Dermatomyositis and interstitial lung disease. Asmin Tulpule, HMS III November 16, 2009 Core Radiology Clerkship
|
|
|
- Chastity Park
- 7 years ago
- Views:
Transcription
1 Dermatomyositis and interstitial lung disease Asmin Tulpule, HMS III November 16, 2009 Core Radiology Clerkship
2 Agenda Presentation of our patient Menu of radiologic tests Basics of interstitial lung disease (ILD) Radiologic survey of ILD Application of radiologic findings to our patient s clinical course
3 Our patient: Initial report Ms. L is a 57 year old F with a recent diagnosis of dermatomyositis (DM) and ILD transferred to BIDMC for worsening dyspnea and hypoxia over the past 2-3 days Initial diagnosis of DM two months prior based on myalgias, Gottron s papules, and heliotrope rash. Confirmed by skin biopsy. Heliotrope rash No respiratory complaints at first and initial CT scan at OSH showed mild ILD. Started on 40 mg prednisone.
4 Note: DM is an idiopathic inflammatory myopathy with a strong association with ILD (30-40%) characterized by pulmonary fibrosis, as well as a predisposition to developing visceral malignancies (stomach, pancreas).
5 Our patient: Past Medical Hx Began developing dyspnea on exertion after a month. Thought to be progressing pulmonary fibrosis associated with DM. Receiving increasing prednisone (up to 60 mg PO qday) and started on intermittent infusions of Solumedrol. She was also tried on IVIG and azathioprine for ILD associated with DM. Her respiratory status did not improve. She was NOT placed on any antibiotic prophylaxis She reports night sweats for the past two months. She denies any fevers, chills, or symptoms of GI illness. No prior history of smoking. No recent international travel history.
6 Our patient: Initial Evaluation On the floor, she reports an acute 2-3 day worsening of respiratory status. She is no longer able to walk more than a few steps without developing acute shortness of breath. Physical Exam: Vital Signs: Tc 97.2 BP 117/79 HR 77 RR 24 O2 sat: 93% on 6L and 70%FM GEN: Ill appearing, speaking in full sentences but appears dyspneic with conversation, occasionally stopping to catch her breath Lungs: clear anteriorly. Posterior fine crackles mid and lower lung fields. No wheezes or rhonchi. Cardiac: RRR. No m/r/g. Prominent S2
7 Let s now discuss the menu of radiologic tests that could help aid us in the diagnosis and management of our patient.
8 Agenda Presentation of our patient Menu of radiologic tests Basics of interstitial lung disease (ILD) Radiologic survey of ILD Application of radiologic findings to our patient s clinical course
9 Menu of Radiologic Tests 1. Chest X-Ray (CXR), both PA and LATERAL PROS: - Excellent initial screening test - Fast and inexpensive - Sensitive for acute pulmonary processes CONS: Shows projection images not sensitive for parenchymal detail or interstitial disease 2. Chest CT (non-contrast) PROS: The gold standard for evaluating interstitial disease. + Contrast for pulmonary nodules and masses CONS: High cost and radiation dose. Not useful as a screening tool
10 Menu of Radiologic Tests cont d Lesser Used Tests: 3. Chest MR - for patients with contrast allergy or renal failure - patients who want to minimize radiation exposure (pregnant women) 4. Specialized nuclear medicine testing - Gallium scan for inflammatory (sarcoidosis) or infectious processes - PET scan monitoring of lymphoma, lung cancer
11 Our patient: Initial CXR w/ interstitial opacities Always compare with prior CXR Diffuse reticular (interstitial) opacities diffusely involving both lungs, most prominent at the bases. Upright PA Chest X-ray BIDMC, PACS
12 So, the CXR helps rule out a lot of common causes of dyspnea. We don t see signs of a lobar pneumonia (like pneumococcal), pulmonary edema, pneumothorax, or congestive heart failure exacerbation. We are dealing with Interstitial Lung Disease (aka Diffuse Parenchymal Lung Disease). What imaging test would you order next?
13 Our patient: Evolution of ILD on Chest CT Initial axial non-contrast chest CT on diagnosis Axial non-contrast chest CT 1 month later Mild ground glass opacities at L lung base BIDMC, PACS Bilateral ground glass opacities at the bases Peripheral honeycombing
14 Summary of Imaging 1) CXR showed diffuse bilateral reticulonodular opacities 2) CT showed ground glass opacities and honeycombing, w/o focal consolidation This is classic imaging of ILD (also known as diffuse parenchymal lung disease DPLD)
15 Summary of Imaging Does this tell us what our patient has? Could it be Pneumocystis carinii pneumonia (PCP) given the fact that our patient received high dose steroids without antibiotic prophylaxis? What about progressive pulmonary fibrosis associated with DM?
