthcare workers who
ARE YOU HIRING YOUR NEXT INJURY?
 ARE YOU HIRING YOUR NEXT INJURY? White Paper Musculoskeletal injuries account for 25 60% of workers compensation claims across Canada. The following white paper will provide details on the benefits of
ARE YOU HIRING YOUR NEXT INJURY? White Paper Musculoskeletal injuries account for 25 60% of workers compensation claims across Canada. The following white paper will provide details on the benefits of
Providing a Lift. New lifting techniques are explored in an effort to prevent injuries of both patients and health care workers.
 March 2006 Search Providing a Lift By Sharon Brumbeloe, RN New lifting techniques are explored in an effort to prevent injuries of both patients and health care workers. According to the Bureau of Labor
March 2006 Search Providing a Lift By Sharon Brumbeloe, RN New lifting techniques are explored in an effort to prevent injuries of both patients and health care workers. According to the Bureau of Labor
Harmful Effects in Personal Assistants Client Transfer Situations
 Send Orders of Reprints at reprints@benthamscience.net The Ergonomics Open Journal, 2014, 7, 1-5 1 Harmful Effects in Personal Assistants Client Transfer Situations Anette Lind 1 and Gunvor Gard *,2 Open
Send Orders of Reprints at reprints@benthamscience.net The Ergonomics Open Journal, 2014, 7, 1-5 1 Harmful Effects in Personal Assistants Client Transfer Situations Anette Lind 1 and Gunvor Gard *,2 Open
An evaluation of a best practices musculoskeletal injury prevention program in nursing homes
 206 ORIGINAL ARTICLE An evaluation of a best practices musculoskeletal injury prevention program in nursing homes J W Collins, L Wolf, J Bell, B Evanoff... Injury Prevention 2004;10:206 211. doi: 10.1136/ip.2004.005595
206 ORIGINAL ARTICLE An evaluation of a best practices musculoskeletal injury prevention program in nursing homes J W Collins, L Wolf, J Bell, B Evanoff... Injury Prevention 2004;10:206 211. doi: 10.1136/ip.2004.005595
BODY STRESSING RISK MANAGEMENT CHECKLIST
 BODY STRESSING RISK MANAGEMENT CHECKLIST BODY STRESSING RISK MANAGEMENT CHECKLIST This checklist is designed to assist managers, workplace health staff and rehabilitation providers with identifying and
BODY STRESSING RISK MANAGEMENT CHECKLIST BODY STRESSING RISK MANAGEMENT CHECKLIST This checklist is designed to assist managers, workplace health staff and rehabilitation providers with identifying and
AV2800 Safe Patient Handling January 2014
 1.0 PURPOSE AV2800 Safe Patient Handling January 2014 To promote safe patient handling procedures to minimize the risk of injury to staff and ensure safe quality of care for the patients. 2.0 DEFINITIONS
1.0 PURPOSE AV2800 Safe Patient Handling January 2014 To promote safe patient handling procedures to minimize the risk of injury to staff and ensure safe quality of care for the patients. 2.0 DEFINITIONS
Implementing a Safe Patient Handling and Movement Program in a Rehabilitation Setting
 Implementing a Safe Patient Handling and Movement Program in a Rehabilitation Setting ABSTRACT Musculoskeletal injuries are a prevalent and costly occupational health problem, particularly in the healthcare
Implementing a Safe Patient Handling and Movement Program in a Rehabilitation Setting ABSTRACT Musculoskeletal injuries are a prevalent and costly occupational health problem, particularly in the healthcare
Putting the meat on the bones Outcomes depend on processes. What is success? Your indicators compared to what? Numbers or Rates
 Safe Patient Handling Programs: Evaluating Outcomes Barbara Silverstein silb235@lni.wa.gov Putting the meat on the bones Outcomes depend on processes processes Hazard assessments Committee meetings Procurement
Safe Patient Handling Programs: Evaluating Outcomes Barbara Silverstein silb235@lni.wa.gov Putting the meat on the bones Outcomes depend on processes processes Hazard assessments Committee meetings Procurement
From the Beginning to the End: Interventions to Prevent Back Injury in Nursing Home Workers
 From the Beginning to the End: Interventions to Prevent Back Injury in Nursing Home Workers James W. Collins, PhD, MSME Associate Director for Science Centers for Disease Control and Prevention National
From the Beginning to the End: Interventions to Prevent Back Injury in Nursing Home Workers James W. Collins, PhD, MSME Associate Director for Science Centers for Disease Control and Prevention National
Safe Lifting and Movement of Nursing Home Residents
 1 2 Safe Lifting and Movement of Nursing Home Residents by: James W. Collins, PhD, MSME Associate Director for Science Division of Safety Research National Institute for Occupational Safety and Health
1 2 Safe Lifting and Movement of Nursing Home Residents by: James W. Collins, PhD, MSME Associate Director for Science Division of Safety Research National Institute for Occupational Safety and Health
PerfectServe Survey Results. Presented by: Nielsen Consumer Insights Public Relations Research April 2015
 PerfectServe Survey Results Presented by: Nielsen Consumer Insights Public Relations Research April 2015 1 Table of Contents Research Method 3 Report Notes 5 Executive Summary 6 Detailed Findings 15 General
PerfectServe Survey Results Presented by: Nielsen Consumer Insights Public Relations Research April 2015 1 Table of Contents Research Method 3 Report Notes 5 Executive Summary 6 Detailed Findings 15 General
SAFE PATIENT HANDLING RISK ASSESSMENT
