HIP FRACTURE SYSTEMS OPERATIVE TECHNIQUE
|
|
|
- Hilary Manning
- 9 years ago
- Views:
Transcription
1 HIP FRACTURE SYSTEMS OPERATIVE TECHNIQUE 1
2 T R O C H A N T E R I C G A M M A L O C K I N G N A I L
3 CONTENTS THE TROCHANTERIC GAMMA LOCKING NAIL 4 INDICATIONS AND DESIGN FEATURES 6 COMPLETE OPERATING GUIDE 8 Pre-operative Planning 9 Patient Positioning, Fracture Reduction 10 Anteversion Guide 11 Incision & Entry Point 12 Preparation of Medullary Cavity 13 Reaming Technique 13 Nail Insertion 14 Nail/Lag Screw Positioning 14 Lag Screw Targeting 15 This publication sets forth detailed recommended procedures for using Stryker Trauma devices and instruments. It offers guidance that you should heed, but, as with any such technical guide, each surgeon must consider the particular needs of each patient and make appropriate adjustments when and as required. Acknowledgements: The Gamma Locking Nail Operating Technique was compiled from the kind contributions of leading surgeons in many countries; the principal authors and commentators were:- Dr. G. Taglang, Dr. A. Grosse, Strasbourg, France Dr. S.C. Halder, Halifax, UK Dr K.S. Leung, Hong Kong Dr. S. Boriani, Bologna, Italy Lag Screw Drilling 17 Lag Screw Selection and Insertion 18 Set Screw Insertion 19 Distal Locking 20 Final Checking 22 Extraction 23 Problem Solving 24 Implants and Instrumentation 29 Instrument Guide 32 Our thanks are due to the many surgeons whose work has helped to confirm the utility of the technique to present and future users of the Gamma Locking Nail family. Warning: Bone screws referenced in this material are not approved for screw attachment or fixation to the posterior elements (pedicles) of the cervical, thoracic or lumbar spine. 3
4 THE TROCHANTERIC GAMMA LOCKING NAIL The Trochanteric Gamma Locking Nail is the latest development in the continuing evolution of the Gamma Locking Nail family. Like the original Gamma and Long Gamma Locking Nails, the Trochanteric Gamma Locking Nail has been designed by surgeons. The requirement, based on the Gamma experience of over three hundred thousand implants world-wide, was to develop an implant specifically for fractures in the trochanteric region, but with all the benefits of the existing Gamma Locking Nail family. The new Trochanteric Gamma Locking Nail is shorter and simpler than the standard Gamma Locking Nail, and has:- only one distal locking screw only one distal diameter 180 mm overall length profile designed for rapid and secure fixation of fractures around the trochanter The Trochanteric Gamma Locking Nail uses the same award-winning instrumentation* as the standard and Long Gamma Locking Nails, with the addition of new targeting sleeves. It combines the strength and biomechanical advantages of the existing Gamma family with a small inventory and simplified technique. And, as the latest development of one of the world s leading locking nails, the design of the Trochanteric Gamma Locking Nail benefits from an unrivalled pedigree of clinical experience. * Design-Innovation 95, awarded for high design quality; Design Centre, Nordrhein Westfalen. Published clinical studies for the Gamma Locking Nail family are among the most extensive for any surgical implant currently available. They consistently illustrate how successfully this evolving range of implants has achieved the original design goals: to improve both the procedure and prognosis for all grades of femoral fracture by extending the application of the established intramedullary principle to set a new standard for treatment: Early weight-bearing 1,2,3,4,5,6,7 through superior strength and stability Reduced trauma 3,4 through closed operating technique 3,4 Low blood loss 5,6, low level of wound problems 5 and low risk of infection 5 More secure fracture fixation through better biomechanics 7 The clinical objective of the Trochanteric Gamma Locking Nail, as with the original and Long Gamma Locking Nails, is:- Rapid mobilization, with fewer complications, for better patient rehabilitation 7 The operating technique for the Trochanteric Gamma Locking Nail is essentially the same as for the standard Gamma Locking Nail, the main variation being in the simpler distal locking process. Instrumentation for the Trochanteric Gamma Nail is also the same as for the rest of the Gamma family, obviating the need for further inventory and training for both the surgeon and the theatre team. The aim of this surgical technique booklet is to provide you with a simple step-by-step operating guide to aid successful adoption of the Trochanteric Gamma Locking Nail into your standard trauma practice. Once the technique has been learned, you should find the operative procedures simple to implement. In fact, many of the basic principles for the Trochanteric Gamma technique are those employed for all intramedullary closed locking nailing. If you are in any doubt as to any part of the operating procedure, please contact your local Stryker Trauma representative or the office shown on the back cover. 4
5 REFERENCES: 1. Grosse A., Favreul E., Taglang G., The Gamma Nail; The results at the CTO Strasbourg Paper presented at the International Symposium Recent Advances in Locking Nails, Hong Kong, Taglang G., Favreul E., Results from the Centre de Traumatologie et d Orthopédie, Strasbourg : Paper presented at the Advanced Course in Intramedullary Locking Nailing, Courchevel, France, February Leung K.S. et al, (Prince of Wales Hospital, Hong Kong), J Bone Joint Surg [Br] 1992; 74B, 3: Boriani S. et al., results of Multicentric Italian Experience on the Gamma Nail. A report on 648 cases, Orthopedics 1991;14,12: Radford P.J.,(University Hospital Queen s Medical Centre, Nottingham, England): Comparison of results of the Gamma Nail and Dynamic Hip Screw in Extracapsular fractures of the Proximal Femur. : Paper presented at Advanced Course in Intramedullary Locking Nailing, Courchevel, France, February Williams J.J., Cohen P.Z., Pittsburgh Orthopaedic Journal, 1990, Volume 1, pages De Groote W., Van Hoye M. et al, (St Jan General Hospital, Bruge/Middelheim General Hospital, Antwerp, Belgium): The Gamma Locking Nail in the treatment of trochanteric fractures Article in press. 5
