Selection of Equipment
|
|
|
- Rodger Edwards
- 10 years ago
- Views:
Transcription
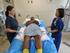
1 Selection of Equipment A key component of a multifaceted, safe, patient-handling program is the integration and use of equipment. This chapter aims to present and describe various types of commercially available equipment that can be utilized in moving and transferring patients. The categories of equipment are also available on the Technology Resource Guide Web site of the U.S. Department of Veterans Affairs ( patientsafetycenter/resguide/ergoguideptone.pdf). It should be noted that this list is not all inclusive and that equipment technologies for the bariatric patient population will be covered in a separate chapter. The purposes of this chapter are to (1) understand the variety of commercially available technology used in patient handling, (2) identify which available technologies are applicable in which clinical areas, (3) identify five categories of sling types and the safety issues involved with sling use, (4) discuss proposed ways of preventing contamination of slings and lifts, and (5) discuss the criteria for selecting lifting and transfer devices. Chapter 4 Selecting Appropriate Lifting Aids Based on the dependency levels of patients on the area, the following methods of lifting and transfer should be employed: Dependent patients. Patients classified as dependent should be lifted and transferred between beds, chairs, toilets, and bathing and weighing facilities by means of a powered lifting device. However, depending upon the patient s condition and weight-bearing capabilities, a sitto-stand lift might be used if determined appropriate in the patient assessment. The determination of which lift to use should be noted and communicated to nursing staff in a standardized way by the facility. In some situations, another means of transfer might be required. Such an option might include the use of a transfer chair that can convert into a stretcher configuration along with a lateral assist transfer device. Determining the average number of dependent patients on an area will help determine how many assistive devices are required. Partial-assist patients. An individual patient-handling plan should be developed for each patient who requires supervision or limited assistance. This plan should be developed by professional medical staff, which may include nurses or physical therapists, based on the individual assessment of the patient. The basics of this plan should be accessible and communicated to the nursing staff in a standardized way by the facility. In some cases, supervision/limited assessment patients may require a powered standassist lift. Depending on the patient s condition, stand-assist aids may be appropriate. These might be freestanding or mounted on the bed and include walking aid devices. The electric height adjustment of a bed may also be used to assist these patients to a standing position. Those patients who require assistance in standing may also be unsteady on their feet and require a walker for assistance. These nonpowered assist devices should provide safety and support to patients while allowing them to use and maintain their functional independence. The use of gait belts with handles or transfer belts that allow the caregiver to get a firm grasp on the patient may also be appropriate for this class of patient. Other lifting aid devices such as sliding boards, which provide a Copyright 2008 Association of Rehabilitation Nurses
2 bridge and means for the patient to slide from a bed to a chair in a seated position, can also be considered. The patient s handling plan should specify what transfer or lifting devices are needed, as well as the number of caregivers required to assist in the transfer. Depending on the patient s condition and ability to assist in the transfer process, at times two caregivers may be required for the transfer. In some situations, because of a patient s weight, a mechanical lift might be specified to protect against an unexpected event during the transfer process. Independent patients. Independent patients are normally capable of bearing their own weight and walking without supervised assistance, though they may require a walking aid. They do not normally require mechanical assistance for transferring, lifting, or repositioning. However, a patient s condition may vary due to any number of factors, and caregivers should be trained to be aware of changes in a patient s abilities. Any time a patient is unable to bear weight or come to a standing position and must be lifted with extensive assistance during the lift or transfer process regardless of how that patient was originally assessed both the patient and caregiver are at risk of injury. Therefore, mechanical lifting devices and lifting aids may be required. Lifts from floor. In almost all situations in which a patient must be lifted from the floor, a floor-based lift or inflatable cushion lift is required. A patient who has fallen to the floor should be assessed for injury prior to being lifted. Training will be provided to nursing staff regarding when a patient should or should not be moved and when a mechanical lift should or should not be used due to patient injury. A plan should be specified in advance for moving and lifting patients in these situations. The plan should specify a minimum number of caregivers needed to assist in any manual lift, as well as the need for specially trained or selected caregivers. Special training should be provided when such manual lifts are required. Where a patient has fallen and can regain a standing position with minimal assistance, a transfer belt or gait belt with handles can be used as a lifting aid, provided an adequate number of staff members are available to provide needed assistance. Repositioning. Whenever possible, patient repositioning should be minimized. When patients require frequent turning or repositioning for therapeutic needs, treatment surfaces on beds can help meet these therapeutic needs and also minimize the physical demands on patient care providers for repositioning tasks. Proper and optimum use of bed control adjustments should also be used to minimize the need for repositioning. Proper bed adjustment can prevent a patient from sliding down in bed. When a patient does slide down to the foot of the bed and repositioning is required, bed controls and features should be evaluated and utilized to the fullest extent possible. This will maximize the ergonomic advantage to the caregiver during these activities. When possible, beds should be raised to the height of the caregiver s elbow. The Trendelenburg position (in which the head of the bed is lower than the foot) should be used when possible to facilitate the repositioning process, if the patient can tolerate this position. A variety of friction-reducing devices and small hand slings are also available to assist in the repositioning process. A mechanical lift should be considered when a major bed repositioning is required. All repositioning in beds should be performed by at least two caregivers. When patients are capable of assisting, they should be involved in the repositioning process. Appropriate chairs and chair adjustments should be used to minimize the need for repositioning of patients in chairs. Chairs with features such as the
3 tilt-in space should be sought to help maintain proper positioning of a patient. When there is a need to reposition a patient in a chair, proper use of a sit-stand lift should be considered as a first option. Gait belts, transfer belts, and hand slings may be used to facilitate the repositioning process. When these lifting aids are used, at least two caregivers should be involved in the repositioning process. When mechanical lift devices cannot be used. Unusual situations in which mechanical lift devices cannot be used should be identified in advance; specific lifting procedures should be designated for those situations. For example, when a patient is admitted who weighs in excess of the safe lifting capacity for the standard mechanical lifts at a facility, appropriate mechanical lifts that accommodate higher weight limits should be obtained. Standard mechanical lifts will normally accommodate patients weighing up to 350 to 400 pounds. More substantial lifts will accommodate 600-pound patients, and bariatric lifts are available that can lift patients up to 1,000 pounds. In addition, a mechanical lift might not be appropriate due to a patient s medical condition. Other methods of transfer might include transfer chairs. These chairs transform into a stretcher configuration, thereby converting a standard bed-to-chair transfer into a lateral transfer. When transfer chairs are employed, lateral transfer assistive devices should be used. These include mechanically powered transfer devices, which pull the patient across one surface to the other, and friction-reducing devices, which aid in sliding a patient from one flat surface to another. In other situations in which mechanical lifting devices are not appropriate, lifting aids such as sliding boards, transfer belts, and gait belts with handles may be specified by the medical professional. In these situations, the minimum number of caregivers needed to assist in the transfer as well as the need for specially trained or selected caregivers should be identified. Special training should be provided for such assisted manual lifts. Combative and mentally impaired patients. It is expected that in most situations, a combative or mentally impaired patient who requires a lift based on dependency needs can be lifted using an appropriate mechanical lifting aid device. Combative or uncooperative patients may require more caregivers to assist in the process. Should a member of the facility s professional staff determine that a mechanical lift is inappropriate for a particular patient because of the patient s mental condition or behavior, that determination should be noted in the accessible records for that patient. Under such circumstances, a specific plan for lifting and transferring that patient should be developed in advance, specifying the number and type of caregivers needed to assist. Equipment availability. An adequate quantity of appropriate equipment should be available for use. Equipment should be stored and available in highly accessible areas. An appropriate maintenance program should be instituted to ensure that equipment is maintained in good working order and that batteries are charged regularly and are readily available. An adequate amount of equipment accessories such as slings must be available in a convenient location. An adequate variety of slings, including various sizes as well as specialty toileting and bathing mesh slings, should be available. In addition to mechanical lifts, facilities should seek out appropriate friction-reducing devices, sliding boards, transfer belts, and gait belts with handles.
