The Hidden Cystic Duct Syndrome and the Infundibular Technique of Laparoscopic Cholecystectomy the Danger of the False Infundibulum
|
|
|
- Rosaline Lawrence
- 7 years ago
- Views:
Transcription
1 The Hidden Cystic Duct Syndrome and the Infundibular Technique of Laparoscopic Cholecystectomy the Danger of the False Infundibulum Steven M Strasberg, MD, FACS, FRCS(C), Christopher J Eagon, MD, Jeffrey A Drebin, MD, FACS Background: The classical biliary injury usually involves misidentification of the common bile duct as the cystic duct. The purpose of this study was to determine if the method of cholecystectomy, specifically the infundibular technique, might be a contributing factor in this injury. Study Design: Twenty-one operative notes of patients who were referred with injury to the common bile duct were examined. Notes were classified as to informativeness. Patient and operative variables potentially related to injury were searched for. Results: Inflammation was the main patient variable associated with injury. The main operative variable was that in most of the injuries the cystic duct was isolated and divided as the first step in the procedure. Often the operative note contained a statement indicating that the surgeon believed that the cystic duct (actually the common bile duct) was emanating from the infundibulum of the gallbladder and that this was the anatomic rationale for identification of the cystic duct. In no case was the triangle of Calot completely dissected before injury. Conclusions: The cystic duct may be hidden in some patients having laparoscopic cholecystectomy, especially in the presence of inflammation. This may lead to the deceptive appearance of a false infundibulum that misleads the surgeon into identifying the common duct as the cystic duct. Biliary injury is more likely when cystic duct identification is made by relying solely on the appearance of the junction of the cystic duct with the infundibulum of the gallbladder, and this technique should be abandoned. ( J Am Coll Surg No competing interests declared. Received May 5, 2000; Revised July 10, 2000; Accepted July 24, From the Section of Hepatobiliary-Pancreatic and Gastrointestinal Surgery, Department of Surgery, Washington University, St Louis, MO. Correspondence address: Steven M Strasberg, MD, FACS, FRCS(C), Box 8109, Suite Queeny Tower, 1 Barnes Hospital Plaza, St Louis, MO ;191: by the American College of Surgeons) Biliary injury during laparoscopic cholecystectomy continues to be an important cause of morbidity. Injury rates are probably decreasing, but have not yet attained the levels that were once present in the era of open cholecystectomy. 1-3 The classical biliary injury occurs when the common bile duct is injured as a consequence of the mistaken belief that it is the cystic duct, ie, it is misidentified. 4 The degree of severity of the injury ranges from simple obstruction to excision of large parts of the extrahepatic biliary tree and, at worst, results in the need for a very high biliary reconstruction 5-7 or even liver resection or transplantation. The problem of misidentification of the common bile duct as the cystic duct during laparoscopic cholecystectomy is well recognized. 1-3,8,9 A number of contributing factors have been recognized, such as direction of traction of the gallbladder and adhesive bands. 12 Most surgeons are aware of these pitfalls. Yet despite this and all that has been written about misidentification, injuries to the common bile duct are still occurring with disturbing frequency. 3 In discussing the mechanism of injury with surgeons who have referred patients for reconstruction, we have been struck by the fact that highly competent, experienced, and informed surgeons have been convinced that they were dissecting the cystic duct when, in fact, they have been isolating a segment of the common bile duct. This has caused us to hypothesize that there might be a flaw in some techniques by which laparoscopic cholecystectomy is performed a flaw associated with a visual deception. There are two well-described methods for ductal identification in laparoscopic cholecystectomy by the American College of Surgeons ISSN /00/$21.00 Published by Elsevier Science Inc. PII S (00)
2 662 Strasberg et al Hidden Cystic Duct Syndrome J Am Coll Surg occurred were examined. The results support the conclusion that the infundibular technique is an unreliable method of ductal identification, especially when local conditions conspire to hide the true cystic duct. Figure 1. The critical view of safety. The triangle of Calot is dissected free of all tissue except for cystic duct and artery, and the base of the liver bed is exposed. When this view is achieved, the two structures entering the gallbladder can only be the cystic duct and artery. It is not necessary to see the common bile duct. (Modified from: Strasberg SM, Hertl M, Soper NJ. An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 1995;180: , with permission.) One is the critical view of safety technique, which we described in This method requires complete dissection of the triangle of Calot and separation of the base of the gallbladder from the liver bed. The anatomic rationale for identification of the cystic structures results from the fact that there are two, and only two, structures entering the gallbladder, which is otherwise still attached only by the upper part of the liver bed 9,13 (Fig. 1). The second and older method has been referred to as the infundibular or infundibular-cystic technique. In this method the cystic duct is isolated by dissection on the front and the back of the triangle of Calot and once isolated it is traced on to the gallbladder. Conclusive identification, ie, the anatomic rationale for identification, occurs as a result of seeing the characteristic flare, as the cystic duct widens to become the gallbladder infundibulum. Often this is referred to as seeing a funnel shape. The infundibular method is the one usually found in texts describing the technique of laparoscopic cholecystectomy. The purpose of this study was to look for contributing factors to the classical injury. Particularly, we wished to determine whether the method of cholecystectomy was a factor in the injury. Operative notes of procedures in which such an injury METHODS Forty-seven patients were referred to us for repair of major biliary injuries in the past 7 years. Twenty patients had injury to aberrant ducts or sustained an injury at open cholecystectomy and were not of interest in this analysis. Twenty-seven patients had undergone laparoscopic cholecystectomy and were found to have a classical injury. The operative note was available in 21 of these patients (78%). It could not be obtained in the other six patients who had a classical injury. Operative records were examined for operative and patient variables that might have contributed to the injury. Patient variables included presence or absence of acute cholecystitis, severe chronic inflammation, wall thickening, tenseness or distension of the gallbladder, stone impaction in the infundibulum, adhesions, abnormal anatomy, and obesity. Operative variables were method of cholecystectomy, particularly whether the triangle of Calot was cleared before clipping cystic structures ( critical view method), or whether the cystic duct was isolated and divided before complete dissection of the triangle of Calot. We sought to ascertain the anatomic rationale for concluding that the structure identified as the cystic duct was, in fact, the cystic duct whether it was traced onto the gallbladder or followed to the common bile duct or whether operative cholangiography was used for this purpose. Excessive bleeding obscuring the field was another operative factor that was searched for. RESULTS Patient demographics and injury type There were 18 women and 3 men, average age 37 years (range 16 to 78 years). The injuries occurred from 1990 to 1999; 11 of the 21 injuries occurred recently, in the years The injury types were E1, three patients; E2, four patients; E3, three patients; E4, eight patients; and E5, three patients (Fig. 2). Although E5 injuries involve damage to an aberrant duct, misidentification of the common
