KNEE LIGAMENTS COLLATERAL DAMAGE TO PHYSICAL THERAPY
|
|
|
- Brooke Holt
- 7 years ago
- Views:
Transcription
1 COLLATERAL DAMAGE TO KNEE LIGAMENTS By Dr Ben Benjamin, PhD INTRODUCTION I worked as a therapist for 14 years before I truly got to understand the injury process. It was while obtaining my PhD in sports medicine that I came across the theories of Dr James Cyriax and Dr Milne Ongley and this revolutionised my thinking. After studying and testing Cyriax s theories on several hundred people, I had to put aside many of his assumptions and long-cherished beliefs. Muscles, muscle injuries and muscle tension were only one small part of understanding the pain and injury process. The first important fact is that the formation of adhesive scar tissue in the tendons, ligaments and joints is often the primary culprit in long-term pain. Although muscles get injured most frequently, they also heal more easily on their own. Tendons, ligaments and joints, on the other hand, may take months or years to heal and often stay injured for a lifetime. There are hundreds of discrete injuries to muscles, tendons, ligaments, bursas, nerves and joints that could be precisely assessed, understood and successfully treated. I learned an effective hands-on technique called friction therapy, which can be used to break down adhesive scar tissue in muscles, tendons, ligaments and fascia. Therapists who work with pain and injury problems must gain an understanding of what I term the essential principles - the underlying principles that govern effective assessment and treatment. If this information is mastered then the most inscrutable symptoms, conditions and pain patterns presented by clients can be understood, including the most difficult pain cases. What follows are There are many approaches to the treatment of pain and injury problems. It is best to have a full and clear understanding of what the problem is before a person is treated. In this article the author outlines some of the principles that are essential to a therapist s overall understanding of the injury process, and demonstrates how to apply these principles to two common knee injuries. some of these important concepts that will help to provide an understanding of the body and its pain in a new way. I will use as an example, two common knee injuries - the lateral and medial collateral ligaments - to show how the application of these essential principles can help you clearly assess and effectively treat your clients. PRINCIPLE: THE NATURE OF INJURY An injury, often called in medicine a lesion, is present when there is tissue damage. The damage could manifest as a swelling in a bursa or a joint; pinching of a nerve or a tendon; micro-tears in a muscle, tendon, ligament or fascia; or a major disruption of tissue like a broken bone or a ruptured tendon. When there is an injury, a part of the body has lost its structural integrity. Application: Injuries to the collateral ligaments of the knee The collateral ligaments of the knee link the leg by connecting the femur to the lower leg on the medial and lateral sides of the knee. 15
2 COLLATERAL DAMAGE TO KNEE LIGAMENTS 2003 Primal Pictures Ltd Patella 2003 Primal Pictures Ltd Lateral ligament Medial collateral ligament - showing attachment of the ligament to the joint capsule and meniscus Joint capsule Meniscus Figure 1a: Medial collateral ligament of the knee (anterior aspect) Figure 1b: Lateral collateral ligament of the knee These ligaments are very important because together they prevent the knee from buckling inwards and outwards and keep it on track for forward-back movement. A person can have a mild sprain of these ligaments, where only a few fibres are damaged; a moderately severe sprain, where many fibres are torn; or an extremely severe one, where the ligament tears more extensively or ruptures completely in half. The medial collateral ligament of the knee is injured more frequently than the lateral collateral ligament. The medial ligament runs from the femur to the tibia while the lateral ligament attaches the femur to the fibula. With either of these ligament sprains, commonly the fibres may have torn either in the middle or near the ends of the ligament at the attachments. The medial collateral ligament is actually attached to the inner aspect of the joint capsule of the knee and is connected to another important ligament in the knee, the medial coronary ligament. Medial collateral and coronary ligament tears therefore often accompany each other and are sometimes confused with one another. The lateral collateral ligament is not contiguous with the joint and therefore causes less or no swelling when injured. PRINCIPLE: PAIN AS A SIGNAL Pain is the signal that something has gone wrong in the body. When the body speaks it is good to listen. If the pain diminishes and disappears within a few days, there is usually nothing to worry about. If the pain persists for more than several days, becomes more frequent or hurts with less and less activity then the body is giving the person an important message: Pay attention! The sooner appropriate healing begins, the better are the person s chances of full recovery. Early warning signals are too frequently ignored and often result in more severe injuries that may incapacitate the person for months or years. Curtailing