16 Can we distinguish between the different causes of ILD? Let s review some lung anatomy
17 Agenda Presentation of our patient Menu of radiologic tests Basics of interstitial lung disease (ILD) Radiologic survey of ILD Application of radiologic findings to our patient s clinical course
18 Interstitial Lung Diseases: Anatomy Alveolar unit ILD = Any infiltration and/or fibrosis of the lung interstitium What can do that? p.a. pulmonary artery p.v. pulmonary vein a.s. alveolar sac l - lymphatics Cells (Immune or Malignant) Infection Fluid Fibrosis (reactive or primary) (Reprint from Gray s Anatomy, 1918)
19 Interstitial Lung Disease: Differential Dx Modified 2002 American Thoracic Society Guidelines for DPLD: Acute vs Chronic: Chronic: 1) Known causes a) Inhaled substances: Inorganic, Silicosis, Asbestosis, Berylliosis b) Connective tissue disorders: Systemic sclerosis, Polymyositis, dermatomyositis, lupus c) Drugs: Antibiotics, Chemotherapeutic, Anti-arrhythmic drugs 2) Granulomatous a) Sarcoidosis b) Hypersensitivity pneumonitis 3) Rare DPLDs a) Langerhans histiocytosis b) Eosinophilic pneumonia
20 Interstitial Lung Disease: Differential Dx Modified 2002 ATS Guidelines for DPLD continued 4) Idiopathic Interstitial Pneumonias (IIPs) * divided pathologically a) Usual Interstitial Pneumonia (UIP) clinical correlate Idiopathic Pulmonary Fibrosis (IPF) b) Non-Specific Intersitial Pneumonia (NSIP) c) Cryptogenic organizing pneumonia Acute: 5) Known Infections - mimics a) Atypical pneumonia b) Pneumocystis pneumonia (PCP) c) Viral pneumonias (RSV) 6) Pulmonary edema - CHF And many others...
21 Interstitial Lung Diseases: Anatomy Can we differentiate the different causes of ILD on CXR or CT? No. But, we can get clues as to more/less likely etiologies. Examples: a) NSIP vs UIP no honeycombing in NSIP b) Hilar adenopathy sarcoid vs lymphoma vs tumor
22 So, imaging can provide us with some insight into the different causes of ILD. Let s take a look at some companion patients with classic findings within the broader category of ILD.
23 Agenda Presentation of our patient Menu of radiologic tests Basics of interstitial lung disease (ILD) Radiologic survey of ILD Application of radiologic findings to our patient s clinical course
24 Companion patient #1: Systemic Sclerosis on CXR Diffuse reticulo-nodular (interstitial) opacities diffusely involving both lungs, perhaps R>L, most prominent at the bases. Looks similar to our patient s CXR, though less severe! Upright PA Chest X-ray BIDMC, PACS
25 Companion patient #1: Systemic Sclerosis on CT Ground glass opacities noted at the lung bases Axial non-contrast chest CT BIDMC, PACS Traction bronchiechtasis due to fibrous tissue tethering of the airways
26 Companion patient #2: Idiopathic Interstitial Pneumonia on CXR Lung bases show fine reticulation and small nodules. Smaller number of tiny nodules are also suggested in the upper lobes Better evaluated with the chest CT to determine whether there is a fibrotic honeycombing and to assess nodules, if any. Upright PA Chest X-ray BIDMC, PACS Why? Fine reticular on CXR = UIP or NSIP
27 Companion patient #2: Idiopathic Interstitial Pneumonia on CT Diffuse ground-glass changes throughout the lower lobes bilaterally No honeycombing. Axial non-contrast chest CT BIDMC, PACS
28 Honeycombing: Recall our patient Axial non-contrast chest CT Peripheral honeycombing BIDMC, PACS
29 Companion patient #2: Idiopathic Interstitial Pneumonia on CT The combination of fine reticular opacities on CXR, with ground glass opacities in the absence of honeycombing on CT, helps to narrow the differential. Most likely due to fibrosing type NSIP Axial non-contrast chest CT BIDMC, PACS
30 Companion patient #3: Sarcoidosis on CXR Diffuse small discrete and confluent nodular opacities of varying sizes, involving both lungs. Bilateral hilar and right paratracheal soft tissue prominence, corresponding to the known adenopathy Upright PA Chest X-ray BIDMC, PACS
31 Companion patient #3: Sarcoidosis on CT Axial non-contrast chest CT BIDMC, PACS Extensive progression of parenchymal ground glass and micronodular opacities with a peribronchovascular and perilymphatic distribution consistent with worsening pulmonary sarcoidosis. No significant fibrosis.
32 We have taken a look at a number of different patients with classic findings of ILD that suggest a specific cause. Now, lets apply what we have learned about ILD to our patient.
33 Agenda Presentation of our patient Menu of radiologic tests Basics of interstitial lung disease (ILD) Radiologic survey of ILD Application of radiologic findings to our patient s clinical course
34 Recall our patient BIDMC, PACS Axial non-contrast chest CT Upright PA Chest X-ray Combining the radiologic findings and clinical history, can we narrow our differential of ILD causes?
35 Recall the Differential Dx for ILD 1) Known causes a) Inhaled substances: Inorganic, Silicosis, Asbestosis, Berylliosis b) Connective tissue disorders: Systemic sclerosis, Polymyositis, dermatomyositis, lupus c) Drugs: Antibiotics, Chemotherapeutic, Anti-arrhythmic drugs 2) Granulomatous a) Sarcoidosis b) Hypersensitivity pneumonitis 3) Rare DPLDs 4) Idiopathic Interstitial Pneumonias (IIPs) * divided pathologically a) UIP clinical correlate IPF b) NSIP 5) Known Infections - mimics a) Atypical pneumonia b) Pneumocystis pneumonia (PCP) c) Viral pneumonias (RSV)
36 Basics of PCP pneumonia Most common cause of interstitial pneumonia in immunocompromised patients (AIDS, high dose steroids, chemotherapy) Imaging: Normal CXR (10-40%) Often starts out as bilateral reticular infiltrates Rapidly continues to diffuse airspace disease Classic CT finding: - Exudative alveolitis w/ accumulation of fluid, organisms, fibrin, debris in alveolar spaces ground glass opacity - Patchy, mosaic appearance of diseased lung next to normal
37 Basics of PCP pneumonia Diagnosis: Sputum or BAL confirmed in our patient Clinical Course: Started on high dose bactrim. Usually responds to bactrim therapy in 5-7 days. Very low levels of resistance. Redistribution of infection to upper lobes Complications: Cystic lung disease Spontaneous pneumothorax, frequently bilateral (6-7%) Or..