 SAFE PATIENT HANDLING RISK ASSESSMENT Swedish Medical Center 2007 This risk assessment consists of two parts: 1) Pre-Site visit forms (Sections 1 & 2): To be completed by facility/unit representative,
SAFE PATIENT HANDLING RISK ASSESSMENT Swedish Medical Center 2007 This risk assessment consists of two parts: 1) Pre-Site visit forms (Sections 1 & 2): To be completed by facility/unit representative,
Florida Hospitals Workforce Challenges: 2012 Workforce Survey Highlights
 2012 Update DATA Brief Florida Hospitals Workforce Challenges: 2012 Workforce Survey Highlights November 2012 DATABrief 2012 FHA Workforce Survey: Nurse and Allied Health Recruitment and Retention A lthough
2012 Update DATA Brief Florida Hospitals Workforce Challenges: 2012 Workforce Survey Highlights November 2012 DATABrief 2012 FHA Workforce Survey: Nurse and Allied Health Recruitment and Retention A lthough
Combined Assessment Program Summary Report. Evaluation of Pressure Ulcer Prevention and Management at Veterans Health Administration Facilities
 Department of Veterans Affairs Office of Inspector General Report No. 14-05132-90 Office of Healthcare Inspections Combined Assessment Program Summary Report Evaluation of Pressure Ulcer Prevention and
Department of Veterans Affairs Office of Inspector General Report No. 14-05132-90 Office of Healthcare Inspections Combined Assessment Program Summary Report Evaluation of Pressure Ulcer Prevention and
Join ARN today. Rehabilitation Nursing. Your Passion Our Purpose. www.rehabnurse.org
 www.rehabnurse.org Rehabilitation Nursing Your Passion Our Purpose How well-informed rehabilitation nurses get the support and information they need. Join ARN today. live your passion expand your knowledge
www.rehabnurse.org Rehabilitation Nursing Your Passion Our Purpose How well-informed rehabilitation nurses get the support and information they need. Join ARN today. live your passion expand your knowledge
BSN, MN, & 11, 2010 2:00 P.M.,
 Testimony of June M. Altaras, RN, BSN, MN, Nurse Executive, Swedish Health Services, Before the Senate Employment and Workplace Safety Subcommittee hearing, Safe Patient Handling & Lifting Standards for
Testimony of June M. Altaras, RN, BSN, MN, Nurse Executive, Swedish Health Services, Before the Senate Employment and Workplace Safety Subcommittee hearing, Safe Patient Handling & Lifting Standards for
Ergonomics In The Laundry / Linen Industry
 Ergonomics In The Laundry / Linen Industry Ergonomics is a key topic of discussion throughout industry today. With multiple changes announced, anticipated, and then withdrawn the Occupational Safety and
Ergonomics In The Laundry / Linen Industry Ergonomics is a key topic of discussion throughout industry today. With multiple changes announced, anticipated, and then withdrawn the Occupational Safety and
Why moving and handling programmes are needed
 section 2 Why moving and handling programmes are needed Contents Injuries from moving and handling people: Prevalence and costs The benefits of moving and handling programmes Preventing injuries to carers
section 2 Why moving and handling programmes are needed Contents Injuries from moving and handling people: Prevalence and costs The benefits of moving and handling programmes Preventing injuries to carers
Manual handling in healthcare
 Loughborough University Institutional Repository Manual handling in healthcare This item was submitted to Loughborough University's Institutional Repository by the/an author. Citation: HIGNETT, S. and
Loughborough University Institutional Repository Manual handling in healthcare This item was submitted to Loughborough University's Institutional Repository by the/an author. Citation: HIGNETT, S. and
Written Statement. for the. Senate Finance Committee of The United States
 Written Statement of Isis Montalvo, RN, MS, MBA Manager, Nursing Practice & Policy American Nurses Association 8515 Georgia Avenue, Suite 400 Silver Spring, MD 20903 for the Senate Finance Committee of
Written Statement of Isis Montalvo, RN, MS, MBA Manager, Nursing Practice & Policy American Nurses Association 8515 Georgia Avenue, Suite 400 Silver Spring, MD 20903 for the Senate Finance Committee of
Risk assessment. section 3. Contents
 section 3 Risk assessment Contents Why risk assessment is important Risks related to moving and handling Identifying hazards in workplaces Workplace hazard management and risk controls The risk assessment
section 3 Risk assessment Contents Why risk assessment is important Risks related to moving and handling Identifying hazards in workplaces Workplace hazard management and risk controls The risk assessment
Patient Lift Teams. By: William Charney, DOH
 Patient Lift Teams By: William Charney, DOH LIFTING TEAMS PUT RISK WHERE IT CAN BE CONTROLLED; IN SMALL GROUPS OF TEAMS RATHER THAN HUNDREDS OR THOUSANDS OF NURSING PERSONNEL ONE OF THE MAJOR RISK
Patient Lift Teams By: William Charney, DOH LIFTING TEAMS PUT RISK WHERE IT CAN BE CONTROLLED; IN SMALL GROUPS OF TEAMS RATHER THAN HUNDREDS OR THOUSANDS OF NURSING PERSONNEL ONE OF THE MAJOR RISK
Changing the culture of any organization is well known to be a long process,
 Creative Nursing, Volume 18, Issue 4, 2012 Impact of Unit Practice Councils on Culture and Outcomes Susan Wessel, MS, MBA, RN, NEA-BC This article describes positive outcomes in culture, Hospital Consumer
Creative Nursing, Volume 18, Issue 4, 2012 Impact of Unit Practice Councils on Culture and Outcomes Susan Wessel, MS, MBA, RN, NEA-BC This article describes positive outcomes in culture, Hospital Consumer
