Medications Requiring Prior Authorization for Medical Necessity
|
|
|
- Samantha Powell
- 9 years ago
- Views:
Transcription
1 January 2017 Medications Requiring Prior Medical Necessity Below is a list of medicines by drug class that will not be covered without a prior authorization for medical necessity, effective January 1, If you continue using one of these drugs without prior approval for medical necessity, you may be required to pay the full cost. If you are currently using one of the drugs requiring prior authorization for medical necessity, ask your doctor to choose one of the generic or brand formulary options listed below. Bolded products represent drugs requiring prior authorization for medical necessity that are new for the 2017 plan year. Category * Allergic Reaction (Anaphylaxis) Treatment * Allergies * Nasal Steroids / Allergies * Ophthalmic Anti-infectives, Antivirals * Cytomegalovirus Agents Anti-infectives, Antivirals * Hepatitis C Agents Anti-infectives, Antivirals * Herpes Agents Antiobesity Agents * Newer Agents Asthma * Beta Agonists, Short-Acting Asthma * Steroid Inhalants Asthma * or Chronic Obstructive Pulmonary Disease (COPD) * Steroid / Beta Agonist Attention Deficit Hyperactivity Disorder Agents * Cancer * Chronic Myelogenous Leukemia Agents ADRENACLICK BECONASE AQ OMNARIS QNASL RHINOCORT AQUA VERAMYST ZETONNA LASTACAFT VALCYTE DAKLINZA OLYSIO TECHNIVIE VIEKIRA PAK ZEPATIER VALTREX QSYMIA PROVENTIL HFA VENTOLIN HFA XOPENEX HFA AEROSPAN ALVESCO SYMBICORT ADDERALL XR INTUNIV GLEEVEC TASIGNA EPIPEN, EPIPEN JR flunisolide spray, fluticasone spray, triamcinolone spray, DYMISTA azelastine, cromolyn sodium, olopatadine, PATADAY, PAZEO valganciclovir EPCLUSA, HARVONI, SOVALDI acyclovir, valacyclovir BELVIQ, CONTRAVE, SAXENDA PROAIR HFA, PROAIR RESPICLICK ASMANEX, FLOVENT, PULMICORT FLEXHALER, QVAR ADVAIR, BREO ELLIPTA, DULERA amphetamine-dextroamphetamine mixed salts, amphetamine-dextroamphetamine mixed salts ext-rel, guanfacine ext-rel, methylphenidate, methylphenidate ext-rel, APTENSIO XR, QUILLIVANT XR, STRATTERA, VYVANSE imatinib mesylate, BOSULIF, SPRYCEL
2 Cancer * Prostate Hormonal Agents, Antiandrogens Cardiovascular Antilipemics * Fibrates Cardiovascular Antilipemics * HMG-CoA Reductase Inhibitors (HMGs or Statins) / Cardiovascular Potassium Supplements * Cardiovascular Pulmonary Arterial Hypertension Agents * Endothelin Receptor Antagonists Carnitine Deficiency Agents * Chronic Obstructive Pulmonary Disease (COPD) * Anticholinergics Cystic Fibrosis * Inhaled Antibiotics Depression * Antidepressants, Selective Norepinephrine Reuptake Inhibitors (SNRIs) Depression * Antidepressants, Miscellaneous Agents Depression *, Schizophrenia * Antipsychotics, Atypicals Dermatology Actinic Keratosis * Dermatology Rosacea * Dermatology Skin Inflammation and Hives * Corticosteroids Dermatology Miscellaneous Skin Conditions * NILANDRON XTANDI TRICOR ADVICOR ALTOPREV CRESTOR LESCOL XL LIPITOR LIPTRUZET LIVALO KLOR-CON/25 OPSUMIT CARNITOR CARNITOR SF INCRUSE ELLIPTA TUDORZA TOBI TOBI PODHALER venlafaxine ext-rel tablet (except 225 mg) CYMBALTA OLEPTRO ABILIFY fluorouracil cream 0.5% CARAC NORITATE clobetasol spray CLOBEX SPRAY OLUX-E APEXICON E ALCORTIN A ALOQUIN NOVACORT bicalutamide, ZYTIGA fenofibrate, fenofibric acid atorvastatin, fluvastatin, lovastatin, pravastatin, rosuvastatin, simvastatin, VYTORIN potassium chloride liquid LETAIRIS, TRACLEER levocarnitine SPIRIVA tobramycin inhalation solution, BETHKIS duloxetine, venlafaxine, venlafaxine ext-rel capsule, PRISTIQ trazodone aripiprazole, clozapine, olanzapine, quetiapine, risperidone, ziprasidone, LATUDA, SEROQUEL XR fluorouracil cream 5%, fluorouracil solution, imiquimod, PICATO, ZYCLARA metronidazole, sulfacetamide-sulfur, FINACEA, SOOLANTRA clobetasol foam desoximetasone, fluocinonide hydrocortisone
3 Biguanides Dipeptidyl Peptidase-4 (DPP-4) Inhibitors Dipeptidyl Peptidase-4 (DPP-4) Inhibitor Injectable Incretin Mimetics FORTAMET GLUMETZA RIOMET NESINA ONGLYZA KAZANO KOMBIGLYZE XR OSENI BYDUREON BYETTA metformin, metformin ext-rel JANUVIA, TRADJENTA JANUMET, JANUMET XR, JENTADUETO, JENTADUETO XR TRULICITY, VICTOZA Insulins APIDRA HUMALOG NOVOLOG HUMALOG MIX 50/50 NOVOLOG MIX 70/30 HUMALOG MIX 75/25 NOVOLOG MIX 70/30 HUMULIN 70/30 2 NOVOLIN 70/30 2 HUMULIN N 2 NOVOLIN N 2 HUMULIN R 2 NOVOLIN R 2 NOTE: Humulin R U-500 concentrate vial will not be subject to prior authorization and will continue to be covered. Long Acting Insulins Insulin Sensitizers Sodium-Glucose Co-transporter 2 (SGLT2) Inhibitors Sodium-Glucose Co-transporter 2 (SGLT2) Inhibitor / Biguanide Supplies, Pen Needles Supplies, Syringes LANTUS TOUJEO ACTOS INVOKANA INVOKAMET ALLISON MEDICAL PEN NEEDLES NOVO NORDISK PEN NEEDLES ULTIMED PEN NEEDLES All other insulin pen needles that are not BD brand ALLISON MEDICAL INSULIN SYRINGES TRIVIDIA INSULIN SYRINGES ULTIMED INSULIN SYRINGES All other insulin syringes that are not BD brand BASAGLAR, LEVEMIR, TRESIBA pioglitazone FARXIGA, JARDIANCE XIGDUO XR BD PEN NEEDLES BD INSULIN SYRINGES
4 Supplies, Test Strips and Kits 3, 4 Erectile Dysfunction * Phosphodiesterase Inhibitors Gastrointestinal Agents * Opioid-induced Constipation Gastrointestinal Agents * Proton Pump Inhibitors (PPIs) Glaucoma * Prostaglandin Analogs Growth Hormones * Hematologic Anticoagulants (oral) * Hematologic Hemophilia Agents * Hematologic * Neutropenia Colony Stimulating Factors Hematologic * Platelet Aggregation Inhibitors Angiotensin II Receptor Antagonists Angiotensin II Receptor Antagonist / Diuretic Angiotensin II Receptor Antagonist / Calcium Channel Blocker Angiotensin II Receptor Antagonist / Calcium Channel Blocker / Diuretic Beta-blocker ACCU-CHEK STRIPS AND KITS BREEZE 2 STRIPS AND KITS CONTOUR NEXT STRIPS AND KITS CONTOUR STRIPS AND KITS FREESTYLE STRIPS AND KITS All other test strips that are not ONETOUCH brand LEVITRA VIAGRA RELISTOR NEXIUM PREVACID PROTONIX ZEGERID LUMIGAN GENOTROPIN NUTROPIN AQ OMNITROPE SAIZEN PRADAXA HELIXATE FS NEUPOGEN PLAVIX ATACAND DIOVAN EDARBI TEVETEN ATACAND HCT DIOVAN HCT EDARBYCLOR TEVETEN HCT EXFORGE EXFORGE HCT DUTOPROL ONETOUCH ULTRA STRIPS AND KITS 3, ONETOUCH VERIO STRIPS AND KITS 3 CIALIS MOVANTIK esomeprazole, lansoprazole, omeprazole, omeprazole-sodium bicarbonate capsule, pantoprazole, DEXILANT latanoprost, travoprost, TRAVATAN Z, ZIOPTAN HUMATROPE, NORDITROPIN warfarin, ELIQUIS, XARELTO KOGENATE FS ZARXIO clopidogrel, BRILINTA, EFFIENT candesartan, eprosartan, irbesartan, losartan, telmisartan, valsartan, BENICAR candesartan-hydrochlorothiazide, irbesartan-hydrochlorothiazide, losartanhydrochlorothiazide, telmisartan-hydrochlorothiazide, valsartan-hydrochlorothiazide, BENICAR HCT amlodipine-telmisartan, amlodipine-valsartan, AZOR amlodipine-valsartan-hydrochlorothiazide, TRIBENZOR metoprolol succinate ext-rel WITH hydrochlorothiazide
