Minimally invasive corpectomy and posterior stabilization for lumbar burst fracture
|
|
|
- Francine Lang
- 7 years ago
- Views:
Transcription
1 The Spine Journal -- (2011) e1 e5 Case Report Minimally invasive corpectomy and posterior stabilization for lumbar burst fracture Jason C. Eck, DO, MS* Department of Orthopedic Surgery, University of Massachusetts, 119 Belmont St, Worcester, MA 01605, USA Received 5 October 2010; revised 6 March 2011; accepted 14 June 2011 Abstract Keywords: BACKGROUND CONTEXT: Surgical indications for lumbar burst fracture remain controversial. Potential indications for surgery include 50% canal compromise, 50% loss of vertebral height, 30 of kyphosis, and posterior element fracture or disruption of the posterior ligamentous complex. Different surgical approaches are available depending on fracture characteristics. It is possible that a minimally invasive approach could allow for a safe and effective treatment with fewer comorbidities than the traditional open technique. PURPOSE: This is a report of an L3 burst fracture treated with a minimally invasive approach for anterior corpectomy and posterior pedicle screw fixation. STUDY DESIGN: Case report. PATIENT SAMPLE: Patient with L3 burst fracture. OUTCOME MEASURES: Radiographs and computed tomography scans to evaluate for fusion and evaluation of pain and neurologic function. METHODS: A 30-year-old male was involved in a head-on motor vehicle collision. Initial imaging revealed an L3 burst fracture with 60% canal compromise, 50% loss of vertebral body height, a large anteriorly displaced fragment consisting of 40% of the vertebral body depth, and a facet fracture. Surgical decompression and stabilization were recommended for this patient because of radiographic signs of instability. After medical clearance and consent, the patient underwent a minimally invasive L3 corpectomy and L2 L4 interbody fusion through a direct lateral approach with placement of a titanium mesh cage filled with local autograft and allograft bone matrix. The patient then underwent a percutaneous stabilization with pedicle screw fixation from L2 to L4. RESULTS: The patient was ambulating on the first postoperative day, and pain was controlled with oral analgesics. Intraoperative blood loss was less than 100 cc. He was discharged to a rehabilitation facility on the second postoperative day. Postoperatively, he complained of some left lower extremity pain and numbness. The pain completely resolved by the 6-month follow-up visit. The numbness in the anterolateral left thigh was improved but not completely resolved at 12 months. He continued to have full strength in all extremities. CONCLUSION: The traditional approach to an anterior lumbar corpectomy and posterior pedicle screw fixation involves significant postoperative pain and frequent ileus. This minimally invasive approach allowed for early mobilization, resumption of diet, and discharge from the hospital on postoperative day two. Ó 2011 Elsevier Inc. All rights reserved. Lumbar burst fracture; Minimally invasive surgery; Corpectomy; Percutaneous fixation FDA device/drug status: Approved (Medtronic Longitude pedicle screws; titantium cage). Not approved for this indication (Medtronic Direct Lateral Interbody Fusion technique). Author disclosures: JCE: Speaking/Teaching Arrangements: Medtronic (B); DePuy (A); Stryker Spine (B). The disclosure key can be found on the Table of Contents and at www. TheSpineJournalOnline.com. * Corresponding author. Department of Orthopedic Surgery, University of Massachusetts, 119 Belmont St, Worcester, MA 01605, USA. Tel.: (508) ; fax: (508) address: jason.eck@umassmemorial.org (J.C. Eck) Introduction Lumbar burst fractures are a common injury resulting from motor vehicle accidents, falls from height, and other modes of trauma. Historically, the guidelines for operative treatment included greater than 50% loss of vertebral body height, greater than 50% canal compromise, greater than 30 of kyphosis, or the presence of a neurologic deficit. These radiographic criteria are felt to indicate mechanical instability, but were retrospectively derived, highly variable /$ - see front matter Ó 2011 Elsevier Inc. All rights reserved. doi: /j.spinee