6 INDICATIONS AND DESIGN FEATURES Indications Intertrochanteric fractures Pertrochanteric fractures High sub-trochanteric fractures Anatomical efficiency The Trochanteric Gamma Locking Nail is designed for optimum efficiency both in operating technique and subsequent rehabilitation. There are two basic components, universal in application to left or right hip fractures, and effective together in a very wide range of clinical situations and fracture complexity. Insertion is entirely by closed surgical technique, minimizing trauma, blood loss and infection potential. The Nail The intramedullary nail itself integrates several important mechanical features. The anatomic design is universal for all indicated applications, with a profile specifically designed for trochanteric fractures, and is 18 centimetres long overall. Variations in femoral neck anatomy are accommodated by a range of angles available for the lag screw entry (125, 130, 135 ). A single distal locking screw is used to prevent rotation in complex fractures. Cannulated for guide wire controlled insertion, and with a conical tip, the nail is available in a single distal diameter, 11 mm. The Lag Screw The lag screw, inserted through a small incision with the aid of a radiolucent targeting device, incorporates a special sliding lock to provide dynamic compression with axial stability. After insertion, a set screw inserted through the proximal head of the nail engages in one of four grooves in the lag screw. As these are of asymmetrical depth profile, they allow the lag screw to slide in one direction, producing dynamic osteosynthesis by compression during early weightbearing. The lag screw incorporates a rounded nose profile and self-tapping thread designed for easy insertion and resistance to cut-out. 6
7 Proximal diameter 17 mm Proximal plug The Gamma advantage strength and stability The Trochanteric Gamma Locking Nail offers significantly greater strength and stability in clinical use through the inherent biomechanical advantage of the intramedullary system. INDICATIONS & DESIGN FEATURES Angles: 125, 130 & 135 Lag Screw Set screw The biomechanical advantage As the load-bearing axis of the Trochanteric Gamma Locking Nail is closer to the hip joint fulcrum, the effective lever on the implant and femur is significantly less than with an external plate, reduced by a factor equivalent to d/d in the diagram (approximately 25%*). The resultant force is transmitted directly down the centre of the femur rather than through the many bone-weakening screws used in the side-plate system, increasing both the strength and reliability of the mechanical repair. Nail Distal diameter 11 mm Length 180 mm The rehabilitation advantage The extra strength effectively gained by the biomechanical advantage of the Trochanteric Gamma Locking Nail, combined with improved control of axial telescoping and rotational instability, allows early weight-bearing even in complex or unstable proximal fractures. Earlier mobilization, combined with dynamic compression and less traumatic operative technique, increases the chance of successful patient recovery and reliable repair. Distal locking screw D d D>d * Leung K.S., The Chinese University of Hong Kong: Gamma AP Anthropometric Study of Proximal Femur, Jan 1991; Data on file, Stryker Trauma. 7
8 COMPLETE OPERATING GUIDE This surgical technique has been devised in consultation with leading surgeons in many countries to be a basic guide, particularly for less experienced users of the Trochanteric Gamma Locking Nail. It is acknowledged that several alternative approaches to certain elements of the procedure are practised, and may have advantages for particular situations or surgeons. Parts of this guide may seem simplistic or redundant for experienced readers, but are included for the guidance of more junior staff. A chart of the complete operating instrumentation is folded into the back of this Operating Guide, and can be folded out for easy reference in conjunction with the text that follows. For easy identification, each instrument referred to in the guide is keyed to the chart by a reference number, and contains pictures of the Instrumentation and Implant cases, shown on page 30 and 31 complete with the catalogue numbers of each item. 8
9 PRE-OPERATIVE PLANNING In the majority of patients the standard 130 neck angle can be used without difficulty. The 125 neck angle may be needed in osteoarthritic coxa vara, and the 135 in coxa valga. Where such variations in femoral anatomy require an alternative, the following method may be used to confirm the nail angle selection:- Implant Selection X-ray templates are very helpful during preoperative planning. Use the X-ray Templates for short and long nails to select the correct implant and the optimal implant size. These templates show the true implant size at a magnification of 15%. The X-rays should be taken at this magnification (15%) for an optimum surgical outcome. If accurate anatomical reduction has been achieved, the X-ray can be taken from the fractured hip or from the contralateral side. NOTE: Please ensure precise alignment of the affected hip joint when using these templates. Template magnification is 15%. All dimensions (target angle and implant sizing) resulting from using these templates must be verified intraoperatively to ensure proper implant selection. COMPLETE OPERATING GUIDE Cat. No
10 PATIENT POSITIONING & FRACTURE REDUCTION Image intensifier positioning The image intensifier is positioned so that anterior-posterior and medio-lateral views of the trochanteric region of the affected femur can be easily obtained. This position is best achieved if the image intensifier can be positioned so that the axis of rotation of the intensifier is centred on the femoral neck of the affected femur. It is important to ensure that a view of both the distal and proximal tips of the nail can be obtained during the procedure without obstruction by the traction table. Figure 1 Fracture reduction The patient is placed in a supine position on the fracture table and closed reduction of the fracture is obtained as shown in figure 1. Traction is applied to the fracture, keeping the leg straight. Maintaining the traction, the leg is internally rotated degrees to complete the reduction of the fracture; the patella should then be either horizontal or slightly internally rotated. Figure 2 IMPORTANT Reduction should be achieved as anatomically as possible. If this is not achievable, reduction in one plane should be achieved, leaving reduction in the other plane to be achieved with the Trochanteric Gamma Locking Nail during insertion. The unaffected leg is abducted as far as possible in order to accommodate the image intensifier. The patient is then prepared and draped as for standard hip fracture fixation, but bear in mind that the incision is rather more proximal when positioning the drapes. 10
11 Figure 3 Anteversion guide insertion With the image intensifier C-arm in the horizontal position to give the lateral view of the femoral neck and head, a 2 mm Kirschner wire is inserted percutaneously, anterior to the shaft and parallel to the axis of the femoral neck and head. This is to provide a guide to the angle of anteversion of the femoral neck during later insertion of the nail, during which the targeting device is kept parallel to the Kirschner wire in the coronal plane (Figure 3). Alternatively, the guide wire can be inserted after the lag screw guide sleeve is placed in position (see page 15). 11
