What Podiatrists Would Like Team Members to Know About Foot Health and Diabetes
|
|
|
- Ariel Stanley
- 8 years ago
- Views:
Transcription
1 What Podiatrists Would Like Team Members to Know About Foot Health and Diabetes 48 In this section, you will find an overview of key medical issues related to foot health and diabetes to inform all members of the health care team about diabetes and how it can affect the health of the patient s feet. The information presented in this section validates key Healthy People 2020 objectives for diabetes and reinforces your value as pharmacy, podiatry, optometry, and dentistry (PPOD) professionals in the team care approach to comprehensive diabetes care. Healthy People 2020 Objectives (Released by the U.S. Department of Health and Human Services each decade, Healthy People is a set of goals and objectives with 10-year targets designed to guide national health promotion and disease prevention efforts to improve the health of all people in the United States.) Diabetes Objective #9 (D 9): Increase the proportion of adults with diabetes who have at least an annual foot examination. Target: 74.8%. Baseline: 68.0% of adults ages 18 years and older with diagnosed diabetes had at least one foot examination by a health professional in the past 12 months, as reported in 2008 (age adjusted to the year 2000 standard population). Target Setting Method: 10% improvement. Data Source: Behavioral Risk Factor Surveillance System (BRFSS), Centers for Disease Control and Prevention (CDC), National Center for Chronic Disease Prevention and Health Promotion.
2 Current Data and Trends Diabetes-related complications may present initially in the foot. Foot symptoms increase the risk for comorbid complications, of which nontraumatic lower-extremity amputations (LEAs) are the greatest concern: In the United States, more than 60% of nontraumatic LEAs occur in people with diabetes. About 65,700 nontraumatic LEAs were performed in 1 year on people with diabetes. 1 In the general population aged 45 years, the incidence of vascular lowerlimb amputation (LLA) at or proximal to the transmetatarsal level is eight times higher in people with diabetes than those without diabetes. 2 The incidence of initial unilateral amputation per 100,000 personyears was 192 for women with diabetes versus 22 for women without diabetes, and 197 for men with diabetes versus 24 for men without diabetes. 2 Patient Case Example A podiatrist notices his 35-yearold patient with diabetes has terrible breath and asks about it. The patient is embarrassed, but admits that he has noticed a bad taste as well. A quick look in the patient s mouth reveals inflamed, swollen gums with pus at the gum line. The podiatrist describes the link between periodontal disease and poor blood glucose control and stresses the need for urgent dental attention for a possible abscess. The podiatrist s office helps the patient obtain a prompt dental appointment for care. The overall 25-year incidence of LEA in people with diabetes was 10.1%. Male gender, smoking, hypertension, diabetic retinopathy, and higher A1C values were associated with a greater risk of LEA. 3 From reported statistics, about 75,000 diabetes-related hospital discharges involve LEA. The LEA rate per 1,000 persons with diabetes is 3.9 among persons ages 65 years and younger, 6.6 among persons ages 65 to 74 years, and 7.9 among persons ages 75 years or older. After their initial amputation, 9% to 17% of patients will experience a second amputation within the same year 4, and 25% to 68% of people with diabetes will have an amputation of the contralateral extremity within 5 years. 5 Working Together to Manage Diabetes: A GUIDE FOR PHARMACY, PODIATRY, OPTOMETRY, AND DENTISTRY 49
3 Foot Health and Diabetes One study found that 80% of nontraumatic LEAs are preceded by a foot ulceration, which provides a portal for infection. 6 According to BRFSS data, approximately 12% of U.S. adults with diabetes have a history of foot ulcer, a risk factor for LEA. 7 Another report identified minor trauma, ulceration, and faulty wound healing as precursors to 73% of LEAs, often in combination with gangrene and infection. 6 Other risk factors include the presence of sensory peripheral neuropathy, altered biomechanics, elevated pressure on the sole of the foot, and limited joint mobility. 8 Diabetes-related Foot Conditions Podiatrists consider the following conditions as they assess the risk for complications when evaluating the feet of people with diabetes. Neuropathy A patient who experiences subjective tingling, burning, numbness, or the sensation of bugs crawling on the skin, especially at night, may be experiencing peripheral sensory neuropathy. On clinical examination, podiatrists can detect this condition in various ways: with an instrument known as a Semmes-Weinstein 5.07 (10-gram) monofilament and also testing for vibratory sense by using a 128mhz tuning fork. You can find a description of how to perform a comprehensive foot exam in the free National Diabetes Education Program (NDEP) health care provider kit, Feet Can Last a Lifetime. People with diabetes who have neuropathy are 1.7 times more likely to develop foot ulceration. In persons with both neuropathy and foot deformity, the risk is 12 times greater, and in those who also have a history of pathology (prior amputation or ulceration), the risk is 36 times greater. 6,9 Factors that increase a patient s risk for lower-extremity ulceration and amputation include: Male sex The existence of documented diabetes for more than 10 years History of tobacco use A history of persistently elevated blood glucose levels The presence of cardiac, retinal, or renal complications or peripheral arterial occlusive disease 8,9,10,11 50
4 Charcot Foot Patients with neuropathy are at risk for painless degenerative arthropathy, which typically affects the midfoot joints, resulting in a red, swollen, and possibly deformed foot that can be mistaken as being affected by cellulitis. One form of arthropathy, called Charcot foot, causes weakening and fracturing of the bones in the foot and occurs most often in people who have significant neuropathy. Radiographs may show collapse of joint structure and can be misinterpreted as osteomyelitis. Charcot foot is a very serious condition that can lead to severe deformity, disability, and even amputation. Treatment for Charcot arthropathy is complicated and requires a specialist. In some instances, surgery is necessary, but most urgently a non-weight-bearing cast is generally advised. After the acute inflammation has resolved, and if the foot is braceable, the podiatrist may prescribe special shoes to correct altered biomechanics. 13 Without treatment, the Charcot foot can progress to further deformity and ulceration and lead ultimately to amputation. Foot Complication Prevention Consider it a red flag when a patient complains to you that his or her shoes no longer fit, or if the patient is wearing slippers or shoes with sections cut out to accommodate changes in foot shape, walks with a new limp, or complains of unilateral swellings. Many people with diabetes who request routine care will have a treatable foot problem. 12 The lifetime incidence of foot ulcers among patients with diabetes is 25%. 12 Most of these are preventable through interventions available in most primary care settings and appropriate self-care. Patients with diabetes who are on dialysis are at extreme risk for foot complications. Increased foot care frequency and educational outreach to this group are associated with improved foot outcomes. A Charcot foot usually causes little to no pain and may be slowly progressive over weeks to months before coming to a health care provider s attention. You can contribute to amputation prevention by referring patients with these signs and symptoms to a foot care specialist. Working Together to Manage Diabetes: A GUIDE FOR PHARMACY, PODIATRY, OPTOMETRY, AND DENTISTRY 51
