Diabetes Foot: Risk Assessment Education Program Participant s Package
|
|
|
- Amy Atkins
- 10 years ago
- Views:
Transcription
1 Diabetes Foot: Risk Assessment Education Program Participant s Package RNAO Developed by a working group of the Alwyn Moyer, Lillian Delmas, Margaret Little, Denise Williams Based on the Registered Nurses Association of Ontario Best Practice Guideline: Reducing Foot Complications for People with Diabetes March 2004
2 Acknowledgement The (RNAO) and the Nursing Best Practice Guidelines Program would like to acknowledge the following individuals and organizations for their contributions to the development of the Diabetes Foot: Risk Assessment Education Program. The (DNIG) is an interest group of the RNAO, and membership is open to all Registered Nurses and nursing students interested in diabetes education and care. As part of their mandate, the DNIG supports continuing nursing education relevant to diabetes education. Within this framework, a Working Group of the facilitated the development of this education program. The RNAO also acknowledges the guideline development panel for the best practice guideline Reducing Foot Complications for People with Diabetes. This best practice guideline is a foundation document for the content of the education program. This program has been developed to support the educational needs of nurses in the implementation of this best practice guideline. Two members of the DNIG Working Group, Alwyn Moyer, RN, MSc(A), PhD and Lillian Delmas, RN, BScN, CRRN, are also members of the guideline development panel, and have provided a strong link between these two groups. In addition, the RNAO wishes to acknowledge the following organizations in Sudbury, Ontario Victorian Order of Nurses Sudbury Branch and Hôpital Régional Sudbury Regional Hospital for their role in pilot testing the guideline and providing the initial outline for this educational resource. The Best Practice Guidelines Program is funded by the Government of Ontario.
3 Table of Contents 1 Diabetes Foot: Risk Assessment Pre-Test/Post-Test 2 Objectives and Critical Behaviours 3 Assessment of Five Key Risk Factors Foot Risk Assessment Form Presence/History of Foot Ulcers Protective Sensation Structural Abnormalities Circulation Self-care Knowledge and Behaviour 4 Diabetes Foot Assessment/Risk Screening Summary 5 Interventions Communicate Risk Status Teach/reinforce Diabetes Self-Care Knowledge and Behaviour Handout Care Tips for the Feet Refer to Diabetes Education/Care Resources Documentation 6 Wrap-up Pre-Test/Post-Test Answers Tips for Client Education: Adult Learning Principles Workshop Evaluation 7 Images The Diabetic Foot
4 Diabetes Foot: Risk Assessment Pre-Test / Post-Test 1. Diabetes mellitus increases the risk of foot amputation by 20 fold. True False 2. Trauma is one of the most common causes of skin ulceration in persons with diabetes. True False 3. List the five key risk factors for foot ulcers in persons with diabetes. 4. Identify the most effective way to measure sensation in the foot of a person with diabetes. 5. Describe where you can palpate a pulse in your foot.
5 6. How often should a health provider reinforce the importance of diabetes foot care for persons at lower risk for the development of foot ulcers? 7. How frequently should a person with diabetes inspect his/her feet? 8. Identify two factors that might make it difficult for a person with diabetes to complete proper foot care. 9. What additional information is required to complete the following advice to a person with diabetes: Wash feet daily, dry thoroughly and apply cream to dry areas. 10. A person with diabetes who develops a foot ulcer should be advised to see a doctor if it does not heal in three days. True False
6 Diabetes Foot: Risk Assessment Objectives and Critical Behaviours At the end of this skills workshop, you will be able to: Objectives 1. Conduct a foot assessment for clients with known diabetes in order to: a. Identify the presence of foot ulceration or history of previous foot ulcers. b. Assess sensation in the foot using a Semmes-Weinstein monofilament. c. Observe the client s feet and assess for physical/structural abnormalities. d. Assess recent history of intermittent claudication and palpate pedal pulses bilaterally. e. Assess previous foot care education. 2. Provide basic education for the prevention of foot ulcers for all clients with diabetes. 3. Implement appropriate actions when clients are assessed at higher risk for foot ulcers and/or amputation. 4. Document a foot risk assessment and classify the level of risk. Critical Behaviours 1. Identify the five key risk factors for foot ulceration and amputation in clients with diabetes. 2. Assess the client s foot for loss of sensation. 3. Assess the client s foot for structural abnormalities. 4. Palpate the dorsalis pedis and posterior tibial pulses. 5. Assess self-care ability to perform foot care. 6. Assess the appropriateness of foot wear. 7. Verbalize the key elements of appropriate foot care. 8. Verbalize instructions to the client on the importance of regular foot examination by a health care professional, based on level of risk. 9. Accurately record a foot assessment.