12 INCISION & ENTRY POINT INCISION Figure 4 Determination of the soft tissue incision position With experience, the tip of the greater trochanter can be located by palpation, and a horizontal skin incision of approximately 5 cm is made from the greater trochanter to the iliac crest. The incision is deepened through the fascia lata, splitting the abductor muscle for approximately 3 cm immediately above the tip of the greater trochanter, thus exposing its tip. A self-retractor is put in place (Figure 4). ENTRY POINT Finding the bone entry point The correct entry point can be identified by touch; it is located at the junction of the anterior third and posterior two-thirds of the tip of the greater trochanter and on the tip itself. Figure 5 Breaching the cortex The medullary canal is opened, under image intensification if necessary; use of the two-part curved awl (1) from the special instrument tray is recommended, as its conical sleeve is designed to be left in place to facilitate passage of the reamer guide wire. Care must be taken to ensure that the awl is not misplaced; this is more likely in the anteriorposterior plane i.e. as seen on the lateral view. The insertion point should be just on the tip of the greater trochanter. If it is very medial (e.g. in the piriform fossa) the nail will not go down the shaft properly, with the danger of fracturing the femur. When the entry point has been made, the reamer guide wire is placed in position so that the proximal femur may be prepared using flexible intramedullary reamers (Figure 5). 12
13 PREPARATION OF MEDULLARY CAVITY Figure 6 PREPARATION OF THE MEDULLARY CAVITY In order to accommodate the proximal end of the Trochanteric Gamma Locking Nail, the trochanteric region MUST be reamed up to 17 mm (Figure 6). The sub-trochanteric cavity must be 2 mm greater than the distal diameter of the nail i.e. at least 13 mm; reaming may be necessary in some patients to achieve this. When reaming is performed, the whole femoral canal should be over-reamed to 13 mm. REAMING TECHNIQUE Figure 7 Figure 8 Pass the reamer guide wire from the tip of the greater trochanter into the shaft of the femur as shown in Figure 7, using the Jacob s chuck (2). Rotating the guide wire during insertion will help it to take up the desired position and avoid it coming out of a posterior fracture line. Flexible reamers are used to ream the shaft of the femur in stages starting from 9 mm diameter and increasing in 0.5 mm increments (Figure 8), in all cases to a minimum of 13 mm. Care must be taken with flexible reamers to ensure that the guide wire is not displaced laterally during reaming. This could lead to resection of more bone on the lateral side of the wire, which in turn would lead to an offset position for the nail and a risk of fracturing the shaft. 13
14 NAIL INSERTION Assembly of targeting device The selected nail is now assembled onto the carbon fibre targeting device (3) as shown in Figure 9, ensuring that the locating peg slots into the corresponding notch; it is held by the nail holding bolt (4), and tightened using the socket wrench (5) and driver extension (6). Figure 9 Nail/Lag Screw Positioning Nail insertion is monitored with the image intensifier C-arm; the projected axis of the lag screw should be measured with a ruler on the monitor screen to ensure that the lag screw will be positioned in the ideal position. Visual estimation has proved to be unreliable. To ensure correct positioning of the lag screw, close attention must be given to the anteversion angle and to the depth of insertion of the nail into the femoral canal. Using anterior-posterior screening, the Trochanteric Gamma Locking Nail is inserted by hand (TAKE CARE TO AVOID UNDUE FORCE DO NOT USE A HAMMER * ) until the axis of the lag screw holes (visible as crescent shapes on the screen) is lined up with the inferior half of the femoral neck. The desired result of this is to ultimately position the lag screw tip just below the centre of the femoral head in the frontal plane (see Figure 15). Figure 10 Check: When the Trochanteric Gamma Locking Nail is inserted to its final depth the plane of the targeting device will be parallel to the percutaneous guide wire positioned earlier (see page 11). This ensures the correct degree of rotation to align the lag screw holes with the angle of anteversion of the femoral neck. * NOTE: It is sometimes difficult to fully insert the nail into the femur; one reason could be that the medullary canal is too narrow. As the Trochanteric Gamma Locking Nail is a very strong, rigid implant, it MUST NOT be forced into the femur e.g. by hammering, as there is a danger of fracturing the femur. If the nail will not go into the femoral cavity far enough to allow correct positioning of the lag screw, further reaming should be carried out in 0.5 mm increments until the nail will go in fully. 14
15 LAG SCREW TARGETING Figure 12 Figure 11 Figure 13 Remove the reaming guide wire using the Jacob s chuck (2), ensuring that the targeting device is supported to prevent rotational movement of the Trochanteric Gamma Nail. With the nail now inserted to the correct depth, slide the Trochanteric Gamma targeting sleeve (colour-coded green) (7) corresponding to the nail angle of the selected Trochanteric Gamma Locking Nail onto the end of the carbon fibre targeting device (3) (Figure 11). ENSURE YOU ARE USING THE TROCHANTERIC SLEEVE (GREEN CODED), NOT THE STANDARD OR LONG GAMMA TARGETING SLEEVES. Please ensure before proceeding that the nail holding bolt (4) is fully tightened. The targeting device (3) may require support by an assistant, to prevent its weight from externally rotating the nail, until the next stage is completed. Next, assemble the soft tissue protector (8) and the guide sleeve for the lag screw (9), and pass them through the targeting sleeve (7) to the level of the skin. This now indicates the position for the small incision to be made, which is developed down to the bone. The guide sleeve and tissue protector assembly is now passed through the incision to press firmly against the lateral cortex (Figure 12). If the guide catches the fascia lata, twisting it will usually allow it to pass through to the bone. If not already inserted, the percutaneous anteversion guide should now be placed (see page 11). The soft tissue protector (8) is removed and the lag screw guide sleeve (9) is firmly abutted to the lateral cortex of the femur to stabilize the targeting device (Figure 13). The thumbwheel on the targeting sleeve (7) should be tightened to lock the guide sleeve (9) in place and further stabilize the targeting assembly (Figure 13 inset). 15