2 e2 J.C. Eck / The Spine Journal -- (2011) e1 e5 among authors, and are not definitively proven to define instability. More recent studies have focused on the integrity of the posterior ligamentous complex in determining stability of lumbar burst fractures [1 3]. There are numerous options for the surgical treatment of unstable burst fractures or those with neurologic injury. Fractures can be approached through an anterior, posterior, or combined technique. The combined approach allows for the greatest stability, minimizes the number of levels fused, and allows for a direct decompression of the spinal canal. Unfortunately, this technique comes with a higher morbidity, frequent ileus, and longer recovery times. Newer techniques have attempted to use less invasive techniques to decrease the associated morbidity. These have included combining vertebral augmentation with pedicle screw instrumentation [4,5] and transpedicular corpectomy with expandable cage combined with pedicle screw fixation [6]. The purpose of the report is to present a case of an L3 burst fracture treated with a minimally invasive anterior and posterior fixation technique. Case report A 30-year-old male was involved in a head-on motor vehicle collision. Initial imaging revealed an L3 burst fracture with 60% canal compromise, 50% loss of vertebral body height, a large anteriorly displaced fragment consisting of 40% of the vertebral body depth, and a facet fracture (Fig. 1). At the scene, he had a sudden onset of complete loss of motor strength and sensation in bilateral lower extremities. On presentation to the emergency department, he had regained full motor strength but had some continued sensory deficits. The sustained sensory deficits did not correspond to a specific nerve root distribution and were more likely the result of central canal stenosis from the fracture fragment retropulsion. The degree of disruption of the anterior and middle column support combined with a fracture through the posterior column in the facet joint suggested that this patient had a mechanical instability that warranted surgical decompression and stabilization. Anterior column reconstruction was recommended to the patient because of the comminution and displacement of the vertebral body. It was felt that short-segment posterior stabilization alone would not be sufficient. By reconstructing the anterior column, a shorter segment fusion could be performed and maximize the patient s remaining available motion segments. After medical clearance and consent, the patient underwent a minimally invasive L3 corpectomy and L2 L4 interbody fusion through a direct lateral approach with placement of a titanium mesh cage filled with local autograft and allograft bone matrix. The patient was positioned on a radiolucent table with an inflatable beanbag in the left lateral position with the left hip and knee flexed to relax the psoas muscle. The beanbag was inflated to increase the available working space between the ribs and the iliac crest. This could also be accomplished with a bending table. Anteroposterior and lateral fluoroscopic images were achieved before prepping and draping the patient to verify adequate visualization. The center of the L3 vertebral body was identified. The skin and subcutaneous tissues were incised and the dissection carried through the abdominal muscles. The retroperitoneal space was reached under direct visualization. The psoas muscle was identified. The neuromonitoring probe was attached to a Jamshidi needle and then docked on and gentle passed through the psoas muscle. Free-running and trigger electromyography (EMG) was used. If a response was generated from the EMG, the dissection was moved more anteriorly on the vertebral body Fig. 1. Initial computed tomography scan (Left, axial; Right, sagittal) of the lumbar spine revealing an L3 burst fracture with 60% canal compromise, 50% loss of vertebral body height, a large anteriorly displaced fragment consisting of 40% of the vertebral body depth, and a facet fracture.
3 J.C. Eck / The Spine Journal -- (2011) e1 e5 e3 to avoid the genitofemoral nerve and exiting nerve roots. Once the lateral aspect of the vertebral body was reached with the monitoring probe, the Jamshidi needle was docked into the vertebral body. The inner stylet was removed, and a guide wire was passed through the outer cannula. Sequential dilation was performed with tubes over the guide wire while performing free-running EMG. A retractor system was then placed over the final dilating tube, and the tubes were removed, leaving the retractor in place. The retractor blades were then gently opened to span the distance from the inferior end plate of L2 to the superior end plate of L4. The EMG probe then verified a safe working area within the retractor blades. Pins were then placed through the retractor blades into the L2 and L4 vertebral bodies to hold it securely in place. The L2 L3 and L3 L4 discs were removed under fluoroscopic guidance to avoid penetrating beyond the contralateral annulus. The comminuted L3 vertebral body was then removed, decompressing the central canal. The end plates were decorticated. A caliper was used to determine the length of the graft. A titanium mesh graft was cut to size and packed with local autograft and