Zimmer MOST Options System
|
|
|
- Hugh Walton
- 10 years ago
- Views:
Transcription
1 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma
2
3 Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction 2 Preoperative Planning 3 Alignment 3 Preoperative Planning for Severe Bone Loss of the Knee or Hip 3 Surgical Options 3 Distal Femoral Replacement 5 Leg Length Measurement 6 Implant Selection 6 Distal Femoral Resection 6 Femoral Canal Preparation 7 Tibial Preparation 7 Patellar Preparation 13 Trial Assembly 13 Component Selection and Assembly 16 Component Implantation 17 Hinge Assembly 19 Proximal Tibial Replacement 21 Leg Length Measurement 22 Implant Selection 22 Proximal Tibial Resection 22 Tibial Preparation 24 Femoral Preparation 25 Trial Assembly 31 Component Selection and Assembly 32 Component Implantation 34 Hinge Assembly 35 Proximal Femoral Replacement 37 Proximal Femoral Options 38 Femoral Measurements and Resection 39 Implant Selection 40 Femoral Canal Preparation 41 Trial Assembly 42 Trial Reduction 42 Bowed Stems Implant Assembly 43 Implantation of the Femoral Component 44 Reattachment of the Greater Trochanter 45 Reattachment of the Abductor Tendon 46 Total Femoral Replacement 47 Implant Configuration 48 Tibial Preparation 49 Component Implantation 50 Implant Assembly 51 Hinge Assembly 52 Component Disassembly 54 Limb Lengthening 55 Appendix A 56 Extramedullary Tibial Option - All poly tibial sleeve 56 Appendix B 60 Intramedullary Tibial Option - Metal-backed tibia without a stem 60 Appendix C 67 Intramedullary Tibial Option - Metal-backed tibia with a long stem 67 Appendix D 73 Patellar Preparation 73 Appendix E 75 Hinged Tibia Augment Preparation 75 Appendix F 76 Hinged Femur Augment Preparation 76
4 2 Zimmer MOST Options System Surgical Technique Introduction As total knee and hip arthroplasty have evolved, so has the need for a constrained system to meet the special requirements for arthroplasty in cases of severe bone loss such as tumor resections, trauma, ligamentous laxity or severe deformity. The Zimmer MOST Options System is designed to facilitate intraoperative decisions with a variety of options for femoral and tibial components, implant connections and fixation of the implants. These options include the basic and soft tissue attachment femoral hip components, hinged femoral, distal femoral, hinged tibial and proximal tibial knee components. The knee components are based on a rotating hinge. The knee components can be adapted to replace bone loss of the femur or tibia. The hinged femoral component can be fitted with distal spacers singularly or in combination to match the patient s needs. The hinge has the advantage of a long post and slight taper angle to significantly reduce the probability of dislocating from the tibial insert. In addition, the hinge position is centralized to reduce the forces on the patellar tendon during flexion. The hinged tibial baseplate has an anterior offset cone for improved placement in the tibial canal. The hinged tibial component can be fitted with spacers singularly or in combination to match the patient s needs. Porous and nonporous tibial revision stem adapters connect with a variety of segments and smooth and fluted stems based on the patient s requirements. The basic proximal femur and proximal femur with soft tissue attachments provide flexibility in addressing severe bone loss of the proximal femur. The segments provide numerous options to make up for lost bone. One advantage of the system is the ability to easily mix and match components to address patients individual needs. Distal Femur Proximal Femur Total Femur Proximal Tibia
5 Zimmer MOST Options System Surgical Technique 3 Preoperative Planning Implants and instruments are designed to provide precise anatomical alignment by using intramedullary guides for the femur. The tibia has the option of intramedullary or extramedullary instrumentation. Tibial alignment is achieved by creating a horizontal plane that is 90 degrees to the anatomic axis of the tibia and the distal femur at 6 degrees of valgus. These angles restore the correct overall anatomic valgus alignment of the leg. In severe bone loss, preoperative planning is important to assist in estimating the proper placement of the implants and their sizes. a c d 4 5 System Overview Distal Femoral Replacement Preoperative templating is also helpful in determining the maximum size and length of the femoral or tibial stems. On the tibial side, preoperative measurements using the fibular head as a reference point will show if tibial bone loss is present and which type of tibial component, stem, augmentations or bone grafts will be necessary. Fig. 1 illustrates one possible combination for each category of the MOST Options System. The possible combinations of proximal femoral components are illustrated in Fig. 2 and the possible combinations of distal femoral, proximal tibial and total femoral components are illustrated in Fig. 3. Fig. 1 a Distal Femoral Replacement b Proximal Tibial Replacement c Proximal Femoral Replacement d Total Femoral Replacement Segment b Basic Proximal Femur Proximal Femur with Tissue Attachment Proximal Tibial Replacement Proximal Femoral Replacement MOST Fluted Bowed Stem MOST Hex Bowed Stem Total Femoral Replacement Fig. 2 47
6 4 Zimmer MOST Options System Surgical Technique Basic Proximal Femur Proximal Femur with Tissue Attachment Bolts /002 Stem Options 75, 125, 175 and 190mm 75mm Smooth / mm Smooth / mm Fluted / mm Fluted Revision Stem / mm Smooth Revision Stem /175 Fluted Hinged Femur 3 sizes, L and R /203 Smooth Femoral Spacers 5 and 10mm /10-101/213 MOST Fluted Bowed Stem /052 All Poly Patella /062 Segments 12.5mm increments /027 MOST Hex Bowed Stem /042 Washers /002 Total Femoral Segment with CSTi Coating Segments 12.5mm increments /027 Distal Femur/Condylar End /011 4mm MOST Options Hinge Kit MOST Hinge Kit Hinged Tibia Inserts 4 sizes; 5 thicknesses /04-006/021 Proximal Tibia Inserts 5 thicknesses /021 Fig. 3 Hinged Tibia 4 sizes /004 Tibial Spacers 6 and 11mm /11-01/04 Plug Stem Options 75, 125, 175 and 190mm Tibial Revision Stem Adapter (Porous) mm Fluted Revision Stem /185 Proximal Tibia Tibial Revision Stem Adapter (Nonporous) mm Smooth Revision Stem /175 All-Poly Tibial Sleeve 4 sizes; 5 thicknesses /04-009/019 Warning!: Screws that are packaged with the 75, 125, 175, 190, and 250mm revision stems will NOT work with the hinged femurs, hinged tibial baseplates, or tibial stem adapters. Use only the collet screws that are packaged with the hinged femoral, hinged tibial, and tibial stem adapter components. Do not use the screw that is packaged with the stem.
7 Zimmer MOST Options System Surgical Technique 5 Distal Femoral Replacement Distal Femoral Replacement
8 6 Zimmer MOST Options System Surgical Technique Distal Femoral Replacement Leg Length Measurement After exposure of the distal femur and proximal tibia has been achieved, the proposed resection levels are marked with the extremity extended in a reproducible position. Resection Level Determine the resection level based on the articular surface of the distal femur. Set the resection guide to the resection level and mark a horizontal line with an osteotome, bovie or marker (Fig. 4). Implant Selection Determine the implant configuration to finalize the resection level. Select the stem/segment combination from Table 1 to determine the final resection level. Fig. 4 Note: Each large taper connection adds 1mm to the total length. The intramedullary length of the bowed stems is 152mm. Distal Femoral Resection Resect the distal femur at or slightly distal (i.e., 0.5mm to 1mm) to the marked resection level. The additional amount is to account for slightly oblique cuts and femoral resection planing. Note: To improve the swing phase of the patient s gait, some surgeons choose to slightly shorten the limb. Table 1 Distal Femoral Resection with Hex and Fluted Bowed Stems with Segments Distal Femur (condylar end) Bowed Stem Segments Total Length 65mm 30mm 0mm 96mm 65mm 30mm 30mm 127mm 65mm 30mm 42.5mm 139.5mm 65mm 30mm 55mm 152mm 65mm 30mm 67.5mm 164.5mm 65mm 30mm 80mm 177mm 65mm 30mm 55+30mm 183mm 65mm 30mm mm 195.5mm 65mm 30mm 105mm 202mm 65mm 30mm 80+30mm 208mm 65mm 30mm mm 220.5mm 65mm 30mm 130mm 227mm 65mm 30mm mm 233mm 65mm 30mm mm 245.5mm 65mm 30mm 155mm 252mm 65mm 30mm mm 258mm 65mm 30mm mm 270.5mm 65mm 30mm mm 283mm Note: Each taper junction adds 1mm
9 Zimmer MOST Options System Surgical Technique 7 Bowed Femoral Stem Preparation Flexible ream the femoral canal until cortical bone through the isthmus is reached. (The flexible reamers are not part of the MOST Options instrument system but are usually available through the hospital.) The intramedullary length of stems is 152mm. Ream to a depth greater than 152mm to allow proper seating of the stem shoulder on cortical bone and placement of a cement restrictor if desired. Recommended reamer diameters are as follows: Stem Size 12mm 14mm 16mm Hex Bowed Stem Ream Diameter 13mm to 14mm 15mm to 16mm 17mm to 18mm Fluted Bowed Stem Ream Diameter 12mm 14mm 16mm Tibial Preparation Direct vertical exposure of the tibial plateau is necessary. This is facilitated by soft tissue releases around the tibial metaphysis, medial and lateral soft tissue retraction with small angled knee retractors and subluxation of the tibia anteriorly with a large angled knee retractor. There are four surgical options for tibial preparation: 1 Extramedullary Tibial Option, which uses a metal-backed hinged tibia without a long stem (See page 7, below), 2 Extramedullary Tibial Option, which uses an all-poly tibial sleeve (See Appendix A, page 56), 3 Intramedullary Tibial Option, which uses the metal-backed tibia without a stem (See Appendix B, page 60), and 4 Intramedullary Tibial Option, which uses a metal-backed tibia with a long stem (See Appendix C, page 67). Fig. 5 Pilot Planer Mallet Distal Femoral Replacement Note: The MOST hex bowed stems are tapered 2mm distally. The fluted bowed stems are sized 0.5mm larger than the reamed hole diameter to enhance the fit within the canal. Planing the Femoral Bone Screw the appropriate-sized pilot for the stem diameter selected (12mm, 14mm or 16mm) to the planer (Fig. 5). Plane the resection using a power tool with a Zimmer adapter until the cortical bone is smooth and even. A Tommy Bar or pin may be inserted in the cross hole to aid in pilot removal after planing. Extramedullary Tibial Option (Using the metal-backed hinged tibia without a long stem) The Extramedullary Tibial Alignment Guide assembly consists of the extramedullary guide, Tibial Saw Guide and a 2mm, 10mm or 15mm Tibial Stylus. Select the appropriate Tibial Stylus based on the amount of required bone resected on the tibia. Adjust the extramedullary guide assembly to the approximate tibial length. Tap the longest pin of the guide into the central portion of the proximal tibia (Fig. 6). This fixes the guide to the tibia but allows for rotation until the second pin is impacted. Tibial Saw Guide Extramedullary Guide Fig. 6
10 8 Zimmer MOST Options System Surgical Technique Rotational Alignment Rotation is selected based on the anterior crest of the tibia and the bimalleolar axis. Make sure the guide is parallel to the crest of the tibia in the anterior/posterior and medial/lateral view. The bottom nut on the ankle cradle should be positioned to maintain a 0 degree tibial slope (Fig. 7). The anterior tibial plateau should be aligned parallel with the cutting block (Fig. 8). Rotation is then locked in place by impacting the second pin into the tibia. Extramedullary Alignment Guide Parallel Bottom Nut Fig. 7 Fig. 8
11 Zimmer MOST Options System Surgical Technique 9 Zero Degree Tibial Slope A zero degree tibial cut is recommended to accommodate the cone of the hinged tibial baseplate into the tibia. Tibial Stylus Level of Resection The 10mm tibial stylus is attached to the tibia saw block. It is used to determine the tibial saw guide position for minimal resection of the proximal tibia (Fig. 9). The total thickness of the hinged tibia, hinged tibial insert, 4mm MOST Options hinge is 15mm. The stylus will position the tibial saw guide 10mm below the point of reference. If additional bone needs to be resected, the tibial saw block may be moved in 2mm increments (Example: 10mm + 2mm = 12mm). Note: A 10mm resection will raise the joint line approximately 5mm. Remember to adjust the distal femoral cut to maintain total length measurement. There is a 15mm tibial stylus in the system that may be used to obtain a 15mm tibial resection. Fig. 9 Distal Femoral Replacement The cutting guide is then stabilized by drilling and pinning through the two outermost holes on the DRILL ON LINE (Fig. 10). This allows for 2mm of adjustment proximally and 4mm distally. The lateral drill point is first placed after retracting the patellar tendon, followed by the medial drill point. If the medial drill point appears to walk, this can be avoided by marking the entry point through the block, then drilling outside the block to pierce the cortex. Re-drill the hole through the block. Turn the knurled nut counterclockwise until it falls free from the guide to disengage the alignment guide from the tibial saw block. Knurled Nut Fig. 10
12 10 Zimmer MOST Options System Surgical Technique Disassemble the jig by removing the stylus and extramedullary alignment guide using a slaphammer (Fig. 11). Cutting the Proximal Tibia A Miller guide (angel wing) can be placed on the tibial saw guide along the medial and lateral edge of the tibia to confirm the level of desired tibial resection. If it appears that an inadequate resection will occur, adjust the tibial saw guide in 2mm increments to a lower level. Use angled retractors to protect soft tissue and ligaments. Cut the proximal tibia with the appropriate saw blade for the saw block (Fig. 12). Slaphammer Note: Saw blades especially designed for this system are recommended. The blades are 1 inch wide with a shank thickness of by 90mm long and will best match the saw guide. Fig. 11 Fig. 12
