SPINE, LOWER EXTREMITY, AND PELVIC IMPAIRMENT SECTION
|
|
|
- Nathan O’Neal’
- 9 years ago
- Views:
Transcription
1 SPINE, LOWER EXTREMITY, AND PELVIC IMPAIRMENT SECTION Lev.II Curriculum Rev. 6/09 99
2 OBJECTIVES FOR SPINAL, LOWER EXTREMITY, AND PELVIC IMPAIRMENT RATING SECTION 1. Demonstrate ability to properly measure range of motion for all joints found in the lower extremity. 2. Be able to use Table 53 - Impairments Due to Specific Disorders of the Spine - to determine impairment for specific clinical diagnoses. 3. Correctly determine pelvic impairment in a case scenario. 4. Determine spinal nerve root dysfunction accurately using a specific case scenario. 5. Use correctly all tables found in this chapter, including: Table 47-Impairment of the Digits Foot Lower Extremity and Whole Person due to Amputations, Table 45-Impairments of the Lower Extremity Due to Other Disorders of the Hip Joint, Table 52-Impairment of the Lower Extremity Due to Peripheral Vascular Disease, and Table 40 Impairment Ratings of the Lower Extremity for other Disorders of the Knee. 6. Demonstrate the ability to combine all the appropriate factors used in a spinal case and determine a correct impairment rating. 7. Report clinical cases properly on Figure 83, Lumbar Range of Motion form, found on Pages 84 and Demonstrate the ability to properly use the inclinometer to measure cervical, thoracic, and lumbar ranges of motion. (Performed in workshop) Lev.II Curriculum Rev. 6/09 100
3 SPINAL, LOWER EXTREMITY, AND PELVIC IMPAIRMENT LOWER EXTREMITY Definition of ankylosis "complete absence of motion or planar restriction of motion preventing the subject from reaching the neutral position of motion in that plane." Amputation When an amputation occurs at a joint the physician is required to calculate the percentage impairment. Refer to Table 47, p.73 for a summary of impairments due to amputations, except when calculating amputation of the toes as stated below. Distal amputation - if the amputation occurs distal to the distal joint, the percentage of lost bone is multiplied by the total percentage of loss given on the table for amputation at the distal joint. See p.56 for example. Proximal amputation - if the loss occurs between 2 joints - the full impairment for the lost distal portion is added to the percentage of the bone lost between the joints multiplied by the remaining impairment at the proximal joint. The remaining impairment at the proximal joint is equal to the impairment given on the appropriate table for amputation at the joint minus the full impairment for amputation at the distal joint. See p.57 for example. Great Toe Measure range of motion of both MTP and IP joints Table 24, p.56, interphalangeal joint - flexion and extension Add the range of motion deficits at each joint. Combine the total ROM deficits for MTP and IP. Combine ROM deficit with any amputation impairment. Convert to foot rating using Table 27, p.59. 2nd through 5th Toe - Range of Motion Determine range of motion of applicable joints. Table 28, p.60 - distal interphalangeal 2nd - 5th Toe dorsi-plantar flexion and amputation Table 29, p.60 - proximal interphalangeal joint 2nd - 5th toe dorsi-plantar flexion and amputation Table 30, p.61 metatarsophalangeal joint - 2nd toe dorsi-plantar flexion and amputation Table 31, p.62-3rd metatarsophalangeal joint dorsi-plantar flexion Table 32, p.62-4th metatarsophalangeal joint dorsi-plantar flexion Table 33, p.63-5th metatarsophalangeal joint dorsi-plantar flexion Lev.II Curriculum Rev. 6/09 101
4 Add range of motion deficits at each joint. Combine the total ROM for each joint. Combine ROM with amputation deficits. Convert to foot rating using Table 34, p. 64. Multiple toe involvement. Impairment of each toe expressed as a percentage of the foot. These values are added to arrive at the total foot impairment. Also see Table 35, p.64 - Impairment of Foot Due to Amputation and Ankylosis of Multiple Digits. Hind Foot Partial Foot Amputations - see Table 47, Page 73. Measure range of motion for dorsal and plantar flexion and inversion and eversion Table 37, p.66 dorsi-plantar flexion of hind foot Table 38, p.67 inversion and eversion of hind foot Add range of motion deficits For ankylosis, - use the larger value for dorsi-plantar flexion and inversion/eversion Do not add or combine. Knee joint Refer to Table 40, p.68 (Disorders of the Knee) for diagnostic and surgical impairments. Measure range of motion - Table 39, p. 68 flexion and extension Add flexion and extension deficits. Combine Table 40 deficits with range of motion deficits. For amputation of leg below knee, see Table 47, p.73. This value would be combined with the knee joint deficit if applicable. Lev.II Curriculum Rev. 6/09 102
5 Hip Joint Measure range of motion of hip - abduction, adduction, flexion, extension and internal and external rotation. Table 41, p.69 flexion Table 42, p.70 extension Table 43, p.70 abduction, adduction Table 44, p.70 internal and external rotation Add all range of motion deficits If joint is ankylosed, determine ankylosis measurements for all ranges of motion. Do not add or combine values. Use the largest impairment rating for ankylosis. Consult Table 45, p.72 for hip diagnoses which may be combined with the range of motion deficit. Other amputation deficits are found on Table 47, p.73. Multiple Unit Involvement Combine ratings in order from distal to most proximal rating using combined value chart. Convert to whole person rating using Table 46, p.72 Remember to report lower extremity and whole person impairment on all forms. Peripheral Nervous System Disorders The nerves are graded for sensory and motor deficits as discussed in the Neurological section. Table 49, p.76 gives maximum