Diabetes Use of subcutaneous insulin and oral hypoglycaemics in the Maternity Unit (GL943)
|
|
|
- Eileen Hall
- 7 years ago
- Views:
Transcription
1 Diabetes Use of subcutaneous insulin and oral hypoglycaemics in the Maternity Unit (GL943) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance Committee 3 rd October 2014 Change History Version Date Author, job title Reason 1.0 March 2014 Deirdre Graham Clinical requirement ) This document is valid only on Last printed 21/10/ :40:00 Page 1of 9
2 Overview Insulin, whether naturally produced or given externally, is essential to bring down the blood glucose within the narrow normal range of, approximately, 4 6 mmol/l. Insulin injections are used to provide insulin to those whose production has ceased, to those whose production is insufficient and to supplement those who are highly resistant to their own insulin. The National Patient Safety Agency and the National Diabetes Inpatient Audit have demonstrated that drug errors commonly occur with the administration of insulin, in some cases leading to death. Women with insulin dependent diabetes form a very small proportion of our pregnant population causing infrequent practise in the care of these women. The abbreviation VRII** (Variable Rate Insulin Infusion**) will be used in place of the term insulin sliding scale and the abbreviation CSII used for continuous subcutaneous insulin infusion Insulin administration Insulin is destroyed in the stomach, therefore cannot be taken orally Insulin is measured in units Insulin is given subcutaneously or intravenously Most women on insulin will use a multi-dose pen. The pen contains a cartridge which, when full, contains 300 units of insulin. The pen may be disposable, or, the pen may be reusable, i.e., the pen has a removable insulin cartridge, which is renewed when needed and the pen retained. The woman attaches a needle to the pen, which should be renewed for each injection given. Due to the risk of sharps injury when changing needles, pens are for patient use only. If a woman arrives at the hospital without her insulin and blood glucose meter, send a relative home to get it immediately. If a delay is expected, suitable insulin should be obtained immediately from pharmacy or from one of the medical wards. Self-administration of insulin Most women, who are not on intravenous insulin, self-administer subcutaneous doses. To protect the woman and the midwives looking after her, the Trust has a Selfadministration of Insulin Policy, which must be followed. The full document may be found on the Trust intranet Policy hub in Policies & Protocols>Clinical documents>diabetes & Endocrinology>Insulin self management protocol. A summary of the procedure, including additional notes for midwives may be found at the end of this document in Appendix 1. Midwife administration of insulin A midwife must use a 10 ml vial of insulin with an insulin syringe and needle. Non-insulin 1 ml syringes must not be used under any circumstances to draw up insulin. When started, a vial of insulin has a shelf life of six weeks. The date of first use must be marked on the ampoule. This document is valid only on Last printed 21/10/ :40:00 Page 2 of 9
3 An insulin cartridge intended for a pen must not be used with a needle and syringe. Insulin syringes come in 2 sizes, i.e., 50 units (0.5ml) or 100 units (1ml). Care should be taken regarding the size of the syringe used when drawing up insulin. Insulin syringes come with a needle attached. Ideally, this should be no longer than 8 mm. Shorter than 8mm are not usually available. Needles of 12.7 mm are sometime seen and their use should be avoided. On administering insulin using an 8mm needle a small skin fold should be pinched up to avoid the insulin being injected into the muscle layer. The needle should be passed through the skin at a right-angle. On administering insulin using a 12.7 mm needle, a skin fold should be pinched up and the needle introduced through the skin at a 45 0 angle. At the end of the injection, the needle should be left in the tissue for 10 seconds to allow all the insulin to leave the syringe and needle. It should be noted that the following commonly used insulin s do not come in 10 ml vials, Novomix 30: women can be changed to Humalog Mix 25 until their own pen is available Levemir (Detemir): women can be changed to Lantus (Glargine) until their own pen is available The following insulin s are interchangeable, on a temporary basis, Novorapid (insulin Aspart) may be interchanged with Humalog (insulin Lispro) and vice versa in the event that pharmacy does not have 10 ml vials of one of these insulin s Insulin delivered by Continuous Subcutaneous Insulin Infusion - CSII (Insulin pump) The hospital protocol for the management of inpatients on insulin pumps is to be found on the Trust intranet Policy hub in Policies & Protocols>Clinical documents>diabetes & Endocrinology>Diabetic Inpatient Insulin Pump Therapy Guidelines) A CSII delivers a small dose of insulin continuously, via a cannula inserted into the subcutaneous fat, from an infusion pump containing a cartridge of insulin. The dose may vary slightly through the 24 hours. At meal times, the woman also gives a bolus dose of insulin via the pump, with the dose adjusted to the amount of carbohydrate taken. The woman will not take any long acting insulin. An inpatient should only remain on a CSII providing she is fully able to manage the pump herself. If the pump needs to be discontinued, this must be done in agreement with the woman In the event of pump removal or malfunction, women using a CSII can develop diabetic ketoacidosis more quickly than in those using individual insulin injections If needed, a VRII** should be commenced before a CSII is removed The CSII must be removed for an MRI, CT scan and X-Ray and should be kept safely out of the room. If the procedure is expected to last longer than 1 hour a VRII** should be started promptly This document is valid only on Last printed 21/10/ :40:00 Page 3 of 9
4 At the present time, intrapartum women are asked to stop using their CSII and insulin is delivered by a VRII**, or, at Elective Caesarean by a glucose/insulin/potassium regimen When a CSII is restarted after a period without use, the VRII** should be continued for at least 60 minutes before the VRII** is stopped When a woman has hypoglycaemia on a CSII, the hypo should be corrected according to the Trust policy and the CSII should not be stopped For women using a CSII admitted with hyperglycaemia, refer to the Trust guidance found on: Trust intranet Policy hub in Policies & Protocols>Clinical documents>diabetes & Endocrinology> Diabetic Inpatient Insulin Pump Therapy Guidelines>Guidelines for managing adult inpatients on continuous subcutaneous insulin (csii) pump therapy Sites for injection Suitable sites are: in the abdomen around the umbilicus, the outer upper thigh, the upper outer fatty part of the hips or the fatty part of the outer upper arm. Insulin is absorbed at different speeds from different injection sites and women will rotate their sites through the day. When a midwife gives a woman insulin, the midwife should ask where the woman would normally inject the dose and that site used. Prescribing Insulin must be prescribed on a drug chart and this is, usually, best done using the variable dose medication sections of the drug chart. Ensure that prescribers always write the word units in full. This must not be abbreviated to u or iu. This may lead to misinterpretation and result in an overdose. Two common insulin regimens are, 2 daily doses of a fixed number of units of rapid/intermediate-acting mixed insulin 4 or 5 daily doses consisting of, 3 short or rapid-acting insulin doses with each meal, with 1 or 2 long-acting doses once or twice daily The 3 short or rapid-acting doses may be decided in one of the following ways, a fixed number of units per dose a ratio of units to carbohydrates, e.g. 1 unit of insulin to 10 gms carbohydrate, often shortened to 1:10. Thus a 50gm carbohydrate meal would need a 5 unit dose of insulin The woman should know her doses but if she is uncertain, check the notes as follows, for antenatal women, the doses written on the most recent antenatal clinic visit will be correct for women immediately postnatal, the doses will be on the Delivery Management page of the Diabetes Care Record if the postnatal woman has delivered prematurely, the postnatal doses may not be on the Delivery Management page, in which case, the pre-pregnancy doses should be used but reduced by about one quarter to one third. The pre-pregnancy doses can be found at the top of page 2 of the Diabetes Care Record This document is valid only on Last printed 21/10/ :40:00 Page 4 of 9