7 Assessment of Five Key Risk Factors Foot Risk Assessment Form Presence/History of Foot Ulcers Examine both feet, without shoes. Sore(s) present? Yes / No Ask: Have you ever had a sore on your foot that took more than two weeks to heal? Yes / No Chart any sores on the diagrams below. Left Foot Top Left Foot Bottom Right Foot Bottom Right Foot Top
8 Protective Sensation Assess using the Semmes-Weinstein Monofilament (10 gram, 5.07). Instructions for use of Semmes-Weinstein Monofilament 1. Show the monofilament to the patient. Place the end of the monofilament on his/her hand or arm to show that the testing procedure will not hurt. 2. Ask the patient to turn his/her head and close his/her eyes or look at the ceiling. 3. Hold the monofilament perpendicular to the skin. skin monofilament Place tip on sole of foot......bend......and release. 4. Place the tip of the monofilament on the sole of the foot. Ask the patient to say yes when he/she feels you touching his/her foot with the monofilament. DO NOT ASK THE PATIENT did you feel that? If the patient does not say yes when you touch a given testing site, continue on to another site. When you have completed the sequence, RETEST the area(s) where the patient did not feel the monofilament. 5. Push the monofilament until it bends, then hold for 1-3 seconds. 6. Lift the monofilament from the skin (Do not brush or slide along the skin). 7. Repeat the sequence randomly at each of the testing sites on each foot (see figure at right). 8. Clean the monofilament according to agency infection control protocols and store according to the manufacturer s instructions. Mark the four, circled areas of the foot. Use a plus sign (+) if they can feel the monofilament and a minus sign ( ) if they cannot. Right Foot Bottom Left Foot Bottom
9 Structural Abnormalities Examine both feet without socks and shoes, standing and sitting or lying down. Check all that apply. Structural Abnormality Yes Toe deformities (e.g., claw or hammer toes) Blisters, Calluses, Fungal Infection (Please circle all that apply) Hallux valgus (Bunion) Amputation (Please specify: Right / Left Level: Year: ) Charcot s joint (foot warm, swollen, red, and painless) Footwear Uneven wear on soles of shoes A wide toe box (1/2 between the tip of the toe and the end of the shoe) Sufficient depth Good arch support Shoe fits without rubbing along any area of the foot See Images The Diabetic Foot for illustrations
10 Circulation a) Assess for Intermittent Claudication Ask: Do you have pain in the calf when walking or on exertion that is relieved by rest within 10 minutes? Yes / No b) Assess Pedal Pulses Pedal Pulse Present Absent Right posterior tibial Left posterior tibial Right dorsalis pedis Left dorsalis pedis Instructions for locating and palpating Pedal Pulses Dorsalis Pedis Place fingers just lateral to the extensor tendon of the great toe. (If you cannot feel a pulse, move fingers more laterally.) Posterior Tibial Place fingers behind and slightly below the medial malleolus of the ankle. (In an obese or edematous ankle, the pulse may be more difficult to feel.) To enhance technique, assume a comfortable position for you and the client. Place hand in position and linger on the site. Varying pressure may assist in picking up a weak pulsation. Do not confuse client s pulse with your own pulsating fingertips. Use your carotid pulse for comparison, if needed.
11 Self-care Knowledge and Behaviour Observe and/or question the client to complete the assessment Self-care Knowledge and Behaviour Yes No Able to see and/or reach the bottom of feet or, has help from someone who has been taught to do daily foot care Able to do own skin and nail care Has received foot care education in the past year Has annual foot examination by a professional Checks condition of feet most days Knows to report foot problems to a health provider (e.g., would seek advice from health provider for a blister on foot) Wears well fitting footwear Takes steps to reduce risk of injury: Avoids going barefoot outside or indoors Checks for foreign objects in shoes before wearing them; Checks water temperature before entering a bath, etc. (using thermometer or wrist, not feet) Knows that having diabetes increases risk for foot problems Knows personal risk factors for foot complications
12 Diabetes Foot Assessment/Risk Screening Summary Use this guide to assess and/or document the presence of potential risk factors for foot ulceration and amputation. Examine both feet and inquire about client self-care practices. Tick the yes or no box next to an assessment element for each potential risk factor. Summarize the findings by circling the level of risk, and/or if a self-care knowledge deficit is identified. Risk Factors Yes No 1. Foot ulcer (a wound that took > 2 weeks to heal) now or in the past 2. Loss of sensation at any one site (determined after testing the 4 sites: great toe, first, third, and fifth metatarsal heads using the 10 gram/5.07 monofilament) 3. Callus present on soles of feet or toes or abnormal foot shape (e.g., claw or hammer toes, bunion, obvious bony prominence, Charcot s foot or joint) 4. Pedal pulses (dorsalis pedis or posterior tibial) not palpable by nurse and positive history of lower limb pain on exertion that is relieved with rest. 5. Client unable to see the bottom of feet and/or unable to reach the bottom of feet and does not have someone who has been taught to perform appropriate foot care/inspection. 6. Poor fitting footwear (shoes too narrow or short, no toe protection, rough or worn interior, uneven wear on sole or heel). 7. Client has not received foot care education before. 8. Client does not check condition of feet most days. Ask How do you know if you have a reddened area or other problem with your feet? or How often do you check your feet? 9. Client does not report foot problems to health care provider. Ask What would you do if you found a blister on your foot? 10. Client does not take steps to reduce risk of injury. Ask if client walks bare foot out or indoors, checks for foreign objects in shoes before wearing them, checks water temperature before entering a bath, etc. If the answer is NO to all items 1 4, the client is at LOWER RISK If the answer is YES to any items 1-4, the client is at HIGHER RISK If the answer is YES to any items 5 10, this indicates an opportunity to enhance self-care knowledge and behaviour. SELF-CARE KNOWLEDGE DEFICIT Adapted from: Sharon Brez, RN, BScN, MA(Ed), CDE, Advanced Practice Nurse, Endocrinology and Metabolism, The Ottawa Hospital, Ottawa, Ontario.