MANAGING RISING HEALTHCARE COSTS SOLUTIONS TO A FRAGMENTED SYSTEM
 Copyright 2014 Veridicus Health tm. All rights reserved. CONTENTS EXECUTIVE SUMMARY 1 INTRODUCTION 2 BY THE NUMBERS HOW VERIDICUS CARE MANAGEMENT IS DIFFERENT 4 COLLABORATION RIGHT PATIENT, RIGHT TIME
Copyright 2014 Veridicus Health tm. All rights reserved. CONTENTS EXECUTIVE SUMMARY 1 INTRODUCTION 2 BY THE NUMBERS HOW VERIDICUS CARE MANAGEMENT IS DIFFERENT 4 COLLABORATION RIGHT PATIENT, RIGHT TIME
The Advantages of Ergonomics
 The Advantages of Ergonomics Workers come in all different sizes. Ergonomics can help make the work more comfortable for the individual worker. What is ergonomics? Ergonomics is designing a job to fit
The Advantages of Ergonomics Workers come in all different sizes. Ergonomics can help make the work more comfortable for the individual worker. What is ergonomics? Ergonomics is designing a job to fit
AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Verificatoin Criterea EFFECTIVE JANUARY 1, 2015. Criterion. Level (1 or 2) Number
 Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Criterion AMERICAN BURN ASSOCIATION BURN CENTER VERIFICATION REVIEW PROGRAM Criterion Level (1 or 2) Number Criterion BURN CENTER ADMINISTRATION 1. The burn center hospital is currently accredited by The
Integrating Quality and Safety (QSEN) Content into Skills and Simulation Curricula
 Integrating Quality and Safety (QSEN) Content into Skills and Simulation Curricula Carol F. Durham MSN RN Clinical Associate Professor Director, Clinical Education & Resource Center The University of North
Integrating Quality and Safety (QSEN) Content into Skills and Simulation Curricula Carol F. Durham MSN RN Clinical Associate Professor Director, Clinical Education & Resource Center The University of North
LICENSED VOCATIONAL NURSE ON CALL PILOT PROGRAM FINAL REPORT. As required by SB 1857, 82 nd Legislature, Regular Session, 2011
 LICENSED VOCATIONAL NURSE ON CALL PILOT PROGRAM FINAL REPORT As required by SB 1857, 82 nd Legislature, Regular Session, 2011 Center for Policy and Innovation December 2015 1 DECEMBER 2015 TABLE OF CONTENTS
LICENSED VOCATIONAL NURSE ON CALL PILOT PROGRAM FINAL REPORT As required by SB 1857, 82 nd Legislature, Regular Session, 2011 Center for Policy and Innovation December 2015 1 DECEMBER 2015 TABLE OF CONTENTS
Overcoming Barriers To Implementing Ergonomics Programs In Healthcare: Case Studies From The Field
 Overcoming Barriers To Implementing Ergonomics Programs In Healthcare: Case Studies From The Field Presented by Lynda Enos, MS, RN, COHN-S, CPE Ergonomist, Oregon Nurses Association Tel: 503-293-0011 x301
Overcoming Barriers To Implementing Ergonomics Programs In Healthcare: Case Studies From The Field Presented by Lynda Enos, MS, RN, COHN-S, CPE Ergonomist, Oregon Nurses Association Tel: 503-293-0011 x301
Work Conditioning Natural Progressions By Nancy Botting, Judy Braun, Charlene Couture and Liz Scott
 Work Conditioning Natural Progressions By Nancy Botting, Judy Braun, Charlene Couture and Liz Scott How a non-traditional, geared-to-work treatment is returning injured workers to full duties quickly,
Work Conditioning Natural Progressions By Nancy Botting, Judy Braun, Charlene Couture and Liz Scott How a non-traditional, geared-to-work treatment is returning injured workers to full duties quickly,
Patient CaringTouch System: An Innovation in Patient-Centered Care
 Patient CaringTouch System: An Innovation in Patient-Centered Care Patricia A. Patrician, PhD, RN, FAAN Colonel, US Army (Retired) Donna Brown Banton Endowed Professor University of Alabama at Birmingham
Patient CaringTouch System: An Innovation in Patient-Centered Care Patricia A. Patrician, PhD, RN, FAAN Colonel, US Army (Retired) Donna Brown Banton Endowed Professor University of Alabama at Birmingham
Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices
 Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices September 29, 2010 Tangee B. Kizer, BSM Executive Director Environmental and Guest Services Carolinas HealthCare
Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices September 29, 2010 Tangee B. Kizer, BSM Executive Director Environmental and Guest Services Carolinas HealthCare
Turning on the Care Coordination Switch in Rural Primary Care Practices
 Turning on the Care Coordination Switch in Rural Primary Care Practices AHRQ Master Contract Task Order #5 HHSA2902007100016I (9/07-11/09) Care Management Plus research at OHSU is supported by funding
Turning on the Care Coordination Switch in Rural Primary Care Practices AHRQ Master Contract Task Order #5 HHSA2902007100016I (9/07-11/09) Care Management Plus research at OHSU is supported by funding
Catholic Mutual..."CARES"
 Catholic Mutual..."CARES" BACK INJURY LOSS CONTROL FOR HEALTH CARE FACILITIES Occupational back injuries are a major loss exposure in the health care industry. Serious back injuries can result when employees
Catholic Mutual..."CARES" BACK INJURY LOSS CONTROL FOR HEALTH CARE FACILITIES Occupational back injuries are a major loss exposure in the health care industry. Serious back injuries can result when employees
Chapter 3 Office of Human Resources Absenteeism Management
 Office of Human Resources Absenteeism Management Contents Section A - Background, Objective and Scope............................ 24 Section B - Criterion 1 - Communicating Expectations.......................