5 A postnatal woman should never continue with her antenatal insulin doses. The insulin requirement rises during pregnancy and doses can increase considerably. The increased requirement ends immediately after delivery of the placenta. If a woman wants to give insulin outside the normal times of administration, or wants to give a dose greater or lesser than the prescribed doses, this should be questioned and medical advice sought. Do not assume that the woman is right. Any insulin dose recommended to be given in addition to the regular doses prescribed must be written up on the Once Only medication on the front of the drug chart. Insulin s commonly used in pregnant women The list below shows that there are different types of insulin and the various types have differing actions. The types of insulin, below, are colour-coded by their action. There are various reasons for the type of insulin used, including, the way the insulin works, the diabetes type and severity, the flexibility it offers for good control and patient preference. Within a type there can be several makes of, similarly-acting, insulin s. These insulin s will be made by different companies. The make of insulin used is often down to prescriber preference. Commonly used insulin s in pregnancy Name of insulin Type of insulin Time to onset of action Novorapid Rapid acting Humalog Rapid acting Apidra Rapid acting Actrapid/HumulinS Short acting Lantus/Glargine Long acting 2 hours Levemir/Detemir Long acting 2 hours Insulatard Humulin I Novomix 30 Humalog Mix 25 Intermediate acting isophane Intermediate acting isophane Rapid/Intermediate acting mix Rapid/Intermediate acting mix 2 hours 2 hours Peak of action hours No peak No peak 6-8 hours 6-8 hours Two peaks Two peaks Duration of action Appearance 3-5 hrs Clear 3-5 hrs Clear 3-5 hrs Clear 6-8 hrs Clear hrs Clear hrs Clear hrs Cloudy hrs Cloudy hrs Cloudy hrs Cloudy Time of administration Immediately before or immediately after food before food At the same time, once or twice daily Twice daily with food Immediately before or immediately after food This document is valid only on Last printed 21/10/ :40:00 Page 5 of 9
6 Hypoglycaemia Insulin injections override the body s normal defence mechanisms against the blood glucose dropping too low (hypoglycaemia) and hypoglycaemia is a common side effect of insulin medication. In pregnancy the target pre-meal blood glucose levels are mmol/l but, in an inpatient, a glucose below 4.0 mmol/l should be regarded as hypoglycaemia. Postnatally, to prevent a severe hypoglycaemic episode, the target glucose in the first few days is 5 10 mmol/l with gradual tightening to 5 7 mmol/l thereafter. Treatment of Hypoglycaemia: Orange juice, Coca Cola, Lucozade or Jelly Babies may be products that the woman already has available. Products to reverse hypoglycaemia are available in the orange coloured Hypoglycaemia Box kept in all areas except Rushey. For mild hypoglycaemia give gms of glucose: Patient must be conscious, able to swallow and allowed to eat for the following products Glucogel oral gel; 10 gm tube GlucoTabs; 4 gm tablets GlucoJuice; 15 gm bottle The following products are available to correct severe hypoglycaemia: 20% IV glucose bags in the Emergency Crash Trolley with instructions give 75 ml Glucagon Kit (in fridge); 1mg vial of powder to be mixed with water from prefilled syringe; May be given IM of IV; normally only required by severely affected or unconscious woman. The blood glucose should be rechecked after 20 minutes and the treatment repeated until the blood glucose is above 4.0 mmol/l. Quick-acting carbohydrate to correct a hypo should be followed by slower-acting carbohydrate, such as toast. Hyperglycaemia Inadequate insulin can result in diabetic ketoacidosis (DKA). With insufficient insulin the cells become depleted of glucose and the response is the creation of glucose from fat stores, resulting in ketonaemia, which is toxic to mother and fetus. Unlike the non-pregnant diabetic, who will present with high blood glucose readings, the pregnant woman can present with normal or near-normal glucose readings. DKA can only be corrected with rehydration and intravenous insulin and this is managed on the Delivery Suite and has its own protocol. Oral hypoglycaemic agents The uses of Metformin and Glibenclamide have been sanctioned for use in pregnancy by NICE since At the RBFT we only use Metformin antenatally. Metformin has 3 effects, it reduces the glucose released in to the blood stream by the liver it reduces the amount of glucose absorbed by the gut it enhances the action of the woman s own insulin This document is valid only on Last printed 21/10/ :40:00 Page 6 of 9
7 It can have side effects and the dose needs to be increased gradually when newly prescribed or recommenced after a break in use. The common side effects are, abdominal bloating flatulence nausea less commonly diarrhoea if the woman experiences extreme fatigue, vomiting and muscular pain she is advised to contact the diabetes midwives side effects are reduced by administering the drug in the middle of, or at the end of a full meal and with a full glass of water Metformin should not be prescribed for people with impaired kidney function For those who have persistent side effects, Metformin modified release can be tried, often with good effect. For antenatal women unable to tolerate Metformin or Metformin modified release, transfer to insulin will be necessary. Commonly used doses of Metformin in pregnancy Metformin 500 mg with evening meal Metformin 500mg bd or tds Metformin up to 1 gm bd Metformin 850 gm tds Higher doses have been used but only when sanctioned by the consultant obstetrician or endocrinologist. Cautions Metformin should be withheld in women at risk of tissue hypoxia or renal impairment, in maternity patients this would include, severe sepsis, severe pre-eclampsia or eclampsia and possibly major haemorrhage. It should only be recommenced after medical consultation. Alternative anti-diabetic therapy may be necessary in the interim. Advice should be sought regarding the use of Metformin in cases of hepatic impairment. Following surgery normal renal function should be ascertained with a laboratory sample for urea and electrolytes. Metformin should be withheld prior to any test using iodine containing contrast media and recommenced not earlier than 48 hours after the test when normal renal function has been ascertained with urea and electrolytes sample. Inpatients administering their own Metformin should be managed under the Selfadministration of Medicines Policy, which can be found on intranet (link please: Policies & Protocols>Clinical documents>0 General Trust wide>self Administration of Medicines Policy (CG061)). Breast feeding Postnatal women may take Metformin This document is valid only on Last printed 21/10/ :40:00 Page 7 of 9
8 Advice should be sought from the paediatricians whether a woman may resume Glibenclamide Other oral and parenteral medication, commonly used with type 2 diabetes, must not be taken and consideration should be given to other anti-diabetic therapies. Bottle feeding All medications may be resumed. Type 2 diabetic women, intending to become pregnant again in the near future, would be advised not to resume anti-diabetic drugs other than Metformin or Glibenclamide. If these therapies are not suitable, a non-teratogenic alternative should be considered and this may have to be insulin. Advice should be sought from the diabetes medical team. References: 1. National Patient Safety Agency (2010) Rapid Response Report NPSA/2010/RRR013: Safer administration of insulin 2. BNF September RBFT Policies and protocols: Guidelines for managing adult inpatients on continuous subcutaneous insulin (csii) pump therapy 4. RBFT Policies & Protocols: Clinical documents>diabetes & Endocrinology>Insulin self management protocol This document is valid only on Last printed 21/10/ :40:00 Page 8 of 9