4 Equipment Categories for Safe Patient Handling and Movement An integral part of implementing ergonomics in the healthcare environment is to understand what technological solutions are currently available for safer patient handling. Healthcare technology has greatly improved, as seen by the evolution of the design and features in patient care slings; lifts for moving patients; beds; powered transport devices; accessories for independent patient moving (lateral slide aids, repositioning devices); and specialty mattresses. These are only a few examples of technological improvements in the healthcare field. The following categories briefly explain and demonstrate the variety of technologies available to improve patient and staff safety. Air-Assisted Lateral Sliding Aids These devices consist of a flexible mattress that is placed under a patient in the same manner as a transfer board. There is a portable air supply that inflates the mattress. Air flows through perforations in the mattress and the patient is moved on a cushioned film of air, allowing staff members to perform the task with much less effort. These technologies are particularly suitable when performing lateral transfers involving patients with special medical conditions, such as pressure sores (Figure 4-1). Figure 4-1. Air-Assisted Lateral Sliding Aid Figures are used with permission of the Veterans Health Administration Friction-Reducing Lateral Sliding Aids Friction-reducing lateral sliding aids can assist with bed-to-stretcher transfers. These devices can be positioned beneath the patient or resident, similar to a transfer board, and provide a surface to slide the patient more easily due to the friction-reducing properties of the device (Figure 4-2). These are simple, low-cost Figure 4-2. Friction-Reducing Lateral Sliding Aid devices, usually made of a smooth fabric that is foldable and very easy to store. Properly designed handles can reduce horizontal reach. A biomechanical evaluation was conducted evaluating 11 of these devices, and results indicated that use of extended pull straps reduced spinal compression on the lower back due to adopting a more upright posture (Lloyd & Baptiste, 2006). Mechanical Lateral Transfer Aids The task of lateral transfers can be made easier by two types of products. One is referred to as a mechanical lateral transfer aid and the other is a stretcher with lateral transfer features. The first type is motorized and is especially useful for bariatric patients or fully dependent patients who are unable to assist with the transfer. Motorized devices work by rolling a rod in the sheet that the patient lays on, then attaching two clamps securely to the rod. The caregiver presses a button which then retracts the belt toward the device, thus pulling the sheet with the patient across to the desired surface. (See Figure 4-3). This type of lateral transfer aid eliminates the
5 need to manually slide the patient, minimizing risk to the caregiver. The second product type is commercially available as a height adjustable stretcher (24 36 ) designed with a manual crank, which moves a mattress pad laterally. This product also has the capability to be converted into a chair, thus eliminating a transfer if the patient needs to be moved from a supine position to a seated one. Figure 4-3. Mechanical Lateral Transfer Aid Transfer/Converta Chair These convert from a seated chair into a stretcher in which the back of the chair pulls down and the leg supports come up to form a flat stretcher (Figure 4-4). These devices Figure 4-4. Transfer/Converta Chair facilitate the lateral transfer of the patient or resident and eliminate the need to perform a vertical lift to a stretcher then a lateral transfer to the bed. Some converta chairs also have a built-in mechanical transfer aid for a bed-to-stretcher transfer (as mentioned previously). This is a positive feature if it eliminates any manual work done by the caregivers yet maintains safety for patients. Ceiling-Mounted Lifts Ceiling-mounted lifts have proven to be a more popular solution than floor-based lifts when transferring patients within a room. Ceiling lifts work by suspending the resident in a sling from a track that is bolted to the ceiling. There are two types of tracks available: a single, or dedicated, track and an X Y track. The single, or dedicated, track limits the patient to being moved along the area that the track covers (i.e., in a straight path). The X Y track has more versatility, because the coverage area is larger and allows the resident to be moved around more in the room. Some patient rooms design ceiling tracks so that they enable patients to be moved from the bedroom into the bathroom. The benefits of using a ceiling track system are that it takes up no floor space and requires less force to operate than a floor-based lift, thus reducing the risk of injury to the caregiver during patient care. Another advantage of using a ceilingmounted device is that there is no need to maneuver it over floors and around furniture. Powered Floor-Based Lifts Probably the most common lifting aid device in use is a floor-based lift (Figure 4-5). The lifts work with the use of a sling that is placed under or around the patient, a spreader bar that connects to the sling, and a portable base unit as shown. Floor-based lifts are appropriate when there are no rugs or carpet, when overhead lifts are impractical or not Figure 4-5. Powered Floor-Based Lift
6 available, and when patient transfers from bed to chair/wheelchair, toileting, and bathing tasks are required. These units are usually not as expensive as ceiling-mounted lifts because the surrounding infrastructure (ceiling) does not have to be modified. Floor-based lifts are usually used for highly dependent patients. A number of models and configurations are available. Newer lifts have special features such as a positioning system that allows the resident to be positioned at a preferred angle in the sling during the transfer. This is important especially for those patients with compromised respiratory systems. Sling type should be compatible with the lift and type of transfer. Use of mismatched slings with manufacturers may void warranty but more importantly may cause an adverse event. Slings An operational definition of a patient care sling is a fabric device used with mechanical lifting equipment to temporarily lift or suspend a body or body part to perform a patient-handling task (VA Patient Safety Research Center, 2005). Patient-handling slings have greatly improved over the years. Early versions of slings were made from ship s canvas and recycled fire hoses (Grant, 1961). Currently, slings are made from light, durable materials such as Figure 4-6. Universal or Seated Sling washable nylon, polyester, or even materials that are disposable after a single patient use. We have categorized slings into five types based on functionality and use: seated, standing, supine or stretcher, ambulation, and limb support slings as shown in the following figures. Development of limb support slings has not been addressed as fully by manufacturers as other types of slings. However, prototypes have been used in Figure 4-7. Sit-to-Stand Sling other countries to suspend an extremity for extended periods while performing prolonged treatment tasks such as dressing changes. (National Back Pain Association [NBPA], 1998, and Royal College of Nursing [RCN], 1998). Seated Sling. This sling type maintains the patient in a sitting position (Figure 4-6). Functional tasks include vertical transfers, toileting, bathing, repositioning in chair, fall Figure 4-8. Supine Sling rescue. Standing Sling. This type of sling provides assistance for standing upright and weight bearing (Figure 4-7). Functional tasks include toileting, vertical transfers, functional sit-stand training/support, dressing, and pericare. Supine Sling. This sling type maintains the patient in a lying position (Figure 4-8). Functional tasks include
7 lateral transfers, making an occupied Figure 4-9. Ambulation Sling bed, toileting, bathing, repositioning in bed, and fall rescue. Ambulation Sling. This sling provides assistance for ambulation (Figure 4-9). Limb Support. This sling maintains limbs in static positions. Functional tasks include limb support for wound debridement, surgical procedures, and bathing (Figures 4-10 and 4-11). Selection of slings is very important. It should be based upon the specific patienthandling activity to be performed and the specific characteristics of the patient. Figure Limb Support Sling with Floor-Based Lift For example, an amputee sling would be inappropriate for a patient with both legs. A sit-stand sling would be inappropriate for toileting. Sling Insertion and Placement. Proper sling insertion and placement is dependent upon sling type and patient tolerance, ability, and medical condition. Proper and safe techniques for sling application need to be taught to healthcare staff prior to sling application Figure Limb Support and equipment use. Adverse events of incorrect sling application can be harmful for the patient. These include tearing of skin, irritation of existing ulcers and bruises, and discomfort or pain under armpits or groin areas, which are common areas that are affected due to improper sling fit. Sling Attachment. Sling attachment is often taken for granted and missed as an important safety issue for both patient and caregiver. Attachment of the sling to the right spreader bar is crucial to maintain patient comfort and safety during the transfer. A wider or longer spreader bar enables a resident with larger girth to have more room while being transferred thus facilitating a safer and more comfortable transfer. There are two types of commercially available lift attachments. For example, some slings are attached to the lift via hooks or clips while other slings are designed with loops that can be hooked onto the lift frame. Sling designs that allow the sling to be attached directly to the frame via plastic clips minimize the magnitude of swing by the patient in the sling (McGuire, Moody, Hanson, & Tigar, 1996). It is significant that caregivers consistently assess pressure points and comfort subsequent to sling application. Subjects have reported discomfort of the upper and lower back, buttocks, thighs, and lower legs in regard to seated slings (McGuire et al., 1996). Sling Removal. Removal of the sling is the final step in a patient transfer using a lift and a sling. The important issues in removing the sling include minimizing shear forces, preventing patient
