The Women s Health Initiative: The Role of Hormonal Therapy in Disease Prevention
|
|
|
- Charity York
- 8 years ago
- Views:
Transcription
1 The Women s Health Initiative: The Role of Hormonal Therapy in Disease Prevention Robert B. Wallace, MD, MSc Departments of Epidemiology and Internal Medicine University of Iowa College of Public Health Iowa City, IA The Women s Health Initiative (WHI) clinical trials on hormone therapy (HT) in postmenopausal women have changed clinical thinking on estrogen therapy in substantial ways, and have clarified clinical guidelines on disease prevention in post-menopausal women. These trials (1,2,3), along with the HERS Trial (4), a secondary prevention trial of HT and coronary artery disease, have been to date the only randomized, double-blind trials of estrogen therapy with sufficient statistical power to explore a broad range of important disease outcomes in post-menopausal women. WHI HT findings have been widely discussed and at times controversial (5), perhaps in part because their findings have been inconsistent with established clinical lore and practice, particularly with respect to the impact of HT on atherosclerotic diseases. Also, WHI findings also caused some reconsideration of basis research programs predicated on the notion that HT was cardio- and neuro-protective in animal models. However, WHI methods and findings have stood up to substantial scrutiny and have in my view become the standard for complex, long-term trials of hormonal intervention in older women. WHI comprised two HT trials: estrogen plus progestin (Prempro ) for women with an intact uterus (E+P); and estrogen alone (E-alone) (Premarin ) for women with prior hysterectomy. They were not intended to explore treatment of menopausal symptoms.
2 Rather, they addressed the value of long-term HT in the prevention of major chronic conditions of women after menopause. The primary outcomes were all-cause mortality, coronary mortality and several major conditions: coronary disease, stroke, breast cancer, hip and other fractures, pulmonary embolism and colo-rectal cancer. As well, there was a global index of these disease outcomes (2). In execution and interpretation, the WHI HT trials were complex, with too much detail for this presentation. Basic WHI HT trial findings are briefly summarized in the table. Major outcomes, primary and secondary, were defined before trial initiation. An ancillary study of dementia outcomes [WHIMS: the WHI Memory Study (6,7)] began within two years of study onset. In general, the findings were similar across the age spectrum under study (50-79 years at entry), although there was some variation. As the table shows, some conditions were increased by HT, and others were decreased. Neither intervention had an impact on total mortality. Coronary disease, breast cancer and pulmonary embolism rates were significantly increased by E+P, but this was not seen with E-alone. Both interventions caused an increase in stroke rates and a decrease in hip fracture rates. E+P caused a decrease in colon cancer rates, but this was not seen with E-alone. Dementia rates were increased with E+P; a similar trend was seen with E-alone, but it was not statistically significant. There was a significant overall increase in dementia outcome rates when the findings from both trials were combined. When there were differential effects between E +P and E-alone, it has been suggested that the progestin (medroxyprogesterone acetate) may be responsible for some of these
3 differences. This may be correct, but the issue will require further study, particularly since the two trial populations were dissimilar in some respects. For example, the E-alone participants had a higher mean body mass index and more years of prior exposure to HT than E + P participants, so interpretation of trial differences must be cautious. Many of the findings were consistent with prior observational epidemiologic studies, with the most important exception being the cardio-vascular outcomes. Also of note, in the E+P trial after one year, there very few differences between intervention and placebo groups in a variety of quality-of-life measures (8), suggesting that in this population there were no important effects in the variety of physical and behavioral domains studied. The WHI has made critically important contributions to our knowledge of disease prevention in post-menopausal women, and has challenged current clinical practice and prevention policies. Given that some types of HT will likely cause some excess morbidity, a particular problem emerges in the treatment of menopausal symptoms, since few other effective treatments exist. Also, many women seek advice on the value of HT at the time of menopause, and provision of counseling is now more complex. Perhaps most importantly, WHI has hopefully changed the decision process related to HT use at the time of menopause, and refocused attention on a very important issue: the best regimen for disease prevention in the patient s next thirty years of life. The U.S. Preventive Services Task Force has recommended against HT for chronic disease prevention in post-menopausal women (9), reinforcing the need for an overall prevention focus.
4 More detailed analyses of WHI HT findings will be forthcoming. Additionally, two other WHI trials are not yet complete: long-term interventions with calcium/vitamin D, and low fat diet. The WHI will continue to help guide our clinical preventive strategies and policies for several years to come. Keywords: women s health, estrogen, progestin, hormone therapy, chronic disease
5 Summary of Findings from the Women s Health Initiative Hormone Therapy Trials Intervention Trial Clinical Outcome E + P E Alone All-cause mortality 0 0 Coronary Heart Disease + 0 Stroke + + Breast cancer + 0 Hip fracture - - Colo-rectal cancer - 0 Pulmonary embolism + 0 Global Index ~ + 0 Dementia = no significant change compared with placebo + = statistically significantly higher rates in the hormone intervention group versus placebo - = statistically significant lower rates in the hormone intervention group versus placebo ~ = global index consisting of cumulative events including non-fatal myocardial infarction and CHD death, stroke, pulmonary embolism, invasive breast cancer, hip fracture, colo-rectal cancer, endometrial cancer and death due to other causes.
6 References 1. Women's Health Initiative Study Group. Design of the Women's Health Initiative clinical trial and observational study. The Control Clin Trials. 1998;19: Writing Group for the Women's Health Initiative Investigators. Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results from the Women's Health Initiative randomized controlled trial. JAMA. 2002;288: Women's Health Initiative Steering Committee. Effects of conjugated equine estrogen in postmenopausal women with hysterectomy: the Women's Health Initiative randomized controlled trial. JAMA. 2004;291: Grady D. Herrington D. Bittner V. Blumenthal R. et al. HERS Research Group. Cardiovascular disease outcomes during 6.8 years of hormone therapy: Heart and Estrogen/progestin Replacement Study follow-up (HERS II). JAMA. 2002;288: Goldman JA. The Women s Health Initiative 2004 Review and Critique. Medscape Ob/Gyn & Women s Health. 2004;6(3). 6. Shumaker SA. Legault C. Rapp SR. et al. WHIMS Investigators. Estrogen plus progestin and the incidence of dementia and mild cognitive impairment in postmenopausal women: the Women's Health Initiative Memory Study: a randomized controlled trial. JAMA. 2003;289: Shumaker SA. Legault C. Kuller L. et al. Conjugated equine estrogens and incidence of probable dementia and mild cognitive impairment in postmenopausal women: Women's Health Initiative Memory Study. JAMA. 2004;291: Hays J. Ockene JK. Brunner RL. et al. Women's Health Initiative Investigators. Effects of estrogen plus progestin on health-related quality of life. N Engl J Med. 2003;348: U. S. Preventive Services Task Force. Chemoprevention for hormone replacement therapy. (Release Date: 2002)
7 [Dr. Wallace is the site principal investigator for the Women s Health Initiative at the University of Iowa. The opinions are solely those of the author and not the Women s Health Initiative investigators, the National Institutes of Health, the American College of Preventive Medicine or any other organization or association]
The WHI 12 Years Later: What Have We Learned about Postmenopausal HRT?