9 Appendix 1 Self-administration of insulin Under the Self-administration of Insulin policy, when safe to do so, women may selfadminister insulin without supervision. The procedure is summarised below. The midwife in charge of the woman s care per shift is responsible and accountable for the woman self-managing her own insulin injections. Give the woman the Self-administration of insulin information leaflet (available in all areas except Marsh and Rushey). Obtain her consent to self-administer her own insulin Ensure that the woman knows to keep her insulin pens and needles safely out of sight The woman should be given a bedside sharps container Complete the self-administration of insulin questionnaire. She must be able to answer no to all these questions in order to self-administer insulin. (Forms are available in all areas, except Marsh and Rushey). In addition to the stated reasons, in the policy, to deny self-administration of insulin, midwives should be cautious regarding women who have not slept for several days prior to being allowed to self-administer insulin Show the woman how to complete the diabetes chart on the obverse side of the Selfadministration of Insulin questionnaire. She must enter the date, time and dose of insulin given. She must also enter her blood glucose result taken prior to the dose of insulin given. To demonstrate the procedure has been explained and agreed, at the commencement of self-administration, both the woman and the midwife must date and sign the Selfadministration of Insulin diabetes chart Each shift, the midwife in charge of the woman s care must make a basic assessment that she feels the woman is still capable of safely administering her own insulin. She must initial the woman s Self-administration of Insulin diabetes chart to this effect Insulin should be prescribed on the woman s drug chart. It is advisable to use the variable dose sections The drug chart must be completed when the woman has given her insulin, noting the dose, date, time and that it was self-administered by marking the chart with no. 5 and commenting on the back of the chart that the dose was self-administered If she feels that a woman is no longer capable of self-administering insulin she must initial the Stop column on the Self-administration of insulin diabetes chart If it is decided that a woman should not self-administer insulin, her insulin pens should be locked away in the ward drug fridge This document is valid only on Last printed 21/10/ :40:00 Page 9 of 9
Safe use of insulin e- learning module
 Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
Safe use of insulin e- learning module Page 1 Introduction Insulin is a hormone produced by the beta cells in the pancreas, it is released when blood glucose levels are raised for example after a meal.
Insulin Pump Therapy during Pregnancy and Birth
 Approvals: Specialist Group: Miss F Ashworth, Dr I Gallen, Dr J Ahmed Maternity Guidelines Group: V1 Dec 2012 Directorate Board: V1 Jan 2013 Clinical Guidelines Subgroup: July 2011 MSLC: V1 Nov 2012 Equality
Approvals: Specialist Group: Miss F Ashworth, Dr I Gallen, Dr J Ahmed Maternity Guidelines Group: V1 Dec 2012 Directorate Board: V1 Jan 2013 Clinical Guidelines Subgroup: July 2011 MSLC: V1 Nov 2012 Equality
ONCE ONLY GLUCAGON and Fast Acting Glucose gel (PGD) For nurse administration under Patient Group Direction (Trust wide PGD in place)
 ADULT INSULIN PRERIPTION AND BLOOD GLUCOSE MONITORING CHART Ward CONSULTANT DATE OF ADMISSION Please affix Patient s label here Ward Ward.../...year PATIENT NAME....... DATE OF BIRTH... NHS NUMBER.......
ADULT INSULIN PRERIPTION AND BLOOD GLUCOSE MONITORING CHART Ward CONSULTANT DATE OF ADMISSION Please affix Patient s label here Ward Ward.../...year PATIENT NAME....... DATE OF BIRTH... NHS NUMBER.......
The safe use of insulin and you
 Ambulatory Care & Local Networks The safe use of insulin and you Information for patients The right insulin The right dose The right way The right time 3 Insulin treatment improves the quality of life
Ambulatory Care & Local Networks The safe use of insulin and you Information for patients The right insulin The right dose The right way The right time 3 Insulin treatment improves the quality of life
INTRODUCTION TO INSULIN
 INTRODUCTION TO INSULIN This section will give you some practical advice about using insulin. Your diabetes team will answer any particular questions that you may have e.g. dose of insulin. TYPES OF INSULIN
INTRODUCTION TO INSULIN This section will give you some practical advice about using insulin. Your diabetes team will answer any particular questions that you may have e.g. dose of insulin. TYPES OF INSULIN
CLASS OBJECTIVES. Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies
 Insulins CLASS OBJECTIVES Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies INVENTION OF INSULIN 1921 The first stills used to make insulin
Insulins CLASS OBJECTIVES Describe the history of insulin discovery List types of insulin Define indications and dosages Review case studies INVENTION OF INSULIN 1921 The first stills used to make insulin
UW MEDICINE PATIENT EDUCATION. Using Insulin. Basic facts about insulin and self-injection. What is insulin? How does diabetes affect the body?
 UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
UW MEDICINE PATIENT EDUCATION Using Insulin Basic facts about insulin and self-injection This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection
GESTATIONAL DIABETES (DIET/INSULIN/METFORMIN) CARE OF WOMEN IN BIRTHING SUITE
 GESTATIONAL DIABETES (DIET/INSULIN/METFORMIN) CARE OF WOMEN IN BIRTHING SUITE DEFINITION A disorder characterised by hyperglycaemia first recognised during pregnancy due to increased insulin resistance
GESTATIONAL DIABETES (DIET/INSULIN/METFORMIN) CARE OF WOMEN IN BIRTHING SUITE DEFINITION A disorder characterised by hyperglycaemia first recognised during pregnancy due to increased insulin resistance
A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration
 of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
of nurse A new insulin order form should be completed for subsequent changes to type of insulin and/or frequency of administration 1. Check times for point of care meter blood glucose testing. Pre-Breakfast
An estimated 280 Australians develop diabetes every day. It is Australia s fastest-growing chronic disease.
 Diabetes and insulin Summary Even with the help of your doctor and diabetes nurse educator, it may take a while to find the right insulin dose to reduce your blood glucose to your target levels. Insulin
Diabetes and insulin Summary Even with the help of your doctor and diabetes nurse educator, it may take a while to find the right insulin dose to reduce your blood glucose to your target levels. Insulin
Insulin. and diabetes. What is insulin? Who needs to inject insulin? Why must it be injected? What if I have to go on to insulin?
 Insulin What is insulin? and diabetes Insulin is a hormone made by special cells, called beta cells, in the pancreas. When we eat, insulin is released into the blood stream where it helps to move glucose
Insulin What is insulin? and diabetes Insulin is a hormone made by special cells, called beta cells, in the pancreas. When we eat, insulin is released into the blood stream where it helps to move glucose
Guidance for self administration of insulin injections
 Guidance for self administration of insulin injections You have been recommended to give yourself insulin by injection during your pregnancy. The diabetes specialist midwife has already shown you how to
Guidance for self administration of insulin injections You have been recommended to give yourself insulin by injection during your pregnancy. The diabetes specialist midwife has already shown you how to
10 to 30 minutes ½ to 3 hours 3 to 5 hours. 30 60 minutes 1 to 5 hours 8 hours. 1 to 4 hours
 Insulin Action There are several types of insulin. They are classified by how long they act: very fast, fast, slow and very slow acting. Each type of insulin has a certain time period in which it works.