3 Vol. 191, No. 6, December 2000 Strasberg et al Hidden Cystic Duct Syndrome 663 bile duct as the cystic duct also occurs during this injury (Fig. 2), so this injury type is included in the analysis. The injury was discovered intraoperatively in 8 of the 21 patients. In the remainder the diagnosis was made in the postoperative period ranging from 2 days to 3 weeks after operation. Of these 13 patients, 7 presented with sepsis including cholangitis, 5 presented with jaundice as the main symptom, and 1 with a bile fistula. Operative notes There was great variability in the length and detail of the operative notes. But the subject matter of all operative notes was uniform up to the point in the dissection at which the cystic duct was clipped and divided. All describe, in varying degrees of detail, the preparation of the patient, creation of the pneumoperitoneum, insertion of trocars, retraction of the gallbladder, and isolation of the cystic duct (and sometimes artery). We divided the operative notes into two categories informative and uninformative, based on whether they contained patient or operative risk factors for biliary injury and whether the surgeon provided the anatomic rationale by which he identified the cystic duct conclusively in other words, what precautions were taken to avoid injury from misidentification. Uninformative operative notes provide almost no account of patient variables. In regard to operative factors, the description of the part of the operation in which the cystic duct was identified and divided in these notes may be paraphrased simply as: The cystic duct was isolated and divided. No statement is made that indicates the anatomic rationale for concluding that the cystic duct had been isolated. There were six notes of this type and they were all much shorter than the informative notes. The median number of text lines was 16 (range 13 to 18) to the point of cystic duct division. Fifteen operative notes were classified as informative. These notes always described conditions causing operative difficulty such as inflammation, and, with one exception, provided the anatomic rationale for identification of the cystic duct. Thirteen of these notes were 20 to 37 text lines in length (median 27) from the beginning of the note up to the point of cystic duct division. The other two notes were 54 and 70 text lines in length up to the Figure 2. Classification of laparoscopic injuries to the biliary tract. Injury types A to E are illustrated. Type E injuries are subdivided according to the Bismuth classification. Type A injuries are cystic duct leaks or leaks from small ducts in the liver bed. Type B and C injuries almost always involve aberrant right hepatic ducts. Type D injuries are lateral injuries to major bile ducts. The notations 2cm and 2cm in Type E1 and Type E2 indicate the length of common hepatic duct remaining. (From: Strasberg SM, Hertl M, Soper NJ. An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 1995;180: , with permission.) point of cystic duct division and went into great detail regarding preparation, draping, and position of personnel. Very few notes gave information regarding instrumentation, eg, type of laparoscope, type of cautery, or actual instruments used to perform the dissection.
4 664 Strasberg et al Hidden Cystic Duct Syndrome J Am Coll Surg Figure 3. Patient variables in 21 classical bile duct injuries. Filled circle indicates that variable was present. Patient variables (Fig. 3). Acute cholecystitis was present in 9 of 21 patients. In all cases it was noted to add to operative difficulty. In three other patients nonacute inflammation, ie, chronic inflammation and scarring, were noted and contributed to the difficulty of the procedure. So, inflammation was present and considered by the surgeon to add to operative difficulty in 12 of 21 patients. Increased thickness of the gallbladder and distension or tenseness of the gallbladder were described in nine and six patients, respectively. All but one description of distension and all but one of increase in wall thickness were found in operative notes of patients with acute cholecystitis. The presence of one or both of these factors was often accompanied by a remark that these factors led to problems in grasping or retracting the gallbladder, ie, operative difficulty. In three patients, all with acute cholecystitis, there was a notation that a large stone was impacted in the infundibulum, and that as a result, grasping and retraction of the gallbladder was made more difficult. Three operative notes indicated that there was trouble grasping the gallbladder because it was intrahepatic, and seven operative notes remarked on considerable numbers of adhesions that required dissection. Unlike the preceding three factors (distension, thickened wall, and impacted stone) intrahepatic site and adhesions were not specifically associated with inflammation (Fig. 3). Only one note described bleeding as a problem in visualizing the cystic duct and this was not in a case of inflammation. Two operative notes describe aberrant arterial anatomy with a cystic artery running in front of the cystic duct, which, in actuality, was probably a right hepatic artery that ran in front of the common hepatic duct, as it does in approximately 15% of patients. Operative variables. By far the most important finding in these notes was that in 17 of 21 procedures (81%) the cystic duct was isolated and divided as the first step in the dissection of the triangle of Calot, and that in none of the 21 patients was the triangle of Calot cleared of fat and fibrous tissue and the base of the gallbladder taken off the liver bed as described in the critical view technique. There is no mention of the cystic artery in these 17 operative notes until after division of the cystic duct. In the four other patients the surgeons note that the cystic artery was visible or was also isolated before division. Nine of 12 patients in whom inflammation was present and 8 of 9 patients in whom inflammation was not present were approached by the method in which the first step in the dissection of the triangle of Calot is the dissection, isolation, and division of the cystic duct.