8 discomfort, and ensuring caregiver safety. Leaving a sling under a patient has been contraindicated especially in cases in which the patient has compromised skin integrity or pressure sores. A frictionreducing device can be used for easier sling removal. Slings and Hygiene Issues. Due to a shortage of slings, frequent sharing, and lack of protocol for appropriate sling use, infections have become a problematic issue related to sling use in the healthcare environment. According to Burke (2003), costs of iatrogenic infections (those acquired after hospital admission or associated with health care) are high for hospitals and patients. Infectionrelated adverse events affect approximately 2 million patients each year in the United States, which result in additional patient care costs of an estimated $4.5 $5.7 billion per year and some 90,000 deaths (Burke). The following are guidelines for lift and sling users to prevent contamination: Assign one sling for each patient and store within their room. Disinfect or launder fabric slings or discard disposable slings that are soiled, damaged, or contaminated. Effective disinfection is determined by both the manufacturer and each facility s infection control department. High drying temperatures can distort a sling s original shape, thereby affecting its size (Boden, 1999a). Hand washing is essential following each patient contact and after handling slings and other patient equipment. Lifts should be stored in a central location for easy accessibility. Provide a sufficient supply of fabric slings. Ensure that users receive adequate training about cleaning and laundering of contaminated slings. Consider onsite laundering for quick turnover of clean slings and to reduce equipment loss. (Boden, 1999a; Boden, 1999b; Barnett, Thomlinson, Perry, Marshall, & MacGowan, 1999). Powered Sit-to-Stand Lifts These lifts provide an alternative Figure Powered Sit-to-Stand Lift way to transfer a patient from sitting to standing without using manual techniques. These types of lifts are very useful where patients are partially dependent and have some weightbearing capabilities. They are excellent for moving patients in and out of chairs and for toileting and dressing tasks. Powered sit-to-stand lifts can be easily maneuvered in restricted areas such as small bathrooms. There are some variations in the sling design, but the basic concept is simple (see Figure 4-12) and very easy to place around the patient. It is important that the resident has sufficient upper body strength and is able to hold on to handles when using this type of lift. Repositioning Devices Repositioning aids are typically made with low-friction fabric and are either tubular in shape or consist of two pieces of material that slide over each other (see Figure 4-13). They are designed to reduce friction, thus making it easier to slide the patient around in bed or in a chair. Repositioning aids are available to reposition a patient upright or turned to their side. There
9 are devices that are used for seated repositioning and those used for supine. Refer to the Technology Resource Guide available at va.gov/patientsafetycenter/resguide/ ErgoGuidePtOne.pdf. A benefit of some devices is the unidirectional feature; when engaged by zipping a section, it prevents the patient from sliding down as friction is reintroduced. The traditional method of repositioning a patient in bed has been to hook under the patient s arms and pull toward the head of the bed. This posture places stress on the caregiver s back and shoulders as he or she is required to reach excessively in a forward bent position, subjecting his or her to a high risk of back and shoulder injury. This procedure is also dangerous for patients as it can result in dislocated shoulders and damage to the nerve bundles under the arm. Figure 4-14 illustrates the poor posture adopted to reposition a patient in bed. Figure Repositioning Device Figure Example of Poor Posture Adopted to Reposition a Patient in Bed Bed Improvements to Facilitate Transfer or Repositioning Current bed technologies incorporate many ergonomic improvements. Some examples include beds that eliminate the need for bed-to-chair transfers by easily converting to a chair configuration. Another innovation in bed design, referred to as a shearless pivot, reduces the need to constantly reposition a patient in bed. The shearless pivot minimizes the amount of patient slippage down to the foot of the bed when raising the head of the bed. Further innovations with bed mattress surfaces can aid rotation and move a patient as needed in many intensive care units by utilizing air bladders incorporated into the mattress surface. Sliding Boards For seated bed-to-chair or chair-to-toilet Figure Sliding Board transfers, low-cost sliding boards are available. Sliding boards are usually made of a smooth, rigid material with a low coefficient to friction, which allows for an easier sliding process. These boards act as a supporting bridge during seated slide transfers. Some manual lifting is still required to move the patient; however, sliding boards offer considerable assistance at a minimal cost. See Figure 4-15 for an example of a suitable use of a sliding board. These devices may also be useful in assisting someone in and out of a car.
10 Gait/Transfer Belt with Handles Figure Gait/Transfer Belt with Handles Gait/transfer belts are typically used to assist partially dependent patients transfer from a seated to a standing position. Gait belts with handles greatly improve the caregiver s grasp, hence reducing injury risk. Gait/transfer belts are positioned on patients around the waist as shown in Figure Small hand-held slings with handles that go around the patient can also facilitate a safe transfer. These options are available for patients with weight-bearing capability who need minimal assistance. Equipment Evaluation Process Equipment evaluations are typically used to compare the usability of competitive equipment types for a specific application. As such, development of an equipment evaluation protocol is highly dependent on equipment type and application. The Safe Patient Movement Technical Advisory Group has defined 12 patient-handling equipment categories and at least nine product applications. Table 4-1 has been modified to include rehabilitation nursing applications. This presents 100 or more equipment type/application combinations, each requiring an individualized evaluation protocol. Table 4-1. Equipment Type/Application Combinations, Defined by The Safe Patient Movement Technical Advisory Group Patient-Handling Equipment Air-assisted lateral sliding aids Bed improvements Ceiling-mounted lifts Dependency chairs Friction-reducing lateral sliding aids Gait belts with handles Mechanical lateral transfer aids Powered floor-based lifts Powered sit-to-stand lifts Repositioning devices Stand assist aids Transfer chairs Sliding boards Slings Equipment Applications ER, radiology, general rehabilitation units, surgical, spinal cord injury (SCI), bariatric units Acute medical/surgical units, SCI, nursing homes, palliative care Acute medical/surgical units, general rehabilitation units, palliative care, SCI, outpatient clinics ER, radiology, general rehabilitation units, nursing homes, outpatient clinics Acute medical/surgical units, ER, radiology, general rehabilitation units, SCI, outpatient clinics Outpatient clinics, general rehabilitation units, nursing homes Operating and recovery rooms Inpatient (general) Intensive care unit (ICU) Acute medical/surgical units, nursing home care units Home care Spinal cord injury units, bariatrics General rehabilitation units, nursing homes Inpatient, ICU, home care Evaluation Team The evaluation team should consist of personnel with expertise in ergonomics, occupational healthcare safety, industrial hygiene, infection control, risk management, and nursing. This team will be responsible for organizing and coordinating the equipment evaluation process, screening of vendors/equipment, developing criteria, and ultimately selecting equipment to buy
11 or rent. Management support is vital for this team to successfully work, and communication at all levels is important. Train-the-trainer meetings might be appropriate to introduce onsite champions and provide educational resources to the central team. Further, an electronic resource such as a news group or Listserv could be set up to encourage communication and sharing of ideas/solutions among site champions. The equipment evaluation process may consist of any or all of these components: understanding sources of information initial review and screening process selection of products for clinical evaluation. Sources of Information Information may be derived from a variety of sources, including product information, literature reviews, external evaluations, references, lab-based, and clinical evaluations. There are advantages and disadvantages to each source of information, which will be briefly described in the following section. Any equipment information received from a manufacturer may or may not be biased and needs to be carefully considered. Literature reviews and external evaluations can be retrieved quite quickly, but present opinions from manufacturing companies may not be objective. References from literature reviews provide helpful information. All of these sources can be completed in a reasonable amount of time, as opposed to lab-based or clinical evaluations. Comparative lab-based evaluations are often time consuming and costly, but they can be very comprehensive and produce objective results, which can be quite useful if they take into account caregiver and patient input. Clinical evaluations that include both caregiver and patient input are strong, but subjective in nature. However, they do provide important results as they are performed in real settings, not a laboratory. Caregiver feedback on organizational and other factors may be learned via this type of evaluation due to the study being conducted in the real work environment. A lab-based evaluation on the use of friction-reducing sliding aids, followed by a clinical evaluation, produced some interesting findings that would not have come to light if the clinical study was not done. The lab results identified one product as the best due to properties that reduced spinal compression. However, the clinical study identified a different product as the most preferred by the nurses due to unique features (Lloyd & Baptiste, 2006). The lab-based evaluation produced objective findings, and the clinical study yielded valuable, subjective feedback from the product users. Understanding the pros and cons of various sources of information is crucial in the equipment selection process. Initial Review and Screening Process The initial review and screening process should typically be initiated by identifying all the products that could be used to perform the desired application in a reasonable and safe manner. It will be useful to develop criteria for the desired product type. A Request for Information (RFI) based on these criteria may be published in Commerce Business Daily. Local contracting staff can assist with this process. Literature for each of these product types should then be requested from each identified product manufacturer. Following an initial review of the product literature to eliminate those products that would not be suitable for the intended application, the evaluation team should approach each manufacturer and request information on any previously performed or ongoing clinical and laboratory-based equipment evaluations. Be aware that if the product manufacturer has performed the equipment evaluation, not an outside research facility, then the findings of such evaluations might be biased or incomplete. A literature search, both peer review and newspaper/industry magazine, should be conducted to determine if other information is available for each product.