gentle impacted into place under fluoroscopic guidance. The beanbag was released to add further compression of the graft. The retractors were removed. A layered closure was performed of the transversalis and external oblique fascia, subcutaneous tissue and skin. The patient was then turned to the prone position and underwent a percutaneous stabilization with pedicle screw fixation from L2 to L4 as described in detail elsewhere (Fig. 2) [7,8]. The patient tolerated the procedure well without complications. Total operative time for the combined procedures was 3 hours. Intraoperative blood loss was less than 100 cc. The patient was ambulating on the first postoperative day, pain was controlled with oral analgesics, and was tolerating a regular diet. He used a lumbar corset for comfort when out of bed. The patient was ambulating well on flat surfaces after the first day, but he had numerous stairs to navigate at his home. He was not yet able to manage the stairs at this point, so he was discharged to a rehabilitation facility on the second postoperative day. Postoperatively, his pain was markedly improved, but he did continue to initially complain of some left lower extremity pain and numbness. The pain completely resolved by the 6-month follow-up visit. The numbness in the anterolateral left thigh was improved but not completely resolved at 12 months. He continued to have full strength in all extremities. He had returned to all activities without restrictions. Discussion Although there are various options available for the surgical management of unstable lumbar burst fractures, many are associated with significant postoperative pain, hospital stay, and ileus. This case presents another potential surgical technique with less morbidity, blood loss, pain, and risk for developing an ileus. Percutaneous pedicle screw instrumentation has been gaining rapid acceptance with expanding indications [7,8]. Reported benefits include decreased muscle damage, less postoperative pain, and decreased blood loss [9]. Fig. 2. Postoperative radiographs (Left, anteroposterior; Right, lateral) showing placement of the corpectomy cage and posterior pedicle screw fixation from L2 to L4.
4 e4 J.C. Eck / The Spine Journal -- (2011) e1 e5 Previous investigators have quantified the amount of muscle damage that occurs with spine surgery with measurements of creatine kinase [10,11]. Open lumbar fusions were found to result in significantly greater levels of creatine kinase than percutaneous techniques. Drawbacks of this technique include increased radiation exposure to the surgeon, staff, and patient, as well as an initially increased operative time during the learning curve [12]. Minimally invasive approaches to the anterior lumbar spine include mini-open techniques, laparoscopic-assisted transacral and trans-psoas approaches. The lateral transpsoas approach to the lumbar spine allows for an anterior approach to the intervertebral disc through a small lateral incision for placement of a large interbody cage on the apophyseal ring. Benefits of this approach include avoiding the need for retraction of the retroperitoneal vessels and sympathetic plexus, less muscle dissection, and less manipulation of the abdominal contents, and subsequent ileus. One of the main disadvantages of the lateral transpsoas approach is the lack of direct visualization compared with the traditional open technique. Instead, the surgeon is dependent on fluoroscopy and EMG. Potential risks include injury to the exiting nerve roots. Anatomic studies have identified the location of the exiting ventral nerve roots in relation to the vertebral body [13]. The safe zone lays at the anterior to middle portion of the vertebral body. This zone narrows at the more caudal levels. The patient in the current case presented with a mechanically unstable lumbar burst fracture. The degree of comminution and displacement of the anterior column were believed to suggest mechanical instability that could not be adequately controlled with bracing alone. Reconstruction of the anterior column was recommended to the patient in an attempt to minimize the number of fusion levels needed and maximize his postoperative motion segments. He had an initial neurologic deficit that improved significantly from the time of injury to presentation at the trauma center. He tolerated the minimally invasive procedure well. Postoperatively, he did complain of left thigh pain and numbness. The pain was completely resolved at 6 months, and the numbness was markedly improved but not completely resolved at the 1-year follow-up visit. It is uncertain if his thigh pain and numbness were related to the transpsoas approach or the result of his injury. There were no abnormal alerts from neuromonitoring