5 Vol. 191, No. 6, December 2000 Strasberg et al Hidden Cystic Duct Syndrome 665 Table 1. Precise Paraphrases of Operative Statements Embodying the Anatomic Rationale for Identifying the Cystic Duct in Eight Patients with Injury to Common Bile Duct Patient No. Statement 1 Dissection was carried proximally along the cystic duct. It appeared to flare into the gallbladder. Dissection was carried onto the gallbladder for 1.5 cm, proving that the duct was the cystic duct. 2 The cystic duct was isolated and there appeared to be a continuous cystic duct coming from the gallbladder. 3 The cystic duct was identified and seen to enter the gallbladder in the appropriate direction. 4 The cystic duct was isolated and appeared to arise at the gallbladder. 5 A tubular structure arising from the inferior aspect of the gallbladder was isolated. The infundibulum was mobilized and the structure was seen to enter the gallbladder. 6 The neck of the gallbladder was identified and the cystic duct dissected and isolated. 7 A structure was identified which came right off the infundibulum. This appeared to be the cystic duct and was dissected circumferentially. 8 Dissection is commenced as close to the gallbladder as possible. The cystic duct is dissected out and a clip is placed next to the gallbladder. Closer scrutiny was made of the 17 procedures in which isolation and division of the cystic duct was the first step in dissection of the triangle of Calot in an attempt to determine how the common bile duct was misidentified as the cystic duct. In 7 of 17 patients there was no statement regarding the anatomic rationale for identification. In two cases the surgeon states that the cystic duct was followed to the junction of the common bile duct. But in the other eight patients the surgeon derived identification from a relationship between what was perceived as the cystic duct and the neck of the gallbladder. The relevant operative statements are given in a precisely paraphrased form in Table 1. Note that in each instance the surgeon believed that he saw the cystic duct emanating from the gallbladder. Stated otherwise, in 8 of 10 operative notes in which the rationale for avoidance of misidentification was available, that rationale was that the surgeon believed he had seen the cystic duct join the gallbladder, ie, the infundibular technique of identification failed in its purpose. Cholangiography was performed in four patients. Dye did not enter upper bile ducts in any these studies. Only the common bile duct and duodenum were seen. In three patients this finding was not considered abnormal and the cystic duct was divided. In fact, the common bile duct was divided and the injury was carried to a much higher level in the subsequent dissection leading to an E3 and two E4 injuries. In two of these patients the common hepatic duct was found to be applied to the gallbladder when the specimen was removed. In the fourth patient, it was recognized that there might be a problem when dye did not fill the upper ducts. The surgeon thought this might be from leakage of dye around the cholangiography catheter. He attempted to improve closure around the catheter but this led to tearing of the common bile duct and an E1 injury. DISCUSSION The infundibular technique of laparoscopic cholecystectomy and biliary injury The major finding of this study is that infundibular technique for identification of the cystic duct appears to be unreliable. Nearly 80% of the injuries examined occurred using a technique in which the cystic duct was identified and divided before dissection of the rest of the triangle of Calot. In 8 of 10 patients in whom the anatomic rationale for identification of ducts was provided, it was that the surgeon thought he saw the cystic duct join the infundibulum of the gallbladder, ie, the anatomic rationale inherent in the infundibular technique was used. Figure 4 illustrates the flaw that appears to be present in the infundibular technique. On the left is what the surgeons believed they have achieved up to the point in the dissection when they are ready to occlude and divide the cystic duct. It appears that the cystic duct can be seen emanating from the gallbladder. This is based on the fact that the sides of the tubular structure, which has been isolated and followed toward the gallbladder, are diverging, ap-
6 666 Strasberg et al Hidden Cystic Duct Syndrome J Am Coll Surg Figure 4. The deception of the hidden cystic duct and the infundibular technique of laparoscopic cholecystectomy. Left: Appearance to surgeon when a duct appearing to be the cystic duct is dissected first. Note that the duct appears to flare (heavy black line), giving the appearance that the cystic duct has been followed onto the infundibulum. Right: True anatomic situation in the case of some classical injuries. The flare (heavy black line) is from the separation of cystic and common hepatic ducts or the side of the common hepatic duct and the side of the gallbladder. Note that such a deception is impossible if the dissection is carried to the critical view (Fig. 1) before dividing any structure. parently to become the infundibulum of the gallbladder. The appearance is deceptively similar to what has been seen on many earlier occasions as the true cystic duct enlarged to become the infundibulum of the gallbladder. The picture on the right shows the true anatomic situation in the case of misidentification; the common bile duct has been isolated and the divergence of its walls as it comes near the gallbladder is from its division into the cystic duct and common hepatic duct. These two structures naturally diverge at this point. As a result of the apparent widening or flaring of the presumed cystic duct, the surgeon concludes that he is on the infundibulum of gallbladder, but it is a false infundibulum. This appearance seems also to be caused sometimes by the inflamed gallbladder overlying the cystic duct, common hepatic duct, or both, so that the sides of the common bile duct do actually appear to expand onto the gallbladder. The surgeon thinks he is operating on the cystic duct at the edge of the gallbladder but actually the dissection is taking place on the common bile duct at the edge of an inflammatory mass in which the cystic duct is hidden. An infundibulum seems to have been identified but again it is a false infundibulum. Hiding the cystic duct the role of inflammation and other factors The operative notes indicate that the problem of a false infundibulum is much more likely under certain conditions. The most important is extensive inflammation, especially acute inflammation. The chief reason for this has already been noted; inflammation of the gallbladder tends to hide the cystic duct. Inability to effectively grasp and retract the gallbladder and thereby straighten and expose the cystic duct also appears to be important. Under these circumstances it seems more likely that dissection will begin below the inflammation around the left and right sides of the common bile duct rather than on the front and back of the triangle of Calot. Other factors that obscure the position of the cystic duct include large impacted stones; effacement of the cystic duct so that it is short or absent, as in Mirizzi s syndrome; and adhesions that tether the common duct to the gallbladder, hiding the cystic duct. 12 The role of intraoperative cholangiography Routine cystic duct cholangiography reduces the incidence of biliary injury, as demonstrated in a recent report from Australia by Fletcher and colleagues. 