5 Foot Health and Diabetes Vasculopathy When a patient experiences cramping of calf muscles when walking (often referred to as a charley horse ) that requires frequent rest periods, he or she may have intermittent claudication. This condition, often caused by insufficient blood supply to the region beneath the knee, indicates the presence of early or moderate occlusion of the arteries, which is common to the lower extremities of people with diabetes. However, the classic symptoms of peripheral artery disease (PAD) may be absent if neuropathy is present. In these instances, patients may complain of painless fatiguing of muscles after walking short distances and indicate that the fatigue is relieved by rest. Remember, PAD is a marker for overall cardiovascular disease. If a patient is diagnosed with PAD, the patient should also be evaluated for cardiovascular risk factors. This may prevent early cardiovascular-related mortality. Patients who experience intense cramping and aching in the toes only at night, called rest pain, can usually relieve the discomfort by hanging their feet over the side of the bed and by walking. Rest pain signifies the end-stage blood vessel disorder and tissue ischemia that precedes diabetic gangrene. Although most clinical research continues to list the loss of sensation/neuropathy as the leading factor in ulceration and associated complications, poor blood supply can contribute to poor ulceration healing and is a significant risk factor for amputation. Both factors need to be addressed in comprehensive diabetes foot care, with diagnostic testing for treatable vascular lesions and intervention as warranted. 52
6 Dermatological Conditions Corns and calluses (hyperkeratotic lesions) of the patient s feet result from elevated mechanical pressure and shearing of the skin. They often precede breakdown of skin and lead to blisters or ulceration, especially in neuropathic patients. Superficial lacerations and heel fissures, or maceration (softening caused by wetness) between the toes, can all serve as portals for infection. Corns, calluses, toenail deformity, and bleeding beneath the nail may signify the presence of sensory neuropathy. Fungal infections are common and should be treated promptly. Musculoskeletal Symptoms Structural changes in the diabetic foot may develop in combination with muscle-tendon imbalances as a result of motor neuropathy. These deformities include the presence of hammertoes, bunions, high-arched foot, or flatfoot all of which increase the potential for focal irritation of the foot in the shoe. People with diabetes may have reduced elasticity of the Achilles tendon, which limits ankle dorsiflexion and increases pressure on the feet. Patient Case Example A 70-year-old man consults a podiatrist because of painful corns on his feet. He says, I don t walk anymore because of these corns, but I guess that doesn t matter I m too old to be walking much. The podiatrist emphasizes the many benefits, including diabetes prevention, of regular physical activity such as walking. He explains that one in five people older than age 60 have diabetes, but that the disease can be prevented or delayed. He treats the man s corns and then shares the NDEP It s Not Too Late to Prevent Diabetes tip sheet with the man. He says, After we get your feet fixed up, you will be out there walking again. Lifestyle and Family History People with diabetes who currently smoke are four times more likely than people without diabetes who smoke to develop lower-extremity vascular disease. Poor food choices and low physical activity levels can lead to persistently elevated A1C levels, which can increase the risk that peripheral nervous system and/or blood vessel disorders will progress. Working Together to Manage Diabetes: A GUIDE FOR PHARMACY, PODIATRY, OPTOMETRY, AND DENTISTRY 53
7 Foot Health and Diabetes A family history of cerebrovascular accidents and coronary artery disease may indicate a further increased risk of developing lowerextremity arterial complications. Inherited foot types (e.g., shapes) may predispose the patient to biomechanical deformities that lead to problems with skin breakdown. Comprehensive Foot Examination A comprehensive foot examination for abnormalities, including evaluation of pulses, sensation, foot biomechanics (i.e., general foot structure and function), and nails, as well as a footwear assessment, helps determine the person s category of risk for developing foot complications. Persons with diabetes who are at high risk have one or more of the following characteristics: Loss of protective sensation Absent pedal pulses Foot deformity History of foot ulcers Prior amputation Foot Risk Status The American Diabetes Association and American Podiatric Medical Association consider two categories of risk for developing foot complications. High Risk (one or more of the following): 1. Loss of protective sensation. 2. Absent pedal pulses. 3. Foot deformity. 4. History of foot ulcers. 5. Prior amputation. Low Risk: None of the above characteristics. See the next box, Highand Low-risk Foot Patient Education, for interventions for patients with high- and low-risk foot status. Low-risk individuals have none of these characteristics. Assessment of risk status identifies people who need more intensive care and evaluation. Further patient education, early intervention, and special footwear, if indicated, can prevent ulcers and ultimately LEAs. To assess risk factors, have the patient remove socks and shoes, and then inspect both feet for acute problems at each visit. 54