38 Our patient: Worsening CXR on Day 11 1 (1) Endotracheal tube (2) PICC (3) Nasogastric tube 2 Findings: Pneumopericardium Pneumomediastinum Small R apical pneumothorax. 3 Slight increased opacity projecting over the mid right lung field may represent atelectasis versus early consolidation. Upright PA Chest X-ray BIDMC, PACS
39 Our Patient: Progression of ILD on CT Diffuse central and peripheral ground-glass opacification, with new involvement of the basal segments of the left lower lobe with atelectasis. Axial non-contrast chest CT BIDMC, PACS
40 Our patient: Outcome Very sadly, after being on the ventilator for 17 days, our patient passed way on 9/14/09. The final conclusion is that the cause of death was diffuse alveolar damage associated with pneumocystis pneumonia.
41 Summary 1) When giving high dose steroids, always prophylax against opportunistic infections. 2) CXR is a great screening tool for identifying ILD, but does not provide many specific clues about etiology. Always consider the first key branchpoint: acute vs chronic process? 3) Hi-resolution CT scan provides parenchymal detail and can identify patterns to narrow the ILD differential (honeycombing, ground glass). However, pathology, microbiology and other studies are almost always needed to confirm a diagnosis.
42 References Spectrum of fibrosing diffuse parenchymal lung disease. Morgenthau AS, Padilla ML. Mt Sinai J Med Feb;76(1):2-23. Diagnosis of interstitial lung diseases. Ryu JH, Daniels CE, Hartman TE, Yi ES. Mayo Clin Proc Aug;82(8): Imaging features of Pneumocystis carinii pneumonia. Crans CA Jr, Boiselle PM. Crit Rev Diagn Imaging Aug;40(4): Review. ATS/ERS international multidisciplinary consensus classification of the idiopathic interstitial pneumonias. Demedts M, Costabel U. Eur Respir J May;19(5):794-6.
43 Acknowledgements Erine Yeh David O Donnell Maria Levantakis Gillian Lieberman
Cystic Lung Diseases. Melissa Price Gillian Lieberman, MD Advanced Radiology Clerkship Beth Israel Deaconess Medical Center November, 2008
 Cystic Lung Diseases Melissa Price Gillian Lieberman, MD Advanced Radiology Clerkship Beth Israel Deaconess Medical Center November, 2008 How do we define a cyst of the lung? Hansell DM, Bankier AA, MacMahon
Cystic Lung Diseases Melissa Price Gillian Lieberman, MD Advanced Radiology Clerkship Beth Israel Deaconess Medical Center November, 2008 How do we define a cyst of the lung? Hansell DM, Bankier AA, MacMahon
Pulmonary interstitium. Interstitial Lung Disease. Interstitial lung disease. Interstitial lung disease. Causes.
 Pulmonary interstitium Interstitial Lung Disease Alveolar lining cells (types 1 and 2) Thin elastin-rich connective component containing capillary blood vessels Interstitial lung disease Increase in interstitial
Pulmonary interstitium Interstitial Lung Disease Alveolar lining cells (types 1 and 2) Thin elastin-rich connective component containing capillary blood vessels Interstitial lung disease Increase in interstitial
Interstitial Lung Diseases ACOI Board Review 2013
 Interstitial Lung Diseases ACOI Board Review 2013 Thomas F. Morley, DO, FACOI, FCCP, FAASM Professor of Medicine Director of the Division of Pulmonary, Critical Care and Sleep Medicine UMDNJ-SOM Restrictive
Interstitial Lung Diseases ACOI Board Review 2013 Thomas F. Morley, DO, FACOI, FCCP, FAASM Professor of Medicine Director of the Division of Pulmonary, Critical Care and Sleep Medicine UMDNJ-SOM Restrictive
Influenza (Flu) Influenza is a viral infection that may affect both the upper and lower respiratory tracts. There are three types of flu virus:
 Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
Respiratory Disorders Bio 375 Pathophysiology General Manifestations of Respiratory Disease Sneezing is a reflex response to irritation in the upper respiratory tract and is associated with inflammation
Online supplements are not copyedited prior to posting.