13 Zimmer MOST Options System Surgical Technique 11 Proximal Tibial Sizing and Drilling To avoid soft tissue impingement, select the appropriate size Tibial Baseplate Sizer/Reamer Guide that adequately covers but does not overhang the proximal tibia. Adjust the guide as far anteriorly as possible and slightly medial to the midline to avoid lateral perforation. Final rotational alignment is referenced off the tibial tubercle with the handle of the guide in the medial one-third of the tubercle. The Baseplate Sizer/Reamer Guide is then stabilized with four pins as the holes are drilled using the 3.2mm (1/8 inch) by 5 inch drill bit (Fig. 13). Check the alignment of the tibial cut with the Axial Alignment Rod through the handle of the Baseplate Sizer/Reamer Guide. The tibial profile dimensions correspond to the following A/P and M/L dimensions. Proximal Tibial Cone Preparation Attach the Baseplate Sizing Bushing to the Tibial Baseplate Sizer/Reamer Guide by turning in the direction of the arrow on the tibial baseplate sizer/reamer guide. Attach the 11mm tibial starter drill to a power tool and place it through the baseplate sizing bushing (Fig. 14). If resistance is encountered, remove the drill and inspect the proximal tibia for cortical thinning or perforation. The correct depth is established when the nose of the power tool touches the top of the Baseplate Sizing Bushing. Remove the Baseplate Sizing Bushing by turning it in the opposite direction of the arrow on the Tibial Baseplate Sizer/Reamer Guide. Distal Femoral Replacement Tibial Size A/P M/L 1 46mm 65mm 2 48mm 71mm 3 51mm 77mm 4 54mm 83mm Baseplate Sizer/Reamer Guide Tibial Starter Drill Baseplate Sizing Bushing Fig. 13 Fig. 14
14 12 Zimmer MOST Options System Surgical Technique Assemble the Primary Cone Reamer to the Cone Reamer Guide (Fig. 15). The Cone Reamer Guide assembly is attached to a power tool with a Zimmer quick disconnect fitting and then assembled to the Baseplate Sizer/ Reamer Guide with a slight turn in the direction of the arrow on the Tibial/ Sizing Reamer Guide. The Baseplate Sizer/Reamer Guide must be clear of all bone materials etc. before the Cone Reamer Guide is assembled (Fig. 16). Ream the tibial cone until the nose of the power tool touches the top of the Cone Reamer Guide (Fig. 16). Remove the reamer guide from the Baseplate Sizer/Reamer Guide by a slight turn in the opposite direction of the arrow on the Tibial/Sizing Reamer Guide. Note: Care needs to be taken to ensure the correct position of the cone reamer in the proximal tibia. If the cone reamer is angled into the tibia in the A/P or M/L planes, the tibial cone may not fully seat or the tibial cortex may be compromised. Primary Cone Reamer Guide Fig. 15 Primary Cone Reamer Fig. 16
15 Zimmer MOST Options System Surgical Technique 13 Tibial Keel Preparation and Tibial Trial Insertion Once a hole has been reamed, the Hinged Tibial Trial and Trial Stem are assembled and then inserted into the tibia. Rotate the Hinged Tibial Trial to the proper position. The Keel Broach and modular handle are assembled and inserted into the Hinged Tibial Trial. The modular handle of the Keel Broach is gently impacted with a mallet until it is fully seated (Fig. 17a). Remove the modular handle from the Hinged Tibial Trial (Fig. 17b). Patellar Preparation The decision to resurface the patella is an individual surgeon preference. Please refer to Appendix D (page 73). Fig. 17a Keeled Broach Fig. 17b Hinged Tibial Trial Distal Femoral Replacement Trial Assembly The Metal-Backed Hinged Tibial Trial uses the 4mm trial hinge. The All-Poly Sleeve uses the Standard Trial Hinge. The 4mm Trial Hinge and Standard Trial Hinge are not interchangeable (Fig. 18). 4mm MOST Options Hinge Kit MOST Hinge Kit Attach the appropriate Distal Femoral Trial to the Bowed Stem Trial. The Hex Bowed Stem Trial has an anterior mark to ensure proper orientation. The Fluted Bowed Stems use the Hex Trial Stems. Insert the Femoral Trial Assembly into the femoral canal and evaluate for fit. Slightly impact the distal end of the Distal Femoral Trial with the Distal Femoral Impactor and a mallet if needed (Fig. 19). Mark the anterior femoral bone in line with the mark on the Bowed Stem Trial to ensure proper orientation of the implant. The surgeon may slightly externally rotate the femoral component based on the anterior femur and linea aspera to assure proper patellar tracking. Fig. 18 Hinged Tibia Inserts Hinged Tibia Bowed Hex Stem Trial All-Poly Tibia Sleeve Hinged Femur Trial Condylar Trial Distal Femoral Impactor Go to the appropriate section for either a Metal-Backed Hinged Tibia (Page 14) or an All-Poly Sleeve (Page 15) for tibial trialing. Fig. 19
16 14 Zimmer MOST Options System Surgical Technique Metal Backed Hinged Tibial Trialing Install the Tibial Baseplate Trial into the tibia. Then, install the final thickness Hinged Tibial Insert Trial into the Hinged Tibial Trial. Finally, install the 4mm Hinge Trial into the Hinge Tibial Insert. Align the hinged femur or distal femur with the 4mm Hinge Trial. The Trial Hinge Pin is installed from either side of the leg (Fig. 20). Note: The 4mm Hinge Trial is used with the Metal Backed Hinged Tibia. It is not interchangeable with the Standard Trial Hinge. The leg should be manipulated through the range of motion. Care must be taken not to pull too hard on the leg due to potential damage incurred to nerve and vascular structures. Attention should be paid to limb rotation. The knee should fully extend, but not hyperextend. The posterior soft tissue should be palpated in full extension to ensure that there is no excessive tension. Removal of Femoral Trial and Hinged Tibia Trial Remove the femoral trial by placing a slaphammer in the hinge pin hole (Fig. 21a). Remove the Tibial Insert Trial from the Trial Baseplate by using an osteotome and turning it slightly clockwise or counterclockwise (Fig. 21b). Remove the Trial Baseplate and Keel Broach by threading the broach handle into the posterior hole of the Hinged Tibia Trial and extracting the assembly with the slaphammer (Fig. 21c). Fig. 20 Hinge Pin Trial Fig. 21a Hinged Tibial Insert Trial Trial Baseplate Slaphammer Femoral Trial Tibial Trial Insert Trial Baseplate 4mm Hinge Trial Slaphammer Broach Handle Hinged Tibia Trial Fig. 21b Fig. 21c
17 Zimmer MOST Options System Surgical Technique 15 All-Poly Tibial Sleeve Trialing Install the appropriate thickness of the All-Poly Tibial Component Trial into the tibia. Then install the Standard Trial Hinge into the All-Poly Tibial Trial. Align the Distal Femoral Trial or Hinged Femoral Trial with the Standard Trial Hinge. The Trial Hinge Pin is installed from either side of the leg (Fig. 22a). The leg should be manipulated through the range of motion. Care must be taken not to pull too hard on the leg due to potential damage incurred to nerve and vascular structures. Removal of Femoral Trial Remove the distal femoral trial by placing a slaphammer in the hinge pin hole (Fig. 22b). Hex Bowed Stem Trial Segment Femoral Trial Standard Trial Hinge Trial Hinge Pin Distal Femoral Replacement All-Poly Tibial Component Trial Fig. 22a Femoral Trial Slaphammer Fig. 22b
18 16 Zimmer MOST Options System Surgical Technique Implant Selection and Assembly The femoral and tibial components are assembled prior to mixing the cement. Note: If fluted stems are used, cement should not be allowed to contact the fluted portion of the stem. Femoral Impacting Plug Stem Stem Impacting Sleeve Distal Femoral Assembly If segments are needed, rest the femoral-articulating surface on the Femoral Impacting Stand prior to impaction of the segment into the distal femur using the Femoral Impacting Plug and a mallet (Fig. 23). Segment Bowed Stem Assembly To impact a bowed stem into a segment or the distal femur, rest the femoralarticulating surface of the distal femur on the Femoral Impacting Stand prior to impaction using the Stem Impacting Sleeve and a mallet (Fig. 24). Hinged Tibia Assembly Assemble the Hinged Tibial Plug onto the distal end of the Hinged Tibial Baseplate. Tighten the screw from the proximal side using the hex bit and handle (Fig. 25). Distal Femur Femoral Impacting Stand Fig. 23 Fig. 24 Handle Segment Distal Femur Femoral Impacting Stand Fig. 25 Hex Bit Hinged Tibial Baseplate Hinged Tibial Plug Warning!: Screws that are packaged with the 75, 125, 175, 190, and 250mm revision stems will NOT work with the hinged femurs, hinged tibial baseplates, or tibial stem adapters. Use only the collet screws that are packaged with the hinged femoral, hinged tibial, and tibial stem adapter components. Do not use the screw that is packaged with the stem.
19 Zimmer MOST Options System Surgical Technique 17 Component Implantation Implantation of the Metal-Backed Hinged Tibial Component Cement is applied to the tibial baseplate, keel and stem using a standard cementing technique. A cement restrictor may be used. Impact the tibial component and insert into place using the Tibial Insert/Baseplate Impactor and a mallet (Fig. 26). Remove any excess cement. Implantation of the All-Poly Tibial Sleeve Component Cement is applied to the undersurface of the All-Poly Tibial Sleeve and keel. A cement restrictor may be used. Impact the tibial component into place using the Tibial Insert/Baseplate Impactor and a mallet (Fig. 27). Remove any excess cement. Fig. 26 Hinged Tibia Tibial Insert Baseplate Impactor Hinged Tibia Insert Distal Femoral Replacement Tibial Insert Baseplate Impactor All-Poly Tibia Fig. 27
20 18 Zimmer MOST Options System Surgical Technique Implantation of the Femoral Component Cement is injected into the femoral canal. A cement restrictor may be used. Cement is also applied to the radius of the stem to ensure adequate cement coverage at the implant/bone interface. The component is impacted into place using the Femoral Impactor using a mallet (Fig. 28). Excess cement is removed. Femoral Impactor Implantation of the Patellar Component If the patella was selected for resurfacing, apply cement to the patellar bone and/or the All- Polyethylene Patellar Implant. The patellar implant is then pressed into place with the Patellar Inserter (Fig. 29). Remove any excess cement. Remove the inserter after the cement is hard. For additional information on patellar preparation, please refer to Appendix D (Page 73). Fig. 28 Bowed Stem Bead of Cement Patellar Inserter Medial Side Fig. 29
21 Zimmer MOST Options System Surgical Technique 19 Hinge Assembly There are two hinges in the MOST Options system. The 4mm hinge is used with the Metal-Backed Hinged Tibia and Proximal Tibia. The standard hinge is used only with the All-Poly Tibial Sleeve. Hinge Pin Bushings Poly Lock Pin 4mm Hinge 4mm Hinge Kit The 4mm Hinge Kit consists of 2 bushings, 1-4mm hinge, 1 hinge pin and 1 poly lock pin (Fig. 30a). Standard Hinge Kit The Standard Hinge Kit consists of 2 bushings, 1 hinge, 1 hinge pin and 1 poly lock pin (Fig. 30b). Fig. 30a Metal-Backed Hinged Tibia Distal Femoral Replacement Note: The 4mm hinge is not compatible with the All Poly Tibial Sleeve and the standard hinge is not compatible with the Metal-Backed Hinged Tibia or Proximal Tibia. Hinge Pin Bushings Poly Lock Pin Standard Hinge Hinge Components Assembly Once the appropriate hinge kit is selected and the cemented implants have set, follow the assembly steps below. Fig. 30b All-Poly Tibial Sleeve Slide the hinge into the hinged tibial insert. Assemble the two hinge bushings into the distal femoral holes via the interarticular slot and align the notches on the bushings anteriorly (Fig. 31). Use the tapered end of the Hinge Pin Aligner to position the bushings with the notches facing anteriorly (Fig. 32). Close-up of Bushing Hinge Pin Aligner Bushing Fig. 31 Fig. 32
22 20 Zimmer MOST Options System Surgical Technique Thread the hinge pin to the Hinge Pin Aligner (Fig. 33a) and slide the hinge pin into the distal femur holes and slightly rotate the Hinge Pin Aligner back and forth until the cross pinhole on the hinge pin is visible through the hinge hole (Fig. 33b). Insert the poly lock pin into the hole on the hinge. Push the poly lock pin with the insert side of the Pin Inserter/ Extractor (Fig. 34a) until the poly lock pin is fully seated into the cross pin hole (Fig. 34b). Hinge Pin Aligner Hinge Pin Cross Pinhole Hinge Hole Note: The poly lock pin can be removed by threading the extractor side of the Pin Inserter/Extractor onto it and pulling it anteriorly. The hinge pin may be removed after the poly lock pin is removed by pushing the hinge pin out with the tapered end of the Hinge Pin Aligner. Fig. 33 b a Patellar alignment and tracking may be best assessed with the tourniquet down. Perform additional lateral patellar retinacular releases if necessary. Pin Inserter/Extractor Poly Lock Pin a Fig. 34 b
23 Zimmer MOST Options System Surgical Technique 21 Proximal Tibial Replacement Proximal Tibial Replacement
24 22 Zimmer MOST Options System Surgical Technique Proximal Tibial Replacement Leg Length Measurement After exposure of the distal femur and proximal tibia has been achieved, the proposed resection levels are noted with the extremity extended in a reproducible position. Set the resection guide or scale to the resection level and mark a horizontal line with an osteotome, bovie or marker (Fig. 35). Implant Selection Determine the implant configuration to finalize the resection level. Select the connection/stem segment combination from Table 2 or 3 to determine the final resection level. Note: Each large taper connection adds one millimeter to the total length. (e.g., The safe margin for proximal tibial tumor removal is 145mm. Using a 30mm segment, porous adapter equals 146mm resection level.) Resection Level The intramedullary length of the 190mm straight stems is 155mm. Proximal Tibial Resection Resect the proximal tibia at or slightly proximal (i.e., 0.5mm to 1mm) to the marked resection level. The additional amount is to account for slightly oblique cuts and tibial resection planing. Note: To improve the swing phase of the patient s gait, some surgeons choose to slightly shorten the limb. Fig. 35
25 Zimmer MOST Options System Surgical Technique 23 Table 2 Proximal Tibial Resection with Porous Adapter and Segments Proximal Tibia Porous Adapter Hinge + 6mm Insert Segments Total Resection Length 85mm 19mm 10mm 0mm 115mm 85mm 19mm 10mm 30mm 146mm 85mm 19mm 10mm 42.5mm 158.5mm 85mm 19mm 10mm 55mm 171mm 85mm 19mm 10mm 67.5mm 183.5mm 85mm 19mm 10mm 80mm 196mm Hinge with Insert 85mm 19mm 10mm 55+30mm 202mm 85mm 19mm 10mm mm 214.5mm 85mm 19mm 10mm 105mm 221mm 85mm 19mm 10mm 80+30mm 227mm 85mm 19mm 10mm mm 239.5mm 85mm 19mm 10mm 130mm 246mm Proximal Tibia Porous Revision Stem Adapter Total Resection Length 85mm 19mm 10mm mm 252mm 85mm 19mm 10mm mm 264.5mm Note: Each large taper connection adds one millimeter to the total length. Table 3 Proximal Tibial Resection with Nonporous Adapter and Segments Proximal Tibia Nonporous Adapter Hinge + 6mm Insert Segments Total Resection Length 85mm 4mm 10mm 0mm 100mm Proximal Tibial Replacement 85mm 4mm 10mm 30mm 131mm 85mm 4mm 10mm 42.5mm 143.5mm 85mm 4mm 10mm 55mm 156mm 85mm 4mm 10mm 67.5mm 168.5mm 190mm Revision Stem 85mm 4mm 10mm 80mm 181mm 85mm 4mm 10mm 55+30mm 187mm 85mm 4mm 10mm mm 199.5mm 85mm 4mm 10mm 105mm 206mm 85mm 4mm 10mm 80+30mm 212mm 85mm 4mm 10mm mm 224.5mm 85mm 4mm 10mm 130mm 231mm Segments Not Shown 85mm 4mm 10mm mm 237mm 85mm 4mm 10mm mm 249.5mm Note: Each large taper connection adds one millimeter to the total length.