8 Patient Education The goal is to prevent low-risk patients from moving to the high-risk category by managing the ABCs (A1C, blood pressure, cholesterol, and smoking cessation). Health care providers can inform all patients about the connection between foot health and diabetes. Encourage patients with diabetes to: Prevent ulcers through self-management education, podiatry care, and use of appropriate footwear. Patients should be taught how to check their own feet every day, including what to look for and when to contact their provider. Get a full foot exam by a podiatrist at least once each year. Patients with diabetes should also make sure their feet are checked at every health care visit. They need to take off their shoes and socks at all visits and be sure to ask for a foot exam. Prevent ulcers through self-management education, podiatry care, and proper use of appropriate footwear. Patients should learn how to check their own feet every day. High- and Low-risk Foot Patient Education The goal for low-risk patients is to keep them low risk by: Controlling the ABCs. Quitting tobacco. The goal for high-risk patients is to prevent foot ulcers by: Educating them on selfmanagement. Stressing the role of minor trauma. Clearing walking spaces of potential hazards. Seeking prompt, same-day care for injuries. Receiving regular podiatry care. Avoid minor foot trauma, such as stubbing a toe, stepping on a sharp object, or experiencing pressure from tight shoes. These can lead to ulcer in patients with diabetes. Be diligent in clearing walking spaces (especially around the bed and the path to the bathroom), using nightlights, and wearing properly fitted shoes. Know when and who to call with specific foot problems. Patients with a puncture wound, ulcer, redness, or new-onset foot pain should call and see their primary care provider or podiatrist that day. Patients with calluses and/or thick or ingrown nails should call a podiatrist and be seen within a few days. Working Together to Manage Diabetes: A GUIDE FOR PHARMACY, PODIATRY, OPTOMETRY, AND DENTISTRY 55
9 Foot Health and Diabetes For a useful exam tool for health care providers, visit NDEP s resource, Feet Can Last a Lifetime: A Health Care Provider s Guide to Preventing Diabetes Foot Problems. For more information for patients, see Diabetes and You: Healthy Feet Matter! and Take Care of Your Feet for a Lifetime Please visit the Resource Center section of the PPOD Guide and Toolkit for other resources on foot health. Key Questions That All Members of the Health Care Team Should Ask Patients About Foot Health Patients should be referred to a podiatrist if the answers to these questions are no or unsure : Do you get a full foot exam by a podiatrist at least once each year? Do you know how diabetes can affect your feet? Do you know how to check your feet every day? Do you check your feet every day? Do you know what to do if you develop foot pain, redness, or sores? Do your shoes fit you correctly? Key Points Podiatrists play a key role in the early identification and treatment of foot problems in people with diabetes. Podiatrists are important in the collaborative interprofessional team care approach for diabetes management. 56
10 References 1. Centers for Disease Control and Prevention. National diabetes fact sheet: National estimates and general information on diabetes and prediabetes in the United States, Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, Johannesson A, Larsson G, Ramstrand N, Turkiewicz A, Wireln AB, Atroshi I. Incidence of lower-limb amputation in the diabetic and nondiabetic general population. Diabetes Care. 2009; 32(2): Sahakyan K, Klein B, Lee K, Myers C, Klein R. The 25-year cumulative incidence of lower extremity amputations in people with type 1 diabetes. Diabetes Care. 2011;34(3): Reiber GE, Boyko EJ, Smith DG, et al. Lower extremity foot ulcers and amputations in diabetes. In: Harris MI, Cowie CC, Stern MP, Boyko EJ, Reiber GE, Bennett PH, eds. Diabetes in America, 2nd edition. Bethesda, MD: National Institutes of Health, 1995; Lavery LA, Van Houtum WH, Harkless LB. In-hospital mortality and disposition of diabetic amputees in the Netherlands. Diabetic Medicine. 1996;13: Armstrong DG, Lavery LA, Harkless LB. Validation of a diabetic wound classification system. The contribution of depth, infection, and ischemia to risk of amputation. Diabetes Care. 1998;21(5): Centers for Disease Control and Prevention. History of foot ulcer among persons with diabetes. MMWR. 2003;52(45): Litzelman DK, Marriott DJ, Vinicor F. Independent physiological predictors of foot lesions in patients with NIDDM. Diabetes Care. 1997;20(8): Boulton AJ, Armstrong DG, Albert SF, et al. Comprehensive foot examination and risk assessment: A report of the Task Force of the Foot Care Interest Group of the American Diabetes Association, with endorsement by the American Association of Clinical Endocrinologists. Diabetes Care. 2008;31(8): Lavery LA, Peters EJ, Williams JR, Murdoch DP, Hudson A, Lavery DC; International Working Group on the Diabetic Foot. Reevaluating the way we classify the diabetic foot: Restructuring the diabetic foot risk classification system of the International Working Group on the Diabetic Foot. Diabetes Care Jan;31(1): Mayfield JA, Reiber GE, Sanders LJ, Janisse D, Pogach LM. Preventive foot care in people with diabetes. Diabetes Care. 1998;21(12): Singh N, Armstrong DG, Lipsky BA. Preventing foot ulcers in patients with diabetes. JAMA. 2005;293(2): Rogers LC, Frykberg RG, Armstrong DG, Bouton AJM, Edmonds M, Ha Van G, et al. The Charcot foot in diabetes. Diabetes Care. 2011; 34(9): Working Together to Manage Diabetes: A GUIDE FOR PHARMACY, PODIATRY, OPTOMETRY, AND DENTISTRY 57
11 Foot Health and Diabetes Gangrene Severe infections may be present but undetected by patients with neuropathy who have difficulty examining their feet. Ulceration of the great toe This deceptively small lesion seriously increases the risk for amputation. Risk factors for amputation include peripheral neuropathy, abnormal biomechanics, peripheral vascular disease, prior ulceration, and prior amputation. Hammer toes The loss of foot musculature has led to abnormal foot biomechanics with the toes drawn up into a hammer toe position. This increases the risk of ulceration and amputation. 58 Peripheral neuropathy Shiny skin, the inability to sweat, and lack of protective sensation compound the risk for amputation in this patient with foot deformity and overriding toes. Treatment includes special footwear, patient education, and vigilant daily foot hygiene and inspection. Ulceration Even large wounds can be painless in the face of neuropathy, and patients may deny there is a problem. The patient with this lesion needs referral for a program of wound management and non-weight-bearing rehabilitation.
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
Diabetes : Foot Education
 Diabetes : Foot Education Dr. Naushira Pandya, M.D., CMD, Sweta Tewary, PhD, MSW Department of Geriatrics Nova Southeastern University Florida Coastal Geriatric Resources, Education, and Training Center
Diabetes : Foot Education Dr. Naushira Pandya, M.D., CMD, Sweta Tewary, PhD, MSW Department of Geriatrics Nova Southeastern University Florida Coastal Geriatric Resources, Education, and Training Center
How can DIABETES affect my FEET? Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust
 How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
How can DIABETES affect my FEET? By: Emma Howard Community Diabetes Lead Podiatrist, Oxford Health NHS Foundation Trust HOW CAN DIABETES AFFECT MY FEET? What is neuropathy? This leaflet explains how diabetes
CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS
 CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS RATIONALE Clinical evidence suggests that there is considerable potential to improve the quality of foot care for people with diabetes.