at baseline or throughout the case to suggest an iatrogenic injury, but this does not rule out the possibility. Another potential source of iatrogenic injury to the patient was during inflation of the beanbag to further open the space between the ribs and the iliac crest. This could have lead to further migration of the unstable fracture fragments. The amount of necessary bending was minimized because of the L3 level being the most accessible. The beanbag was released after placement of the cage to minimize any iatrogenic scoliosis. Although this technique is certainly not recommended for routine use in lumbar burst fractures, it was a safe and effective approach for this patient and allowed for an expedited recovery compared with the traditional open techniques. The specific characteristics of this case that made it amenable to the less invasive approach were the patient size and the location of the fracture. The patient s vertebral body heights were approximately 24 mm, and the distance between the end plates of L2 and L4 was 27 mm. The smaller size of his vertebrae allowed access to the L3 fracture and securing the retractors to the neighboring end plates. During the approach, sequential dilation with tube dilators is performed up to 22 mm. An expandable retractor system is then inserted over the dilators and secured to the vertebrae. This retractor can be expanded to a final distance of 30 mm. Additionally, each blade can be angled up to 30. In the present case, the titanium mesh cage was able to be directly inserted through the dilated retractor. The system would not allow for sufficient exposure for patients with larger vertebral body heights. The location of the fracture at the L3 level was also advantageous. The lateral transpsoas technique is best used between L2 andl4. Caudal to that level, there is increased risk to the exiting nerve roots and limitations from the overlying iliac crest. Above that level, there is possible overlap of the diaphragm. This case presents a novel minimally invasive technique for the treatment of certain lumbar burst fractures that allows for improved blood loss and muscle damage, with an expedited recovery period. References [1] Vaccaro AR, Zeiller SC, Hurlbert RJ, et al. The thoracolumbar injury severity score: a proposed treatment algorithm. J Spinal Disord Tech 2005;18: [2] Vaccaro AR, Lee JY, Schweitzer KM, et al. Assessment of injury to the posterior ligamentous complex in thoracolumbar spine trauma. Spine J 2006;6: [3] Vaccaro AR, Rihn JA, Saravanja D, et al. Injury of the posterior ligamentous complex of the thoracolumbar spine: a prospective evaluation of the diagnostic accuracy of magnetic resonance imaging. Spine 2009;34:E [4] Korovessis P, Hadjipavlou A, Repantis T. Minimally invasive short posterior instrumentation plus balloon kyphoplasty with calcium phosphate for burst and severe compression lumbar fractures. Spine 2008;33: [5] Pflugmacher R, Agarwal A, Kandziora F, Klostermann C. Balloon kyphoplasty combined with posterior instrumentation for the treatment of burst fractures of the spine: 1-year results. J Orthop Trauma 2009;23: [6] Chou D, Wang VY, Gupta N. Transpedicular corpectomy with posterior expandable cage placement for L1 burst fracture. J Clin Neurosci 2009;16: [7] Fuentes S, Blondel B, Metellus P, et al. Percutaneous kyphoplasty and pedicle screw fixation for the management of thoraco-lumbar burst fractures. Eur Spine J 2010;19: [8] Harris EB, Massey P, Lawrence J, et al. Percutaneous techniques for minimally invasive posterior lumbar fusion. Neurosurg Focus 2008;25:E12. [9] Dickerman RD, East JW, Winters K, et al. Anterior and posterior lumbar interbody fusion with percutaneous pedicle screws: comparison to muscle damage and minimally invasive techniques. Spine 2009;34:E923 5.
5 J.C. Eck / The Spine Journal -- (2011) e1 e5 e5 [10] Arts MP, Nieborg A, Brand R, Peul WC. Serum creatine phosphokinase as an indicator of muscle injury after various spinal and nonspinal surgical procedures. J Neurosurg Spine 2007;7: [11] Kumbhare D, Parkinson W, Dunlop B. Validity of serum creatine kinase as a measure of muscle injury produced by lumbar surgery. J Spinal Disord Tech 2008;21: [12] Bindal RK, Glaze S, Ognoskie M, et al. Surgeon and patient radiation exposure in minimally invasive transforaminal lumbar interbody fusion. J Neurosurg Spine 2008;9: [13] Regev GJ, Chen L, Dhawwan M, et al. Morphometric analysis of the ventral nerve roots and retroperitoneal vessels with respect to the minimally invasive lateral approach in normal and deformed spines. Spine 2009;34:
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
MINIMAL ACCESS SPINE SURGERY
 MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Value Analysis Brief MIS Lateral Approach to Interbody Fusion
 Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
The goals of modern spinal surgery are to maximize
 SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
SPRING 2013 Robot-Guided Spine Surgery Christopher R. Good, M.D., F.A.C.S. and Blair K. Snyder, P.A.-C. The goals of modern spinal surgery are to maximize patient function and accelerate a return to a
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
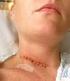 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
ICD-10-PCS Documentation and Coding for Spinal Procedures October 22, 2015
 Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spinal Compression Fractures A Patient's Guide to Spinal Compression Fractures
 Arcata Chiropractic Office Larry J. Kleefeld D.C. Spinal Compression Fractures A Patient's Guide to Spinal Compression Fractures Introduction Compression fractures are the most common type of fracture
Arcata Chiropractic Office Larry J. Kleefeld D.C. Spinal Compression Fractures A Patient's Guide to Spinal Compression Fractures Introduction Compression fractures are the most common type of fracture
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Spinal Compression Fractures
 A Patient s Guide to Spinal Compression Fractures 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Spinal Compression Fractures 228 West Main, Suite C Missoula, MT 59802 Phone: info@spineuniversity.com DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Biomechanics of the Lumbar Spine
 Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Lateral Lumbar Interbody Fusion (LLIF or XLIF)
 Lateral Lumbar Interbody Fusion (LLIF or XLIF) NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Aleve, Ibuprofen, Motrin, Naprosyn, Mobic, etc) OR ASPIRIN PRODUCTS
Lateral Lumbar Interbody Fusion (LLIF or XLIF) NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Aleve, Ibuprofen, Motrin, Naprosyn, Mobic, etc) OR ASPIRIN PRODUCTS
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis
 Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Surgical Procedures and Clinical Results of Endoscopic Decompression for Lumbar Canal Stenosis Munehito Yoshida, Akitaka Ueyoshi, Kazuhiro Maio, Masaki Kawai, and Yukihiro Nakagawa Summary. The purpose
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro
 Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 healtheephan@yahoo.com ABSTRACT
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 healtheephan@yahoo.com ABSTRACT
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Abstract. Introduction. Case Report. imedpub Journals http://www.imedpub.com/
 Case Report imedpub Journals http://www.imedpub.com/ Unusual 2-Stages Posterior Approach Surgical Treatment for Complete Fracture Dislocation of the Upper Thoracic Spine without Neurologic Deficit: A Case
Case Report imedpub Journals http://www.imedpub.com/ Unusual 2-Stages Posterior Approach Surgical Treatment for Complete Fracture Dislocation of the Upper Thoracic Spine without Neurologic Deficit: A Case
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY
 ORIGINAL RESEARCH ARTICLE http://www.eternalpublication.com InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY IJAPB: Volume: 1; Issue: 1; October 2014 ISSN(Online):2394-3440 A Morphometric Study
ORIGINAL RESEARCH ARTICLE http://www.eternalpublication.com InternatIonal JOURNAL OF ANATOMY PHYSIOLOGY and BIOCHEMISTRY IJAPB: Volume: 1; Issue: 1; October 2014 ISSN(Online):2394-3440 A Morphometric Study
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
Her past medical history was non significant. She never had surgery, had no history or family history of cancer and was a nonsmoker.
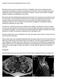 Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
-Increases the safety, accuracy and efficiency of certain spine procedures
 Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
Chapter 13: Spinal Navigation Ben J Garrido, MD, Rick C Sasso, MD I. Key Points -Allows intraoperative real time navigation of instruments relative to the spinal anatomy -Provides 3-D real time anatomical
Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular bone grafting
 Eur Spine J (2002) 11 :435 440 DOI 10.1007/s00586-002-0390-1 ORIGINAL ARTICLE A. Kaminski E. J. Müller G. Muhr Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular
Eur Spine J (2002) 11 :435 440 DOI 10.1007/s00586-002-0390-1 ORIGINAL ARTICLE A. Kaminski E. J. Müller G. Muhr Burst fracture of the fifth lumbar vertebra: results of posterior internal fixation and transpedicular
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach
 Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Case Study: Reduction and Stabilization of Grade III L5-S1 Dysplastic Spondylolisthesis in 15-Year-Old Female Using Posterior Approach Terrence L. Piper, MD Piper Spine Care Background Context: A female