Office of Human Resources Absenteeism Management Contents Section A - Background, Objective and Scope............................ 24 Section B - Criterion 1 - Communicating Expectations.......................
Sample Business Plan. Employee Wellness Program for (location) VA Hospital. Table of Contents. 1. Executive Summary. 2. Description. 3.
 Sample Business Plan Employee Wellness Program for (location) VA Hospital Table of Contents 1. Executive Summary 2. Description 3. Background 4. Organizational Assessment 5. Proposed Services 6. Target
Sample Business Plan Employee Wellness Program for (location) VA Hospital Table of Contents 1. Executive Summary 2. Description 3. Background 4. Organizational Assessment 5. Proposed Services 6. Target
ERGONOMIC PATIENT HANDLING PASSPORT - A CONCRETE TOOL FOR IMPROVING NURSES' COMPETENCE IN ERGONOMICS
 ERGONOMIC PATIENT HANDLING PASSPORT - A CONCRETE TOOL FOR IMPROVING NURSES' COMPETENCE IN ERGONOMICS Tamminen-Peter, L. 1 and Fagerström, V. 2 1 Ergosolutions BC Oy Ab, Niittykulmantie 84, FI -20380 Turku
ERGONOMIC PATIENT HANDLING PASSPORT - A CONCRETE TOOL FOR IMPROVING NURSES' COMPETENCE IN ERGONOMICS Tamminen-Peter, L. 1 and Fagerström, V. 2 1 Ergosolutions BC Oy Ab, Niittykulmantie 84, FI -20380 Turku
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES PATIENT LIFT SYSTEMS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance Program (CMAP) on the requirements for
PROVIDER POLICIES & PROCEDURES PATIENT LIFT SYSTEMS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance Program (CMAP) on the requirements for
How To Get A Nursing Certification At Ulaa
 Nursing Specialty Certification: Validation of Knowledge 1 Definition of Certification American Nurses Association (ANA) The documented validation of specific qualifications demonstrated by the individual
Nursing Specialty Certification: Validation of Knowledge 1 Definition of Certification American Nurses Association (ANA) The documented validation of specific qualifications demonstrated by the individual
JOGNN. Typically, we do not think of nursing as
 JOGNN Understanding Risks of Workplace Injury in Labor and Delivery Jaynelle F. Stichler, Judd L. Feiler, and Kimberlie Chase Correspondence Jaynelle F. Stichler, DNS, RN, FACHE, FAAN, P.O. Box 28278,
JOGNN Understanding Risks of Workplace Injury in Labor and Delivery Jaynelle F. Stichler, Judd L. Feiler, and Kimberlie Chase Correspondence Jaynelle F. Stichler, DNS, RN, FACHE, FAAN, P.O. Box 28278,
System is a not-forprofit
 ABOUT THE PROJECT The Pioneer Employer Initiative is based on the idea that employers who do good, do well. It is an effort to discover and promote the next generation of best practices in workforce management,
ABOUT THE PROJECT The Pioneer Employer Initiative is based on the idea that employers who do good, do well. It is an effort to discover and promote the next generation of best practices in workforce management,
Ergonomic Evaluation Acute Care Nursing Health Center
 Ergonomic Evaluation Acute Care Nursing Health Center Caroline Hegarty Jamie Rosenberg Rachel Stecker May 1, 2003 Most Injury Inducing Tasks (Owen & Garg, 1990) RESEARCH 1. Chair / toilet transfers 2.
Ergonomic Evaluation Acute Care Nursing Health Center Caroline Hegarty Jamie Rosenberg Rachel Stecker May 1, 2003 Most Injury Inducing Tasks (Owen & Garg, 1990) RESEARCH 1. Chair / toilet transfers 2.
Falls and falls injury prevention activity audit for residential aged care facilities
 Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Ergonomics for Schoolchildren and Young Workers
 Ergonomics for Schoolchildren and Young Workers Schoolchildren and Backpacks Schoolchildren everywhere are being asked to carry more and more weight around on their backs. There are many reasons why children
Ergonomics for Schoolchildren and Young Workers Schoolchildren and Backpacks Schoolchildren everywhere are being asked to carry more and more weight around on their backs. There are many reasons why children
Workforce Retention, Absence and Disability Management: Summary of DMEC/VCU Survey
 Workforce Retention, Absence and Disability Management: Summary of DMEC/VCU Survey Presented to DMEC 13 th Annual International Absence and Disability Management Conference Denver, Colorado August, 2008
Workforce Retention, Absence and Disability Management: Summary of DMEC/VCU Survey Presented to DMEC 13 th Annual International Absence and Disability Management Conference Denver, Colorado August, 2008
The University of Toledo Digital Repository. The University of Toledo. Lisa R. Slusser The University of Toledo. Master s and Doctoral Projects
 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects 2010 Safe patient handling curriculum in occupational therapy and occupational therapy assistant programs
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects 2010 Safe patient handling curriculum in occupational therapy and occupational therapy assistant programs
Rehabilitation NURSING
 Rehabilitation NURSING Myths and Facts About Safe Patient Handling in Rehabilitation Audrey Nelson, PhD RN FAAN Kenneth J. Harwood, PhD PT CIE Catherine A. Tracey, MS RN CRRN Kathleen L. Dunn, MS RN CRRN-A
Rehabilitation NURSING Myths and Facts About Safe Patient Handling in Rehabilitation Audrey Nelson, PhD RN FAAN Kenneth J. Harwood, PhD PT CIE Catherine A. Tracey, MS RN CRRN Kathleen L. Dunn, MS RN CRRN-A
Healthy workplaces and productivity
 Making the healthy workplace business case and leading change Graham S. Lowe, Ph.D. Presentation at The European Network of Enterprise for Health, Mondragón, Spain, 14 October 2003. www.grahamlowe.ca Copyright
Making the healthy workplace business case and leading change Graham S. Lowe, Ph.D. Presentation at The European Network of Enterprise for Health, Mondragón, Spain, 14 October 2003. www.grahamlowe.ca Copyright
Partnering with Academic Partners to Enhance Student Experiences and Transitions into Practice
 Partnering with Academic Partners to Enhance Student Experiences and Transitions into Practice Holly Lorenz, RN, MSN Sandra Rader, DNP, MSA, RN, NEA-BC Melanie Shatzer, DNP, RN Pittsburgh, PA UPMC Objectives
Partnering with Academic Partners to Enhance Student Experiences and Transitions into Practice Holly Lorenz, RN, MSN Sandra Rader, DNP, MSA, RN, NEA-BC Melanie Shatzer, DNP, RN Pittsburgh, PA UPMC Objectives
What is Musculoskeletal Wellness?
