Managing airway obstruction
|
|
|
- Meredith Douglas
- 9 years ago
- Views:
Transcription
1 Managing airway obstruction Introduction Recognizing airway compromise is a fundamental skill for junior doctors as they will frequently be first managing these patients. By appreciating the causes of an obstructed airway, treatment with oxygen and a number of simple manoeuvres can be delivered swiftly, preserving airway patency and passage of oxygen to the lungs for ventilation. Ventilation is the mechanical movement of air into and out of the respiratory system, resulting in the exchange of carbon dioxide. Airway obstruction results in hypoventilation, increased work of breathing and impaired gas exchange, with development of hypercarbia and ultimately hypoxaemia if left untreated. Provision of supplemental oxygen in the setting of airway obstruction (i.e. oxygenation) will not resolve the problem of hypercapnia associated with hypoventilation and impaired alveolar ventilation. Obstruction may be partial or complete, depending on the mechanism or cause. Complete airway obstruction will rapidly cause hypoxia and cardiac arrest, whereas partial obstruction may be more insidious in onset. Reduced alveolar ventilation in the obtunded patient and the obstructed airway leads to hypercapnia, respiratory acidosis and hypoxaemia. Noisy breathing characterizes a partially obstructed airway, and ominous absence of airway noises heralds total airway obstruction Causes of an obstructed airway The airway may be subdivided into upper and lower airway the upper airway comprises the conduit from the nares and lips to the larynx, while the lower airway contains the tracheobronchial tree, consisting of 23 generations of passages from trachea to alveoli. The level of obstruction will Dr Kirstie McPherson is Specialist Registrar in Anaesthesia and Dr Robert CM Stephens is Consultant Anaesthetist in the Department of Anaesthetics, University College Hospital, London NW1 2BU Correspondence to: Dr K McPherson ([email protected]) commonly be related to the cause or pathogenesis of disease process. There are a large number of causes of airway obstruction (Table 1), and it is important to look out for at-risk groups in whom airway compromise is more common. Patients with a reduced conscious level are unable to clear their own secretions and cannot protect their own airway. A Glasgow Coma Scale of 8/15 or below is often considered the threshold at which intubation is necessary. Patients with reduced conscious level are at risk of aspiration and alveolar hypoventilation, with development of hypercarbia and respiratory acidosis. In practice, a more focused approach is taken when deciding to intubate patients, bearing in mind factors such as the potential for further deterioration, and moving from a place of safety to one of greater isolation (e.g. transfer from resuscitation department to radiology department). In these instances, a more conservative approach is taken, and patients with a higher Glasgow Coma Scale may warrant early intubation. Also, think about patients in whom surgery, trauma or burns may contribute to airway compromise, e.g. from haematoma and oedema. In the case of burns or history of smoke inhalation, adopt a high index of suspicion for airway injury. Signs such as carbonaceous sputum, soot around the face and mouth, and singed hair warrant urgent anaesthetic input. These patients must always be assessed early by an anaesthetist, as these are Table 1. Classifying causes of airway obstruction Mode of obstruction Intraluminal contents Central drive (obtunded) External compression Direct trauma Artificial airways Excessive granulation tissue Neurocognitive and neuromuscular disorders dynamic situations that may rapidly progress from one of stability to one of a threatened and compromised airway. As such early intubation is undertaken in these at-risk groups. External compression from an adjacent pathology, e.g. goitre, lymphadenopathy, tumour and haematoma (e.g. post-thyroidectomy), may be insidious or rapid in onset. In patients with underlying malignancy, it is important for clinicians to be vigilant in identifying features suggestive of airway compromise. Airway obstruction may occur at any point from the mouth down to the trachea and bronchial tree. The commonest site for obstruction in the obtunded unconscious patient is at the pharynx, because the tongue falls back against the posterior pharyngeal wall, and a lack of muscle tone causes narrowing of the airway diameter. The soft tissues in the pharyx and larynx are vulnerable to swelling and oedema if traumatized, or