5 Calcium Channel Blockers NORVASC CARDIZEM CARDIZEM CD CARDIZEM LA (and its generics) Matzim LA amlodipine diltiazem ext-rel (except generic of CARDIZEM LA) Huntington's Disease Agents * XENAZINE tetrabenazine Inflammatory Bowel Disease (IBD), Ulcerative Colitis * Aminosalicylates Kidney Disease * Phosphate Binders Multiple Sclerosis Agents * ASACOL HD DELZICOL FOSRENOL AVONEX EXTAVIA PLEGRIDY balsalazide, sulfasalazine, sulfasalazine delayed-rel, APRISO, LIALDA, PENTASA, UCERIS calcium acetate, PHOSLYRA, RENVELA, VELPHORO glatiramer, AUBAGIO, BETASERON, COPAXONE 40 MG, GILENYA, REBIF, TECFIDERA Musculoskeletal Agents * AMRIX cyclobenzaprine Opioid Dependence Agents * ZUBSOLV buprenorphine-naloxone sublingual tablet, SUBOXONE FILM Opioid Reversal Agents * EVZIO NARCAN NASAL SPRAY Osteoarthritis * Viscosupplements Overactive Bladder / Incontinence * Urinary Antispasmodics Pain * Headache Agents Pain * Transmucosal Immediaterelease Fentanyl Agents Pain and Inflammation * Corticosteroids Pain and Inflammation * Nonsteroidal Antiinflammatory Drugs (NSAIDs) / Prostate Condition * Benign Prostatic Hyperplasia Agents / Sleep * Hypnotics, Nonbenzodiazepines Testosterone Replacement * Androgens EUFLEXXA MONOVISC ORTHOVISC DETROL LA ENABLEX GELNIQUE OXYTROL butalbital-acetaminophen-caffeine capsule ABSTRAL DEXPAK MILLIPRED RAYOS ARTHROTEC PENNSAID NAPRELAN JALYN INTERMEZZO LUNESTA ROZEREM testosterone gel 1% 5 ANDROGEL FORTESTA NATESTO TESTIM VOGELXO GEL-ONE, HYALGAN, SUPARTZ FX oxybutynin ext-rel, tolterodine, tolterodine ext-rel, trospium, trospium ext-rel, MYRBETRIQ, TOVIAZ, VESICARE naratriptan, rizatriptan, sumatriptan, zolmitriptan, RELPAX, ZOMIG NASAL SPRAY fentanyl transmucosal lozenge, FENTORA, SUBSYS dexamethasone, methylprednisolone, prednisone celecoxib; diclofenac sodium, meloxicam or naproxen WITH esomeprazole, lansoprazole, omeprazole, omeprazole-sodium bicarbonate capsule, pantoprazole or DEXILANT diclofenac sodium, diclofenac sodium solution, meloxicam, naproxen, VOLTAREN GEL celecoxib, diclofenac sodium, meloxicam, naproxen dutasteride or finasteride WITH alfuzosin ext-rel, doxazosin, tamsulosin, terazosin or RAPAFLO eszopiclone, zolpidem, zolpidem ext-rel, SILENOR ANDRODERM, AXIRON
6 Autoimmune and Hepatitis C * Generics Hyperinflation New-to-Market Agents 1 Specialty For Autoimmune and Hepatitis C, CVS Caremark will be implementing an Indication Based Formulary for 2017 which may result in additional exclusions announced in both classes. Limited source generics may be evaluated when appropriate and potentially excluded. Products with significant cost inflation throughout the year may be evaluated and potentially excluded. New-to-market products and new variations of products already in the marketplace will not be added to the formulary until the product has been evaluated, determined to be clinically appropriate and cost-effective, and approved by the CVS Caremark Pharmacy and Therapeutics Committee (or other appropriate reviewing body). As new specialty products launch, all existing products in the class will be re-evaluated to determine appropriate formulary placement and potentially excluded, added back to formulary or not listed. The listed formulary options are subject to change. List of Medical Necessity - Carry Over from 2016 ABILIFY ACCU-CHEK STRIPS AND KITS 4 ACTOS ADDERALL XR ADRENACLICK ADVICOR AEROSPAN ALTOPREV ALVESCO AMRIX ANDROGEL APEXICON E APIDRA ARTHROTEC ASACOL HD ATACAND ATACAND HCT AVONEX BECONASE AQ BREEZE 2 STRIPS AND KITS 4 BYDUREON BYETTA CARAC CARDIZEM CARDIZEM CD CARDIZEM LA (and its generics) clobetasol spray CLOBEX SPRAY CONTOUR NEXT STRIPS AND KITS 4 CONTOUR STRIPS AND KITS 4 CYMBALTA DELZICOL DETROL LA DIOVAN DIOVAN HCT EDARBI EDARBYCLOR EUFLEXXA EXFORGE EXFORGE HCT EXTAVIA fluorouracil cream 0.5% FORTAMET FORTESTA FOSRENOL FREESTYLE STRIPS AND KITS 4 GENOTROPIN GLUMETZA HUMALOG HUMALOG MIX 50/50 HUMALOG MIX 75/25 HUMULIN 70/30 2 HUMULIN N 2 HUMULIN R 2 INCRUSE ELLIPTA INTERMEZZO INTUNIV INVOKAMET INVOKANA JALYN KAZANO KOMBIGLYZE XR LASTACAFT LESCOL XL LEVITRA LIPITOR LIPTRUZET LIVALO LUMIGAN LUNESTA Matzim LA MONOVISC NAPRELAN NATESTO NESINA NORITATE NORVASC NUTROPIN AQ OLEPTRO OLUX-E OMNARIS OMNITROPE ONGLYZA ORTHOVISC OSENI OXYTROL PENNSAID PLAVIX PLEGRIDY PREVACID PROTONIX QNASL QSYMIA RAYOS RELISTOR RHINOCORT AQUA RIOMET ROZEREM SAIZEN SYMBICORT TESTIM testosterone gel 1% 5 TEVETEN TEVETEN HCT TRICOR TUDORZA VALCYTE VALTREX VERAMYST VIAGRA VIEKIRA PAK VOGELXO XOPENEX HFA ZETONNA ZUBSOLV
7 List of Medical Necessity - New for 2017 ABSTRAL ALCORTIN A ALOQUIN ALLISON MEDICAL INSULIN SYRINGES ALLISON MEDICAL PEN NEEDLES butalbital-acetaminophen-caffeine capsule CARNITOR CARNITOR SF CRESTOR DAKLINZA DEXPAK DUTOPROL ENABLEX EVZIO GELNIQUE GLEEVEC HELIXATE FS KLOR-CON/25 LANTUS MILLIPRED NEUPOGEN NEXIUM NILANDRON NOVACORT NOVO NORDISK PEN NEEDLES OLYSIO OPSUMIT PRADAXA PROVENTIL HFA TASIGNA TECHNIVIE TOBI TOBI PODHALER TOUJEO TRIVIDIA INSULIN SYRINGES ULTIMED INSULIN SYRINGES ULTIMED PEN NEEDLES venlafaxine ext-rel tablets (except for 225 mg) VENTOLIN HFA XENAZINE XTANDI ZEGERID ZEPATIER
8 There may be additional drugs subject to prior authorization or other plan design restrictions. Please consult your plan for further information. This list represents brand products in CAPS, branded generics in upper- and lowercase Italics, and generic products in lowercase italics. This is not an all-inclusive list of available drug options. Log in to to check coverage and copay information for a specific drug. Discuss this information with your doctor or health care provider. This information is not a substitute for medical advice or treatment. Talk to your doctor or health care provider about this information and any health-related questions you have. CVS Caremark assumes no liability whatsoever for the information provided or for any diagnosis or treatment made as a result of this information. This list is subject to change. Subject to applicable laws and regulations. * This list indicates the common uses for which the drug is prescribed. Some drugs are prescribed for more than one condition. 1 If your doctor believes you have a specific clinical need for one of these products, he or she should contact the Prior Authorization department at: Rebranded or private label formulations are not covered without a prior authorization for medical necessity (i.e., RELION). 3 A ONETOUCH blood glucose meter may be provided at no charge by the manufacturer to those individuals currently using a meter other than ONETOUCH. For more information on how to obtain a blood glucose meter, call: ONETOUCH brand test strips are the only preferred options. 5 Listing reflects the authorized generics for TESTIM and VOGELXO. Your privacy is important to us. Our employees are trained regarding the appropriate way to handle your private health information. This document contains confidential and proprietary information of CVS Caremark and cannot be reproduced, distributed or printed without written permission from CVS Caremark. CVS Caremark may receive rebates, discounts and service fees from pharmaceutical manufacturers for certain listed products. This document contains references to brand-name prescription drugs that are trademarks or registered trademarks of pharmaceutical manufacturers not affiliated with CVS Caremark. Listed products are for informational purposes only and are not intended to replace the clinical judgment of the doctor CVS Caremark. All rights reserved B Document date: August 1, 2016
Formulary Drug Removals