 What is Musculoskeletal Wellness? What is musculoskeletal wellness and why should employers care about it? Musculoskeletal wellness used in an occupational setting is best defined as a coordinated and
What is Musculoskeletal Wellness? What is musculoskeletal wellness and why should employers care about it? Musculoskeletal wellness used in an occupational setting is best defined as a coordinated and
Good Body Mechanics/ Employee Safety: A Skills Update THIS PROGRAM COVERS: 4) How to Maintain Healthy Lifestyle Habits to Help Prevent Injury
 In-Service Training Good Body Mechanics/ Employee Safety: A Skills Update THIS PROGRAM COVERS: 1) Definition of Ergonomics 2) How Repetitive Movements Can Lead to Injury 3) The Basic Steps to Using Good
In-Service Training Good Body Mechanics/ Employee Safety: A Skills Update THIS PROGRAM COVERS: 1) Definition of Ergonomics 2) How Repetitive Movements Can Lead to Injury 3) The Basic Steps to Using Good
MANUAL OF UNIVERSITY POLICIES PROCEDURES AND GUIDELINES. Applies to: faculty staff students student employees visitors contractors
 Page 1 of 5 Title/Subject: CMU ERGONOMICS PROGRAM Applies to: faculty staff students student employees visitors contractors Effective Date of This Revision: May 1, 2012 Contact for More Information: Human
Page 1 of 5 Title/Subject: CMU ERGONOMICS PROGRAM Applies to: faculty staff students student employees visitors contractors Effective Date of This Revision: May 1, 2012 Contact for More Information: Human
White Paper: INTRODUCTION
 White Paper: STRATEGIES TO IMPROVE PATIENT AND HEALTH CARE PROVIDER SAFETY IN PATIENT HANDLING AND MOVEMENT TASKS: A COLLABORATIVE EFFORT OF THE AMERICAN PHYSICAL THERAPY ASSOCIATION, ASSOCIATION OF REHABILITATION
White Paper: STRATEGIES TO IMPROVE PATIENT AND HEALTH CARE PROVIDER SAFETY IN PATIENT HANDLING AND MOVEMENT TASKS: A COLLABORATIVE EFFORT OF THE AMERICAN PHYSICAL THERAPY ASSOCIATION, ASSOCIATION OF REHABILITATION
Rehabilitation Where You Recover. Inpatient Rehabilitation Services at Albany Medical Center
 Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
Rehabilitation Where You Recover Inpatient Rehabilitation Services at Albany Medical Center You're Here and So Are We As the region s only academic medical center, Albany Medical Center offers a number
How To Treat Musculoskeletal Injury In Sonographers
 MUSCULOSKELETAL DISORDERS IN SONOGRAPHERS: ARE WE DOING ENOUGH? Many terms are used to refer to work related injuries among sonographers. Musculosketetal injury (MSI) Repetitive motion injury (RMI) Repetitive
MUSCULOSKELETAL DISORDERS IN SONOGRAPHERS: ARE WE DOING ENOUGH? Many terms are used to refer to work related injuries among sonographers. Musculosketetal injury (MSI) Repetitive motion injury (RMI) Repetitive
Lifting Patients/Residents/Clients in Health Care Washington State 2005
 Lifting Patients/Residents/Clients in Health Care Washington State 2005 Report to the Washington State Legislature House Commerce and Labor Committee January 2006 Prepared by Department of Labor and Industries
Lifting Patients/Residents/Clients in Health Care Washington State 2005 Report to the Washington State Legislature House Commerce and Labor Committee January 2006 Prepared by Department of Labor and Industries
Department of Veterans Affairs VHA DIRECTIVE 2010-034 Veterans Health Administration Washington, DC 20420 July 19, 2010
 Department of Veterans Affairs VHA DIRECTIVE 2010-034 Veterans Health Administration Washington, DC 20420 STAFFING METHODOLOGY FOR VHA NURSING PERSONNEL 1. PURPOSE: This Veterans Health Administration
Department of Veterans Affairs VHA DIRECTIVE 2010-034 Veterans Health Administration Washington, DC 20420 STAFFING METHODOLOGY FOR VHA NURSING PERSONNEL 1. PURPOSE: This Veterans Health Administration
Given below are three important steps for your successful job search.