activities or resting for a few days may be all that is needed. In other circumstances it may be necessary for the person to be treated by a physician or hands-on healthcare practitioner. It is essential to see a doctor if: The pain is very severe There is paralysis There is numbness or constant pins and needles in the arms, hands, legs or feet The area is swollen A snapping sound or tearing sensation accompanied the injury There is weakness of the injured body part There is extreme limitation of movement or inability to use the injured area There is malfunction of the bladder or bowel There is associated nausea, vomiting or blurred vision The person is disorientated, dizzy or cannot perform normal activities because of the injury. Application: Pain signals at the medial and lateral aspects of the knee In a medial or lateral collateral knee injury, regardless of where along the ligament the lesion is, pain is felt directly on the medial or lateral side of the knee. A collateral ligament sprain generally arrives in one of two ways. Suddenly, as if hit by lightning, a person finds themselves on the ground. They fell or were tackled, and the knee buckled inwards (medial collateral) or outwards (lateral collateral). Perhaps the person heard a snapping sound, but more likely it was missed in the confusion of the fall. The person s knee hurts everywhere and often the patient hobbles off trying not to bend it. Over the next few hours the knee swells, feels hot to the touch, and continues to ache. With the passing hours, the knee stiffens, making bending and straightening difficult, and by the next day the pain begins to concentrate on the inner or outer side of the knee. Activity automatically becomes limited because walking is painful and anything more strenuous is impossible. In the second case, a person might start feeling a twinge of pain 16
3 now and then while playing tennis, running or hiking. After a few weeks the pain settles on the inside of the knee and is more constant. There may be slight swelling or maybe not. The person begins to notice pain as he begins an activity, then the pain goes away and an hour or so, after finishing the activity it hurts again. The pain mysteriously disappears in the midst of activity because the ligament warms up (and this often relieves the pain). Eventually the person can no longer do certain strenuous activities without pain. In both these cases the problem is the same - a torn medial or lateral collateral ligament. This mysterious injury has many personalities. It can come on quickly with mild, moderate or severe pain or it may develop more slowly and be either mild or moderately painful. No matter how it starts it often lingers for a long time, causing confusion by coming and going. The medial collateral ligament injury usually prompts the phrase my dodgy knee, as the pain has a habit of appearing and disappearing mysteriously. When the injury results from trauma, it s easy to understand what caused it. When it appears slowly, the causes are subtle and often interlocking: poor leg alignment with knees turned-in or out; excess muscle tension, which leads to early fatigue; or loose or stretched ligaments caused by old sprains or poor stretching exercises. PRINCIPLE: SCAR TISSUE AS THE SECRET OF CHRONIC PAIN Sometimes the acute pain of an injury disappears completely and the patient is never bothered by it again. Sometimes pain becomes a chronic problem. Most people do not realise that the cause of most chronic pain from soft tissue injuries is the initial poor healing of the injury. Adhesive scar tissue forms, binding the originally damaged tissue to the adjacent soft tissues. Scar tissue formation is normal when soft tissue injuries are repairing. When scar tissue forms in the appropriate places, it is the biological glue that holds torn fibres together. However, if this healing process occurs in a random fashion, the scar tissues form a jumbled mass of adhesions that tear on normal movement. Scar tissue within the musculo-skeletal system forms primarily in ligaments, tendons, muscles, fascia and joint capsules. When scar tissue forms in the fascial tissue, it often binds the skin to its underlying fascia, limiting the movement of the skin. If this abnormal scar tissue is placed under tension, the nerve endings in the skin and the underlying fascia are stimulated, producing pain. Fascia also lies deep in the body, where its purpose is to envelope and to provide a gliding surface for muscles, tendons, ligaments and other structures. Putting tension on this scar tissue in the deeper fascia again stimulates local nerve endings and produces pain. Methods of fascial release can be employed with beneficial results. However, until all the abnormal adhesive scar tissue is removed from all of the affected structures, a pain-free state cannot be achieved. Movements that excessively stress the damaged tissue result in reinjury. This re-injury results in the formation of more adhesive scar tissue. Understanding how to encourage the correct healing of tissues prevents these complications. Breaking the cycle of tearing and re-tearing of adhesive scar tissue is the key to effective treatment. Application: Scar tissue and chronic pain at the medial and lateral knee A complication of torn collateral ligaments is the