 AACE 23 rd Annual Scientific and Clinical Congress (2014) Syllabus Materials: The WHI 12 Years Later: What Have We Learned about Postmenopausal HRT? JoAnn E. Manson, MD, DrPH, FACP, FACE Chief, Division
AACE 23 rd Annual Scientific and Clinical Congress (2014) Syllabus Materials: The WHI 12 Years Later: What Have We Learned about Postmenopausal HRT? JoAnn E. Manson, MD, DrPH, FACP, FACE Chief, Division
The Women s Health Initiative where are we a decade later?
 The Women s Health Initiative where are we a decade later? Henry G. Burger MIMR-PHI Institute & Jean Hailes for Women s Health, Melbourne, Australia Disclosures: Henry Burger Sources of Funding Pharmaceutical
The Women s Health Initiative where are we a decade later? Henry G. Burger MIMR-PHI Institute & Jean Hailes for Women s Health, Melbourne, Australia Disclosures: Henry Burger Sources of Funding Pharmaceutical
(212) 733-2324 mackay.jimeson@pfizer.com
 For immediate release: July 9, 2012 Media Contacts: MacKay Jimeson (212) 733-2324 mackay.jimeson@pfizer.com Pfizer Recognizes 10 th Anniversary Of The Women s Health Initiative: A Modern Day Perspective
For immediate release: July 9, 2012 Media Contacts: MacKay Jimeson (212) 733-2324 mackay.jimeson@pfizer.com Pfizer Recognizes 10 th Anniversary Of The Women s Health Initiative: A Modern Day Perspective
Hormone therapy and breast cancer: conflicting evidence. Cindy Farquhar Cochrane Menstrual Disorders and Subfertility Group
 Hormone therapy and breast cancer: conflicting evidence Cindy Farquhar Cochrane Menstrual Disorders and Subfertility Group The world of hormone therapy in the 1990 s Throughout the 1970s, 1980s and 1990s
Hormone therapy and breast cancer: conflicting evidence Cindy Farquhar Cochrane Menstrual Disorders and Subfertility Group The world of hormone therapy in the 1990 s Throughout the 1970s, 1980s and 1990s
Hormone Replacement Therapy : The New Debate. Susan T. Hingle, M.D.
 Hormone Replacement Therapy : The New Debate Susan T. Hingle, M.D. Background Hormone replacement therapy (HRT) is extensively used in the United States, especially for: *treatment of menopausal symptoms
Hormone Replacement Therapy : The New Debate Susan T. Hingle, M.D. Background Hormone replacement therapy (HRT) is extensively used in the United States, especially for: *treatment of menopausal symptoms
Neal Rouzier responds to the JAMA article on Men and Testosterone
 Neal Rouzier responds to the JAMA article on Men and Testosterone On the first day the JAMA article was released I received 500 emails from physicians and patients requesting my opinion of the article
Neal Rouzier responds to the JAMA article on Men and Testosterone On the first day the JAMA article was released I received 500 emails from physicians and patients requesting my opinion of the article
Randomized trials versus observational studies
 Randomized trials versus observational studies The case of postmenopausal hormone therapy and heart disease Miguel Hernán Harvard School of Public Health www.hsph.harvard.edu/causal Joint work with James
Randomized trials versus observational studies The case of postmenopausal hormone therapy and heart disease Miguel Hernán Harvard School of Public Health www.hsph.harvard.edu/causal Joint work with James
ABSTRACT. Home Current Issue All Issues Online First Specialties & Topics CME Multimedia Quizzes For Authors Subscribe
 SIGN IN (Create a Free Personal Account) Journals > Specialties & Topics Store Physician Jobs About Mobile Search The JAMA Network Search JAMA Advanced Search Home Current Issue All Issues Online First
SIGN IN (Create a Free Personal Account) Journals > Specialties & Topics Store Physician Jobs About Mobile Search The JAMA Network Search JAMA Advanced Search Home Current Issue All Issues Online First
How To Know The Risks And Benefits Of Estrogen Plus Progestin
 ORIGINAL CONTRIBUTION JAMA-EXPRESS Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women Principal Results From the Women s Health Initiative Randomized Controlled Trial Writing
ORIGINAL CONTRIBUTION JAMA-EXPRESS Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women Principal Results From the Women s Health Initiative Randomized Controlled Trial Writing
Use of Hormone Replacement Therapy in the Asymptomatic Postmenopausal Woman: What is the Current Evidence?
 CPD Paper 5 605 Use of Hormone Replacement Therapy in the Asymptomatic Postmenopausal Woman: What is the Current Evidence? F H Loh,*FAMS, MRCOG (Lond), M Med (O & G) Abstract The publication of the Women
CPD Paper 5 605 Use of Hormone Replacement Therapy in the Asymptomatic Postmenopausal Woman: What is the Current Evidence? F H Loh,*FAMS, MRCOG (Lond), M Med (O & G) Abstract The publication of the Women
Case Study 11: Hormone Replacement Therapy
 Case Study 11: Hormone Replacement Therapy October 2000 Scenario Ann McDonnald is a successful 55 year old business executive She starts her first consult with you by saying I m getting hot flushes It
Case Study 11: Hormone Replacement Therapy October 2000 Scenario Ann McDonnald is a successful 55 year old business executive She starts her first consult with you by saying I m getting hot flushes It
Hormone Restoration: Is It Right for You? Patricia A. Stafford, M.D. Founder, Wellness ReSolutions
 Hormone Restoration: Is It Right for You? Patricia A. Stafford, M.D. Founder, Wellness ReSolutions IMPORTANCE OF HORMONE BALANCE Importance of Hormone Balance Help you live a long, healthy life Help you
Hormone Restoration: Is It Right for You? Patricia A. Stafford, M.D. Founder, Wellness ReSolutions IMPORTANCE OF HORMONE BALANCE Importance of Hormone Balance Help you live a long, healthy life Help you
Endocrinology & Women s Health + Adult Immunizations Exotic Asia CME Cruise June 15 24, 2015. Menopause & Osteoporosis update 2015.