14 Cholangiography was performed in only 4 of 21 patients in this series and was misinterpreted in 3 patients. Intraoperative cholangiography, if correctly interpreted, undoubtedly would have prevented, or at least reduced, the extent of injury in many patients in this series. Obviously, a cholangiogram is of little use if it is not correctly interpreted. Cholangiography has problems other than that images may be misinterpreted and injury still occur. Mistaken cannulation of the common bile duct for the purpose of anatomic identification may not be innocuous. It will, at the least, require conversion and repair over a T-tube and, at worst, require biliary reconstruction. This was shown in one patient in this series in whom attempts at cholangiography, through what was mistakenly believed to be the cystic duct, led to an E1 injury of the common bile duct. Also cystic duct cholangiography does not reliably identify the presence of aberrant right hepatic ducts 9 and may not prevent these types of injuries (Type B and C, Fig. 2), which are much more common when performing laparoscopic cholecystectomy than
7 Vol. 191, No. 6, December 2000 Strasberg et al Hidden Cystic Duct Syndrome 667 open cholecystectomy. 15 In the era of open cholecystectomy, routine cholangiography was not advocated as the standard technique of anatomic identification, but rather as a technique of bile duct stone identification. The standard technique of conclusive identification was by dissection using a method analogous to the critical view technique. Teaching laparoscopic cholecystectomy Although this series is small, there is a very high degree of consistency in the findings. They strongly suggest that the infundibular technique for identification of the cystic duct is unreliable, especially under conditions of acute inflammation. Given the serious consequences of a biliary injury and the fact that other, more secure methods for identification exist, it would be logical to abandon the infundibular technique. This technique is advocated in many texts on laparoscopic surgery, and is in common use. Its proponents would argue that the technique is good, the failure in the cases in this series being from misapplication of the method, and not from a flaw in the rationale. But it is apparent that well-trained, skilled, and experienced surgeons are involved in these injuries and there is now a clear understanding of how surgeons can be misled by a hidden cystic duct and the appearance of false infundibulum. Our findings suggest that it is unsafe and should be abandoned as a standard method of laparoscopic cholecystectomy. None of the injuries occurred in operations in which the cystic duct was fully dissected out as recommended in the critical view technique. Cholangiography demonstrated an abnormality in all patients in whom it was used, and injury would have been avoided or reduced if interpretation had been appropriate. In the critical view technique, isolation of the cystic duct is not the object of the initial part of the dissection as in the infundibular technique. The object is to clear the triangle of Calot entirely of fat and fibrous tissue so that two, and only two, structures are seen to enter the gallbladder, and the base of the gallbladder is taken off the liver bed. It is highly unlikely that visual deception will occur if the dissection is carried to this point. If the critical view is not attainable the dissection is stopped. Then the operation is converted or a cholangiogram is performed for the purpose of anatomic identification. The use of cholangiography selectively under these circumstances mimics its use for anatomic identification in open cholecystectomy. Our study suggests that either one adopt this approach or that routine cholangiography, as suggested by others, 14 be used once the presumed cystic duct is isolated. Our bias is that anatomic identification be done by dissection rather than cholangiography, for reasons stated above. The infundibular technique, meaning a technique in which one relies on the shape of the infudibulocystic junction as the sole method of anatomic identification should be abandoned. References 1. Bernard HR. Laparoscopic cholecystectomy: the New York experience. J Laparoendosc Surg 1993;3: Adamsen S, Hansen OH, Funch-Jensen P, et al. Bile duct injury during laparoscopic cholecystectomy: a prospective nationwide series. J Am Coll of Surg 1997;184: Russell JC, Walsh SJ, Mattie AS, Lynch JT. Bile duct injuries, A statewide experience. Connecticut Laparoscopic Cholecystectomy Registry. Arch Surg 1996;131: Davidoff AM, Pappas TN, Murray EA, et al. Mechanisms of major biliary injury during laparoscopic cholecystectomy [see comments]. Ann Surg 1992;215: Lillemoe KD, Martin SA, Cameron JL, et al. Major bile duct injuries during laparoscopic cholecystectomy. Follow-up after combined surgical and radiologic management. Ann Surg 1997; 225: Murr MM, Gigot JF, Nagorney DM, et al. Long-term results of biliary reconstruction after laparoscopic bile duct injuries. Arch Surg 1999;134: Walsh RM, Henderson JM, Vogt DP, et al. Trends in bile duct injuries from laparoscopic cholecystectomy. J Gastrointest Surg 1998;2: Anonymous. A prospective analysis of 1518 laparoscopic cholecystectomies. The Southern Surgeons Club. N Engl J of Med 1991;324: Strasberg SM, Hertl M, Soper NJ. An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 1995;180: Hunter JG. Avoidance of bile duct injury during laparoscopic cholecystectomy. Am J Surg 1991;162: Asbun HJ, Rossi RL, Lowell JA, Munson JL. Bile duct injury during laparoscopic cholecystectomy: mechanism of injury, prevention, and management. World J Surg 1993;17: Brunt LM, Soper NJ. Laparoscopic cholecystectomy; early results and complications. Compl Surg 1993;12: Strasberg SM. Laparoscopic cholecystectomy. In: Cameron JL, ed. Current surgical therapy. 6th ed. Baltimore, MD: Mosby; 1998: Fletcher DR, Hobbs MS, Tan P, et al. Complications of cholecystectomy: risks of the laparoscopic approach and protective effects of operative cholangiography: a population-based study. Ann Surg 1999;229: Meyers WC, Peterseim DS, Pappas TN, et al. Low insertion of hepatic segmental duct VII VIII is an important cause of major biliary injury or misdiagnosis. Am J Surg 1996;171:
Bile Leaks After Laparoscopic Cholecystectomy. Kings County Hospital Center Eliana A. Soto, MD
 Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Biliary Injury in Laparoscopic Surgery: Part 1. Processes Used in Determination of Standard of Care in Misidentification Injuries
 EDUCATION Biliary Injury in Laparoscopic Surgery: Part 1. Processes Used in Determination of Standard of Care in Misidentification Injuries Steven M Strasberg, MD, FACS Biliary injury is a major cause
EDUCATION Biliary Injury in Laparoscopic Surgery: Part 1. Processes Used in Determination of Standard of Care in Misidentification Injuries Steven M Strasberg, MD, FACS Biliary injury is a major cause
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives
 Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Gallbladder - gallstones and surgery