dodgy-knee syndrome. In one way or another, the ligament has been sprained, and though there are brief reprieves and the person begins to think, It s gone, I ve beaten the problem, the pain then returns. It can recur with what was seemingly a simple activity such as helping a friend move some boxes up a flight of stairs, squatting for five minutes while weeding in the garden, running a mile every other day for two weeks, or making a dash to catch the bus. Troublesome adhesive scar tissue that keeps re-tearing is the key to understanding this mystery. When the knee bends and straightens, the collateral ligaments normally move freely across the bone on the medial and lateral sides of the knee. If a collateral ligament is injured and heals properly, the scar tissue that s formed within the ligament does not interfere with its free movement. However, if the injury doesn t heal well, scar tissue may form a matted scar within the ligament or between the ligament and the bone where it is not supposed to be attached. This scar tissue often acts like glue, adhering the ligament to the bone so that its free-sliding movement becomes more limited. If activities are strenuous and jarring, or involve twisting, the scar tissue does not hold and tears repeatedly. When a ligament warms up during activity, pain often diminishes or disappears temporarily. An hour or two later, when the ligament has cooled down, the pain intensifies or returns. This cycle of poor healing and scar tissue re-tearing can happen hundreds of times over many months or years. In its most extreme form the ligament completely ruptures and the knee becomes unstable. This event tends to only occur in very serious accidents or severe falls. If it does occur, the person should see a doctor immediately. 17
4 COLLATERAL DAMAGE TO KNEE LIGAMENTS PRINCIPLE: INJURY VERIFICATION THROUGH RESISTED AND PASSIVE TESTING A therapist should begin the assessment of a client by obtaining a complete history of the injury, including a description of the location of the pain, any traumatic event that led to the injury and any factors that aggravate or relieve the pain. The therapist can further verify the injury through palpation and by applying a series of simple tests to the region. These tests will help the therapist pinpoint the location of injured structures, evaluate the severity of the injury and develop a rationale for a treatment plan. A resisted test is an isometric contraction against resistance that does not involve movement of the limb. This type of test primarily tests for injury to muscles and tendons (ie. those structures which initiate movement). It also tests for weakness when there is disc pressure on the nerve. A passive test is when the client behaves like a rag doll and does not assist during the movement that the therapist takes the client through. Passive tests primarily check for injury to ligaments, joints and bursas, structures that do not initiate movement. Application: Verification of collateral ligament knee injuries One of the clearest signs of a collateral ligament injury in the knee is the location of the pain. If you know how to palpate these ligaments, you can find the precise source of the pain. The lateral collateral ligament is easy to find. When a person crosses their legs, the lateral collateral becomes taut and sticks right out at the lateral knee. To find it place your finger on the head of the fibula just below the lateral knee while the legs are crossed and move superiorly until you come to the attachment on the femur. The medial collateral ligament is a little trickier to find because the ligament is flattened against the bone. To locate it let the person lie supine and bend the knee so that the foot is on the table. Place your finger at the inferior pole of the patella - this puts you at the joint line. Slide your finger medially in the crevice of the joint line ninety degrees until you reach the ligament. It is relatively close to the skin surface. Injuries to this ligament often occur at the joint line in the middle of the ligament. Resisted tests should not cause pain in cases of collateral ligament injuries, since the resistance tests active structures such as muscles rather than the ligaments. The following list offers one palpation test and four passive tests to help you assess whether the collateral ligaments of the knee are injured. TESTS Testing for heat Place the back of your hand alternately on the inner side and then outer side of both knees and compare their relative heat. If there is active inflammation and swelling in one knee, there is usually a heat differential. Figure 2a+b: Testing for heat differential on medial and lateral aspects of the knee 18