 Functional Impact of a Spectrum of Interstitial Lung Abnormalities in Rheumatoid Arthritis Tracy J. Doyle, MD, MPH; Paul F. Dellaripa, MD; Kerri Batra, MD; Michelle L. Frits, BA; Christine K. Iannaccone,
Functional Impact of a Spectrum of Interstitial Lung Abnormalities in Rheumatoid Arthritis Tracy J. Doyle, MD, MPH; Paul F. Dellaripa, MD; Kerri Batra, MD; Michelle L. Frits, BA; Christine K. Iannaccone,
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing
 Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
Restrictive lung diseases
 Restrictive lung diseases Characterized by reduced compliance of the lung. Prominent changes in the interstitium (interstitial lung disease). Important signs and symptoms: - Dyspnea. - Hypoxia. - With
Restrictive lung diseases Characterized by reduced compliance of the lung. Prominent changes in the interstitium (interstitial lung disease). Important signs and symptoms: - Dyspnea. - Hypoxia. - With
Radiation-Induced Lung Injury
 May 2001 Radiation-Induced Lung Injury Warren Phipps, Harvard Medical School Year III Our Patient D.C. is a 50 year-old woman with a 30-pack year history of smoking who presented to the ED because she
May 2001 Radiation-Induced Lung Injury Warren Phipps, Harvard Medical School Year III Our Patient D.C. is a 50 year-old woman with a 30-pack year history of smoking who presented to the ED because she
Tina Mosaferi, Harvard Medical School Year III Gillian Lieberman, MD
 July 2014 Tina Mosaferi, Harvard Medical School Year III 1. Our Patient-Introduction 2. Asbestos Basics 3. Pulmonary Findings Manifestations demonstrated by companion patients 4. Our patient-conclusion
July 2014 Tina Mosaferi, Harvard Medical School Year III 1. Our Patient-Introduction 2. Asbestos Basics 3. Pulmonary Findings Manifestations demonstrated by companion patients 4. Our patient-conclusion
SARCOIDOSIS. Signs and symptoms associated with specific organ involvement can include the following:
 SARCOIDOSIS Sarcoidosis is a disease that occurs when areas of inflammation develop in different organs of the body. Very small clusters of inflammation, called granulomas, are seen with sarcoidosis. They
SARCOIDOSIS Sarcoidosis is a disease that occurs when areas of inflammation develop in different organs of the body. Very small clusters of inflammation, called granulomas, are seen with sarcoidosis. They
Interstitial Lung Disease (Diffuse Parenchymal Lung Disease) Focusing on Idiopathic Pulmonary Fibrosis
 Interstitial Lung Disease (Diffuse Parenchymal Lung Disease) Focusing on Idiopathic Pulmonary Fibrosis J. D Urbano, RCP, RRT Founder / CEO: BreathSounds, LLC E-Mail: jdurbano@breathsounds.org Mobile: (480)
Interstitial Lung Disease (Diffuse Parenchymal Lung Disease) Focusing on Idiopathic Pulmonary Fibrosis J. D Urbano, RCP, RRT Founder / CEO: BreathSounds, LLC E-Mail: jdurbano@breathsounds.org Mobile: (480)
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Recurrent or Persistent Pneumonia
 Recurrent or Persistent Pneumonia Lower Respiratory Tract Dr T Avenant Recurrent or Persistent Pneumonia Definitions Recurrent pneumonia more than two episodes of pneumonia in 18 months Persistent pneumonia
Recurrent or Persistent Pneumonia Lower Respiratory Tract Dr T Avenant Recurrent or Persistent Pneumonia Definitions Recurrent pneumonia more than two episodes of pneumonia in 18 months Persistent pneumonia
INTERSTITIAL LUNG DISEASE Paul F. Simonelli, MD, Ph.D.
 INTERSTITIAL LUNG DISEASE Paul F. Simonelli, MD, Ph.D. Definition: Interstitial lung disease (ILD) refers to a broad range of conditions that have common clinical, physiological, and radiological features.
INTERSTITIAL LUNG DISEASE Paul F. Simonelli, MD, Ph.D. Definition: Interstitial lung disease (ILD) refers to a broad range of conditions that have common clinical, physiological, and radiological features.
Occupational Lung Disease. David Perlman, MD
 Occupational Lung Disease David Perlman, MD What causes occupational lung diseases? Breathing bad stuff into your lung Mechanism of particle deposition Large particles (>0.5μM) Impaction Gravitational
Occupational Lung Disease David Perlman, MD What causes occupational lung diseases? Breathing bad stuff into your lung Mechanism of particle deposition Large particles (>0.5μM) Impaction Gravitational
 September 2008 [KT 168] Sub. Code: 2063 M.D. DEGREE EXAMINATION Branch XVII Tuberculosis and Respiratory Diseases NON-TUBERCULOSIS CHEST DISEASES Common to Part II Paper II - (Old /New/Revised Regulations)
September 2008 [KT 168] Sub. Code: 2063 M.D. DEGREE EXAMINATION Branch XVII Tuberculosis and Respiratory Diseases NON-TUBERCULOSIS CHEST DISEASES Common to Part II Paper II - (Old /New/Revised Regulations)
Interstitial lung disease in a rheumatic electrician
 Interstitial lung disease in a rheumatic electrician Case history The case presented here concerns a male, born in 1931, who was an electrician for 34 years. He had frequent and close contact with asbestos,
Interstitial lung disease in a rheumatic electrician Case history The case presented here concerns a male, born in 1931, who was an electrician for 34 years. He had frequent and close contact with asbestos,
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
 Pulmonary Complications from Lung Cancer Treatment, Part 1: Chemotherapy-Induced Pneumonitis by Dr. Gerard Silvestri, Medical University of South Carolina Dr. West: Hello, and welcome to our webinar with
