Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department
|
|
|
- Clifton Peters
- 7 years ago
- Views:
Transcription
1 The new england journal of medicine original article Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department Gregory J. Moran, M.D., Anusha Krishnadasan, Ph.D., Rachel J. Gorwitz, M.D., M.P.H., Gregory E. Fosheim, M.P.H., Linda K. McDougal, M.S., Roberta B. Carey, Ph.D., and David A. Talan, M.D., for the EMERGEncy ID Net Study Group* Abstract From the Department of Emergency Medicine (G.J.M., A.K., D.A.T.) and the Division of Infectious Diseases (G.J.M., D.A.T.), Olive View UCLA Medical Center, Sylmar, Calif.; and the Division of Healthcare Quality Promotion, National Center for Infectious Diseases, Centers for Disease Control and Prevention, Atlanta (R.J.G., G.E.F., L.K.M., R.B.C.). Address reprint requests to Dr. Moran at the Department of Emergency Medicine, Olive View UCLA Medical Center, Olive View Dr., North Annex, Sylmar, CA 91342, or at *Members of the EMERGEncy ID Net Study Group are listed in the Appendix. N Engl J Med 2006;355: Copyright 2006 Massachusetts Medical Society. Background Methicillin-resistant Staphylococcus aureus (MRSA) is increasingly recognized in infections among persons in the community without established risk factors for MRSA. Methods We enrolled adult patients with acute, purulent skin and soft-tissue infections presenting to 11 university-affiliated emergency departments during the month of August Cultures were obtained, and clinical information was collected. Available S. aureus isolates were characterized by antimicrobial-susceptibility testing, pulsed-field gel electrophoresis, and detection of toxin genes. On MRSA isolates, we performed typing of the staphylococcal cassette chromosome mec (SCCmec), the genetic element that carries the meca gene encoding methicillin resistance. Results S. aureus was isolated from 320 of 422 patients with skin and soft-tissue infections (76 percent). The prevalence of MRSA was 59 percent overall and ranged from 15 to 74 percent. Pulsed-field type USA300 isolates accounted for 97 percent of MRSA isolates; 74 percent of these were a single strain (USA ). SCCmec type IV and the Panton Valentine leukocidin toxin gene were detected in 98 percent of MRSA isolates. Other toxin genes were detected rarely. Among the MRSA isolates, 95 percent were susceptible to clindamycin, 6 percent to erythromycin, 60 percent to fluoroquinolones, 100 percent to rifampin and trimethoprim sulfamethoxazole, and 92 percent to tetracycline. Antibiotic therapy was not concordant with the results of susceptibility testing in 100 of 175 patients with MRSA infection who received antibiotics (57 percent). Among methicillin-susceptible S. aureus isolates, 31 percent were USA300 and 42 percent contained pvl genes. Conclusions MRSA is the most common identifiable cause of skin and soft-tissue infections among patients presenting to emergency departments in 11 U.S. cities. When antimicrobial therapy is indicated for the treatment of skin and soft-tissue infections, clinicians should consider obtaining cultures and modifying empirical therapy to provide MRSA coverage. 666
2 Methicillin-resistant staphylococcus aureus (MRSA) emerged in the 1960s as a cause of infection among patients exposed to the bacteria in health care settings. 1 More recently, MRSA infections have been reported among persons without such exposure (community-associated MRSA). 2,3 Community-associated outbreaks of MRSA infection have occurred among prisoners, intravenous-drug users, athletes, military trainees, and men who have sex with men. 4-6 Community-associated MRSA has primarily been described as a cause of skin and soft-tissue infections, but it has also been associated with sepsis and necrotizing pneumonia. 7-9 As compared with health care associated MRSA isolates, community-associated MRSA isolates tend to be resistant to fewer antibiotics, to produce different toxins, 10 and to have different types of the gene complex known as staphylococcal cassette chromosome mec (SCCmec); this complex contains the meca gene that confers methicillin resistance. 10 Pulsed-field gel electrophoresis (PFGE) and other methods have identified a small number of molecular types that have accounted for most community-associated MRSA isolates characterized in the United States. 11 Some institutions have a high prevalence of MRSA isolated from patients with sporadic skin and soft-tissue infections that are not associated with an outbreak. 12,13 However, data are limited regarding the prevalence of MRSA as a cause of skin and soft-tissue infections among patients in several communities throughout the United States and the S. aureus isolates associated with these infections. Therefore, we determined the prevalence of MRSA as a cause of skin infections among adult patients presenting to emergency departments in several geographically diverse, metropolitan areas in the United States. We also determined the bacteriologic characteristics of S. aureus isolated from skin and soft-tissue infections and evaluated factors potentially associated with MRSA infections of skin and soft tissue. Methods We conducted a prospective prevalence study involving adult patients with skin and soft-tissue infections who presented to hospitals in the EMERGEncy ID Net, a network of university-affiliated emergency departments in 11 U.S. cities: Albuquerque; Atlanta; Charlotte, N.C.; Kansas City, Mo.; Los Angeles; Minneapolis; New Orleans; New York; Philadelphia; Phoenix, Ariz.; and Portland, Oreg. These departments had a combined approximate total of 900,000 visits per year. 14 The study was approved by the institutional review board at each site. Patients 18 years of age or older presenting in August 2004 with purulent skin and soft-tissue infections of less than one week s duration (excluding perirectal abscesses) were enrolled in the study. Consent was obtained in writing at eight sites and orally with provision of an information sheet at three sites. Information on demographic characteristics, clinical presentation, potential risk factors for MRSA infection, and treatments provided was collected by emergency department physicians using standardized forms. Management decisions were made on an individual basis by physicians in the emergency department. Follow-up data were obtained by telephone approximately two to three weeks after enrollment. Specimens were obtained from the single largest area of infection with the use of sterile Dacron swabs and were processed and cultured at hospital laboratories according to standard techniques. 15 Each laboratory determined the antimicrobial susceptibility of S. aureus isolates to the panel of agents routinely tested at that laboratory. 16 Available S. aureus isolates were forwarded to the Centers for Disease Control and Prevention (CDC) for further characterization. The inducibility of clindamycin resistance was determined by the D-zone disk-diffusion test. 17 The presence of genes for staphylococcal enterotoxins A through E and H, toxic shock syndrome toxin 1 (TSST-1), and Panton Valentine leukocidin (pvl) and the type of SCCmec were determined by the polymerase chain reaction. All isolates were typed by PFGE with the use of SmaI restriction endonuclease. Additional methods are described in detail in the Supplementary Appendix (available with the full text of this article at Descriptive statistics were used to summarize the characteristics of the patients and the prevalence of MRSA. To identify potential risk factors for MRSA infection among patients with skin and soft-tissue infections, we calculated adjusted odds ratios and 95 percent confidence intervals. Variables associated with MRSA infection in bivariate analyses were explored further with the use of multivariate logistic regression. Audits of emergency department and laboratory logs for patients with a discharge diagnosis of ab- 667