CLINICAL PROTOCOL FOR THE MANAGEMENT OF FOOT CARE FOR DIABETIC PATIENTS RATIONALE Clinical evidence suggests that there is considerable potential to improve the quality of foot care for people with diabetes.
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS
 APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
APPENDIX 1: INTERDISCIPLINARY APPROACH TO PREVENTION AND MANAGEMENT OF DIABETIC FOOT COMPLICATIONS Template: Regional Foot Programs should develop a list of available health professionals in the following
Treat Your Feet: Foot care for people with diabetes
 Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Treat Your Feet: Foot care for people with diabetes UHN People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to keep your feet healthy. Please visit the UHN Patient
Diabetes Foot Screening and Risk Stratification Tool
 Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Diabetes Foot Screening and Risk Stratification Tool Welcome to the Diabetes Foot Screening and Risk Stratification Tool This tool is based on the work of the Scottish Foot Action Group (SFAG). It has
Critically evaluate the organization of diabetic foot ulcer services and interdisciplinary team working
 Rationale of Module Accurate nursing assessment is the key to effective diabetic foot ulcer prevention, treatment and management. A comprehensive assessment identifies ulcer aetiology and the factors which
Rationale of Module Accurate nursing assessment is the key to effective diabetic foot ulcer prevention, treatment and management. A comprehensive assessment identifies ulcer aetiology and the factors which
WHY DO MY LEGS HURT? Veins, arteries, and other stuff.
 WHY DO MY LEGS HURT? Veins, arteries, and other stuff. Karl A. Illig, MD Professor of Surgery Chief, Division of Vascular Surgery Mitzi Ekers, ARNP April 2013 Why do my legs hurt? CONFLICTS OF INTEREST
WHY DO MY LEGS HURT? Veins, arteries, and other stuff. Karl A. Illig, MD Professor of Surgery Chief, Division of Vascular Surgery Mitzi Ekers, ARNP April 2013 Why do my legs hurt? CONFLICTS OF INTEREST
Facts About Peripheral Arterial Disease (P.A.D.)
 Facts About Peripheral Arterial Disease (P.A.D.) One in every 20 Americans over the age of 50 has P.A.D., a condition that raises the risk for heart attack and stroke. Peripheral arterial disease, or P.A.D.,
Facts About Peripheral Arterial Disease (P.A.D.) One in every 20 Americans over the age of 50 has P.A.D., a condition that raises the risk for heart attack and stroke. Peripheral arterial disease, or P.A.D.,
Podiatric Medicine. What is a Podiatrist?
 Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Page 3 Podiatric Medicine Podiatric Medicine is the profession that strives to improve the overall health and wellbeing of patients by focusing on preventing, diagnosing, and treating conditions associated
Practice Guidelines for the
 1 Treatment goals: Practice Guidelines for the The goal of treatment is to keep blood sugar at normal or near-normal levels. This reduces the risk of complications associated with diabetes. A normal fasting
1 Treatment goals: Practice Guidelines for the The goal of treatment is to keep blood sugar at normal or near-normal levels. This reduces the risk of complications associated with diabetes. A normal fasting
DIABETES A chronic, debilitating and often deadly disease A global epidemic Diabetes in Africa
 DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
DIABETES A chronic, debilitating and often deadly disease Diabetes is a chronic condition that arises when the pancreas does not produce enough insulin, or when the body cannot effectively use the insulin
There are three major forms of this disease.
 For more information about diabetes and it s risk factors, visit our website at: doh.sd.gov/diabetes or visit the South Dakota Diabetes Association at: www.sddiabetescoalition.org/ Your body needs insulin
For more information about diabetes and it s risk factors, visit our website at: doh.sd.gov/diabetes or visit the South Dakota Diabetes Association at: www.sddiabetescoalition.org/ Your body needs insulin
Diabetic Foot Ulcers and Pressure Ulcers. Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences
 Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
The Family Library. Understanding Diabetes
 The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
The Family Library Understanding Diabetes What is Diabetes? Diabetes is caused when the body has a problem in making or using insulin. Insulin is a hormone secreted by the pancreas and is needed for the
Diabetes Brief. Pre diabetes occurs when glucose levels are elevated in the blood, but are not as high as someone who has diabetes.
 Diabetes Brief What is Diabetes? Diabetes mellitus is a disease of abnormal carbohydrate metabolism in which the level of blood glucose, or blood sugar, is above normal. The disease occurs when the body
Diabetes Brief What is Diabetes? Diabetes mellitus is a disease of abnormal carbohydrate metabolism in which the level of blood glucose, or blood sugar, is above normal. The disease occurs when the body
TERMS FOR UNDERSTANDING YOUR TYPE 2 DIABETES. Definitions for Common Terms Related to Type 2 Diabetes
 TERMS FOR UNDERSTANDING YOUR TYPE 2 DIABETES Definitions for Common Terms Related to Type 2 Diabetes TYPE 2 DIABETES AND BLOOD SUGAR 1-3 This list of terms may help you beter understand type 2 diabetes,
TERMS FOR UNDERSTANDING YOUR TYPE 2 DIABETES Definitions for Common Terms Related to Type 2 Diabetes TYPE 2 DIABETES AND BLOOD SUGAR 1-3 This list of terms may help you beter understand type 2 diabetes,
More hospital days are spent treating diabetic foot infections than any other complication of this disease.