 Menopause and Osteoporosis Update 2015 Post WHI-Update CCFP, MHSc, FRCP,FCFP,, NAMS Accredited Menopause Expert Associate Professor University of Toronto www.seacourses.com 1 Canadian Population Pyramid:
Menopause and Osteoporosis Update 2015 Post WHI-Update CCFP, MHSc, FRCP,FCFP,, NAMS Accredited Menopause Expert Associate Professor University of Toronto www.seacourses.com 1 Canadian Population Pyramid:
Promoting the Fountain of Youth: Low-T and Estrogen Deficiency
 Promoting the Fountain of Youth: Low-T and Estrogen Deficiency Adriane Fugh-Berman MD Georgetown University Medical Center ajf29@georgetown.edu Hormone Therapy in Women Animal glandulars became popular
Promoting the Fountain of Youth: Low-T and Estrogen Deficiency Adriane Fugh-Berman MD Georgetown University Medical Center ajf29@georgetown.edu Hormone Therapy in Women Animal glandulars became popular
February 1, 2014 RESTORING STRENGTH AND VITALITY THROUGH HORMONES FACTS, FANTASIES, POSSIBILITIES, AND PITFALLS
 February 1, 2014 RESTORING STRENGTH AND VITALITY THROUGH HORMONES FACTS, FANTASIES, POSSIBILITIES, AND PITFALLS Calvin Hirsch, MD Professor of Clinical Internal Medicine (Geriatrics) UC Davis School of
February 1, 2014 RESTORING STRENGTH AND VITALITY THROUGH HORMONES FACTS, FANTASIES, POSSIBILITIES, AND PITFALLS Calvin Hirsch, MD Professor of Clinical Internal Medicine (Geriatrics) UC Davis School of
The Women s Health Initiative (WHI) Clinical Trial of Estrogen plus Progestin in Postmenopausal Women
 The Women s Health Initiative (WHI) Clinical Trial of Estrogen plus Progestin in Postmenopausal Women Funded by the National Heart, Lung, and Blood Institute Bethesda, Maryland Conducted by 40 Clinical
The Women s Health Initiative (WHI) Clinical Trial of Estrogen plus Progestin in Postmenopausal Women Funded by the National Heart, Lung, and Blood Institute Bethesda, Maryland Conducted by 40 Clinical
Health risks and benefits from calcium and vitamin D supplementation: Women's Health Initiative clinical trial and cohort study
 DOI 10.1007/s00198-012-2224-2 ORIGINAL ARTICLE Health risks and benefits from calcium and vitamin D supplementation: Women's Health Initiative clinical trial and cohort study R. L. Prentice & M. B. Pettinger
DOI 10.1007/s00198-012-2224-2 ORIGINAL ARTICLE Health risks and benefits from calcium and vitamin D supplementation: Women's Health Initiative clinical trial and cohort study R. L. Prentice & M. B. Pettinger
The menopausal transition usually has three parts:
 The menopausal transition usually has three parts: Perimenopause begins several years before a woman s last menstrual period, when the ovaries gradually produce less estrogen. In the last 1-2 years of
The menopausal transition usually has three parts: Perimenopause begins several years before a woman s last menstrual period, when the ovaries gradually produce less estrogen. In the last 1-2 years of
PROVERA (medroxyprogesterone acetate) Product Monograph Page 34 of 38
 PART III: CONSUMER INFORMATION PR PROVERA* (medroxyprogesterone acetate) This leaflet is part III of a three-part "Product Monograph" published when PROVERA was approved for sale in Canada and is designed
PART III: CONSUMER INFORMATION PR PROVERA* (medroxyprogesterone acetate) This leaflet is part III of a three-part "Product Monograph" published when PROVERA was approved for sale in Canada and is designed
Hormones and cardiovascular disease, what the Danish Nurse Cohort learned us
 Hormones and cardiovascular disease, what the Danish Nurse Cohort learned us Ellen Løkkegaard, Clinical Associate Professor, Ph.d. Dept. Obstetrics and Gynecology. Hillerød Hospital, University of Copenhagen
Hormones and cardiovascular disease, what the Danish Nurse Cohort learned us Ellen Løkkegaard, Clinical Associate Professor, Ph.d. Dept. Obstetrics and Gynecology. Hillerød Hospital, University of Copenhagen
Getting Started: The Anatomy and Physiology of Clinical Research
 Getting Started: The Anatomy and Physiology of Clinical Research Stephen B. Hulley, Thomas B. Newman, and Steven R. Cummings This chapter introduces clinical research from two viewpoints, setting up themes
Getting Started: The Anatomy and Physiology of Clinical Research Stephen B. Hulley, Thomas B. Newman, and Steven R. Cummings This chapter introduces clinical research from two viewpoints, setting up themes
What is an Evidence-Based, Value-Based Health Care System? (Part 1)
 Evidence-Based Medicine What is an Evidence-Based, Value-Based Health Care System? (Part 1) By Sheri Strite and Michael E. Stuart, MD IN THIS ARTICLE The two biggest issues facing health care organizations
Evidence-Based Medicine What is an Evidence-Based, Value-Based Health Care System? (Part 1) By Sheri Strite and Michael E. Stuart, MD IN THIS ARTICLE The two biggest issues facing health care organizations
PROMISE & PITFALLS OF OUTCOMES RESEARCH USING EMR DATABASES. Richard L. Tannen, M.D., Mark Weiner, Dawei Xie
 PROMISE & PITFALLS OF OUTCOMES RESEARCH USING EMR DATABASES Richard L. Tannen, M.D., Mark Weiner, Dawei Xie GOALS OF STUDY Determine Whether Studies Using EMR Database Yield Valid Outcome Assessment Major
PROMISE & PITFALLS OF OUTCOMES RESEARCH USING EMR DATABASES Richard L. Tannen, M.D., Mark Weiner, Dawei Xie GOALS OF STUDY Determine Whether Studies Using EMR Database Yield Valid Outcome Assessment Major
Hormone replacement therapy:
 www.bpac.org.nz keyword: hrt Hormone replacement therapy: latest evidence and treatment recommendations Key advisor: Dr Helen Roberts, Senior Lecturer, Department of Obstetrics and Gynaecology, Faculty
www.bpac.org.nz keyword: hrt Hormone replacement therapy: latest evidence and treatment recommendations Key advisor: Dr Helen Roberts, Senior Lecturer, Department of Obstetrics and Gynaecology, Faculty
New Cholesterol Guidelines: Carte Blanche for Statin Overuse Rita F. Redberg, MD, MSc Professor of Medicine
 New Cholesterol Guidelines: Carte Blanche for Statin Overuse Rita F. Redberg, MD, MSc Professor of Medicine Disclosures & Relevant Relationships I have nothing to disclose No financial conflicts Editor,
New Cholesterol Guidelines: Carte Blanche for Statin Overuse Rita F. Redberg, MD, MSc Professor of Medicine Disclosures & Relevant Relationships I have nothing to disclose No financial conflicts Editor,
With Big Data Comes Big Responsibility
 With Big Data Comes Big Responsibility Using health care data to emulate randomized trials when randomized trials are not available Miguel A. Hernán Departments of Epidemiology and Biostatistics Harvard
With Big Data Comes Big Responsibility Using health care data to emulate randomized trials when randomized trials are not available Miguel A. Hernán Departments of Epidemiology and Biostatistics Harvard
POSTMENOPAUSAL ESTROGEN REPLACEMENT THERAPY
 POSTMENOPAUSAL ESTROGEN REPLACEMENT THERAPY Dorie W. Schwertz, PhD (2/01) University of Illinois at Chicago Hormone Replacement Therapy (HRT) and Estrogen Replacement Therapy (ERT) Menopause - loss of
POSTMENOPAUSAL ESTROGEN REPLACEMENT THERAPY Dorie W. Schwertz, PhD (2/01) University of Illinois at Chicago Hormone Replacement Therapy (HRT) and Estrogen Replacement Therapy (ERT) Menopause - loss of
Randomised trials on the long-term effects of hormone replacement therapy: Criticism of Women s Health Initiative Study
 HIPPOKRATIA 2002, 6, 2: 51-56 HIPPOKRATIA 2002, 6, 2 51 EDITORIAL COMMENTS Randomised trials on the long-term effects of hormone replacement therapy: Criticism of Women s Health Initiative Study Panidis
HIPPOKRATIA 2002, 6, 2: 51-56 HIPPOKRATIA 2002, 6, 2 51 EDITORIAL COMMENTS Randomised trials on the long-term effects of hormone replacement therapy: Criticism of Women s Health Initiative Study Panidis
Case studies of bias in real life epidemiologic studies. Bias File 1. The Rise and Fall of Hormone Replacement Therapy
 Case studies of bias in real life epidemiologic studies Bias File 1. The Rise and Fall of Hormone Replacement Therapy Compiled by Madhukar Pai, MD, PhD Jay S Kaufman, PhD Department of Epidemiology, Biostatistics
Case studies of bias in real life epidemiologic studies Bias File 1. The Rise and Fall of Hormone Replacement Therapy Compiled by Madhukar Pai, MD, PhD Jay S Kaufman, PhD Department of Epidemiology, Biostatistics
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes
 Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
Guidance for Industry Diabetes Mellitus Evaluating Cardiovascular Risk in New Antidiabetic Therapies to Treat Type 2 Diabetes U.S. Department of Health and Human Services Food and Drug Administration Center
Hormone Replacement Therapy (HRT) a is the term used for the. Hormone Replacement Therapy: Real Concerns and False Alarms REVIEW ARTICLE
 REVIEW ARTICLE Hormone Replacement Therapy: Real Concerns and False Alarms Avrum Z. Bluming, MD, and Carol Tavris, PhD Abstract: From 2002 to 2008, reports from the Women s Health Initiative (WHI) claimed
REVIEW ARTICLE Hormone Replacement Therapy: Real Concerns and False Alarms Avrum Z. Bluming, MD, and Carol Tavris, PhD Abstract: From 2002 to 2008, reports from the Women s Health Initiative (WHI) claimed
Medications to Prevent and Treat Osteoporosis
 Medications to Prevent and Treat Osteoporosis National Institutes of Health Osteoporosis and Related Bone Diseases ~ National Resource Center 2 AMS Circle Bethesda, MD 20892-3676 Tel: (800) 624-BONE or
Medications to Prevent and Treat Osteoporosis National Institutes of Health Osteoporosis and Related Bone Diseases ~ National Resource Center 2 AMS Circle Bethesda, MD 20892-3676 Tel: (800) 624-BONE or
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group
 Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Komorbide brystkræftpatienter kan de tåle behandling? Et registerstudie baseret på Danish Breast Cancer Cooperative Group Lotte Holm Land MD, ph.d. Onkologisk Afd. R. OUH Kræft og komorbiditet - alle skal
Not All Clinical Trials Are Created Equal Understanding the Different Phases
 Not All Clinical Trials Are Created Equal Understanding the Different Phases This chapter will help you understand the differences between the various clinical trial phases and how these differences impact
Not All Clinical Trials Are Created Equal Understanding the Different Phases This chapter will help you understand the differences between the various clinical trial phases and how these differences impact
Chapter 6. Conclusions
 Chapter 6 Conclusions Contents Page DETERMINING THE RELATIONSHIP BETWEEN THE MENOPAUSE AND DISEASES OF AGING....*.*...**...,..****,...*.**.* 101 RANDOMIZED CLINICAL TRIALS ARE NEEDED..............................
Chapter 6 Conclusions Contents Page DETERMINING THE RELATIONSHIP BETWEEN THE MENOPAUSE AND DISEASES OF AGING....*.*...**...,..****,...*.**.* 101 RANDOMIZED CLINICAL TRIALS ARE NEEDED..............................