Insulin Action There are several types of insulin. They are classified by how long they act: very fast, fast, slow and very slow acting. Each type of insulin has a certain time period in which it works.
TYPE 2 DIABETES MELLITIS (INSULIN AND/OR METFORMIN) CARE OF WOMEN IN BIRTHING SUITE
 TYPE 2 DIABETES MELLITIS (INSULIN AND/OR METFORMIN) CARE OF WOMEN IN BIRTHING SUITE DEFINITION Type 2 Diabetes is characterised by insulin resistance and relative impairment of insulin secretion leading
TYPE 2 DIABETES MELLITIS (INSULIN AND/OR METFORMIN) CARE OF WOMEN IN BIRTHING SUITE DEFINITION Type 2 Diabetes is characterised by insulin resistance and relative impairment of insulin secretion leading
Guidelines for Education and Training
 Aim These protocols aim to provide the necessary guidance to enable insulin to be initiated safely and effectively Objectives 1. To provide the suggested procedure for the initiation of insulin for people
Aim These protocols aim to provide the necessary guidance to enable insulin to be initiated safely and effectively Objectives 1. To provide the suggested procedure for the initiation of insulin for people
INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco
 INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco CLINICAL RECOGNITION Background: Appropriate inpatient glycemic
INPATIENT DIABETES MANAGEMENT Robert J. Rushakoff, MD Professor of Medicine Director, Inpatient Diabetes University of California, San Francisco CLINICAL RECOGNITION Background: Appropriate inpatient glycemic
Lead Clinician(S) (DATE) Approved by Diabetes Directorate on: Approved by Medicines Safety Group on: This guideline should not be used after end of:
 Guideline for members of the diabetes team and dietetic department for advising on insulin dose adjustment and teaching the skills of insulin dose adjustment to adults with type 1 or type 2 diabetes mellitus
Guideline for members of the diabetes team and dietetic department for advising on insulin dose adjustment and teaching the skills of insulin dose adjustment to adults with type 1 or type 2 diabetes mellitus
Why is Insulin so Important?
 Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
Insulin Therapy Why is Insulin so Important? If the glucose stays in your blood it doesn t do your cells (body) any good The glucose has to get inside the cells for the body to use it What Does Insulin
Onset Peak Duration Comments
 Rapid- Acting 5-15 minutes 0.5-3 hours 3-5 hours Meal should be available before administering, ideally taking within 10 minutes of eating). Good in refrigerator (36-46 F) until expiration date. Protect
Rapid- Acting 5-15 minutes 0.5-3 hours 3-5 hours Meal should be available before administering, ideally taking within 10 minutes of eating). Good in refrigerator (36-46 F) until expiration date. Protect
Step-by-Step Patient Injection Guide
 Step-by-Step Patient Injection Guide 1 Your step-by-step guide to injection. 3 Table of Contents How your insulin works... 1 o Definitions to review Insulin action curves... 2 o Rapid-acting insulin o
Step-by-Step Patient Injection Guide 1 Your step-by-step guide to injection. 3 Table of Contents How your insulin works... 1 o Definitions to review Insulin action curves... 2 o Rapid-acting insulin o
Insulin Pens. Basic facts. What is insulin? What are the different types of insulin?
 UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
UW MEDICINE PATIENT EDUCATION Insulin Pens Basic facts This handout explains what insulin is, the different types of insulin, how to store it, how to give an injection with an insulin pen, and other important
insulin & diabetes What is insulin? Why must it be injected? What if I have to go on to insulin? Are there different types of insulin?
 Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Insulin and Diabetes
 Insulin What is Insulin? Insulin is a hormone produced by special cells in the pancreas These cells that are produced are called beta cells Insulin allows the glucose from food we eat to enter the cells
Insulin What is Insulin? Insulin is a hormone produced by special cells in the pancreas These cells that are produced are called beta cells Insulin allows the glucose from food we eat to enter the cells
Insulin onset, peak and duration of action
 Insulin onset, peak and duration of action Insulin was first discovered in the early 190 s. Before then, diabetes could not be treated. Insulin was then taken from cow and pig pancreases, but nearly all
Insulin onset, peak and duration of action Insulin was first discovered in the early 190 s. Before then, diabetes could not be treated. Insulin was then taken from cow and pig pancreases, but nearly all
Continuous Subcutaneous Insulin Infusion (CSII) pump therapy
 Continuous Subcutaneous Insulin Infusion (CSII) pump therapy GHPI1267_04_15 Department: Diabetes team Review due: April 2018 www.gloshospitals.nhs.uk 21 BETTER FOR YOU BETTER FOR YOU 1 Introduction This
Continuous Subcutaneous Insulin Infusion (CSII) pump therapy GHPI1267_04_15 Department: Diabetes team Review due: April 2018 www.gloshospitals.nhs.uk 21 BETTER FOR YOU BETTER FOR YOU 1 Introduction This
Surgery and Procedures in Patients with Diabetes
 Surgery and Procedures in Patients with Diabetes University Hospitals of Leicester NHS Trust DEFINITIONS Minor Surgery and Procedures: expected to be awake, eating and drinking by the next meal, total
Surgery and Procedures in Patients with Diabetes University Hospitals of Leicester NHS Trust DEFINITIONS Minor Surgery and Procedures: expected to be awake, eating and drinking by the next meal, total
Insulin pen start checklist
 Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
Insulin pen start checklist Topic Instruction Date & Initials 1. Cognitive Assessment 2. Insulin Delivery loading appropriate mixing priming shot dialing up dose delivery of insulin 3. Insulin type/action
at The Valley Hospital (TVH) for Nursing Students/Nursing Instructors 2012
 at The Valley Hospital (TVH) for Nursing Students/Nursing Instructors 2012 Subject - Insulin Safety Background Insulin known to be high risk medication Can promote serious hypoglycemia if given incorrectly
at The Valley Hospital (TVH) for Nursing Students/Nursing Instructors 2012 Subject - Insulin Safety Background Insulin known to be high risk medication Can promote serious hypoglycemia if given incorrectly
DIABETES MEDICATION INSULIN
 Section Three DIABETES MEDICATION INSULIN This section will tell you: About insulin. How to care and store your insulin. When to take your insulin. Different ways of taking insulin. WHAT IS INSULIN? Insulin
Section Three DIABETES MEDICATION INSULIN This section will tell you: About insulin. How to care and store your insulin. When to take your insulin. Different ways of taking insulin. WHAT IS INSULIN? Insulin
Inpatient Guidelines: Insulin Infusion Pump Management
 Inpatient Guidelines: Insulin Infusion Pump Management Developed by the Statewide Diabetes Clinical Network Steering Committee July 2012 Clinical Access and Redesign Unit Table of Contents Purpose...4
Inpatient Guidelines: Insulin Infusion Pump Management Developed by the Statewide Diabetes Clinical Network Steering Committee July 2012 Clinical Access and Redesign Unit Table of Contents Purpose...4
A Guide to Monitoring Blood Glucose for Patients with diabetes in Care Homes
 A Guide to Monitoring Blood Glucose for Patients with diabetes in Care Homes 1. Summary... 1 2. Background... 2 3. Purpose 2 4. Responsibilities. 2 5. Blood Glucose Monitoring. 2 6. Resident Groups that
A Guide to Monitoring Blood Glucose for Patients with diabetes in Care Homes 1. Summary... 1 2. Background... 2 3. Purpose 2 4. Responsibilities. 2 5. Blood Glucose Monitoring. 2 6. Resident Groups that
Insulin Safety. The safe use of insulin and you. Patient Information Booklet
 Insulin Safety The safe use of insulin and you The Right insulin The Right dose The Right way The Right time Hypoglycaemia Diabetes Patient Information Booklet Adapted from the National Patient Safety