16 With the guide sleeve (9) firmly engaged in the cortex, the awl (10) should be inserted and turned in order to pierce the lateral cortex (Figure14). Check for correct positioning on both anterior-posterior and lateral intensifier views. NOTE: Before proceeding, check that the guide wire for the flexible reamer used earlier has been removed. The soft tissue protector (8) is now re-inserted to act as a guide sleeve for the lag screw guide wire (11), which is inserted using the Jacob s chuck (2). The guide wire should be screwed into the subchondral bone, checking for position on both the anterior-posterior and lateral intensifier views. Checking is essential if you are to ensure good lag screw positioning. The tip of the guide wire (11) must be placed in the inferior half of the femoral head in the frontal plane, and on the midline in the lateral plane. The objective is to place the lag screw below the centre of the femoral head on the anterior-posterior view and centrally on the lateral view, to decrease the risk of it cutting superiorly out of the femoral head. (see Figure 15). If the guide wire (11) is too anterior or posterior it must be repositioned; this should seldom be necessary if the anteversion-guiding percutaneous wire has been inserted correctly (see page 11). If the guide wire (11) is mispositioned, the first step is to withdraw the guide wire itself, and then to withdraw the nail. Rotate the nail in the appropriate direction and re-insert as before. The guide wire is then re-drilled and control screening is carried out as before. Figure 14 Figure 15 16
17 LAG SCREW DRILLING Figure 16a After achieving a satisfactory position for the guide wire (11), the lag screw length required is measured using the lag screw length measuring gauge (12). Before starting to measure, ensure that the guide sleeve (9) is pressed firmly against the lateral cortex of the femur. Take the measuring gauge (12) and place it directly under the guide wire (11) as shown in Figures 16a & b. The measurement on the gauge is now transferred to the adjustable stop on the lag screw step drill (13). It should be noted that the adjustable stop is positioned with the chosen length next to the stop on the side towards the drill tip (Figure 17a). The collar is used to lock the stop in position (Figure 17b). Figure 16b Figure 17a Figure 17b 17
18 LAG SCREW SELECTION & INSERTION The soft tissue protector (8) is now removed and the lag screw step drill (13) is passed over the guide wire (11), through the guide sleeve (9) (see Figure 18a). The path for the lag screw is drilled using the Jacob s chuck (2). If exceptional resistance is encountered, a power drill may be used with great care. Drilling should continue until the stop impacts against the guide sleeve (see Figure 18b), ensuring that the targeting device is well supported to prevent backing out and rotation. If you check on the image intensifier at this stage you should see the tip of the guide wire protruding slightly from the step drill (Figure 18c). This is because the threaded portion of the guide wire is deliberately excluded from the drill measurement to prevent joint penetration by the drill. The correct length lag screw is chosen by selecting a size at least 5 mm longer than the measurement previously made on the lag screw gauge (12) for drilling (see Figure 16). It is important that the lag screw protrudes at least 5 mm from the lateral femoral cortex to retain rotational stability and to permit sliding. The correct size lag screw is now assembled with the lag screwdriver (14). The end thumbwheel must be pulled back, and the screw and driver connected as shown (Figure 19). After pulling back and connecting, the end thumbwheel is tightened to secure the connection. The lag screw is now passed over the guide wire (11), through the guide sleeve (9), and threaded up to the subchondral part of the head (Figure 20). If the guide wire is inadvertently removed, then the screw may still be passed without it provided that the guide sleeve is still in contact with the cortex. After tightening the screw ensure that the handle of the lag screwdriver (14) is either parallel or perpendicular to the targeting device (3) so that the set screw will engage in one of the four lag screw grooves (see Figure 21c). Figure 18a Figure 18c Figure 19 Figure 18b NOTE: It is important to observe the K-wire during drilling with the step drill on the intensifier to make sure that under no circumstances the k-wire will be pushed into the pelvis. This may damage large bloodvessels. 18
19 SET SCREW INSERTION Figure 20 Figure 21a The set screw is inserted through the opening in the carbon fibre targeting device (3) and the nail holding bolt (4) at the proximal end of the nail (Figure 21b). It is then tightened fully using the set screwdriver (15) and socket wrench (5). You may find this a little stiff because the screw has a nylon insert in the threads to prevent spontaneous loosening. The screw should then be unscrewed one quarter of a turn to ensure free sliding of the lag screw. Ensure that the set screw is still engaged in the groove by checking that the lag screw cannot now be rotated with the lag screwdriver (14). A proximal plug (see Fig 21c) is available to prevent ingrowth from becoming trapped in the proximal threads of the nail; where used, this is tightened using the set screwdriver (15). If distal locking is not indicated, disconnect the lag screwdriver (14) using the end thumbwheel, remove the lag screwdriver (14), guide sleeve (9), guide wire (11), targeting device (3) and sleeve (7), then complete the operation as described on page 22. If distal locking is indicated then leave the targeting device (3) and sleeve (7) in position and continue. Figure 21b Figure 21c 19
20 DISTAL LOCKING SCREW The decision to use the distal locking screw must be made according to the pattern of the fracture. Figure 22 It should be used:- When the fracture is unstable To control the length of a comminuted fracture of the proximal femoral shaft When there is a great disparity between the diameter of the nail and the femoral cavity Distal Screw targeting Insert the distal soft tissue protector (16) into the distal guide sleeve (17). Slacken the thumbwheel on the targeting sleeve (7), then pass the guide sleeve and protector through the hole in the targeting device (3). This indicates where the incision is to be made. ENSURE YOU ARE USING THE TROCHANTERIC SLEEVE (GREEN CODED), NOT THE STANDARD OR LONG GAMMA TARGETING SLEEVES. Figure 23 The incision is developed down to the lateral cortex, and the tissue protector sleeve assembly passed through as shown in Figure 22. The soft tissue protector (16) is now removed and the guide sleeve (17) is pushed into contact with the cortex. The guide sleeve should be locked into position using the thumbwheel provided (Figure 23). 20