 DIABETIC FOOT CARE The disease known as DIABETES MELLITUS affects many parts of the body, especially the feet. It is very important that a diabetic give the feet very special care. A small problem in a
DIABETIC FOOT CARE The disease known as DIABETES MELLITUS affects many parts of the body, especially the feet. It is very important that a diabetic give the feet very special care. A small problem in a
Diabetes Foot: Risk Assessment Education Program Participant s Package
 Diabetes Foot: Risk Assessment Education Program Participant s Package RNAO Developed by a working group of the Alwyn Moyer, Lillian Delmas, Margaret Little, Denise Williams Based on the Registered Nurses
Diabetes Foot: Risk Assessment Education Program Participant s Package RNAO Developed by a working group of the Alwyn Moyer, Lillian Delmas, Margaret Little, Denise Williams Based on the Registered Nurses
NZSSD PodSIG Michele Garrett, Steve York, Claire O Shea, Leigh Shaw, Fiona Angus, Judy Clarke and Karyn Ballance
 Welcome to the Diabetes Foot Screening and Risk Stratification Tool. This tool is based on the work of the Scottish Foot Action Group (SFAG). It has been adapted (with SFAG permission) by the New Zealand
Welcome to the Diabetes Foot Screening and Risk Stratification Tool. This tool is based on the work of the Scottish Foot Action Group (SFAG). It has been adapted (with SFAG permission) by the New Zealand
LUPUS. and the Feet LUPUSUK 2015
 16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
16 LUPUS and the Feet LUPUSUK 2015 LUPUS and the Feet This factsheet explains about some of the foot problems associated with lupus though it is important to remember that not all will develop these problems.
Diabetes Complications
 Diabetes Complications Constant diabetes management is the first key to success when it comes to diabetes complications. We can't stress that enough! Getting control of your blood glucose levels with healthy
Diabetes Complications Constant diabetes management is the first key to success when it comes to diabetes complications. We can't stress that enough! Getting control of your blood glucose levels with healthy
Wound and Skin Assessment. Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center
 Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Medicare Podiatry Services: Information for Medicare Fee-For-Service Health Care Professionals
 R DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services FACT SHEET Medicare Podiatry Services: Information for Medicare Fee-For-Service Health Care Professionals Overview This
R DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services FACT SHEET Medicare Podiatry Services: Information for Medicare Fee-For-Service Health Care Professionals Overview This
Preventing & Managing Complications of Diabetes
 Preventing & Managing Complications of Diabetes Target Audience: Persons with diabetes and family members Objectives: Participants will be able to: 1. identify the complications associated with diabetes
Preventing & Managing Complications of Diabetes Target Audience: Persons with diabetes and family members Objectives: Participants will be able to: 1. identify the complications associated with diabetes
Take Charge of Your Diabetes
 Take Charge of Your Diabetes A Reinforcement Booklet for People With Diabetes Purpose and Acknowledgments This simplified and shortened overview of CDC s 1997 publication, Take Charge of Your Diabetes,
Take Charge of Your Diabetes A Reinforcement Booklet for People With Diabetes Purpose and Acknowledgments This simplified and shortened overview of CDC s 1997 publication, Take Charge of Your Diabetes,
Model of Care for the Diabetic Foot
 Model of Care for the Diabetic Foot National Diabetes Programme Clinical Strategy and Programmes Directorate 2011 Document Control Revision number: 01 Document drafted by: National Diabetes Programme Working
Model of Care for the Diabetic Foot National Diabetes Programme Clinical Strategy and Programmes Directorate 2011 Document Control Revision number: 01 Document drafted by: National Diabetes Programme Working
Diabetes and your feet
 The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
The Society of Chiropodists and Podiatrists Diabetes and your feet A guide to maintaining healthy feet for people with diabetes Diabetes and your feet 3 Diabetes and your feet Many people with diabetes
Modifiers Q7, Q8, and Q9
 1-47 Modifiers Q7, Q8, and Q9 (Routine Foot Care) CPT Modifier Q7 One Class A finding Q8 Two Class B findings Q9 One Class B and two Class C findings General Information The Office of Inspector General
1-47 Modifiers Q7, Q8, and Q9 (Routine Foot Care) CPT Modifier Q7 One Class A finding Q8 Two Class B findings Q9 One Class B and two Class C findings General Information The Office of Inspector General
SEPTEMBER IS P.A.D. AWARENESS MONTH
 NEWSLETTER SEPTEMBER 2014 SEPTEMBER IS P.A.D. AWARENESS MONTH STEVEN PRINGLE, BSN, RN Peripheral Artery Disease, or P.A.D., is a condition that affects the arteries that carry blood to your legs and other
NEWSLETTER SEPTEMBER 2014 SEPTEMBER IS P.A.D. AWARENESS MONTH STEVEN PRINGLE, BSN, RN Peripheral Artery Disease, or P.A.D., is a condition that affects the arteries that carry blood to your legs and other
What Pharmacists Would Like Team Members to Know About Medication Therapy for Diabetes
 What Pharmacists Would Like Team Members to Know About Medication Therapy for Diabetes 38 In this section, you will find an overview of key issues related to medication therapy management and diabetes
What Pharmacists Would Like Team Members to Know About Medication Therapy for Diabetes 38 In this section, you will find an overview of key issues related to medication therapy management and diabetes
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Treatment of diabetes In order to survive, people with type 1 diabetes must have insulin delivered by a pump or injections.
 National Diabetes Statistics What is diabetes? Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action, or both.
National Diabetes Statistics What is diabetes? Diabetes mellitus is a group of diseases characterized by high levels of blood glucose resulting from defects in insulin production, insulin action, or both.
Who Is At Risk of Limb Loss And What To Do About It?
 Journal of Rehabilitation Research and Development Vol. 31 No. 4, November 1994 Pages 357 362 CLINICAL REPORT Who Is At Risk of Limb Loss And What To Do About It? An Invited Presentation at the VA Rehabilitation
Journal of Rehabilitation Research and Development Vol. 31 No. 4, November 1994 Pages 357 362 CLINICAL REPORT Who Is At Risk of Limb Loss And What To Do About It? An Invited Presentation at the VA Rehabilitation
Improving the Compliance of the Annual Foot Examination and Monofilament Testing in
 Improving the Compliance of the Annual Foot Examination and Monofilament Testing in Diabetic Patients at Centromed Principal Investigator: Velen Tat, Physician Assistant Student 2016, University of Southern
Improving the Compliance of the Annual Foot Examination and Monofilament Testing in Diabetic Patients at Centromed Principal Investigator: Velen Tat, Physician Assistant Student 2016, University of Southern
PLANTAR FASCITIS (Heel Spur Syndrome)
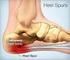 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
This article discusses concerns amputees may have
 The War Amps For Your Information Tel.: 1 877 622-2472 Fax: 1 855 860-5595 Diabetes Diabetes presents very specific issues for amputees. Healthy Living for Amputees This article discusses concerns amputees
The War Amps For Your Information Tel.: 1 877 622-2472 Fax: 1 855 860-5595 Diabetes Diabetes presents very specific issues for amputees. Healthy Living for Amputees This article discusses concerns amputees
Previous history of ulcers on feet which were alleviated by introduction of Propet stretch shoes
 EDP- A case study for Vasyli medical trialling diabetic insole and Dr Comfort footwear BY SALLY LAXTON BAppSci(Pod) PODIATRIST- Knox Community Health Service EDP is a 68 year old female solid build Medical
EDP- A case study for Vasyli medical trialling diabetic insole and Dr Comfort footwear BY SALLY LAXTON BAppSci(Pod) PODIATRIST- Knox Community Health Service EDP is a 68 year old female solid build Medical
Disability Evaluation Under Social Security
 Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
Disability Evaluation Under Social Security Revised Medical Criteria for Evaluating Endocrine Disorders Effective June 7, 2011 Why a Revision? Social Security revisions reflect: SSA s adjudicative experience.