13 Interventions 1 Communicate Risk Status 2 Teach/Reinforce Diabetes Self-care Knowledge and Behaviour 3 Refer to Diabetes Education/Care Resources 4 Documentation Communicate Risk Status Explain the level of risk and provide information on how to reduce the risk through self-care and regular foot examination, paying particular attention to the gaps in self-care knowledge. Risk Classification and Nursing Intervention Guide LOWER RISK Explain risk for foot complications related to diabetes. HIGHER RISK Explain risk for foot complications related to diabetes. Inform client of personal risk factors identified in this nursing assessment. Teach or reinforce basic foot care practices and strategies for foot injury prevention. Teach or reinforce basic foot care practices and strategies for foot injury prevention. Reinforce benefits of annual foot examination. Reinforce benefits of regular professional foot exam and risk assessment (every 3-6 months). Refer patient to primary care provider or diabetes care/ education program for further assessment and follow-up. Teach or Reinforce Self-care Knowledge and Behaviour Please refer to the resource Care Tips for the Feet on the next page.
14 Care Tips for the Feet Did you know that having diabetes puts you at risk of developing complications such as foot ulcers? Managing your blood sugar is important for healthy feet. See your healthcare provider Get complete diabetes education! YEARLY EXAM NEEDED! Have a health professional examine your feet at least once a year. Find out if you have lower or higher risk feet. RISK FACTORS A previous foot ulcer Loss of normal feeling in your feet Abnormal shaped foot, including calluses and bunions Poor circulation to your feet Protect your feet! Follow these simple guidelines: 1. Check your feet daily Look for red areas, blisters or any open area. If you cannot do this yourself, have someone else check for you. See your doctor or foot specialist right away if you find a problem! 2. Protect your feet - always wear shoes! Wear shoes that fit well, support your foot and are not too tight. Do not wear shoes that cause reddened or sore areas. See a specialist for footwear advice if you have a higher risk foot. 3. Keep your skin clean and soft Wash your feet regularly, but do not soak them. Dry well between your toes. Check that the water is not too hot before putting your feet in it. Use unscented creams. Do not put cream between the toes. 4. Don t hurt yourself with nail clippers or razors Cut your nails straight across. Get help to cut your nails, if needed. Don t cut calluses. See a local foot care clinic. Many are covered by the Ontario Health Insurance Plan (OHIP).
15 Referral Refer as appropriate, depending on risk status. Diabetes Education/Care Resources Diabetes education may be available in a variety of settings, depending upon your local resources. The best source to readily identify what is available in your community would be the national office of the Canadian Diabetes Association. They maintain a national directory and will be able to provide you with contact information specific to your community. Then contact your local chapter of the Canadian Diabetes Association for direction to available diabetes education and care resources. It may be a hospital, Community Health Centre, Home Health Agency or other agency. Contacting any one of these agencies will then provide you with a list of potential referral points for Specialized Diabetes Foot Care and Education. National Office, Canadian Diabetes Association BANTING ( ) or Local Chapter of the Canadian Diabetes Association Local Diabetes Education Resources for those in Northern Ontario go directly to: Local Diabetic Foot Care Specialists
16 Documentation Intervention Yes No Explained risk for diabetes foot complications due to history of foot ulcers, impaired sensation, structural abnormalities or impaired circulation. (Tailor to individual risk and need.) Provided/reinforced diabetes foot self-care and injury prevention as outlined in handout Care Tips for the Feet. Gave handout to client/caregiver. Provided information and handout on local diabetes resources. Referred for further assessment and follow-up: Primary health care provider Diabetes education program Other (Please specify)
17 Wrap-up 1 Pre-Test/Post-Test Answers 2 Tips for Client Education: Adult Learning Principles 3 Workshop Evaluation Pre-Test / Post-Test Answers 1. Diabetes mellitus increases the risk of foot amputation by 20 fold. True. Up to 15% of patients with diabetes may develop foot ulcers in their lifetime (ADA, 1999; Palumbo & Melton, 1985; Pham et al., 2000). In one study, a non healing foot ulcer preceded 84% of diabetic lower limb amputations (Pecoraro, Reiber, & Burgess, 1990; Reiber et al., 1999). In Ontario, the evidence suggests that effective outpatient care for diabetic foot ulcers and infections is reducing minor amputation rates (Hux, Jacka, Fung, & Rothwell, 2002). Three important actions to prevent peripheral vascular disease include: Stop smoking Improve blood glucose control Get regular foot care (Hux et al., 2002) 2. Trauma is one of the most common causes of skin ulceration in persons with diabetes True. The most frequent component causes for lower extremity ulcers are trauma, neuropathy and deformity. Traumatic event can be the result of 1) low pressure and continuing stress, or 2) high pressure of short duration that results in a break in the skin or tissue damage (Reiber et al., 1999). 3. List the five key risk factors for foot ulcers in persons with diabetes. Foot ulcer, now or in the past Diminished sensation Structural abnormalities Impaired circulation Lack of foot care education (self-care knowledge deficit) 4. Identify the most effective way to measure sensation in the foot of a person with diabetes. Semmes Weinstein monofilament (10 gram, 5.07).