Insulin Safety The safe use of insulin and you The Right insulin The Right dose The Right way The Right time Hypoglycaemia Diabetes Patient Information Booklet Adapted from the National Patient Safety
Glycaemic Control in Adults with Type 1 Diabetes
 Glycaemic Control in Adults with Type 1 Diabetes Aim(s) and objective(s) This document aims to provide guidance on good clinical practice in managing glycaemic control in adult patients with Type 1 Diabetes
Glycaemic Control in Adults with Type 1 Diabetes Aim(s) and objective(s) This document aims to provide guidance on good clinical practice in managing glycaemic control in adult patients with Type 1 Diabetes
INSULINThere are. T y p e 1 T y p e 2. many different insulins for
 T y p e 1 T y p e 2 INSULINThere are many different insulins for Characteristics The three characteristics of insulin are: Onset. The length of time before insulin reaches the bloodstream and begins lowering
T y p e 1 T y p e 2 INSULINThere are many different insulins for Characteristics The three characteristics of insulin are: Onset. The length of time before insulin reaches the bloodstream and begins lowering
Department of Health Commencing insulin therapy
 Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
Department of Health Commencing insulin therapy Great state. Great opportunity. State of Queensland (Queensland Health) 2008 2013 This work is licensed under a Creative Commons Attribution No Derivatives
INSULIN PUMP THERAPY
 INSULIN PUMP THERAPY Information Leaflet Your Health. Our Priority. Page 2 of 5 Insulin management plan for pregnant women using insulin pump therapy If at any point, you are not able to control your blood
INSULIN PUMP THERAPY Information Leaflet Your Health. Our Priority. Page 2 of 5 Insulin management plan for pregnant women using insulin pump therapy If at any point, you are not able to control your blood
Insulin Pump Therapy
 CHILDREN S SERVICES Insulin Pump Therapy These guidelines are not intended for starting a patient on an insulin pump. They are intended to give staff not part of the diabetic team information regarding
CHILDREN S SERVICES Insulin Pump Therapy These guidelines are not intended for starting a patient on an insulin pump. They are intended to give staff not part of the diabetic team information regarding
MANAGEMENT OF HYPOGLYCAEMIA IN ADULT PATIENTS
 This document is uncontrolled once printed. Please refer to the Trusts Intranet site for the most up to date version MANAGEMENT OF HYPOGLYCAEMIA IN ADULT PATIENTS NGH-GU-567 Document Reference Number:
This document is uncontrolled once printed. Please refer to the Trusts Intranet site for the most up to date version MANAGEMENT OF HYPOGLYCAEMIA IN ADULT PATIENTS NGH-GU-567 Document Reference Number:
insulin & diabetes What is insulin? Why must it be injected? What if I have to go on to insulin? Are there different types of insulin?
 Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Talking diabetes No.24 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with type 2 diabetes
Parenteral Dosage of Drugs
 Chapter 11 Parenteral Dosage of Drugs Parenteral Route of administration other than gastrointestinal Intramuscular (IM) Subcutaneous (SC) Intradermal (ID) IV Parenteral Most medications prepared in liquid
Chapter 11 Parenteral Dosage of Drugs Parenteral Route of administration other than gastrointestinal Intramuscular (IM) Subcutaneous (SC) Intradermal (ID) IV Parenteral Most medications prepared in liquid
Insulin Pens & Improving Patient Adherence
 Insulin Pens & Improving Patient Adherence Bonnie Pepon, RN, BSN, CDE Certified Diabetes Educator Conemaugh Diabetes Institute Kip Benko, MD FACEP Asst Clinical Professor University of Pittsburgh School
Insulin Pens & Improving Patient Adherence Bonnie Pepon, RN, BSN, CDE Certified Diabetes Educator Conemaugh Diabetes Institute Kip Benko, MD FACEP Asst Clinical Professor University of Pittsburgh School
Types of insulin and How to Use Them
 Diabetes and Insulin Pumps Amy S. Pullen Pharm.D ISHP Spring Meeting April 2012 Objectives Describe the different types of insulin used in diabetes Identify the types of insulin that are compatible with
Diabetes and Insulin Pumps Amy S. Pullen Pharm.D ISHP Spring Meeting April 2012 Objectives Describe the different types of insulin used in diabetes Identify the types of insulin that are compatible with
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org
 written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
written by Harvard Medical School Insulin Therapy Managing Your Diabetes www.patientedu.org What Is Insulin? The cells of your body need energy and one source of energy is sugar in your blood. Insulin
NSW Adult Subcutaneous Insulin Prescribing Chart User Guide
 NSW Adult Subcutaneous Insulin Prescribing Chart User Guide Adult Subcutaneous Insulin Prescribing Chart User Guide - 13 August 2013 Contents Target audience:... 1 Exceptions:... 1 1. Introduction... 2
NSW Adult Subcutaneous Insulin Prescribing Chart User Guide Adult Subcutaneous Insulin Prescribing Chart User Guide - 13 August 2013 Contents Target audience:... 1 Exceptions:... 1 1. Introduction... 2
Scottish Medicines Consortium
 Scottish Medicines Consortium insulin glulisine for subcutaneous injection 100 units/ml (Apidra ) No. (298/06) Sanofi Aventis 4 August 2006 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium insulin glulisine for subcutaneous injection 100 units/ml (Apidra ) No. (298/06) Sanofi Aventis 4 August 2006 The Scottish Medicines Consortium (SMC) has completed its assessment
Management of Diabetes Mellitus in Custody
 Recommendations The medico-legal guidelines and recommendations published by the Faculty are for general information only. Appropriate specific advice should be sought from your medical defence organisation
Recommendations The medico-legal guidelines and recommendations published by the Faculty are for general information only. Appropriate specific advice should be sought from your medical defence organisation
2. What Should Advocates Know About Diabetes? O
 2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
2. What Should Advocates Know About Diabetes? O ften a school district s failure to properly address the needs of a student with diabetes is due not to bad faith, but to ignorance or a lack of accurate
insulin & diabetes Talking diabetes No.24 Revised 2012
 Talking diabetes No.24 Revised 2012 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with
Talking diabetes No.24 Revised 2012 insulin & diabetes Insulin injections are required when the body produces little or no insulin, as with type 1 diabetes. They are also required for some people with
Therapy Insulin Practical guide to Health Care Providers Quick Reference F Diabetes Mellitus in Type 2
 Ministry of Health, Malaysia 2010 First published March 2011 Perkhidmatan Diabetes dan Endokrinologi Kementerian Kesihatan Malaysia Practical guide to Insulin Therapy in Type 2 Diabetes Mellitus Quick
Ministry of Health, Malaysia 2010 First published March 2011 Perkhidmatan Diabetes dan Endokrinologi Kementerian Kesihatan Malaysia Practical guide to Insulin Therapy in Type 2 Diabetes Mellitus Quick
PATIENT INFORMATION. Medicine To Treat: D iabetes. What You Need to Know About. Insulin
 PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
PATIENT INFORMATION Medicine To Treat: D iabetes What You Need to Know About Insulin INTRODUCTION The insulin preparations currently available in Singapore are mostly from human origin; pork or bovine
Diabetes Information
 Diabetes Information Your diabetes team includes: Consultant Paediatric Endocrinologist Paediatric Diabetes Clinical Nurse Specialists Senior Clinical Nutritionists/Dietitians Senior Clinical Psychologist
Diabetes Information Your diabetes team includes: Consultant Paediatric Endocrinologist Paediatric Diabetes Clinical Nurse Specialists Senior Clinical Nutritionists/Dietitians Senior Clinical Psychologist
Information for Patients
 Information for Patients Guidance for Diabetic Persons having bowel preparation for a flexible sigmoidoscopy or a colonoscopy or a combined gastroscopy and colonoscopy This guidance is provided to assist