3 The new england journal of medicine scess, cellulitis, or wound infection were conducted at all study sites (except Atlanta) to determine the proportion of patients meeting eligibility criteria who were enrolled in the study. Demographic and clinical characteristics of enrolled patients were compared with those of unenrolled patients. Results A total of 422 patients with skin and soft-tissue infections were enrolled. The median age was 39 years (range, 18 to 79; interquartile range, 28 to 47), and 62 percent were men. Race or ethnic group was determined by the clinicians: 49 percent of patients were non-hispanic blacks, 25 percent were non-hispanic whites, 22 percent were Hispanic, and 4 percent belonged to other groups. Infections were located on the upper extremities in 29 percent of patients, lower extremities in 27 percent, torso in 17 percent, perineum in 14 percent, and head and neck in 13 percent. Infections were classified as an abscess in 81 percent of patients, an infected wound in 11 percent, and as cellulitis with purulent exudate in 8 percent. S. aureus was isolated from skin and soft-tissue infections in 320 patients (76 percent); 249 of the S. aureus isolates (78 percent) were MRSA. MRSA was isolated from 59 percent of patients (Table 1). The prevalence of MRSA ranged from 15 to 74 percent, and MRSA was the most common identifiable cause of skin and soft-tissue infections in 10 of 11 emergency departments. MRSA was isolated from 61 percent of abscesses, 53 percent of purulent wounds, and 47 percent of cases of cellulitis with purulent exudate. Other organisms isolated from 1 percent or more of infections included 71 isolates of methicillin-susceptible S. aureus (MSSA) (17 percent); 30 isolates of streptococcus species (7 percent) including 6 group B streptococcus, 2 group A streptococcus, 3 non group A and non group B β-hemolytic streptococcus, 4 anaerobic or microaerophilic streptococcus, and 15 viridans group streptococcus; 12 isolates of coagulase-negative staphylococci (3 percent); and 6 isolates of Proteus mirabilis (1 percent). Cultures from 31 patients were polymicrobial; 10 of these patients had MRSA. No microorganism was isolated from 38 patients (9 percent). A total of 218 MRSA isolates (88 percent) and 55 MSSA isolates (77 percent) from 10 emergency departments were sent to the CDC for genetic and phenotypic characterization. The pulsed-field types of 216 of the MRSA isolates (99 percent) tested were characteristic of community-associated MRSA: 212 were type USA300, 2 were type USA400, and 2 were type USA ,18 Of 212 MRSA isolates Table 1. Bacterial Isolates from Purulent Skin and Soft-Tissue Infections in 11 U.S. Emergency Departments.* Site No. of Patients Enrolled (N = 422) MRSA (N = 249) MSSA (N = 71) Other Bacteria (N = 64) number (percent) No Bacterial Growth (N = 38) Albuquerque (60) 10 (24) 3 (7) 4 (10) Atlanta (72) 4 (12) 3 (9) 2 (6) Charlotte, N.C (68) 0 4 (16) 4 (16) Kansas City, Mo (74) 6 (10) 4 (7) 5 (9) Los Angeles (51) 6 (13) 8 (17) 9 (19) Minneapolis (39) 4 (14) 9 (32) 4 (14) New Orleans (67) 11 (16) 9 (13) 3 (4) New York 20 3 (15) 8 (40) 5 (25) 4 (20) Philadelphia (55) 12 (21) 12 (21) 2 (3) Phoenix, Ariz (60) 8 (27) 4 (13) 0 Portland, Oreg (54) 2 (15) 3 (23) 1 (8) * A total of 31 cultures, including 10 cultures from which MRSA was isolated, were polymicrobial. Because of rounding, percentages may not total 100. MSSA denotes methicillin-resistant Staphylococcus aureus. P<0.001 for the test for homogeneity of MRSA prevalence across sites. Other bacteria isolated were as follows: MSSA (17 percent), streptococcus species (7 percent), coagulase-negative staphylococci (3 percent), and Proteus mirabilis (1 percent). 668
4 characterized as type USA300, 156 (74 percent) had a single pulsed-field pattern (strain USA ). SCCmec type IV, characteristic of community-associated MRSA, 19 was found in 214 (98 percent) of the MRSA isolates, and pvl toxin genes were present in 213 (98 percent). Genes for staphylococcal enterotoxins A, B, C, D, E, and H and TSST-1 were identified in five or fewer MRSA isolates. Eight S. aureus isolates collected at the Atlanta site in April 2005 were similar to other study isolates with regard to PFGE and toxin characteristics. USA300 was also the most common pulsedfield type among MSSA isolates, accounting for 17 of 55 MSSA isolates (31 percent) sent to the CDC. Among these type USA300 isolates, 8 (47 percent) had a pulsed-field pattern closely related to that of the MRSA strain USA In addition, pvl genes were detected in 23 MSSA isolates (42 percent), including 17 (100 percent) of the isolates characterized as USA300. MRSA susceptibilities were as follows: 100 percent were susceptible to trimethoprim sulfamethoxazole (217 of 217) and to rifampin (186 of 186); 95 percent were susceptible to clindamycin (215 of 226), 92 percent to tetracycline (207 of 226), 60 percent to fluoroquinolones (106 of 176), and 6 percent to erythromycin (13 of 226). Although the proportion of all S. aureus isolates (MRSA and MSSA) that were resistant to clindamycin was less than 15 percent at 10 of the study sites, 6 of 10 S. aureus isolates from New York City (60 percent) were resistant to clindamycin. Among the isolates that were sent to the CDC, 11 of 218 MRSA isolates (5 percent) and 7 of 55 MSSA isolates (13 percent) were not susceptible to clindamycin, including 4 (2 percent) MRSA isolates and 5 (9 percent) MSSA isolates with inducible clindamycin resistance detected by an antimicrobialsusceptibility D-zone disk-diffusion test. Sixty-six patients with MRSA infections (27 percent) had one or more established risk factors for health care associated MRSA; these included 43 patients who had been hospitalized within the past year, 28 with a history of MRSA infection, 2 who resided in a long-term care facility, and 1 who was undergoing dialysis. Isolates from 55 of these patients were evaluated at the CDC, and 54 (98 percent) had pulsed-field types characteristic of community-associated MRSA. Features associated with the isolation of MRSA as compared with the isolation of any other bacteria (Table 2) included antibiotic use in the month before enrollment, the presence of an abscess or a lesion attributed to a spider bite at enrollment, history of MRSA infection, and a recent history of close contact with someone with a similar skin infection. The presence of an underlying illness and characterization as belonging to the other category of race or ethnic background were negatively associated with the isolation of MRSA. In multivariate logistic-regression analyses, all these factors were associated with MRSA infection, with the exception of the presence of an abscess (Table 3). Black race was independently associated with MRSA infection. Controlling for study site did not affect the association between any of these factors and MRSA infection. Among 64 patients with none of these factors, 31 (48 percent) were infected with MRSA. The only factor that was significantly associated with isolation of MRSA, as compared with MSSA, was the presence of abscess at enrollment (odds ratio, 2.3; 95 percent confidence interval, 1.2 to 4.4). Complete information about treatment was available for 406 of the 422 patients (96 percent). Of these, 79 (19 percent) were treated with incision and drainage alone, 39 (10 percent) received antibiotics alone, 267 (66 percent) were treated with both incision and drainage and antibiotics, and 21 (5 percent) neither underwent incision and drainage nor received antibiotics. Of 400 patients for whom information about the outcome was available, 59 (15 percent) were admitted to the hospital. An antistaphylococcal penicillin or cephalosporin was given to 198 of 311 patients who received antibiotics (64 percent). In 100 of 175 MRSA infections for which antibiotic treatment was provided (57 percent), antibiotic therapy was not concordant with the results of susceptibility testing. Of the 422 patients, 248 (59 percent) were contacted for follow-up 15 to 21 days (median, 17) after their visit to the emergency department, and 238 (96 percent) of those patients who were contacted for follow-up reported that their infection had resolved or improved. There were no significant differences in the outcome between patients infected with MRSA and those infected with other bacteria or between patients in whom the infecting MRSA isolate was resistant and those in whom the isolate was susceptible to the prescribed antibiotic. Baseline characteristics were similar for patients with and those without follow-up information. 669