loss for L 3 -S 1 nerve roots. Other nerve tables are found on pages 76 and 77. Use Table 10, p.42 for sensation gradation and Table 11, p.42 for motor gradation. Strength testing is based on confrontational resistance testing. Vascular disorders of the lower extremity Rated per Table 52, p.79 Summary of evaluation of impairment of the lower extremity Complete the lower extremity impairment form found on the following page Make all measurements in relation to the "Neutral Position." Work within 1 unit at a time toes, ankle, knee, hip. A. Make all of the pertinent measurements, unit by unit. B. Multiple planes of motion 1 joint ADD individual impairments. C. Multiple joints 1 unit COMBINE individual impairments. D. Ankylosis use only the plane of motion yielding the highest impairment. E. Amputations Sliding scale based on % of amputation. F. COMBINE B through E above to determine unit impairment. Only combine impairments from individual units after they have been converted to the same level toe, foot or lower extremity. Lev.II Curriculum Rev. 6/09 103
6 Convert each total unit impairment to lower extremity impairment and combine distal to proximal. Remember the additional lower extremity impairments for specific disorders of the knee (Table 40) and hip (Table 45). Consider impairment due to Peripheral Nervous System. Consider impairment due to Peripheral Vascular Disease. Combine all impairments obtained in the above to obtain Total Lower Extremity Impairment. Use Table 46 on page 72 to obtain the equivalent Whole Person Impairment and report both. When impairment is bilateral, each lower extremity is rated as whole person separately and both ratings are combined for final whole person rating. Lev.II Curriculum Rev. 6/09 104
7 Lower Extremity Impairment Record Patient Name: Lev.II Curriculum Rev. 6/09 105
8 Part II (Hind Foot, Knee, Hip) Side: Right Left Date: Abnormal Motion H I N D F O O T K N E E Table 37 Dorsiflex Plantar Ankylosis Impair % Angle Impairment Table 38 Inversion Eversion Ankylosis Impair % Angle Impairment List Other Disorders Regional Impairment % Add Impairment % of ROM or use largest Ankylosis: (1) Impairment % (2) Combine (1) and (2) = Table 39 Flexion Extension Ankylosis Impair % Angle Impairment Table 40 Diagnosis: Amputation Impairment % (Table 47) H I P Add Impairment % of ROM or use largest Ankylosis: (1) Impairment % (2) Combine (1) and (2) = Table 41, 42 Flexion Extension Ankylosis Impair % Angle Impairment Table 43 Abduction Adduction Ankylosis Impair % Angle Impairment Table 44 Rotations Angle Impairment Internal External Ankylosis Impair % Table 45 Diagnosis: Add Impairment % of ROM or use largest Ankylosis: (1) Impairment % (2) Combine (1) and (2) = I. Combine all the above Impairments: [Foot= ] [Hind Foot= ] [Knee= ] [ Hip= ]:Combined Total= II. Peripheral Nervous System Impairment Computations: A. Sensation: B. Motor: Combined Sensory and Motor= III. Peripheral Vascular System Impairment Computations: Total Lower Extremity Impairment: Impairment of the Whole Person (Table 46) Lev.II Curriculum Rev. 6/09 106
9 SPINAL IMPAIRMENT Essential Elements of the Exam Report all of the following physical findings: Inspection Palpation Range of Motion Testing Sensation Muscle Strength Reflexes Straight Leg Raise Psychometric Testing Additional elements that must be reviewed and commented on include: chief complaint, history of present illness, past medical history, review of systems, family history and social history. Rating must be done when the patient does not have an acute illness or acute spasm. Use Table 53 or 54 to determine if the patient qualifies for a spinal impairment. If Table 53 rating is used, spinal range of motion must be completed and applied to the rating. Diagnoses Related Factors Only the primary diagnoses in a given region can be considered for rating. For example, if a patient received an L 4 fracture he should not receive ratings for the cervical, thoracic and lumbar portions of the spine since only the lumbar area was injured. On the other hand, if the patient fractured a cervical vertebrae and L 4 then he would receive ratings for the cervical and the lumbar areas. Table 53, p.80 gives ratings for fractures, intervertebral discs, soft tissue lesions, spondylolysis and spondylolisthesis as well as spinal stenosis. Table 54, p.86 cannot be used in addition to Table 53 but may be used instead of Table 53 if ankylosis is determined by radiography. Table 54 cannot be combined with range of motion. Table 53, p.80 Fractures Vertebral body compression fractures Posterior element fractures - combine (not add!) Dislocations - combine (not add!) Lev.II Curriculum Rev. 6/09 107
10 Intervertebral disc or other soft tissue lesions Review this section. Medically documented rigidity associated with an injury -related diagnosis is the minimum requirement for a rating. Note subparagraph F - deals with the issue of multiple levels, and G with multiple operations - 1 or 2% is added per level depending on the situation. Spondylolysis and spondylolisthesis, non-operated Grades I and II - note requirements Grades III and IV - note requirements Spinal stenosis, segmental instability, or spondylolisthesis, operated The "fine print" Address the regions of the spine separately. Combine above impairments with other residuals using the Combined Values Chart. Definition of "residual signs or symptoms" - Ankylosis - Abnormal motion in spine or extremities - Spinal cord or spinal nerve root injuries with neuropathic impairment - Note absence of chronic pain complaints Range of Motion Testing Recognize the complexity of spinal motion Impossible to isolate, selected segmental motion Measure the upper and lower extremes of the segment to be rated The ROM tester is encouraged to have the examinee stretch thoroughly before beginning measurements. The pelvis must remain stationary throughout the straight leg raising measurement. As soon as the tester begins to feel a rocking motion of the pelvis the straight leg raising motion should cease. The straight leg raising is not a passive measurement. Inclinometer method will be reviewed in the workshop. Range of motion testing of the spine Use maximum range of motion measurements. Test Validity Criteria for Spinal ROM (amended as of July 22, 1994) Lev.II Curriculum Rev. 6/09 108