12 Local contracting staff should be involved early in the process and may assist with performance or cost of operation measures pertaining to both the equipment and vendor. Performance measures considered by contracting staff include the following: special features of the product not offered by comparable products trade-in considerations probable life of the product compared to comparable products warranty considerations maintenance requirements and availability past performance environmental and energy efficiency considerations. Contracting staff may also contact the Federal Drug Administration (FDA) and National Reporting Office (NPO) for any information pertaining to equipment-related incidents and recall information. Discussion with vendor customer referrals can present very useful information for the evaluation process. If possible, follow-up meetings with select referred facilities might be conducted at their site. The purpose of such meetings is to view equipment operation, hold discussions with facility staff and patients, and try to attain cost of operation information (incidence/maintenance and adverse events). A referred facility might even be willing to provide access to patients and staff for a clinical study of mutual benefit. Selection of Products for Clinical Evaluation Before embarking upon a clinical evaluation, the number of products tested should be reduced to three to five competitive products. Often, due to the specialized nature of the equipment, this can be achieved by carrying out an effective initial review and screening process. If this preliminary process yields only one suitable product, and that product appears to reasonably satisfy the task requirements without imposing increased risk to either the patient or caregiver, then the evaluation is probably complete. If the preliminary process identifies more than three suitable products, more products need to be selected for a clinical assessment. There is no set rule for identifying a select few products for further evaluation, but a good organizing principle is to identify the following criteria: best choice based upon the preliminary evaluation (initial review/screening) most popular based on sales information upper and lower functionality extremes e.g., most basic and most comprehensive products on the market any product that presents an innovative approach to the task feedback from equipment fairs. Oftentimes, one particular product will satisfy two or more of the above criteria, thereby reducing the overall number of products needed for further evaluation. Equipment vendors might also be invited on-site to present their products to the entire nursing staff and appropriate patient populations at an Equipment Day exhibition. Product samples may be set up and demonstrated in the hospital auditorium. Nurses and patients should be encouraged to examine each product and provide feedback via a structured evaluation questionnaire. A compilation of results from this rapid evaluation process can be useful in identifying the top three to five products for further evaluation. Clinical Evaluations Clinical evaluations are the preferred method for comparative equipment evaluations as they yield reasonable results. See Figures 4 17 through 4 24 for examples of tools that can be used to facilitate a clinical evaluation. Contact manufacturers of products identified from the above preliminary evaluation and
13 preselection processes to provide a product sample for on-site evaluation purposes. It is highly likely that all manufacturers will be eager to provide a sample for potential sales. The number of groups involved in the clinical study should equal the number of products available for testing, plus a control group that performs the task in the same manner as typically performed. The groups should be balanced; each study group should include participants. This number is not based on any statistical power analysis, but it is based on experience and should provide reasonably reliable results. If the selected products are quite dissimilar, it may be possible to reduce the number of subjects to If the products are highly similar, it might be necessary to increase the number of patients. If there are not enough caregivers and patients within the facility or department to provide adequate numbers of subjects for each group, it will be necessary to perform evaluations on each product in random order. Institutional review board approval may be necessary before enrolling any caregivers or patients in the clinical evaluation study. If a product already has FDA approval for its intended application, the evaluation may be exempt from board review. Check with your local institution board review office for clarification at the earliest opportunity. Caregivers should receive training in the appropriate use of the equipment, typically provided by the product manufacturer immediately preceding use of that equipment. If the equipment is highly complex, it might be necessary to provide a resource for questions and a follow-up training session several weeks after introduction of the equipment. A follow-up training session also provides an opportunity to train staff who may have been off-duty during the initial training session. Objective methods of data collection are rarely utilized in clinical studies, though simple measurement systems, such as EMG (electromyography) or video/photography might be utilized for a select few subjects as an alternative to performing a costly laboratory-based evaluation. Data for clinical evaluations is often compiled based on caregiver and patient reporting. To minimize subjective variability, a structured form is often developed for this purpose. Dedicated forms are developed for caregiver and patient populations. See Figures 4 17 through 4 24 for tools to facilitate a clinical evaluation. One method is to identify the key features across product types and ask each caregiver and patient to report their perceived findings on a structured scale. Key features might include: length, balance, texture, grip, aesthetics, safety, stability, durability, comfort, and ease of use. Response options for the rating scales may be formulated in a number of ways. The most common format is to provide a horizontal numerical scale (1 5), often with anchor words to identify the meaning of the scale (e.g., strongly agree and strongly disagree). The subject circles the number that best represents their perception of acceptability of that feature. Another commonly used format, referred to as the visual analog scale, provides a continuous line in which a mark is placed between the two endpoints, indicating perception of acceptability. While the latter method may be more sensitive to differences among products, it may be misunderstood by the respondent and is more difficult to score, and therefore requires vigilance by the evaluation team or local peer leader. Questionnaires may be presented to each subject at defined intervals throughout the evaluation process. These intervals should be determined by the evaluation team based upon the protocol and may be weekly, monthly, or at the commencement and conclusion of the evaluation period. One advantage of the cross design method is that it allows caregivers and patients to rank design features across all products tested, since they have had the opportunity to personally experience each product. At the conclusion of the study, all product samples should be made available to the participants, who are asked to rank their preferences for each feature. As discussed earlier, protocol development is highly dependent upon equipment types and applications. As such, it is not possible to present one questionnaire that could be used across
14 all equipment evaluations. These questionnaires should be developed with the assistance of the central evaluation team for each equipment evaluation. See examples of product rating forms for both caregiver and patient in Figures 4-17 through These can be developed or modified to suit individual needs that better reflect pertinent factors or indicators of interest. Leasing Versus Purchasing Decision Once a decision has been reached, local contracting staff must be consulted to assist with negotiating the purchasing procedures. Since the procurement of assistive transfer devices is intended to reduce risk of injury to caregivers and patients, we have, in the past, successfully negotiated a guarantee with equipment vendors. Knowledge of this process might prove to be useful in your own purchasing negotiations. Essentially, vendors are asked to guarantee that procurement of their product will lead to a certain reduction in injuries among staff. Anticipated injury reduction may range from 20% to 50% and is dependent upon the equipment type and application. If the negotiated injury reduction potential were not achieved within a specified time frame, then the contract would call for a purchase refund. This process achieves many objectives, including capital investment justification to equipment procurement committees and enhanced after-sales service from the equipment vendor. The following factors may be considered when purchasing or renting equipment: number and frequency of admissions equipment purchase cost rental cost space demands including fit through doorways and hallways patient care needs type of tasks needed equipment storage needs length of stay equipment cleaning and maintenance needs. Criteria for Selecting Lifting and Transferring Devices 1. The devices should be appropriate for the task that is to be accomplished. 2. The device must be safe for both the patient and the caregiver. It must be stable and strong enough to secure and hold the patient. Use of the device should not subject the caregivers to excessive awkward postures or high exertion of forces when gripping or operating equipment. 3. The device must be comfortable for the patient. It should not produce or intensify pain, contribute to bruising of the skin, or tear the skin. 4. Operation of the device should be understood and managed with relative ease. 5. The time required to use the device must be efficient. 6. Need for maintenance should be minimal. 7. Storage requirements should be reasonable. 8. The device must be maneuverable in a confined workspace. 9. The device should be versatile. 10. The device must be easily cleaned and concur with infection control requirements. (Refer to the previous section on slings for further information on infection control regarding sling use.) 11. There must be an adequate number of the device on hand so that it is accessible. 12. The cost must be reasonable. Directions for the Future Gaps in patient-handling research include patient egress from cars. Low vehicles make it extremely difficult to assist a dependent patient out of a car. Most lifts cannot accommodate the required low level or maneuver efficiently to safely accommodate this transfer.
15 Options for car egress are quite limited, including slide boards used to assist patients from the car seat to the wheelchair and some floor-based car lifts. The least favored option (with the highest injury risk) is when the caregivers resort to using the traditional manual technique of stand, support patient, and pivot to wheelchair manually. This places both the caregiver and patient at a high risk of injury. The development and evaluation of technology that can help patients with car egress is definitely needed to ensure safe car transfers for both caregivers and patients. References Barnett, J., Thomlinson, D., Perry, C., Marshall, R., & MacGowan, A. P. (1999). An audit of the use of manual handling equipment and their microbiological flora Implications for infection control. Journal of Hospital Infection, 43, Boden, M. (1999a). Contamination in moving and handling equipment. Professional Nurse 14, Boden, M. (1999b). Infection control in moving and handling. Professional Nurse, 14, Burke, J. P. (2003). Infection control A problem for patient safety. New England Journal of Medicine, 348, Grant, W. R. (1961). Principles of rehabilitation. III. Hoists and slings. Practitioner, 186, Lloyd, J., & Baptiste, A. (2006). Friction-reducing devices for lateral patient transfers: A biomechanical evaluation. AAOHN, 54, McGuire, T., Moody, J., Hanson, M., & Tigar, F. (1996). A study into clients attitudes towards mechanical aids. Nursing Standard, 11, National Back Pain Association & Royal College of Nursing. (1998). The guide to the handling of patients: Introducing a safer handling policy (4th ed.). Middlesex, UK: National Back Pain Association. U.S. Department of Veterans Affairs. (2005). Patient care ergonomics resource guide: Safe patient handling and movement. Retrieved July 17, 2008, from patientsafetycenter/resguide/ergoguideptone.pdf.