5 Passive knee flexion test Lift the knee slightly toward the chest and gently flex the knee by bringing the heel toward the buttock. If you reach the buttock without pain or limitation, give the foot a slight push toward the buttock. If the knee is swollen you will not be able to bring the heel to the buttock, so do not force it. If the motion is limited, check the other knee to see that it is not just the person s natural structure. Figure 3: Passive knee flexion test Passive knee extension test Place one hand under the Achilles tendon and the other hand above the knee. Now press down with the hand above the knee, while simultaneously pulling up with the hand under the Achilles. You are gently, passively trying to straighten the knee. If the knee is swollen, movement will be slightly limited and/or painful. Figure 4: Passive knee extension test Valgus stressing of the medial knee Standing next to the knee facing the person s head, place your outer hand on the lateral aspect of the knee with your fingers just under the knee. Then, place the palm of your inner hand on the medial ankle as shown in the photograph. Now apply a shearing force in opposing directions to stress the medial knee. In other words push laterally with the hand on the medial ankle and medially with the hand on the lateral knee. If there is no pain when the knee is taut, give it a slight extra push. If there is still no pain, slide the leg off the table laterally and repeat the test with the knee slightly bent (about one inch). Figure 5: Valgus knee stress test Varus stressing of the lateral knee Facing the client s head, place your outer hand on the lateral ankle. Then place your inner hand on the medial knee with your fingers just under the knee. Now apply a shearing force in opposing directions to stress the lateral knee, that is, press laterally with the hand on the medial knee and push medially with the hand on the lateral ankle. If there is no pain when the knee is taut, give it a slight extra push. If there is still no pain, repeat the test with the knee bent only one inch by slipping the leg off the table. If the valgus test or the varus test causes pain, you have verified a strain of the medial collateral or lateral collateral ligament respectively. It should hurt where the person normally feels pain. If the injury is severe, you have to exert only a small amount of pressure during the test. If it is mild, you must exert more pressure. If passive flexion and/or passive extension are painful or limited in the ability to move through a full range of movement it means that there is some swelling accompanying the collateral ligament injury. Collateral ligament injuries are often accompanied by a tear of a ligament that attaches the meniscus to the tibia (the coronary ligament). These two ligaments are often injured simultaneously. Figure 6: Varus knee stress test PRINCIPLE: HEALING INJURED TISSUES Most of the body s healing processes proceed without our conscious direction. When musculo-skeletal structures are damaged or torn, the body s wisdom ensures that the damage, whenever possible, will be repaired. However, to a large extent the degree and quality of this repair depends upon our own participation. The natural mechanisms of inflammation and wound healing are usually excessive for the job at hand. The body over-compensates when it responds to injury. More plasma, red and white cells, blood platelets and chemical mediators are released than are actually needed to allow full healing to occur. Therefore, additional scar tissue is likely to form. This scar tissue often binds together damaged and undamaged structures, resulting in adhesions that, as we have seen, can lead to re-injury and to chronic pain. There are several methods by which we can help the body limit the formation of adhesive scar tissue and/or recover from adhesions that have already formed. The first of these methods is friction therapy. A therapist applies cross-fibre friction therapy in a controlled manner to break up specifically targeted areas of adhesive scar tissue. When friction therapy is accompanied by the second method, healing in the presence of a full range of motion, healthy tissue can grow without the re-formation of adhesions. This means that in order to heal properly, the body part must be regularly moved through its full range of movement during the healing process so that adhesions do not form. If the injured person is able to collaborate with the body s healing processes by adequate 19
6 COLLATERAL DAMAGE TO KNEE LIGAMENTS physical movement, complete healing is more likely. If the person is unable to perform the required exercises by him or herself, it is important to have a therapist assist the person in a full range of motion of the injured part. Application: Treatment for injuries to the collateral ligaments of the knee Friction therapy applied to injured collateral ligaments, along with full range of movement of the knee, can be a safe and effective treatment for these injuries. The therapist should also be aware of other treatment options and refer the client to other practitioners when necessary. TREATMENTS 1. Deep massage and friction therapy This is an effective treatment for medial and lateral collateral knee ligament injuries if done twice a week for three to four weeks. It speeds the healing of the ligament and prevents scartissue formation, especially if done soon after the initial injury. In long-standing cases, treatment may take longer and may need to be combined with manipulation by a physiotherapist, chiropractor or osteopath to free the ligament from the bone. Friction therapy for the medial collateral ligament Sit on a stool next to the injured knee and place your index finger at the lower pole of the patella. Now trace the joint line with a moderate pressure as you move around the knee toward the table in a straight line medially. Half way down toward the table you