Dr. Friedman s Guide to Estrogen Replacement
 Dr. Friedman s Guide to Estrogen Replacement There are risks and benefits with all medicines and estrogen replacement is no exception. In fact, estrogen replacement is one of the most controversial topics
Dr. Friedman s Guide to Estrogen Replacement There are risks and benefits with all medicines and estrogen replacement is no exception. In fact, estrogen replacement is one of the most controversial topics
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results
 Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Systolic Blood Pressure Intervention Trial (SPRINT) Principal Results Paul K. Whelton, MB, MD, MSc Chair, SPRINT Steering Committee Tulane University School of Public Health and Tropical Medicine, and
Main Effect of Screening for Coronary Artery Disease Using CT
 Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Main Effect of Screening for Coronary Artery Disease Using CT Angiography on Mortality and Cardiac Events in High risk Patients with Diabetes: The FACTOR-64 Randomized Clinical Trial Joseph B. Muhlestein,
Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial
 Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial Connie N. Hess, MD, MHS, Stefan James, MD, PhD, Renato D. Lopes, MD, PhD, Daniel M. Wojdyla,
Apixaban Plus Mono vs. Dual Antiplatelet Therapy in Acute Coronary Syndromes: Insights from the APPRAISE-2 Trial Connie N. Hess, MD, MHS, Stefan James, MD, PhD, Renato D. Lopes, MD, PhD, Daniel M. Wojdyla,
The benefits of oestrogen following menopause: why hormone replacement therapy should be offered to postmenopausal women
 The benefits of oestrogen following menopause: why hormone replacement therapy should be offered to postmenopausal women Barry G Wren For over 70 years, women have used oestrogen-based hormone replacement
The benefits of oestrogen following menopause: why hormone replacement therapy should be offered to postmenopausal women Barry G Wren For over 70 years, women have used oestrogen-based hormone replacement
Menopause Guidance on management and prescribing HRT for GPs based on NICE guidance 2015
 PRIMARY CARE WOMEN S HEALTH FORUM GUIDELINES Menopause Guidance on management and prescribing HRT for GPs based on NICE guidance 2015 Written by Dr Imogen Shaw This guidance is designed to support you
PRIMARY CARE WOMEN S HEALTH FORUM GUIDELINES Menopause Guidance on management and prescribing HRT for GPs based on NICE guidance 2015 Written by Dr Imogen Shaw This guidance is designed to support you
ECONOMIC COSTS OF PHYSICAL INACTIVITY
 ECONOMIC COSTS OF PHYSICAL INACTIVITY This fact sheet highlights the prevalence and health-consequences of physical inactivity and summarises some of the key facts and figures on the economic costs of
ECONOMIC COSTS OF PHYSICAL INACTIVITY This fact sheet highlights the prevalence and health-consequences of physical inactivity and summarises some of the key facts and figures on the economic costs of
Hôpitaux Universitaires de Genève Lipides, métabolisme des hydrates de carbonne et maladies cardio-vasculaires
 Hôpitaux Universitaires de Genève Lipides, métabolisme des hydrates de carbonne et maladies cardio-vasculaires Prof. J. Philippe Effect of estrogens on glucose metabolism : Fasting Glucose, HbA1c and C-Peptide
Hôpitaux Universitaires de Genève Lipides, métabolisme des hydrates de carbonne et maladies cardio-vasculaires Prof. J. Philippe Effect of estrogens on glucose metabolism : Fasting Glucose, HbA1c and C-Peptide
Statins and Risk for Diabetes Mellitus. Background
 Statins and Risk for Diabetes Mellitus Kevin C. Maki, PhD, FNLA Midwest Center for Metabolic & Cardiovascular Research and DePaul University, Chicago, IL 1 Background In 2012 the US Food and Drug Administration
Statins and Risk for Diabetes Mellitus Kevin C. Maki, PhD, FNLA Midwest Center for Metabolic & Cardiovascular Research and DePaul University, Chicago, IL 1 Background In 2012 the US Food and Drug Administration
LIVING WATERS MEDICAL SPA AND WELLNESS CENTER
 November 2014 LIVING WATERS MEDICAL SPA AND WELLNESS CENTER Contents Benefits and Risks of Hormone Replacement 1-3 Liposuction Pictures 4-6 Remember to get your Botox before Christmas! Menopause and male
November 2014 LIVING WATERS MEDICAL SPA AND WELLNESS CENTER Contents Benefits and Risks of Hormone Replacement 1-3 Liposuction Pictures 4-6 Remember to get your Botox before Christmas! Menopause and male
Observational studies, clinical trials, and the women s health initiative
 Lifetime Data Anal (2007) 13:449 462 DOI 10.1007/s10985-007-9047-z Observational studies, clinical trials, and the women s health initiative Ross L. Prentice Received: 5 July 2007 / Accepted: 16 July 2007
Lifetime Data Anal (2007) 13:449 462 DOI 10.1007/s10985-007-9047-z Observational studies, clinical trials, and the women s health initiative Ross L. Prentice Received: 5 July 2007 / Accepted: 16 July 2007
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 13 October 2005 Doc. Ref. EMEA/CHMP/021/97 Rev. 1 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE
European Medicines Agency Pre-authorisation Evaluation of Medicines for Human Use London, 13 October 2005 Doc. Ref. EMEA/CHMP/021/97 Rev. 1 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE
How To Know The Benefits And Risks Of Hormone Therapy
 Menopause: The Journal of The North American Menopause Society Vol. 19, No. 3, pp. 257/271 DOI: 10.1097/gme.0b013e31824b970a * 2012 by The North American Menopause Society POSITION STATEMENT The 2012 Hormone
Menopause: The Journal of The North American Menopause Society Vol. 19, No. 3, pp. 257/271 DOI: 10.1097/gme.0b013e31824b970a * 2012 by The North American Menopause Society POSITION STATEMENT The 2012 Hormone
ABOUT XARELTO CLINICAL STUDIES
 ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
ABOUT XARELTO CLINICAL STUDIES FAST FACTS Xarelto (rivaroxaban) is a novel, oral direct Factor Xa inhibitor. On September 30, 2008, the European Commission granted marketing approval for Xarelto for the
Obesity and the Menopause. Vanessa M. Barnabei, MD, PhD Professor and Chair Department of Obstetrics and Gynecology
 Obesity and the Menopause Vanessa M. Barnabei, MD, PhD Professor and Chair Department of Obstetrics and Gynecology Educational Objectives Review normal menopausal transition Review health risks of obesity
Obesity and the Menopause Vanessa M. Barnabei, MD, PhD Professor and Chair Department of Obstetrics and Gynecology Educational Objectives Review normal menopausal transition Review health risks of obesity
NHS outcomes framework and CCG outcomes indicators: Data availability table
 NHS outcomes framework and CCG outcomes indicators: Data availability table December 2012 NHS OF objectives Preventing people from dying prematurely DOMAIN 1: preventing people from dying prematurely Potential
NHS outcomes framework and CCG outcomes indicators: Data availability table December 2012 NHS OF objectives Preventing people from dying prematurely DOMAIN 1: preventing people from dying prematurely Potential
Success factors in Behavioral Medicine
 Success factors in Behavioral Medicine interventions post myocardial infarction Depression Gunilla post myocardial Burell, PhD infarction Department of Public Health, Uppsala University, Sweden XIII Svenska
Success factors in Behavioral Medicine interventions post myocardial infarction Depression Gunilla post myocardial Burell, PhD infarction Department of Public Health, Uppsala University, Sweden XIII Svenska
University of Ulsan College of Medicine, Asan Medical Center on behalf of the REAL-LATE and the ZEST-LATE trial
 Duration of Dual Antiplatelet Therapy After Drug-Eluting Stent Implantation A Pooled Analysis of the REAL-LATE and the ZEST-LATE Trial Seung-Jung Park MD PhD Seung-Jung Park, MD, PhD, University of Ulsan
Duration of Dual Antiplatelet Therapy After Drug-Eluting Stent Implantation A Pooled Analysis of the REAL-LATE and the ZEST-LATE Trial Seung-Jung Park MD PhD Seung-Jung Park, MD, PhD, University of Ulsan
BMC Med 7/19/2007; Simvastatin linked to reduced incidence of dementia, Parkinson s disease.