Pulmonary Complications from Lung Cancer Treatment, Part 1: Chemotherapy-Induced Pneumonitis by Dr. Gerard Silvestri, Medical University of South Carolina Dr. West: Hello, and welcome to our webinar with
Idiopathic Pulmonary Fibrosis
 Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Francine Lortie-Monette, MD, MSc, CSPQ, MBA Department of Epidemiology and Biostatistics University of Western Ontario 2003
 ASBESTOS Francine Lortie-Monette, MD, MSc, CSPQ, MBA Department of Epidemiology and Biostatistics University of Western Ontario 2003 Asbestosis Asbestosis is a model for other dust diseases as well as
ASBESTOS Francine Lortie-Monette, MD, MSc, CSPQ, MBA Department of Epidemiology and Biostatistics University of Western Ontario 2003 Asbestosis Asbestosis is a model for other dust diseases as well as
Pulmonary Patterns VMA 976
 Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
Pulmonary Complications of Cancer Therapy. Marc B. Feinstein, MD Pulmonary Division Memorial Sloan-Kettering Cancer Center
 Pulmonary Complications of Cancer Therapy Marc B. Feinstein, MD Pulmonary Division Memorial Sloan-Kettering Cancer Center Tobacco About 85% of lung cancers occur in current/former smokers. Tobacco causes
Pulmonary Complications of Cancer Therapy Marc B. Feinstein, MD Pulmonary Division Memorial Sloan-Kettering Cancer Center Tobacco About 85% of lung cancers occur in current/former smokers. Tobacco causes
Hodgkin Lymphoma Disease Specific Biology and Treatment Options. John Kuruvilla
 Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
Objectives COPD. Chronic Obstructive Pulmonary Disease (COPD) 4/19/2011
 Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Objectives Discuss assessment findings and treatment for: Chronic Obstructive Pulmonary Disease Bronchitis Emphysema Asthma Anaphylaxis Other respiratory issues Provide some definitions Chronic Obstructive
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Asbestos: The Range of Its Ill-Effects. Ezra Cohen, MS III Dr. Gillian Lieberman, MD Core Radiology Clerkship, BIDMC April 16 th, 2010
 Asbestos: The Range of Its Ill-Effects Ezra Cohen, MS III Dr. Gillian Lieberman, MD Core Radiology Clerkship, BIDMC April 16 th, 2010 Outline of Presentation Patient Presentation Anatomy Defining the disease
Asbestos: The Range of Its Ill-Effects Ezra Cohen, MS III Dr. Gillian Lieberman, MD Core Radiology Clerkship, BIDMC April 16 th, 2010 Outline of Presentation Patient Presentation Anatomy Defining the disease
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Asbestos Related Diseases
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease Asbestosis and Mesothelioma (LUNG CANCER) Support Group 1800 017 758 www.amsg.com.au ii Helping you and your family through
CPT codes are for information only; consult your payer organization for reimbursement information.
 CPT codes are for information only; consult your payer organization for reimbursement information. Coverage for Spirometry/Oximetry Spirometry is a component of pulmonary function testing (PFTs). PFTs
CPT codes are for information only; consult your payer organization for reimbursement information. Coverage for Spirometry/Oximetry Spirometry is a component of pulmonary function testing (PFTs). PFTs
Approach to Lower Extremity Osteomyelitis. A radiologic tour of a patient encounter
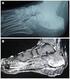 Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Approach to Lower Extremity Osteomyelitis A radiologic tour of a patient encounter David Guo,, HMS III Gillian Lieberman, MD BIDMC, October 2009 Our learning goals Review lower extremity anatomy Discuss
Position Statement from the Irish Thoracic Society on the treatment of Idiopathic Pulmonary Fibrosis
 BACKGROUND Position Statement from the Irish Thoracic Society on the treatment of Idiopathic Pulmonary Fibrosis Idiopathic Pulmonary Fibrosis (IPF) is a rare, chronic and fatal disease characterised by
BACKGROUND Position Statement from the Irish Thoracic Society on the treatment of Idiopathic Pulmonary Fibrosis Idiopathic Pulmonary Fibrosis (IPF) is a rare, chronic and fatal disease characterised by
Diagnosis & Treatment Of Cough
 Diagnosis & Treatment Of Cough a.diagnosis : - Details History - Physical Examination - Investigation b. Treatment of cough Detail history provides valuables clues for etiology of the cough - Acute or
Diagnosis & Treatment Of Cough a.diagnosis : - Details History - Physical Examination - Investigation b. Treatment of cough Detail history provides valuables clues for etiology of the cough - Acute or
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease)
 Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Spine University s Guide to Vertebral Osteonecrosis (Kummel's Disease) 2 Introduction Kummel's disease is a collapse of the vertebrae (the bones that make up the spine). It is also called vertebral osteonecrosis.
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
CERVICAL MEDIASTINOSCOPY WITH BIOPSY
 INFORMED CONSENT INFORMATION ADDRESSOGRAPH DATA CERVICAL MEDIASTINOSCOPY WITH BIOPSY You have decided to have an important procedure and we appreciate your selection of UCLA Healthcare to meet your needs.
INFORMED CONSENT INFORMATION ADDRESSOGRAPH DATA CERVICAL MEDIASTINOSCOPY WITH BIOPSY You have decided to have an important procedure and we appreciate your selection of UCLA Healthcare to meet your needs.
Systemic Lupus Erythematosus
 Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
HEALTH CARE FOR EXPOSURE TO ASBESTOS. 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.
 HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
Idiopathic Pulmonary Fibrosis (IPF) Research
 Idiopathic Pulmonary Fibrosis (IPF): Why Early Referral is Critical Even if Your Patient is Not Eligible for a Clinical Trial Idiopathic Pulmonary Fibrosis (IPF) Research Management of IPF requires a confident
Idiopathic Pulmonary Fibrosis (IPF): Why Early Referral is Critical Even if Your Patient is Not Eligible for a Clinical Trial Idiopathic Pulmonary Fibrosis (IPF) Research Management of IPF requires a confident
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
pulmonary fibrosis patient information guide [ENGLISH]
![pulmonary fibrosis patient information guide [ENGLISH] pulmonary fibrosis patient information guide [ENGLISH]](/thumbs/40/21037027.jpg) pulmonary fibrosis patient information guide [ENGLISH] contents 2 about this guide 3 defining pulmonary fibrosis 5 prevalence and incidence 6 causes 10 symptoms 11 diagnostic tests and assessments 15 treatment
pulmonary fibrosis patient information guide [ENGLISH] contents 2 about this guide 3 defining pulmonary fibrosis 5 prevalence and incidence 6 causes 10 symptoms 11 diagnostic tests and assessments 15 treatment
Best Practice Model for Imaging of Community Acquired Pneumonia. Karen E. Conner, MD
 Best Practice Model for Imaging of Community Acquired Pneumonia Karen E. Conner, MD Chest Radiology and CT Section Chief, Intermountain Healthcare; Chair, QA Committee, Mountain Medical Physician Specialists
Best Practice Model for Imaging of Community Acquired Pneumonia Karen E. Conner, MD Chest Radiology and CT Section Chief, Intermountain Healthcare; Chair, QA Committee, Mountain Medical Physician Specialists
Radiological Findings in BO
 Radiological Findings in BO BO-Meeting 2016 Schloss Johannisberg Geisenheim - Rheingau Germany Dr. Simon Martin Department of Diagnostic and Interventional Radiology University Hospital Frankfurt Bronchiolitis
Radiological Findings in BO BO-Meeting 2016 Schloss Johannisberg Geisenheim - Rheingau Germany Dr. Simon Martin Department of Diagnostic and Interventional Radiology University Hospital Frankfurt Bronchiolitis
Your Go-to COPD Guide
 Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Your Go-to COPD Guide Learning how to live with chronic obstructive pulmonary disease (COPD) Inside, you ll learn: COPD facts COPD symptoms and triggers How to talk with your doctor Different treatment
Exploring the Role of Vitamins in Achieving a Healthy Heart
 Exploring the Role of Vitamins in Achieving a Healthy Heart There are many avenues you can take to keep your heart healthy. The first step you should take is to have a medical professional evaluate the
Exploring the Role of Vitamins in Achieving a Healthy Heart There are many avenues you can take to keep your heart healthy. The first step you should take is to have a medical professional evaluate the
PLAN OF ACTION FOR. Physician Name Signature License Date
 PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
PLAN OF ACTION FOR Patient s copy (patient s name) I Feel Well Lignes I feel short directrices of breath: I cough up sputum daily. No Yes, colour: I cough regularly. No Yes I Feel Worse I have changes
Pneumonia Education and Discharge Instructions
 Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults
 CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
SUMMARY OF S.B. 15 ASBESTOS/SILICA LITIGATION REFORM BILL
 SUMMARY OF S.B. 15 ASBESTOS/SILICA LITIGATION REFORM BILL S.B. 15, the asbestos/silica litigation reform bill, distinguishes between the claims of people who are physically impaired or sick due to exposure
SUMMARY OF S.B. 15 ASBESTOS/SILICA LITIGATION REFORM BILL S.B. 15, the asbestos/silica litigation reform bill, distinguishes between the claims of people who are physically impaired or sick due to exposure
Role of HRCT in Diagnosis of Asbestos Related Pleuro Pulmonary Disease
 Cairo University Role of HRCT in Diagnosis of Asbestos Related Pleuro Pulmonary Disease ESSAY Submitted for partial fulfillment of Master degree in Radio-diagnosis By Rania Adel Abd ElRahem Elghetany (M.B.B.CH.,
Cairo University Role of HRCT in Diagnosis of Asbestos Related Pleuro Pulmonary Disease ESSAY Submitted for partial fulfillment of Master degree in Radio-diagnosis By Rania Adel Abd ElRahem Elghetany (M.B.B.CH.,
Asbestos Disease: An Overview for Clinicians Asbestos Exposure
 Asbestos Asbestos Disease: An Overview for Clinicians Asbestos Exposure Asbestos: A health hazard Exposure to asbestos was a major occupational health hazard in the United States. The first large-scale
Asbestos Asbestos Disease: An Overview for Clinicians Asbestos Exposure Asbestos: A health hazard Exposure to asbestos was a major occupational health hazard in the United States. The first large-scale
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Pulmonary Disorders. Chronic Obstructive Pulmonary Disease (COPD) Chronic Obstructive Pulmonary Disease (COPD)
 RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Pulmonary Disorders Chronic Obstructive Pulmonary Disease (COPD) Characterized by decreased expiratory airflow Reduction in expiratory
RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Pulmonary Disorders Chronic Obstructive Pulmonary Disease (COPD) Characterized by decreased expiratory airflow Reduction in expiratory
General Thoracic Surgery ICD9 to ICD10 Crosswalks. C34.11 Malignant neoplasm of upper lobe, right bronchus or lung