will feel the ligament under your finger. It feels about a quarter of an inch wide and a sixteenth of an inch thick. It isn t that easy to find until you know it. Place your middle or index finger over the ligament and apply a friction stroke upwards, then relax as you bring your hand back to your original position. Friction for five or six minutes, take a break and repeat again for five or six minutes. Most often the ligament is injured here at the joint line, but it may be injured as well at the tibial attachment or at the femoral attachment. In that case, those areas must be frictioned also. Friction therapy for the lateral collateral ligament Sit on a stool next to the injured knee and place your thumb on the head of the fibula just below the lateral knee. Now move superiorly toward the condyle of the femur with a moderate pressure. Halfway towards the femur you will feel the ligament under your finger. It feels like a tight band about a quarter of an inch wide. It is sometimes easier to find if the client crosses the leg, placing the ankle of the bad knee just above the opposite knee. This causes the lateral collateral ligament to protrude out from the knee. Once you have located the ligament, palpate for where the pain is felt. This is where the primary scar tissue is located. Using your middle or index finger over the ligament, apply a friction stroke upwards, then relax as you bring your hand back to your original position. Friction five or six minutes as described above, take a break and repeat again. Most often the ligament is injured here at the joint line, but it may be injured as well toward the fibula attachment or toward the femoral attachment. In that case, those areas must be frictioned also. After frictioning the ligament, deep massage should be applied to the front thigh and knee area. This will enhance the circulation and speed healing and the removal of waste products. Don t neglect working on the other leg as it is usually doing double work to compensate for the injured leg. 2. Exercise therapy The knee must be moved under a little stress so that adhesive scar tissue does not reform. As a first exercise have the client sit and swing the leg for two or three minutes several times a day. After three or four treatments have the person lean against a door and do 10 to 20 mini knee squats where the knee bends no more than 45 degrees. As the knee improves the squats should deepen so that the thigh and lower leg are at a 90 degree angle. These exercises prevent the re-establishment of adhesive scar tissue while building strength in the muscles and ligaments. 3. Manipulation This is only effective where there is an external adhesion to the femur. This occurs with medial collateral ligament tears only. 4. Anti-inflammatory injection An anti-inflammatory injection is helpful in stopping inflamma- RESOURCES Cyriax JH. Cyriax s Illustrated Manual of Orthopaedic Medicine. Butterworth Heinemann ISBN: Dr Milne Ongley is a leading expert in the field of nonsurgical reconstructive therapy. For more information
7 tion and pain and preventing internal adhesions when friction is not successful. It is also effective in the chronic stage when there are adhesions to the bone. The injection, when properly given, ruptures the adhesions and prevents additional adhesions from forming. 5. Proliferant injection If the ligament has been excessively stretched and weakened, massage, exercise, oral medication, manipulation, or other methods of treatment cannot, to my knowledge, tighten the ligaments. Proliferant injections cause the ligaments to tighten and strengthen. A proliferant is usually composed of dextrose (a sugar), glycerine (which helps the blood congeal), xilocane (the stuff the dentist uses to numb your mouth) and phenol (which acts as a sterilising agent). The dextrose is the main active substance; it irritates the ligament or tendon tissues and tricks the brain into producing (proliferating) many like cells of tissue. There are three goals of the proliferant treatment procedure: first, to break up adhesive scar tissue, second, to tighten the stretched ligaments and third to strengthen the weakened ligament fibres. 6. Surgery If the ligament has been completely ruptured, surgical repair is best performed as soon as possible. After the initial recovery period, rehabilitative exercise therapy and deep massage aid in the healing process. CONCLUSION The principles discussed here not only changed the way I view injury and the healing process, but also changed the ways in which I assess, verify and treat the people who come to me with acute and chronic pain. I hope you have gained a picture of the importance these principles can have in your day-to-day work with your own clients. The techniques described here take time and practise to master. These who wish to gain proficiency in this very precise approach to pain and injury may wish to pursue further training. As you gain more experience with orthopaedic massage - performing assessment tests, locating injured structures and practising friction therapy - your treatments will be more effective and your clients will improve more quickly. THE AUTHOR Ben Benjamin holds a PhD in sports medicine and education and is the founder and president of the Muscular Therapy Institute in Cambridge Massachusetts. He