18 5. Describe where you can palpate a pulse in the foot. Dorsalis Pedis: dorsal aspect of foot, lateral to extensor tendon of big toe Posterior Tibial: ankle, behind medial malleolus A positive history of lower limb intermittent claudication combined with non-palpable pedal pulses bilaterally increases the likelihood of identifying PVD in diabetes (Boyko et al., 1997). 6. How often should a health provider reinforce the importance of diabetes foot care for persons at lower risk for the development of foot ulcers? Each visit 7. How frequently should a person with diabetes inspect his/her feet? Daily 8. Identify two factors that might make it difficult for a person with diabetes to complete proper foot care. Poor vision Decreased mobility Lack of energy (Reinforce importance of getting support) 9. What additional information is required to complete the following advice to a person with diabetes: Wash feet daily, dry thoroughly and apply cream to dry areas. but do not apply cream between the toes because it will predispose to maceration and skin breakdown. 10. A person with diabetes who develops a foot ulcer should be advised to see a doctor if it does not heal in three days. False. Should be advised to consult a doctor immediately.
19 Tips for Client Education Adult Learning Principles Diabetes education should be interactive, solution focused and based on the experiences of the learner, as well as staged and tailored to meet individual needs and abilities. Group education and sustained long-term followup have both been shown to enhance knowledge, and produce positive outcomes (CDA, 2003). Adult motivation to learn is driven by: Success: Adults want to be successful learners. Volition: Adults want to feel a sense of choice in their learning. Value: Adults want to learn something they value. Enjoyment: Adults want to experience the learning as pleasurable. Skills and characteristics of good, motivating instructors: Expertise: knowing the material and having mastery of the skills to be conveyed; Empathy: realistically understanding the learner s needs and expectations and adapting the instruction to meet the learner s level of experience, skill and perspectives; Enthusiasm: showing commitment and value in what is being taught and being able to convey this with appropriate degrees of emotion, animation and energy; Clarity: organizing material and using language that can be understood and followed by most learners, and providing the learner with opportunity for repetition and clarification. (Knowles, Holton and Swanson, l998, pp )
20 Diabetes Foot: Risk Assessment Education Program Evaluation Form Please circle the number which corresponds to your evaluation. Strongly Disagree Strongly Agree NA= Not Applicable Presenter Well informed Spoke clearly Managed time well Answered questions Encouraged participation Topic Highly relevant Written resources High quality, clear Pertinent, facilitated understanding Enough time allocated For questions For practice session For evaluation Objectives Were clearly stated Were adequately met Outcomes (resulting from this session) I will change my practice I plan to use the resources in my practice I plan to obtain additional information on this topic Comments Please return this evaluation to the workshop facilitator.
21 Images The Diabetic Foot Deformities Mallet Toe With a mallet toe, the joint nearest the tip of the toe is bent. Hammer Toe With a hammer toe, the middle joint is bent. Hallux Valgus (Mild/Moderate) A small bump (sometimes called a bunion) forms when the big toe turns in toward the second toe. The joint at the base of the big toe is pushed to the side. Hallax Valgus (Severe) The angulation of the big toe is marked, forming a large bunion. The big toe may move under the second toe. Claw Toe With a claw toe, the joint at the base of the toe is bent up. The middle joint is bent down. Pressure Related Corns A corn is a conical, horny induration and thickening of the skin caused by friction or pressure. Hard corns may develop on the tops or tips of the toes. Soft corns develop between the toes. Calluses A callus is a horny layer of skin caused by pressure or friction. It may spread across the ball of the foot or along the outer edge of the heel or big toe. A callus may develop a central core or plug of tissue where the pressure is greatest. Published with permission Nancy A. Bauer, BA, Bus Admin., RN, ET
22 Infections Hot Spots Red hot spots on the feet are signs of pressure or friction. If pressure is not relieved, a hot spot may develop into a blister. Left untreated, a blister may turn into an open wound or a corn or callus. Ulcers If corns or calluses press into the foot, they destroy underlying skin layers, and an ulcer results. Ulcers may lead to infection. In some cases, skin from a callus or corn may cover an open wound, making it difficult to assess. Infected Ulcers Infected ulcers may result in the death of healthy tissue. Symptoms of infection include white, yellow or green discharge, bleeding or odour. Fungal Nails Fungal nails may be the result of fungal infections such as Athlete s Foot, the use of artificial nails or nail polish, or injury to the nail. Fungal nails may become thickened, inflamed, and sensitive and may turn unnatural colours. Charcot Joint Charcot joint is a form of neuroarthropathy that occurs most often in the foot. Nerve damage from diabetes causes decreased sensation, muscle atrophy and subsequent joint instability. Walking on an insensitive joint makes it worse. In the acute stage there is inflammation and bone reabsorption which weakens the bone. In later stages, the arch falls and the foot may develop a rocker bottom appearance. Early treatment can stop bone destruction and help healing. Published with permission Nancy A. Bauer, BA, Bus Admin., RN, ET
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
Treat Your Feet: Foot care for people with diabetes
 Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS
 CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS RATIONALE Clinical evidence suggests that there is considerable potential to improve the quality of foot care for people with diabetes.
CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS RATIONALE Clinical evidence suggests that there is considerable potential to improve the quality of foot care for people with diabetes.
How can DIABETES affect my FEET? Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
Diabetes : Foot Education
 Diabetes : Foot Education Dr. Naushira Pandya, M.D., CMD, Sweta Tewary, PhD, MSW Department of Geriatrics Nova Southeastern University Florida Coastal Geriatric Resources, Education, and Training Center
Diabetes : Foot Education Dr. Naushira Pandya, M.D., CMD, Sweta Tewary, PhD, MSW Department of Geriatrics Nova Southeastern University Florida Coastal Geriatric Resources, Education, and Training Center
Diabetes and your feet
 The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Improving the Compliance of the Annual Foot Examination and Monofilament Testing in
 Improving the Compliance of the Annual Foot Examination and Monofilament Testing in Diabetic Patients at Centromed Principal Investigator: Velen Tat, Physician Assistant Student 2016, University of Southern
Improving the Compliance of the Annual Foot Examination and Monofilament Testing in Diabetic Patients at Centromed Principal Investigator: Velen Tat, Physician Assistant Student 2016, University of Southern
More hospital days are spent treating diabetic foot infections than any other complication of this disease.
 DIABETIC FOOT CARE The disease known as DIABETES MELLITUS affects many parts of the body, especially the feet. It is very important that a diabetic give the feet very special care. A small problem in a
DIABETIC FOOT CARE The disease known as DIABETES MELLITUS affects many parts of the body, especially the feet. It is very important that a diabetic give the feet very special care. A small problem in a
WorryFree DME SM Diabetic Shoe Order Entry Form
 WorryFree DME SM Diabetic Shoe Order Entry Form Non-Physician Supplier Medicare Compliance Documentation Guide Shoe Fitter Responsibility/Actions 1. Complete Patient Evaluation Prior to Shoe Selection.
WorryFree DME SM Diabetic Shoe Order Entry Form Non-Physician Supplier Medicare Compliance Documentation Guide Shoe Fitter Responsibility/Actions 1. Complete Patient Evaluation Prior to Shoe Selection.
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
This is caused by muscle strain to the Achilles tendon in the heel of the foot.
 Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Critically evaluate the organization of diabetic foot ulcer services and interdisciplinary team working
 Rationale of Module Accurate nursing assessment is the key to effective diabetic foot ulcer prevention, treatment and management. A comprehensive assessment identifies ulcer aetiology and the factors which
Rationale of Module Accurate nursing assessment is the key to effective diabetic foot ulcer prevention, treatment and management. A comprehensive assessment identifies ulcer aetiology and the factors which
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Modifiers Q7, Q8, and Q9
 1-47 Modifiers Q7, Q8, and Q9 (Routine Foot Care) CPT Modifier Q7 One Class A finding Q8 Two Class B findings Q9 One Class B and two Class C findings General Information The Office of Inspector General
1-47 Modifiers Q7, Q8, and Q9 (Routine Foot Care) CPT Modifier Q7 One Class A finding Q8 Two Class B findings Q9 One Class B and two Class C findings General Information The Office of Inspector General
Wound and Skin Assessment. Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center
 Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
LUPUS. and the Feet LUPUSUK 2015
 16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
What Podiatrists Would Like Team Members to Know About Foot Health and Diabetes
 What Podiatrists Would Like Team Members to Know About Foot Health and Diabetes 48 In this section, you will find an overview of key medical issues related to foot health and diabetes to inform all members
What Podiatrists Would Like Team Members to Know About Foot Health and Diabetes 48 In this section, you will find an overview of key medical issues related to foot health and diabetes to inform all members
Rheumatoid Arthritis of the Foot and Ankle
 Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
DIABETES A chronic, debilitating and often deadly disease A global epidemic Diabetes in Africa
 DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
NZSSD PodSIG Michele Garrett, Steve York, Claire O Shea, Leigh Shaw, Fiona Angus, Judy Clarke and Karyn Ballance
 Welcome to the Diabetes Foot Screening and Risk Stratification Tool. This tool is based on the work of the Scottish Foot Action Group (SFAG). It has been adapted (with SFAG permission) by the New Zealand
Welcome to the Diabetes Foot Screening and Risk Stratification Tool. This tool is based on the work of the Scottish Foot Action Group (SFAG). It has been adapted (with SFAG permission) by the New Zealand
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS
 APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Diabetes Programme Clinical Strategy and Programmes Directorate 2011 Document Control Revision number: 01 Document drafted by: National Diabetes Programme Working
Model of Care for the Diabetic Foot National Diabetes Programme Clinical Strategy and Programmes Directorate 2011 Document Control Revision number: 01 Document drafted by: National Diabetes Programme Working
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Plantar Fascia Release
 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Podiatric Medicine. What is a Podiatrist?
 Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Facts About Peripheral Arterial Disease (P.A.D.)
 Facts About Peripheral Arterial Disease (P.A.D.) One in every 20 Americans over the age of 50 has P.A.D., a condition that raises the risk for heart attack and stroke. Peripheral arterial disease, or P.A.D.,
Facts About Peripheral Arterial Disease (P.A.D.) One in every 20 Americans over the age of 50 has P.A.D., a condition that raises the risk for heart attack and stroke. Peripheral arterial disease, or P.A.D.,
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION. Statement of LICENSURE Violations
 (X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
(X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
Type 2 Diabetes. Increase of diabetic complications as HAIC increases
 Type 2 Diabetes Diabetes is a disease of too much sugar (glucose) in the blood. Type 2 diabetes is caused by insulin resistance of the cells and abnormal insulin production by the pancreas. Insulin is
Type 2 Diabetes Diabetes is a disease of too much sugar (glucose) in the blood. Type 2 diabetes is caused by insulin resistance of the cells and abnormal insulin production by the pancreas. Insulin is
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
Diabetes Brief. Pre diabetes occurs when glucose levels are elevated in the blood, but are not as high as someone who has diabetes.
 Diabetes Brief What is Diabetes? Diabetes mellitus is a disease of abnormal carbohydrate metabolism in which the level of blood glucose, or blood sugar, is above normal. The disease occurs when the body
Diabetes Brief What is Diabetes? Diabetes mellitus is a disease of abnormal carbohydrate metabolism in which the level of blood glucose, or blood sugar, is above normal. The disease occurs when the body
Working together to prevent pressure ulcers (prevention and pressure-relieving devices)
 Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Heel pain and Plantar fasciitis
 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Align. Strengthen. Restore.
 Correct Toes Manual Align. Strengthen. Restore. Index Our Story 4 Spread Your Toes 6 Correct Toes 8 Foot Problems 10 Benefits of Correct Toes 12 Instructions for Use and Care 14 Before You Begin 14 How
Correct Toes Manual Align. Strengthen. Restore. Index Our Story 4 Spread Your Toes 6 Correct Toes 8 Foot Problems 10 Benefits of Correct Toes 12 Instructions for Use and Care 14 Before You Begin 14 How
PLANTAR FASCITIS (Heel Spur Syndrome)
 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Anyone who has difficulty moving can get a pressure sore. But you are more likely to get one if you:
 Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Basic Stretch Programme 3. Exercise Circuit 4
 Basic Stretch Programme 3 Exercise Circuit 4 2 1 Calves Stand approximately 1 metre away from wall with legs straight and heels on floor. Step and lean forward and slowly push hips towards wall. Should
Basic Stretch Programme 3 Exercise Circuit 4 2 1 Calves Stand approximately 1 metre away from wall with legs straight and heels on floor. Step and lean forward and slowly push hips towards wall. Should
Take Charge of Your Diabetes
 Take Charge of Your Diabetes A Reinforcement Booklet for People With Diabetes Purpose and Acknowledgments This simplified and shortened overview of CDC s 1997 publication, Take Charge of Your Diabetes,
Take Charge of Your Diabetes A Reinforcement Booklet for People With Diabetes Purpose and Acknowledgments This simplified and shortened overview of CDC s 1997 publication, Take Charge of Your Diabetes,
Preventing & Managing Complications of Diabetes
 Preventing & Managing Complications of Diabetes Target Audience: Persons with diabetes and family members Objectives: Participants will be able to: 1. identify the complications associated with diabetes
Preventing & Managing Complications of Diabetes Target Audience: Persons with diabetes and family members Objectives: Participants will be able to: 1. identify the complications associated with diabetes
KINESIOLOGY TAPING GUIDE
 KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
Diabetic Foot Ulcers and Pressure Ulcers. Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences
 Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS.
 ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
What are Core Muscles?... 2. A Healthy Lumbar Spine...3. What is Low Back Pain?...4. Rehabilitation...6. Stages of Rehabilitation...
 Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Community home-based prevention of disability due to lymphatic filariasis
 Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE
 PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
the Role of Patricia Turner BSN, RN, CWCN, CWS
 Understanding the Role of Outpatient Wound Centers Patricia Turner BSN, RN, CWCN, CWS Outpatient wound centers are somewhat of a specialty unto themselves within the world of wound care. The focus of the
Understanding the Role of Outpatient Wound Centers Patricia Turner BSN, RN, CWCN, CWS Outpatient wound centers are somewhat of a specialty unto themselves within the world of wound care. The focus of the
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
SELF-MASSAGE HANDOUTS
 SELF-MASSAGE HANDOUTS Self-Massage for the Head and Face Self-Massage for the Low Back and Buttocks Self-Massage for Runners Self-Massage for the Neck Self-Massage for the Feet Self-Massage for the Arms
SELF-MASSAGE HANDOUTS Self-Massage for the Head and Face Self-Massage for the Low Back and Buttocks Self-Massage for Runners Self-Massage for the Neck Self-Massage for the Feet Self-Massage for the Arms
THE PREVENTION AND REHABILITATION OF SPORTS INJURIES THE PREVENTION AND REHABILITATION OF SPORTS INJURIES. NO, there isn t.
 THE PREVENTION AND REHABILITATION OF SPORTS INJURIES VILMOS DANI M.D. Department of Family Medicine Faculty of Medicine, Semmelweis University Budapest, Hungay GIZELLA PERÉNYI M.D. Department of Rehabilitation
THE PREVENTION AND REHABILITATION OF SPORTS INJURIES VILMOS DANI M.D. Department of Family Medicine Faculty of Medicine, Semmelweis University Budapest, Hungay GIZELLA PERÉNYI M.D. Department of Rehabilitation
Louisiana State Board of Nursing
 Louisiana State Board of Nursing DECLARATORY STATEMENT ON THE ROLE AND SCOPE OF PRACTICE OF THE REGISTERED NURSE IN PERFORMING FOOT CARE INTERVENTIONS Preamble The Louisiana State Board of Nursing believes
Louisiana State Board of Nursing DECLARATORY STATEMENT ON THE ROLE AND SCOPE OF PRACTICE OF THE REGISTERED NURSE IN PERFORMING FOOT CARE INTERVENTIONS Preamble The Louisiana State Board of Nursing believes
12/10/2011. All About Bunions! The Ballet Blog Webinars Lisa Howell (B.Phty)
 12/10/2011 All About Bunions! The Ballet Blog Webinars Lisa Howell (B.Phty) All About Bunions! Please meet Lilly... And her feet! Lilly is a 19 year old professional Classical Dancer, having a lot of problems
12/10/2011 All About Bunions! The Ballet Blog Webinars Lisa Howell (B.Phty) All About Bunions! Please meet Lilly... And her feet! Lilly is a 19 year old professional Classical Dancer, having a lot of problems
Patient Information. and Physical Activity Diary. Wythenshawe Hospital Cardiac Rehabilitation. Name:... The ticker club Registered Charity No.
 Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
Forefoot deformity correction
 Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
Contact us Pharmacy Medicines Helpline If you have any questions or concerns about your medicines, please speak to the staff caring for you or call our helpline. t: 020 7188 8748 9am to 5pm, Monday to
FEET and PSORIATIC ARTHRITIS. Louise Skipp Podiatrist, Sirona Care and Health, Bath
 FEET and PSORIATIC ARTHRITIS Louise Skipp Podiatrist, Sirona Care and Health, Bath What would you like to know? Common problems Practical tips What you can do to help yourself When to seek help and from
FEET and PSORIATIC ARTHRITIS Louise Skipp Podiatrist, Sirona Care and Health, Bath What would you like to know? Common problems Practical tips What you can do to help yourself When to seek help and from
Strength Training HEALTHY BONES, HEALTHY HEART
 Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Ensure that the chair you use is sturdy and stable. Wear comfortable clothes and supportive footwear.
 Page 1 Safety Ensure that the chair you use is sturdy and stable. Wear comfortable clothes and supportive footwear. Prepare a space and have your exercise band and a glass of water (for afterwards) ready
Page 1 Safety Ensure that the chair you use is sturdy and stable. Wear comfortable clothes and supportive footwear. Prepare a space and have your exercise band and a glass of water (for afterwards) ready
Minor Lid Surgery. Information for patients
 Minor Lid Surgery Information for patients This leaflet has been produced to give you information about the problems you have been having with your eyelid. If you have any questions or require further
Minor Lid Surgery Information for patients This leaflet has been produced to give you information about the problems you have been having with your eyelid. If you have any questions or require further
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Chapter 5. Objectives. Normal Ankle Range of Motion. Lateral Ankle Sprains. Lateral Ankle Sprains. Assessment of Lateral Ankle Sprains
 Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Endoscopic Plantar Fasciotomy
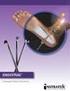 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Carpal Tunnel Release. Relieving Pressure in Your Wrist
 Carpal Tunnel Release Relieving Pressure in Your Wrist Understanding Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a problem that affects the wrist and hand. If you have CTS, tingling and numbness
Carpal Tunnel Release Relieving Pressure in Your Wrist Understanding Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a problem that affects the wrist and hand. If you have CTS, tingling and numbness
Our feet are much more important to our health than we imagine and giving them the care they deserve will benefit you.
 Insoles Our feet are much more important to our health than we imagine and giving them the care they deserve will benefit you. Our feet may ache due to different biomechanical problems, anatomical or orthopedic
Insoles Our feet are much more important to our health than we imagine and giving them the care they deserve will benefit you. Our feet may ache due to different biomechanical problems, anatomical or orthopedic
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
Below is a diagram showing the main bones together with written text on their order of compilation.