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
REPUTATION MANAGEMENT: SPINAL FUSION SURGERY
 REPUTATION MANAGEMENT: SPINAL FUSION SURGERY Meaningful and Positive Progress in Spinal Fusion Results: A Journey towards Excellence Paul J. Slosar, M.D. SpineCare Medical Group As a practicing spine surgeon,
REPUTATION MANAGEMENT: SPINAL FUSION SURGERY Meaningful and Positive Progress in Spinal Fusion Results: A Journey towards Excellence Paul J. Slosar, M.D. SpineCare Medical Group As a practicing spine surgeon,
www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862
 Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Non-Profit ORG. U.S. Postage PAID West Palm BCH. FL. PERMIT NO. 4709 www.backandspinefl.com Back and Spine Center 509 Riverside Dr., Suite 203 Stuart, FL 34994 Phone: (772) 288-5862 The evolution of neurosurgery
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Vivian Gonzalez Gillian Lieberman, MD. January 2002. Lumbar Spine Trauma. Vivian Gonzalez, Harvard Medical School Year III Gillian Lieberman, MD
 January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
January 2002 Lumbar Spine Trauma Vivian Gonzalez, Harvard Medical School Year III Agenda Anatomy and Biomechanics of Lumbar Spine Three-Column Concept Classification of Fractures Our Patient Imaging Modalities
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ)
 The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
The Furcal nerve. Ronald L L Collins,MB,BS(UWI),FRCS(Edin.),FICS (Fort Lee Surgical Center, Fort Lee,NJ) The furcal nerve is regarded as an anomalous nerve root, and has been found with significant frequency
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Thoracolumbar and Lumbar Burst Fractures. Sussan Salas, MD Thomas Jefferson University Hospital Department of Neurological Surgery
 Thoracolumbar and Lumbar Burst Fractures Sussan Salas, MD Thomas Jefferson University Hospital Department of Neurological Surgery Thoracolumbar/Lumbar Burst Fractures: Overview Epidemiology Anatomy Initial
Thoracolumbar and Lumbar Burst Fractures Sussan Salas, MD Thomas Jefferson University Hospital Department of Neurological Surgery Thoracolumbar/Lumbar Burst Fractures: Overview Epidemiology Anatomy Initial
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
coligne treatment technology
 coligne treatment technology coligne a strategy in spine Leadership begins before the patient enters the surgical theater, among the spine care professionals forming the coalliance. This may be a small
coligne treatment technology coligne a strategy in spine Leadership begins before the patient enters the surgical theater, among the spine care professionals forming the coalliance. This may be a small
DRAFT. EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques. Leiden The Netherlands 5 November 8 November 2012
 EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques DRAFT Leiden The Netherlands 5 November 8 November 2012 Provisional Course Programme Monday 5 th November Trauma
EANS Advanced Course in Spinal Surgery Module II: Thoracolumbar Interventional Techniques DRAFT Leiden The Netherlands 5 November 8 November 2012 Provisional Course Programme Monday 5 th November Trauma
Surgical Spine Care Center
 OUTCOMES DIVISION OF MEDICINE Surgical Spine Care Center About Cleveland Clinic Florida Cleveland Clinic Florida s medical staff are dedicated physicians who have joined the clinic as salaried doctors
OUTCOMES DIVISION OF MEDICINE Surgical Spine Care Center About Cleveland Clinic Florida Cleveland Clinic Florida s medical staff are dedicated physicians who have joined the clinic as salaried doctors
2013 North American SSL Certificate
 2013 2014 INSERT COMPANY LOGO HERE 2014 North American 2013 North American SSL Certificate Minimally Invasive Spinal Surgical Solutions Product Product Line Leadership Strategy Leadership Award Award Background
2013 2014 INSERT COMPANY LOGO HERE 2014 North American 2013 North American SSL Certificate Minimally Invasive Spinal Surgical Solutions Product Product Line Leadership Strategy Leadership Award Award Background
Magnetic Resonance Imaging
 Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Research Article Partial Facetectomy for Lumbar Foraminal Stenosis
 Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Advances in Orthopedics, Article ID 534658, 4 pages http://dx.doi.org/10.1155/2014/534658 Research Article Partial Facetectomy for Lumbar Foraminal Stenosis Kevin Kang, 1 Juan Carlos Rodriguez-Olaverri,
Anatomy of the Spine. Figure 1. (left) The spine has three natural curves that form an S-shape; strong muscles keep our spine in alignment.