Sling Guide. Joerns Healthcare. Redefining patient handling
 Sling Guide Joerns Healthcare Redefining patient handling Contents Introduction 3 Oxford Sling Models 4 FIM Scoring 7 Oxford Slings Feature 8 Sling Accessories 10 Cradle Options 10 Range of Sizes 12 Weight
Sling Guide Joerns Healthcare Redefining patient handling Contents Introduction 3 Oxford Sling Models 4 FIM Scoring 7 Oxford Slings Feature 8 Sling Accessories 10 Cradle Options 10 Range of Sizes 12 Weight
Patient Lifts SAFETY GUIDE
 Patient Lifts SAFETY GUIDE Caregiver Safety Tips.... 1 Know Your Lift... 2 Check Patient's Condition.... 3 Select Patient's Sling Size.... 4 Choose Sling and Sling Bar.... 5 Prepare Environment.... 6 Prepare
Patient Lifts SAFETY GUIDE Caregiver Safety Tips.... 1 Know Your Lift... 2 Check Patient's Condition.... 3 Select Patient's Sling Size.... 4 Choose Sling and Sling Bar.... 5 Prepare Environment.... 6 Prepare
Transfer and Positioning
 Transfer P O Box 4791 Ferndown Dorset BH22 9WB Tel: 07857 603031 Fax: 01202 877240 Email: [email protected] 25 years of simple solutions for great results SystemRoMedic unique easy transfer concept,
Transfer P O Box 4791 Ferndown Dorset BH22 9WB Tel: 07857 603031 Fax: 01202 877240 Email: [email protected] 25 years of simple solutions for great results SystemRoMedic unique easy transfer concept,
SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN
 Department of Veterans Affairs VHA DIRECTIVE 2010-032 Veterans Health Administration Washington, DC 20420 SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN 1. PURPOSE: This Veterans Health Administration
Department of Veterans Affairs VHA DIRECTIVE 2010-032 Veterans Health Administration Washington, DC 20420 SAFE PATIENT HANDLING PROGRAM AND FACILITY DESIGN 1. PURPOSE: This Veterans Health Administration
http://intranet.urmc-sh.rochester.edu/policy/smhpolicies/section10/10-22.pdf
 APPENDIX B Patient Care Lifting Guidelines Patient handling, including lifting, transferring, and repositioning, is covered by SMH Policy 10.22 Minimal Lift for Patient Handling, which can be found at:
APPENDIX B Patient Care Lifting Guidelines Patient handling, including lifting, transferring, and repositioning, is covered by SMH Policy 10.22 Minimal Lift for Patient Handling, which can be found at:
Equipment for moving and handling people
 section 7 Equipment for moving and handling people Contents Using equipment for moving and handling people Types of equipment Examples of moving and handling equipment Slide sheets Transfer belts Transfer
section 7 Equipment for moving and handling people Contents Using equipment for moving and handling people Types of equipment Examples of moving and handling equipment Slide sheets Transfer belts Transfer
Redefining Patient Handling
 Redefining Patient Handling Sling Guide Joerns.co.uk Contents Introduction 3 Oxford Sling Models 4 Sling Accessories 9 Oxford Sling Features 10 User Guide 12 Identification Label 12 Weight Capacity 12
Redefining Patient Handling Sling Guide Joerns.co.uk Contents Introduction 3 Oxford Sling Models 4 Sling Accessories 9 Oxford Sling Features 10 User Guide 12 Identification Label 12 Weight Capacity 12
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Hoist and sling assessment guidelines. www.safepatienthandling.co.uk. Hoist and sling assessment guidelines
 Hoist and sling assessment guidelines www.safepatienthandling.co.uk 21 Contents 1.0 Introduction 4 2.0 Key risk assessment principles 5 3.0 Functional Independence Measurement 6 4.0 Stand assist and mobile
Hoist and sling assessment guidelines www.safepatienthandling.co.uk 21 Contents 1.0 Introduction 4 2.0 Key risk assessment principles 5 3.0 Functional Independence Measurement 6 4.0 Stand assist and mobile
Physiotherapy Database Exercises for people with Spinal Cord Injury
 Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Physiotherapy Database Exercises for people with Spinal Cord Injury Compiled by the physiotherapists associated with the following Sydney (Australian) spinal units : Last Generated on Mon Mar 29 16:57:20
Guidelines for Nursing. Homes. Ergonomics for the Prevention. Musculoskeletal Disorders OSHA 3182-3R 2009
 Guidelines for Nursing Homes OSHA 3182-3R 2009 Ergonomics for the Prevention of Musculoskeletal Disorders Guidelines for Nursing Homes Ergonomics for the Prevention of Musculoskeletal Disorders U.S. Department
Guidelines for Nursing Homes OSHA 3182-3R 2009 Ergonomics for the Prevention of Musculoskeletal Disorders Guidelines for Nursing Homes Ergonomics for the Prevention of Musculoskeletal Disorders U.S. Department
Maxi Sky 2 Plus The complete ceiling lift system
 Maxi Sky 2 Plus The complete ceiling lift system A twin cassette ceiling lift system for patients up to 454 kg/1000 lbs with people in mind A versatile ceiling lift system for bariatric patients and the
Maxi Sky 2 Plus The complete ceiling lift system A twin cassette ceiling lift system for patients up to 454 kg/1000 lbs with people in mind A versatile ceiling lift system for bariatric patients and the
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES PATIENT LIFT SYSTEMS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance Program (CMAP) on the requirements for
PROVIDER POLICIES & PROCEDURES PATIENT LIFT SYSTEMS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance Program (CMAP) on the requirements for
Policy & Procedure. Safe Patient Handling (No Lift Policy)
 Effective date signifies approval of this MHS policy by the Performance Improvement Leadership Oversight Team (PILOT) (see minutes). Policy. Policy & Procedure Safe Patient Handling ( Lift Policy) Effective
Effective date signifies approval of this MHS policy by the Performance Improvement Leadership Oversight Team (PILOT) (see minutes). Policy. Policy & Procedure Safe Patient Handling ( Lift Policy) Effective
Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices
 Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices September 29, 2010 Tangee B. Kizer, BSM Executive Director Environmental and Guest Services Carolinas HealthCare
Fundamental of a Successful Team Environmental Services and Patient Transport Best Practices September 29, 2010 Tangee B. Kizer, BSM Executive Director Environmental and Guest Services Carolinas HealthCare
Move and position individuals in accordance with their plan of care
 Move and position individuals in accordance with their plan of care Page 1 of 21 Level 2 Diploma in Health and Social Care Unit HSC 2028 Tutor Name: Akua Quao Thursday 12 th September 2013 Release Date:
Move and position individuals in accordance with their plan of care Page 1 of 21 Level 2 Diploma in Health and Social Care Unit HSC 2028 Tutor Name: Akua Quao Thursday 12 th September 2013 Release Date:
How to Conduct a Risk Assessment: A 5-Step Ergonomic Workplace Assessment of Rehabilitation Patient Care Environments
 How to Conduct a Risk Assessment: A 5-Step Ergonomic Workplace Assessment of Rehabilitation Patient Care Environments Chapter Introduction Ergonomics is the science of matching job tasks to workers capabilities.
How to Conduct a Risk Assessment: A 5-Step Ergonomic Workplace Assessment of Rehabilitation Patient Care Environments Chapter Introduction Ergonomics is the science of matching job tasks to workers capabilities.
Rehabilitation Aids Sling Range
 Product Guide Silvalea has designed a selection of rehabilitation aids, stand aid or stand slings which address anatomy pressure points/suitability (male/female) as well as consider activity, such as rehabilitation
Product Guide Silvalea has designed a selection of rehabilitation aids, stand aid or stand slings which address anatomy pressure points/suitability (male/female) as well as consider activity, such as rehabilitation
Transfer Assist Devices for the Safer Handling of Patients. A Guide for Selection and Safe Use
 Transfer Assist Devices for the Safer Handling of Patients A Guide for Selection and Safe Use About this guide Health care professionals can use this guide as a resource for evaluating and selecting appropriate
Transfer Assist Devices for the Safer Handling of Patients A Guide for Selection and Safe Use About this guide Health care professionals can use this guide as a resource for evaluating and selecting appropriate
HUR Rehab Line H E A L T H & F I T N E S S E Q U I P M E N T
 H E A L T H & F I T N E S S E Q U I P M E N T HUR Rehab Line HUR naturally different Contents HUR naturally different HUR SmartCard 1 HUR Rehab Line key to rehabilitation 2 SmartCard FCM Rehab Line computerized
H E A L T H & F I T N E S S E Q U I P M E N T HUR Rehab Line HUR naturally different Contents HUR naturally different HUR SmartCard 1 HUR Rehab Line key to rehabilitation 2 SmartCard FCM Rehab Line computerized
How To Buy A Rifton Tram
 Rifton TRAM Sample LMN for the Rifton TRAM School-based Therapy with Adolescents EVERY REASONABLE EFFORT HAS BEEN MADE TO VERIFY THE ACCURACY OF THE INFORMATION. HOWEVER, THE SAMPLE LETTERS OF MEDICAL
Rifton TRAM Sample LMN for the Rifton TRAM School-based Therapy with Adolescents EVERY REASONABLE EFFORT HAS BEEN MADE TO VERIFY THE ACCURACY OF THE INFORMATION. HOWEVER, THE SAMPLE LETTERS OF MEDICAL
Patient handling techniques to prevent MSDs in health care
 28 Introduction Patient handling techniques Work-related musculoskeletal disorders (MSDs) are a serious problem among hospital personnel, and in particular the nursing staff. Of primary concern are back
28 Introduction Patient handling techniques Work-related musculoskeletal disorders (MSDs) are a serious problem among hospital personnel, and in particular the nursing staff. Of primary concern are back
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
Compella Bariatric Bed Advancing bariatric care.