 Students Manual Given below are three important steps for your successful job search. 1) Create a CV and Cover Letter 2) Setup email alerts 3) Apply to jobs regularly on your career portal Create a CV
Students Manual Given below are three important steps for your successful job search. 1) Create a CV and Cover Letter 2) Setup email alerts 3) Apply to jobs regularly on your career portal Create a CV
NURSING INFORMATICS CHAPTER 1 OVERVIEW OF NURSING INFORMATICS
 NURSING INFORMATICS CHAPTER 1 1 OVERVIEW OF NURSING INFORMATICS CHAPTER OBJECTIVES 2 1. Define nursing informatics (NI) and key terminology. 2. Explore NI Metastructures, concepts and tools 3. Reflect
NURSING INFORMATICS CHAPTER 1 1 OVERVIEW OF NURSING INFORMATICS CHAPTER OBJECTIVES 2 1. Define nursing informatics (NI) and key terminology. 2. Explore NI Metastructures, concepts and tools 3. Reflect
Trauma Center Alcohol Screening. Michael Mello, MD, MPH Injury Prevention Center at Rhode Island Hospital /Hasbro Children s Hospital
 Trauma Center Alcohol Screening and Intervention Michael Mello, MD, MPH Injury Prevention Center at Rhode Island Hospital /Hasbro Children s Hospital Disclosures I have no affiliations, sponsorship, financial
Trauma Center Alcohol Screening and Intervention Michael Mello, MD, MPH Injury Prevention Center at Rhode Island Hospital /Hasbro Children s Hospital Disclosures I have no affiliations, sponsorship, financial
Back Pain Musculoskeletal Disorder Updated October 2010
 Back Pain Musculoskeletal Disorder Updated October 2010 According to the Health and Safety Executive back pain is the most common health problem for British workers. Approximately 80% of people experience
Back Pain Musculoskeletal Disorder Updated October 2010 According to the Health and Safety Executive back pain is the most common health problem for British workers. Approximately 80% of people experience
CENTRE FOR MUSCULOSKELETAL AND NEUROLOGICAL REHABILITATION GHENT UNIVERSITY HOSPITAL
 CENTRE FOR MUSCULOSKELETAL AND NEUROLOGICAL REHABILITATION GHENT UNIVERSITY HOSPITAL Historical background The centre was established in 1964 by Professor Hendrik Claessens, MD. Its primary goal was the
CENTRE FOR MUSCULOSKELETAL AND NEUROLOGICAL REHABILITATION GHENT UNIVERSITY HOSPITAL Historical background The centre was established in 1964 by Professor Hendrik Claessens, MD. Its primary goal was the
The Importance and Impact of Nursing Informatics Competencies for Baccalaureate Nursing Students and Registered Nurses
 IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 5, Issue 1 Ver. IV (Jan. - Feb. 2016), PP 20-25 www.iosrjournals.org The Importance and Impact of Nursing
IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 5, Issue 1 Ver. IV (Jan. - Feb. 2016), PP 20-25 www.iosrjournals.org The Importance and Impact of Nursing
TORONTO STROKE FLOW INITIATIVE - Outpatient Rehabilitation Best Practice Recommendations Guide (updated July 26, 2013)
 Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
Objective: To enhance system-wide performance and outcomes for persons with stroke in Toronto. Goals: Timely access to geographically located acute stroke unit care with a dedicated interprofessional team
American Sentinel University DNP Practice Experience Quick Start Guide
 American Sentinel University DNP Practice Experience Quick Start Guide This Quick Start Guide is designed to guide your preparation, practice experiences, and reflective journaling within each nursing
American Sentinel University DNP Practice Experience Quick Start Guide This Quick Start Guide is designed to guide your preparation, practice experiences, and reflective journaling within each nursing
How To Buy A Rifton Tram
 Rifton TRAM Sample LMN for the Rifton TRAM School-based Therapy with Adolescents EVERY REASONABLE EFFORT HAS BEEN MADE TO VERIFY THE ACCURACY OF THE INFORMATION. HOWEVER, THE SAMPLE LETTERS OF MEDICAL
Rifton TRAM Sample LMN for the Rifton TRAM School-based Therapy with Adolescents EVERY REASONABLE EFFORT HAS BEEN MADE TO VERIFY THE ACCURACY OF THE INFORMATION. HOWEVER, THE SAMPLE LETTERS OF MEDICAL
Enclosure I. NIOSH Assessment of Risks for 16- and 17-Year Old Workers Using Power-Driven Patient Lift Devices
 Objective Enclosure I NIOSH Assessment of Risks for 16- and 17-Year Old Workers Using Power-Driven Patient Lift Devices Thomas R. Waters, Ph.D., James Collins, Ph.D. and Dawn Castillo, MPH Centers for
Objective Enclosure I NIOSH Assessment of Risks for 16- and 17-Year Old Workers Using Power-Driven Patient Lift Devices Thomas R. Waters, Ph.D., James Collins, Ph.D. and Dawn Castillo, MPH Centers for
How Are We Doing? A Hospital Self Assessment Survey on Patient Transitions and Family Caregivers
 How Are We Doing? A Hospital Self Assessment Survey on Patient Transitions and Family Caregivers Well-planned and managed transitions are essential for high quality care and patient safety. Transitions
How Are We Doing? A Hospital Self Assessment Survey on Patient Transitions and Family Caregivers Well-planned and managed transitions are essential for high quality care and patient safety. Transitions
Engagement Rubric for Applicants
 Engagement Rubric for Applicants Updated: June 6, 2016 Published: February 4, 2014 To cite this document, please use: PCORI Engagement Rubric. PCORI (Patient-Centered Outcomes Research Institute) website.
Engagement Rubric for Applicants Updated: June 6, 2016 Published: February 4, 2014 To cite this document, please use: PCORI Engagement Rubric. PCORI (Patient-Centered Outcomes Research Institute) website.