26 24 Zimmer MOST Options System Surgical Technique Tibial Preparation Straight Stem Preparation The 190mm straight stem options are shown in Tables 4 and 5. The overall I/M length of 190mm is based on the length of the stem and the tibial component. The intramedullary length of the stems is 155mm. Table 4 190mm Straight Smooth Stem Options Size I/M Length 9.5mm 11.5mm 13.5mm 15.5mm 17.5mm 190mm 155mm X X X X X Table 5 190mm Straight Fluted Stem Options Size I/M Length 10.5mm 11.5mm 12.5mm 13.5mm 14.5mm 16.5mm 18.5mm 190mm 155mm X X X X X X X The following are the acronyms used on the reamers. HF = Hinged Femur DF = Distal Femur T-Handle HT = Hinged Tibia PT = Proximal Tibia Planer When using a proximal tibial component with a straight stem, ream to the DF/PT mark on the reamer. Incrementally ream the tibial canal starting with the 9.5mm Femoral/Tibial Reamers using a T-handle with Zimmer adapter (Fig. 36). Ream until the DF/PT mark is flush with the resected bone and the reamer diameter contacts cortical bone. Femoral/Tibial Reamer DF/PT mark 190mm Trial Stem Planing the Tibial Bone Screw the appropriate 190mm trial stem selected to the planer (Fig. 37). Plane the resection using a power drill with a Zimmer adapter until cortical bone is smooth and even. Attaching the trial stem to the planer will ensure the hole depth is deep enough for the implants. A tommy bar or pin may be inserted in the cross hole to aid in trial stem removal after planing. Fig. 36 Fig. 37 Cross Hole
27 Zimmer MOST Options System Surgical Technique 25 Femoral Preparation Femoral Medullary Canal Preparation The femoral instrumentation of the MOST Options System is keyed off the intramedullary stem position. Open the femoral canal with the 8mm (5/16 ) drill bit just above the superior edge of the intercondylar notch (Fig. 38). 8mm (5/16 ) Drill Bit Incrementally ream the femoral canal starting with the 9.5mm Femoral/Tibial Reamers using a T-handle with Zimmer adapter (Fig. 39a). The depth of the hole is based on the straight stem selected. The depth marking on the reamer includes the amount of bone being resected (Fig. 39b). The markings on the reamers designate the type of implant being used and the stem length. Although blunt tips are on the reamers, hand reaming is recommended to prevent notching and perforation of the anterior femoral cortex. The following are the acronyms used on the reamers. Fig. 38 Proximal Tibial Replacement HF = Hinged Femur T-Handle DF = Distal Femur HT = Hinged Tibia PT = Proximal Tibia The reamers are marked as shown below. HF BOSS 75HF 75HT/125HF DF/PT 125HT/175HF 190HF (Only on the 16.5mm Reamer to prepare for the Hinged Femoral Boss) Note: The combined markings on the reamers indicate different overall lengths are equal if used with another component (75HT/125HF, hinged tibia with a 75mm stem = hinged femur with 125mm stem). Fig. 39a Fig. 39b
28 26 Zimmer MOST Options System Surgical Technique Similar to the tibial stem preparation, the diameter of the last reamer size used will correspond to the diameter of the stem trial to be used with the femoral instrumentation. The straight stem options are shown in Tables 6 and 7. For example, if a 14.5mm reamer was last used, then a 14.5mm stem trial will be used. The proper length stem trial is determined by using the length marked on the reamer. For proper seating of the femoral stem, the reamer should be flush with the distal surface of the femur for the length stem desired. The 75mm, 125mm, 175mm and 190mm straight stems are used on the system. The length marking on the implant label designates the overall composite length of the stems from the distal femoral cut. This length includes the 35mm length of the femoral boss (Fig. 39c). The actual intramedullary length of the stem is calculated as shown. 75mm stem -35mm boss (length of Hinged Femoral Boss) 40mm intramedullary length of stem* * This calculation will work on any of the stems used in the system. Size I/M Length of Stem This length should closely correspond to the preoperatively templated length. (If the femoral stem diameter is smaller than 16.5mm, the femoral canal will need to be reamed distally to accept the Femoral Component Stem Boss (Fig. 39b). This can be accomplished by reaming with the 16.5mm reamer to the depth marked HF BOSS. ) HF BOSS (35mm) 16.5mm Hinged Femur (HF) Note: When cementing straight stems, it should be noted that the stem trial diameter should be one size larger than the actual implant. Fig. 39c Table 6 Straight Smooth Stem Options Size I/M Length 9.5mm 10.5mm 11.5mm 12.5mm 13.5mm 14.5mm 15.5mm 16.5mm 17.5mm 18.5mm 75mm 40mm X X X X X 125mm 90mm X X X X X 190mm 155mm X X X X X Table 7 Straight Fluted Stem Options Size I/M Length 10.5mm 11.5mm 12.5mm 13.5mm 14.5mm 16.5mm 18.5mm 20.5mm 22.5mm 175mm 140mm X X X X X X 190mm 155mm X X X X X X X Note: Fluted 175mm and 190mm stems have an oversized diameter to allow for a 0.5mm press fit above trial size.
29 Zimmer MOST Options System Surgical Technique 27 Femoral Alignment and Distal Femoral Cut Thread the proper stem trial onto the 8mm (5/16 ) trial stem adapter and connect the quick disconnect handle. With the handle in the Open position, the 8mm trial stem adapter locks into place by clicking the handle manually to the Locked position. Insert the stem trial into the femoral canal until the HF (hinged femur) line on the adapter is flush with the distal femoral bone surface (Fig. 40). Remove the handle by clicking it to the open position and disconnecting it. Detachable Handle Trial Stem Adapter Trial Stem Make sure that the left/right bushing located on the Distal Femoral Alignment Guide is positioned correctly for the appropriate side. Attach the alignment guide and saw block assembly onto the stem trial located in the femoral canal. Ensure that the alignment guide is in contact with the distal femoral bone. Note: The threaded screws on the alignment guide should be dialed out so that they are not in contact with the distal femur surface. For revision cases where bone has been removed from the distal femur, use the Revision Distal Saw Block (Fig. 41). This assembly is designed to position the saw block for a 2mm distal femoral resection. The total distal thickness of the hinged femur is 20mm. The revision cut block has the ability to remove additional amounts of bone in 2mm increments to achieve the 20mm distal resection for the hinged femur (ex. 20mm resection - primary implant removed distal thickness 10mm - 2mm bone loss = 8mm resection). The guide would be set at the +6mm marks (2mm clean-up cut +6mm of additional bone). Align the Femoral Alignment Guide handles to approximate the rotation of the femur using the epicondyles as reference points (Fig. 42). This rotation should be as close as possible to the final position as only minor rotational adjustments may be possible in subsequent steps in the technique. Proximal Tibial Replacement Fig. 40 Primary Distal Saw Block Revision Distal Saw Block Assemble the Primary Distal Saw Block onto the Distal Femoral Alignment Guide (Fig. 41). These holes will position the saw block such that a 20mm distal femoral resection will be made. The total distal thickness of the hinged femur is 20mm. The Primary Cut Block has the ability to remove less bone (in 2mm increments) to achieve a change in joint line position by moving the Primary Saw Block (ex. 20mm resection -2mm = 18mm resection). Fig. 41 Fig. 42 Left/Right Bushing Distal Femoral Alignment Guide
30 28 Zimmer MOST Options System Surgical Technique An optional Extramedullary Alignment Tower and Alignment Rod can be placed on the Distal Primary Saw Block for an extramedullary check of the varus/valgus cut of the distal femur (Fig. 43). For proper alignment, this rod should point two-finger breadths medial to the anterior superior spine. Stabilize the Distal Femoral Alignment Guide by drilling and pinning through the threaded holes located on the medial and lateral side of the guide. Secure the Slotted Distal Femoral Primary Saw Block to the anterior cortex by drilling and pinning the two holes located on the Drill On Line scribed onto the block (Fig. 44). Once the Primary Saw Block is stabilized, remove the femoral alignment guide, the stem trial and adapter (Fig. 45). The distal cut can now be made using a 1.5mm saw blade along the slots in the Primary Saw Block. Note: For the MOST Options System, cutting blocks use a 1.5mm (.058 inch) thick saw blade. Fig. 43 Distal Femoral Alignment Guide Alignment Rod Distal Primary Saw Block Fig. 44 Fig. 45
31 Zimmer MOST Options System Surgical Technique 29 Femoral Sizing a Guide b c Trial Stem Adapter Correct Sizing Under Sized Over Sized Fig. 46 Femoral Sizing Reinsert the trial stem and trial stem adapter. Slide the Femoral Sizing Guide over the trial stem adapter. Size the femur by spinning the stylus marked Size 1, 2 or 3 until there is zero-tominimal gap between the sizing guide and the stylus boss (Fig. 46a). If there if is no gap between the anterior cortex and the stylus but a gap between the housing and the sizing guide, then the femoral implant is under sized (Fig. 46b). Stylus Proximal Tibial Replacement If there is a gap between the anterior cortex and the stylus, and no gap between the housing and sizing guide, then the femoral implant is over sized (Fig. 46c). There are secondary visual references for the medial/lateral and posterior sizing (Fig. 47). Fig. 47 M/L Sizing Size 1 Size 2 Size 3 Posterior Sizing Size 1 Size 2 Size 3
32 30 Zimmer MOST Options System Surgical Technique Slide the A/P Sizing Block over the stem trial adapter. Prior to pinning the Speed Block, verify that the size chosen is not going to significantly undercut the femur by placing a 1.5mm (.060 ) Miller guide (angel wing) through the anterior cut slot of the A/P Cutting Block (Fig. 48). Once the proper size Speed Block has been chosen, rotation of the Speed Block is established by locating the medial and lateral femoral epicondyles and aligning them so that they are parallel with the medial and lateral oblique pin holes on the Speed Block. This results in slight external rotation. No internal rotation of the Speed Blocks should be allowed. Fig. 48 A/P Sizing Block Stem Trial Adapter Miller Guide (angel wing) Note: The posterior condyles should not be the sole reference for orientation. When rotation has been determined, stabilize the Speed Block by using a 3.2mm (1/8 ) drill bit and then pinning the two oblique holes with headed pins (Fig. 49). Headed pins are recommended to prevent the pins from being recessed below the oblique holes upper surface. Fig. 49 The anterior and posterior cuts can now be made using the A/P Cutting Block. The posterior cut is made through the captured posterior angled slot (Fig. 50). Note: The size 3 A/P Cutting Block requires an anterior chamfer cut. To remove the A/P Cutting Block, pull both the medial and lateral headed pins. Remove the 8mm trial stem adapter and stem trial by attaching the Quick Disconnect Handle. 8mm Trial Stem Adapter Fig. 50
33 Zimmer MOST Options System Surgical Technique 31 Patella Preparation The decision to resurface the patella is a surgeon preference. Please refer to Appendix D (page 73). Trial Assembly Femoral Impactor Femoral Trial Assembly Attach the appropriate hinged femoral trial to the appropriate length and diameter trial stem. Impact the femoral trial onto the distal femur using the Femoral Impactor and a mallet and evaluate for fit (Fig. 51). Be sure that the posterior condyles engage posterior femoral bone to give rotational stability of the femoral implant. Tibial Impactor Fig. 51 Trial Stem Femoral Trial Adapter, Stem and Proximal Tibia Assembly Screw the appropriate trial stem to the appropriate trial stem adapter. Assemble any segments to the proximal tibial trial. Assemble the trial stem and adapter to the Proximal Tibial Trial. Insert the Proximal Tibial Trial assembly into the tibia using the Tibial Impactor and a mallet if needed (Fig. 52). Proximal Tibial Trial Trial Stem Adapter Trial Hinge Pin 4mm Trial Hinge Proximal Tibial Insert Trial Proximal Tibial Replacement Install the final thickness Proximal Tibial Insert Trial into the Proximal Tibial Trial. Then install the 4mm trial hinge into the tibial insert trial. Align the femoral trial with the hinge. The trial hinge pin is installed from either side on the leg (Fig. 53). The leg should be manipulated through the range of motion. Fig. 52 Trial Stem Fig. 53 Slaphammer Trial Removal Remove the hinged femoral trial by placing the slaphammer into the posterior slot of the hinged femoral trial (Fig. 54a). The porous and nonporous trials are also removed using the stem extractor and slap hammer (Fig. 54b). Remove the Proximal Tibial Insert Trial from the Trial Baseplate by using an osteotome and turning it slightly clockwise or counterclockwise (Fig. 55). Fig. 54a Slaphammer Fig. 54b Revision Adapter Trial Extractor Revision Adapter Trial Revision Stem Trial
34 32 Zimmer MOST Options System Surgical Technique Component Selection and Assembly When cementing a femoral stem, downsize at least one stem diameter (2mm) to allow for an adequate cement mantle. For example, if the 14.5mm reamer was the final reamer and the 14.5mm stem trial was used for instrumentation, then use the 12.5mm stem diameter and the proper length smooth stem for cementing. A plastic cement restrictor may be used to permit the cement to be manually pressurized. Fluted 175mm and 190mm revision stems are sized 0.5mm larger than the reamer/trial to enhance the fit within the canal. Fluted stems are numbered the same as the trials (for a 14.5mm trial, the stem is numbered 14.5mm, but has a true diameter (with fins) of 15mm). Note: If fluted stems are used, cement should not be allowed to contact the fluted portion of the stem. The femoral and tibial components are assembled prior to mixing the cement. The stem can be attached to the hinged femur by resting the femoral articulating surface on the Femoral Impacting Stand prior to impaction of the stem to the femur. Impact the femoral stem onto the Hinged Femur Boss Taper using the Revision Stem Impactor and a mallet (Fig. 56). The stem collet screw that is packaged with the hinged femur should be used to secure the stem to the Femoral Boss Taper. Tighten the screw from the articular side of the femoral intercondylar housing using the hex bit and handle (Fig. 57). When the screw tightens snugly, the stem has been properly retained. The self-capture feature may be tested by loosening the screw and backing out until a hard stop is detected. If the screw comes out without force, it has not engaged the self-capturing interface. Reinstall until the hard stop is detected when loosening the screw. Fig. 55 Fig. 57 Warning!: Screws that are packaged with the 75, 125, 175, 190, and 250mm revision stems will NOT work with the hinged femurs, hinged tibial baseplates, or tibial stem adapters. Use only the collet screws that are packaged with the hinged femoral, hinged tibial, and tibial stem adapter components. Do not use the screw that is packaged with the stem. Fig. 56 Screw packaged with Hinged Femur Hex Bit Handle