Information for Patients Guidance for Diabetic Persons having bowel preparation for a flexible sigmoidoscopy or a colonoscopy or a combined gastroscopy and colonoscopy This guidance is provided to assist
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
Prior Authorization Guideline Guideline: PC (CO) - Insulin Delivery Systems Therapeutic Class: Hormones and Synthetic Substitutes Therapeutic Sub-Class: Insulin Delivery Systems Client: CO Approval Date:
Injectable Insulin During Pregnancy
 Injectable Insulin During Pregnancy What is insulin? Insulin is a hormone made by the pancreas. The pancreas is a small organ that lies behind and below the stomach. Insulin allows the food you eat to
Injectable Insulin During Pregnancy What is insulin? Insulin is a hormone made by the pancreas. The pancreas is a small organ that lies behind and below the stomach. Insulin allows the food you eat to
Anchor Bay School District Diabetic Medical Care Plan. Student Name Date Grade Teacher
 Rev: 4/2009 Anchor Bay School District Diabetic Medical Care Plan Place Child s Picture Here Student Name Date Grade Teacher Emergency Contact information (Please list in order to be called) #1 Parent
Rev: 4/2009 Anchor Bay School District Diabetic Medical Care Plan Place Child s Picture Here Student Name Date Grade Teacher Emergency Contact information (Please list in order to be called) #1 Parent
A patient guide to the use of insulin for diabetes
 A patient guide to the use of insulin for diabetes Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A patient guide to the use of insulin for diabetes Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Diabetes Fundamentals
 Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
Diabetes Fundamentals Prevalence of Diabetes in the U.S. Undiagnosed 10.7% of all people 20+ 23.1% of all people 60+ (12.2 million) Slide provided by Roche Diagnostics Sources: ADA, WHO statistics Prevalence
Guideline for the Administration of Insulin by Nursing Staff
 Guideline for the Administration of Insulin by Nursing Staff Aims and objectives In Lanarkshire the number of people with Diabetes on insulin treatment is growing, as both the population ages and people
Guideline for the Administration of Insulin by Nursing Staff Aims and objectives In Lanarkshire the number of people with Diabetes on insulin treatment is growing, as both the population ages and people
Resident s Guide to Inpatient Diabetes
 Resident s Guide to Inpatient Diabetes 1. All patients with diabetes of ANY TYPE, regardless of reason for admission, must have a Hemoglobin A1C documented in the medical record within 24 hours of admission
Resident s Guide to Inpatient Diabetes 1. All patients with diabetes of ANY TYPE, regardless of reason for admission, must have a Hemoglobin A1C documented in the medical record within 24 hours of admission
Insulin therapy in various type 1 diabetes patients workshop
 Insulin therapy in various type 1 diabetes patients workshop Bruce H.R. Wolffenbuttel, MD PhD Dept of Endocrinology, UMC Groningen website: www.umcg.net & www.gmed.nl Twitter: @bhrw Case no. 1 Male of
Insulin therapy in various type 1 diabetes patients workshop Bruce H.R. Wolffenbuttel, MD PhD Dept of Endocrinology, UMC Groningen website: www.umcg.net & www.gmed.nl Twitter: @bhrw Case no. 1 Male of
INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE
 INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE We welcome feedback on this policy and the way it operates. We are interested to know of any possible or actual adverse impact that this policy/procedure
INSULIN INITIATION IN TYPE 2 DIABETES IN PRIMARY CARE We welcome feedback on this policy and the way it operates. We are interested to know of any possible or actual adverse impact that this policy/procedure
Diabetes How to manage illness
 York Teaching Hospital NHS Foundation Trust Diabetes How to manage illness For adults with Type 1 diabetes on a basal bolus insulin regime For more information, please contact: Diabetes and Endocrinology
York Teaching Hospital NHS Foundation Trust Diabetes How to manage illness For adults with Type 1 diabetes on a basal bolus insulin regime For more information, please contact: Diabetes and Endocrinology
My Sick Day Plan for Type 1 Diabetes on an Insulin Pump
 My Sick Day Plan for Type 1 Diabetes on an Insulin Pump When you are sick, your blood sugar levels may be harder to keep under control. Your blood sugar may go too high or too low. Use this guide to help
My Sick Day Plan for Type 1 Diabetes on an Insulin Pump When you are sick, your blood sugar levels may be harder to keep under control. Your blood sugar may go too high or too low. Use this guide to help
Rapid Response Report NPSA/2010/RRR013: Safer administration of insulin
 Rapid Response Report NPSA/2010/RRR013: Safer administration of insulin June 2010 Supporting Information Contents 1. Introduction...2 2. Background...2 3. Review of evidence of harm...4 References...7
Rapid Response Report NPSA/2010/RRR013: Safer administration of insulin June 2010 Supporting Information Contents 1. Introduction...2 2. Background...2 3. Review of evidence of harm...4 References...7
Humulin R (U500) insulin: Prescribing Guidance
 Leeds Humulin R (U500) insulin: Prescribing Guidance Amber Drug Level 2 We have started your patient on Humulin R (U500) insulin for the treatment of diabetic patients with marked insulin resistance requiring
Leeds Humulin R (U500) insulin: Prescribing Guidance Amber Drug Level 2 We have started your patient on Humulin R (U500) insulin for the treatment of diabetic patients with marked insulin resistance requiring
Diabetes in Pregnancy: Management in Labour
 1. Purpose The standard management of labour applies to women with diabetes, and includes the following special considerations: Timing of birth. Refer to guideline: Diabetes Mellitus - Management of Pre-existing
1. Purpose The standard management of labour applies to women with diabetes, and includes the following special considerations: Timing of birth. Refer to guideline: Diabetes Mellitus - Management of Pre-existing
INSULIN INJECTION KNOW-HOW
 0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
0-0- INSULIN INJECTION KNOW-HOW Learning how to Congratulations for making the move to insulin therapy. It won t be long before you start enjoying better blood sugar control, more energy, and a host of
Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes
 Diabetes Sans Frontières Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes 1. Introduction This guideline has been developed in order to support practices to undertake insulin therapeutic
Diabetes Sans Frontières Guideline for Insulin Therapeutic Review in patients with Type 2 Diabetes 1. Introduction This guideline has been developed in order to support practices to undertake insulin therapeutic
SAMPLE. iabetes insulin use it safel. A patient information booklet for adults who have diabetes and use insulin. Diabetes: insulin, use it safely
 urther information Read this booklet and the Insulin Passport alongside all the other information about diabetes that your diabetes nurse or doctor has given to you. You will also need to read the technical
urther information Read this booklet and the Insulin Passport alongside all the other information about diabetes that your diabetes nurse or doctor has given to you. You will also need to read the technical
Getting started with Insulin Injections
 Getting started with Insulin Injections Table of Contents Introduction........................2 Insulin Injection Devices...............3 Blood Glucose Levels Hyperglycemia.....................15 Table
Getting started with Insulin Injections Table of Contents Introduction........................2 Insulin Injection Devices...............3 Blood Glucose Levels Hyperglycemia.....................15 Table
Insulin pump: advice for schools
 Insulin pump: advice for schools Information for school staff Dr Gray s Hospital Your pupil.. has Type 1 insulin dependent diabetes. This means that the pancreas has stopped making the hormone insulin.