 January 2015 Below is a list of medicines by drug class that have been removed from your plan s formulary. This list is effective January 1, 2015. If you continue using one of the drugs listed below and
January 2015 Below is a list of medicines by drug class that have been removed from your plan s formulary. This list is effective January 1, 2015. If you continue using one of the drugs listed below and
Medications Requiring Prior Authorization for Medical Necessity
 January 2015 Medications Requiring Medical Necessity Below is a list of medicines by drug class that will not be covered without a prior authorization for medical necessity, effective January 1, 2015.
January 2015 Medications Requiring Medical Necessity Below is a list of medicines by drug class that will not be covered without a prior authorization for medical necessity, effective January 1, 2015.
Medications Requiring Prior Authorization for Medical Necessity
 Medications Requiring Prior Medical Necessity July 2016 Below is a list of medicines by drug class that will not be covered without a prior authorization for medical necessity. If you continue using one
Medications Requiring Prior Medical Necessity July 2016 Below is a list of medicines by drug class that will not be covered without a prior authorization for medical necessity. If you continue using one
Formulary Drug Removals
 July 2016 Below is a list of medicines by drug class that have been removed from your plan s formulary. If you continue using one of the drugs listed below and identified as a Removal, you may be required
July 2016 Below is a list of medicines by drug class that have been removed from your plan s formulary. If you continue using one of the drugs listed below and identified as a Removal, you may be required
Formulary Drug Removals
 January 2016 Below is a list of medicines by drug class that have been removed from your plan s formulary. This list is effective January 1, 2016. If you continue using one of the drugs listed below and
January 2016 Below is a list of medicines by drug class that have been removed from your plan s formulary. This list is effective January 1, 2016. If you continue using one of the drugs listed below and
Messenger. Fall Message from the Fund s Executive Director. Michigan Conference of Teamsters Welfare Fund V OLUME 33, ISSUE 2 F ALL 2015
 Michigan Conference of Teamsters Welfare Fund Dear Teamster Families: With the extraordinarily rapid and unsettling transformation that we re all experiencing in the delivery and funding of health care
Michigan Conference of Teamsters Welfare Fund Dear Teamster Families: With the extraordinarily rapid and unsettling transformation that we re all experiencing in the delivery and funding of health care
Excluded Drug List. Drug Class Excluded Product Clinical Alternative(s) ABSORICA ONEXTON GEL ANDRODERM FORTESTA VOGELXO BRINTELLIX DESVENLAFAXINE ER
 Value Formulary Excluded Drug List Catamaran offers diverse formulary alternatives that help our clients select what works best for them. The Value Formulary is a partially-closed formulary that excludes
Value Formulary Excluded Drug List Catamaran offers diverse formulary alternatives that help our clients select what works best for them. The Value Formulary is a partially-closed formulary that excludes
Avoid paying too much for your prescriptions
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2016 Aetna Rx Step Program Medicine List Avoid paying too much for your prescriptions It s important to try to
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions 2016 Aetna Rx Step Program Medicine List Avoid paying too much for your prescriptions It s important to try to
MEDICATION(S) SUBJECT TO STEP THERAPY
 ACE/ARB COMBO AZOR 5-20 MG TABLET, AZOR 5-40 MG TABLET, BENICAR HCT, MICARDIS HCT, TARKA, TEKTURNA HCT, TELMISARTAN-HYDROCHLOROTHIAZID, TRIBENZOR Claims for formulary step 2 ACE Inhibitor combination products
ACE/ARB COMBO AZOR 5-20 MG TABLET, AZOR 5-40 MG TABLET, BENICAR HCT, MICARDIS HCT, TARKA, TEKTURNA HCT, TELMISARTAN-HYDROCHLOROTHIAZID, TRIBENZOR Claims for formulary step 2 ACE Inhibitor combination products
Effective January 1, 2016
 Effective January 1, 2016 CONTENTS Prescription Benefit Changes...2 2016 Prescription Drug Benefit Highlights...3 Comparing Your Options...4 Filling Your Prescriptions...4 Benefit Coverage Tiers...5 Prescription
Effective January 1, 2016 CONTENTS Prescription Benefit Changes...2 2016 Prescription Drug Benefit Highlights...3 Comparing Your Options...4 Filling Your Prescriptions...4 Benefit Coverage Tiers...5 Prescription
Avoid paying too much for your prescriptions 2015 Aetna Rx Step Program Medicine List
 Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Avoid paying too much for your prescriptions 2015 Aetna Rx Step Program Medicine List 05.03.392.1 C (10/14) It
Quality health plans & benefits Healthier living Financial well-being Intelligent solutions Avoid paying too much for your prescriptions 2015 Aetna Rx Step Program Medicine List 05.03.392.1 C (10/14) It
Contraceptives Available at no Cost to HealthChoice Members. HealthChoice Basic and Basic Alternative Plan Changes for 2015. Ambulance Services
 FALL 2014 Contraceptives Available at no Cost to HealthChoice Members Effective immediately, medroxyprogesterone acetate (J1050) and Skyla (J7301) are available at no cost to HealthChoice members. The
FALL 2014 Contraceptives Available at no Cost to HealthChoice Members Effective immediately, medroxyprogesterone acetate (J1050) and Skyla (J7301) are available at no cost to HealthChoice members. The
Performance Drug List
 January 2016 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
January 2016 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
BayCare Health System Drug List
 July 2016 BayCare Health System Drug List The BayCare Health System Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
July 2016 BayCare Health System Drug List The BayCare Health System Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
SAVE ON MEDICAL SERVICES and PRESCRIPTION DRUGS for ongoing conditions
 SAVE ON MEDICAL SERVICES and PRESCRIPTION DRUGS for ongoing conditions With Dickinson College s Value Based Insurance Design (VBID) If you have an ongoing condition, you can live well. You will need to
SAVE ON MEDICAL SERVICES and PRESCRIPTION DRUGS for ongoing conditions With Dickinson College s Value Based Insurance Design (VBID) If you have an ongoing condition, you can live well. You will need to
2014 Valley Baptist Medicare D Formulary Step Therapy Criteria
 2014 Valley Baptist Medicare D Formulary Step Therapy Products Affected ACTONEL TAB Last Updated 11/1/2014 Requires a trial of alendronate. 1 APLENZIN TAB Patient must have tried bupropion SR or bupropion
2014 Valley Baptist Medicare D Formulary Step Therapy Products Affected ACTONEL TAB Last Updated 11/1/2014 Requires a trial of alendronate. 1 APLENZIN TAB Patient must have tried bupropion SR or bupropion
Drug Class Excluded Product Clinical Alternative(s) ABSORICA ONEXTON GEL ANDRODERM FORTESTA VOGELXO MENTHOCIN PAD LIDOCAINE SCAR PATCH