35 Zimmer MOST Options System Surgical Technique 33 Warning!: Screws that are packaged with the 75, 125, 175, 190, and 250mm revision stems will NOT work with the hinged femurs, hinged tibial baseplates, or tibial stem adapters. Use only the screws that are packaged with the hinged femoral, hinged tibial, and tibial stem adapter components. Do not use the screw that is packaged with the stem. Revision Stem Impactor Collet Screw packaged with Tibial Revision Stem Adapter Place the appropriate tibial stem adapter into the Adapter Impaction Stand. Impact the tibial stem onto the appropriate adapter using the same revision stem impactor as used with the femoral stem using a mallet (Fig. 58). Insert the collet screw that is provided with the tibial stem adapter into the adapter and tighten it using the hex bit and handle (Fig. 59). Note: The screw must be inserted before the adapter/stem is assembled to the proximal tibia because there is no access to install it afterwards. When the screw tightens snugly, the stem has been properly retained. If a segment is used, place the proximal tibia into the Tibial Stand. Impact the segment into the proximal tibia using the impacting plug (Fig. 60). Tibial Revision Stem Adapter Fig. 58 Fig. 59 Tibial Revision Stem Adapter Revision Stem Femoral Stem Impacting Sleeve Proximal Tibial Replacement Next, place the adapter/stem assembly into either the segment or proximal tibia and impact the adapter/stem using the Femoral Stem Impacting Sleeve and a mallet (Fig. 61). Impacting Plug Segment Proximal Tibia Segment Proximal Tibia Tibial Stand Fig. 60 Fig. 61
36 34 Zimmer MOST Options System Surgical Technique Component Implantation Implantation of the Distal Femoral Component Cement is applied to the hinged femur, femoral stem and canal. If fluted stems are used, cement should not be allowed to contact the fluted portion of the stem. The distal femur is impacted into place using the femoral impactor and a mallet (Fig. 62). Excess cement is removed. Femoral Impactor Implantation of the Tibial Component Cement is applied to the undersurface of the Tibial Revision Stem Adapter and tibial canal. Impact the proximal tibial component into place using the Tibial Insert/Baseplate Impactor and a mallet (Fig. 63a). Remove any excess cement. The polyethylene liner is inserted with the Tibial Insert/Baseplate Impactor and a mallet (Fig. 63b). Fig. 62 Tibial Insert/ Baseplate Impactor Implant Extraction The hinged femur and distal femur are removed using the femur distractor and slap hammer (Fig. 64). The porous and nonporous adapters are removed using the Revision Stem Extractor and slap hammer. Fig. 63a Fig. 63b Fig. 64
37 Zimmer MOST Options System Surgical Technique 35 Implantation of the Patellar Component If the patella was selected for resurfacing, apply cement to the patellar bone and/or the All Polyethylene Patellar Implant. The patellar implant is then pressed into place with the Patellar Inserter (Fig. 65). Remove any excess cement. Remove the inserter after the cement is hard. Please refer to Appendix D for additional information on patellar preparation. Medial Side Hinge Assembly Fig. 65 Hinge Components There are two hinges in the MOST Options system. The 4mm hinge is used with the Metal-Backed Hinge Tibia and the Proximal Tibia. The standard hinge is used only with the All-Poly Tibia Sleeve. The 4mm hinge is not compatible with the All-Poly Sleeve and the standard hinge is not compatible with the Metal Backed Hinged Tibia. The Proximal Tibia shown in Fig. 66 will only accept the 4mm hinge. 4mm Hinge Kit Proximal Tibial Replacement 4mm Hinge Kit The 4mm hinge kit consists of 2 bushings, 1-4mm hinge, 1 hinge pin and 1 poly lock pin (Fig. 66). Fig. 66
38 36 Zimmer MOST Options System Surgical Technique Once the cemented implants have set, slide the 4mm hinge into the proximal tibial insert. Assemble the two bushings into the hinged femoral holes via the interarticular slot and align the notches on the bushings anteriorly. Use the tapered end of the Hinge Pin aligner to position the bushings (Fig. 67). Hinge Pin Aligner Thread the hinge pin to the Hinge Pin Aligner (Fig. 68) and slide the hinge pin into the hinged femoral holes until the cross pinhole on the hinge pin is visible through the hinge hole (Fig. 68 inset). The Hinge Pin Aligner may need to be rotated back and forth to fully seat the hinge pin. Fig. 67 Bushings Notch Insert the poly lock pin into the hole on the hinge and push the poly lock pin with the insert (smooth) side of the pin insert/extractor (Fig. 69) until the poly lock pin is fully seated into the cross pinhole (Fig. 69 inset). Note: The poly lock pin can be removed by threading the extractor side of the Pin Inserter/Extractor onto it and pulling it anteriorly. The hinge pin may be removed after the poly lock pin is removed by pushing the hinge pin out with the tapered end of the Hinge Pin Aligner. Fig. 68 Hinge Pin Aligner Hinge Pin Cross Pin Hole Hinge Hole Patellar alignment and tracking may be best assessed with the tourniquet down. Pin Inserter/Extractor Fig. 69
39 Zimmer MOST Options System Surgical Technique 37 Proximal Femoral Replacement Proximal Femoral Replacement
40 38 Zimmer MOST Options System Surgical Technique Proximal Femoral Replacement Proximal Femoral Options There are two proximal femoral options available: the Basic Proximal Femur (Fig. 70) and the Proximal Femur with Tissue Attachments (Fig. 71). Basic Proximal Femur The Basic Proximal Femur is used for attachment of soft tissue when the trochanteric bone cannot be salvaged. The soft tissues are sutured through the holes of the proximal femur for temporary fixation during the healing process. The Basic Femur is preferred because of its smooth profile which may reduce the chance of developing trochanteric bursitis. If trochanteric bone can be salvaged, use of the Proximal Femur with Tissue Attachments may be considered. For possible improved function of the abductors, attach them by the strongest possible means to the remaining lateral soft tissues, i.e., iliotibial band. Optimal candidates for this method of fixation are those in whom a resection can be performed with sacrifice of not more than 1cm of native abductor tendon. Sacrifice of more than this amount of abductor tendon may leave the abductor mechanism with insufficient tendon for fixation using the pronged washers. Restriction of post operative rehabilitation activity and or bracing should be individualized for each case to prevent dislocation. Fig. 70 Fig. 71 Proximal Femur with Tissue Attachments
41 Zimmer MOST Options System Surgical Technique 39 Femoral Measurement and Resection Use the Proximal Femoral Ruler (Fig. 72) and the 50cm scale to mark the appropriate segment length distal to the preoperatively determined femoral resection level as well as rotational alignment (Fig. 73). Proximal Femoral Ruler The minimum resection required to implant either type of proximal femur component is 111mm. Fig. 72 Basic Femur 80mm Bowed Stem 111mm 50cm Scale Proximal Femoral Replacement Fig. 73
42 40 Zimmer MOST Options System Surgical Technique Implant Selection Determine the implant configuration to finalize the resection level. Select the proper segment from Table 8 to determine the final resection level. (Example: If the safe margin for proximal femoral tumor removal is 140mm, use a 30mm segment and a bowed stem to obtain a 142mm resection level.) Note: Each large taper connection between components adds 1mm to the total length. The intramedullary length of the bowed stems is 152mm. Using a neutral offset head, segment lengths correspond to resection lengths in the table shown. Set the resection guide to the final resection level and mark the proximal femur. Resect the proximal femur slightly proximal (i.e., 0.5mm to 1mm) to the marked level. The additional amount is to account for slightly oblique cuts and femoral resection planing. Note: To improve the swing phase of the patient s gait, some surgeons choose to slightly shorten the limb. Table 8 Proximal Femoral Resection with Bowed Stems with Segments Proximal Femur Bowed Stem Segments Total Length 80mm 30mm 0mm 111mm 80mm 30mm 30mm 142mm 80mm 30mm 42.5mm 154.5mm 80mm 30mm 55mm 167mm 80mm 30mm 67.5mm 179.5mm 80mm 30mm 80mm 192mm 80mm 30mm 55+30mm 198mm 80mm 30mm mm 210.5mm 80mm 30mm 105mm 217mm 80mm 30mm 80+30mm 223mm 80mm 30mm mm 235.5mm 80mm 30mm 130mm 242mm 80mm 30mm mm 248mm 80mm 30mm mm 260.5mm 80mm 30mm 155mm 267mm 80mm 30mm mm 273mm 80mm 30mm mm 285.5mm 80mm 30mm mm 298mm Note: Each large taper connection adds one millimeter to the total length.
43 Zimmer MOST Options System Surgical Technique 41 Femoral Canal Preparation Flexibly ream the femoral canal until cortical bone through the isthmus is reached. (The flexible reamers are not part of the MOST Options instrument system but are usually available through the hospital). The intermedullary length of stems is 152mm. Ream to a depth greater than 152mm to allow proper seating of stem shoulder on cortical bone. Recommended reamer diameters are as follows: Planer Pilot Planer Stem Size 12mm 14mm 16mm Cemented Hex Stem Ream Diameter 13mm to 14mm 15mm to 16mm 17mm to 18mm Fluted Stem Ream Diameter 12mm 14mm 16mm Note: The hex bowed stems are tapered 2mm distally. The fluted bowed stems are sized 0.5mm larger than the reamed hole diameter to enhance the fit within the canal. Planing the Femoral Bone Screw the appropriate-sized pilot for the stem diameter selected (12mm, 14mm or 16mm) to the planer (Fig. 74). Plane the resection using a power drill with a Zimmer adapter until cortical bone is smooth and even. A pin may be inserted in the cross hole to aid in pilot removal after planing. Fig. 74 Proximal Femoral Replacement
44 42 Zimmer MOST Options System Surgical Technique Trial Assembly Attach the appropriate proximal femur to the bowed stem. The bowed stem trial has an anterior mark to insure proper orientation. The fluted bowed stems use the hex trial stems. Insert the femoral trial assembly into the femoral canal and evaluate for fit (Fig. 75). When using a bowed stem, mark the anterior femoral bone in line with the mark on the bowed stem trial to ensure proper orientation of the implant. Place the femoral component in approximately 0-20 degrees of anteversion. Check stability while externally rotating the limb. Support the reconstruction with nonabsorbable suture if needed. Note: Consider decreasing the amount of anteversion to reduce risk of anterior dislocation. Use caution not to over-lengthen the reconstruction in order to achieve longitudinal stability. Trial Reduction Firmly assemble the appropriate trials together by hand. It is not necessary to impact the trials together. The trial heads are selected as follows; 26mm, 28mm and 32mm options (-4mm, neutral, +4mm and +8mm necks). Prepare the acetabulum as needed for a Converge, Bipolar or Unipolar acetabular component. If the acetabulum is normal, a bipolar head is suggested for stability. Perform the trial reduction. If leg length, alignment, range of motion and stability are acceptable, proceed with the next step. If the joint is tight at full extension or during push-pull, try a shorter offset head trial or recheck the cuts and remove bone from the femur as necessary. If the joint is loose at full extension or during push-pull, try the longer offset head trial or recheck cuts and try the next length segment trial. An option of a shorter neck but longer stem (medialize) may decrease apparent abduction weakness. Fig. 75
45 Zimmer MOST Options System Surgical Technique 43 Bowed Stem Implant Assembly Assemble the selected segment to the Basic Proximal Femur using the Impacting Stand (or the Proximal Femur with Tissue Attachments using the Proximal Femur with Attachment Impacting Stand) and the Impactor Plug (Fig. 76). Use a mallet to firmly tap the tapers to the seated position. Using the impaction sleeve, assemble the hex I/M stem or the I/M fluted stem to the proximal components, while still in the Proximal Femur Impacting Stand (Fig. 77). Ensure that the stem tip extends anatomically posteriorly with respect to the proximal femur. Then, firmly tap the taper to the seated position with a mallet and the Stem Impacting Sleeve. Impactor Plug Impaction Sleeve Segment Basic Proximal Femur Proximal Femoral Replacement Impacting Stand Fig. 76 Fig. 77
46 44 Zimmer MOST Options System Surgical Technique Implantation of the Femoral Component Cement the femoral assembly into the femur using a standard cementing technique (Fig. 78). A cement restrictor may be used. Cement is injected into the femoral canal. Cement is also applied to the radius of the stem to ensure adequate cement coverage at the implant/bone interface. The component is impacted into place using the femoral impactor and a mallet. Excess cement is removed. Implantation of hex stems should be guided by the anterior bow. A trial head is assembled to the proximal femur and a mallet is used to lightly tap the implant in using the head impaction instrument if needed. Assemble the chosen head using a femoral head impactor. Bowed Stem Bead of Cement The surgeon will choose a standard closure technique. Secure all remaining abductors to the lateral fascia to help restore hip abduction. Fig. 78
47 Zimmer MOST Options System Surgical Technique 45 Reattachment of the Greater Trochanter First, advance the bone over the lateral surface of the Proximal Femoral Implant with Tissue Attachment with the limb positioned in 30 degrees of abduction to optimize the resting tension in the abductor mechanism. The bone is over the distal hole and the muscle tissue is over the two proximal holes. Mark the approximate position of the distal hole on the bone and drill with a 1/4 inch drill from the inside (implant side) out (tissue side). The first bolt/washer combination, generally a short (5mm) washer and a long bolt (20mm), can now be placed against the bone and into the distal hole under direct vision. The hex driver is used to advance the washer until the tips of the prongs are firmly embedded in the bone. This limits the prominence of the fixation to 2mm to 3mm above the native cortex. Fig. 79 Once the first bolt/washer couple has been placed, the square hole of the Proximal Femur Attachment Template can be placed over the square washer to guide the next two bolt/washer couple placement (Fig. 79). After making a longitudinal incision through the middle of one of the square holes, a Kelly Hemostat can be used to spread the tissue so that the next combination can be placed under direct vision. The hex driver is used to advance the washer until the tips of the prongs are firmly compressed into the textured surface. Proximal Femoral Replacement The final bolt/washer (if required) can be placed in a similar fashion. This placement through the soft tissue provides a shear stop for the combination placed through the greater trochanter and prevents weakening of the trochanter with multiple holes.