5 The new england journal of medicine Table 2. Potential Risk Factors for Infection with MRSA, as Compared with Other Bacteria, in Patients with Purulent Skin and Soft-Tissue Infections in 11 U.S. Emergency Departments.* MRSA (N = 249) Other Bacteria (N = 135) Odds Ratio (95% CI) Risk Factor no./total no. (%) Race or ethnic group Non-Hispanic white 61/247 (25) 37/135 (27) 1.0 Non-Hispanic black 134/247 (54) 53/135 (39) 1.6 ( ) Hispanic 48/247 (19) 36/135 (27) 0.8 ( ) Other 4/247 (2) 9/135 (7) 0.3 ( ) Intravenous-drug user 26/244 (11) 11/135 (8) 1.3 ( ) Taken any antibiotic in past mo 84/245 (34) 24/134 (18) 2.4 ( ) Taking antibiotic for the infection 61/244 (25) 24/134 (18) 1.5 ( ) Prison or jail in past yr 53/244 (22) 19/135 (14) 1.7 ( ) Competitive sports involving contact in past mo 21/246 (9) 8/135 (6) 1.5 ( ) Homeless in past yr 40/246 (16) 17/135 (13) 1.3 ( ) Abscess 203/243 (84) 97/131 (74) 1.8 ( ) Spontaneous infection (no apparent precipitating factor) 100/248 (40) 49/135 (36) 1.2 ( ) Reported spider bite 71/248 (29) 17/135 (13) 2.8 ( ) Underlying illness 25/249 (10) 34/135 (25) 0.3 ( ) HIV infection 11/249 (4) 4/135 (3) 1.5 ( ) History of MRSA infection 28/242 (12) 5/132 (4) 3.3 ( ) Hospitalized in past yr 43/247 (17) 32/135 (24) 0.7 ( ) Resident in long-term care facility 2/244 (1) 2/134 (1) 0.6 ( ) Health care worker 17/244 (7) 5/135 (4) 1.9 ( ) Homosexual male contact 7/132 (5) 5/79 (6) 0.8 ( ) Close contact with person with similar infection 43/245 (18) 8/135 (6) 3.4 ( ) Household contact with MRSA infection 15/245 (6) 3/131 (2) 2.8 ( ) Household contact with health care exposure 46/249 (18) 30/135 (22) 0.8 ( ) Household contact with jail exposure 42/243 (17) 15/131 (11) 1.6 ( ) Household contact with intravenous-drug use 27/245 (11) 11/133 (8) 1.4 ( ) * CI denotes confidence interval, and HIV human immunodeficiency virus. Missing data were excluded in these calculations. Information regarding race was missing for two patients. This group served as the reference group for other race variables. P<0.05. This category includes hospitalization or residence in a long-term care facility in past year, employment as a health care worker, receipt of dialysis, or presence of an indwelling catheter or tube. Case-finding audits revealed that approximately 42 percent of eligible patients were enrolled. As compared with enrolled patients, unenrolled patients were similar in terms of age (mean, 38 years; range, 18 to 82), sex (63 percent were male), and race or ethnic group (57 percent were white non- Hispanic or Hispanic, 39 percent were black, and 4 percent were in other groups). MRSA was isolated in 135 of 236 eligible but unenrolled patients from whom wound cultures were obtained (57 percent). Discussion MRSA has emerged as the most common identifiable cause of skin and soft-tissue infections in several metropolitan areas across the United States. Although more than 80 percent of patients with 670
6 skin and soft-tissue infections associated with MRSA in this study received empirical antimicrobial therapy for their infection, the infecting isolate was resistant to the agent prescribed for 57 percent of these patients. This finding suggests a need to reconsider empirical antimicrobial choices for skin and soft-tissue infections in areas where MRSA is prevalent in the community. Our findings are consistent with the dramatic trend of increasing reports of outbreaks and increased prevalence of community-associated MRSA during the past few years. MRSA was uncommon in community-acquired skin and soft-tissue infections before 2000 and accounted for only 3 percent of staphylococcal isolates submitted to Minnesota laboratories in Between 2001 and 2004, the prevalence of MRSA among patients with skin and soft-tissue infections at our Los Angeles institution increased from 29 percent to 64 percent. 13 Virtually all (99 percent) MRSA strains isolated from skin and soft-tissue infections in this study had pulsed-field types characteristic of community-associated MRSA, even though more than 25 percent of patients had established risk factors for health care associated MRSA. A single pulsed-field type (USA300) accounted for 97 percent of MRSA isolates and 31 percent of MSSA isolates. A single strain (USA ) associated with previously reported community outbreaks 5 accounted for 72 percent of MRSA isolates, and a closely related strain was the single most common MSSA strain identified. Pulsed-field type USA300 has been linked to community-associated MRSA outbreaks throughout the country 5,11 and represents the leading cause of communityassociated MRSA in single-center prevalence studies. 12,21 USA300 has rapidly replaced other pulsedfield types to become predominant among centers that have conducted longitudinal studies. 22 Our finding of the genetic similarity of MRSA and MSSA isolates from community-associated infections is consistent with previous reports. 7,8,21,23 This similarity suggests the acquisition of SCCmec by S. aureus strains established in the community or the loss of SCCmec by community-associated MRSA strains. The predominance of isolates from one genetic background may be related to virulence or transmissibility factors that confer unusual fitness. Ninety-eight percent of MRSA isolates and more than 40 percent of MSSA isolates in our study contained pvl genes; these findings are Table 3. Results of Multivariate Logistic-Regression Analyses to Identify Potential Risk Factors for MRSA Infection.* Adjusted Odds Ratio Characteristic (95% CI)* Race Non-Hispanic white 1.0 Non-Hispanic black 1.9 ( ) Other 0.3 ( ) Use of any antibiotic in past mo (vs. no use) 2.4 ( ) Reported spider bite (vs. other cause of infection) 3.0 ( ) Underlying illness (vs. no underlying infection) 0.3 ( ) History of MRSA infection (vs. absence of such history) 3.4 (1.1 10) Close contact with person with similar infection 3.8 ( ) (vs. no close contact) * Estimates were adjusted for all other variables in the table. CI denotes confidence interval. This group served as the reference group for other race variables. consistent with other recent reports. 24,25 S. aureus strains containing pvl genes have been associated with spontaneous skin and soft-tissue infections and necrotizing pneumonia; however, the role of pvl toxin in the pathogenesis of S. aureus skin and soft-tissue infections has not been fully elucidated. 26 Most patients in our study were treated with β-lactam agents such as cephalexin and dicloxacillin, to which MRSA isolates are not susceptible. Although we had limited follow-up information, we found no association between patients outcomes and the susceptibility of the pathogen to the prescribed antimicrobial agents. This absence of an association, which is consistent with previous reports, 3,27 suggests that most simple skin abscesses, even when caused by MRSA, can be cured with adequate drainage alone. Nonetheless, when antibiotics are clinically indicated and MRSA is prevalent in the community, it is difficult to justify empirical use of agents known to be inactive against MRSA. The susceptibility of a given pathogen to prescribed antimicrobial agents may be more likely to affect the outcome among patients with cellulitis or purulent wounds. Unfortunately, there were insufficient numbers of these patients with follow-up information in our study to assess this relationship. Although we identified several clinical and epidemiologic factors associated with MRSA infection, it does not appear that the presence or absence of these factors would be useful to guide decisions about the 671
7 The new england journal of medicine use of empirical antibiotics. Most patients without MRSA had at least one of these factors, and almost half of those without any of these factors were found to have MRSA. Various antimicrobial agents, such as clindamycin, trimethoprim sulfamethoxazole, and doxycycline, have been recommended for outpatient empirical treatment of community-associated skin and soft-tissue infections that may be attributable to MRSA More than 90 percent of MRSA isolates in our study were susceptible to each of these agents. Likewise, 100 percent of the MRSA isolates were susceptible to rifampin. Although resistance to rifampin monotherapy has occurred rapidly, the combination of rifampin plus trimethoprim sulfamethoxazole has been shown to eradicate MRSA colonization and has been suggested for the treatment of MRSA infection in the community. 31 Resistance to macrolides and fluoroquinolones was prevalent among MRSA isolates in this and other studies. 3,12,13 Although the prevalence of clindamycin resistance, including inducible resistance, was low overall, it varied geographically. Clindamycin has been used successfully in the treatment of infections with MRSA isolates possessing inducible resistance. 29,32 However, clinical treatment failures have also been reported. 33 Therefore, if clindamycin therapy is being considered, S. aureus isolates with the potential for inducible clindamycin resistance (i.e., isolates resistant to erythromycin but susceptible to clindamycin on initial testing) should be evaluated for inducible resistance by D-zone disk-diffusion testing. 17 Patients with nonpurulent cellulitis were not included in our study. Previous studies have shown that a large proportion of cellulitis may be attributable to group A streptococcus. 