 Gallbladder - gallstones and surgery Summary Gallstones are small stones made from cholesterol, bile pigment and calcium salts, which form in a person s gall bladder. Medical treatment isn t necessary
Gallbladder - gallstones and surgery Summary Gallstones are small stones made from cholesterol, bile pigment and calcium salts, which form in a person s gall bladder. Medical treatment isn t necessary
Insurer s Spin Defense to Bile Duct Transection
 Insurer s Spin Defense to Bile Duct Transection By: Thomas T. Dunbar All agree that a common bile duct transection arising from a gallbladder surgery can be a devastating injury, life-threatening, and
Insurer s Spin Defense to Bile Duct Transection By: Thomas T. Dunbar All agree that a common bile duct transection arising from a gallbladder surgery can be a devastating injury, life-threatening, and
Gallbladder Diseases and Problems
 Gallbladder Diseases and Problems Introduction Your gallbladder is a pear-shaped organ under your liver. It stores bile, a fluid made by your liver to digest fat. There are many diseases and problems that
Gallbladder Diseases and Problems Introduction Your gallbladder is a pear-shaped organ under your liver. It stores bile, a fluid made by your liver to digest fat. There are many diseases and problems that
Biliary Stone Disease
 Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Biliary Stone Disease Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm You have
Clinical Anatomy of the Biliary Apparatus: Relations & Variations
 Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 24 January 2012 Lawrence M. Witmer, PhD Professor of Anatomy Department
Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 24 January 2012 Lawrence M. Witmer, PhD Professor of Anatomy Department
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS
 WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
WHAT S WRONG WITH MY GALL BLADDER? GALL BLADDER POLYPS This is a patient information booklet providing specific practical information about gall bladder polyps in brief. Its aim is to provide the patient
Preoperative Diagnosis and Efficacy of Laparoscopic Procedures in the Treatment of Mirizzi Syndrome
 Preoperative Diagnosis and Efficacy of Laparoscopic Procedures in the Treatment of Mirizzi Syndrome A-Hon Kwon, MD, Hiroaki Inui, MD BACKGROUND: STUDY DESIGN: RESULTS: CONCLUSIONS: The role of laparoscopic
Preoperative Diagnosis and Efficacy of Laparoscopic Procedures in the Treatment of Mirizzi Syndrome A-Hon Kwon, MD, Hiroaki Inui, MD BACKGROUND: STUDY DESIGN: RESULTS: CONCLUSIONS: The role of laparoscopic
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Bile Duct Diseases and Problems
 Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
UCLA Asian Liver Program
 CLA Program Update Program Faculty Myron J. Tong, PhD, MD Professor of Medicine Hepatology Director, Asian Liver Program Surgery Ronald W. Busuttil, MD, PhD Executive Chair Department of Surgery Director,
CLA Program Update Program Faculty Myron J. Tong, PhD, MD Professor of Medicine Hepatology Director, Asian Liver Program Surgery Ronald W. Busuttil, MD, PhD Executive Chair Department of Surgery Director,
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
 Redo Banding After Band Erosion Advantages of the MiniMizer Extra Band Conclusion Approximately 67% of the patients suffering from erosion have sought revisional surgery. The choice of redo procedures
Redo Banding After Band Erosion Advantages of the MiniMizer Extra Band Conclusion Approximately 67% of the patients suffering from erosion have sought revisional surgery. The choice of redo procedures
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Red Flags. Whether you handle malpractice. in General Surgical Malpractice Cases
 10 Red Flags in General Surgical Malpractice Cases Whether you handle malpractice cases regularly or you have a general personal injury practice, at some point you likely will need to evaluate a general
10 Red Flags in General Surgical Malpractice Cases Whether you handle malpractice cases regularly or you have a general personal injury practice, at some point you likely will need to evaluate a general
Facing Gallbladder Surgery? Learn why Single-Site da Vinci Surgery may be your best option for virtually scarless results.
 Facing Gallbladder Surgery? Learn why Single-Site da Vinci Surgery may be your best option for virtually scarless results. The Condition: Gallstones and Gallbladder Diseases Your gallbladder is a pear-shaped
Facing Gallbladder Surgery? Learn why Single-Site da Vinci Surgery may be your best option for virtually scarless results. The Condition: Gallstones and Gallbladder Diseases Your gallbladder is a pear-shaped
Pathway for the Management of Acute Gallstone Diseases
 Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
Gallstone Ileus. Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005
 Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
Gallstone Ileus Audrey C. Durrant,, M.D. SUNY Downstate Medical Center May 20, 2005 Gallstone Ileus Diagnosis and Management Background Misnomer coined by Bartolin in 1654 Not a true ileus True mechanical
restricted to certain centers and certain patients, preferably in some sort of experimental trial format.
 Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Computer Graphics in Medicine
 Computer Graphics in Medicine Loren Block For my presentation, I will discuss several different papers that are related to graphics and imaging in the medical field. The main areas that the papers cover
Computer Graphics in Medicine Loren Block For my presentation, I will discuss several different papers that are related to graphics and imaging in the medical field. The main areas that the papers cover
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY. Dr. Shailesh V. Shrikhande
 PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
PANCREATIC AND PERIAMPULLARY TUMORS: PANCREATICODUODENECTOMY Dr. Shailesh V. Shrikhande Associate Professor & Consultant Surgeon GI and HPB Surgical Oncology Tata Memorial Hospital, Mumbai INDIA HELICAL
Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct)
 Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct) Section 1 Service Details Service ID: 7540540 Service Comments: Referrer Alert: Service
Service Definition with all Clinical Terms Service: Laprascopic Cholecystectomy Clinic (No Gallstones in bile duct) Section 1 Service Details Service ID: 7540540 Service Comments: Referrer Alert: Service
Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy
 CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
Laparoscopic Cholecystectomy (Removal of the Gallbladder)
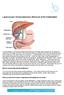 Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
Laparoscopic Cholecystectomy (Removal of the Gallbladder) The gall bladder is a small pear-shaped organ that lies in the right upper quadrant of your abdomen under your liver (under your ribs). The liver
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
COMPLICATIONS OF FISTULA REPAIR SURGERY. Sherif Mourad
 COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
COMPLICATIONS OF FISTULA REPAIR SURGERY Sherif Mourad In the developing world, the true incidence of obstetric fistulas is unknown, as many patients with this condition suffer in silence and isolation.