48 46 Zimmer MOST Options System Surgical Technique Reattachment of the Abductor Tendon (Optional Technique) Fixation of soft tissue is performed using short (13.5mm) or long (20mm) bolts and either short-prong (5mm) or long-prong (9mm) washers, depending on the thickness of the soft tissue. Advance the abductor tendon and available gluteus medius over the lateral surface of the proximal femoral component using sutures in the provided suture holes or a towel clip. The limb should be positioned in 30 degrees of abduction to optimize the resting tension in the abductor mechanism. Make a longitudinal incision over the distal hole and spread the tissue using a Kelly Hemostat so that the first bolt/washer combination can be placed under direct vision. The hex driver is used to advance the washer until the tips of the prongs are firmly compressed into the textured surface. Note: This design traps soft tissue securely against the textured surface while preventing the crushing and limiting associated devascularization of tissue. Secure fixation of the washer tips into the textured surface enhances fixation by broadening the bending moment on the bolt. This also serves to limit motion of metallic components against one another and should limit generation of debris at this site. Notches between the spikes of the bolts are widened and smoothed to allow the maximum tissue volume to be trapped and to limit the risk of shearing soft tissue on sharp metal edges. Once the first bolt/washer couple has been placed, the square hole of the proximal femoral attachment template can be placed over the square washer to guide the next bolt-washer couple placement. The next bolt/washer combination can be placed in a similar fashion to the first. If the bolts/washers are unable to advance fully (i.e., the washer prongs are not firmly compressed or the bolt is not snug in the washer) the combination should be removed, even if it feels tight. The thread sights should be cleaned and extra care should be taken to avoid clogging the threads with tissue in advancing the bolt on the next try. Backout may occur if the combination is not advanced properly. Use the standard closure technique.
49 Zimmer MOST Options System Surgical Technique 47 Total Femoral Replacement Total Femoral Replacement
50 48 Zimmer MOST Options System Surgical Technique Total Femoral Replacement Implant Configuration In the event that a Total Femur is required, the procedure for doing a Proximal Femur and a Distal Femur is essentially combined. The suggested procedures take place after a routine approach has been performed for opening and exposing the acetabulum, femur and proximal tibia. It is critical that leg length be checked and noted prior to any bone resection. Care should be taken during the reconstruction to avoid stretch injury to the neurovascular structures. Determine the implant configuration based on the bone replacement requirements. Refer to Table 9. Note: Each large taper connection adds one millimeter to total length. Proximal Femur Total Segment (200mm) Segment Distal Femur Table 9 Total Femur with Segments Proximal Femur Distal Femur Segments Total Length 80mm 65mm 200mm 347mm 80mm 65mm mm 378mm 80mm 65mm mm 390.5mm 80mm 65mm mm 403mm 80mm 65mm mm 415.5mm 80mm 65mm mm 428mm 80mm 65mm mm 434mm 80mm 65mm mm 446.5mm 80mm 65mm mm 453mm 80mm 65mm mm 459mm 80mm 65mm mm 471.5mm 80mm 65mm mm 478mm 80mm 65mm mm 484mm 80mm 65mm mm 496.5mm 80mm 65mm mm 503mm 80mm 65mm mm 509mm 80mm 65mm mm 521.5mm 80mm 65mm mm 534mm 80mm 65mm mm 546.5mm Note: Each large taper connection adds one millimeter to the total length.
51 Zimmer MOST Options System Surgical Technique 49 Tibial Preparation There are four surgical options for tibial preparation: 1 Extramedullary Tibial Option, which uses a metal-backed hinged tibia without a long stem (Page 7), 2 Extramedullary Tibial Option, which uses an all-poly tibial sleeve (See Appendix A, page 56), Proximal Femur Total Segment (200mm) 3 Intramedullary Tibial Option, which uses the metal-backed tibia without a stem (See Appendix B, page 60), and 4 Intramedullary Tibial Option, which uses a metal-backed tibia with a long stem (See Appendix C, page 67). Trial Reduction The Metal-Backed Hinged Tibial Trial uses the 4mm trial hinge. The All- Poly Tibia Sleeve uses the standard trial hinge. The 4mm trial hinge and the standard trial hinge are not interchangeable. The total femoral segment has two tab orientations at the proximal portion. These are left/right specific and provide 15 of anteversion for the proximal femur. Distal Femur 4mm MOST Options Hinge Kit Segment MOST Hinge Kit Hinged Tibia Inserts Hinged Tibia Tibial Spacers All-Poly Tibia Sleeve Total Femoral Replacement Fig. 80
52 50 Zimmer MOST Options System Surgical Technique Component Implantation Implantation of the Metal- Backed Hinged Tibial Component Cement is applied to the undersurface of the tibial baseplate, keel and stem. Impact the tibial component and insert into place using the Tibial Insert/ Baseplate Impactor and a mallet (Fig. 81). Remove any excess cement. Implantation of the All-Poly Tibial Sleeve Component Cement is applied to the undersurface of the All-Poly Tibial Sleeve and stem. Impact the tibial component into place using the Tibial Insert/Baseplate Impactor and a mallet (Fig. 82). Remove any excess cement. Fig. 81 Tibial Insert Baseplate Impactor Hinged Tibia Insert Hinged Tibia Tibial Insert Baseplate Impactor All-Poly Tibial Sleeve Fig. 82
53 Zimmer MOST Options System Surgical Technique 51 Implant Assembly Assemble the porous or nonporous Total Femoral Segment to the Basic Proximal Femur using the Basic Proximal Femoral Impacting Stand (or the Proximal Femur with Tissue Attachments using the Proximal Femur with Attachment Impacting Stand), and impacting plug (Fig. 83). The Proximal Femur should be assembled and anteverted appropriately for a left or right in accordance with the patient s affected side. Use a mallet to firmly tap the tapers to the seated position. If segments are needed, the segment can be attached to the distal femur by resting the femur-articulating surface on the Femoral Impacting Stand prior to impaction of the segment into the distal femur using the Femoral Impacting Plug and a mallet (Fig. 84). Femoral Impacting Plug Total Segment Segment Note: The femoral and tibial components are assembled prior to mixing the cement. The distal femur and selected segments are placed in the Femoral Impacting Stand and then the selected Total Femoral Segment and the Basic Proximal Femoral Component are placed into the segment and impacted together using the Proximal Femoral Stand (Fig. 85). Fig. 83 Basic Proximal Femur Impacting Stand Distal Femur Femoral Impacting Stand Fig. 84 Total Femoral Replacement Fig. 85
54 52 Zimmer MOST Options System Surgical Technique Hinge Assembly There are two hinges in the MOST Options system. The 4mm hinge is used only with the Metal-Backed Hinged Tibia and Proximal Tibia. The standard hinge is used only with the All-Poly Tibial Sleeve. 4mm Hinge Kit The 4mm hinge kit consists of 2 bushings, 1-4mm hinge, 1 hinge pin and 1 poly lock pin (Fig. 86a). Standard Hinge Kit The standard hinge kit consists of 2 bushings, 1 hinge, 1 hinge pin and 1 poly lock pin (Fig. 86b). Note: The 4mm hinge is not compatible with the All-Poly Tibial Sleeve and the standard hinge is not compatible with the metal-backed hinged tibia. Hinge Components Assembly Once the appropriate hinge kit is selected and the cemented implants have cured, follow the assembly steps below. Slide the hinge into the hinged tibial insert. Assemble the two hinge bushings into the distal femoral holes via the interarticular slot and align the notches on the bushings anteriorly (Fig. 87). Use the tapered end of the Hinge Pin Aligner to position the bushings with the notches facing anteriorly (Fig. 88). Hinge Pin Fig. 86a Hinge Pin Fig. 86b Bushings Poly Lock Pin 4mm Hinge Metal-Backed Hinged Tibia Bushings Poly Lock Pin Standard Hinge All-Poly Tibial Sleeve Close-up of Bushing Hinge Pin Aligner Bushing Fig. 87 Fig. 88
55 Zimmer MOST Options System Surgical Technique 53 Thread the hinge pin to the Hinge Pin Aligner (Fig. 89a) and slide the hinge pin into the distal femur holes and slightly rotate the Hinge Pin Aligner back and forth until the cross pinhole on the hinge pin is visible through the hinge hole (Fig. 89b). Insert the poly lock pin into the hole on the hinge. Push the poly lock pin with the insert side of the Pin Inserter/ Extractor (Fig. 90a) until the poly lock pin is fully seated into the cross pin hole (Fig. 90b). Hinge Pin Aligner Hinge Pin Cross Pinhole Hinge Hole Note: The poly lock pin can be removed by threading the extractor side of the Pin Inserter/Extractor onto it and pulling it anteriorly. The hinge pin may be removed after the poly lock pin is removed by pushing the hinge pin out with the tapered end of the Hinge Pin Aligner. Fig. 89 b a Patellar alignment and tracking may be best assessed with the tourniquet down. Perform additional lateral patellar retinacular releases if necessary. Concentrate on a complete closure of the fascia, especially over the proximal tibia. If elevation of the proximal tibial crest and tubercle has been done, this is reattached with wires or a #5 nonabsorbable suture through drill holes into the tibia and fragment. Pin Inserter/Extractor a Poly Lock Pin Total Femoral Replacement Fig. 90 b
56 54 Zimmer MOST Options System Surgical Technique Component Disassembly In the event that the components need to be disassembled, two taper distractors have been provided. Either distractor may be used to disassemble the components. Place the Taper Distractor Jaws between the tab and slot of the mating components with the curvature of the jaws facing the curved slot and the flat of the jaws facing the tab; firmly rotate (Fig. 91). Alternatively, the Wedge Stem Distractor may also be used on any of the MOST Options components connected by taper interfaces (Fig. 92). Note: A surgical implant should not be reused under any circumstances. Once implanted and subsequently removed, an implant should be discarded. Even though the implant appears undamaged, it may have small defects and internal stresses that may lead to failure. Fig. 91 Warning: When using the MOST Options Wedge Stem Distractor, be sure to fully engage the instrument into the implants to be separated prior to the application of impaction force. This instrument MUST be aligned perpendicular to the implants to be separated. The impaction should be parallel to the long axis of the distractor. Any force off this axis would cause a levering affect which could lead to breakage. Warning: The MOST Options Distractor must never be used as a lever or pry device to separate implants. The distractor is only intended to be used in the manner shown in Fig. 92. Use of the MOST Options Distractor as a lever or a pry device may result in fracture of the mating geometry of the instrument and potentially metal debris at the surgical site. Wedge Stem Distractor Note: The Wedge Stem Distractor is only intended to be used in the manner shown in Fig. 92. Any application of force in a direction transverse to the instrument could result in fracture of the mating geometry of the instrument and potentially metal debris at the surgical site. Fig. 92
57 Zimmer MOST Options System Surgical Technique 55 Limb Lengthening If a patient requires limb lengthening, the surgeon may choose to remove a femoral segment by use of the distraction instrument and replace it with the next size larger femoral segment. Note: Attention must be given to soft tissue release at the time of limb lengthening. Total Femoral Replacement Fig. 94
58 56 Zimmer MOST Options System Surgical Technique Appendix A Extramedullary Tibial Option All-poly tibial sleeve The Extramedullary Tibial Alignment Guide assembly consists of the extramedullary guide, Tibial Saw Guide and 2mm, 10mm or 15mm Tibial Stylus. Select the appropriate Tibial Stylus based on the amount of bone requiring resection on the tibia. Adjust the extramedullary guide assembly to the approximate tibial length. Tap the longest pin of the guide into the central portion of the proximal tibia (Fig. 95). This fixes the guide to the tibia but allows for rotation until the second pin is impacted. Fig. 95 Mallet Extramedullary Guide Tibial Saw Guide Rotational Alignment Rotation is selected based on the anterior crest of the tibia and the bimalleolar axis. Make sure the guide is parallel to the crest of the tibia in the anterior/posterior and medial/lateral planes. The bottom nut on the ankle cradle should be positioned to maintain a zero degree tibial slope (Fig. 96). The anterior tibial plateau should be aligned parallel with the cutting block (Fig. 97). Rotation is then locked in place by impacting the second pin into the tibia. Fig. 96 Extramedullary Alignment Guide Bottom Nut Parallel Fig. 97
59 Zimmer MOST Options System Surgical Technique 57 Zero Degree Tibial Slope A zero degree tibial cut is recommended to accommodate the cone of the hinged tibial baseplate into the tibia. The instruments are preset to provide a zero degree tibial cut. No adjustment is needed. Tibial Stylus Appendix A Level of Resection Use the 10mm Tibial Stylus to determine the Tibial Saw Guide position for minimal resection of the proximal tibia (Fig. 98). The tip of the stylus is placed on the lower side. The total thickness of the 9mm All-Poly Tibial Sleeve and standard hinge (6mm) is 15mm. The stylus will position the tibial saw guide 10mm below the point of reference. If additional bone needs to be resected, the Tibia Saw Guide could be moved in 2mm increments (Ex. 10mm + 2mm =12mm). Note: A 10mm resection will raise the joint line approximately 5mm. There is a 15mm tibial stylus in the system that may be used to obtain a 15mm tibial resection if raising the joint line is not desired. Fig. 98 Tibial Saw Guide The cutting guide is then stabilized by drilling and pinning through the two outer most holes on the DRILL ON LINE (Fig. 99). This allows for 2mm of adjustment proximally and 4mm distally. The lateral drill point is first placed after retracting the patellar tendon, followed by the medial drill point. If the medial drill point appears to walk, this can be easily avoided by marking the entry point through the block, then drilling outside the block to pierce the cortex. Redrill the hole through the block. Fig. 99 Knurled Nut
60 58 Zimmer MOST Options System Surgical Technique Disassemble the jig by removing the stylus and extramedullary alignment guide using a slaphammer (Fig. 100). Place the alignment rod on the zero degree tibial alignment guide. The rod should pass through the center to no more than a few millimeters lateral to the center of the ankle. Cutting the Proximal Tibia A Miller guide (angel wing) can be placed on the tibial saw guide along the medial and lateral edge of the tibia to confirm the level of desired tibial resection. Place the saw capture on the tibial saw guide. If it appears that an inadequate resection will occur, adjust the tibial saw guide in 2mm increments to a lower level. Angled retractors are used to protect soft tissue and ligaments. Cut the proximal tibia with the appropriate saw blade for the saw guide (Fig. 101). Stylus Slaphammer Note: Saw blades especially designed for this system are recommended. The blades are 1 inch wide with a shank thickness of and will best match the saw guide. Fig. 100 Fig. 101