 Value Formulary Key Exclusions and Their Alternatives Catamaran offers diverse formulary alternatives that help our clients select what works best for them. The Value Formulary is a partially-closed formulary
Value Formulary Key Exclusions and Their Alternatives Catamaran offers diverse formulary alternatives that help our clients select what works best for them. The Value Formulary is a partially-closed formulary
Performance Drug List
 October 2015 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
October 2015 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
Monthly Copays. Medications must be tried for 30 days before ordering through Aspire Indiana CanaRx.
 Introduction: Aspire Indiana CanaRx is an international mail order option for eligible Employees and their Dependents of Aspire Indiana, Inc. For your convenience, a list of eligible medications is located
Introduction: Aspire Indiana CanaRx is an international mail order option for eligible Employees and their Dependents of Aspire Indiana, Inc. For your convenience, a list of eligible medications is located
Pharmacy Management Drug Policy
 PAGE: Page 1 of 9 DESCRIPTION: Step Therapy encourages use of safe, cost-effective medications within different therapeutic drug categories. The entry of new generics and cost-effective therapeutic alternatives
PAGE: Page 1 of 9 DESCRIPTION: Step Therapy encourages use of safe, cost-effective medications within different therapeutic drug categories. The entry of new generics and cost-effective therapeutic alternatives
CalPERS Basic Plan Drug List
 July 2016 CalPERS Basic Plan Drug List The CalPERS Basic Plan Drug List contains non-specialty generic and preferred brand drugs for the outpatient prescription drug benefit program administered by CVS
July 2016 CalPERS Basic Plan Drug List The CalPERS Basic Plan Drug List contains non-specialty generic and preferred brand drugs for the outpatient prescription drug benefit program administered by CVS
Burlington Scripts Vs. Current local purchase plan. Current Copays
 Introduction: Burlington Scripts is a voluntary prescription drug program that is available to eligible Employees, Retirees and their Dependents of the Town of Burlington, MA. For your convenience, a list
Introduction: Burlington Scripts is a voluntary prescription drug program that is available to eligible Employees, Retirees and their Dependents of the Town of Burlington, MA. For your convenience, a list
VIVA Health Custom Drug List
 April 2016 VIVA Health Custom Drug List The VIVA Health Custom Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
April 2016 VIVA Health Custom Drug List The VIVA Health Custom Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
Monthly Copays. Union Copays Crestor 20MG - Tier 2,10% Eliquis 5mg - Tier 3, 20% Non-Union Copays Crestor 20MG - Tier 2, $25
 Introduction: MCSMeds is an international mail order option for eligible Employees, Retirees and Dependents of Muncie Community Schools. Your list of qualified maintenance medications is on the reverse.
Introduction: MCSMeds is an international mail order option for eligible Employees, Retirees and Dependents of Muncie Community Schools. Your list of qualified maintenance medications is on the reverse.
Performance Drug List
 January 2015 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
January 2015 Performance Drug List The CVS/caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
VA Premier CompleteCare Drugs that Require Step Therapy Last Updated: 09/23/2014
 Atelvia Atelvia Claim will pay automatically for Atelvia if enrollee has a paid claim for at least a 1 days supply of alendronate in the past 365 days. Otherwise, Atelvia requires a step therapy exception
Atelvia Atelvia Claim will pay automatically for Atelvia if enrollee has a paid claim for at least a 1 days supply of alendronate in the past 365 days. Otherwise, Atelvia requires a step therapy exception
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY
 GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
GEORGIA MEDICAID FEE-FOR-SERVICE ASTHMA and COPD AGENTS PA SUMMARY Preferred Anticholinergics and Combinations Atrovent HFA (ipratropium) Combivent Respimat (ipratropium/albuterol) Ipratropium neb inhalation
GEHA Drug List. July 2015 PLAN MEMBER HEALTH CARE PROVIDER
 July 2015 GEHA Drug List The GEHA Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line of prescribing.
July 2015 GEHA Drug List The GEHA Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line of prescribing.
HMO and PPO Updates May 2013- Commercial Results
 HMO and PPO Updates May 2013- Commercial Results ELIQUIS Non Triple Tier Formular y 4th Tier Applicable Traditional Alternatives warfarin, Xarelto, Pradaxa TAMIFLU - EXPANDED INDICATION 2 No 2 No No None
HMO and PPO Updates May 2013- Commercial Results ELIQUIS Non Triple Tier Formular y 4th Tier Applicable Traditional Alternatives warfarin, Xarelto, Pradaxa TAMIFLU - EXPANDED INDICATION 2 No 2 No No None
Performance Drug List
 January 2014 Performance Drug List The CVS Caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
January 2014 Performance Drug List The CVS Caremark Performance Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered
Prescription Drug Utilization and Cost Trends, 2009-2013
 Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
Agenda Item 7 Attachment 1 Prescription Drug Utilization and Cost Trends, 2009-2013 Pension and Health Benefits Committee October 14, 2014 Melissa Mantong, PharmD CalPERS Pharmacist Overview Trends in
May 31, 2013. Ms. Debra Lansey American College of Physicians 190 North Independence Mall West Philadelphia, PA 19106
 P.O. Box 30449 Salt Lake City, UT 84130-0449 May 31, 2013 Ms. Debra Lansey American College of Physicians 190 North Independence Mall West Philadelphia, PA 19106 Re: Pharmacy Benefit Coverage Changes Effective
P.O. Box 30449 Salt Lake City, UT 84130-0449 May 31, 2013 Ms. Debra Lansey American College of Physicians 190 North Independence Mall West Philadelphia, PA 19106 Re: Pharmacy Benefit Coverage Changes Effective
PA Start Date Therapeutic Class P&T Review Date 1/1/16 TOP$ (Single Drug Reviews) include:
 Maryland Department of Health and Mental Hygiene PDL Prior Authorization Implementation Schedule PA Start Therapeutic Class P&T Review 1/1/16 11/5/15 Acne Agents, Topical (Epiduo Forte Gel W/Pump) Androgenic
Maryland Department of Health and Mental Hygiene PDL Prior Authorization Implementation Schedule PA Start Therapeutic Class P&T Review 1/1/16 11/5/15 Acne Agents, Topical (Epiduo Forte Gel W/Pump) Androgenic
Alla chme nl A EFFECTIVE 07/01/2014 BUREAU FOR MEDICAL SERVICES WEST VIRGINIA MEDICAID PREFERRED DRUG LIST WITH PRIOR AUTHORIZATION CRITERIA
 A. Re-Review 1. Bethkis ANTIBIOTICS, INHALED BETHKIS (tobramycin) TOBI (tobramycin) 2. Effient CAYSTON (aztreonam) TOBI POOHALER tobramycin PLATELET AGGREGATION INHIBITORS AGGRENOX (dipyridamole/asa) BRIUNTA
A. Re-Review 1. Bethkis ANTIBIOTICS, INHALED BETHKIS (tobramycin) TOBI (tobramycin) 2. Effient CAYSTON (aztreonam) TOBI POOHALER tobramycin PLATELET AGGREGATION INHIBITORS AGGRENOX (dipyridamole/asa) BRIUNTA
PEBTF Drug List. July 2013 PLAN MEMBER HEALTH CARE PROVIDER
 July 2013 PEBTF Drug List The PEBTF Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line of prescribing.