11 - A set of valid measurements for the maximum cervical, thoracic and lumbar angles consists of 3 measurements of a motion which are within ± 10% or 5º of the median value. - A minimum of two sets of three full measurements must be taken before invalidating the first trial. If these do not meet validity criteria then additional measurements, up to two sets of three, must be taken on a separate testing date before the examiner can declare the range of motion results invalid. - There is an additional test for validity which pertains to Lumbar flexion only. The tightest of the two maximum straight leg raise angles minus (hip flexion + hip extension) must be 10º. Add whole person impairments due to restriction of motion in each plane to attain whole person impairment due to restriction of motion. Ankylosis measurements. Ankylosis nicely defined in this edition - Page Complete absence of motion. - Inability to achieve the neutral position of motion in a given plane. Ankylosis and restriction of motion in a given plane are mutually exclusive. Table 55, p.88 - Cervical flexion extension Table 56, p.90 - Cervical lateral flexion Table 57, p.90 - Cervical rotation Table 58, p.96 - Thoracic flexion extension Table 59, p.96 - Thoracic rotation Table 60, p.98 - Lumbar flexion and extension Remember that the "true lumbar flexion" angle is found by subtracting the sacral (hip) inclination from the T 12 inclination and the "true lumbar extension" is found by subtracting the sacral (hip) angle from the T 12 inclinometer angle. Table 61, p.98 - Lumbar lateral flexion Neurological Findings See Neurological section and Lower Extremity section. Remember to translate all impairment into whole body ratings before combining with other spinal impairments. No "double dipping" - e.g., Do not rate both restriction of motion of ankle dorsiflexion and decreased motor strength of muscles dorsiflexing the ankle due to nerve root injury - unless they are independent processes. Lev.II Curriculum Rev. 6/09 109
12 Use of standardized forms in the Guides is required by the Division Figures for Range of Motion/Validity checks [NOTE: In some copies an error exists on Fig. 83. Please check your book and correct as necessary. Under Straight Leg Raising, Right and Left, 10% should read 10º.] Figure 84 for Spine Impairment Summary May be reproduced without permission by A.M.A. Summary of the spine impairment process Determine the primarily injured region Determine diagnosis-related whole person impairment "only the primary diagnosis should be considered" Determine regional range of motion to obtain whole person impairment due to loss of motion/ankylosis Remember mandatory validity checks Combine diagnosis-related and range of motion/ankylosis-based whole person impairments Repeat the preceding process for secondarily impaired spinal regions Combine whole person impairments for the various spinal regions Determine additional extremity impairments due to radiculopathy and convert these impairments to whole person impairment Combine the whole person impairments obtained in the previous two steps to determine the total whole personal impairment to the spine Combine spine-related whole person impairment with any whole person impairment due to other organ system conditions to arrive at a final whole person impairment If apportionment is appropriate because the patient qualified for a pre-injury rating under Table 53 but no pre-injury range of motion measurements were taken, complete the ROM apportionment worksheet found at the end of the administrative section of this curriculum. PELVIS Fractures of the pelvis are rated per p.101. Whole person ratings are given for healed fractures with and without displacement, deformity, and residuals. Lev.II Curriculum Rev. 6/09 110
13 Spinal Measurement Techniques Inclinometer Method Philosophy: The healthy spine is composed of 24 moving vertebrae, 1 sacrum and 1 coccyx. Each segment has the potential to move and this movement is measurable as is common of diarthrodial joints. (1) The loss of spinal mobility may lead to disability and loss of function. (2) It is, therefore, medically necessary to ascertain any loss of motion and document it accurately. Objectives: 1. Measure the cervical, thoracic and lumbopelvic motions in the classic planes as defined by Dr. Tom Mayer, et.al. 2. Implement validity checks to ensure that the measurements are indeed valid, accurate and reproducible 3. Identify invalid range of motion efforts Bubble Inclinometer Measurement Techniques: 1. The patient must be an appropriate candidate for impairment rating as outlined in the AMA Guides to Impairment. 2. Instruct patient in proper movements, three to five repetitions 3. Landmark 4. Inclinometer placement 5. Measure spinal motion A. Cervical 1. Landmark: a. upper inclinometer: Midsagittal line of the occipital bone or midcoronal line of the parietal bone b. lower inclinometer: Midsagittal line of the first thoracic vertebrae Lev.II Curriculum Rev. 6/09 111