34 In contrast, among infections characterized as cellulitis with purulent drainage in our study, MRSA was isolated from 47 percent and group A streptococcus was rarely isolated. Although generally susceptible in vitro to clindamycin, most group A streptococci are resistant to trimethoprim sulfamethoxazole. To provide coverage for streptococcal infection, the use of clindamycin or a combination of a β-lactam plus trimethoprim sulfamethoxazole may be preferable for nonpurulent cellulitis. Optimal empirical therapy for severely ill hospitalized patients with complicated skin and softtissue infections has not been established; however, broad-spectrum intravenous therapy including an agent such as vancomycin for MRSA coverage remains appropriate. One study reported that clindamycin therapy was successful in children with invasive community-associated MRSA infections. 29 In recent randomized clinical trials, newer agents with MRSA activity had efficacy similar (daptomycin and tigecycline) or superior (linezolid) to that of vancomycin for the treatment of complicated skin and soft-tissue infections or skin and soft-tissue infections associated with MRSA As compared with patients with other bacterial infections of the skin, patients with MRSA infection were more likely to report a spider bite as the reason for their skin lesion, perhaps because of the propensity for MRSA strains circulating in the community to cause painful lesions in the absence of previous skin trauma. Thus, clinicians should consider the possibility of MRSA infection in patients who report spider bites. Eighteen percent of patients with skin and soft-tissue infections associated with MRSA reported close contact with a person who had a similar infection. This finding highlights the importance of educating patients about methods to prevent further transmission of infection, including keeping lesions covered with clean, dry bandages; practicing good hand hygiene; and avoiding the sharing of contaminated items. The high prevalence of MRSA among patients with community-associated skin and soft-tissue infections has implications for hospital policies regarding infection control. Standard precautions (including the use of gowns and gloves by health care workers for contact with wound drainage) should be used for all patients. Contact precautions, which include the use of gowns and gloves for all contact with patients or their environment, have been recommended for patients in acute care inpatient facilities who are known to be infected or colonized with MRSA. 38 Our results suggest that strategies used for patients with confirmed MRSA infections should be considered for all patients with purulent skin and soft-tissue infections in areas with a high prevalence of MRSA. In many U.S. cities, MRSA is now the most common pathogen isolated in the emergency department from patients with skin and soft-tissue infections. Clinicians should consider obtaining cultures from patients with skin and soft-tissue infections and modifying standard empirical therapy to provide MRSA coverage when antibiotics are indicated. Further studies are needed to 672
8 determine the extent of this infection in other locations, follow trends in antimicrobial susceptibility, and identify optimal therapy. Supported by a cooperative agreement (U50/CCU912342) with the CDC. The findings and conclusions of this report are those of the authors and do not necessarily represent the views of the funding agency. Dr. Moran reports having received consulting fees from or having served on advisory boards for Schering-Plough and Pfizer; lecture fees from Schering-Plough, Pfizer, Aventis, and Cubist; and research support from Pfizer and Aventis. Dr. Talan reports having received consulting fees from or having served on advisory boards for Pfizer and Ortho-McNeil; lecture fees from Schering-Plough; and research support from Pfizer and Aventis. No other potential conflict of interest relevant to this article was reported. We are indebted to Daniel Jernigan, Sigrid McAllister, Jean Patel, David Lonsway, George Killgore, Brandi Limbago, and Laura Jevitt at the CDC for providing technical and laboratory assistance; to the following site research coordinators: Ricky Amii, Cynthia Nguyen, Deborah Sibley, Mehr Merabodi, Carolyn Oakes, Marlena Wald, Tove Ryman, Yvonne Sanchez, Joni Kopitzke, Karen Pfaff, Sara Newton, Mary Mulrow, and Carol Von Hofen; and to the physicians at our study sites who assisted with data collection. appendix The following investigators participated in the EMERGEncy ID Net Study Group: Olive View University of California at Los Angeles Medical Center, Sylmar: F.M. Abrahamian; Hennepin County Medical Center, Minneapolis: M. Biros; University of New Mexico Health Sciences Center, Albuquerque: P.R. Cheney; Bellevue Hospital Center, New York: W.K. Chiang; Louisiana State University Health Science Center, New Orleans: L.M. Dunbar; Maricopa Medical Center, Phoenix, Ariz.: E. Gross; Emory University School of Medicine, Atlanta: K.L. Heilpern; Oregon Health Sciences University, Portland: J. Jui; Temple University School of Medicine, Philadelphia: D.J. Karras; University of Missouri Kansas City, Kansas City: M.T. Steele; Carolinas Medical Center, Charlotte, N.C.: M. Sullivan. References 1. Barrett FF, McGehee RF Jr, Finland M. Methicillin-resistant Staphylococcus aureus at Boston City Hospital: bacteriologic and epidemiologic observations. N Engl J Med 1968;279: Herold BC, Immergluck LC, Maranan MC, et al. Community-acquired methicillin-resistant Staphylococcus aureus in children with no identified predisposing risk. JAMA 1998;279: Fridkin SK, Hageman JC, Morrison M, et al. Methicillin-resistant Staphylococcus aureus disease in three communities. N Engl J Med 2005;352: [Erratum, N Engl J Med 2005;352:2362.] 4. Outbreaks of community-associated methicillin-resistant Staphylococcus aureus skin infections Los Angeles County, California, MMWR Morb Mortal Wkly Rep 2003;52: Kazakova SV, Hageman JC, Matava M, et al. A clone of methicillin-resistant Staphylococcus aureus among professional football players. N Engl J Med 2005;352: Zinderman CE, Conner B, Malakooti MA, LaMar JE, Armstrong A, Bohnker BK. Community-acquired methicillin-resistant Staphylococcus aureus among military recruits. Emerg Infect Dis 2004;10: Gonzalez BE, Martinez-Aguilar G, Hulten KG, et al. Severe staphylococcal sepsis in adolescents in the era of communityacquired methicillin-resistant Staphylococcus aureus. Pediatrics 2005;115: Mongkolrattanothai K, Boyle S, Kahana MD, Daum RS. Severe Staphylococcus aureus infections caused by clonally related community-acquired methicillin-susceptible and methicillin-resistant isolates. Clin Infect Dis 2003;37: Francis JS, Doherty MC, Lopatin U, et al. Severe community-onset pneumonia in healthy adults caused by methicillin- resistant Staphylococcus aureus carrying the Panton-Valentine leukocidin genes. Clin Infect Dis 2005;40: Naimi TS, LeDell KH, Como-Sabetti K, et al. Comparison of community- and health care-associated methicillin-resistant Staphylococcus aureus infection. JAMA 2003;290: McDougal LK, Steward CD, Killgore GE, Chaitram JM, McAllister SK, Tenover FC. Pulsed-field gel electrophoresis typing of oxacillin-resistant Staphylococcus aureus isolates from the United States: establishing a national database. J Clin Microbiol 2003;41: Frazee BW, Lynn J, Charlebois ED, Lambert L, Lowery D, Perdreau-Remington F. High prevalence of methicillinresistant Staphylococcus aureus in emergency department skin and soft tissue infections. Ann Emerg Med 2005;45: Moran GJ, Amii RN, Abrahamian FM, Talan DA. Methicillin-resistant Staphylococcus aureus in community-acquired skin infections. Emerg Infect Dis 2005;11: Talan DA, Moran GJ, Mower W, et al. EMERGEncy ID NET: an emergency department-based emerging infections sentinel network. Ann Emerg Med 1998;32: Bannerman TL. Staphylococci and other catalase positive cocci that grow aerobically. In: Murray PR, Baron EJ, Jogensen JH, eds. Manual of clinical microbiology. 8th ed. Washington, D.C.: ASM Press, 2003: Performance standards for antimicrobial susceptibility testing: 14th informational supplement. M1000-S14. Wayne, Pa.: National Committee for Clinical Laboratory Standards, Performance standards for antimicrobial susceptibility testing: 16th informa- tional supplement. M100-S16. Wayne, Pa.: Clinical and Laboratory Standards Institute, Pan ES, Diep BA, Charlebois ED, et al. Population dynamics of nasal strains of methicillin-resistant Staphylococcus aureus and their relation to community-associated disease activity. J Infect Dis 2005; 192: Daum RS, Ito T, Hiramatsu K, et al. A novel methicillin-resistance cassette in community-acquired methicillin-resistant Staphylococcus aureus isolates of diverse genetic backgrounds. J Infect Dis 2002;186: Naimi TS, LeDell KH, Boxrud DJ, et al. Epidemiology and clonality of community-acquired methicillin-resistant Staphylococcus aureus in Minnesota, Clin Infect Dis 2001;33: Mishaan AM, Mason EO Jr, Martinez- Aguilar G, et al. Emergence of a predominant clone of community-acquired Staphylococcus aureus among children in Houston, Texas. Pediatr Infect Dis J 2005;24: Chavez-Bueno S, Bozdogan B, Katz K, et al. Inducible clindamycin resistance and molecular epidemiologic trends of pediatric community-acquired methicillinresis tant Staphylococcus aureus in Dallas, Texas. Antimicrob Agents Chemother 2005; 49: Adem PV, Montgomery CP, Husain AN, et al. Staphylococcus aureus sepsis and the Waterhouse Friderichsen syndrome in children. N Engl J Med 2005;353: Yamasaki O, Kaneko J, Morizane S, et al. The association between Staphylococcus aureus strains carrying Panton-Valentine leukocidin genes and the development of deep-seated follicular infection. Clin Infect Dis 2005;40: Issartel B, Tristan A, Lechevallier S, et al. Frequent carriage of Panton-Valentine 673