 Compella Bariatric Bed Advancing bariatric care. Compella Bariatric Bed Overcoming barriers to efficient, safe and dignified bariatric care. Impact of obesity on health care providers: More than 34% of
Compella Bariatric Bed Advancing bariatric care. Compella Bariatric Bed Overcoming barriers to efficient, safe and dignified bariatric care. Impact of obesity on health care providers: More than 34% of
Patient Slings. Owner s Operator and Maintenance Manual. DEALER: This manual must be given to the user of the product.
 Owner s Operator and Maintenance Manual Patient Slings DEALER: This manual must be given to the user of the product. USER: BEFORE using this product, read this manual and save for future reference. For
Owner s Operator and Maintenance Manual Patient Slings DEALER: This manual must be given to the user of the product. USER: BEFORE using this product, read this manual and save for future reference. For
Access To Medical Care For Individuals With Mobility Disabilities
 U.S. Department of Justice Civil Rights Division Disability Rights Section U.S. Department of Health and Human Services Office for Civil Rights Americans with Disabilities Act Access To Medical Care For
U.S. Department of Justice Civil Rights Division Disability Rights Section U.S. Department of Health and Human Services Office for Civil Rights Americans with Disabilities Act Access To Medical Care For
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
CRASH PROTECTION FOR CHILDREN IN AMBULANCES Recommendations and Procedures* Marilyn J. Bull, M.D., Kathleen Weber, Judith Talty, Miriam Manary
 CRASH PROTECTION FOR CHILDREN IN AMBULANCES Recommendations and Procedures* Marilyn J. Bull, M.D., Kathleen Weber, Judith Talty, Miriam Manary A joint project of the Indiana University School of Medicine
CRASH PROTECTION FOR CHILDREN IN AMBULANCES Recommendations and Procedures* Marilyn J. Bull, M.D., Kathleen Weber, Judith Talty, Miriam Manary A joint project of the Indiana University School of Medicine
Indications for a PMD as Reasonable and Necessary and Types of PMD Categories Available
 Appendix K The face-to-face examination provides the clinical information needed to determine if a patient needs a Power Mobility Device (PMD) and what type of PMD may be needed. This information needs
Appendix K The face-to-face examination provides the clinical information needed to determine if a patient needs a Power Mobility Device (PMD) and what type of PMD may be needed. This information needs
APPENDIX K. Design/Layout Considerations for Ceiling/Overhead Lift Tracks. Ceiling Lift Motor Charging Options
 ArjoHuntleigh APPENDIX K Design/Layout Considerations for Ceiling/Overhead Lift Tracks At present, not all clinical units or areas require 100 percent ceiling lift coverage (Table I-1), but with expansion
ArjoHuntleigh APPENDIX K Design/Layout Considerations for Ceiling/Overhead Lift Tracks At present, not all clinical units or areas require 100 percent ceiling lift coverage (Table I-1), but with expansion
Maxi sky 600. with people in mind
 Maxi sky 600 The complete, customised ceiling lift system with people in mind 2 Maxi Sky 600 A TOTAL CEILING LIFT CONCEPT Maxi Sky 600 is a ceiling lift system that enables patients and residents to be
Maxi sky 600 The complete, customised ceiling lift system with people in mind 2 Maxi Sky 600 A TOTAL CEILING LIFT CONCEPT Maxi Sky 600 is a ceiling lift system that enables patients and residents to be
Chapter. Some days I m so stiff. But even then, your firm yet gentle guidance always helps me move more easily. MOVING AND POSITIONING
 15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
SECTION 11: EQUIPMENT MAINTENANCE
 SECTION 11: EQUIPMENT MAINTENANCE Who should read this section? This section should be read by equipment managers and staff, unit managers and health and safety managers. It is also relevant to a range
SECTION 11: EQUIPMENT MAINTENANCE Who should read this section? This section should be read by equipment managers and staff, unit managers and health and safety managers. It is also relevant to a range
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
SLING SOLUTIONS. For every need. with people in mind
 SLING SOLUTIONS For every need with people in mind 2 Sling Solutions the comfort level of your lifter is determined by the sling ArjoHuntleigh is dedicated to improving patient handling by providing the
SLING SOLUTIONS For every need with people in mind 2 Sling Solutions the comfort level of your lifter is determined by the sling ArjoHuntleigh is dedicated to improving patient handling by providing the
Transferring Safety: Prevent Back Injuries
 Transferring Safety: Prevent Back Injuries OBJECTIVES: At the end of this class you will be able to: 1. Describe the back and what it does. 2. List things that you can do everyday in your home and at work
Transferring Safety: Prevent Back Injuries OBJECTIVES: At the end of this class you will be able to: 1. Describe the back and what it does. 2. List things that you can do everyday in your home and at work
ERGONOMICS. Improve your ergonomic intelligence by avoiding these issues: Awkward postures Repetitive tasks Forceful exertions Lifting heavy objects
 ERGONOMICS The goal of ergonomics is to reduce your exposure to work hazards. A hazard is defined as a physical factor within your work environment that can harm your body. Ergonomic hazards include working
ERGONOMICS The goal of ergonomics is to reduce your exposure to work hazards. A hazard is defined as a physical factor within your work environment that can harm your body. Ergonomic hazards include working
Featuring Blue Seal TM HANDLING WITH CARE. Safe Patient Handling Transfer and Turning
 R Featuring Blue Seal TM HANDLING WITH CARE Safe Patient Handling Transfer and Turning HANDLING WITH CARE Featuring Blue Seal TM At last a One Way Slide that really works! Blue Seal TM All SlideAssist
R Featuring Blue Seal TM HANDLING WITH CARE Safe Patient Handling Transfer and Turning HANDLING WITH CARE Featuring Blue Seal TM At last a One Way Slide that really works! Blue Seal TM All SlideAssist
Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses
 Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses This course has been awarded two (2.0) contact hours. This course expires on April 15, 2017. Copyright 2014 by RN.com. All Rights Reserved.
Ergonomics and Safe Patient Handling and Mobility (SPHM) for Nurses This course has been awarded two (2.0) contact hours. This course expires on April 15, 2017. Copyright 2014 by RN.com. All Rights Reserved.
SAFE PATIENT HANDLING RISK ASSESSMENT
 SAFE PATIENT HANDLING RISK ASSESSMENT Swedish Medical Center 2007 This risk assessment consists of two parts: 1) Pre-Site visit forms (Sections 1 & 2): To be completed by facility/unit representative,
SAFE PATIENT HANDLING RISK ASSESSMENT Swedish Medical Center 2007 This risk assessment consists of two parts: 1) Pre-Site visit forms (Sections 1 & 2): To be completed by facility/unit representative,
Chief Executive Office Risk Management Division P.O. Box 1723, Modesto, CA 95354 Phone (209) 525-5710 Fax (209) 525-5779
 Employer: Occupation: Company Contact: Analysis Provided By: Stanislaus County Resident Physician Risk Management 1010 10 th Street Modesto, California 95354 (209) 525-5770 Date: October 2008 Lyle Andersen,
Employer: Occupation: Company Contact: Analysis Provided By: Stanislaus County Resident Physician Risk Management 1010 10 th Street Modesto, California 95354 (209) 525-5770 Date: October 2008 Lyle Andersen,
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Back Safety and Lifting
 Back Safety and Lifting Structure of the Back: Spine The spine is the part of the back that supports the trunk and head. It protects the spinal cord as well as giving flexibility to the body. Vertebrae
Back Safety and Lifting Structure of the Back: Spine The spine is the part of the back that supports the trunk and head. It protects the spinal cord as well as giving flexibility to the body. Vertebrae
MAXI MOVE A MOBILE PASSIVE LIFTER FOR DEMANDING CARE ENVIRONMENTS. ...with people in mind
 MAXI MOVE A MOBILE PASSIVE LIFTER FOR DEMANDING CARE ENVIRONMENTS...with people in mind 2 Maxi Move A PROVEN ASSET FOR ALL CARE ENVIRONMENTS Maxi Move, the most complete mobile lifter system available,
MAXI MOVE A MOBILE PASSIVE LIFTER FOR DEMANDING CARE ENVIRONMENTS...with people in mind 2 Maxi Move A PROVEN ASSET FOR ALL CARE ENVIRONMENTS Maxi Move, the most complete mobile lifter system available,
Welcome to your LOW BACK PAIN treatment guide
 Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Lifting & Moving Patients. Lesson Goal. Lesson Objectives 9/10/2012
 Lifting & Moving Patients Lesson Goal Learn the correct techniques, equipment, & positioning for moving patients safely and effectively in a variety of situations &locations Lesson Objectives Define body
Lifting & Moving Patients Lesson Goal Learn the correct techniques, equipment, & positioning for moving patients safely and effectively in a variety of situations &locations Lesson Objectives Define body
Bulging Disc Back Pain Relief at Home Using Lumbar Traction Techniques.
