Mantle cell lymphoma: 2017 update on diagnosis, risk-stratification, and clinical management
|
|
|
- Gordon Cunningham
- 3 years ago
- Views:
Transcription
1 Received: 18 May 2017 Accepted: 18 May 2017 DOI: /ajh ANNUAL CLINICAL UPDATES IN HEMATOLOGICAL MALIGNANCIES: A CONTINUING MEDICAL EDUCATION SERIES Mantle cell lymphoma: 2017 update on diagnosis, risk-stratification, and clinical management Julie M. Vose Division of Hematology/Oncology, University of Nebraska Medical Center, Omaha, Nebraska Correspondence Julie M. Vose, Division of Hematology/ Oncology, University of Nebraska Medical Center, Omaha, NE jmvose@unmc.edu Abstract Disease Overview: Mantle cell lymphoma (MCL) is a non-hodgkin lymphoma characterized by involvement of the lymph nodes, spleen, blood and bone marrow with a short remission duration to standard therapies and a median overall survival (OS) of 4-5 years. Diagnosis: Diagnosis is based on lymph node, bone marrow, or tissue morphology of centrocytic lymphocytes, small cell type, or blastoid variant cells. A chromosomal translocation t (11:14) is the molecular hallmark of MCL, resulting in the overexpression of cyclin D1. Cyclin D1 is detected by immunohistochemistry in 98% of cases. The absence of SOX-11 or a low Ki-67 may correlate with a more indolent form of MCL. The differential diagnosis of MCL includes small lymphocytic lymphoma, marginal zone lymphoma, and follicular lymphoma. Risk Stratification: The MCL International Prognostic Index (MIPI) is the prognostic model most often used and incorporates ECOG performance status, age, leukocyte count, and lactic dehydrogenase. A modification of the MIPI also adds the Ki-67 proliferative index if available. The median OS for the low-risk group was not reached (5-year OS of 60%). The median OS for the intermediate risk group was 51 months and 29 months for the high risk group. Risk-Adapted Therapy: For selected indolent, low MIPI MCL patients, initial observation may be appropriate therapy. For younger patients with intermediate or high risk MIPI MCL, aggressive therapy with a cytotoxic Regimen followed by autologous stem cell transplantation should be considered. Rituximab maintenance after autologous stem cell transplantation has also improved the progression-free and overall survival. For older symptomatic MCL patients with intermediate or high risk MIPI, combination chemotherapy with R-CHOP, R-Bendamustine, or a clinical trial should be considered. In addition, rituximab maintenance therapy may prolong the progression-free survival. At the time of relapse, agents directed at activated pathways in MCL cells such as bortezomib (NFkB inhibitor), lenalidamide (anti-angiogenesis) and Ibruitinib (Bruton s Tyrosine Kinase [BTK] inhibitor) have demonstrated excellent clinical activity in MCL patients. Autologous or allogeneic stem cell transplantation can also be considered in young patients. Clinical trials with novel agents are always a consideration for MCL patients. 1 DISEASE OVERVIEW Mantle cell lymphoma (MCL) was originally identified in the Kiel classification as a centrocytic lymphoma. 1 This type of lymphoma was termed a lymphocytic lymphoma of intermediate differentiation by Berard. 2 A distinct subtype of MCL was characterized by atypical small lymphoid cells with wide mantles around benign germinal centers and was called a mantle zone lymphoma. 3 With the advent of the revised European-American (REAL) and the later World Health Organization (WHO) classifications, MCL was made a distinct lymphoma subtype and was termed an aggressive lymphoma. 4,5 MCL represents about 4% of all lymphomas in the US and 7 9% in Europe VC 2017 Wiley Periodicals, Inc. wileyonlinelibrary.com/journal/ajh Am J Hematol. 2017;92:
2 807 FIGURE 1 A proposed model of molecular pathogenesis and progression of MCL (From Jares et al. 18 ). Patients with MCL have a median age in their 60s and have a striking male predominance (2:1). Patients generally have stage III/IV disease and present with extensive lymphadenopathy, blood and bone marrow involvement, and splenomegaly. 7 Eighty percent of the patients with the mantle zone variant have splenomegaly which may be massive. The MCL patients can present with pancytopenia or a leukemic presentation with extensive leukocytosis. 8 Some degree of peripheral blood involvement can be detected in most cases by flow cytometry. 9 Other extranodal sites include the gastrointestinal tract either in the stomach or colon, liver, or in Waldeyer s ring. 10 Some patients have sheets of lymphomatous polyps of the large bowel, lymphomatous polyposis, which sometimes leads to the diagnosis of MCL. 11 If random blind biopsies are done of normal appearing mucosa of the colon in patients who have been diagnosed with MCL in other locations, a large percentage are positive for MCL involvement. 11 Other extranodal sites for MCL involvement include the skin, lacrimal glands, and central nervous system DIAGNOSIS The diagnosis is made on a biopsy of a lymph node, tissue, bone marrow or blood phenotype which shows the typical morphology of mono-morphic small to medium sized lymphoid cells with irregular nuclear contours. 5 Four cytologic variants of MCL are recognized, including the Division of Hematology/Oncology, University of Nebraska Medical Center, Omaha, Nebraska small cell variant, mantle zone variant; diffuse variant, and the blastic variant. 12 Immunophenotyping is commonly used with the MCL cells being CD201, CD51, and positive for Cyclin D1 while being negative for CD10 and Bcl6. 5 The hallmark chromosomal translocation t (11:14) (q13; 32) identifies MCL, and can be shown in most cases. 13 This translocation leads to the aberrant expression of cyclin D1, which is not typically expressed in normal lymphocytes. A few cyclin D1 negative cases have been identified and appear to have an overexpression of cyclin D2 or D3 instead. 14 Overexpression of the transcription factor, SOX11, has been described as a diagnostic marker for MCL with the absence of SOX11 a characteristic of indolent MCL. 15 Biologic features such as a high Ki-67 proliferation index or p53 mutations and p16 deletions are closely related to the more aggressive MCL subtypes such as the blastoid variants. 16 Amodel of molecular pathogenesis and progression of MCL was originally proposed by Jares et al. 17 This molecular pathogenesis model has recently been updated with the additional information on mutational status and SOX11 status 18 (Figure 1). Staging procedures should include a complete blood count, chemistry profile, a lactic dehydrogenase (LDH), a bone marrow evaluation, with immunophenotyping by flow cytometry of the bone marrow and blood, and computed tomography of the chest, abdomen, and pelvis or FDG-PET/CT. The standard uptake values (SUV s) of sites involved with MCL often have low or intermediate values. 19 Evaluation of the
3 808 TABLE 2 Simplified MIPI index Points Age, years ECOG PS LDH/ULN LDH WBC, 109/L 0 < <0.67 < FIGURE 2 Overall survival for low, intermediate, and high risk MCL according to the MIPI classification (From Hoster et al. 22 ) gastrointestinal tract with endoscopy is warranted if there are clinical symptoms or if a dose intense regimen will be used. Evaluation of the cerebral spinal fluid is not usually done unless there are neurologic symptoms or if the patient has the blastoid variant or a high Ki The majority of patients have stage III or IV disease after complete staging is completed. 3 RISK STRATIFICATION The International Prognostic Index (IPI) was first developed for patients with diffuse large B-cell non-hodgkin lymphoma. 21 This was used for patients with MCL but was not very discriminatory, particularly for the lower risk patients. More recently the first prognostic index for MCL, the Mantle cell International Prognostic Index (MIPI), was formulated by the European MCL Network. 22 The independent prognostic factors for shorter overall survival (OS) from the MIPI were higher age, worse ECOG performance status, higher LDH, and a higher white blood cell count at diagnosis (Table 1). These were calculated as a continuous parameter and three groups emerged: MIPI low-risk with the median OS not reached (5-year OS 60%), MIPI intermediate risk with a median OS of 51 months, and a MIPI high risk group with a median OS of 29 months (Figure 2). 22 This index has now been validated by other groups. 23 A simplified modification of the MIPI has also been developed which has high concordance to the original MIPI, but slightly less discriminatory power 23 (Table 2). The addition of the Ki-67 proliferation index also provides some additional discriminatory power. 23 TABLE 1 The original MIPI score calculations [ age in (years)] 3 age (years) (if ECOG performance status > 1) log 10 (LDH/ULN LDH) log10(white blood cells per 106 L) For each prognostic factor, 0 3 points are given and the points are summed up to a maximum of 11. Patients with 0 3 points are low risk, patients with 4 5 points are intermediate risk, and patients with 6 11 points are high risk. These risk categories correspond to the categories of the original MIPI. 23 Gene expression profiling has been performed on a large series of MCL patients to evaluate a molecular predictor consisting of 20 proliferation associated genes. 14 However, a microarray-based technique is not feasible on a wide scale. Therefore, further testing of a minimum number of genes by formalin-fixed, paraffin-embedded tissue specimens has been studied. 24 This study identified five genes including RAN, MYC, TNFRSF10B, POLE2, and SLC29A2 which were validated by a quantitative reverse-transcriptase polymerase chain reaction (qrt- PCR) based test and predicted survival in 73 patients with MCL. Further validation of these genes and technique is needed before this is used outside a research context. 4 RISK-ADAPTED THERAPY MCL is responsive to a variety of initial therapies, but relatively shortterm remissions are achieved with conventional chemotherapy regimens. The median duration of remission in most previous trials was years and the median OS was 3 6 years with standard chemotherapy. However, there is a wide variation in outcomes with some patients having a very aggressive presentation and succumbing to their disease in a short period of time, while other patients at the opposite end of the spectrum have a very indolent clinical course. Due to the rarity of MCL, most trials have not been large randomized trials and much of the available information is based on smaller phase II trials with historical controls. 4.1 Initial management of asymptomatic low MIPI or elderly MCL patients Given the unfavorable prognosis and the fact that standard therapy does not appear to cure patients with MCL, a watch and wait strategy for patients with asymptomatic, low MIPI or elderly MCL patients should be considered. This strategy would be similar to that used for asymptomatic patients with follicular or other indolent lymphomas. In a study from Weill-Cornell Medical Center, 97 patients with MCL were evaluated. 25 Of the 97, 31 (32%) were observed at the time of initial evaluation. These MCL patients were 46% low- MIPI index as compared to 32% low-mipi in the patients who received initial treatment. The median time to treatment for the