21 Figure 24 Figure 25 If required, the distal awl (18) may be passed through the distal guide sleeve (17) and turned gently to make a small impression in the lateral cortex of the femur (Figure 24). Care should be taken to avoid causing fissures through excessive force e.g. through use of a hammer. The awl (18), if used, is now removed and the 5.5 mm drill guide sleeve (colour-coded blue) (19) is inserted. The 5.5 mm distal drill (colour-coded blue) (20) is used, making sure the distal guide sleeve (17) is held firmly engaged in the cortex at all times during the drilling (Figure 25). Figure 26 Distal Screw length measurement After drilling, measurement of the distal screw length is made by using the distal screw depth gauge (21), first removing the distal drill guide (19). The gauge passes through the distal guide sleeve (17) with its tip passing into the medial cortex (Figure 26). A measure of the distal screw length is therefore taken from a direct reading of the depth gauge (21). 25 and 30 mm screws are the most commonly used lengths. The correct size of distal self-tapping screw is introduced through the distal guide sleeve (17) and tightened using the distal screwdriver (22) (Figure 27). Figure 27 21
22 FINAL CHECKING FINAL CHECKING Figure 28a Figure 28b Remove the guide sleeve (17) and targeting device (3). Check the final position of the implant using the image intensifier in the anterior-posterior and lateral planes (Figures 28a & b). Close the wounds (don t forget the small stab wound) with one drain proximally. POSTOPERATIVE CARE AND REHABILITATION After the wound is closed, elastic bandage is applied from the toes to the hip. Active and passive mobilization of the lower limbs should be started immediately. The injured limb is kept elevated. The drain is removed when the drainage stops and usually within the first 48 hours. Walking can be started on the third day. For stable fractures with dynamic locking, full weightbearing walking can be started immediately. For unstable fractures with static locking, immediate full weight-bearing walking is allowed in fractures with good bone contact. For fractures with poor bone contact due to comminution and large medial third fragment, partial weight-bearing walking is allowed for the first 6 to 8 weeks. Full weight-bearing walking can be commenced when there is a bridging callus formed on the medial side as evident on the follow up X-ray. Dynamization of the fracture may be performed if delayed union is noted between four and six months after operation. If the implants are going to be removed after the fracture is healed, removal of the distal locking screw (dynamization) six months prior to implant removal is recommended in order to further improve the quality of the medial cortical bone. 22
23 EXTRACTION Figure 29 EXTRACTION OF TROCHANTERIC GAMMA LOCKING NAIL Where extraction is indicated, please proceed as follows:- Step I Remove the distal screw if fitted. Figure 31 Step II Make a small incision through the old scar below the greater trochanter to expose the outer end of the lag screw. Remove any bony ingrowth which may be obstructing the outer end or internal thread of the lag screw as necessary to ensure correct connection for the lag screwdriver (14). The lag screw guide wire (11) is then passed up to the lag screw into the head of the femur. The lag screwdriver (14) is passed over the guide wire, using the guide sleeve (9) as a tissue protector, and engaged with the distal end of the lag screw (Figure 29). Check that ingrowth does not obstruct secure engagement of the lag screwdriver (14), otherwise the lag screw or driver may be damaged and extraction made much more difficult. Figure 30 Step III An incision is made over the proximal tip of the nail, the proximal plug is removed, and the set screwdriver (15) is engaged with the set screw. The screw is rotated anticlockwise with the socket wrench (5) far enough to disengage it from the lag screw groove (Figure 30). The set screw does not need to be completely extracted. Step IV The lag screw is extracted by rotating the lag screwdriver (14) in an anticlockwise direction. The lag screw guide wire (11) must then be removed. Step V The nail extraction rod (23) is then threaded into the proximal end of the nail (Figure 31). A sliding hammer assembly (from the G & K system) is attached and the nail extracted. Finally the wounds are closed. EXTRACTION & PROBLEM SOLVING 23
24 PROBLEM SOLVING PROBLEM SOLVING Figure 32 Resistance to nail insertion Sometimes it is difficult to introduce the nail far enough into the femur. In the case below (Figure 32), the lower end of the nail is impinging on the anterior cortex of the femur. DO NOT hammer the targeting device (3). Some femurs are highly curved anteriorly and hammering will break the anterior cortex or the base of the greater trochanter. The cortex should be reamed again using a 13 mm reamer and the nail re-introduced (Figure 33). Figure 33 24
25 Figure 34 Bent guide wire If insertion of the guide wire (11) is repeated in order to get a satisfactory position, the wire may be bent due to its passing through a previous track. This makes it difficult to pass the step drill (13) over the bent wire (Fig 34). If the guide wire (11) is only slightly bent then the step drill (13) can be passed over it using a to and fro movement (Fig 35). If the guide wire (11) is markedly bent then it should be removed and a new guide wire inserted; alternatively, the step drill (13) can be passed smoothly up to the sub-chondral bone without wire (Fig 36). Figure 35 Figure 36 25
26 Posterior displacement In the case of a comminuted fracture, there is a tendency for the fracture to become displaced downwards, i.e. posteriorly, making it difficult to pass the guide wire (11) into the centre of the neck or head. This should be solved by lifting the nail insertion targeting device (3). Alternatively, the assistant could lift the greater trochanter up with his hand, and support it with a sandbag. This will maintain the neck and the femur in nearly the same axis, so that it will be easy to pass the guide wire (11) through the centre of the neck and head (Figures 37a, b, c). The position should then be checked on both anterior-posterior and lateral views using the image intensifier. Care is required to avoid radiation risk to the assistant. Figure 37a Figure 37b Figure 37c 26