Safe Patient Handling Training and Competency. Valerie Beecher, MS Ergonomic Specialist Upstate University Hospital Syracuse, NY
 Safe Patient Handling Training and Competency Valerie Beecher, MS Ergonomic Specialist Upstate University Hospital Syracuse, NY Upstate Ergonomics Program Background Ergonomics Specialist hired 2004 Ergonomics
Safe Patient Handling Training and Competency Valerie Beecher, MS Ergonomic Specialist Upstate University Hospital Syracuse, NY Upstate Ergonomics Program Background Ergonomics Specialist hired 2004 Ergonomics
7 DRIVERS FOR BUILDING EMPLOYEE ENGAGEMENT: FROM HIRE TO RETIRE
 7 DRIVERS FOR BUILDING EMPLOYEE ENGAGEMENT: FROM HIRE TO RETIRE Insights from Ceridian s 4th Annual Pulse of Talent Survey EXECUTIVE SUMMARY The insights provided by more than 800 working Canadians show
7 DRIVERS FOR BUILDING EMPLOYEE ENGAGEMENT: FROM HIRE TO RETIRE Insights from Ceridian s 4th Annual Pulse of Talent Survey EXECUTIVE SUMMARY The insights provided by more than 800 working Canadians show
How To Be A Medical Flight Specialist
 Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Selection of Equipment
 Selection of Equipment A key component of a multifaceted, safe, patient-handling program is the integration and use of equipment. This chapter aims to present and describe various types of commercially
Selection of Equipment A key component of a multifaceted, safe, patient-handling program is the integration and use of equipment. This chapter aims to present and describe various types of commercially
THE COSTS AND BENEFITS OF ACTIVE CASE MANAGEMENT AND REHABILITATION FOR MUSCULOSKELETAL DISORDERS
 This document is the abstract and executive summary of a report prepared by Hu-Tech Ergonomics for HSE. The full report will be published by Health and Safety Executive on their website in mid-august 2006.
This document is the abstract and executive summary of a report prepared by Hu-Tech Ergonomics for HSE. The full report will be published by Health and Safety Executive on their website in mid-august 2006.
How To Improve A Nursing Practice
 Making Lemonade from a Lemon of an NDNQI RN Survey: Nurse Managers and Clinical Nurses Collaborating to Improve the Practice Environment Session ID#: L8 Kathie Krause MSN, RN, NNP-BC, NEA-BC Vice President
Making Lemonade from a Lemon of an NDNQI RN Survey: Nurse Managers and Clinical Nurses Collaborating to Improve the Practice Environment Session ID#: L8 Kathie Krause MSN, RN, NNP-BC, NEA-BC Vice President
Sample Return-to-Work Program
 Hanover Risk Solutions Sample Return-to-Work Program To create your own Return-to-Work Program, copy and paste the information below into a word processing document, to which you may wish to add your own
Hanover Risk Solutions Sample Return-to-Work Program To create your own Return-to-Work Program, copy and paste the information below into a word processing document, to which you may wish to add your own
Safe Lifting Programs at Long-Term Care Facilities and Their Impact on Workers Compensation Costs
 NCCI RESEARCH BRIEF March 2011 by Tanya Restrepo, Frank Schmid, Harry Shuford, and Chun Shyong Safe Lifting Programs at Long-Term Care Facilities and Their Impact on Workers Compensation Costs Introduction
NCCI RESEARCH BRIEF March 2011 by Tanya Restrepo, Frank Schmid, Harry Shuford, and Chun Shyong Safe Lifting Programs at Long-Term Care Facilities and Their Impact on Workers Compensation Costs Introduction
Members respond to help identify what makes RNs unique and valuable to healthcare in Alberta.
 CARNA - Uniquely RN Members respond to help identify what makes RNs unique and valuable to healthcare in Alberta. RNs have expressed that their role is not always understood by colleagues, employers and
CARNA - Uniquely RN Members respond to help identify what makes RNs unique and valuable to healthcare in Alberta. RNs have expressed that their role is not always understood by colleagues, employers and
College Quarterly. A Simulation-based Training Partnership between Education and Healthcare Institutions. Louanne Melburn & Julie Rivers.
 College Quarterly Winter 2012 - Volume 15 Number 1 Home Contents A Simulation-based Training Partnership between Education and Healthcare Institutions Louanne Melburn & Julie Rivers Abstract Partnership
College Quarterly Winter 2012 - Volume 15 Number 1 Home Contents A Simulation-based Training Partnership between Education and Healthcare Institutions Louanne Melburn & Julie Rivers Abstract Partnership
Postgraduate Certificate in Moving and Handling at AUT
 Postgraduate Certificate in Moving and Handling at AUT Fiona Trevelyan fiona.trevelyan@aut.ac.nz Health and Rehabilitation Research Centre Auckland University of Technology New Zealand Moving and handling
Postgraduate Certificate in Moving and Handling at AUT Fiona Trevelyan fiona.trevelyan@aut.ac.nz Health and Rehabilitation Research Centre Auckland University of Technology New Zealand Moving and handling
Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses
 Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses This course has been awarded two (2.0) contact hours. This course expires on April 15, 2017. Copyright 2014 by RN.com. All Rights Reserved.
Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses This course has been awarded two (2.0) contact hours. This course expires on April 15, 2017. Copyright 2014 by RN.com. All Rights Reserved.