4 809 observation group was 12 months (range months). 25 When this observational patient group needed treatment, the majority received cyclophosphamide, doxorubicin, oncovin, and prednisone (CHOP) like treatment (55%), with some patients receiving rituximab monotherapy (13%), and at the time of publication five patients had never received any therapy. 25 When the asymptomatic elderly MCL patient population does become symptomatic and requires therapy, a number of options are available for treatment. Probably the most commonly used regimen in the past has been an anthracycline-based therapy such as CHOP. 26 Rituximab monotherapy has some modest activity in MCL. 27 Over the last decade, rituximab has been added to the drugs in CHOP (R-CHOP) and tested in MCL. The first report of R-CHOP for the treatment of MCL was in 40 previously untreated patients and yielded an overall response rate (ORR) of 96%, including a complete response (CR) of 48%. 28 Despite 36% of the patients having a molecular CR, there was no difference in the median progression-free survival (PFS) between the patients who achieved a molecular CR (16.5 months) and those who did not (18.8 months). 28 There were similar results from a randomized study in the German lymphoma study group which compared front-line CHOP to R-CHOP. In this study, the addition of rituximab to CHOP improved the ORR (94% vs. 75%, P ) and the CR rate (34% vs. 7%, P ). 29 However, this did not translate into significant improvements in PFS or OS in this study. 29 Some clinical studies are testing agents used in relapsed MCL in combinations in the front-line setting such as R-CHOP 1 Bortezomib. 30 A large phase III trial of R-CHOP vs. bortezomib, rituximab, cyclophosphamide, doxorubicin, and prednisone (VR-CAP) demonstrated a 59% improvement in PFS (median 14.4 mo. vs mo.; P <.001) the median OS was 56.3% vs. not reached (hazard ratio 0.80). 30 This may be an option in patients who are not eligible for transplant and do not have pre-existing peripheral neuropathy. Purine analogues have also been used for the treatment of MCL in the older patient population. Single agent fludarabine demonstrated an ORR < 40%; however, when combined with cyclophosphamide and rituximab the response rate is closer to 60%. 31 More recently, a large randomized trial done in Germany demonstrated that R-CHOP was superior to R-FC in the older MCL patient population with a 4 year OS of 65% for R-CHOP and 50% for R-FC (P ). 32 In addition, a second randomization was done for maintenance either with rituximab or interferon. The arm that produced the best PFS and OS, was R-CHOP followed by rituximab maintenance (MR) with a 4-year OS of 87%. 32 This is the first large randomized trial which demonstrated a benefit for MR in PFS for patients with MCL. Another agent that has been tested in patients with MCL which demonstrated good activity is Bendamustine. A randomized trial done in Europe compared R-CHOP to R-Bendamustine in a number of different lymphomas. 33 In this trial, the patients with MCL had a similar ORR (89% for BR and 95% for R-CHOP). The BR regimen was associated with a lower progression rate 42% vs. 63% for the R-CHOP arm. 33 In addition, the hematologic toxicity and alopecia were less in the R-Bendamustine arm. 33 A second study evaluating R-CHOP vs. R- Bendamustine did not demonstrate a superior outcome for the R- Bendamustine, but did demonstrate an equivalent outcome. 34 MR therapy has been demonstrated to prolong the PFS in patients following induction chemotherapy. A meta-analysis of 3 large randomized clinical trials of 434 adults with MCL demonstrated an improvement in PFS with MR (HR 0.60, 95% CI: ) and a decrease in mortality rate with MR (HR 0.67, 95% CI 0.46 to 0.98). There was no statistically significant difference in infection rates with or without MR (RR 0.80, 95% CI: ). 35 Recommendations: Asymptomatic elderly or low-mipi patients can be observed without any therapy. When the patients become symptomatic, first line therapy choices include R-Bendamustine, RCHOP(1/- rituximab maintenance), or a clinical trial. 4.2 Initial management of a young symptomatic patient Several studies have suggested that aggressive therapies in younger patients with MCL may improve the outcomes. One of the first studies to evaluate this was the European MCL Network study where responding patients under age 65 years were randomized after induction therapy to receive either myeloablative radio-chemotherapy followed by autologous stem cell transplantation (ASCT) or maintenance interferon. 36 In this study, the patients in the ASCT arm had an improved PFS over those in the interferon arm. 36 Several other single arm and retrospective studies have suggested patients receiving an induction regimen that contains high-dose cytarabine, such as hyperfractioned cyclophosphamide, vincristine, doxorubicin, and dexamethasone alternating with high-dose cytarabine and methotrexate (Hyper- CVAD 6 rituximab) experience improved survival. 37 The addition to rituximab to 6 8 cycles of HyperCVAD alternating with high dose cytarabine and methotrexate yielded a CR rate of 87% and had a 7-year failure-free survival rate of 52% and OS of 68%. 37 This regimen was tested in a multicenter trial and was found to have a similar ORR of 88% and CR rate of 58%; however, there was grade IV hematologic toxicity in 87% of the patients making this regimen difficult to give in some community settings. 38 It was also suggested in a retrospective study that patients receiving R-HyperCVAD as an induction with auto ASCT in CR1 had an improved outcome as compared to R-CHOP. 39 However a further analysis of a separate cohort of MCL patients demonstrated that when corrected for the MIPI, the outcomes may be similar. 40 Since the R-HyperCVAD alternating with methotrexate/cytarabine is difficult to administer, modifications which drop the methotrexate portion 41 or drop both the methotrexate and cytarabine have been tested. 42 In the study from Geisler et al., younger MCL patients received rituximab 1 maxi-chop, alternating with rituximab 1 cytarabine. Responders received high-dose chemotherapy with ASCT. The 6- year PFS was 66% and the OS was 70%. Compared to a historical control without the cytarabine, the results were much improved with the regimen as outlined. 41 In a small pilot trial in an older population, the
5 810 rituximab Hyper CVAD regimen without the methotrexate or cytarabine, but with maintenance rituximab demonstrated an ORR of 77% and a median PFS of 37 months. 42 Another approach has been for patients to receive R-CHOP 3 three cycles, then Rituximab, cisplatin, cytarabine, dexamethasone (R-DHAP) 3 3, followed by high dose chemotherapy and ASCT. 43 This study also demonstrated an excellent 5-year OS of 75%. 43 The role of ASCT in CR1 has not been tested in a randomized trial. However in a retrospective analysis of 167 MCL patients under age 65, the patients received either R-HyperCVAD or R-CHOP followed by an auto ASCT in CR1 had an improved PFS compared to R-CHOP alone (P <.004), even when corrected for prognostic factors. 44 The best induction regimen before transplant has not been defined, but the ability to attain a CR may be the most important characteristic. The use of post-transplant maintenance rituximab has recently been demonstrated to prolong the 4-year PFS and OS. 45 Recommendations: For young symptomatic patients with MCL, considerations include R-HyperCVAD with high-dose cytarabine (6Methotrexate) or a modified regimen such as the Nordic regimen, followed by ASCT in CR1 for selected patients. For patients who are not candidates for standard R-HyperCVADwithhighdosecytarabine/methotrexate,possiblealternatives include R-CHOP, R- CHOP alternating with R-DHAP, or R-Bendamustine. If possible, ASCT in CR1 should still be considered for these patients as well as post-transplant maintenance rituximab. 4.3 Management of relapse/refractory MCL For patients with relapsed but asymptomatic MCL, further watch and wait may be possible as there are a percentage of patients with indolent MCL who may not need therapy for months or years. Once the patient becomes symptomatic many options are considerations. The Bendamustine rituximab (BR) regimen has also been tested in relapsed MCL patients. A phase II study of BR in 63 patients with relapsed/ refractory MCL demonstrated an ORR or 90% with a CR of 60% and a median PFS of 30 months. 46 The addition of cytarabine to the BR regimen (R-BAC) demonstrated a high ORR of 80% and a CR rate of 70% in relapsed/refractory MCL patients. However, there was significant cytopenias with this regimen. 47 Since many standard lymphoma salvage regimens have limited activity in MCL, novel treatment approaches based on targeting known signaling pathways have been tested. The first such agent to be tested as a proteasome inhibitor, bortezomib. As a monotherapy, bortezomib has demonstrated ORRs in the 30 40% range. 48 In a large phase II study of 141 evaluable MCL patients treated with bortezomib, there was an ORR of 33% with a CR rate of 8%. 49 With further follow up, the phase II study of bortezomib demonstrated a median time to progression of 6.7 months and a median OS of 23.5 months. 50 Bortezomib has also been combined with other agents such as Bendamustine and rituximab in the BVR regimen which also had excellent activity. In patients with MCL the ORR rate for the BVR regimen was 71%. 51 The PI3Kinase/Akt/mTOR pathway is implicated in the pathogene-sis of MCL. 52 Based upon this information the mtor inhibitor, temsirolimus was tested in a phase II study of patients with relapsed/refractory MCL. In this study, temsirolimus demonstrated moderate activity with an ORR of 44%. 53 In a phase III study of 162 relapsed/refractory patients with MCL, high doses of temsirolimus (175 mg/75 mg) resulted in an ORR of 22% and a PFS of 4.8 months. 54 Other mtor inhibitors, such as everolimus, have also demonstrated activity in MCL. 55 The immunomodulatory agent lenalidomide has also shown promising activity against MCL. In a phase II study, Zinzani et al. 56 reported an ORR of 41% in 39 MCL patients treated with lenalidomide. The larger EMERGE trial tested single agent lenalidomide in 134 patients with relapsed MCL. The ORR was 28% with a 7.5% CR rate. 57 There studies led to the FDA approval of lenalidomide for patients with relapsed MCL who had failed bortezomib. Lenalidomide has also been combined with rituximab with promising results. In a study by Wang et al., patients with recurrent MCL were treated with lenalidamide and rituximab for recurrent disease. In this study, the ORR was 58% and the CR rate was 33% with the combination being well tolerated. Recently, brutons tyrosine kinase (BTK) inhibitor (Ibruitinib) was FDA approved for patients with relapsed MCL. In a study of 111 MCL patients, the BTK inhibitor was reported to have a 68% ORR and a CR rate of 21%, with no differences between bortezomib naeıve and patients who had relapsed after receiving bortezomib. 59 PI3Kinase inhibitor (GS-1101, Idelalisib) which targets the B-cell receptor pathways has demonstrated a 48% ORR in a study of 38 relapsed MCL patients. 60 There is not much data available for standard involved field irradiation in MCL. However, there is data with the use of radioimmunotherapy (RIT) with Yttrium 90 Ibritumomab Tiuxetan in patients with relapsed MCL demonstrating an ORR of 31%. 61 When RIT is used to consolidate after immunochemotherapy, it resulted in improvement of the percentages of responses compared with historical controls. 62 The use of high-dose chemotherapy and ASCT for patients with relapsed MCL has not demonstrated as promising results as with frontline use. However, an analysis of the CIBMTR data demonstrated in 159 MCL patients receiving an autologous transplant for relapsed disease, the 5-year OS was 44% and for 99 patients receiving an allogeneic transplant for MCL, the 5-year OS was 32%. 63 In appropriate patients with relapsed MCL who had a long initial remission and have been successfully salvaged, ASCT in CR2 maybe a consideration. Allogeneic stem cell transplantation is felt to be the only potentially curative treatment for advanced MCL. A number of small studies using various reduced intensity preparative regimens with an allogeneic source of stem cell have been reported. 64,65 In a study by Tam et al., patients with relapsed MCL receiving a reduced intensity regimen with an allogeneic stem cell transplant. With a median follow up of 56 months, the 6-year PFS was 46% and the 6-year actuarial OS was 53%. 64 Although the relapse rates are less with allogeneic transplantation, the risks of graft-versus host disease and infectious complications are much higher resulting in similar short term but apparently improved long term results compared to ASCT for relapsed MCL.