 March 3, 2012 BD Response to FDA statement regarding Statins The Food and Drug Administration announced on Tuesday (February 28, 2012) the changes to the safety information on the labels of statins regarding
March 3, 2012 BD Response to FDA statement regarding Statins The Food and Drug Administration announced on Tuesday (February 28, 2012) the changes to the safety information on the labels of statins regarding
Prevention of stroke and systemic embolism in adult patients with non-valvular atrial fibrillation (AF) with one or more risk factors
 News Release For use outside the US and UK only Bayer Pharma AG 13342 Berlin Germany Tel. +49 30 468-1111 www.bayerpharma.com Bayer s Xarelto Approved in the EU for the Prevention of Stroke in Patients
News Release For use outside the US and UK only Bayer Pharma AG 13342 Berlin Germany Tel. +49 30 468-1111 www.bayerpharma.com Bayer s Xarelto Approved in the EU for the Prevention of Stroke in Patients
Postmenopausal Hormone Replacement Therapy and Cardiovascular Disease
 This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or a basis for reimbursement and coverage policies. AHRQ
This report may be used, in whole or in part, as the basis for development of clinical practice guidelines and other quality enhancement tools, or a basis for reimbursement and coverage policies. AHRQ
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study
 DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
Aging Well - Part V. Hormone Modulation -- Growth Hormone and Testosterone
 Aging Well - Part V Hormone Modulation -- Growth Hormone and Testosterone By: James L. Holly, MD (The Your Life Your Health article published in the December 4th Examiner was a first draft. It was sent
Aging Well - Part V Hormone Modulation -- Growth Hormone and Testosterone By: James L. Holly, MD (The Your Life Your Health article published in the December 4th Examiner was a first draft. It was sent
ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Effects of a fixed combination of the ACE inhibitor, perindopril,
ADVANCE: a factorial randomised trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Effects of a fixed combination of the ACE inhibitor, perindopril,
COULD IT BE LOW TESTOSTERONE?
 COULD IT BE LOW TESTOSTERONE? By Dr. Lauren M. Bramley For thousands of years women have been recognized for their sensitivity to hormones. PMS, post partum depression, menopause have long been plights
COULD IT BE LOW TESTOSTERONE? By Dr. Lauren M. Bramley For thousands of years women have been recognized for their sensitivity to hormones. PMS, post partum depression, menopause have long been plights
Listen to your heart: Good Cardiovascular Health for Life
 Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
Listen to your heart: Good Cardiovascular Health for Life Luis R. Castellanos MD, MPH Assistant Clinical Professor of Medicine University of California San Diego School of Medicine Sulpizio Family Cardiovascular
BREAST CANCER RISK ASSESSMENT AND PRIMARY PREVENTION FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1
 FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1 Hello, my name is Rachel Jankowitz, I m an assistant professor of medicine in the Division of Hematology Oncology at the University of Pittsburgh
FOR HIGH RISK PATIENTS, RACHEL CATHERINE JANKOWITZ, MD 1 Hello, my name is Rachel Jankowitz, I m an assistant professor of medicine in the Division of Hematology Oncology at the University of Pittsburgh
CASE A1 Hypoglycemia in an Elderly T2DM Patient with Heart Failure
 Hypoglycemia in an Elderly T2DM Patient with Heart Failure 1 I would like to introduce you to Sophie, an elderly patient with long-standing type 2 diabetes, who has a history of heart failure, a common
Hypoglycemia in an Elderly T2DM Patient with Heart Failure 1 I would like to introduce you to Sophie, an elderly patient with long-standing type 2 diabetes, who has a history of heart failure, a common
Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement
 Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement Rebecca Ferrini, MD, Elizabeth Mannino, MD, Edith Ramsdell, MD and Linda Hill, MD, MPH Burden
Screening Mammography for Breast Cancer: American College of Preventive Medicine Practice Policy Statement Rebecca Ferrini, MD, Elizabeth Mannino, MD, Edith Ramsdell, MD and Linda Hill, MD, MPH Burden
Stress is linked to exaggerated cardiovascular reactivity. 1) Stress 2) Hostility 3) Social Support. Evidence of association between these
 Psychosocial Factors & CHD Health Psychology Psychosocial Factors 1) Stress 2) Hostility 3) Social Support Evidence of association between these psychosocial factors and CHD Physiological Mechanisms Stress
Psychosocial Factors & CHD Health Psychology Psychosocial Factors 1) Stress 2) Hostility 3) Social Support Evidence of association between these psychosocial factors and CHD Physiological Mechanisms Stress
DUAL ANTIPLATELET THERAPY. Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania
 DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
DUAL ANTIPLATELET THERAPY Dr Robert S Mvungi, MD(Dar), Mmed (Wits) FCP(SA), Cert.Cardio(SA) Phy Tanzania Cardiac Society Dar es Salaam Tanzania DUAL ANTIPLATELET THERAPY (DAPT) Dual antiplatelet regimen
Testosterone; What s all the hype? KRISTEN WYRICK, LTCOL,USAFR, MC USUHS, FAMILY MEDICINE JOINT BASE LANGLEY-EUSTIS
 Testosterone; What s all the hype? KRISTEN WYRICK, LTCOL,USAFR, MC USUHS, FAMILY MEDICINE JOINT BASE LANGLEY-EUSTIS The faces of Low Testosterone What your patients are seeing Pharmacy Industry Testosterone
Testosterone; What s all the hype? KRISTEN WYRICK, LTCOL,USAFR, MC USUHS, FAMILY MEDICINE JOINT BASE LANGLEY-EUSTIS The faces of Low Testosterone What your patients are seeing Pharmacy Industry Testosterone
Bayer Initiates Rivaroxaban Phase III Study to Support Dose Selection According to Individual Benefit-Risk Profile in Long- Term VTE Prevention
 Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Long-term prevention of venous blood clots (VTE): Bayer Initiates Rivaroxaban
Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Long-term prevention of venous blood clots (VTE): Bayer Initiates Rivaroxaban
Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts?