 ICD-9 Code ICD-9 Description ICD-10 Code ICD-10 Description 150.3 Malignant neoplasm of upper third of esophagus C15.3 Malignant neoplasm of upper third of esophagus 150.4 Malignant neoplasm of middle
ICD-9 Code ICD-9 Description ICD-10 Code ICD-10 Description 150.3 Malignant neoplasm of upper third of esophagus C15.3 Malignant neoplasm of upper third of esophagus 150.4 Malignant neoplasm of middle
Respiratory Concerns in Children with Down Syndrome
 Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Respiratory Concerns in Children with Down Syndrome Paul E. Moore, M.D. Associate Professor of Pediatrics and Pharmacology Director, Pediatric Allergy, Immunology, and Pulmonary Medicine Vanderbilt University
Lesson 7: Respiratory and Skeletal Systems and Tuberculosis
 Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Glossary 1. asthma: when the airways of the lungs narrow, making breathing difficult 2. bacteria: tiny living creatures that can only be seen with a microscope; some bacteria help the human body, and other
Occupational Lung Disease. SS Visser Internal Medicine UP
 Occupational Lung Disease SS Visser Internal Medicine UP Classification Anorganic ( mineral ) dust/pneumoconiosis Fibrogenic - silica, asbestos, talc, silicates Non-fibrogenic - Fe, barium, tin Immunologic/Pharmcologic
Occupational Lung Disease SS Visser Internal Medicine UP Classification Anorganic ( mineral ) dust/pneumoconiosis Fibrogenic - silica, asbestos, talc, silicates Non-fibrogenic - Fe, barium, tin Immunologic/Pharmcologic
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
2011 Pulmonary Pathology Society Biennial Meeting Program
 2011 Pulmonary Pathology Society Biennial Meeting Program Thursday, August 18, 2011 7:00 AM Registration and Continental Breakfast 7:45 AM Welcome: Donald Guinee / Elisabeth Brambilla 8:00 AM Interstitial
2011 Pulmonary Pathology Society Biennial Meeting Program Thursday, August 18, 2011 7:00 AM Registration and Continental Breakfast 7:45 AM Welcome: Donald Guinee / Elisabeth Brambilla 8:00 AM Interstitial
Acute Fibrinous and Organizing Pneumonia. A Histologic Pattern of Lung Injury and Possible Variant of Diffuse Alveolar Damage
 Acute Fibrinous and Organizing Pneumonia A Histologic Pattern of Lung Injury and Possible Variant of Diffuse Alveolar Damage Mary Beth Beasley, MD; Teri J. Franks, MD; Jeffrey R. Galvin, MD; Bernadette
Acute Fibrinous and Organizing Pneumonia A Histologic Pattern of Lung Injury and Possible Variant of Diffuse Alveolar Damage Mary Beth Beasley, MD; Teri J. Franks, MD; Jeffrey R. Galvin, MD; Bernadette
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
COPD and Asthma Differential Diagnosis
 COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
COPD and Asthma Differential Diagnosis Chronic Obstructive Pulmonary Disease (COPD) is the third leading cause of death in America. Learning Objectives Use tools to effectively diagnose chronic obstructive
Diseases. Inflammations Non-inflammatory pleural effusions Pneumothorax Tumours
 Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
Pleura Visceral pleura covers lungs and extends into fissures Parietal pleura limits mediastinum and covers dome of diaphragm and inner aspect of chest wall. Two layers between them (pleural cavity) contains
PARTICLE SIZE AND CHEMISTRY:
 Pneumoconioses LW/Please note: This information is additional to Davidson s Principles and Practice of Medicine. /Hierdie inligting is aanvullend tot Davidson s Principles and Practice of Medicine. Pneumoconioses
Pneumoconioses LW/Please note: This information is additional to Davidson s Principles and Practice of Medicine. /Hierdie inligting is aanvullend tot Davidson s Principles and Practice of Medicine. Pneumoconioses
Prevention of Acute COPD exacerbations
 December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
December 3, 2015 Prevention of Acute COPD exacerbations George Pyrgos MD 1 Disclosures No funding received for this presentation I have previously conducted clinical trials with Boehringer Ingelheim. Principal
Asbestos Related Diseases. Asbestosis Mesothelioma Lung Cancer Pleural Disease. connecting raising awareness supporting advocating
 Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
Asbestos Related Diseases Asbestosis Mesothelioma Lung Cancer Pleural Disease connecting raising awareness supporting advocating 1800 017 758 www.asbestosassociation.com.au Asbestos lagging was widely
EMPHYSEMA THERAPY. Information brochure for valve therapy in the treatment of emphysema.
 EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
EMPHYSEMA THERAPY Information brochure for valve therapy in the treatment of emphysema. PATIENTS WITH EMPHYSEMA With every breath, lungs deliver oxygen to the rest of the body to perform essential life
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
ASTHMA IN INFANTS AND YOUNG CHILDREN
 ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
ASTHMA IN INFANTS AND YOUNG CHILDREN What is Asthma? Asthma is a chronic inflammatory disease of the airways. Symptoms of asthma are variable. That means that they can be mild to severe, intermittent to
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Documenting & Coding. Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC
 Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Documenting & Coding Chronic Obstructive Pulmonary Disease (COPD) Presented by: David S. Brigner, MLA, CPC Sr. Provider Training & Development Consultant Professional Profile David Brigner currently performs
Emphysema. Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
ASK A DOC. Clinical Trial Update May 28, 2014. Welcome!