studies with Dr James Cyriax the father of orthopaedic medicine and has applied his insights to the healing of soft tissue injuries through skilled massage therapy. He has been in private practice for more than 40 years and teaches extensively. JOBS AND CLASSIFIED A full time position has become available for a fully qualified Sports Massage Therapist at London Wasps rugby club. 25 hours per week plus attendance at all home and away matches. Minimum 3 years experience needed. Dedicated, confident professional required to join our championship winning team. Must have SMA membership and Insurance Salary 25K All Applicants please send c.v. to roger.knibbs@wasps.co.uk. Closing Date for Applications 29th April Inj Prev 12th page.pdf (this needs to be pulled in) sportex medicine magazine covers articles on sports performance and injury prevention. It is aimed at sports massage practitioners, sports therapists and coaches.a subscription costs 26 a year. Call or visit To advertise your educational events in this section please contact Paul Harris on
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Shoulder Tendonitis. Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696
 Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
ESSENTIALPRINCIPLES. Wrist Pain. Radial and Ulnar Collateral Ligament Injuries. By Ben Benjamin
 ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
ESSENTIALPRINCIPLES Wrist Pain Radial and Ulnar Collateral Ligament Injuries By Ben Benjamin 92 MASSAGE & BODYWORK FEBRUARY/MARCH 2005 Ulnar Collateral Ligament Radial Collateral Ligament Right wrist,
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
INFORMATION FOR YOU. Lower Back Pain
 INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
ACL Reconstruction Rehabilitation
 ACL Reconstruction Rehabilitation The following exercises are commonly used for rehabilitation following ACL reconstruction surgery. However, each knee surgery is unique and each person s condition is
ACL Reconstruction Rehabilitation The following exercises are commonly used for rehabilitation following ACL reconstruction surgery. However, each knee surgery is unique and each person s condition is
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
For Deep Pressure Massage
 T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica
 Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella)
 EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Medial Collateral Ligament Sprain: Exercises
 Medial Collateral Ligament Sprain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off
Medial Collateral Ligament Sprain: Exercises Your Kaiser Permanente Care Instructions Here are some examples of typical rehabilitation exercises for your condition. Start each exercise slowly. Ease off
FROZEN SHOULDER OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU. Frozen Shoulder FROZEN SHOULDER
 OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
OXFORD SHOULDER & ELBOW CLINIC INFORMATION FOR YOU Frozen Shoulder The aim of this information sheet is to give you some understanding of the problem you may have with your shoulder. It has been divided
What are Core Muscles?... 2. A Healthy Lumbar Spine...3. What is Low Back Pain?...4. Rehabilitation...6. Stages of Rehabilitation...
 Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
PLANTAR FASCITIS (Heel Spur Syndrome)
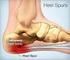 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Hip Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Plantar Fascia Release
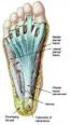 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Heel pain and Plantar fasciitis
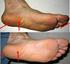 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Cervical Exercise: How important is it? What can be done? The Backbone of Spine Treatment. North American Spine Society Public Education Series
 Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
Hand Injuries and Disorders
 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
KINESIOLOGY TAPING GUIDE
 KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
KINESIOLOGY TAPING GUIDE What is Kinesiology tape and how does Kinesiology tape work? How to apply Kinesiology tape Examples of application of UP Kinesiology tape for common injuries and conditions Introduction
The Lateral Collateral Ligament Sprain. Ashley DeMarco. Pathology and Evaluation of Orthopedic Injuries I. Professor Rob Baerman
 1 The Lateral Collateral Ligament Sprain Ashley DeMarco Pathology and Evaluation of Orthopedic Injuries I Professor Rob Baerman 2 The Lateral Collateral Ligament Sprain Ashley DeMarco Throughout my research
1 The Lateral Collateral Ligament Sprain Ashley DeMarco Pathology and Evaluation of Orthopedic Injuries I Professor Rob Baerman 2 The Lateral Collateral Ligament Sprain Ashley DeMarco Throughout my research
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Common Injuries in Bodybuilding
 Common Injuries in Bodybuilding There is nothing that can slow you down like an injury. Sometimes it seems just when you are starting to make progress in your workouts, you suffer a nagging injury that
Common Injuries in Bodybuilding There is nothing that can slow you down like an injury. Sometimes it seems just when you are starting to make progress in your workouts, you suffer a nagging injury that