14 2. Place the inclinometers on the landmarks so that gravity will affect the liquid within the inclinometer (sagittal plane). 3. Hold the inclinometer firmly in place and request the patient to complete the desired motion. 4. Repeat the measurements three (3) times and check for consistency of efforts. 5. Pitfalls: often the inclinometer is not held steady as the patient flexes the neck. B. Thoracic 1. Landmark: a. upper inclinometer: Midsagittal line of the spinous process of the first thoracic vertebrae b. lower inclinometer: Midsagittal line of the spinous process of the twelfth thoracic vertebrae 2. Place the inclinometer over the landmarks so that gravity will affect the liquid within. For measuring kyphosis and flexion, the inclinometer must be in the sagittal plane and for measuring rotation, the inclinometer must be in the coronal plane. 3. Hold the inclinometer firmly in place and request the patient to complete the desired motion. 4. Repeat steps 4 and 5 of the cervical section 5. Pitfalls: a. scapular retraction will tilt the inclinometer and inflate the upper inclinometer reading during rotation. b. knee flexion of the contralateral side will affect the readings during rotation. c. often the patient cannot bend to 90 degrees of trunk flexion when measuring rotation and consequently, the inclinometer must be angled perpendicular to gravity in order to get the proper reading. d. when reading minimum kyphosis, it is easiest to add the T-1 and T-12 measurements, i.e., values above the zero are positive and values below zero are negative. Subtraction of a negative number is defined as changing the sign and adding. Lev.II Curriculum Rev. 6/09 112
15 C. Lumbar 1. Landmark a. upper inclinometer: Midsagittal line of the spinous process of the twelfth thoracic vertebrae b. Midsagittal line of the second fused vertebrae of the sacrum. 2. Place the inclinometer over the landmark so that gravity will affect the liquid within the inclinometer. 3. Repeat steps 3, 4 and 5 of the cervical section. 4. Pitfalls: a. Patient bends knees b. Patient lifts foot during side bending c. The inclinometer moves D. Straight leg raise 1. Landmark: a. distal two thirds of the anterior tibia 2. Place the inclinometer over the landmark 3. Request patient to complete a straight leg raise while holding the opposite leg down. 4. Read the correct scale of the inclinometer once the end of range is achieved and document it. 5. Repeat the motions three times and check for consistency of efforts. 6. Pitfalls: a. patient bends the knees b. patient jerks the leg at end range 6. Calculate validity of efforts as outline in the AMA Guides 7. Notifying the patient of their efforts A. Valid efforts B. Invalid efforts Physician must retest the patient once in an attempt to obtain a valid range of motion exam. 8. Correlate findings to norms and calculate impairment rating if all of the criterion are reached. Lev.II Curriculum Rev. 6/09 113
16 Spinal Apportionment form goes here. May be found on Division s website as DeskAid 10 (DK 10), Lev.II Curriculum Rev. 6/09 114
17 CURRICULUM - LEVEL II ACCREDITATION DAY 2 TOPICS Impairment of the Pulmonary/Cardiovascular System Impairment for Skin Diseases - to include scars and disfigurement Impairment Ratings for Vision, Hearing, Ear, Nose, and Throat and Gastrointestinal conditions Mental Impairment Workshops: Pulmonary/Cardiovascular Mental Impairment Written Accreditation Examination *Order of topics for actual seminar agenda is subject to change Lev.II Curriculum Rev. 6/09 115
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
AMA Guides 6 th Edition AADEP SPINE EXAMPLES
 AMA Guides 6 th Edition AADEP SPINE EXAMPLES 1 Questions? James B. Talmage MD, Occupational Health Center, 315 N. Washington Ave, Suite 165 Cookeville, TN 38501 Phone 931-526-1604 (Fax 526-7378) [email protected]
AMA Guides 6 th Edition AADEP SPINE EXAMPLES 1 Questions? James B. Talmage MD, Occupational Health Center, 315 N. Washington Ave, Suite 165 Cookeville, TN 38501 Phone 931-526-1604 (Fax 526-7378) [email protected]
SPINE. Postural Malalignments 4/9/2015. Cervical Spine Evaluation. Thoracic Spine Evaluation. Observations. Assess position of head and neck
 SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
SPINE Observations Body type Postural alignments and asymmetries should be observed from all views Assess height differences between anatomical landmarks Figure 25-9 Figure 25-10 Figure 25-11 & 12 Postural
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE
 PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
The Essential Lower Back Exam
 STFM National Convention 2011 New Orleans The Essential Lower Back Exam Judith A. Furlong, M.D., Cathee McGonigle, D.O. & Rob Rutherford, MD Objectives Brief review of the anatomy of the back, (hip and
STFM National Convention 2011 New Orleans The Essential Lower Back Exam Judith A. Furlong, M.D., Cathee McGonigle, D.O. & Rob Rutherford, MD Objectives Brief review of the anatomy of the back, (hip and
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds
 Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
International Standards for the Classification of Spinal Cord Injury Motor Exam Guide
 C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
Guidelines for the table of injuries. For injuries on or after 2 November 2005
 For injuries on or after 2 November 2005 Background Changes to the Table of injuries (TOI) were made in 2005 and are now adopted by the Medical Assessment Tribunal at Q-COMP. The major differences between
For injuries on or after 2 November 2005 Background Changes to the Table of injuries (TOI) were made in 2005 and are now adopted by the Medical Assessment Tribunal at Q-COMP. The major differences between
2. Whenever possible, and reasonable, impairment ratings will be established strictly in accordance with the Rating Schedule attached as Appendix A.