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS)
 SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
SCRIPT NUMBER 122 VARICOSE VEINS - 2 (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: VARICOSE VEINS - 2 PROGRAM NUMBER: 122 SUBJECT: SYMPTOMS, CAUSES, TREATMENT, PREVENTION OF VARICOSE VEINS
Type 2 Diabetes. Increase of diabetic complications as HAIC increases
 Type 2 Diabetes Diabetes is a disease of too much sugar (glucose) in the blood. Type 2 diabetes is caused by insulin resistance of the cells and abnormal insulin production by the pancreas. Insulin is
Type 2 Diabetes Diabetes is a disease of too much sugar (glucose) in the blood. Type 2 diabetes is caused by insulin resistance of the cells and abnormal insulin production by the pancreas. Insulin is
This is caused by muscle strain to the Achilles tendon in the heel of the foot.
 Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Louisiana State Board of Nursing
 Louisiana State Board of Nursing DECLARATORY STATEMENT ON THE ROLE AND SCOPE OF PRACTICE OF THE REGISTERED NURSE IN PERFORMING FOOT CARE INTERVENTIONS Preamble The Louisiana State Board of Nursing believes
Louisiana State Board of Nursing DECLARATORY STATEMENT ON THE ROLE AND SCOPE OF PRACTICE OF THE REGISTERED NURSE IN PERFORMING FOOT CARE INTERVENTIONS Preamble The Louisiana State Board of Nursing believes
Plantar Fasciitis. Plantar Fascia
 Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Halloween Costume Ideas - The Ultimate Party Planning Formula
 Patient Type 2 Diabetes Aboriginal Health Workers Audiologists Chiropractors Diabetes Educators Dietitians Exercise Physiologists Mental Health Nurses Mental Health Social Workers Occupational Therapists
Patient Type 2 Diabetes Aboriginal Health Workers Audiologists Chiropractors Diabetes Educators Dietitians Exercise Physiologists Mental Health Nurses Mental Health Social Workers Occupational Therapists
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Post-Transplant Diabetes: What Every Patient Needs to Know
 Post-Transplant Diabetes: What Every Patient Needs to Know International Transplant Nurses Society What is Diabetes? Diabetes is an illness that effects how your body makes and uses a hormone called insulin.
Post-Transplant Diabetes: What Every Patient Needs to Know International Transplant Nurses Society What is Diabetes? Diabetes is an illness that effects how your body makes and uses a hormone called insulin.
WorryFree DME SM Diabetic Shoe Order Entry Form
 WorryFree DME SM Diabetic Shoe Order Entry Form Non-Physician Supplier Medicare Compliance Documentation Guide Shoe Fitter Responsibility/Actions 1. Complete Patient Evaluation Prior to Shoe Selection.
WorryFree DME SM Diabetic Shoe Order Entry Form Non-Physician Supplier Medicare Compliance Documentation Guide Shoe Fitter Responsibility/Actions 1. Complete Patient Evaluation Prior to Shoe Selection.
Imagine LIFE WITHOUT PAIN
 Imagine LIFE WITHOUT PAIN High Dosage Laser Therapy (HDLT) What does it do? High Dosage Laser Therapy (HDLT) from Diowave offers a powerful new solution for numerous painful conditions previously refractive
Imagine LIFE WITHOUT PAIN High Dosage Laser Therapy (HDLT) What does it do? High Dosage Laser Therapy (HDLT) from Diowave offers a powerful new solution for numerous painful conditions previously refractive
Background (cont) World Health Organisation (WHO) and IDF predict that this number will increase to more than 1,3 million in the next 25 years.