July 2013 PEBTF Drug List The PEBTF Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line of prescribing.
Aetna 2015 Formulary updates for self insured and custom fully insured commercial plans
 Key: #- ; $0^-Health Care Reform Zero-Dollar; OTC-Over-the-Counter abacavir PB SPB Moved to Specialty abacavir/lamivudine/ PB SPB Moved to Specialty zidovudine ABILIFY (PA, ST) 3 3 olanzapine, quetiapine,
Key: #- ; $0^-Health Care Reform Zero-Dollar; OTC-Over-the-Counter abacavir PB SPB Moved to Specialty abacavir/lamivudine/ PB SPB Moved to Specialty zidovudine ABILIFY (PA, ST) 3 3 olanzapine, quetiapine,
Preferred Drug List. January 2014 PLAN MEMBER HEALTH CARE PROVIDER
 January 2014 Preferred Drug List The Preferred Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line
January 2014 Preferred Drug List The Preferred Drug List is a guide within select therapeutic categories for clients, plan members and health care providers. Generics should be considered the first line
UnitedHealthcare Group Medicare Advantage (PPO)
 Your Plan Explained UnitedHealthcare Group Medicare Advantage (PPO) UHEX11MP3230855_001 Y0066_100616_09113 Your Medicare. This brochure explains your Medicare Advantage plan, a type of health plan also
Your Plan Explained UnitedHealthcare Group Medicare Advantage (PPO) UHEX11MP3230855_001 Y0066_100616_09113 Your Medicare. This brochure explains your Medicare Advantage plan, a type of health plan also
NALC Health Benefit Plan Formulary Drug List
 NALC Health Benefit Plan Formulary Drug List January 2014 The NALC Health Benefit Plan Formulary Drug List is a guide within select therapeutic categories for clients, plan members and health care providers.
NALC Health Benefit Plan Formulary Drug List January 2014 The NALC Health Benefit Plan Formulary Drug List is a guide within select therapeutic categories for clients, plan members and health care providers.
2015 EMPIRE PLAN FLEXIBLE FORMULARY DRUG LIST Administered by CVS/caremark
 January 2015 2015 EMPIRE PLAN FLEXIBLE FORMULARY DRUG LIST Administered by CVS/caremark The Empire Plan Flexible Formulary is a guide within select therapeutic categories for enrollees and health care
January 2015 2015 EMPIRE PLAN FLEXIBLE FORMULARY DRUG LIST Administered by CVS/caremark The Empire Plan Flexible Formulary is a guide within select therapeutic categories for enrollees and health care
Drug Formulary Update, July 2014 Commercial and State Programs
 Drug ormulary Update, July 2014 Commercial and State Programs Updates to the HealthPartners Drug ormularies are listed below. Changes start July 1 unless noted otherwise. Updates apply to all Commercial
Drug ormulary Update, July 2014 Commercial and State Programs Updates to the HealthPartners Drug ormularies are listed below. Changes start July 1 unless noted otherwise. Updates apply to all Commercial
MArch 2015. The 2014 Drug Trend Report
 MArch 2015 The 2014 Drug Report content Introduction 3 MedicaRE 58 Commercially Insured Year in Review Medicare Year in Review A Look at Overall Drug for 2014 A Look at Medicare Overall Drug for 2014 Therapy
MArch 2015 The 2014 Drug Report content Introduction 3 MedicaRE 58 Commercially Insured Year in Review Medicare Year in Review A Look at Overall Drug for 2014 A Look at Medicare Overall Drug for 2014 Therapy
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services
 scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
scriptsourcing THE NEXT 5 YEARS OF RX COSTS AND HOW THEY WILL IMPACT YOUR BOTTOM LINE ScriptSourcing Prescription Advocacy Services Gary Becker, CEO Benefit Consultant, Risk Mitigation Expert, and Author
AETNA BETTER HEALTH Prior Authorization guidelines for Step Therapy
 AETNA BETTER HEALTH Prior Authorization guidelines for Step Therapy Definition A form of automated Prior Authorization whereby one or more prerequisite medications, which may or may not be in the same
AETNA BETTER HEALTH Prior Authorization guidelines for Step Therapy Definition A form of automated Prior Authorization whereby one or more prerequisite medications, which may or may not be in the same
Anthem Blue Cross and Blue Shield Medicaid: Pharmacy and Therapeutics Advisory Committee meeting
 Anthem Blue Cross and Blue Shield Medicaid: Pharmacy and Therapeutics Advisory Committee meeting 1. Inhaled corticosteroids (ICS) VAC 4q14 Inhaled corticosteroids for asthma Reason for review: Category
Anthem Blue Cross and Blue Shield Medicaid: Pharmacy and Therapeutics Advisory Committee meeting 1. Inhaled corticosteroids (ICS) VAC 4q14 Inhaled corticosteroids for asthma Reason for review: Category
Approximate Cost Reference List i for Antihyperglycemic Agents
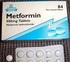 Alpha Glucosidase Inhibitor Acarbose (Glucobay ) Biguanides Metformin (Glucophage, generic) Metformin ER (Glumetza ) Approximate Cost Reference List i for Antihyperglycemic Agents Incretin Agents - DPP-4
Alpha Glucosidase Inhibitor Acarbose (Glucobay ) Biguanides Metformin (Glucophage, generic) Metformin ER (Glumetza ) Approximate Cost Reference List i for Antihyperglycemic Agents Incretin Agents - DPP-4
612 Program Midtown Express Pharmacy
 ALENDRONATE SOD TAB 35MG (max 1 per week) $37.00 $70.00 ALENDRONATE SOD TAB 70MG (max 1 per week) $37.00 $70.00 ALLOPURINOL TAB 100MG $20.00 $38.00 ALLOPURINOL TAB 300MG $20.00 $38.00 AMITRIPTYLINE TAB
ALENDRONATE SOD TAB 35MG (max 1 per week) $37.00 $70.00 ALENDRONATE SOD TAB 70MG (max 1 per week) $37.00 $70.00 ALLOPURINOL TAB 100MG $20.00 $38.00 ALLOPURINOL TAB 300MG $20.00 $38.00 AMITRIPTYLINE TAB
The 365-day period begins with the first dispensing transaction for each Ontario Drug Benefit (ODB) recipient on or after October 1, 2015.