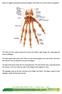 Below is a diagram showing the main bones together with written text on their order of compilation. The hand and wrist contain twenty-seven bones and tendons, eight carpals, five metacarpals and fourteen
Below is a diagram showing the main bones together with written text on their order of compilation. The hand and wrist contain twenty-seven bones and tendons, eight carpals, five metacarpals and fourteen
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Skin biopsy. Delivering the best in care. UHB is a no smoking Trust
 Skin biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A skin biopsy is a
Skin biopsy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm A skin biopsy is a
Background (cont) World Health Organisation (WHO) and IDF predict that this number will increase to more than 1,3 million in the next 25 years.
 Diabetes Overview Background What is diabetes Non-modifiable risk factors Modifiable risk factors Common symptoms of diabetes Early diagnosis and management of diabetes Non-medical management of diabetes
Diabetes Overview Background What is diabetes Non-modifiable risk factors Modifiable risk factors Common symptoms of diabetes Early diagnosis and management of diabetes Non-medical management of diabetes
Preventing Falls. Strength and balance exercises for healthy ageing
 Preventing Falls Strength and balance exercises for healthy ageing Exercise should be comfortable and fun. To get the most out of your home exercise book, join a class for older people to check your exercises
Preventing Falls Strength and balance exercises for healthy ageing Exercise should be comfortable and fun. To get the most out of your home exercise book, join a class for older people to check your exercises
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Triage Documentation. Keeping Yourself Out Of Court. Joy McCarron RN BScN
 Triage Documentation Keeping Yourself Out Of Court Joy McCarron RN BScN Objectives Review of documentation standards CNO NENA CTAS Complexities that Challenge Documentation Triage Documentation Downfalls
Triage Documentation Keeping Yourself Out Of Court Joy McCarron RN BScN Objectives Review of documentation standards CNO NENA CTAS Complexities that Challenge Documentation Triage Documentation Downfalls
My Diabetic Foot Ulcer
 16 You are doing WELL when: Any pain is diminishing or gone You are able to participate in selfcare of your wound The wound is becoming smaller Your blood glucose levels are stable CALL your nursing agency
16 You are doing WELL when: Any pain is diminishing or gone You are able to participate in selfcare of your wound The wound is becoming smaller Your blood glucose levels are stable CALL your nursing agency
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Other Noninfectious Diseases. Chapter 31 Lesson 3
 Other Noninfectious Diseases Chapter 31 Lesson 3 Diabetes Diabetes- a chronic disease that affects the way body cells convert food into energy. Diabetes is the seventh leading cause of death by disease
Other Noninfectious Diseases Chapter 31 Lesson 3 Diabetes Diabetes- a chronic disease that affects the way body cells convert food into energy. Diabetes is the seventh leading cause of death by disease
Recent Injuries. www.physiofirst.org.uk
 Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
How To Manage Diabetes
 How To Manage Diabetes HHC Health & Home Care Serving New Yorkers For Over 45 Years 1-866-NYC-HOME www.homecarenyc.org Contents Your Blood Sugar Goals 4 Testing Your Blood Sugar 5 Blood Sugar Control
How To Manage Diabetes HHC Health & Home Care Serving New Yorkers For Over 45 Years 1-866-NYC-HOME www.homecarenyc.org Contents Your Blood Sugar Goals 4 Testing Your Blood Sugar 5 Blood Sugar Control
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Herniated Disk in the Lower Back
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
GET A HANDLE ON YOUR HEEL PAIN GUIDE
 GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
Arthritis of the Big Toe
 Arthritis of the Big Toe A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Arthritis of the Big Toe - Hallux Rigidus Fred Robinson
Arthritis of the Big Toe A patient s guide Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon www.cambridgefootandankle.com Arthritis of the Big Toe - Hallux Rigidus Fred Robinson
When lifting and carrying weight, do these things:
 F O R Y O U R H E A L T H Protect Your Back While Working What is back pain? Back pain happens when there is a problem with your muscles, nerves, bones, joints and other parts of the back. Back pain can
F O R Y O U R H E A L T H Protect Your Back While Working What is back pain? Back pain happens when there is a problem with your muscles, nerves, bones, joints and other parts of the back. Back pain can
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
Arthritis www.patientedu.org
 written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
A Pocket Guide. Application and Cutting Guide
 A Pocket Guide Application and Cutting Guide Developed by Pia Carlsen, RN, Denmark Jacqui Fletcher, Principal Lecturer, MSc BSc (Hons) PG Dip (ED) RN ILT, UK Maria Mousley, AHP, Consultant Podiatrist,
A Pocket Guide Application and Cutting Guide Developed by Pia Carlsen, RN, Denmark Jacqui Fletcher, Principal Lecturer, MSc BSc (Hons) PG Dip (ED) RN ILT, UK Maria Mousley, AHP, Consultant Podiatrist,
How To Stretch Your Body
 Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