 ASK A DOC Clinical Trial Update May 28, 2014 Welcome! ASK A DOC CLINICAL TRIAL UPDATE Dr. Gregory Cosgrove PFF Chief Medical Officer Dr. Kevin Flaherty Chairman Steering Committee PFF CCN and PFF Registry
ASK A DOC Clinical Trial Update May 28, 2014 Welcome! ASK A DOC CLINICAL TRIAL UPDATE Dr. Gregory Cosgrove PFF Chief Medical Officer Dr. Kevin Flaherty Chairman Steering Committee PFF CCN and PFF Registry
Spectrum of Asbestosis and other Asbestos related diseases from a Radiological viewpoint
 Aditya Pawaskar, Final Year Date of Rotation: 4/1/2013 to 4/28/2013 Spectrum of Asbestosis and other Asbestos related diseases from a Radiological viewpoint Aditya Pawaskar Lokmanya Tilak Municipal Medical
Aditya Pawaskar, Final Year Date of Rotation: 4/1/2013 to 4/28/2013 Spectrum of Asbestosis and other Asbestos related diseases from a Radiological viewpoint Aditya Pawaskar Lokmanya Tilak Municipal Medical
Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects
 Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects This document lists sample learning objectives by subject matter The numerical ranking in parenthesis following
Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects This document lists sample learning objectives by subject matter The numerical ranking in parenthesis following
Overview. Geriatric Overview. Chapter 26. Geriatrics 9/11/2012
 Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
Chapter 26 Geriatrics Slide 1 Overview Trauma Common Medical Emergencies Special Considerations in the Elderly Medication Considerations Abuse and Neglect Expanding the Role of EMS Slide 2 Geriatric Overview
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Interstitial lung disease
 Interstitial lung disease William D Travis Abstract Idiopathic interstitial pneumonias represent an important group of interstitial lung diseases, encompassing seven entities: (1) usual interstitial pneumonia
Interstitial lung disease William D Travis Abstract Idiopathic interstitial pneumonias represent an important group of interstitial lung diseases, encompassing seven entities: (1) usual interstitial pneumonia
Tuberculosis: FAQs. What is the difference between latent TB infection and TB disease?
 Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
Tuberculosis: FAQs What is TB disease? Tuberculosis (TB) is a disease caused by bacteria (germs) that are spread from person to person through the air. TB usually affects the lungs, but it can also affect
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
CT Scan Thorax and Upper Abdomen. Respiratory Unit Patient Information Leaflet
 CT Scan Thorax and Upper Abdomen Respiratory Unit Patient Information Leaflet Introduction This leaflet gives you general information about your CT (computerised tomography) scan. It does not replace the
CT Scan Thorax and Upper Abdomen Respiratory Unit Patient Information Leaflet Introduction This leaflet gives you general information about your CT (computerised tomography) scan. It does not replace the
CT Scan UHN. Information for patients and families
 CT Scan UHN Information for patients and families Read this information to learn: what a CT scan is how to prepare for the scan what to expect who to contact if you have any questions Joint Department
CT Scan UHN Information for patients and families Read this information to learn: what a CT scan is how to prepare for the scan what to expect who to contact if you have any questions Joint Department
Low-dose CT Imaging. Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital
 Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
Lung Cancer Screening with Low-dose CT Imaging Edgar Fearnow, M.D. Section Chief, Computed Tomography, Lancaster General Hospital Despite recent declines in the incidence of lung cancer related to the
CIBMTR Infection Data and the New Infection Inserts.
 CIBMTR Infection Data and the New Infection Inserts. Marcie Tomblyn, MD, MS Scientific Director, CIBMTR Infection and Immune Reconstitution Working Committee Overview Indication for expanded data collection
CIBMTR Infection Data and the New Infection Inserts. Marcie Tomblyn, MD, MS Scientific Director, CIBMTR Infection and Immune Reconstitution Working Committee Overview Indication for expanded data collection
by Lee S. Newman, M.D., and Cecile S. Rose, M.D., M.P.H.
 OCCUPATIONAL ASBESTOSIS AND RELATED DISEASES by Lee S. Newman, M.D., and Cecile S. Rose, M.D., M.P.H. A 63-year-old man consulted an internist complaining of dyspnea on exertion. He reported the following:
OCCUPATIONAL ASBESTOSIS AND RELATED DISEASES by Lee S. Newman, M.D., and Cecile S. Rose, M.D., M.P.H. A 63-year-old man consulted an internist complaining of dyspnea on exertion. He reported the following:
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
Transcript for Asbestos Information for the Community
 Welcome to the lecture on asbestos and its health effects for the community. My name is Dr. Vik Kapil and I come to you from the Centers for Disease Control and Prevention, Agency for Toxic Substances
Welcome to the lecture on asbestos and its health effects for the community. My name is Dr. Vik Kapil and I come to you from the Centers for Disease Control and Prevention, Agency for Toxic Substances
Pneumonia. Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid.
 Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Pneumonia Pneumonia is an infection that makes the tiny air sacs in your lungs inflamed (swollen and sore). They then fill with liquid. People with mild (not so bad) pneumonia can usually be treated at
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
MEDICATION GUIDE mitoxantrone (mito-xan-trone) for injection concentrate
 MEDICATION GUIDE mitoxantrone (mito-xan-trone) for injection concentrate Read this Medication Guide before you start receiving mitoxantrone and each time you receive mitoxantrone. There may be new information.
MEDICATION GUIDE mitoxantrone (mito-xan-trone) for injection concentrate Read this Medication Guide before you start receiving mitoxantrone and each time you receive mitoxantrone. There may be new information.
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Congestive Heart Failure
 William Herring, M.D. 2002 Congestive Heart Failure In Slide Show mode, to advance slides, press spacebar or click left mouse button Congestive Heart Failure Causes of Coronary artery disease Hypertension
William Herring, M.D. 2002 Congestive Heart Failure In Slide Show mode, to advance slides, press spacebar or click left mouse button Congestive Heart Failure Causes of Coronary artery disease Hypertension
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Frequently Asked Questions
 This fact sheet was written by the Agency for Toxic Substances and Disease Registry (ATSDR), a federal public health agency. ATSDR s mission is to serve the public by using the best science, taking responsive
This fact sheet was written by the Agency for Toxic Substances and Disease Registry (ATSDR), a federal public health agency. ATSDR s mission is to serve the public by using the best science, taking responsive