at the site of infection. Post-extubation laryngeal oedema may be seen after traumatic and multiple attempts at intubation, and in patients receiving prolonged periods of intubation where high cuff pressures may cause oedema of laryngeal mucosa. Local trauma following foreign body ingestion, e.g. a fish bone embedded in soft pharyngeal tissues, can cause significant airway compromise, and in some cases development of pharyngeal abscess. In children, whose airways are relatively smaller, mucosal swelling, upper respiratory obstruction and stridor may be associated with infections such as laryngo- Example Blood, vomitus, foreign body, secretions, intraluminal tumours Head injury (with reduced conscious level), drugs: benzodiazepine, opiates, alcohol, raised intracranial pressure Haematoma, tumour, goitre Blunt trauma to maxilla, larynx, mandible, burns, smoke inhalation Blockage or displacement of tracheostomy, displacement of tracheal stent Prolonged mechanical ventilation, tracheal stenosis, supraglottic stenosis Increased risk of aspiration, e.g. Parkinson s disease, post-stroke, myasthenia gravis C156 British Journal of Hospital Medicine, October 2012, Vol 73, No 10 CTD_C156_C160_Airways.indd /09/ :31
2 Tips From The Shop Floor tracheobronchitis (croup) and epiglottitis. The latter (seen less following the advent of widespread vaccination) causes enlargement of the epiglottis, and may progress to complete airway obstruction. Classically children will adopt a sitting tripod position, with jaw thrust forward and drooling saliva. The importance of getting expert help swiftly cannot be over-emphasized if these pathologies are suspected. Distress and examination of the pharynx may precipitate complete airway obstruction. Get help early. Upper airway stimulation in the presence of secretions or inhalation of foreign material may cause laryngeal spasm with adduction of the vocal cords, preventing passage of air to the lungs and leading to development of hypoxaemia. Table 2. Features of airway obstruction Recognizing airway obstruction It is important to assess airway patency in any patient at risk of airway obstruction. This forms part of the ABC approach, sequentially assessing airway, breathing and circulation as described by Nolan et al (2010) in life support algorithms. A conscious and alert patient, speaking in full sentences, is reassuring. Features suggestive of obstructed airway include complete absence of airway sounds (complete obstruction), or added sounds of laboured breathing where air entry is diminished (partial obstruction). Tachycardia and tachypnoea may reflect respiratory distress (Table 2). Use of accessory muscles of respiration is typical in the partially obstructed airway, and signs include tracheal tug, paradoxical chest and abdominal movement ( see-sawing ), with supraclavicular and intercostal in-drawing. Stridor is the harsh, highpitched sound occurring in upper airway obstruction. Its origin is from the Latin stridere, to creak. Inspiratory stridor indicates laryngeal obstruction, since the negative intrathoracic pressures exacerbate extrathoracic obstruction during inspiration. Intrathoracic obstruction may cause expiratory stridor, as the airways are compressed during expiration. Children are more susceptible to stridor, given the relatively smaller diameter of their airways. Irritability, agitation and reduced conscious level commonly reflect hypoxaemia and hypercarbia. Do not rely on cyanosis as a feature in identifying the obstructed airway this is a very late preterminal sign. Observe or ask about best breathing position. Be aware that the patient may have positioned him-/herself for optimal airflow in the setting of airway obstruction. Moving the patient into a supine position may precipitate loss of the airway altogether. Low pulse oximetry readings (SpO 2 ) reflect inadequacy of oxygenation, although it is important to remember that pulse oximetry provides a measure of oxygenation and is not the same as ventilation. Arterial blood gas sampling may be helpful but should not delay management. A respiratory acidosis, with a high carbon dioxide tension (PaCO 2 ) and reduced ph, reflects alveolar hypoventilation. When assessing patients look carefully for these signs and symptoms and always call for help early from an anaesthetist if you suspect airway compromise. The young can compensate well initially, masking impending desaturation and hypoxaemia. Be mindful of injuries that will compromise the airway, such as facial burns, bleeding and foreign bodies obstructing the airway. Always provide high flow oxygen with a reservoir