27 Figure The 3.5 mm guide wire is then positioned parallel to the X-ray beam (as judged by the position of the image intensifier) and tapped gently in order to engage the sharp end into the cortex. Its position is then checked again on the image intensifier. 6. The 3.5 mm guide wire is then drilled through the lateral cortex, the power driver removed, leaving the guide wire in situ, and its position re-checked using the image intensifier to see that it lies in the centre of the circular hole. Distal repositioning Malposition of the distal locking screw hole can only happen due to loose fitting of the targeting device (3). It is unwise to try and make a further hole having tightened the targeting device, as the drill (20) will tend to follow its old track. A free-hand technique to drill the distal screw hole is recommended using the following procedure: Steps to be taken are: 7. The 3.5 mm guide wire is drilled through the medial cortex and its position checked with the image intensifier. It is then removed. 8. The 5.5 mm distal drill (19) from the case is then placed in the hole in the lateral cortex made by the 3.5 mm guide wire and its position checked with the image intensifier in both planes. The drill is held horizontal and passed through both cortices. It is then left in situ and its position checked with the image intensifier. It should be in the centre of the circular shadow as viewed on the image intensifier. 1. Remove the targeting device (3). 2. Place the image intensifier in a true lateral position (Figure 38) and obtain an image of the distal holes in the nail. 9. The screw is then selected and placed in position in the usual manner. 3. Rotate the Image intensifier C-arm until you see the nail hole as a perfect circle on the image intensifier. 4. A very sharp pointed 3.5 mm guide wire is fitted to the power drill, and its pointed end is placed on the outer cortex of the femur in the centre of the shadow of the round hole of the nail, as viewed on the image intensifier. 27
28 STERILE IMPLANTS The Trochanteric Gamma Nail has been available in a new sterile packaging, since the autumn of The nail is packed together with the set screw in one box, because the use of the set screw is required in every case. Cat No Description S Trochanteric Nail Kit S Trochanteric Nail Kit S Trochanteric Nail Kit
29 IMPLANTS & INSTRUMENTATION Trochanteric Gamma Locking Nail Implant Case Gamma Locking Nail Instrument Case 2A Trochanteric Trochanteric 130 Trochanteric Ø6, 28 x 25 Ø6, 28 x 30 Ø6, 28 x 35 Ø6, 28 x 40 Ø6, 28 x 45 Ø6, 28 x 50 CAT. No. DESCRIPTION CAT. No. DESCRIPTION Trochanteric Locking Nail Trochanteric Locking Nail Trochanteric Locking Nail S Set screw 8 x 22 mm S Lag screw 70 mm S Lag screw 75 mm S Lag screw 80 mm Small extraction rod Distal awl Distal screw depth gauge Distal obturator Jacob s chuck & key (S) Drill 5.5 mm dia. x 300 mm, blue Instrument case 2A & B (empty) S Lag screw 85 mm S Lag screw 90 mm S Lag screw 95 mm S Lag screw 100 mm S Lag screw 105 mm S Lag screw 110 mm S Lag screw 120 mm S Distal screw 25 mm S Distal screw 30 mm S Distal screw 35 mm S Distal screw 40 mm S Distal screw 45 mm S Distal screw 50 mm S Proximal plug Targeting sleeve / metal green Targeting sleeve / metal green Targeting sleeve / metal green Implant case (empty) S= sterile IMPLANTS & INSTRUMENTATION Note: For non sterile products remove S 29
30 Gamma Locking Nail Instrument Case 2B Gamma Locking Nail Instrument Case 3 CAT. No. DESCRIPTION CAT. No. DESCRIPTION Socket wrench Set screwdriver bit SW Lag screw guide sleeve Lag screw awl Kirschner wire guide sleeve (S) Kirschner wire 3.2 x 450 mm Lag screw length gauge Lag screw step drill Lag screwdriver Carbon-fibre targeting device Nail holding bolt Screwdriver for nail holding bolt Distal tissue protector Targeting sleeve Targeting sleeve Targeting sleeve Drill guide sleeve 5.5 mm (S) Drill bit 5.5 mm x 300 mm, blue Distal screwdriver Final Impactor Instrument case 3 empty Not stored on tray part curved awl Note: The Standard Gamma Targeting Sleeves (metal colour) are NOT for use with the Trochanteric Gamma Nail. 30
31 OPTIONAL INSTRUMENTS Optional Instruments not stored on tray One Shot Device Cannulated cutter Guide pin for cannulated cutter, 4 mm x 400 mm Prox. drill guide sleeve f. lag screw, 5.5 mm x 250 mm, blue Trochanteric targeting sleeve 125 (plastic) Trochanteric targeting sleeve 130 (plastic) Trochanteric targeting sleeve 135 (plastic) Gamma Extraction Set, complete, consists of: Universal rod Wrench 10/8 mm Sliding hammer Screwdriver, 5 mm x 250 mm, self-retaining Inserter for set screw, self-retaining Lag screwdriver Socket wrench Extraction rod conical Gamma extraction box Screwdriver, 5 mm x 250 mm, self-retaining Proximal femur drill, 17 mm x 300 mm Proximal femur guide sleeve, 300 mm Awl, curved S Guide wire 3.0 mm x 1000 mm, ball tip Guide wire handle Guide wire handle chuck Tap for lag screw X-Ray Templates X-ray template Trochanteric Gamma Nail (TGN) X-ray template Long Gamma Nail (LGN) 31
32 INSTRUMENT GUIDE 2. Jacob s chuck 1. Two-part curved awl 4. Nail holding bolt 3. Carbon fibre targeting device 7. Targeting sleeve 5. Socket wrench 6. Screwdriver for nail holding bolt 8. Kirschner wire guide sleeve (for lag screw) 9. Lag screw guide sleeve 10. Lag screw awl 11. Kirschner wire 13. Lag screw step drill 12. Lag screw length gauge 14. Lag screwdriver 15. Set screwdriver bit 16. Distal opturator 17. Distal tissue protector 18. Distal awl 19. Drill guide sleeve (for 5.5 mm distal drill) 20. Drill bit 5.5 mm, blue, callibrated, with centre tip 22. Distal screwdriver 21. Distal screw depth measuring gauge 23. Nail extraction rod 32
33 Fold out this page to show instrument guide for operating technique. DEVELOPED BY SURGEONS FOR FRACTURES AROUND THE TROCHANTER
34 The TGN is the latest development in Orthinox, the continuing evolution of the Gamma Locking Nail family designed for rapid and secure fixation of intertrochanteric and pertrochanteric fractures. Combining strength and biomechanical advantages of the existing Gamma family it is the Golden standard for proximal femoral fractures. The Long Gamma Nail is a specialised development of the original Gamma Locking Nail allowing surgeons to extend the benefits of the highly successful standard implant for trochanteric fractures. It has been designed to treat subtrochanteric, ipsilateral neck and shaft fractures as well as for prophylactic use. The OMEGA PLUS Compression Hip Screw System integrates innovative features such as sideplate made of superstrong alloy material and improved instrumentation. OMEGA PLUS Plates and Lag Screws are available in Sterile or Non-Sterile packaging for customer preference and convenience. This new generation of Cannulated Screws has been designed to optimise surgical outcomes while simplifying procedures. The ASNIS III System offers the surgeon a complete choice of implants, material and packaging combined with a new userfriendly instrumentation. PIN SYSTEM This innovative device has been developed for Femoral Neck Fracture and Slipped Capital Femoral Epiphysis treatments. The Hansson Pin System is a simple and precise instrumentation combined with a unique implant. This unthreaded pin with a spreading hook allows a strong and stable fixation through a simple and short procedure, thus preserving the blood supply and the bone integrity. GAM/05.03/HEI To ensure the best quality of its products and their improvements Stryker reserves the right to modify all or part of their products. Caution: Federal law (U.S.A) restricts this device to sale by or on the order of a licensed physician. MANUFACTURER: Stryker Trauma GmbH Prof.-Küntscher-Straße 1 5 D Schönkirchen Germany REF NO: B /Rev.04 LOT Stryker Corporation. All rights reserved.