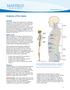 1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
1 2 Anatomy of the Spine Overview The spine is made of 33 individual bony vertebrae stacked one on top of the other. This spinal column provides the main support for your body, allowing you to stand upright,
Objectives. Spinal Fractures: Classification Diagnosis and Treatment. Level of Fracture. Neuro exam Muscle Grading
 Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Assessment & Treatment of Fractures and Dislocations of the Thoracic and Lumbar Spine. Brian Drew, MD
 Assessment & Treatment of Fractures and Dislocations of the Thoracic and Lumbar Spine Brian Drew, MD Introduction Mechanism of injuries to the thoracolumbar spine Assessment of spinal stability Treatment
Assessment & Treatment of Fractures and Dislocations of the Thoracic and Lumbar Spine Brian Drew, MD Introduction Mechanism of injuries to the thoracolumbar spine Assessment of spinal stability Treatment
Spinal fusion for degenerative disease of the lumbar
 ORIGINAL ARTICLE Minimally Invasive Lumbar Transfacet Screw Fixation in the Lateral Decubitus Position After Extreme Lateral Interbody Fusion A Technique and Feasibility Study Jean-Marc Voyadzis, MD and
ORIGINAL ARTICLE Minimally Invasive Lumbar Transfacet Screw Fixation in the Lateral Decubitus Position After Extreme Lateral Interbody Fusion A Technique and Feasibility Study Jean-Marc Voyadzis, MD and
Compression Fractures
 September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
September 2006 Compression Fractures Eleanor Adams Harvard Medical School Year IV Overview Spine Anatomy Thoracolumbar Fractures Cases Compression Fractures, Ddx Radiologic Tests of Choice Treatment Options
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Lower Back Pain. Introduction. Anatomy
 Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure
 Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
Effects of Vertebral Axial Decompression (VAX-D) On Intradiscal Pressure Gustavo Ramos, M.D., William Marin, M.D. Journal of Neursurgery 81:35-353 1994 Departments of Neurosurgery and Radiology, Rio Grande
A Healthy Lumbar Spine... 2. A Problem Lumbar Spine... 3. Understanding Your Surgery... 4. Preparing for Surgery... 5. Day of Surgery...
 Table of Contents A Healthy Lumbar Spine................. 2 A Problem Lumbar Spine................. 3 Understanding Your Surgery.............. 4 Preparing for Surgery.................... 5 Day of Surgery.........................
Table of Contents A Healthy Lumbar Spine................. 2 A Problem Lumbar Spine................. 3 Understanding Your Surgery.............. 4 Preparing for Surgery.................... 5 Day of Surgery.........................
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
enspire Interventional, Novel approach in Percutaneous Discectomy in Percutaneous Discectomy Samyadev Datta, MD, FRCA Center for Pain Management
 enspire Interventional, Novel approach in Percutaneous Discectomy in Percutaneous Discectomy Samyadev Datta, MD, FRCA Center for Pain Management Anatomy Intervertebral Disc: Fibrocartilaginous joint Makes
enspire Interventional, Novel approach in Percutaneous Discectomy in Percutaneous Discectomy Samyadev Datta, MD, FRCA Center for Pain Management Anatomy Intervertebral Disc: Fibrocartilaginous joint Makes
Surgical Procedures of the Spine
 Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis
 Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Advances in Orthopedics Volume 2012, Article ID 645321, 5 pages doi:10.1155/2012/645321 Review Article Minimal Invasive Decompression for Lumbar Spinal Stenosis Victor Popov 1 and David G. Anderson 1,
Spine Injury and Back Pain in Sports
 Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Thoracolumbar Spine Fractures. Outline. Outline. Holmes Criteria. Disclosure:
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Department of Radiology Virginia Mason Medical Center Affiliate Professor, University of Washington Disclosure: Book Royalties, Springer-Verlag
R/F. Applications and Present Issues of Tomosynthesis in Spine Surgery. 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4
 R/F Applications and Present Issues of Tomosynthesis in Spine Surgery 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4 Professor and Chairman Department of Orthopaedic Surgery
R/F Applications and Present Issues of Tomosynthesis in Spine Surgery 87th Annual Meeting of the Japanese Orthopaedic Association Evening Seminar 4 Professor and Chairman Department of Orthopaedic Surgery