bag at 15 litres/minute, and reassess frequently, looking for signs of deterioration. Managing a compromised airway Oxygen therapy is required urgently in the obstructed airway. An oxygen mask with reservoir bag and an oxygen flow rate of 15 litres/minute will provide a high inspired fraction of oxygen, and can be found on all wards and resuscitation areas. Remember blood oxygen saturation will be restored more quickly if the inspired fraction of oxygen is high. The recovery (lateral) position pushes the tongue and jaw forward under gravity, improving the airway. This position is one of relative safety for patients with a depressed conscious level, e.g. as a result of alcohol excess, or in a post-ictal state. In addition, a head-down tilt (tilting facility available on most hospital trolleys) provides passage for secretions or vomit out of the mouth, with the help of gravity. Patients with an artificial airway, e.g. tracheostomy, with features of respiratory distress require urgent and skilled airway help. Do not delay in summoning immediate assistance from an anaesthetist. These devices may have become blocked or displaced. Apply high flow oxygen to both the face and the tracheostomy. Simple manoeuvres Simple manoeuvres in an obtunded patient may help to improve the patency of the airway, allowing passage of air into and out of the lungs. These are described below. Practice them on a manikin or in theatre with an anaesthetist. Chin lift Head tilt and chin lift can be used to relieve upper airway obstruction. Place the fingertips underneath the patient s chin and gently lift upwards. Jaw thrust The jaw thrust is achieved by combined flexion of the neck and extension at the atlanto-occipital joint, lifting the angles of the mandible forward (Figure 1). This Figure 1. Jaw thrust. Snoring Stridor (caused by obstruction at or above the laryngeal level) Expiratory wheeze (caused by obstruction of lower airways) Gurgling (vomit, blood or secretions in airway) Reduced conscious level Tripod positioning seen in children (for maximal air passage to lungs) British Journal of Hospital Medicine, October 2012, Vol 73, No 10 C157 CTD_C156_C160_Airways.indd /09/ :31
3 manoeuvre lifts the tongue and moves the larynx forward, allowing passage of air into the lungs. Cautionary points Avoid neck extension and risks to the spinal cord in patients in whom a cervical spine injury is suspected. In these patients jaw thrust in combination with manual in-line stabilization is recommended. Upward pressure on the soft tissues of the floor of the mouth in young children can cause obstruction. Be mindful of this when performing jaw thrust in this population. Adjuncts The oropharyngeal airway (Guedel) and nasopharyngeal airway are simple adjuncts, useful in maintaining a patent airway (Figure 2). They relieve backward tongue displacement and soft palate obstruction. Careful insertion under direct vision is important. Avoid using a nasopharyngeal airway in patients for whom a base of skull fracture or coagulopathy is suspected. An oropharyngeal airway is sized by measuring the distance from the incisors to the angle of the jaw. The most common technique for placing an oropharyngeal airway is by inserting the airway into the mouth upside-down, and then rotating through 180 at the junction between the soft and hard palate. The airway is then advanced until it rests in the pharynx. Suction should always be available to clear the airway of any visible secretions or foreign body. Conscious patients, in whom laryngeal reflexes are present, will not tolerate an oropharyngeal airway and inserting one may precipitate gagging, vomiting and laryngospasm. Bag-valve-mask ventilation Patients with reduced conscious level and inadequate spontaneous ventilation will require artificial ventilation in addition to the manoeuvres described above. Connect a bag-valve-mask apparatus (ambu-bag) to a high flow oxygen source (this should be Figure 2. Adjuncts for supporting airway and laryngeal mask. a. Bag-valve-mask system with high flow oxygen source. b. Oropharyngeal and nasopharyngeal airways. c. Laryngeal mask. d. Wide-bore rigid sucker. a b c d available on all wards and resuscitation areas). This will require a two-person technique to achieve a gas-tight seal between the patient s face and the mask, enabling ventilation without leak. One person should hold the mask onto the face, maintaining a jaw thrust, while the assistant squeezes the bag. Laryngeal mask airway Should bag-valve-mask ventilation prove difficult with the two-person technique and the use of the oropharyngeal airway adjunct, alternative