9 leucocidin genes by Staphylococcus aureus isolates from surgically drained abscesses. J Clin Microbiol 2005;43: Lina G, Piemont Y, Godail-Gamot F, et al. Involvement of Panton-Valentine leukocidin-producing Staphylococcus aureus in primary skin infections and pneumonia. Clin Infect Dis 1999;29: Lee MC, Rios AM, Aten MF, et al. Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2004;23: Kaplan SL. Treatment of communityassociated methicillin-resistant Staphylococcus aureus infections. Pediatr Infect Dis J 2005;24: Martinez-Aguilar G, Hammerman WA, Mason EO Jr, Kaplan SL. Clindamycin treatment of invasive infections caused by community-acquired, methicillin-resistant and methicillin-susceptible Staphylo- coccus aureus in children. Pediatr Infect Dis J 2003;22: Rybak MJ, LaPlante KL. Communityassociated methicillin-resistant Staphylococcus aureus: a review. Pharmacotherapy 2005; 25: Chambers HF. Treatment of infection and colonization caused by methicillinresistant Staphylococcus aureus. Infect Control Hosp Epidemiol 1991;12: Drinkovic D, Fuller ER, Shore KP, Holland DJ, Ellis-Pegler R. Clindamycin treatment of Staphylococcus aureus expressing inducible clindamycin resistance. J Antimicrob Chemother 2001;48: Siberry GK, Tekle T, Carroll K, Dick J. Failure of clindamycin treatment of methicillin-resistant Staphylococcus aureus expressing inducible clindamycin resistance in vitro. Clin Infect Dis 2003;37: Bernard P, Bedane C, Mounier M, Denis F, Catanzano G, Bonnetblanc JM. Streptococcal cause of erysipelas and cel- lulitis in adults: a microbiologic study using a direct immunofluorescence technique. Arch Dermatol 1989;125: Weigelt J, Itani K, Stevens D, et al. Linezolid versus vancomycin in treatment of complicated skin and soft tissue infections. Antimicrob Agents Chemother 2005; 49: Carpenter CF, Chambers HF. Daptomycin: another novel agent for treating infections due to drug-resistant gram-positive pathogens. Clin Infect Dis 2004;38: Nathwani D. Tigecycline: clinical evidence and formulary positioning. Int J Antimicrob Agents 2005;25: Garner JS. Guidelines for isolation precautions in hospitals. Part I. Evolution of isolation practices. Am J Infect Control 1996;24: Copyright 2006 Massachusetts Medical Society. PERSONAL ARCHIVES IN THE JOURNAL ONLINE Individual subscribers can store articles and searches using a feature on the Journal s Web site ( called Personal Archive. Each article and search result links to this feature. Users can create personal folders and move articles into them for convenient retrieval later. 674
Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults
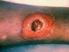 1 of 6 9/24/2010 11:16 AM Official reprint from UpToDate www.uptodate.com 2010 UpToDate Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults Author
1 of 6 9/24/2010 11:16 AM Official reprint from UpToDate www.uptodate.com 2010 UpToDate Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults Author
Interim Guidelines for the Management of Community-Associated Methicillin-Resistant Staphylococcus aureus Infections in Primary Care February 2006
 Table of Contents 1. Background... 2 2. Diagnosis... 2 3. Susceptibility Patterns of MRSA... 3 4. Management... 3 5. Decolonization of the Patient... 4 6. Prevention and Control... 5 7. Information for
Table of Contents 1. Background... 2 2. Diagnosis... 2 3. Susceptibility Patterns of MRSA... 3 4. Management... 3 5. Decolonization of the Patient... 4 6. Prevention and Control... 5 7. Information for
 Skin and Soft tissue Infections: new bugs, old drugs Disclosure Statement Sponsor: Goodman Photographic Presented by: Dr. Kristopher Wiebe, MD, CCFP (EM) Presented to: BC Chapter, Canadian Society of Hospital
Skin and Soft tissue Infections: new bugs, old drugs Disclosure Statement Sponsor: Goodman Photographic Presented by: Dr. Kristopher Wiebe, MD, CCFP (EM) Presented to: BC Chapter, Canadian Society of Hospital
Methicillin-resistant S taphylococcus
 Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection
 REVIEW ARTICLE Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection Robert C. Moellering, Jr. Beth Israel Deaconess Medical Center, Harvard Medical School,
REVIEW ARTICLE Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection Robert C. Moellering, Jr. Beth Israel Deaconess Medical Center, Harvard Medical School,
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY. Methicillin-resistant Staph aureus: Management in the Outpatient Setting
 EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections
 ARTICLES Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections AUTHORS: Aaron E. Chen, MD, a Karen C. Carroll, MD, b Marie Diener-West, PhD, c Tracy Ross,
ARTICLES Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections AUTHORS: Aaron E. Chen, MD, a Karen C. Carroll, MD, b Marie Diener-West, PhD, c Tracy Ross,
Received 20 March 2007/Returned for modification 10 July 2007/Accepted 27 August 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED
 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections
 Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Federal Bureau of Prisons Clinical Practice Guidelines April 2012 Clinical guidelines are made available to the public for informational
Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Federal Bureau of Prisons Clinical Practice Guidelines April 2012 Clinical guidelines are made available to the public for informational
It s Not a Spider Bite, It s Community-Acquired
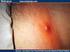 BRIEF REPORTS It s Not a Spider Bite, It s Community-Acquired Methicillin-Resistant Staphylococcus aureus Tamara J. Dominguez, MD Skin and soft tissue infections caused by hospitalacquired methicillin-resistant
BRIEF REPORTS It s Not a Spider Bite, It s Community-Acquired Methicillin-Resistant Staphylococcus aureus Tamara J. Dominguez, MD Skin and soft tissue infections caused by hospitalacquired methicillin-resistant
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Staphylococcus aureus Bloodstream Infection Treatment Guideline
 Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
MRSA, Hand Hygiene and Contact Precautions
 MRSA, Hand Hygiene and Contact Precautions Wesley Medical Center Department of Education May 2007 Authors: Lois Rahal, RN, BSN, CIC Brandy Jackson, RN, BSN Hope Helferich, RNC, BSN 1 Objectives Upon completion
MRSA, Hand Hygiene and Contact Precautions Wesley Medical Center Department of Education May 2007 Authors: Lois Rahal, RN, BSN, CIC Brandy Jackson, RN, BSN Hope Helferich, RNC, BSN 1 Objectives Upon completion
PRIORITY RESEARCH TOPICS
 PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings
 Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Introduction to Infection Control
 CHAPTER 3 Introduction to Infection Control George Byrns and Mary Elkins Learning Objectives 1 Define terms used in infection control. 2. Review significant risk factors for infection. 3. Identify the
CHAPTER 3 Introduction to Infection Control George Byrns and Mary Elkins Learning Objectives 1 Define terms used in infection control. 2. Review significant risk factors for infection. 3. Identify the
Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG)
 Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG) Clinical Practice Guideline Protocol Approved by: Division of Pediatric Emergency Medicine Date of Approval: 4/14 2013 SSM
Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG) Clinical Practice Guideline Protocol Approved by: Division of Pediatric Emergency Medicine Date of Approval: 4/14 2013 SSM
How Common is MRSA in Adult Septic Arthritis?
 INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I)
 ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus Bacteraemia Annual Report, Part I The annual
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus Bacteraemia Annual Report, Part I The annual
Develop an understanding of the differential diagnosis of pseudomembranous colitis
 Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
Does referral from an emergency department to an. alcohol treatment center reduce subsequent. emergency room visits in patients with alcohol
 Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Does referral from an emergency department to an alcohol treatment center reduce subsequent emergency room visits in patients with alcohol intoxication? Robert Sapien, MD Department of Emergency Medicine
Risk Factors for Neonatal Methicillin-Resistant
 infection control and hospital epidemiology april 2007, vol. 28, no. 4 original article Risk Factors for Neonatal Methicillin-Resistant Staphylococcus aureus Infection in a Well-Infant Nursery Dao M. Nguyen,
infection control and hospital epidemiology april 2007, vol. 28, no. 4 original article Risk Factors for Neonatal Methicillin-Resistant Staphylococcus aureus Infection in a Well-Infant Nursery Dao M. Nguyen,
Lab ID Events MRSA Bloodstream Infection and C. difficile
 Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Skin and soft tissue infections (SSTIs) are a frequent emergency
 Emergency Department Infections In The Era Of Community-Acquired MRSA A 45-year-old man presents to the ED complaining of a painful lump on his right thigh that appeared yesterday and has become progressively
Emergency Department Infections In The Era Of Community-Acquired MRSA A 45-year-old man presents to the ED complaining of a painful lump on his right thigh that appeared yesterday and has become progressively
GUIDELINES FOR THE MANAGEMENT OF PVL ASSOCIATED STAPHYLOCOCCUS AUREUS INFECTIONS IN THE HOSPITAL ENVIRONMENT
 GUIDELINES FOR THE MANAGEMENT OF PVL ASSOCIATED STAPHYLOCOCCUS AUREUS INFECTIONS IN THE HOSPITAL ENVIRONMENT Post holder responsible for Policy: Directorate/Department responsible for Policy: Lead Nurse
GUIDELINES FOR THE MANAGEMENT OF PVL ASSOCIATED STAPHYLOCOCCUS AUREUS INFECTIONS IN THE HOSPITAL ENVIRONMENT Post holder responsible for Policy: Directorate/Department responsible for Policy: Lead Nurse
Chapter 20: Analysis of Surveillance Data
 Analysis of Surveillance Data: Chapter 20-1 Chapter 20: Analysis of Surveillance Data Sandra W. Roush, MT, MPH I. Background Ongoing analysis of surveillance data is important for detecting outbreaks and
Analysis of Surveillance Data: Chapter 20-1 Chapter 20: Analysis of Surveillance Data Sandra W. Roush, MT, MPH I. Background Ongoing analysis of surveillance data is important for detecting outbreaks and
Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps
 Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps AUGUST 2005 Navy Environmental Health Center 620 John
Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps AUGUST 2005 Navy Environmental Health Center 620 John
Infectious Disease. Update. July 2008
 July 2008 Antibiotic eview ubcommittee of the Pharmacy & Therapeutics Committee Update Infectious Disease Community-Acquired Methicillin-esistant taphylococcus aureus (CA-MA) kin & oft Tissue Infections
July 2008 Antibiotic eview ubcommittee of the Pharmacy & Therapeutics Committee Update Infectious Disease Community-Acquired Methicillin-esistant taphylococcus aureus (CA-MA) kin & oft Tissue Infections
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
8/5/2014. We have no commercial or financial conflict of interest
 Erica Runningdeer, MSN, MPH, RN Illinois Department of Public Health Gail Itokazu, PharmD John H Storger Jr. Hospital of Cook County Sarah Becca Peglow, MD Rush University Medical Center John H Stroger,
Erica Runningdeer, MSN, MPH, RN Illinois Department of Public Health Gail Itokazu, PharmD John H Storger Jr. Hospital of Cook County Sarah Becca Peglow, MD Rush University Medical Center John H Stroger,
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Methicillin Resistant Staphylococcus aureus (MRSA) in Tasmanian Rural Hospitals and Non Acute Health Settings
 Methicillin Resistant Staphylococcus aureus (MRSA) in Tasmanian Rural Hospitals and Non Acute Health Settings Guidance for the management of patients with MRSA in Tasmania's rural hospitals and non acute
Methicillin Resistant Staphylococcus aureus (MRSA) in Tasmanian Rural Hospitals and Non Acute Health Settings Guidance for the management of patients with MRSA in Tasmania's rural hospitals and non acute
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey
 2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
Clinical Review. Evidence-based approach to abscess management
 Clinical Review Evidence-based approach to abscess management Christina Korownyk MD CCFP G. Michael Allan MD CCFP ABSTRACT Objective To provide family physicians with an overview of the evidence for managing
Clinical Review Evidence-based approach to abscess management Christina Korownyk MD CCFP G. Michael Allan MD CCFP ABSTRACT Objective To provide family physicians with an overview of the evidence for managing
STATISTICAL BRIEF #137
 Medical Expenditure Panel Survey STATISTICAL BRIEF #137 Agency for Healthcare Research and Quality August 26 Treatment of Sore Throats: Antibiotic Prescriptions and Throat Cultures for Children under 18
Medical Expenditure Panel Survey STATISTICAL BRIEF #137 Agency for Healthcare Research and Quality August 26 Treatment of Sore Throats: Antibiotic Prescriptions and Throat Cultures for Children under 18
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I)
 ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus bacteraemia annual report, part I The format
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus bacteraemia annual report, part I The format
Meningococcal Disease Among Men Who Have Sex with Men United States, January 2012 - June 2015
 Meningococcal Disease Among Men Who Have Sex with Men United States, January 2012 - June 2015 Temitope A. Folaranmi MBChB MPH MPP Advisory Committee on Immunization Practices February 24, 2016 National
Meningococcal Disease Among Men Who Have Sex with Men United States, January 2012 - June 2015 Temitope A. Folaranmi MBChB MPH MPP Advisory Committee on Immunization Practices February 24, 2016 National
NASAL COLONIZATION BY MICROORGANISMS IN NURSING PROFESSIONALS IN UNITS SPECIALIZING IN HIV/AIDS
 University of Sa o Paulo at Ribeira o Preto College of Nursing. WHO Collaborating Centre for Nursing Research Development. Ribeirão Preto (SP), Brazil. RENAIDST Rede Nacional NASAL COLONIZATION BY MICROORGANISMS
University of Sa o Paulo at Ribeira o Preto College of Nursing. WHO Collaborating Centre for Nursing Research Development. Ribeirão Preto (SP), Brazil. RENAIDST Rede Nacional NASAL COLONIZATION BY MICROORGANISMS
Disease Site Breast. Less than 120 kg: Cefazolin 2 grams IV Greater than or equal to 120 kg: Cefazolin 3 grams IV. Head & Neck
 Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
TREATMENT OF PERITONEAL DIALYSIS (PD) RELATED PERITONITIS. General Principles
 WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
Blue Team Teaching Module: Periorbital/Orbital Infections
 Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
State of Kuwait Ministry of Health Infection Control Directorate. Guidelines for Prevention of Surgical Site Infection (SSI)
 State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Publication Year: 2013