6 811 Recommendations: My first choice for a relapsed MCL patient would be ibrutinib. bendamustine/rituximab is an option in patients who have not previously received bendamustine. Other options would include rituximab alone, a bortezomib containing regimen, lenalidamide, or a clinical trial. If the patient is a candidate for stem cell transplantation, consideration for an autologous transplant if there was a long first remission or a reduced intensity allogeneic stem cell transplant should be given. CONFLICT OF INTEREST Nothing to report. REFERENCES [1] Gerard-Marchant R, Hamlin, I, Lennert K, et al. Classification of non-hodgkin s lymphomas [let-ter]. Lancet. 1974;2: [2] Berard CW, Dorfman RF. Histopathology of malignant lymphomas. Clin Haematol. 1974;3: [3] Weisenburger DD, Kim H, Rappaport H. Mantle-zone lymphoma. A follicular variant of intermediate lymphocytic lymphoma. Cancer. 1982;49: [4] Harris NL, Jaffe, ES, Stein H, et al. A revised European-American classification of lymphoid neoplasms: A proposal from the International Lymphoma Study Group. Blood. 1994;84: [5] Swerdlow SH, Campo, E, Harris N, et al. WHO Classification of tumors of the haematopietic and lymphoid tissues. Lyon, France: IARC; [6] Non-Hodgkin s Lymphoma Classification Project. A clinical evaluation of the International Lymphoma Study Group. Blood. 1997;89: [7] Tiemann M, Schrader, C, Klapper W, et al. Histopathology, cell proliferation indices and clinical outcome in 304 patients with mantle cell lymphoma (MCL): A clinicopathological study from the European MCL Network. Br J Haematol. 2005;131: [8] Ferrer A, Salaverria, I, Bosch F, et al. Leukemic involvement is a common feature in mantle cell lymphoma. Cancer. 2007;109: [9] Ghielmini M, Zucca E. How I treat mantle cell lymphoma. Blood. 2009;114: [10] Samaha H, Dumontet, C, Ketterer N, et al. Mantle cell lymphoma: A retrospective study of 121 cases. Leukemia. 1998;34: [11] Romaguera JE, Medeiros, LJ, Hagemeister FB, et al. Frequency of gastrointestinal involvement and its clinical significance in mantle cell lym-phoma. Cancer. 2003;97: [12] Bertoni R, Ponzoni M. The cellular origin of mantle cell lymphoma. Int J Biochem Cell Biol. 2007;39: [13] Bertoni F, Rinaldi A, Zucca E, Cavalli F. Update on the molecular biology of mantle cell lymphoma. Hematol Oncol. 2006;24: [14] Rosenwald A, Wright, G, Wiestner A, et al. The proliferation gene expression signature is a quantitative integrator of oncogenic events that predicts survival in mantle cell lymphoma. Cancer Cell. 2003;3: [15] Fernandez V, Salamero, O, Espinet B, et al. Genomic and gene expression profiling defines indolent forms of mantle cell lymphoma. Cancer Res. 2010;70: [16] Bernard M, Gressin, R, Lefrere F, et al. Blastic variant of mantle cell lymphoma: A rare but highly aggressive subtype. Leukemia. 2001; 15: [17] Jares P, Colomer D, Campo E. Genetic and molecular pathogenesis of mantle cell lymphoma: Perspectives for new targeted therapeutics. Nat Rev Cancer. 2007;7: [18] Jares P, Colomer, D, Campo E, et al. Molecular pathogenesis of mantle cell lymphoma. J Clin Invest. 2012;122: [19] Gill S, Wolf, M, Prince HM, et al. [18F] fluorodeoxyglucose positron emission tomography scanning for staging, response assessment, and disease surveillance in patients with mantle cell lymphoma. Clin Lymph Myeloma. 2008;8: [20] Ferrer A, Bosch, F, Villamor N, et al. Central nervous system involvement in mantle cell lymphoma. Ann Oncol. 2008;19: [21] International Non-Hodgkin s Lymphoma Prognostic Factors Project. A predictive model for aggressive non-hodgkin s lymphoma. N Engl J Med. 1993;329: [22] Hoster E, Dreyling, M, Klapper W, et al. A new prognostic index (MIPI) for patients with advanced mantle cell lymphoma. Blood. 2008;111: [23] Geisler CH, Kolstad, A, Laurell A, et al. The mantle cell lymphoma International Prognostic Index (MIPI) is superior to the International Prognostic Index (IPI) in predicting survival following intensive first line immunochemotherapy and autologous stem cell transplantation (ASCT). Blood. 2010;115: [24] Hartmann E, Fernandez, V, Moreno V, et al. Five-gene model to predict survival in mantle-cell lymphoma using frozen or formalinfixed, paraffin-embedded tissue. J Clin Oncol. 2008;26: [25] Martin P, Chadburn, A, Christos P, et al. Out-come of deferred initial therapy in mantle-cell lymphoma. J Clin Oncol. 2009;27: [26] Weisenburger DD, Vose, JM, Greiner TC, et al. Mantle cell lymphoma: A clinicopathologic study of 68 cases from the Nebraska Lymphoma Study Group. Am J Hematol. 2000;64: [27] Foran JM, Rohatiner, AZ, Cunningham D, et al. European phase II study of rituximab (chimeric anti-cd20 monoclonal antibody) for patients with newly diagnosed mantle-cell lymphoma and previously treated mantle-cell lymphoma, immunocytoma, and small B-cell lymphocytic lymphoma. J Clin Oncol. 2000;18: [28] Howard OM, Gribben, JG, Neuberg DS, et al. Rituximab and CHOP induction therapy for newly diagnosed mantle-cell lymphoma: Molec-ular complete responses are not predictive of progressionfree survival. J Clin Oncol. 2002;20: [29] Lenz G, Dreyling, M, Hoster E, et al. Immuno-chemotherapy with rituximab and cyclophos-phamide, doxorubicin, vincristine, and prednisone significantly improves response and time to treatment failure, but not long term out-come in patients with previously untreated man-tle cell lymphoma: Results of a prospective randomized trial of the German Low Grade Lymphoma Study Group (GLSG). J Clin Oncol. 2005;23: [30] Robak T, Huang H, Jin J, et al. Bortezomib-based therapy for newly diagnosed mantle-cell lymphoma. N Engl J Med. 2015;372: [31] Cohen BJ, Moskowitz, C, Straus D, et al. Cyclophsphamide/fludarabine (CF) is active in the treatment of mantle cell lymphoma. Leuk Lymphoma. 2001;42: [32] Kluin-Nelemans JC, Hoster, E, Hermine O, et al. Treatment of older patients with mantle cell lymphoma. N Engl J Med. 2012;376: [33] Rummel M, Niederle, N, Maschmeyer G, et al. Bendamustine plus rituximab versus CHOP plus rituximab as first-line treatment for patients with indolent and mantle-cell lymphomas: An open-label, muticentre, randomised, phase 3 non-inferiority trial. Lancet. 2013; 381:
7 812 [34] Flinn IW, Van der Jagt RH, Kahl BS, et al. An open-level, randomized study of bendamustine and rituximab (BR) compared with rituximab, cyclophosphamide, vincristine, and prednisone (R-CVP) or rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP) in first-line treatment of patients with advanced indolent non-hodgkin s lymphoma (NHL) or mantle cell lymphoma (MCL): The Bright Study. Blood. 2014;123: [35] Vidal L, Gafter-Gvili A, Dreyling M, et al. Rituximab maintenance (MR) for patients with mantel cell lymphoma (MCL) A systemic review and meta-analysis of the randomized controlled trials (RCTs). Blood. 2016;128:1802. [36] Dreyling M, Lenz, G, Hoster E, et al. Early con-solidation by myeloablative radiochemotherapy followed by autologous stem cell transplantation in first remission significantly prolongs progression-free survival in mantle cell lymphoma: Results of a prospective randomized trial of the European MCL Network. Blood. 2005;105: [37] Romaguera JE, Fayad, L, Rodriguez MA, et al. High rate of durable remission after treatment of newly diagnosed aggressive mantle-cell lymphoma with rituximab plus HyperCVAD Alternating with Rituximab plus high-dose methotrexate and cytarabine. J Clin Oncol. 2005;23: [38] Bernstein SH, Epner E, Unger JM, et al. A phase II multicenter trial of HyperCVAD MTX/Ara-C and rituximab in patients with previously untreated mantle cell lymphoma: SWOG Ann Oncol. 2013;24: [39] Vose J, Loberiza, F, Bierman P, et al. Mantle cell lymphoma (MCL): Induction therapy with HyperCVAD/high dose methotrexate and cytarabine (MC) 6 rituximab improves results of autologous stem cell transplant in first remission. J Clin Oncol. 