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES
 CHAPTER ELEVEN COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES To reduce the risk of pain in your neck and shoulders, stay within these recommended ranges of movement: Neck Flexion: 0 o -15 o (bending
CHAPTER ELEVEN COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES To reduce the risk of pain in your neck and shoulders, stay within these recommended ranges of movement: Neck Flexion: 0 o -15 o (bending
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Patellofemoral Joint: Superior Glide of the Patella
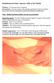 Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Patellofemoral Joint: Superior Glide of the Patella Purpose: To increase knee extension. Precautions: Do not compress the patella against the femoral condyles. Do not force the knee into hyperextension
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Plantar Fasciitis. Plantar Fascia
 Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and
 A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and competition. A warm-up is designed to prepare an athlete
A proper warm-up is important before any athletic performance with the goal of preparing the athlete both mentally and physically for exercise and competition. A warm-up is designed to prepare an athlete
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
MANAGING BACK PAIN GETTING YOU BACK INTO ACTION MANAGING BACK PAIN. www.healthcare-rm.com
 H E A L T H R I S K M A N A G E M E N T MANAGING BACK PAIN MANAGING BACK PAIN GETTING YOU BACK INTO ACTION GETTING YOU BACK INTO ACTION www.healthcare-rm.com Who is this for? CONTENTS Introduction about
H E A L T H R I S K M A N A G E M E N T MANAGING BACK PAIN MANAGING BACK PAIN GETTING YOU BACK INTO ACTION GETTING YOU BACK INTO ACTION www.healthcare-rm.com Who is this for? CONTENTS Introduction about
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Overuse injuries. 1. Main types of injuries
 OVERUSE INJURIES Mr. Sansouci is an ardent runner and swimmer. To train for an upcoming 10-km race, he has decided to increase the intensity of his training. Lately, however, his shoulder and Achilles
OVERUSE INJURIES Mr. Sansouci is an ardent runner and swimmer. To train for an upcoming 10-km race, he has decided to increase the intensity of his training. Lately, however, his shoulder and Achilles
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
PERFORMANCE RUNNING. Piriformis Syndrome
 Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Psoas Syndrome. The pain is worse from continued standing and from twisting at the waist without moving the feet.
 Psoas Syndrome The iliopsoas muscle is a major body mover but seldom considered as a source of pain. Chronic lower back pain involving the hips, legs, or thoracic regions can often be traced to an iliopsoas
Psoas Syndrome The iliopsoas muscle is a major body mover but seldom considered as a source of pain. Chronic lower back pain involving the hips, legs, or thoracic regions can often be traced to an iliopsoas
Most Common Running Injuries
 Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Coccydynia. (Coccyx Pain) Information for patients. Outpatients Physiotherapy Tel: 01473 703312
 Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Information for patients Coccydynia (Coccyx Pain) Outpatients Physiotherapy Tel: 01473 703312 DPS ref: 4508-12(RP) Issue 1: February 2013 Review date: January 2016 The Ipswich Hospital NHS Trust, 2013.
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Fact sheet Exercises for older adults undergoing rehabilitation
 Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
Fact sheet Exercises for older adults undergoing rehabilitation Flexibility refers to the amount of movement possible around a joint and is necessary for normal activities of daily living such as stretching,
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS.
 ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
SPINE SURGERY - LUMBAR DECOMPRESSION
 SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
SPINE SURGERY - LUMBAR DECOMPRESSION Information Leaflet Your Health. Our Priority. Page 2 of 7 Introduction This booklet has been compiled by the physiotherapy department to help you understand lumbar
Lumbar/Core Strength and Stability Exercises
 Athletic Medicine Lumbar/Core Strength and Stability Exercises Introduction Low back pain can be the result of many different things. Pain can be triggered by some combination of overuse, muscle strain,
Athletic Medicine Lumbar/Core Strength and Stability Exercises Introduction Low back pain can be the result of many different things. Pain can be triggered by some combination of overuse, muscle strain,
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
M A S S A G E & B O D Y WO R K
 ESSENTIALSKILLS 108 MASSAGE & BODYWORK FEBRUARY/MARCH 2006 The Mystery of Low-Back Pain, Part II Ligament Tears By Ben E. Benjamin In the first article in this series, we examined the anatomy of the low
ESSENTIALSKILLS 108 MASSAGE & BODYWORK FEBRUARY/MARCH 2006 The Mystery of Low-Back Pain, Part II Ligament Tears By Ben E. Benjamin In the first article in this series, we examined the anatomy of the low
This is caused by muscle strain to the Achilles tendon in the heel of the foot.
 Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Avoid The Dreaded Back Injury by Proper Lifting Techniques
 Avoid The Dreaded Back Injury by Proper Lifting Techniques If you ve ever strained your back while lifting something, you ll know the importance of lifting safely. Agenda Introduction About the Back The
Avoid The Dreaded Back Injury by Proper Lifting Techniques If you ve ever strained your back while lifting something, you ll know the importance of lifting safely. Agenda Introduction About the Back The
Herniated Disk. This reference summary explains herniated disks. It discusses symptoms and causes of the condition, as well as treatment options.
 Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
Herniated Disk Introduction Your backbone, or spine, has 24 moveable vertebrae made of bone. Between the bones are soft disks filled with a jelly-like substance. These disks cushion the vertebrae and keep
How To Treat Heel Pain
 Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Qigong. Ba Duan Jin. The Eight Pieces of Brocade
 Qigong Ba Duan Jin The Eight Pieces of Brocade by Col and g Hamilton Yiheyuan Martial Arts Contents Page Introduction 2 Preparation 2 1. Hold up the Sky 3 2. The Archer 4 3. Join Heaven and Earth 5 4a.
Qigong Ba Duan Jin The Eight Pieces of Brocade by Col and g Hamilton Yiheyuan Martial Arts Contents Page Introduction 2 Preparation 2 1. Hold up the Sky 3 2. The Archer 4 3. Join Heaven and Earth 5 4a.
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
SELF-MASSAGE HANDOUTS
 SELF-MASSAGE HANDOUTS Self-Massage for the Head and Face Self-Massage for the Low Back and Buttocks Self-Massage for Runners Self-Massage for the Neck Self-Massage for the Feet Self-Massage for the Arms
SELF-MASSAGE HANDOUTS Self-Massage for the Head and Face Self-Massage for the Low Back and Buttocks Self-Massage for Runners Self-Massage for the Neck Self-Massage for the Feet Self-Massage for the Arms
TheraCane. Owner's Manual
 TheraCane Owner's Manual THERA CANE 411 Thera Cane is a therapeutic massager that allows you to apply pressure to treat muscle dysfunction. Benefits of using the Thera Cane Eliminate painful knots in your
TheraCane Owner's Manual THERA CANE 411 Thera Cane is a therapeutic massager that allows you to apply pressure to treat muscle dysfunction. Benefits of using the Thera Cane Eliminate painful knots in your
Hip Pain HealthshareHull Information for Guided Patient Management
 HealthshareHull Information for Guided Patient Management Index Introduction 2 About your hip 2 Common causes of hip pain 3 Trochanteric bursitis/greater trochanter pain syndrome 4 Impingement 5 Referred
HealthshareHull Information for Guided Patient Management Index Introduction 2 About your hip 2 Common causes of hip pain 3 Trochanteric bursitis/greater trochanter pain syndrome 4 Impingement 5 Referred
Treatment Options for Rotator Cuff Tears A Guide for Adults
 Treatment Options for Rotator Cuff Tears A Guide for Adults Is This Guide for Me? YES, if your doctor has told you that you have a rotator cuff tear, which is an injury to one or more of the muscles and
Treatment Options for Rotator Cuff Tears A Guide for Adults Is This Guide for Me? YES, if your doctor has told you that you have a rotator cuff tear, which is an injury to one or more of the muscles and
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
A Stretch-Break Program for Your Workplace! www.healthyworkplaceweek.ca
 www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
www.healthyworkplaceweek.ca A Stretch-Break Program for Your Workplace! Why is stretching at work important? Sitting at a desk or computer; or standing at your work station for extended periods of time