 IMPACT OF A CLINICAL DECISION SUPPORT TOOL IN THE EMERGENCY DEPARTMENT ON ANTIMICROBIAL PRESCRIBING PATTERNS FOR THE TREATMENT OF PNEUMONIA UNIVERSITY OF PENNSYLVANIA HEALTH SYSTEM Publication Year: 2013
IMPACT OF A CLINICAL DECISION SUPPORT TOOL IN THE EMERGENCY DEPARTMENT ON ANTIMICROBIAL PRESCRIBING PATTERNS FOR THE TREATMENT OF PNEUMONIA UNIVERSITY OF PENNSYLVANIA HEALTH SYSTEM Publication Year: 2013
SHEA Guideline for Preventing Nosocomial Transmission of Multidrug-Resistant Strains of Staphylococcus aureus and Enterococcus
 362 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY May 2003 Special Report SHEA Guideline for Preventing Nosocomial Transmission of Multidrug-Resistant Strains of Staphylococcus aureus and Enterococcus Carlene
362 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY May 2003 Special Report SHEA Guideline for Preventing Nosocomial Transmission of Multidrug-Resistant Strains of Staphylococcus aureus and Enterococcus Carlene
ANTIBIOTICS IN SEPSIS
 ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
MRSA Prevention and Control in County Correctional Facilities in the Greater Dayton Area
 Wright State University CORE Scholar Master of Public Health Program Student Publications Master of Public Health Program 10-2007 MRSA Prevention and Control in County Correctional Facilities in the Greater
Wright State University CORE Scholar Master of Public Health Program Student Publications Master of Public Health Program 10-2007 MRSA Prevention and Control in County Correctional Facilities in the Greater
Wound Care on the Field. Objectives
 Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
HLA-Cw*0602 associates with a twofold higher prevalence. of positive streptococcal throat swab at the onset of
 1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL
 PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
Reducing Barriers, Enforcing Standards, and Providing Incentives to Immunize
 Reducing Barriers, Enforcing Standards, and Providing Incentives to Immunize Institute of Medicine National Vaccine Plan Meeting: Goal 4 July 24, 2008 Chicago, Illinois Lance E Rodewald, MD Immunization
Reducing Barriers, Enforcing Standards, and Providing Incentives to Immunize Institute of Medicine National Vaccine Plan Meeting: Goal 4 July 24, 2008 Chicago, Illinois Lance E Rodewald, MD Immunization
APIC Practice Guidance Committee: Implementation Insights Prevention & Control of Pertussis
 1275 K Street, NW, Suite 1000 Washington, DC 20005-4006 Phone: 202/789-1890 Fax: 202/789-1899 apicinfo@apic.org www.apic.org APIC Practice Guidance Committee: Implementation Insights Prevention & Control
1275 K Street, NW, Suite 1000 Washington, DC 20005-4006 Phone: 202/789-1890 Fax: 202/789-1899 apicinfo@apic.org www.apic.org APIC Practice Guidance Committee: Implementation Insights Prevention & Control
Annex A: Screening, Testing and Surveillance for Antibiotic-Resistant Organisms (AROs)
 Annex A: Screening, Testing and Surveillance for Antibiotic-Resistant Organisms (AROs) In All Health Care Settings Provincial Infectious Diseases Advisory Committee (PIDAC) Revised: February 2013 The Ontario
Annex A: Screening, Testing and Surveillance for Antibiotic-Resistant Organisms (AROs) In All Health Care Settings Provincial Infectious Diseases Advisory Committee (PIDAC) Revised: February 2013 The Ontario
Rapid HIV Testing of Clients of a Mobile STD/HIV Clinic ABSTRACT
 AIDS PATIENT CARE and STDs Volume 19, Number 4, 2005 Mary Ann Liebert, Inc. Rapid HIV Testing of Clients of a Mobile STD/HIV Clinic THOMAS S. LIANG, M.P.H., 1 EMILY ERBELDING, M.D., M.P.H., 3 CLAUDE A.
AIDS PATIENT CARE and STDs Volume 19, Number 4, 2005 Mary Ann Liebert, Inc. Rapid HIV Testing of Clients of a Mobile STD/HIV Clinic THOMAS S. LIANG, M.P.H., 1 EMILY ERBELDING, M.D., M.P.H., 3 CLAUDE A.
Taking the Bite out of Dog ma
 Taking the Bite out of Dog ma Dr. Michael Woo MD, CCFP(EM), RDMS Director, Emergency Medicine Ultrasonography Associate Professor, Department of Emergency Medicine Ultrasound uottawa DEM 25 May 2013 ACKNOWLEDGEMENTS
Taking the Bite out of Dog ma Dr. Michael Woo MD, CCFP(EM), RDMS Director, Emergency Medicine Ultrasonography Associate Professor, Department of Emergency Medicine Ultrasound uottawa DEM 25 May 2013 ACKNOWLEDGEMENTS
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Community Health Administration
 Community Health Administration 300 North San Antonio Road Santa Barbara, CA 93110-1332 805/681-5439 FAX 805/681-5200 Takashi M. Wada, MD, MPH Director/Health Officer Anne M. Fearon Deputy Director Suzanne
Community Health Administration 300 North San Antonio Road Santa Barbara, CA 93110-1332 805/681-5439 FAX 805/681-5200 Takashi M. Wada, MD, MPH Director/Health Officer Anne M. Fearon Deputy Director Suzanne
FACULTY OF MEDICAL SCIENCE
 Doctor of Philosophy Program in Microbiology FACULTY OF MEDICAL SCIENCE Naresuan University 171 Doctor of Philosophy Program in Microbiology The time is critical now for graduate education and research
Doctor of Philosophy Program in Microbiology FACULTY OF MEDICAL SCIENCE Naresuan University 171 Doctor of Philosophy Program in Microbiology The time is critical now for graduate education and research
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico
 Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico Ruth Ríos-Motta, PhD, José A. Capriles-Quirós, MD, MPH, MHSA, Mario
Disparities in Realized Access: Patterns of Health Services Utilization by Insurance Status among Children with Asthma in Puerto Rico Ruth Ríos-Motta, PhD, José A. Capriles-Quirós, MD, MPH, MHSA, Mario
Advice for those affected by MRSA outside of hospital
 Advice for those affected by MRSA outside of hospital If you have MRSA this leaflet provides information and advice for managing your day-to-day life. 1 About MRSA There are lots of different types or
Advice for those affected by MRSA outside of hospital If you have MRSA this leaflet provides information and advice for managing your day-to-day life. 1 About MRSA There are lots of different types or
CF ATLANTA Research & Development Program at Emory University and Georgia Tech (CF@LANTA) Clinical & Translational Research Core
 CF ATLANTA Research & Development Program at Emory University and Georgia Tech (CF@LANTA) Clinical & Translational Research Core Arlene Stecenko, MD Director, Emory + Children s Cystic Fibrosis Care Center
CF ATLANTA Research & Development Program at Emory University and Georgia Tech (CF@LANTA) Clinical & Translational Research Core Arlene Stecenko, MD Director, Emory + Children s Cystic Fibrosis Care Center
Competency 1 Describe the role of epidemiology in public health
 The Northwest Center for Public Health Practice (NWCPHP) has developed competency-based epidemiology training materials for public health professionals in practice. Epidemiology is broadly accepted as
The Northwest Center for Public Health Practice (NWCPHP) has developed competency-based epidemiology training materials for public health professionals in practice. Epidemiology is broadly accepted as
ESCMID Online Lecture Library. by author
 Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
Do statins improve outcomes of patients with sepsis and pneumonia? Jordi Carratalà Department of Infectious Diseases Statins for sepsis & community-acquired pneumonia Sepsis and CAP are major healthcare
The National Antimicrobial Resistance Monitoring System (NARMS)
 The National Antimicrobial Resistance Monitoring System (NARMS) Strategic Plan 2012-2016 Table of Contents Background... 2 Mission... 3 Overview of Accomplishments, 1996-2011... 4 Strategic Goals and Objectives...