2006;24:424a. [40] Budde LE, Guthrie, KA, Till GB, et al. Mantel cell lymphoma International Prognostic Index but not pretransplantation induction regimen predicts survival for patients with mantle-cell lymphoma receiving high-dose therapy and autologous stem cell transplantation. J Clin Oncol. 2011;29: [41] Giesler CH, Kolstad, A, Lurell A, et al. Long-term progression-free survival of mantle cell lymphoma after intensive front-line immunochemotherapy with in vivo-purged stem cell rescue: A nonrandomized phase 2 multicenter study by the Nordic Lymphoma Group. Blood. 2008;112: [42] Kahl BS, Longo, WL, Eickhoff JC, et al. Maintenance rituximab following induction chemoimmunotherapy may prolong progressionfree survival in mantle cell lymphoma: A pilot study from the Wisconsin Oncology Network. Ann Oncol. 2006;17: [43] Delarue R, Haioun, C, Ribrag V, et al. CHOP and DHAP plus rituximab followed by autologous stem cell transplantation in mantle cell lymphoma: A phase 2 study from the Groupe d Etude des Lymphomes de l Adulte. Blood. 2013;121: [44] Le Gouill S, thieblemont C, Oberic L, et al: Rituximab maintenance after autologous stem cell transplantation prolongs survival in younger patients with mantel cell lymphoma: final results of the randomized phase 3 LyMa Trial of the Lysa/Goelams Group. Blood. 2016;128:145. [45] LeCase AS, Vandergrift, JL, Rodriguez MA, et al. Comparative outcome of initial therapy for younger patients with mantle cell lymphoma: An analysis form the NCCN NHL Database. Blood. 2012; 119: [46] Rummel M, Atta J, Welslau M. Bendamustine and rituximab (BR) are effective and has a favorable toxicity profile in the treatment of mantle cell and low-grade non-hodgkin s lymphoma. J Clin Oncol. 2005;23: [47] Visco C, Finotto, S, Pomponi F, et al. Combination of rituximab, bendamustine, and cytarabine for patients with mantle cell non- Hodgkin lymphoma ineliglible for intensive regimens or autologous transplantation. J Clin Oncol. 2013;31: [48] O Connor OA, Wright, J, Moskowitz C, et al. Phase II clinical experience with the novel proteasome inhibitor bortezomib in patients with indolent non-hodgkin s lymphoma and mantle cell lymphoma. J Clin Oncol. 2005;23: [49] Fisher RI, Bernstein SH, Kahl BS, et al. Multicenter phase II study of bortezomib in pateints with relapsed or refractory mantle cell lymphoma. J Clin Oncol. 2006;24: [50] Goy A, Bernstein, SH, Kahl BS, et al. Bortezomib in patients with relapsed or refractory mantle cell lymphoma: Updated time-toevent analyses of the multicenter phase 2 PINNACLE study. Ann Oncol. 2009;20: [51] Friedberg JW, Vose, JM, Kelly JL, et al. The combination of bendamustine, bortezomib, and rituximab for patients with relapsed/ refractory indolent and mantle cell lymphoma. Blood. 2011;117: [52] Perez-Galan P, Dreyling M, Wiestner A. Mantle cell lymphoma: Biology, pathogenesis, and the molecular basis of treatment in the genomic era. Blood. 2011;117: [53] Ansell SM, Inwards, DJ, Rowland KM, et al. low-dose single-agent temsirolimus for relapsed mantle cell lymphoma: A phase 2 trial in the North Central Cancer Treatment Group. Cancer. 2008;113: [54] Hess G, Herbrecht, R, Romaguera J, et al. Phase III study to evaluate temsirolimus compared with investigator s choice therapy for the treatment of relapsed or refractory mantle cell lymphoma. J Clin Oncol. 2009;27: [55] Witzig TE, Reeder, CB, LaPlant BR, et al. A phase II trial of the oral mtor inhibitor everoliumus in relapsed aggressive lymphoma. Leukemia. 2011;25: [56] Zinzani PL, Witzig TE, Vose J, et al. Confirmation of the efficacy and safety of lenalidomide oral monotherapy in patients with relapsed or refractory mantle cell lymphoma: Results of an international study (NHL-003). Blood. 2008;112: [57] Goy A, Sinha R, Williams ME, et al. Singleagent lenalidomide in patients with mangle-cellymphoma who relapsed or progressed after or were refractory to bortezomib: Phase IIMCL-001 (EMERGE) Study. J Clin Oncol. 2013;49:2835. [58] Wang M, Fayad, L, Wagner-Bartak N, et al. Lenalidamide in combination with rituximab for patients with relapsed or refractory mantle-cell lymphoma: A phase 1/2 clinical trial. Lancet Oncol. 2012;13: [59] Wang L, Rule, S, Martin P, et al. Targeting BTK with Ibruitinib in relapsed or refractory mantle cell lymphoma. N Engl J Med. 2014; 369: [60] Kahl B, Spurgeon, S, Furman RI, et al. Significant clinical activity of CAL-101, an isoform selective inhibitor of phosphatidylinositol 3 kinase P110D, in patients with relapsed or refractory indolent and mantle cell lymphoma. Blood. 2014;123: [61] Wang M, Oki Y, Pro B, et al. Phase II study of Yttrium-90 Ibritumomab tiuxetan in patients with relapsed or refractory mantle cell lymphoma. J Clin Oncol. 2009;27: [62] Smith MR, Linjun, A, Gordon LI, et al. Phase II study of rituximab plus cyclophosphamide, doxorubicin, vincristine, and prednisone immunochemotherapy followed by 90Y-Ibritumomab tiuxetan in untreated mantle cell lymphoma: Eastern Cooperative Oncology Group Study E1499. J Clin Oncol. 2012;30:
8 813 [63] Fenske TS, Carreras, J, Zhang M, et al. Outcome of patients with mantle cell lymphoma undergoing autologous versus reducedintensity allogeneic transplantation. JClinOncol.2013;49: [64] Tam CS, Bassett, R, Ledesma C, et al. Mature results of the M. D. Anderson Cancer Center risk-adapted transplantation strategy in mantle cell lymphoma. Blood 2009;113: [65] Maris MB, Sandmaier, M, Storer FE, et al. Allogeneic hematopoietic cell transplantation after fludarabine and 2 Gy total body irradiation for relapsed and refractory mantle cell lymphoma. Blood. 2004;104: How to cite this article: Vose JM. Mantle cell lymphoma: 2017 update on diagnosis, risk-stratification, and clinical management. Am J Hematol. 2017;92:
Mantle Cell Lymphoma Understanding Your Treatment Options
 New Developments in Mantle Cell Lymphoma John P. Leonard, M.D. Richard T. Silver Distinguished Professor of Hematology and Medical Oncology Associate Dean for Clinical Research Vice Chairman, Department
New Developments in Mantle Cell Lymphoma John P. Leonard, M.D. Richard T. Silver Distinguished Professor of Hematology and Medical Oncology Associate Dean for Clinical Research Vice Chairman, Department
New Targets and Treatments for Follicular Lymphoma. Disclosures
 Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Disclosures Consulting fees from:
Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Disclosures Consulting fees from:
Lauren Berger: Why is it so important for patients to get an accurate diagnosis of their blood cancer subtype?
 Hello, I m Lauren Berger and I m the Senior Director of Patient Services Programs at The Leukemia & Lymphoma Society. I m pleased to welcome Dr. Rebecca Elstrom. Dr. Elstrom is an Assistant Professor in
Hello, I m Lauren Berger and I m the Senior Director of Patient Services Programs at The Leukemia & Lymphoma Society. I m pleased to welcome Dr. Rebecca Elstrom. Dr. Elstrom is an Assistant Professor in
Prior Authorization Guideline
 Prior Authorization Guideline Guideline: PS Inj - Velcade Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antineoplastic Client: PS Inj Approval Date: 10/2/2004 Revision Date: 5/22/2007
Prior Authorization Guideline Guideline: PS Inj - Velcade Therapeutic Class: Antineoplastic Agents Therapeutic Sub-Class: Antineoplastic Client: PS Inj Approval Date: 10/2/2004 Revision Date: 5/22/2007
Therapeutic Options in Refractory or Relapsed CD20-positive Follicular Lymphoma
 a report by Martin Dreyling Therapeutic Options in Refractory or Relapsed CD20-positive Follicular Lymphoma Head, Lymphoma Section, Department of Medicine III, University Hospital Großhadern, Ludwig Maximilians-University
a report by Martin Dreyling Therapeutic Options in Refractory or Relapsed CD20-positive Follicular Lymphoma Head, Lymphoma Section, Department of Medicine III, University Hospital Großhadern, Ludwig Maximilians-University
Audience Response Question?