means of ventilation are needed. In these instances, senior support should be sought early, with involvement of an anaesthetist with expert airway management skills. The laryngeal mask airway is a device for supporting and maintaining the airway without tracheal intubation. It does not protect the airway from soiling unlike tracheal intubation and is not a secure airway. However, it may serve as an interim measure in the unconscious patient, when intubation has failed, or lack of skill and experience precludes intubation. The head of the laryngeal mask is inserted into the mouth to lie against the back of the pharynx. A circumferential cuff is then inflated to provide an adequate seal to enable ventilation. The end can then be connected to an ambu-bag device to provide artificial ventilation. Incorrect placement increases the risk of aspiration of stomach contents, as the stomach may become gas-filled during ventilation. The laryngeal mask does not guarantee protection from aspiration of gastric contents into the bronchial tree and will not be tolerated in patients in whom laryngeal reflexes are preserved. Again, try to familiarize yourself with the insertion technique with practice on a manikin, or under supervision from an anaesthetist in theatre. Securing an airway A secure airway is one in which the trachea and bronchial tree are protected from aspiration of gastric contents or secretions by the presence of a cuffed endotracheal tube (or a tracheostomy). This is the gold standard for an unconscious patient at risk of aspiration, but should only be attempted by those trained and familiar with the technique of tracheal intubation. This will C158 British Journal of Hospital Medicine, October 2012, Vol 73, No 10 CTD_C156_C160_Airways.indd /09/ :31
4 Tips From The Shop Floor most frequently be the anaesthetist, and it is important to stress again the importance of calling early for help and advice from an anaesthetist in patients with a reduced conscious level. Meticulous attention to detail is needed when preparing for intubation, to avoid mishaps and potentially life-threatening consequences of aspiration and hypoxia. Equipment required for intubation includes an appropriately sized endotracheal tube, a tie to secure it, a laryngoscope (with alternative blade size available), and equipment on standby should intubation prove difficult (Figure 3). This includes a gum-elastic bougie, and alternative means of ventilating, e.g. with a laryngeal mask airway. An ambu-bag or alternative means of ventilation connected to a high flow oxygen source will be connected to the endotracheal tube once in place. Guidelines published by the Difficult Airway Society (Henderson et al, 2004) provide algorithms on procedure for failed intubation, and it is advisable to be familiar with these if you have responsibility for managing airways in patients. Most importantly, a trained anaesthetic nurse or practitioner must assist, and all equipment needs checking and carefully assembly before commencing intubation. In an emergency setting, where patients are not starved and are at risk of aspiration, a rapid sequence induction for tracheal intubation is performed. Anaesthesia and relaxation of the vocal cords must be provided for passage of the endotracheal tube into the trachea. Given the risk of aspiration in a population presenting with reduced conscious level, a rapid sequence induction provides these optimal conditions in the larynx with rapid onset. Preparation is vital for rapid sequence induction, as the anaesthetist needs to react quickly in the event of aspiration. Drugs are prepared beforehand and the tilting capacity of the trolley is confirmed, with suction (wide bore rigid sucker) under the pillow (important in the event of aspiration). The patient is preoxygenated with a tight-fitting mask, for at least 3 minutes or until end-tidal oxygen fraction >0.8. Reassure the patient about what is happening and when possible explain your actions, as this will be an alarming time for the patient. Before loss of consciousness, cricoid pressure is applied pressure with the thumb and index finger over the cricoid cartilage (used since it forms the only complete ring of the larynx and trachea). Pressure over this cartilage displaces the larynx backwards, compressing the oesophagus between the cricoid cartilage and the vertebrae behind. This prevents passive regurgitation of gastric contents during induction of anaesthesia. In the event of active vomiting, cricoid pressure should be released, as this could cause Figure 3. Equipment required for intubation. a. Gum elastic