Insulin pump: advice for schools Information for school staff Dr Gray s Hospital Your pupil.. has Type 1 insulin dependent diabetes. This means that the pancreas has stopped making the hormone insulin.
Dear Parent/Guardian and Physician of
 DIABETIC MANAGEMENT PLAN Parent Consent and Physician Authorization POWAY UNIFIED SCHOOL DISTRICT HEALTH SERVICES 15250 Avenue of Science San Diego CA 92128 Dear Parent/Guardian and Physician of California
DIABETIC MANAGEMENT PLAN Parent Consent and Physician Authorization POWAY UNIFIED SCHOOL DISTRICT HEALTH SERVICES 15250 Avenue of Science San Diego CA 92128 Dear Parent/Guardian and Physician of California
human insulin (prb) 30% soluble insulin 70% isophane insulin A Guide to Starting Humulin M3
 human insulin (prb) 30% soluble insulin 70% isophane insulin A Guide to Starting Humulin M3 This booklet is intended only for those who have been Prescribed Humulin M3. It is intended to be used in addition
human insulin (prb) 30% soluble insulin 70% isophane insulin A Guide to Starting Humulin M3 This booklet is intended only for those who have been Prescribed Humulin M3. It is intended to be used in addition
This guideline is for the management of Adult patients with Diabetes Mellitus using insulin pump therapy during admission to hospital
 CLINICAL GUIDELINE FOR THE MANAGEMENT OF ADULT PATIENTS DIABETES MELLITUS USING INSULIN PUMP THERAPY (Continuous Subcutaneous Insulin Infusion (CSII)), DURING ADMISSION TO HOSPITAL 1. Aim/Purpose of this
CLINICAL GUIDELINE FOR THE MANAGEMENT OF ADULT PATIENTS DIABETES MELLITUS USING INSULIN PUMP THERAPY (Continuous Subcutaneous Insulin Infusion (CSII)), DURING ADMISSION TO HOSPITAL 1. Aim/Purpose of this
THE INS AND OUTS OF INSULIN. Mary Beth Wald, RN,BSN,CDE
 THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
THE INS AND OUTS OF INSULIN Mary Beth Wald, RN,BSN,CDE WHAT HAPPENS IN MY BODY? When we eat, the food gets changed into glucose, a type of sugar. Glucose travels in the blood to all the cells in your body
ROYAL HOSPITAL FOR WOMEN
 ROYAL HOSPITAL FOR WOMEN LOCAL OPERATING PROCEDURE CLINICAL POLICIES, PROCEDURES & GUIDELINES Approved by Quality & Patient Safety Committee 17 April 2014 INSULIN INFUSION PROTOCOL INSULIN DEXTROSE INFUSION
ROYAL HOSPITAL FOR WOMEN LOCAL OPERATING PROCEDURE CLINICAL POLICIES, PROCEDURES & GUIDELINES Approved by Quality & Patient Safety Committee 17 April 2014 INSULIN INFUSION PROTOCOL INSULIN DEXTROSE INFUSION
Guidelines. for Sick Day Management for People with Diabetes
 Guidelines for Sick Day Management for People with Diabetes When to Follow Sick Day Guidelines These guidelines apply when the person with diabetes is feeling unwell or noticing signs of an illness and/
Guidelines for Sick Day Management for People with Diabetes When to Follow Sick Day Guidelines These guidelines apply when the person with diabetes is feeling unwell or noticing signs of an illness and/
End of Life Diabetes Care
 End of Life Diabetes Care Commissioned by Diabetes UK Supplementary Documents and Flowcharts Endorsed By: Diabetes Phases of End of Life and Medications A - Blue: All From Diagnosis Stable With Year Plus
End of Life Diabetes Care Commissioned by Diabetes UK Supplementary Documents and Flowcharts Endorsed By: Diabetes Phases of End of Life and Medications A - Blue: All From Diagnosis Stable With Year Plus
Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes.
 PROTOCOL Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes. A. This the revised protocol (April 2002) B. Review team Contact for correspondence: Dr Jill Colquitt
PROTOCOL Clinical and cost-effectiveness of continuous subcutaneous insulin infusion therapy in diabetes. A. This the revised protocol (April 2002) B. Review team Contact for correspondence: Dr Jill Colquitt
A Guide to Starting. Humalog Mix25
 A Guide to Starting Humalog Mix25 This booklet is intended only for those individuals who have been prescribed Humalog Mix 25. It is intended to be used in addition to the Patient Information Leaflet (PIL)
A Guide to Starting Humalog Mix25 This booklet is intended only for those individuals who have been prescribed Humalog Mix 25. It is intended to be used in addition to the Patient Information Leaflet (PIL)
User guide Basal-bolus Insulin Dosing Chart: Adult
 Contacts and further information Local contact Clinical pharmacy or visiting pharmacy Diabetes education service Director of Medical Services Visiting or local endocrinologist or diabetes physician For
Contacts and further information Local contact Clinical pharmacy or visiting pharmacy Diabetes education service Director of Medical Services Visiting or local endocrinologist or diabetes physician For
Insulin pens workshop Making the complex simple
 Agenda: Insulin doses Needles Insulin Pen Devices Insulin storage Key information (Patient &HCP) Injection sites Hypoglycaemia Home blood glucose testing Sick day advice Traveling Sharps Insulin pens workshop
Agenda: Insulin doses Needles Insulin Pen Devices Insulin storage Key information (Patient &HCP) Injection sites Hypoglycaemia Home blood glucose testing Sick day advice Traveling Sharps Insulin pens workshop
Medication Guide. SYMLIN (SĬM-lĭn) (pramlintide acetate) injection
 Page 1 Medication Guide SYMLIN (SĬM-lĭn) (pramlintide acetate) injection Read the Medication Guide and the Patient Instructions for Use that come with your SYMLIN product before you start using it and
Page 1 Medication Guide SYMLIN (SĬM-lĭn) (pramlintide acetate) injection Read the Medication Guide and the Patient Instructions for Use that come with your SYMLIN product before you start using it and
Clinical Guideline Diabetes management during surgery (adults)
 Clinical Guideline Diabetes management during surgery (adults) Standard 8 of the National Service Framework for Diabetes states that all children, young people and adults with diabetes admitted to hospital,
Clinical Guideline Diabetes management during surgery (adults) Standard 8 of the National Service Framework for Diabetes states that all children, young people and adults with diabetes admitted to hospital,
Shropshire Children s Diabetes Team Insulin Pump Training Workbook & Care Plan
 Shropshire Children s Diabetes Team Insulin Pump Training Workbook & Care Plan Table of Contents Overview of training for insulin pump starts... 3 On the initiation visit... 4 General pump Information
Shropshire Children s Diabetes Team Insulin Pump Training Workbook & Care Plan Table of Contents Overview of training for insulin pump starts... 3 On the initiation visit... 4 General pump Information
Blood Glucose - How to test
 Blood Glucose - How to test no nurse should use blood glucose monitoring equipment without complete training the ward manager is responsible for ensuring staff are trained in Blood Glucose testing Calibration
Blood Glucose - How to test no nurse should use blood glucose monitoring equipment without complete training the ward manager is responsible for ensuring staff are trained in Blood Glucose testing Calibration
Insulin T Y P E 1 T Y P E 2
 T Y P E 1 T Y P E 2 INSULIN There are many different insulins for many different situations and lifestyles. This section should help you and your doctor decide which insulin or insulins are best for you.