61 Zimmer MOST Options System Surgical Technique 59 Proximal Tibial Sizing and Drilling To avoid soft tissue impingement, select the appropriate size Tibial Baseplate Sizer/Reamer Guide that best fills but does not overhang the proximal tibia. The medial/central hole is drilled and filled. Final rotational alignment is referenced off the tibial tubercle with the handle of the guide in the medial one-third of the tubercle. It is then stabilized with four pins as the holes are drilled using the 3.2mm (1/8 inch) by 5 inch drill bit. Check the alignment of the tibial cut with the Axial Alignment Rod through the handle of the Baseplate Sizer/ Reamer Guide (Fig. 102).The tibial profile dimensions correspond to the following A/P and M/L dimensions. Fig. 102 Baseplate Sizer/ Reamer Guide Axial Alignment Rod Appendix A Tibial Size A/P M/L 1 46mm 65mm 2 48mm 71mm 3 51mm 77mm 4 54mm 83mm Tibial Stem Preparation and Tibial Trial Insertion Using the appropriate tibial sizing template, ream with the tibial reamer and guide assembly using a power drill with Zimmer adapter (Fig. 103); broach the proximal tibial canal with the tibial broach and cage assembly (Fig. 104). Note: Both reamer and broach need to be fully seated for correct tibial preparation. If resistance is met, remove and inspect for cortical thinning or perforation. For hinge selection and trial assembly, please refer to page 13. Tibial Reamer and Guide Assembly Fig. 103 Fig. 104 Tibial Broach and Cage Assembly
62 60 Zimmer MOST Options System Surgical Technique Appendix B Intramedullary Tibial Option Metal backed tibia without a stem Tibial Medullary Canal Preparation Direct vertical exposure of the tibial plateau is necessary. This is facilitated by soft tissue releases around the tibial metaphysis, medial and lateral soft tissue retraction with the small angled knee retractors and subluxation of the tibia anteriorly with the large angled knee retractor. Fig. 105 The reference hole should be centered from medial to lateral. Anterior/ posterior positioning should fall between the middle and anterior one-third of the tibial plateau (Fig. 105). Placement of the intramedullary guide or I/M rod is accomplished by first drilling a 8mm (5/16 ) hole in the proximal tibia (Fig. 106). 8mm (5/16 ) Drill Bit Fig. 106
63 Zimmer MOST Options System Surgical Technique 61 Intramedullary Tibial Option 2 only Reference Hole While Using a 8mm I/M Rod Attach the 8mm (5/16 ) I/M rod to the Quick Disconnect Handle. With the handle in the Open position, the 8mm adapter is locked into place by clicking the handle manually to the Locked position. Detachable Handle Slowly insert the I/M rod into the tibial canal (Fig. 107). Remove the handle by clicking it to the open position and disconnecting it. Tibial Alignment and Proximal Tibia Cuts Connect the fixed zero degree intramedullary alignment guide to the slotted tibial cut guide with a 10mm single ended stylus (Fig. 108 on the following page). The zero degree guide is then placed onto the 8mm (5/16 ) trial stem adapter located in the tibial canal. If no bone is present on which to rest the 10mm stylus, the thumbscrew located on the fixed zero degree intramedullary alignment guide is used to secure the stylus tip by touching the least involved portion of the tibial plateau. Fig mm I/M Rod Appendix B
64 62 Zimmer MOST Options System Surgical Technique Rotational Alignment Rotation is selected based on any remaining landmarks. The most reliable landmark will be the tibial tubercle. For proper internal/external rotation, the center of the saw block should be positioned directly over the medial onethird of the tibial tubercle (not medial to the tubercle). It can be helpful to mark this medial one-third of the tubercle with a longitudinal methylene blue line. Extramedullary confirmation of the internal/external rotation can also be achieved by using an alignment rod placed through the outer hole of the alignment guide. The external guide rod should align with the tibial tubercle or at the ankle over the anterior tibialis tendon (Fig. 108). Ideally, both references should be used. Rotation is then locked in place by impacting the set pin with a mallet. Zero Degree Alignment Guide Tibial Stylus Tibial Saw Block Zero Degree Tibia Slope A zero degree tibial cut is recommended to accommodate the cone of the hinged tibial baseplate into the tibia. The instruments are preset to provide a zero degree tibia cut. Fig. 108
65 Zimmer MOST Options System Surgical Technique 63 Level of Resection The 10mm Tibial Stylus is used to determine the tibial saw guide position for minimal resection of the proximal tibia. The stylus will position the tibial saw guide 10mm below the point of reference. The tip of the stylus is placed on the lower side. Note: A 10mm resection will raise the joint line approximately 5mm. There is a 15mm Tibial Stylus in the system that may be used to obtain a 15mm tibial resection. Stabilize the cutting guide by drilling and pinning through the two outer most holes on the DRILL ON LINE (Fig. 109). This allows for 2mm adjustment proximally and 4mm distally. The lateral drill point is first placed after retracting the patellar tendon, followed by the medial drill point. If the medial drill point appears to walk, this can be easily avoided by marking the entry point through the block, then drilling outside the block to pierce the cortex. Redrill the hole through the block. To recheck alignment, place the alignment rod on the zero degree tibial alignment guide to confirm the correct rotational position. The rod should pass through the center to no more than a few millimeters lateral to the center of the ankle (Fig. 110). Remove the tibial alignment guide, alignment rod and I/M rod from the tibial canal. Fig. 109 Appendix B Cutting the Proximal Tibia A Miller guide (angel wing) can be placed on the tibial saw guide along the medial and lateral edge of the tibia to confirm the level of desired tibial resection. If it appears that an inadequate resection will occur, adjust the tibial saw guide in 2mm increments to a lower level. Angled retractors are used to protect soft tissue and ligaments. Fig. 110
66 64 Zimmer MOST Options System Surgical Technique Cut the proximal tibia with the appropriate saw blade for the saw guide (Fig. 111). Note: Saw blades especially designed for this system are recommended. The blades are 25mm (1 ) wide by 90mm (3.5 ) long with a shank thickness of 1.5mm (0.058 ) and will best match the saw guide. Disassemble the jig by removing the stylus and trial stem adapter. A slaphammer may be placed under the body of the guide to aid in removal of the trial stem adapter and jig, leaving the saw guide fixed to the anterior face of the tibia. Fig. 111 Proximal Tibial Cone Preparation Attach the Baseplate Sizing Bushing to the Tibial Baseplate Sizer/Reamer Guide by turning it in the direction of the arrow on the baseplate sizer/ reamer guide. Attach the 11mm tibial starter drill to a power tool and place it through the Baseplate Sizing Bushing (Fig. 112). If resistance is encountered, remove the drill and inspect the proximal tibia for cortical thinning or perforation. The correct depth is established when the nose of the power tool touches the top of the baseplate sizing bushing. Remove the bushing by turning it in the opposite direction of the arrow on the Baseplate Sizer/Reamer Guide. Tibial Starter Drill Baseplate Sizing Bushing Fig. 112
67 Zimmer MOST Options System Surgical Technique 65 Assemble the Primary Cone Reamer to the Cone Reamer Guide (Fig. 113). The cone reamer guide assembly is attached to a power tool with a Zimmer quick disconnect fitting and then assembled to the Baseplate Sizer/ Reamer Guide with a slight turn in the direction of the arrow on the Tibial/ Sizing Reamer Guide. The Baseplate Sizer/Reamer Guide must be clear of all bone materials, etc. before the cone reamer guide is assembled. Ream the tibial cone until the nose of the power tool touches the top of the Cone Reamer Guide (Fig. 114). Remove the reamer guide from the Baseplate Sizer/Reamer Guide by a slight turn in the opposite direction of the arrow on the Tibial/Sizing Reamer Guide. Note: Care needs to be taken to insure the position of the cone reamer in the proximal tibia. If the cone reamer is angled into the tibia in the A/P or M/L planes, the tibial cone may not fully seat or the tibial cortex may be compromised. Fig. 113 Primary Cone Reamer Guide Primary Cone Reamer Appendix B Fig. 114
68 66 Zimmer MOST Options System Surgical Technique Tibial Keel Preparation and Tibial Trial Insertion Once the appropriate size tibia has been selected, the Hinged Tibial Trial and trial stem are assembled and then inserted into the tibia. Rotate the Hinged Tibial Trial to the proper position. The keel broach and modular handle are assembled and inserted into the Hinged Tibial Trial. The modular handle of the keel broach is gently impacted until it is fully seated using a mallet (Fig. 115a). Remove the modular handle from the Hinged Tibial Trial (Fig. 115b). Attention at this point is directed to the femoral preparation. Modular Handle Fig. 115 a b Hinged Tibial Trial
69 Zimmer MOST Options System Surgical Technique 67 Appendix C Intramedullary Tibial Option Metal-backed tibia with a long stem Tibial Preparation Tibial Medullary Canal Preparation Direct vertical exposure of the tibial plateau is necessary. This is facilitated by soft tissue releases around the tibial metaphysis, medial and lateral soft tissue retraction with the small angled knee retractors and subluxation of the tibia anteriorly with the large angled knee retractor. Fig. 116 The reference hole for the Intramedullary Tibial option should be centered from medial to lateral. Anterior/posterior positioning should fall between the middle and anterior one-third of the tibial plateau (Fig. 116). Placement of the intramedullary guide is accomplished by first drilling a 8mm (5/16 ) hole in the proximal tibia (Fig. 117). Appendix C 8mm (5/16 ) Drill Bit Fig. 117
70 68 Zimmer MOST Options System Surgical Technique Table 10 Straight Smooth Stem Options Size I/M Length Total Length 9.5mm 10.5mm 11.5mm 12.5mm 13.5mm 14.5mm 15.5mm 16.5mm 17.5mm 18.5mm 75mm 40mm 122mm X X X X X 125mm 90mm 172mm X X X X X 190mm 155mm 237mm X X X X X Table 11 Straight Fluted Stem Options Size I/M Length Total Length 10.5mm 11.5mm 12.5mm 13.5mm 14.5mm 16.5mm 18.5mm 20.5mm 22.5mm 175mm 140mm 222mm X X X X X X 190mm 155mm 237mm X X X X X X X Intramedullary Tibial only - Reference Hole While Using a Tibial Intramedullary Stem Incrementally ream the tibial canal starting with the 9.5mm femoral/tibial reamers using a T-handle with Zimmer adapter (Fig. 118 on the next page). The depth of the hole is based on the straight stem selected. The depth marking on the reamer includes the amount of bone being resected. The markings on the reamers designate the type of implant being used and the stem length. The following are the acronyms used on the reamers. HF = Hinged Femur DF = Distal Femur HT = Hinged Tibia PT = Proximal Tibia The 75mm, 125mm, 175mm and 190mm straight stems are used on the system. The length marking on the implant label designates the over all composite length of the stems from the proximal tibial cut. The hinged tibial baseplate has a cone length of 82mm. The stem options recommended are a plug, a 75mm, 125mm smooth, or the 190mm smooth or fluted stems that are shown on Tables 10 and 11. The reamers are marked as shown below. HF BOSS 75HF 75HT/125HF DF/PT 125HT/175HF 190HF (Only on the 16.5mm reamer to prepare for the Hinged Femur Boss) The combined markings on the reamers indicate that different overall lengths are equal if used with another component (ex. 75HT/125HF, hinged tibia with a 75mm stem = hinged femur with 125mm stem). Cone Length Total Length I/M Length
71 Zimmer MOST Options System Surgical Technique 69 The appropriate trial stem is attached to the Trial Stem Adapter. With the handle in the Open position, the 8mm adapter can be locked into place by clicking the handle manually to the Locked position and the assembly is inserted into the tibial canal (Fig. 119). The quick disconnect handle is removed. T-handle Detachable Handle Tibial Alignment and Proximal Tibial Cuts Connect the fixed zero degree Intramedullary Alignment Guide to the Slotted Tibial Cut Guide with a 10mm single ended stylus. The zero degree guide is then placed onto the 8mm (5/16 ) Trial Stem Adapter located in the tibial canal. If no bone is present on which to rest the 10mm stylus, the thumbscrew located on the fixed zero degree Intramedullary Alignment Guide is used to secure the stylus tip by touching the least involved portion of the tibial plateau. Rotational Alignment Rotation is selected based on any remaining landmarks. The most reliable landmark will be the tibial tubercle. For proper internal/external rotation, the center of the saw block should be positioned directly over the medial one-third of the tibial tubercle (not medial to the tubercle). Extramedullary confirmation of the internal/external rotation can also be achieved by using an alignment rod placed through the outer hole of the alignment guide. This external guide rod should align with the tibial tubercle or at the ankle over the anterior tibialis tendon (Fig. 120). Ideally, both references should be used. Rotation is then locked in place by impacting the set pin with a mallet. Fig. 118 Fig. 119 Fig Degree Alignment Guide Femoral/Tibial Reamer Tibial Saw Block Tibial Stylus Trial Stem Adapter Trial Stem Appendix C
72 70 Zimmer MOST Options System Surgical Technique Zero Degree Tibial Slope A zero degree tibial cut is recommended to accommodate the cone of the Hinged Tibial Baseplate into the tibia. The instruments are preset to provide a zero degree tibial cut. Level of Resection The 10mm tibial stylus is used to determine the tibial saw guide position for minimal resection of the proximal tibia. The stylus will position the tibial saw guide 10mm below the point of reference. The tip of the stylus is placed on the lower side. Fig. 121 Note: A 10mm resection will raise the joint line approximately 5mm. There is a 15mm tibial stylus in the system that may be used to obtain a 15mm tibial resection. Stabilize the cutting guide by drilling and pinning through the two outer most holes on the DRILL ON LINE (Fig. 121). This allows for 2mm adjustment proximally and 4mm distally. The lateral drill point is first placed after retracting the patellar tendon, followed by the medial drill point. If the medial drill point appears to walk, this can be easily avoided by marking the entry point through the block, then drilling outside the block to pierce the cortex. Redrill the hole through the block. To recheck alignment, place the alignment rod on the zero degree Tibial Alignment Guide to confirm the correct rotational position. The rod should pass through the center to no more than a few millimeters lateral to the center of the ankle (Fig. 122). Remove the Tibial Alignment Guide, alignment rod, trial stem and trial stem adapter from the tibial canal. Fig. 122