bougie. b. Suxamethonium and thiopentone. c. Endotracheal tube with tie and syringe to inflate cuff. d. Laryngoscope. e. Wide bore rigid sucker. a b c d e rupture of the oesophagus. Pressure is applied until the anaesthetist has confirmed placement of the endotracheal tube with the cuff inflated. Incorrectly performed cricoid pressure may distort the laryngeal anatomy, making successful laryngoscopy extremely difficult for the operator. A rapid sequence induction comprises quick intravenous induction of anaesthesia and neuromuscular blockade facilitating intubation. Following administration of these drugs, laryngoscopy may be performed securing the airway with a cuffed endotracheal tube in the trachea to prevent further soiling of the airway. The combination of thiopentone and suxamethonium have been described in the classical rapid sequence induction, and while still in use, a greater variety of drugs are now used in a modified rapid sequence induction, largely for their superior side-effect profile, as demonstrated by Morris and Cook (2001) in a national survey of practice of the technique. A predetermined dose of induction agent is administered, followed by a muscle relaxant, with rapid onset of action. This negates the need to provide facemask ventilation while waiting for onset of neuromuscular blockade, which risks insufflation of the stomach and aspiration of its contents. The choice of drugs used will depend on both the pharmacodynamic characteristics and the experience of the doctor. The dose should reflect the haemodynamic status of the patient, and hypotension should be anticipated, with readily available provision for vasopressors and sufficient intravenous access to optimize preload. After successful intubation with connection of the tracheal tube to a ventilating device, checks must be carried out to confirm correct placement of the tube in the trachea. These include auscultation of both lungs, observing chest movement, fogging of the tube as warm humidified air is expired from the lungs and capnography confirming the presence of end-tidal carbon dioxide. Consecutive breaths seen on capnography remain the gold standard for ruling out oesophageal intubation, and guidelines published by the Association of Anaesthetists of Great Britain and Ireland (2011) require its provision for all anaesthetized patients and those undergoing British Journal of Hospital Medicine, October 2012, Vol 73, No 10 C159 CTD_C156_C160_Airways.indd /09/ :31
5 KEY POINTS advanced life support, regardless of the location of the patient. A flat capnograph trace indicates lack of ventilation of the lungs: the tube is either not in the trachea or the airway is completely obstructed. Only when you are satisfied with the correct placement of the endotracheal tube, should you ask the assistant to release the cricoid pressure. Failure to identify an endotracheal tube misplaced in the oesophagus will lead to life-threatening hypoxia. The National Audit Project on airway management (Cook et al, 2011) found evidence of avoidable deaths as a result of airway complications in the intensive care unit and the emergency department. Several major events occurred when there were clear indications for a rapid sequence induction but this was not performed. Failure to correctly interpret a capnograph trace led to several oesophageal intubations going unrecognized. The absence of capnography, or the failure to use it properly, contributed to 80% of deaths from airway complications in the intensive care unit and 50% of deaths from airway complications in the emergency department. Active efforts should be taken to positively exclude these diagnoses. Be aware of features of airway compromise, and identify and treat patients with airway obstruction early. Call for help early from an anaesthetist, and anticipate deterioration in patients with airway compromise. Use of simple airway manoeuvres, with basic adjuncts (as required), will often achieve a patent airway. Remember, oxygenation is paramount. Make every attempt to provide high oxygen concentration to patients in whom airway compromise is suspected. Delivering oxygen at the mouth that does not reach the alveolus is not a treatment for airway obstruction. These patients require artificial ventilation for adequate gas exchange. Call for help early, and prepare for intubation in a timely fashion. Recognize the dangerous sequelae of hypoxia and aspiration. Expert help from an anaesthetist will help reduce these risks. Practice in a simulation centre and in theatre, with an anaesthetist, will improve your skills in recognizing, managing and