 Section Policy 40 44.90.10 Section Title: Benefits Administration - Adjudication & Compensation Subject: Permanent Impairment Rating Effective Date: For decisions on or after January 1, 2015 GENERAL INFORMATION
Section Policy 40 44.90.10 Section Title: Benefits Administration - Adjudication & Compensation Subject: Permanent Impairment Rating Effective Date: For decisions on or after January 1, 2015 GENERAL INFORMATION
Structure and Function of the Hip
 Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Structure and Function of the Hip Objectives Identify the bones and bony landmarks of the hip and pelvis Identify and describe the supporting structures of the hip joint Describe the kinematics of the
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions *
 ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions * Finding the ICD-10 equivalent for an ICD-9 code can be a challenge. This resource of frequently used codes can help when
ICD-10 Cheat Sheet Frequently Used ICD-10 Codes for Musculoskeletal Conditions * Finding the ICD-10 equivalent for an ICD-9 code can be a challenge. This resource of frequently used codes can help when
Chiropractic ICD 9 Code List
 Use of valid ICD 9 codes, billed with appropriate and corresponding CPT codes, benefits providers by facilitating treatment authorization and claims payment. The use of valid and appropriate codes also
Use of valid ICD 9 codes, billed with appropriate and corresponding CPT codes, benefits providers by facilitating treatment authorization and claims payment. The use of valid and appropriate codes also
Pain Management Top Diagnosis Codes (Crosswalk)
 Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
Spine Evaluation. Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Spine Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling? Mechanism:
Spine Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling? Mechanism:
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Spinal Anatomy. * MedX research contends that the lumbar region really starts at T-11, based upon the attributes of the vertebra.
 Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
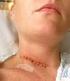 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
LOW BACK PAIN EXAMINATION
 LOW BACK PAIN EXAMINATION John Petty, M.D. Medical Director Department of Physical Medicine & Rehabilitation Kettering Medical Center February 8, 2014 PRE-TEST QUESTION What part of the low back physical
LOW BACK PAIN EXAMINATION John Petty, M.D. Medical Director Department of Physical Medicine & Rehabilitation Kettering Medical Center February 8, 2014 PRE-TEST QUESTION What part of the low back physical
Workplace Health, Safety and Compensation Commission of Newfoundland and Labrador. Permanent Functional Impairment (PFI) rating schedule
 Safety and Compensation Commission of Newfoundland and Labrador Permanent Functional Impairment (PFI) rating schedule Safety and Compensation Commission of Newfoundland and Labrador Permanent Functional
Safety and Compensation Commission of Newfoundland and Labrador Permanent Functional Impairment (PFI) rating schedule Safety and Compensation Commission of Newfoundland and Labrador Permanent Functional
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Chapter 3 Impairment of Spine and Limbs
 Chapter 3 of Spine and Limbs This chapter contains six parts: Part 3.1 Upper Limbs Part 3.2 Lower Limbs Part 3.3 Spine Part 3.4 Resting Joint Pain Part 3.5 Ranges of Joint Movement Part 3.6 Spine and Limbs
Chapter 3 of Spine and Limbs This chapter contains six parts: Part 3.1 Upper Limbs Part 3.2 Lower Limbs Part 3.3 Spine Part 3.4 Resting Joint Pain Part 3.5 Ranges of Joint Movement Part 3.6 Spine and Limbs
Massage and Movement
 Massage and Movement Incorporating Movement into Massage Part One: Theory and Technique in Prone With Lee Stang, LMT NCBTMB #450217-06 1850 West Street Southington, CT 06489 860.747.6388 www.bridgestohealthseminars.com
Massage and Movement Incorporating Movement into Massage Part One: Theory and Technique in Prone With Lee Stang, LMT NCBTMB #450217-06 1850 West Street Southington, CT 06489 860.747.6388 www.bridgestohealthseminars.com
Info. from the nurses of the Medical Service. LOWER BACK PAIN Exercise guide
 Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Info. from the nurses of the Medical Service LOWER BACK PAIN Exercise guide GS/ME 03/2009 EXERCISE GUIDE One of the core messages for people suffering with lower back pain is to REMAIN ACTIVE. This leaflet
Objectives. Spinal Fractures: Classification Diagnosis and Treatment. Level of Fracture. Neuro exam Muscle Grading
 Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Objectives Spinal Fractures: Classification Diagnosis and Treatment Johannes Bernbeck,, MD Review and apply the understanding of incidence and etiology of VCF. Examine conservative and operative management
Florida Uniform Permanent Impairment Rating Schedule
 1996 Flida Unifm Permanent Impairment Rating Schedule 1996 FLORIDA UNIFORM PERMANENT IMPAIRMENT RATING SCHEDULE ii 1996 FLORIDA UNIFORM PERMANENT IMPAIRMENT RATING SCHEDULE This impairment rating guide
1996 Flida Unifm Permanent Impairment Rating Schedule 1996 FLORIDA UNIFORM PERMANENT IMPAIRMENT RATING SCHEDULE ii 1996 FLORIDA UNIFORM PERMANENT IMPAIRMENT RATING SCHEDULE This impairment rating guide
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Integrated Low Back Examination
 Integrated Low Back Examination William Thomas, DO, VCOM PPC/OMM Internal Medicine, Pediatrics and Sports Medicine October 2015 Special thanks and appreciation to Mark Rogers, DO Objectives Utilize history
Integrated Low Back Examination William Thomas, DO, VCOM PPC/OMM Internal Medicine, Pediatrics and Sports Medicine October 2015 Special thanks and appreciation to Mark Rogers, DO Objectives Utilize history
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Colossus Important Diagnoses. Instructions for How to List Diagnoses
 1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information
 Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
Lumbar Spondylolisthesis or Anterolisthesis Patient Educational Information What is a Spondylolisthesis or Anterolisthesis? Spondylolisthesis is a condition of the spine when one of the vertebra slips
CHA SERIES. Key Chiropractic Concepts for the CHA. Ontario Chiropractic Association. Treatment That Stands Up.