Magnet Readiness in the Operating Room
 Magnet Readiness in the Operating Room Samantha K. Madonis, RN, MSN, CNOR Wakana Litwinczuk, RN, BSN, CNOR Michelle Robison, RN, MSN, CNOR Surgical Services UCLA Santa Monica Hospital Disclosure Samantha
Magnet Readiness in the Operating Room Samantha K. Madonis, RN, MSN, CNOR Wakana Litwinczuk, RN, BSN, CNOR Michelle Robison, RN, MSN, CNOR Surgical Services UCLA Santa Monica Hospital Disclosure Samantha
Improving Our Services for Older People in Cardiff and the Vale of Glamorgan. The Development of Clinical Gerontology Services
 Improving Our Services for Older People in Cardiff and the Vale of Glamorgan The Development of Clinical Gerontology Services What s this document about? Cardiff and Vale University Health Board (UHB)
Improving Our Services for Older People in Cardiff and the Vale of Glamorgan The Development of Clinical Gerontology Services What s this document about? Cardiff and Vale University Health Board (UHB)
Running head: LEADERSHIP STRATEGY ANALYSIS 1
 Running head: LEADERSHIP STRATEGY ANALYSIS 1 Leadership Strategy Analysis Cheryl A. Nienaber Ferris State University LEADERSHIP STRATEGY ANALYSIS 2 Abstract Nurses have the duty to provide a safe environment
Running head: LEADERSHIP STRATEGY ANALYSIS 1 Leadership Strategy Analysis Cheryl A. Nienaber Ferris State University LEADERSHIP STRATEGY ANALYSIS 2 Abstract Nurses have the duty to provide a safe environment
OSHAcademy Course 774 Study Guide. Safe Patient Handling Program
 Safe Patient Handling Program OSHAcademy Course 774 Study Guide Safe Patient Handling Program Copyright 2014 Geigle Safety Group, Inc. No portion of this text may be reprinted for other than personal use.
Safe Patient Handling Program OSHAcademy Course 774 Study Guide Safe Patient Handling Program Copyright 2014 Geigle Safety Group, Inc. No portion of this text may be reprinted for other than personal use.
Sheila Gansemer DNP, RN Chief Nurse Executive. Amy Ketchum MS, RN, OCNS-C Clinical Nurse Specialist
 CNO/CNS Partnership to Implement Shared Governance and Support Professional Nursing Practice Midwest Orthopedic Specialty Hospital/ Wheaton Franciscan Healthcare Franklin Sheila Gansemer DNP, RN Chief
CNO/CNS Partnership to Implement Shared Governance and Support Professional Nursing Practice Midwest Orthopedic Specialty Hospital/ Wheaton Franciscan Healthcare Franklin Sheila Gansemer DNP, RN Chief
Title: uthor: Background Knowledge: Local Problem: Intended Improvement:
 1. Title: The Use of a Cognitive Aid within the Electronic Record can greatly improve the effectiveness of communication among care givers and reduce patient injuries from falls. 2. Author: M. Kathleen
1. Title: The Use of a Cognitive Aid within the Electronic Record can greatly improve the effectiveness of communication among care givers and reduce patient injuries from falls. 2. Author: M. Kathleen
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment
 Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Prevention of Injury at Work: Promoting Staff Health and Psychological Well-being. Susan Goodwin Gerberich, PhD University of Minnesota, USA
 Prevention of Injury at Work: Promoting Staff Health and Psychological Well-being Susan Goodwin Gerberich, PhD University of Minnesota, USA OVERVIEW Healthcare Workforce: Globally and in the United States
Prevention of Injury at Work: Promoting Staff Health and Psychological Well-being Susan Goodwin Gerberich, PhD University of Minnesota, USA OVERVIEW Healthcare Workforce: Globally and in the United States
Factors that Influence the Occupational Health and Safety Curricula. Jeffery Spickett. Division of Health Sciences Curtin University Australia
 Factors that Influence the Occupational Health and Safety Curricula Jeffery Spickett Division of Health Sciences Curtin University Australia 1.0 INTRODUCTION Occupational health and safety has undergone
Factors that Influence the Occupational Health and Safety Curricula Jeffery Spickett Division of Health Sciences Curtin University Australia 1.0 INTRODUCTION Occupational health and safety has undergone
Preventing Overuse Injuries at Work
 Preventing Overuse Injuries at Work The Optimal Office Work Station Use an adjustable chair with good lumbar support. Keep your feet flat on a supportive surface (floor or foot rest). Your knees should
Preventing Overuse Injuries at Work The Optimal Office Work Station Use an adjustable chair with good lumbar support. Keep your feet flat on a supportive surface (floor or foot rest). Your knees should
Penn State Hershey Medical Center s Journey to State-of-the-Art Telemedicine
 Telemedicine Case Study Penn State Hershey Medical Center s Journey to State-of-the-Art Telemedicine Based in South Central Pennsylvania, Penn State Hershey Medical Center (PSHMC) is a 563-bed academic
Telemedicine Case Study Penn State Hershey Medical Center s Journey to State-of-the-Art Telemedicine Based in South Central Pennsylvania, Penn State Hershey Medical Center (PSHMC) is a 563-bed academic
REACHING ZERO DEFECTS IN CORE MEASURES. Mary Brady, RN, MS Ed, Senior Nursing Consultant, Healthcare Transformations LLC,
 REACHING ZERO DEFECTS IN CORE MEASURES Mary Brady, RN, MS Ed, Senior Nursing Consultant, Healthcare Transformations LLC, 165 Lake Linden Dr., Bluffton SC 29910, 843-364-3408, marybrady6@gmail.com Primary
REACHING ZERO DEFECTS IN CORE MEASURES Mary Brady, RN, MS Ed, Senior Nursing Consultant, Healthcare Transformations LLC, 165 Lake Linden Dr., Bluffton SC 29910, 843-364-3408, marybrady6@gmail.com Primary