73 Zimmer MOST Options System Surgical Technique 71 Cutting the Proximal Tibia A Miller guide (angel wing) can be placed on the tibial saw guide along the medial and lateral edge of the tibia to confirm the level of desired tibial resection. Place the saw capture on the tibial saw guide. If it appears that an inadequate resection will occur, adjust the tibial saw guide in 2mm increments to a lower level. Angled retractors are used to protect soft tissue and ligaments. Cut the proximal tibia with the appropriate saw blade for the saw capture (Fig. 123). Note: Saw blades especially designed for this system are recommended. The blades are 25mm (1 ) wide by 90mm (3.5 ) long with a shank thickness of and will best match the saw guide. Disassemble the jig by removing the stylus and Trial Stem Adapter. A slaphammer may be placed under the body of the guide to aid in removal of the Trial Stem Adapter and jig, leaving the saw guide fixed to the anterior face of the tibia. Fig. 123 Appendix C Tibial Cone Preparation (Intramedullary Tibial Option with a long stem only) To prepare the tibial cone, attach the appropriate trial stem to the revision cone reamer. The reaming is done with a power reamer or with the reamer attached to the T-handle via a Zimmer fitting (Fig. 124). Ream until the end of the reamer is just above the tibial plateau. Fig. 124 Revision Cone Reamer Trial Stem
74 72 Zimmer MOST Options System Surgical Technique Proximal Tibia Sizing and Drilling Select the appropriate size tibial profile by using the Tibial Baseplate Sizer/ Reamer Guide and Baseplate Sizing Bushing. Place the assembly over the Revision Cone Reamer and trial stem assembly that are still in the tibia (Fig. 125). Baseplate Sizing Bushing The tibial profile dimensions correspond to the following A/P and M/L dimensions. Tibial Size A/P M/L 1 46mm 65mm 2 48mm 71mm 3 51mm 77mm 4 54mm 83mm Tibial Keel Preparation and Tibial Trial Insertion Once the appropriate size tibia has been selected, the Hinged Tibial Trial and trial stem are assembled and then inserted into the tibia. Rotate the Hinged Tibial Trial to the proper position. The keel broach and modular handle are assembled and inserted into the Hinged Tibial Trial. The modular handle of the keel broach is gently impacted until it is fully seated (Fig. 126). Remove the modular handle from the Hinged Tibial Trial (Fig. 127). For hinge selection and trial assembly, please refer to page 13. Fig. 125 Modular Handle Hinged Tibial Trial Fig. 126 Fig. 127
75 Zimmer MOST Options System Surgical Technique 73 Appendix D Patella Caliper Patellar Preparation Stabilize the patella with two towel clips or a rake retractor to keep the patella everted. Incise soft tissue around the patella down to the insertion of the quadriceps and the patellar tendons. Use the patella caliper to measure the existing patellar thickness (Fig. 128). This measurement is compared to the preoperatively determined patellar thickness that usually ranges between 20mm and 26mm. Fig. 128 Calculate the amount of additional bone resection required to reproduce the normal patella height using the following as a reference. Any MOST Options System patella can be used on any size femoral component. Size Dimensions Thickness Small 29mm x 32mm 7.55mm Patella Sizing Template Medium Large 32mm x 35mm 35mm x 38mm 8mm 10mm Select the patella size using the patella-sizing template (Fig. 129). Apply the patella osteotomy guide to the patella parallel to the dorsal surface with the stylus set to the desired additional bone resection. Fig. 129 Appendix D Cut the patella with the oscillating saw (Fig. 130). Patella Osteotomy Guide Fig. 130
76 74 Zimmer MOST Options System Surgical Technique Apply the patella bushing toward the medial side of the resected patellar bone (Fig. 131). The reamer is used if additional bone resection or countersinking is desired (Fig. 132). Insert the Patella Drill Guide and drill the three holes drilled for the pegs with the Patella Stop Drill Bit (Fig. 133). The trial patellar component is inserted and overall patellar thickness is confirmed (Fig. 134). Patellar tracking can be checked, but additional soft tissue releases to improve patellar tracking should be delayed until after the tourniquet is deflated. Fig. 131 Patella Bushing Medial Side Patella Stop Drill Bit Patella Cutter Fig. 132 Patella Drill Guide Fig. 133 Fig. 134
77 Zimmer MOST Options System Surgical Technique 75 Appendix E Hinged Tibia Augment Preparation Tibial Spacer Cuts Note: It is recommended that a trial reduction be performed PRIOR to preparation for tibial spacers. It is critical to remember that this cut will determine the final rotational position of the tibial implant. Attach the Tibial Spacer Cut Block to the sagittal cut block using the thumbscrew on the Tibial Spacer Cut Block. With the stem trial and the 8mm trial stem adapter in the tibial canal, slide the sagittal cut block over the 8mm trial adapter and position it on the proximal tibial surface and against the anterior cortex. For proper internal/external rotation of the Tibial Spacer Cut Block, position the center of the block directly over the medial one-third of the tibial tubercle (not medial to the tubercle). With the Tibial Spacer Cut Block positioned against the anterior cortex, drill and pin the block using the two holes in the middle and two of the oblique holes located at the bottom of the block. Pins can also be used to secure the Tibial Spacer Sagittal Cut Block. When the cutting block has been secured, medial or lateral spacer cuts are made through the 6mm or 11mm slots (Fig. 135). The initial cut is made horizontally, anterior to posterior. A notch osteotome should be placed through the spacer cut block to protect the sagittal cut from going too deep into the tibia (Fig. 136). When both cuts are complete, remove the pins and unthread the block. Remove the trial stem adapter and the trial stem using the quick disconnect handle. If tibial spacers are used, they can be assembled onto the underside of the tibial baseplate with the use of two screws packaged with each spacer (Fig. 137). Sagittal Cut Block Spacer Cut Block Notch Osteotome Appendix E Fig. 135 Fig. 136 Fig. 137
78 76 Zimmer MOST Options System Surgical Technique Appendix F Appendix F Hinged Femur Augment Preparation Distal Femoral Spacer Cuts If additional bone resection is needed, as determined from pre-operative templating, the saw block can be moved proximally on the fixed pins in 2mm increments to position a slot at the desired level. If there is asymmetrical bone loss, medial or lateral distal femoral spacer cuts can be made through the slots marked 5mm or 10mm (Fig. 138). If the femur has been prepared for distal femoral spacers, the 5mm and 10mm spacer trials can be attached to the A/P cutting block (Fig. 139). This will help to ensure instrument stability by providing total contact between the A/P cutting block and the distal femoral bone surface. Fig. 138 Distal Femur Spacer If femoral spacers are used, attach them with the screw included using the hex bit and handle (Fig. 140). A/P Cutting Block Fig. 139 Fig. 140
79 Zimmer MOST Options System Surgical Technique 77
80 78 Zimmer MOST Options System Surgical Technique
81 Zimmer MOST Options System Surgical Technique 79
82 80 Zimmer MOST Options System Surgical Technique
83
84 This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the products and procedures contained in this document is of a general nature and does not represent and does not constitute medical advice or recommendations. Because this information does not purport to constitute any diagnostic or therapeutic statement with regard to any individual medical case, each patient must be examined and advised individually, and this document does not replace the need for such examination and/or advice in whole or in part. Please refer to the package inserts for important product information, including, but not limited to, contraindications, warnings, precautions, and adverse effects MM Printed in USA 2005, 2011, 2012 Zimmer, Inc. Contact your Zimmer representative or visit us at
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
DRAFT. Triathlon TS Knee System. Surgical Protocol. Version 1
 DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
The information contained in this document is intended for healthcare professionals only. Monogram Total Knee Instruments Modular Rotating Hinge Knee System Keel Baseplate Using Monogram IM Revision Instruments
Trabecular Metal Femoral Component. Surgical Technique
 Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer Segmental System. Distal Femoral Surgical Technique
 Zimmer Segmental System Distal Femoral Surgical Technique INTRO Zimmer Segmental System Distal Femoral Surgical Technique Introduction The Zimmer Segmental System is designed to address significant bone
Zimmer Segmental System Distal Femoral Surgical Technique INTRO Zimmer Segmental System Distal Femoral Surgical Technique Introduction The Zimmer Segmental System is designed to address significant bone
Zimmer NexGen LCCK. Surgical Technique for use with LCCK 4-in-1 Instrumentation. Contact your Zimmer representative or visit us at www.zimmer.
 Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
Zimmer NexGen LCCK Surgical Technique for use with LCCK 4-in-1 Instrumentation DISCLAIMER: This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the
S-ROM NOILES. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
 S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
S-ROM NOILES This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE CONTENTS INTRODUCTION S-ROM NOILES Rotating Hinge Knee System 2 SURGICAL TECHNIQUE Initial Preparation of
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
Zimmer NexGen CR-Flex and LPS-Flex Knees. Surgical Technique with Posterior Referencing Instrumentation
 Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation INTRO Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation
Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation INTRO Zimmer NexGen CR-Flex and LPS-Flex Knees Surgical Technique with Posterior Referencing Instrumentation
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System family of knee implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System family of knee implants with the INTUITION Instrumentation.
NEXGEN COMPLETE KNEE SOLUTION. Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees
 NEXGEN COMPLETE KNEE SOLUTION Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees INTRODUCTION Successful total knee arthroplasty is directly dependent on reestablishment
NEXGEN COMPLETE KNEE SOLUTION Epicondylar Instrumentation Surgical Technique For Legacy Posterior Stabilized Knees INTRODUCTION Successful total knee arthroplasty is directly dependent on reestablishment
Zimmer M/L Taper Hip Prosthesis. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Zimmer M/L Taper Hip Prosthesis Surgical Technique Zimmer M/L Taper Hip Prosthesis 1 Zimmer M/L Taper Hip Prosthesis Surgical Technique Table of Contents Preoperative Planning 2 Determination of Leg Length
Surgical Technique and Reference Guide
 Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
Surgical Technique and Reference Guide Revision total knee arthroplasty presents many complex problems for the orthopaedic surgeon. Hard tissue defects can be caused by significant bone loss, massive osteolysis,
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique
 NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique For the NexGen Cruciate Retaining & Legacy Posterior Stabilized Knee INTRODUCTION Successful total knee arthroplasty is directly
NexGen Complete Knee Solution Intramedullary Instrumentation Surgical Technique For the NexGen Cruciate Retaining & Legacy Posterior Stabilized Knee INTRODUCTION Successful total knee arthroplasty is directly
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology. Surgical Technique
 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical Technique Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology 1 Zimmer M/L Taper Hip Prosthesis with Kinectiv Technology Surgical
Scorpio NRG CR & PS. Single Radius Primary Knee System Surgical Protocol. Anterior Referencing
 Scorpio NRG CR & PS Single Radius Primary Knee System Surgical Protocol AR Anterior Referencing This document is intended to be used by healthcare professionals only. Scorpio NRG AR Single Radius Primary
Scorpio NRG CR & PS Single Radius Primary Knee System Surgical Protocol AR Anterior Referencing This document is intended to be used by healthcare professionals only. Scorpio NRG AR Single Radius Primary
Restoration Modular. Revision Hip System Surgical Protocol
 Orthopaedics Restoration Modular Revision Hip System Restoration Modular Calcar Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Revision Hip System Orthopaedics
Orthopaedics Restoration Modular Revision Hip System Restoration Modular Calcar Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Revision Hip System Orthopaedics
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique
 Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
Restoration Modular Cone Body/Conical Distal Stem Femoral Components Using the Restoration Modular Instrument System Surgical Technique CONE CONICAL BROACHED CALCAR MILLED CONE MT3 FLUTED PLASMA CONICAL
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
PRIMARY KNEE SYSTEM SIGMA SURGICAL TECHNIQUE. Balanced Surgical Technique INSTRUMENTS
 SIGMA PRIMARY KNEE SYSTEM Balanced Surgical Technique SURGICAL TECHNIQUE INSTRUMENTS Contemporary total knee arthoplasty demands high performance instrumentation that provides enhanced efficiency, precision
SIGMA PRIMARY KNEE SYSTEM Balanced Surgical Technique SURGICAL TECHNIQUE INSTRUMENTS Contemporary total knee arthoplasty demands high performance instrumentation that provides enhanced efficiency, precision
Zimmer Persona Adverse Events Reported to FDA Through 3/27/2015
 Event Description: IT IS REPORTED THAT THE PATIENT WAS REVISED DUE TO GROSS ASEPTIC LOOSENING. Manufacturer 1822565-2015- 00224 PERSONA STEMMED CEMENTED TIBIAL COMPONENT 2/23/15 1/21/15 Injury Narrative:
Event Description: IT IS REPORTED THAT THE PATIENT WAS REVISED DUE TO GROSS ASEPTIC LOOSENING. Manufacturer 1822565-2015- 00224 PERSONA STEMMED CEMENTED TIBIAL COMPONENT 2/23/15 1/21/15 Injury Narrative:
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
High-Flex Solutions for the MIS Era. Zimmer Unicompartmental High Flex Knee System
 High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
High-Flex Solutions for the MIS Era Zimmer Unicompartmental High Flex Knee System Zimmer Unicompartmental High Flex Knee Built On Success In today s health care environment, meeting patient demands means
Zimmer Natural Nail System. Cephalomedullary Nail Surgical Technique STANDARD
 Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Technique Guide. Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
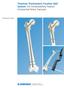 Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique
 Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Expert LFN. Lateral Femoral Nail.
 Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique. Table of Contents
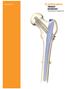 Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
Surgical Technique TRIGEN INTERTAN Intertrochanteric Antegrade Nail Surgical Technique As described by: Andreas H. Ruecker, MD Thomas A. Russell, MD Roy W. Sanders, MD Paul Tornetta, MD Table of Contents
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
Technique Guide. VersiTomic. Michael A. Rauh, MD. Anterior Cruciate Ligament Reconstruction
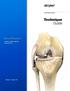 Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide. Orthopaedic Cable System. Cerclage solutions for general surgery.
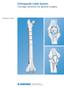 Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique
 M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation 1 Surgical Techniques for Fixation of Femoral Fractures
M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation Surgical Technique M/DN Femoral Interlocking & Recon Nail Intramedullary Fixation 1 Surgical Techniques for Fixation of Femoral Fractures
Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique
 Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with the NexGen Complete Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Bigliani/Flatow The Complete Shoulder Solution TSA
 Bigliani/Flatow The Complete Shoulder Solution TSA Surgical Technique Replicates natural shoulder mobility, balance, and stability Bigliani/Flatow The Complete Shoulder Solution Surgical Technique 1 Bigliani/Flatow
Bigliani/Flatow The Complete Shoulder Solution TSA Surgical Technique Replicates natural shoulder mobility, balance, and stability Bigliani/Flatow The Complete Shoulder Solution Surgical Technique 1 Bigliani/Flatow
Surgical technique. Sagitta EVL
 Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
Surgical technique Sagitta EVL Sagitta EVL The range Offset 7 mm The collar neck increases by mm from the size. 1 Size L (mm) Standard Offset DP+ 1. / 0 10 6 L 0+ 1 6.. 1 16 6.6.6 10 7 1 7.. 160 0 7 16
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
TFN Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
Metasul LDH Large Diameter Head
 Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System
 Knee Series Technique Guide ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System Stuart Fromm, M.D. As described by: Stuart Fromm, M.D. Black Hills Orthopedic
Knee Series Technique Guide ACL Reconstruction with Bone-Tendon-Bone Transplants Using the ENDOBUTTON CL BTB Fixation System Stuart Fromm, M.D. As described by: Stuart Fromm, M.D. Black Hills Orthopedic
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
INTRODUCTION Cerclage Cable Vs. Monofilament Wire
 B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
How To Perform An Elbow Operation
 Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Coonrad/Morrey Total Elbow Surgical Technique Interchangeability, Anterior Flange, Clinical History Coonrad/Morrey Total Elbow Surgical Technique 1 Coonrad/Morrey Total Elbow Surgical Technique Table
Knotilus TM. Anchor Instability Repair. Technique Guide
 Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Design surgeon list. Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team:
 Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
Surgical Technique Design surgeon list Smith & Nephew thanks the following surgeons for their participation as part of the R3 system design team: Robert Barrack, MD St. Louis, Missouri Robert Bourne, MD
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
TRIGEN TAN and FAN Intramedullary Nails
 Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
Surgical Technique TRIGEN TAN and FAN Intramedullary Nails Surgical Technique Table of Contents Indications...2 TRIGEN TAN and FAN Case Examples...3 Design Features: TAN...4 Implant Specifications: TAN...5
Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts
 Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts Advancing ACL Reconstruction with implant absorption and ossification of the Implant site 2,3,5 The MILAGRO BR Interference Screw
Anteromedial ACL Reconstruction Surgical Technique for Soft Tissue Grafts Advancing ACL Reconstruction with implant absorption and ossification of the Implant site 2,3,5 The MILAGRO BR Interference Screw
Surgical procedure. METS Modular Distal Femur
 Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Versa-Fx II Femoral Fixation System Surgical Techniques
 Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Exeter. Surgical Technique. V40 Stem Cement-in-Cement. Orthopaedics
 Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Exeter Orthopaedics V40 Stem Cement-in-Cement Surgical Technique Exeter V40 Stem Cement-in-Cement Surgical Technique Table of Contents Indications and Contraindications...2 Warnings and Precautions...2
Scorpio Total Stabiliser Revision Knee System. Surgical Protocol
 Scorpio Total Stabiliser Revision Knee System Surgical Protocol Surgical Protocol Scorpio Total Stabiliser Revision Knee System Patented single axis design Improved ligament stability Varus/valgus stability
Scorpio Total Stabiliser Revision Knee System Surgical Protocol Surgical Protocol Scorpio Total Stabiliser Revision Knee System Patented single axis design Improved ligament stability Varus/valgus stability
ACCOLADE II. Orthopaedics. Femoral Hip System. Surgical Technique
 ACCOLADE II Femoral Hip System Orthopaedics Surgical Technique Indications The indications for use of the total hip replacement prostheses include: Noninflammatory degenerative joint disease, including
ACCOLADE II Femoral Hip System Orthopaedics Surgical Technique Indications The indications for use of the total hip replacement prostheses include: Noninflammatory degenerative joint disease, including
ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION. Total Shoulder Arthroplasty Surgical Technique
 ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION Total Shoulder Arthroplasty Surgical Technique BIGLIANI/FLATOW THE COMPLETE SHOULDER SOLUTION SURGICAL TECHNIQUE Instruments and surgical technique
ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION Total Shoulder Arthroplasty Surgical Technique BIGLIANI/FLATOW THE COMPLETE SHOULDER SOLUTION SURGICAL TECHNIQUE Instruments and surgical technique
Accolade. System. Brochure. Achieving Perfect Balance. Cemented and Cementless Femoral Hip System
 Accolade System Brochure Achieving Perfect Balance Cemented and Cementless Femoral Hip System Accolade Cemented Hip System Potential for Perfect Balance The Accolade C Femoral Component: A perfect balance
Accolade System Brochure Achieving Perfect Balance Cemented and Cementless Femoral Hip System Accolade Cemented Hip System Potential for Perfect Balance The Accolade C Femoral Component: A perfect balance
Introduction to the Bertram Hip Spacer
 Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Introduction to the Bertram Hip Spacer Approximately 200,000 hip replacement surgeries are done every year in United States. Fortunately the incidence of infection is routinely 0.5 percent-1 percent. However
Aesculap Veterinary Orthopaedics. Targon VET Interlocking Nail
 Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
iassist Knee Surgical Technique 2-Pod Version Instruments
 iassist Knee Surgical Technique 2-Pod Version Instruments Table of Contents Page 1. Overview 4 1.1 Indication for Use 4 1.2 Training 4 1.3 Implant Indications 4 1.4 Contraindications 4 1.5 Complications
iassist Knee Surgical Technique 2-Pod Version Instruments Table of Contents Page 1. Overview 4 1.1 Indication for Use 4 1.2 Training 4 1.3 Implant Indications 4 1.4 Contraindications 4 1.5 Complications
Aesculap Orthopaedics Metha
 Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Comprehensive Reverse Shoulder System
 Comprehensive Reverse Shoulder System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon
Comprehensive Reverse Shoulder System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon
NCB Periprosthetic Femur Plate System. Surgical Technique
 NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
Michael Ries, MD Chief of Arthroplasty UCSF Medical Center San Francisco, CA. Jan Victor, MD Orthopaedic Department AZ Sint-Lucas Brugge, Belgium
 Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Fred D Cushner, MD Insall Scott Kelly Institute for
Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Fred D Cushner, MD Insall Scott Kelly Institute for
OptiLock Periarticular Plating System For Proximal Tibial Fractures. Pre-Launch Surgical Technique
 OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
Surgical technique. End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue.
 Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
Surgical technique End Cap for TEN. For axial stabilization and simultaneous protection of soft tissue. Table of contents Indications and contraindications 3 Implants 4 Instruments 4 Preoperative planning
SALVATION. Fusion Bolts and Beams SURGICAL TECHNIQUE
 SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
Expert TN. Tibial Nail.
 Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert TN. Tibial Nail. Surgical Technique Expert Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Technique Guide. Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
MDM. Surgical Technique. Modular Dual Mobility Acetabular System. Orthopaedics
 MDM X3 Modular Dual Mobility Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint disease
MDM X3 Modular Dual Mobility Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint disease
MDMTM. Surgical Technique. Modular Dual Mobility TM Acetabular System. Orthopaedics
 MDMTM X3 Modular Dual Mobility TM Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint
MDMTM X3 Modular Dual Mobility TM Acetabular System Orthopaedics Surgical Technique Indications The indications for use of total hip replacement prostheses include: Non-inflammatory degenerative joint
CuttingEdge Hip Instrumentation Femoral Surgical Technique for Primary Press-Fit and Cemented Hip Implants.
 CuttingEdge Hip Instrumentation Femoral Surgical Technique for Primary Press-Fit and Cemented Hip Implants. Surgical Protocol Table of Contents INTRODUCTION....2 FEMORAL SURGICAL TECHNIQUE Surgical Approach
CuttingEdge Hip Instrumentation Femoral Surgical Technique for Primary Press-Fit and Cemented Hip Implants. Surgical Protocol Table of Contents INTRODUCTION....2 FEMORAL SURGICAL TECHNIQUE Surgical Approach
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Rejuvenate Total Hip System Surgical Protocol. Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility
 Rejuvenate Total Hip System Surgical Protocol Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility Rejuvenate Total Hip System Surgical Protocol Table of Contents
Rejuvenate Total Hip System Surgical Protocol Rejuvenate Modular Hip Stem Enhanced Stability 1 Proven Modularity 2 Intraoperative Flexibility Rejuvenate Total Hip System Surgical Protocol Table of Contents
Lentur Cable System. Surgical Technique
 Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Technique Guide. Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting.
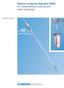 Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Knee Kinematics and Kinetics
 Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
Knee Kinematics and Kinetics Definitions: Kinematics is the study of movement without reference to forces http://www.cogsci.princeton.edu/cgi-bin/webwn2.0?stage=1&word=kinematics Kinetics is the study
CPT 12/14 Hip System. Primary Hip Athroplasty Surgical Technique
 1 CPT 12/14 Hip System Primary Hip Athroplasty Surgical Technique 2 CPT 12/14 Hip System Surgical Technique CPT 12/14 Hip System Surgical Technique 3 PRIMARY SURGICAL TECHNIQUE FOR THE CPT 12/14 COLLARLESS
1 CPT 12/14 Hip System Primary Hip Athroplasty Surgical Technique 2 CPT 12/14 Hip System Surgical Technique CPT 12/14 Hip System Surgical Technique 3 PRIMARY SURGICAL TECHNIQUE FOR THE CPT 12/14 COLLARLESS
Cable System. For Orthopaedic Trauma Surgery.
 Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Shoulder Restoration System
 Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Primary V40 Surgical Protocol. Exeter. total hip system
 Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
Primary V40 Surgical Protocol Exeter total hip system V40 SURGICAL PROTOCOL HIGHLIGHTS 44mm Head diameter mm 22 26 28 30 32 36 1. Pre-operative Planning: Pre-operative templating is important to select
ACCORD Cable System. Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri. Paul Di Cesare, MD New York, New York
 Surgical Technique Innovations in Hip Surgery 2 ACCORD Cable System Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri Paul Di Cesare, MD New York, New York Fares
Surgical Technique Innovations in Hip Surgery 2 ACCORD Cable System Surgical technique completed in conjunction with: Robert Barrack, MD St. Louis, Missouri Paul Di Cesare, MD New York, New York Fares
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM
 INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
INSTRUCTIONS FOR USING THE KNEE SOCIETY RADIOGRAPHIC EVALUATION FORM Routine standing and recumbent anterior-posterior, lateral, and skyline patellar roentgenograms are made pre-operative, at time of hospital
INSTALLATION AND OPERATING INSTRUCTIONS For Model GL1 Gate Locks
 Securitron Magnalock Corp. www.securitron.com ASSA ABLOY, the global leader Tel 800.624.5625 [email protected] in door opening solutions INSTALLATION AND OPERATING INSTRUCTIONS For Model GL1 Gate
Securitron Magnalock Corp. www.securitron.com ASSA ABLOY, the global leader Tel 800.624.5625 [email protected] in door opening solutions INSTALLATION AND OPERATING INSTRUCTIONS For Model GL1 Gate
MIS Direct Anterior Approach Surgical Protocol
 Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
METAL HEMI. Great Toe Implant SURGICAL TECHNIQUE
 METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