 CHA SERIES Key Chiropractic Concepts for the CHA AGENDA Welcome & Introductions About Chiropractic Terminology ABOUT CHIROPRACTIC You will get lots of questions about the profession & chiropractic care
CHA SERIES Key Chiropractic Concepts for the CHA AGENDA Welcome & Introductions About Chiropractic Terminology ABOUT CHIROPRACTIC You will get lots of questions about the profession & chiropractic care
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
PHYSICAL EXAMINATION
 The Evidence Based Clinical Examination of the Lumbar Spine, Pelvis, & Hip POSITION Standing PHYSICAL EXAMINATION Neurologic -Motor: Heel Walk (L4-5) Toe Raise (L5-S1) Squat or Step-up (L3-4) Observation/Palpation
The Evidence Based Clinical Examination of the Lumbar Spine, Pelvis, & Hip POSITION Standing PHYSICAL EXAMINATION Neurologic -Motor: Heel Walk (L4-5) Toe Raise (L5-S1) Squat or Step-up (L3-4) Observation/Palpation
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Diagnostic Imaging Exams
 Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Workplace Health, Safety & Compensation Review Division
 Workplace Health, Safety & Compensation Review Division WHSCRD Case No: 14152-06 WHSCC Claim No: 606499 and 791748 Decision Number: 14147 Lloyd Piercey Review Commissioner The Review Proceedings 1. The
Workplace Health, Safety & Compensation Review Division WHSCRD Case No: 14152-06 WHSCC Claim No: 606499 and 791748 Decision Number: 14147 Lloyd Piercey Review Commissioner The Review Proceedings 1. The
Coaching the Injury Prone Athlete. www.englandathletics.org www.englandathletics.org/east
 Coaching the Injury Prone Athlete Injury! The Causes? Frequently the consequence of poor physical preparation ( accidents excluded) Exceeding training loads the athlete can handle at that time Volume,
Coaching the Injury Prone Athlete Injury! The Causes? Frequently the consequence of poor physical preparation ( accidents excluded) Exceeding training loads the athlete can handle at that time Volume,
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Stretching the Low Back THERAPIST ASSISTED AND CLIENT SELF-CARE STRETCHES FOR THE LUMBOSACRAL SPINE
 EXPERT CONTENT by Joseph E. Muscolino photos by Yanik Chauvin body mechanics THE ESSENCE OF MOST MANUAL THERAPIES, and certainly clinical orthopedic massage therapy, is to loosen taut soft tissues, thereby
EXPERT CONTENT by Joseph E. Muscolino photos by Yanik Chauvin body mechanics THE ESSENCE OF MOST MANUAL THERAPIES, and certainly clinical orthopedic massage therapy, is to loosen taut soft tissues, thereby
Injury Prevention for the Back and Neck
 Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
MET: Posterior (backward) Rotation of the Innominate Bone.
 MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
MET: Posterior (backward) Rotation of the Innominate Bone. Purpose: To reduce an anterior rotation of the innominate bone at the SI joint. To increase posterior (backward) rotation of the SI joint. Precautions:
Request for Designated Doctor Examination Type (or print in black ink) each item on this form
 Texas Department of Insurance Division of Workers Compensation 7551 Metro Center Drive, Suite 100 MS-603 Austin, TX 78744-1645 (512) 804-4380 phone (512) 804-4121 fax Complete, if known: DWC Claim # Carrier
Texas Department of Insurance Division of Workers Compensation 7551 Metro Center Drive, Suite 100 MS-603 Austin, TX 78744-1645 (512) 804-4380 phone (512) 804-4121 fax Complete, if known: DWC Claim # Carrier
Claim closing and other impairment-focused examinations and forms for reporting impairments
 Oregon Kate Brown, Governor Department of Consumer and Business Services Workers Compensation Division 350 Winter St. NE PO Box 14480 Salem, OR 97309-0405 1-800-452-0288, 503-947-7810 www.wcd.oregon.org
Oregon Kate Brown, Governor Department of Consumer and Business Services Workers Compensation Division 350 Winter St. NE PO Box 14480 Salem, OR 97309-0405 1-800-452-0288, 503-947-7810 www.wcd.oregon.org
How To Write An Icd10
 Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
ICD10 Chiropractic Diagnosis Codes
 ICD10 Chiropractic Diagnosis Codes Disclaimer: When the ICD-10 code requires a 7th character, the code shown assumes "initial." Disclaimer: This information is based on the General Equivalency Mapping
ICD10 Chiropractic Diagnosis Codes Disclaimer: When the ICD-10 code requires a 7th character, the code shown assumes "initial." Disclaimer: This information is based on the General Equivalency Mapping
Spine Injury and Back Pain in Sports
 Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Spine Biomechanics, Intervertebral Disc &LBP
 Spine Biomechanics, Intervertebral Disc &LBP Spine Cervical Spine Seven vertebrae C 1-71 More flexible Supports the head Wide range of motion Rotation to left and right Flexion Up and down Peripheral
Spine Biomechanics, Intervertebral Disc &LBP Spine Cervical Spine Seven vertebrae C 1-71 More flexible Supports the head Wide range of motion Rotation to left and right Flexion Up and down Peripheral
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
The Petrylaw Lawsuits Settlements and Injury Settlement Report BACK INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Back Injury Cases The Petrylaw Lawsuits Settlements and Injury
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
Vertebral anatomy study guide. Human Structure Summer 2015. Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey.
 Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Application for a Medical Impairment Rating (MIR)
 STATE OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT Workers Compensation Division Medical Impairment Rating Program 220 French Landing Drive Nashville, TN 37243-1002 Phone (615) 253-1613 Fax
STATE OF TENNESSEE DEPARTMENT OF LABOR AND WORKFORCE DEVELOPMENT Workers Compensation Division Medical Impairment Rating Program 220 French Landing Drive Nashville, TN 37243-1002 Phone (615) 253-1613 Fax
Guidelines for the assessment of the degree of permanent impairment
 13 July 2007 OFFICIAL NOTICES 4581 Guidelines for the assessment of the degree of permanent impairment 1 October 2007 4582 OFFICIAL NOTICES 13 July 2007 Guidelines for the assessment of the degree of permanent
13 July 2007 OFFICIAL NOTICES 4581 Guidelines for the assessment of the degree of permanent impairment 1 October 2007 4582 OFFICIAL NOTICES 13 July 2007 Guidelines for the assessment of the degree of permanent
Body Mechanics for Mammography Technologists
 Body Mechanics for Mammography Technologists Diane Rinella RT(R)(M)(BD)RDMS(BR)CDT Objectives Recognize causes and risk factors for Musculoskeletal Disorders (MSDs) for mammography technologists Understand
Body Mechanics for Mammography Technologists Diane Rinella RT(R)(M)(BD)RDMS(BR)CDT Objectives Recognize causes and risk factors for Musculoskeletal Disorders (MSDs) for mammography technologists Understand
PATHOLOGIC GAIT -- MUSCULOSKELETAL. Focal Weakness. Ankle Dorsiflexion Weakness COMMON GAIT ABNORMALITIES
 Pathological Gait I: Musculoskeletal - 1 PATHOLOGIC GAIT -- MUSCULOSKELETAL Normal walking is the standard against which pathology is measured Efficiency is often reduced in pathology COMMON GAIT ABNORMALITIES
Pathological Gait I: Musculoskeletal - 1 PATHOLOGIC GAIT -- MUSCULOSKELETAL Normal walking is the standard against which pathology is measured Efficiency is often reduced in pathology COMMON GAIT ABNORMALITIES
Coding and Documentation in Practice
 Coding and Documentation in Practice Great Exam Documentation By: Kathy Mills Chang Kathy Mills Chang is a Certified Medical Compliance Expert, Reimbursement Consultant, Medicare Specialist, and a Documentation
Coding and Documentation in Practice Great Exam Documentation By: Kathy Mills Chang Kathy Mills Chang is a Certified Medical Compliance Expert, Reimbursement Consultant, Medicare Specialist, and a Documentation
Tasmanian Workers Compensation Guidelines for the Assessment of Permanent Impairment under the Workers Rehabilitation and Compensation Act 1988
 Tasmanian Workers Compensation Guidelines for the Assessment of Permanent Impairment under the Workers Rehabilitation and Compensation Act 1988 (WorkCover Tasmania Guidelines) November 2001 WORKCOVER TASMANIA
Tasmanian Workers Compensation Guidelines for the Assessment of Permanent Impairment under the Workers Rehabilitation and Compensation Act 1988 (WorkCover Tasmania Guidelines) November 2001 WORKCOVER TASMANIA
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro
 Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 [email protected] ABSTRACT
Study on Structural Behaviour of Human Vertebral Column Using Staad.Pro Healtheephan alexis. S Post graduate student, Government College of Technology, Coimbatore 641 013 [email protected] ABSTRACT
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS
 ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
MD 2016. Back Muscles & Movements Applied Anatomy. A/Prof Chris Briggs Anatomy & Neuroscience
 MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2016 Back Muscles & Movements Applied Anatomy A/Prof Chris Briggs Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Manual Therapy for the Upper and Lower Quadrant: What Do I Need to Know? Objectives
 Manual Therapy for the Upper and Lower Quadrant: What Do I Need to Know? Objectives 1. Describe the current best evidence for manual therapy in the management of a variety of disorders. 2. Recognize subgroups
Manual Therapy for the Upper and Lower Quadrant: What Do I Need to Know? Objectives 1. Describe the current best evidence for manual therapy in the management of a variety of disorders. 2. Recognize subgroups
Spine University s Guide to Kinetic MRIs Detect Disc Herniations
 Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
Spine University s Guide to Kinetic MRIs Detect Disc Herniations 2 Introduction Traditionally, doctors use a procedure called magnetic resonance imaging (MRI) to diagnose disc injuries. Kinetic magnetic
First Year. PT7040- Clinical Skills and Examination II
 First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
First Year Summer PT7010 Anatomical Dissection for Physical Therapists This is a dissection-based, radiographic anatomical study of the spine, lower extremity, and upper extremity as related to physical
No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe
 No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe Introduction Program designed to be performed in a circuit. Perform exercises in sequence without rest 2-3 times. Increase
No Equipment Agility/Core/Strength Program for Full Body No Equip Trainer: Rick Coe Introduction Program designed to be performed in a circuit. Perform exercises in sequence without rest 2-3 times. Increase
Spinal Decompression
 Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Spinal Decompression Spinal decompression is just one more tool we have to treat radiculopathy. With appropriate education and exercises, this modality has been proven to assist in the resolution of symptoms
Nature of Accident Nature of Injury Body Part Code Table
 Nature of Accident Burn or Scald; Heat or Cold Exposure Contact With Chemicals 01 Hot Objects or Substances (Contact with Hot Objects) 02 Temperature Extremes 03 Fire or Flame 04 Steam or Hot Fluids 05
Nature of Accident Burn or Scald; Heat or Cold Exposure Contact With Chemicals 01 Hot Objects or Substances (Contact with Hot Objects) 02 Temperature Extremes 03 Fire or Flame 04 Steam or Hot Fluids 05
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Determining the Posture, Shape and Mobility of the Spine
 Determining the Posture, Shape and Mobility of the Spine The World of Biomechanics Assessment of the Mobility Function Using a special Triple Cervical marker set comprising miniature ultrasound transmitters,
Determining the Posture, Shape and Mobility of the Spine The World of Biomechanics Assessment of the Mobility Function Using a special Triple Cervical marker set comprising miniature ultrasound transmitters,
How to Get and Keep a Healthy Back. Amy Eisenson, B.S. Exercise Physiologist
 How to Get and Keep a Healthy Back Amy Eisenson, B.S. Exercise Physiologist Lesson Objectives Statistics of Back Pain Anatomy of the Spine Causes of Back Pain Four Work Factors Core Muscles Connection
How to Get and Keep a Healthy Back Amy Eisenson, B.S. Exercise Physiologist Lesson Objectives Statistics of Back Pain Anatomy of the Spine Causes of Back Pain Four Work Factors Core Muscles Connection
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Cervical Fusion Protocol
 REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
REHABILITATION DEPARTMENT Cervical Fusion Protocol The following protocol for physical therapy rehabilitation was designed based on the typical patient seen at the Texas Back Institute for the procedure
Spine and Spinal Cord Injuries. William Schecter, MD
 Spine and Spinal Cord Injuries William Schecter, MD Anatomy of the Spine http://education.yahoo.com/reference/gray/fig/387.html Anatomy of the spine 7 cervical vertebrae 12 thoracic vertebrae 5 lumbar
Spine and Spinal Cord Injuries William Schecter, MD Anatomy of the Spine http://education.yahoo.com/reference/gray/fig/387.html Anatomy of the spine 7 cervical vertebrae 12 thoracic vertebrae 5 lumbar
Sciatic Nerve A Case Report of the Treatment of Piriformis Syndrome (Muscle Related)
 Sciatic Nerve A Case Report of the Treatment of Piriformis Syndrome (Muscle Related) Elyse Silvia West August 5, 2007 Pacific Palisades Abstract Objective: The study assessed the benefits of Pilates training
Sciatic Nerve A Case Report of the Treatment of Piriformis Syndrome (Muscle Related) Elyse Silvia West August 5, 2007 Pacific Palisades Abstract Objective: The study assessed the benefits of Pilates training
TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO?
 Cox Case Report #59 by Dr. James Cox published 4/08 1 TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO? A 26-year-old, white,
Cox Case Report #59 by Dr. James Cox published 4/08 1 TWO CONTRASTING CASES OF SCIATIC RADICULOPATHY: ONE WITH NORMAL MRI AND ONE WITH A FREE FRAGMENT. WHAT S A CHIROPRACTOR TO DO? A 26-year-old, white,
THE RELATIONSHIP BETWEEN POSTURE AND HEALTH
 THE RELATIONSHIP BETWEEN POSTURE AND HEALTH Roger Sperry, Ph.D. (Nobel Prize in Physiology or Medicine 1981) discovered that 90% of the brain's activity is used to balance your body within the gravitational
THE RELATIONSHIP BETWEEN POSTURE AND HEALTH Roger Sperry, Ph.D. (Nobel Prize in Physiology or Medicine 1981) discovered that 90% of the brain's activity is used to balance your body within the gravitational
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Evaluation and Treatment of Spine Fractures. Lara C. Portmann, MSN, ACNP-BC
 Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Evaluation and Treatment of Spine Fractures Lara C. Portmann, MSN, ACNP-BC Nurse Practitioner, Neurosurgery, Trauma Services, Intermountain Medical Center; Salt Lake City, Utah Objectives: Identify the
Low Back: Sacroiliac Dysfunction. Presented by Dr. Ben Benjamin
 Debilitating Orthopedic Injury Sampler #1 Low Back: Sacroiliac Dysfunction Presented by Dr. Ben Benjamin 1 Instructor: Ben Benjamin, Ph.D. 2 Instructor: Ben Benjamin, Ph.D. [email protected] 3 1 Thank
Debilitating Orthopedic Injury Sampler #1 Low Back: Sacroiliac Dysfunction Presented by Dr. Ben Benjamin 1 Instructor: Ben Benjamin, Ph.D. 2 Instructor: Ben Benjamin, Ph.D. [email protected] 3 1 Thank
Divisions of the Skeletal System
 OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
 Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
Low Back Pain Mansour Dib MD Physical Medicine and Rehabilitation Pain generators Disc Posterior elements Sacro-iliac joint Education - Spine Positioning Neutral Extension Flexion Disc disease Discogenic
ALBERTA PERMANENT CLINICAL IMPAIRMENT GUIDE
 ALBERTA PERMANENT CLINICAL IMPAIRMENT GUIDE Effective June 1, 1996 BoD Resolution 96/05/33 Table of Contents Introduction The PCI charts and schedules which follow are designed to provide in percentage
ALBERTA PERMANENT CLINICAL IMPAIRMENT GUIDE Effective June 1, 1996 BoD Resolution 96/05/33 Table of Contents Introduction The PCI charts and schedules which follow are designed to provide in percentage