Zimmer Natural Nail System. Cephalomedullary Nail Surgical Technique STANDARD
 Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Technique Guide. Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Expert LFN. Lateral Femoral Nail.
 Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
TRIGEN TAN and FAN Intramedullary Nails
 Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique
 M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation 1 Surgical Techniques for Fixation of Femoral Fractures
M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation 1 Surgical Techniques for Fixation of Femoral Fractures
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique. Table of Contents
 Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Versa-Fx II Femoral Fixation System Surgical Techniques
 Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Expert ALFN. Adolescent Lateral Femoral Nail.
 Expert ALFN. Adolescent Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Expert ALFN. Adolescent Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Surgical technique. End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue.
 Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Technique Guide. Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting.
 Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Implant Extraction Guide Module One & Two
 Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
Aesculap Veterinary Orthopaedics. Targon VET Interlocking Nail
 Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
DRAFT. Triathlon TS Knee System. Surgical Protocol. Version 1
 DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
Expert TN. Tibial Nail.
 Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
PFNA. With Augmentation Option.
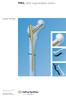 PFNA. With Augmentation Option. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
PFNA. With Augmentation Option. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
Zimmer Periarticular Elbow Locking Plate System
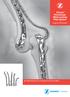 Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide. Orthopaedic Cable System. Cerclage solutions for general surgery.
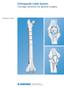 Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
TwinFix Cannulated Compression Screw
 TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
Zimmer M/L Taper Hip Prosthesis. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Titanium Wire with Barb and Needle. For canthal tendon procedures.
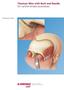 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Technique Guide. 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis.
 Technique Guide 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis. Table of Contents Introduction 3.5 mm and 4.5 mm Curved Locking Compression 2 Plates (LCP)
Technique Guide 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis. Table of Contents Introduction 3.5 mm and 4.5 mm Curved Locking Compression 2 Plates (LCP)
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Technique Guide. 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System.
 Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique
 Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
INTRODUCTION Cerclage Cable Vs. Monofilament Wire
 B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
DHS/DCS System. Including LCP DHS and DHS Blade.
 DHS/DCS System. Including LCP DHS and DHS Blade. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents
DHS/DCS System. Including LCP DHS and DHS Blade. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents
NCB Periprosthetic Femur Plate System. Surgical Technique
 NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Restoration Modular. Revision Hip System Surgical Protocol
 Orthopaedics Restoration Modular Revision Hip System Restoration Modular Calcar Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Revision Hip System Orthopaedics
Orthopaedics Restoration Modular Revision Hip System Restoration Modular Calcar Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Revision Hip System Orthopaedics
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
OptiLock Periarticular Plating System For Proximal Tibial Fractures. Pre-Launch Surgical Technique
 OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
TABLE OF CONTENTS. Indications and Contraindications 3. Features and Benefits 4. Ease of connection 4 Stable fixation concept 5
 Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Technique Guide. Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
SALVATION. Fusion Bolts and Beams SURGICAL TECHNIQUE
 SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
Zimmer MOST Options System
 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
Expert HAN. Expert Hindfoot Arthrodesis Nail.
 Expert HAN. Expert Hindfoot Arthrodesis Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Expert HAN. Expert Hindfoot Arthrodesis Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Metasul LDH Large Diameter Head
 Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
MIS Direct Anterior Approach Surgical Protocol
 Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Exeter X3 RimFit. Acetabular Cup Surgical Protocol
 Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
Exeter X3 RimFit Acetabular Cup Surgical Protocol 2 Exeter X3 RimFit Surgical Protocol Table of Contents Indications and Contraindications... 4 Introduction... 5 Surgical Protocol... 6 Step 1 - Pre-Operative
NCB Proximal Humerus System. Surgical Technique
 NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
Technique Guide. VersiTomic. Michael A. Rauh, MD. Anterior Cruciate Ligament Reconstruction
 Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
MINI FRAGMENT SYSTEM. Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW
 MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
Exeter. Surgical Technique. V40 Stem Cement-in-Cement. Orthopaedics
 Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Cable System. For Orthopaedic Trauma Surgery.
 Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
VariAx Distal Radius Locking Plate System. Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates
 VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Zimmer NexGen LCCK. Surgical Technique for use with LCCK 4-in-1 Instrumentation. Contact your Zimmer representative or visit us at www.zimmer.
 Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
Knotilus TM. Anchor Instability Repair. Technique Guide
 Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation
 1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
1 Proximal Hip Fracture Open Reduction/Internal Fixation and Rehabilitation Surgical indications and Considerations Anatomical Considerations: The hip is a ball and socket joint with the femoral head aligned
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
P REPLACEMENT SURGERY
 P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
P REPLACEMENT SURGERY DIRECT ANTERIOR APPROACH M I N I M I Z I N G R E C O V E R Y. M A X I M I Z I N G R E S U L T S. CENTER FOR MINIMAL INVASIVE JOINT SURGERY 2301 25TH STREET SOUTH FARGO ND 58103 701-241-9300
How To Perform An Elbow Operation
 Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
LCP Compact Foot/Compact Hand.
 LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
Wagner Cone Prosthesis Hip Stem. Surgical Technique
 Wagner Cone Prosthesis Hip Stem Surgical Technique Wagner Cone Prosthesis Hip Stem Surgical Technique 3 Surgical Technique Wagner Cone Prosthesis Table of Contents History 4 Design Features 4 Wagner Cone
Wagner Cone Prosthesis Hip Stem Surgical Technique Wagner Cone Prosthesis Hip Stem Surgical Technique 3 Surgical Technique Wagner Cone Prosthesis Table of Contents History 4 Design Features 4 Wagner Cone
STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13
 STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13 (See Supplemental Instructions for trailers with heavy duty round footplates and/or Power Leveling Systems) PHONE SUPPORT
STEADYfast Stabilizer Installation Notes Fifth Wheel and Travel Trailers 11/23/13 (See Supplemental Instructions for trailers with heavy duty round footplates and/or Power Leveling Systems) PHONE SUPPORT
Introduction to the Bertram Hip Spacer
 Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Surgical Technique and Reference Guide
 Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
ACCOLADE II. Orthopaedics. Femoral Hip System. Surgical Technique
 ACCOLADE II Femoral Hip System Orthopaedics Surgical Technique Indications The indications for use of the total hip replacement prostheses include: Noninflammatory degenerative joint disease, including
ACCOLADE II Femoral Hip System Orthopaedics Surgical Technique Indications The indications for use of the total hip replacement prostheses include: Noninflammatory degenerative joint disease, including
Zimmer Segmental System. Distal Femoral Surgical Technique
 Zimmer Segmental System Distal Femoral Surgical Technique INTRO Zimmer Segmental System Distal Femoral Surgical Technique Introduction The Zimmer Segmental System is designed to address significant bone
Zimmer Segmental System Distal Femoral Surgical Technique INTRO Zimmer Segmental System Distal Femoral Surgical Technique Introduction The Zimmer Segmental System is designed to address significant bone
Surgical technique. Sagitta EVL
 Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
*smith&nephew SLR-PLUS
 Surgical Technique *smith&nephew SLR-PLUS Cementless Revision Stem SLR-PLUS Table of Contents Comments from the Author s Clinic... 3 Indications... 4 Contraindications... 5 Preoperative Planning... 5
Surgical Technique *smith&nephew SLR-PLUS Cementless Revision Stem SLR-PLUS Table of Contents Comments from the Author s Clinic... 3 Indications... 4 Contraindications... 5 Preoperative Planning... 5
Technique Guide. 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system.
 Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Lentur Cable System. Surgical Technique
 Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Primary V40 Surgical Protocol. Exeter. total hip system
 Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
TriLock 1.5 Implants for the Phalanges
 P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
S-ROM NOILES. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
 S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique
 Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
for Image Scaling Enabling Digital Orthopaedics
 Calibration Devices, Use & Positioning for Image Scaling Enabling Digital Orthopaedics DIGITAL IMAGE SCALING As Radiology becomes filmless. Current planning practices used by surgeons with acetate sheets
Calibration Devices, Use & Positioning for Image Scaling Enabling Digital Orthopaedics DIGITAL IMAGE SCALING As Radiology becomes filmless. Current planning practices used by surgeons with acetate sheets
Rebuild Instructions for 70001 and 70010 Transmission
 Rebuild Instructions for 70001 and 70010 Transmission Brinn, Incorporated 1615 Tech Drive Bay City, MI 48706 Telephone 989.686.8920 Fax 989.686.6520 www.brinninc.com Notice Read all instructions before
Rebuild Instructions for 70001 and 70010 Transmission Brinn, Incorporated 1615 Tech Drive Bay City, MI 48706 Telephone 989.686.8920 Fax 989.686.6520 www.brinninc.com Notice Read all instructions before
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
Double Bone Plug Meniscus Reconstruction Surgical Technique
 Double Bone Plug Meniscus Reconstruction Surgical Technique Double Bone Plug Meniscus Low Profile Reamer 2-0 FiberWire Meniscus Repair Needles Collared Pin & Coring Reamer Set RetroConstruction Drill Guide
Double Bone Plug Meniscus Reconstruction Surgical Technique Double Bone Plug Meniscus Low Profile Reamer 2-0 FiberWire Meniscus Repair Needles Collared Pin & Coring Reamer Set RetroConstruction Drill Guide
Design surgeon list. Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team:
 Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
Original Assembly Guide
 TCT Multipurpose Single Bevel Sliding Compound Mitre Saw Original Assembly Guide Read instructions before assembling this tool. Table of Contents GB Assembly Guide Read instructions before assembling this
TCT Multipurpose Single Bevel Sliding Compound Mitre Saw Original Assembly Guide Read instructions before assembling this tool. Table of Contents GB Assembly Guide Read instructions before assembling this