 Presenter Disclosure Information Session 4: 3:30 PM - 4:15 PM Non-Hodgkin s Lymphomas: Optimizing Therapeutic Choices for Initial Management Speaker: Arnold S. Freedman, MD The following relationships
Presenter Disclosure Information Session 4: 3:30 PM - 4:15 PM Non-Hodgkin s Lymphomas: Optimizing Therapeutic Choices for Initial Management Speaker: Arnold S. Freedman, MD The following relationships
亞 東 紀 念 醫 院 Follicular Lymphoma 臨 床 指 引
 前 言 : 惡 性 淋 巴 瘤 ( 或 簡 稱 淋 巴 癌 ) 乃 由 體 內 淋 巴 系 統 包 括 淋 巴 細 胞 淋 巴 管 淋 巴 腺 及 一 些 淋 巴 器 官 或 組 織 如 脾 臟 胸 腺 及 扁 桃 腺 等 所 長 出 的 惡 性 腫 瘤 依 腫 瘤 病 理 組 織 型 態 的 不 同 可 分 為 何 杰 金 氏 淋 巴 瘤 (Hodgkin s disease) 與 非 何 杰 金
前 言 : 惡 性 淋 巴 瘤 ( 或 簡 稱 淋 巴 癌 ) 乃 由 體 內 淋 巴 系 統 包 括 淋 巴 細 胞 淋 巴 管 淋 巴 腺 及 一 些 淋 巴 器 官 或 組 織 如 脾 臟 胸 腺 及 扁 桃 腺 等 所 長 出 的 惡 性 腫 瘤 依 腫 瘤 病 理 組 織 型 態 的 不 同 可 分 為 何 杰 金 氏 淋 巴 瘤 (Hodgkin s disease) 與 非 何 杰 金
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY
 CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
CHAPTER 26 LATE BREAKING DEVELOPMENTS: IMPACT OF ANTI-CD20 MONOCLONAL ANTIBODIES ON LYMPHOMA THERAPY 26.1 Introduction rituximab Subsequent to the completion of drafts for the guidelines earlier in 2004,
Guidelines for the Management of Follicular Lymphoma
 Guidelines for the Management of Follicular Lymphoma Scope The following guidance for first- and second-line therapy applies to follicular lymphoma histological grades 1, 2 and 3a according to the World
Guidelines for the Management of Follicular Lymphoma Scope The following guidance for first- and second-line therapy applies to follicular lymphoma histological grades 1, 2 and 3a according to the World
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Lenalidomide (LEN) in Patients with Transformed Lymphoma: Results From a Large International Phase II Study (NHL-003)
 Lenalidomide (LEN) in Patients with Transformed Lymphoma: Results From a Large International Phase II Study (NHL-003) Reeder CB et al. Proc ASCO 2010;Abstract 8037. Introduction > Patients (pts) with low-grade
Lenalidomide (LEN) in Patients with Transformed Lymphoma: Results From a Large International Phase II Study (NHL-003) Reeder CB et al. Proc ASCO 2010;Abstract 8037. Introduction > Patients (pts) with low-grade
Outline of thesis and future perspectives.
 Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
Outline of thesis and future perspectives. This thesis is divided into two different sections. The B- section involves reviews and studies on B- cell non- Hodgkin lymphoma [NHL] and radioimmunotherapy
Audience Response Question? Non-Hodgkin s Lymphomas: Optimizing Therapeutic Choices for Initial Management. Presenter Disclosure Information
 Welcome to Master Class for Oncologists Session 4: 10:00 AM - 10:45 AM Miami, FL December 18, 2009 Non-Hodgkin s Lymphomas: Optimizing Therapeutic Choices for Initial Management Speaker: Arnold S. Freedman,
Welcome to Master Class for Oncologists Session 4: 10:00 AM - 10:45 AM Miami, FL December 18, 2009 Non-Hodgkin s Lymphomas: Optimizing Therapeutic Choices for Initial Management Speaker: Arnold S. Freedman,
Frequency of NHL Subtypes in Adults
 Chemotherapy Options Stephanie A. Gregory, M.D. The Elodia Kehm Professor of Medicine Director, Section of Hematology Rush University Medical Center Chicago, Illinois Frequency of NHL Subtypes in Adults
Chemotherapy Options Stephanie A. Gregory, M.D. The Elodia Kehm Professor of Medicine Director, Section of Hematology Rush University Medical Center Chicago, Illinois Frequency of NHL Subtypes in Adults
Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics
 Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics Disclosure(s) I do not intend to discuss an off-label use
Are CAR T-Cells the Solution for Chemotherapy Refractory Diffuse Large B-Cell Lymphoma? Umar Farooq, MD University of Iowa Hospitals and Clinics Disclosure(s) I do not intend to discuss an off-label use
EVIDENCE IN BRIEF OVERALL CLINICAL BENEFIT
 perc also deliberated on the alignment of bendamustine with patient values. perc noted that bendamustine has a progression-free survival advantage, may be less toxic than currently available therapies
perc also deliberated on the alignment of bendamustine with patient values. perc noted that bendamustine has a progression-free survival advantage, may be less toxic than currently available therapies
What is non-hodgkin lymphoma, how is it treated, and what is the unmet need?
 What is non-hodgkin lymphoma, how is it treated, and what is the unmet need? Tim Illidge BSc PhD MRCP FRCR FRCPath Institute of Cancer Sciences, University of Manchester Manchester Cancer Research Centre,
What is non-hodgkin lymphoma, how is it treated, and what is the unmet need? Tim Illidge BSc PhD MRCP FRCR FRCPath Institute of Cancer Sciences, University of Manchester Manchester Cancer Research Centre,
Hodgkin Lymphoma Disease Specific Biology and Treatment Options. John Kuruvilla
 Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA
 2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
Update on Follicular Lymphoma. Brad Kahl, M.D.
 Update on Follicular Lymphoma Brad Kahl, M.D. Follicular Lymphoma: 25% of NHL Cases Other subtypes (9%) T and NK cell (12%) Burkitt (2.5%) Diffuse large B cell (DLBCL) (30%) Mantle cell (6%) Follicular
Update on Follicular Lymphoma Brad Kahl, M.D. Follicular Lymphoma: 25% of NHL Cases Other subtypes (9%) T and NK cell (12%) Burkitt (2.5%) Diffuse large B cell (DLBCL) (30%) Mantle cell (6%) Follicular
Bendamustine with rituximab for the first-line treatment of advanced indolent non-hodgkin's and mantle cell lymphoma
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine with rituximab for the first-line treatment of advanced indolent non-hodgkin's and mantle cell lymphoma Bendamustine with rituximab for the first-line
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine with rituximab for the first-line treatment of advanced indolent non-hodgkin's and mantle cell lymphoma Bendamustine with rituximab for the first-line
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
An overview of CLL care and treatment. Dr Dean Smith Haematology Consultant City Hospital Nottingham
 An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
Michael Crump MD. Lymphoma Site Leader Princess Margaret Hospital University of Toronto
 Evolution of Lymphoma Therapy: What can we expect for the rest of the millenium decade? Michael Crump MD Lymphoma Site Leader Princess Margaret Hospital University of Toronto disclaimers Served on advisory
Evolution of Lymphoma Therapy: What can we expect for the rest of the millenium decade? Michael Crump MD Lymphoma Site Leader Princess Margaret Hospital University of Toronto disclaimers Served on advisory
Histopathologic results
 Self evaluation 1 Clinical Case 55-year-old woman Bilateral enlargement of cervical, axillary and inguinal lymph nodes, largest diameter > 6 cm Hepatosplenomegaly. Enlargement of retroperitoneal, mesenteric
Self evaluation 1 Clinical Case 55-year-old woman Bilateral enlargement of cervical, axillary and inguinal lymph nodes, largest diameter > 6 cm Hepatosplenomegaly. Enlargement of retroperitoneal, mesenteric
6/3/2013. Follicular and Other Slow Growing Lymphomas. Stephen Ansell, MD, PhD Mayo Clinic
 Follicular and Other Slow Growing Lymphomas Stephen Ansell, MD, PhD Mayo Clinic 1 Learning Objectives Start with an overview of Follicular and other slow growing lymphomas Discuss current and emerging
Follicular and Other Slow Growing Lymphomas Stephen Ansell, MD, PhD Mayo Clinic 1 Learning Objectives Start with an overview of Follicular and other slow growing lymphomas Discuss current and emerging
Follicular Lymphoma. Aruna K. Reddy, MD. Hematology& Oncology Peace Health Southwest Medical Center
 Follicular Lymphoma Aruna K. Reddy, MD Hematology& Oncology Peace Health Southwest Medical Center Follicular Lymphoma Malignant neoplasm resulting from clonal proliferation of malignant B-cells Second
Follicular Lymphoma Aruna K. Reddy, MD Hematology& Oncology Peace Health Southwest Medical Center Follicular Lymphoma Malignant neoplasm resulting from clonal proliferation of malignant B-cells Second
Perspectives on Recent Non-Hodgkin s Lymphoma (NHL) Data
 Perspectives on Recent Non-Hodgkin s Lymphoma (NHL) Data Summary Article James O. Armitage, MD Presented through a strategic collaboration by A series of 5 expert interviews were conducted, focusing on
Perspectives on Recent Non-Hodgkin s Lymphoma (NHL) Data Summary Article James O. Armitage, MD Presented through a strategic collaboration by A series of 5 expert interviews were conducted, focusing on
EU Media Inquiries: Satu Kaarina Glawe Phone: +49 (0) 2638 947 9218 Mobile: +49 (172) 294 6264 Email: sglawe@its.jnj.com
 EU Media Inquiries: Satu Kaarina Glawe Phone: +49 (0) 2638 947 9218 Mobile: +49 (172) 294 6264 Email: sglawe@its.jnj.com Investor Relations: Stan Panasewicz Phone: +1 732-524-2524 Louise Mehrotra Phone:
EU Media Inquiries: Satu Kaarina Glawe Phone: +49 (0) 2638 947 9218 Mobile: +49 (172) 294 6264 Email: sglawe@its.jnj.com Investor Relations: Stan Panasewicz Phone: +1 732-524-2524 Louise Mehrotra Phone:
GLSG/OSHO Study Group. Supported by Deutsche Krebshilfe
 GLSG/OSHO Study Group Supported by Deutsche Krebshilfe GLSG/OSHO Study Group Study Concepts Follicular Lymphomas Mantel Cell Lymphomas Waldenstroem s Disease Key Steps in Improving Treatment for Follicular
GLSG/OSHO Study Group Supported by Deutsche Krebshilfe GLSG/OSHO Study Group Study Concepts Follicular Lymphomas Mantel Cell Lymphomas Waldenstroem s Disease Key Steps in Improving Treatment for Follicular