 Ontario Public Drug Programs, Ministry of Health and Long-Term Care Chronic-use Medications List by In accordance with subsection 18 (11.1) of Ontario Regulation 201/96 made under the Ontario Drug Benefit
Ontario Public Drug Programs, Ministry of Health and Long-Term Care Chronic-use Medications List by In accordance with subsection 18 (11.1) of Ontario Regulation 201/96 made under the Ontario Drug Benefit
USP Medicare Model Guidelines v6.0 (Categories and Classes)
 USP Medicare Model Guidelines v6.0 (Categories and Classes) USP Category Analgesics Nonsteroidal Anti-inflammatory Drugs Opioid Analgesics, Long-acting Opioid Analgesics, Short-acting Anesthetics Local
USP Medicare Model Guidelines v6.0 (Categories and Classes) USP Category Analgesics Nonsteroidal Anti-inflammatory Drugs Opioid Analgesics, Long-acting Opioid Analgesics, Short-acting Anesthetics Local
MArch 2015. The 2014 Drug Trend Report MEDICAID
 MArch 2015 The 2014 Drug Report MEDICAID content medicaid 3 Medicaid Year in Review A Look at Medicaid Overall Drug for 2014 Medicaid: Traditional Therapy Classes and Insights Top 10 Medicaid Traditional
MArch 2015 The 2014 Drug Report MEDICAID content medicaid 3 Medicaid Year in Review A Look at Medicaid Overall Drug for 2014 Medicaid: Traditional Therapy Classes and Insights Top 10 Medicaid Traditional
Preferred Drug List Updates Effective: Jan. 1, 2016
 Molina Healthcare regularly reviews and updates the Preferred Drug List (PDL). Items may be added, removed or changed. Below is the list of updates made to the PDL this quarter. Some items require a prior
Molina Healthcare regularly reviews and updates the Preferred Drug List (PDL). Items may be added, removed or changed. Below is the list of updates made to the PDL this quarter. Some items require a prior
Extra Value Drug List. *
 List. * Brand Diabetes Levemir 100 units/ml Vial 10mL $122.29 Levemir FlexPen 100 units/ml 15mL $203.03 NovoLog 100 units/ml Vial 10mL $116.84 NovoLog FlexPen Syringe 15mL $222.41 NovoLog 100 units/ml
List. * Brand Diabetes Levemir 100 units/ml Vial 10mL $122.29 Levemir FlexPen 100 units/ml 15mL $203.03 NovoLog 100 units/ml Vial 10mL $116.84 NovoLog FlexPen Syringe 15mL $222.41 NovoLog 100 units/ml
ACTEMRA. Step Therapy Criteria HEALTH CHOICE EXCHANGE 2016 Effective Date: 01/01/2016. PRODUCT(s) AFFECTED ACTEMRA
 ACTEMRA ACTEMRA Claim will pay automatically for Actemra if enrollee has a paid claim for at least a 1 days supply of Enbrel and Humira in the past 365 days. Otherwise, Actemra requires a step therapy
ACTEMRA ACTEMRA Claim will pay automatically for Actemra if enrollee has a paid claim for at least a 1 days supply of Enbrel and Humira in the past 365 days. Otherwise, Actemra requires a step therapy
Retiree Bulletin IMPORTANT CHANGES NYC PBA HEALTH & WELFARE. >>> Plan design updates for better benefits, lower costs
 June 2014 NYC PBA HEALTH & WELFARE Retiree Bulletin www.nycpba.org Patrick J. Lynch President Plan Changes Page 1 Dental Implant Program Page 1 Medicare Part D Page 2 Coming Soon: New SPD Page 3 New Step
June 2014 NYC PBA HEALTH & WELFARE Retiree Bulletin www.nycpba.org Patrick J. Lynch President Plan Changes Page 1 Dental Implant Program Page 1 Medicare Part D Page 2 Coming Soon: New SPD Page 3 New Step
COVERAGE MANAGEMENT PROGRAMS
 COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
COVERAGE MANAGEMENT PROGRAMS The purpose of coverage management programs is to help improve the quality of care by encouraging the right patient and provider behaviors to avoid compromised care and unnecessary
Prescription Drug Plan
 Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
Prescription Drug Plan The prescription drug plan helps you pay for prescribed medications using either a retail pharmacy or the mail order program. For More Information Administrative details and procedures
Guidelines for Type 2 Diabetes Diagnosis
 Guidelines for Type 2 Diabetes Diagnosis Fasting Plasma Glucose (in asymptomatic individuals, repeat measurement to confirm the test) Normal FPG < 100 2-hr OGTT < 140 HbA1C < 5.5% Impaired Fasting Glucose
Guidelines for Type 2 Diabetes Diagnosis Fasting Plasma Glucose (in asymptomatic individuals, repeat measurement to confirm the test) Normal FPG < 100 2-hr OGTT < 140 HbA1C < 5.5% Impaired Fasting Glucose
Type 2 Diabetes Medicines: What You Need to Know
 Type 2 Diabetes Medicines: What You Need to Know Managing diabetes is complex because many hormones and body processes are at work controlling blood sugar (glucose). Medicines for diabetes include oral
Type 2 Diabetes Medicines: What You Need to Know Managing diabetes is complex because many hormones and body processes are at work controlling blood sugar (glucose). Medicines for diabetes include oral
DIABETES EDUCATION. *Read package insert each time you refill your medications in case there is new information SULFONYLUREAS
 DIABETES EDUCATION *Read package insert each time you refill your medications in case there is new information SULFONYLUREAS ACTION: Sulfonylureas stimulate the pancreas to make more insulin (pancreas
DIABETES EDUCATION *Read package insert each time you refill your medications in case there is new information SULFONYLUREAS ACTION: Sulfonylureas stimulate the pancreas to make more insulin (pancreas
QUANTITY LIMITS TABLE
 S TABLE / TABLA DE ABILIFY ARIPIPRAZOLE ORAL SOLUTION 900 ML IN 30 DAYS ABILIFY DISCMELT 10 MG ARIPIPRAZOLE TAB RAPDIS 30 TABS IN 30 DAYS ABILIFY DISCMELT 15 MG ARIPIPRAZOLE TAB RAPDIS 60 TABS IN 30 DAYS
S TABLE / TABLA DE ABILIFY ARIPIPRAZOLE ORAL SOLUTION 900 ML IN 30 DAYS ABILIFY DISCMELT 10 MG ARIPIPRAZOLE TAB RAPDIS 30 TABS IN 30 DAYS ABILIFY DISCMELT 15 MG ARIPIPRAZOLE TAB RAPDIS 60 TABS IN 30 DAYS
Potential Savings from Generic Drugs in Upstate New York
 T H E F A C T S A B O U T Potential Savings from Generic Drugs in Upstate New York $880 Million in Potential Savings for Upstate New York Counties Finger Lakes Region $141 million Western New York Region
T H E F A C T S A B O U T Potential Savings from Generic Drugs in Upstate New York $880 Million in Potential Savings for Upstate New York Counties Finger Lakes Region $141 million Western New York Region
The JPMorgan Chase Prescription Drug Plan Effective January 1, 2010 (CVS Caremark web site version)
 The JPMorgan Chase Prescription Drug Plan Effective January 1, 2010 (CVS Caremark web site version) OVERVIEW This Bulletin provides an overview of, as well as detail on changes to, the JPMorgan Chase Prescription
The JPMorgan Chase Prescription Drug Plan Effective January 1, 2010 (CVS Caremark web site version) OVERVIEW This Bulletin provides an overview of, as well as detail on changes to, the JPMorgan Chase Prescription
PHARMACOLOGY UPDATE: BOOMER DRUGS
 PHARMACOLOGY UPDATE: BOOMER DRUGS Sandra Brownstein, PharmD Evercare Clinical Pharmacy Director West Region Objectives: Review the new drugs that have recently been approved by the FDA Determine the role