T Y P E 1 T Y P E 2 INSULIN There are many different insulins for many different situations and lifestyles. This section should help you and your doctor decide which insulin or insulins are best for you.
Diabetes Medical Management Plan (DMMP)
 Diabetes Medical Management Plan (DMMP) This plan should be completed by the student s personal diabetes health care team, including the parents/guardian. It should be reviewed with relevant school staff
Diabetes Medical Management Plan (DMMP) This plan should be completed by the student s personal diabetes health care team, including the parents/guardian. It should be reviewed with relevant school staff
Starting insulin treatment for people with type 2 diabetes. What you need to know
 Starting insulin treatment for people with type 2 diabetes What you need to know Contents Information 3 Any questions? 3 Glossary of terms 3 Why do I need insulin? 4 What does insulin do? 5 Why are there
Starting insulin treatment for people with type 2 diabetes What you need to know Contents Information 3 Any questions? 3 Glossary of terms 3 Why do I need insulin? 4 What does insulin do? 5 Why are there
Peri-Operative Guidelines for Management of Diabetes Patients
 Peri-Operative Guidelines for Management of Diabetes Patients Target blood glucose 6-10 mmol/l for all patients Acceptable blood glucose 4-11 mmol/l for all patients Definitions Non-Insulin Glucose Lowering
Peri-Operative Guidelines for Management of Diabetes Patients Target blood glucose 6-10 mmol/l for all patients Acceptable blood glucose 4-11 mmol/l for all patients Definitions Non-Insulin Glucose Lowering
INSULIN INJECTION KNOW-HOW
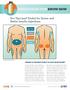 0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
Lothian Diabetes Handbook MANAGEMENT OF DIABETIC KETOACIDOSIS
 MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
MANAGEMENT OF DIABETIC KETOACIDOSIS 90 MANAGEMENT OF DIABETIC KETOACIDOSIS Diagnosis elevated plasma and/or urinary ketones metabolic acidosis (raised H + /low serum bicarbonate) Remember that hyperglycaemia,
A pictorial guide to diabetes care, supplies, and devices
 A pictorial guide to diabetes care, supplies, and devices Caution: This publication contains depictions of blood, needles and medical procedures related to diabetes care. This publication may be reproduced
A pictorial guide to diabetes care, supplies, and devices Caution: This publication contains depictions of blood, needles and medical procedures related to diabetes care. This publication may be reproduced
Planning Your Diabetes Care...
 My Doctor Says I Should Plan for Diabetes Care During a Disaster... What Do I Need to do? BD Getting Started Planning Your Diabetes Care... During Disaster Conditions In 1993, the Garden State Association
My Doctor Says I Should Plan for Diabetes Care During a Disaster... What Do I Need to do? BD Getting Started Planning Your Diabetes Care... During Disaster Conditions In 1993, the Garden State Association
Introduction to Insulin Pump Therapy
 Introduction to Insulin Pump Therapy What is an insulin pump and how does it work? An insulin pump is a small electronic device which provides a continuous infusion of very fast acting insulin (Novorapid
Introduction to Insulin Pump Therapy What is an insulin pump and how does it work? An insulin pump is a small electronic device which provides a continuous infusion of very fast acting insulin (Novorapid
Electronic copy to all appropriate staff Intranet Notification in Staff Focus Related Trust Policies (to be read in conjunction with)
 Diabetes Management for Children and Young People undergoing Surgery (0-16 yrs) Clinical Guideline Register No: 10096 Status: Public Developed in response to: Updated national guidelines Contributes to
Diabetes Management for Children and Young People undergoing Surgery (0-16 yrs) Clinical Guideline Register No: 10096 Status: Public Developed in response to: Updated national guidelines Contributes to
INJEX Self Study Program Part 1
 INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
INJEX Self Study Program Part 1 What is Diabetes? Diabetes is a disease in which the body does not produce or properly use insulin. Diabetes is a disorder of metabolism -- the way our bodies use digested
BOLUS INSULIN DOSAGES H. Peter Chase, MD and Erin Cobry, BS
 CHAPTER 6: BOLUS INSULIN DOSAGES H. Peter Chase, MD and Erin Cobry, BS WHAT IS BOLUS INSULIN? Bolus insulin dosages refer to the quick bursts of insulin given to cover the carbohydrates in meals or snacks
CHAPTER 6: BOLUS INSULIN DOSAGES H. Peter Chase, MD and Erin Cobry, BS WHAT IS BOLUS INSULIN? Bolus insulin dosages refer to the quick bursts of insulin given to cover the carbohydrates in meals or snacks
Volume 5; Number 16 October 2011
 Volume 5; Number 16 October 2011 This Bulletin provides an update on the current supply problems affecting insulin glulisine (Apidra) and on the planned discontinuation of Opticlik, Opticlik Pro 1 and
Volume 5; Number 16 October 2011 This Bulletin provides an update on the current supply problems affecting insulin glulisine (Apidra) and on the planned discontinuation of Opticlik, Opticlik Pro 1 and
Type 2 Diabetes. Management and Medication. HELPLINE: 01604 622837 www.iddtinternational.org
 I N D E P E N D E N T D I A B E T E S T R U S T Type 2 Diabetes Management and Medication A charity supporting and listening to people who live with diabetes HELPLINE: 01604 622837 www.iddtinternational.org
I N D E P E N D E N T D I A B E T E S T R U S T Type 2 Diabetes Management and Medication A charity supporting and listening to people who live with diabetes HELPLINE: 01604 622837 www.iddtinternational.org