MALIGNANT LYMPHOMAS. Dr. Olga Vujovic (Updated August 2010)
 MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
Lymphoma Diagnosis and Classification
 Lymphoma Diagnosis and Classification By Atef Shrit, MD, Pathology B- and T/NK-cell lymphomas are clonal neoplasms of immature and mature B-lymphocytes, T-lymphocytes or natural killer cells at various
Lymphoma Diagnosis and Classification By Atef Shrit, MD, Pathology B- and T/NK-cell lymphomas are clonal neoplasms of immature and mature B-lymphocytes, T-lymphocytes or natural killer cells at various
IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN
 + IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN Rena Buckstein MD FRCPC Head Hematology Site Group Sunnybrook Odette Cancer Center (OCC) Head of Hematology Clinical Trials Group at OCC + Outline Start
+ IF AT FIRST YOU DON T SUCCEED: TRIAL, TRIAL AGAIN Rena Buckstein MD FRCPC Head Hematology Site Group Sunnybrook Odette Cancer Center (OCC) Head of Hematology Clinical Trials Group at OCC + Outline Start
FDA approves Rituxan/MabThera for first-line maintenance use in follicular lymphoma
 Media Release Basel, 31 January 2011 FDA approves Rituxan/MabThera for first-line maintenance use in follicular lymphoma Approval provides option that improves the length of time people with incurable
Media Release Basel, 31 January 2011 FDA approves Rituxan/MabThera for first-line maintenance use in follicular lymphoma Approval provides option that improves the length of time people with incurable
J Clin Oncol 23:8447-8452. 2005 by American Society of Clinical Oncology INTRODUCTION
 VOLUME 23 NUMBER 33 NOVEMBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T New Treatment Options Have Changed the Survival of Patients With Follicular Lymphoma Richard I. Fisher, Michael
VOLUME 23 NUMBER 33 NOVEMBER 20 2005 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T New Treatment Options Have Changed the Survival of Patients With Follicular Lymphoma Richard I. Fisher, Michael
Mantle Cell Lymphoma and New Treatments on the Horizon
 MANTLE CELL LYMPHOMA Mantle Cell Lymphoma and New Treatments on the Horizon Presented by James Armitage, MD University of Nebraska Medical Center Pierluigi Porcu, MD The Ohio State University Comprehensive
MANTLE CELL LYMPHOMA Mantle Cell Lymphoma and New Treatments on the Horizon Presented by James Armitage, MD University of Nebraska Medical Center Pierluigi Porcu, MD The Ohio State University Comprehensive
Many people with non-hodgkin lymphoma have found an educational support group helpful. Support
 Track 2: Treatment Options [Narrator] Many people with non-hodgkin lymphoma have found an educational support group helpful. Support groups take many forms: some meet the needs of people with all kinds
Track 2: Treatment Options [Narrator] Many people with non-hodgkin lymphoma have found an educational support group helpful. Support groups take many forms: some meet the needs of people with all kinds
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
INITIAL EVALUATION PATHOLOGIC DIAGNOSIS ESSENTIAL:
 te: Consider Clinical Trials as treatment options for eligible patients. PATHOLOGIC DIAGNOSIS ESSENTIAL: Hematopathology review of all slides with at least one tumor paraffin block. Rebiopsy if consult
te: Consider Clinical Trials as treatment options for eligible patients. PATHOLOGIC DIAGNOSIS ESSENTIAL: Hematopathology review of all slides with at least one tumor paraffin block. Rebiopsy if consult
Treatment of low-grade non-hodgkin lymphoma
 Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
Produced 28.02.2011 Due for revision 28.02.2013 Treatment of low-grade non-hodgkin lymphoma Lymphomas are described as low grade if the cells appear to be dividing slowly. There are several kinds of low-grade
Non-Hodgkin s lymphomas (NHLs) are a
 Oncology 33 Non-Hodgkin s lymphoma in the elderly The incidence of non-hodgkin s lymphoma (NHL) is increasing, and this increase is even more rapid in the older population. Although treatment of NHL in
Oncology 33 Non-Hodgkin s lymphoma in the elderly The incidence of non-hodgkin s lymphoma (NHL) is increasing, and this increase is even more rapid in the older population. Although treatment of NHL in
CHRONIC LYMPHOCYTIC LEUKEMIA
 CHRONIC LYMPHOCYTIC LEUKEMIA Executive Summary Chronic lymphocytic leukemia (CLL) is the most common form of leukemia in the Western world, but is significantly less frequent in Asia. The median age of
CHRONIC LYMPHOCYTIC LEUKEMIA Executive Summary Chronic lymphocytic leukemia (CLL) is the most common form of leukemia in the Western world, but is significantly less frequent in Asia. The median age of
Anti-HCV therapy in HCV-related NHL
 Gabriele Pozzato M.D. University of Trieste Anti-HCV therapy in HCV-related NHL Questions about HCV+ in NHL Is the NHL related with HCV infection? Which is the best therapeutic strategy? Is the antiviral
Gabriele Pozzato M.D. University of Trieste Anti-HCV therapy in HCV-related NHL Questions about HCV+ in NHL Is the NHL related with HCV infection? Which is the best therapeutic strategy? Is the antiviral
Update in Hematology Oncology Targeted Therapies. Mark Holguin
 Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Shaji Kumar, M.D. Multiple Myeloma: Multiple myeloma (MM) is the second most common hematological
 An update on the management of multiple myeloma and amyloidosis Shaji Kumar, M.D. Multiple Myeloma: Multiple myeloma (MM) is the second most common hematological malignancy in this country affecting nearly
An update on the management of multiple myeloma and amyloidosis Shaji Kumar, M.D. Multiple Myeloma: Multiple myeloma (MM) is the second most common hematological malignancy in this country affecting nearly
Two Retroperitoneal Low-Grade B-Cell Lymphoma Successfully Treated With a Combination of Chimeric Anti-CD20 Monoclonal Antibody and CHOP Chemotherapy
 Two Retroperitoneal Low-Grade B-Cell Lymphoma Successfully Treated With a Combination of Chimeric Anti-CD20 Monoclonal Antibody and CHOP Chemotherapy Yoichi Kitamura, MD Kazuhiko Hayashi, MD Kazumi Uchida,
Two Retroperitoneal Low-Grade B-Cell Lymphoma Successfully Treated With a Combination of Chimeric Anti-CD20 Monoclonal Antibody and CHOP Chemotherapy Yoichi Kitamura, MD Kazuhiko Hayashi, MD Kazumi Uchida,
Bendamustine for the fourth-line treatment of multiple myeloma
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for the fourth-line treatment of multiple myeloma Contents Summary 1 Background 2 Epidemiology 3 Cost 6 References 7 Summary There is no standard
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for the fourth-line treatment of multiple myeloma Contents Summary 1 Background 2 Epidemiology 3 Cost 6 References 7 Summary There is no standard
Mantle Cell Lymphoma Understanding Your Treatment Options
 WELCOME AND INTRODUCTIONS Operator Greetings and welcome to the Mantle Cell Lymphoma (MCL), Understanding Your Treatment Options telephone and Web education program. It is now my pleasure to introduce
WELCOME AND INTRODUCTIONS Operator Greetings and welcome to the Mantle Cell Lymphoma (MCL), Understanding Your Treatment Options telephone and Web education program. It is now my pleasure to introduce
Management of low grade glioma s: update on recent trials
 Management of low grade glioma s: update on recent trials M.J. van den Bent The Brain Tumor Center at Erasmus MC Cancer Center Rotterdam, the Netherlands Low grades Female, born 1976 1 st seizure 2005,
Management of low grade glioma s: update on recent trials M.J. van den Bent The Brain Tumor Center at Erasmus MC Cancer Center Rotterdam, the Netherlands Low grades Female, born 1976 1 st seizure 2005,
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on
 A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
STEM CELL TRANSPLANTATION IN MULTIPLE MYELOMA
 STEM CELL TRANSPLANTATION IN MULTIPLE MYELOMA Sundar Jagannath MD Professor of Medicine St. Vincent s Comprehensive Cancer Center New York, NY Where is transplant today in the management of Myeloma? Autologous
STEM CELL TRANSPLANTATION IN MULTIPLE MYELOMA Sundar Jagannath MD Professor of Medicine St. Vincent s Comprehensive Cancer Center New York, NY Where is transplant today in the management of Myeloma? Autologous
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA PROGNOSIS IN ACUTE MYELOID LEUKEMIA
 PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA UNFAVORABLE Advanced age High leukocyte count at diagnosis Presence of myeloid antigens Late achievement of CR Chromosomal abnormalities: t(9:22)(q34:q11) t(4;11)(q21;q23)
PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA UNFAVORABLE Advanced age High leukocyte count at diagnosis Presence of myeloid antigens Late achievement of CR Chromosomal abnormalities: t(9:22)(q34:q11) t(4;11)(q21;q23)
Cure versus control: Which is the best strategy?
 Cure versus control: Which is the best strategy? Barcelona 8-9-2012 Mario Boccadoro DIVISIONE UNIVERSITARIA DI EMATOLOGIA AZIENDA OSPEDALIERA SAN GIOVANNI TORINO, ITALY MULTIPLE MYELOMA Cure versus control
Cure versus control: Which is the best strategy? Barcelona 8-9-2012 Mario Boccadoro DIVISIONE UNIVERSITARIA DI EMATOLOGIA AZIENDA OSPEDALIERA SAN GIOVANNI TORINO, ITALY MULTIPLE MYELOMA Cure versus control
National Pharmaceutical Pricing Authority 3 rd Floor, YMCA Cultural Centre 1 Jai Singh Road New Delhi 110001 File No. 23(01)2014/Div.