The National Antimicrobial Resistance Monitoring System (NARMS) Strategic Plan 2012-2016 Table of Contents Background... 2 Mission... 3 Overview of Accomplishments, 1996-2011... 4 Strategic Goals and Objectives...
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008
 Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Highlights of the Revised Official ICD-9-CM Guidelines for Coding and Reporting Effective October 1, 2008 Please refer to the complete ICD-9-CM Official Guidelines for Coding and Reporting posted on this
Appropriate Treatment for Children with Upper Respiratory Infection
 BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
Black Hills Healthcare System
 Black Hills Healthcare System Methicillin Resistant Staphylococcal Aureus (MRSA) Patient and Family Information What is MRSA? Staphylococcus Aureus, often referred to simply as staph, is a bacteria commonly
Black Hills Healthcare System Methicillin Resistant Staphylococcal Aureus (MRSA) Patient and Family Information What is MRSA? Staphylococcus Aureus, often referred to simply as staph, is a bacteria commonly
Laboratory confirmation requires isolation of Bordetella pertussis or detection of B. pertussis nucleic acid, preferably from a nasopharyngeal swab.
 Pertussis Epidemiology in New Zealand New Zealand has continued to experience outbreaks of pertussis in recent decades. This is in part due to historically low immunisation rates and in part because immunity
Pertussis Epidemiology in New Zealand New Zealand has continued to experience outbreaks of pertussis in recent decades. This is in part due to historically low immunisation rates and in part because immunity
The first report in Brazil of severe infection caused by community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA)
 ISSN 0100-879X Volume 42 (8) 692-775 August 2009 CLINICAL INVESTIGATION Braz J Med Biol Res, August 2009, Volume 42(8) 756-760 The first report in Brazil of severe infection caused by community-acquired
ISSN 0100-879X Volume 42 (8) 692-775 August 2009 CLINICAL INVESTIGATION Braz J Med Biol Res, August 2009, Volume 42(8) 756-760 The first report in Brazil of severe infection caused by community-acquired
Components of CVC Care Bundle. selection
 Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC
 Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol
 Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * COLLECTION OF CASE STUDIES
 COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
Policy for Screening Patients for MRSA Colonisation
 Policy for Screening Patients for MRSA Colonisation To whom this document applies: All staff in Colchester Hospital University Foundation Trust screening Patients for MRSA Procedural Documents Approval
Policy for Screening Patients for MRSA Colonisation To whom this document applies: All staff in Colchester Hospital University Foundation Trust screening Patients for MRSA Procedural Documents Approval
Skin and Soft Tissue Infections
 Skin and Soft Tissue Infections Cellulitis Note: The most common etiology of cellulitis with purulent drainage is S. aureus, although Group A streptococci and other streptococcal species can also present
Skin and Soft Tissue Infections Cellulitis Note: The most common etiology of cellulitis with purulent drainage is S. aureus, although Group A streptococci and other streptococcal species can also present
Surveillance cultures PRO. Kurt Espersen ICU 4131 Rigshospitalet Copenhagen
 Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Use of Azithromycin in Children with Non-Cystic Fibrosis Bronchiectasis or Chronic Suppurative Lung Disease
 Use of Azithromycin in Children with Non-Cystic Fibrosis Bronchiectasis or Chronic Suppurative Lung Document ID CHQ-GDL-01061 Version no. 2.0 Approval date 28/08/2015 Executive sponsor Executive Director
Use of Azithromycin in Children with Non-Cystic Fibrosis Bronchiectasis or Chronic Suppurative Lung Document ID CHQ-GDL-01061 Version no. 2.0 Approval date 28/08/2015 Executive sponsor Executive Director
Do general practitioners prescribe more antimicrobials when the weekend comes?
 DOI 10.1186/s40064-015-1505-6 RESEARCH Open Access Do general practitioners prescribe more antimicrobials when the weekend comes? Meera Tandan 1*, Sinead Duane 1 and Akke Vellinga 1,2 Abstract Inappropriate
DOI 10.1186/s40064-015-1505-6 RESEARCH Open Access Do general practitioners prescribe more antimicrobials when the weekend comes? Meera Tandan 1*, Sinead Duane 1 and Akke Vellinga 1,2 Abstract Inappropriate
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project
 1 California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project Hospital Association of Southern California Conference February 26, 2015 Vicki Keller, RN,MSN,CIC
1 California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project Hospital Association of Southern California Conference February 26, 2015 Vicki Keller, RN,MSN,CIC
Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities
 Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities Prepared By The MRSA Interagency Advisory Committee in conjunction
Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities Prepared By The MRSA Interagency Advisory Committee in conjunction
STATISTICAL BRIEF #117
 Medical Expenditure Panel Survey STATISTICAL BRIEF #117 Agency for Healthcare Research and Quality March 2006 Children s Dental Visits and Expenses, United States, 2003 Erwin Brown, Jr. Introduction Regular
Medical Expenditure Panel Survey STATISTICAL BRIEF #117 Agency for Healthcare Research and Quality March 2006 Children s Dental Visits and Expenses, United States, 2003 Erwin Brown, Jr. Introduction Regular
Bachir K. Younes, M.D., M.P.H.
 Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital
 Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
MRSA. Living with. Acknowledgements. (Methicillin-Resistant Staphylococcus aureus)
 How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM
 ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013
 Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health
Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January June 2013 by Michael E. Martinez, M.P.H., M.H.S.A., and Robin A. Cohen, Ph.D. Division of Health
Enhancing Respiratory Infection Surveillance on the Arizona-Sonora Border BIDS Program Sentinel Surveillance Data
 Enhancing Respiratory Infection Surveillance on the Arizona-Sonora Border BIDS Program Sentinel Surveillance Data Catherine Golenko, MPH, Arizona Department of Health Services *Arizona border population:
Enhancing Respiratory Infection Surveillance on the Arizona-Sonora Border BIDS Program Sentinel Surveillance Data Catherine Golenko, MPH, Arizona Department of Health Services *Arizona border population:
PCORnet Use Cases. Cluster randomized trial: Routine decolonization of non-icu medical surgical patients to prevent healthcare associated infections
 PCORnet Use Cases Cluster randomized trial: Routine decolonization of non-icu medical surgical patients to prevent healthcare associated infections 1 Susan Huang, MD MPH University of California, Irvine
PCORnet Use Cases Cluster randomized trial: Routine decolonization of non-icu medical surgical patients to prevent healthcare associated infections 1 Susan Huang, MD MPH University of California, Irvine
Clinical Infectious Diseases Advance Access published January 4, 2011
 Clinical Infectious Diseases Advance Access published January 4, 2011 IDSA GUIDELINES Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of Methicillin-Resistant
Clinical Infectious Diseases Advance Access published January 4, 2011 IDSA GUIDELINES Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of Methicillin-Resistant
CCHCS Care Guide: Skin & Soft Tissue Infections
 GOALS Early diagnosis and treatment of skin and soft tissue infections Infection control measures to prevent transmission to others Incision & drainage if abscess present Evidence based use of antibiotics
GOALS Early diagnosis and treatment of skin and soft tissue infections Infection control measures to prevent transmission to others Incision & drainage if abscess present Evidence based use of antibiotics
Strep Throat. Group Members: Rebecca Okinczyc
 Strep Throat Group Members: Rebecca Okinczyc Andrew Miclat Joshua Savage Introduction It is the purpose of this paper to present a comprehensive and exhaustive description of the disease Streptococcal
Strep Throat Group Members: Rebecca Okinczyc Andrew Miclat Joshua Savage Introduction It is the purpose of this paper to present a comprehensive and exhaustive description of the disease Streptococcal
COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE
 COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE The two most common bacteria to cause skin infections are staphylococcus aureus (staph aureus ) and streptococcus pyogenes ( strep) (see Table 1). Staphylococcus
COMMON BACTERIAL SKIN INFECTIONS IN GENERAL PRACTICE The two most common bacteria to cause skin infections are staphylococcus aureus (staph aureus ) and streptococcus pyogenes ( strep) (see Table 1). Staphylococcus