 Telephone: (212) 986-9415 Fax: (212) 697-8658 www.teausa.org 362 5th AVENUE, SUITE 801, NEW YORK, NY 10001 Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts? New Findings Released
Telephone: (212) 986-9415 Fax: (212) 697-8658 www.teausa.org 362 5th AVENUE, SUITE 801, NEW YORK, NY 10001 Smaller Waistlines, Sharper Minds, Stronger Bones and Healthier Hearts? New Findings Released
Peri Menopause and Menopause
 Peri Menopause and Menopause Gary S. Donovitz, M.D., F.A.C.O.G Peri Menopause Perimenopause means "around menopause" and refers to the time period during which a woman's body makes its natural transition
Peri Menopause and Menopause Gary S. Donovitz, M.D., F.A.C.O.G Peri Menopause Perimenopause means "around menopause" and refers to the time period during which a woman's body makes its natural transition
The largest clinical study of Bayer's Xarelto (rivaroxaban) Wednesday, 14 November 2012 07:38
 Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
Bayer HealthCare has announced the initiation of the COMPASS study, the largest clinical study of its oral anticoagulant Xarelto (rivaroxaban) to date, investigating the prevention of major adverse cardiac
Diabetes Complications
 Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES
 PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES Why should mood difficulties in individuals with a health condition be addressed? Many people with health conditions also experience mood difficulties
PCHC FACTS ABOUT HEALTH CONDITIONS AND MOOD DIFFICULTIES Why should mood difficulties in individuals with a health condition be addressed? Many people with health conditions also experience mood difficulties
Mediterranean diet: A heart-healthy eating plan Source: mayoclinic.org/mediterranean-diet
 Mediterranean diet: A heart-healthy eating plan Source: mayoclinic.org/mediterranean-diet The heart-healthy Mediterranean is a healthy eating plan based on typical foods and recipes of Mediterranean-style
Mediterranean diet: A heart-healthy eating plan Source: mayoclinic.org/mediterranean-diet The heart-healthy Mediterranean is a healthy eating plan based on typical foods and recipes of Mediterranean-style
Butler Memorial Hospital Community Health Needs Assessment 2013
 Butler Memorial Hospital Community Health Needs Assessment 2013 Butler County best represents the community that Butler Memorial Hospital serves. Butler Memorial Hospital (BMH) has conducted community
Butler Memorial Hospital Community Health Needs Assessment 2013 Butler County best represents the community that Butler Memorial Hospital serves. Butler Memorial Hospital (BMH) has conducted community
Long-term effects of adjuvant tamoxifen treatment on cardiovascular disease and cancer
 Linköping University Medical Dissertations No. 1430 Long-term effects of adjuvant tamoxifen treatment on cardiovascular disease and cancer Johan Rosell Linköping University, Faculty of Health Sciences
Linköping University Medical Dissertations No. 1430 Long-term effects of adjuvant tamoxifen treatment on cardiovascular disease and cancer Johan Rosell Linköping University, Faculty of Health Sciences
Description of the OECD Health Care Quality Indicators as well as indicator-specific information
 Appendix 1. Description of the OECD Health Care Quality Indicators as well as indicator-specific information The numbers after the indicator name refer to the report(s) by OECD and/or THL where the data
Appendix 1. Description of the OECD Health Care Quality Indicators as well as indicator-specific information The numbers after the indicator name refer to the report(s) by OECD and/or THL where the data
Menopause & Hormone Therapy
 Menopause & Hormone Therapy The Verdict! In 2012 there were two important medical articles that brought clarity to a decade of fear and confusion regarding the risks and benefits of hormone therapy in
Menopause & Hormone Therapy The Verdict! In 2012 there were two important medical articles that brought clarity to a decade of fear and confusion regarding the risks and benefits of hormone therapy in
DISCLOSURES RISK ASSESSMENT. Stroke and Heart Disease -Is there a Link Beyond Risk Factors? Daniel Lackland, MD
 STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
STROKE AND HEART DISEASE IS THERE A LINK BEYOND RISK FACTORS? D AN IE L T. L AC K L AN D DISCLOSURES Member of NHLBI Risk Assessment Workgroup RISK ASSESSMENT Count major risk factors For patients with
Key Health Areas Mapped to Out of Hospital Programme Areas
 1 Key Area (according to letter from David Nicholson) Reducing the number of years of life lost by the people of England from treatable conditions (e.g. including cancer, stroke, heart disease, respiratory
1 Key Area (according to letter from David Nicholson) Reducing the number of years of life lost by the people of England from treatable conditions (e.g. including cancer, stroke, heart disease, respiratory
Karen Kovach M.S, R.D Chief Scientific Officer Weight Watchers International Inc.
 Waking up to real solutions to Chronic Disease: Tackling obesity can reduce the burden of chronic disease and deliver substantial cost savings to struggling European healthcare systems Karen Kovach M.S,
Waking up to real solutions to Chronic Disease: Tackling obesity can reduce the burden of chronic disease and deliver substantial cost savings to struggling European healthcare systems Karen Kovach M.S,
Investor News. Phase III J-ROCKET AF Study of Bayer s Xarelto (rivaroxaban) Meets Primary Endpoint. Not intended for U.S.
 Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Phase III J-ROCKET AF Study of Bayer s Xarelto (rivaroxaban) Meets Primary Endpoint
Investor News Not intended for U.S. and UK Media Bayer AG Investor Relations 51368 Leverkusen Germany www.investor.bayer.com Phase III J-ROCKET AF Study of Bayer s Xarelto (rivaroxaban) Meets Primary Endpoint
CHAPTER 17: HEALTH PROMOTION AND DISEASE MANAGEMENT
 CHAPTER 17: HEALTH PROMOTION AND DISEASE MANAGEMENT HEALTH SERVICES AND PROGRAMS The Plan s Health Promotion and Disease Management Department seeks to improve the health and overall well-being of our
CHAPTER 17: HEALTH PROMOTION AND DISEASE MANAGEMENT HEALTH SERVICES AND PROGRAMS The Plan s Health Promotion and Disease Management Department seeks to improve the health and overall well-being of our
Fast Facts on Osteoporosis
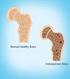 Fast Facts on Osteoporosis Definition Prevalence Osteoporosis, or porous bone, is a disease characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an
Fast Facts on Osteoporosis Definition Prevalence Osteoporosis, or porous bone, is a disease characterized by low bone mass and structural deterioration of bone tissue, leading to bone fragility and an
Grand Rounds: Hysterectomy sans oophorectomy: The case for leaving a woman's ovaries alone
 Grand Rounds: Hysterectomy sans oophorectomy: The case for leaving a woman's ovaries alone If there's no cancer present, why remove a woman's ovaries during hysterectomy? Does the reduced risk of ovarian
Grand Rounds: Hysterectomy sans oophorectomy: The case for leaving a woman's ovaries alone If there's no cancer present, why remove a woman's ovaries during hysterectomy? Does the reduced risk of ovarian
16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS
 16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS Goal Reduce the impact of several major musculoskeletal conditions by reducing the occurrence, impairment, functional limitations, and limitation
16. ARTHRITIS, OSTEOPOROSIS, AND CHRONIC BACK CONDITIONS Goal Reduce the impact of several major musculoskeletal conditions by reducing the occurrence, impairment, functional limitations, and limitation
Thrombosis and Hemostasis
 Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
Thrombosis and Hemostasis Wendy Lim, MD, MSc, FRCPC Associate Professor, Department of Medicine McMaster University, Hamilton, ON Overview To review the important developments in venous thromboembolism
Vitamin D and Calcium: A Systematic Review of Health Outcomes (Update) Executive Summary
 Evidence Report/Technology Assessment Number 217 Vitamin D and Calcium: A Systematic Review of Health Outcomes (Update) Executive Summary Background In 2009, the Tufts Evidence-based Practice Center (EPC)
Evidence Report/Technology Assessment Number 217 Vitamin D and Calcium: A Systematic Review of Health Outcomes (Update) Executive Summary Background In 2009, the Tufts Evidence-based Practice Center (EPC)
Cardiovascular Endpoints
 The Malmö Diet and Cancer Study Department of Clinical Sciences Malmö University Hospital Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 31 Dec * Report:
The Malmö Diet and Cancer Study Department of Clinical Sciences Malmö University Hospital Lund University The Malmö Diet and Cancer Study CV-cohort Cardiovascular Endpoints End of follow-up: 31 Dec * Report:
Medicines to Reduce Breast Cancer Risk
 Medicines to Reduce Breast Cancer Risk Should I take a drug to help reduce my breast cancer risk? If you are a woman who has a higher than average risk of breast cancer, you should know that drugs like
Medicines to Reduce Breast Cancer Risk Should I take a drug to help reduce my breast cancer risk? If you are a woman who has a higher than average risk of breast cancer, you should know that drugs like
A list of FDA-approved testosterone products can be found by searching for testosterone at http://www.accessdata.fda.gov/scripts/cder/drugsatfda/.
 FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
FDA Drug Safety Communication: FDA cautions about using testosterone products for low testosterone due to aging; requires labeling change to inform of possible increased risk of heart attack and stroke
The benefits of prevention: healthy eating and active living
 The benefits of prevention: healthy eating and active living A Summary of Findings By increasing the proportion of the NSW population who are a healthy weight by 2018 (so that one in two adults are of
The benefits of prevention: healthy eating and active living A Summary of Findings By increasing the proportion of the NSW population who are a healthy weight by 2018 (so that one in two adults are of
Efficacy and Tolerability of Antidepressant Duloxetine for Treatment of Hot Flushes in Menopausal Women
 Efficacy and Tolerability of Antidepressant Duloxetine for Treatment of Hot Flushes in Menopausal Women Irina Shestakova, MD, PhD Research Center of Obstetrics, Gynecology and Perinatology Department of
Efficacy and Tolerability of Antidepressant Duloxetine for Treatment of Hot Flushes in Menopausal Women Irina Shestakova, MD, PhD Research Center of Obstetrics, Gynecology and Perinatology Department of
patient education Fact Sheet PFS003: Hormone Therapy APRIL 2015
 patient education Fact Sheet PFS003: Hormone Therapy APRIL 2015 Hormone Therapy Menopause is the time in a woman s life when she naturally stops having menstrual periods. Menopause marks the end of the
patient education Fact Sheet PFS003: Hormone Therapy APRIL 2015 Hormone Therapy Menopause is the time in a woman s life when she naturally stops having menstrual periods. Menopause marks the end of the
Managing Menopausal Symptoms Kirsten J. Lund, M.D. Associate Professor, OB-GYN University of Colorado
 Managing Menopausal Symptoms Kirsten J. Lund, M.D. Associate Professor, OB-GYN University of Colorado Disclosures No ties, financial or otherwise, to pharmaceutical companies Will identify non-fda approved
Managing Menopausal Symptoms Kirsten J. Lund, M.D. Associate Professor, OB-GYN University of Colorado Disclosures No ties, financial or otherwise, to pharmaceutical companies Will identify non-fda approved
Cardiovascular Effects of Drugs to Treat Diabetes
 Cardiovascular Effects of Drugs to Treat Diabetes Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies Clinical Trials:
Cardiovascular Effects of Drugs to Treat Diabetes Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies Clinical Trials:
Barefoot Lady by BarefootLady on May 29, 2016 http://barefoot.lady.zdatingwzef.top/barefoot/lady.pdf. Barefoot Lady
 2... 2 two types of risk factors of cancer 3... 5 or gate 4... 6 dating after 50 in tallahassee 1... 8 types of risks in international business 2... 9 page 1 / 10 2 P. BarefootLady ABSTRACT Suicide Risk
2... 2 two types of risk factors of cancer 3... 5 or gate 4... 6 dating after 50 in tallahassee 1... 8 types of risks in international business 2... 9 page 1 / 10 2 P. BarefootLady ABSTRACT Suicide Risk
Spinal Disorders Claims in Long Term Care Insurance
 Spinal Disorders Claims in Long Term Care Insurance It s such a pain, why bother? Stephen K. Holland, MD Chief Medical Officer Univita Health, Inc. Long Term Care International Forum, May 2011 Albuquerque,
Spinal Disorders Claims in Long Term Care Insurance It s such a pain, why bother? Stephen K. Holland, MD Chief Medical Officer Univita Health, Inc. Long Term Care International Forum, May 2011 Albuquerque,
Florida Breast Health Specialists Breast Cancer Information and Facts
 Definition Breast cancer is a cancer that starts in the tissues of the breast. There are two main types of breast cancer: Ductal carcinoma starts in the tubes (ducts) that move milk from the breast to
Definition Breast cancer is a cancer that starts in the tissues of the breast. There are two main types of breast cancer: Ductal carcinoma starts in the tubes (ducts) that move milk from the breast to
JESSE HUANG ( 黄 建 始 ),MD,MHPE,MPH,MBA Professor of Epidemiology Assistant President
 Breast Cancer Epidemiology i in China JESSE HUANG ( 黄 建 始 ),MD,MHPE,MPH,MBA Professor of Epidemiology Assistant President Chinese Academy of Medical Sciences Peking Union Medical College Medical Center
Breast Cancer Epidemiology i in China JESSE HUANG ( 黄 建 始 ),MD,MHPE,MPH,MBA Professor of Epidemiology Assistant President Chinese Academy of Medical Sciences Peking Union Medical College Medical Center