 Dated 21 st November 2014 NPPA Invites Comments of Pharmaceutical Industry & Trade, Consumer Organisations, Public Health Experts and other Stakeholders on the Recommendations of Tata Memorial Centre under
Dated 21 st November 2014 NPPA Invites Comments of Pharmaceutical Industry & Trade, Consumer Organisations, Public Health Experts and other Stakeholders on the Recommendations of Tata Memorial Centre under
Rituximab in the Management of Follicular Lymphoma
 Hong Kong J Radiol. 2011;14(Suppl):S63-7 REVIEW ARTICLE Rituximab in the Management of Follicular Lymphoma YL Kwong Department of Medicine, Professorial Block, Queen Mary Hospital, Pokfulam Road, Hong
Hong Kong J Radiol. 2011;14(Suppl):S63-7 REVIEW ARTICLE Rituximab in the Management of Follicular Lymphoma YL Kwong Department of Medicine, Professorial Block, Queen Mary Hospital, Pokfulam Road, Hong
NATIONAL CANCER DRUG FUND PRIORITISATION SCORES
 NATIONAL CANCER DRUG FUND PRIORITISATION SCORES Drug Indication Regimen (where appropriate) BORTEZOMIB In combination with dexamethasone (VD), or with dexamethasone and thalidomide (VTD), is indicated
NATIONAL CANCER DRUG FUND PRIORITISATION SCORES Drug Indication Regimen (where appropriate) BORTEZOMIB In combination with dexamethasone (VD), or with dexamethasone and thalidomide (VTD), is indicated
Chemotherapy or Not? Anthracycline or Not? Taxane or Not? Does Density Matter? Chemotherapy in Luminal Breast Cancer: Choice of Regimen.
 Chemotherapy in Luminal Breast Cancer: Choice of Regimen Andrew D. Seidman, MD Attending Physician Breast Cancer Medicine Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Cornell
Chemotherapy in Luminal Breast Cancer: Choice of Regimen Andrew D. Seidman, MD Attending Physician Breast Cancer Medicine Service Memorial Sloan Kettering Cancer Center Professor of Medicine Weill Cornell
Multiple Myeloma (Event Driven)
 Brochure More information from http://www.researchandmarkets.com/reports/2234830/ Multiple Myeloma (Event Driven) Description: The 2010 multiple myeloma (myeloma) market garnered impressive sales despite
Brochure More information from http://www.researchandmarkets.com/reports/2234830/ Multiple Myeloma (Event Driven) Description: The 2010 multiple myeloma (myeloma) market garnered impressive sales despite
DECISION AND SUMMARY OF RATIONALE
 DECISION AND SUMMARY OF RATIONALE Indication under consideration Clinical evidence Clofarabine in the treatment of relapsed acute myeloid leukaemia (AML) The application was for clofarabine to remain in
DECISION AND SUMMARY OF RATIONALE Indication under consideration Clinical evidence Clofarabine in the treatment of relapsed acute myeloid leukaemia (AML) The application was for clofarabine to remain in
PERSPECTIVES ON THE TREATMENT OF MANTLE CELL LYMPHOMA AND FOLLICULAR LYMPHOMA IN 2015 AND BEYOND
 PERSPECTIVES ON THE TREATMENT OF MANTLE CELL LYMPHOMA AND FOLLICULAR LYMPHOMA IN 2015 AND BEYOND Summary of presentations from the Celgene satellite symposium, held at the 20 th Congress of the European
PERSPECTIVES ON THE TREATMENT OF MANTLE CELL LYMPHOMA AND FOLLICULAR LYMPHOMA IN 2015 AND BEYOND Summary of presentations from the Celgene satellite symposium, held at the 20 th Congress of the European
Hematopoietic Stem Cell Transplantation. Imad A. Tabbara, M.D. Professor of Medicine
 Hematopoietic Stem Cell Transplantation Imad A. Tabbara, M.D. Professor of Medicine Hematopoietic Stem Cells Harvested from blood, bone marrow, umbilical cord blood Positive selection of CD34 (+) cells
Hematopoietic Stem Cell Transplantation Imad A. Tabbara, M.D. Professor of Medicine Hematopoietic Stem Cells Harvested from blood, bone marrow, umbilical cord blood Positive selection of CD34 (+) cells
Interesting Case Series. Periorbital Richter Syndrome
 Interesting Case Series Periorbital Richter Syndrome MarkGorman,MRCS,MSc, a Julia Ruston, MRCS, b and Sarath Vennam, BMBS a a Division of Plastic Surgery, Royal Devon and Exeter Hospital, Exeter, Devon,
Interesting Case Series Periorbital Richter Syndrome MarkGorman,MRCS,MSc, a Julia Ruston, MRCS, b and Sarath Vennam, BMBS a a Division of Plastic Surgery, Royal Devon and Exeter Hospital, Exeter, Devon,
Rituximab in Non - Hodgkins Lymphoma. Fatima Bassa, Dept. of Haematology October 2008
 Rituximab in Non - Hodgkins Lymphoma Fatima Bassa, Dept. of Haematology October 2008 World Health Organization lymphoma classification (2001) Peripheral B-cell neoplasms: B-chronic lymphocytic leukemia/small
Rituximab in Non - Hodgkins Lymphoma Fatima Bassa, Dept. of Haematology October 2008 World Health Organization lymphoma classification (2001) Peripheral B-cell neoplasms: B-chronic lymphocytic leukemia/small
David Loew, LCL MabThera
 MabThera The star continues to rise David Loew, LCL MabThera MabThera the star continues to raise Group sales (CHF bn) 4,5 4,0 3,5 3,0 2,5 2,0 1,5 1,0 0,5 0,0 2001 2002 2003 2004 2005 Outstanding clinical
MabThera The star continues to rise David Loew, LCL MabThera MabThera the star continues to raise Group sales (CHF bn) 4,5 4,0 3,5 3,0 2,5 2,0 1,5 1,0 0,5 0,0 2001 2002 2003 2004 2005 Outstanding clinical
-Examination of key pipeline candidates with in-depth clinical and commercial profiles of Phase III candidates
 Brochure More information from http://www.researchandmarkets.com/reports/1215469/ Pipeline Insight: Lymphomas, Multiple Myeloma & Myelodysplastic Syndromes - Optimization of clinical practice creates opportunities
Brochure More information from http://www.researchandmarkets.com/reports/1215469/ Pipeline Insight: Lymphomas, Multiple Myeloma & Myelodysplastic Syndromes - Optimization of clinical practice creates opportunities
MEDICAL COVERAGE POLICY
 Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms of your particular benefit plan. Each
Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms of your particular benefit plan. Each
Chronic Lymphocytic Leukemia. Case Study. AAIM Triennial October 2012 Susan Sokoloski, M.D.
 Chronic Lymphocytic Leukemia AAIM Triennial October 2012 Susan Sokoloski, M.D. Case Study 57 year old male, trial application for $1,000,000 Universal Life coverage Cover letter from sales agent indicates
Chronic Lymphocytic Leukemia AAIM Triennial October 2012 Susan Sokoloski, M.D. Case Study 57 year old male, trial application for $1,000,000 Universal Life coverage Cover letter from sales agent indicates
Effective for dates of service on or after September 1, 2015, refer to: https://www.bcbsal.org/providers/drugpolicies/index.cfm
 Effective for dates of service on or after September 1, 2015, refer to: https://www.bcbsal.org/providers/drugpolicies/index.cfm Name of Policy: Uses of Monoclonal Antibodies for the Treatment of Non-Hodgkin
Effective for dates of service on or after September 1, 2015, refer to: https://www.bcbsal.org/providers/drugpolicies/index.cfm Name of Policy: Uses of Monoclonal Antibodies for the Treatment of Non-Hodgkin
Radioimmunotherapy in the Treatment of Non-Hodgkin Lymphoma. Original Policy Date
 MP 8.01.28 Radioimmunotherapy in the Treatment of Non-Hodgkin Lymphoma Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
MP 8.01.28 Radioimmunotherapy in the Treatment of Non-Hodgkin Lymphoma Medical Policy Section Therapy Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013
In the last decade, passive immunotherapy
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Immunotherapy with Rituximab in Follicular Lymphomas Carmen SAGUNA, MD a ; Ileana Delia MUT, MD, PhD a ; Anca Roxana LUPU, MD, PhD a ; Mihaela TEVET,
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Immunotherapy with Rituximab in Follicular Lymphomas Carmen SAGUNA, MD a ; Ileana Delia MUT, MD, PhD a ; Anca Roxana LUPU, MD, PhD a ; Mihaela TEVET,
Treatment results with Bortezomib in multiple myeloma
 Treatment results with Bortezomib in multiple myeloma Prof. Dr. Orhan Sezer Hamburg University Medical Center Circulating proteasome levels are an independent prognostic factor in MM 1.0 Probability of
Treatment results with Bortezomib in multiple myeloma Prof. Dr. Orhan Sezer Hamburg University Medical Center Circulating proteasome levels are an independent prognostic factor in MM 1.0 Probability of
Chemoimmunotherapy resistant follicular lymphoma A single institutional study
 Cancer Research Journal 2014; 2(5): 93-97 Published online September 30, 2014 (http://www.sciencepublishinggroup.com/j/crj) doi: 10.11648/j.crj.20140205.13 ISSN: 2330-8192 (Print); ISSN: 2330-8214 (Online)
Cancer Research Journal 2014; 2(5): 93-97 Published online September 30, 2014 (http://www.sciencepublishinggroup.com/j/crj) doi: 10.11648/j.crj.20140205.13 ISSN: 2330-8192 (Print); ISSN: 2330-8214 (Online)
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Pro Cure in Multiple Myeloma. Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany
 Pro Cure in Multiple Myeloma Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany Pro Cure in Multiple Myeloma Several hematological malignancies can be cured
Pro Cure in Multiple Myeloma Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany Pro Cure in Multiple Myeloma Several hematological malignancies can be cured
Follicular lymphoma. What is follicular lymphoma? Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.
 Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk is a cancer of the lymphatic system, a type of non-hodgkin lymphoma. Even though more than 12,000 people are diagnosed
Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk is a cancer of the lymphatic system, a type of non-hodgkin lymphoma. Even though more than 12,000 people are diagnosed
The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma
 The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma 11 th Annual National Leadership Summit on Health Disparities Innovation Towards Reducing Disparities Congressional Black
The Blood Cancer Twice As Likely To Affect African Americans: Multiple Myeloma 11 th Annual National Leadership Summit on Health Disparities Innovation Towards Reducing Disparities Congressional Black
Lymphomas after organ transplantation
 Produced 21.03.2011 Revision due 21.03.2011 Lymphomas after organ transplantation People who have undergone an organ transplant are more at risk of developing lymphoma known as post-transplant lymphoproliferative
Produced 21.03.2011 Revision due 21.03.2011 Lymphomas after organ transplantation People who have undergone an organ transplant are more at risk of developing lymphoma known as post-transplant lymphoproliferative
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Characteristics and Prognosis of Patients with Richter s Transformation of Chronic Lymphocytic Leukemia: Experience with FDG/PET
 Characteristics and Prognosis of Patients with Richter s Transformation of Chronic Lymphocytic Leukemia: Experience with FDG/PET Lorenzo Falchi, Long Trinh, Edith M Marom, Mylene Truong, Ellen J Schlette,
Characteristics and Prognosis of Patients with Richter s Transformation of Chronic Lymphocytic Leukemia: Experience with FDG/PET Lorenzo Falchi, Long Trinh, Edith M Marom, Mylene Truong, Ellen J Schlette,
Bone Marrow Evaluation for Lymphoma. Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital
 Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
1. Introduction. 2. Clinical aspects
 1. Introduction MabThera (rituximab) is a genetically engineered chimeric mouse/human monoclonal antibody which binds specifically to the transmembrane antigen, CD20. This antigen is located on pre-b-
1. Introduction MabThera (rituximab) is a genetically engineered chimeric mouse/human monoclonal antibody which binds specifically to the transmembrane antigen, CD20. This antigen is located on pre-b-
Non-Hodgkin Lymphoma Richard Orlowski, MD
 Non-Hodgkin Lymphoma Richard Orlowski, MD The American Cancer Society (ACS) estimates that 69,740 Americans will be diagnosed with non-hodgkin lymphoma (NHL) in 2013. Excluding non-melanoma skin cancers,
Non-Hodgkin Lymphoma Richard Orlowski, MD The American Cancer Society (ACS) estimates that 69,740 Americans will be diagnosed with non-hodgkin lymphoma (NHL) in 2013. Excluding non-melanoma skin cancers,
Future strategies for myeloma: An overview of novel treatments In development
 Future strategies for myeloma: An overview of novel treatments In development Dr. Matthew Streetly Guys and St. Thomas NHS Trust How far have we come? Melphalan and prednisolone VAD Autologous SCT Thalidomide
Future strategies for myeloma: An overview of novel treatments In development Dr. Matthew Streetly Guys and St. Thomas NHS Trust How far have we come? Melphalan and prednisolone VAD Autologous SCT Thalidomide
Long Term Low Dose Maintenance Chemotherapy in the Treatment of Acute Myeloid Leukemia
 Long Term Low Dose Chemotherapy in the Treatment of Acute Myeloid Leukemia Murat TOMBULO LU*, Seçkin ÇA IRGAN* * Department of Hematology, Faculty of Medicine, Ege University, zmir, TURKEY ABSTRACT In
Long Term Low Dose Chemotherapy in the Treatment of Acute Myeloid Leukemia Murat TOMBULO LU*, Seçkin ÇA IRGAN* * Department of Hematology, Faculty of Medicine, Ege University, zmir, TURKEY ABSTRACT In
Indolent Lymphomas. American Academy of Insurance Medicine 121 st Annual Meeting. Hilton LaJolla October 2012
 Indolent Lymphomas American Academy of Insurance Medicine 121 st Annual Meeting Hilton LaJolla October 2012 Scottsdale, Arizona Rochester, Minnesota Jacksonville, Florida Joseph Mikhael, MD, MEd, FRCPC,
Indolent Lymphomas American Academy of Insurance Medicine 121 st Annual Meeting Hilton LaJolla October 2012 Scottsdale, Arizona Rochester, Minnesota Jacksonville, Florida Joseph Mikhael, MD, MEd, FRCPC,
FOLLICULAR LYMPHOMA. Executive Summary
 FOLLICULAR LYMPHOMA Executive Summary Follicular lymphoma (FL) is the most common indolent lymphoma and the second most common non-hodgkin lymphoma accounting for about 10-20% of all lymphomas in Western
FOLLICULAR LYMPHOMA Executive Summary Follicular lymphoma (FL) is the most common indolent lymphoma and the second most common non-hodgkin lymphoma accounting for about 10-20% of all lymphomas in Western
Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
 Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
DIFFUSE LARGE B-CELL LYMPHOMA
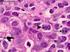 DIFFUSE LARGE B-CELL LYMPHOMA Executive Summary Diffuse large B-cell lymphoma (DLBCL) is the most common subtype of non-hodgkin lymphoma (NHL), constituting up to 40% of all cases globally.[1] This subtype
DIFFUSE LARGE B-CELL LYMPHOMA Executive Summary Diffuse large B-cell lymphoma (DLBCL) is the most common subtype of non-hodgkin lymphoma (NHL), constituting up to 40% of all cases globally.[1] This subtype
Why discuss CLL? Common: 40% of US leukaemia. approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time
 Why discuss CLL? Common: 40% of US leukaemia approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time Median age of dx is 65 (30s. Incurable, survival 2-202 20 years Require ongoing supportive care
Why discuss CLL? Common: 40% of US leukaemia approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time Median age of dx is 65 (30s. Incurable, survival 2-202 20 years Require ongoing supportive care
Hodgkin and Non-Hodgkin Lymphoma Pre-HCT Data
 (Form 2018) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Hodgkin and Non-Hodgkin Lymphoma Pre-HCT Data Form. E-mail comments regarding the content
(Form 2018) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Hodgkin and Non-Hodgkin Lymphoma Pre-HCT Data Form. E-mail comments regarding the content
CLL: Disease Course, Treatment, Diagnosis, and Biomarkers
 CLL: Disease Course, Treatment, Diagnosis, and Biomarkers Amy E. Hanlon Newell, Ph.D. Manager, Scientific Affairs Abbott Molecular Overview: Today s Take-away Understanding of: Cell phenotype and clinical
CLL: Disease Course, Treatment, Diagnosis, and Biomarkers Amy E. Hanlon Newell, Ph.D. Manager, Scientific Affairs Abbott Molecular Overview: Today s Take-away Understanding of: Cell phenotype and clinical
Background Information Myeloma
 Myeloma FAST FACTS Myeloma, also known as multiple myeloma, is a type of cancer that develops from plasma cells which originate in the bone marrow 1 Myeloma is the second most common type of blood cancer
Myeloma FAST FACTS Myeloma, also known as multiple myeloma, is a type of cancer that develops from plasma cells which originate in the bone marrow 1 Myeloma is the second most common type of blood cancer
Rituximab for the first-line maintenance treatment of follicular non-hodgkin s lymphoma
 Issue date: June 2011 Rituximab for the first-line maintenance treatment of follicular non-hodgkin s lymphoma This guidance was developed using the the single technology appraisal process NICE technology
Issue date: June 2011 Rituximab for the first-line maintenance treatment of follicular non-hodgkin s lymphoma This guidance was developed using the the single technology appraisal process NICE technology
Summary & Conclusion
 The prognostic value of angiogenesis markers in patients with non-hodgkin lymphoma. Summary & Conclusion The current study aims to asses the prognostic value of some angiogenesis markers in patients with
The prognostic value of angiogenesis markers in patients with non-hodgkin lymphoma. Summary & Conclusion The current study aims to asses the prognostic value of some angiogenesis markers in patients with
Avastin in Metastatic Breast Cancer
 Non-interventional study Avastin in Metastatic Breast Cancer ML 21165 / 2007 Clinical Study Report Synopsis ROCHE ML21165 / WiSP Project RH09 / V. 1.0 / 24.06.2013 ROCHE ML21165-2 - Name of Sponsor Roche
Non-interventional study Avastin in Metastatic Breast Cancer ML 21165 / 2007 Clinical Study Report Synopsis ROCHE ML21165 / WiSP Project RH09 / V. 1.0 / 24.06.2013 ROCHE ML21165-2 - Name of Sponsor Roche
What is a Stem Cell Transplantation?
 What is a Stem Cell Transplantation? Guest Expert: Stuart, MD Associate Professor, Medical Oncology www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with Drs. Ed and Ken. I am
What is a Stem Cell Transplantation? Guest Expert: Stuart, MD Associate Professor, Medical Oncology www.wnpr.org www.yalecancercenter.org Welcome to Yale Cancer Center Answers with Drs. Ed and Ken. I am
Interesting Case Review. Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA
 Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
ICML CLL: Therapie des Rezidivs
 ICML CLL: Therapie des Rezidivs Thomas Elter Universitätsklinikum Köln Deutsche CLL Studiengruppe 14.09.2013 Hamburg LUGANO: WAS GIBT ES ZUR CLL IN DER 2. LINIE? Publikationen zur CLL insgesamt: 55 Diagnostik
ICML CLL: Therapie des Rezidivs Thomas Elter Universitätsklinikum Köln Deutsche CLL Studiengruppe 14.09.2013 Hamburg LUGANO: WAS GIBT ES ZUR CLL IN DER 2. LINIE? Publikationen zur CLL insgesamt: 55 Diagnostik