 Bulging Disc Back Pain Relief at Home Using Lumbar Traction Techniques. A no-nonsense Guide Written By Tommy Hoffman, P.T. 1 Copyright 2009 by Tommy Hoffman All rights reserved under the Pan-American and
Bulging Disc Back Pain Relief at Home Using Lumbar Traction Techniques. A no-nonsense Guide Written By Tommy Hoffman, P.T. 1 Copyright 2009 by Tommy Hoffman All rights reserved under the Pan-American and
Patient s Handbook. Provincial Rehabilitation Unit ONE ISLAND HEALTH SYSTEM ONE ISLAND FUTURE 11HPE41-30364
 Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Patient Capability Assessment Readiness for Transfers and Repositioning
 These guidelines have been formed with the opinion that in healthcare settings, manual lifting should be avoided whenever possible. Therefore, there needs to be a mechanism for licensed healthcare professionals
These guidelines have been formed with the opinion that in healthcare settings, manual lifting should be avoided whenever possible. Therefore, there needs to be a mechanism for licensed healthcare professionals
Lifting, Moving and Positioning Patients From Brady s First Responder (8th Edition) 44 Questions
 Lifting, Moving and Positioning Patients From Brady s First Responder (8th Edition) 44 Questions 1. Approximately how much of the log roll will be complete before the rescuer at the patient's head will
Lifting, Moving and Positioning Patients From Brady s First Responder (8th Edition) 44 Questions 1. Approximately how much of the log roll will be complete before the rescuer at the patient's head will
Moving and Handling Techniques
 Moving and Handling Techniques Introduction Manual handling involves any activity that requires the use of force exerted by a person to lift, lower, push, pull, carry or otherwise move or hold an object.
Moving and Handling Techniques Introduction Manual handling involves any activity that requires the use of force exerted by a person to lift, lower, push, pull, carry or otherwise move or hold an object.
PATIENT HANDLING FOR HEALTHCARE WORKERS
 PATIENT HANDLING FOR HEALTHCARE WORKERS TABLE OF CONTENTS Musculoskeletal Injury Among Health Care Workers:. 1 What Causes Musculoskeletal Injury? 1 Common Back Musculoskeletal Disorders. 1 What are Work
PATIENT HANDLING FOR HEALTHCARE WORKERS TABLE OF CONTENTS Musculoskeletal Injury Among Health Care Workers:. 1 What Causes Musculoskeletal Injury? 1 Common Back Musculoskeletal Disorders. 1 What are Work
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
Ergonomic Evaluation Acute Care Nursing Health Center
 Ergonomic Evaluation Acute Care Nursing Health Center Caroline Hegarty Jamie Rosenberg Rachel Stecker May 1, 2003 Most Injury Inducing Tasks (Owen & Garg, 1990) RESEARCH 1. Chair / toilet transfers 2.
Ergonomic Evaluation Acute Care Nursing Health Center Caroline Hegarty Jamie Rosenberg Rachel Stecker May 1, 2003 Most Injury Inducing Tasks (Owen & Garg, 1990) RESEARCH 1. Chair / toilet transfers 2.
Info. from the nurses of the Medical Service. LOWER BACK PAIN Exercise guide
 Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
JTF 2 Pre-Selection Physical Fitness Testing
 JTF 2 Pre-Selection Physical Fitness Testing 1. General. This evaluation is used to predict a member s physical capability and their readiness to apply for JTF 2. 2. On top of these physical standards,
JTF 2 Pre-Selection Physical Fitness Testing 1. General. This evaluation is used to predict a member s physical capability and their readiness to apply for JTF 2. 2. On top of these physical standards,
Safe Patient Handling Training for Schools of Nursing
 Safe Patient Handling Training for Schools of Nursing Curricular Materials Thomas R. Waters, Ph.D., NIOSH Audrey Nelson, Ph.D., VHA Nancy Hughes, Ph.D., ANA Nancy Menzel, Ph.D., University of Las Vegas,
Safe Patient Handling Training for Schools of Nursing Curricular Materials Thomas R. Waters, Ph.D., NIOSH Audrey Nelson, Ph.D., VHA Nancy Hughes, Ph.D., ANA Nancy Menzel, Ph.D., University of Las Vegas,
Risk Control Bulletin Back Injury Risk Control for Healthcare Facilities
 Risk Control Bulletin Back Injury Risk Control for Healthcare Facilities Occupational back injuries are a major loss exposure in the healthcare industry. Serious back injuries can result when employees
Risk Control Bulletin Back Injury Risk Control for Healthcare Facilities Occupational back injuries are a major loss exposure in the healthcare industry. Serious back injuries can result when employees
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Functional Job Requirements For the Position of Special Education Teacher Department of Education, Training and the Arts Queensland
 Department of Education, Training and the Arts Queensland This document was developed for the following purposes: assisting in the development of rehabilitation programs for injured or ill employees, and
Department of Education, Training and the Arts Queensland This document was developed for the following purposes: assisting in the development of rehabilitation programs for injured or ill employees, and
SEAT BELT Installation Manual
 SEAT BELT Installation Manual You have purchase a premium set of Simpson Seat Belts. They are designed with attention to detail, just like your entire Simpson safety system. WARNING: THIS ARTICLE IS SOLD
SEAT BELT Installation Manual You have purchase a premium set of Simpson Seat Belts. They are designed with attention to detail, just like your entire Simpson safety system. WARNING: THIS ARTICLE IS SOLD
Slings & Accessories. With people in mind
 Slings & Accessories With people in mind Slings & accessories for improved care... ARJO is committed to making patient handling safer and more comfortable for both patient and carer. By eliminating manual
Slings & Accessories With people in mind Slings & accessories for improved care... ARJO is committed to making patient handling safer and more comfortable for both patient and carer. By eliminating manual
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Sling systems from Horcher Quality for your security
 Sling systems from Horcher Quality for your security At a glance. Simple, quick and in brief... Very strong ideal for bathing and dries quickly. -polyester Very durable for everyday use. Latest fabric,
Sling systems from Horcher Quality for your security At a glance. Simple, quick and in brief... Very strong ideal for bathing and dries quickly. -polyester Very durable for everyday use. Latest fabric,
Assisting Students Who Use Wheelchairs:
 Quick-Guide Extra Assisting Students Who Use Wheelchairs: Guidelines for School Personnel Michael F. Giangreco, Irene McEwen, Timothy Fox, and Deborah Lisi-Baker Quick-Guides to Inclusion 3: Ideas for
Quick-Guide Extra Assisting Students Who Use Wheelchairs: Guidelines for School Personnel Michael F. Giangreco, Irene McEwen, Timothy Fox, and Deborah Lisi-Baker Quick-Guides to Inclusion 3: Ideas for
Implementing a Fall Alarm Program to Reduce Fall Risk Rein Tideiksaar, PhD FallPrevent, LLC
 Implementing a Fall Alarm Program to Reduce Fall Risk Rein Tideiksaar, PhD FallPrevent, LLC This program was supported by a grant from Implementing a Fall Alarm Program to Reduce Fall Risk Rein Tideiksaar,
Implementing a Fall Alarm Program to Reduce Fall Risk Rein Tideiksaar, PhD FallPrevent, LLC This program was supported by a grant from Implementing a Fall Alarm Program to Reduce Fall Risk Rein Tideiksaar,
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
MAXI MOVE. with people in mind
 MAXI MOVE A mobile passive lifter for demanding care environments with people in mind 2 Maxi Move A Proven Asset for All Care Environments Maxi Move, the most complete mobile lifter system available, is
MAXI MOVE A mobile passive lifter for demanding care environments with people in mind 2 Maxi Move A Proven Asset for All Care Environments Maxi Move, the most complete mobile lifter system available, is
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
HELPFUL HINTS FOR A HEALTHY BACK
 HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
HELPFUL HINTS FOR A HEALTHY BACK 1. Standing and Walking For correct posture, balance your head above your shoulders, eyes straight ahead, everything else falls into place. Try to point toes straight ahead
CAREGIVER GUIDE. A doctor. He or she authorizes (approves) the rehab discharge.