treating these patients. TOP TIPS Check all your equipment before using it; inflate and deflate cuffs of laryngeal mask and endotracheal tubes and lubricate well with jelly. Always have a variety of sizes available for laryngeal mask or endotracheal tube and oropharyngeal airway insertion. Familiarize yourself with the kit available in your own hospital, including that available on airway trolleys in the emergency department and on the resuscitation trolleys found on the wards. Think carefully about the safety of your patient when planning a transfer, within or outside of the hospital. Is the airway protected or at risk? An anaesthetist should assess and may decide to pre-emptively secure the airway with an endotracheal tube and artificial ventilation. When performing preoxygenation for rapid sequence induction, position the patient semi-inclined, with head up and a tight seal around the face mask to maximize body oxygen stores once the patient is apnoeic. Many of the key findings of the report relate specifically to the vigilant approach that must be taken when performing rapid sequence induction in the emergency department and in settings outside of the safer confines of the anaesthetic room. Most events in the emergency department were complications of rapid sequence induction. Rapid sequence induction outside the operating theatre requires the same level of equipment and support as is needed during anaesthesia. This includes capnography and access for equipment needed to manage routine and difficult airway problems. Conclusions Recognizing and acting on airway compromise reduces morbidity and mortality in patients. Pulse oximetry is a poor indicator of airway compromise, and falling arterial haemoglobin oxygen saturation reflects depleted stores of oxygen in the lungs and is a late sign of impending hypoxaemia. Basic airway manoeuvres (with supplementary oxygen) will often improve the patency of an obstructed airway. Getting help from an anaesthetist early is a priority. Before definitive control of the airway is possible, provide 100% oxygen with a tight-fitting mask to optimize body oxygen stores. BJHM Conflict of interest: none. Association of Anaesthetists of Great Britain & Ireland (2011) AAGBI safety statement capnography outside the operating theatre. Updated statement from the Association of Anaesthetists of Great Britain & Ireland (AAGBI) May Safety%20Statement%20-%20The%20use%20 of%20capnography%20outside%20the%20 operating%20theatre%20may%202011_0.pdf (accessed 24 July 2012) Cook TM, Woodall N, Harper J et al (2011) Fourth National Audit Project. Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 2: intensive care and emergency departments. Br J Anaesth 106: Henderson JJ, Latto IP, Pearce AC, Popat MT (2004) Difficult Airway Society guidelines for management of the unanticipated difficult intubation. Anaesthesia 59: Morris J, Cook TM (2001) Rapid sequence induction: a national survey of practice. Anaesthesia 56: Nolan JP, Soar J, Zideman DA et al (2010) European resuscitation council guidelines for resuscitation 2010 section 1 Executive summary. Resuscitation 81: C160 British Journal of Hospital Medicine, October 2012, Vol 73, No 10 CTD_C156_C160_Airways.indd /09/ :31
Difficult Pre-hospital Airway Management
 Difficult Pre-hospital Airway Management Frans L. Rutten, MD, FDSA Elisabeth Hospital Tilburg, The Netherlands In management of patients with an emergency, airway management and ventilatory care are the
Difficult Pre-hospital Airway Management Frans L. Rutten, MD, FDSA Elisabeth Hospital Tilburg, The Netherlands In management of patients with an emergency, airway management and ventilatory care are the
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
The EMT Instructional Guidelines in this section include all the topics and material at the EMR level PLUS the following material:
 Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
AIRWAY MANAGEMENT. Angkana Lurngnateetape, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
Airway assessment. Bran Retnasingham Andy McKechnie
 Airway assessment Bran Retnasingham Andy McKechnie The average Camberwell patient? Airway assessment There is one skill above all else that an anaesthetist is expected to exhibit and that is to
Airway assessment Bran Retnasingham Andy McKechnie The average Camberwell patient? Airway assessment There is one skill above all else that an anaesthetist is expected to exhibit and that is to
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Management of airway burns and inhalation injury PAEDIATRIC
 Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING.
 LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
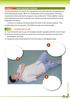 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
Rapid Sequence Intubation A Guide for Assistants
 Rapid Sequence Intubation A Guide for Assistants Working outwith the theatre setting Contents Course Aim...1 Course Objectives...1 Basic Airway Care and Oxygenation...2 Rapid Sequence Intubation...2 Definition...2
Rapid Sequence Intubation A Guide for Assistants Working outwith the theatre setting Contents Course Aim...1 Course Objectives...1 Basic Airway Care and Oxygenation...2 Rapid Sequence Intubation...2 Definition...2
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Virginia Office of Emergency Medical Services Scope of Practice - Procedures for EMS Personnel
 Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
Specific tasks in this document shall refer to the Virginia Education Standards. AIRWAY TECHNIQUES Airway Adjuncts Airway Maneuvers Alternate Airway Devices Cricothyrotomy Obstructed Airway Clearance Intubation
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
In-hospital resuscitation. Superseded by
 6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
6 In-hospital resuscitation Introduction These guidelines are aimed primarily at healthcare professionals who are first to respond to an in-hospital cardiac arrest and may also be applicable to healthcare
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Basic ATLS. The Primary Survey. Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon
 Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
ACLS Provider Manual Supplementary Material
 ACLS Provider Manual Supplementary Material 2012 American Heart Association 1 Contents Airway Management... 4 Part 1: Basic Airway Management... 4 Devices to Provide Supplementary Oxygen... 4 Overview...
ACLS Provider Manual Supplementary Material 2012 American Heart Association 1 Contents Airway Management... 4 Part 1: Basic Airway Management... 4 Devices to Provide Supplementary Oxygen... 4 Overview...
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Objectives. Burn Assessment and Management. Questions Regarding the Case Study. Case Study. Patient Assessment. Patient Assessment
 Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES
 QTP4N0X1C-9 02 July 2015 AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES Volume 9 TOTAL FORCE, TOTAL CARE EVERYTIME, ANYWHERE 383d TRAINING SQUADRON/XUFB
QTP4N0X1C-9 02 July 2015 AEROSPACE MEDICAL SERVICE SPECIALTY INDEPENDENT DUTY MEDICAL TECHNICIAN EMERGENCY MEDICINE PROCEDURES Volume 9 TOTAL FORCE, TOTAL CARE EVERYTIME, ANYWHERE 383d TRAINING SQUADRON/XUFB
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Emergency Medical Responder Mid-Course Knowledge Evaluation
 Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
PHSW Procedural Sedation Post-Test Answer Key. For the following questions, circle the letter of the correct answer(s) or the word true or false.
 PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
Chapter 2 - Anatomy & Physiology of the Respiratory System
 Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services
 State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
Respiratory failure and Oxygen Therapy
 Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz
 Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM
 Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
a guide to understanding pierre robin sequence
 a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy.
 Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Gastroscopy (OGD) The Procedure Explained You have been advised by your GP or hospital doctor to have an investigation known as a Gastroscopy. This procedure requires your formal consent. If you are unable
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT
 CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
CLINICAL SKILLS: THE 'DR ABCDE' ASSESSMENT The 'DR ABCDE' approach to assessing an acutely unwell patient should be at the front of every junior doctor's mind whenever they get bleeped or asked to see
ANAESTHESIA FOR CAESARIAN SECTION PART 3 GENERAL ANAESTHESIA ANAESTHESIA TUTORIAL OF THE WEEK 97
 ANAESTHESIA FOR CAESARIAN SECTION PART 3 GENERAL ANAESTHESIA ANAESTHESIA TUTORIAL OF THE WEEK 97 16 th JUNE 2008 Dr James Brown. Royal Devon & Exeter Hospital, UK Correspondence to: [email protected]
ANAESTHESIA FOR CAESARIAN SECTION PART 3 GENERAL ANAESTHESIA ANAESTHESIA TUTORIAL OF THE WEEK 97 16 th JUNE 2008 Dr James Brown. Royal Devon & Exeter Hospital, UK Correspondence to: [email protected]
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS
 CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
ADMINISTERING EMERGENCY OXYGEN
 FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
Respiratory System. Chapter 21
 Respiratory System Chapter 21 Structural Anatomy Upper respiratory system Lower respiratory system throat windpipe voice box Function of Respiratory System Gas exchange Contains receptors for sense of