Laparoscopic Sleeve gastrectomy
 Restrictive procedure Laparoscopic Sleeve gastrectomy Dr. R. Peterli Professional Education 1 2 Introduction Gastric sleeve resection is the restrictive part of the biliopancreatic diversion duodenal switch,
Restrictive procedure Laparoscopic Sleeve gastrectomy Dr. R. Peterli Professional Education 1 2 Introduction Gastric sleeve resection is the restrictive part of the biliopancreatic diversion duodenal switch,
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience
 Bahrain Medical Bulletin 29, No. 3, September 2007 Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience Mohamed H. Durazi, FRCS ED, FRCSI* Reem Al-Bareeq, MRCSI, CAB(Urol)** Mohamed
Bahrain Medical Bulletin 29, No. 3, September 2007 Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience Mohamed H. Durazi, FRCS ED, FRCSI* Reem Al-Bareeq, MRCSI, CAB(Urol)** Mohamed
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
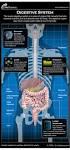 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
CHAPTER 10 Uterine Synechiae
 CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
CHAPTER 10 Uterine Synechiae Uterine synechiae are intrauterine adhesions. They may involve small focal areas of the endometrium (Figures 10.1a e), or they can be so extensive that they obliterate the
Berkeley, CA 94720 ABSTRACT. In conjunction with eorts, based on task and error analysis, in the Videoscopic Training Center at UCSF to
 Development of Virtual Environments for Training Skills and Reducing Errors in Laparoscopic Surgery Frank Tendick a, Michael Downes b, M. Cenk Cavusoglu b, Walter Gantert a, and Lawrence W. Way a adepartment
Development of Virtual Environments for Training Skills and Reducing Errors in Laparoscopic Surgery Frank Tendick a, Michael Downes b, M. Cenk Cavusoglu b, Walter Gantert a, and Lawrence W. Way a adepartment
VIRTUAL ENVIRONMENTS FOR TRAINING CRITICAL SKILLS IN LAPAROSCOPIC SURGERY
 VIRTUAL ENVIRONMENTS FOR TRAINING CRITICAL SKILLS IN LAPAROSCOPIC SURGERY MICHAEL DOWNES (1), M. Cenk Cavusoglu, MS (1), Walter Gantert, MD (2), Lawrence W. Way, MD (2), Frank Tendick, PhD (2) (1) Department
VIRTUAL ENVIRONMENTS FOR TRAINING CRITICAL SKILLS IN LAPAROSCOPIC SURGERY MICHAEL DOWNES (1), M. Cenk Cavusoglu, MS (1), Walter Gantert, MD (2), Lawrence W. Way, MD (2), Frank Tendick, PhD (2) (1) Department
Presumptive Cancers Due to Agent Orange Exposure & Cholangiocarcinoma (Bile Duct - Liver Fluke Cancer)
 Presumptive Cancers Due to Agent Orange Exposure & Cholangiocarcinoma (Bile Duct - Liver Fluke Cancer) Presumptive Cancers Due to Agent Orange Exposure Prostate Cancer - Cancer of the prostate; one of
Presumptive Cancers Due to Agent Orange Exposure & Cholangiocarcinoma (Bile Duct - Liver Fluke Cancer) Presumptive Cancers Due to Agent Orange Exposure Prostate Cancer - Cancer of the prostate; one of
KnifeLight. Carpal Tunnel Ligament Release. Operative Technique
 KnifeLight Carpal Tunnel Ligament Release Operative Technique Contents Page 1. Features & Benefits 3 Intended Use and Indications 3 Contraindications 3 Features & Benefits 3 2. Operative Technique 4 Antegrade
KnifeLight Carpal Tunnel Ligament Release Operative Technique Contents Page 1. Features & Benefits 3 Intended Use and Indications 3 Contraindications 3 Features & Benefits 3 2. Operative Technique 4 Antegrade
ERCP in Post Surgical Anatomy
 ERCP in Post Surgical Anatomy ACG Western Regional Course, 2013 John G. Lee, MD Division of Gastroenterology University of California, Irvine Medical Center Common surgical alterations Intact pancreaticobiliary
ERCP in Post Surgical Anatomy ACG Western Regional Course, 2013 John G. Lee, MD Division of Gastroenterology University of California, Irvine Medical Center Common surgical alterations Intact pancreaticobiliary
Minilaparoscopic cholecystectomy the new non-visible scars technique. Preliminary report of first series
 Original paper Videosurgery Minilaparoscopic cholecystectomy the new non-visible scars technique. Preliminary report of first series Tadeusz M. Wróblewski 1, Konrad Kobryń 1, Łukasz Nazarewski 1, Marta
Original paper Videosurgery Minilaparoscopic cholecystectomy the new non-visible scars technique. Preliminary report of first series Tadeusz M. Wróblewski 1, Konrad Kobryń 1, Łukasz Nazarewski 1, Marta
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality. Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006
 The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
The Whipple Operation for Pancreatic Cancer: Optimism vs. Reality Franklin Wright UCHSC Department of Surgery Grand Rounds September 11, 2006 Overview Pancreatic ductal adenocarcinoma Pancreaticoduodenectomy
Heel Pain Syndromes DELLON INSTITUTES FOR PERIPHERAL NERVE SURGERY
 Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
Long-term follow-up after biliary stent placement for postoperative bile duct stenosis
 Long-term follow-up after biliary stent placement for postoperative bile duct stenosis Jacques J. G. H. M. Bergman, MD, Lotje Burgemeister, MD, Marco J. Bruno, MD, Erik A. J. Rauws, MD, Dirk J. Gouma,
Long-term follow-up after biliary stent placement for postoperative bile duct stenosis Jacques J. G. H. M. Bergman, MD, Lotje Burgemeister, MD, Marco J. Bruno, MD, Erik A. J. Rauws, MD, Dirk J. Gouma,
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
2FORMATS AND CONVENTIONS
 2FORMATS AND CONVENTIONS OF DIAGNOSIS CODING SYSTEMS Learning Outcomes After completing this chapter, students should be able to 2.1 Explain the layout of the ICD-9-CM and ICD-10-CM manuals. 2.2 Differentiate
2FORMATS AND CONVENTIONS OF DIAGNOSIS CODING SYSTEMS Learning Outcomes After completing this chapter, students should be able to 2.1 Explain the layout of the ICD-9-CM and ICD-10-CM manuals. 2.2 Differentiate
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
IN THE CIRCUIT COURT OF THE STATE OF OREGON FOR THE COUNTY OF [COUNTY]
![IN THE CIRCUIT COURT OF THE STATE OF OREGON FOR THE COUNTY OF [COUNTY] IN THE CIRCUIT COURT OF THE STATE OF OREGON FOR THE COUNTY OF [COUNTY]](/thumbs/26/8837397.jpg) IN THE CIRCUIT COURT OF THE STATE OF OREGON FOR THE COUNTY OF [COUNTY] [PLAINTIFF], CASE NO. Plaintiff, (Negligence Medical Malpractice v. Claim Not Subject to Mandatory Arbitration [NAMES] (Prayer Amount
IN THE CIRCUIT COURT OF THE STATE OF OREGON FOR THE COUNTY OF [COUNTY] [PLAINTIFF], CASE NO. Plaintiff, (Negligence Medical Malpractice v. Claim Not Subject to Mandatory Arbitration [NAMES] (Prayer Amount
SILS. Port Insertion By Homero Rivas, MD, MBA, FACS. Single incision. Single port. Simple choice.