 Diabetes Overview Background What is diabetes Non-modifiable risk factors Modifiable risk factors Common symptoms of diabetes Early diagnosis and management of diabetes Non-medical management of diabetes
Diabetes Overview Background What is diabetes Non-modifiable risk factors Modifiable risk factors Common symptoms of diabetes Early diagnosis and management of diabetes Non-medical management of diabetes
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
Graduated compression hosiery (stockings)
 What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
What is compression hosiery? Compression hosiery are elasticated stockings which give support to your legs. In graduated compression hosiery, the pressure given by the stockings is greater at the ankle
Patients suffering from critical limb ischemia (CLI)
 Building a Successful Amputation Prevention Program Our single-center experience implementing an amputation prevention algorithm and how it has led to a trend in reduced amputation rates. By Jihad A. Mustapha,
Building a Successful Amputation Prevention Program Our single-center experience implementing an amputation prevention algorithm and how it has led to a trend in reduced amputation rates. By Jihad A. Mustapha,
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Healthy at Heart FEELING GOOD. Reduce Your CV Risk. It s Not Just Your Body. It s Your Outlook, Too. Issue 3
 Issue 3 Healthy at Heart Reduce Your CV Risk FEELING GOOD It s Not Just Your Body. It s Your Outlook, Too. Inside: Tips for staying active and feeling good all over Speak to your healthcare provider before
Issue 3 Healthy at Heart Reduce Your CV Risk FEELING GOOD It s Not Just Your Body. It s Your Outlook, Too. Inside: Tips for staying active and feeling good all over Speak to your healthcare provider before
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study
 DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
DCCT and EDIC: The Diabetes Control and Complications Trial and Follow-up Study National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What
DIABETES MELLITUS. By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria
 DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
DIABETES MELLITUS By Tracey Steenkamp Biokineticist at the Institute for Sport Research, University of Pretoria What is Diabetes Diabetes Mellitus (commonly referred to as diabetes ) is a chronic medical
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Wade Steeves MD Board Certified Neurologist Rockwood Clinic DIABETIC PERIPHERAL NEUROPATHY
 Wade Steeves MD Board Certified Neurologist Rockwood Clinic DIABETIC PERIPHERAL NEUROPATHY NERVOUS SYSTEM OVERVIEW Diabetic neuropathies This is a family of nerve disorders caused by diabetes. Diabetes
Wade Steeves MD Board Certified Neurologist Rockwood Clinic DIABETIC PERIPHERAL NEUROPATHY NERVOUS SYSTEM OVERVIEW Diabetic neuropathies This is a family of nerve disorders caused by diabetes. Diabetes
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Podo Pediatrics Identifying Biomechanical Pathologies
 Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Heel pain and Plantar fasciitis
 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
Plantar Fascia Release
 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Nutrition. Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT
 1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
1 Nutrition Type 2 Diabetes: A Growing Challenge in the Healthcare Setting NAME OF STUDENT 2 Type 2 Diabetes: A Growing Challenge in the Healthcare Setting Introduction and background of type 2 diabetes:
Rheumatoid Arthritis of the Foot and Ankle
 Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs
 T H E F A C T S A B O U T Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs Upstate New York Adults with diagnosed diabetes: 2003: 295,399 2008: 377,280 diagnosed
T H E F A C T S A B O U T Upstate New York adults with diagnosed type 1 and type 2 diabetes and estimated treatment costs Upstate New York Adults with diagnosed diabetes: 2003: 295,399 2008: 377,280 diagnosed
Therapeutic shoes (for individuals with diabetes) and foot (in-shoe) orthotics are reimbursable under Plans administered by QualCare, Inc.
 Subject: Foot Orthotics and Diabetic Shoes* Effective Date: October 1, 1999 Department(s): Utilization Management Policy: Objective: Procedure: Therapeutic shoes (for individuals with diabetes) and foot
Subject: Foot Orthotics and Diabetic Shoes* Effective Date: October 1, 1999 Department(s): Utilization Management Policy: Objective: Procedure: Therapeutic shoes (for individuals with diabetes) and foot
Working Feet. A practical guide to looking after your feet at work. www.feetforlife.org. The Society of Chiropodists and Podiatrists
 Working Feet A practical guide to looking after your feet at work The Society of Chiropodists and Podiatrists Your feet bear the brunt of your daily working life Contents Feet at work... 3 Foot pain...
Working Feet A practical guide to looking after your feet at work The Society of Chiropodists and Podiatrists Your feet bear the brunt of your daily working life Contents Feet at work... 3 Foot pain...
Podiatry Specialty ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Podiatry and Top 20 codes
 Podiatry Specialty ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Podiatry and Top 20 codes Chapter 1 Certain Infectious and Parasitic Diseases Terminology changes: The term sepsis (ICD-10-CM)
Podiatry Specialty ICD-10-CM Coding Tip Sheet Overview of Key Chapter Updates for Podiatry and Top 20 codes Chapter 1 Certain Infectious and Parasitic Diseases Terminology changes: The term sepsis (ICD-10-CM)
Connecticut Diabetes Statistics
 Connecticut Diabetes Statistics What is Diabetes? State Public Health Actions (1305, SHAPE) Grant March 2015 Page 1 of 16 Diabetes is a disease in which blood glucose levels are above normal. Blood glucose
Connecticut Diabetes Statistics What is Diabetes? State Public Health Actions (1305, SHAPE) Grant March 2015 Page 1 of 16 Diabetes is a disease in which blood glucose levels are above normal. Blood glucose
Lower extremity ulcers and amputations are an
 Chapter 18 Lower Extremity Foot Ulcers and Amputations in Diabetes Gayle E. Reiber, MPH, PhD; Edward J. Boyko, MD, MPH; and Douglas G. Smith, MD SUMMARY Lower extremity ulcers and amputations are an increasing
Chapter 18 Lower Extremity Foot Ulcers and Amputations in Diabetes Gayle E. Reiber, MPH, PhD; Edward J. Boyko, MD, MPH; and Douglas G. Smith, MD SUMMARY Lower extremity ulcers and amputations are an increasing
Diabetes 101. Francisco J. Prieto, M.D. American Diabetes Association National Advocacy Committee Latino Diabetes Action Council
 Diabetes 101 Francisco J. Prieto, M.D. American Diabetes Association National Advocacy Committee Latino Diabetes Action Council www.diabetes.org 1-800-DIABETES www.diabetes.org 1-800-DIABETES Age-Adjusted
Diabetes 101 Francisco J. Prieto, M.D. American Diabetes Association National Advocacy Committee Latino Diabetes Action Council www.diabetes.org 1-800-DIABETES www.diabetes.org 1-800-DIABETES Age-Adjusted
DIABETES CARE. Advice. Blood Pressure. Cholesterol. Diabetes control. Eyes. Feet. Guardian Drugs
 DIABETES CARE What happens if you follow the Alphabet Strategy? As patients reach their targets, the chances of developing serious complications of diabetes will be reduced! 1 Stroke Eye disease Heart
DIABETES CARE What happens if you follow the Alphabet Strategy? As patients reach their targets, the chances of developing serious complications of diabetes will be reduced! 1 Stroke Eye disease Heart
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
An Integrated, Holistic Approach to Care Management Blue Care Connection
 An Integrated, Holistic Approach to Care Management Blue Care Connection With health care costs continuing to rise, both employers and health plans need innovative solutions to help employees manage their
An Integrated, Holistic Approach to Care Management Blue Care Connection With health care costs continuing to rise, both employers and health plans need innovative solutions to help employees manage their
Diabetes Complications
 Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
Managing Diabetes: It s s Not Easy But It s s Worth It Presenter Disclosures W. Lee Ball, Jr., OD, FAAO (1) The following personal financial relationships with commercial interests relevant to this presentation
TakeCHARGE. Diabetes. Community Health Reports. Personal actions for better health
 TakeCHARGE Community Health Reports Personal actions for better health Diabetes A nonprofit independent licensee of the BlueCross BlueShield Association Are we taking charge of our own health? Most of
TakeCHARGE Community Health Reports Personal actions for better health Diabetes A nonprofit independent licensee of the BlueCross BlueShield Association Are we taking charge of our own health? Most of
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
ASSESSMENT/DIAGNOSIS. Complete history Nutritional Assessment. Vascular Assessment ABI + toe pressures Early referral to vascular surgeon if indicated
 DIABETIC FOOT ULCER ASSESSMENT AND MANAGEMENT ALGORITHM ASSESSMENT/DIAGNOSIS Complete history Nutritional Assessment Assess for Infection +/- culture swab CBC X-ray/ESR to rule out osteomyelitis Probe
DIABETIC FOOT ULCER ASSESSMENT AND MANAGEMENT ALGORITHM ASSESSMENT/DIAGNOSIS Complete history Nutritional Assessment Assess for Infection +/- culture swab CBC X-ray/ESR to rule out osteomyelitis Probe
Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused by too little insulin, resistance to insulin, or both.
 Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
Diabetes Definition Diabetes is a chronic (lifelong) disease marked by high levels of sugar in the blood. Causes Insulin is a hormone produced by the pancreas to control blood sugar. Diabetes can be caused
F e e t Ca n La s t. A Health Care Provider s Guide to Preventing Diabetes Foot Problems
 F e e t Ca n La s t a Li fet i m e A Health Care Provider s Guide to Preventing Diabetes Foot Problems F eet Can Last A Lifetime was produced by the National Diabetes Education Program (NDEP). The NDEP
F e e t Ca n La s t a Li fet i m e A Health Care Provider s Guide to Preventing Diabetes Foot Problems F eet Can Last A Lifetime was produced by the National Diabetes Education Program (NDEP). The NDEP
Statistics of Type 2 Diabetes
 Statistics of Type 2 Diabetes Of the 17 million Americans with diabetes, 90 percent to 95 percent have type 2 diabetes. Of these, half are unaware they have the disease. People with type 2 diabetes often
Statistics of Type 2 Diabetes Of the 17 million Americans with diabetes, 90 percent to 95 percent have type 2 diabetes. Of these, half are unaware they have the disease. People with type 2 diabetes often
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
MAGDALENA ANNERSTEN GERSHATER PREVENTION OF FOOT ULCERS IN PATIENTS with DIABETES MELLITUS
 MALMÖ UNIVERSITY HEALTH AND SOCIETY DOCTORAL DISSERTATION 2011:5 MAGDALENA ANNERSTEN GERSHATER PREVENTION OF FOOT ULCERS IN PATIENTS with DIABETES MELLITUS Nursing in outpatient settings PREVENTION OF
MALMÖ UNIVERSITY HEALTH AND SOCIETY DOCTORAL DISSERTATION 2011:5 MAGDALENA ANNERSTEN GERSHATER PREVENTION OF FOOT ULCERS IN PATIENTS with DIABETES MELLITUS Nursing in outpatient settings PREVENTION OF
John M. Sigle, DPM, FACFAS Foot & Ankle Center of Illinois (217) 787-2700 www.myfootandanklecenter.com
 The MiToe implant is manufactured by Wright Medical, the recognized leader of surgical solutions for foot and ankle. Wright has been in business for more than 60 years and markets products in over 60 countries,
The MiToe implant is manufactured by Wright Medical, the recognized leader of surgical solutions for foot and ankle. Wright has been in business for more than 60 years and markets products in over 60 countries,
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Integra. Subtalar MBA Implant
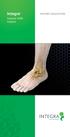 Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933
 Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933 www.grhsonline.org Important Notice The information contained in this document is for informational
Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933 www.grhsonline.org Important Notice The information contained in this document is for informational
Other Noninfectious Diseases. Chapter 31 Lesson 3
 Other Noninfectious Diseases Chapter 31 Lesson 3 Diabetes Diabetes- a chronic disease that affects the way body cells convert food into energy. Diabetes is the seventh leading cause of death by disease
Other Noninfectious Diseases Chapter 31 Lesson 3 Diabetes Diabetes- a chronic disease that affects the way body cells convert food into energy. Diabetes is the seventh leading cause of death by disease
Rheumatoid Arthritis: Symptoms, Causes, and Treatments of Rheumatoid Foot and Ankle
 Rheumatoid arthritis is the most common form of inflammatory arthritis, affecting about two to three million Americans. Rheumatoid arthritis is a symmetric disease, meaning that it will usually involve
Rheumatoid arthritis is the most common form of inflammatory arthritis, affecting about two to three million Americans. Rheumatoid arthritis is a symmetric disease, meaning that it will usually involve
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Type 2 diabetes Definition
 Type 2 diabetes Definition Type 2 diabetes is a lifelong (chronic) disease in which there are high levels of sugar (glucose) in the blood. Type 2 diabetes is the most common form of diabetes. Causes Diabetes
Type 2 diabetes Definition Type 2 diabetes is a lifelong (chronic) disease in which there are high levels of sugar (glucose) in the blood. Type 2 diabetes is the most common form of diabetes. Causes Diabetes
Markham Stouffville Hospital
 Markham Stouffville Hospital Adult Diabetes Education Frequently Asked Questions What is diabetes? Diabetes is a disease in which blood glucose levels are above normal. Most of the food we eat is turned
Markham Stouffville Hospital Adult Diabetes Education Frequently Asked Questions What is diabetes? Diabetes is a disease in which blood glucose levels are above normal. Most of the food we eat is turned
X-Plain Diabetes - Introduction Reference Summary
 X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
X-Plain Diabetes - Introduction Reference Summary Introduction Diabetes is a disease that affects millions of Americans every year. Your doctor may have informed you that you have diabetes. Although there
CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY
 CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY What is GSC s new orthotics and orthopedic shoe policy? Only certain health professionals can prescribe and provide you with custom orthotics, orthopedic shoes,
CUSTOM ORTHOTICS/SHOES FAQ AND GLOSSARY What is GSC s new orthotics and orthopedic shoe policy? Only certain health professionals can prescribe and provide you with custom orthotics, orthopedic shoes,