Respiratory System Chapter 21 Structural Anatomy Upper respiratory system Lower respiratory system throat windpipe voice box Function of Respiratory System Gas exchange Contains receptors for sense of
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
trust clinical guideline
 CG04 VERSION 1.0 1/5 Guideline ID CG04 Version 1.0 Title Approved by Allergic Reactions Clinical Effectiveness Group Date Issued 01/01/2013 Review Date 31/12/2016 Directorate Authorised Staff Clinical
CG04 VERSION 1.0 1/5 Guideline ID CG04 Version 1.0 Title Approved by Allergic Reactions Clinical Effectiveness Group Date Issued 01/01/2013 Review Date 31/12/2016 Directorate Authorised Staff Clinical
Patient Assessment/Management Trauma
 Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
PROCEDURE FOR USING A NASAL CANNULA
 PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
PROCEDURE FOR USING A NASAL CANNULA
 FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
UNDERGOING OESOPHAGEAL STENT INSERTION
 UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
UNDERGOING OESOPHAGEAL STENT INSERTION Information Leaflet Your Health. Our Priority. Page 2 of 5 Introduction This leaflet tells you about the procedure known as oesophageal stent insertion, explains
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Clinical Performance Director of Nursing Allison Bussey
 PGD 0314 Patient Group Direction Administration of Adrenaline (Epinephrine) 1:1000 (1mg/ml) Injection By Registered Nurses employed by South Staffordshire & Shropshire Healthcare Foundation NHS Trust This
PGD 0314 Patient Group Direction Administration of Adrenaline (Epinephrine) 1:1000 (1mg/ml) Injection By Registered Nurses employed by South Staffordshire & Shropshire Healthcare Foundation NHS Trust This
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice
 PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
Obstetric Emergencies
 Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
Package for Emergency Resuscitation and Intensive Care Unit
 Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit
Package for Emergency Resuscitation and Intensive Care Unit Extracted from WHO manual Surgical Care at the District Hospital and WHO Integrated Management for Emergency & Essential Surgical Care toolkit
Rapid Sequence Intubation in Pre-Hospital Care
 Rapid Sequence Intubation in Pre-Hospital Care Dr Adam Chesters Specialist Registrar in Emergency Medicine and Pre-Hospital Care London s Air Ambulance CV University of Leicester Medical School Emergency
Rapid Sequence Intubation in Pre-Hospital Care Dr Adam Chesters Specialist Registrar in Emergency Medicine and Pre-Hospital Care London s Air Ambulance CV University of Leicester Medical School Emergency
Eileen Whitehead 2010 East Lancashire HC NHS Trust
 Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Airways Resistance and Airflow through the Tracheobronchial Tree
 Airways Resistance and Airflow through the Tracheobronchial Tree Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: [email protected] Useful links: www.sallyosborne.com
Airways Resistance and Airflow through the Tracheobronchial Tree Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: [email protected] Useful links: www.sallyosborne.com
THE AIRWAY IN AEROMEDICAL EVACUATION. PBLD (Problem Based Learning Discussion)
 THE AIRWAY IN AEROMEDICAL EVACUATION PBLD (Problem Based Learning Discussion) D. John Doyle MD PhD 2012 Edition Image Credit: http://www.arabianaerospace.aero/media/images/stories/medevac%20services.jpg
THE AIRWAY IN AEROMEDICAL EVACUATION PBLD (Problem Based Learning Discussion) D. John Doyle MD PhD 2012 Edition Image Credit: http://www.arabianaerospace.aero/media/images/stories/medevac%20services.jpg
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
Basic techniques of pulmonary physical therapy (I) 100/04/24
 Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Artificial Ventilation Theory into practice
 Artificial Ventilation Theory into practice Keith Simpson BVSc MRCVS MIET(Electronics) www.vetronic.co.uk [email protected] June 13 th 2014 Today we will discuss the administration of IPPV to anaesthetised
Artificial Ventilation Theory into practice Keith Simpson BVSc MRCVS MIET(Electronics) www.vetronic.co.uk [email protected] June 13 th 2014 Today we will discuss the administration of IPPV to anaesthetised
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
GRADE 11F: Biology 3. UNIT 11FB.3 9 hours. Human gas exchange system and health. Resources. About this unit. Previous learning.
 GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Electroconvulsive Therapy - ECT
 Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
Electroconvulsive Therapy - ECT Introduction Electroconvulsive therapy, or ECT, is a safe and effective treatment that may reduce symptoms related to depression or mental illness. During ECT, certain parts