 SILS Port Insertion By Homero Rivas, MD, MBA, FACS Single incision. Single port. Simple choice. SILS Port Insertion By Homero Rivas, MD, MBA, FACS For the last 20 years, there has given surgical procedure.
SILS Port Insertion By Homero Rivas, MD, MBA, FACS Single incision. Single port. Simple choice. SILS Port Insertion By Homero Rivas, MD, MBA, FACS For the last 20 years, there has given surgical procedure.
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Guidelines for the Clinical Application of Laparoscopic Biliary Tract Surgery
 Guidelines for the Clinical Application of Laparoscopic Biliary Tract Surgery I. PREAMBLE Laparoscopic cholecystectomy has become the standard of care for patients requiring the removal of the gallbladder.
Guidelines for the Clinical Application of Laparoscopic Biliary Tract Surgery I. PREAMBLE Laparoscopic cholecystectomy has become the standard of care for patients requiring the removal of the gallbladder.
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Endoscopic Management of Strictures and Leaks. Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center
 Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
Endoscopic Management of Strictures and Leaks Prepared by Aurora D. Pryor, MD Presented by Dana Portenier, MD Duke University Medical Center What can go wrong? Bleeding (2%) Sleeve too big Angulated Too
BACKGROUND MEDIA INFORMATION Fast facts about liver disease
 BACKGROUND MEDIA INFORMATION Fast facts about liver disease Liver, or hepatic, disease comprises a wide range of complex conditions that affect the liver. Liver diseases are extremely costly in terms of
BACKGROUND MEDIA INFORMATION Fast facts about liver disease Liver, or hepatic, disease comprises a wide range of complex conditions that affect the liver. Liver diseases are extremely costly in terms of
Liver Diseases. An Essential Guide for Nurses and Health Care Professionals
 Brochure More information from http://www.researchandmarkets.com/reports/1047385/ Liver Diseases. An Essential Guide for Nurses and Health Care Professionals Description: Liver disease is a rapidly growing
Brochure More information from http://www.researchandmarkets.com/reports/1047385/ Liver Diseases. An Essential Guide for Nurses and Health Care Professionals Description: Liver disease is a rapidly growing
Journal Name: International Journal of Hepatobiliary and Pancreatic Diseases (IJHPD)
 ACCEPTED MAN U SCRIPT EARLY VIEW ARTICLE Early View Article: Online published version of an accepted article before inclusion in an issue of International Journal of Hepatobiliary and Pancreatic Diseases
ACCEPTED MAN U SCRIPT EARLY VIEW ARTICLE Early View Article: Online published version of an accepted article before inclusion in an issue of International Journal of Hepatobiliary and Pancreatic Diseases
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Liver Transplantation for Hepatocellular Carcinoma. John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco
 Liver Transplantation for Hepatocellular Carcinoma John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco Hepatocellular Carcinoma HCC is the 5th most common
Liver Transplantation for Hepatocellular Carcinoma John P. Roberts, MD Chief, Division of Transplant Service University of California, San Francisco Hepatocellular Carcinoma HCC is the 5th most common
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Surgeon perception is not a good predictor of peri-operative outcomes in robot-assisted radical prostatectomy
 DOI 10.1007/s11701-011-0293-4 ORIGINAL ARTICLE Surgeon perception is not a good predictor of peri-operative outcomes in robot-assisted radical prostatectomy Joshua Stern Saurabh Sharma Pierre Mendoza Mary
DOI 10.1007/s11701-011-0293-4 ORIGINAL ARTICLE Surgeon perception is not a good predictor of peri-operative outcomes in robot-assisted radical prostatectomy Joshua Stern Saurabh Sharma Pierre Mendoza Mary
Bile Leak after Laparoscopic Cholecystectomy. Sybile Val MD Long Island College Hospital September 22, 2006
 Bile Leak after Laparoscopic Cholecystectomy Sybile Val MD Long Island College Hospital September 22, 2006 History and Physical Chief Complaint: Severe abdominal pain x one day HPI: Patient is a xx year
Bile Leak after Laparoscopic Cholecystectomy Sybile Val MD Long Island College Hospital September 22, 2006 History and Physical Chief Complaint: Severe abdominal pain x one day HPI: Patient is a xx year
By James D. Gould, MD FACS
 By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
SURGICAL PREAMBLE SPECIFIC ELEMENTS SURGICAL SERVICES WHICH ARE NOT LISTED AS A "Z" CODE
 Surgical PreambleApril 1, 2015 PREAMBLE SPECIFIC ELEMENTS In addition to the common elements, all surgical services include the following specific elements. A. Supervising the preparation of and/or preparing
Surgical PreambleApril 1, 2015 PREAMBLE SPECIFIC ELEMENTS In addition to the common elements, all surgical services include the following specific elements. A. Supervising the preparation of and/or preparing
PLASTIC SURGERY RESIDENTS HANDBOOK
 PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
Plantar Fascia Release
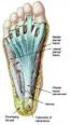 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
Basic Laparoscopy and Lap. Suturing and Stapling course Course Contents
 Online Courses on Laparoscopic GI Surgery for GISurgery.info Lap Skills course Harshad Soni 1. Basic Laparoscopy and Lap. Suturing and Stapling course H. Soni 2. Laparoscopic UGI Surgery Course J Mistry
Online Courses on Laparoscopic GI Surgery for GISurgery.info Lap Skills course Harshad Soni 1. Basic Laparoscopy and Lap. Suturing and Stapling course H. Soni 2. Laparoscopic UGI Surgery Course J Mistry
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery
 Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
AORTOENTERIC FISTULA. Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005
 AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
AORTOENTERIC FISTULA Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA diagnosis and management Mark H. Tseng MD Brooklyn VA Hospital February 11, 2005 AORTOENTERIC FISTULA Aortoenteric
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
sufficiently during choledochostomy to result in stricture formation; however, the biliary tract in the prevention of these lesions.