 Guide for Discharge to Home From Inpatient Rehab Who Is on the Discharge Team? Many people help plan a rehab discharge, and they are often referred to as a team. The team members include: A doctor. He
Guide for Discharge to Home From Inpatient Rehab Who Is on the Discharge Team? Many people help plan a rehab discharge, and they are often referred to as a team. The team members include: A doctor. He
Supporting people to move at home
 Supporting people to move at home Practical tips and techniques for carers and support workers Acknowledgements This brochure is an initiative between Home and Community Health Association and Carers New
Supporting people to move at home Practical tips and techniques for carers and support workers Acknowledgements This brochure is an initiative between Home and Community Health Association and Carers New
The Path to Excellence: How One Facility Received and Maintained a CMS 5 Star Rating
 The Path to Excellence: How One Facility Received and Maintained a CMS 5 Star Rating South Mountain Healthcare and Rehabilitation Center 2385 Springfield Avenue Vauxhall, NJ 07088 Author: Antonio Onday,
The Path to Excellence: How One Facility Received and Maintained a CMS 5 Star Rating South Mountain Healthcare and Rehabilitation Center 2385 Springfield Avenue Vauxhall, NJ 07088 Author: Antonio Onday,
Loss Prevention Reference Note. Adjusting the Computer Workstation. Glare Viewing Distance. Line of Sight Neck Posture Arm Posture Back Posture
 Loss Prevention Reference Note Adjusting the Computer Workstation Line of Sight Neck Posture Arm Posture Back Posture Adjustability Glare Viewing Distance Work Surfaces Mouse Position Leg Space Leg Support
Loss Prevention Reference Note Adjusting the Computer Workstation Line of Sight Neck Posture Arm Posture Back Posture Adjustability Glare Viewing Distance Work Surfaces Mouse Position Leg Space Leg Support
SECTION 9. Mobility, positioning, and transfers. Moving after a stroke 9.1. Fatigue. Loss of sensation. Loss of motor function.
 SECTION 9 Mobility, positioning, and transfers Section overview This section looks at: Moving after a stroke Assisting with mobility Positioning Managing the affected limb Transfers Wheelchair use Walking
SECTION 9 Mobility, positioning, and transfers Section overview This section looks at: Moving after a stroke Assisting with mobility Positioning Managing the affected limb Transfers Wheelchair use Walking
Recovery and Rehabilitation after Stroke
 Recovery and Rehabilitation after Stroke NICK WARD UCL INSTITUTE OF NEUROLOGY QUEEN SQUARE [email protected] Follow us on Twitter @WardLab For more information go to http://www.ucl.ac.uk/ion/departments/sobell/research/nward
Recovery and Rehabilitation after Stroke NICK WARD UCL INSTITUTE OF NEUROLOGY QUEEN SQUARE [email protected] Follow us on Twitter @WardLab For more information go to http://www.ucl.ac.uk/ion/departments/sobell/research/nward
Managing at home with your arm in a polysling following shoulder surgery
 Managing at home with your arm in a polysling following shoulder surgery Exceptional healthcare, personally delivered Contents Page Introduction...04 Restrictions in movement following shoulder surgery...04
Managing at home with your arm in a polysling following shoulder surgery Exceptional healthcare, personally delivered Contents Page Introduction...04 Restrictions in movement following shoulder surgery...04
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Computer Workstation Ergonomic Self Evaluation
 Computer Workstation Ergonomic Self Evaluation Use this guidance to perform a preliminary evaluation of your workstation, and make any adjustments that are necessary to achieve a correct neutral posture.
Computer Workstation Ergonomic Self Evaluation Use this guidance to perform a preliminary evaluation of your workstation, and make any adjustments that are necessary to achieve a correct neutral posture.
IMPORTANT INFORMATION - PLEASE READ. Table of Contents. Introduction. General Information
 IMPORTANT INFORMATION - PLEASE READ Introduction Congratulations! Welcome to the world of the ELLIPTICAL CROSS TRAINER. The ELLIPTICAL CROSS TRAINER is one of the finest and most comprehensive pieces of
IMPORTANT INFORMATION - PLEASE READ Introduction Congratulations! Welcome to the world of the ELLIPTICAL CROSS TRAINER. The ELLIPTICAL CROSS TRAINER is one of the finest and most comprehensive pieces of
Manufactured by: D & K Engineering 15890 Bernardo Center Drive San Diego, CA 92127
 Manufactured by: D & K Engineering 15890 Bernardo Center Drive San Diego, CA 92127 Manufactured for: Bioness Inc 25103 Rye Canyon Loop Valencia, CA 91355 USA Telephone: 800.211.9136 Email: [email protected]
Manufactured by: D & K Engineering 15890 Bernardo Center Drive San Diego, CA 92127 Manufactured for: Bioness Inc 25103 Rye Canyon Loop Valencia, CA 91355 USA Telephone: 800.211.9136 Email: [email protected]
HOSPITALITY RISK FACTORS & BEST PRACTICES - LAUNDRY
 Responsibilities of commercial laundry staff can include washing, drying, steaming, ironing, and chemically treating fabrics for use in hospitals, hotels, and other settings. Laundry can be heavy, treated
Responsibilities of commercial laundry staff can include washing, drying, steaming, ironing, and chemically treating fabrics for use in hospitals, hotels, and other settings. Laundry can be heavy, treated
EMPLOYEE FALL PROTECTION
 EMPLOYEE FALL PROTECTION You can fall from any height and be seriously injured or killed. In the construction industry, as well as any other industry, when falls from heights happen, they are usually very
EMPLOYEE FALL PROTECTION You can fall from any height and be seriously injured or killed. In the construction industry, as well as any other industry, when falls from heights happen, they are usually very
Ergonomic Workplace Evaluation ISE 210, Human Factors and Ergonomics San Jose State University Fall 2003
 Ergonomic Workplace Evaluation ISE 210, Human Factors and Ergonomics San Jose State University Fall 2003 Robert Murphy Table of Contents Introduction... 2 Task... 2 Equipment... 4 Workers... 5 Observations
Ergonomic Workplace Evaluation ISE 210, Human Factors and Ergonomics San Jose State University Fall 2003 Robert Murphy Table of Contents Introduction... 2 Task... 2 Equipment... 4 Workers... 5 Observations
HOPE EXERCISE RECOVERY RESOURCES RELATIONSHIPS INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RELATIONSHIPS MOVEMENT. A Stroke Recovery Guide
 INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION C 04/26/2015. Statement of Licensure Violations:
 (X1) PROVER/SUPPLIER/LIA ENTIFIATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) REGULATORY OR LS ENTIFYING INFORMATION) Final Observations Statement of Licensure Violations: 300.610a) 300.1210b)
(X1) PROVER/SUPPLIER/LIA ENTIFIATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) REGULATORY OR LS ENTIFYING INFORMATION) Final Observations Statement of Licensure Violations: 300.610a) 300.1210b)
Catholic Mutual..."CARES"
 Catholic Mutual..."CARES" BACK INJURY LOSS CONTROL FOR HEALTH CARE FACILITIES Occupational back injuries are a major loss exposure in the health care industry. Serious back injuries can result when employees
Catholic Mutual..."CARES" BACK INJURY LOSS CONTROL FOR HEALTH CARE FACILITIES Occupational back injuries are a major loss exposure in the health care industry. Serious back injuries can result when employees
For Deep Pressure Massage
 T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
Texas Department of Insurance. Office Ergonomics. Provided by. Division of Workers Compensation HS03-003C (03-09)
 Texas Department of Insurance Office Ergonomics Provided by Division of Workers Compensation HS03-003C (03-09) Contents Introduction 1 The Ergonomic Checklist 1 Sharp Edge Hazards 1 Equipment Adjustability
Texas Department of Insurance Office Ergonomics Provided by Division of Workers Compensation HS03-003C (03-09) Contents Introduction 1 The Ergonomic Checklist 1 Sharp Edge Hazards 1 Equipment Adjustability
Do s and Don ts with Low Back Pain
 Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
SHOULDER REHABILITATION EXERCISE PROGRAM. Phase I
 Franklin Orthopedics 7400 W Rawson Ave, Suite 225 Franklin, WI 53132 414-425-8232 SHOULDER REHABILITATION EXERCISE PROGRAM Phase I PENDULUM EXERCISES: Bending over at the waist and balancing with the good
Franklin Orthopedics 7400 W Rawson Ave, Suite 225 Franklin, WI 53132 414-425-8232 SHOULDER REHABILITATION EXERCISE PROGRAM Phase I PENDULUM EXERCISES: Bending over at the waist and balancing with the good
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
HealthStream Regulatory Script
 HealthStream Regulatory Script Back Safety Version: May 2007 Lesson 1: Introduction Lesson 2: Back Injury Lesson 3: Spinal Anatomy and Physiology Lesson 4: Safe Operation of the Spine Lesson 5: Preventive
HealthStream Regulatory Script Back Safety Version: May 2007 Lesson 1: Introduction Lesson 2: Back Injury Lesson 3: Spinal Anatomy and Physiology Lesson 4: Safe Operation of the Spine Lesson 5: Preventive