PHARMACOLOGY UPDATE: BOOMER DRUGS Sandra Brownstein, PharmD Evercare Clinical Pharmacy Director West Region Objectives: Review the new drugs that have recently been approved by the FDA Determine the role
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information
 Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Express Scripts/Medco Prescription Plan Information For Drug Coverage Review, Prior Authorization Process and Personalized Medicine Information The endowed health plan offers faculty and staff members
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
 Cara Liday, PharmD, CDE Associate Professor, Idaho State University Clinical Pharmacist and CDE, InterMountain Medical Center Pocatello, ID The planners and presenter have disclosed no conflict of interest,
Cara Liday, PharmD, CDE Associate Professor, Idaho State University Clinical Pharmacist and CDE, InterMountain Medical Center Pocatello, ID The planners and presenter have disclosed no conflict of interest,
2016 Employee Benefits Guide
 2016 Employee Benefits Guide I am pleased to present to you Lake Charles Memorial s benefit guide for 2016. In this guide you will find valuable information to assist with selecting the plans that are
2016 Employee Benefits Guide I am pleased to present to you Lake Charles Memorial s benefit guide for 2016. In this guide you will find valuable information to assist with selecting the plans that are
November 5, 2015 Quarterly pharmacy formulary change notice
 November 5, 2015 Quarterly pharmacy formulary change notice The formulary changes listed in the table below were reviewed and approved at the 2nd Quarter Pharmacy and Therapeutics (P&T) Committee meetings
November 5, 2015 Quarterly pharmacy formulary change notice The formulary changes listed in the table below were reviewed and approved at the 2nd Quarter Pharmacy and Therapeutics (P&T) Committee meetings
Drug Formulary Update, July 2013
 Drug Formulary Update, July 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
Drug Formulary Update, July 2013 Updates to the HealthPartners Drug Formularies are listed below. Updates for the Commercial Drug Formularies and the Minnesota Health Care Programs (Medicaid and Minnesota
COLORADO MEDICAID P&T COMMITTEE MEETING MINUTES July 8, 2014
 COLORADO MEDICAID P&T COMMITTEE MEETING MINUTES July 8, 2014 Members Present Lynn Parry, MD Shilpa Kinikar, PharmD, BCPS Neil Stafford, MD Roy J. Durbin Jr., MD Kimberly Nordstrom, MD, JD Patricia Lanius,
COLORADO MEDICAID P&T COMMITTEE MEETING MINUTES July 8, 2014 Members Present Lynn Parry, MD Shilpa Kinikar, PharmD, BCPS Neil Stafford, MD Roy J. Durbin Jr., MD Kimberly Nordstrom, MD, JD Patricia Lanius,
MEDICATIONS COMMONLY USED IN CHRONIC KIDNEY DISEASE. HealthPartners Kidney Health Clinic 2011
 MEDICATIONS COMMONLY USED IN CHRONIC KIDNEY DISEASE HealthPartners Kidney Health Clinic 2011 People with chronic kidney disease (CKD) require multiple medications. This handout will help explain the reason
MEDICATIONS COMMONLY USED IN CHRONIC KIDNEY DISEASE HealthPartners Kidney Health Clinic 2011 People with chronic kidney disease (CKD) require multiple medications. This handout will help explain the reason
Follow-up Medical History (FH-1)
 9FH126 Jan 10 Citalopram for Agitation in Alzheimer s Disease CitAD (FH-1) Reference #: Purpose: Record the interval medical history. When: At F3, F6, and F9. Completed by: CitAD certified clinician. Instructions:
9FH126 Jan 10 Citalopram for Agitation in Alzheimer s Disease CitAD (FH-1) Reference #: Purpose: Record the interval medical history. When: At F3, F6, and F9. Completed by: CitAD certified clinician. Instructions:
Mary Bruskewitz APN, MS, RN, BC-ADM Clinical Nurse Specialist Diabetes
 Mary Bruskewitz APN, MS, RN, BC-ADM Clinical Nurse Specialist Diabetes Objectives Pathophysiology of Diabetes Acute & Chronic Complications Managing acute emergencies Case examples 11/24/2014 UWHealth
Mary Bruskewitz APN, MS, RN, BC-ADM Clinical Nurse Specialist Diabetes Objectives Pathophysiology of Diabetes Acute & Chronic Complications Managing acute emergencies Case examples 11/24/2014 UWHealth
www.oxfordhealth.com
 www.oxfordhealth.com Oxford s HMO products are underwritten by Oxford Health Plans (NY), Inc., Oxford Health Plans (NJ), Inc., and Oxford Health Plans (CT), Inc., and insurance products are underwritten
www.oxfordhealth.com Oxford s HMO products are underwritten by Oxford Health Plans (NY), Inc., Oxford Health Plans (NJ), Inc., and Oxford Health Plans (CT), Inc., and insurance products are underwritten
SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. Formulary Updates. New Generics: Drug Name PDL Category Comments AGENTS
 SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE SEPTEMBER 2015 ISSUE 3 HELPFUL NUMBERS FOR PROVIDERS Passport Health Plan Magellan: 1-800-846-7971 Bin: 016523 Processor control:
SUPPORTING OUR PROVIDER PARTNERS THROUGH COMMUNICATION AND COLLABORATION. DATE SEPTEMBER 2015 ISSUE 3 HELPFUL NUMBERS FOR PROVIDERS Passport Health Plan Magellan: 1-800-846-7971 Bin: 016523 Processor control:
THERAPEUTIC INTERCHANGES ***Not Applied to patients <18 years of age*** Proton Pump Inhibitors
 ***Not Applied to patients
***Not Applied to patients
NLPDP Coverage Status Table December 2015. Initial and maintenance fills are limited to a maximum 30 days
 Coverage Table December 2015 02238646 282 MEP TABLET OPEN No 500 0.2103 02234510 282 TABLET OPEN No 500 0.0726 02238645 292 TABLET OPEN No 50 0.1877 02192691 3TC 10 MG/ML SOLUTION OPEN No 240 0.3454 02192683
Coverage Table December 2015 02238646 282 MEP TABLET OPEN No 500 0.2103 02234510 282 TABLET OPEN No 500 0.0726 02238645 292 TABLET OPEN No 50 0.1877 02192691 3TC 10 MG/ML SOLUTION OPEN No 240 0.3454 02192683
10/30/2012. Anita King, DNP, RN, FNP, CDE, FAADE Clinical Associate Professor University of South Alabama Mobile, Alabama
 Faculty Medications for Diabetes Satellite Conference and Live Webcast Wednesday, November 7, 2012 2:00 4:00 p.m. Central Time Anita King, DNP, RN, FNP, CDE, FAADE Clinical Associate Professor University
Faculty Medications for Diabetes Satellite Conference and Live Webcast Wednesday, November 7, 2012 2:00 4:00 p.m. Central Time Anita King, DNP, RN, FNP, CDE, FAADE Clinical Associate Professor University
2015 new member prescription benefits program guide. putting your family first. MagnaCare Rx. we rise above. MagnaCareRx.com
 2015 new member prescription benefits program guide putting your family first. MagnaCare Rx 410 Peachtree Parkway Suite 4225 Cumming, Georgia 30041 member services: 888.975.0988 MagnaCareRx.com RxGRP 3381
2015 new member prescription benefits program guide putting your family first. MagnaCare Rx 410 Peachtree Parkway Suite 4225 Cumming, Georgia 30041 member services: 888.975.0988 MagnaCareRx.com RxGRP 3381