 STRICTURES OF THE COMMON DUCT* WARREN H. COLE, M.D., JOHN T. REYNOLDS, M.D., AND CARL IRENEUS, JR., M.D. CHICACO, ILL. ALTHOUGH THERE HAS BEEN GREAT IMPROVEMENT in the results following repair of strictures
STRICTURES OF THE COMMON DUCT* WARREN H. COLE, M.D., JOHN T. REYNOLDS, M.D., AND CARL IRENEUS, JR., M.D. CHICACO, ILL. ALTHOUGH THERE HAS BEEN GREAT IMPROVEMENT in the results following repair of strictures
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON. Director of surgical department of Lefkos Stavros of Athens
 Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
GIANT HERNIA REPAIR MY EXPERIENCE
 GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
GIANT HERNIA REPAIR MY EXPERIENCE Giorgobiani G. Department of Surgery at Tbilisi State Medical University. The AVERSI Clinic.Tbilisi, Georgia. If we could artificially produce tissue of the density and
Case 1. 79 y old woman Medical history: Diabetes insuline treatment Hypertension Obesity CABG + Pacemaker Ilocolic resection for T2 colonadenoca 2009
 Cholangitis Difficult stone management D. De Wulf AZ Delta Roeselare UZ Gent Case 1 79 y old woman Medical history: Diabetes insuline treatment Hypertension Obesity CABG + Pacemaker Ilocolic resection
Cholangitis Difficult stone management D. De Wulf AZ Delta Roeselare UZ Gent Case 1 79 y old woman Medical history: Diabetes insuline treatment Hypertension Obesity CABG + Pacemaker Ilocolic resection
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
PLANTAR FASCITIS (Heel Spur Syndrome)
 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
When, Why, and How to Revise a Failed Sleeve Gastrectomy
 When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
LIVER CARE CENTER. stlouischildrens.org
 LIVER CARE CENTER stlouischildrens.org One of North America s Premier Pediatric Liver Care Centers The Liver Care Center at St. Louis Children s Hospital and Washington University School of Medicine is
LIVER CARE CENTER stlouischildrens.org One of North America s Premier Pediatric Liver Care Centers The Liver Care Center at St. Louis Children s Hospital and Washington University School of Medicine is
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery
 Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
An External Audit of Laparoscopic Cholecystectomy Performed
 ANNALS OF SURGERY Vol. 220, No. 5,626-634 A 1994 J. B. Lippincott Company An External Audit of Laparoscopic Cholecystectomy Performed in Medical Treatment Facilities of the Department of Defense David
ANNALS OF SURGERY Vol. 220, No. 5,626-634 A 1994 J. B. Lippincott Company An External Audit of Laparoscopic Cholecystectomy Performed in Medical Treatment Facilities of the Department of Defense David
Gallstones. National Digestive Diseases Information Clearinghouse
 Gallstones National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health and Human Services
Gallstones National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health and Human Services
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
"Statistical methods are objective methods by which group trends are abstracted from observations on many separate individuals." 1
 BASIC STATISTICAL THEORY / 3 CHAPTER ONE BASIC STATISTICAL THEORY "Statistical methods are objective methods by which group trends are abstracted from observations on many separate individuals." 1 Medicine
BASIC STATISTICAL THEORY / 3 CHAPTER ONE BASIC STATISTICAL THEORY "Statistical methods are objective methods by which group trends are abstracted from observations on many separate individuals." 1 Medicine
Impact of Model-based Risk Analysis for Liver Surgery Planning
 Impact of Model-based Risk Analysis for Liver Surgery Planning C. Hansen¹, S.Zidowitz 1, B. Preim 2, G. Stavrou 3, K. J. Oldhafer 3, H. K. Hahn 1 1 Fraunhofer MEVIS, Institute for Medical Image Computing,
Impact of Model-based Risk Analysis for Liver Surgery Planning C. Hansen¹, S.Zidowitz 1, B. Preim 2, G. Stavrou 3, K. J. Oldhafer 3, H. K. Hahn 1 1 Fraunhofer MEVIS, Institute for Medical Image Computing,
Corneal Collagen Cross-Linking (CXL) With Riboflavin
 Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Dr. Paul J. Dubord, MD, FRCSC Clinical Professor Department of Ophthalmology and Visual Sciences University of British Columbia Patient Information Guide Corneal Collagen Cross-Linking (CXL) With Riboflavin
Laparoscopic Trainer Product Catalog
 Laparoscopic Trainer Product Catalog Laparoscopic Trainer Product Catalog Simsei Table of Contents Laparoscopic Trainers 6 Organ Models 8 Skill Exercises 11 Accessories 12 Additional Information About
Laparoscopic Trainer Product Catalog Laparoscopic Trainer Product Catalog Simsei Table of Contents Laparoscopic Trainers 6 Organ Models 8 Skill Exercises 11 Accessories 12 Additional Information About
PROPERTY OF ELSEVIER SAMPLE CONTENT - NOT FINAL
 Oncoplastic breast conservation surgery Melvin J Silverstein C H A P T E R 5 Introduction Oncoplastic breast conservation surgery combines oncologic principles with plastic surgical techniques. But it
Oncoplastic breast conservation surgery Melvin J Silverstein C H A P T E R 5 Introduction Oncoplastic breast conservation surgery combines oncologic principles with plastic surgical techniques. But it
Women s Health Laparoscopy Information for patients
 Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
Women s Health Laparoscopy Information for patients This leaflet is for women who have been advised to have a laparoscopy. It outlines the common reasons doctors recommend this operation, what will happen
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy. Case Series
 ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