Your Guide to Prescription Drug Benefits. 2013 Preferred Formulary and Prescription Drug List
 Your Guide to Prescription Drug Benefits 2013 Preferred Formulary and Prescription Drug List How to Contact Us By Telephone For more information about your prescription drug benefit, call BlueCross BlueShield
Your Guide to Prescription Drug Benefits 2013 Preferred Formulary and Prescription Drug List How to Contact Us By Telephone For more information about your prescription drug benefit, call BlueCross BlueShield
Type 2 Diabetes Medications: SGLT2 Inhibitors
 Type 2 Diabetes Medications: SGLT2 Inhibitors SGLT2 inhibitors are a class of type 2 diabetes medications used along with diet and exercise to lower blood glucose How are they taken? SGLT2 inhibitors is
Type 2 Diabetes Medications: SGLT2 Inhibitors SGLT2 inhibitors are a class of type 2 diabetes medications used along with diet and exercise to lower blood glucose How are they taken? SGLT2 inhibitors is
Members enjoy more Pharmacy savings *
 Sam s Plus Members enjoy more Pharmacy savings 5 prescription drugs available for FREE Generic medications: Donepezil, Pioglitazone, Escitalopram, Finasteride and Vitamin D2 50,000IU are $ 0 for a 30-day
Sam s Plus Members enjoy more Pharmacy savings 5 prescription drugs available for FREE Generic medications: Donepezil, Pioglitazone, Escitalopram, Finasteride and Vitamin D2 50,000IU are $ 0 for a 30-day
$10.00 PRESCRIPTION PROGRAM DETAILS
 $10.00 PRESCRIPTION PROGRAM DETAILS 1. The $10.00 program applies only to certain generic drugs at commonly prescribed 90 day usage dosages. (See list). 2. The Program may change without notification and
$10.00 PRESCRIPTION PROGRAM DETAILS 1. The $10.00 program applies only to certain generic drugs at commonly prescribed 90 day usage dosages. (See list). 2. The Program may change without notification and
2015 Medicare Part D Step Therapy Requirements. Effective: November 01, 2015
 2015 Medicare Part D Step Therapy Requirements Effective: November 01, 2015 Formulary ID 15293, Version 17 Last Updated: 10/27/2015 BISPHOSPHONATE THERAPY ACTONEL 30 MG TABLET ACTONEL 35 MG TABLET ACTONEL
2015 Medicare Part D Step Therapy Requirements Effective: November 01, 2015 Formulary ID 15293, Version 17 Last Updated: 10/27/2015 BISPHOSPHONATE THERAPY ACTONEL 30 MG TABLET ACTONEL 35 MG TABLET ACTONEL
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. sacubitril/valsartan film-coated tablets
 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr ENTRESTO TM sacubitril/valsartan film-coated tablets Read this carefully before you start taking ENTRESTO TM and
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr ENTRESTO TM sacubitril/valsartan film-coated tablets Read this carefully before you start taking ENTRESTO TM and
Tier 1 Formulary Drug Quantity Limits 2016
 Tier 1 Formulary Drug Quantity Limits 2016 Updated: 11/20/2015 Effective: 01/01/2016 What are Quantity Limits? For certain drugs, we limit the amount of the drug that you can have by limiting how much
Tier 1 Formulary Drug Quantity Limits 2016 Updated: 11/20/2015 Effective: 01/01/2016 What are Quantity Limits? For certain drugs, we limit the amount of the drug that you can have by limiting how much
It Pays to Shop: Variation in Out-of-Pocket Costs for Medicare Part D Enrollees in 2016
 It Pays to Shop: Variation in Out-of-Pocket Costs for Medicare Part D Enrollees in 2016 Medicare Part D drug plans differ considerably in the drugs they list on their formularies, their use of formulary
It Pays to Shop: Variation in Out-of-Pocket Costs for Medicare Part D Enrollees in 2016 Medicare Part D drug plans differ considerably in the drugs they list on their formularies, their use of formulary
GUIDE TO PRESCRIPTION DRUG BENEFITS. Capital BlueCross is an Independent Licensee of the BlueCross BlueShield Association
 GUIDE TO PRESCRIPTION DRUG BENEFITS Capital BlueCross is an Independent Licensee of the BlueCross BlueShield Association TABLE OF CONTENTS 1 Contact Us Phone Number Website 2-3 Using Your Prescription
GUIDE TO PRESCRIPTION DRUG BENEFITS Capital BlueCross is an Independent Licensee of the BlueCross BlueShield Association TABLE OF CONTENTS 1 Contact Us Phone Number Website 2-3 Using Your Prescription
Add: 2 nd generation sulfonylurea or glinide or Add DPP-4 inhibitor Start or intensify insulin therapy if HbA1c goals not achieved with the above
 Guidelines for Type Diabetes - Diagnosis Fasting Plasma Glucose (confirm results if borderline) HbAIC Normal FPG < 00 < 5.5 Impaired Fasting Glucose (IFG) 00 to < 5.7%-.5% Diabetes Mellitus (or random
Guidelines for Type Diabetes - Diagnosis Fasting Plasma Glucose (confirm results if borderline) HbAIC Normal FPG < 00 < 5.5 Impaired Fasting Glucose (IFG) 00 to < 5.7%-.5% Diabetes Mellitus (or random
Pharmacy and Therapeutics Committee-approved Therapeutic Interchange
 Therapeutic Interchanges Therapeutic Interchange Revision Date Alpha Blockers 08/11 Alpha Reductase Inhibitors 05/16 ACE Inhibitors 08/11 Angiotensin Receptor Blockers 08/11 Buprenorphine 09/11 Calcium
Therapeutic Interchanges Therapeutic Interchange Revision Date Alpha Blockers 08/11 Alpha Reductase Inhibitors 05/16 ACE Inhibitors 08/11 Angiotensin Receptor Blockers 08/11 Buprenorphine 09/11 Calcium
Pharmacy Handbook For non-grandfathered members
 Pharmacy Handbook For non-grandfathered members Table of Contents Formulary... 2 Pharmacy Programs... 2 Mail Order Programs... 2 Injectable and High Cost Medications Program... 2 Step Therapy Program...
Pharmacy Handbook For non-grandfathered members Table of Contents Formulary... 2 Pharmacy Programs... 2 Mail Order Programs... 2 Injectable and High Cost Medications Program... 2 Step Therapy Program...
How To Treat Diabetes
 Overview of Diabetes Medications Marie Frazzitta DNP, FNP c, CDE, MBA Senior Director of Disease Management North Shore LIJ Health Systems Normal Glucose Metabolism Insulin is produced by beta cells in
Overview of Diabetes Medications Marie Frazzitta DNP, FNP c, CDE, MBA Senior Director of Disease Management North Shore LIJ Health Systems Normal Glucose Metabolism Insulin is produced by beta cells in
Medications for chronic pain
 Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Medications for chronic pain When it comes to treating chronic pain with medications, there are many to choose from. Different types of pain medications are used for different pain conditions. You may
Pharmacology 260 Online Course Schedule Spring 2012
 Pharmacology 260 Online Course Spring 2012 The topics listed below do not necessarily correspond to a 1 - hour lecture period. You should cover the topics for each week at some time during that week. Readings
Pharmacology 260 Online Course Spring 2012 The topics listed below do not necessarily correspond to a 1 - hour lecture period. You should cover the topics for each week at some time during that week. Readings
